Professional Documents
Culture Documents
Osteonecrosis of The Knee: Michael B. Boyd, William D. Bugbee
Uploaded by
Jaime Vázquez ZárateOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Osteonecrosis of The Knee: Michael B. Boyd, William D. Bugbee
Uploaded by
Jaime Vázquez ZárateCopyright:
Available Formats
CHA P T E R 54
Osteonecrosis of the Knee
Michael B. Boyd, DO
William D. Bugbee, MD
Osteonecrosis of the knee is a difficult clinical entity. Three Signs and Symptoms
general categories include idiopathic or spontaneous Spontaneous Osteonecrosis
osteonecrosis (also known as Ahlbäck disease), secondary
● Sudden pain usually over the medial aspect of the
or atraumatic osteonecrosis, and traumatic osteonecrosis.
knee (may be initiated by a minor injury)
The diagnosis of osteonecrosis can be arduous. A common
error is to misdiagnose degenerative subchondral bone ● Increased pain at night and with activity
cysts of osteoarthritis as spontaneous osteonecrosis. There Atraumatic Osteonecrosis
are several theories of the etiology of spontaneous osteo-
● Long-standing insidious pain (note: some patients
necrosis and atraumatic osteonecrosis, but in general,
these premises are not well understood. Traumatic osteo- may be asymptomatic)
necrosis hypothetically occurs after fracture or surgery. ● Pain may be difficult to localize
This chapter focuses on the unique presentations and
various treatment options of spontaneous osteonecrosis Physical Examination
and atraumatic osteonecrosis.
Typical Findings
Spontaneous Osteonecrosis
Preoperative Considerations ● Range of motion may be decreased secondary to pain,
muscle spasm, or subchondral collapse
History ● High sensitivity to touch over the lesion (usually, the
medial femoral condyle)
A thorough history may simplify the diagnosis of osteone- ● Swelling (±), effusion (±)
crosis. Risk factors for atraumatic osteonecrosis include
● Ligaments: stable
corticosteroid use, alcohol consumption, Gaucher disease,
sickle cell disease, caisson disease, coagulopathy, and sys- Atraumatic Osteonecrosis
temic lupus erythematosus. The typical patient with spon- ● Range of motion may be decreased secondary to pain,
taneous osteonecrosis is an obese woman older than 55 muscle spasm, or subchondral collapse
years. Spontaneous osteonecrosis is usually unilateral and
● Nonspecific knee pain (especially with multiple
typically affects just one condyle. Atraumatic osteonecrosis
lesions)
often presents bilaterally and can affect multiple condyles
or plateaus. In addition, it is frequently seen in other ● No swelling, no effusion
joints. ● Ligaments: stable
527
ch054-X3447.indd 527 10/17/2007 2:49:05 PM
Surgical Techniques of the Articular Cartilage
Imaging Optional
● Merchant view of patellofemoral joint
Radiography ● Long-leg anteroposterior mechanical axis view to
● Weight-bearing anteroposterior radiograph of knee in evaluate for malalignment
full extension with a radiopaque magnification marker Other Modalities
(Fig. 54-1A)
Magnetic resonance imaging can help confirm the diagno-
● Non–weight-bearing 90-degree-flexion lateral view of
sis and the extent of the lesion (Fig. 54-2)
knee (Fig. 54-1B) Technetium Tc 99 m bone scan is generally unreli-
● Notch (Fig. 54-1C) or Rosenberg view of knee able but may assist in diagnosis when radiographs are
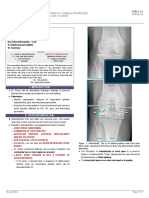
Figure 54-1 A, Anteroposterior standing radiograph of a knee with a
radiopaque magnification marker (the arrow demonstrates the tibial width
dimension used for allograft sizing). B, Non–weight-bearing 90-degree flexion
lateral view of a knee demonstrating atraumatic osteonecrosis. C, Notch
view of a knee depicting atraumatic osteonecrosis.
C
528
ch054-X3447.indd 528 10/17/2007 2:49:07 PM
Osteonecrosis of the Knee
Box 54-1 Aglietti Classification for Spontaneous Osteonecrosis
(Modified Koshino)
Stage I Normal radiographs; magnetic resonance imaging
abnormalities
Stage II Some flattening of the weight-bearing portion of the
condyle
Stage III Subchondral radiolucency with surrounding sclerosis
without sequestration
Stage IV ↑ Sclerosis with subchondral collapse and
sequestration; visible as a calcium plate
54
Stage V Secondary degenerative changes (narrowing of joint
space, osteophyte formation, subchondral sclerosis)
associated with some erosions
Box 54-2 Mont and Hungerford Classification for Atraumatic Osteonecrosis
(Modified Ficat-Arlet)
Stage I Normal radiographs, magnetic resonance imaging
A abnormalities
Stage II Cysts and sclerosis present
Stage III Subchondral collapse is seen as the crescent sign
Stage IV Secondary degenerative changes (narrowing of joint
space, osteophyte formation) on both sides of joint
Staging
The Aglietti classification for spontaneous osteonecrosis
(modified Koshino) and the Mont and Hungerford classi-
fication for atraumatic osteonecrosis (modified Ficat-
Arlet) are described in Boxes 54-1 and 54-2.
