Professional Documents
Culture Documents
Obstetrics - Antepartum Hemorrhage
Uploaded by
Jonathan0 ratings0% found this document useful (0 votes)
61 views4 pagesObstetrical hemorrhage can occur during pregnancy or postpartum and has several potential causes. Two important causes of antepartum hemorrhage are abruptio placentae and placenta previa. Abruptio placentae is the premature separation of the normally implanted placenta, which can be partial or total. It occurs in around 1 in 200 deliveries and carries risks of perinatal mortality up to 25% and long-term neurologic sequelae in 15% of surviving infants. Clinical diagnosis is based on signs of vaginal bleeding, uterine tenderness, back pain, fetal distress, or preterm labor.
Original Description:
Obstetrics - Antepartum Hemorrhage
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentObstetrical hemorrhage can occur during pregnancy or postpartum and has several potential causes. Two important causes of antepartum hemorrhage are abruptio placentae and placenta previa. Abruptio placentae is the premature separation of the normally implanted placenta, which can be partial or total. It occurs in around 1 in 200 deliveries and carries risks of perinatal mortality up to 25% and long-term neurologic sequelae in 15% of surviving infants. Clinical diagnosis is based on signs of vaginal bleeding, uterine tenderness, back pain, fetal distress, or preterm labor.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
61 views4 pagesObstetrics - Antepartum Hemorrhage
Uploaded by
JonathanObstetrical hemorrhage can occur during pregnancy or postpartum and has several potential causes. Two important causes of antepartum hemorrhage are abruptio placentae and placenta previa. Abruptio placentae is the premature separation of the normally implanted placenta, which can be partial or total. It occurs in around 1 in 200 deliveries and carries risks of perinatal mortality up to 25% and long-term neurologic sequelae in 15% of surviving infants. Clinical diagnosis is based on signs of vaginal bleeding, uterine tenderness, back pain, fetal distress, or preterm labor.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 4
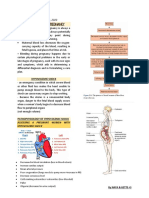
OBSTETRICAL HEMORRAGE
AIDA V. SAN JOSE, MD
2. ABRUPTIO PLACENTA
Causes of obstetrical hemorrhage Separation of the placenta located elsewhere (normally
Happening in the first half of pregnancy and those occurring implanted) in the uterine cavity
in the second half of pregnancy. For the causes of bleeding The normal implantation of the placenta is where? Upper
for the first half of pregnancy: fundal (antero fundal, sabi ni dra)
Abortion, ectopic pregnancy, gestational trophoblastic… and Severe abruption placenta = >50% separation of the
of course the two important causes of Antepartum placenta
hemorrhage we have abruptio placenta and placenta previa,
we also include vasa previa, and these are the cause of 3. VASA PREVIA
bleeding for the first half. Velamentous insertion of the umbilical cord with rupture
of a fetal vessel at the time of rupture of the membranes
Antepartum Hemorrhage (2nd half of pregnancy) resulting to fetal hemorrhage
Placental abruption Somewhat rare; fatal
Placenta previa
Vasa previa cause these three entities cause more bleeding ABRUPTIO PLACENTA
late in to the 2nd trimester or in to the early trimester DEFINITION:
o “Ablation” - separation
Postpartum Hemorrhage o The premature separation of the normally implanted
Uterine atony (most common) placenta (at upper uterine segment)
Hemorrhage from retained placental fragments o Other terms are: ABLATIO PLACENTA or rendering
Placenta accreta, increta, and percreta asunder biglang nag seseparateang placenta
