Professional Documents
Culture Documents
Efficacy of Prone Position in Acute Respiratory Distress Syndrome Overview of Systematic Reviews
Uploaded by
Rose Nirwana HandayaniCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Efficacy of Prone Position in Acute Respiratory Distress Syndrome Overview of Systematic Reviews
Uploaded by
Rose Nirwana HandayaniCopyright:
Available Formats
Review DOI: http://dx.doi.org/10.
1590/S1980-220X2016048803251
Efficacy of prone position in acute respiratory distress
syndrome: overview of systematic reviews
Efetividade da posição prona na síndrome do desconforto
respiratório agudo: overview de revisões sistemáticas
Efectividad de la posición prona en el síndrome de dificultad
respiratoria aguda: overview de revisiones sistemáticas
Michel Marcos Dalmedico1,2, Dafne Salas1, Andrey Maciel de Oliveira2, Fátima Denise Padilha Baran2, Jéssica Tereza
Meardi1, Michelle Caroline Santos2
How to cite this article:
Dalmedico MM, Salas D, Oliveira AM, Baran FDP, Meardi JT, Santos MC. Efficacy of prone position in acute respiratory distress syndrome: overview of
systematic reviews. Rev Esc Enferm USP. 2017;51:e03251. DOI: http://dx.doi.org/10.1590/S1980-220X2016048803251
1
Universidade Positivo, Curso de ABSTRACT
Enfermagem, Curitiba, PR, Brazil.
Objective: To identify and integrate the available scientific evidence related to the
2
Universidade Federal do Paraná, use of the prone position in patients with acute respiratory distress syndrome for the
Programa de Pós-Graduação em reduction of the outcome variable of mortality compared to the dorsal decubitus position.
Enfermagem, Curitiba, PR, Brazil.
Method: Overview of systematic reviews or meta-analyzes of randomized clinical trials.
It included studies that evaluated the use of prone positioning in patients with acute
respiratory distress syndrome published between 2014 and 2016. The AMSTAR tool was
used to determine the methodological quality of studies. The GRADE system was used
to establish the overall quality of evidence for the mortality outcome. Results: From the
search strategy, were retrieved seven relevant manuscripts of high methodological quality.
Conclusion: Scientific evidence supports that combined use of protective ventilatory
strategy and prone positioning for periods between 16 and 20 hours in patients with
acute respiratory distress syndrome and PaO2/FiO2 ratio lower than 150 mm/Hg results
in significant reduction of mortality rate.
DESCRIPTORS
Critical Care; Prone Position; Respiratory Distress Syndrome, Adult; Evidence-Based
Nursing; Evidence-Based Practice; Review.
Corresponding author:
Michel Marcos Dalmedico
Rua Jacarezinho, 1006 – Mercês
CEP 80710-150 – Curitiba, PR, Brazil Received: 12/24/2016
micheldalmedico@yahoo.com.br Approved: 04/24/2017
www.ee.usp.br/reeusp Rev Esc Enferm USP · 2017;51:e03251 1
Efficacy of prone position in acute respiratory distress syndrome: overview of systematic reviews
INTRODUCTION benefits were limited to PaO2 improvement without direct
interference of this phenomenon in reduction of mortality.
Acute Respiratory Distress Syndrome (ARDS) is a
In fact, the improvement in oxygenation (increase of
potentially devastating form of hypoxemic respiratory failure
at least 20% in PaO2/FiO2 ratio or ≥ 20 mmHg in arterial
caused by acute inflammatory lung injury(1). Its character-
oxygenation) is not directly associated with a reduction in
istics are the sudden onset, presence of a triggering factor
overall mortality rates. This suggests that oxygenation itself is
(diffuse bilateral pulmonary infiltrate), and normally there
not determinant in improved survival of patients submitted
is no left heart failure (non-cardiogenic pulmonary edema)
to ventilation in the prone position(13).
or circulatory overload(2).
This panorama underwent substantial changes after pub-
In 2012, was proposed a new model for the standard-
lication of the PROSEVA study, a randomized multicenter
ization of diagnostic concepts of acute respiratory distress
clinical trial of 466 individuals with ARDS, PaO2/FIO2
syndrome that took into account the severity of the disease
<150 mm/Hg, and ventilatory support (PEEP ≥5 cm H2O,
(ARDS Definition Task Force). The name of the recom-
FIO2 ≥ 0.6). The results showed that early use (between 12
mendation is Berlin Definition, and patients with ARDS are
and 24 hours after ARDS diagnosis) of prone position for a
stratified into three categories, namely: mild (PaO2/FiO2 ≤
prolonged time significantly reduced mortality in the inter-
300 mm/Hg with PEEP or CPAP ≥ 5 cmH2O); moderate
vention group. Mortality at 28 days was 16% in the prone
(PaO2/FiO2 ≤ 200 mm/Hg with PEEP ≥ 5cm/H2O); and
position group and 32.8% in the control group (P < 0.001),
severe (PaO2/FiO2 ≤ 100 mm/Hg with PEEP > 5 cm/H2O)(3).
ARDS is a high incidence phenomenon in the field of and at 90 days, it was 23.6% in the intervention group versus
intensive care. In this regard, 29,144 patients admitted to 41.0% in the supine group (P < 0.001)(14).
intensive care units were evaluated in a multicenter, inter- ARDS is one of the most important clinical illness of
national and prospective cohort study. It was found that modern intensive medicine because of its high rates of inci-
3,022 patients (10.4%) met the clinical criteria for ARDS. dence, mortality and long-term sequelae in survivors(15), and
Of these, 2,377 patients developed the disease within the patients usually have longer hospitalizations and greater con-
first 48 hours and required invasive ventilatory support to sumption of resources, resulting in increased hospital costs.
suppress severe acute respiratory failure. The mortality rate These facts justify the development of the present study.
was directly proportional to the severity of disease, as fol- Therefore, when considering a synthesis that integrates
lows: 35% among patients with mild ARDS, 40% among the evidence found in systematic reviews, the present study
patients with moderate ARDS, and 46% for patients with may contribute to identify the gaps in this topic, support the
severe ARDS. Incidence rates of this aggravation in western development of future research, and guide clinical practice
countries are between 6% and 7%(4). based on evidence. The aim of the study is to identify and
Considering the disease relevance in the context of integrate the available scientific evidence related to the use of
intensive care, clinical diagnosis and the adoption of early prone positioning in patients with acute respiratory distress
therapeutic interventions (specially the use of protective ven- syndrome for reduction of the outcome variable of mortality,
tilatory strategies) are determinants for reducing morbidity when compared to dorsal decubitus.
and increasing patients’ survival(5).