Treatment
B
Figure 54-2 Magnetic resonance images of a knee exhibiting spontaneous Nonoperative
osteonecrosis (A) and atraumatic osteonecrosis (B).
● Anti-inflammatory medicines (? benefit)
● Analgesics
● Pharmacologic treatment based on underlying disease
process
● Activity modifications, protective weight bearing
● Closed-chain quadriceps exercises
normal. Bipolar uptake is more indicative of osteoarthritis, ● Unloader knee brace
except in the late stages of osteonecrosis. Conversely,
Operative
simultaneous atraumatic osteonecrosis of the ipsilateral
tibial plateau and femoral condyle is certainly possible ● Arthroscopy ± débridement
during any stage and usually presents with more intense ● Core decompression by extra-articular drilling ± bone
uptake than with osteoarthritis. grafting
529
ch054-X3447.indd 529 10/17/2007 2:49:07 PM
Surgical Techniques of the Articular Cartilage
● Osteochondral allograft for large lesions versus
osteochondral autograft for small lesions
Core Decompression
● Realignment procedure: high tibial osteotomy for genu
Brief Description
varum versus distal femoral osteotomy for genu
valgum
Extra-articular drilling is recommended in the treatment of
● Unicompartmental knee arthroplasty versus total knee symptomatic osteonecrosis of the knee in pre–subchondral
arthroplasty collapse stages. Core decompression can be done in con-
Because of the heterogeneous nature of osteonecrosis of junction with knee arthroscopy. A small incision is made
the knee in both etiology and stage, no single technique is just proximal to the metaphyseal flare for femoral lesions
always preferred. Treatment should be individualized. and adjacent to the tubercle for tibial lesions. With fluoro-
Core decompression and allografting with or without scopic guidance, a 3- to 6-mm trephine is advanced to within
realignment are our preferred treatments for the younger 3 mm of the subchondral bone. The surgeon may elect to
population of patients and are further discussed in this lightly pack autologous iliac crest bone graft inside the
chapter. Our general treatment algorithm is presented in lesion. Postoperatively, the patient is restricted to 50%
Figure 54-3. partial weight bearing for 4 to 6 weeks.
SONK I, II, or III SONK IV SONK V
AONK I or II AONK III AONK IV
Nonoperative treatment - Fresh OCA
- OATS
(+/– Realignment procedure)
YES - Core decompression
Persistent
- Bone grafting
symptoms?
- Realignment procedure Persistent
symptoms?
NO YES
Persistent
symptoms?
Success TKA vs UKA
NO YES
NO
Radiographic
progression? YES TKA vs UKA
(consider fresh OCA +/–
NO realignment in pt younger
Bone Joint than 55 years old)
symptoms? symptoms?
Success
YES YES
Repeat core Arthroscopic débridement
decompression (consider fresh OCA vs OATS)
Figure 54-3 Treatment algorithm for osteonecrosis of the knee (modified Mont algorithm). SONK, spontaneous osteonecrosis; AONK, atraumatic osteonecrosis;
OATS, osteochondral autograft; OCA, osteochondral allograft; TKA, total knee arthroplasty; UKA, unicompartmental knee arthroplasty.
530
ch054-X3447.indd 530 10/17/2007 2:49:08 PM
Osteonecrosis of the Knee
Fresh Osteochondral Allografting Surgical Technique: Fresh
for Osteonecrosis of the Knee Osteochondral Allografting
Indications and Contraindications Anesthesia and Positioning
Fresh osteochondral allografting can be used as a salvage Anesthesia
procedure in patients for whom other treatments of osteo-
● General
necrosis have failed, including nonoperative care, arthros-
● Epidural
copy, and core decompression. Allografts are used as an
alternative to arthroplasty in the young population. Typi- ● Spinal
cally, the lesions should be more than 2 cm (approximately) ● Regional (±) 54
in diameter. Osteochondral autografting is an excellent
alternative for smaller lesions with compromised articular
Positioning
cartilage.
Relative contraindications to fresh osteochondral ● Supine on a standard operating room table
allografting include uncorrected limb malalignment and ● Padded thigh tourniquet
joint instability. The senior author has not found steroid ● Leg holder to position knee between 70 and 100
dependency to be a contraindication to fresh osteochon- degrees of flexion for access to the lesion
dral allografts, as previously reported in the literature.7a
Allografting should not be considered an alternative to
total knee arthroplasty or unicompartmental knee arthro-
plasty in a patient with symptoms, age, and activity level Surgical Landmarks, Incisions,
appropriate for prosthetic replacement. Finally, fresh and Portals
osteochondral allografting should not be performed in
the individual with advanced multicompartmental knee Landmarks
arthrosis.
Patella
Patellar tendon
Joint line
Tibial tubercle
Surgical Planning
Approaches
Concomitant Procedures ● Mini medial parapatellar arthrotomy
● Mini lateral parapatellar arthrotomy
Significant limb malalignment, ligamentous instability, or ● Standard medial parapatellar arthrotomy for
meniscal disease can be addressed either before or con- bicondylar lesions
comitant with fresh osteochondral allograft transplanta-
tion. Concomitant distal femoral osteotomy or femoral
condyle osteochondral allografting is not recommended Structures at Risk
and should be staged because of the increased fear of ● Medial parapatellar approach: anterior horn of medial
nonunion. meniscus, patellar tendon
● Lateral parapatellar approach: anterior horn of lateral
meniscus, patellar tendon
Allograft Sizing
Examination Under Anesthesia
A measurement of the width of the tibia, a few millimeters and Diagnostic Arthroscopy
inferior to the plateau, is made from a standing anteropos-
terior knee radiograph with a radiopaque magnification Examine the knee’s range of motion and stability under
marker (see Fig. 54-1A). The measurement is corrected for anesthesia. Perform a diagnostic arthroscopy before the
magnification and sent to the tissue bank for a matched allografting procedure if questions about the meniscus or
donor. articular cartilage exist.
