Professional Documents
Culture Documents
St. Luke's College of Medicine - William H. Quasha Memorial: Physiology
Uploaded by
Mavic VillanuevaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
St. Luke's College of Medicine - William H. Quasha Memorial: Physiology
Uploaded by
Mavic VillanuevaCopyright:
Available Formats
St. Luke’s College of Medicine – William H.
Quasha Memorial
PHYSIOLOGY BLOCK 1
Lecture: 9 – Autonomic Nervous System Date: August 17, 2015
Lecturer: Dr. Arlene R. Ng, M.D., Ph.D. Trans Team: Capinpin, Capistrano, Caseñas,
Cayetano
Topic Outline
I. General Organization of the Autonomic Nervous
System
A. Sympathetic Nervous System Subconscious
B. Parasympathetic Nervous System sensory signals
C. Enteric Nervous System
II. Characteristics of the Sympathetic and
Parasympathetic Function
A. Response
B. Neurotransmitters
C. Receptors
III. Autonomic Effects on Various Organs of the Body
IV. Autonomic Reflexes Subconscious
V. Sympathetic and Parasympathetic Tone reflex responses
VI. Mass Discharge of the Sympathetic Nervous System
VII. Specific Localized Responses from the
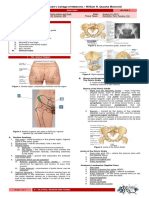
Parasympathetic System Figure 2.Process of eliciting a response in the ANS.
VIII. Medullary, Pontine, Mesenteric Control of the ANS
IX. Pharmacology of the Autonomic Nervous System Two major subdivisions
LEGEND A. Sympathetic Nervous System
PPT Trans Audio Trans Book Trans B. Parasympathetic Nervous System
A. Sympathetic Nervous System
I. General Organization of the Autonomic Nervous
The sympathetic nerve fibers originate in the spinal cord
System along with the spinal nerves between cord segments T1
Autonomic Nervous System and L2 and pass first in to the sympathetic chain and then
Portion of the nervous system that controls most visceral to the tissues and organs that are stimulated by the
functions of the body sympathetic nerves
Functions on its own automatically Thoracolumbar outlflow (T1 to L2)
Helps to control arterial pressure, gastrointestinal motility, Sympathetic Chain – ganglia located just beside the spinal
gastrointestinal secretion, urinary bladder emptying, cord; axons of the SNS synapse here before going to the
sweating, body temperature, etc. different organ systems
In coordination with higher centers of the brain Two main ganglion to be remembered are the (1) celiac
Rapidity and intensity with which it can change visceral ganglion and (2) hypogastric plexus
functions For every sympathetic nerve that innervates an organ there is
Activated mainly by centers located in the spinal cord, brain usually a corresponding parasympathetic innervation.
stem, and hypothalamus(major control center)
Figure 1. Location of the autonomic control centers in the brain,
(1) Brain Stem (mid-brain, pons and medulla), (2) Hypothalamus,
(3) Spinal Cord.
Limbic Cortex
portion of the Cerebral Cortex
controls emotion
o when scared, anxious, angry, the autonomic system reacts
accordingly
o example: going to the toilet before exams, increase of cardiac
rate, sweating and turning red when mad, turning red at the
mention of something or someone
can transmit signals to the lower centers and in this way
influence autonomic control
automatic and subconscious
Visceral Reflex
The autonomic nervous system often operates through this
o Subconscious signals from visceral organs can enter the
autonomic ganglia, the brain stem, or the hypothalamus and
then return the subconscious reflex response directly back to
the visceral organs to control their activities
All autonomic reflexes are polysynaptic with at least one
synapse in the CNS and another in the autonomic
ganglion. Figure 3.The Sympathetic Nervous System.
