Professional Documents
Culture Documents
JR Bangsal 2 Ke I
JR Bangsal 2 Ke I
Uploaded by
Fitri Kasmita SariOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
JR Bangsal 2 Ke I
JR Bangsal 2 Ke I
Uploaded by
Fitri Kasmita SariCopyright:
Available Formats
practice
Effectiveness of topical application
of amino acids to chronic wounds:
a prospective observational study
● Objective: To evaluate whether the topical application of an amino acid dressing,Vulnamin, aids the
management of chronic wounds.
● Method: A total of 160 patients with non-infected cutaneous chronic wounds were recruited. Before
treatment, wound size was assessed using digital planimetry. Treatment lasted for a maximum of six
weeks. Wound area measurements were repeated two and six weeks after starting treatment.
● Results: There was a significant reduction in the mean wound area after two weeks (7.4 ± 8.7cm2)
and six weeks (4.6 ± 6.3cm2) of treatment, when compared with baseline (11.2 ± 12.1cm2, p<0.01). At
the final follow up, 23% of patients (n=36) healed and 34% (n=54) achieved a greater than 60% reduction
in wound size. Seventy-six per cent (n=120) achieved positive outcomes (defined as a greater than 40%
reduction in the ulcer size).
● Conclusion: Although further investigations on the potential effects of this product on chronic
wound healing are required, these data suggest it may promote healing in venous, pressure and
diabetic ulcers.
● Declaration of interest: This study was sponsored by Professional Dietetics, Milan (Italy).
amino acids; leg ulcers; pressure ulcers; neuropathic ulcers; wound bed preparation
T
he concepts of wound bed preparation wound treatment as it helps regenerate tissue and R. Cassino, MD, Critical
and TIME have been developed to aid the re-epithelialise cutaneous lesions.12-15 Wounds Unit, San Luca
Clinic, Pecetto Torinese,
assessment and management of chronic Studies on experimentally induced cutaneous
Turin, Italy;
wounds.1 However, in some cases wound wounds in aged and diabetic animals13 demonstrat- E. Ricci, MD, Critical
healing is impaired by systemic condi- ed that topical Vulnamin stimulated fibroblast pro- Wounds Unit, San Luca
tions, such as malnutrition,2-5 which therefore also liferation and the production of collagen fibres. Clinic, Pecetto Torinese,
need to be addressed. Moreover, it can modulate the inflammatory phase Turin, Italy.
Email: cassino@vulnera.it
Using this example, wound management would by reducing inducible nitric oxide (i-NOS) expres-
need to include an optimal supply of the nutrients sion, thereby decreasing nitric oxide (NO) levels,
that affect the wound healing process.6-8 One such which prolong the inflammatory phase.14 Prelimi-
nutrient is protein, which plays a key role in inflam- nary patient data have suggested that Vulnamin
mation, the immune response and the development may accelerate healing of chronic wounds.15
of granulation tissue.9,10 This prospective, observational study aimed to
The development of novel ‘interactive’ wound determine the effect of topical Vulnamin (the test
dressings, such as products based on collagen or product) on chronic wounds of varying aetiologies.
hyaluronic acid scaffolds, led us to investigate the
possibility of applying nutrients that aid healing, Materials and method
such as basic elements for protein synthesis, directly This non-randomised, multicentre, observational
onto the wound bed, rather than through diet. study was conducted between January 2007 and
We were also inspired by evidence that a macro- March 2008. Each of the 28 participating centres
molecule such as albumin can be absorbed at tissue received a study protocol and dedicated data-collec-
level.11 It therefore seemed reasonable to speculate tion forms, and were asked to recruit 3–10 patients.
that small molecules, such as amino acids, can be Inclusion criteria were:
absorbed easily into granulation tissue, which is ● The presence of a cutaneous chronic ulcer (of any
rich in newly formed vessels. aetiology) of over six weeks’ duration.
Vulnamin (Professional Dietetics, Milan, Italy) is a ● Wound bed preparation grade A or B (defined as
medical preparation (regulation 93/42/CEE MDD) mostly clean wounds — that is, more than 50%
comprising a mixture of amino acids (glycine, L- granulation tissue).16
lysine hydrochloride, L-Leucine, L-Proline) and Exclusion criteria were:
▲
hyaluronic acid. It is approved as an adjuvant ● Wound size greater than 15 x 15cm
J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0 29
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
practice
Table 1. Baseline patient demographic details
Males Females
No. of patients (%) 66 (41.25) 94 (58.75)
Age
Mean age (years) ± SD (range) 72.9 ± 10.2 (37–91) 77.7 ± 9.6 (55–94) p=0.0022
<65 years (n=20) 15.2% 10.6%
66–74 years (n=48) 39.4% 23.4%
>75 years (n=92) 45.5% 66.0% p=0.0339
SD = standard deviation
● Wounds presenting with eschar and/or infected
Table 2. Wound characteristics at baseline tissue
● Traumatic wounds and wounds whose aetiology
Gender Age
could not be determined
● Patients aged under 18 years
Males Females <65 years 66–74 years >75 years
(n=66) (n=94) (n=20) (n=48) (n=92) ● Terminally ill patients
● Pregnant or breastfeeding patients
Wound location (p=0.3335) (p=0.0159) ● Patients who were allergic to any of the dressing
Sacrum (n=18) 9.1% 12.8% 0% 16.7% 11.3% components.
Patients with sloughy wounds were not excluded
Trocanter (n=5) 6.1% 1.1% 10% 4.2% 3.1% due to the potential debriding abilities of the test
product.
