Professional Documents
Culture Documents
Relapsing Polychondritis PDF
Uploaded by
Fazal Dalal0 ratings0% found this document useful (0 votes)
35 views23 pagesRelapsing polychondritis is a multi-system autoimmune disease characterized by recurrent inflammation and deterioration of cartilage. It commonly causes ear inflammation that spares the earlobe, as well as saddle nose deformity from nasal cartilage inflammation. It can also affect the eyes, airways, heart valves, joints, skin and kidneys. Diagnosis requires 3 of 6 criteria including bilateral ear inflammation. Treatment begins with NSAIDs and may include steroids, dapsone or immunosuppressants for refractory cases.
Original Description:
Original Title
Relapsing Polychondritis.pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRelapsing polychondritis is a multi-system autoimmune disease characterized by recurrent inflammation and deterioration of cartilage. It commonly causes ear inflammation that spares the earlobe, as well as saddle nose deformity from nasal cartilage inflammation. It can also affect the eyes, airways, heart valves, joints, skin and kidneys. Diagnosis requires 3 of 6 criteria including bilateral ear inflammation. Treatment begins with NSAIDs and may include steroids, dapsone or immunosuppressants for refractory cases.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
35 views23 pagesRelapsing Polychondritis PDF
Uploaded by
Fazal DalalRelapsing polychondritis is a multi-system autoimmune disease characterized by recurrent inflammation and deterioration of cartilage. It commonly causes ear inflammation that spares the earlobe, as well as saddle nose deformity from nasal cartilage inflammation. It can also affect the eyes, airways, heart valves, joints, skin and kidneys. Diagnosis requires 3 of 6 criteria including bilateral ear inflammation. Treatment begins with NSAIDs and may include steroids, dapsone or immunosuppressants for refractory cases.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 23
Relapsing Polychondritis
Mark Stillwell, MD, FACP
Relapsing Polychondritis- Introduction
• Relapsing Polychondritis- Introduction.....*a multi-system condition
characterized by repeated episodes of inflammation and deterioration
of cartilage, thought to be due to an autoimmune attack on protein
matrix in cartilage, with a component of genetic susceptibility.
• I. A painful disease that can cause joint deformity and be life-
threatening if the respiratory tract, heart valves or blood vessels are
affected.
• II. BOARDS- ***classically causing inflammation of ear (sparing ear
lobe) or nose (resulting in saddle-nose deformity).
Relapsing Polychondritis- Epidemiology
• Relapsing Polychondritis- Epidemiology
• I. Genetic susceptibility
• A. Association with HLA-DR4......56% of patients
• II. Frequent association with immune-mediated connective
tissue/vasculitic (PAN, Wegener’s, Behcet’s, microscopic polyangiitis),
endocrine (e.g. Grave’s disease, Hashimoto’s thyroiditis), inflammatory
bowel disease, myelodysplastic (11%) disorders.
Relapsing Polychondritis- Path
• Relapsing Polychondritis- Path
• I. Both humeral (antibody) and cell-mediated (HLA-DR-positive
antigen-presenting cells and CD4-positive T lymphocytes seen at
lesional areas) autoimmunity to extracellular matrix components of
cartilage such as types II, IX and XI collagen, matrilin and proteoglycan
constituent factors.
• II. Selective decreases in natural killer regulatory T cells (a linage
distinct from traditional NK cells), that normally modulates the
balance of cytokine expression.
• III. Ultimately, there is induction of apoptosis in chondrocytes via
expression of matrix metalloproteinase-3 and cathepsin-K.
Relapsing Polychondritis- Clinical
• Relapsing Polychondritis- Clinical.......it may have either a benign, episodic,
smoldering or fulminant course.
• I. **Ear- unilateral or bilateral external ear inflammation is the most common
presenting sign (90% of patients develop this at some point in time, on primary
presentation in 40%).
• A. Acute or subacute presentation
• B. Pain and tenderness often pronounced, initially often misdiagnosed as
infection.
• C. Diffuse, erythematous or violaceous, sparing non-cartilaginous ear lobes.
• D. Repeated or sustained episodes can cause “floppy ear” or “cauliflower ear.”
• E. 1/3 develop auditory canal/vestibular involvement leading to impaired
hearing, tinnitus, vertigo or destruction of the Eustachian tube. Vasculitis of the
internal auditory artery can cause sensorineural hearing loss.