Thus, ventilatory support is considered the cornerstone METHOD
of ARDS treatment, despite the changes in the goals of this This is an overview of systematic reviews of random-
support in recent years. Such changes prioritize the main- ized clinical trials based on the Cochrane Handbook for
tenance of normal physiological parameters to avoid venti- Systematic Reviews of the recommendations of Interventions.
lator-induced lung injury and enable proper gas exchange(1). The Overview is a study design that integrates and synthe-
In patients with hypoxemia refractory to ventilatory sup- sizes information from existing systematic reviews on a par-
port or pulmonary failure (PaO2/FiO2 ≤ 100 mm/Hg), the ticular topic from the analysis of interventions available for a
use of ventilation in the prone position should be considered. treatment or prevention of this clinical condition. Its aim is to
It consists of providing ventilatory support with the patient provide an expanded view of multiple revisions of interven-
lying down in ventral decubitus position as additional therapy tions that address the effects of two or more potential inter-
for the treatment of severe hypoxemia caused by ARDS(6-7). ventions for a single health condition or problem in order
By adopting the prone position, the most important to identify the effects and trends of the studied variables(16).
physiological effect achieved is significant improvement The identification and evaluation process of all published
in oxygenation given the decreased atelectasis, redistribu- reviews allows that researchers describe the quality of this
tion of alveolar ventilation and perfusion, changes in the evidence base, summarize and compare the study findings,
conformation of pulmonary structure and diaphragm, and and discuss their strength.
consequent reduction of the gravitational gradient of pleu- The elaboration of the research question to guide the
ral pressures(8). scope of the study was based on the domains of the PICOS
Despite the relevance of prone positioning in the treat- acronym (P – population or problem, I – intervention, C –
ment of acute respiratory distress syndrome patients, sev- comparison, O – outcomes, S – Study design), in which: P
eral studies on the subject with publication before 2013 – Patients with acute respiratory distress syndrome (mod-
presented unfavorable results regarding the outcome of erate or severe); I – Use of prone positioning; C – Dorsal
mortality reduction(7,9-12). In summary, the prone position decubitus; O – reduction of mortality; S – Systematic review
2 Rev Esc Enferm USP · 2017;51:e03251 www.ee.usp.br/reeusp
Dalmedico MM, Salas D, Oliveira AM, Baran FDP, Meardi JT, Santos MC
or meta-analysis. Thus, the research question structured was: Review or Meta-analysis. Descriptors and terms related to
What is the efficacy of the prone position in mortality reduc- the research problem (acute respiratory distress syndrome),
tion in patients with moderate or severe acute respiratory intervention (prone position) and study design (systematic
distress syndrome in ventilatory support when compared to review or meta-analysis) were used. The terms combined by
the use of dorsal decubitus position? means of Boolean operators AND, OR, added to trunca-
The eligibility criteria were the systematic reviews with tion symbols formed the basis of the search equation, later
meta-analysis published between 2014 and 2016 that adapted to specifications of each base.
included the use of prone positioning in the treatment The relevant studies were retrieved through searches
of acute respiratory distress syndrome. The temporal cut in the following electronic databases: Medical Literature
is explained by the publication of results obtained in the Analysis and Retrieval System Online/Pubmed
PROSEVA trial(14). The findings of such study demonstrated (MEDLINE), Cochrane Central Register of Controlled
a left-hand deviation in forest plot graphs, showing the Trials (CENTRAL) and Cumulative Index to Nursing &
prone position as an intervention that could be associated Allied Health Literature (CINAHL). The last search update
with better mortality outcomes. Only articles in English was made in September 2016. The search strategies were
were chosen for the selection of secondary studies. formulated according to the criteria and manuals of each
Descriptors and their synonyms in English were used in database (Chart 1). In addition, was performed a manual
the search for secondary studies in the previously established search for relevant studies not indexed in the databases, such
databases: Medical Subject Headings (MeSH) – Prone as research reports from academic and non-academic institu-
Position; Acute Respiratory Distress Syndrome. In addi- tions, government agency documents, theses, dissertations,
tion, were defined the following types of study: Systematic and other publications known as ‘gray literature’.
Chart 1 – Search strategies and respective bases.
Base Search strategy
SEARCH #1 ((((“ Prone Position” [MeSH Terms]) OR Prone Position [Title/Abstract]) OR Prone Positioning [Title/
Abstract]) OR Prone Positions [Title/Abstract])
SEARCH #2 ((((“Respiratory Distress Syndrome, Adult” [MeSH Terms] OR “Respiratory Distress Syndrome,
Adult”[Title/Abstract]) OR Acute Respiratory Distress Syndrome” [MeSH Terms]) OR Acute Respiratory Distress
Syndrome[Title/Abstract])
MEDLINE/PUBMED
SEARCH #3 ((((Systematic Review [Publication Type]) OR Systematic Review [Title/Abstract]) OR Meta-analysis
[MeSH Terms]) OR Meta-analysis [Title/Abstract])
SEARCH #4 = #1 AND #2 AND #3
SEARCH #5 prone posit$.mp.
SEARCH # 6 = #4 AND #5
SEARCH #1 (ARDS or acute respiratory distress syndrome or adult respiratory distress syndrome)
SEARCH #2 (“Prone Position” OR “Prone Positioning”)
Cochrane CENTRAL SEARCH #3 (“Systematic Review” OR “Meta-analysis”).
SEARCH #4 = #1 AND #2 AND #3
Limiters − Date of publication: 2014-2016
SEARCH (“Prone Position” OR “Prone Positioning”) AND (“Acute Respiratory Distress Syndrome” OR “ARDS”)
CINAHL AND (“Systematic Review” OR “Meta-analysis”).
Limiters − Date of publication: 2014-2016
Source: Prepared by the authors.
The selection of systematic reviews (SR), data extraction meetings, there was support from a third reviewer for cases
and qualitative evaluations were performed in duplicate. The of disagreement. The results obtained were organized in a
inclusion process had two phases: a) first screening – evalua- narrative summary (Chart 2).
tion of titles and abstracts of all identified studies; b) reading All the included studies were evaluated with the
in full – evaluation of the full text. In the first consensus AMSTAR tool (Assessing the Methodological Quality of
meeting, the previously selected studies were evaluated in Systematic Reviews) to determine the methodological qual-
full with application of the eligibility criteria. In the sec- ity of systematic reviews. A score was assigned to each SR
ond consensus meeting, were defined the studies included from the sum of all positive responses to the questionnaire
and excluded from the review to compose the final sample. items. The included reviews were classified as follows: scores
The Kappa coefficient was applied to determine agreement between 8-11 were considered as high quality, scores 4-7
between evaluators, and scores ranged from 1 (complete were average quality, and scores 0-3 were considered as low
agreement) to -1 (complete disagreement). In consensus quality. In cases of studies with low AMSTAR scores, were
www.ee.usp.br/reeusp Rev Esc Enferm USP · 2017;51:e03251 3
Efficacy of prone position in acute respiratory distress syndrome: overview of systematic reviews
performed sensitivity analyzes to determine the potential Divergences were resolved with intervention of a third
risk of bias. reviewer at a second consensus meeting.