531
ch054-X3447.indd 531 10/17/2007 2:49:08 PM
Surgical Techniques of the Articular Cartilage
Specific Steps (Box 54-3) or plug (generally 20 mm or larger) is the preferred tech-
nique as the instrumentation facilitates the procedure
1. Exposure (Fig. 54-5). This is the typical scenario for spontaneous
A standard midline incision is made from approximately osteonecrosis. Often, however, the disease is too extensive
the center of the patella to the tip of the tibial tubercle for a dowel or multiple dowels, and a freehand shell tech-
(Fig. 54-4). A medial or lateral parapatellar arthrotomy is nique is performed (typical for atraumatic osteonecrosis
then made extending from the superomedial or superolat- lesions).
eral aspect of the patella down to the distal end of the With the dowel technique, the lesion is inspected
incision. The incision can be extended for bicondylar and probed to assess its margins. A guide wire is then
lesions. Care is taken to preserve the anterior horn of the drilled perpendicular to the curvature of the articular
meniscus after incision through the infrapatellar fat pad. surface into the center of the lesion. The graft is sized with
For access to deep posterior femoral condyle lesions, the cannulated dowels. A cannulated cutting reamer is used to
meniscus may need to be taken down, leaving a cuff of penetrate the remaining articular cartilage. Next, 3 to
tissue for later repair. Retractors are placed medially and 4 mm of subchondral bone is removed with the appropri-
laterally to better expose the condyle. One of these retrac- ately sized cannulated bone reamer. If it is indicated, more
tors is carefully placed in the notch, retracting the patella necrotic bone can be reamed down to bleeding margins,
and protecting the cruciate ligaments. The knee is then not to exceed 6 to 10 mm. The guide wire is then removed
flexed to the appropriate level to deliver the lesion to the (Fig. 54-6). The depth of the lesion is measured in four
arthrotomy. If additional mobilization of the patella is nec-
essary, the fat pad can be released further, staying anterior
to the anterior horn of the opposite meniscus.
2. Recipient Site Preparation
Two techniques are used for osteochondral allografting,
the dowel and the shell techniques. When possible, a dowel
Box 54-3 Surgical Steps
1. Exposure
2. Recipient site preparation
3. Fresh osteochondral allograft preparation
4. Graft insertion and fixation
5. Closure Figure 54-5 Dowel technique instrumentation and fresh hemicondylar
femoral allograft.
Figure 54-4 Standard midline incision, medial parapatellar approach. Figure 54-6 Dowel technique—lesion reamed down to bleeding bone.
532
ch054-X3447.indd 532 10/17/2007 2:49:09 PM
Osteonecrosis of the Knee
quadrants (Fig. 54-7). If necessary, multiple small drill securely by an assistant with a large tenaculum bone clamp.
holes can be made to decompress the lesion. Curettage and A saw guide is placed perpendicular to the articular surface.
autologous bone grafting (i.e., iliac crest bone graft) can be The appropriately sized tube saw is placed over the guide
performed for extensive bone deficiency. At times, a second and used to core the graft (Fig. 54-10). The graft is then
graft is necessary to cover the entire lesion. In this case, amputated from the condyle with a cut at its base by an
the dowel technique is repeated, overlapping the grafts oscillating saw. The previously measured recipient site
(Fig. 54-8). depths are marked at the four corresponding quadrants of
Alternatively, the entire condyle might be involved, the graft. The graft is placed in a special bone holder, and
rendering it difficult to graft with simple dowels (Fig. 54- the oscillating saw is used to make the final cut at the
9A). In this situation, the recipient site is prepared by a marks. Fine adjustments can be made with a bone rasp.
freehand technique with osteotomes and burs. The goal is To reduce its immunogenicity, the graft is then copiously
to produce a simple geometric pattern (Fig. 54-9B). This irrigated with bacitracin solution by the jet lavage system 54
often incorporates the entire hemicondyle. The dimen- to remove any remaining bone marrow elements
sions and position of the prepared site are measured and (Fig. 54-11).
transferred to the allograft. With the shell technique, the cuts are made free-
hand, forming a geometric match of the recipient site (Fig.
3. Fresh Osteochondral Allograft Preparation 54-12). Repeated trial fittings are performed. The graft is
With the dowel technique, the matching anatomic loca-
tion on the donor graft is identified. The graft is held
A
Figure 54-7 Depth measurements of a dowel in four quadrants.
B
Figure 54-9 A, Severe atraumatic osteonecrosis lesion of the lateral femoral
hemicondyle requiring a shell technique. B, Lesion after débridement into
Figure 54-8 Overlapping dowel technique. simple geometric configuration.
533
ch054-X3447.indd 533 10/17/2007 2:49:12 PM
Surgical Techniques of the Articular Cartilage
A A
B B
Figure 54-10 A, Preparation of dowel allograft with a reamer. B, View of Figure 54-12 A, Example of shell allograft. B, Shell allograft implanted in
dowel allograft before amputation. lesion seen in Figure 54-9.
modified accordingly until the articular geometry is
restored.
