Professional Documents
Culture Documents
Activity 2 Case Study of Pneumonia
Uploaded by
Edelweiss Marie CayetanoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Activity 2 Case Study of Pneumonia
Uploaded by
Edelweiss Marie CayetanoCopyright:
Available Formats
CASE STUDY (PNEUMONIA)
HISTORY OF PRESENT ILLNESS:
A 50-year-old female presents after admission to the general medical/surgical hospital ward with a chief complaint of shortness of breath on
exertion. She reports that she was seen for similar symptoms previously at her primary care physician’s office six months ago. At that time,
she was diagnosed with acute bronchitis and treated with bronchodilators, empiric antibiotics, and a short course oral steroid taper. This
management did not improve her symptoms, and she has gradually worsened over six months. She reports a 20-pound intentional weight loss
over the past year. She denies any sick contacts. A brief review of systems is negative for fever, night sweats, palpitations, chest pain, nausea,
vomiting, diarrhea, constipation, abdominal pain, neural sensation changes, muscular changes, and increased bruising or bleeding. She admits
a cough, shortness of breath, and shortness of breath on exertion.
Social History: Her tobacco use is 33 pack-years; however, she quit smoking shortly prior to the onset of symptoms, six months ago. She
denies alcohol and illicit drug use. She is married, in a monogamous relationship, and has three children aged 15 months to 5 years. She is
employed as clinical instructor. She has two pet cats. She loves to travel.
Allergies: No known medicine, food, or environmental allergies.
Past Medical History: Essential Hypertension
Past Surgical History: Appendectomy and CS
Medications: Lisinopril 10mg by mouth every day
Physical Exam:
Vitals: Temperature, 105. F; heart rate 108; respiratory rate, 26; blood pressure 130/86; BMI 26.
General: She is well appearing but anxious, a pleasant female lying on a hospital stretcher. She is conversing freely, with respiratory
distress causing her to stop mid-sentence.
Respiratory: She has diffuse rales and mild wheezing; tachypneic.
Cardiovascular: She has an irregular rate and rhythm with PSVT
Gastrointestinal: Bowel sounds X4. No bruits or pulsatile mass.
INITIAL EVALUATION:
Laboratory Studies: Initial work-up from the emergency department revealed pancytopenia with a platelet count of 74,000 per mm3;
hemoglobin, 8.3 g per and mild transaminase elevation, AST 90 and ALT 112. Blood cultures were drawn and currently negative for
bacterial growth or Gram staining.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
I. PATIENT HISTORY
GENERAL DATA
This is a case of Pneumonia of a 50-year-old female. The patient is admitted to the general medical/surgical hospital with a chief
complaint of shortness of breath on exertion.
PRESENT HEALTH HISTORY
Prior to admission the patient has cough, shortness of breath, and shortness of breath on exertion.
PAST HEALTH HISTORY
Six months ago, the patient reports that she was seen similar symptoms at her primary care physician’s office. At that time, she
was diagnosed with acute bronchitis and treated with bronchodilators, empiric antibiotics, and a short course oral steroid taper.
This management did not improve her symptoms, and she has gradually worsened over six months. She reports a 20-pound
intentional weight loss over the past year.
PAST MEDICAL HISTORY
Essential Hypertension
PAST SURGICAL HISTORY
Appendectomy and CS
NUTRITIONAL HISTORY (ALLERGIES)
No known medicine, food, or environmental allergies.
SOCIAL HISTORY
Her tobacco use is 33 pack-years; however, she quit smoking shortly prior to the onset of symptoms, six months ago. She denies
alcohol and illicit drug use. She is married, in a monogamous relationship, and has three children aged 15 months to 5 years. She
is employed as clinical instructor. She has two pet cats. She loves to travel.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
PATIENT’S HEALTH ASSESSMENT
GENERAL
She is well appearing but anxious, a pleasant female lying on a hospital stretcher. She is conversing freely, with respiratory distress
causing her to stop mid-sentence.
RESPIRATORY
She has diffuse rales and mild wheezing; tachypneic.
CARDIOVASCULAR
She has an irregular rate and rhythm with PSVT
GASTROINTESTINAL
Bowel sounds X4. No bruits or pulsatile mass.