Acute chondritis of auricle, *spares earlobe
Source: merckmanuals.com
“Cauliflower ear”, a sequela
Source: emedicine.medscape.com
“Floppy ear,” a sequela
Relapsing Polychondritis- Clinical
• Relapsing Polychondritis- Clinical
• II. **Nose- affected in 65% of patients
• A. 25% eventually get saddle-nose deformity due to smoldering or episodic nasal
chondritis. Nasal congestion, decreased sense of smell, crusting, rhinorrhea or epistaxis
can be problematic.......(saddle-nose deformity can also be seen as a sequela of trauma,
radiation therapy, surgery, congenital Syphilis, Wegener’s Granulomatosis, Lepromatous
Leprosy, Crohn’s disease, Down syndrome, Sarcoidosis, malignancy and cocaine abuse)
• III. **Eye- affected in 65% of patients.
• A. Episcleritis
• B. Scleritis
• C. Uveitis
• D. Ulcerative keratitis
• E. “Salmon patch” conjunctival lesion due to reactive lymphoid hyperplasia
• F. Proptosis due to inflammation of the choroid, posterior elements of the globe and
periocular tissues.....can lead to ophthalmoplegia, chemosis
Acute nasal chondritis can be seen in acute flares
Source: accessmedicine.mhmedical.com
Saddle-nose deformity after chronic relapsing polychondritis
Source: what-when-how.com
Keratitis and episcleritis
Source: merckmanuals.com
Diffuse external eye involvement
Source:
Relapsing Polychondritis- Clinical
• Relapsing Polychondritis- Clinical
• IV. Large airway involvement-tracheobronchomalacia
• A. 50% develop laryngotracheal disease and 25% have
laryngotracheal stricture
• V. *Joint involvement-
• A. *Involvement of parasternal joints is typical (sternoclavicular,
costochondral, manubriosternal)
• B. 50-70% have arthritis of peripheral joints (large and small)
• V. Cardiac- 10%.....AI > MR > combined valvular regurgitation
Subglottic involvement
Source: smw.ch
Migratory arthritis can be seen
Source:findarthritistreatment.com
Relapsing Polychondritis- Clinical
• Relapsing Polychondritis- Clinical
• VI. Renal
• A. 25% with hematuria/proteinuria.....some have ANCA-positive
vasculitis
• VII. Nervous system involvement- usually due to vasculitis
• VIII. Skin- 36% have vasculitic skin and mucosal lesions
Relapsing Polychondritis- Lab/Diagnosis
• Relapsing Polychondritis- Lab/Diagnosis
• I. Lab-
• A. *Elevated ESR/CRP with leukocytosis, thrombocytosis and
anemia are typical......10% have eosinophilia....complement studies
are usually normal
• B. *22-60% are ANA-positive (homogenous or speckled
pattern)....and 1/3-1/2 may be ANCA-positive
• C. RF-positive in 16%....false-positive RPR and antiphospholipid
antibodies are occasionally seen
• D. dsDNA, Smith, RNP and SS-a/SS-b antibodies are not typical
• E. < 50% have anti-type II collagen antibodies
Relapsing Polychondritis- Lab/Diagnosis
• Relapsing Polychondritis- Lab/Diagnosis
• II. Diagnosis- needs 3 or more of the following McAdam criteria:
• A. Bilateral auricular chondritis
• B. Nonerosive, seronegative inflammatory polyarthritis
• C. Nasal chondritis
• D. Ocular inflammation (conjunctivitis, keratitis,
scleritis/episcleritis, uveitis)
• E. Respiratory tract chondritis (laryngeal or tracheal cartilages)
• F. Cochlear/vestibular dysfunction (sensorineural hearing loss,
tinnitus, vertigo)
Relapsing Polychondritis- Treatment
• Relapsing Polychondritis- Treatment
• I. **NSAIDs- initial therapy
• II. Second-line treatment- Steroids or Dapsone
• III. Refractory- Methotrexate, Azathioprine, Cyclophosphamide, TNF-
alpha inhibitors
Anopheles Mosquito
Source: insectcop.net
Anopheles Mosquito
Source: insectcop.net
Anopheles Mosquito
Source: insectcop.net
You might also like
