Professional Documents
Culture Documents
Untitled
Uploaded by
Joshilin Herhuay Inca0 ratings0% found this document useful (0 votes)
4 views3 pagesCopyright
© © All Rights Reserved
Available Formats
TXT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as TXT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
4 views3 pagesUntitled
Uploaded by
Joshilin Herhuay IncaCopyright:
© All Rights Reserved
Available Formats
Download as TXT, PDF, TXT or read online from Scribd
You are on page 1of 3
Professor: All right, now that we
have gone through the different steps that
are needed for a good impact evaluation,
it is time to go on a journey with me of an actual impact
evaluation.
This is in our city that I conducted in Karnataka state
in India, with Professor Rima Khanna at the Harvard Kennedy
School.
And the National Health Mission of government of Karnataka,
with support from USAID's development innovations
venture.
The links to the paper, as well as a J-PAL summary and policy
insight are included in the resources for this lecture.
So what was the challenge, or the problem
that policymakers were confronting?
Despite high healthcare spending,
health outcomes in India are unsatisfactory
with very slow improvements over time.
When you talk to policymakers, one reason
they will often highlight is that health staff absenteeism
is widespread, leading to suboptimal care.
For example, surveys have shown that healthcare workers
in India are absent 43% of the time they should be at work.
We found that the numbers were about 40% absenteeism
in Karnataka state.
While another study found that in Udaipur,
in the state of Rajasthan, health centers
were closed 56% of the time that they should have been open.
What is causing the doctors not to show up for work?
And how can we improve their attendance?
If we address this, will it improve the quality of care,
and therefore the health outcomes?
So what are possible contributing factors
to the problem?
Potentially, there is not enough health staff.
Or it could be that the health staff
has low intrinsic motivation.
So they don't want to show up to work.
It could also be that they are discouraged from showing up
due to a lack of basic facilities and medicines
at the clinics.
Or it could be that information about attendance
is not properly collected.
Or that there is a lack of enforcement
against those absent leading to furthermore absenteeism.
Depending on what the underlying causes,
there are different possible solutions.
If you think there is not enough health personnel,
you can hire additional staff.
If instead you believe intrinsic motivation is
the main contributing factor, you
may want to remind health staff of the importance
of their work.
If the lack of basic facilities and medicines
may discourage workers from coming to the clinics
you could invest in the infrastructure and medicine
availability.
And finally, if the underlying source
is the lack of information on attendance
and poor enforcement, you could make attendance data
available to the supervisors.
To decide which of these options is best suited to our context,
we need to pair a good understanding of the problem
and knowledge of local conditions
with rigorous evidence from around the world.
In this case, the government decided
to improve attendance data via a tracking system
that would collect fingerprints from present staff,
and transmit the data in real time using cell phones.
It is important to note, that this was a program
that the government itself conceived, based
on a similar model that had worked very well for government
staff working in the state capital of Bangalore, now
Bengaluru.
They were going to expand it to all primary health
centers in the state.
And were in the process of securing funding to do so.
But before doing that, they invited us to work with them
and to hone down the theory of change.
And add in an impact evaluation of a pilot rollout
to understand if it really works or not,
before they scale it up.
So kudos to the state government of Karnataka
for their foresight, as most government programs
in my experience, just go straight from an idea,
to a grand announcement, to an ad scale rollout.
With consequences that we are all
well aware of in terms of bad implementation,
and a lack of impact.
Next, we collaboratively develop the program's theory of change.
That is, the envisioned change process from the identified
problem or need.
What are the direct input and outputs
to the desired intermediate, and to the final outcome.
In our example, the government had the theory
that the tracking machines will improve attendance and thereby,
lead to better care and health outcomes.
Let's go through the theory of change step by step.
As discussed, the identified need
is the low attendance of health staff and poor health outcomes.
We have also already talked about the suggested program
or input.
Namely, the installment of a biometric attendance tracking
system in primary health care centers
to transmit attendance data in real time.
The output of this program is that data
is available in real time and is being used.
Sometimes it can feel a bit artificial
to distinguish between inputs and outputs,
but differentiating the two is really important.
Imagine the program is not implemented as planned.
You will be able to see this because you will not
observe the outputs.