BODY MASS INDEX
Patient is classified as overweight with a BMI of 26.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
VITAL SIGNS
Normal Findings Actual Findings Interpretation
Elevated body temperature is a
sign that there is something
wrong with the body system
Temperature 36.5 – 37.5 oC 40.6 oC and the patient’s fever is due to
her present illness.
Cardiac rate is above normal.
The patient’s cardiac rate can
60 – 100 bpm 108 bpm
reflect exposure to stress and
Cardiac Rate
illness.
Increased respiratory rate. The
Respiratory Rate 12 – 20 bpm 26 bpm patient is experiencing
tachypnea.
Blood Pressure Pre-hypertension is a little
higher blood pressure than it
120/80 130/86 mmHg should be and means that the
patient can possibly develop
high blood pressure.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
II. ANATOMY OF THE AFFECTED ORGAN
The lungs are the major organs of
the respiratory system and are
responsible for performing gas
exchange. The lungs are paired
and separated into lobes; the left
lung consists of two lobes,
whereas the right lung consists of
three lobes. Blood circulation is
very important, as blood is
required to transport oxygen from
the lungs to other tissues
throughout the body. The
function of the pulmonary
circulation is to aid in gas
exchange. The pulmonary artery
provides deoxygenated blood to
the capillaries that form
respiratory membranes with the
alveoli, and the pulmonary veins
return newly oxygenated blood to
the heart for further transport
throughout the body. The lungs
are innervated by the
parasympathetic and sympathetic nervous systems, which coordinate the bronchodilation and bronchoconstriction of the airways. The
lungs are enclosed by the pleura, a membrane that is composed of visceral and parietal pleural layers. The space between these two
layers is called the pleural cavity. The mesothelial cells of the pleural membrane create pleural fluid, which serves as both a lubricant
(to reduce friction during breathing) and as an adhesive to adhere the lungs to the thoracic wall (to facilitate movement of the lungs
during ventilation).
ANNE DOMINIQUE S. LANUZO
BSN – 3A
III. PATHOPHYSIOLOGY
Predisposing Factors Etiology Precipitating Factors
Age Virulent Microorganisms Lifestyle
Sex Streptococcus Pneumoniae Environment
Microorganism enters the nose (nasal passage)
Passes to the pharynx, larynx, trachea
Microorganism enters and affects both airway and lung parenchyma
Airway Damage Lung Invasion
Infiltration of Bronchi Flattening of Eptithelial Cells
ANNE DOMINIQUE S. LANUZO
BSN – 3A
Infectious organism lodges Macrophages and Leukocytes
stimulation in bronchioles
Mucus and phlegm production
Alveolar wall collapse
COUGHING
Increase pyrogen in the body
FEVER
Necrosis of bronchial
tissues
Narrowing of air passage
Infiltration of pulmonary tissues
DIFFICULTY OF BREATHING
Overwhelming sepsis
DEATH
ANNE DOMINIQUE S. LANUZO
BSN – 3A
IV. DIAGNOSTIC TEST
Result Normal Value Unit Remarks
Platelet Count 74,000 150,000 – 400,000 mcL L
Hemoglobin 8.3 (m)13.5 – 17.5 (f) 12.0 – 15.5 g/dL L
AST 90 5 – 40 u/l H
ALT 112 7 – 56 u/l H
Laboratory Studies:
Initial work-up from the emergency department revealed pancytopenia with a platelet count of 74,000 per mm3; hemoglobin, 8.3 g per and
mild transaminase elevation, AST 90 and ALT 112. Blood cultures were drawn and currently negative for bacterial growth or Gram
staining.
