Professional Documents
Culture Documents
Infantile Respiratory Distress Syndrome
Uploaded by
Roy D Roger0 ratings0% found this document useful (0 votes)
33 views27 pagesOriginal Title
infantile_respiratory_distress_syndrome.ppt
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
33 views27 pagesInfantile Respiratory Distress Syndrome
Uploaded by
Roy D RogerCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 27
LECTURE
INFANT RESPIRATORY
DISTRESS SYNDROME
(IRDS)
Lecturer: associate professor Volosin A.N.
Definition
Symptom complex of severe respiratory failure, which
arises as a rule during the first hours of baby’s life.
Most often this syndrome is determined by neonatal
pneumopathy.
Neonatal pneumopathies are the group of perinatal lungs
diseases, which aren’t associated with any infection.
IRDS also called neonatal respiratory distress
syndrome or respiratory distress syndrome of
newborn is first of all a syndrome caused in premature
infants by the insufficiency of surfactant production
and structural immaturity in the lungs
CLASSIFICATION
OF NEONATAL PNEUMOPATHIES
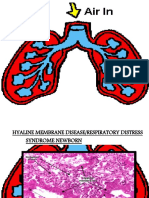
• Hyaline membrane disease (HMD);
• Edematic-hemorrhagic syndrome;
• Atelectasis of newborn.
IRDS and HMD are the synonyms in English language sources
Short description of pneumopathies
HM are dense protein mass, which is formed from blood proteins
and is mainly composed of fibrin.
These membranes cover the inner surface of pulmonary alveoli.
Edematic-hemorrhagic syndrome is characterized by diffuse
edema of lungs with multiple haemorrhages in pulmonary tissue.
Atelectasis is condition of alveoli, when their cavities deflate and
have slit-like form. Primary and secondary atelectasises are
marked out. We also distinguish disseminated and segmental atelectases.
PATHOGENESIS OF IRDS
Surfactant is substance, which ensures elasticity of pulmonary
tissue. In case of its deficiency pulmonary tissue deflates and
respiratory failure develops.
Surfactant deficit leads to:
• severe hypoxemia and hypoxia, hypercapnia, acidosis,
hypoglycemia, hypocalcemia and other metabolic derangements;
• pulmonary hypertension and systemic hypotension, hypovolemia,
microcirculation disturbance, peripheric edemas;
• muscular hypotonia;
• neurologic disorders;
• heart failure;
• inclination to hypothermia;
• functional intestinal obstruction.
EPIDEMIOLOGY
IRDS
affects about 1% of newborn infants and is the
leading cause of death in preterm infants. The
incidence decreases with advancing gestational age,
from about 50% in babies born at 26–28 weeks, to
about 25% at 30–31 weeks. The syndrome is more
frequent in the second born of premature twins.
RISK FACTORS OF IRDS
• Premature delivery
• Infants delivered via Caesarean section (without maternal labor)
• Perinatal hipoxia
• Delivery complications that lead to acidosis in the newborn
at birth (e.g. acute hemorrhage)
• Maternal diabetes
• Fetal [prenatal] infections
• Multiple pregnancy (twins or more)
• Rapid labor
• Male infants
• Hypothermia
• Family history of IRDS
The incidence of IRDS decreases with:
– The usage of antenatal steroids;
– Pregnancy-induced or chronic maternal
hypertension;
– Prolonged rupture of membranes;
– Maternal narcotic addiction.
CLINICAL SYMPTOMS OF IRDS
The symptoms usually appear within first minutes of birth.
In case of HMD clinical symptoms of respiratory failure are
revealed in 1-4 hours after birth.
• Bluish color of the skin and mucus membranes (cyanosis)
• Brief stop in breathing (apnea)
• Decreased urine output
• Grunting
• Nasal flaring
• Puffy or swollen arms or legs
• Rapid breathing (dyspnea - more than 60 breaths/min)
• Shallow breathing
• Blowing of cheeks
• Spumous saliva around patient’s mouth
• Unusual breathing movement – drawing back of the chest during
inspiration
Clinical features of neonatal respiratory distress
The photo depicts a preterm newborn with RDS exhibiting
substernal and intercostal retractions, nasal flaring,
and circumoral cyanosis.
