Professional Documents
Culture Documents
PASS - Principles - For - Predictable - Bone.8
Uploaded by
Pedro PachecoOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
PASS - Principles - For - Predictable - Bone.8
Uploaded by
Pedro PachecoCopyright:
Available Formats
“PASS” Principles for Predictable
Bone Regeneration
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
Hom-Lay Wang, DDS, MSD,* and Lakshmi Boyapati, BDS†
uided bone regeneration (GBR) Guided bone regeneration is a supply and undifferentiated mesen-
G describes a surgical technique
that increases and augments al-
veolar bone volume in areas designated
well-established technique used for
augmentation of deficient alveolar
ridges. Predictable regeneration re-
chymal cells, space maintenance/
creation to facilitate adequate space
for bone ingrowth, and stability of
for future implant placement, or around quires both a high level of technical wound and implant to induce blood
previously placed implants. The princi-
skill and a thorough understanding clot formation and uneventful heal-
ple of GBR is based on the principles of
guided tissue regeneration.1-4 The prin- of underlying principles of wound ing events. In addition, a novel flap
Y6JAw== on 03/30/2023
ciples delineated by Melcher5 described healing. This article describes the 4 design and clinical cases using this
the need for cell exclusion to enable the major biologic principles (i.e., principle are presented. (Implant
healing wound to be populated by cells PASS) necessary for predictable Dent 2006;15:8 –17)
thought to be more favorable for regen- bone regeneration: primary wound Key Words: guided bone regenera-
eration. In GBR, the cells that are re- closure to ensure undisturbed and tion, bone grafts, horizontal bone
quired to repopulate the wound are uninterrupted wound healing, angio- augmentation, implants
primarily osteoblasts. Osteoblasts are genesis to provide necessary blood
responsible for laying down new alveo-
lar bone and for future bone remodeling.
By selectively excluding epithelium and creation/maintenance, and stability of and overall tissue remodeling. In ad-
connective tissue with the use of bone both the initial blood clot and implant dition, postoperative discomfort may
grafting and barrier materials, bone is fixture (PASS). be reduced as a result of less exposure
“guided” into the desired position. of underlying connective tissue. Most
Dahlin et al6 were the first to show that investigators have advocated the ne-
bony defects created in rat mandibles PRIMARY CLOSURE
cessity of primary closure following
could be successfully closed using The 2 basic methods of wound implant placement to ensure predict-
guided tissue regeneration procedures. healing are termed healing by primary able GBR outcomes,7,12-15 while others
The success and predictability of intention and secondary intention, re-
have disputed its importance. 16,17
GBR have since vastly broadened the spectively. In healing by primary in-
Nonetheless, there is a consensus that
applicability of implant therapy. Im- tension, the edges of a wound are
primary wound coverage should be ac-
plants can now be placed in areas of placed together in virtually the same
position they held before the injury. complished whenever possible.
previously deficient bone volume,
Secondary intention describes healing Examining the effect of mem-
with success rates reported higher than
95%.7-11 However, to ensure predict- that occurs when wound edges cannot brane exposure on bone volume gains
ability of this technique, clinical pro- be closely approximated, resulting in a highlights the importance of primary
cedures should be based on sound wound that is slower to heal, requires wound closure. Machtei18 performed a
biologic principles. This article out- more collagen remodeling, and is metaanalysis to evaluate the effects of
lines the 4 major principles underlying more likely to result in scar formation. membrane exposure on treatment out-
successful GBR (Fig. 1): primary Realistically, true healing by primary comes in guided tissue regeneration
wound closure, angiogenesis, space intention is often difficult to achieve. and GBR. When looking at guided
However, primary wound closure is a tissue regeneration cases alone, ex-
fundamental surgical principle for posed membranes showed only 0.47
*Professor and Director of Graduate Periodontics, Department GBR because it creates an environ- mm less attachment gain compared to
of Periodontics and Oral Medicine, School of Dentistry,
University of Michigan, Ann Arbor, MI. ment that is undisturbed/unaltered by membranes that remained submerged.
†Resident, Department of Periodontics and Oral Medicine,
School of Dentistry, University of Michigan, Ann Arbor, MI. outside bacterial or mechanical insult. In comparison, membrane exposure
Passive closure of wound edges seemed to have a significant deleteri-
ISSN 1056-6163/06/01501-008
Implant Dentistry enables the wound to heal with less ous effect on bone formation. In cases
Volume 15 • Number 1
Copyright © 2006 by Lippincott Williams & Wilkins reepithelialization, collagen formation in which the membrane remained sub-
DOI: 10.1097/01.id.0000204762.39826.0f and remodeling, wound contraction, merged, a mean 3.01 mm of new bone
8 “PASS” PRINCIPLES FOR PREDICTABLE BONE REGENERATION
supporting and space maintaining
device.43-45
In a series of 2 reports on local-
ized ridge augmentation using GBR,
Buser et al46,47 advocated primary soft
tissue healing, to avoid membrane ex-
posure, by using a lateral incision
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
technique. Other techniques that have
been advocated in an effort to gain
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
tension-free primary wound closure
include a buccal rotational flap,48
coronally positioned palatal sliding
flap,49 split palatal rotated flap,50 and,
more recently, a palatal advanced
Fig. 1. Principles of successful GBR.
flap.15 Together, the aforementioned
studies highlight the importance of
primary wound closure. Correct flap
was noted, whereas in cases with was attained, and clinical evaluation design, tension-free flap approxima-
membrane exposure, an average of was performed after 4 months of heal- tion, and postoperative care of the
0.56 mm of new bone was noted. ing. In cases in which the membranes wound site are keys to achieving, and
Similar results of a reduced remained covered, 14/19 sites with de-
Y6JAw== on 03/30/2023
maintaining, primary closure. Flaps
amount of bone formation subsequent hiscence showed 100% bone fill in the should be carefully designed and exe-
to membrane exposure have been space created by the membrane. How- cuted to ensure passive closure with-
reported.11,18-22 Simion et al20 exam- ever, in the areas of membrane expo- out tension on the wound margins.