Page 1 of 6 9 – AUTONOMIC NERVOUS SYSTEM
PHYSIOLOGY BLOCK 1
2 portions of the Autonomic Nervous System: Some of the postganglionic fibers pass back from the
i. Preganglionic Portion sympathetic chain into the spinal nerves through the gray
ii. Postganglionic Portion rami at all levels of the cord
The ganglia are located outside the spinal cord Theses sympathetic fibers are all very small type C fibers,
and they extend to all parts of the body by way of the
Table 1. Difference between the Innervation of Skeletal Muscles skeletal nerves
and Innervation of the Autonomic Nervous System Type C fibers
Innervation of Innervation of the Autonomic o Thinly, if not unmyelinated nerve fibers
Skeletal Nervous System o They control the blood vessels, sweat glands, and the
Muscles pilo-erector muscles of the hairs
Number of Single neuron in Two neurons: a pre-ganglionic Segmental Distribution of the Sympathetic Nerve Fibers
neurons the skeletal and a post-ganglionic neuron (not necessarily distributed to the same part of the body as
motor pathway the somatic spinal nerve fibers from the same segments)
Spinal cord Nerve cells in Axon fibers pass through the T1 : head
exit the spinal cord anterior root of the spinal cord T2 : neck
exit anteriorly into the corresponding spinal T3 to T6 : thorax
(anterior /motor nerve. After the spinal nerve T7 to T11 : abdomen
root of the passes through the spinal canal, T12, L1, L2 : legs
spinal cord) the pre-ganglionic fibers leave The distribution of sympathetic nerves to each organ is
the spinal nerve and pass determined partly by the locus in the embryo by which
through the white ramus (aka the organ originated
white ramus communicans) of Adrenal Medullae
one of the ganglia of the Located on top of the kidneys
sympathetic chain Innervated by sympathetic fibers
Formation No Yes Secretory cells embryologically derived from nervous
of Synapse In the sympathetic chain: fate tissue and are actually postganglionic neurons; the
outside the number 1 and 2 endings of these fibers secrete the adrenal hormones
spinal cord Before the target organ: fate epinephrine and norepinephrine
number 3
Pathway Goes directly to In the sympathetic chain, the B. Parasympathetic Nervous System
Fibers leave the central nervous system through cranial
the muscle that fate of the pre-ganglionic fiber
nerves III, VII, IX, and X; additional parasympathetic fibers
it innervates – can be one of the following:
leave the lowermost part of the spinal cord through the
to the 1. It can synapse with post- second and third sacral spinal nerves and occasionally the
neuromuscular ganglionic neurons of the first and fourth sacral nerves
junction then ganglion that it entered Craniosacral outflow
the muscle itself 2. It can pass upward or Parasympathetic ganglia are located near the end organs.
downward in the chain and The presynaptic fiber is very long, the postsynaptic axon is
synapse with another relatively short.
ganglion of the sympathetic Vagus Nerve (CN X)
chain o Heart, lungs, esophagus, stomach, entire small
3. It can pass through the chain intestine, proximal half of colon, liver, GB, pancreas,
and exit through one of the kidneys, upper portion of the uterus
sympathetic nerves radiating o Almost all the visceral organs
outward from the chain and Cranial Nerve III
synapse in a peripheral o Pupillary sphincter and ciliary muscle of the eye
sympathetic ganglion Cranial Nerve VII
The post-ganglionic o Lacrimal, nasal, and submandibular glands
sympathetic neurons thus Cranial Nerve IX
originate either from one of the o Parotid gland
Sacral Fibers (Pelvic Nerves)
sympathetic chain ganglia OR
o Pass through spinal nerve sacral plexus at S2 and S3
from one of the peripheral
levels
sympathetic ganglia. From o Descending colon, rectum, urinary bladder, lower
either of the two sources, the portions of the ureters, external genitalia
post-ganglionic fibers travel to Preganglionic fibers pass uninterrupted all the way to the
their target organs. organ that is to be controlled and synapse with
postganglionic neurons in the wall of the organ
Figure 4. Comparison of ANS and Somatic Nervous System
Page 2 of 6 9 – AUTONOMIC NERVOUS SYSTEM
PHYSIOLOGY BLOCK 1
II. Characteristics of the Sympathetic and
Parasympathetic Function
A. Responses
a. Sympathetic response – Stress; flight or fight
b. Parasympathetic response – Peace; rest and digest
B. Neurotransmitters
Normally, neurotransmitters are present for a short period of
time and then broken down but in the adrenal medulla,
neurotransmitters last a little longer than normal for them to
have their effect in the other organs
Table 2. Neurotransmitters of the ANS
Sympathetic Parasympathetic
Nervous System Nervous System
Pre- Cholinergic Cholinergic
ganglionic (Acetylcholine) (Acetylcholine)
Neurons
