Professional Documents
Culture Documents
(Surg2) 5.4 Urology Part 3
Uploaded by
AlloiBialbaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(Surg2) 5.4 Urology Part 3
Uploaded by
AlloiBialbaCopyright:
Available Formats
UROLOGY PART 3 SURGERY
Dr. GENLINUS YUSI
January 13, 2021 5.4
Outline
I. Testicular Cancer
II. Seminoma
III. Non-Seminomatous
IV. Renal Cell Carcinoma
V. Benign Solid Renal Tumors
VI. Renal Vein/IVC Tumor Thrombus
VII. Erectile Dysfunction
VIII. Urologic Emergencies
A. Acute Scrotum
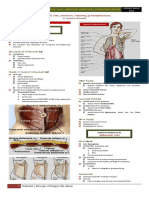
B. Torsion of testicular or epididymal appendage Figure 1: Patient had bilateral Undescended Testes with left scrotal
C. Fournier’s Gangrene mass. Lifted from PPT.
IX. Acute Urinary Retention
X. Bladder Outlet Obstruction PATHOLOGY
XI. Bladder Dysfunction
XII. Priapism • Most arise from Germ Cells.
A. Ischemic • Subdivided into:
B. Non-ischemic o Seminomatous (more common)
XIII. Paraphimosis o Non-seminomatous (poorer prognosis)
XIV. Emphysematous pyelonephritis. o Mixed
• Non-germ cell tumors arise from the Leydig’s or Sertoli
LEGEND Cells (more benign course)
Book Recording Previous Trans Must know
• The pathology determines the course of management.
Important Concept Very Important yung pathology. Because the treatment
for Seminomatous is different from Non-seminomatous.
References:
1. PowerPoint Lecture
TESTICULAR CANCER
• Most common solid malignancy in men ages 15 to 35 years
old.
• Most common presentation is an asymptomatic enlarging
intra-scrotal mass.
Curable but remember it is a cancer for young men.
RELATIONSHIP WITH UNDESCENDED TESTIS (UDT)
• Germinal dysplasia and genetic changes
There is relationship of testicular cancer with
undescended testis. The testis descends into the scrotum
very late in the gestation period. In fact, halos just before
panganak sila saka bumababa yung testis. The testis
does not go down due to germinal dysplasia and genetic
changes. This predisposes the patient an increased risk
for testicular cancer.
• 8x increased risk for cancer
• 8-9% of tumors have prior history of Undescended Testis
(UDT)
• Increased risk as well in normal contralateral testis
o 8% will develop tumor in contralateral testis if a tumor is
in the UDT.
• Orchidopexy (operation to bring down the undescended
testis into scrotum) does NOT decrease the risk, but
improves fertility and simplifies monitoring for future Figure 2: Lifted from PPT, this is what it looks like when you request
development of a mass, for ultrasound with color doppler. Ultrasound Shows Normal
If after 1 year after birth di pa din bumabagsak yung Testis. We can see the central tendon (white arrow). Color Doppler
bayag or undescended testicle pa din, do orchidopexy. allows us to visualize the blood supply. We can see the normal
Why do we do orchidopexy? pattern of lobulations.
It CANNOT change the increased risk for cancer kasi
nandyian parin yung germinal dyplasia. However, kung
ilalagay ang testes sa loob ng scrotum at nagcacancer,
madali siya madetect and could be diagnosed early.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 1 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
Figure 3: Lifted from PPT, In this ultrasound, Color Doppler shows
that the Testis is highly vascular. Before the Color Doppler was
Figure 4: Lifted from PPT, This is your Right Testis (Red Arrow),
turned on, we can see that there is a Mass (Red Arrow). So, there
we can actually bring it out through the inguinal area. This is a
is a distinct lesion on the testes, when we turned on the Color
RADICAL ORCHIECTOMY.
Doppler (Yellow Arrow), it shows that the mass is highly vascular
which is very suspicious for a testicular cancer.
• Biopsies are not usually done, unless…
A malignant focus inside the testis, seen as increase o Testicular tumor is suspected to be metastatic
vascularity. instead of primary
o Such biopsies are done inguinally.
Normal fan shape is replaced by neovascularity
o Most common metastatic testicular cancer is
METASTASIS Lymphoma.
• Chest and abdominal wall imaging. o Lymphoma usually has evidence of the disease
• Most common site of spread is the Retroperitoneal elsewhere or may manifest in the testis as a relapse
Lymph Nodes ( paracaval, inter-aortocaval, periaortic after medical treatment.
nodes), extending from Common Iliac Vessels to the Kung medyo matanda na si patient, mag isip ka ng
lymphoma.
Renal Vessels.
Metastasis of testicular cancer is very remote (malayo
Children Oncology Group (COG) System
pero hindi unlikely). Because remember your lymphatic
drainage is based on embryology. Remember Testis
didn’t come from the genitourinary sinus so ang kanyang
lymphatic supply is different from the penis and sa
bladder. It came from beside the kidney so ang tendency
nang blood supply and lymphatic drainage nang testis is
similar to the kidneys. That’s why when we do metastatic
workup we do abdominal and chest wall imaging kasi its
metastasis is commonly the LUNG.
• Evaluation of the lymphatics of the great vessels via CT or
MRI is needed.
RETROPERITONEAL LN (RPLN) METASTASIS
• RPLN are the earliest extra-gonadal metastatic site. Figure 5: Testicular Cancer Stages lifted from PPT.
• Embryologic development of the testis and the kidneys
(mesonephric ducts) occur close to each other. Stage 1- Still in the testes
Stage 2- With lymph node involvement
• They have similar lymphatics and to some extent blood Stage 3- Distant lymph node involvement
supply. T Staging
• Thus, the lymphatic drainage of the testis are at the RPLN. pTx T cannot be assessed (Prior to Radical Orchiectomy)
pT0 No evidence of T (e.g., histologic scar in testis)
MANAGEMENT
pTis Intratubular germ cell neoplasia (carcinoma in situ)
• Basic principles of surgical management of testicular CA: pT1 Limited to the testis and epididymis, no
o Prevent contamination or seeding of the scrotum by vascular/lymphatic invasion.
tumor, upstaging it to T4 to avoid an inguinal LN pT2 Limited to the testis and epididymis with
metastasis which occurs relatively early. vascular/lymphatic invasion or tumor extending
through tunica albuginea with involvement of
Kasi you want to keep the contamination of the testis tunica vaginalis.
sa tunica lang (dun lang sa kanya), wag mong paabutin pT3 Invades the spermatic cord with or without
sa scrotum kasi pag natamaan yung scrotum biglang vascular/lymphatic invasion
upstage yan papangit agad prognosis niyan. N Staging
o Percutaneous scrotal incisions or biopsies are avoided. NX Regional lymph nodes cannot be assessed
NO No regional lymph node metastasis
o All access to the testis are done via the inguinal route. N1 LN mass <2 cm in greatest dimension or multiple
So we don’t stick the needle through the scrotum, lymph node masses, none >2 cm in greatest
what we do through anesthesia we pull the testis to the dimension.
inguinal area.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 2 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
N2 LN mass >2 cm but <5 cm in greatest dimension, or SEMINOMA
multiple LN masses, any one mass >2 but <5cm in
greatest dimension.
N3 LN mass >5cm in greatest dimension
M Staging
M0 No evidence of distant metastases
M1 Non-regional nodal or pulmonary metastases
M2 Non-pulmonary visceral masses
TREATMENT
Initial Treatment
• Radical Orchiectomy (aka Radical Inguinal or Inguinal
Orchiectomy) Incision is at the inguinal area. Figure 8: Seminoma Lifted from PPT
o Spermatic cord is dissected and mobilized down into the
external ring and scrotal chamber. • Can be pure or mixed
o Testis and tumor is pushed through the external ring, en • Most common type of testicular cancer
bloc into inguinal incision. • Pure seminoma generally has normal tumor markers.
• 20% of pure seminomas can have elevated Beta-hcg.
You can do tumor marker before the surgery and
normally, seminoma is normal tumor marker, pero kung
may elevation, most probably it is non-seminomatous.
• Mixed tumors can have elevated Alpha-Feto Protein.