The overall quality of the evidence for the studied out-
come was assessed using the GRADE system (Grading MEDLINE/PubMed - 19
CENTRAL - 1
of Recommendations Assessment, Development and CINAHL - 6
Evaluation). This approach identifies four elements that Gray Literature - 0
influence the quality of evidence: study design, study qual- 2 studies excluded:
ity (risk of bias), consistency (comparison of effect estimates •duplicate studies
across studies), and direction (applicability of participants,
interventions, and outcomes for the clinical issue in con- Selected studies - 24 17 studies excluded:
sideration). Evaluating and combining these components •9 review studies
determines the initial quality of evidence as: •1 retrospective study
•1 RCT
High: further research is very unlikely to change confi- •1 observational study
dence on the effect estimate. •1 case report
•4 letters to the editor or
Moderate: further studies are likely to have a significant Complete studies evaluated commented articles
according to eligibility
impact on the confidence of the effect estimate and may criteria - 7
alter this estimate.
Low: other studies are likely to have a significant impact
on the confidence of the effect estimate and to change
the estimate.
Very low: any estimate of effect is very uncertain. Studies included in the overview-7
The use of the GRADE system requires a clear defini-
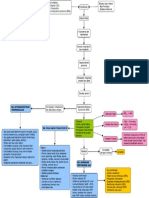
tion of population, intervention, comparison, and studied Figure 1 – Flowchart for identification, selection and inclusion of
studies – Curitiba, Paraná, Brazil, 2017.
outcomes (PICO) to determine the strength of evidence.
Thus, the GRADE system was applied to the following Chart 2 presents the selected studies with the respective
outcome measures: adult participants with severe hypoxemia; references, year of publication, number of patients evaluated,
mechanical ventilation with lower tidal volumes; mainte- analyzed outcome and main results obtained.
nance of the prone position for 16 or more hours per day. The present study included clinical trials on the use
There was no conflict of interest and no type of funding of prone position in different periods of time, patients
involved in the performance of this review. with moderate or severe ARDS, and low (<6 ml/kg) or
high (> 6 ml/kg) tidal volumes. The analysis of these ele-
RESULTS ments was adjusted in subgroups according to the identi-
Systematic reviews and meta-analyzes of randomized fied heterogeneity.
controlled trials comparing the effects of prone position Stratification by tidal volume accounted for more than
(intervention) and dorsal decubitus position (control) in half of heterogeneity among the randomized clinical trials
patients with moderate or severe acute respiratory distress observed in the non-stratified analysis of the sample(17).
syndrome were included. The search strategies resulted in 26 Table 1 demonstrates the most significant relative risk was
studies. Of these, two were published in two electronic data- found for the 60-day hospitalization period in the condi-
bases. After the first selection phase (screening), 17 studies tions under study(18). Statistical significance for the reduc-
were excluded because they did not meet the study objective tion of mortality from prone positioning was verified in
nor answer the guiding question. six out of the 11 studies included, especially in those in
Thus, after independent analysis by two reviewers, seven which protective ventilation was used(19). The results were
studies were evaluated in full and met the eligibility criteria more favorable to the long-term prone position (= to or >
therefore, they composed the final sample of this review 90 days)(21). There was statistical significance in the reduc-
(Figure 1). The Kappa score among observers regarding tion of mortality when performing the adjusted analysis for
the inclusion or exclusion of studies was 0.517 (p= <0.004). lower tidal volume(23).
Chart 2 – Main characteristics of included studies.
Study N (Clinical trial/Patients) Outcomes Main findings
When stratified by high or low tidal volume, randomized
clinical trials combining prone positioning and protective
Beitler et al. 2014(17) Seven clinical trials (N = 2,119). Risk of death within 60 days
ventilatory strategy (reduced volumes) showed a
significant decrease in the risk of death (p=0.002).
Compared to the supine position, the prone position
reduced mortality at 30 (p=0.003), 60 (p=0.04) and 90
Nine clinical trials (N = 2,242
Hu et al. 2014 (18)
Mortality at 30, 60 and 90 days days (0.0001) in patients with severe ARDS. Length of
patients).
stay longer than 12 daily hours in the prone position
contributes to mortality reduction (p=0.04).
continued…
4 Rev Esc Enferm USP · 2017;51:e03251 www.ee.usp.br/reeusp
Dalmedico MM, Salas D, Oliveira AM, Baran FDP, Meardi JT, Santos MC
…continuation
Study N (Clinical trial/Patients) Outcomes Main findings
The analysis of high quality evidence showed that prone
positioning during mechanical ventilation reduces
11 randomized clinical trials
Sud et al. 2014(19) Mortality from any cause mortality among ARDS patients who receive protective
(N = 2,341).
lung ventilation (reduced tidal volumes) when compared
to the use of high tidal volumes or supine positioning.
The reduction in overall mortality was significantly higher
in the intervention group (p=0.039). These results were
11 randomized clinical trials
Lee et al. 2014(20) Mortality higher in the subgroup in which duration of ventilation
(N = 2,246)
in prone position was greater than 10 hours/session
compared to the subgroup with shorter duration (p=0.039).
In the subgroups: recruited within 48 hours, treated
in prone position for 16 or more hours per day, and
Bloomfield et al. Nine clinical trials
Short and long-term mortality participants with more severe hypoxemia, there were
2014(21) (N = 2,149 individuals).
statistically significant results for the outcome of
mortality r eduction.
Mortality rates were lower in the intervention group
compared to the control group (41% and 47%,
Eight randomized clinical trials respectively). In the subgroups of mechanical ventilation
Park et al. 2015(22) Mortality
(N = 2,141 patients). with protective strategy and duration of prone positioning
greater than 12 hours, mortality rates were significantly
reduced (p=0.0002 and p <0.0001, respectively).
When patients submitted to the prone position were
stratified by subgroups, there was a significant decrease
Mora-Arteaga et al. Seven blind controlled studies
Reduced risk of death in mortality risk in ventilated patients with low tidal
2015(23) (N = 2,119 patients).
volume, the first 48 hours of disease evolution, and
severe h
ypoxemia.
Source: Prepared by the authors.
Table 1 – Measures of effect of the PRONE position in reducing the mortality of patients with ARDS compared to the supine position
– Curitiba, Paraná, Brazil, 2017.
Allocation
Study Sample size R.R. O.R. C.I. (95%) p-value
Prone position Supine position
Beitler et al., 2014 (17)
2,119 1,088 1,031 0.83 (0.68 - 1.02) 0.002
Hu et al., 2014(18) 2,242 1,150 1,092 0.82 (0.68 - 0.99) 0.004
Sud(19) 1,016 510 506 0.74 (0.59 - 0.95)
Lee(20) 2,246 1,142 1,104 0.77 (0.59 - 0.99) 0.039
Bloofield(21) 2,165 1,107 1,041 0.86 (0.72 - 1.03)
Park(22) 2,141 1,099 1,042 0.90 (0.82 - 0.98) 0.02
Mora-Arteaga(23) 2,119 1,088 1,031 0.76 (0.54 - 1.06)
Source: Prepared by the authors.