Post- Mostly adrenergic Cholinergic
ganglionic (Norepinephrine) (Acetylcholine)
Neurons Occasionally
acetylcholine
a. Acetylcholine
o Produced in the pre-synaptic terminal button
o Cholinergic neurons in the sympathetic nervous system: found
in sweat glands, pilo-erector muscles and some blood vessels;
use acetylcholine as their neurotransmitter to subserve the
sympathethic function of these cells
o Degradation: acetylcholinesterase
Figure 5. The Parasympathetic Nervous System
b. Norepinephrine
o Produced in the proximal area of the neuron before it
C. Enteric Nervous System (ENS) ends up in vesicles
Controls function of the gastrointestinal tract, pancreas, o Postganglionic in SNS Adrenergic
and gallbladder o Removal of norepinephrine
Contains local sensory, motor and inter-neurons a. Reuptake
Responsible for: b. Diffusion at the synaptic cleft and into the surrounding
o Alteration in the gut walls body fluids then into the blood
o Changes in the chemical environment of the gut c. Destruction using enzymes
Control smooth muscles of the gut, local blood vessels, i. Catechol-O-methyl transferase (COMT)
secretion of mucosa ii. Monoamine oxidase
Has 80 to 100 million neurons
Two major plexus: C. Receptors
1. Myenteric (Auchbach’s) plexus - Binding of neurotransmitters cause:
Between the outer longitudinal and inner circular o Change in cell permeability to one or more ions
muscle layer o Activation or inactivation of an enzyme attached to the
Controls gut motility other end of the receptor protein
2. Submucous (Meissner’s) plexus - 2nd messenger systems
Between the circular muscle layer and mucosa
Controls secretory function (regulates fluid -Acetylcholine receptors
homeostasis) o Muscarinic – found on all effector cells (except NMJ)
Connected with ANS, but functions separately that are stimulated by the postganglionic cholinergic
Relatively independent of the CNS neurons of either the parasympathetic nervous system
With inputs from ANS or the sympathetic system
Controls the peristalsis of the gastrointestinal tract o Nicotinic – Found in the autonomic ganglia at the
ANS influence on ENS synapses between the preganglionic and postganglionic
The parasympathetic nervous system stimulates gut motility neurons of both the sympathetic and parasympathetic
systems
The sympathetic nervous system decreases gut motility
- More proximal than the muscarinic receptors
- Also present at many non-autonomic nerve endings
(e. g. neuro-muscular junctions in skeletal muscle)
Muscarinic
Receptors
M1 M2 M3 M4 M5
Smooth
CNS Heart CNS CNS
Muscle
Nicotinic Receptors
N1 N2
Neuromuscular Autonomic ganglia, CNS
Junction and adrenal medulla
Mainly post-ganglionic
Pre-ganglionic Figure 7. Types of acetylcholine receptors and their locations
Figure 6. Enteric and Autonomic Nervous System
Page 3 of 6 9 – AUTONOMIC NERVOUS SYSTEM
PHYSIOLOGY BLOCK 1
-Adrenergic receptors (Sympathetic Nervous System only) - tone can be affected by removal or denervation so that there would
o Alpha receptors be hypersensitivity to certain stimuli when the tone is removed
- α1 Denervation supersensitivity
- α2 - Upregulation of receptors
o Beta receptors - Effect of norepinephrine: decreases blood flow due to
- β1 vasoconstriction
- β2 - Giving a test dose of norepinephrine decreases blood pressure
- β3 - Stellate ganglionectomy: loss of normal sympathetic tone
- If stellate ganglion is removed, there would be an increase in
o Norepinephrine blood flow in the arm (action of the sympathetic nervous system is
- Excites mainly alpha receptors but excites the beta vasoconstriction so if the tone is removed, there would be increase
receptors to a lesser extent as well in blood flow due to vasodilation)
- More specific; if you want to give a medication that - Blood flow would eventually go down but not necessarily
targets alpha receptors, give norepinephrine instead of normalize
epinephrine - A test dose of norepinephrine after ganglionectomy will cause a
o Epinephrine greater than the effect than the test dose given before the
- Excites both types of receptors equally procedure because of the upregulation of receptors that happened
with denervation during ganglionectomy
Table 3. Function of Adrenergic Receptors
Alpha Receptors Beta receptors
Vasoconstriction Vasodilation (β2)
Iris dilation Cardioacceleration (β1)
Intestinal relaxation Increased myocardial strength
(β1)
Intestinal sphincter Intestinal relaxation (β2)
contraction Uterus relaxation (β2)
Pilomotor contraction Bronchodilation (β2)
Bladder sphincter contraction Calorigenesis (β2)
Inhibits neurotransmitter Glycogenolysis (β2)
release (α2) Lipolysis (β1)
Bladder wall relaxation (β2)
Thermogenesis (β3) Figure 9. Effect of sympathectomy on blood flow in the arm, and
effect of a test dose of norepinephrine before and after