Laboratory Interpretation:
Diagnostic test revealed that there is a decreased platelet count and decreased hemoglobin level. The body needs all of these blood cells
to carry oxygen throughout the body and to allow blood to form clots. The result shown that the patient is suffering from pancytopenia
which causes the respiratory distress. Increased aspartate aminotransferase (AST) and alanine aminotransferase (ALT) may mean that
there is some types of liver damage. These enzymes are normally predominantly contained within liver cells and to a lesser degree in
the muscle cells. If the liver is injured or damaged, the liver cells spill these enzymes into the blood, raising the AST and ALT enzyme
blood levels and signaling liver disease. Thus, the exact levels of these enzymes cannot be used to determine the degree of liver disease
or predict the future prognosis of liver function.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
V. MEDICATIONS
MECHANISM OF ADVERSE SPECIAL
DRUG CLASSIFICATION INDICATIONS DOSAGES CONTRAINDICATION
ACTION REACTION PRECAUTION
Lisinopril ACE Mild to Adult: PO As Description: Lisinopril Hypersensitivity to Volume depletion and Hepatic cirrhosis,
Inhibitors/Direct moderate HTN. tab containing competitively inhibits sulphonamide drugs. electrolyte imbalance severe heart failure,
Renin Inhibitors / lisinopril ACE from converting (eg hyperkalaemia); oedema, renal
Diuretics (mg)/hydrochlor angiotensin I to Patients with anuria, dry mouth, thirst; impairment (including
othiazide (mg): angiotensin II resulting aortic stenosis or lethargy, drowsiness; haemodialysis
10/12.5, in increased plasma hyperkalaemia. muscle pain, cramps; patients), unilateral
20/12.5. renin activity and hypotension; renal artery stenosis,
Usual: 1 tab reduced aldosterone History of hypersensitivity hepatic impairment,
once daily, up secretion, causing angioneurotic reactions eg, rashes, diabetes, gout,
to 2 tab once reduced BP and sodium oedema related to use photosensitivity, hyperuricaemia, left
daily if needed. and water retention. of ACE inhibitors. thrombocytopenia, ventricular
Hydrochlorothiazide jaundice, pancreatitis; hypertrophy and/or
increases renal excretion Hereditary or fatigue; weakness; ventricular ectopics
of sodium and chloride idiopathic may precipitate an (extrasystoles),
and reduces cardiac load. angioedema. attack of gout electrolyte
The two drugs exert (hyperuricaemia); disturbances (e.g.
additive effects in Lactation. impotence, hyperkalaemia),
hypertension. hyperglycaemia; collagen vascular
anorexia, gastric disease, valvular
Onset: Lisinopril: 1 hr; irritation, nausea, stenosis, renovascular
hydrochlorothiazide: vomiting, constipation, hypertension,
diuresis: approx 2 hr. diarrhoea; sialadenitis; hypercholesterolemia.
dizziness; Before, during or
Duration: Lisinopril: 24 hypercalcaemia; immediately after
hr; hydrochlorothiazide: headache; cough; anaesthesia; surgery.
6-12 hr. chest pain; Assess renal function
angioneurotic oedema; before initiation.
Pharmacokinetics: occasional increase in Patients with
liver enzymes and hypertension should
serum bilirubin; renal be stabilised on
function deterioration; individual components
alopecia; before starting
oliguria/anuria; combination. Therapy
should not be started
ANNE DOMINIQUE S. LANUZO
BSN – 3A
Absorption: Lisinopril: urticaria, pruritis; after MI if systolic
Well absorbed, diaphoresis. blood pressure <100
unaffected by food; peak Potentially Fatal: mmHg. Hypotension
effect: approx 6 hr. Seizures; cholestatic may occur after initial
Hydrochlorothiazide: jaundice; neutropenia dose in patients who
approx 50-80%; peak and agranulocytosis are hypovolaemic
effect: 4-6 hr. (with or without and/or salt depleted
myeloid hyperplasia); (diuretic should be
Distribution: Plasma acute renal failure, discontinued for 2-3
protein binding: oliguria; progressive days and then
lisinopril: 25%; azotemia; haemolytic lisinopril initiated
hydrochlorothiazide: anaemia; angioedema alone). Discontinue
68%. Distribution of associated with before carrying
hydrochlorothiazide: 3.6- laryngeal oedema. parathyroid function
7.8 L/kg. test.
Metabolism: Lisinopril:
Not significantly
metabolised.
Hydrochlorothiazide:
Not metabolised.
Excretion: Half-life
elimination: lisinopril:
11-12 hr;
hydrochlorothiazide: 5.6-
14.8 hr. Excretion:
lisinopril Mainly via
urine as unchanged drug
(lisinopril and
hydrochlorothiazide).