DISCUSSION points). Considering the elements of the AMSTAR mea-
suring tool, all the included studies described the following:
Assuming that mortality outcome is critical for decision
clinical question and inclusion criteria; selection and data
making, the aim of this study was to identify and integrate
extraction by peers; conduction of a comprehensive literature
the main available scientific evidence related to the use of
survey; list of studies (included and excluded); characteristics
prone position compared to dorsal decubitus position in of the included studies; assessment of the scientific quality of
patients with acute respiratory distress syndrome for the included studies; the use of the scientific quality of studies
outcome variable of reduction in mortality. Prone position- in the formulation of conclusions; appropriate combination
ing has been widely used as a therapeutic resource in clinical of study results; risk assessment of bias.
practice, hence high-quality scientific basis is fundamental The search for relevant studies in gray literature was
to support its indication. Seven high-quality meta-analyzes not contained in the inclusion criteria of three system-
were analyzed, all of which evaluated the prone position as atic reviews(17-18,23). Six studies did not state the conflicts
an intervention. They all included 14 randomized clinical of interest(17-20,22-23).
trials with 2,372 patients with moderate or severe ARDS The quality of evidence reported by the primary studies
randomly distributed (intervention and control) for the out- in the included reviews was assessed using the GRADE
come of mortality reduction. method, and considered moderate for the following sub-
The mean methodological quality of the analyzed sys- groups: rapid intervention, severe hypoxemia and protective
tematic reviews was 9.71 (SD=0.76), with 95% confidence ventilation. These data are compatible with the findings of a
interval between 9.15 and 10.27. This leads to the conclusion Cochrane systematic review(21).
that the systematic reviews included have high scientific Despite the impossibility of blinding (concealment) the
rigor when assessing the maximum AMSTAR score (11 intervention (prone position), when the overall mortality
www.ee.usp.br/reeusp Rev Esc Enferm USP · 2017;51:e03251 5
Efficacy of prone position in acute respiratory distress syndrome: overview of systematic reviews
outcome is analyzed, masking is irrelevant. The research- patients has shown reductions in tidal volume or increases
er’s knowledge about which treatment the patient under- in PEEP are beneficial only if associated with maintain-
went would not imply the inadequate classification of ing driving pressure (difference between plateau pressure
this outcome. and PEEP) lower than 16 cmH2O. Driving pressure was
Regarding the studied intervention, a meta-analysis with pointed out as the main variable determining the best prog-
nine clinical trials maintains there is no convincing evidence nosis for the mortality outcome in patients with moderate
of the beneficial or detrimental effect of the universal appli- or severe ARDS(27).
cation of prone positioning in adults with hypoxemia under In summary, under specific conditions and indications,
mechanical ventilatory support. However, when analyzing prone position ventilation is a feasible, safe and inexpen-
three distinct subgroups, namely: implementation of the sive therapy(28) that improves alveolar gas exchange in more
prone position within 48 hours of disease course; prone than two thirds of patients with severe acute respiratory
position for 16 or more hours per day; and more severe failure(29). Prone positioning is a viable maneuver for most
hypoxemia, statistically significant benefits in reduction of intensive care units, and its application should be part of
mortality were obtained when using the prone position(21). the institutional protocol because it requires trained per-
The early use of prone position during ventilatory sup- sonnel, who consider the particularities of each service and
port for severe acute respiratory distress syndrome in patients each patient(30).
requiring relatively high PEEP levels and reduced tidal vol-
umes is associated with the best physiological response of CONCLUSION
collapsed alveolar units. As these units are more susceptible By analyzing the results obtained, this overview provides
to be open (alveolar recruitment) during the initial phase of consistent scientific evidence on the incorporation of use of
disease (exudative), it implies on a significant reduction in the prone position in patients with acute respiratory distress
mortality(14,18,23). Another relevant aspect of using the prone syndrome. The use of ventilatory interventions such as lower
position refers to the analysis of the subgroup ‘PaO2/FiO2 tidal volumes and high PEEP associated with adjuvant thera-
ratio’ that indicated a significant reduction in the additional pies such as prone positioning in patients with severe acute
mortality rate in patients with severe hypoxemia or other hypoxemic respiratory failure results in a significant reduction
severe clinical conditions associated(14). Severely hypoxemic in overall mortality. The intervention efficacy was statistically
patients appear to respond better to the intervention. significant in three subgroups: rapid implementation of the
Mortality reduction is related to the overall effects of prone position (< 48 hours of disease course); prolonged stay
prone positioning, such as hemodynamic improvement in in ventral decubitus position (> 16 consecutive hours); and
gas exchange (optimization of alveolar recruitment, perfu- severe hypoxemia (PaO2/FiO2 < 150 mm/Hg).
sion and ventilation) and respiratory mechanics. There is Thus, the available scientific evidence suggests that early
also reduction of deleterious effects caused by mechanical combination of using protective ventilatory strategy with a
ventilation-induced lung injury given the homogenization sustained driving pressure of less than 16 cmH2O and prone
of stress and tension on the pulmonary parenchyma(23-24), positioning for periods of 16 to 20 hours in patients with
allowing a reduction in FIO2 values and lower airway pres- severe acute respiratory distress syndrome results in benefits
sure to obtain adequate oxygenation(25). on mortality reduction.
Another important fact is the tidal volume used dur- The rigorous search for studies with high scientific and
ing ventilatory support. A randomized study showed that methodological quality and careful analysis of their findings
lower tidal volume (6 ml/kg of predicted weight) resulted corroborate the expressiveness of the evidence obtained, and
in decreased mortality (31% versus 39.8%, P=0.007) and demonstrate the scientific findings that can be incorporated
reduction in days of ventilatory support (P=0.007), when into clinical practice.
compared to the use of ventilation strategy with high tidal In view of the above, this study supports the use of
volume(13). Ventilatory strategies associating low tidal vol- prone positioning in clinical practice of intensive care units.
umes and pressure-volume (P-V) relationship guided by Moreover, for the effective benefit of patients with acute
PEEP static curve, FiO2-guided, high PEEP, and prone- respiratory distress syndrome from use of the prone position,
position ventilation are potentially the best alternative for it is imperative that the production of scientific evidence is
ventilatory support in terms of improved survival in patients complemented by highly trained professionals involved in
with moderate or severe ARDS(26). the care, and who understand the clinical dimensions and
Although tidal volume is an important determinant of practices of this intervention for the promotion of a safer
mortality reduction, a meta-analysis of approximately 2,000 and evidence-based bedside service.
RESUMO
Objetivo: Identificar e integrar as evidências científicas disponíveis relacionadas à utilização da posição prona em pacientes com
síndrome do desconforto respiratório agudo para a redução da variável de desfecho mortalidade, quando comparada ao decúbito dorsal.
Método: Overview de revisões sistemáticas ou metanálises de ensaios clínicos randomizados. Foram incluídos estudos publicados no
período entre 2014 e 2016, que avaliaram a utilização de posição prona em pacientes com síndrome do desconforto respiratório agudo.