So it is useful to define those in advance.
What are the outcomes of interest?
Note, that intermediate outcomes often
refer to a change in attitudes or behavior.
Our theory was, that the program would
lead to improved attendance of staff.
And that staff would spend more time with patients.
Or more patients would show up to be examined.
Finally, we hope that these intermediate outcomes
would lead to better standards of care and better health
outcomes.
Note, that for there to actually be a change in health outcomes,
a number of other assumptions have to hold.
For example, visits with doctors have
to result in better care due to accurate diagnosis.
Given the focus of this lecture, we
will not go into all those details today.
You might also like
- The Clinical Practice Program: A How-to-Guide for Physician Leaders On Starting Up a Successful ProgramFrom EverandThe Clinical Practice Program: A How-to-Guide for Physician Leaders On Starting Up a Successful ProgramNo ratings yet
- Candidate D Muet AssigmentDocument6 pagesCandidate D Muet AssigmentMadoka HayashidaNo ratings yet
- The Value Analysis Program: A How-to-Guide for Physician Leaders On Starting Up a Successful ProgramFrom EverandThe Value Analysis Program: A How-to-Guide for Physician Leaders On Starting Up a Successful ProgramNo ratings yet
- Clinician-Scientists in Public Sector Hospitals - Why and HowDocument3 pagesClinician-Scientists in Public Sector Hospitals - Why and HowPierce ChowNo ratings yet
- Hospital Nabh Final ProjectDocument50 pagesHospital Nabh Final ProjectTarun Soni81% (21)
- Environmental Health Noncompliance: A Sanitarian's Search for a New SystemFrom EverandEnvironmental Health Noncompliance: A Sanitarian's Search for a New SystemNo ratings yet
- Improving Quality of Care at Sunlight HospitalDocument7 pagesImproving Quality of Care at Sunlight HospitalTooba SiddiquiNo ratings yet
- Lesson 1 (His) - Reflective LearningDocument1 pageLesson 1 (His) - Reflective LearningCristina PitongNo ratings yet
- TranscriptDocument3 pagesTranscriptDanna Sofia Gomez DuqueNo ratings yet
- Patient Health Data Form AssessmentDocument35 pagesPatient Health Data Form AssessmentErica DulayNo ratings yet
- Improve Healthcare QualityDocument12 pagesImprove Healthcare Qualitykasthu75No ratings yet
- And Employee Satisfaction Survey in Kulwanti HospitalDocument52 pagesAnd Employee Satisfaction Survey in Kulwanti HospitalAfaq Sana100% (1)
- A Survey Report On Scaling of Public Health Units As Sub Centers, PHC and CHC of Uttar Pradesh State, India.Document71 pagesA Survey Report On Scaling of Public Health Units As Sub Centers, PHC and CHC of Uttar Pradesh State, India.Voice of People100% (1)
- Dissertation Topics Masters Public HealthDocument6 pagesDissertation Topics Masters Public HealthPsychologyPaperWritingServiceHartford100% (1)
- Thesis Hospital AdministrationDocument8 pagesThesis Hospital Administrationjanaclarkbillings100% (1)
- Health Care Term PapersDocument6 pagesHealth Care Term Papersafmzkbuvlmmhqq100% (1)
- PSIP 6 Test GroupDocument10 pagesPSIP 6 Test GroupNCPQSWNo ratings yet
- Health Promotions Paper-Phillips PrinsDocument15 pagesHealth Promotions Paper-Phillips Prinsapi-621599790No ratings yet
- Four Strategies Health Care Leaders Can Use To Improve Safety and Quality in Their Organizations - Reader ViewDocument4 pagesFour Strategies Health Care Leaders Can Use To Improve Safety and Quality in Their Organizations - Reader ViewShuaib KauchaliNo ratings yet