• Very radiosensitive
• Also, quite chemo-sensitive
Most of the time, combined ang radiotherapy and
chemotherapy for the treatment of seminoma.
• Good prognosis
Mas madaling gamutin ang seminoma kaysa sa non-
Figure 6: Radical Orchiectomy lifted from PPT seminomatous.
We prefer to do chemotherapy first before radiation
therapy, because if you do it the other way around, sunog
ang blood vessels baka di na pumasok ang gamot for
chemotherapy. Kung hindi parin lumiliit then you can do
salvage radiation therapy.
NON-SEMINOMATOUS
Figure 9: Non-Seminomatous lifted from PPT
Figure 7: Radical Orchiectomy (lifted from PPT), dissect the spermatic • Embroyonal CA, Yolk Sac tumor, Polyembryonal,
cord, immobilize it down to the external ring then push the scrotum Choriocarcinoma, Teratoma, etc
up para mag pop out yung testis into the inguinal incision. This is the • Responds well to chemotherapy but not with radiation
gubernaculum testis this is what keeps it in the scrotum (Red Arrow). • Elevated tumor markers (B-HCG, AFP)
So puputulin mo yan then divide that para ma reduce yung scrotum. Tumor marker get done before preop, pag inoperahan
mo tingnan mo kung babagsak.
• Retroperitoneal lymph node metastasis is common
Metastasis is more common in non-seminomas. Do a
dual CT scan of the abdomen to see the metastasis in
lymph nodes.
• Poor prognosis
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 3 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
RETROPERITONEAL LN DISSECTION
Figure 12: Renal Cell Carcinoma or Kidney Cancer lifted from PPT.
Figure 10: Retroperitoneal Lymph Node Dissection lifted from PPT
No need to memorize
Right testes (A), nodes to take out are paracaval, intra- Clear cell CA- most common
Sarcomatoid-worst prognosis
aortocaval, paraaortic, then on the same side of testes, obturator
node ang aalisin. Same goes sa left side (B). PRESENTATION:
Essentially you get all the lymph nodes except for the • Most common presentation is painless hematuria,
paraaortic (you leave this alone). You get the paracaval, intra- microscopic or gross.
aorta caval, common iliac and everything down. Hematuria could also be cause by UTI, kidney stones or
tumors. Lahat yan can present with hematuria. Kaya it is
important to determine the cause of hematuria.
• Classic Triad of Renal Cell CA:
o Painless hematuria
o Flank pain
o Abdominal mass
Bihira na lang itong symptom na to kasi nauunahan
na ng pagdiscover since andaming clearance for work
like UTZ, kitang kita agad na may mass.
Pag napapalpate mo na yung mass, ibig sabihin
malaki na talaga siya. Kidney is a retroperitoneal
organ, below the ribs. Kaya pag napalpate mo na siya
ibig sabihin sobrang laki na.
• Smoking is the only risk factor identified
• Classic “triad” is seen in only 10% of cases
• Most cases are caught due to advances & ubiquity of
Figure 11: Kocher Maneuver lifted from PPT ultrasonography.
• Various histologic subtypes include:
Kocher maneuver is a surgical maneuver to expose o Clear cell
structures in the retroperitoneum behind the duodenum and o Papillary (types I and II)
pancreas. First is to immobilize ang ascending colon then o Chromophobe
extend excision towards the Ligamentum Treitz para maiiswing o Collecting duct
o Unclassified forms
mo sa isang side yung lahat ng bituka. Bale dapat makikita yung
likod na part ng peritoneum. Then get all the lymph nodes. BENIGN SOLID RENAL TUMORS
This is transabdominal procedure; you have to expose the
great vessels, so it is like a trauma operation. You do the incision
at level of the ligament of Treitz right beside the inferior
mesenteric artery and vein.
RENAL CELL CARCINOMA
• A.K.A. - Hypernephroma, Adenocarcinoma of the
kidney, Internist’s Tumor.
• Malignancy of the renal epithelium that can arise from any
component of the nephron,
o Most are said to be from the proximal convoluted
tubule (PCT). Figure 13: Oncocytoma lifted from PPT
• Most are sporadic
o Some are hereditary or congenital factors may be Very few, very rare
involved. • Benign lesions, which are more commonly found when
• These frequently involve a germ line mutation in a tumor- small tumors are removed, include oncocytomas and
suppression gene angiomyolipomas.
o Such as Von Hippel-Lindau (VHL gene) Syndrome Oncocytoma, spokewheel appearance. Central tendon
which can have bilateral tumors. gap. Very distinct.
Sounds malignant but this is benign.
Angiomyolipoma, Angio = blood vessel; Myo = muscle;
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 4 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
Lipoma = fat. Makikita sa ultrasound is hyperechoic solid
renal mass of the fat. Minsan makikita mo na sa result ng
ultrasound na diagnose as angiomyolipoma but this should
be diagnosed histologically.
Sobrang lumalaki ito but still benign pa din.
• ALL solid renal tumors are considered malignant until
proven otherwise.
Almost a hundred percent ng lahat ng solid renal tumor
is nagrerecommend kami to undergo surgery.
• Benign tumors are rare & are thus unlikely when a solid
renal tumor is encountered.
RENAL CYSTS
Figure 14: Renal Cyst lifted from PPT
Common in Mid-40s and up, but 98% of them are benign
but still have to test them.
• Renal cancers are usually solid, but they may appear
cystic.
• ALL renal cysts have to be evaluated for the possibility
of being malignant.
CLASSIFICATIONS OF RENAL CYSTS
• Evaluation is guided by the Bosniak Renal Cyst
Classification, which requires a CT-Scan with Contrast.
But we don’t do CT Scan with Contrast in Bosniak 1 and
2 (small and few) which can be diagnosed with ultrasound.
The the only ones that require CT Scan with contrast are
large, multiple cyst and cyst with malignant features in
ultrasound.
o Simple renal cysts
▪ Commonly observed in normal kidneys
▪ Increasing incidence as an individual ages.
▪ Benign, asymptomatic Bosniak Classification in CT Scan.
▪ Rarely require treatment. • Bosniak 1
o Complex renal cysts o Simple and Thin-walled cyst (Red circle)
▪ Higher incidence of malignancy
• Bosniak 2
• BOSNIAK CLASSIFICATION o Maliit na Calcification, hindi pa yan nag
enhance(Purple Circle)
• Bosniak 2F
o Contains multiple hairline septa(Sky Blue
Circle)
• Bosniak 3
o Thick wall cyst, may enhancement (Yellow
Circle)
• Bosniak 4
o Enhanicing solid component, meron nang
solid lesion sa loob, malignany nayan. (Pink
Circle)
Get housefield unit of the cysts before and after the contrast
then compare. If di nag-enhance, benign yon. One big feature
for malignancy is ti enhances when you give contrast.
Figure 15: Bosniak Classification lifted from PPT (enlarged image at Bosniak 2F is higher than 2 but still considered benign. It is
the appendix) a dense cyst but it does not enhance
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 5 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
MANAGEMENT OF RENAL CYSTS
• Bozniak 1 to 2f cysts are considered benign, they however
differ in how they are followed up
o Bozniak 1: Requires only yearly follow-up with
creatinine and renal ultrasonography.
o Bozniak 2: Requires follow-up every 6 months.
o Bozniak 2F: Requires follow-up every 3 months for a
year, then every 6 months, if there is no change.
Bosniak 3: Consider surgery
Bosniak 4: Malignant na
METASTASIS
• Most common sites of metastasis are the retroperitoneal
lymph nodes, lungs but liver, bone, and brain also are
common sites of spread.
• 20-30% present already with metastatic disease.
• Tests for metastasis include Chest CT, Bone Scan & Liver
Function Tests.
Figure 18: TNM Staging (enlarged image at the appendix)
RADICAL NEPHRECTOMY
• Gold standard for the curative treatment of Renal cell
carcinoma
• Radical nephrectomy includes the kidney and upper urinary
tract plus:
o Gerota’s fascia
o Perirenal fat
o Ureter
o Adrenal gland (if the tumor is large grossly
involving the adrenal or if it is predominantly upper
pole)
Figure 16: Staging of Renal Cell Carcinoma
Sa stage 1 and 2, kaya pang tanggalin completely. Figure 19: Bilateral Chevron Incision (Left Image), Radical
Pag nag extend beyond Gerota’s fascia or perinephric fascia Nephrectomy (Right Image)
which is a great barrier from infection, stage 3 na. Mahirap na
tanggalin. Bilateral Chevron incision (Left Image) following the contour
of the costal ribcages. Thoraco-abdominal incision so
Stage 4, meron ka na adjacent organ involvement.
pumapasok sa luob nang thoracic cage into the peritoneum, we
do this for large tumors that extend superiorly.
