Professional Documents
Culture Documents
Mujer Con Torsades de Pointes
Uploaded by
Aníbal José Arroyo RodríguezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Mujer Con Torsades de Pointes
Uploaded by
Aníbal José Arroyo RodríguezCopyright:
Available Formats
Clinical Review & Education
JAMA Cardiology Clinical Challenge
A Woman With Recurrent Torsade de Pointes
Cody McCoy, MD; John M. Miller, MD; Tanyanan Tanawuttiwat, MD, MPH
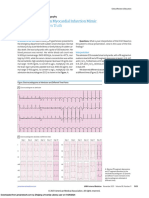
Figure 1. The 12-lead electrocardiogram obtained on day 15 of admission. Alternans in T-wave polarity is evident in most
leads (especially V3-V6) while alternans in T-wave amplitude is seen in leads II and aVF.
A woman in her mid-40s presented to the emergency department after a fall with head
trauma. A head computed tomography showed a 0.9-cm left subdural hematoma with a WHAT WOULD YOU DO NEXT?
mild left to right midline shift. Her ethanol level was 202 mg/dL (to convert to millimoles
per liter, multiply by 0.2171); magnesium, 1.7 mg/dL (to convert to millimoles per liter, mul- A. Discontinue metoprolol, start
tiply by 0.4114); potassium, 4.4 mEq/L (to convert to millimoles per liter, multiply by 1); and sotalol
ionized calcium, 4.6 mg/dL (to convert to millimoles per liter, multiply by 0.25). The pa-
tient developed cardiac arrest due to ventricular arrhythmias in the emergency depart-
B. Start intravenous amiodarone
ment and was successfully resuscitated. Echocardiography demonstrated a left ventricu-
lar ejection fraction of 50% and no regional wall motion abnormalities. She subsequently
underwent embolization of the middle meningeal artery. After embolization, however, a C. Start intravenous magnesium
worsening rightward midline shift was discovered. As a result, on the 11th day of her hos-
pitalization, she had a burr hole evacuation. During day 15 of admission, the patient had 3 D. Emergent implantable
episodes of torsade de pointes (TdP) while receiving 50 mg of metoprolol succinate daily, cardioverter defibrillator implant
and her 12-lead electrocardiogram (ECG) is shown in Figure 1.
Quiz at jamacmelookup.com
Diagnosis resulting in pseudo QRS widening of the next beat, mimicking pre-
T-wave alternans mature ventricular contractions (PVCs) in a bigeminal pattern. The
simultaneous narrow QRS in V2-V4, when compared with seeming
What to Do Next J waves or QRS widening in other leads, confirmed that the appar-
C. Start intravenous magnesium ent QRS widening was due to T-wave “contamination.” This finding
preceded the development of TdP (Figure 2).
Discussion TWA is defined as a transient beat-to-beat oscillation in
The ECG in Figure 1 shows T-wave alternans (TWA). The beat-to- T-wave timing, axis, morphology, and/or amplitude in sinus rhythm
beat opposite T-wave polarity was obvious in leads V3-V6, but only without associated QRS variability or clinically significant changes
amplitude alternans was noted in leads III and aVF. The T wave, in the RR interval.1 It is considered an indicator of myocardial
with a QTc of 670 milliseconds, extended to the next QRS complex, electrical instability and harbinger of life-threatening ventricular
jamacardiology.com (Reprinted) JAMA Cardiology Published online January 18, 2023 E1
© 2023 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Anibal Arroyo Rodriguez on 01/26/2023
Clinical Review & Education JAMA Cardiology Clinical Challenge
Figure 2. Telemetry tracing recorded shortly after the electrocardiogram ventricular tachycardia diagnosed as torsade de pointes.
diagnosis of T-wave alternans. The telemetry tracing showed polymorphic
arrhythmias. TWA is particularly associated with congenital long QT implantable cardioverter defibrillator (ICD) should be considered in
syndrome but occurs in a wide range of clinical conditions, such as individuals with long QT experiencing sustained ventricular arrhyth-
alcoholism, cardiomyopathy, electrolyte imbalances, medication ad- mias or sudden cardiac arrest despite taking β-blockers.5 After
verse effects, and ischemia. Experimental evidence is that abnor- attempting the above-mentioned conservative treatment, PVC ab-
mal intracellular Ca2+ handling is the ionic basis for TWA.2 In- lation can be taken into consideration in individuals with drug-
creased and unstable cardiac Ca2+ dynamics and suppressed K+ refractory, recurrent TdP caused by monomorphic PVCs.