EDEMATIC-HEMORRHAGIC
SYNDROME
• Diagnostic sign is bloody discharge from
patient’s nose, mouth or endotracheal tube,
spumous fluid of pink color, which runs
from baby’s mouth.
• Apart from pulmonary edema and
pneumorrhagias, skin hemorrhagic
syndrome and intestinal bleedings can be
detected.
SILVERMAN SCORE
Feature Score Score Score
observed «0» «1» «2»
Chest Synchronized Lag on Seesaw
Movement Respiration Respirations Respirations
Intercostal
None Just Visible Marked
Retractions
Xiphoid Just Visible
None Marked
Retractions
Nares Dilation None Marked
Minimal
Expiratory None Audible With Audible With
Grunt Stethoscope Unaided Ear
EVALUATION OF RESPIRATORY STATUS
(Silverman score)
Total Score of 0 indicates no respiratory
distress.
Total Score of 1-3 indicates feebly apparent
respiratory distress.
Total Score of 4-6 indicates moderated distress.
Total Score of 7-10 indicates severe distress.
DIFFERENTIAL DIAGNOSIS
• Pulmonary air leaks (e.g., pneumothorax, interstitial emphysema,
pneumomediastinum, pneumopericardium);
• Any infection may cause respiratory distress and may co-exist with IRDS;
Pneumonia is often caused by beta-haemolytic streptococcus and often co-
exists with IRDS.
• Aspiration of amniotic fluid, blood, or meconium may occur.
• Intracranial birth injury.
• Transient tachypnoea of the newborn usually occurs in term or near-term
infants and usually after caesarean delivery.
• Congenital anomalies of upper airways (e.g., choanal atresia)
• Congenital anomalies of the lungs (e.g., diaphragmatic hernia, lobar
emphysema, pulmonary sequestration).
• Congenital heart anomalies.
• Primary persistent pulmonary hypertension of the newborn (persistent fetal
circulation).
• Metabolic problems (e.g. hypothermia, hypoglycaemia).
• Haematological problems (e.g. anemia, polycytaemia).
BRONCHOPULMONARY DYSPLASIA
(BPD)
Wilson-Mikity’s syndrome develops in babies at gestational age less than 32
weeks and body weight less than 1500 g. Usually BPD becomes apparent on
15-35-th day of life.
Reason: immaturity of elastic elements of pulmonary tissue
• Dyspnea – up to 60 breaths/min;
• Cyanosis;
• Fits of apnea;
• Dry cough;
• Drawing back of the chest during inspiration;
• Intoxication syndrome isn’t typical;
• Duration of clinical presentations of BPD is from 1 month to 1
year and more.
BPD in a 33-day-old preterm infant
Frontal chest X-ray demonstrates uniform distribution of reticular opacities
and small clearings
EXAMINATION
• Blood gases: respiratory and metabolic acidosis along with
hypoxia. Metabolic acidosis results from poor tissue
perfusion.
• Pulse oximetry is used as a non-invasive tool to monitor
oxygen saturation, which should be maintained at 90-95%.
• Chest X-ray.
• Monitor full blood count, electrolytes, glucose, renal and
liver function.
• Echocardiogram to rule out structural heart diseases.
• Bacteriological examinations to rule out sepsis.
COMPLICATIONS OF IRDS
– Complications related to procedures, e.g. trauma to vocal
cords because of tracheal intubation; infection, embolism or
thrombosis from venous or arterial catheterisation.
– Alveolar rupture: pneumothorax, pneumomediastinum etc.
– Intracranial haemorrhage: the risk is increased in those who
require mechanical ventilation.
– Persistent pulmonary hypertension.
– Occurrence of pulmonary haemorrhage increases in very
premature infants, especially following surfactant therapy.