4. Graft Insertion and Fixation
With the appropriate orientation, the allograft dowel is
manually inserted and gently tapped in place until flush. If
necessary, the recipient site can be opened up farther with
an oversized dilator. Fine adjustments to the allograft are
made. An excellent press fit is typically noted (Fig. 54-13);
however, the graft can be secured further with bioabsorb-
able pins. With a shell graft, fixation is obtained with a
combination of bioabsorbable pins and small titanium
screws. The knee is then put through a range of motion to
assess for graft stability and possible impingement, espe-
cially at the notch.
5. Closure
Figure 54-11 The allograft is washed thoroughly with a jet lavage system to Standard layered closure of the arthrotomy is performed
remove bone marrow elements.
over a 1/8-inch drain.
534
ch054-X3447.indd 534 10/17/2007 2:49:15 PM
Osteonecrosis of the Knee
● With meniscal detachment or repair and large
posterior grafts, flexion is limited to 60 degrees for
4 to 6 weeks.
● Progressive weight-bearing begins at 6 to 12 weeks.
● Sports and recreation are resumed at 6 months.
Complications
● Delayed union or nonunion of the allograft
Infection
●
54
● Arthrofibrosis
A
PEARLS AND PITFALLS
General
● Degenerative subchondral bone cysts (usually large, isolated defects
about the medial femoral condyle) are commonly misdiagnosed as
osteonecrosis but are rather a variant presentation of early
osteoarthritis.
● Defining the stage and lesion size (volume and surface area) is key
to sound application of our treatment algorithm.
● Subchondral fracture or collapse drastically alters prognosis and
limits treatment options.
Surgical
● Concomitant distal femoral osteotomy or femoral condyle
osteochondral allografting is not recommended and should be staged
because of fear of nonunion.
● For access to deep posterior femoral condyle lesions, the meniscus
may need to be taken down, leaving a cuff of tissue for later repair.
B
● If mobilization of the patella is necessary, the fat pad can be
Figure 54-13 A, Example of dowel graft adjacent to recipient site. released, staying anterior to the anterior horn of the opposite
B, Excellent press fit of dowel graft. meniscus.
Results
Postoperative Considerations
Core decompression can be an effective way to treat osteo-
Hospital Course necrosis of the knee, especially before the development of
subchondral collapse. Recent data have shown a 94%
● Hospital admission for 23 to 48 hours success rate with fresh osteochondral allografting with or
without realignment in steroid-induced osteonecrosis of
● Intravenous antibiotics for 24 hours
the knee in the young patient. Unicompartmental knee
● Drain removed on postoperative day 1 arthroplasty has been shown to be successful for the treat-
ment of end-stage spontaneous osteonecrosis. Total knee
arthroplasty is an excellent treatment for all end-stage
Rehabilitation osteonecroses. The use of cemented stems during total
knee arthroplasty improves the long-term results in
● Immediate touch-down weight bearing is permitted patients with mutifocal osteonecrosis. Uncemented total
with unlimited range of motion and quadriceps knee arthroplasty is no longer recommended in the treat-
strengthening for 6 to 12 weeks. ment of osteonecrosis. These results are summarized in
● Stationary bicycling is started at 4 weeks. Table 54-1.
535
ch054-X3447.indd 535 10/17/2007 2:49:20 PM
Surgical Techniques of the Articular Cartilage
Table 54-1 Clinical Results of Various Treatment Options of Osteonecrosis
Procedure Osteonecrosis Author Mean Miscellaneous Notes Outcome
Type Follow-up
High tibial osteotomy Spontaneous Koshino9 (1982) 5.1 years 23 knees with concomitant core 35 of 37 (95%)
decompression or bone grafting successful
Unicompartmental knee Spontaneous Aglietti et al1 4.4 years 35 total, 2 unicompartmental; all 35 of 37 (95%)
arthroplasty, total knee (1983) stages included successful
arthroplasty
Fresh osteochondral Atraumatic, Bayne et al2 4.8 years 3 of 3 patients with steroid- 6 of 13 (46%)
allograft, débridement, spontaneous, (1985) induced osteonecrosis treated spontaneous
high tibial osteotomy, traumatic with only fresh osteochondral successful; 4 of 7
core decompression allograft failed after 18 months (57%) atraumatic