Kidney Position (Right Image) there is a broken table, para
may angle to push the kidney more superficially.
Figure 17: TNM Staging (enlarged image at the appendix)
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 6 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
PARTIAL NEPHRECTOMY
Figure 20 Partial Nephrectomy lifted from PPT
Figure 24 Partial Nephrectomy lifted from PPT
Sometimes we do partial nephrectomy if the tumor is So, in partial nephrectomy, first locate the vessels, ligate
EXOPHYTIC or nakalabas siya. the vessels, next is wedge the tumor, next is fix the
When we already immobilized the kidney then we put it collecting systems, then lastly, repair and fix the kidney
under Ice Slush then we clamp the artery. capsule.
Since it is just a Partial Nephrectomy the rest of the
kidneys should restore itself.
Figure 21 Partial Nephrectomy lifted from PPT Figure 25 Partial Nephrectomy lifted from PPT
This one for large tumor, minsan di na nakukuha yan pero
For example, the encircled structure is a mid-portion this one kinaya first locate the vessels then ligate it, wedge
tumor so what we do here is locate the posterior the tumor then repair.
segmental artery ligate it in order to wedge the tumor then
dugtong ulit.
The pointed structure is a superior pole tumor, we can do
partial nephrectomy also.
Figure 26 Partial Nephrectomy lifted from PPT
This is a very large mid-portion tumor of the kidney. What
we do here is slice the kidney into half so kalahati nalang
ang kidney but make sure the blood supply are intact as well
as the ureter. I think we did It once pero successful naman
Figure 23 Partial Nephrectomy lifted from PPT
kasi very rare na sobrang perfect na nasa middle portion
If the tumor is really a large middle portion we can do and tumor.
something like a donor nephrectomy. Take out the kidney
take note mahaba yung vessels ang gagawin naming
tatapyasin namin then irerepair.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 7 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
RADICAL NEPHRECTOMY
Figure 30 Radical Nephrectomy Left Anterior Aspect lifted from
PPT
Figure 27 Radical Nephrectomy lifted from PPT Now this is the gross specimen, so this is a radical
This is a plain CT Scan without IV contrast although meron nephrectomy of the left kidney. The encircled portion is
considered as normal kidney tissue. So, if you will observe
na ditong intestinal contrast, it shows a solid mass in the left the other portions are the mass itself indicating that this is
kidney. Kitang kita dito na there is no delineation as an exophytic tumor. The problem here is sobrang dikit ng
compare to normal kidneys. tumor sa normal kidney mula sa superior pole down to
inferior pole kaya hindi na partial nephrectomy ang
procedure na ginawa dito.
Figure 28 Radical Nephrectomy lifted from PPT
Figure 31 Radical Nephrectomy Left Posterior Aspect lifted from
This is now a CT scan with contrast, you can see now the
enhancing mass. PPT
The encircled portion is considered as normal kidney tissue
of the posterior aspect.
Figure 29 Radical Nephrectomy lifted from PPT
Figure 32 Radical Nephrectomy Left Sectioned Sagittal lifted
We can now see the delineation of the mass and the normal
from PPT
kidney.
In this gross specimen the vessel is already involve within
the tumor affected kidney portion.
The encircled portion is the normal kidney parenchyma. As
you can see it is impossible to do partial nephrectomy here.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 8 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
MINIMALLY INVASIVE SURGERY
• Laparoscopic Radical Nephrectomy is considered
the “gold standard”.
• More rapid convalescence and decreased narcotic
requirements.
• Laparoscopic Partial Nephrectomy can also be
done but is still not considered the “standard of care”.
Conventional Partial Nephrectomy still is.
• Most small renal masses are low grade with a slow
growth rate, and patients very rarely progress to
metastatic disease after limited follow-up of 2 to 3
years.
Figure 33 Laparoscopic Radical Nephrectomy lifted from PPT
Figure 35 Laparoscopic Radical Nephrectomy lifted from PPT
Laparoscopic radical nephrectomy is done in this
manner under general anesthesia. So here ipapasok transabdominal then to the
peritoneum.
Figure 36 Laparoscopic Radical Nephrectomy lifted from PPT
This is a left side case so here just displaced the
descending colon from the tumor and the kidney.
Figure 34 Laparoscopic Radical Nephrectomy lifted from PPT
Usually, 3 tusok yan sometimes 4. All the surgeons on
one side
Figure 37 Laparoscopic Radical Nephrectomy lifted from PPT
Locate the ureter and dissect it up. Here hindi dapat
masyado mobilized ang kidney kasi otherwise
babagsak ang kidney.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 9 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
Figure 41 Laparoscopic Radical Nephrectomy lifted from PPT
Figure 38 Laparoscopic Radical Nephrectomy lifted from PPT Pagnatapyas na put it in the lap sac already in preparation
to exploralize.
Once madisplaced na ang ureter you can now go to the
pedicle or renal hilum.
Figure 42 Laparoscopic Radical Nephrectomy lifted from PPT
For very large tumor, imomorcellate.(Morcellation-Cutting
tissues into small pieces to allow removal
laparoscopically).
RENAL VEIN/ IVC TUMOR THROMBUS
• 10% of RCC invades the lumen of the Renal Vein or
the Inferior Vena Cava (Tumor Thrombus).
• Tumor Thrombus Embolization to the pulmonary
Figure 39 Laparoscopic Radical Nephrectomy lifted from PPT artery is rare but known complication during these
cases is associated with a high mortality.
This is very complicated procedure that is why we
Once in the pedicle already, locate the artery first, usually do this procedure with thoracic surgeon.
divide, ligate, then follow the vein. Pagnaputol mo There is one case we handled talagang umabot sa
nayan lalambot nayan. atrium yung thrombi what we did was we transferred
the patient to heart center don ginawa ang procedure.
The thrombus is usually not adherent to the vessel wall.
Kaya talagang lulutang lutang lang ang thrombus sa
IVC so pag biglang umakyat ang thrombus it might
cause sudden severe pulmonary embolism which is
deadly.
Figure 40 Laparoscopic Radical Nephrectomy lifted from PPT
Once maputol na ang pedicle you can now mobilize the
kidney completely.
Figure 43 IVC Tumor Thrombus lifted from PPT
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 10 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
ERECTILE DYSFUNCTION
Most common form of male sexual dysfunction.
• Erectile dysfunction is defined as the inability to
achieve and maintain an erection sufficient for
satisfactory sexual intercourse.
• Erection is a neurovascular event.
• Most common cause of ED is psychogenic.
• Erection is modulated by the parasympathetic NS.
Stress and performance anxiety will make ED worse.
• Similar to ejaculation which is modulated by the
sympathetic NS, stress and anxiety will cause
premature ejaculation.
Figure 46 GTP and Nitric Oxide Pathway lifted from PPT
This is just the GTP and Nitric Oxide pathway.
Figure 44 Flaccid and Erect State lifted from PPT
Flaccid State: ABG result no or low arterial blood
and not well oxygenated.
Erect State: ABG result more arterial blood and
Figure 47 Causes of ED lifted from PPT
very well oxygenated.
The common causes of ED are neurogenic,
psychogenic, vasculogenic, and endocrine.
Other causes are also shown here in this illustration
like the surgical, drugs, diabetes and so forth.
CAUSES OF ERECTYLE DYSFUNCTION
Figure 45 Drugs for Erection and their MOA lifted from PPT
This illustrates only the pharmacodynamic of
drugs for erection and where their target action is Figure 48 Causes of ED lifted from PPT for larger image see
exerted. appendix
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 11 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
▪
Nitrate-based drugs used in
conjunction with PDE5Is are an
absolute contraindication:
Because nitrate-based drugs also
use the nitric oxide pathway.
