Professional Documents
Culture Documents
Tropmed 92 883 PDF
Uploaded by
David Dwiadiputra Hartanto0 ratings0% found this document useful (0 votes)
23 views1 pageOriginal Title
tropmed-92-883.pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
23 views1 pageTropmed 92 883 PDF
Uploaded by
David Dwiadiputra HartantoCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 1
Am. J. Trop. Med. Hyg., 92(5), 2015, p.
883
doi:10.4269/ajtmh.14-0770
Copyright © 2015 by The American Society of Tropical Medicine and Hygiene
Images in Clinical Tropical Medicine
Bakua: Tinea Imbricata in the Solomon Islands
Daniel Mason and Michael Marks*
Royal Children’s Hospital, Melbourne, Centre for International Child Health, Parkville, Victoria, Australia; Clinical Research Department,
Faculty of Infectious and Tropical Diseases, London School of Hygiene and Tropical Medicine, London, United Kingdom;
The Hospital for Tropical Diseases, London, United Kingdom
Tinea imbricata or tokelau is a chronic superficial mycosis
caused by Trichophyton concentricum.1 The disease is endemic
in the Pacific, including on the Solomon Islands, where it is
known as bakua. The disease predominantly affects individuals
living in poor rural communities with limited access to hygiene.
It is estimated that between 10% and 20% of individuals in
some Pacific countries are affected. Tinea imbricata begins in
childhood and affects both sexes. Skin lesions can affect the
whole body, but the limbs and torso are most commonly
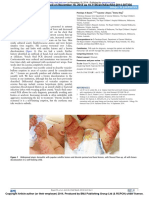
involved. Lesions begin as concentric, annular plaques with or
without erythema (Figure 1). Over time, multiple overlapping
lesions develop (Figure 2). Pruritus is frequent. The florid
nature of tinea imbricata can make infection socially stigma-
tizing. The disease has a classical appearance, and diagnosis is
clinical, although fungal scrapings and culture are possible.
There is thought to be a genetic pre-disposition, with both
Figure 2. Multiple overlapping lesions of tinea imbricata on the
legs of the same child from the western province of the Solomon
Islands.
autosomal-recessive and -dominant inheritance described. Indi-
viduals who develop tinea imbricata have impaired immune
responses to fungal antigens, but the precise mechanism is
not well understood.1 Current treatment options are limited,
with griseofulvin or oral terbinafine preferred.2 Even with
prolonged treatment, recurrence rates are high, and a more
efficacious treatment regimen is needed.
Received December 1, 2014. Accepted for publication December
10, 2014.
Financial support: M.M. is supported by Wellcome Trust Clinical
Research Fellowship 102807.
Authors’ addresses: Daniel Mason, Royal Children’s Hospital,
Melbourne, Parkville, VIC, Australia, E-mail: danmason84@yahoo
.com. Michael Marks, Clinical Research Department, Faculty of
Infectious and Tropical Diseases, London School of Hygiene and
Tropical Medicine, London, United Kingdom and The Hospital for
Tropical Diseases, London, United Kingdom, E-mail: michael.marks@
lshtm.ac.uk.
This is an open-access article distributed under the terms of the
Creative Commons Attribution License, which permits unrestricted
use, distribution, and reproduction in any medium, provided the
original author and source are credited.
Figure 1. Classical lesion of tinea imbricata on the arm of a child
from the Solomon Islands. REFERENCES
1. Bonifaz A, Archer-Dubon C, Saúl A, 2004. Tinea imbricata or
Tokelau. Int J Dermatol 43: 506–510.
*Address correspondence to Michael Marks, Clinical Research 2. Wingfield AB, Fernandez-Obregon AC, Wignall FS, Greer DL,
Department, Faculty of Infectious and Tropical Diseases, London 2004. Treatment of tinea imbricata: a randomized clinical trial
School of Hygiene and Tropical Medicine, Keppel Street, London using griseofulvin, terbinafine, itraconazole and fluconazole.
WC1E 7HT, United Kingdom. E-mail: michael.marks@lshtm.ac.uk Br J Dermatol 150: 119–126.