channels (both IKr and IKs) lead to prolonged repolarization in ven-
tricular myocytes, action potential duration alternans, and beat-to- Patient Outcome
beat alternation during repolarization giving rise to TWA on the ECG.2 Loading doses of intravenous magnesium sulfate and lidocaine were
The relationship between TWA and heterogeneity of repolariza- administered to the patient. Isoproterenol was not given as her in-
tion is observed frequently with discordant TWA, when myocytes trinsic heart rate was 100 to 120 beats/min. Lidocaine infusion was
in proximity repolarize out of phase, thereby markedly enhancing transitioned to oral mexiletine in the next few days. Even with car-
heterogeneity of repolarization and establishing the preconditions diac and neurologic stabilization along with a β-blocker and mexi-
for conduction block, reentry, and life-threatening arrhythmias.3 letine, her QT prolongation persisted (QTc 580 milliseconds). Ge-
Initial management should focus on TdP prevention. The first- netic testing revealed a heterozygous mutation in the potassium
line therapy is intravenous magnesium sulfate, which can prevent voltage-gated channel subfamily Q member 1 (KCNQ1) gene at exon
TdP by suppressing development of early afterdepolarizations that 1, c.352A>C. This mutation has been observed in individuals with clini-
initiate episodes, regardless of serum magnesium concentration. All cal features of long QT syndrome, but because the available evi-
QT-prolonging medications, including amiodarone, should be dis- dence is currently insufficient, it has been classified as a variant of
continued and avoided. Hypokalemia should be treated to main- uncertain significance. She eventually underwent an ICD implant.
tain serum potassium concentrations in the high-normal range. Iso- At the 3-month follow-up, the patient did not take mexiletine for a
proterenol infusion and/or temporary pacing can be considered to month but continued to take metoprolol. Repeated ECG showed ab-
prevent pause-dependent TdP. Lidocaine and mexiletine can sence of TWA and a QTc 520 milliseconds. ICD interrogation showed
be used to diminish QT prolongation.4 After TdP is controlled, an no ventricular arrhythmia events. Mexiletine was resumed.
ARTICLE INFORMATION REFERENCES the Council on Clinical Cardiology, the Council on
Author Affiliations: Division of Cardiovascular 1. Shimizu W, Antzelevitch C. Cellular and ionic Cardiovascular Nursing, and the American College
Medicine, Indiana University, Indianapolis. basis for T-wave alternans under long-QT of Cardiology Foundation. Prevention of torsade de
conditions. Circulation. 1999;99(11):1499-1507. pointes in hospital settings: a scientific statement
Corresponding Author: Tanyanan Tanawuttiwat, from the American Heart Association and the
MD, MPH, Division of Cardiovascular Medicine, doi:10.1161/01.CIR.99.11.1499
American College of Cardiology Foundation.
Indiana University, 1800 N Capitol Ave, Room 2. Bao M, Zhang J, Huang C, Jiang H, Liu J, Zhao D. Circulation. 2010;121(8):1047-1060. doi:10.1161/
300B, Indianapolis, IN 46202 (ttanawu@iu.edu). Abnormal intracellular calcium handling underlying CIRCULATIONAHA.109.192704
Published Online: January 18, 2023. T-wave alternans and its hysteresis. Cardiology.
2007;108(3):147-156. doi:10.1159/000096566 5. Al-Khatib SM, Stevenson WG, Ackerman MJ,
doi:10.1001/jamacardio.2022.5094 et al. 2017 AHA/ACC/HRS Guideline for
Conflict of Interest Disclosures: Dr Miller reports 3. Nieminen T, Verrier RL. Usefulness of T-wave Management of Patients With Ventricular
fellowship support and lecture fees from alternans in sudden death risk stratification and Arrhythmias and the Prevention of Sudden Cardiac
Medtronic, Boston Scientific, Biosense-Webster, guiding medical therapy. Ann Noninvasive Death: A Report of the American College of
Abbott Electrophysiology, and Biotronik, Inc. Electrocardiol. 2010;15(3):276-288. doi:10.1111/j.1542- Cardiology/American Heart Association Task Force
474X.2010.00376.x on Clinical Practice Guidelines and the Heart
Additional Contributions: The authors are grateful
to Peng-Seng Chen, MD, for his invaluable 4. Drew BJ, Ackerman MJ, Funk M, et al; American Rhythm Society. J Am Coll Cardiol. 2018;72(14):e91-
suggestions. We also thank the patient for granting Heart Association Acute Cardiac Care Committee of e220. doi:10.1016/j.jacc.2017.10.054
permission to publish this information.
