Professional Documents
Culture Documents
Osteoarthritis Learning Objectives PDF
Uploaded by
Waseem Khan AfridiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Osteoarthritis Learning Objectives PDF
Uploaded by
Waseem Khan AfridiCopyright:
Available Formats
lOMoARcPSD|845420
Osteoarthritis - Learning Objectives
Integrated Pharmacotherapy 1 (Purdue University)
StuDocu is not sponsored or endorsed by any college or university
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
Osteoarthritis
Describe normal joint physiology, etiology, incidence, pathophysiology, clinical
presentation, potential complications and prognosis of OA
o Degenerative changes occur in cartilage and associated bone
o Characterized by increased destruction and subsequent proliferation of
cartilage and bone; regenerated articular surfaces do not possess the
same qualities and architecture as original joint
o Observed more commonly in older patients
Almost 85% of patients older than 75 (severity increases with
age)
Females more at risk than males
o Joints most commonly affected
Distal interphalangeal joint
Hips
Knees
o OA vs. RA
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
o Risk factors for OA
Increasing age
Obesity
Congenital/anatomical defects
Muscle weakness
Female gender
Repetitive stress
Major joint trauma
Heredity
o Clinical Manifestations/Presentation of OA
Pain that worsens w/ activity
AM stiffness is brief (< 1 hour)
Crepitus (crackling sound)
Inflammation is observed in more advanced disease and pain at
rest
Asymmetric involvement
Muscle atrophy
No systemic symptoms
Instability of weight bearing joints
Herberden’s nodes
Bouchard’s nodes
Describe therapeutic use of drugs used to treat OA, including drugs, dosing,
MOAs, place in therapy, adverse effects, warnings & contraindications and
monitoring
o Goals/Desired outcomes of therapy
Relief of pain/discomfort
Maintain function and strength of joint
Prevent deformities and progressive changes
o Step 1: non-pharmacologic therapy
Psychological support & education
Rest, physical activity & exercise
Heat/ice
PT and/or OT
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
Weight loss
o Step 2: pharmacologic therapy
Acetaminophen (2-4 week trial)
MOA: inhibits synthesis of prostaglandins
Dose: 1g q4-6 hours
Max dose: 3g/day
Patients at risk for hepatotoxicity: heavy alcohol intake,
pre-existing liver disease, monitor ALT/AST annually if on
routine doses
Topical Therapy
Menthol/Camphor/Oil of Wintergreen
o Topical counter irritant
o Apply sparingly
o Dose: apply multiple times/day
o Avoid contact with eyes
Capsaicin Cream
o MOA: depletes substance p
o Dose: apply sparingly to affected joints 2-4x/day
o Wait 2-4 weeks to evaluate maximum effect
o Educate patient about proper application
procedures
o Adverse effects: burning, stinging and redness
Diclofenac Topical Gel 1%
o MOA: local inhibition of COX-2 enzymes
o Dose: apply to joint QID, 16g max at any one joint
per day
o Not recommended in combo w/ systemic NSAID
therapy
o Adverse: pruritus, burning, pain & rash
Diclofenac Topical Solution 1.5%
o Dose: 40 drops to each knee QID, apply 10 drops at
a time
o Garlic smell/taste, DMSO vehicle
Glucosamine/Chondroitin
o MOA: stimulate proteoglycan synthesis from
articular cartilage
o Dose
Glucosamine: 500mg PO TID
Chondroitin: 400mg PO TID
o Concern about standardization of products
o Some concern about use in patients with DM, HTN,