ANNE DOMINIQUE S. LANUZO
BSN – 3A
VI. NURSING CARE PLAN
NURSING
ASSESSMENT PLANNING INTERVENTION RATIONALE EVALUATION
DIAGNOSIS
Subjective: Ineffective breathing SHORT TERM: Assess and record It is important to take SHORT TERM:
The patient pattern related to respiratory rate and action when there is
complaining of infection/inflammatory After 4 hours of depth at least every 4 After 4 hours of
an alteration in the
shortness of breath at process as evidenced nursing intervention, hours. nursing intervention,
pattern of breathing to
rest and on exertion. by cough, shortness of the patient will be the patient is able to:
detect early signs of
Reports of tobacco breath on exertion, able to: respiratory Maintained an
use for 33 pack/years mild wheezing, and compromise. effective breathing
and quit smoking tachypnea. Maintain an pattern, as
shortly prior effective breathing Assess ABG levels, This monitors evidenced by
to the onset of pattern, as according to facility oxygenation and relaxed breathing
symptoms, six evidenced by policy. ventilation status. at normal rate and
months ago. relaxed breathing depth and absence
at normal rate and Observe for breathing Unusual breathing of dyspnea.
Objective: depth and absence patterns. patterns may imply an Established a
Cough of dyspnea. underlying disease respiratory rate
Mild Wheezing process or that remains within
Tachypnea Establish a dysfunction. normal limits.
Observed to be well respiratory rate that
appearing but anxious remains within Auscultate breath This is to detect
Result of normal limits. sounds at least every decreased or LONG TERM:
electrocardiogram four (4) hours. adventitious breath
that shows irregular sounds. After 1 – 2 days of
rate and rhythm with LONG TERM: nursing intervention,
Paroxysmal Assess for use of Work of breathing the patient is able to:
supraventricular After 1 – 2 days of accessory muscle. increases greatly as
tachycardia (PSVT) nursing intervention, lung compliance
the patient will be decreases.
able to:
ANNE DOMINIQUE S. LANUZO
BSN – 3A
Apply techniques Monitor for Paradoxical Applied
that would improve diaphragmatic muscle movement of the techniques that
breathing pattern. fatigue or weakness abdomen (an inward would improve
(paradoxical motion). versus outward breathing pattern.
Verbalize movement during
awareness of inspiration) is Verbalized
causative factors. indicative of awareness of
respiratory muscle causative factors.
Initiate needed fatigue and weakness.
lifestyle changes. Initiated the
Observe for These signs signify an needed lifestyle
retractions or flaring increase in respiratory changes.
of nostrils. effort.
Place patient with A sitting position
proper body permits maximum
alignment for lung excursion and
maximum breathing chest expansion.
pattern.
Encourage sustained It promotes deep
deep breaths and inspiration, which
educate patient or increases oxygenation
significant other and prevents
proper breathing and atelectasis. Controlled
coughing. breathing methods
may also aid slow
respirations in
patients who are
tachypneic.
Prolonged expiration
prevents air trapping.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
Encourage frequent Extra activity can
rest periods and teach worsen shortness of
patient to pace breath. Ensure the
activity. patient rests between
strenuous activities.
Encourage small This prevents
frequent meals. crowding of the
diaphragm.
Avail a fan in the Moving air can
room. decrease feelings of
air hunger.
