Professional Documents
Culture Documents
Disease Summary: Osteoarthritis Disease Summary: Osteoarthritis
Uploaded by
Waseem Khan AfridiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Disease Summary: Osteoarthritis Disease Summary: Osteoarthritis
Uploaded by
Waseem Khan AfridiCopyright:
Available Formats
lOMoARcPSD|845420
Disease summary: Osteoarthritis
Medicine (University of Dundee)
StuDocu is not sponsored or endorsed by any college or university
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
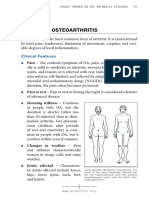
Osteoarthritis
A very common non-inflammatory arthritis, usually affecting the neck, back, hip,
knee, hand and feet joints. It doesn’t spare the DIP joints. It is a degenerative
disease caused by gradual wear and tear of joints loss of cartilage during daily
life.
Aetiology:
Mostly women over the age of 50
Usually primary but can be secondary to
o other joint disease
o obesity
o haemochromatosis
Occupational – heavy lifting, repetitive work
Some forms may have a genetic component
Symptoms:
Gradual onset of mechanical pain (as opposed to inflammatory pain in RA)
o worse on exertion; relieved by rest
o worst at the end of the day
o hip (radiating to groin) and knee pain
Joint stiffness lasting < 30 minutes
Crepitus – grinding/creaking of joints
Swelling
Signs:
Bony enlargements at DIP joints – Heberden’s nodes (think distal – D 2nd)
Bony enlargements at PIP joints – Bouchard’s nodes (think proximal – B 1st)
Squaring of the thumbs
Effusions – particularly knee joint
Baker’s cyst (swelling in popliteal fossa)
Genu varum – bow-legged
Osteophytes – bony projections
Pathophysiology:
Caused primarily by loss of cartilage (mostly type 2 collagen) in the joint cavity.
Mechanical wear and tear triggers inflammation, mediated by cytokines such as TNF
and interleukins. Chronic inflammation causes fibrosis – much of the joint space is
lost to this. Osteoblasts attempt to repair the worn bone, forming osteophytes (bony
spurs) which further reduce the joint space, leading to joint deformity and loss of
function. The bone becomes sclerotic (hardened). In addition, the synovium can
thicken and fluid may escape into the joint cavity, causing effusions.
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
Investigations:
Inflammatory markers – usually normal, but should be done to exclude
inflammatory arthritis
Serum antibodies – again, will be negative for RF, anti-CCP etc.
X-ray is gold standard:
o L – loss of joint space
o O – osteophytes
o S – sclerosis
o S – subchondral cysts
Treatment:
Non-pharmacological
o Physiotherapy to strengthen muscles
o OT – aids, footwear
o Weight loss through low impact exercise
Pharmacological
o Analgesia – paracetamol +/- NSAIDs
o Alternative analgesics – amitriptyline, gabapentin
o IA steroids
All of these are for symptomatic relief only.
Surgery – joint replacement
o may be best way to improve QOL if patient can withstand surgery
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
You might also like
- Osteoarthritis Clinical Pattern Sheet PDFDocument5 pagesOsteoarthritis Clinical Pattern Sheet PDFWaseem Khan AfridiNo ratings yet
- Degenerative Joint Disease: BY: DR Mehrunnisa Umar Assisstant Professor Department of MedicineDocument27 pagesDegenerative Joint Disease: BY: DR Mehrunnisa Umar Assisstant Professor Department of MedicinedrusmanjamilhcmdNo ratings yet
- Arthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR JaneDocument73 pagesArthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR Janeumanantini06No ratings yet
- Osteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRDocument28 pagesOsteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRgita cahayaNo ratings yet