sympathectomy, showing supersensitization of the vasculature to
norepinephrine
V. Autonomic reflexes
- Cardiovascular autonomic reflexes
o Baroreceptor reflex
If there is a decrease in blood flow, pressure receptors in the
carotid bodies and the aorta will notice it and the SNS can
constrict the blood vessels to increase blood pressure
Can also send signals to the cardiovascular center in the
medulla so that it will send signal to the spinal cord to increase
cardiac output through sympathetic stimulation to bring back
the blood pressure (NOT parasympathetic because it decreases
blood pressure)
- Gastrointestinal autonomic reflexes
o food in mouth
Signals to vagal, glossopharyngeal and salivatory nuclei of
brainstem parasympathetic transmission to secretory
glands of mouth and stomach increase secretion of
digestive juices
o fecal matter in rectum
Stretching of rectumsacral spinal cordreflex signal
through parasympathetics to distal colonstrong
peristaltic contractionsdefecation
- Urinary reflex
Bladder stretchsacral cordreflex bladder contraction
and urinary sphincter relaxationurination
- Sexual reflex (initiated by psychic stimuli from the brain and
stimuli from the sexual organs) converge on sacral cord
a. Erection (parasympathetic)
b. Ejaculation (partially sympathetic)
VI. Mass Discharge of the Sympathetic System
- Happens when there is an intense stimuli (eg. fight or flight
Figure 8. Location of Muscarinic and Nicotinic Receptors condition)
- All portions of the sympathetic nervous system discharge
III. Autonomic Effects on Various Organs of the Body simultaneously
- Alarm or stress response
Hypothalamic activation by fright or severe pain
Please see Appendix 1. Widespread reaction throughout the body
Advice from Dr. Ng: REMEMBER THE TABLE
“Alarm” or “Stress” Response of the Sympathetic Nervous
IV. Sympathetic and Parasympathetic “Tone” System
- tone allows a single nervous system to both increase and - Mass discharge increases ability of the body to perform
decrease the activity of a stimulated organ vigorous muscle activity
- when parts of the SNS and PNS function, they do not start from o Increased arterial pressure
zero (it has an underlying tone) so that minute corrections in the o Increased blood flow to active muscles concurrent with
function can happen decreased blood flow to organs such as the
- effect of sympathetic tone on systemic arterioles gastrointestinal tract and the kidneys that are not needed
o denervation effects for rapid motor activity
- Intrinsic tone tends to restore normal function o Increased rates of cellular metabolism throughout the
o chemical adaptation body
o Increased blood glucose concentration
Page 4 of 6 9 – AUTONOMIC NERVOUS SYSTEM
PHYSIOLOGY BLOCK 1
o Increased glycolysis in the liver and in the muscle - Include intravenous norepinephrine, epinephrine and
o Increased muscle strength methoxamine
o Increased mental activity
- In contrast, alpha and beta receptor blockers can block
o Increased rate of blood coagulation
- Happens in highly emotional states andrenergic activity
o Rage Parasympathomimetic drugs
Hypertensionbrainstem ret formation spinal cord - Also called cholinergic drugs
massive sympathetic discharge - Stimulate parasympathetic effector organs
- Sympathetic alarm reaction (fight or flight)
- In contrast, cholinergic activities can be blocked with anti-
- Heat regulation: control of sweating and blood flow
acetylcholinesterase drugs (same as those discussed in NMJ
o Plexus beneath the skin is composed of blood vessels that
would control loss of heat via constriction lecture)
X. References
- Local reflexes affecting sensory afferent fibers
Dr. Ng’s lecture
o Heating the skin
Textbook of Medical Physiology 12th edition by Guyton
Figure 1. Location of the autonomic control centers in the
VII. Specific Localized Responses from the
brain:
Parasympathetic System
http://www2.estrellamountain.edu/faculty/farabee/biobk/biob
- Cardiovascular reflexes
ooknerv.html
- Secretion of mouth and stomach glands
Figure 4. Comparison of ANS and Somatic Nervous System:
- Rectal emptying
http://antranik.org/the-autonomic-nervous-system/
VIII. Medullary, Pontine, Mesencephalic Control of the Figure 6. Enteric and Autonomic Nervous System:
Autonomic Nervous System https://upload.wikimedia.org/wikipedia/commons/2/29/Neural
- All ANS activities are made possible by the control of the _control_gut.png
higher centers and the hypothalamus Figure 8. Location of Muscarinic and Nicotinic Receptors:
- will be discussed separately in another block :) http://higheredbcs.wiley.com/legacy/college/tortora/0470565
101/hearthis_ill/pap13e_ch15_illustr_audio_mp3_am/simulat
ions/hear/neuron_chol_adre.html
V. QUIZ
1. This neurotransmitter is released from the axon terminal of
pre-ganglionic fibers.