ANNE DOMINIQUE S. LANUZO
BSN – 3A
You might also like
- Nursing Care Plan For Myocardial InfarctionDocument7 pagesNursing Care Plan For Myocardial Infarctionmariejo95% (125)
- Chest Drain ManagementDocument7 pagesChest Drain ManagementanuzNo ratings yet
- NCPDocument10 pagesNCPbabycheska08No ratings yet
- Treatment Protocol for Intern DoctorsDocument120 pagesTreatment Protocol for Intern DoctorsGB Majumder100% (1)
- Clinical Transfusion Practice Guidelines For Medical Interns BangladeshDocument42 pagesClinical Transfusion Practice Guidelines For Medical Interns Bangladeshratriprimadiati100% (1)
- Pathophysiology of DMDocument5 pagesPathophysiology of DMRgn Mckl100% (3)
- Philippine Guidelines for Rational Blood UseDocument70 pagesPhilippine Guidelines for Rational Blood Usedebbie o. azcunaNo ratings yet
- Philippine Guidelines for Rational Blood UseDocument70 pagesPhilippine Guidelines for Rational Blood Usedebbie o. azcunaNo ratings yet
- Case Study of BronchoPneumoniaDocument64 pagesCase Study of BronchoPneumoniaJomari Zapanta100% (2)
- Intercostal Drainage and Its ManagementDocument36 pagesIntercostal Drainage and Its ManagementAnusha Verghese67% (3)
- Clopidogrel Drug StudyDocument2 pagesClopidogrel Drug StudyEdelweiss Marie CayetanoNo ratings yet
- Blood Transfusion GuidelineDocument402 pagesBlood Transfusion GuidelineAdam Razi0% (1)
- Discharge Plan Patient Teaching Pleural Effusion CastleDocument6 pagesDischarge Plan Patient Teaching Pleural Effusion Castleapi-341263362100% (2)
- Dr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDocument26 pagesDr. S.K. Haldar's Lectures On Industrial Health For AFIH Students - Occu. Lung Dis Asbestosis Silicosis ByssinosisDr. Prakash Kulkarni100% (2)
- Parapneumonic Effusion - Case Study Adult IDocument59 pagesParapneumonic Effusion - Case Study Adult IJunior Future-Gastroenterologist Henry100% (1)
- Camarines Sur Polytechnic Colleges: Cues/Clues Nursing Diagnosis Plan Intervention Rationale EvaluationDocument8 pagesCamarines Sur Polytechnic Colleges: Cues/Clues Nursing Diagnosis Plan Intervention Rationale EvaluationEdelweiss Marie CayetanoNo ratings yet
- Aspirin Drug StudyDocument2 pagesAspirin Drug StudyEdelweiss Marie CayetanoNo ratings yet
- Final Reqt NCM 109 RLEDocument1 pageFinal Reqt NCM 109 RLEEdelweiss Marie Cayetano0% (1)
- NCP HyperthermiaDocument2 pagesNCP HyperthermiaMeljonesDaanNo ratings yet
- Angel Therisse B. Ramelb BSN Ii-C Nursing DiagnosisDocument2 pagesAngel Therisse B. Ramelb BSN Ii-C Nursing DiagnosisSalvaje CaballeroNo ratings yet
- PA Tool Sample - JIJIDocument35 pagesPA Tool Sample - JIJIJirah RuedasNo ratings yet
- Arixtra Drug StudyDocument2 pagesArixtra Drug StudyEdelweiss Marie Cayetano100% (1)
- Isordil Drug StudyDocument2 pagesIsordil Drug StudyEdelweiss Marie CayetanoNo ratings yet
- Drug Study PostpartumDocument6 pagesDrug Study PostpartumFrederene JavelonaNo ratings yet
- Journal Pcap CDocument3 pagesJournal Pcap CKit LaraNo ratings yet
- Case Study: Obstructive JaundiceDocument11 pagesCase Study: Obstructive JaundiceZhy CaluzaNo ratings yet
- IMCI Learning FeedbackDocument1 pageIMCI Learning Feedbackinah krizia lagueNo ratings yet
- PCAPDocument2 pagesPCAPMizpah DuculanNo ratings yet
- Case Study NCP ActualDocument3 pagesCase Study NCP Actualdhamy florNo ratings yet
- Pregnancy Pressure Leads to Urinary Tract InfectionDocument2 pagesPregnancy Pressure Leads to Urinary Tract InfectionChriz LechNo ratings yet