Ischium (n=3) 3% 1.1% 10% 2.1% 1.9%
The study was approved by all of the participating
Leg (n=82) 47% 54.3% 40% 47.9% 51.3% hospitals’ institutional review boards and performed
in accordance with the ethical principles stated in
Malleolus (n=16) 13.6% 7.4% 10% 12.5% 10%
the Declaration of Helsinki.
Heel (n=11) 4.5% 8.5% 5% 2.1% 6.9% All eligible patients were fully informed of the
study aims, that no physical, social or legal risks
Foot (plantar) (n=9) 7.6% 4.3% 15% 8.3% 5.6% were involved and that participation was voluntary.
Written consent was obtained.
Other (n=16) 9.1% 10.6% 10% 6.3% 10%
Wound aetiology (p=0.4773) (p=0.0558) Treatment protocol
The wounds were treated with the test product for a
Venous (n=31) 22.7% 17% 20% 18.8% 19.6%
maximum of six weeks. The product is available as
Arterial (n=31) 16.7% 21.3% 5% 18.8% 22.8% either a sterile powder or cream; wounds could be
treated with either version, depending on the inves-
Mixed (n=16) 12.1% 8.5% 0% 8.3% 13% tigator’s preference, although the powder is recom-
Lymphatic (n=1) 0% 1.1% 0% 2.1% 0% mended for highly exuding wounds (but can also be
used on other exudate levels). The composition of
Pressure (n=43) 22.7% 29.8% 25% 29.2% 26.1% the powder and cream is the same, with both hav-
ing the same carrying medium of hyaluronic acid,
Neuropathic (n=9) 9.1. % 3.2% 15% 10.4% 1.1%
which is believed to have no effect on healing. (Most
Other (n=29) 16.7% 19.1% 35% 12.5% 17.4% patients received both powder and cream, so it was
not possible to give separate results for the two for-
Wound depth (p=0.0808) (p=0.2407) mulations.)
Superficial (n=64) 48.5% 34% 45% 47.9% 34.8% Dressing change frequency was determined by
the condition of the wound, based on the practi-
Medium (n=87) 43.9% 61.7% 55% 50% 56.5% tioner’s clinical judgment.
The management regimen comprised:
Deep (n=9) 7.6% 4.3% 0% 2.1% 8.7%
● Cleansing with saline
● Drying with sterile gauze
30 J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
practice
● Application of the test product to the wound bed
followed by a secondary wound dressing, selected Fig 1. Overall outcomes according to the percentage
on the basis of the wound aetiology and the centre’s reduction in wound size
protocol.
Before enrolment, patients had previously received 40
various advanced dressings/technologies, to which
they had not responded; some were new referrals
and had not received prior treatment. 30
Wounds (%)
Assessment
At the study start, each wound was assessed to deter- 20
mine the wound aetiology (with a view to ensuring
appropriate management) and given a wound bed
preparation score.16 10
Any reduction in wound area was measured objec-
tively using digital planimetry (Visitrak) two and six
weeks after starting treatment. Adverse events were 0
also recorded.
en le
g
led
nin
em ab
em te
t
t
en
ov ra
ov er
en
All data collected by each participating centre
ea
se
ov o
pr de
pr sid
em
H
or
pr N
im Mo
W
im on
during the study period were sent to the study
C
research office for chart review and data extraction.
im
Based on the extent of reduction in wound area at
the end of the treatment period, wound outcomes
were classified as:
● Considerable improvement, defined as a reduction
Table 3. Relationship between change in wound area (cm2) and
in wound size of over 60%
patient demographic data and wound characteristics
● Moderate improvement, defined as a reduction in
wound size of 40–60% Mean size Mean size Mean size
● No improvement, defined as a reduction in wound at baseline on day 14 on day 42
size of less than 40%
All patients 11.2 ± 12.1 7.4 ± 8.7* 4.6 ± 6.3*†
● Worsening, defined as an increase in wound size.
The primary outcome measure was the reduction Sex (p=0.769 between subgroups)
in wound area. We also aimed to assess any correla-
tion between the test product and patient demo- Men (n=66) 11.2 ± 11.3 7.6 ± 11.3* 5.2 ± 9.1*†
graphic and wound-associated factors on healing Women (n=94) 11.1 ± 12.6 7.2 ± 8.5* 4.3 ± 4.9*†
outcomes.
Age (p=0.673 between subgroups)
Statistical analysis
<65 years (n=20) 10.0 ± 10.4 5.7 ± 5.4* 4.2 ± 5.0*
Continuous variables are reported as mean values ±
standard deviations. Statistical analysis of independ- 66–74 years (n=48) 9.8 ± 7.4 6.7 ± 6.0* 4.2 ± 4.2*
ent variables was performed using the Student’s
t-test and variance analysis and, in case of multiple >75 years (n=92) 12.1 ± 8.1 8.1 ± 10.3* 5.0 ± 7.5*†
comparisons, using the Bonferroni correction for Wound aetiology (p=0.775 between subgroups)
the critical value of statistical significance.