6 Rev Esc Enferm USP · 2017;51:e03251 www.ee.usp.br/reeusp
Dalmedico MM, Salas D, Oliveira AM, Baran FDP, Meardi JT, Santos MC
Utilizou-se da ferramenta AMSTAR para determinar a qualidade metodológica dos estudos e o sistema GRADE para estabelecer a
qualidade geral da evidência para o desfecho mortalidade. Resultados: A partir da estratégia de busca foram recuperados sete manuscritos
relevantes de alta qualidade metodológica. Conclusão: As evidências científicas sustentam que a utilização combinada de estratégia
ventilatória protetora e posição prona por períodos entre 16 e 20 horas em pacientes com síndrome do desconforto respiratório agudo,
com relação PaO2/FiO2 inferior à 150 mm/Hg, resulta em redução significativa da taxa de mortalidade.
DESCRITORES
Cuidados Críticos; Decúbito Ventral; Síndrome do Desconforto Respiratório do Adulto; Enfermagem Baseada em Evidências; Prática
Clínica Baseada em Evidências; Revisão.
RESUMEN
Objetivo: Identificar e integrar las evidencias científicas disponibles relacionadas con la utilización de la posición prona en pacientes con
síndrome de dificultad respiratoria aguda para la reducción de la variable de resultado mortalidad, cuando comparado al decúbito dorsal.
Método: Panorama de revisiones sistemáticas o metaanálisis de ensayos clínicos randomizados. Fueron incluidos estudios publicados en
el período entre 2014 y 2016, que evaluaron la utilización de posición prona en pacientes con síndrome de dificultad respiratoria aguda.
Se utilizó la herramienta AMSTAR para determinar la calidad metodológica de los estudios y el sistema GRADE para establecer la
calidad general de la evidencia para el resultado mortalidad. Resultados: A partir de la estrategia de búsqueda fueron recuperados siete
manuscritos relevantes de alta calidad metodológica. Conclusión: Las evidencias científicas sostienen que la utilización combinada de
estrategia ventilatoria protectora y posición prona por períodos entre 16 y 20 horas en pacientes con síndrome de dificultad respiratoria
aguda, con relación PaO2/FiO2 inferior a 150 mm/Hg, resulta en reducción significativa de la tasa de mortalidad.
DESCRIPTORES
Cuidados Críticos; Posición Prona; Síndrome de Dificultad Respiratoria del Adulto; Enfermería Basada en la Evidencia; Práctica
Clínica Basada en la Evidencia; Revisión.
REFERENCES
1. Silversides JA, Ferguson ND. Clinical review: acute respiratory distress syndrome - clinical ventilator management and adjunct therapy.
Crit Care [Internet]. 2013 [cited 2016 Jan 13];17(2):225. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3672489/
2. Barbas CS, Isola AM, Caser EB. What is the future of acute respiratory distress syndrome after the Berlin definition? Curr Opin Crit Care.
2014;20(1):10-6.
3. ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, et al. Acute respiratory distress
syndrome: the Berlin Definition. JAMA. 2012;307(23):2526-33.
4. Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A, et al. Epidemiology, patterns of care, and mortality for patients with acute
respiratory distress syndrome in Intensive Care Units in 50 countries. JAMA 2016;315(8):788-800.
5. Papazian L, Forel JM, Gacouin A, Penot-Ragon C, Perrin G, Loundou A, et al. Neuromuscular blockers in early acute respiratory distress
syndrome. N Engl J Med. 2010;363(12):1107-16.
6. Matthay MA, Ware LB, Zimmerman GA. The acute respiratory distress syndrome. J Clin Invest [Internet]. 2012 [cited 2016 May
11]:122(8):2731-40. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3408735/
7. Sud S, Friedrich JO, Taccone P, Polli F, Adhikari NK, Latini R, et al. Prone ventilation reduces mortality in patients with acute respiratory
failure and severe hypoxemia: systematic review and meta-analysis. Intensive Care Med. 2010;36(4):585-99.
8. Seguras Llanes O, Yora Orta, R, Gutiérrez Gutiérrez, L, García Gómez, A. Ventilación prona en pacientes con daño pulmonar agudo
ingresados en cuidados intensivos. Rev Cuba Anestesiol Reanim [Internet]. 2011 [citado 2016 Abr 23];10(1): 43-51. Disponible en: http://
bvs.sld.cu/revistas/scar/vol_10_1_11/ane06111.htm
9. Curley MA. Prone positioning of patients with acute respiratory distress syndrome: a systematic review. Am J Crit Care. 1999;8(6):397-405.
10. Mebazaa MS, Abid N, Frikha N, Mestiri T, Ben Ammar MS. The prone position in acute respiratory distress syndrome: a critical systematic
review. Ann Fr Anesth Reanim. 2007;26(4):307-18.
11. Kopterides P, Siempos II, Armaganidis A. Prone positioning in hypoxemic respiratory failure: meta-analysis of randomized controlled trials.
J Crit Care. 2009;24(1):89-100.
12. Sud S, Sud M, Friedrich JO, Adhikari NK. Effect of mechanical ventilation in the prone position on clinical outcomes in patients with acute
hypoxemic respiratory failure: a systematic review and meta-analysis. CMAJ [Internet]. 2008 [cited 2016 Apr 23]:178(9):1153-61 Available
from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4081236/
13. The Acute Respiratory Distress Syndrome Network, Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, Wheeler A. Ventilation
with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl
J Med [Internet]. 2000 [cited 2016 July 23];342(18):1301-8. Available from: http://www.nejm.org/doi/full/10.1056/NEJM200005043421801
14. Guérin C, Reignier J, Richard JC, Beuret P, Gacouin A, Boulain T, et al. PROSEVA Study Group. Prone positioning in severe acute
respiratory distress syndrome. N Engl J Med [Internet]. 2013 [cited 2016 May 10];368(23):2159-68. Available from: http://www.nejm.org/
doi/full/10.1056/NEJMoa1214103
15. Cardinal-Fernández P, Correger E, Villanueva J, Rios F. Acute respiratory distress: from syndrome to disease. Med Intensiva. 2016;40(3):169-
75.
16. Becker LA, Oxman AD. Overviews of reviews. In: Higgins JPT, Green S, editors. Cochrane Handbook for Systematic Review of Interventions.
Version 5.1.0 [Internet]. Oxford: The Cochrane Library; 2011 [cited 2016 Jan 10]. Available from: http://handbook.cochrane.org/
www.ee.usp.br/reeusp Rev Esc Enferm USP · 2017;51:e03251 7
Efficacy of prone position in acute respiratory distress syndrome: overview of systematic reviews
17. Beitler JR, Shaefi S, Montesi SB, Devlin A, Loring SH, Talmor D, et al. Prone positioning reduces mortality from acute respiratory distress
syndrome in the low tidal volume era: a meta-analysis. Intensive Care Med [Internet]. 2014 [cited 2016 June 23]:40(3):332-41. Available
from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3976426/
18. Hu SL, He HL, Pan C, Liu AR, Liu SQ, Liu L, et al. The effect of prone positioning on mortality in patients with acute respiratory distress
syndrome: a meta-analysis of randomized controlled trials. Crit Care [Internet]. 2014 [cited 2016 June 12]:28;18(3):R109. Available from:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4075407/
19. Sud S, Friedrich JO, Adhikari NK, Taccone P, Mancebo J, Polli F, et al. Effect of prone positioning during mechanical ventilation on mortality
among patients with acute respiratory distress syndrome: a systematic review and meta-analysis. CMAJ [Internet]. 2014 [cited 2016 July
10];186(10):E381-90. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4081236/
20. Lee JM, Bae W, Lee YJ, Cho YJ. The efficacy and safety of prone positional ventilation in acute respiratory distress syndrome: updated study-
level meta-analysis of 11 randomized controlled trials. Crit Care Med [Internet]. 2014 [cited 2016 May 05];42(5):1252-62. Available from:
https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0061924/
21. Bloomfield R, Noble DW, Sudlow A. Prone position for acute respiratory failure in adults. Cochrane Database Syst Rev. 2015;(11):CD008095.