- SDG Goal No 3Document10 pagesSDG Goal No 3Prasun SharmaNo ratings yet
- Quality Improvement ProcessDocument10 pagesQuality Improvement Processapi-284596154No ratings yet
- tmpDA48 TMPDocument6 pagestmpDA48 TMPFrontiersNo ratings yet
- Singapore Healthcare Lessons from TaiwanDocument3 pagesSingapore Healthcare Lessons from TaiwanCrystal ChiaNo ratings yet
- Chapter 1Document7 pagesChapter 1Jeremias Cruz CalaunanNo ratings yet
- Importance of understanding local healthcare systems for EBP implementationDocument2 pagesImportance of understanding local healthcare systems for EBP implementationJimmy Reece100% (3)
- A Study On An Analysis of Employee Wellness Interventions in It/ites SectorDocument10 pagesA Study On An Analysis of Employee Wellness Interventions in It/ites SectorAnonymous CwJeBCAXpNo ratings yet
- Research Paper Topics Health Care ManagementDocument8 pagesResearch Paper Topics Health Care Managementhjqojzakf100% (1)
- Sept 13 Journalreview 2 DocxDocument3 pagesSept 13 Journalreview 2 DocxHarold Mantaring LoNo ratings yet
- Qi ProjectDocument14 pagesQi Projectapi-641501601No ratings yet
- Issues and ChallengesDocument3 pagesIssues and ChallengesRosin JkNo ratings yet
- 1.7 Estudio de Caso Evaluación de ImpactoDocument2 pages1.7 Estudio de Caso Evaluación de ImpactoJoshilin Herhuay IncaNo ratings yet
- Ritchey Nurs660 ReflectionpaperDocument7 pagesRitchey Nurs660 Reflectionpaperapi-284230154No ratings yet
- Lynne Maher Original Transcript FinalDocument5 pagesLynne Maher Original Transcript Finalvinh vũNo ratings yet
- Brown Et Al., 2020Document5 pagesBrown Et Al., 2020LauraNo ratings yet
- Health and Social Care Unit 3 Promoting Good Health CourseworkDocument4 pagesHealth and Social Care Unit 3 Promoting Good Health Courseworkbcqneexy100% (1)
- Hospital Administration Research PapersDocument6 pagesHospital Administration Research Papersafmcbmoag100% (1)
- Chapter 1Document5 pagesChapter 1Angelo TarucNo ratings yet
- PSIP 7 Test SubmissionsDocument7 pagesPSIP 7 Test SubmissionsNCPQSWNo ratings yet
- Challenges of Rural Healthcare Diagnostic SoftwareDocument2 pagesChallenges of Rural Healthcare Diagnostic SoftwareCliqueLearn E-LearningNo ratings yet
- HLL ReportDocument138 pagesHLL ReportAparna K Das100% (1)
- EXPLANATIONSXZZZZDocument5 pagesEXPLANATIONSXZZZZSAMUEL REYESNo ratings yet
- Research Paper On The Welfare Effects of Behavioural InterventionsDocument4 pagesResearch Paper On The Welfare Effects of Behavioural InterventionshuhuNo ratings yet
- Running Head: FINAL EXAMDocument7 pagesRunning Head: FINAL EXAMapi-307874398No ratings yet
- 2020 MUSE Conference - Sessions - March 6 2020Document73 pages2020 MUSE Conference - Sessions - March 6 2020Michele LambertNo ratings yet
- Literature Review Melissa AguirreDocument7 pagesLiterature Review Melissa Aguirreapi-385824900No ratings yet
- Thesis Statement About Health Care ManagementDocument9 pagesThesis Statement About Health Care Managementubkciwwff100% (2)
- What Is The Role of Regulatory Agencies in Continuous Quality ImprovementDocument14 pagesWhat Is The Role of Regulatory Agencies in Continuous Quality ImprovementJana-Tae KerrNo ratings yet
- Why Nurses Need StatisticsDocument24 pagesWhy Nurses Need Statisticslizzy garciaNo ratings yet
- Report New 201 D - RemovedDocument15 pagesReport New 201 D - RemovedTEJESNo ratings yet
- Do You Think That The Philippines Have Achieved The Goals and Functions of A Health SystemDocument3 pagesDo You Think That The Philippines Have Achieved The Goals and Functions of A Health SystemPittzman Acosta0% (1)