Discrete variables were analysed using non-para- Venous (n=31) 10.4 ± 8.7 6.3 ± 6.1* 3.9 ± 5.3*
metric methods such as the chi-square test, with the
Arterial (n=31) 10.7 ± 9.7 6.3 ± 5.1* 3.6 ± 3.8*
Yates correction where appropriate.17-19
Mixed (n=16) 18.9 ± 25.5 15.3 ± 18.7* 9.5 ± 13.0*
Results
Pressure (n=43) 11.6 ± 10.1 8.2 ± 7.6* 5.5 ± 5.3*
In all, 160 patients were evaluated. Baseline patient
demographic details are summarised in Table 1. The Neuropathic (n=9) 8.7 ± 7.0 5.2 ± 6.5* 3.3 ± 5.5*
difference in the mean age of men and women (72.9
versus 77.7 years), although moderate, was statisti- Other (n=30) 8.4 ± 9.0 4.8 ± 5.2* 3.1 ± 4.5*
cally significant, with a significantly higher percent-
age of females (66% versus 45.5% males) in the sub- Results are given as mean ± SD;
* p<0.01 versus baseline;
group of patients aged over 75 years. † p<0.01 versus day 14
Ulcer aetiology comprised:
▲
● Venous (19.4%)
J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0 31
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
practice
groups, such a result should only be interpreted in a
Table 4. Relationship between percentage reduction in wound descriptive manner.
size and patient demographic and wound characteristics The product was well tolerated and no adverse
events were experienced.
Wound >60% area >40% area
healed reduction reduction
Wound area reduction
Sex p=0.526 p=0.275 p=0.266 Fig 1 outlines the reduction in wound area. Statisti-
cal analysis revealed a significant reduction in the
Men (n=66) 25.8% 62.2% 69.7% mean wound area after two (7.4 ± 8.7cm2) and
Women (n=94) 20.2% 52.1% 78.7% six weeks (4.6 ± 6.3cm2) compared with baseline
(11.2 ± 12.1cm2, p<0.01) (Table 3).
Age p=0.537 p=0.992 p=0.713 Interestingly, the mean wound area had also sig-
nificantly reduced after six weeks when compared
<65 years (n=20) 15% 55% 75%
with after two weeks of treatment (p<0.01). No sta-
66–74 years (n=48) 25% 56.3% 70.8% tistically significant difference in the trend between
aetiologies was observed (p=0.775, Anova test with
>75 years (n=92) 22.8% 56.6% 77.2%
Bonferroni correction).
Wound aetiology p=0.337 p=0.649 p=0.544 No significant relationship was observed between
the reduction in wound area and gender (p=0.769,
Venous (n=31) 25.8% 61.3% 74.2% Anova test with Bonferroni correction) or age
Arterial (n=31) 19.4% 64.6% 87.1%
(p=0.673, Anova test with Bonferroni correction)
(Table 3).
Mixed (n=16) 12.5% 43.8% 62.5% At the final follow-up:
● 36 patients (23%) had healed
Pressure (n=43) 16.3% 48.9% 72.1% ● 54 (34%) had improved considerably
● 30 (19%) had moderately improved
Neuropathic (n=9) 44.4% 55.5% 77.8%
● 27 (17%) were stagnating
Other (n=30) 30% 60% 73.3% ● 13 (8%) were worsening.
Wound depth p=0.044 p=0.002 p=0.052 Just over three-quarters of the patients (n=120,
76%) had positive outcomes (>40% reduction in
Superficial (n=64) 31.3% 71.9% 81.3% ulcer size).
Fig 2 shows examples of wounds before treatment
Medium (n=87) 18.4% 48.3% 73.6%
and at the final follow-up.
Deep (n=9) 0% 22.2% 44.4% More men (25.8%) than women (20.2%) healed
completely (Table 4). Although healing outcomes
Baseline area p=0.000 p=0.002 p=0.140 varied with wound aetiology, no statistically sig-
<5cm2 (n=54) 42.6% 75.9% 85.2% nificant differences were observed; none of the
deep wounds healed, with only 44.4% achieving a
5–9cm2 (n=41) 12.2% 36.6% 65.9% >40% reduction. Conversely, 31.3% of the superfi-
cial and 18.4% of the medium-sized wounds
10–19cm2 (n=40) 15% 52.5% 75%
healed, while 81.3% of the superficial and 73.6%
>20cm2 (n=25) 8% 52% 68% of the medium-sized wounds achieved a positive
outcome.
Cost-analysis
References ● Arterial (19.4%) From a sample of 97 patients, we collected data on
1 Falanga V. Wound bed ● Mixed venous/arterial (10%) the number and quantity of dressings used for a pre-
preparation: science applied
● Lymphatic (0.6%) liminary pharmaco-economic evaluation (Table 5).
to practice. In: European
Wound Management ● Pressure (26.9%) The sample comprised the first 100 patients enrolled
Association (EWMA). ● Neuropathic (5.6%) into the study minus three drop-outs.
position document. Wound
● Other (18.1%) The average number of test-product applications
Bed Preparation in Practice.
MEP, 2004. All patients with venous leg ulcers received com- changes per week varied from 2.2 (for superficial
2 Russell, L. The pression both before and during the trial. wounds) to 2.9 (deep wounds), with no statistically
importance of patients’
nutritional status in wound Details on the baseline wound characteristics are significant difference regarding depth.
healing. In: White, J.R. (ed). given in Table 2. Distribution of wound types and The average cost per product (excluding nursing
Trends in Wound Care.
grade did not vary significantly with sex or age, costs) was €3.58 for superficial wounds, €3.53 and
Volume II. Quay Books,
2003. although location appeared to vary significantly €4.40 for medium and deep wounds, respectively;
with age. However, due to the small size of the sub- the average cost for each test product was €3.63.
32
J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
practice
3 British Association for
Parenteral and Enteral
Fig 2. Healing of chronic wounds during treatment with the test product Nutrition. MUST
(Malnutrition Universal
Screening Tool) Nutritional
Vascular ulcer at the dorsum Assessment Tool. BAPEN;
of the foot before treatment 2003. Available at: http://
(a) and at final follow-up (b); www.bapen.org.uk/
4 National Institute for
heel pressure ulcer at the Health and Clinical
initial visit (c) and at final Excellence. Nutritional
follow-up (d); Support in Adults. NICE
guideline. NICE, 2006.