22. Park SY, Kim HJ, Yoo KH, Park YB, Kim SW, Lee SJ, et al. The efficacy and safety of prone positioning in adults patients with acute respiratory
distress syndrome: a meta-analysis of randomized controlled trials. J Thorac Dis [Internet]. 2015 [cited 2016 June 21];7(3): 356–367.
Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4387391/
23. Mora-Arteaga JA, Bernal-Ramírez OJ, Rodríguez SJ. The effects of prone position ventilation in patients with acute respiratory distress
syndrome: a systematic review and metaanalysis. Med Intensiva. 2015;39(6):359-72.
24. Koulouras V, Papathanakos G, Papathanasiou A, Nakos G. Efficacy of prone position in acute respiratory distress syndrome patients: a
pathophysiology-based review. World J Crit Care Med [Internet]. 2016 [cited 2016 July 01];5(2):121-36. Available from: http://www.ncbi.
nlm.nih.gov/pmc/articles/PMC4848155/
25. Gattinoni L, Pesenti A, Carlesso E. Body position changes redistribute lung computed-tomographic density in patients with acute respiratory
failure: impact and clinical fallout through the following 20 years. Int Care Med. 2013;39(11):1909-15.
26. Wang C, Wang X, Chi C, Guo L, Guo L, Zhao N, et al. Lung ventilation strategies for acute respiratory distress syndrome: a systematic
review and network meta-analysis. Sci Rep [Internet]. 2016 [cited 2016 Jul 11];6:22855. Available from: http://www.ncbi.nlm.nih.gov/
pmc/articles/PMC4783789/
27. Amato MBP, Meade MO, Slutsky AS, Brochard L, Costa ELV, Schoenfeld DA, et al. Driving pressure and survival in the acute respiratory
distress syndrome. N Engl J Med [Internet]. 2015 [cited 2016 May 23];372(8):747-55. Available from: http://www.nejm.org/doi/full/10.1056/
NEJMsa1410639#t=article
28. Agrawal SP, Goel AD. Prone position ventilation in Acute Respiratory Distress Syndrome: an overview of the evidences. Indian J Anaesth
[Internet]. 2015 [cited 2016 July 30];59(4):246-8. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4408655/
29. Cornejo R, Romero C, Ugalde D, Bustos P, Diaz G, Galvez R, et al. High-volume hemofiltration and prone ventilation in subarachnoid
hemorrhage complicated by severe acute respiratory distress syndrome and refractory septic shock. Rev Bras Ter Intensiva [Internet]. 2014
[cited 2016 July 13];26(2):193-9. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4103947/
30. Setten M, Plotnikow GA, Accoce M. Prone position in patients with acute respiratory distress syndrome. Rev Bras Ter Intensiva [Internet].
2016 [cited 2017 Mar 03]; 28(4):452-62. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5225921/
This is an open-access article distributed under the terms of the Creative Commons Attribution License.
8 Rev Esc Enferm USP · 2017;51:e03251 www.ee.usp.br/reeusp
You might also like
- Essentials in Lung TransplantationFrom EverandEssentials in Lung TransplantationAllan R. GlanvilleNo ratings yet
- Ventilación en SDRA - Guia ClinicaDocument18 pagesVentilación en SDRA - Guia ClinicaPablo PradoNo ratings yet
- 2023 Ards PelosiDocument25 pages2023 Ards PelosiMiky DinuNo ratings yet
- Algoritma ARDSDocument7 pagesAlgoritma ARDSSri AgustinaNo ratings yet
- CF Ventilation ManagementDocument10 pagesCF Ventilation ManagementSherry SaidNo ratings yet
- Airway Pressure Release VentilatiDocument9 pagesAirway Pressure Release VentilatiDavid ParraNo ratings yet
- E006812 FullDocument8 pagesE006812 FullabhiNo ratings yet
- Naresuan University Journal: Evidence-Based Management of ARDSDocument14 pagesNaresuan University Journal: Evidence-Based Management of ARDSshofwaNo ratings yet
- ARDSDocument10 pagesARDSLaiosAndreaNo ratings yet
- Antacid Therapy and Disease Progression in Patients With Idiopathic Pulmonary Fibrosis Who Received PirfenidoneDocument9 pagesAntacid Therapy and Disease Progression in Patients With Idiopathic Pulmonary Fibrosis Who Received PirfenidoneAquiles CastroNo ratings yet
- Adverse Events of Prone Positioning in Mechanically Ventilated AdultsDocument44 pagesAdverse Events of Prone Positioning in Mechanically Ventilated Adultsrodrigo jacobsNo ratings yet
- 1 s2.0 S2529984017300277 Main PDFDocument10 pages1 s2.0 S2529984017300277 Main PDFindahNo ratings yet
- ARDS Subphenotypes: Understanding A Heterogeneous Syndrome: Review Open AccessDocument8 pagesARDS Subphenotypes: Understanding A Heterogeneous Syndrome: Review Open AccessAlex CroNo ratings yet
- Art:10.1186/s13063 016 1456 4Document10 pagesArt:10.1186/s13063 016 1456 4dani yan sNo ratings yet
- Prone Ventilation in Acute Respiratory Distress SyndromeDocument10 pagesProne Ventilation in Acute Respiratory Distress Syndromecelma44No ratings yet
- (PULMO) 2012 ARDS - The New Berlin DefinitionDocument4 pages(PULMO) 2012 ARDS - The New Berlin DefinitionerikaNo ratings yet
- Vincent-Slutsky2020 Article WeVeNeverSeenAPatientWithARDSDocument3 pagesVincent-Slutsky2020 Article WeVeNeverSeenAPatientWithARDSHoracio Panzardo GonzálezNo ratings yet
- Acute Life-Threatening Hypoxemia During Mechanical VentilationDocument8 pagesAcute Life-Threatening Hypoxemia During Mechanical VentilationCesar Rivas CamposNo ratings yet
- Hfo 2Document9 pagesHfo 2markus_danusantosoNo ratings yet
- HipertensiDocument7 pagesHipertensiAchmad HafirulNo ratings yet
- Efficiency of Prolonged Prone Positioning For Mechanically Ventilated Patients Infected With COVID-19Document11 pagesEfficiency of Prolonged Prone Positioning For Mechanically Ventilated Patients Infected With COVID-19Riyan NuelNo ratings yet
- Current Incidence and Outcome of The Acute Respiratory Distress SyndromeDocument6 pagesCurrent Incidence and Outcome of The Acute Respiratory Distress Syndromedarius2311No ratings yet
