Professional Documents
Culture Documents
Hyperphosphataemia PDF
Uploaded by
Mohamed Abbas0 ratings0% found this document useful (0 votes)
13 views1 pageOriginal Title
Hyperphosphataemia.pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
13 views1 pageHyperphosphataemia PDF
Uploaded by
Mohamed AbbasCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 1
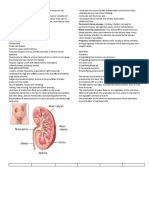
(i) renal failure
- most common cause
- causes hyperphosphataemia because the renal excretion by
the kidneys is impaired
(i) limit phosphate intake - serum phosphate is usually normal until the creatinine clearance
(ii) enhance urinary phosphate excretion is less than 30ml/min
- in the absence of end stage renal disease, phosphate excretion (ii) increased renal resorption
can be optimised with saline infusion and diuretics - hypoparathyroidism
- diuretics that work on the proximal tubule such as acetazolamide causes - thyrotoxicosis
are particularly effective for enhancing phosphate excretion (iii) cellular injury with release of phosphate
- any patient with life threatening hyperphosphataemia should receive dialysis - tumour lysis syndrome
(iii) oral phosphate binders hyperphosphataemia - rhabdomyolysis
- calcium and aluminium salts are widely used; however calcium salts may produce treatment - haemolysis
metastatic calcification and aluminium salts are toxic.
[created by Paul (iv) medication related
- in dialysis patients, chronic management with calcium free phosphate binders such Young 17/12/07] - abuse of phosphate containing laxatives
as sevelamer hydrochloride may reduce long-term mortality by preventing long-term - excessive phosphate administration
cardiovascular complications associated with a high calcium phosphorus product - bisphosphonate therapy
NB: in the acute management of patients with hyperphosphataemia accompanied
by hypocalcaemia, the likelihood and clinical significance of metastatic calcification - most manifestations are due to associated hypocalcaemia which is produced by
with acute calcium administration is unclear (i) precipitation with calcium (leading to nepholithiasis)
(ii) interference with parathyroid hormone-mediated resorption of bone
manifestations (iii) decreased vitamin D levels
- manifestations of hypocalcaemia include muscle cramping, tetany,
hyperreflexia and seizures as well as cardiovascular manifestations
You might also like
- HYPERPARATHYROIDISMDocument1 pageHYPERPARATHYROIDISMPhilip Gene II MalacasNo ratings yet
- HypophosphatemiaDocument26 pagesHypophosphatemiaOxy GenNo ratings yet
- ElectrolyteDocument4 pagesElectrolyteRon Vien'sNo ratings yet
- Calcium Metabolism in Renal Failure: York, New YorkDocument9 pagesCalcium Metabolism in Renal Failure: York, New Yorkstella pangestikaNo ratings yet
- Electrolyte Imbalances 103123Document14 pagesElectrolyte Imbalances 103123grazelantonette.calubNo ratings yet
- Chronic Kidney Disease: Uremia SyndromeDocument8 pagesChronic Kidney Disease: Uremia SyndromeMartien Silviandy SetiawanNo ratings yet
- Group 11 Hyperphosphatemia HandoutsDocument2 pagesGroup 11 Hyperphosphatemia HandoutsRisha Ethel BerondoNo ratings yet
- Veterinary Clinics: Phosphorus: A Quick ReferenceDocument5 pagesVeterinary Clinics: Phosphorus: A Quick ReferenceDanilo JimenezNo ratings yet
- Causes of Acute Renal FailureDocument11 pagesCauses of Acute Renal FailureAndrea Roman chavezNo ratings yet
- Kahoots 8 - Renal Physiology PDFDocument3 pagesKahoots 8 - Renal Physiology PDFJoshua LanzonNo ratings yet
- Hypernatremia From HarrisonDocument3 pagesHypernatremia From HarrisonNobel LaureateNo ratings yet
- Parathyroi D HormoneDocument25 pagesParathyroi D HormoneChatie PipitNo ratings yet
- Hypo Phosphate MiaDocument15 pagesHypo Phosphate Miacute_maimaiNo ratings yet
- Calcium Homeostasis: HypocalcemiaDocument4 pagesCalcium Homeostasis: Hypocalcemia075 Keerthighaa SNo ratings yet