hyperlipidemias due to increased insulin
resistance
o Adverse effects: gas, bloating, cramping, nausea
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
o Step 3
NSAIDs
MOA: blocks prostaglandin synthesis by inhibition of COX
enzymes
Selection based on cost, side effects, dosing convenience,
other medical conditions, other meds, risk of bleeding,
risk of peptic ulcer disease (PUD)
Dosing
o Analgesic: 220mg q8-12hrs
o Anti-inflammatory: 440mg q8-12hrs
1-2 week trial for pain and 2-4 week trial if inflammation
exists
Major adverse effects
o GI upset/ulcers
o Bleeding
o Renal dysfunction
o Effects on BP
Patients at greatest risk for ADRs from NSAIDs
o Dose dependent
o Elderly
o History of GI bleed/PUD
o Anticoagulant therapy
o Antiplatelet therapy
o Glucocorticoids
o Patients with CHF, HTN, renal dysfunction and
dehydration are at increased risk of
nephrotoxicity
Monitor
o BP
o Symptoms of edema or weight gain
o BUN/SCr every 3 months
o Hgb/Hct every 6-12 months
o Signs of dehydration
Consider
o COX-2 inhibitor (celecoxib): 100-200mg
o NSAID + PPI: Vimovo (naproxen + esomeprazole)
o NSAID + misoprostol: Arthrotec (Diclofenac +
misoprostol)
Potential benefits of COX-2 inhibitors: once daily dosing
o Lower incidence of severe GI bleeding
Potential risks associated with COX-2 inhibitors
o Increased risk of CV disease
o Increased costs
o Same impact on renal functions and INR
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
o Step 4
Opioid Analgesics
Used PRN for breakthrough pain
Watch total dose of APAP closely
Dosing: start low/go slow, use long acting SR and short
acting IR
Adverse: nausea, somnolence, constipation, dizziness
Tramadol
MOA: affinity for μ receptor; inhibits norepinephrine and
serotonin
Dose: 25-50mg q4-6hrs, max: 400mg/day
Adverse effects/precautions: nausea, vomiting, dizziness
and constipation
Intra-articular corticosteroid injections
Only used for isolated joints
No more often than q4-6 months
Peak pain relief in 7-10 days
Hyaluronate injections
MOA: temporarily increase viscosity of joint
Dose: injected once weekly x3-5 weeks into joint (minor
swelling)
Max benefit in 8-12 weeks
Patients who don’t tolerate other treatments or are not
candidates for surgery
Adverse effects: local, minor swelling
o Step 5
Joint Resurfacing Surgery and Joint Replacement Surgery
Relives pain
Restores function to joint
Monitoring Parameters for Patients with OA
Pain at rest
Joint stability and function
Risk of fall
ROM
X-rays
Degree of disability
Weight
ADRs from medications
Compliance with non-drug measures
QOL issues
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
Develop a pharmacotherapy plan for OA patient, including pharmacologic and
nonpharmacologic therapy, monitoring, expected/desired outcomes & patient
education
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
lOMoARcPSD|845420
Downloaded by Waseem Afridi (cadetwaseem@hotmail.com)
You might also like
- Osteoarthritis and Rheumatoid Arthritis in PracticeDocument7 pagesOsteoarthritis and Rheumatoid Arthritis in PracticeWaseem Khan AfridiNo ratings yet
- Role of Dmards in Ra-Psa-Sp2019Document94 pagesRole of Dmards in Ra-Psa-Sp2019GregNo ratings yet
- Pharm Chapter's Focus Review 2Document16 pagesPharm Chapter's Focus Review 2Briana SmetNo ratings yet
- DRUGS1Document7 pagesDRUGS1Maria Frances Antoniette PerezNo ratings yet
- Edited: DR - Dairion Gatot M.Ked SP - PD-KHOMDocument57 pagesEdited: DR - Dairion Gatot M.Ked SP - PD-KHOMayuhati siregarNo ratings yet