ined membrane exposure in cases of sure, little bone regeneration occurred. Collagen membranes, with their che-
GBR at the implant placement. The These findings have further been con- motactic function, may facilitate pri-
investigators found that 99.6% bone firmed in a beagle dog model30,31 and mary wound coverage, even after
regeneration was obtained around fix- more recently in human beings.32 membrane exposure.42
tures where membrane exposure did The majority of membrane expo-
not occur for 6-8 months following sure data relate to nonresorbable mem-
implant placement. In contrast, only branes, both reinforced and nonreinforced. ANGIOGENESIS
48.6% of bone regeneration was found The development and widespread use of
when membrane exposure occurred absorbable collagen membranes may Wound healing around implants is
earlier. Other studies have examined circumvent this problem. Indeed, in similar to wound healing events in
early versus late membrane exposure addition to a reduced risk of mem- other parts of the oral cavity, with
or removal.19,23,24 It seems that if a brane exposure,22 the reported advan- several important exceptions. In par-
membrane can remain covered for a tages of these membranes are a lack of ticular, bone regeneration progresses
significant period, up to 6-8 months, need for second stage surgery and in a sequence that closely parallels its
bone regeneration is predictable. physiologically favorable properties normal formation.51 The surface of the
Factors that impede wound heal- of the membranes themselves, such as implant provides a platform on which
ing in an otherwise healthy individual hemostatic, chemotactic, and cell ad- an initial blood clot may form. The
are foreign materials, necrotic tissue, hesion functions.33-35 addition of bone grafting materials and
compromised blood supply, and Advantages of collagen mem- membranes, in accordance with the
wound tension. These factors may branes include their hemostatic func- principles of GBR, serves to create
partly explain the reduced bone forma- tion by platelet aggregation, which space and mediate osteogenesis via
tion around exposed membranes. facilitates early clot formation and potential release of bone morphoge-
Other possible reasons for the reduced wound stabilization. Both early clot netic proteins. Following implant place-
amount of bone formation are contam- formation and wound stabilization are ment, the first 24 hours are characterized
ination of the membrane with oral mi- considered essential for successful re- by formation of a blood clot around im-
croflora caused by an open wound.25-28 generation.36 Collagen also possesses plant and in the space created by mem-
More rapid resorption of bone grafting a chemotactic function for fibroblasts branes and bone grafting material. The
materials in areas of membrane expo- that assists in cell migration to pro- initial blood clot is removed by neutro-
sure has also been reported. Jovanovic mote primary wound closure.37 Colla- phils and macrophages, and initial for-
et al29 examined 11 patients with de- gen membranes are also effective in mation of granulation tissue begins
hiscence defects on the facial aspect of inhibiting epithelial migration and within the next days and weeks. The
19 threaded implants. A unique promoting new connective tissue granulation tissue is rich in blood ves-
method of providing space was by attachment.38-42 Predictable treatment sels, and it is these vessels that are key
placing the membrane over the im- outcomes have been shown using to osteoid formation and subsequent
plants and fixating them with the im- absorbable collagen membranes in mineralization to woven bone.52 Pri-
plant cover screw. Primary closure conjunction with bone mineral as a marily deposited woven bone will be
IMPLANT DENTISTRY / VOLUME 15, NUMBER 1 2006 9
converted into mature lamellar bone ports regarding the beneficial effect of collagen membranes (i.e., BioGide;
by secondary remodeling.53 regional acceleratory phenomenon Osteohealth Co., Shirley, NY, and Bio-
There is an intimate relationship have also been reported.65,70,71 Lun- Mend Extend; Zimmer Dental Inc.,
between newly formed blood vessels dgren et al65 used a rabbit calvarial Carlsbad, CA) on GBR in surgically
and de novo bone formation.54 It has model to evaluate the effects of decor- created buccal implant dehiscence de-
been shown that between 6 and 9 tication. There were 2 titanium cylin- fects. Membrane exposure occurred at
months are needed to fill completely ders with titanium lids inserted in the 9 of 15 sites and was associated with
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
the wound space, initially filled with skulls of 8 rabbits. In each animal, the poorer regenerative outcomes. In ad-
blood clot, then with new bone.55 test side had the outer layer of cortical dition, a pattern of membrane collapse
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
Buser et al47 found that introducing bone removed, while the control side in most of the exposed sites (8 of 9)
cortical perforations (i.e., intra-bone was left with an intact cortex. Block was associated with less regeneration.
marrow penetration) allowed migra- section and histology performed at 3 The investigators concluded that space
tion of cells with angiogenic and os- months in all animals revealed no dif- maintenance and membrane coverage
teogenic potential. Nonetheless, some ference in total amount of augmented were the 2 most important factors af-
studies have showed that bone regen- tissue (75.5% compared to 71.2%) or fecting GBR using bioabsorbable col-
eration can occur even from a nonin- the augmented mineralized bone tissue lagen membranes.
jured cortical layer.56,57 Future studies (17.8% compared to 16.0%). Together, Reinforced membranes allow
in this area are certainly encouraged. the aforementioned literature shows the space maintenance by preventing
The concept of a regional accel- need for adequate blood supply and an- membrane collapse that may occur
eratory phenomenon was introduced giogenesis for bone regeneration to oc- from pressure of overlying tissues. A
several decades ago.58-61 Melcher and cur. Although, to date, no consensus has titanium mesh incorporated into the
Y6JAw== on 03/30/2023
Dryer62 also emphasized the impor- been established on the beneficial effect membrane also improves the strength
tance of the blood clot in healing of of cortical perforation. of the membrane and allows adaptabil-
bony defects. Several potential advan- ity to the shape of the osseous defect.
tages of decortication exist. Providing Jovanovic et al81 used a canine model
communication with marrow spaces SPACE CREATION/MAINTENANCE and compared 3 treatment groups in
may enhance revascularization. Growth Providing adequate space for bone terms of bone regeneration. Group 1
factors, such as platelet derived growth regeneration is a fundamental princi- had a titanium-reinforced membrane,
factor, and bone morphogenetic proteins ple of GBR. Space is needed to ensure group 2 had a standard expanded poly-
can be released to enhance periodontal the proliferation of bone forming cells tetrafluoroethylene membrane, and
regeneration63 and peri-implant bone while excluding unwanted epithelial group 3 was a control and had no
formation.64 Osteogenic cells important and connective tissue cells. For exam- membrane. A marked gain of alveolar
to bone healing can be derived from 3 ple, in areas of natural space mainte- bone volume, resulting in complete
main sources: the periosteum, en- nance, such as after the placement of supracrestal regeneration, was noted
dosteum, and undifferentiated pluripo- immediate implants, there is evidence in both expanded polytetrafluoroethyl-
tential mesenchymal cells. The marrow to suggest that the addition of bone ene groups (1.82 and 1.9 mm) com-
provides a rich source of these undiffer- grafting materials and membranes has pared to only 0.53 mm achieved in the
entiated cells that can be transformed no beneficial effect over no mem- control group. Several other studies
into osteoblasts and osteoclasts. In ad- brane/no graft control sites.50,72,73 A have compared the use of reinforced
dition, the perforations through the consensus has yet to be formed regard- nonresorbable and absorbable mem-
cortical bone provide a mechanical in- ing the need for the use of barrier branes using various bone grafting
terlock with the newly regenerated materials and/or bone grafts around materials.22,43,82-84 From the available
bone. It has even been suggested that immediately placed implants.74-78 It literature, it can be concluded that
the cortical plate may act as a temporary may be that assuming the critical when a significant volume of bone is
hindrance for access of desirable cells jumping distance has not been ex- required for implant placement, the
and tissue components from the marrow ceeded, the space formed between the use of reinforced membranes or addi-
because resorption of the cortical bone extraction socket and implant fixture tional bone grafts is more beneficial.
has to take place before access to bone provides an ideal environment for When higher amounts of bone re-
forming components is achieved.65 clot stabilization and subsequent generation are required, space making
Beneficial effects of regional ac- osteogenesis.79,80 with a barrier membrane is critical. As
celeratory phenomenon have been re- Various animal studies have mentioned previously, absorbable mem-
ported in several animal studies.52,66-68 proved that by excluding the epithe- branes have various beneficial proper-
Larger perforations have been associ- lium and connective tissue, a secluded ties. However, a major challenge of using
ated with a shorter time to obtain bone space is thereby created, allowing an absorbable membrane alone is mem-
fill but without any differences in the slowly migrating osteoblast cells to brane collapse that may be caused by
total amount of new bone formed.68 populate the wound, resulting in en- the overlying soft tissue pressure. Var-
Misch69 has advocated the use of both hanced bone formation.4,6,57 In a clin- ious techniques have been developed
buccal and lingual decortication to en- ical and histomorphometric study in a to overcome this challenge. Using
hance bony healing 2-10 times higher canine model, Oh et al31 used a beagle coronally advanced flaps, placing
than normal. However, conflicting re- dog model to compare the effects of 2 bone grafting materials under the
10 “PASS” PRINCIPLES FOR PREDICTABLE BONE REGENERATION
membrane, or using other methods of ing.84,87,93,94 It is understood that when mineralized bone allograft to augment
mechanical support such as screws, the initial blood clot formation and a horizontal ridge defect in conjunc-
pins, or internal membrane frame- wound stability, as well as initial im- tion with implant placement.