Inversion of the uterus o Accidental hemorrhage
o Maybe total or partial
Genital tract laceration
o Total – entire placenta has separated, most severe type,
Puerperal hematomas
accompanied by fetal death
Rupture of the uterus o Partial – can cause death sometimes
Rupture of the scarred uterus FREQUENCY: 1 in 200 deliveries
INTENSITY: depends on the promptness in consultation and
OBSTETRICAL HEMORRHAGE management
Obstetrical hemorrhage, along with hypertension and
PERINATAL MORBIDITY AND MORTALITY:
infection, is one of the infamous “triad” of causes of maternal
o Perinatal mortality: 25% (119/1000)
deaths
o Stillbirths- 10-12%
The single most important cause of maternal death; half of all o With fetal survival, there may be adverse sequelae
postpartum death significant neurologic sequelae within the first year of
Acceptable obstetric care requires facilities that allow prompt life (15%)
administration of blood
Coombs et al. 1991 defined hemorrhage as postpartum drop
of 10 volume percent or by a need for transfusion ->
incidence was 3.9%
CAUSES OF PREGNANCY- RELATED DEATHS DUE TO
HEMORRHAGE
CAUSE OF PERCENTAGE (%)
HEMORRHAGE
Uterine atony 19%
Placental abruption 17%
DIC 16%
Laceration 14%
Placenta accreta/ 12%
increta/percreta
(3rd stage hemorrhage)
Uterine placental bleeding 6%
Placenta previa 7% Chronic Hypertension – MOST COMMON
Retained placenta 4% Multifetal Gestation –d/t very large placenta, delivery of the 1st
of twin
ANTEPARTUM HEMORRHAGE Prior abruption - possibility of recurrent, problem with this is
1. PLACENTA PREVIA the timing of delivery or onset of abruption. Difficult to tell and
Separation of the placenta which is implanted in the manage. 40 years or more are more prone to develop abruption
immediate vicinity of the cervical canal Increased age and parity (Elderly primigravida)- 1st time
Refers to implantation of the placenta of the lower pregnancy of a >35 y.o. woman; Best age to get pregnant: 20
uterine segment either totally or partially covering the to 25 years old
internal os Uterine leiomyoma- Placenta implanted over a submucous type
of leiomyoma
1|O B S T E T R I C S , 2 0 1 4
Trans by: Macasaet, T. Edited By CK Lorenzo, Kaisoo, Dedeem, Grallohnll
RECURRENCE: ABRUPTIO PLACENTA CLINICAL DIAGNOSIS:
The risk is high in subsequent pregnancies SIGNS AND SYMPTOMS:
Management is difficult Vaginal bleeding
o Most prominent manifestation
PATHOLOGY: o Profuse external
Initiated by hemorrhage into the decidua basalis which then o Scanty external bleeding
splits and leaves a thin layer adherent to the myometrium o Characteristic of blood is said to be dark appearance
The earliest stage is the development of a decidual hematoma which can be clotted blood or dark black as compared
separation of the basal portion compression to placenta previa wherein the bleeding is red and fresh
destruction of adjacent placenta Uterine tenderness, back pain
There maybe no clinical symptoms in the early stages Frequent uterine contraction or persistent uterine hypertonous
A circumscribed area of depression on examination – (tetanic uterine contraction without adequate time for uterine
location where hematoma was used to be relaxation)
confirm the dx of abruption P = Blod clot = will create Fetal distress esp. if there is a complete separation of
depression on maternal surface of the placenta placenta
Idiopathic preterm labor
ABRUPTIO PLACENTA TYPES: Dead fetus after complete separation
1. EXTERNAL HEMORRHAGE o We call these uterine tenderness, back pain, abdominal
Bleeding that insinuates between the membranes and pain = painful bleeding, where as in previa is generally
uterus and escapes through the cervix as painless hge.