- Polypharmacy and Drug-Drug InteractionsDocument28 pagesPolypharmacy and Drug-Drug Interactionsapi-583778137No ratings yet
- Case 2Document7 pagesCase 2Vineth MartinNo ratings yet
- DR - Girish Meravanige College of Medicine, KFUDocument28 pagesDR - Girish Meravanige College of Medicine, KFUNOT ZUXNo ratings yet
- Steroid GuidelinesDocument5 pagesSteroid GuidelinesAdia MasooraNo ratings yet
- OsteoarthritisDocument0 pagesOsteoarthritisYunita MarwahNo ratings yet
- RHEUMATOLOGY1 - RA Refractory To DMARDsDocument4 pagesRHEUMATOLOGY1 - RA Refractory To DMARDsEunice PalloganNo ratings yet
- MethylprednisoloneDocument4 pagesMethylprednisoloneadryananestesiNo ratings yet
- NDR Vivlodex Project DP 1Document7 pagesNDR Vivlodex Project DP 1api-665600383No ratings yet
- GoutDocument47 pagesGoutsyifasqaNo ratings yet
- PrednisoneDocument3 pagesPrednisoneShaira TanNo ratings yet
- Bays 2016Document13 pagesBays 2016Rosa Gloria GarciaNo ratings yet
- RDU Case On Bone & Joint DisordersDocument22 pagesRDU Case On Bone & Joint DisordersATHENA MINERVA MORDENONo ratings yet
- Merck Manual: Professional VersionDocument9 pagesMerck Manual: Professional VersionDwina Wiranti PutriNo ratings yet
- Medication Card CelebrexDocument2 pagesMedication Card CelebrexTSPAN100% (1)
- TORADOLDocument30 pagesTORADOLb3djo_76No ratings yet
- Musculoskeletal Drugs 2020Document34 pagesMusculoskeletal Drugs 2020Anna Lin YeeNo ratings yet
- Brand Name: Generic Name: Classification: Recommended Dosage, Route, and FrequencyDocument2 pagesBrand Name: Generic Name: Classification: Recommended Dosage, Route, and FrequencyChristine Pialan SalimbagatNo ratings yet
- Drug Used in Orthopedic ConditionsDocument105 pagesDrug Used in Orthopedic ConditionsnavenNo ratings yet
- DactinomycinDocument4 pagesDactinomycinKeith MadarangNo ratings yet
- AmlodipineDocument2 pagesAmlodipineAnonymous QqyLDoW1No ratings yet
- Management of Gout in AdultsDocument3 pagesManagement of Gout in AdultsZubair Mahmood KamalNo ratings yet
- Brand NameDocument8 pagesBrand NameChristine Joy CamachoNo ratings yet
- CortisoneDocument2 pagesCortisoneJulioNo ratings yet
- IT 7 - Gout - RADDocument40 pagesIT 7 - Gout - RADIsal MutaqqienNo ratings yet
- GOUTDocument36 pagesGOUTGanesha Gamma 2017100% (1)
- Corticosteroid Guidelines PDFDocument6 pagesCorticosteroid Guidelines PDFMariskaNo ratings yet
- Naproxen PDFDocument3 pagesNaproxen PDFMichelle EgeraNo ratings yet
- Overview and Recommendations: BackgroundDocument46 pagesOverview and Recommendations: BackgroundRubén Casas BenítezNo ratings yet
- ADPTBDocument41 pagesADPTBHarlinda myraNo ratings yet
- Mat Lecture Otc Meds2Document56 pagesMat Lecture Otc Meds2api-586369243No ratings yet
- Pharmacology HESI Study Guide 2013Document16 pagesPharmacology HESI Study Guide 2013naijababy89100% (12)
- Product Name: New Zealand Data Sheet Apo-PrednisoneDocument13 pagesProduct Name: New Zealand Data Sheet Apo-PrednisonedomNo ratings yet
- Solu-Cortef (Hydrocortisone)Document3 pagesSolu-Cortef (Hydrocortisone)E100% (2)
- Chapter 25 GlucocorticoidsDocument4 pagesChapter 25 GlucocorticoidsRachaelNo ratings yet
- Hyperthyroidism MedicationsDocument7 pagesHyperthyroidism Medicationsamier90No ratings yet
- 596 Ifosfamide Etoposide Ie TherapyDocument6 pages596 Ifosfamide Etoposide Ie Therapyravindra0504090No ratings yet
- Dilcofenac GelDocument23 pagesDilcofenac GelGiulianospharmacyNo ratings yet