- OsteoarthritisDocument4 pagesOsteoarthritisDharti PatelNo ratings yet
- Osteophytes, Commonly Referred To As Bone Spurs,: Are Projections That Form Along Margins. PathophysiologyDocument1 pageOsteophytes, Commonly Referred To As Bone Spurs,: Are Projections That Form Along Margins. PathophysiologyJoy G. NomilNo ratings yet
- Disorders of BonesDocument3 pagesDisorders of BonesAnonymous 0pSLjJYNo ratings yet
- I. Definition of Disease: Start in The Teens and 20sDocument4 pagesI. Definition of Disease: Start in The Teens and 20sAriaNo ratings yet
- Oestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Document3 pagesOestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Waseem Khan AfridiNo ratings yet
- Osteoarthritis - Dont EraseDocument3 pagesOsteoarthritis - Dont EraseLynlyn AlforqueNo ratings yet
- General Bone DiseasesDocument3 pagesGeneral Bone DiseasesMohamed MahmoudNo ratings yet
- Osteoarthritis & Rheumatoid ArthritisDocument60 pagesOsteoarthritis & Rheumatoid ArthritisSaya MenangNo ratings yet
- Arm:Leg Fracture PDFDocument11 pagesArm:Leg Fracture PDFHannaNo ratings yet
- Muskuloskeletal Disorders: Submitted By: Jho Ann Labor Bsn-Iv Submitted To: Mrs. Dapnhny HatudDocument9 pagesMuskuloskeletal Disorders: Submitted By: Jho Ann Labor Bsn-Iv Submitted To: Mrs. Dapnhny HatudjhoanNo ratings yet
- Osteoarthritis and OsteoporosispptDocument92 pagesOsteoarthritis and OsteoporosispptDian Puspa0% (1)
- OsteoarthritisDocument7 pagesOsteoarthritisWaseem Khan AfridiNo ratings yet
- Discuss Nursing Interventions That Prevent Complications of ImmobilityDocument19 pagesDiscuss Nursing Interventions That Prevent Complications of ImmobilityLilly Ann Vaughan50% (2)
- Skeletal DiseasesDocument3 pagesSkeletal Diseasessweetheart10No ratings yet
- Osteoarthritis: Seti Aji HadinotoDocument48 pagesOsteoarthritis: Seti Aji HadinotoSeti Aji HNo ratings yet
- OSTEOARTHRITISDocument36 pagesOSTEOARTHRITISHzm Mus83% (12)
- Chapter II. OsteoarthritisDocument23 pagesChapter II. OsteoarthritisWilliam C ChishaNo ratings yet
- Osteoarthritis - HarrisonDocument17 pagesOsteoarthritis - HarrisonNovian Adi SaputraNo ratings yet
- X FactorDocument6 pagesX Factorlestari bmNo ratings yet
- Arthritis DR SalmanDocument41 pagesArthritis DR SalmanSaliha AkramNo ratings yet
- Oa OsteoaethritisDocument30 pagesOa Osteoaethritismohamed mowafeyNo ratings yet
- ArthritisDocument6 pagesArthritisChristel Mariz SantellaNo ratings yet
- OsteoarthritisDocument39 pagesOsteoarthritisRohit RajeevNo ratings yet
- ArthritisDocument30 pagesArthritisprasherpratik1984No ratings yet
- OsteoarthritisDocument26 pagesOsteoarthritisRidwan MuttaqinNo ratings yet
- AnatomyDocument10 pagesAnatomyapi-3845840No ratings yet
- Osteoarthritis 191016103144Document49 pagesOsteoarthritis 191016103144dr.abouzaid098No ratings yet
- Rheumatoid Arthritis, Osteoarthritis & GoutDocument51 pagesRheumatoid Arthritis, Osteoarthritis & GoutКеиNo ratings yet
- Assignment: Rheumatoid Arthritis, Osteo-Arthritis & Bone DisordersDocument9 pagesAssignment: Rheumatoid Arthritis, Osteo-Arthritis & Bone DisordersPrabesh PrabeshNo ratings yet
- Degenerative Joint DiseaseDocument5 pagesDegenerative Joint DiseaseskittypieNo ratings yet
- ArthritisDocument57 pagesArthritisSella Septi EkasariNo ratings yet
- 2010 Chapter OsteoarthritisDocument7 pages2010 Chapter OsteoarthritisLizbeth AcevedoNo ratings yet
- ArthritisDocument21 pagesArthritisBasil KuriakoseNo ratings yet
- Ra and Osteoarthritis R IfDocument43 pagesRa and Osteoarthritis R IfsnfhanNo ratings yet