o Px complaint of vaginal bleeding
2. CONCEALED HEMORRHAGE (MORE DANGEROUS) Signs and symptoms Frequency (%)
Blood that does not escape externally but is retained Vaginal bleeding 78
between the detached placenta and uterus Uterine tenderness 66
Carries a greater maternal danger due to: Fetal distress 60
o Extent of bleeding cannot be appreciated Preterm labor 22
o Risks of consumptive coagulopathy or DIC High- frequency 17
Could lead to shock; previous description of contraction
this type is “shock out of proportion to Hypertonus 17
amount of bleeding” Dead fetus 15
From Hurd and associates (1983)
CONCEALED/RETAINED HEMORRHAGE
1. Blood effused behind the placenta but its margins are still ULTRASOUND:
adherent Highly dx of placenta previa
2. Placenta is completely separated but the membranes remain
If findings (-) previa, or if placenta is N located then
adherent to the uterine wall
probably it is abruption P
3. Blood enters the amniotic cavity after breaking through
Negative findings DO NOT exclude placental abruption; 24%
membranes –most acceptable reason
sensitivity
4. A closely related applied fetal head in the lower uterine
In most cases, diagnosis is based on clinical grounds
segment so that blood is prevented from escaping. Usually
though the membrane are gradually detached from the uterine Usually requested right away, and usually abdominal UZ, but
wall and blood eventually escapes – not credible the abdominal UZ will not give us an accurate dx of
abruption placenta. It cannot determine the presence of clot
CHRONIC PLACENTAL ABRUPTION of the maternal surface of the placenta because the clot
brought about by the abruption and cotyledons can have the
Occurs in a few cases in which hemorrhage with
same echogenicity on UZ. So it is not recognized by UZ often
retroplacental hematoma is formed and is arrested completely
times, unless there is a big clot. Diagnosis is usually made on
without delivery; CAOS (chronic abruption oligohydramnios
clinical grounds but UZ is usually requested to rule out the
sequence): > MSAF (elevated)
possibility of placenta previa. Internal examination is not
Incidence rate is low
performed because it can cause torrential hge. If you already
ruled out placenta previa you can now perform I.E to
FETAL TO MATERNAL HEMORRHAGE
determine if px. Is in labor, often times abruption is
Blood in the retroplacental hematoma is almost always accompanied by labor, uterine contraction, hypertonous.
maternal but sometimes it can be fetal
Non-traumatic PA – evidence of feto-maternal hge in 20% SHOCK
(<10ml) – more on maternal origin May be due to massive or torrential hge; can develop with
Traumatic PA- significant fetal bleeding, more on fetal in concealed abruption
origin Prompt treatment of hypotension of crystalloid and blood
infusion to restore vital signs and reverse oliguria
Can cause renal failure requiring dialysis
AKI can lead to tubular necrosis
2|O B S T E T R I C S , 2 0 1 4
Trans by: Macasaet, T. Edited By CK Lorenzo, Kaisoo, Dedeem, Grallohnll
CONSUMPTIVE COAGULOPATHY TOCOLYSIS
Defibrination syndrome or DIC: 30% of cases of severe o Clinically evident placental abruption is
abruption with fetal death will have overt contraindication to tocolytic therapy except in selected
hypofibrinogenemia (<150 mg/dl of plasma) along with cases of extreme prematurity in which the separation is
elevated levels of fibrinogen- fibrin degradation products, d- minor and maternal hemodynamic status is stable-
dimer, and variable decreases in other coagulation factors- ACOG 1993
despite increase in levels, they will NOT be able to
compensate for the hypofibrogenemia AMNIOTOMY