works have all been evaluated with plant stability, are achieved, a predict-
positive results.85,86 Several case re- able wound healing sequence will occur. Technique
ports and clinical studies were per- This sequence will ensure predictable • Baseline information analysis
formed in the early 1990s to develop a bone formation. The initial blood clot (Figs. 2A and 2B): A preoperative
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
predictable surgical protocol that is a rich source of cytokines (e.g., clinical and radiographic evalua-
would enable the maintenance of a interleukin-1, interleukin-8, tumor ne- tion is needed to assess the need
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
secluded space that could be occu- crosis factor), growth factors (e.g., plate- for bone augmentation during im-
pied by cells with an osteogenic let derived growth factor, insulin-like plant placement.
potential.2,46,51,84,87 growth factor, fibroblast growth factor), • Initial incision (Fig. 2C): An at-
Whether the use of bone graft ma- and signaling molecules that recruit tempt is always made to locate the
terial has any additional use other than clearing cells to the wound site. Platelet initial incision away from the de-
space maintenance is debatable. 88 derived growth factor in particular is a fect site so that closure is not
Mellonig et al83 reported results from potent mitogen and chemoattractant for directly over the defect site. Ver-
human cases in a delayed implant with neutrophils and monocytes.95 The blood tical releasing incisions, either fol-
simultaneous GBR technique. There clot serves as the precursor of initial lowing the mucogingival junction
were 3 treatment groups compared highly vascular granulation tissue. The or extending beyond mucogingival
(i.e., bioabsorbable membrane with granulation tissue is then the site of ini- junction, are used whenever indi-
decalcified freeze-dried bone allograft tial intramembranous bone formation cated. Mucogingival junction inci-
Y6JAw== on 03/30/2023
[DFDBA], expanded polytetrafluoro- and remodeling.51 sion is a beveled vertical incision
ethylene with DFDBA, and bioabsorb- In addition to clot stabilization, dropped toward the buccal aspect,
able membrane alone) in nonspace primary stability of the implant fixture with a wider base down to the
making buccal dehiscence type defects. is a key to successful regeneration and mucogingival junction. This inci-
Comparable percent of bone-to-implant long-term implant survival.96-98 The sion is continued along the mu-
contact and amount of new bone vol- lack of primary stability leads to cogingival junction until adequate
ume, both in height and width, were micromotion at the bone to implant visualization of the surgical site is
observed in both groups using DFDBA. interface, which leads to fibrous en- attained. The primary purpose of
However, the control membrane-only capsulation of the implant.99 Some this flap is to provide a wide base
group had a less favorable outcome, investigators have even advocated en- of blood supply and minimize the
which the investigators attributed to lack gaging 2 cortical layers whenever pos- scar tissue formation because the
of space making characteristics and sub- sible to enhance initial stability.100,101 scar formed is likely to be hidden
sequent membrane collapse.83 Resonance frequency analysis is a by the natural mucogingival junc-
Similar results were shown using novel method that may be used to as- tion. This effect is more predict-
a bioabsorbable membrane alone in a sess implant stability. In this tech- able to achieve in patients with a
monkey model,89 or using a Teflon nique, a transducer is attached to the wide band of keratinized gingiva.
(DuPont Co., Wilmington, DE) mem- implant fixture and excited over a de- • Reflection (Fig. 2D): A full thick-
brane alone in a rat model. 90 In fined frequency range. There are 2 ness mucoperiosteal flap is re-
contrast, when a stiff, dome-shaped factors that determine the resulting flected 2-3 mm beyond the
bioabsorbable membrane was used in resonance frequency measurement: margins of the defect. Traction is
a rabbit calvaria, no difference in the the degree of stability at the implant- then placed on the flap, and an
amount of regenerated bone was found bone interface and the level of the incision is made through the peri-
between the membrane alone group bone surrounding the transducer.102-106 osteum. The reflection is then
and the membrane with bone graft Using resonance frequency analysis, continued by blunt dissection,
group.91 The literature seems to suggest Meredith et al102 examined 56 im- creating a split thickness flap that
that the major role of bone grafting ma- plants during their first year of inser- can be repositioned tension free
terial is space creation/maintenance. tion in 9 patients. The resonance over the area to be treated, and
Osteogenic and/or osteoconductive frequency increased from 7473 to primary closure be obtained. Sev-
properties of various bone grafts may 7915 Hz on average after 8 months. eral periosteal scorings within the
also likely play a minor role. There were 2 implant failures (failure buccal alveolar mucosa are also
to integrate) characterized by lower performed to allow easy segmental
resonance frequency readings. How- flap advancement, without placing
STABILITY ever, its usage in detecting implant excessive tension on the flap base.
The role of a barrier membrane is stability during or following GBR re- Usually, each periosteal scoring al-
twofold. In addition to excluding un- mains to be addressed. lows 2-3-mm flap advancement.
wanted cells, it also acts to stabilize the • Débridement (Fig. 2E): Granula-
blood clot.56,57,84,87,91,92 The importance Clinical Case and Technique tion tissue is completely removed
of initial clot adhesion and wound sta- Fig. 2 illustrates the use of an absorb- to help stop bleeding and allow
bilization is critical in wound heal- able collagen membrane with human careful inspection of the defect.
IMPLANT DENTISTRY / VOLUME 15, NUMBER 1 2006 11
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
Y6JAw== on 03/30/2023
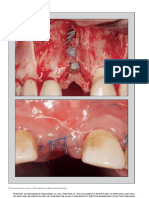
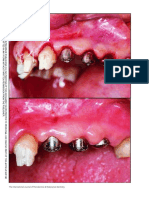
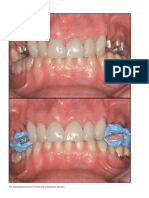
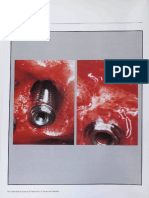
Fig. 2. Case No. 2. Augmentation of horizontal ridge defect in conjunction with implant placement. A, Preoperative view showing inadequate
ridge width and height. B, Presurgical radiograph illustrated potential apical lesion. C, Initial incisions depict 2 divergent vertical releasing
incisions. D, Surgical view showing ridge defects with granulomatous tissues. E, Area was débrided to the bare bone. F, Initial implant drill
following the surgical guide to indicate ideal buccolingual location. G, Implant placement with horizontal ridge deficiency. H, Intra-bone marrow
penetration using half-round bur. I, Sandwich bone augmentation. First layer of bone graft aimed at promoting better bone to implant contact
(human mineralized cancellous bone allograft, Puros; Zimmer Dental Inc.). J, Sandwich bone augmentation. Second layer of bone graft aimed
at creating/maintaining space (human mineralized bone cortical allograft, Puros) was used for barrier support and space creation, both
horizontally and vertically. K, Sandwich bone augmentation. Outer layer used for barrier support and space creation, both horizontally and
vertically (collagen membrane, BioMend Extend). L, Suture with 4-0 and 5-0 Vicryl suture (primary coverage with passive flap tension). M,
Four-week healing indicated uneventful healing. N, Reentry at 6 months showing new bone formation.