E2 JAMA Cardiology Published online January 18, 2023 (Reprinted) jamacardiology.com
© 2023 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Anibal Arroyo Rodriguez on 01/26/2023
You might also like
- 1 s2.0 S0749070421001020 MainDocument12 pages1 s2.0 S0749070421001020 MainEliseu AmaralNo ratings yet
- Nascimento Et Al. - 2013 - Wearable Cardioverter Defibrillator in Stress Cardiomyopathy and Cardiac ArrestDocument4 pagesNascimento Et Al. - 2013 - Wearable Cardioverter Defibrillator in Stress Cardiomyopathy and Cardiac ArrestflashjetNo ratings yet
- Cardiac Arrhythmia RisksDocument17 pagesCardiac Arrhythmia RisksAnel ConquetNo ratings yet
- An Important Cause of Wide Complex Tachycardia: Case PresentationDocument2 pagesAn Important Cause of Wide Complex Tachycardia: Case PresentationLuis Fernando Morales JuradoNo ratings yet
- Memory T-Waves, A Rare Cause of T-Wave Inversion in The Emergency Department - PMCDocument7 pagesMemory T-Waves, A Rare Cause of T-Wave Inversion in The Emergency Department - PMCfiat.2dindaNo ratings yet
- Hiperkalemia 1 PDFDocument5 pagesHiperkalemia 1 PDFablfilaNo ratings yet
- Jamainternal Zhang 2021 Ce 210028 1635441147.09994Document2 pagesJamainternal Zhang 2021 Ce 210028 1635441147.09994gwyneth.green.512No ratings yet
- R On T PhenomeneonDocument3 pagesR On T Phenomeneonpradeep danielNo ratings yet
- Incessant VT VFDocument9 pagesIncessant VT VFTor JaNo ratings yet
- 2018 - Manifestaciones Electrocardiograficas de La Hiperkalemia SeveraDocument4 pages2018 - Manifestaciones Electrocardiograficas de La Hiperkalemia SeveraNANDY LUZ FERIA DIAZNo ratings yet
- Diagnosis of Acute Myocardial InfarctDocument5 pagesDiagnosis of Acute Myocardial InfarctOscar SanNo ratings yet
- Arritmias VentricularesDocument11 pagesArritmias VentricularesJesusIsmaelCoronaNo ratings yet
- Journal of ElectrocardiologyDocument3 pagesJournal of ElectrocardiologyFederico FalsettiNo ratings yet
- ICU Rounds: Recognizing and Treating Ventricular TachycardiaDocument4 pagesICU Rounds: Recognizing and Treating Ventricular TachycardiaDicky SaputraNo ratings yet
- Torsades de Pointes in 3 Patients With Leukemia Treated With Arsenic TrioxideDocument4 pagesTorsades de Pointes in 3 Patients With Leukemia Treated With Arsenic TrioxideStanley PhanNo ratings yet
- Patofisiologi and Clinical Manifest LQTSDocument9 pagesPatofisiologi and Clinical Manifest LQTSNonameNo ratings yet
- Antiarrhythmic Drugs: Understanding Risks and BenefitsDocument14 pagesAntiarrhythmic Drugs: Understanding Risks and Benefitsreinaldo valdes iznagaNo ratings yet
- Electrocardiographic Manifestations of Hyperkalemia: Amal Mattu, MD, William J. Brady, MD, and David A. Robinson, MDDocument9 pagesElectrocardiographic Manifestations of Hyperkalemia: Amal Mattu, MD, William J. Brady, MD, and David A. Robinson, MDLe TrungNo ratings yet
- 7InitialDraft 4Document8 pages7InitialDraft 4pigzeniNo ratings yet
- ECG Manifestations of Multiple Electrolyte Imbalance: Peaked T Wave To P Wave ("Tee Pee Sign")Document5 pagesECG Manifestations of Multiple Electrolyte Imbalance: Peaked T Wave To P Wave ("Tee Pee Sign")Mohammad AlzawiNo ratings yet
- 1 s2.0 S2666084923003509 MainDocument6 pages1 s2.0 S2666084923003509 MainThato PaulusNo ratings yet