- Paper 8, Raymandos 2012Document10 pagesPaper 8, Raymandos 2012NITIN SENTHILKUMARNo ratings yet
- Cap AsmaDocument10 pagesCap AsmaAuliaNo ratings yet
- Jurnal ARDSDocument8 pagesJurnal ARDSrifki yulinandaNo ratings yet
- HHS Public Access: Understanding the Acute Respiratory Distress SyndromeDocument52 pagesHHS Public Access: Understanding the Acute Respiratory Distress SyndromeRaqi QatulawanisNo ratings yet
- 8. Negative-_versus_positive-pressure_ventilation_in_Document11 pages8. Negative-_versus_positive-pressure_ventilation_in_Dwi Putri SekariniNo ratings yet
- ESICM Guidelines On ARDS 2023Document33 pagesESICM Guidelines On ARDS 2023ctsakalakisNo ratings yet
- Respiratory - ARDS Vent Revised - QuestionsDocument6 pagesRespiratory - ARDS Vent Revised - QuestionsRyan ReNo ratings yet
- High Flow Nasal Cannula For Acute Respiratory Distress Syndrome Due To Covid 19Document5 pagesHigh Flow Nasal Cannula For Acute Respiratory Distress Syndrome Due To Covid 19Cesar C SNo ratings yet
- Dead Space in ARDS Die HardDocument3 pagesDead Space in ARDS Die HardJose Morato E FlavianeNo ratings yet
- 8016-Article Text-28205-1-10-20220228Document11 pages8016-Article Text-28205-1-10-20220228Andreas Dhymas DmkNo ratings yet
- 1 s2.0 S2173572722003095 MainDocument10 pages1 s2.0 S2173572722003095 Maintaaaatan.04No ratings yet
- Intubación CovidDocument16 pagesIntubación CovidJulietPérezNo ratings yet
- 10 1002@ppul 24581Document6 pages10 1002@ppul 24581Roberto Guerrero MonsivaisNo ratings yet
- Preoxygenation For Tracheal Intubation in Critically Ill Patients: One Technique Does Not Fit AllDocument5 pagesPreoxygenation For Tracheal Intubation in Critically Ill Patients: One Technique Does Not Fit AllMarcela ParraNo ratings yet
- Jurnal Dari Aak 4Document8 pagesJurnal Dari Aak 4rifqi rizalNo ratings yet
- Guérin - 2013-DikonversiDocument19 pagesGuérin - 2013-DikonversiCindy KarmilaNo ratings yet
- Epistimologi B.inggrisDocument3 pagesEpistimologi B.inggrisbudiNo ratings yet
- The Acute Respiratory Distress Syndrome: Review SeriesDocument10 pagesThe Acute Respiratory Distress Syndrome: Review Seriesadek07No ratings yet
- Ards Prone PositionDocument9 pagesArds Prone PositionAnonymous XHK6FgHUNo ratings yet
- ARDS PathophysiologyDocument2 pagesARDS PathophysiologyIntanAgustiFernandesNo ratings yet
- Gaudry2017 Article PronePositioningInAcuteRespiraDocument8 pagesGaudry2017 Article PronePositioningInAcuteRespiraEmmanuel Guar HuaNo ratings yet
- ALI and ARDS - Challenges and Advances - An Issue of Critical Care ClinicsDocument324 pagesALI and ARDS - Challenges and Advances - An Issue of Critical Care ClinicsOanamikaela VaidaNo ratings yet
- Ventilacion protectivaDocument11 pagesVentilacion protectivaDavid Davoas A. SolizNo ratings yet
- Case Report GUP - Respi FailureDocument26 pagesCase Report GUP - Respi Failureunggul.pribadiNo ratings yet
- Evidence-Based Management of Acute Lung Injury and Acute Respiratory Distress SyndromeDocument17 pagesEvidence-Based Management of Acute Lung Injury and Acute Respiratory Distress SyndromeretNo ratings yet
- Medi 101 E29940Document5 pagesMedi 101 E29940Bella FebriantiNo ratings yet
- HFNCDocument10 pagesHFNCDollenz Maldonado Natalie CamilaNo ratings yet
- Journal of Intensive MedicineDocument10 pagesJournal of Intensive MedicineARELHI ROSARIO GARCIA MONROYNo ratings yet
- Fan 2018Document13 pagesFan 2018Andi sutandiNo ratings yet
- Invasive Mechanical Ventilation PDFDocument4 pagesInvasive Mechanical Ventilation PDFRaquel AguilarNo ratings yet
- Effect of A Protective-Ventilation Strategy On Mortality in The Acute Respiratory Distress SyndromeDocument8 pagesEffect of A Protective-Ventilation Strategy On Mortality in The Acute Respiratory Distress Syndromeiturraspe12No ratings yet
- Comparison of The Berlin Defnition For Acute Respiratory Distress Syndrome With Autopsy Thille2013Document7 pagesComparison of The Berlin Defnition For Acute Respiratory Distress Syndrome With Autopsy Thille2013matias bertozziNo ratings yet
- Prone Position in Management of COVID-19 Patients A CommentaryDocument3 pagesProne Position in Management of COVID-19 Patients A CommentaryJoseLuisNo ratings yet
- Decubito Prono en SDRA - NEJM 2013Document10 pagesDecubito Prono en SDRA - NEJM 2013Dr. Sergio Oscar AlunniNo ratings yet
- Long-Term Azithromycin With Severe CopdDocument8 pagesLong-Term Azithromycin With Severe Copdlaksono_adeNo ratings yet
- Acute Respiratory Distress Syndrome - ReviewDocument13 pagesAcute Respiratory Distress Syndrome - ReviewMr. L0% (1)
- Jurnal 2Document16 pagesJurnal 2AndiirmaNo ratings yet
- Evolvingepidemiology Anddefinitionsofthe Acuterespiratorydistress Syndromeandearlyacute LunginjuryDocument16 pagesEvolvingepidemiology Anddefinitionsofthe Acuterespiratorydistress Syndromeandearlyacute LunginjuryVijay KumarNo ratings yet
- Ten Tips For Building Strong RelationshipsDocument1 pageTen Tips For Building Strong RelationshipsRose Nirwana HandayaniNo ratings yet
- Berg Balance ScaleDocument1 pageBerg Balance Scale69016No ratings yet
- Pediatric Case 4: Sabina Vasquez (Complex) : Documentation AssignmentsDocument1 pagePediatric Case 4: Sabina Vasquez (Complex) : Documentation AssignmentsRose Nirwana Handayani0% (1)
- 1241 2436 1 SMDocument6 pages1241 2436 1 SMDian Dewy LestaryNo ratings yet
- Born Preterm A Public Health IssueDocument12 pagesBorn Preterm A Public Health IssueRose Nirwana HandayaniNo ratings yet
- Prone Position For Acute Respiratory Distress Syndrome. A Systematic Review and Meta-AnalysisDocument9 pagesProne Position For Acute Respiratory Distress Syndrome. A Systematic Review and Meta-AnalysisRose Nirwana HandayaniNo ratings yet