– Hospital acquired infection.
– Necrotising enterocolitis and/or gastrointestinal perforation.
– Apnoea of prematurity is common in immature infants, and
its incidence increases with surfactant therapy, possibly due
to early extubation.
TREATMENT OF IRDS
(etiotropic)
Nowadays such preparations of natural surfactant as Curosurf,
Survanta, Alveofact, Biosurf and synthetic surfactant as Exosurf
neonatal are used most often.
• Exogenous surfactants are introduced into trachea. The earlier
it is introduced the better results we can get. The term for its
effective introduction is the first 6-8 hours after birth. In case
of necessity introduction of surfactant may be repeated.
• For example, initial dose for Curosurf is 200 mg/kg
(2,5 ml/kg). Repeat dose is 50 % of initial dose.
It may be introduced twice every 12 hours.
Chest X-ray in a premature infant with RDS
Left, initial X-ray shows poor lung expansion, air bronchogram, and
appearance of reticular nodose granular net.
Right, repeat chest X-ray made 3 hours later after surfactant therapy
demonstrates marked improvement.
Symmetric surfactant effect in a 36-week-gestationalage infant of a diabetic
mother.
(a) Pretreatment radiograph shows diminished lung expansion, diffuse bilateral
reticulogranular opacities, and air bronchograms.
(b) Repeat radiograph, made 6 hours later after endotracheal introduction of one dose of
surfactant, reveals marked improvement in lung aeration
Asymmetric surfactant effect in a 2-day-old, 32-week-gestational age newborn
with RDS
Frontal chest radiograph demonstrates multifocal residual consolidations similar to
pneumonia or meconium aspiration syndrome
TREATMENT OF IRDS
(continuation 1)
Temperature protection
• It is necessary for the prevention of hypothermia of newborn child,
as far as on the background of hypothermia surfactant synthesis
either decreases or stops at all. Temperature in infant incubator must
be 34-35° C.
Ensuring of patency of airways
• At first aspiration contents from airways is prescribed. Some time
later vibratory massage, physiotherapy and aerosol therapy are used
for that.
Feeding and infusion therapy
• During the first 2-3 days enteral feeding isn’t used because the risk of
arising of cardiopulmonary decompensation is very high at that time
• Correction of metabolic acidosis (blood pH less than 7,25) with the
help of 4 % sodium hydrogen carbonate solution.
TREATMENT OF IRDS
(continuation 2)
Control of gas composition of blood
• Oxygenotherapy in infant incubator or artificial lung ventilation.
Control of PaO2 and PaCO2 (carbon dioxide).
Control of hematocrit (packed cell volume (PCV))
• If PCV drops lower than 0,4 then whole blood or packed red cell
transfusion is prescribed.
Treatment of hypovolemia
• Intravenous transfusions of 5-10 % albumin solution, fresh frozen
plasma (FFP), 0,9 % sodium chloride and 5 % glucose solutions.
Control of arterial pressure (AP)
• If systolic pressure is lower than 45 millimeter of mercury then
cardiotonic agents are prescribed (e.g. dopamine).
TREATMENT OF IRDS
(termination)
Antibiotic therapy
• Combination of one of semisynthetic penicillins or
cephalosporins with one of aminoglycosides is used most
often.
Vitamin therapy
• Vitamins E and A are prescribed obligatory. Vitamin E
decreases frequency of the development of retinopathy and
vitamin A - necrotizing enterocolitis in newborn children.
Other drugs
• Diuretics. Furosemide is used only in case of pulmonary
edema.
• Glucocorticoids are used on the background of signs of
adrenal failure.
PROGNOSIS
• The outcome has improved in recent years with
the increased use of antenatal steroids to improve
pulmonary maturity, early postnatal surfactant
therapy to replace surfactant deficiency and
gentler techniques of ventilation to minimise
damage to the immature lungs.
• The prognosis is much better for babies weighing
over 1500g.