Major mechanism: intravascular and retroplacental induction o Early amniotomy was advocated because the escape of
of coagulopathy amniotic fluid might:
Important consequence of intravascular coagulation: Decrease bleeding from the implantation site
activation of plasminogen to plasmin lysis of fibrin Reduce the entry into the maternal circulation of
microemboli maintenance of microcirculation patency thromboplastin and perhaps activated coagulation
Pathologic levels- >100ug/ml of fibrinogen-fibrin factors from the retroplacental clot – more
degradation products in maternal serum- not clinically useful important function
ACUTE KIDNEY INJURY VAGINAL DELIVERY
Renal dysfunction that develops in severe forms of abruption o The preferred route if the fetus is already dead unless
especially when hypovolemia is not promptly corrected- in ¾ the hemorrhage is brisk and there are other obstetrical
of cases, reversible acute tubular necrosis accounts for the complication precluding vaginal delivery
Renal Failure o Course of labor is shorter in cases of placenta previa
Major factors in its development
o Impaired renal perfusion- massive bleeding reduces CEASAREAN SECTION
cardiac output o Often management of abruption placenta
o Coexisting hypertensive disordered can cause renal o Done to deliver the live distress fetus rapidly
vasospam o If fetus is alive but CS is not carried out there must be
Prompt and vigorous treatment of hemorrhage with blood and continuous fetal monitoring and delivered once signs of
electrolyte solution will often prevent significant renal distress manifest
dysfunction o Serious coagulation defect may prove difficult during
CS
UTEROPLACENTAL APOPLEXY (COUVELAIRE The longer the interval between admission and
UTERUS) delivery, the higher the mortality
In severe form of abruption placenta
Widespread extravasation of blood into the uterine PLACENTA PREVIA
musculature and beneath the uterine serosa, tubal serosa, Implantation of the placenta on the lower uterine segment
between the leaves of the broad ligament, ovarian substance, The degree depends on the cervical dilatation
peritoneal cavity Cervical examination to determine dilatation can incite
Demonstrated conclusively at laparotomy torrential hemorrhage and is therefore not usually carried out
Seldom interfere with uterine contraction and is not an unless there is a “double set up”
indication for hysterectomy o The patient and facility is ready for either CS or
o Color of the uterus is similar to that of an eggplant due vaginal delivery
to extravasation of blood to the serosa o Rarely done d/t presence of UZ
o Apoplexy- it means stroke IE: no low lying uterine segment abruptio placenta
vaginal delivery
CAUSES OF FETAL DISTRESS IE: with low lying uterine segment placenta previa
Placental separation prompt delivery cesarean section
Maternal hemorrhage vigorous transfusion and prompt Placenta previa usually does not become symptomatic until
deliver the late second or early third trimester when bleeding ensues
Fetal hemorrhage immediate delivery and fetal transfusion which is classically but not always painless
Uterine hypertonus prompt delivery
PLACENTA PREVIA DEGREE
MANAGEMENT: TOTALIS- internal OS is completely covered by placenta
Varies depending on fetomaternal status and AOG PARTIALIS- internal OS is partially covered by placenta
Massive bleeding intensive blood replacement and prompt MARGINALIS- edge of placenta is at the margin of the
delivery internal OS - fall under the low lying
With lesser and slower blood loss, mgt. is influenced by fetal LOW-LYING- placenta is implanted in the lower uterine
status, live uncompromised fetus (esp. if immature), no segment such that the placental edge does not reach the os but