- AnalgetikDocument58 pagesAnalgetiksaraswaty710No ratings yet
- Seminar On DMARDSDocument57 pagesSeminar On DMARDSusamadaifallahNo ratings yet
- Amiodarone (PACERONE)Document1 pageAmiodarone (PACERONE)Amanda CoadNo ratings yet
- SR 3Document30 pagesSR 3hussein alnasryNo ratings yet
- Ra OaDocument44 pagesRa OaAgustiantyNo ratings yet
- Temozolomide Adjuvant NHSDocument5 pagesTemozolomide Adjuvant NHSSyed Touseef AhmedNo ratings yet
- Gout and HyperuricemiaDocument41 pagesGout and HyperuricemiaMA 09No ratings yet
- Burchum: Ch. 30, 70, 71, 79, 80 & 81Document79 pagesBurchum: Ch. 30, 70, 71, 79, 80 & 81Mario LemirNo ratings yet
- RX413 Therapeutics 1 Pain Case Fall 2023 KEYDocument4 pagesRX413 Therapeutics 1 Pain Case Fall 2023 KEYrachelmatthews0122No ratings yet
- Clinical Med CardsDocument26 pagesClinical Med CardsLila DanielsNo ratings yet
- Fluorouracil Drug StudyDocument8 pagesFluorouracil Drug StudyAlexandrea MayNo ratings yet
- FLUOROURACIL Drug StudyDocument8 pagesFLUOROURACIL Drug StudyAlexandrea MayNo ratings yet
- VeIP GU TESDocument6 pagesVeIP GU TESMohan KumarNo ratings yet
- Menadment of PainDocument4 pagesMenadment of PainMirza CoricNo ratings yet
- Drugs Related To Male Reproductive System Bsn202n 2Document21 pagesDrugs Related To Male Reproductive System Bsn202n 2Rej hNo ratings yet
- Dr. Joseph P. SibaraniDocument59 pagesDr. Joseph P. SibaraniSarahGultomNo ratings yet
- Oestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Document3 pagesOestoarthritis Oestoarthritis: Physiotherapy (Cardiff University) Physiotherapy (Cardiff University)Waseem Khan AfridiNo ratings yet
- Osteoarthritis Summary Pathophysiology PDFDocument5 pagesOsteoarthritis Summary Pathophysiology PDFWaseem Khan AfridiNo ratings yet
- Osteogenesis Imperfecta: by DR - Naveed Khan Mphil Scholar Oral PathologyDocument20 pagesOsteogenesis Imperfecta: by DR - Naveed Khan Mphil Scholar Oral PathologyWaseem Khan Afridi100% (1)
- Chapter 2. Acute and Chronic InflammationDocument6 pagesChapter 2. Acute and Chronic InflammationWaseem Khan AfridiNo ratings yet
- Comparison of Rheumatoid and OsteoarthritisDocument4 pagesComparison of Rheumatoid and OsteoarthritisWaseem Khan AfridiNo ratings yet
- Osteoarthritis Clinical Pattern Sheet PDFDocument5 pagesOsteoarthritis Clinical Pattern Sheet PDFWaseem Khan AfridiNo ratings yet
- Pathology: Osteoarthritis Pathology: OsteoarthritisDocument4 pagesPathology: Osteoarthritis Pathology: OsteoarthritisWaseem Khan AfridiNo ratings yet
- Disease Summary: Osteoarthritis Disease Summary: OsteoarthritisDocument3 pagesDisease Summary: Osteoarthritis Disease Summary: OsteoarthritisWaseem Khan AfridiNo ratings yet
- Discussion Osteoarthritis Discussion OsteoarthritisDocument3 pagesDiscussion Osteoarthritis Discussion OsteoarthritisWaseem Khan AfridiNo ratings yet
- Dental CariesDocument32 pagesDental CariesWaseem Khan AfridiNo ratings yet
- OsteoarthritisDocument7 pagesOsteoarthritisWaseem Khan AfridiNo ratings yet
- 4.3 Susunan Sistem Saraf, Fgs Sinaps & Substansi TransmitterDocument47 pages4.3 Susunan Sistem Saraf, Fgs Sinaps & Substansi TransmitterindahNo ratings yet
- AM - ICD-10-AM GuideDocument26 pagesAM - ICD-10-AM GuidedrrskhanNo ratings yet
- PneumoniaDocument28 pagesPneumoniaHoward SakalaNo ratings yet
- Myasthenia Gravis Case Study 2Document2 pagesMyasthenia Gravis Case Study 2PJHGNo ratings yet
- 2.plasma ProteinsDocument5 pages2.plasma ProteinsAnusuya SNo ratings yet