Implant drills were performed ac- defects associated with existing the margins of the defect in all
cording to manufacturer’s recom- implants, epithelium should be re- directions. Usually, the collagen
mended protocol. In addition, moved from the inner surface of membrane is hydrated in sterile
drilling was based upon the prefab- the flap using a sharp curette or saline or sterile water for 5-10
ricated surgical guides that consider diamond bur. The implant surface minutes before use, to improve
proper esthetic profile (Fig. 2F). should then be detoxified with ap- handling (malleability), however,
Fig. 2G shows implant placement propriate agents (e.g., 50 mg/mL this is not mandatory.
in a proper position with an obvious tetracycline for 3 minutes). • Fitting the flap: The flap is
horizontal ridge deficiency. • Fitting the membrane: Collagen checked and trimmed if necessary
• Removal of epithelium: Where membrane is trimmed and fitted to ensure that primary tension-
appropriate, as in treatment of so that it extends 2-3 mm beyond free closure is possible.
12 “PASS” PRINCIPLES FOR PREDICTABLE BONE REGENERATION
• Cortical perforations (Fig. 2H): cells, space maintenance/creation to tries. Int J Periodontics Restorative Dent.
Cortical perforations are made facilitate adequate space for bone in- 1997;17:292-299.
10. Zitzmann NU, Scharer P, Marinello
with a half-round bur to create growth, and stability of wound and
CP. Long-term results of implants treated
bleeding at the defect site and al- implant to induce blood clot formation with guided bone regeneration: A 5-year
low egress of progenitor cells. and uneventful healing events. This prospective study. Int J Oral Maxillofac Im-
• Bone replacement graft placement article has reviewed the biologic foun- plants. 2001;16:355-366.
(Figs. 2I and 2J): Graft material (e.g., dation that is essential for successful 11. Blanco J, Alonso A, Sanz M. Long-
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
mineralized bone allograft) is GBR. In addition, the technique in- term results and survival rate of implants
placed at the defect site to support volved in this principle was clearly treated with guided bone regeneration: A
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
5-year case series prospective study. Clin
the tented membrane. Tenting illustrated. Oral Implants Res. 2005;16:294-301.
screw(s) can also be used for this 12. Gher ME, Quintero G, Sandifer JB,
purpose, either alone or in con- Disclosure et al. Combined dental implant and guided
junction with graft material(s). The authors do not have any finan- tissue regeneration therapy in humans. Int
• Membrane placement (Fig. 2K): J Periodontics Restorative Dent. 1994;14:
cial interests, either directly or indi- 332-347.
The membrane is then adapted at rectly, in the products listed in the study.
the defect site. If the membrane is 13. Becker W, Becker BE. Flap de-
signs for minimization of recession adja-
stable, no attempt is made to fix cent to maxillary anterior implant sites:
it. However, if the membrane is ACKNOWLEDGMENTS A clinical study. Int J Oral Maxillofac
not stable, then pins, bone screws, This study was partially supported Implants. 1996;11:46-54.
or tacks may be needed to assist by the University of Michigan, Peri- 14. Fugazzotto PA. Maintenance of
the membrane stability. soft tissue closure following guided bone
Y6JAw== on 03/30/2023
odontal Graduate Student Research
• Closing (Fig. 2L): The surgical regeneration: Technical considerations
Fund. and report of 723 cases. J Periodontol.
site is closed with Vicryl (Ethi-
1999;70:1085-1097.
con, Inc., Johnson & Johnson, 15. Goldstein M, Boyan BD, Schwartz
Somerville, NJ), Teflon, or silk REFERENCES Z. The palatal advanced flap: A pedicle flap
suture with passive tension. 1. Nyman S, Karring T, Lindhe J, et al. for primary coverage of immediately
Healing following implantation of periodon- placed implants. Clin Oral Implants Res.
POSTOPERATIVE CARE titis-affected roots into gingival connective 2002;13:644-650.
tissue. J Clin Periodontol. 1980;7:394-401. 16. Lazzara RJ. Immediate implant
Antibiotic (e.g., Amoxicillin 2 2. Nyman S, Lang NP, Buser D, et al. placement into extraction sites: Surgical and
g/day for 10 days) can be prescribed Bone regeneration adjacent to titanium restorative advantages. Int J Periodontics
for the patient. The patient is placed dental implants using guided tissue Restorative Dent. 1989;9:332-343.
on warm saltwater rinses for the first regeneration: A report of two cases. Int 17. Dahlin C, Lekholm U, Becker W, et
J Oral Maxillofac Implants. 1990;5:9-14. al. Treatment of fenestration and dehis-
2-3 weeks to encourage normal flap 3. Karring T, Nyman S, Lindhe J. Heal- cence bone defects around oral implants
healing without disturbing migrating ing following implantation of periodontitis using the guided tissue regeneration
cells. Chlorhexidine gluconate 0.12% affected roots into bone tissue. J Clin Peri- technique: A prospective multicenter
(i.e., Peridex威; Zila Pharmaceuticals, odontol. 1980;7:96-105. study. Int J Oral Maxillofac Implants. 1995;
Inc., Phoenix, AZ)or Periogard威 4. Dahlin C, Sennerby L, Lekholm U, et 10:312-318.
(Colgate-Palmolive, New York, NY) al. Generation of new bone around tita- 18. Machtei EE. The effect of
mouthrinse will then be used for the nium implants using a membrane membrane exposure on the outcome of
technique: An experimental study in rab- regenerative procedures in humans: A
next 3 weeks to facilitate plaque con- bits. Int J Oral Maxillofac Implants. 1989;4: meta-analysis. J Periodontol. 2001;72:
trol. Sutures are removed at 10-14 19-25. 512-516.
days. The surgical site should be 5. Melcher AH. On the repair potential 19. Lekholm U, Becker W, Dahlin C, et
checked every 2 weeks for a period of of periodontal tissues. J Periodontol. 1976; al. The role of early versus late removal of
2 months (Fig. 2M). Final result is 47:256-260. GTAM membranes on bone formation at oral
usually assessed at the implant uncov- 6. Dahlin C, Linde A, Gottlow J, et al. implants placed into immediate extraction
Healing of bone defects by guided tissue sockets. An experimental study in dogs. Clin
ering, typically 4-6 months after initial
regeneration. Plast Reconstr Surg. 1988; Oral Implants Res. 1993;4:121-129.
surgery (Fig. 2N). 81:672-676. 20. Simion M, Baldoni M, Rossi P, et al.