successful
Core decompression Atraumatic Jacobs et al8 4.5 years 16 of 18 patients with steroid- 7 of 7 (100%) stage
(1989) induced osteonecrotic lesions I-II successful; 11 of
21 (52%) stage III
successful
Total knee arthroplasty Atraumatic, Bergman and 4 years Only a 68% 5-year predicted 33 of 38 (87%)
spontaneous Rand3 (1991) implant survivorship by revision successful
due to pain as end point
Unicompartmental knee Spontaneous Marmor10 5.5 years 2 of 4 failures due to subsequent 30 of 34 (88%)
arthroplasty (1993) osteonecrosis of opposite femoral successful
condyle
Fresh-frozen Atraumatic, Flynn et al5 4.2 years Young patient group, 2 patients 12 of 17 (71%)
osteochondral allograft spontaneous, (1994) with steroid-induced osteonecrosis successful
traumatic converted to total knee
arthroplasty
Nonoperative treatment Atraumatic Mont et al11 11 years Mean asymptomatic period, 11 26 of 32 (81%)
(1997) months; all but 6 required total unsuccessful
knee arthroplasty by 6 years
Core decompression Spontaneous Forst et al6 3 years No late stages 16 of 16 (100%)
(1998) successful
Total knee arthroplasty Atraumatic Seldes et al14 5.3 years 5 patients required revision (3, 26 of 31 (84%)
(1999) aseptic loosening; 2, sepsis) successful
Core decompression Atraumatic Mont et al12 7 years No late stages; 15 successful 72 of 91 (79%)
(2000) knees needed repeated surgery successful
Total knee arthroplasty Atraumatic, Mont et al13 9 years Improved results attributed to use 31 of 32 (97%)
spontaneous (2002) of cement in all patients and successful
stems as warranted
Iliac crest autograft Atraumatic Fukui et al7 6.6 years Young patient group with large 9 of 10 (90%)
with periosteum (2002) steroid-induced osteonecrotic successful
lesions
Fresh osteochondral Atraumatic Bugbee et al4 5.3 years Young patient group with large 17 of 18 (94%)
allograft (2004) steroid-induced osteonecrotic successful
lesions
536
ch054-X3447.indd 536 10/17/2007 2:49:23 PM
Osteonecrosis of the Knee
References
1. Aglietti P, Insall JN, Buzzi R. Idiopathic osteonecrosis of the knee. 7a. Gross AF, McKee NH, Pritzker KP, et al. Reconstruction of skeletal
Aetiology, prognosis and treatment. J Bone Joint Surg Br deficits of the knee: a comprehensive osteochondral transplant
1983;65:588-597. program. Clin Orthop 1983;174:96-106.
2. Bayne O, Langer F, Pritzker KP, et al. Osteochondral allografts in the 8. Jacobs MA, Loeb PE, Hungerford DS. Core decompression of the
treatment of osteonecrosis of the knee. Orthop Clin North Am distal femur for avascular necrosis of the knee. J Bone Joint Surg Br
1985;16:727-740. 1989;71:583-587.
3. Bergman NR, Rand JA. Total knee arthroplasty in osteonecrosis. 9. Koshino T. The treatment of spontaneous osteonecrosis of the knee
Clin Orthop 1991;273:77-82. by high tibial osteotomy with and without bone-grafting or drilling
4. Bugbee WD, Khadivi B, Jamali A. Fresh osteochondral allografting of the lesion. J Bone Joint Surg Am 1982;64:47-58.
in the treatment of osteonecrosis of the knee [paper No. 108]. Amer- 10. Marmor L. Unicompartmental arthroplasty for osteonecrosis of the
ican Academy of Orthopaedic Surgeons annual meeting; San Fran- knee joint. Clin Orthop 1993;294:247-253.
cisco, Calif; 2004. 11. Mont MA, Tomek IM, Hungerford DS. Core decompression for 54
5. Flynn JM, Springfield DS, Mankin HJ. Osteoarticular allografts to avascular necrosis of the distal femur—long term followup. Clin
treat distal femoral osteonecrosis. Clin Orthop 1994;303:38-43. Orthop 1997;334:124-130.
6. Forst J, Forst R, Heller KD, Adam G. Spontaneous osteonecrosis of 12. Mont MA, Baumgarten KM, Rifai A, et al. Atraumatic osteonecrosis
the femoral condyle: casual treatment by early core decompression. of the knee. J Bone Joint Surg Am 2000;82:1279-1290.
Arch Orthop Trauma Surg 1998;117:18-22. 13. Mont MA, Rifai A, Baumgarten KM, et al. Total knee arthroplasty
7. Fukui N, Kurosawa H, Kawakami A, et al. Iliac bone graft for for osteonecrosis. J Bone Joint Surg Am 2002;84:599-603.
steroid-associated osteonecrosis of the femoral condyle. Clin Orthop 14. Seldes RM, Tan V, Duffy G, et al. Total knee arthroplasty for steroid-
2002;401:185-193. induced osteonecrosis. J Arthroplasty 1999;14:533-537.