- Presentation Mobile HealthDocument19 pagesPresentation Mobile Healthapi-242869850No ratings yet
- DSFDFSDGDFSGDocument9 pagesDSFDFSDGDFSGadasdaNo ratings yet
- Public Health Masters Thesis ExamplesDocument6 pagesPublic Health Masters Thesis Examplesybkpdsgig100% (2)
- M&E EvaluatnDocument2 pagesM&E EvaluatnNaa OdoiNo ratings yet
- Week 5 Assignment: Business, Government and SocietyDocument2 pagesWeek 5 Assignment: Business, Government and Societyarshdeep singhNo ratings yet
- BUS6004 Quality Management in A Care Setting - EditedDocument13 pagesBUS6004 Quality Management in A Care Setting - EditedMashaal FNo ratings yet
- A Study On The Relationship Between Corporate Wellness Programs and Employees' Stress, Job Satisfaction and AbsenteeismDocument16 pagesA Study On The Relationship Between Corporate Wellness Programs and Employees' Stress, Job Satisfaction and Absenteeismlinda_thomas1989No ratings yet
- Dissertation On Care HomesDocument4 pagesDissertation On Care HomesBuyingCollegePapersCanada100% (1)
- Final Paper MCDocument11 pagesFinal Paper MCapi-254038474No ratings yet
- 1.8 El Futuro de Las EvaluacionesDocument2 pages1.8 El Futuro de Las EvaluacionesJoshilin Herhuay IncaNo ratings yet
- 2.2 Estudio de Mujeres Como Hacedoras de PolíticasDocument3 pages2.2 Estudio de Mujeres Como Hacedoras de PolíticasJoshilin Herhuay IncaNo ratings yet
- HBS Professor Nava Ashraf Discusses Measuring ImpactsDocument2 pagesHBS Professor Nava Ashraf Discusses Measuring ImpactsJoshilin Herhuay IncaNo ratings yet
- 1.7 Estudio de Caso Evaluación de ImpactoDocument2 pages1.7 Estudio de Caso Evaluación de ImpactoJoshilin Herhuay IncaNo ratings yet
- Implementing a biometric tracking system in Karnataka health centersDocument2 pagesImplementing a biometric tracking system in Karnataka health centersJoshilin Herhuay IncaNo ratings yet
- UntitledDocument1 pageUntitledJoshilin Herhuay IncaNo ratings yet
- Impact Evaluation DesignDocument2 pagesImpact Evaluation DesignJoshilin Herhuay IncaNo ratings yet
- UntitledDocument2 pagesUntitledJoshilin Herhuay IncaNo ratings yet
- UntitledDocument2 pagesUntitledJoshilin Herhuay IncaNo ratings yet
- Getting lost in a desert is most dangerousDocument8 pagesGetting lost in a desert is most dangerousJoshilin Herhuay IncaNo ratings yet
- 5.1 - NetworkingDocument25 pages5.1 - NetworkingJoshilin Herhuay IncaNo ratings yet
- 4.5 - Describing A Place To StayDocument9 pages4.5 - Describing A Place To StayJoshilin Herhuay IncaNo ratings yet
- LP Trauma Kapitis PDFDocument29 pagesLP Trauma Kapitis PDFPajoNo ratings yet
- D&D 5eDocument4 pagesD&D 5eranaculaeNo ratings yet
- Important Issues in IHRMDocument3 pagesImportant Issues in IHRMsam130488No ratings yet
- Behaviorist Learning TheoryDocument2 pagesBehaviorist Learning TheoryBadine De LeonNo ratings yet
- Effective Leadership Theory Cases and Applications 1st Edition Humphrey Test BankDocument9 pagesEffective Leadership Theory Cases and Applications 1st Edition Humphrey Test Bankhillyobsidian8hi42g100% (36)
- The Relationship Between Lower Intelligence Crime and Custodial Outcomes A Brief Literary Review of A Vulnerable GroupDocument16 pagesThe Relationship Between Lower Intelligence Crime and Custodial Outcomes A Brief Literary Review of A Vulnerable GroupSteveNo ratings yet
- CONCRETING TITLEDocument5 pagesCONCRETING TITLEChristian Bulaong100% (1)
- Hemodynamic Effects of Dexmedetomidine vs ClonidineDocument12 pagesHemodynamic Effects of Dexmedetomidine vs ClonidinezzzzNo ratings yet