- Spondyloarthropathies - Ankylosing Spondylitis, Psoriatic Arthritis, Reactive-Enteropathic Arthritis and HLA-B27 2020 PDFDocument125 pagesSpondyloarthropathies - Ankylosing Spondylitis, Psoriatic Arthritis, Reactive-Enteropathic Arthritis and HLA-B27 2020 PDFFazal Dalal100% (1)
- Otorhinolaryngology PDFDocument19 pagesOtorhinolaryngology PDFالطالب الطبيبNo ratings yet
- Preauricular Sinus and Its ManagmentDocument12 pagesPreauricular Sinus and Its ManagmentDr. T. Balasubramanian100% (7)
- Dr. Sana Bashir DPT, MS-CPPTDocument46 pagesDr. Sana Bashir DPT, MS-CPPTbkdfiesefll100% (1)
- Common Throat Infections: A ReviewDocument5 pagesCommon Throat Infections: A ReviewharryNo ratings yet
- Otologic Manifestation of Systemic DiseaseDocument57 pagesOtologic Manifestation of Systemic DiseaseHERIZALNo ratings yet
- Uworld ENT NotesDocument4 pagesUworld ENT Notes808kailuaNo ratings yet
- OPP 3 Study Guide Exam 3Document158 pagesOPP 3 Study Guide Exam 3Fazal DalalNo ratings yet
- BronchiectasisDocument60 pagesBronchiectasisArulNo ratings yet
- Bimbingan UKMPPD (UKDI) - THTDocument152 pagesBimbingan UKMPPD (UKDI) - THTAvicenna_MSC100% (7)
- (Optima) Sopem Optima THT-KL Sep'19Document333 pages(Optima) Sopem Optima THT-KL Sep'19Ory LarasNo ratings yet
- Veterinary Aspects of Pigeon Breeding 2010Document78 pagesVeterinary Aspects of Pigeon Breeding 2010Iancu SebastianNo ratings yet
- LMU DCOM SecondaryDocument1 pageLMU DCOM SecondaryFazal Dalal50% (2)
- EennttDocument13 pagesEennttSuresh Kumar BansalNo ratings yet
- 5+6. Nasal Polyp & DNS PDFDocument43 pages5+6. Nasal Polyp & DNS PDFJames StiltonNo ratings yet
- LabyrinthitisDocument7 pagesLabyrinthitisChristie ZamoraNo ratings yet
- Fungal InfectionsDocument23 pagesFungal Infections180045No ratings yet
- Cavernous Sinus Thrombosis: Clinical FeaturesDocument4 pagesCavernous Sinus Thrombosis: Clinical FeaturesStefanus ChristianNo ratings yet
- Bacterial Uveitis - DR ArnavDocument59 pagesBacterial Uveitis - DR ArnavDr Arnav SaroyaNo ratings yet
- Presented By:-Dr. Saqib Majeed Salik Resident Maxillofacial Supervised By: - Dr. Suad A Ahmad Consultant Maxillofacial King Abdullah Hospital BishaDocument53 pagesPresented By:-Dr. Saqib Majeed Salik Resident Maxillofacial Supervised By: - Dr. Suad A Ahmad Consultant Maxillofacial King Abdullah Hospital BishaSaqib Majeed SalikNo ratings yet
- Anat Med & Surg March 7Document24 pagesAnat Med & Surg March 7sb medexNo ratings yet
- Diseases of AdenoidsDocument19 pagesDiseases of AdenoidsMacktevin FraterinNo ratings yet
- Behcet's DiseaseDocument21 pagesBehcet's DiseaseFazal DalalNo ratings yet
- BronchiectasisDocument17 pagesBronchiectasisShannon RamsumairNo ratings yet
- Orbital CellulitisDocument42 pagesOrbital CellulitisDita HannaNo ratings yet
- Echinococcosis 1Document38 pagesEchinococcosis 1Nadine SellersNo ratings yet
- ASOMDocument41 pagesASOMArunkumar S KumarNo ratings yet
- Respiratory Module Pathology Lecture 1, Upper Respiratory Tract, Atelectasis, ARDSDocument29 pagesRespiratory Module Pathology Lecture 1, Upper Respiratory Tract, Atelectasis, ARDSalielabadi10No ratings yet
- ENT 2marksDocument10 pagesENT 2marksSaileekitha AjamoniNo ratings yet
- Bacterial, Viral, Fungal and Protozoal InfectionsDocument60 pagesBacterial, Viral, Fungal and Protozoal Infectionsmaroosh.khalidNo ratings yet
- Clinical Findings: A. Specimens, Microscopic Examination, and CultureDocument3 pagesClinical Findings: A. Specimens, Microscopic Examination, and CultureLeah VicenteNo ratings yet
- Suppurative Lung Diseases.Document37 pagesSuppurative Lung Diseases.Salman KhanNo ratings yet
- Common Fungal InfectionsDocument23 pagesCommon Fungal Infections180045No ratings yet
- PneumoniaDocument24 pagesPneumoniaWidhi AstutiNo ratings yet