537
ch054-X3447.indd 537 10/17/2007 2:49:23 PM
You might also like
- Recovery in Credit GrantedDocument21 pagesRecovery in Credit GrantedMaria Ysabella Yee80% (5)
- LC - Gunk SqueezesDocument5 pagesLC - Gunk SqueezesHeris SitompulNo ratings yet
- Cii Seniorcareindustryreportindia2018 180524043125Document36 pagesCii Seniorcareindustryreportindia2018 180524043125N InbasagaranNo ratings yet
- 7 How To Build The Super-Parasol Part IDocument6 pages7 How To Build The Super-Parasol Part IkroitorNo ratings yet
- Acute Traumatic Knee RadiographsDocument10 pagesAcute Traumatic Knee RadiographsPrashant GuptaNo ratings yet
- The Role of Arthroscopy in Instability of The Elbow 2023 JSES InternationalDocument6 pagesThe Role of Arthroscopy in Instability of The Elbow 2023 JSES Internationaligor gayosoNo ratings yet
- The Stiff Elbow: Review Articles of TopicsDocument12 pagesThe Stiff Elbow: Review Articles of TopicsArif Kurniawan ListiantoNo ratings yet
- Avascular Necrosis of Hip - (Johannes)Document29 pagesAvascular Necrosis of Hip - (Johannes)EntesipatyNo ratings yet
- Complications After Arthroscopic Knee SurgeryDocument4 pagesComplications After Arthroscopic Knee SurgeryEma.diazNo ratings yet
- ArtosDocument22 pagesArtosRia Rahmadiyani IINo ratings yet
- Arthroscopic Management of Rare Intra-Articular Lesions of The ShoulderDocument6 pagesArthroscopic Management of Rare Intra-Articular Lesions of The ShoulderJaime Vázquez ZárateNo ratings yet
- 65 The Arthritic Hi 2018 Clinical Orthopaedic Rehabilitation A Team ApproDocument5 pages65 The Arthritic Hi 2018 Clinical Orthopaedic Rehabilitation A Team ApproJessica HongNo ratings yet
- Achilles Tendon Rupture: Basic InformationDocument3 pagesAchilles Tendon Rupture: Basic InformationDiah Rindayani HasbiNo ratings yet
- Sonography of The Knee Joint PDFDocument8 pagesSonography of The Knee Joint PDFChavdarNo ratings yet
- Osteochondral Defects in The Ankle: Why Painful?: &) M. L. Reilingh M. ZengerinkDocument11 pagesOsteochondral Defects in The Ankle: Why Painful?: &) M. L. Reilingh M. ZengerinkGeraldine Alvarez ANo ratings yet
- Osteoid Osteoma: Multimodality Imaging With Focus On Hybrid ImagingDocument18 pagesOsteoid Osteoma: Multimodality Imaging With Focus On Hybrid ImagingCătălin Paul CernișencuNo ratings yet
- Focused ReviewDocument6 pagesFocused ReviewGina GiammalvoNo ratings yet
- 29 Acl Aj Unhan PDFDocument26 pages29 Acl Aj Unhan PDFMario MarcellinoNo ratings yet
- Osgood SlaterDocument5 pagesOsgood Slaterpruebaunodos123No ratings yet
- Compression FractureDocument4 pagesCompression FracturepuchioNo ratings yet
- Fraktur PatellaDocument6 pagesFraktur PatellaPutri AndiraNo ratings yet
- OA Presentation Parth SinghDocument20 pagesOA Presentation Parth Singhparthsingh4211No ratings yet
- Arthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR JaneDocument73 pagesArthritis: Prepared By: Salini D/O Vasudevan Supervisor: DR Janeumanantini06No ratings yet
- Knee Disorders of The Inert Structures Capsular and Non-Capsular PatternsDocument16 pagesKnee Disorders of The Inert Structures Capsular and Non-Capsular PatternsFrankChenNo ratings yet
- Osteonecrosis: Avascular NecrosisDocument8 pagesOsteonecrosis: Avascular NecrosisJezreel BonaNo ratings yet
- Medscape Knee OCDDocument16 pagesMedscape Knee OCDDita Ambarsari SyafruddinNo ratings yet
- Codo DolorDocument9 pagesCodo DolorPe T. ErNo ratings yet
- Arthroscopy: If You Have Persistent Joint Pain, Your Doctor May Suggest ArthrosDocument4 pagesArthroscopy: If You Have Persistent Joint Pain, Your Doctor May Suggest ArthrosCaty RamosNo ratings yet
- RAD Radiographic Features of Common ArthritidesDocument7 pagesRAD Radiographic Features of Common ArthritidesLA BriguelaNo ratings yet
- Osteoarthritis of HipDocument3 pagesOsteoarthritis of Hipjcachica21No ratings yet
- Radio Logical Assessment of OA FinalDocument60 pagesRadio Logical Assessment of OA FinaltarikeopsNo ratings yet
- New Advances in Wrist ArthrosDocument13 pagesNew Advances in Wrist ArthrosDiego Maté MartínNo ratings yet
- Total Knee Arthroplasty in Osteopetrosis Using Patient-Specific InstrumentationDocument4 pagesTotal Knee Arthroplasty in Osteopetrosis Using Patient-Specific InstrumentationDavidBeatonComuladaNo ratings yet
- Rehabilitacion ReumatologicaDocument22 pagesRehabilitacion ReumatologicaRosa M. AlcaláNo ratings yet
- Ortho ACLDocument18 pagesOrtho ACLKamila Furqani DjibranNo ratings yet
- Bone ScanDocument22 pagesBone ScanChrysi TsiouriNo ratings yet
- Clinical Review: The Orthopaedic Approach To Managing Osteoarthritis of The KneeDocument5 pagesClinical Review: The Orthopaedic Approach To Managing Osteoarthritis of The KneeRina WatiNo ratings yet