serious maternal hypovolemia or anemia close watch, is in close proximity to it
immediate intervention if condition deteriorates (immediate
cesarean section)
3|O B S T E T R I C S , 2 0 1 4
Trans by: Macasaet, T. Edited By CK Lorenzo, Kaisoo, Dedeem, Grallohnll
ETIOLOGY:
1. Multiparity – 5 or more DIAGNOSIS:
2. Advancing age – age 40 and up or age 35 elderly An I.E is not done because of risk of torrential hemorrhage
primigravida unless there are provision for immediate CS (double set-up)
3. Prior CS or induced abortion and delivery is planned
4. Inflammatory or atrophic changes Localization by SONOGRAPHY: simplest, most precise
5. Smoking (90%) and safest method of placental localization
6. Cocaine use Magnetic resonance imaging: unlikely to replace ultrasound
7. Large placentas- erythroblastosis. Twin etc in placental localization
8. Association- accreta, increta, percreta poorly
developed decidua in the lower uterine segment MANAGEMENT:
FOUR CONDITIONS IN PREVIA
CLINICAL FINDINGS: 1. Women with preterm fetuses but no pressing need for delivery
PAINLESS BLEEDING (no active bleeding)- observe, confine in hospital meanwhile
The most characteristic event which takes place in the late 2. Women with reasonably mature fetuses- PARKLAND:
second or early third trimesters recommend termination at 37-38wks by CS
Without warning and prior prenatal course may be uneventful 3. Women in labor – double set-up – baka naman hndi placenta
Initial bleeding is often not profuse and ceases spontaneously previa, sometimes can do vaginal delivery
but RECURS 4. Women with severe hemorrhage that delivery is mandated
Usual presenting history: mother waking up in the middle of painless of AOG- CS right away
the night lying on a pool of blood Procrastination but in hospital setting although the
Formation of LUS (lower uterine segment) and cervical women maybe discharge if bleeding stops and fetus is
dilatation tearing of placental attachment torn vessels healthy
which cannot be constricted because myometrial fibers in Delivery: CS preferred method
LUS are unable to contract bleeding
DIFFERENTIATION BETWEEN PLACENTA PREVIA AND ABRUPTIO PLACENTA
DIFFERENTIATION ABRUPTIO PLACENTA PLACENTA PREVIA
HISTORY Frequent association of preeclampsia or hypertension No association with preeclampsia
from any cause
A single attack of vaginal bleeding which usually Repeated “warming” hemorrhage, often occurring over a
continues until delivery period of weeks
Abdominal pain Usually no abdominal pain
Abdominal Local uterine tenderness, hypertonic “woody” uterus Normal uterine tone and usually no tenderness
examination in a concealed abruption Patient rarely in labor
Patient usually in labor Presenting part above brim, malpresentation frequently
Presenting part often engaged found
Fetal parts may be difficult to palpate Fetal parts usually palpable
Fetal heart tone often absent Fetal heart tones present
Ancillary (ultrasound) Placenta in upper uterine segment Placenta in lower uterine segment
Vaginal examination Double-set up reveals no placenta within 5cm of Double-set up reveals placenta implanted on the lower
internal OS uterine segment
Management No place for expectant treatment when this is If bleeding stops and fetus is less than 36 weeks old,
diagnosis is made expectant treatment may be indicated
NOTE: pain cannot be the basis of differentiation bet abruption P and P previa, although painfull bleeding is more common in P previa, it may
also occur on abruption P, depending on the case..
4|O B S T E T R I C S , 2 0 1 4
Trans by: Macasaet, T. Edited By CK Lorenzo, Kaisoo, Dedeem, Grallohnll
You might also like
- UntitledDocument6 pagesUntitledFritz Angelo BullonNo ratings yet