7. Gelb DA. Immediate implant sur- A comparative study of the effectiveness of
CONCLUSIONS gery: Three-year retrospective evaluation e-PTFE membranes with and without early
of 50 consecutive cases. Int J Oral exposure during the healing period. Int J
GBR can be a very predictable Maxillofac Implants. 1993;8:388-399. Periodontics Restorative Dent. 1994;14:
treatment modality in the partially or 8. Buser D, Dula K, Lang NP, et al. 166-180.
fully edentulous implant patient. The Long-term stability of osseointegrated im- 21. Becker W, Dahlin C, Becker BE,
success of the technique is based on plants in bone regenerated with the et al. The use of e-PTFE barrier mem-
several biologically supported princi- membrane technique. 5-year results of a branes for bone promotion around tita-
ples, such as PASS: primary wound prospective study with 12 implants. Clin nium implants placed into extraction
Oral Implants Res. 1996;7:175-183. sockets: A prospective multicenter study. Int
closure to ensure undisturbed and un- 9. Fugazzotto PA, Shanaman R, Ma- J Oral Maxillofac Implants. 1994;9:31-40.
interrupted wound healing, angiogen- nos T, et al. Guided bone regeneration 22. Zitzmann NU, Naef R, Scharer P.
esis to provide necessary blood supply around titanium implants: Report of the Resorbable versus nonresorbable mem-
and undifferentiated mesenchymal treatment of 1,503 sites with clinical reen- branes in combination with Bio-Oss for
IMPLANT DENTISTRY / VOLUME 15, NUMBER 1 2006 13
guided bone regeneration. Int J Oral Max- 36. Steinberg AD, LeBreton G, Willey procedures. Clinical evaluation of 26 con-
illofac Implants. 1997;12:844-852. R, et al. Extravascular clot formation and secutive cases. Clin Oral Implants Res.
23. Lim SC, Lee MJ, Yeo HH. Effects of platelet activation on variously treated root 2000;11:83-90.
various implant materials on regeneration surfaces. J Periodontol. 1986;57:516-522. 51. Schenk RK, Buser D, Hardwick
of calvarial defects in rats. Pathol Int. 2000; 37. Postlethwaite AE, Seyer JM, Kang WR, et al. Healing pattern of bone regen-
50:594-602. AH. Chemotactic attraction of human fi- eration in membrane-protected defects: A
24. Lima LA, Fuchs-Wehrle AM, Lang broblasts to type I, II, and III collagens and histologic study in the canine mandible. Int
NP, et al. Surface characteristics of im- collagen-derived peptides. Proc Natl Acad J Oral Maxillofac Implants. 1994;9:13-29.
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
plants influence their bone integration after Sci U S A. 1978;75:871-875. 52. Schmid J, Wallkamm B, Hammerle
simultaneous placement of implant and 38. Wang HL, O’Neal RB, Thomas CL, CH, et al. The significance of angiogenesis
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
GBR membrane. Clin Oral Implants Res. et al. Evaluation of an absorbable collagen in guided bone regeneration. A case report
2003;14:669-679. membrane in treating class II furcation de- of a rabbit experiment. Clin Oral Implants
25. Mombelli A, Lang NP, Nyman S. fects. J Periodontol. 1994;65:1029-1036. Res. 1997;8:244-248.
Isolation of periodontal species after 39. Wang HL, MacNeil RL. Guided tis- 53. Hammerle CH, Schmid J, Olah AJ,
guided tissue regeneration. J Periodontol. sue regeneration. Absorbable barriers. et al. Osseous healing of experimentally
1993;64:1171-1175. Dent Clin North Am. 1998;42:505-522. created defects in the calvaria of rabbits
26. Simion M, Trisi P, Maglione M, et al. 40. Chen CC, Wang HL, Smith F, et al. using guided bone regeneration. A pilot
A preliminary report on a method for study- Evaluation of a collagen membrane with study. Clin Oral Implants Res. 1992;3:144-
ing the permeability of expanded polytetra- and without bone grafts in treating peri- 147.
fluoroethylene membrane to bacteria in odontal Intrabony defects. J Periodontol. 54. Winet H. The role of microvascula-
vitro: A scanning electron microscopic and 1995;66:838-847. ture in normal and perturbed bone healing
histological study. J Periodontol. 1994;65: 41. Wang HL, O’Neal RB, MacNeil LM. as revealed by intravital microscopy. Bone.
755-761. Regenerative treatment of periodontal de- 1996;19:39S-57S.
27. Nowzari H, London R, Slots J. The fects utilizing a bioresorbable collagen 55. Hammerle CH, Schmid J, Olah AJ,
Y6JAw== on 03/30/2023
importance of periodontal pathogens in membrane. Pract Periodontics Aesthet et al. A novel model system for the study of
guided periodontal tissue regeneration and Dent 1995;7:59-66. experimental guided bone formation in hu-
guided bone regeneration. Compend Con- 42. Bunyaratavej P, Wang HL. Colla- mans. Clin Oral Implants Res. 1996;7:
tin Educ Dent. 1995a;16:1042-1046. gen membranes: A review. J Periodontol. 38-47.
28. Nowzari H, Matian F, Slots J. Peri- 2001;72:215-229. 56. Kostopoulos L, Karring T, Uraguchi
odontal pathogens on polytetrafluoroethylene 43. Simion M, Scarano A, Gionso L, et R. Formation of jawbone tuberosities by
membrane for guided tissue regeneration al. Guided bone regeneration using resorb- guided tissue regeneration. An experimen-
inhibit healing. J Clin Periodontol. 1995b; able and nonresorbable membranes: A tal study in the rat. Clin Oral Implants Res.
22:469-474. comparative histologic study in humans. Int 1994;5:245-253.
29. Jovanovic SA, Spiekermann H, J Oral Maxillofac Implants. 1996;11:735- 57. Kostopoulos L, Karring T. Aug-
Richter EJ. Bone regeneration around tita- 742. mentation of the rat mandible using guided
nium dental implants in dehisced defect 44. Simion M, Misitano U, Gionso L, et tissue regeneration. Clin Oral Implants
sites: A clinical study. Int J Oral Maxillofac al. Treatment of dehiscences and fenestra- Res. 1994;5:75-82.
Implants. 1992;7:233-245. tions around dental implants using resorb- 58. Frost HM. The regional accelera-
30. Celletti R, Davarpanah M, Etienne able and nonresorbable membranes tory phenomenon: A review. Henry Ford
D, et al. Guided tissue regeneration around associated with bone autografts: A com- Hosp Med J. 1983;31:3-9.
dental implants in immediate extraction parative clinical study. Int J Oral Maxillofac 59. Shih MS, Norrdin RW. Regional ac-
sockets: Comparison of e-PTFE and a new Implants. 1997;12:159-167. celeration of remodeling during healing of
titanium membrane. Int J Periodontics Re- 45. Hammerle CH, Lang NP. Single bone defects in beagles of various ages.
storative Dent. 1994;14:242-253. stage surgery combining transmucosal im- Bone. 1985;6:377-379.
31. Oh TJ, Meraw SJ, Lee EJ, et al. plant placement with guided bone regen- 60. Frost HM. The biology of fracture
Comparative analysis of collagen mem- eration and bioresorbable materials. Clin healing. An overview for clinicians. Part I.
branes for the treatment of implant dehis- Oral Implants Res. 2001;12:9-18. Clin Orthop Relat Res. 1989;248:283-293.
cence defects. Clin Oral Implants Res. 46. Buser D, Dula K, Belser U, et al. 61. Frost HM. The biology of fracture
2003;14:80-90. Localized ridge augmentation using healing. An overview for clinicians. Part II.
32. Haas R, Baron M, Dortbudak O, et guided bone regeneration. 1. Surgical pro- Clin Orthop Relat Res. 1989;248:294-309.
al. Lethal photosensitization, autogenous cedure in the maxilla. Int J Periodontics 62. Melcher AH, Dryer CJ. Protection
bone, and e-PTFE membrane for the treat- Restorative Dent. 1993;13:29-45. of the blood clot in healing of circum-
ment of peri-implantitis: Preliminary re- 47. Buser D, Dula K, Belser UC, et al. scribed bone defects. J Bone Joint Surg.
sults. Int J Oral Maxillofac Implants. 2000; Localized ridge augmentation using 1962;44B:424-429.