Available at: http://guidance.
leg ulcer after surgical nice.org.uk/CG32
removal of nodular 5 Legendre C., Debure C.,
a b neoformation before (e) and Meaume S. et al. Impact of
after six weeks of treatment protein deficiency on
(f) venous ulcer healing. J Vasc
Sur 2008; 48: 688-693.
6 Pinchcofsky-Devin, G.
Nutrition and wound
healing. J Wound Care
1994; 3: 231-234.
7 Pinchcofsky-Devin, G,
Kavinski, M.V. Correlation
of pressure sores and
nutritional status. JAGS
c d 1986; 34: 435-440.
8 Harding, K.G., Morris, H.
L., Patel, G.K. Science,
medicine and the future:
healing chronic wounds.
BMJ 2002; 324: 160-163.
9 Gray, D., Cooper, P.
Nutrition and wound
healing: what is the link? J
Wound Care 2001;10:
86-89.
e f
Discussion In our experience, controlling persistent inflam-
Preclinical evidence of the test product as a modula- mation in chronic open wounds may restart the
tor of the inflammatory phase and preliminary healing process, an observation that is strengthened
results, presented at a meeting, from a small number by our results. Indeed, ulcers that achieved good
of patients provided the rationale for this observa- results within 15 days had the best outcomes. This
tional study. The primary outcome was the change suggests that, as well as providing nutrients topical-
in ulcer area during the six-week treatment period. ly to the wound, the product may have helped to
A significant mean reduction was reported after modulate inflammation.
only two weeks. In our study, 23% of the wound healed complete-
The efficacy of early healing as a prognostic indi- ly within six weeks and 53% reduced by over 40%,
cator is not unanimously supported,20,21 although resulting in 76% having positive outcomes. While
some believe that it is a strong predictor of the heal- we believe these results are encouraging, it is diffi-
ing trajectory,21-26 and a percentage reduction after cult to compare them with most other clinical stud-
two weeks of treatment has been suggested as a reli- ies as they assessed healing over a longer period
able prognostic index for the healing of deep venous (12–24 weeks).
leg ulcers.27,28 Our data are consistent with those of Jones et al.,30
Unfortunately, there were too few (11/160) deep who found that neither sex, age nor wound aetiol-
ulcers in out study for the latter point to be relevant ogy were associated with healing.
here. Nevertheless, we believe that the significant In our study, smaller wounds achieved the high-
reductions in ulcer area achieved after two weeks of est rates of healing, whereas deeper wounds achieved
treatment in wounds that had been ‘stuck’ for six the poorest outcomes, which is consistent with oth-
months — a duration that is associated with poor er studies.30-34
healing29 — might indicate a ‘reawakening’ of the Study limitations include the lack of a control
healing mechanisms. group. However, literature data, along with our clin-
33
J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
practice
ical experience, indicated that the test product may
Table 5. Cost-analysis data promote wound healing. In addition, it is difficult
to establish the causality of some of the significant
Superficial Medium Deep Total
associations as subdividing the subgroups — for
wounds wounds wounds
example, comparing different sized wounds for dif-
No. of ulcers 47 44 6 97 ferent age groups — resulted in small sample sizes
that lacked analytical power.
Treatment duration 1597 1580 252 3429 Finally, we only used the reduction in wound size
(total, days)
to monitor the progression towards healing,
Mean duration of 33.9 ± 10.6 35.9 ± 10.5 42.0 ± 0* although it should be noted that this was objective-
treatment (days) ly assessed. Other outcome measures, such as clini-
cal judgment35 and wound bed preparation score,16
No. of medications (total) 517 577 105 1199
are also of value in this regard. However, we are in
Mean no. of medications 11.0 ± 5.2 13.1 ± 5.4 17.5 ± 5.6† the process of evaluating such parameters: our goal
is to provide a more comprehensive overview of the
No. of dressing changes potential benefits of the topical use of this product.
per week 2.2 ± 1.0 2.7 ± 1.3 2.9 ± 0.9
Total cream used (g) 1120 607 80 1807 Conclusion
The data reported in this study indicate that the
Total amount of powder 213 309 77 599 topical application of a product that applies amino
used (no. of blisters) acids directly to the wound bed might help to pro-
Cost of cream (€) 716.80 388.48 51.20 1156.48 mote healing of chronic wound such as venous,
pressure and diabetic ulcers. The treatment was
Cost of powder (€) 1136.00 1648.00 410.67 3194.67 shown to be well tolerated, and is similarly priced to
other advanced wound therapies.