2. Post-ganglionic sympathetic neurons release the following
neurotransmitter(s):
a. Ach c. Epinephrine e. a, b and c
b. NEpinephrine d. a and b only
3. Which of the ff is true about ENS?
a. Connected with ANS, but functions separately
b. Not connected with ANS, and functions separately
c. Connected with ANS, but has no influence on it
d. Influenced and controlled by ANS
4. True or False: Norepinephrine can leak into the bloodstream.
Figure 10. Autonomic Control Centers in the Brain Stem 5. What compensates for the removal of tone caused by
and the Hypothalamus denervation?
IX. Pharmacology of the ANS Answers:
Sympathomimetic drugs 1. Ach
- Also called andrenergic drugs 2. e
3. a
- Stimulate sympathetic effector organs 4. True
5. Progressive increase/decrease of intrinsic tone
Appendix 1. Autonomic Effects on Various Organs of the Body
Page 5 of 6 9 – AUTONOMIC NERVOUS SYSTEM
PHYSIOLOGY BLOCK 1
Page 6 of 6 9 – AUTONOMIC NERVOUS SYSTEM
You might also like
- (PHYSIO) 1.05 Autonomic Nervous System (EGBartolome)Document7 pages(PHYSIO) 1.05 Autonomic Nervous System (EGBartolome)Izza Mari DeLeon Laurio100% (2)
- Physiology: Block 1Document5 pagesPhysiology: Block 1Mavic VillanuevaNo ratings yet
- Physiology: Guevara, Henaku-Larbi, Inciong, JutizDocument3 pagesPhysiology: Guevara, Henaku-Larbi, Inciong, JutizMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic Villanueva100% (1)
- Brainstem Lesions Trans 2019 PDFDocument8 pagesBrainstem Lesions Trans 2019 PDFVon HippoNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument4 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha MemorialDocument3 pagesSt. Luke's College of Medicine - William H. Quasha MemorialMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: Block 1Document9 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: Block 1Mavic Villanueva100% (1)
- Autonomic Nervous SystemDocument12 pagesAutonomic Nervous SystemKaye NeeNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- 7.1 (LEC) - Functional Anatomy of Respiratory System and Mechanics of BreathingDocument9 pages7.1 (LEC) - Functional Anatomy of Respiratory System and Mechanics of BreathingKenneth TorresNo ratings yet
- 01 - Overview of The Cardiovascular Physiology - ACPDocument6 pages01 - Overview of The Cardiovascular Physiology - ACPMavic VillanuevaNo ratings yet
- 1.02 Physiology Trans - Muscle PhysiologyDocument10 pages1.02 Physiology Trans - Muscle PhysiologyMineTagraNo ratings yet
- Chapter 33, 36 - GuytonDocument8 pagesChapter 33, 36 - GuytonRoderick Palattao100% (2)
- 1 Digestive System DevelopmentDocument3 pages1 Digestive System DevelopmentDianne IgnacioNo ratings yet
- OS 206 Renal PhysiologyDocument9 pagesOS 206 Renal Physiologyalphius_mendoza100% (1)
- PLM AbdomenDocument11 pagesPLM AbdomenClaudine Victoria Taracatac100% (1)
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- Examination of Cerebellum and MeningesDocument4 pagesExamination of Cerebellum and MeningesAngelaTrinidadNo ratings yet
- REV Micro HSB RemedsDocument16 pagesREV Micro HSB RemedsPatricia HariramaniNo ratings yet
- 2 - Renal PhysiologyDocument8 pages2 - Renal PhysiologyKunware TropaNo ratings yet
- Biochem 2.1 Introduction To MetabolismDocument5 pagesBiochem 2.1 Introduction To Metabolismlovelots1234No ratings yet
- MTHISTO100 Lesson 2 Excretory SystemDocument9 pagesMTHISTO100 Lesson 2 Excretory SystemJaeri HuangNo ratings yet
- Neuroanatomy NotesDocument8 pagesNeuroanatomy NotesJustine May Gervacio100% (1)
- OSCE Cerebellar Examination PDFDocument6 pagesOSCE Cerebellar Examination PDFriczen vilaNo ratings yet