PREVENTION OF IRDS
• Antenatal corticosteroids (dexamethasone)
accelerate fetal surfactant production and lung
maturation. They reduce IRDS, intraventricular
haemorrhage and mortality by 40%.
• Tocolytics, e.g. atosiban, nifedipine or ritodrine,
may delay premature delivery by 48 hours and
therefore enable time for antenatal corticosteroids
to be given.
• Good control of maternal diabetes.
• Avoid hypothermia in the neonate.
THANK YOU FOR YOUR ATTENTION
You might also like
- Respiratory Distress Syndrome Hmd-Ttnb-Mas-Neonatal PneumoniaDocument65 pagesRespiratory Distress Syndrome Hmd-Ttnb-Mas-Neonatal PneumoniaBLOBLOBNo ratings yet
- RDS Ppts 2021Document37 pagesRDS Ppts 2021Mohammad NajjarNo ratings yet
- RESPIRATORY Distress New NewDocument20 pagesRESPIRATORY Distress New NewAdegboye Sherifdeen AdedejiNo ratings yet
- Paediatric Chest RadiologyDocument120 pagesPaediatric Chest Radiologysunielgoel100% (6)
- Illness in The NewbornDocument34 pagesIllness in The NewbornVivian Jean TapayaNo ratings yet
- Approach To Respiratory Distress in NewbornDocument79 pagesApproach To Respiratory Distress in NewbornNikhil100% (1)
- RESPIRATORY DIS-WPS OfficeDocument12 pagesRESPIRATORY DIS-WPS OfficeGiselle EstoquiaNo ratings yet
- Respiratory Distress SyndromDocument19 pagesRespiratory Distress Syndromapi-19916399100% (2)
- Respiratory Distress in Newborn: Presented By: Dr. Walaa MousaDocument74 pagesRespiratory Distress in Newborn: Presented By: Dr. Walaa MousasalamredNo ratings yet
- Respiratory Distress SyndromeeDocument42 pagesRespiratory Distress SyndromeeRoman MamunNo ratings yet
- MK BronchiolitisDocument6 pagesMK BronchiolitisMoses Jr Kazevu100% (1)
- Respiratory DiseasesDocument58 pagesRespiratory DiseasesSarahNo ratings yet
- Peritonitis Dan PermasalahannyaDocument52 pagesPeritonitis Dan PermasalahannyaNindyNo ratings yet
- Respiratory Distress SyndromeDocument41 pagesRespiratory Distress SyndromedicksonsamboNo ratings yet
- Illness in NewbornDocument2 pagesIllness in Newbornitsjamyca najorraNo ratings yet
- Case Report "Hidrocephalus With Broncopneumonia + TB"Document24 pagesCase Report "Hidrocephalus With Broncopneumonia + TB"Indah LindianaNo ratings yet
- Pedi 2Document25 pagesPedi 2Roba ANo ratings yet
- Respiratory Distress SyndromeDocument121 pagesRespiratory Distress Syndromeinno so qtNo ratings yet
- Respiratory Distress Syndrome (Iniego Carlo Jay)Document9 pagesRespiratory Distress Syndrome (Iniego Carlo Jay)Carlojay IniegoNo ratings yet
- Respiratory Distress in NewbornDocument52 pagesRespiratory Distress in NewbornNadia SalwaniNo ratings yet
- Respiratory Distress Syndrome: NewbornDocument17 pagesRespiratory Distress Syndrome: NewbornLoloNo ratings yet
- Diseases of The Newborn IDocument40 pagesDiseases of The Newborn InewazNo ratings yet
- Respiratory Distress Sydrome Year 5-2Document36 pagesRespiratory Distress Sydrome Year 5-2chebetnaomi945No ratings yet
- Modul Skills KKD4 Reproduksi 2018Document31 pagesModul Skills KKD4 Reproduksi 2018rizkiya novitaNo ratings yet
- Respiratory Distress in The Neonate and InfantDocument8 pagesRespiratory Distress in The Neonate and InfantMikey ZhitnitskyNo ratings yet