Total cost of medication (€) 1852.80 2036.48 461.87 4351.15
Further evaluations need to be conducted using
Average cost/medication (€) 3.58 3.53 4.40 3.63 other outcome measures, plus a control group, to
provide a more comprehensive overview of its ben-
Results reported as mean ± SD (standard deviation) efits for clinical practice. This is essential to provide
*p<0.003 versus superficial and medium wounds (Student’s t-test) a research-based rationale to support its use in the
†p<0.01 versus superficial wounds (Student’s t-test)
clinical setting. ■
10 Schools, J.M., Heyman, H., cutanee croniche. Acta Vulnologica 23 Phillips, T.J., Machado, F., Trout, compression bandages? Am J Med
Meijer, E.P. Nutritional support in 2005; 3: 111-115. R. et al. Prognostic indicators in 2000; 109: 15-19.
the treatment and prevention of 16 Falanga,V. Classifications for venous ulcers. J Am Acad 30 Jones, K.R., Fennie, K., Lenihan,
pressure ulcers: an overview of wound bed preparation and Dermatol. 2000; 43: 627-630. A. Chronic Wounds: factors
studies with an arginine enriched stimulation of chronic wounds. 24 Tallman P., Muscare E., Carson influencing healing within 3
oral nutritional supplement. J Wound Rep Regen 2000; 8: 347- P. et al. Initial rate of healing months and nonhealing after 5-6
Tissue Viability 2009; 18: 72-79. 352. predicts complete healing of months of care. Wounds 2007; 19:
11 Schaefer H., Redelmaier T.E. 17 Armitage, P., Berry, G., venous ulcers. Arch Dermatol 51-63.
Skin barrier: principles of Matthews, J.N.S. Statistical 1997; 133: 1231-1234. 31 Skene, A.I., Smith, J.M., Dore,
percutaneous absorption. Basel: Methods in Medical Research (4th 25 Gelfand, J.M., Hoffstad, O., C.J. et al.Venous leg ulcers: a
Karger; 1996. edn). Blakwell Sciencitific, 2002. Margolis, D.J. Surrogate endpoints prognostic index to predict time
12 Vulnamin cream and powder 18 Siegel, S., Castellan, N.J. Jr. for the treatment of venous leg to healing. BMJ 1992; 305: 1119-
product descriptions. Available at: Statistica non Parametrica (2nd ulcers. J Invest Dermatol 2002; 1121.
http://www.professionaldietetics. edn). McGraw-Hill, 1992. 119: 1420-1425. 32 Thomas, D.R. Prevention and
it/products/vulnamin/Vulnamin%2 19 BMDP Statistical Software. 26 Sheehan, P., Jones, P., Caselli, A. treatment of pressure ulcers.
0sterile%20powder.pdf, http:// University of California Press, et al. Percent change in wound JAMDA 2006; 7: 1, 46-59.
www.professionaldietetics.it/ 2009. area of diabetic foot ulcers over a 33 Margolis, D.J., Berlin, J.A.,
products/vulnamin/ 4-week period is a robust Strom, B.L. Which venous leg
20 Hill, D., Poore, S., Wilson, J. et
Vulnamin%20cream.pdf predictor of complete healing in a ulcers will heal with limb
al. Initial healing rates of venous
13 Corsetti, G., D’Antona, G. ulcers: are they useful as 12-week prospective trial. compression bandages? Am J Med
Azione del Vulnamin® crema nella predictors of healing? Am J Surg Diabetes Care 2003; 26: 1879- 2000; 109: 15-19.
riparazione di lesioni cutanee 2004;188: Suppl 1A, 22-25. 1882. 34 Stotts, N.A., Rodeheaver, G.T.,
sperimentalmente indotte nel 27 van Rijswijk, L., Polansky, M. Thomas, D.R. et al. An instrument
21 Cardinal, M., Phillips, T.,
ratto anziano e diabetico. Acta Predictors of time to healing deep to measure healing in pressure
Eisenbud, D.E. et al. Non-linear
Vulnologica 2008; 6: Suppl 1, 41- pressure ulcers. Ostomy Wound ulcers: development and
modeling of venous leg ulcer
42. Manage 1994; 40: 40-48. validation of the pressure ulcer
healing rates. BMC Dermatol
14 Witte, M.B., Barbul, A. Role of 2009; 9: 1-8. 28 van Rijswijk, L. Full-thickness scale for healing (PUSH). J
nitric oxide in wound repair. Am J leg ulcers: patient demographics Gerontol A Biol Sci Med Sci 2001;
22 Kantor, J., Margolis, D.J. A
Surg 2002; 183: 406-412. and predictors of healing. Multi- 56: M795-799.
multicentre study of percentage
15 Cassino, R., Ricci, E. Amino change in venous leg ulcer area as Center Leg Ulcer Study Group. J 35 Romanelli, M., Dini,V., Bertone,
acidi e letto di ferita: a prognostic index of healing at Fam Pract 1993; 36: 625-632. M.S., Brilli, C. Measuring wound
un’interazione possibile per un 24 weeks. Br J Dermatol 2000; 29 Margolis, D.J. Berlin, J.A., outcomes. Wounds 2007; 19:
intervento sia locale sia generale 142: 960-964. Strom, B.L. Which venous leg 294-298.
nella riparazione delle lesioni ulcers will heal with limb
34 J O U R N A L O F WO U N D C A R E V O L 1 9 , N O 1 , J A N U A RY 2 0 1 0
© MA Healthcare Ltd. Downloaded from magonlinelibrary.com by 129.127.145.240 on September 6, 2017.
Use for licensed purposes only. No other uses without permission. All rights reserved.