883
You might also like
- 02 Descending Necrotizing Mediastinitis As A Complication of Odontogenic InfectionDocument3 pages02 Descending Necrotizing Mediastinitis As A Complication of Odontogenic Infectiondr.antonio.velasquezNo ratings yet
- Bryant2014 PDFDocument2 pagesBryant2014 PDFBilel DhaouadiNo ratings yet
- Hand, Foot and Mouth Disease: Australian Family Physician September 2003Document3 pagesHand, Foot and Mouth Disease: Australian Family Physician September 2003giselaNo ratings yet
- Ebola Virus Disease: Potential Use of Melatonin As A TreatmentDocument4 pagesEbola Virus Disease: Potential Use of Melatonin As A Treatmenteva sekarNo ratings yet
- Cancer HBO-BMLDocument3 pagesCancer HBO-BMLThumiso MasohaNo ratings yet
- Clinical Review - FullDocument6 pagesClinical Review - Fullilham thohirNo ratings yet
- Actinomicose Cervico-Facial. 2020Document7 pagesActinomicose Cervico-Facial. 2020Vinícius FlorentinoNo ratings yet
- Oral Tuberculosis: Case ReportDocument2 pagesOral Tuberculosis: Case ReportMauriceNo ratings yet
- TineaDocument2 pagesTineaGail AidNo ratings yet
- ScabiesDocument9 pagesScabiesBhoomi GoyaniNo ratings yet
- Dog Bites: BMJ (Online) March 2007Document6 pagesDog Bites: BMJ (Online) March 2007Fitri Pite SiNo ratings yet
- A Child With Complicated Diphtheria in This Vaccine Era: A Case ReportDocument2 pagesA Child With Complicated Diphtheria in This Vaccine Era: A Case Reportummu yayaNo ratings yet
- Special: Noma: Life Cycle of A Devastating Sore - Case Report and Literature ReviewDocument6 pagesSpecial: Noma: Life Cycle of A Devastating Sore - Case Report and Literature ReviewEl Defensor Teas: 100 NaturalNo ratings yet
- Chronic Figurate Skin LesionsDocument3 pagesChronic Figurate Skin Lesionswarisa nuhurridhaNo ratings yet
- Oral Myiasis in A Cerebral Palsy Patient: A Case Report: Jain S, Gupta S, Jindal SK, Singla ADocument3 pagesOral Myiasis in A Cerebral Palsy Patient: A Case Report: Jain S, Gupta S, Jindal SK, Singla AWella Vista EdwardNo ratings yet
- CH 04Document80 pagesCH 04flock_duxNo ratings yet
- TPMD 200176Document2 pagesTPMD 200176Marcelita DuwiriNo ratings yet
- Tinea Corporis An Updated ReviewDocument12 pagesTinea Corporis An Updated ReviewM Ilham FadillahNo ratings yet
- 2020 - Tinea Corporis An Updated ReviewDocument12 pages2020 - Tinea Corporis An Updated ReviewYunita SariNo ratings yet
- Variants of Erythema Multiforme: A Case Report and Literature ReviewDocument8 pagesVariants of Erythema Multiforme: A Case Report and Literature Reviewranz ibonkNo ratings yet
- Ources of Antimicrobial ResistanceDocument3 pagesOurces of Antimicrobial ResistanceKoorosh IraniNo ratings yet
- Communicable Disease Nursing PDFDocument47 pagesCommunicable Disease Nursing PDFma.crissacpenaNo ratings yet
- Heim 2017Document13 pagesHeim 2017Muhamad SaifuddinNo ratings yet
- The Kerion An Angry Tinea Capitis PBDocument7 pagesThe Kerion An Angry Tinea Capitis PBprajnamitaNo ratings yet
- 26 Rosmini J1a120221-BingDocument5 pages26 Rosmini J1a120221-BingRosmini MansurNo ratings yet
- Review: Tinea Corporis: An Updated ReviewDocument22 pagesReview: Tinea Corporis: An Updated ReviewMade SetiadjiNo ratings yet
- Ent 11 2 2Document5 pagesEnt 11 2 2ilomurtalaNo ratings yet
- Tinea CorporisDocument2 pagesTinea CorporisImas Puterii MuntheNo ratings yet
- Oral and Maxillofacial Surgery CasesDocument5 pagesOral and Maxillofacial Surgery Casesvaleria lindaNo ratings yet
- Comparative Study of Efficacy of Oral Terbinafine Alone and Oral Terbinafine With Topical 8% Ciclopirox Olamine in OnychomycosisDocument7 pagesComparative Study of Efficacy of Oral Terbinafine Alone and Oral Terbinafine With Topical 8% Ciclopirox Olamine in OnychomycosisIJAR JOURNALNo ratings yet