In the history the first thing to ask is
what are the medications you are
currently taking.
• Sublingual nitroglycerin,
ISDN, ISMN, Amyl nitrate.
• Can produce a potentially
fatal sudden drop in blood
pressure.
▪ Alpha-adrenergic blockers
• Terazosin and Doxazosin,
especially Alfuzosin and
Tamsulosin have lesser
Figure 49 Sexual Health Inventory for Men (SHIM) lifted from interactions.
PPT for larger image see appendix TREATMENT: INTRACAVERNOUS INJECTION
For research purposes
• 1-7 Severe ED
• 8-11 Moderate ED
• 12-16 Mild to Moderate ED
• 17-21 Mild ED
• 22-25 No ED
IMPLICATIONS OF ED
• The presence of ED in a known healthy man can signify
the evaluation of early systemic diseases that
commonly affect the vascular system, such as: Figure 50 Intracavernous Injection lifted from
o Diabetes Mellitus PPT
o Hypertension
o Atherosclerosis
Prostaglandin E1 (APROSTADIL)
• The penis has among the smallest arteries, and any It is self-injected medication. Meaning yung patient
vascular dysfunction will first affect erectile function mismo ang mag-iinject in certain area of their penis.
being a purely neurovascular phenomenon. Iiwasan nila yung dorsal vein and penile nerve.
TREATMENT: GENERAL Inject directly to one corpus cavernosum kahit sa isa
• Clean Living lang pareho na titigas.
The only problem here is lakasan ng loob talaga kasi
• Quit Smoking isipin niyo yung patient mismo ang mag iinjetion sa
• Lose Weight sarili tapos sa ari pa medyo ang hirap isipin paano nila
• More Exercise gagawin yun diba. The patient here should be very
highly motivated na talaga gusto nilang mag erection.
• Complete Sleep TREATMENT: INTRAURETHRAL SUPPOSITORY
• Avoid Alcohol
TREATMENT: ORAL DRUG THERAPY
• Phosphodiesterase-5-inhibitors (PDE5I)
o Viagra or Sildenafil
o Phosphodiesterase converts cGMP to 5’
cGMP.
o Enhances the effect of nitric oxide by
inhibiting the breakdown of cGMP, which
accumulates and in turn enhances and
prolongs cavernous muscle relaxation.
o Examples: Sildenafil, Vardenafil, Tadalafil
o Improves the response, they do not trigger
an automatic erection.
o Usually taken at least an hour before sexual Figure 51 Intraurethral Suppository lifted from
activity. “On-demand” pill. PPT
o There is a need for the usual sexual
This product naman is intraurethral ipapasok mismo sa
stimulation and attraction.
urethra then pag naipasok na patient will press the
o Generally, 70% success rate.
button to release the tablet.
o Drug Interactions:
But base sa experience ng mga patient ko this is not
so effective because it is a little bit hassle to use kasi
pagkatapos mo iinject mamassage massage mo pa
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 12 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
para matunaw yung tablet at para mag spread minsan • Torsion patients usually have a congenital high
naiinip and napapagod na ang patient tapos tinatamad attachment of the tunica vaginalis, such that the testicle
na pagkatapos so this product is not so successful, but can rotate freely on the spermatic cord.
it is still available in the market.
• Known as a “Bell-Clap Deformity”
• The testicle lies transverse as opposed to a longitudinal
lie of the affected testes.
• This congenital abnormality is present in approximately
12% of males.
• Twists spontaneously on the spermatic cord, causing
venous occlusion and engorgement, with subsequent
arterial ischemia and infarction.
• Experimental evidence indicates that 720 degrees twist
is required.
• In neonates, the testicle frequently has not yet
descended into the scrotum, after which it becomes
attached within the tunica vaginalis.
o This increased mobility of the testicle
Figure 52 Vacuum Erection Device lifted from PPT predisposes it to torsion (extravaginal
testicular torsion)
So this is a very classical device and very effective way
to sustain an erection. It has penile ring that should be
put first, then put the suction device. So ang gagawin
ng device na ito hihilain niya ang penis ng patient to
have a suction effect sa cavernous to have a very good
blood flow. So pag okay na put out the suction tube
since may penile ring na nakakabit sa penis ni patient
it will prevent the backflow of blood by that sustaining
the erection.
UROLOGIC EMERGENCIES
ACUTE SCROTUM
• “Acute Scrotum” is the urologist’s counterpart of the
General Surgeon’s “Acute Abdomen”
• Both conditions are guided by similar management
principles.
• Management:
o The mainstay for acute scrotum is history and
physical examination.
o Imaging merely complements, and will NOT
replace good clinical judgement. Figure 53 Normal Location of Testis lifted from PPT
o When in doubt, EXPLORE! Normally, the testis is embedded in tunica vaginalis
• Causes of Acute Scrotum kaya hindi talaga iiktot yan. Yung tunica vaginalis na
o Ischemia tinuturo diyan ay nagseserve as shock absorber and
o Trauma
nag cocool down sa bayag kasi ang gusto nga naten
o Infectious
o Inflammatory ay malamig na bayag kasi for fertility purposes.
▪ Scrotal wall Heinrech-Scholein
purpura (HSP), Fat Necrosis
o Hernia
▪ Incarcerated, Strangulated; with or
without testicular ischemia.
o Acute on Chronic Events
▪ Rupture/hemorrhage/infection of
Spermatocele, Hydrocoele,
Testicular Tumor
o Markedly Symptomatic Varicocele
TORSION (ISCHEMIA)
• When the testicle spontaneously twists thus
obstructing the blood supply, causing necrosis and Figure 54 Location of Testis lifted from PPT
pain.
A. normal location di magrorotate yan.
• The testicle is normally adherent to the tunica vaginalis
on the postero-medial aspect, thus limiting the twisting B. ito medyo magrorotate ito
movement. C. ito magrorotate talaga ito
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 13 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
A. Intravaginal Torsion which is the most common.
B. The Extravaginal Torsion is usually seen in
neonates kasi shempre diba nakadescend ng maayos
ang testes ng mga neonates.
C. The Torsion is due to long mesorchium most often
occur as a consequence of anomalies of epididymal
disjunction or elongated epididymis, conditions that are
highly frequent in cryptorchism.
CLINICAL PRESENTATION
• Left testicle more commonly affected.
• Among neonatal testicular torsion cases, 70% occur
prenatally and 30% occur postnatally.
• The testis salvage rate approaches 100% in patients
who undergo detorsion within 6 hours of the start of
Figure 55 Normal Scrotum VS Bell-Clapper Deformity lifted from pain.
PPT First thing to ask if you are suspecting testicular
tortion is anong oras po unang sumakit ang bayag
So, this is another diagram the blue here is the
niyo?
potential space that will determine if the testis will rotate Pagkatapos dalhin na agad sa operating room.
or not. So pag sakop na sakop niya ang testis na
• However, there is only a 20% viability rate if detorsion
parang nakalutang na ang testis tataas ang chance na occurs >12 hours.
mag rorotate talaga ito tulad ng sa pangalawang
• Virtually no viability if detorsion is delayed >24 hours.
picture.
• Rapid or sudden of onset of severe testicular swelling
and pain.
• The onset of pain can be preceded by trauma, physical
activity, or more commonly, by no activity (e.g. During
sleep).
Kaya usually pinagpapabukas pa kasi usually
madaling araw siya nangyayare eh diba sabi
ko very important ang 6 hours para mataas pa
ang viability na hindi pa nag undergo ng
infarction ang testes.
The problem pa sa torsion pwede din
mamaga yan edi mapagkakamalan pang
epididymoorchitis eh ito naman wala
problema pwedeng pwede na antibiotic
therapy eh paano pag torsion eh urologic
emergency ito that is why clinical judgement
is very important.
Figure 56 Testicular Torsion Deformity lifted from PPT
• So, this illustration shows na sa testicular torsion
nakailang ikot talaga yan diba 720 degrees so
maraming ikot yun so meaning two 360 rotation ang
usually nangyayare.
Figure 58 Clinical Presentation of Torsion lifted from PPT
The first picture is a neonatal testicular torsion
parang namutla lang ditto yung scrotum ng
patient.
Second picture ang sinasabi lang dito is we
can do transillumination kasi baka naman
tubig lang ang laman.