- Microbial Diseases of The Different Organ System and Epidem.Document36 pagesMicrobial Diseases of The Different Organ System and Epidem.Ysabelle GutierrezNo ratings yet
- PatomekanismeDocument18 pagesPatomekanismeEdwin Pasha Jr.No ratings yet
- 8 Bacterial DiseasesDocument51 pages8 Bacterial DiseasesDavid JamuNo ratings yet
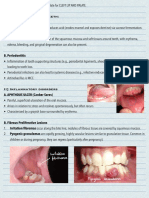
- Oral Medicine - Update For The Dental Practitioner Lumps and SwellingsDocument9 pagesOral Medicine - Update For The Dental Practitioner Lumps and SwellingsGowriNo ratings yet
- PneumoniaDocument48 pagesPneumoniaDammaqsaa W BiyyanaaNo ratings yet
- Orbital CellulitisDocument42 pagesOrbital Cellulitismuhammad iqbalNo ratings yet
- Chronic Suppurative Otitis Media: Drhpsingh Additional ProfessorDocument44 pagesChronic Suppurative Otitis Media: Drhpsingh Additional ProfessorIndieNo ratings yet
- Ear Infections: These Include Otitis Externa, Otitis Media, MastoiditisDocument32 pagesEar Infections: These Include Otitis Externa, Otitis Media, Mastoiditiseugene ugayNo ratings yet
- Eye DiseaseDocument31 pagesEye DiseaseTsegaye YalewNo ratings yet
- Bronchiectasis DesieDocument77 pagesBronchiectasis DesieAbebe GelawNo ratings yet
- Disorders of Middle EarDocument32 pagesDisorders of Middle EarAhmad fayazNo ratings yet
- CBL Blok 8 Group 1Document6 pagesCBL Blok 8 Group 1Laura Putri TraviraNo ratings yet
- RhinosinusitisDocument10 pagesRhinosinusitisErika De JesusNo ratings yet
- 25.suppurative Lung DiseasesDocument6 pages25.suppurative Lung DiseasesDIVEN SolvonNo ratings yet
- StreptococciDocument43 pagesStreptococciAyeshaNo ratings yet
- Group 11 MastoiditisDocument23 pagesGroup 11 MastoiditisYen-Naah AdamsNo ratings yet
- Sino Nasal Polyposis SsDocument42 pagesSino Nasal Polyposis SsJeffrinNo ratings yet
- Nasal Polyps: LECTURER Ass: DR Hussein Omar ZukeDocument26 pagesNasal Polyps: LECTURER Ass: DR Hussein Omar ZukeAbdiqani MahdiNo ratings yet
- Deafness & Otosclerosis: Midhun JDocument44 pagesDeafness & Otosclerosis: Midhun JRohit R PillaiNo ratings yet
- ENT Emergencies LectureDocument29 pagesENT Emergencies LectureThea Bertea100% (1)
- NoseDocument37 pagesNoseDawit workalemNo ratings yet
- The Oral Cavity - GIT PathologyDocument3 pagesThe Oral Cavity - GIT PathologyAakashNo ratings yet
- Infectious Uveitis AyuDocument19 pagesInfectious Uveitis AyuAndi Ayu LestariNo ratings yet
- Cavernous Sinus SyndromeDocument8 pagesCavernous Sinus SyndromeMuresan Ioana Catalina100% (1)
- Incidence: Specific Types of UveitisDocument15 pagesIncidence: Specific Types of UveitisImatunnisaZiNo ratings yet
- Suddensnhl 160220190525Document80 pagesSuddensnhl 160220190525mariahovhannisyanNo ratings yet
- 14-Diphtheria - Pertussis - and Brucellosis 44-45Document40 pages14-Diphtheria - Pertussis - and Brucellosis 44-45Manar AlhakamiNo ratings yet
- Behcet's DiseaseDocument21 pagesBehcet's DiseaseFazal DalalNo ratings yet
- Mirelesh Et Al, 1985 - Valproate and Clonazepam Comedication in Epilepsy-EpilepsiaDocument5 pagesMirelesh Et Al, 1985 - Valproate and Clonazepam Comedication in Epilepsy-EpilepsiaFazal DalalNo ratings yet
- Kwan Et Al 2000 - Epilepsy After The First Drug Fails Substitution or Addon?Document5 pagesKwan Et Al 2000 - Epilepsy After The First Drug Fails Substitution or Addon?Fazal DalalNo ratings yet
- French Et Al 2009 - Rational PolytherapyDocument6 pagesFrench Et Al 2009 - Rational PolytherapyFazal DalalNo ratings yet
- Baulac Et Al 2007 - Efficacy and Safety of Adjunctive Zonisamide Therapy For Refractory Partial SeizuresDocument9 pagesBaulac Et Al 2007 - Efficacy and Safety of Adjunctive Zonisamide Therapy For Refractory Partial SeizuresFazal DalalNo ratings yet