- Diseases of The EarDocument6 pagesDiseases of The EarSimret SolomonNo ratings yet
- 1 s2.0 S2214541921000353 MainDocument4 pages1 s2.0 S2214541921000353 Mainrahmania alikhlashNo ratings yet
- Denture Stomatitis 3Document4 pagesDenture Stomatitis 3Utami MayasariNo ratings yet
- Insect BitesDocument26 pagesInsect BiteszeniafadilaNo ratings yet
- Lecture On MEASLESDocument16 pagesLecture On MEASLESNicole Villanueva, BSN - Level 3ANo ratings yet
- Gupta Ak Et Al Fungal Skin Infections PDFDocument17 pagesGupta Ak Et Al Fungal Skin Infections PDFValeria BeltranNo ratings yet
- Nursing Care For A Family Caring For Children With Infectious DiseaseDocument4 pagesNursing Care For A Family Caring For Children With Infectious DiseasekdfhjfhfNo ratings yet
- Infectious DiseaseDocument6 pagesInfectious DiseaseJoshua AjomNo ratings yet
- As SIS Textbook AnswersAVDocument84 pagesAs SIS Textbook AnswersAVNamTrầnNo ratings yet
- Fungal Skin Infections: Education GapDocument17 pagesFungal Skin Infections: Education GapAncuta CalimentNo ratings yet
- Pinworms (E.vermicularis) Mimicking Acute AppendicitisDocument2 pagesPinworms (E.vermicularis) Mimicking Acute AppendicitisMedtext PublicationsNo ratings yet
- Pearls On Child SkinDocument2 pagesPearls On Child SkinAarifNo ratings yet
- Case Study (Serencio's Group) FINALDocument4 pagesCase Study (Serencio's Group) FINALMarjorie EragNo ratings yet
- Bed Bug Outbreak in A Neonatal UnitDocument6 pagesBed Bug Outbreak in A Neonatal UnitfikirudinNo ratings yet
- Translate 5Document22 pagesTranslate 5Dahliawati MohiNo ratings yet
- Communicable Disease Prevention and ControlDocument197 pagesCommunicable Disease Prevention and Controldennisjamesbartz100% (1)
- Noma امجد حمزة عبد حسينDocument8 pagesNoma امجد حمزة عبد حسينSaif HaiderNo ratings yet
- Case 32Document16 pagesCase 32Prashant MishraNo ratings yet
- Perbandingan 3 - IndiaDocument4 pagesPerbandingan 3 - IndiaElva PatabangNo ratings yet
- A. Introduction OsteomyelitisDocument10 pagesA. Introduction OsteomyelitisMa. Gina DerlaNo ratings yet
- Molluscum Contagiosum:: What's New and True?Document6 pagesMolluscum Contagiosum:: What's New and True?79lalalaNo ratings yet
- Case Report: A Case of Terbinafine-Resistant Tinea Cruris Caused byDocument3 pagesCase Report: A Case of Terbinafine-Resistant Tinea Cruris Caused bydzulfiNo ratings yet
- Recurrent FurunculosisDocument4 pagesRecurrent FurunculosisIvan KurniadiNo ratings yet
- Tinea Faciei - Relato de CasoDocument3 pagesTinea Faciei - Relato de CasoJosé Paulo Ribeiro JúniorNo ratings yet
- Erythema Multiforme: A Case Series and Review of Literature: November 2018Document8 pagesErythema Multiforme: A Case Series and Review of Literature: November 2018Nurlina NurdinNo ratings yet
- Miliariapustulosa in Post Craniotomy Patient: IOP Conference Series: Earth and Environmental ScienceDocument6 pagesMiliariapustulosa in Post Craniotomy Patient: IOP Conference Series: Earth and Environmental ScienceHanni HaeraniNo ratings yet
- Activity 2 - Case StudyDocument5 pagesActivity 2 - Case StudyGrace MendozaNo ratings yet
- Canina Fossa Abscess and Treatment: Muhammad H. ChandhaDocument4 pagesCanina Fossa Abscess and Treatment: Muhammad H. ChandhaasadNo ratings yet
- Topic 01Document8 pagesTopic 01PLH MusicNo ratings yet
- Cooper Lee The Chinese Language For BeginnersDocument44 pagesCooper Lee The Chinese Language For BeginnersmatildeNo ratings yet