- Comminuted Patella FracturesDocument8 pagesComminuted Patella FracturesKirana lupitaNo ratings yet
- Osteoarthritis, Gouty Arthritis, and Rheumatoid ArthritisDocument37 pagesOsteoarthritis, Gouty Arthritis, and Rheumatoid ArthritisDianaNo ratings yet
- 1982 4378 Rbort 54 06 0736Document3 pages1982 4378 Rbort 54 06 0736azevedoNo ratings yet
- Rheumatoid Disorder Imaging - Refarat Radiologi IkramDocument18 pagesRheumatoid Disorder Imaging - Refarat Radiologi Ikramikram hanafiNo ratings yet
- Arthritis, Spine Imaging, and Beyond - : Dr. Harun Gupta's TalkDocument20 pagesArthritis, Spine Imaging, and Beyond - : Dr. Harun Gupta's TalkDonna MaharaniNo ratings yet
- Orthopaedics EmergenciesDocument63 pagesOrthopaedics EmergencieszzooooeeeeeeNo ratings yet
- Osteoarthritis 191016103144Document49 pagesOsteoarthritis 191016103144dr.abouzaid098No ratings yet
- Endoscopic Resection of Symptomatic Osteochondroma of The Distal FemurDocument4 pagesEndoscopic Resection of Symptomatic Osteochondroma of The Distal FemurAlex CirlanNo ratings yet
- Total Knee Arthroplasty For Severe Valgus Deformity: J Bone Joint Surg AmDocument15 pagesTotal Knee Arthroplasty For Severe Valgus Deformity: J Bone Joint Surg AmAbdiel NgNo ratings yet
- Knee Cartilage and MeniscalDocument4 pagesKnee Cartilage and MeniscalKapil LakhwaraNo ratings yet
- Osteo Arthit IsDocument19 pagesOsteo Arthit IsShaa ShawalishaNo ratings yet
- Braddom RheumatologyDocument22 pagesBraddom RheumatologynesNo ratings yet
- Senior Citizen's Day - 21 August 2021Document2 pagesSenior Citizen's Day - 21 August 2021Times MediaNo ratings yet
- Percutaneous Femoral Derotational Osteotomy For Excessive Femoral TorsionDocument7 pagesPercutaneous Femoral Derotational Osteotomy For Excessive Femoral TorsionDouglas PrinaNo ratings yet
- Amputation Related PainDocument9 pagesAmputation Related Painvandrade_635870No ratings yet
- Arthritis AlgorithmDocument1 pageArthritis Algorithmaniqahmed6565No ratings yet
- Loose Bodies Tips PearlsDocument10 pagesLoose Bodies Tips PearlsGus AbellaNo ratings yet
- Knee Osteoarthritis: DefinitionDocument19 pagesKnee Osteoarthritis: DefinitionShrouq BadrNo ratings yet
- Basic Knee Arthroscopy Part 4Document2 pagesBasic Knee Arthroscopy Part 4Diego BellingNo ratings yet
- Arthroscopy Synovectomy and Lateral ReleaseDocument2 pagesArthroscopy Synovectomy and Lateral Releasevenkata ramakrishnaiahNo ratings yet
- Diagnostic Imaging - 12 - Regional Pathologies and Evaluation - Tendon - Muscle - Cartilage - Nerve - Prof - Dr.i̇smet TAMERDocument18 pagesDiagnostic Imaging - 12 - Regional Pathologies and Evaluation - Tendon - Muscle - Cartilage - Nerve - Prof - Dr.i̇smet TAMERAly MssreNo ratings yet
- Group 10 NCM 112 - (Osteonecrosis)Document8 pagesGroup 10 NCM 112 - (Osteonecrosis)Jezreel BonaNo ratings yet
- A Flexion Osteotomy For Correction of A Distal Tibial Recurvatum Deformity - A Retrospective Case SeriesDocument9 pagesA Flexion Osteotomy For Correction of A Distal Tibial Recurvatum Deformity - A Retrospective Case SeriesHamelinYangNo ratings yet
- Classification of Wrist FracturesDocument6 pagesClassification of Wrist FracturesshinhyejjNo ratings yet
- Outcome Assesment of Proximal Fibular Osteotomy in Medial Compartment Knee OsteoarthritisDocument3 pagesOutcome Assesment of Proximal Fibular Osteotomy in Medial Compartment Knee OsteoarthritisPrashant GuptaNo ratings yet
- Cartilage Injury of the Knee: State-of-the-Art Treatment and ControversiesFrom EverandCartilage Injury of the Knee: State-of-the-Art Treatment and ControversiesAaron J. KrychNo ratings yet
- Surgery of the Cranio-Vertebral JunctionFrom EverandSurgery of the Cranio-Vertebral JunctionEnrico TessitoreNo ratings yet
- Arthroscopic Treatment of Internal Impingement: Matthew T. Boes, Craig D. MorganDocument15 pagesArthroscopic Treatment of Internal Impingement: Matthew T. Boes, Craig D. MorganJaime Vázquez ZárateNo ratings yet
- Hamstring Tendon Autograft For Anterior Cruciate Ligament ReconstructionDocument22 pagesHamstring Tendon Autograft For Anterior Cruciate Ligament ReconstructionJaime Vázquez ZárateNo ratings yet
- CHAPTER 14 - Treatment of Bone Def - 2008 - Surgical Techniques of The ShoulderDocument11 pagesCHAPTER 14 - Treatment of Bone Def - 2008 - Surgical Techniques of The ShoulderJaime Vázquez ZárateNo ratings yet
- Medial Collateral Ligament Repair and Reconstruction: Other Surgical Techniques of The KneeDocument8 pagesMedial Collateral Ligament Repair and Reconstruction: Other Surgical Techniques of The KneeJaime Vázquez ZárateNo ratings yet