15:374-382. guided bone regeneration. II. Surgical pro- 63. Giannobile WV, Ryan S, Shih MS,
33. Locci P, Calvitti M, Belcastro S, et cedure in the mandible. Int J Periodontics et al. Recombinant human osteogenic
al. Phenotype expression of gingival fibro- Restorative Dent. 1995;15:10-29. protein-1 (OP-1) stimulates periodontal
blasts cultured on membranes used in 48. Becker W, Becker BE. Guided tis- wound healing in class III furcation defects.
guided tissue regeneration. J Periodontol. sue regeneration for implants placed into J Periodontol. 1998;69:129-137.
1997;68:857-863. extraction sockets and for implant 64. Fiorellini JP, Buser D, Riley E, et al.
34. Takata T, Wang HL, Miyauchi M. dehiscences: Surgical techniques and Effect on bone healing of bone morphoge-
Migration of osteoblastic cells on various case report. Int J Periodontics Restorative netic protein placed in combination with
guided bone regeneration membranes. Dent. 1990;10:376-391. endosseous implants: A pilot study in bea-
Clin Oral Implants Res. 2001;12:332-338. 49. Tinti C, Parma-Benfenati S. Coro- gle dogs. Int J Periodontics Restorative
35. Wang HL, Miyauchi M, Takata T. nally positioned palatal sliding flap. Int J Dent. 2001;21:41-47.
Initial attachment of osteoblasts to various Periodontics Restorative Dent. 1995;15: 65. Lundgren AK, Lundgren D, Ham-
guided bone regeneration membranes: An 298-310. merle CH, et al. Influence of decortication
in vitro study. J Periodontal Res. 2002;37: 50. Nemcovsky CE, Artzi Z, Moses O. of the donor bone on guided bone aug-
340-344. Rotated palatal flap in immediate implant mentation. An experimental study in the
14 “PASS” PRINCIPLES FOR PREDICTABLE BONE REGENERATION
rabbit skull bone. Clin Oral Implants Res. eds. Proceedings of the 3rd European 91. Wallkamm B, Schmid J, Hammerle
2000;11:99-106. Workshop on Periodontology (Berlin). Im- CH, et al. Effect of bioresorbable fibers
66. Biewer B, Vanheusden A, Rompen plant Dent. 1999;1:520-534. (Polyfibre) and a bioresorbable foam (Poly-
EH. In vivo study of enhancing factors for 79. Cornelini R, Scarano A, Covani U, foam) on new bone formation. A short term
guided bone formation. Paper presented at: et al. Immediate one-stage postextraction experimental study on the rabbit skull. Clin
European Society of Periodontology; May implant: A human clinical and histologic Oral Implants Res. 2003;14:734-742.
15-17, 1997; Florence, Italy. Abstract 97. case report. Int J Oral Maxillofac Implants. 92. Weng D, Hurzeler MB, Quinones
67. Rompen EH, Biewer R, Vanheus- 2000;15:432-437. CR, et al. Contribution of the periosteum to
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
den A, et al. The influence of cortical per- 80. Paolantonio M, Dolci M, Scarano bone formation in guided bone regenera-
forations and of space filling with peripheral A, et al. Immediate implantation in fresh tion. A study in monkeys. Clin Oral Im-
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
blood on the kinetics of guided bone gen- extraction sockets. A controlled clinical plants Res. 2000;11:546-554.
eration. A comparative histometric study in and histological study in man. J Periodon- 93. Wikesjo UM, Nilveus RE, Selvig KA.
the rat. Clin Oral Implants Res. 1999;10: tol. 2001;72:1560-1571. Significance of early healing events on peri-
85-94. 81. Jovanovic SA, Schenk RK, Orsini odontal repair: A review. J Periodontol.
68. Nishimura I, Shimizu Y, Ooya K. M, et al. Supracrestal bone formation 1992;63:158-165.
Effects of cortical bone perforation on around dental implants: An experimental 94. Haney JM, Nilveus RE, McMillan
experimental guided bone regeneration. dog study. Int J Oral Maxillofac Implants. PJ, et al. Periodontal repair in dogs: Ex-
Clin Oral Implants Res. 2004;15:293-300. 1995;10:23-31. panded polytetrafluoroethylene barrier
69. Misch CE. Bone augmentation for 82. Mellonig JT, Nevins M, Sanchez R. membranes support wound stabilization
implant placement: Keys to bone grafting. Evaluation of a bioabsorbable physical and enhance bone regeneration. J Peri-
In: Misch CE, ed. Contemporary Implant barrier for guided bone regeneration. Part odontol. 1993;64:883-890.
Dentistry. 2nd ed. St. Louis, MO: Mosby; I. Material alone. Int J Periodontics Restor- 95. Anusaksathien O, Giannobile WV.
1999:462. ative Dent. 1998;18:139-149. Growth factor delivery to re-engineer peri-
70. Slotte C, Lundgren D. Impact of 83. Mellonig JT, Nevins M, Sanchez R. odontal tissues. Curr Pharm Biotechnol.
Y6JAw== on 03/30/2023
cortical perforations of contiguous donor Evaluation of a bioabsorbable physical 2002;3:129-139.
bone in a guided bone augmentation barrier for guided bone regeneration. Part 96. Romanos G, Toh CG, Siar CH, et
procedure: An experimental study in the II. Material and a bone replacement graft. al. Peri-implant bone reactions to immedi-
rabbit skull. Clin Implant Dent Relat Res. Int J Periodontics Restorative Dent. 1998; ately loaded implants. An experimental
2002;4:1-10. 18:129-137. study in monkeys. J Periodontol. 2001;72:
71. Slotte C, Lundgren D, Sennerby L. 84. Wang H-L, Carroll J. Utilizing ab- 506-511.
Bone morphology and vascularization of sorbable collagen membranes for guided 97. Becker W, Sennerby L, Bedrossian
untreated and guided bone augmentation- tissue regeneration, guided bone regener- E, et al. Implant stability measurements for
treated rabbit calvaria: Evaluation of an ation, and in the treatment of gingival implants placed at the time of extraction: A
augmentation model. Clin Oral Implants recession. Compendium. 2000;21:399- cohort, prospective clinical trial. J Peri-
Res. 2005;16:228-235. 414. odontol. 2005;76:391-397.
72. Covani U, Bortolaia C, Barone A, et 85. Stentz WC, Mealey BL, Nummiko- 98. Degidi M, Piattelli A. 7-year
al. Bucco-lingual crestal bone changes af- ski PV, et al. Effects of guided bone regen- follow-up of 93 immediately loaded tita-
ter immediate and delayed implant place- eration around commercially pure titanium nium dental implants. J Oral Implantol.
ment. J Periodontol. 2004;75:1605-1612. and hydroxyapatite-coated dental im- 2005;31:25-31.
73. Chen ST, Darby IB, Adams GG, et plants. I. Radiographic analysis. J Peri- 99. Brunski JB, Moccia AF Jr, Pollack
al. A prospective clinical study of bone odontol. 1997;68:199-208. SR, et al. The influence of functional use of
augmentation techniques at immediate im- 86. Stentz WC, Mealey BL, Gunsolley endosseous dental implants on the tissue-
plants. Clin Oral Implants Res. 2005;16: JC, et al. Effects of guided bone regener- implant interface. I. Histological aspects.
176-184. ation around commercially pure titanium J Dent Res. 1979;58:1953-1969.