- Fluid and Elctrolyte Balance.... Power PointDocument40 pagesFluid and Elctrolyte Balance.... Power PointMarwan M.100% (1)
- Burn Injury ABCDocument96 pagesBurn Injury ABCSheryl Ann Barit PedinesNo ratings yet
- Antenatal Care: Physiological Changes in PregnancyDocument2 pagesAntenatal Care: Physiological Changes in PregnancyAlexander Ennes100% (1)
- Nursing Mnemonics TsekDocument2 pagesNursing Mnemonics TsekRaymark MoralesNo ratings yet
- Common Health Problems - InfancyDocument76 pagesCommon Health Problems - InfancyAmiel Francisco Reyes100% (1)
- Disorders of The Reproductive SystemDocument10 pagesDisorders of The Reproductive SystemRose Kathreen Quintans AuxteroNo ratings yet
- NCM QuizDocument7 pagesNCM QuizKyla Marie NabongNo ratings yet
- HIGH RISK NEWBORN 13 Student VersionDocument43 pagesHIGH RISK NEWBORN 13 Student VersionsimmyvashishtNo ratings yet
- Pediatric Nursing, Introduction To Maternity and Pediatric NursingDocument82 pagesPediatric Nursing, Introduction To Maternity and Pediatric NursingJose Joseph0% (1)
- Excreta & Sewage Disposal LectDocument79 pagesExcreta & Sewage Disposal LectKathy YoungNo ratings yet
- Pediatric Nursing or Child Health NusrsingDocument20 pagesPediatric Nursing or Child Health NusrsingGenynne RagasaNo ratings yet
- Maternal and Child Care Nursing Module 1Document90 pagesMaternal and Child Care Nursing Module 1Andrea Monique R. Galasinao100% (1)
- Fanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandFanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Peds Exam 3Document61 pagesPeds Exam 3Katie Morgan EdwardsNo ratings yet
- OSCE On 14/3/2008: Describe Gynaecoid PelvisDocument82 pagesOSCE On 14/3/2008: Describe Gynaecoid PelvisKahing LiNo ratings yet
- Bleeding During PregnancyDocument4 pagesBleeding During PregnancyCarl Andre ReyesNo ratings yet
- Pre Natal Care Book BasedDocument9 pagesPre Natal Care Book BasedAngelaTrinidadNo ratings yet
- MCN Skills Lab 2021Document25 pagesMCN Skills Lab 2021irene mancaoNo ratings yet
- MCH BulletsDocument13 pagesMCH BulletsPatziedawn GonzalvoNo ratings yet
- OB-0102D-Obstetric History and PEDocument6 pagesOB-0102D-Obstetric History and PESiselle FajardoNo ratings yet
- CHN MCN Pedia Power BulletsDocument12 pagesCHN MCN Pedia Power BulletsPaul Jhon VergaraNo ratings yet
- NCLEX-RN Exam Prep 2024-2025: 500 NCLEX-RN Test Prep Questions and Answers with ExplanationsFrom EverandNCLEX-RN Exam Prep 2024-2025: 500 NCLEX-RN Test Prep Questions and Answers with ExplanationsNo ratings yet
- Expanded Program On Immunization (EPI) DiseasesDocument12 pagesExpanded Program On Immunization (EPI) DiseasesMaryjoy Gabriellee De La CruzNo ratings yet
- Colorectal CancerDocument31 pagesColorectal CancerIrene RealinoNo ratings yet
- Integratedhealt 150201183122 Conversion Gate02 PDFDocument145 pagesIntegratedhealt 150201183122 Conversion Gate02 PDFVhince PiscoNo ratings yet
- OBGYNE Must-KnowsDocument10 pagesOBGYNE Must-KnowsPigwet KwisNo ratings yet
- Kernicterus, (Bilirubin Encephalopathy) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandKernicterus, (Bilirubin Encephalopathy) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- PE Form - NeonateDocument3 pagesPE Form - NeonateStef ReyesNo ratings yet
- Genitourinary Assessment: Jan Bazner-Chandler RN, MSN, CNS, CPNPDocument27 pagesGenitourinary Assessment: Jan Bazner-Chandler RN, MSN, CNS, CPNPJason Nisky100% (1)
- Maternal and Child Health Nursing (NCM 101 Lect) Part 2Document2 pagesMaternal and Child Health Nursing (NCM 101 Lect) Part 2yunjung0518100% (1)
- Antepartum 1Document3 pagesAntepartum 1Emily DavisNo ratings yet
- Obstetrics and GynecologyDocument36 pagesObstetrics and GynecologyLeiNo ratings yet