- Introduction To OrthopaedicsDocument42 pagesIntroduction To Orthopaedicsgus_lions100% (1)
- RHEUMA OsteoarthritisDocument4 pagesRHEUMA OsteoarthritisHajime NakaegawaNo ratings yet
- OsteoarthritisDocument23 pagesOsteoarthritisGoutham VGouthamNo ratings yet
- Orthopaedic SlidesDocument163 pagesOrthopaedic SlidesVivian ChepkemeiNo ratings yet
- Muscloskeletal System (Disorders) .Document27 pagesMuscloskeletal System (Disorders) .Younas BhattiNo ratings yet
- OsteoarthritisDocument3 pagesOsteoarthritisVanessa Da CruzNo ratings yet
- Osteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Document64 pagesOsteoarthritis: (Degenerative Arthritis/osteoarthrosis/hypertrophic Arthritis)Linda SugiartoNo ratings yet
- Algodystrophy (AD) : Prof. Hazem Abdel Azeem (MD)Document179 pagesAlgodystrophy (AD) : Prof. Hazem Abdel Azeem (MD)tarikeopsNo ratings yet
- OsteoarthritisDocument10 pagesOsteoarthritisMogtaba M HilalNo ratings yet
- ArthritisDocument54 pagesArthritisPeby M. Ramdhan100% (1)
- OsteoarthritisDocument45 pagesOsteoarthritisMar ClrNo ratings yet
- Diseases and Disorders of The Skeletal SystemDocument11 pagesDiseases and Disorders of The Skeletal SystemJames Roy100% (1)
- Arthritis Joint Pain ReliefDocument14 pagesArthritis Joint Pain ReliefSam CookNo ratings yet
- Disorders of Skeletal SystemDocument24 pagesDisorders of Skeletal SystemAleksa JovanovicNo ratings yet
- Osteoarthritis 1583-170210113823Document34 pagesOsteoarthritis 1583-170210113823Angelic khanNo ratings yet
- Lateral and Medial Epicondylitis-1Document21 pagesLateral and Medial Epicondylitis-1Jalil AhmadNo ratings yet
- Bilateral OsteoarthritisDocument58 pagesBilateral OsteoarthritisMaya VilNo ratings yet
- Review Sistem GerakDocument63 pagesReview Sistem GerakDanur AdiNo ratings yet
- Rheumatoid Disorder Imaging - Refarat Radiologi IkramDocument18 pagesRheumatoid Disorder Imaging - Refarat Radiologi Ikramikram hanafiNo ratings yet
- BONESDocument73 pagesBONESsafa_sabaNo ratings yet
- Dr. Abdul Rashad Senior Lecturer DPT, Mphill (Opt) Mppta United College of Physical TherapyDocument32 pagesDr. Abdul Rashad Senior Lecturer DPT, Mphill (Opt) Mppta United College of Physical Therapypasha100% (1)
- Osteoarthritis Learning Objectives PDFDocument8 pagesOsteoarthritis Learning Objectives PDFWaseem Khan AfridiNo ratings yet
- Oestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Document3 pagesOestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Waseem Khan AfridiNo ratings yet
- Osteoarthritis and Rheumatoid Arthritis in PracticeDocument7 pagesOsteoarthritis and Rheumatoid Arthritis in PracticeWaseem Khan AfridiNo ratings yet
- Comparison of Rheumatoid and OsteoarthritisDocument4 pagesComparison of Rheumatoid and OsteoarthritisWaseem Khan AfridiNo ratings yet
- Osteoarthritis Summary Pathophysiology PDFDocument5 pagesOsteoarthritis Summary Pathophysiology PDFWaseem Khan AfridiNo ratings yet
- Chapter 2. Acute and Chronic InflammationDocument6 pagesChapter 2. Acute and Chronic InflammationWaseem Khan AfridiNo ratings yet
- Osteogenesis Imperfecta: by DR - Naveed Khan Mphil Scholar Oral PathologyDocument20 pagesOsteogenesis Imperfecta: by DR - Naveed Khan Mphil Scholar Oral PathologyWaseem Khan Afridi100% (1)
- Pathology: Osteoarthritis Pathology: OsteoarthritisDocument4 pagesPathology: Osteoarthritis Pathology: OsteoarthritisWaseem Khan AfridiNo ratings yet
- Discussion Osteoarthritis Discussion OsteoarthritisDocument3 pagesDiscussion Osteoarthritis Discussion OsteoarthritisWaseem Khan AfridiNo ratings yet
- OsteoarthritisDocument7 pagesOsteoarthritisWaseem Khan AfridiNo ratings yet
- Dental CariesDocument32 pagesDental CariesWaseem Khan AfridiNo ratings yet