- PNS Exam Full Study GuideDocument25 pagesPNS Exam Full Study GuideJean-JeanGwoNo ratings yet
- Embryo Trans Unofficial TransDocument14 pagesEmbryo Trans Unofficial TransMark LopezNo ratings yet
- Muscles of The Neck PDFDocument1 pageMuscles of The Neck PDFEdreyn DellosaNo ratings yet
- Neuroanatomy SamplexDocument2 pagesNeuroanatomy SamplexMineTagraNo ratings yet
- Introduction To The Endocrine System NotesDocument12 pagesIntroduction To The Endocrine System NotesJulioNo ratings yet
- Ascending Tracts Spinal CordDocument1 pageAscending Tracts Spinal CordChristopher Samuel0% (1)
- PHYSIO Samplex Motor SystemDocument42 pagesPHYSIO Samplex Motor SystemMelissa SalayogNo ratings yet
- Chapter 34 Guyton and HallDocument5 pagesChapter 34 Guyton and Hallg_komolafeNo ratings yet
- Physiology Summary Chapter 21Document5 pagesPhysiology Summary Chapter 21gail018No ratings yet
- Physio Blood TransDocument7 pagesPhysio Blood TransRoderick PalattaoNo ratings yet
- Diploma in Occupational TherapyDocument47 pagesDiploma in Occupational TherapyAzmi Plus100% (2)
- 21-Spinal Cord TractsDocument23 pages21-Spinal Cord TractsALFAHRUL CAHYADINo ratings yet
- St. Anthony College of Roxas City, Inc.: Diagnostic Examination: Anatomy & Physiology December 15, 2018Document6 pagesSt. Anthony College of Roxas City, Inc.: Diagnostic Examination: Anatomy & Physiology December 15, 2018JoherNo ratings yet
- Anatomy MnemonicsDocument51 pagesAnatomy MnemonicsDrKhawarfarooq SundhuNo ratings yet
- MOCK QUIZ - Head & Neck EmbryoDocument3 pagesMOCK QUIZ - Head & Neck EmbryoLanz RomuloNo ratings yet
- Key of SEQs Heart, Nerve and Muscle Revision TestDocument11 pagesKey of SEQs Heart, Nerve and Muscle Revision TestMudassar Roomi100% (2)
- PHYSIO Prelims SamplexDocument11 pagesPHYSIO Prelims SamplexCarlos NiñoNo ratings yet
- F.1 - Respiratory Physio (For Quiz Muna)Document7 pagesF.1 - Respiratory Physio (For Quiz Muna)Mac Vince HipolitoNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument4 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- Trans of Harper's Illustrated Biochemistry CH 32Document3 pagesTrans of Harper's Illustrated Biochemistry CH 32Richelle Dianne Ramos-Giang100% (1)
- Practicals Histology Prelims ADocument36 pagesPracticals Histology Prelims AShaylla BretañaNo ratings yet
- Limbs 1b - Overview of Anatomy of Upper and Lower LimbsDocument5 pagesLimbs 1b - Overview of Anatomy of Upper and Lower LimbsTarmizi Md NorNo ratings yet
- Histology of Nervous Tissue and Medulla SpinalisDocument32 pagesHistology of Nervous Tissue and Medulla SpinalisSuhas Kapse100% (1)
- Tips For Ust Med FreshmenDocument3 pagesTips For Ust Med FreshmenFred EvidorNo ratings yet
- Lec - 1H - Special Senses System ReviewerDocument18 pagesLec - 1H - Special Senses System ReviewerProfessor GhoulNo ratings yet
- Essentials of Anatomy & Physiology: The SensesDocument22 pagesEssentials of Anatomy & Physiology: The SensesKBS100% (1)
- Gross Anatomy-Review NotesDocument56 pagesGross Anatomy-Review NotesJohnNo ratings yet
- (PHY) 3.03 Mechanical Properties of The Heart - Dr. JerezDocument12 pages(PHY) 3.03 Mechanical Properties of The Heart - Dr. JerezKate Lynne CamonayanNo ratings yet
- Guyton Hall PHYSIOLOGY Chapter 1 PDFDocument3 pagesGuyton Hall PHYSIOLOGY Chapter 1 PDFOsman NazirNo ratings yet
- Lesion Localization in NeurologyDocument34 pagesLesion Localization in NeurologyValeria Leon AbadNo ratings yet
- Physiology of ANS Lecture 1 by Dr. Mudassar Ali RoomiDocument19 pagesPhysiology of ANS Lecture 1 by Dr. Mudassar Ali RoomiMudassar RoomiNo ratings yet