You might also like
- The Posterior Temporal supraSMAS Minimally Invasive LiftingDocument8 pagesThe Posterior Temporal supraSMAS Minimally Invasive Liftingletty3gape100% (1)
- Adolescent and Young Adult Rheumatology in Clinical Practice - 2019Document305 pagesAdolescent and Young Adult Rheumatology in Clinical Practice - 2019Samaria EsquiveellNo ratings yet
- Nursing Care Plan and Soap Notes (Konversi s.5)Document10 pagesNursing Care Plan and Soap Notes (Konversi s.5)Metha SusantiNo ratings yet
- Whitefish Care and Rehab - First Amended Complaint - 11.19Document39 pagesWhitefish Care and Rehab - First Amended Complaint - 11.19NBC Montana100% (1)
- Kelompok 2, Jurnal 3Document4 pagesKelompok 2, Jurnal 3Okim NawarNo ratings yet
- Collagen Regeneration Template in The Management of Full-Thickness Wounds - A Prospective Multicentre Study. Alet2019Document8 pagesCollagen Regeneration Template in The Management of Full-Thickness Wounds - A Prospective Multicentre Study. Alet2019Li A VélezNo ratings yet
- 10 1111@jocd 14091Document4 pages10 1111@jocd 14091adissa benandaNo ratings yet
- Publicación Suero AutologoDocument7 pagesPublicación Suero AutologoJenny AlcendraNo ratings yet
- Research ArticleDocument6 pagesResearch Articletri sutrianiNo ratings yet
- Combination of Modern Dressing and Bagging Ozone Therapy For Speed Up The Process of Wound Healing of Grade II Diabetic Ulcer PatientsDocument5 pagesCombination of Modern Dressing and Bagging Ozone Therapy For Speed Up The Process of Wound Healing of Grade II Diabetic Ulcer PatientsMuhammad AphanNo ratings yet
- Rat As A Wound Healing ModelDocument5 pagesRat As A Wound Healing ModelHelena SkalnikNo ratings yet
- Pediatric Circumcision Using N-Butyl-Cyanoacrylate Plus MSDocument5 pagesPediatric Circumcision Using N-Butyl-Cyanoacrylate Plus MSIcchank JheNo ratings yet
- Cry Op Reserved Amniotic MembraneDocument26 pagesCry Op Reserved Amniotic MembraneSangeeta SehrawatNo ratings yet
- Time-Concept Wound Bed PreparationDocument8 pagesTime-Concept Wound Bed PreparationFabio BaroniNo ratings yet
- A Comparative Study of Collagen Granule Dressing Versus Conventional Dressing in Deep WoundsDocument6 pagesA Comparative Study of Collagen Granule Dressing Versus Conventional Dressing in Deep WoundsInternational Organization of Scientific Research (IOSR)No ratings yet
- 6 Chalazion ManagementDocument3 pages6 Chalazion ManagementIGusti Ngurah AgungNo ratings yet
- Ajd 12390Document5 pagesAjd 12390Ratih Anindita Rahajeng RipyonoNo ratings yet
- Cosmetic Pterygium Surgery Techniques and Long-Term OutcomesDocument7 pagesCosmetic Pterygium Surgery Techniques and Long-Term OutcomesrhizkyNo ratings yet
- Journal PDFDocument16 pagesJournal PDFPutra TalEdy NdruNo ratings yet
- Ref 6Document7 pagesRef 6Ferdi ArdiNo ratings yet
- Wounds in GeneralDocument19 pagesWounds in GeneralMuhammad ReyhanNo ratings yet
- J of Cosmetic Dermatology - 2022 - Adatto - Clinical Evaluation of The Efficacy of Fractional Radiofrequency For TheDocument8 pagesJ of Cosmetic Dermatology - 2022 - Adatto - Clinical Evaluation of The Efficacy of Fractional Radiofrequency For TheA KhanNo ratings yet
- Zhou 2023Document6 pagesZhou 2023saraunimedNo ratings yet
- Research ArticleDocument6 pagesResearch Articlepolomska.kmNo ratings yet
- Analysis of Clinical Efficacy, Sideeffects, and Laboratory Changesamong Patients With Acnevulgaris Receiving Single Versustwice Daily Dose Oforal IsotretinoinDocument7 pagesAnalysis of Clinical Efficacy, Sideeffects, and Laboratory Changesamong Patients With Acnevulgaris Receiving Single Versustwice Daily Dose Oforal IsotretinoinKadir KUCUKNo ratings yet
- Coconut Shell Liquid Smoke Promotes Burn Wound HealingDocument5 pagesCoconut Shell Liquid Smoke Promotes Burn Wound HealingStephany Reyes RocaboNo ratings yet
- RETINOL (Improvement of Naturally Age Skin)Document7 pagesRETINOL (Improvement of Naturally Age Skin)produksi roiNo ratings yet
- v10 Combining Cell Therapy With Biopolymer Films Improves Wound Healing in A Juvenile Dermatomyositis PatientDocument7 pagesv10 Combining Cell Therapy With Biopolymer Films Improves Wound Healing in A Juvenile Dermatomyositis PatientAlisNo ratings yet
- Short-Term Treatment Outcomes of Facial RejuvenatiDocument8 pagesShort-Term Treatment Outcomes of Facial Rejuvenatihuyenthanh1807No ratings yet
- Journal of The American Academy of Dermatology Volume 76 Issue 6 2017 (Doi 10.1016 - J.jaad.2017.04.518) - Evaluation of The Prevalence, Risk Factors, Clinical Characteristics, and Burden of Acne ScaDocument1 pageJournal of The American Academy of Dermatology Volume 76 Issue 6 2017 (Doi 10.1016 - J.jaad.2017.04.518) - Evaluation of The Prevalence, Risk Factors, Clinical Characteristics, and Burden of Acne ScaRusefFandiNo ratings yet