- Anak 1Document72 pagesAnak 1Nency PurmayaNo ratings yet
- Hypoplasia of The Lung: Helmilubis Ridwanm. Daulay Wismandalimunthe RinisavitridaulayDocument29 pagesHypoplasia of The Lung: Helmilubis Ridwanm. Daulay Wismandalimunthe RinisavitridaulayM Rizky Assilmy LubisNo ratings yet
- Respiratory Distress SyndromeDocument30 pagesRespiratory Distress SyndromeDennis MiritiNo ratings yet
- Pedia Concepts 2:: From Respiratory Problems To HematologicDocument119 pagesPedia Concepts 2:: From Respiratory Problems To HematologicarudarbmeeNo ratings yet
- Goljan Respiratory NotesDocument21 pagesGoljan Respiratory Notesmedic2424100% (1)
- Neonatal PneumoniaDocument16 pagesNeonatal Pneumoniaelyuchan100% (1)
- 1) Respiratory Distress Syndrome (RDS) Hyaline Membrane Disease (HMD)Document9 pages1) Respiratory Distress Syndrome (RDS) Hyaline Membrane Disease (HMD)ُEssraa AdeelNo ratings yet
- Croup: Dr. Shveta Sethi Narula A.P. MicrobiologyDocument14 pagesCroup: Dr. Shveta Sethi Narula A.P. Microbiology12. Akshit AtwalNo ratings yet
- (Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Document43 pages(Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Haider Nadhem AL-rubaiNo ratings yet
- Kel Kongenital HMDDocument15 pagesKel Kongenital HMDSilvia RizkaNo ratings yet
- #10 - NCM109 (Pedia) - TransesDocument70 pages#10 - NCM109 (Pedia) - TransesJaimie BanaagNo ratings yet
- Paed Respiratory DistressDocument45 pagesPaed Respiratory Distressaboje ochekwuNo ratings yet
- Ass. of NewbornDocument54 pagesAss. of NewbornMahad Maxamed AxmedNo ratings yet
- Respiratory Distress SyndromeDocument41 pagesRespiratory Distress Syndromef.abrahamNo ratings yet
- Transient Tachypnea of The Newborn OutlineDocument7 pagesTransient Tachypnea of The Newborn OutlineMarceline GarciaNo ratings yet
- Respiratory Distress SyndromeDocument13 pagesRespiratory Distress SyndromeKenneth UbaldeNo ratings yet
- Pulmonary Hemorrhage: Dr. Habibur RahimDocument46 pagesPulmonary Hemorrhage: Dr. Habibur Rahimallaaobeid1987No ratings yet
- RD in Newborn by Yong Part 2Document37 pagesRD in Newborn by Yong Part 2semangat akreNo ratings yet
- Sistem Respirasi Sesak Napas: Problem Based LearningDocument61 pagesSistem Respirasi Sesak Napas: Problem Based LearningAkbar IskandarNo ratings yet
- Infant Respiratory Distress SyndromeDocument39 pagesInfant Respiratory Distress SyndromeIoana MuntianuNo ratings yet
- NEONATAL APNOEA SMNRDocument18 pagesNEONATAL APNOEA SMNRAswathy RC100% (1)
- Kelainan Kongenital 2010Document29 pagesKelainan Kongenital 2010Winson ChitraNo ratings yet
- Abnormality in NeonatesDocument30 pagesAbnormality in NeonatesEggyDsNo ratings yet
- Lower Respiratory Tract Diseases - KeyDocument45 pagesLower Respiratory Tract Diseases - KeyYugmaPandyaNo ratings yet
- Respiratory Distress Syndrome: Islamic University Nursing CollegeDocument21 pagesRespiratory Distress Syndrome: Islamic University Nursing Collegeyaumil agisnaNo ratings yet
- Congenital Cystic Adenomatoid Malformation (CCAM)Document7 pagesCongenital Cystic Adenomatoid Malformation (CCAM)sarguss14No ratings yet