- Calcium Metabolism (PTH, Vitamin D, and Calcitonin)Document4 pagesCalcium Metabolism (PTH, Vitamin D, and Calcitonin)Saima SiddiqiNo ratings yet
- Hypercalcemia (F&e)Document3 pagesHypercalcemia (F&e)Sarah Grace CajucomNo ratings yet
- RicketsDocument3 pagesRicketsSaloni GanganNo ratings yet
- HypoparathyroidismDocument2 pagesHypoparathyroidismLorelyn Santos CorpuzNo ratings yet
- Lange Nephrology EssentialsDocument9 pagesLange Nephrology EssentialsAlejandro GarcíaNo ratings yet
- Acute Renal FailureDocument25 pagesAcute Renal FailurenyarieNo ratings yet
- CKD Pead IllustratedDocument3 pagesCKD Pead IllustratedakeelNo ratings yet
- Parathyroid Gland AnatomyDocument27 pagesParathyroid Gland AnatomyABUBEKER BESHIRNo ratings yet
- Rta PDFDocument4 pagesRta PDFtraceyNo ratings yet
- APNC 520 Exam 10 Study Guide Musculoskeletal DisordersDocument15 pagesAPNC 520 Exam 10 Study Guide Musculoskeletal DisordersMariaNo ratings yet
- CC Lec Mod 3Document13 pagesCC Lec Mod 38wgmhh9ks9No ratings yet
- Nephrolithiasis: Grade A ReferencesDocument8 pagesNephrolithiasis: Grade A ReferencesEngin AltınkayaNo ratings yet
- Hypo Phosphate MiaDocument7 pagesHypo Phosphate MiaChristian Manuel Chiara ChiletNo ratings yet
- Renal Stone Types, Causes and SymptomsDocument29 pagesRenal Stone Types, Causes and Symptomsarim100% (1)
- Rickets in ChildrenDocument61 pagesRickets in ChildrenmdNo ratings yet
- Diuretics Module - Promote Excretion of Water and ElectrolytesDocument7 pagesDiuretics Module - Promote Excretion of Water and ElectrolytesBenzy Anne MermalNo ratings yet
- Rickets Metabolic Bone DiseasesDocument61 pagesRickets Metabolic Bone DiseasesKrameshNo ratings yet
- Acute Renal FailureDocument6 pagesAcute Renal FailureFrancine Kyle SusanoNo ratings yet
- Anemia and Hematologic Drugs - KatzungDocument4 pagesAnemia and Hematologic Drugs - Katzungsarguss14100% (1)
- Pediatrics DiseaseDocument7 pagesPediatrics DiseaseHaslam UdaraniNo ratings yet
- Phosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaDocument5 pagesPhosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaMahipal Reddy NimmalaNo ratings yet
- 2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportDocument2 pages2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportHany Elbarougy0% (1)
- SAJAA (V27) p126-130 2691 FCA SupplementDocument5 pagesSAJAA (V27) p126-130 2691 FCA SupplementVivek PatangeNo ratings yet
- Rickets: Causes, Symptoms, Diagnosis and TreatmentDocument49 pagesRickets: Causes, Symptoms, Diagnosis and TreatmentMis Bah100% (1)
- SodiumDocument3 pagesSodiumEmily FernandezNo ratings yet
- Chronic Kidney DiseaseDocument4 pagesChronic Kidney DiseaseImnot YouNo ratings yet
- FLUID, ELECTROLYTES AND ACID BASE IMBALANCESDocument2 pagesFLUID, ELECTROLYTES AND ACID BASE IMBALANCESSamantha BolanteNo ratings yet
- Calicum Metabolisim DisoodersDocument12 pagesCalicum Metabolisim DisoodersDr-Dalya ShakirNo ratings yet
- Urolithiasis: ObjectivesDocument11 pagesUrolithiasis: ObjectivesOkki Masitah Syahfitri NasutionNo ratings yet
- Labs UgibDocument4 pagesLabs UgibRomwella May AlgoNo ratings yet
- Pharmacology Final TermDocument19 pagesPharmacology Final TermDWIGHT LESTER O. MANGILANo ratings yet
- Parathyroid Glands: Hyperparathyroidism and HypoparathyroidismDocument3 pagesParathyroid Glands: Hyperparathyroidism and HypoparathyroidismStrong Woman Bong SoonNo ratings yet
- HEPATOBILIARYDocument6 pagesHEPATOBILIARYjsreyes.402No ratings yet
- Rickets, Osteomalacia and Renal OsteodystrophyDocument13 pagesRickets, Osteomalacia and Renal Osteodystrophyesther_aprilNo ratings yet
- Chronic Renal FailureDocument54 pagesChronic Renal Failuresanjivdas100% (3)
- Kidney DiseaseDocument10 pagesKidney Disease42tdgcrpxhNo ratings yet
- د.وليد سعد urineDocument26 pagesد.وليد سعد urineAbdulmalik Al-harthyNo ratings yet