- Promote Severe Wound Healing by Pvpi Dry Powder Spray Case Series ReportDocument4 pagesPromote Severe Wound Healing by Pvpi Dry Powder Spray Case Series ReportShira michaelNo ratings yet
- Campanati 2010Document6 pagesCampanati 2010Valentina CarreroNo ratings yet
- Clinical Experiences of Using A Cellulose Dressing On Burns and Donor Site WoundsDocument4 pagesClinical Experiences of Using A Cellulose Dressing On Burns and Donor Site WoundsabdmaliknasNo ratings yet
- Fish Skin Graft As Wound Dressing To Provide Acceleration of Wound Healing: A Narrative ReviewDocument4 pagesFish Skin Graft As Wound Dressing To Provide Acceleration of Wound Healing: A Narrative ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Efektifitas Massage Dengan Virgin Coconut Oil Terhadap Pencegahan Luka Tekan Di Intensive Care UnitDocument11 pagesEfektifitas Massage Dengan Virgin Coconut Oil Terhadap Pencegahan Luka Tekan Di Intensive Care UnitPratiwi Catur WahyuniNo ratings yet
- 1561-Article Text-2615-1-10-20181106Document5 pages1561-Article Text-2615-1-10-20181106ilhamNo ratings yet
- Int Wound Journal 4-2007Document9 pagesInt Wound Journal 4-2007filippo boNo ratings yet
- Content 86Document8 pagesContent 86Anonymous C4huq0No ratings yet
- 2 Garoufalis Poster - SawcDocument1 page2 Garoufalis Poster - SawcKamal MohamedNo ratings yet
- Pharmaceutics 12 00735Document30 pagesPharmaceutics 12 00735Patrícia Lima D'AbadiaNo ratings yet
- DressingsDocument16 pagesDressingsJose VergaraNo ratings yet
- J Ocul Pharma 2017 ARTICULO 2Document9 pagesJ Ocul Pharma 2017 ARTICULO 2fiorellaNo ratings yet
- Coccygectomy Z PlastyDocument5 pagesCoccygectomy Z PlastyJayesh BhanushaliNo ratings yet
- DermatologyDocument8 pagesDermatologypatricknuncioNo ratings yet
- Collagenase For Enzymatic Debridement A.2Document8 pagesCollagenase For Enzymatic Debridement A.2Agung GinanjarNo ratings yet
- The Chronic Catarrhal Gingivitis Diagnos 60720913Document5 pagesThe Chronic Catarrhal Gingivitis Diagnos 60720913wafiqah izzatul auliahNo ratings yet
- Jurnal Mengenai Pewarnaan KolagenDocument6 pagesJurnal Mengenai Pewarnaan KolagenrahmaaaaaNo ratings yet
- 0 Younan 2011Document10 pages0 Younan 2011Athena DiggoryNo ratings yet
- Journal of Periodontology - 2022 - Monje - Significance of Barrier Membrane On The Reconstructive Therapy ofDocument13 pagesJournal of Periodontology - 2022 - Monje - Significance of Barrier Membrane On The Reconstructive Therapy of安西 泰規No ratings yet
- Rahma Amalia SDocument30 pagesRahma Amalia SRahma AmaliaNo ratings yet
- Biodentine Vs MtaDocument3 pagesBiodentine Vs MtaAndreea Andrei AndreeaNo ratings yet
- 1 PBDocument7 pages1 PBShadowruneNo ratings yet
- Consensus-Based Acne Classification System and Treatment Algorithm For Spain - 1-S2.0-S1578219016303626-MainDocument12 pagesConsensus-Based Acne Classification System and Treatment Algorithm For Spain - 1-S2.0-S1578219016303626-Mainhimanshu24ai018No ratings yet
- Kiran, - Issue 49, Dec 07Document7 pagesKiran, - Issue 49, Dec 07Dadi SindhuNo ratings yet
- A Comparative Study of Effectiveness Between Topical Insulin Versus Normal Saline Dressings in Management of Diabetic Foot UlcersDocument13 pagesA Comparative Study of Effectiveness Between Topical Insulin Versus Normal Saline Dressings in Management of Diabetic Foot UlcersIJAR JOURNALNo ratings yet
- Article 5Document5 pagesArticle 5bestin athappillyNo ratings yet
- Artigo Publicado RevistaDocument7 pagesArtigo Publicado RevistaMara DufflesNo ratings yet
- The Effect of Epidermal Growth Factor On The Pseudo 2021 Brazilian Journal oDocument6 pagesThe Effect of Epidermal Growth Factor On The Pseudo 2021 Brazilian Journal oNavin SNNo ratings yet
- 127 241 1 SMDocument5 pages127 241 1 SMifrs kojaNo ratings yet
- A Topical Cell Therapy Approach For Diabetic Chronic Ulcers Effects of Mesenchymal Stromal Cells Associated With Plateletrich PlasmDocument10 pagesA Topical Cell Therapy Approach For Diabetic Chronic Ulcers Effects of Mesenchymal Stromal Cells Associated With Plateletrich Plasmgrasiela camposNo ratings yet
- Wound Healing: Stem Cells Repair and Restorations, Basic and Clinical AspectsFrom EverandWound Healing: Stem Cells Repair and Restorations, Basic and Clinical AspectsNo ratings yet
- Total Scar Management: From Lasers to Surgery for Scars, Keloids, and Scar ContracturesFrom EverandTotal Scar Management: From Lasers to Surgery for Scars, Keloids, and Scar ContracturesRei OgawaNo ratings yet