- Nursing Care Plan For Myasthenia Gravis Assessment Nursing Diagnosis Inference Objectives Nursing Intervention Rationale EvaluationDocument2 pagesNursing Care Plan For Myasthenia Gravis Assessment Nursing Diagnosis Inference Objectives Nursing Intervention Rationale EvaluationJobelle AcenaNo ratings yet
- FDARDocument1 pageFDARSeth Amiel MotaNo ratings yet
- Pedia Care Study - Appendix B - Drug StudyDocument8 pagesPedia Care Study - Appendix B - Drug Studyryan100% (1)
- Republic ActDocument36 pagesRepublic ActjanNo ratings yet
- Ethical Principles for StewardsDocument7 pagesEthical Principles for StewardsElla EllaNo ratings yet
- Ineffective Tissue Perfusion - NCPDocument7 pagesIneffective Tissue Perfusion - NCPVianah Eve EscobidoNo ratings yet
- NeoblocDocument2 pagesNeoblocianecunar100% (2)
- Nueva Ecija University of Science And: O V A ADocument2 pagesNueva Ecija University of Science And: O V A ABeverly DatuNo ratings yet
- Nursing Responsibilities For Oxygen AdministrationDocument3 pagesNursing Responsibilities For Oxygen AdministrationJahseh WolfeNo ratings yet
- Journal Pcap CDocument3 pagesJournal Pcap CKit Lara50% (2)
- Medications To Continue at Home Exercise Treatments Health Teachings Outpatient Diet Sexuality/ SpiritualityDocument2 pagesMedications To Continue at Home Exercise Treatments Health Teachings Outpatient Diet Sexuality/ SpiritualityMae EstilloreNo ratings yet
- Educating HypertensionDocument4 pagesEducating HypertensionMariel GamaloNo ratings yet
- Activity intolerance, fear, infection risks in thalassemiaDocument1 pageActivity intolerance, fear, infection risks in thalassemiaHannah Clarisse Monge IgniNo ratings yet
- Drug Study Pedia WardDocument2 pagesDrug Study Pedia WardCayanne ChuaNo ratings yet
- Sample (Concept Map)Document1 pageSample (Concept Map)NMDNMSSDNo ratings yet
- Concept MapDocument1 pageConcept MapNicole Ivy GorimoNo ratings yet
- NCP & Drug Study (Tondo Med)Document5 pagesNCP & Drug Study (Tondo Med)Kevin_Remollo_2431No ratings yet
- Nursing Care Plan for Fluid Volume DeficitDocument9 pagesNursing Care Plan for Fluid Volume DeficitYesha Mae MartinNo ratings yet
- Simple Schematic Diagram of PneumoniaDocument1 pageSimple Schematic Diagram of PneumoniaJason A. AdoyoganNo ratings yet
- Pharmacologic Class: Contraindications: CNS: Headache, BeforeDocument4 pagesPharmacologic Class: Contraindications: CNS: Headache, BeforeGwyn RosalesNo ratings yet
- Observe Patient's 10 Rights of Medication AdministrationDocument2 pagesObserve Patient's 10 Rights of Medication AdministrationRyan Paul BalotNo ratings yet
- Essential care universally available at affordable cost defined as primary health careDocument11 pagesEssential care universally available at affordable cost defined as primary health careAngelina Janiya NicoleNo ratings yet
- Sodium Bicarbonate Drug StudyDocument3 pagesSodium Bicarbonate Drug StudyShaira Suzane SabidoNo ratings yet
- F&E Drug StudyDocument2 pagesF&E Drug Studychelle_asenjoNo ratings yet
- Drug StudyDocument4 pagesDrug StudyKristine Young100% (1)
- LP2 ncm105Document8 pagesLP2 ncm105Margarette GeresNo ratings yet
- #27 - Web 2.0, Blogs, WikisDocument19 pages#27 - Web 2.0, Blogs, WikisMissy PNo ratings yet
- Evidence Based ActivityDocument3 pagesEvidence Based ActivityRegine CuntapayNo ratings yet
- Reaction to the Black Suede Medical ScandalDocument1 pageReaction to the Black Suede Medical ScandalRej GarbosaNo ratings yet
- Pneumonia Drug StudyDocument3 pagesPneumonia Drug Studyatienza02No ratings yet