- Health Promotion Test QuestionsDocument5 pagesHealth Promotion Test QuestionsAyesha khanNo ratings yet
- Ob-Gyn NG Skills Lab File 2015-2016Document91 pagesOb-Gyn NG Skills Lab File 2015-2016Seydel DucosquelNo ratings yet
- Procedural ReportDocument14 pagesProcedural ReportiamcharraeNo ratings yet
- Hirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Med Online 21Document61 pagesMed Online 21Kumah WisdomNo ratings yet
- NCM 107 Worksheet Week 16.v2Document2 pagesNCM 107 Worksheet Week 16.v2Andrei BorataNo ratings yet
- AnemiaDocument35 pagesAnemiaAgus SyaifudinNo ratings yet
- Communicablediseases 110227001506 Phpapp02 PDFDocument30 pagesCommunicablediseases 110227001506 Phpapp02 PDFCrystal Ann Monsale TadiamonNo ratings yet
- Different Field of Nursing: Geronimo C. Burce JRDocument44 pagesDifferent Field of Nursing: Geronimo C. Burce JRBiway RegalaNo ratings yet
- MANUAL OF PLACENTAL PATHOLOGY FinaleDocument24 pagesMANUAL OF PLACENTAL PATHOLOGY FinaleAnonymous wE02eRNo ratings yet
- Nursing Performance SkillsDocument41 pagesNursing Performance SkillsAhmad Khalil Al SadiNo ratings yet
- PediaDocument6 pagesPediaエニエルカム オレーバンNo ratings yet
- Stages of Fetal DevelopmentDocument92 pagesStages of Fetal DevelopmentMelissa Diego-sarmiento100% (1)
- Prenatal Care 2Document3 pagesPrenatal Care 2Joan Rose Rendon-HungNo ratings yet
- Cardiovascular SystemDocument26 pagesCardiovascular SystemJenny Torreda100% (1)
- Basic Concepts in Pregnancy: Prenatal Care and Health TeachingsDocument12 pagesBasic Concepts in Pregnancy: Prenatal Care and Health Teachingswanda100% (2)
- Introduction To Obstetrics: Professor Nasrin Sultana Juyena, PHDDocument27 pagesIntroduction To Obstetrics: Professor Nasrin Sultana Juyena, PHDShakil MahmodNo ratings yet
- Nutrition: Recommendation: No More Than 30% of Calories Avoid Butter and Coconut OilDocument48 pagesNutrition: Recommendation: No More Than 30% of Calories Avoid Butter and Coconut OilKira100% (3)
- Neurocardio NursingDocument101 pagesNeurocardio NursingMatt Lao DionelaNo ratings yet
- Nclex QuestionaireDocument4 pagesNclex QuestionaireJelai ParaisoNo ratings yet
- (OBS) 3.08b Sexually Transmitted Diseases in Pregnancy - Bongala (Nov 30)Document18 pages(OBS) 3.08b Sexually Transmitted Diseases in Pregnancy - Bongala (Nov 30)Gerben VillanuevaNo ratings yet
- Nursing Seminar 1 SAS Session 4Document8 pagesNursing Seminar 1 SAS Session 4ZiaNo ratings yet
- 1st Bi PediaDocument19 pages1st Bi PediaBeo Adelynn - AiiyuNo ratings yet
- Intrapartum QuizDocument21 pagesIntrapartum QuizJan AudanNo ratings yet
- Obstetrics - Operative Vaginal DeliveryDocument5 pagesObstetrics - Operative Vaginal DeliveryJonathanNo ratings yet
- Obstetrics - HypertensionDocument4 pagesObstetrics - HypertensionJonathan100% (1)
- Obstetrics - Obstretical HemorrhageDocument9 pagesObstetrics - Obstretical HemorrhageJonathanNo ratings yet
- Obstetrics - Cardiovascular Disease in PregnancyDocument3 pagesObstetrics - Cardiovascular Disease in PregnancyJonathanNo ratings yet
- Obstetrics - HepaticDocument4 pagesObstetrics - HepaticJonathanNo ratings yet
- Obstetrics - EndocrineDocument6 pagesObstetrics - EndocrineJonathanNo ratings yet
- Obstetrics - Fetal Growth DisorderDocument4 pagesObstetrics - Fetal Growth DisorderJonathanNo ratings yet
- Obstetrics - Neoplastic Disease of The Ovary (Epithelial) 2014 FinalDocument3 pagesObstetrics - Neoplastic Disease of The Ovary (Epithelial) 2014 FinalJonathanNo ratings yet
- Obstetrics - GastrointestinalDocument6 pagesObstetrics - GastrointestinalJonathanNo ratings yet
- Obstetrics - Puerperal InfectionDocument4 pagesObstetrics - Puerperal InfectionJonathanNo ratings yet