- Physiology 100q.with TopicsDocument11 pagesPhysiology 100q.with TopicsdocaliNo ratings yet
- Physiology: Block 1Document3 pagesPhysiology: Block 1Mavic VillanuevaNo ratings yet
- Histology Finals Quiz 2Document15 pagesHistology Finals Quiz 2RYABELLE JESUSA SANCHEZNo ratings yet
- Riverside College, Inc. Department of Physical Therapy Physiology01 Module 4 Lesson 3 Autonomic Nervous SystemDocument8 pagesRiverside College, Inc. Department of Physical Therapy Physiology01 Module 4 Lesson 3 Autonomic Nervous SystemNeonil Dequina CaceresNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- 01 - Overview of The Cardiovascular Physiology - ACPDocument6 pages01 - Overview of The Cardiovascular Physiology - ACPMavic VillanuevaNo ratings yet
- Physiology: Block 1Document3 pagesPhysiology: Block 1Mavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument4 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument4 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- Physiology: Table 1. Distinguishing Properties of Electrical and Chemical SynapsesDocument5 pagesPhysiology: Table 1. Distinguishing Properties of Electrical and Chemical SynapsesMavic VillanuevaNo ratings yet
- 08.17.2015 - Physiology - Lecture10 - ARN (EA)Document3 pages08.17.2015 - Physiology - Lecture10 - ARN (EA)Mavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: Block 1Document9 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: Block 1Mavic Villanueva100% (1)
- St. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: PhysiologyMavic VillanuevaNo ratings yet
- 08.17.15 - Histology Lab Epithelial Tissues and Skin Session01Document11 pages08.17.15 - Histology Lab Epithelial Tissues and Skin Session01Mavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: Block 1 Lab Session: 1 Facilitator: Dr. Arturo DecanoDocument11 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: Block 1 Lab Session: 1 Facilitator: Dr. Arturo DecanoMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha MemorialDocument3 pagesSt. Luke's College of Medicine - William H. Quasha MemorialMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument6 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument7 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument2 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- 08.05.15 - Histology Lab Muscles Bones Cartilages Session01Document13 pages08.05.15 - Histology Lab Muscles Bones Cartilages Session01Mavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: EmbryologyDocument23 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: EmbryologyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: I. A. 1. 2. 3. B. 1. I. Ii. 2. C. 1. 2. 3. II. Iii. ADocument7 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: I. A. 1. 2. 3. B. 1. I. Ii. 2. C. 1. 2. 3. II. Iii. AMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument3 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument10 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument4 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument6 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- General Pathology Supertrans Block 1Document10 pagesGeneral Pathology Supertrans Block 1Mavic VillanuevaNo ratings yet
- Basic Science Research: Lecture 1: Post-Ischemic Neovascularization and Blood FlowDocument3 pagesBasic Science Research: Lecture 1: Post-Ischemic Neovascularization and Blood FlowMavic VillanuevaNo ratings yet
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocument7 pagesSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaNo ratings yet