- Pseudo-Myocardial Infarction Versus Pseudo-Pseudo-Myocardial InfarctionDocument3 pagesPseudo-Myocardial Infarction Versus Pseudo-Pseudo-Myocardial InfarctionAngel NspNo ratings yet
- HSR3 10 BerlotDocument4 pagesHSR3 10 Berlotserena7205No ratings yet
- Cardiac Arrest and Successful Extracorporeal CardiDocument4 pagesCardiac Arrest and Successful Extracorporeal CardiDelia DeNo ratings yet
- ECG Series: Narrow QRS-complex tachycardia: Part 2Document5 pagesECG Series: Narrow QRS-complex tachycardia: Part 2KenWin NguyễnNo ratings yet
- DownloadDocument2 pagesDownloadTiffaniNo ratings yet
- Circulation 2002 Wu 675 6Document3 pagesCirculation 2002 Wu 675 6konyekNo ratings yet
- Can't Miss ECG FindingsDocument61 pagesCan't Miss ECG FindingsVikrantNo ratings yet
- Perioperative Cardiac Arrhythmias: A. Thompson and J. R. BalserDocument9 pagesPerioperative Cardiac Arrhythmias: A. Thompson and J. R. BalsererzaraptorNo ratings yet
- PIIS0007091217355952Document9 pagesPIIS0007091217355952Said Qadaru ANo ratings yet
- Idiopathic Fascicular LV Tachycardia Case Report - Kadek Agus Putra - Edit 1Document8 pagesIdiopathic Fascicular LV Tachycardia Case Report - Kadek Agus Putra - Edit 1putra udayanaNo ratings yet
- NEONARYTDocument28 pagesNEONARYToctaviena zakariaNo ratings yet
- Pseudonormalization of T Waves After Coronary Angioplasty A Medical Emergency 6656Document3 pagesPseudonormalization of T Waves After Coronary Angioplasty A Medical Emergency 6656Veer VajraNo ratings yet
- Idiopathic Fascicular Left Ventricular Tachycardia: A Case ReportDocument4 pagesIdiopathic Fascicular Left Ventricular Tachycardia: A Case ReportAde BayunataNo ratings yet
- Premature Ventricular ContractionDocument17 pagesPremature Ventricular Contractiondr_jofrilNo ratings yet
- Current Concepts in QT ProlongationDocument9 pagesCurrent Concepts in QT ProlongationSuresh KumarNo ratings yet
- Ventricular Tachyarrhythmias: Roger D. White, M.DDocument2 pagesVentricular Tachyarrhythmias: Roger D. White, M.DEugene VovchukNo ratings yet
- 247 FullDocument6 pages247 FullBryan FarrelNo ratings yet
- Dengue Myocarditis: Case ReportDocument3 pagesDengue Myocarditis: Case Reportallfanz_krenNo ratings yet
- Supraventricular TachycardiDocument8 pagesSupraventricular TachycardiHairunisa 0049No ratings yet
- Kharel - Implications of Localized ST Depression in A Vascular Territory and Altered Precordial T-Wave Balance in Ischemic Heart DiseaseDocument6 pagesKharel - Implications of Localized ST Depression in A Vascular Territory and Altered Precordial T-Wave Balance in Ischemic Heart DiseaseM. PurnomoNo ratings yet
- Pheochromocytoma An ECG DiagnosisDocument3 pagesPheochromocytoma An ECG DiagnosisPeter Albeiro Falla CortesNo ratings yet
- Delayed Intrinsicoid Deflection - Electrocardiographic Harbinger of Heart DiseaseDocument9 pagesDelayed Intrinsicoid Deflection - Electrocardiographic Harbinger of Heart DiseaseABDULLAH ALHASANNo ratings yet
- Sudden Cardiac Arrest in Takotsubo Cardiomyopathy - A Case StudyDocument5 pagesSudden Cardiac Arrest in Takotsubo Cardiomyopathy - A Case StudyzenyxtaNo ratings yet
- Chapter 32 - Genetic Cardiac ArrythmiasDocument7 pagesChapter 32 - Genetic Cardiac ArrythmiasReda SoNo ratings yet