- Acute phosphate nephropathy: causes, pathology, and risk factorsDocument12 pagesAcute phosphate nephropathy: causes, pathology, and risk factorsOlga BabiiNo ratings yet
- 2.nephrotic SyndromeDocument7 pages2.nephrotic SyndromeHemanth PrakashNo ratings yet
- MCEM Toxicology MCQDocument110 pagesMCEM Toxicology MCQAnkita Sinha100% (4)
- Renal Osteodystrophy: From Wikipedia, The Free EncyclopediaDocument5 pagesRenal Osteodystrophy: From Wikipedia, The Free EncyclopediaRandy PangestuNo ratings yet
- Uromodulin-Associated Kidney Disease: Tubular DisorderDocument13 pagesUromodulin-Associated Kidney Disease: Tubular DisorderInah RelucioNo ratings yet
- UROLITHIASISDocument9 pagesUROLITHIASISRimbun SidaurukNo ratings yet
- Hypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- USMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangDocument3 pagesUSMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangMohamed AbbasNo ratings yet
- EMQs in SurgeryDocument25 pagesEMQs in Surgerynob2011nob100% (2)
- Wu Step 2 CK Study PlanDocument5 pagesWu Step 2 CK Study PlanLeti Sefa TaNo ratings yet
- Jason Wolfe's ATLS Trauma Moulage: (Thoughts On The Management of The Multiply Injured Patient)Document22 pagesJason Wolfe's ATLS Trauma Moulage: (Thoughts On The Management of The Multiply Injured Patient)igorNo ratings yet
- USMLE Step 1 FA Rapid Review - Classic - Relevant Treatments (FA 2019) Flashcards - Memorang PDFDocument5 pagesUSMLE Step 1 FA Rapid Review - Classic - Relevant Treatments (FA 2019) Flashcards - Memorang PDFMohamed AbbasNo ratings yet
- USMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangDocument3 pagesUSMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangMohamed AbbasNo ratings yet
- NBME Pediatrics Flashcards - MemorangDocument3 pagesNBME Pediatrics Flashcards - MemorangMohamed AbbasNo ratings yet
- Free Surgery Flashcards About ATLS Chapters 1-3Document3 pagesFree Surgery Flashcards About ATLS Chapters 1-3Mohamed AbbasNo ratings yet
- Cardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangDocument4 pagesCardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangMohamed Abbas0% (2)
- Gynecology GY Emtyaz Quiz JordanDocument40 pagesGynecology GY Emtyaz Quiz JordanVicviclookThekingNo ratings yet
- USMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangDocument8 pagesUSMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangMohamed AbbasNo ratings yet
- Surgery NotesDocument2 pagesSurgery NotesChristopher Garrett100% (1)
- Revision Notes Psychiatry PDFDocument613 pagesRevision Notes Psychiatry PDFAshbirZammeri100% (4)
- NATIONAL BOARD OF EXAMINATIONS FMGE RESULTS DECEMBER 2019Document105 pagesNATIONAL BOARD OF EXAMINATIONS FMGE RESULTS DECEMBER 2019Mohamed AbbasNo ratings yet
- Closing Ranks R1 2019 - Complete Info PDFDocument161 pagesClosing Ranks R1 2019 - Complete Info PDFAshok Abraham VargheseNo ratings yet
- Surgery - King Faisal Specialist Hospital & Research CentreDocument22 pagesSurgery - King Faisal Specialist Hospital & Research CentreMohamed AbbasNo ratings yet
- Dr. Dilip COVID19 in ICUDocument22 pagesDr. Dilip COVID19 in ICUMohamed AbbasNo ratings yet
- Selective Digestive Decontamination PDFDocument1 pageSelective Digestive Decontamination PDFMohamed AbbasNo ratings yet
- Gynecology GY Emtyaz Quiz JordanDocument40 pagesGynecology GY Emtyaz Quiz JordanVicviclookThekingNo ratings yet
- Dr. Heba Ahmed Taher Head Dermatologist Job DescriptionDocument2 pagesDr. Heba Ahmed Taher Head Dermatologist Job DescriptionMohamed AbbasNo ratings yet
- Gynecology and ObstetricsDocument10 pagesGynecology and ObstetricsMohamed AbbasNo ratings yet
- Pregnancy (Y)Document64 pagesPregnancy (Y)Mohamed AbbasNo ratings yet
- Treating multidrug-resistant infections with linezolidDocument1 pageTreating multidrug-resistant infections with linezolidMohamed AbbasNo ratings yet