- Student Centered Objectives-TicudDocument2 pagesStudent Centered Objectives-TicudFely Theresa Lanes LorenoNo ratings yet
- Prevalence of Bioethical IssuesDocument4 pagesPrevalence of Bioethical IssuesPatricia Jean FaeldoneaNo ratings yet
- NCP Form Hyper ThermDocument1 pageNCP Form Hyper ThermomarskyNo ratings yet
- FDAR (After Tracheostomy)Document2 pagesFDAR (After Tracheostomy)Maribeth DantesNo ratings yet
- DRUG ACTIONDocument3 pagesDRUG ACTIONGwyn RosalesNo ratings yet
- Assessment Nursing Diagnosis Planning Nursing Intervention Rationale EvaluationDocument2 pagesAssessment Nursing Diagnosis Planning Nursing Intervention Rationale EvaluationKenj PereñaNo ratings yet
- Ampicillin 2Document1 pageAmpicillin 2Kristine YoungNo ratings yet
- NCP EsrdDocument2 pagesNCP EsrdAziil LiizaNo ratings yet
- Resource Unit On Common Drugs (LRDR Rotation)Document37 pagesResource Unit On Common Drugs (LRDR Rotation)kiamoiNo ratings yet
- Lifestyle Modification: Asterlyn T. Coniendo Bsn-IvDocument4 pagesLifestyle Modification: Asterlyn T. Coniendo Bsn-IvAsterlyn ConiendoNo ratings yet
- Table 4.2 and 4.3 q1Document4 pagesTable 4.2 and 4.3 q1JOVEMEA LIRAYNo ratings yet
- Nursing Care Plan for Hypertension ManagementDocument5 pagesNursing Care Plan for Hypertension Managementbhavana100% (1)
- Introduction Case StudyDocument10 pagesIntroduction Case StudyJoshua VillarbaNo ratings yet
- Drug Study Pen G FuroDocument3 pagesDrug Study Pen G Furokuro hanabusaNo ratings yet
- Tramadol Drug StudyDocument4 pagesTramadol Drug StudyJust A Nsg StudentNo ratings yet
- What Is Tonsillitis?: City of Malolos, BulacanDocument7 pagesWhat Is Tonsillitis?: City of Malolos, BulacanElijah AmbeguiaNo ratings yet
- Im Case Study 04Document49 pagesIm Case Study 04Shaine BalverdeNo ratings yet
- Drug Name Mechanism of Action Indication Contraindication Adverse Effect Nursing ResponsibilitiesDocument4 pagesDrug Name Mechanism of Action Indication Contraindication Adverse Effect Nursing Responsibilitiesangel cenaNo ratings yet
- COPD - Case PresentationDocument68 pagesCOPD - Case PresentationJaslir MendozaNo ratings yet
- CASE STUDY PheumoniaDocument5 pagesCASE STUDY PheumoniaEdelweiss Marie CayetanoNo ratings yet
- Nursing Care Plan For Myocardial InfarctionDocument6 pagesNursing Care Plan For Myocardial InfarctionEdelweiss Marie CayetanoNo ratings yet
- Case StudyDocument21 pagesCase StudyEdelweiss Marie CayetanoNo ratings yet
- Losartan Drug StudyDocument1 pageLosartan Drug StudyEdelweiss Marie CayetanoNo ratings yet
- What Documents Do You Need After A Blood Transfusion?: BT Checklist 1Document5 pagesWhat Documents Do You Need After A Blood Transfusion?: BT Checklist 1Edelweiss Marie CayetanoNo ratings yet
- Assessment of Hematologic Function and Treatment Modalities Assessment of Hematologic Function and Treatment ModalitiesDocument26 pagesAssessment of Hematologic Function and Treatment Modalities Assessment of Hematologic Function and Treatment ModalitiesEdelweiss Marie CayetanoNo ratings yet
- Drug Study on Aminophylline and AlbuterolDocument7 pagesDrug Study on Aminophylline and AlbuterolEdelweiss Marie CayetanoNo ratings yet
- Social Inclusion of Older Adults in Care: Is It Just A Question of Providing Activities?Document11 pagesSocial Inclusion of Older Adults in Care: Is It Just A Question of Providing Activities?Edelweiss Marie CayetanoNo ratings yet
- Case Study NCM 112 RLEDocument2 pagesCase Study NCM 112 RLEEdelweiss Marie CayetanoNo ratings yet