- 285 Perioperative Cardiac Dysrhythmias - Part 2 v2Document12 pages285 Perioperative Cardiac Dysrhythmias - Part 2 v2afid2912No ratings yet
- VT Types and CharacteristicsDocument14 pagesVT Types and CharacteristicsSasya AndriansyahNo ratings yet
- Cellular Mechanisms Underlying The Long QT Syndrome: Charles Antzelevitch,, and Wataru ShimizuDocument9 pagesCellular Mechanisms Underlying The Long QT Syndrome: Charles Antzelevitch,, and Wataru ShimizuGiulia AndreeaNo ratings yet
- Gene Therapy For Cardiac ArrhythmiasDocument9 pagesGene Therapy For Cardiac ArrhythmiasIdada EzekielNo ratings yet
- ECG Quiz: Sonia Chacko, 5th Year MedicineDocument2 pagesECG Quiz: Sonia Chacko, 5th Year MedicineAņņå SëiŗÿúùNo ratings yet
- Bipolar Blindness in MappingDocument5 pagesBipolar Blindness in MappingTanah PantaiNo ratings yet
- ECG Frequency Changes inDocument13 pagesECG Frequency Changes inArief KamilNo ratings yet
- TachycardiaDocument7 pagesTachycardiamikiNo ratings yet
- Criem2020 4159526Document5 pagesCriem2020 4159526m.fahimsharifiNo ratings yet
- Epsilon WaveDocument3 pagesEpsilon WaveMiguel SilvaNo ratings yet
- ECG Manifestations of Multiple Electrolyte Imbalance: Peaked T Wave To P Wave ("Tee-Pee Sign")Document4 pagesECG Manifestations of Multiple Electrolyte Imbalance: Peaked T Wave To P Wave ("Tee-Pee Sign")Victor CutiNo ratings yet
- 58-63 DallAra JIC 2020 Feb WMDocument6 pages58-63 DallAra JIC 2020 Feb WMJose Manuel Ornelas-AguirreNo ratings yet
- Escaping A Storm Alive: A Case Report of A Young Woman's Acute Presentation of Thyroid Storm Leading To Cardiac Arrest Salvaged by VA-ECMODocument5 pagesEscaping A Storm Alive: A Case Report of A Young Woman's Acute Presentation of Thyroid Storm Leading To Cardiac Arrest Salvaged by VA-ECMOputriayuratnasariNo ratings yet
- Management of ventricular electrical storm: a contemporary appraisalDocument13 pagesManagement of ventricular electrical storm: a contemporary appraisalAníbal José Arroyo RodríguezNo ratings yet
- 1 s20 S0002934322006295 Main - 221027 - 063744Document10 pages1 s20 S0002934322006295 Main - 221027 - 063744Vaomir DiazNo ratings yet
- AJHP HenryCohenDocument5 pagesAJHP HenryCohenBagus Satrio NurwitoNo ratings yet
- Nice. Manejo de Los LípidosDocument7 pagesNice. Manejo de Los LípidosAníbal José Arroyo RodríguezNo ratings yet
- Antidepresivos. JamaDocument2 pagesAntidepresivos. JamaAníbal José Arroyo RodríguezNo ratings yet
- ECG Normal Sinus Rhythm GuideDocument10 pagesECG Normal Sinus Rhythm GuideNakul GaurNo ratings yet
- Anaesthesia - 2022 - Thomas - Guidelines For The Peri Operative Management of People With Cardiac Implantable ElectronicDocument10 pagesAnaesthesia - 2022 - Thomas - Guidelines For The Peri Operative Management of People With Cardiac Implantable Electronicsohil elfarNo ratings yet
- Automated External Defibrillator (AED) : Standard Operating ProcedureDocument1 pageAutomated External Defibrillator (AED) : Standard Operating ProcedureRichard LazanasNo ratings yet
- EKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture SeriesDocument85 pagesEKG Interpretation: UNS Cardiovascular Dept Medical Student Lecture Seriesandina rosmalianti100% (1)