- BSR Supertrans Block 2Document9 pagesBSR Supertrans Block 2Mavic VillanuevaNo ratings yet
- Mindfulness in Primary School Children ADocument15 pagesMindfulness in Primary School Children AMuhammad Irfan AneesNo ratings yet
- Consumer Markets andDocument35 pagesConsumer Markets andanon_159262080100% (1)
- Lesson 4 Module Title: Leadership TrainingDocument8 pagesLesson 4 Module Title: Leadership TrainingAnamae Detaro DarucaNo ratings yet
- Advances in Scanning Force Microscopy For Dimensional MetrologyDocument38 pagesAdvances in Scanning Force Microscopy For Dimensional MetrologyDiana Alejandra Bermudez FajardoNo ratings yet
- Colloquia Latina D Ooge PDFDocument104 pagesColloquia Latina D Ooge PDFHadaixx100% (1)
- Urban Design Assessment ReyesJanMerckM. 4BDocument17 pagesUrban Design Assessment ReyesJanMerckM. 4BREYES, JAN MERCK M.No ratings yet
- SSTMZG528: Assignment 1Document4 pagesSSTMZG528: Assignment 1D V BHASKARNo ratings yet
- Us Navy Flight Test ManualDocument881 pagesUs Navy Flight Test ManualDavid Russo100% (8)
- D375A-6 Cooling SystemDocument26 pagesD375A-6 Cooling Systemalcowo100% (3)
- Case Study in Architectural Structures: A-7E Avionics System - ADocument36 pagesCase Study in Architectural Structures: A-7E Avionics System - Ajckz8No ratings yet
- Compresor Atlas Copco GA30Document16 pagesCompresor Atlas Copco GA30Florin Maria Chirila100% (1)
- Atq Experiment 8 Chem 261 PDF FreeDocument7 pagesAtq Experiment 8 Chem 261 PDF FreeAliNo ratings yet
- Ancient Norse RunesDocument19 pagesAncient Norse Runess_avgerNo ratings yet
- CRSQ 1984 Volume 21 Number 3 PDFDocument60 pagesCRSQ 1984 Volume 21 Number 3 PDFCole ThompsonNo ratings yet
- Morphology and Culture - MoldsDocument8 pagesMorphology and Culture - Moldslisa.angle204No ratings yet
- Lab ManualDocument12 pagesLab ManualAsad KhalidNo ratings yet
- Parts of Speech (Updated) - 1Document33 pagesParts of Speech (Updated) - 1Ramzan MemonNo ratings yet
- Textbook of Respiratory Disease in Dogs and Cats Diaphragmatic HerniaDocument9 pagesTextbook of Respiratory Disease in Dogs and Cats Diaphragmatic HerniaDiego CushicóndorNo ratings yet
- Technology Can Provide Much-Needed SupportDocument3 pagesTechnology Can Provide Much-Needed SupportPaz MoscosoNo ratings yet
- Book 2 - Chapter 24 - Project Management ConceptsDocument27 pagesBook 2 - Chapter 24 - Project Management ConceptsTariq Ali SumalaniNo ratings yet
- Fib Congress Freyssinet by ShushkewichDocument28 pagesFib Congress Freyssinet by ShushkewichpablokrahlNo ratings yet
- HBSC1203 V2Document6 pagesHBSC1203 V2TAY JIUN HOANG MoeNo ratings yet
- Resume For Restaurant WaitressDocument8 pagesResume For Restaurant Waitresszpaaedifg100% (2)
- Explosive Strength Program-McCraneDocument17 pagesExplosive Strength Program-McCraneJusuf AlajbegovicNo ratings yet
- Decay Heat CalculationDocument12 pagesDecay Heat CalculationUdit OjhaNo ratings yet
- Geography: (Mains) Question Paper 1988 Paper - IDocument3 pagesGeography: (Mains) Question Paper 1988 Paper - INakka JaswanthNo ratings yet
- Fm-npd-16 (Temp. Change Request Note)Document1 pageFm-npd-16 (Temp. Change Request Note)akash.vd.1603No ratings yet
- Consumer Perception Icici Bank SynopsisDocument8 pagesConsumer Perception Icici Bank Synopsisbantu121No ratings yet
- Chapter 23 Seatwork KEYDocument4 pagesChapter 23 Seatwork KEYJayvee M FelipeNo ratings yet
- Improved HSe Profile of Green StimulationDocument6 pagesImproved HSe Profile of Green StimulationwasayrazaNo ratings yet