- Eni Rahmawati, S.Kep., NS., M.KepDocument46 pagesEni Rahmawati, S.Kep., NS., M.KepLisa Qoriana RohmaniNo ratings yet
- Amniotic Fluid Disoder: Muhammad IzzatDocument26 pagesAmniotic Fluid Disoder: Muhammad IzzatcopperNo ratings yet
- Croup (Laryngotracheobronchitis) : EtiologyDocument13 pagesCroup (Laryngotracheobronchitis) : EtiologyOmar mohamedNo ratings yet
- Hyaline Membrane Disease-1Document24 pagesHyaline Membrane Disease-1JOSLIN100% (1)
- SGADocument5 pagesSGAChary HorladorNo ratings yet
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- Rare and Interesting Cases in Pulmonary MedicineFrom EverandRare and Interesting Cases in Pulmonary MedicineRating: 4 out of 5 stars4/5 (1)
- Autoimmune Disease Clinical Research: ExpertsDocument2 pagesAutoimmune Disease Clinical Research: ExpertsRoy D RogerNo ratings yet
- The Influenza & Parainfluenza VirusesDocument35 pagesThe Influenza & Parainfluenza VirusesRoy D RogerNo ratings yet
- Methods and Technique of Endoscopic Research of ENT-organs. Clinical Anatomy and Physiology of Auditory AnalyzerDocument56 pagesMethods and Technique of Endoscopic Research of ENT-organs. Clinical Anatomy and Physiology of Auditory AnalyzerRoy D RogerNo ratings yet
- Agarwal2014 Article TreatmentAndPreventionOfRhIsoiDocument8 pagesAgarwal2014 Article TreatmentAndPreventionOfRhIsoiRoy D RogerNo ratings yet
- CH 24Document3 pagesCH 24Roy D RogerNo ratings yet
- Hypotonic Hypohydration .Metabolic Acidosis. Classification of Acute PoisoningDocument2 pagesHypotonic Hypohydration .Metabolic Acidosis. Classification of Acute PoisoningRoy D RogerNo ratings yet
- Reference ID: 3975973Document2 pagesReference ID: 3975973Aldrin LampareroNo ratings yet
- Endoscopic Diagnosis of Diseases of The Intestine.Document12 pagesEndoscopic Diagnosis of Diseases of The Intestine.Roy D RogerNo ratings yet
- Case Study - Multiple SclerosisDocument11 pagesCase Study - Multiple SclerosisMyrhaida BairullaNo ratings yet
- Concluding Lesson-1Document5 pagesConcluding Lesson-1Roy D RogerNo ratings yet
- Workbook 2016 StomDocument186 pagesWorkbook 2016 StomAysenNo ratings yet
- Laparoscopic Repair of Perforated Duodenal UlcerDocument3 pagesLaparoscopic Repair of Perforated Duodenal UlcerRoy D RogerNo ratings yet
- Advantages and Disadvantages of Ultra Sonic Skin Care DevicesDocument3 pagesAdvantages and Disadvantages of Ultra Sonic Skin Care DevicesMuqarrub Ali KhanNo ratings yet
- Case Study - Tennis Elbow: Suresh BandaruDocument9 pagesCase Study - Tennis Elbow: Suresh BandaruCarl MacCordNo ratings yet
- Duodenal GistDocument5 pagesDuodenal Gistmudasir61No ratings yet
- PolydactylyDocument16 pagesPolydactylyGupies100% (1)
- International Classification of Diseases: Presented By: DR Arijit Kundu Guided By: Prof. Sumitra PattanaikDocument56 pagesInternational Classification of Diseases: Presented By: DR Arijit Kundu Guided By: Prof. Sumitra PattanaikpriyagerardNo ratings yet
- Goljan Errata SheetDocument11 pagesGoljan Errata SheetVishala MishraNo ratings yet
- Determination of DeathDocument8 pagesDetermination of DeathZam PamateNo ratings yet