Third picture shows na namamaga yung
Figure 57 Types of Torsion Deformity lifted from PPT kaliwa eh diba usually affected is left.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 14 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
• It most often occurs in children or adolescents but may
occur at any age.
• Torsion should be in the differential for any sudden
acute scrotal pain or swelling.
• Exquisitely tender testicle with a high, horizontal lie.
• The twisted cord can be palpated through the scrotum
when examined early, but later edema and
inflammation will make the hemiscrotum appear like a
confluent mass (12-24).
Figure 61 Color Doppler Ultrasound lifted from PPT
Figure no. 39 shows that the left testis has no blood
flow in the color doppler ultrasound suggesting
possible testicular torsion.
• The mainstay of diagnosis is an emergency Color-
Doppler Ultrasound.
• Color-Doppler will show decreased perfusion for
torsion and increased for epididymitis.
• Ultrasound will also diagnose other possible causes of
acute scrotum such as hernia and trauma.
Figure 59 Acute Epididymoorchitis lifted from PPT
• When swelled, it will appear indistinguishable from
acute epididymoorchitis.
This one is acute epididymoorchitis which is commonly
the top differential diagnosis of torsion.
Figure 62 Whirlpool Sign lifted from PPT
The whirlpool sign is the spermatic cord na nagtwist.
Figure 60 Prehn Sign lifted from PPT
• Prehn Sign- gently elevate the testis with your hand. If
the pain is relieved upon lifting over the symphysis
pubis, this is recorded as a (+) Prehn Sign, which is
indicative more for epididymoorchitis.
The patient is in supine position, then elevate the testis
kung baga parang babawasan mo yung tension ng
testis so if the pain is relieved then that is a positive
prehn sign pag lalo sumakit torsion yun.
Figure 63 Testicular Torsion lifted from PPT
This picture is a good summary of the testicular
torsion.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 15 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
TREATMENT
• It is better to explore a testis unnecessarily than to
neglect to do so when needed.
AGAIN, WHEN IN DOUBT EXPLORE!
• Best results are obtained when exploration is done
within 4-6 hours of the incident.
• >12 hours, testicular atrophy is significant.
Pag more than 12 hours usually makikita mona itim na
so pag ganon mag orchiectomy kana lang.
• If >24 hrs or with no improvement after detorsion,
orchiectomy or orchidectomy is done.
Even if may konting improvement, pag more than 24
hours wala ng detorsion, orchiectomy agad kasi baka
mamatay din eventually, you’ll have dead tissue then Figure 65: UTZ. Arrow is pointing to the testicular
mag abscess yun and result to sepsis. appendage that is edematous. Lifted from PPT.
• An orchidopexy or orchiopexy is ALWAYS performed
on the contralateral as the “Bell-Clapper Deformity” is
usually bilateral.
You would suture the testis to the tunica vaginalis
posteriorly, otherwise baka yung contralateral testis
naman ang magtorsion
• If the testis is to be preserved, an orchidopexy is also
performed.
• Orchidopexy is done by anchoring the tunica albuginea
of the testis to the overlying parietal tunica vaginalis
and scrotal dartos muscle.
• Some patients can have “Intermitted Torsion”, a
Figure 66 Color Doppler study showing no blood supply to
bilateral prophylactic orchidopexy can be done. the testicular appendage pointed by arrow while there is
"Intermittent" testicular torsion is a well-recognized entity in hyperemic LE (Left epididymis) and LT (Left Testis)
which a classic torsion history is obtained, but physical
examination and ultrasound findings are normal. TREATMENT
Intermittent torsion – sumasakit ung testis then • The process is often self-limited, with the infarcted
nawawala spontaneously. Don't wait for it to be full appendage undergoing atrophy with time.
blown testicular torsion, mag orchidopexy kaagad. for most cases, self-limiting. Just give antibiotics.
TORSION OF TESTICULAR OR EPIDIDYMAL • If exploration is pursued, the appendage is simply
APPENDAGES excised and no orchidopexy is needed.
• Small polypoid appendages are often found attached to the can appear as an acute scrotum so sometimes it is
testis or epididymis and are either Mullerian or Wolffian duct more prudent to do exploration.
remnants. FOURNIER’S GANGRENE
• Can also present with the acute onset of scrotal pain and
mass.
• The testis is palpable and has a normal lie(longitudinal).
• When examined early, the edematous, torsed appendage
can often be palpated at the upper pole of the testis.
• If the torsed appendage is ecchymotic, it can usually be
seen through the skin and represents the "blue-dot
sign."
Sometimes may makikita na kulay blue
Figure 64 Arrow is pointing to the testicular Figure 67 Fournier’s Gangrene
appendage that undergo torsion. Lifted from PPT.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 16 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
• Scrotal wall infections may result from infected sebaceous EPIDIDYMITIS & EPIDIDYMOORCHITIS
cysts, folliculitis, or other dermatologic conditions. Epididymitis progressed to epididymoorchitis
Starts as parang pimple then nangati, kinamot lang, o Most of the time due to retrograde infection which
nagkagalos, diabetic yung patient then nag gangrene. comes from the urine, enters vas deferens to the
• Fasciitis of scrotum and groin, termed Fournier’s gangrene, epididymis then eventually mainvolved yung testis to
involves a rapidly progressive, life threatening infection of become epididymoorchitis.
the genital soft tissues. o It is very rare to have pure orchitis, kung meron man
• Associated with predisposing issues including urethral due to blood borne staphylococcus infection or TB.
perforation and periurethral abscess and is most often seen • Differential when patient presented with acute scrotum, very
in the immunocompromised or diabetic patient. common.
• Diffuse enlargement, thickening and erythema of the scrotal
• May be difficult to distinguish from scrotal trauma or testis
wall, groin, and perineum.
torsion.
• There may be necrotic black or ecchymotic patches of
• However, treatment is medical.
genital skin present.
Antibiotics lang yan and pain reliever
• The most diagnostic is the finding of crepitus, a spongy,
cracking feeling within the skin that indicates gas- • Affects males of virtually all ages.
producing microorganisms that is methane underneath that • Usually results from the spread of infection from the
can be felt in the scrotum or perineum. An early sign of bladder, urethra, or prostate via the ejaculatory ducts and
fournier’s gangrene vas deferens into the epididymis.
Crepitus – pag hinawakan mo ang skin parang may ETIOLOGY
cellophane sa ilalim ng skin. • Infectious: Sexually transmitted Disease, UTI, Bladder
In patients with uncontrolled DM, more sugar, more Outlet Obstruction, BPH
• Non-Infectious: Adverse drug reaction, Urinary reflux in
microorganisms that will then produce methane gas
that would insinuate under the skin producing crepitus. ejaculatory ducts, sperm fluid extravasation from
vasectomy or blunt trauma
• When left untreated, can progress over more hours and • In boys, related to UTI and/or underlying GU congenital
result in overwhelming bacterial sepsis with an associated
high mortality rate. anomaly
TREATMENT • In elderly men, BPH and associated stasis, UTI, and
catheterization is the most common cause of epididymitis.
• Therefore, broad spectrum antibiotics that cover aerobic
and anaerobic organisms, and urgent and repeated surgical • Bacterial prostatitis and/or seminal vesiculitis are
drainage and debridement are required to control the associated with epididymal infection in postpubertal males
infection. of all ages.
Repeated surgical drainage and debridement – • STDs for younger men <35 y/o
halos araw araw ang surgery, you keep doing it until • Can progress to involve the orchitis as well, becoming
kulay pink, walang mabaho at malinis na malinis. “epididymo-orchitis”
• Incision and drainage with gauze packing and broad- • Most common organisms:
spectrum antibiotics are prescribed for these superficial o Coliforms or bacteriuria organisms
conditions. o For younger men <35 y/o heterosexuals, usually N.
• Aggressive treatment is mandatory even for superficial gonnorhea and C. trachomatis
conditions since these can easily progress. o For homosexual men, usually E. coli and H. influenzae
o Mycobacteria
Especially for patients with Diabetes and
o Viral, Fungal, Mycoplasma or parasitic but very rare.
immunosuppressed like HIV and transplant patient.