74. Lang NP, Bragger U, Hammerle and hydroxyapatite-coated dental im- 100. Ivanoff CJ, Sennerby L, Lekholm
CH, et al. Immediate transmucosal im- plants. II. Histologic analysis. J Periodon- U. Influence of soft tissue contamination on
plants using the principle of guided tissue tol. 1997;68:933-949. the integration of titanium implants. An ex-
regeneration. I. Rationale, clinical proce- 87. Wang H-L, Misch C, Neiva RF. perimental study in rabbits. Clin Oral Im-
dures and 30-month results. Clin Oral Im- Sandwich bone augmentation technique: plants Res. 1996;7:128-132.
plants Res. 1994;5:154-163. Rationale and report of pilot cases. Int J 101. Ivanoff CJ, Sennerby L, Lekholm
75. Schwartz-Arad D, Chaushu G. Periodontics Restorative Dent. 2004;24: U. Influence of initial implant mobility on the
Placement of implants into fresh extraction 232-245. integration of titanium implants. An exper-
sites: 4 to 7 years retrospective evaluation 88. Polimeni G, Koo KT, Qahash M, et imental study in rabbits. Clin Oral Implants
of 95 immediate implants. J Periodontol. al. Prognostic factors for alveolar Res. 1996;7:120-127.
1997;68:1110-1116. regeneration: Effect of a space-providing 102. Meredith N, Alleyne D, Cawley P.
76. Schwartz-Arad D, Chaushu G. The biomaterial on guided tissue regeneration. Quantitative determination of the stability
ways and wherefores of immediate place- J Clin Periodontol. 2004;31:725-729. of the implant-tissue interface using reso-
ment of implants into fresh extraction sites: 89. Hurzeler MB, Kohal RJ, Naghsh- nance frequency analysis. Clin Oral Im-
A literature review. J Periodontol. 1997;68: bandi J, et al. Evaluation of a new plants Res. 1996;7:261-267.
915-923. bioresorbable barrier to facilitate guided 103. Meredith N, Shagaldi F, Alleyne D,
77. Kohal RJ, Mellas P, Hurzeler MB, et bone regeneration around exposed im- et al. The application of resonance fre-
al. The effects of guided bone regeneration plant threads. An experimental study in the quency measurements to study the stabil-
and grafting on implants placed into imme- monkey. Int J Oral Maxillofac Surg. 1998; ity of titanium implants during healing in the
diate extraction sockets. An experimental 27:315-320. rabbit tibia. Clin Oral Implants Res. 1997;
study in dogs. J Periodontol. 1998;69: 90. Mardas N, Kostopoulos L, Stavro- 8:234-243.
927-937. poulos A, et al. Osteogenesis by guided 104. Meredith N, Book K, Friberg B, et
78. Mayfield LJA. Immediate, delayed tissue regeneration and demineralized al. Resonance frequency measurements
and late submerged and transmucosal im- bone matrix. J Clin Periodontol. 2003;30: of implant stability in vivo. A cross-
plants. In: Lang NP, Karring T, Lindhe J, 176-183. sectional and longitudinal study of reso-
IMPLANT DENTISTRY / VOLUME 15, NUMBER 1 2006 15
nance frequency measurements on analysis study. Int J Oral Maxillofac Surg.
implants in the edentulous and partially 1999;28:266-272.
dentate maxilla. Clin Oral Implants Res.
1997;8:226-233. Reprint requests and correspondence to:
105. Friberg B, Sennerby L, Meredith Hom-Lay Wang, DDS, MSD
N, et al. A comparison between cutting Professor and Director of Graduate
torque and resonance frequency measure- Periodontics
ments of maxillary implants. A 20-month Department of Periodontics and Oral Medicine
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
clinical study. Int J Oral Maxillofac Surg. University of Michigan School of Dentistry
1999;28:297-303.
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
1011 North University Avenue
106. Friberg B, Sennerby L, Linden B, Ann Arbor, MI 48109-1078
et al. Stability measurements of one-stage Tel: (734) 763-3383
Brånemark implants during healing in man- Fax: (734) 936-0374
dibles. A clinical resonance frequency E-mail: homlay@umich.edu
Abstract Translations [German, Spanish, Portugese, Japanese]
Y6JAw== on 03/30/2023
AUTOR(EN): Hom-Lay Wang, DDS, MSD*, “PASS”-Prinzipien für eine vorhersagbar erfolgreiche Knochengewebsregeneration
Lakshmi Boyapati, BDS**. *Professor und
Leiter des Graduiertenkollegs für Orthodon- ABSTRACT: Die geleitete Knochengewebswiederherstellung stellt eine eingeführte
tie, Abteilung für Orthodontie und Oralmedi- Methode zur Anreicherung unzureichender Alveolarleisten dar. Eine vorhersagbare gute
zin, zahnmedizinische Fakultät, Universität Regeneration bedarf sowohl der groen technischen Fähigkeiten wie auch eines pro-
von Michigan, Ann Arbot, MI, USA. **Assis- funden Kenntnisstandes bezüglich der einer erfolgreichen Wundheilung zu Grunde lieg-
tenzarzt, Abteilung für Orthodontie und enden Prinzipien. Die vorliegende Arbeit beschreibt die vier wesentlichen biologischen
Oralmedizin, zahnmedizinische Fakultät, Uni- Prinzipien (d.h. PASS), die für eine vorhersagbar gute Knochenregeneration erforderlich
versität von Michigan, Ann Arbot, MI, USA. sind. Hierzu gehören: der primäre Wundverschluss zur Gewährleistung einer ungestörten
Schriftverkehr: Dr. Hom-Lay Wang, Professor und ununterbrochenen Wundheilung; Gefäbildung zur Bereitstellung eines aus-
und Leiter des Graduiertenkollegs für Orth- reichenden Blutzuflusses sowie unveränderte Mesenchymalzellen; Raumerhaltung oder
odontie (Professor and Director of Graduate -schaffung, um den entsprechenden Platz für Neuknochenbildung bereit zu stellen; und
Periodontics), Abteilung für Orthodontie und Wund- sowie Implantatstabilität zur Vermeidung von Blutgerinnselbildung und unerwün-
Oralmedizin (Department of Periodontics and schten Begleiterscheinungen bei der Heilung. Auerdem werden in der Abhandlung eine
Oral Medicine), zahnmedizinische Fakultät neuartige Lappenkonstruktion sowie klinische Fälle, die dieses Prinzip praktisch zur
der Universität von Michigan (University of Anwendung gebracht haben, vorgestellt.