- 5 ECG Changes of Hyperkalemia You Need To Know: 1. Tall 'Tented' T WavesDocument4 pages5 ECG Changes of Hyperkalemia You Need To Know: 1. Tall 'Tented' T Wavesricky hutagalungNo ratings yet
- Basic ECG Interpretation 20-Question Practice TestDocument7 pagesBasic ECG Interpretation 20-Question Practice Testemmaaziz100% (1)
- Acls Pre Course Self Assessment Study GuideDocument7 pagesAcls Pre Course Self Assessment Study Guidenova939100% (5)
- Tatalaksana KegawatdaruratanDocument9 pagesTatalaksana KegawatdaruratanBennyNo ratings yet
- Cardioversion and DefibrillationDocument66 pagesCardioversion and DefibrillationAbnet WondimuNo ratings yet
- An Interesting Case of "Trigeminal Tachycardia"Document3 pagesAn Interesting Case of "Trigeminal Tachycardia"ABDULLAH ALHASANNo ratings yet
- Prognosis of Patients With Complete Heart BlockDocument7 pagesPrognosis of Patients With Complete Heart BlockRaul OrtegaNo ratings yet
- ECG Basics: Acute Myocardial InfarctionDocument34 pagesECG Basics: Acute Myocardial InfarctionnengninisNo ratings yet
- Presentation 1 - DR Martin RoyleDocument66 pagesPresentation 1 - DR Martin Royleশরীফ উল কবীরNo ratings yet
- College of Nursing: (Dalubhasaan NG Narsing)Document4 pagesCollege of Nursing: (Dalubhasaan NG Narsing)Anna Sofia ReyesNo ratings yet
- Puskesmas Kampala ECG report invalid barcodeDocument3 pagesPuskesmas Kampala ECG report invalid barcodeAkram KastiranNo ratings yet
- Basic Life SupportDocument6 pagesBasic Life SupportRyan Mathew ScottNo ratings yet
- TV 2021Document17 pagesTV 2021c4fcz9dj4fNo ratings yet
- Normal Varient ECGDocument64 pagesNormal Varient ECGShah NahidNo ratings yet
- ECG LictureDocument25 pagesECG LictureALi NursingNo ratings yet
- What Is A Cardiac Dysrhythmia?Document6 pagesWhat Is A Cardiac Dysrhythmia?Megan N. ReyesNo ratings yet
- ACLS AgorithmDocument55 pagesACLS AgorithmkpsuanNo ratings yet
- Interpretasi EKGDocument43 pagesInterpretasi EKGAmalia Frantika WihardjoNo ratings yet
- Dysrhythmias ChartDocument6 pagesDysrhythmias Chartjkrix100% (1)
- Cardiac Action Potential: Aswin R. MDocument53 pagesCardiac Action Potential: Aswin R. MRaghu NadhNo ratings yet
- 12 Lead ECG Color Codes 1 - 04Document62 pages12 Lead ECG Color Codes 1 - 04ChrisieNo ratings yet
- Sugiyono, S.Kep., Ners., M.KepDocument48 pagesSugiyono, S.Kep., Ners., M.KepHervin RamadhaniNo ratings yet
- Ecg Interpretation New TemplateDocument88 pagesEcg Interpretation New TemplateJonathan NgNo ratings yet
- How To Choose Between Rate and Rhythm Control Strategy: Review ArticleDocument9 pagesHow To Choose Between Rate and Rhythm Control Strategy: Review ArticleAngga Aryo LukmantoNo ratings yet
- Ecg MonitoringDocument26 pagesEcg Monitoringclaire yowsNo ratings yet
- Ecg MCQSDocument2 pagesEcg MCQSZafar Iqbal Manj100% (2)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (15)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 3.5 out of 5 stars3.5/5 (33)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 5 out of 5 stars5/5 (5)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- The Tennis Partner: A Doctor's Story of Friendship and LossFrom EverandThe Tennis Partner: A Doctor's Story of Friendship and LossRating: 4.5 out of 5 stars4.5/5 (4)