- Monica Velarde Behind The ScrubsDocument25 pagesMonica Velarde Behind The ScrubsEdelweiss Marie CayetanoNo ratings yet
- CAYETANOEMC BRONCHIAL ASTHMACOPDscenario1Document4 pagesCAYETANOEMC BRONCHIAL ASTHMACOPDscenario1Edelweiss Marie CayetanoNo ratings yet
- Case Study 2Document2 pagesCase Study 2Edelweiss Marie CayetanoNo ratings yet
- PlatoDocument6 pagesPlatoEdelweiss Marie CayetanoNo ratings yet
- Case Study 2Document2 pagesCase Study 2Edelweiss Marie CayetanoNo ratings yet
- Health Care Delivery and Evidence-Based Nursing Practice Health Care Delivery and Evidence-Based Nursing PracticeDocument24 pagesHealth Care Delivery and Evidence-Based Nursing Practice Health Care Delivery and Evidence-Based Nursing PracticeEdelweiss Marie CayetanoNo ratings yet
- CasestudyDocument2 pagesCasestudyEdelweiss Marie CayetanoNo ratings yet
- DocumentDocument1 pageDocumentEdelweiss Marie CayetanoNo ratings yet
- Functions of Monosaccharides and Effects of AldoseDocument5 pagesFunctions of Monosaccharides and Effects of AldoseEdelweiss Marie CayetanoNo ratings yet
- Lower Resp TractDocument32 pagesLower Resp TractTakshikaNo ratings yet
- Ko 2020Document48 pagesKo 2020npr00No ratings yet
- Pleural Effusion PatophysiologyDocument2 pagesPleural Effusion PatophysiologyDivine LavaNo ratings yet
- Understanding Pneumothorax PathophysiologyDocument8 pagesUnderstanding Pneumothorax PathophysiologyKyle FernandezNo ratings yet
- Emergency Chest ImagingDocument156 pagesEmergency Chest ImagingAshutosh KafleNo ratings yet
- Chest Tube Drainage System SetupDocument5 pagesChest Tube Drainage System SetupDan Dan ManaoisNo ratings yet
- Hafizah Hoshni PneumothoraxDocument47 pagesHafizah Hoshni PneumothoraxhafizahhoshniNo ratings yet
- Interpreting Pleural Fluid Results 2019Document5 pagesInterpreting Pleural Fluid Results 2019Anthony Jason Castro JustinianoNo ratings yet
- Tes Lab RespiratoryDocument80 pagesTes Lab RespiratoryShandy BethanNo ratings yet
- NCP (Innefective Breathing Pattern)Document3 pagesNCP (Innefective Breathing Pattern)Ghale Annetoinette ReyesNo ratings yet
- Respiratory System...Document145 pagesRespiratory System...Cheghe PerezNo ratings yet
- Ocean BlueHandbook 010140Document40 pagesOcean BlueHandbook 010140huwahuNo ratings yet
- Hemothorax - Background, Anatomy, Pathophysiology PDFDocument6 pagesHemothorax - Background, Anatomy, Pathophysiology PDFHendriawan PutraNo ratings yet
- Baseline Vital Signs KeyDocument39 pagesBaseline Vital Signs KeycaputmedusaNo ratings yet
- The LungsDocument6 pagesThe LungsnandaNo ratings yet
- Pleura & LungsDocument36 pagesPleura & LungsSyafi'ie SyukriNo ratings yet
- Physiology of the Pleural Space: Visceral Pleura, Parietal Pleura, and Fluid FormationDocument78 pagesPhysiology of the Pleural Space: Visceral Pleura, Parietal Pleura, and Fluid FormationAhmad RafiqiNo ratings yet
- Chest Tube ManagementDocument27 pagesChest Tube ManagementIanne Merh100% (2)
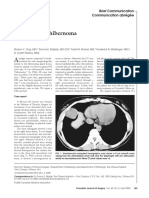
- Intrathoracic Hibernoma: Brief Communication Communication AbrégéeDocument2 pagesIntrathoracic Hibernoma: Brief Communication Communication AbrégéeM Ali AdrianNo ratings yet
- Patho Respiratory - KatherineDocument9 pagesPatho Respiratory - KatherineKayla MayerNo ratings yet
- Understanding Pleural EffusionDocument23 pagesUnderstanding Pleural EffusionYousra ShaikhNo ratings yet
- Shaukat Khanum Memorial Cancer Hospital & Research CentreDocument2 pagesShaukat Khanum Memorial Cancer Hospital & Research CentreMa BeNo ratings yet