- Safety Data Sheet: Butyrylcholinesterase Inhibitor Screening Kit (Colorimetric)Document6 pagesSafety Data Sheet: Butyrylcholinesterase Inhibitor Screening Kit (Colorimetric)Verliyanti BastariNo ratings yet
- 18.20.04 - BSSL Seafarers Health Self Declaration With COVID 19 Test And... (1) - 3Document3 pages18.20.04 - BSSL Seafarers Health Self Declaration With COVID 19 Test And... (1) - 3Dean IL RE JamesNo ratings yet
- 1st Quarter Exam Pe and Health 11Document4 pages1st Quarter Exam Pe and Health 11Irish John GulmaticoNo ratings yet
- Clinical Handbook of Psychotropic Drugs, 25e (May 8, 2023)_(0889376328)_(Hogrefe Publishing) ( Etc.) (Z-Library)Document555 pagesClinical Handbook of Psychotropic Drugs, 25e (May 8, 2023)_(0889376328)_(Hogrefe Publishing) ( Etc.) (Z-Library)Dragutin PetrićNo ratings yet
- FomaDocument1,218 pagesFomaosamaeNo ratings yet
- Skilling For LivelihoodDocument19 pagesSkilling For LivelihoodPawanKumarNo ratings yet
- Recreation Healthcare Centre: Navya'S ClinicDocument3 pagesRecreation Healthcare Centre: Navya'S ClinicMitali MeherkarNo ratings yet
- 4.1.10 Practice Grammar FeedbackDocument10 pages4.1.10 Practice Grammar FeedbackbaileyNo ratings yet
- Long-Term Abstinence Following Holotropic Breathwork As Adjunctive Treatment of Substance Use Disorders and Related Psychiatric ComorbidityDocument7 pagesLong-Term Abstinence Following Holotropic Breathwork As Adjunctive Treatment of Substance Use Disorders and Related Psychiatric ComorbiditymghuesoNo ratings yet
- Basic Safety GuideDocument214 pagesBasic Safety Guide180190105084rabadiyahenilNo ratings yet
- Nursing Board Exam Answer Key and Test QuestionsDocument44 pagesNursing Board Exam Answer Key and Test Questionsrem_cen24100% (1)
- Computerized Medical Imaging and GraphicsDocument10 pagesComputerized Medical Imaging and Graphicshimanish shekhar DasNo ratings yet
- How To Negotiate With Nursing Authority Figures (Rough)Document2 pagesHow To Negotiate With Nursing Authority Figures (Rough)Meet DandiwalNo ratings yet
- OSHA Complaint FinalDocument3 pagesOSHA Complaint FinalBethanyNo ratings yet
- Differences and similarities among the three dopamine receptor partial agonistsDocument10 pagesDifferences and similarities among the three dopamine receptor partial agonistsolivukovic100% (1)
- Pediatric Nursing CareDocument7 pagesPediatric Nursing Carearcci balinasNo ratings yet
- Unpredictability of Fighter Pilots G Duration Tolerance by Anthropometric and Physiological Characteristics - CompressDocument5 pagesUnpredictability of Fighter Pilots G Duration Tolerance by Anthropometric and Physiological Characteristics - CompressMenatic muchNo ratings yet
- Timeless Beauty - Over 100 Tips, Secrets, and Shortcuts To Looking Great (PDFDrive)Document488 pagesTimeless Beauty - Over 100 Tips, Secrets, and Shortcuts To Looking Great (PDFDrive)Isabel Matta100% (1)
- WKF Para-Karate Kata Competition RulesDocument14 pagesWKF Para-Karate Kata Competition RulesMohamad IbrahimNo ratings yet
- Privacy NurseDocument62 pagesPrivacy NurseGerryNo ratings yet
- Lecture 3.2.3: Erection III: Steel Construction: Fabrication and ErectionDocument4 pagesLecture 3.2.3: Erection III: Steel Construction: Fabrication and ErectionMihajloDjurdjevicNo ratings yet
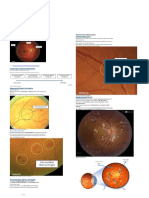
- Funduscopy Guide to Retinal and Optic Nerve PathologiesDocument4 pagesFunduscopy Guide to Retinal and Optic Nerve PathologiesavininditaNo ratings yet