- Full Test Bank For Human Heredity Principles and Issues 10Th Edition Cummings PDF Docx Full Chapter ChapterDocument36 pagesFull Test Bank For Human Heredity Principles and Issues 10Th Edition Cummings PDF Docx Full Chapter Chapteroverspanchitter4abo100% (11)
- The Gatekeepers of DuatDocument1 pageThe Gatekeepers of DuatMarcus LibertatesNo ratings yet
- MSH Regulated Sexual ConductsDocument3 pagesMSH Regulated Sexual ConductsthekarlpazNo ratings yet
- Esquisse - Sec ADocument6 pagesEsquisse - Sec AMR P PinnyNo ratings yet
- Alemayehu Regassa Senbetu, EthiopiaDocument8 pagesAlemayehu Regassa Senbetu, EthiopiaAlemayehu RegassaNo ratings yet
- XX Postnatal ExcerciseDocument6 pagesXX Postnatal ExcerciseNeicu VladNo ratings yet
- CNZ French Food Cheat SheetDocument2 pagesCNZ French Food Cheat SheetJulien Le HoanganNo ratings yet
- EarthAndLifeScience (SHS) Q2 Mod23 PerpetuationOfLife V1Document23 pagesEarthAndLifeScience (SHS) Q2 Mod23 PerpetuationOfLife V1Roseman TumaliuanNo ratings yet
- Test Bank For Ekg Plain and Simple 4th Edition by Ellis Chapters 12-15-18 Not IncludedDocument11 pagesTest Bank For Ekg Plain and Simple 4th Edition by Ellis Chapters 12-15-18 Not Includedcanebrutalfniy66No ratings yet
- Chapter 12Document47 pagesChapter 12Инж. Лазарина ЕвлогиеваNo ratings yet
- If Conditional: A. Complete The Sentence With The Correct Form of The Verb in ParenthesesDocument3 pagesIf Conditional: A. Complete The Sentence With The Correct Form of The Verb in ParenthesesJose Ronal TerrazasNo ratings yet
- Descriptive Text About Place: DolphinsDocument2 pagesDescriptive Text About Place: DolphinsIsmiweningNo ratings yet
- Modifiers 02Document2 pagesModifiers 02jaysakeNo ratings yet
- #1 Points 2 Kool Medic PDFDocument137 pages#1 Points 2 Kool Medic PDFSyed Ali Raza NaqviNo ratings yet
- Included in The Biochemical Profile (SMA-12) : Normal Lab ValuesDocument5 pagesIncluded in The Biochemical Profile (SMA-12) : Normal Lab ValueszuftNo ratings yet
- Pathophysiology Exam 4 - ReviewDocument18 pagesPathophysiology Exam 4 - ReviewWaqas GillNo ratings yet
- Human Resource Management International Digest: Article InformationDocument4 pagesHuman Resource Management International Digest: Article InformationHanna BaranyaiNo ratings yet
- Questions 1-3 Choose THREE Letters, A-E. Which THREE of The Following Arguments Are Stated in The Passage?Document3 pagesQuestions 1-3 Choose THREE Letters, A-E. Which THREE of The Following Arguments Are Stated in The Passage?Ozoda TuxliyevaNo ratings yet
- Fact About Teeth in Animals: By: K.V Nivitha ShriDocument6 pagesFact About Teeth in Animals: By: K.V Nivitha Shrivictor_venki9955No ratings yet
- Robinson Crusoe: Zooloretto The Dice GameDocument5 pagesRobinson Crusoe: Zooloretto The Dice GameMuneeb ArshadNo ratings yet
- Aunt Catfish MenuDocument2 pagesAunt Catfish MenudddsNo ratings yet
- Best Dog Grooming Near Me 0121Document3 pagesBest Dog Grooming Near Me 0121Arch. ZionNo ratings yet
- Squid Game CharactersDocument20 pagesSquid Game CharactersJose Ramon Batiller100% (1)
- d2008 Molo District Paper 2 AnswersDocument9 pagesd2008 Molo District Paper 2 AnswersGodfrey MuchaiNo ratings yet
- Services Fifty Shades of Furr Inc 2Document1 pageServices Fifty Shades of Furr Inc 2Austin DormanNo ratings yet
- Tomberlin and Adler 1998Document6 pagesTomberlin and Adler 1998ayakashimajorinNo ratings yet
- Acute Gastroenteritis (Age)Document37 pagesAcute Gastroenteritis (Age)Jay Ar SantiagoNo ratings yet
- Sniffy The Virtual Rat Simulated Operant ConditionDocument9 pagesSniffy The Virtual Rat Simulated Operant ConditionPsychieNo ratings yet
- The Hiram W Bleeker Coat of Arms NarrativeDocument26 pagesThe Hiram W Bleeker Coat of Arms Narrativeapi-366143603No ratings yet