- Salivary Gland Cancer: From Diagnosis to Tailored TreatmentFrom EverandSalivary Gland Cancer: From Diagnosis to Tailored TreatmentLisa LicitraNo ratings yet
- Relationship Between Cd4 Level With Condyloma Acuminata inDocument39 pagesRelationship Between Cd4 Level With Condyloma Acuminata inFitri Kasmita SariNo ratings yet
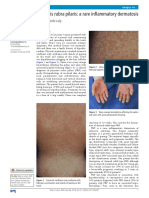
- Pityriasis Rubra Pilaris: A Rare Inflammatory Dermatosis: Aine Kelly, Aoife LallyDocument2 pagesPityriasis Rubra Pilaris: A Rare Inflammatory Dermatosis: Aine Kelly, Aoife LallyFitri Kasmita SariNo ratings yet
- Nano Fat Combined With Platelet Rich Plasma Injection Versus Nano Fat Injection Alone in The Treatment of Atrophic ScarDocument10 pagesNano Fat Combined With Platelet Rich Plasma Injection Versus Nano Fat Injection Alone in The Treatment of Atrophic ScarFitri Kasmita SariNo ratings yet
- Saxena 2019Document4 pagesSaxena 2019Fitri Kasmita SariNo ratings yet
- Bozkuri 2020Document2 pagesBozkuri 2020Fitri Kasmita SariNo ratings yet
- ReferatDocument9 pagesReferatFitri Kasmita SariNo ratings yet
- Motivation and Stress in Physical Fitness LessonDocument5 pagesMotivation and Stress in Physical Fitness LessonRaynz Gerald PatronNo ratings yet
- Resume - Parand GheshlaghiDocument3 pagesResume - Parand Gheshlaghimohammadrezahajian12191100% (1)
- Communicable Disease SurveillanceDocument60 pagesCommunicable Disease SurveillanceAmeer MuhammadNo ratings yet
- Surgery LMRP 2019Document65 pagesSurgery LMRP 2019skNo ratings yet
- Edu Adhd PaperDocument8 pagesEdu Adhd Paperapi-534406008No ratings yet
- Chapter 11 Gene Therapy - ModifiedDocument27 pagesChapter 11 Gene Therapy - ModifiedPRINCESS JEAN DELOS REYESNo ratings yet
- Bag TechniqueDocument64 pagesBag TechniqueKailash Nagar100% (1)
- ClonazepamDocument14 pagesClonazepamVaibhav MalviyaNo ratings yet
- PSSS-Mata Tenang Visus Turun PerlahanDocument48 pagesPSSS-Mata Tenang Visus Turun PerlahanYesi 'faiqa Putir100% (1)
- Daftar Penerimaan Buku Pengadaan 2018 JBRDocument136 pagesDaftar Penerimaan Buku Pengadaan 2018 JBRdika YudatamaNo ratings yet
- Nutrition For Patients With Gastrointestinal Disorders Lec 7Document20 pagesNutrition For Patients With Gastrointestinal Disorders Lec 7Youssif Menam100% (1)
- M.Sc. Emergency and Trauma Care TechnologyDocument24 pagesM.Sc. Emergency and Trauma Care TechnologyChinmoyjyotiNo ratings yet
- Efektivitas Quadriceps Setting Exercise (QSE) Dalam Meningkatkan Kemampuan Fungsional Pada Pasien Osteoartritis Lutut Genu BilateralDocument8 pagesEfektivitas Quadriceps Setting Exercise (QSE) Dalam Meningkatkan Kemampuan Fungsional Pada Pasien Osteoartritis Lutut Genu BilateralSiti lestarinurhamidahNo ratings yet
- Quit SmokingDocument2 pagesQuit Smokingsummair showkatNo ratings yet
- Long-Term Efficacy of Shunt Therapy in Idiopathic Normal Pressure HydrocephalusDocument6 pagesLong-Term Efficacy of Shunt Therapy in Idiopathic Normal Pressure HydrocephalusLeoberto Batista Pereira SobrinhoNo ratings yet
- Nifedepine Drug StudyDocument1 pageNifedepine Drug StudyMa. Sheenadel ZamudioNo ratings yet
- Nutrition Issues in GastroenterologyDocument10 pagesNutrition Issues in GastroenterologyjinniNo ratings yet
- 8Cc Getting Oxygen WorksheetDocument2 pages8Cc Getting Oxygen WorksheetInas SalehNo ratings yet
- Presentation On Blood DisordersDocument122 pagesPresentation On Blood Disordersvarshasharma05No ratings yet
- RH Morbidity Group - March 12017Document20 pagesRH Morbidity Group - March 12017Bijay Kumar MahatoNo ratings yet
- Breast Cancer Pathology Fact SheetDocument6 pagesBreast Cancer Pathology Fact SheetBallisticsNo ratings yet
- Formulir Claim Group Ver 1.0Document2 pagesFormulir Claim Group Ver 1.0Arif KesumaningtyasNo ratings yet
- WORKSHEET 7.2 Gaseous Exchange Across The Respiratory Surfaces and Transport of Gases in HumansDocument5 pagesWORKSHEET 7.2 Gaseous Exchange Across The Respiratory Surfaces and Transport of Gases in HumansGhanapathi RamanathanNo ratings yet
- Lithotomy Position V/s Lloyd Davis PositionDocument1 pageLithotomy Position V/s Lloyd Davis Positiondr_ella44No ratings yet
- TEST-20 Menopause: Part ADocument18 pagesTEST-20 Menopause: Part ANimisha akhil AkhilNo ratings yet
- Acute Appendicitis & NPI - Edmalyn GozarDocument78 pagesAcute Appendicitis & NPI - Edmalyn GozarKM100% (1)
- 3 NHS Resolution ED Report Hospital Acquired Pressure Ulcers and FallsDocument28 pages3 NHS Resolution ED Report Hospital Acquired Pressure Ulcers and FallsPaulo'RodriguesNo ratings yet