- Hypoxic Brain Injury PDFDocument1 pageHypoxic Brain Injury PDFMohamed AbbasNo ratings yet
- GeneralDocument1 pageGeneralMohamed AbbasNo ratings yet
- Hyperphosphataemia PDFDocument1 pageHyperphosphataemia PDFMohamed AbbasNo ratings yet
- Periodic ParalysisDocument1 pagePeriodic ParalysisMohamed AbbasNo ratings yet
- Selective Digestive Decontamination PDFDocument1 pageSelective Digestive Decontamination PDFMohamed AbbasNo ratings yet
- Hypoxic Brain Injury PDFDocument1 pageHypoxic Brain Injury PDFMohamed AbbasNo ratings yet
- Molar Pregnancy CaseDocument1 pageMolar Pregnancy CaseJM PunzalanNo ratings yet
- Daftar Stok Slow Moving & Dead Stock Daftar Stok Slow Moving & Dead StockDocument11 pagesDaftar Stok Slow Moving & Dead Stock Daftar Stok Slow Moving & Dead StockFebriyana SalehNo ratings yet
- Questions 5 To 8Document26 pagesQuestions 5 To 8Stefannus Wibisono100% (1)
- Tutorial 1Document16 pagesTutorial 1ronaldo muslimNo ratings yet
- Drug Study AspirinDocument1 pageDrug Study AspirinMaria Charis Anne Indanan100% (1)
- 60 Second EMTDocument29 pages60 Second EMTstripec30No ratings yet
- Cases BSN2-5Document17 pagesCases BSN2-5AnonymousTargetNo ratings yet
- DYHFS10 Cancer Prevention Mar 2005Document2 pagesDYHFS10 Cancer Prevention Mar 2005Ngaire TaylorNo ratings yet
- Torch InfectionsDocument27 pagesTorch InfectionsSimi SaiPrasoonNo ratings yet
- CHN DrugstudyDocument2 pagesCHN DrugstudyNathalie OmalNo ratings yet
- Ped OsceDocument4 pagesPed OsceAJ JeyakumarNo ratings yet
- Skan's Step 3 CocktailDocument82 pagesSkan's Step 3 CocktailVS100% (6)
- FNP Review - AANP Immunization PearlsDocument94 pagesFNP Review - AANP Immunization PearlsJamila Ziyaeva100% (14)
- PATHOGNOMONIC SIGN Is Widely Used in The Field of Medicine For It Gives The Doctors A Hint of The Disease Condition The Client Is ExperiencingDocument3 pagesPATHOGNOMONIC SIGN Is Widely Used in The Field of Medicine For It Gives The Doctors A Hint of The Disease Condition The Client Is ExperiencingTammy Tam100% (1)
- OSCE DermaDocument8 pagesOSCE DermaameerabestNo ratings yet
- Nephrotic SyndromeDocument2 pagesNephrotic SyndromeAnnruby NefielNo ratings yet
- High Yield PediatricsDocument78 pagesHigh Yield Pediatricsjose100% (1)
- Pelvic Inflammatory Disease - Clinical Features - Management - TeachMeObGynDocument4 pagesPelvic Inflammatory Disease - Clinical Features - Management - TeachMeObGynLiridon SopajNo ratings yet
- Symtoms and Signs of The Respiratory SystemDocument33 pagesSymtoms and Signs of The Respiratory SystemmohammedNo ratings yet
- HMIS Data Analysis - 2015 - 16 Karnataka - BangaloreDocument27 pagesHMIS Data Analysis - 2015 - 16 Karnataka - BangaloreholysaatanNo ratings yet
- Abdullah MarfadiDocument12 pagesAbdullah MarfadiZH. omg sarNo ratings yet
- Top-200-Drug ETSYDocument31 pagesTop-200-Drug ETSYBetsy Brown ByersmithNo ratings yet
- Health Problems Sopa de LetrasDocument1 pageHealth Problems Sopa de LetrasJason RojasNo ratings yet
- Govt. medical college Kannauj MCQ's on measlesDocument27 pagesGovt. medical college Kannauj MCQ's on measlesnikhil73% (11)
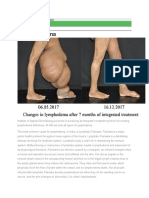
- Integrative Lymphedema Treatment ProtocolDocument7 pagesIntegrative Lymphedema Treatment ProtocolSalamontiey Kit-KatNo ratings yet
- Child Immunization Record: Age in Months Nutrional StatusDocument14 pagesChild Immunization Record: Age in Months Nutrional StatusMa. Jesica Salve LasundinNo ratings yet
- Brochure RotavirusDocument4 pagesBrochure RotavirusMaria Chacón CarbajalNo ratings yet
- Code Product Name ListDocument1,230 pagesCode Product Name ListdomNo ratings yet
- Drug-Study Hepa BDocument2 pagesDrug-Study Hepa BPauline Doronila100% (1)
- Medication dosage and treatment options quizDocument2 pagesMedication dosage and treatment options quizYanyan071680% (10)