- Transtibial Tunnel Posterior Cruciate Ligament ReconstructionDocument9 pagesTranstibial Tunnel Posterior Cruciate Ligament ReconstructionJaime Vázquez ZárateNo ratings yet
- Open Repair of Anterior Shoulder Instability: Michael J. PagnaniDocument11 pagesOpen Repair of Anterior Shoulder Instability: Michael J. PagnaniJaime Vázquez ZárateNo ratings yet
- Distal Realignment For Patellofemoral Disease: Jack FarrDocument13 pagesDistal Realignment For Patellofemoral Disease: Jack FarrJaime Vázquez ZárateNo ratings yet
- CHAPTER 19 - Mini Open Rota - 2008 - Surgical Techniques of The Shoulder ElbowDocument7 pagesCHAPTER 19 - Mini Open Rota - 2008 - Surgical Techniques of The Shoulder ElbowJaime Vázquez ZárateNo ratings yet
- Arthroscopic Management of Rare Intra-Articular Lesions of The ShoulderDocument6 pagesArthroscopic Management of Rare Intra-Articular Lesions of The ShoulderJaime Vázquez ZárateNo ratings yet
- CHAPTER 8 - Arthroscopic Repair of - 2008 - Surgical Techniques of The ShoulderDocument11 pagesCHAPTER 8 - Arthroscopic Repair of - 2008 - Surgical Techniques of The ShoulderJaime Vázquez ZárateNo ratings yet
- Pebble in The Pond by David MerrillDocument22 pagesPebble in The Pond by David MerrillKangdon Lee100% (3)
- Smart School EseiDocument15 pagesSmart School Eseiz89100% (1)
- Javascript: Case Study To Be Used For Hands-On SessionsDocument14 pagesJavascript: Case Study To Be Used For Hands-On SessionsSettiNagarajuNo ratings yet
- Electronic Unit Injector - Remove: C6.6 Industrial EngineDocument12 pagesElectronic Unit Injector - Remove: C6.6 Industrial EngineBassieNo ratings yet
- Effect of Temperature On SolubilityDocument8 pagesEffect of Temperature On SolubilityMuzahid KhatryNo ratings yet
- Ppe Training NTTFDocument47 pagesPpe Training NTTFAkshatha M100% (1)
- Irfan Byna Nur Akbar MT PresentationDocument14 pagesIrfan Byna Nur Akbar MT PresentationirfanNo ratings yet
- DFX8 WebDocument2 pagesDFX8 Websamer8saifNo ratings yet
- CBT Nuggets Ccent & Ccna - Season 1 ListDocument5 pagesCBT Nuggets Ccent & Ccna - Season 1 ListRusu AlexandruNo ratings yet
- Vitamins and Minerals Lecture NotesDocument9 pagesVitamins and Minerals Lecture NotesJoymae Olivares Tamayo100% (1)
- Independent Contractor Agreement For Accountant & BookkeeperDocument7 pagesIndependent Contractor Agreement For Accountant & BookkeeperWen' George BeyNo ratings yet
- LFS EksellDisplayDocument7 pagesLFS EksellDisplayillustratio.academyNo ratings yet
- Progress Audio Script 2Document1 pageProgress Audio Script 2groniganNo ratings yet
- Application Form Safety Program Pg1Document1 pageApplication Form Safety Program Pg1Mark Jayson GarciaNo ratings yet
- Vacancy For Ceo-Tanzania Association of Accountants-RevisedDocument2 pagesVacancy For Ceo-Tanzania Association of Accountants-RevisedOthman MichuziNo ratings yet
- Review of Process Parameters For Biodiesel Production From Different FeedstocksDocument9 pagesReview of Process Parameters For Biodiesel Production From Different FeedstocksHow Heoy GeokNo ratings yet
- Forex Money Management - Scaling Out Is A MustDocument4 pagesForex Money Management - Scaling Out Is A MustThomas SteinNo ratings yet
- Choose The Best Answer From The Four Options (Marked A, B, C, or D) To Complete The Sentences. Exercise 1Document6 pagesChoose The Best Answer From The Four Options (Marked A, B, C, or D) To Complete The Sentences. Exercise 1Van AnhNo ratings yet
- Digital Systems Design and PrototypingDocument633 pagesDigital Systems Design and PrototypingAshish Shrivastava50% (2)
- Oral Case Presentation Benchmarks - : Identifying Information & Chief ConcernDocument9 pagesOral Case Presentation Benchmarks - : Identifying Information & Chief ConcernManisanthosh KumarNo ratings yet
- Soal Pas B.ing KLS 7Document2 pagesSoal Pas B.ing KLS 7Hernadi TaLaNo ratings yet
- OCI Introduction: Presented By: Rahul MiglaniDocument21 pagesOCI Introduction: Presented By: Rahul Miglanisss pppNo ratings yet
- East Anglian Sea School: T: 01473 659992 Suffolk Yacht Harbour, Levington, Suffolk IP10 0LN EDocument2 pagesEast Anglian Sea School: T: 01473 659992 Suffolk Yacht Harbour, Levington, Suffolk IP10 0LN Etom hesterNo ratings yet
- Research Youth EmpowermentDocument18 pagesResearch Youth EmpowermentShiba Tatsuya0% (2)
- Roxas Claire B. Science Technology and Society 09 Activity 1Document1 pageRoxas Claire B. Science Technology and Society 09 Activity 1Eldrick Neil Reyes100% (1)
- The Marine WorkoutDocument7 pagesThe Marine WorkoutAndres Eco AldeanoNo ratings yet