DIAGNOSIS
Result from any kind of purulent infection in the
perineum in the elderly male in the scrotum but can • PE: localizes the tenderness to the epididymis.
happen in women as well. • Most patients at the time of presentation will have testicular
involvement in the inflammatory process with pain,
epididymoorchitis.
• Spermatic cord is usually tender and swollen.
• Pain starts early in the tail of the epididymis, later involving
its entirety, with edema, epididymitis can become so large
that it can be indistinguishable from the testis.
• Primary goal initially is to distinguish between and
epididymoorchitis and testicular torsion.
• (+) Prehn’s sign
On PE, the affected hemiscrotum is elevated. This
action relieves the pain of epididymitis but
Figure 68: Fournier’s Gangrene Figure 69: Fournier’s Gangrene. exacerbates the pain of torsion.
CT scan showing gas packets as • Torsion will have a transverse lie.
pointed by the white arrow. • Later stages, more difficult to distinguish clinically.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 17 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
• Color-Doppler UTZ is the gold standard.
BLADDER DYSFUNCTION
• Decreased or absent bladder contractility
o Diabetic neuropathy
o Multiple sclerosis
o Parkinson’s disease
o Spinal cord lesions or injuries (S1-3)
o Narcotic or Anti-cholinergic meds
ACUTE URINARY RETENTION
• If the urinary retention has lasted several days (often
accompanied by overflow incontinence), patients may be in
Figure 70: Acute Epididymo-orchitis. Figure 71: Acute Epididymo-orchitis. renal failure.
Heterogenous epididymis & testis. Color Doppler shows increased • Treatment should be placement of urethral catheter as
Enlargement of epididymal head. vascularity of testis and epididymis. quickly as possible.
Reactive hydrocele
• If urethral catheterization attempt fails, a percutaneous
TREATMENT suprapubic tube cystostomy should be done.
• If a patient is toxic with high-grade fever, chills, nausea &
vomiting, treatment is similar to Acute Pyelonephritis or
Acute Prostatitis.
• Treatment with hydration, parenteral fluoroquinolones.
• May shift to oral, once afebrile for 24 hours without
antipyretics.
• 3-4 weeks treatment
long term because of the blood-testis barrier,
antibiotics do not usually get to the parenchyma of the
Figure 73: Tip of Coude catheter Figure 74: Foley catheter.
organ, so instead of giving high doses, we give it more
which is slightly rigid and angled.
long term for minimum of one month.
This is a special kind of catheter
ACUTE URINARY RETENTION for patients with enlarged
• Voiding is a function of 2 synergistic processes: prostate and elevated bladder
o Bladder contraction neck.
o Bladder outlet opening
• Both processes should be working for efficient voiding to .
happen. A problem in at least one can progress to AUR.
BLADDER OUTLET OBSTRUCTION
• Functional Bladder outlet obstruction
o Constipation
o Detrusor-Sphincter Dyssynergia
Figure 75: Three-way
catheter. The uppermost
tube is for irrigation. The Figure 76: Suprapubic catheter.
middle is where urine exits
and one with the green tip is
for inflation of balloon.
PRIAPRISM
• Voiding is a function of 2 synergistic processes:
• Persistent erection for greater than 4 hours unrelated to
sexual stimulation.
• From Priapus, who was a minor rustic fertility god, protector
of livestock, fruit plants, gardens, and male genitalia.
Figure 72: Detrusor Sphincter • Priapus is marked by his absurdly oversized, persistent,
Dyssynergia. There is overactive bladder erection.
and sphincter. • The main features that distinguishes the erection in
priapism compared to a normal erections are:
• Anatomical
. Bladder outlet obstruction
o Persistent & prolonged (> 4 hrs)
o BPH
o Painful or tender
o Blood clot
o Flaccid glans
o Bladder Neck Stenosis
o Unrelated to sexual stimulation
o Meatal stenosis
• Types of Priapism
o Urethral Stricture (M) / Urethral Stenosis (F)
o Ischemic priapism
o Non-Ischemic priapism
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 18 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
ISCHEMIC PRIAPRISM
• Most common.
• Urologic emergency.
• The penis is very tender and both cavernosal bodies will be
rigid while the glans will be flaccid.
• In the normal erection, there is decreased venous outflow
with persistent arterial inflow resulting in increased
intracorporal pressure, followed by the release of venous
outflow & subsequent tumescence.
• With ischemic priapism, release of venous outflow is
impaired, erection is thus prolonged. Figure 78: Using a big bore needle, puncture the apex of
• Decreased or absent bladder contractility. cavernous body so there would be communication between
cavernous body and glans.
Figure 77: Ischemic priapism. PCO2 <40
mmHg, pH 7.4 but similar to venous
blood
• Intracavernous
. arterial blood becomes hypooxygenated
resulting in tissue hypoxia, acidosis, and edema and results
in long-term fibrosis & impotence, and sometimes necrosis.
• Risk factors include sickle cell disease or trait, malignancy,
medications, cocaine abuse, certain antidepressants, and
total parenteral nutrition.
• If a cause cannot be identified, hematologic work-up has to
be done to rule-out malignancies or a blood dyscrasia.
• A true Urologic emergency since if left untreated for days,
will result in permanent erectile dysfunction.
Figure 79: Sometimes it is so bad that you need to make a
• 100% of men had intact erectile function when priapism was larger incision, remove a chunk of cavernosus para
reversed by 12 hours. sigurado na gumana yung shunt.
• 78% when reversed by 12 to 24 hours.
• 44% when reversed by 24 to 36 hours. .
• No patient reported spontaneous erections after priapism
duration of longer than 36 hours.
TREATMENT
• Thus, the basic principle in the management of priapism is
rapid detumescence with the goal of preservation of
erectile function.
• Preservation of erectile function requires that the
cavernous bodies be reperfused by oxygenated blood.
• Insertion of a g18 into the lateral aspect of one corporal
body allows aspiration of hypoxic/thrombosed blood with
alternate irrigation with saline. Figure 80: Sometimes, gagawin yung shunt sa
• Injection of dilute phenylephrine or epinephrine can help. may shaft. Make an incision between corpus
Would cause vasoconstriction.
spongiosum and cavernosa, make longitudinal
incisions then isuture parang arteriovenous
• Initially, dark venous blood is aspirated, later bright red
fistula
blood is a good sign.
Replace venous with NSS.
• SURGICAL MANAGEMENT
o Problem is the inability of the blood in the cavernous
bodies to exit.
o Goal of surgery is to “shunt” the blood out of the
cavernous bodies, most commonly into the corpus
spongiosum.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 19 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
NON-ISCHEMIC PRIAPRISM
Figure 84: Another technique. Sobrang edematous.
Tinusok tusok nya ng g24 needle until magleak, then
nung mabawasan ang edema tsaka nagmanual
reduction.
Figure 81 If it is really bad, you can do it on both sides
but not on the same level • When manual reduction fails, surgical intervention is done,
usually a dorsal slit circumcision.
• Aka High Flow or Traumatic Priapism.
• Rare form.
• Related to perineal trauma (straddle injury) resulting in a
fistula between a cavernous artery & the corporal body.
• Not painful & not ischemic.
• Can be managed conservatively.
• Many cases resolve spontaneously.
PARAPHIMOSIS
• Foreskin emergency.
• Completely different from “phimosis”
Figure 85: You can also do a dorsal slit para bumitaw
• Usually iatrogenic.
o Iatrogenic when medical professionals fail to unretract ang constriction ring
the prepuce after examination or instrumentation EMPHYSEMATOUS PYELONEPHRITIS
• When the foreskin or prepuce is retracted for prolonged • Life-threatening infection that results from a complicated
periods, constriction of the glans may ensue. pyelonephritis by gas-producing organisms.
• With constriction, venous backflow is restricted, edema of • Acute necrotizing infection in the kidneys seen usually in
the glans can happen which worsens the outflow. diabetic patients.
• Ischemia can ensue. • Patients usually present with sepsis & ketoacidosis.
• Escherichia coli is the most common organism.
Figure 82: Paraphimosis. Pointed by the arrow is
edematous glans.
TREATMENT
.
• Penile blocks, pain medication & sedation may be needed
prior to manual reduction.
Figure 86: Emphysematous pyelonephritis. There is
gas in the perinephric area of the kidney.