- Obstetrics - Abnormalities of The Amniotic FluidDocument6 pagesObstetrics - Abnormalities of The Amniotic FluidJonathanNo ratings yet
- Different Varieties of English C1 WSDocument5 pagesDifferent Varieties of English C1 WSLaurie WNo ratings yet
- RMK Akl 2 Bab 5Document2 pagesRMK Akl 2 Bab 5ElineNo ratings yet
- EARTH SCIENCE NotesDocument8 pagesEARTH SCIENCE NotesAlthea Zen AyengNo ratings yet
- Essay 1 John WatsonDocument4 pagesEssay 1 John Watsonapi-259502356No ratings yet
- HOPE 2A MODULE 1 Introduction To SportsDocument11 pagesHOPE 2A MODULE 1 Introduction To SportsChristian Ray Lucnagan ReyesNo ratings yet
- 2.peace Treaties With Defeated PowersDocument13 pages2.peace Treaties With Defeated PowersTENDAI MAVHIZANo ratings yet
- Fallout Unwashed Assets Monsters and NpcsDocument4 pagesFallout Unwashed Assets Monsters and NpcsVeritas VeritatiNo ratings yet
- Animals Living in LithuaniaDocument12 pagesAnimals Living in LithuaniaSuiliwasNo ratings yet
- How To Be A Well Rounded Jazz PianistDocument3 pagesHow To Be A Well Rounded Jazz PianistNelson Danny Junior100% (1)
- Education Under The Philippine RepublicDocument25 pagesEducation Under The Philippine RepublicShanice Del RosarioNo ratings yet
- Lecture 1. Introducing Second Language AcquisitionDocument18 pagesLecture 1. Introducing Second Language AcquisitionДиляра КаримоваNo ratings yet
- Hellinger, Bert - GenoGraph 2.1 ManualDocument16 pagesHellinger, Bert - GenoGraph 2.1 ManualGladys Achurra DíazNo ratings yet
- Fiche 2 ConnexionsDocument2 pagesFiche 2 ConnexionsMaria Marinela Rusu50% (2)
- Case Study: Direct Selling ConceptDocument20 pagesCase Study: Direct Selling Conceptbansi2kk0% (1)
- Derivative Pakistan PerspectiveDocument99 pagesDerivative Pakistan PerspectiveUrooj KhanNo ratings yet
- The Mystery of The Secret RoomDocument3 pagesThe Mystery of The Secret RoomNur Farhana100% (2)
- Case: Iridium LLC: Bhanu - Divya - Harsh - NamitaDocument9 pagesCase: Iridium LLC: Bhanu - Divya - Harsh - NamitaHarsh AgrawalNo ratings yet
- Factor Affecting Child Dental Behaviour PedoDocument19 pagesFactor Affecting Child Dental Behaviour PedoFourthMolar.comNo ratings yet
- Corruption CricketDocument21 pagesCorruption CricketAshwin NaraayanNo ratings yet
- My Cook BookDocument66 pagesMy Cook BookAkshay KumariNo ratings yet
- Registrable and Non-Registrable Adverse ClaimsDocument18 pagesRegistrable and Non-Registrable Adverse ClaimsJacob Castro100% (1)
- Chapter One A CellDocument46 pagesChapter One A CellLeon MarkoNo ratings yet
- Heredity and Variation IDocument21 pagesHeredity and Variation Ismbdy tbhhhNo ratings yet
- Apollo Hospital Chennai: NO: 16, BSNL TELESHOPPE, Greams Road 044 2999 1606Document9 pagesApollo Hospital Chennai: NO: 16, BSNL TELESHOPPE, Greams Road 044 2999 1606Manas ChandaNo ratings yet
- Missions ETC 2020 SchemesOfWarDocument10 pagesMissions ETC 2020 SchemesOfWarDanieleBisignanoNo ratings yet
- MNDCS-2024 New3 - 231101 - 003728Document3 pagesMNDCS-2024 New3 - 231101 - 003728Dr. Farida Ashraf AliNo ratings yet
- We Don't Need No MBADocument9 pagesWe Don't Need No MBAsharad_khandelwal_2No ratings yet
- Certified List of Candidates For Congressional and Local Positions For The May 13, 2013 2013 National, Local and Armm ElectionsDocument2 pagesCertified List of Candidates For Congressional and Local Positions For The May 13, 2013 2013 National, Local and Armm ElectionsSunStar Philippine NewsNo ratings yet
- Kebutuhan Modal Kerja Pada Cv. Cipta Karya Mandiri Di SamarindaDocument7 pagesKebutuhan Modal Kerja Pada Cv. Cipta Karya Mandiri Di SamarindaHerdi VhantNo ratings yet
- Main CharacterDocument5 pagesMain CharacterFluffy RabbitNo ratings yet