- Peripheral Nerve Field Stimulation For Sacroiliac Joint PainDocument4 pagesPeripheral Nerve Field Stimulation For Sacroiliac Joint PainAna Cristina MartinsNo ratings yet
- Ear, Nose and Throat EmergenciesDocument3 pagesEar, Nose and Throat Emergenciesfmta100% (1)
- Ass Triangle of Human EcologyDocument6 pagesAss Triangle of Human EcologyClarissa Marie Limmang100% (1)
- Super Final 220-Zoonotic Infectious Diseases Exam Questions 8 SOLVED by ANKIT AKELADocument37 pagesSuper Final 220-Zoonotic Infectious Diseases Exam Questions 8 SOLVED by ANKIT AKELAYara AlmouallemNo ratings yet
- Tomografía Computarizada para El Diagnóstico de La Apendicitis Aguda en Pacientes AdultosDocument199 pagesTomografía Computarizada para El Diagnóstico de La Apendicitis Aguda en Pacientes AdultosMarco Jimenez HerreraNo ratings yet
- Nurselabs PEDIA QuestionsDocument13 pagesNurselabs PEDIA QuestionsSteffi MurielNo ratings yet
- Hematologic System Practice QuestionsDocument3 pagesHematologic System Practice QuestionsJoslyn GrossNo ratings yet
- Proceedings of The 16th Italian Association of Equine Veterinarians CongressDocument4 pagesProceedings of The 16th Italian Association of Equine Veterinarians CongressCabinet VeterinarNo ratings yet
- What Are Bacteria - Streptococcus FaecalisDocument3 pagesWhat Are Bacteria - Streptococcus FaecalisAnkan PalNo ratings yet
- Nursing Care Plan Diarrhea Assessment Diagnosis Planning Interventions Rationale EvaluationDocument8 pagesNursing Care Plan Diarrhea Assessment Diagnosis Planning Interventions Rationale EvaluationKrahNo ratings yet
- PTS - Soal Bahasa Inggris Kelas IXDocument6 pagesPTS - Soal Bahasa Inggris Kelas IXRini YusmayantiNo ratings yet
- Food HygieneDocument31 pagesFood Hygienehemihema100% (1)
- Name of The Course:-M.Phil, Economics: Result of Delhi University Entrance Test (DUET) - 2018Document5 pagesName of The Course:-M.Phil, Economics: Result of Delhi University Entrance Test (DUET) - 2018Saiganesh RameshNo ratings yet
- Types of Diabetes MellitusDocument5 pagesTypes of Diabetes MellitusKlinik MaleoNo ratings yet
- HCIA Study Guide 2023Document22 pagesHCIA Study Guide 2023consultasluisfloresdrNo ratings yet
- 2803NRS Acute Nursing Practice Exam NotesDocument18 pages2803NRS Acute Nursing Practice Exam NotesGrace CallowNo ratings yet
- Document PDFDocument11 pagesDocument PDFYANDA PELIA ANo ratings yet
- NEJM Image Challenges Album Part 4 2014 PDFDocument56 pagesNEJM Image Challenges Album Part 4 2014 PDFAntoun Kamel100% (1)
- Pathophysiology of Breast Cancer: Unkno Predisposing Factors: Precipitating FactorsDocument3 pagesPathophysiology of Breast Cancer: Unkno Predisposing Factors: Precipitating FactorsKevin Ercia100% (1)
- Thromboembolic Disease PDFDocument5 pagesThromboembolic Disease PDFBáĦẳá Y. Ẳl-mársǾúmiNo ratings yet
- Ismail's Undergraduate ThesisDocument82 pagesIsmail's Undergraduate ThesisAbiola IbrahimNo ratings yet
- Anthroposophical Approach To Cancer Rita Leroi MDDocument26 pagesAnthroposophical Approach To Cancer Rita Leroi MD144bob144No ratings yet
- 1 s2.0 S014067362300020X MainDocument14 pages1 s2.0 S014067362300020X MainGERIATRIA 72No ratings yet