Figure 83: Reduction. Usually done under
anesthesia, put clamp all around the tip of foreskin,
hilahin then itulak until maipasok sya then wait until
edema subsides.
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 20 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
Figure 87: Emphysematous pyelonephritis.
Presence of gas, itim na itim, even in the
paranephric space.
TREATMENT
• Emphysematous pyelonephritis is a surgical emergency.
• Most patients are septic & fluid resuscitation with broad-
spectrum antimicrobial therapy are essential.
• Supportive care, IV antibiotics & relief of any urinary tract
obstruction.
• Aggressive intervention is essential.
• If the kidney is functioning, medical therapy is considered.
• Nephrectomy is recommended for patients who do not
improve after a few days of therapy.
• If the affected kidney is nonfunctioning and not obstructed,
nephrectomy should be performed because medical
treatment alone is usually lethal.
• If a kidney is obstructed, catheter drainage must be
instituted.
o If the patient’s condition improves, nephrectomy may
be deferred pending a complete urologic evaluation.
-----------------------------END OF TRANS--------------------------------
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 21 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
APPENDIX
Appendix 1 Causes of ED
Appendix 2: Bosniak Classification
Appendix 3: TNM STAGING
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 22 of 23
SURGERY UROLOGY PART 3 LECTURE 5.4
Appendix 4 Sexual Health Inventory for Men (SHIM)
[DERAIN, PALAY, SALE] EDITOR: [NAVARRO, H.] Page 23 of 23
You might also like
- 4 PEDIA 8 - Bleeding DisordersDocument5 pages4 PEDIA 8 - Bleeding DisordersRainy Liony DuhNo ratings yet
- Penetrating Abdominal Injury DiagnosisDocument3 pagesPenetrating Abdominal Injury DiagnosisRaquel ReyesNo ratings yet
- Bosniak ClassificationDocument19 pagesBosniak ClassificationGirish Kumar100% (1)
- (PLM) Oral Cavity Salivary Glands Pharynx and EsophagusDocument9 pages(PLM) Oral Cavity Salivary Glands Pharynx and EsophagusJovilyn SilongaNo ratings yet
- Surgical Oncology and Breast BiopsyDocument12 pagesSurgical Oncology and Breast Biopsybo gum parkNo ratings yet
- (Surg2) 5.3 Urology Part 2 - Dr. YusiDocument19 pages(Surg2) 5.3 Urology Part 2 - Dr. YusiAlloiBialbaNo ratings yet
- (DERMA) 03 TineasDocument9 pages(DERMA) 03 TineasJolaine ValloNo ratings yet
- (SURG) 5.4b Management of Soft Tissue SarcomaDocument6 pages(SURG) 5.4b Management of Soft Tissue SarcomaKenneth TorresNo ratings yet
- 3 Surgery - Mediastinum and PleuraDocument6 pages3 Surgery - Mediastinum and PleuraCassey Koi FarmNo ratings yet
- Gynecology: Recurrent Pregnancy LossDocument6 pagesGynecology: Recurrent Pregnancy LossDawn Marco100% (1)
- Internal Medicine - Nephrology Lecture on Cystic Kidney DiseasesDocument3 pagesInternal Medicine - Nephrology Lecture on Cystic Kidney DiseasesVon HippoNo ratings yet
- (Surg2) 5.2 Urology Part 1 - Dr. YusiDocument18 pages(Surg2) 5.2 Urology Part 1 - Dr. YusiAlloiBialbaNo ratings yet
- Schwartz Hour - BurnDocument62 pagesSchwartz Hour - BurnM3 SURGERY100% (1)
- UROLOGY 2020 (Doc BarcenasDocument33 pagesUROLOGY 2020 (Doc BarcenasJüdith Marie Reyes BauntoNo ratings yet
- (Medicalstudyzone - Com) Surgery Vol 1 4.0Document266 pages(Medicalstudyzone - Com) Surgery Vol 1 4.0medico designNo ratings yet
- Understanding Neoplasia and Tumor NomenclatureDocument17 pagesUnderstanding Neoplasia and Tumor NomenclatureCherry RahimaNo ratings yet
- Pathology 5.05b Vagina and Vulva - DR - Dy (Final Edit)Document11 pagesPathology 5.05b Vagina and Vulva - DR - Dy (Final Edit)Dranreb Berylle MasangkayNo ratings yet
- Plastic Surgery TechniquesDocument4 pagesPlastic Surgery TechniquesErald PaderangaNo ratings yet
- Embryology of The Renal SystemDocument8 pagesEmbryology of The Renal SystemStd DlshsiNo ratings yet
- Surgery QuestionsDocument19 pagesSurgery QuestionsdocaliNo ratings yet
- DISC, Drugs, Infection, Thick Basal MembraneDocument5 pagesDISC, Drugs, Infection, Thick Basal MembraneHOPENo ratings yet
- ENT Benign Neck MassesDocument2 pagesENT Benign Neck MassesLucyellowOttemoesoeNo ratings yet
- (Surg 3A) Spleen and Friends-Dr. Segismundo, Dr. Broqueza (Aisle Paler, Joseph Tolentino)Document15 pages(Surg 3A) Spleen and Friends-Dr. Segismundo, Dr. Broqueza (Aisle Paler, Joseph Tolentino)Aria Jean MostajoNo ratings yet
- Treatment of Hemostasis DisordersDocument17 pagesTreatment of Hemostasis DisordersDiana HyltonNo ratings yet
- (Basic Surg A) Immunology and TransplantationDocument7 pages(Basic Surg A) Immunology and TransplantationAimie DagaleaNo ratings yet
- BURNS - Surgery Trans2Document9 pagesBURNS - Surgery Trans2JAMPTNo ratings yet
- Schwartz 9th Ed: Chapter Outline: The SpleenDocument22 pagesSchwartz 9th Ed: Chapter Outline: The SpleenKathryn Reunilla100% (1)
- Physio Ob ReviewDocument368 pagesPhysio Ob ReviewMark LopezNo ratings yet
- ENT Summery TABLEDocument19 pagesENT Summery TABLEtaliya. shvetzNo ratings yet
- Spindle Cell LesionsDocument8 pagesSpindle Cell LesionsdrmanishsharmaNo ratings yet
- Surgical Anatomy of The Chest Wall, Pleura, and MediastinumDocument8 pagesSurgical Anatomy of The Chest Wall, Pleura, and MediastinumNooneNo ratings yet
- Gyne ReflectionDocument18 pagesGyne ReflectionKC Dela RosaNo ratings yet
- Esophageal Achalasia DysphagiaDocument14 pagesEsophageal Achalasia DysphagiaTirtha Taposh100% (1)
- 6 Head and Neck Trauma - Thoracic and Cardiovascular TraumaDocument7 pages6 Head and Neck Trauma - Thoracic and Cardiovascular TraumaMyrtle Yvonne RagubNo ratings yet
- Distal To Ligament of Treitz: CausesDocument8 pagesDistal To Ligament of Treitz: CausesKiara GovenderNo ratings yet
- Surgery BreastDocument11 pagesSurgery BreastLady ElocinNo ratings yet
- 4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Document7 pages4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Miguel C. DolotNo ratings yet
- Medicine 6.1b Approach To Cancer Patients - FernandoDocument7 pagesMedicine 6.1b Approach To Cancer Patients - FernandoAbigail LausNo ratings yet
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Document13 pagesSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101No ratings yet
- Head & Neck: Most CommonDocument6 pagesHead & Neck: Most CommonJüdith Marie Reyes BauntoNo ratings yet
- 5B Surgery 1st-2nd SE #28-32 #17-18Document3 pages5B Surgery 1st-2nd SE #28-32 #17-18Liza SoberkaayoNo ratings yet
- Management of Acute Appendicitis in Adults - UpToDateDocument28 pagesManagement of Acute Appendicitis in Adults - UpToDateaulia rachman100% (1)