- Woc RDSDocument1 pageWoc RDSRose Nirwana HandayaniNo ratings yet
- Efficacy of Prone Position in Acute Respiratory Distress Syndrome Overview of Systematic ReviewsDocument8 pagesEfficacy of Prone Position in Acute Respiratory Distress Syndrome Overview of Systematic ReviewsRose Nirwana HandayaniNo ratings yet
- Management of Common Neonatal ProblemsDocument6 pagesManagement of Common Neonatal ProblemsRose Nirwana HandayaniNo ratings yet
- Ethical Issues in Emergency Care and Research PDFDocument9 pagesEthical Issues in Emergency Care and Research PDFRose Nirwana HandayaniNo ratings yet
- F. Moyra Allen: A Life in Nursing, 1921-1996: Meryn Stuart, R.N., PH.DDocument9 pagesF. Moyra Allen: A Life in Nursing, 1921-1996: Meryn Stuart, R.N., PH.DRose Nirwana HandayaniNo ratings yet
- Management of Acute Asthma in Adults in The Emergency Department Nonventilatory Managemen PDFDocument13 pagesManagement of Acute Asthma in Adults in The Emergency Department Nonventilatory Managemen PDFRose Nirwana HandayaniNo ratings yet
- The Essentials of Baccalaureate Education For Professional Nursing PracticeDocument63 pagesThe Essentials of Baccalaureate Education For Professional Nursing PracticeBaye HickinsNo ratings yet
- Pathophysiology of Respiratory FailureDocument6 pagesPathophysiology of Respiratory FailurevidagurlNo ratings yet
- ABG InterpretationDocument38 pagesABG Interpretationmahmod omerNo ratings yet
- Writing LettersDocument12 pagesWriting LettersCristina CepragaNo ratings yet
- Non-invasive Ventilation Techniques for Respiratory FailureDocument58 pagesNon-invasive Ventilation Techniques for Respiratory FailuresachinNo ratings yet
- N118 0XYGEN Checklist FinalDocument7 pagesN118 0XYGEN Checklist FinalAmandaNo ratings yet
- PulmCrit - Understanding Happy Hypoxemia PhysiologyDocument13 pagesPulmCrit - Understanding Happy Hypoxemia PhysiologyhardianNo ratings yet
- II. Modul 5 - Terapi OksigenDocument81 pagesII. Modul 5 - Terapi OksigenPerisha VeeraNo ratings yet
- PGY Duty Round整合版pdf 2020 v2Document134 pagesPGY Duty Round整合版pdf 2020 v2Jacky 許智凱No ratings yet
- Guidelines For Use of Bubble-CPAP ConcentratorsDocument10 pagesGuidelines For Use of Bubble-CPAP ConcentratorsevanNo ratings yet
- Acute Stroke Case: Rapid Identification and Initial ManagementDocument19 pagesAcute Stroke Case: Rapid Identification and Initial ManagementAsep BageurNo ratings yet
- Anesthesia and Analgesia For Geriatric Veterinary Patients: Courtney L. Baetge,, Nora S. MatthewsDocument11 pagesAnesthesia and Analgesia For Geriatric Veterinary Patients: Courtney L. Baetge,, Nora S. MatthewsPaula Andrea RodriguezNo ratings yet
- Mechanical Ventilation in ChildrenDocument74 pagesMechanical Ventilation in ChildrenBhawna PandhuNo ratings yet
- Small Animal Oxygen TherapyDocument10 pagesSmall Animal Oxygen Therapytaner_soysuren100% (1)
- Acute Respiratory Distress SyndromeDocument77 pagesAcute Respiratory Distress SyndromeAnnisa Dyah ChairiniNo ratings yet
- Fetal Movements As A Predictor of HealthDocument8 pagesFetal Movements As A Predictor of HealthWordtreader PtNo ratings yet
- I Am Sharing 'Case Study NCM 118' With YouDocument6 pagesI Am Sharing 'Case Study NCM 118' With YouQusai BassamNo ratings yet
- Cor Pulmonale EmedicineDocument16 pagesCor Pulmonale EmedicineHengki Permana PutraNo ratings yet
- Managing COPD: Nursing Care for Breathing Issues, Nutrition, Infection RiskDocument2 pagesManaging COPD: Nursing Care for Breathing Issues, Nutrition, Infection RiskAl RizkyNo ratings yet
- Oxygen - Medical Clinical Policy Bulletins - AetnaMUYMUYBUENO PDFDocument25 pagesOxygen - Medical Clinical Policy Bulletins - AetnaMUYMUYBUENO PDFSantiagochz Osuna ChairezNo ratings yet
- High Flow Nasal Prongs - Deranged PhysiologyDocument17 pagesHigh Flow Nasal Prongs - Deranged Physiologypradeep danielNo ratings yet
- Sari Clinical Care Training Learning Sequence 6 Oxygen TherapyDocument22 pagesSari Clinical Care Training Learning Sequence 6 Oxygen TherapyEstefania Cuta HernandezNo ratings yet
- Test Questionnaire in Research 1Document2 pagesTest Questionnaire in Research 1ReyaAwaliNo ratings yet
- MSC Nursing: Ruhs Entrance Examination 2019 Question PaperDocument21 pagesMSC Nursing: Ruhs Entrance Examination 2019 Question PaperSAKET TYAGINo ratings yet
- NCP For OxygenationDocument6 pagesNCP For OxygenationChriz LechNo ratings yet
- NCP Ineffective Airway ClearanceDocument1 pageNCP Ineffective Airway ClearanceImation DataNo ratings yet
- Lower Respiratory Tract InfectionsDocument19 pagesLower Respiratory Tract InfectionsCHRISTIE MONTANO100% (1)
- Oxygen TherapyDocument7 pagesOxygen TherapySudhir TyagiNo ratings yet
- Cardiogenic Shock and Septic Shock: Perioperative ManagementDocument21 pagesCardiogenic Shock and Septic Shock: Perioperative ManagementachyutsharmaNo ratings yet
- RFH COVID-19 ICU Resource Pack FULL PDFDocument15 pagesRFH COVID-19 ICU Resource Pack FULL PDFQuique GarciaNo ratings yet
- Understanding Hepatopulmonary Syndrome (HPSDocument27 pagesUnderstanding Hepatopulmonary Syndrome (HPSSidan EmozieNo ratings yet
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (15)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 3.5 out of 5 stars3.5/5 (33)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 5 out of 5 stars5/5 (5)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- The Tennis Partner: A Doctor's Story of Friendship and LossFrom EverandThe Tennis Partner: A Doctor's Story of Friendship and LossRating: 4.5 out of 5 stars4.5/5 (4)