- Intussusception - A Case ReportDocument3 pagesIntussusception - A Case ReportAgustinus HuangNo ratings yet
- Rheumatic FeverDocument21 pagesRheumatic FeverUmar Azlan50% (2)
- 2231 - AMedP-5.1 EDA V1 EDocument52 pages2231 - AMedP-5.1 EDA V1 EDaniel CharlesNo ratings yet
- Relapse PreventionDocument10 pagesRelapse PreventionDawn FarmNo ratings yet
- AAE Position On Vital Pulp Therapy July ProviderDocument8 pagesAAE Position On Vital Pulp Therapy July ProviderSweet ToothNo ratings yet
- Ureteritis Cystica Causing ObstructionDocument2 pagesUreteritis Cystica Causing ObstructionDeba P SarmaNo ratings yet
- Normal Random Blood Sugar - Google SearchDocument1 pageNormal Random Blood Sugar - Google SearchmechNo ratings yet
- Literature Review On UTIDocument31 pagesLiterature Review On UTINishchal Dhakal0% (1)
- UntitledDocument22 pagesUntitledBenjamin Swami100% (7)
- 2Document6 pages2muiNo ratings yet
- History of Toxicity TestingDocument4 pagesHistory of Toxicity TestingIja Nur100% (1)
- Nooriya Prabhakaran Visualcv Resume 2017Document2 pagesNooriya Prabhakaran Visualcv Resume 2017api-372799602No ratings yet
- HSE Commitment and Policy?Document6 pagesHSE Commitment and Policy?radhesrikrishnaNo ratings yet
- Maritime Declaration of Health: Safety Management System FormsDocument2 pagesMaritime Declaration of Health: Safety Management System FormsTJames PaulinNo ratings yet
- EO-GA-32 Continued Response To COVID-19 IMAGE 10-07-2020Document7 pagesEO-GA-32 Continued Response To COVID-19 IMAGE 10-07-2020Jakob RodriguezNo ratings yet
- Star Health and Allied Insurance Company Limited: Customer Information Sheet - Family Health Optima Insurance PlanDocument12 pagesStar Health and Allied Insurance Company Limited: Customer Information Sheet - Family Health Optima Insurance Plananiket goyalNo ratings yet
- A Bump Start.Document3 pagesA Bump Start.Speech & Language Therapy in PracticeNo ratings yet
- The Effects of Sleep Deprivation On Your BodyDocument21 pagesThe Effects of Sleep Deprivation On Your BodyFaradilah Binti Ajma'inNo ratings yet
- Kriyakala AvastaDocument13 pagesKriyakala Avastakundagol100% (1)
- Automation in Pharmacy PDFDocument39 pagesAutomation in Pharmacy PDFanthonyNo ratings yet
- Cultural Perspectives in ChildbearingDocument4 pagesCultural Perspectives in ChildbearingdulceRNNo ratings yet
- Nursing Research: Unit 1Document8 pagesNursing Research: Unit 1KiranNo ratings yet
- Deepak Prasad Kandel SopDocument2 pagesDeepak Prasad Kandel SopromanNo ratings yet
- Nursing Care Plan: Risk For InfectionDocument3 pagesNursing Care Plan: Risk For Infectiongeorgeborja414726100% (3)
- Assessment of Knowledge Attitude and Perception of Dental Students Towards Obesity in Kanpur CityDocument6 pagesAssessment of Knowledge Attitude and Perception of Dental Students Towards Obesity in Kanpur CityAdvanced Research PublicationsNo ratings yet
- Features of CHN: Learning ObjectivesDocument6 pagesFeatures of CHN: Learning ObjectivesAkeroNo ratings yet
- Behcet DiseaseDocument6 pagesBehcet DiseasejbahalkehNo ratings yet
- OT in The ICU Student PresentationDocument37 pagesOT in The ICU Student PresentationMochammad Syarief HidayatNo ratings yet
- Surgery KGMU Proff Chapterwise by Arif Naseem 2009-2021Document4 pagesSurgery KGMU Proff Chapterwise by Arif Naseem 2009-2021DR. PARDEEP SHARMANo ratings yet
- Mitchell H. Katz-Evaluating Clinical and Public Health Interventions - A Practical Guide To Study Design and Statistics (2010)Document176 pagesMitchell H. Katz-Evaluating Clinical and Public Health Interventions - A Practical Guide To Study Design and Statistics (2010)Lakshmi SethNo ratings yet