- Atlas of Radiology (MODIFIED)Document150 pagesAtlas of Radiology (MODIFIED)sarahhhNo ratings yet
- NeutropeniaDocument12 pagesNeutropeniaTayyeba SyeddainNo ratings yet
- Inv PedDocument21 pagesInv PedGoha BashaNo ratings yet
- Medicine Revision E6.5 (Medicalstudyzone - Com)Document209 pagesMedicine Revision E6.5 (Medicalstudyzone - Com)Diya B johnNo ratings yet
- Sahya Part 4Document116 pagesSahya Part 4Homeopathy Torrents100% (1)
- College Entrance Test Reviewer Source CMU 1Document21 pagesCollege Entrance Test Reviewer Source CMU 1Vhea Czaryse Ibañez LokingNo ratings yet
- Quest Gi Psych LMDocument10 pagesQuest Gi Psych LMtetmetrangmail.com tet101486No ratings yet
- Movie Analysis A Moment To RememberDocument7 pagesMovie Analysis A Moment To RememberJoia De LeonNo ratings yet
- Multiple SclerosisDocument21 pagesMultiple Sclerosisjhodane100% (1)
- Rett SyndromeDocument55 pagesRett SyndromeSnezana MihajlovicNo ratings yet
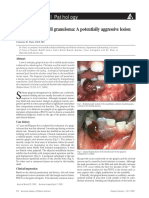
- Peripheral Giant Cell Granuloma: A Potentially Aggressive Lesion in ChildrenDocument2 pagesPeripheral Giant Cell Granuloma: A Potentially Aggressive Lesion in ChildrenYeni PuspitasariNo ratings yet
- Health and Disease Status of Thai Pangas, Bangladesh: Pangasius Hypophthalmus Cultured in Rural Ponds of MymensinghDocument3 pagesHealth and Disease Status of Thai Pangas, Bangladesh: Pangasius Hypophthalmus Cultured in Rural Ponds of MymensinghgooedliaNo ratings yet
- BSBMED301: Assessment 1: What You Have To DoDocument8 pagesBSBMED301: Assessment 1: What You Have To DoPrayas AmatyaNo ratings yet
- BoneDocument5 pagesBoneTaha IsmailNo ratings yet
- Current Clinical Strategies, Critical Care and Cardiac Medicine (2005) BM OCR 7.0-2Document79 pagesCurrent Clinical Strategies, Critical Care and Cardiac Medicine (2005) BM OCR 7.0-2api-3709022100% (2)
- Dermatology QuizDocument10 pagesDermatology QuizSyed Ali Haider0% (1)
- Cancer Chemotherapy: Acronym of RegimenDocument13 pagesCancer Chemotherapy: Acronym of RegimenVaibhav Bharat100% (1)
- Untitled PresentationDocument228 pagesUntitled PresentationSafira WasimNo ratings yet
- Family Names of DrugsDocument1 pageFamily Names of DrugsangelNo ratings yet
- Chapter 28Document13 pagesChapter 28George LeahuNo ratings yet
- Augmentin DdsDocument12 pagesAugmentin DdsQureshi imtiyazNo ratings yet
- Irritablebowelsyndrome: What Treatments Really WorkDocument16 pagesIrritablebowelsyndrome: What Treatments Really WorkTeodora RaindropNo ratings yet
- Acquired CataractDocument39 pagesAcquired CataractRaja Taha Yaseen KhanNo ratings yet
- Endometrial Polyps: MR Imaging Features: Acta Med. Okayama, Vol., No., PPDocument11 pagesEndometrial Polyps: MR Imaging Features: Acta Med. Okayama, Vol., No., PPapache_sp2208465No ratings yet
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (30)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (81)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (5)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisFrom EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisRating: 5 out of 5 stars5/5 (8)
- Empath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainFrom EverandEmpath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainRating: 4 out of 5 stars4/5 (95)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (61)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (60)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (45)