- Pediatric Surgery Dr. A. IgamaDocument6 pagesPediatric Surgery Dr. A. IgamaMarco Paulo Reyes NaoeNo ratings yet
- Trans Congenital MalformationsDocument10 pagesTrans Congenital MalformationsRemelou Garchitorena AlfelorNo ratings yet
- A Disease Study On: AppendectomyDocument8 pagesA Disease Study On: Appendectomybryan leguiabNo ratings yet
- MS SurgeryDocument118 pagesMS SurgeryLove wattaNo ratings yet
- 1.1 - SURG1 - Wound HealingDocument10 pages1.1 - SURG1 - Wound HealingGeriz Daniella VigoNo ratings yet
- Schreibman - Bone Tumors in 1 Simple ChartDocument31 pagesSchreibman - Bone Tumors in 1 Simple ChartborstNo ratings yet
- L6-PATHO-Neoplasia (Sept2821)Document12 pagesL6-PATHO-Neoplasia (Sept2821)Erald PaderangaNo ratings yet
- TOPNOTCH Diagnostic Exam ANSWER KEY September 2018Document20 pagesTOPNOTCH Diagnostic Exam ANSWER KEY September 2018CDNo ratings yet
- The Spleen - A Surgical Perspective: by Col. Abrar Hussain ZaidiDocument43 pagesThe Spleen - A Surgical Perspective: by Col. Abrar Hussain Zaidiabrar_zaidiNo ratings yet
- Intussusception TransDocument4 pagesIntussusception TransJames Maravillas100% (1)
- Chapter 15 Lung Pathology ErnieDocument20 pagesChapter 15 Lung Pathology ErnieZandra Lyn AlundayNo ratings yet
- 2011-07-PATHO-Basic Pathology of SkinDocument17 pages2011-07-PATHO-Basic Pathology of SkindtimtimanNo ratings yet
- Small BowelDocument4 pagesSmall Bowelsarguss14100% (1)
- Examination of Head and Neck SwellingsDocument22 pagesExamination of Head and Neck SwellingsObehi EromoseleNo ratings yet
- Abdominal Trauma Diagnosis and ManagementDocument9 pagesAbdominal Trauma Diagnosis and ManagementMyrtle Yvonne RagubNo ratings yet
- Patho Common Stuff - RobbinsDocument7 pagesPatho Common Stuff - RobbinsMaf BNo ratings yet
- HyphemaDocument19 pagesHyphemaLiyanti RinceNo ratings yet
- Review Slides OphthaDocument14 pagesReview Slides OphthaSUSHMITA MAE ROSE CONTRERASNo ratings yet
- Effect of antenatal screening and treatment of genitourinary infections on birth outcomesDocument2 pagesEffect of antenatal screening and treatment of genitourinary infections on birth outcomesAlloiBialbaNo ratings yet
- (Template) PediaDocument7 pages(Template) PediaAlloiBialbaNo ratings yet
- Bialba TB PharmaDocument2 pagesBialba TB PharmaAlloiBialbaNo ratings yet
- Reflection 6Document2 pagesReflection 6AlloiBialbaNo ratings yet
- Alloi: Li, X., Et Al. (2020)Document2 pagesAlloi: Li, X., Et Al. (2020)AlloiBialbaNo ratings yet
- CAP Nelsons DR - Atienza 2020-2021Document15 pagesCAP Nelsons DR - Atienza 2020-2021AlloiBialbaNo ratings yet
- (Surg2) 5.2 Urology Part 1 - Dr. YusiDocument18 pages(Surg2) 5.2 Urology Part 1 - Dr. YusiAlloiBialbaNo ratings yet
- (Surg2) 5.1a Introduction To Anesthesia Part 1Document21 pages(Surg2) 5.1a Introduction To Anesthesia Part 1AlloiBialbaNo ratings yet
- Health Care For PublishDocument99 pagesHealth Care For PublishAlloiBialbaNo ratings yet
- Case LegMedDocument1 pageCase LegMedAlloiBialbaNo ratings yet
- Pharmacotherapeutic (Medpharma30) AY 2020-2021 Treatment Drug SelectionDocument2 pagesPharmacotherapeutic (Medpharma30) AY 2020-2021 Treatment Drug SelectionAlloiBialbaNo ratings yet
- Medical Students Experiences of Moral Distress .33Document7 pagesMedical Students Experiences of Moral Distress .33AlloiBialbaNo ratings yet
- (Surg2) 5.1c Anesthesia Video TranscriptionDocument5 pages(Surg2) 5.1c Anesthesia Video TranscriptionAlloiBialbaNo ratings yet
- (Surg2) 5.1b Introduction To Anesthesia-Part 2Document16 pages(Surg2) 5.1b Introduction To Anesthesia-Part 2AlloiBialbaNo ratings yet
- Pharmacotherapy During Pregnancy, Childbirth and LactationDocument6 pagesPharmacotherapy During Pregnancy, Childbirth and Lactationfiras frsNo ratings yet
- Wooten Review ArticleDocument9 pagesWooten Review ArticleAlloiBialbaNo ratings yet
- (Surg2) 5.1d Anesthesia PointersDocument12 pages(Surg2) 5.1d Anesthesia PointersAlloiBialbaNo ratings yet
- Paediatric Pharmacokinetics: Key Considerations: Hannah Katharine Batchelor & John Francis MarriottDocument10 pagesPaediatric Pharmacokinetics: Key Considerations: Hannah Katharine Batchelor & John Francis MarriottAlloiBialbaNo ratings yet
- Review of Basic Pharmacology ConceptsDocument11 pagesReview of Basic Pharmacology ConceptsAlloiBialbaNo ratings yet
- Surger YII Clinic AL Case: Group 4B Bernabe, Bernardo, Bialba, BigorniaDocument39 pagesSurger YII Clinic AL Case: Group 4B Bernabe, Bernardo, Bialba, BigorniaAlloiBialbaNo ratings yet
- Don't Use AbbreviationDocument3 pagesDon't Use AbbreviationSara tarekNo ratings yet
- Paediatric Pharmacokinetics: Key Considerations: Hannah Katharine Batchelor & John Francis MarriottDocument10 pagesPaediatric Pharmacokinetics: Key Considerations: Hannah Katharine Batchelor & John Francis MarriottAlloiBialbaNo ratings yet
- Good Prescribing GuideDocument142 pagesGood Prescribing GuideTheresa ValleriNo ratings yet
- Neuropreceptorial ChecklistDocument33 pagesNeuropreceptorial ChecklistAlloiBialba0% (1)
- Rational Prescribing: The Principles of Drug Selection: Author: Simon RJ MaxwellDocument6 pagesRational Prescribing: The Principles of Drug Selection: Author: Simon RJ MaxwellAlloiBialbaNo ratings yet
- Over-the-Counter Medications in PregnancyDocument8 pagesOver-the-Counter Medications in PregnancyAlloiBialbaNo ratings yet
- Tratamiento - Integral.de - Las.quemaduras EspañolDocument21 pagesTratamiento - Integral.de - Las.quemaduras EspañolPablo HenríquezNo ratings yet
- Neuropreceptorial ChecklistDocument33 pagesNeuropreceptorial ChecklistAlloiBialba0% (1)
- CystDocument2 pagesCystElly LazaroNo ratings yet
- Renal Cortical CystDocument2 pagesRenal Cortical Cystra222j239No ratings yet
- Renal Ultrasound Renal Ultrasound Basic Principles of Ultrasound ExaminationDocument41 pagesRenal Ultrasound Renal Ultrasound Basic Principles of Ultrasound ExaminationSav GaNo ratings yet
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsDocument17 pagesWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsmiloradNo ratings yet
- The Role of Bosniak ClassificationDocument6 pagesThe Role of Bosniak ClassificationraduNo ratings yet
- Discover the Types and Causes of Renal CystsDocument6 pagesDiscover the Types and Causes of Renal CystsManoj PradhanNo ratings yet
- Bosniak Classification For Complex RenalDocument6 pagesBosniak Classification For Complex RenalraduNo ratings yet
- Bosniak 2F Cysts - GuidelinesDocument9 pagesBosniak 2F Cysts - Guidelinesfelixsafar3243No ratings yet
- Renal Cyst PDFDocument6 pagesRenal Cyst PDFManoj PradhanNo ratings yet
- Hemorrhagic Renal Cyst Symptoms, Diagnosis, and TreatmentDocument3 pagesHemorrhagic Renal Cyst Symptoms, Diagnosis, and Treatmentcurly perkyNo ratings yet