Michigan School of Dentistry), 1011 North
University Avenue, Ann Arbor, Michigan SCHLÜSSELWÖRTER: Geleitete Knochengewebswiederherstellung, Knochentrans-
48109-1078, USA. Telefon: (734) 763-3383, plantat, horizontale Knochengewebsanreicherung, Implantate
Fax: (734) 936-0374. eMail: homlay@umich.
edu
AUTOR(ES): Hom-Lay Wang, DDS, MSD*, Los principios “PASS” para la regeneración pronosticable del hueso
Lakshmi Boyapati, BDS**. *Profesor y Direc-
tor de Periodóntica Graduada, Departamento ABSTRACTO: La regeneración guiada del hueso es una técnica bien establecida para
de Periodóntica y Medicina Oral, Facultad de aumentar crestas alveolares deficientes. La regeneración pronosticable requiere un alto
Odontologı́a, Universidad de Michigan, Ann Ar- nivel de aptitud técnica y un completo entendimiento de los principios de curación de una
bor, MI, EE.UU. **Residente, Departamento de herida. Esta manuscrito describe los cuatro principios biológicos principales (PASS)
Periodóntica y Medicina Oral, Facultad de Od- necesarios para la regeneración pronosticable del hueso; cierre de la herida principal para
ontologı́a, Universidad de Michigan, Ann Arbor, asegurar una curación de la herida sin problemas y sin interrupciones; angiogénesis para
MI, EE.UU. Correspondencia a: Dr. Hom-Lay proporcionar el suministro necesario de sangre y células mesenquimales indiferenciadas;
Wang, Professor and Director of Graduate Pe- mantenimiento/creación del espacio para facilitar un espacio adecuado para el crecimiento
riodontics, Departament of Periodontics and del hueso; y estabilidad para la herida y el implante para inducir la formación de un
Oral Medicine, University of Michigan School of coágulo sanguı́neo y una curación sin dificultades. Además, se presentan un diseño nuevo de
Dentistry, 1011 North University Avenue, Ann la aleta y casos clı́nicos que utilizan este principio.
Arbor, MI 48109-1078, U.S.A. Teléfono: (734)
763-3383 Fax: (734) 936-0374. Dirección PALABRAS CLAVES: GBR; regeneración guiada del hueso; injertos de hueso; aumento
electrónica: horizontal del hueso, implantes.
16 “PASS” PRINCIPLES FOR PREDICTABLE BONE REGENERATION
AUTOR(ES): Hom-Lay Wang, Cirurgião- Princı́pios “PASS” para Regeneração Óssea Previsı́vel
Dentista, Doutor em Odontologia*, Lakshmi
Boyapati, Bacharel em Odontologia**. *Pro- RESUMO: A Regeneração Óssea Guiada é uma técnica consagrada usada para aumento
fessor e Diretor de Periodontia Graduada, de rebordos alveolares deficientes. A regeneração previsı́vel exige tanto um alto nı́vel de
Departamento de Periodontia e Medicina habilidade técnica quanto um entendimento completo dos princı́pios subjacentes da cura
Oral, Faculdade de Odontologia, Univer- de feridas. Este manuscrito descreve os quatro princı́pios biológicos principais (i.e.,
sidade de Michigan, Ann Arbor, MI, EUA. PASS) necessários para a regeneração óssea previsı́vel: Fechamento primário da ferida
**Residente, Departamento de Periodontia e para assegurar a cura tranqüila e ininterrupta de feridas; Angiogênese para fornecer
JwVa93F9JHuZpY16WP/IWpKuyjFAAey9CrMG8PzRJD3Io/V098jj3cPUFsLN2GvVxggw/O/eTcQclC58kVBbkXOs3QbUXOCxxpH4
Medicina Oral, Faculdade de Odontologia, suprimento necessário de sangue e células mesenquimais indiferenciadas; Manutenção/
Universidade de Michigan, Ann Arbor, MI, criação de espaço para facilitar espaço adequado para crescimento para dentro do osso; e
Downloaded from http://journals.lww.com/implantdent by bZsZQaOAP7HH4caWlYQDTgZ529buIBmoVjGMgGSjk5sGU
EUA.Correspondência para: Dr. Hom-Lay estabilidade de ferida e implante para induzir a formação de coágulo sangüı́neo e eventos
Wang, Professor and Director of Graduate de cura tranqüilos. Além disso, um original design de borda e casos clı́nicos que utilizam
Periodontics, Department of Periodontics and este princı́pio são apresentados.
Oral Medicine, University of Michigan School
of Dentistry, 1011 North University Avenue, PALAVRAS-CHAVE: GBR; Regeneração óssea guiada; enxertos ósseos; aumento hor-
Ann Arbor, Michigan 48109-1078, USA. Tele- izontal do osso; implantes.
fone: (734) 763-3383, Fax: (734) 936-0374.
E-mail: homlay@umich.edu
Y6JAw== on 03/30/2023
IMPLANT DENTISTRY / VOLUME 15, NUMBER 1 2006 17
You might also like
- PASS Principles For Predictable Bone.8Document10 pagesPASS Principles For Predictable Bone.8medNo ratings yet
- PASS Principles For Predictable Bone.8Document10 pagesPASS Principles For Predictable Bone.8Alex Martins AlbaneseNo ratings yet
- Principles For Vertical Ridge Augmentation 2017Document8 pagesPrinciples For Vertical Ridge Augmentation 2017marlene tamayoNo ratings yet
- Principles For Vertical Ridge Augmentation in The Atrophic Posterior Mandible - A Technical Review - Urban2017Document8 pagesPrinciples For Vertical Ridge Augmentation in The Atrophic Posterior Mandible - A Technical Review - Urban2017Claudio GuzmanNo ratings yet
- 04 Fixation of Soft Tissue To Bone TechniquesDocument13 pages04 Fixation of Soft Tissue To Bone TechniqueskenthepaNo ratings yet
- Jaaos D 1Document10 pagesJaaos D 1Mohan DesaiNo ratings yet
- Functional and Radiological Outcomes of Impaction Grafts and Cemented Cup For The Treatment of Acetabular Bone Deficiency 2022Document7 pagesFunctional and Radiological Outcomes of Impaction Grafts and Cemented Cup For The Treatment of Acetabular Bone Deficiency 2022abass elananiNo ratings yet
- Controversiesin Traditionaloraland MaxillofacialreconstructionDocument13 pagesControversiesin Traditionaloraland MaxillofacialreconstructionSheetal HNo ratings yet
- Urban 2016 Técnica de La SalchichaDocument8 pagesUrban 2016 Técnica de La SalchichaLukas Lopez RamirezNo ratings yet
- 10 11607@prd 00 0454Document8 pages10 11607@prd 00 0454Alejandro FereñoNo ratings yet
- Petersons Principles of Oral and Maxillofacial Surgery 2nd Ed 2004 (PDF - Io)Document115 pagesPetersons Principles of Oral and Maxillofacial Surgery 2nd Ed 2004 (PDF - Io)Edgar RenèNo ratings yet
- Soft Tisue Management ImplantologyDocument18 pagesSoft Tisue Management ImplantologyAlex DaniciNo ratings yet
- The International Journal of Periodontics & Restorative DentistryDocument8 pagesThe International Journal of Periodontics & Restorative DentistrySeptimiu TiplicaNo ratings yet
- Bone Grafts Oh Dec 2015Document15 pagesBone Grafts Oh Dec 2015د.محمد مليحةNo ratings yet
- Protected: Computer-Aided Surgery in Orthopedics: From Strength To StrengthDocument2 pagesProtected: Computer-Aided Surgery in Orthopedics: From Strength To Strengthlaine03_tntNo ratings yet
- 2003 Most Et AlDocument11 pages2003 Most Et AlGERARDO TORRES RUIZNo ratings yet
- Tissue Engineering Solutions For Tendon Repair: Review ArticleDocument9 pagesTissue Engineering Solutions For Tendon Repair: Review ArticleJay ChaNo ratings yet
- Seminar: Course Instructor-Prof Dr. S. DharaDocument14 pagesSeminar: Course Instructor-Prof Dr. S. Dharaskycall28No ratings yet
- Successful Treatment of Full Thickness Frontal Skull Bone Defect With Dermal Fat Grafting and Artificial Bone GraftsDocument5 pagesSuccessful Treatment of Full Thickness Frontal Skull Bone Defect With Dermal Fat Grafting and Artificial Bone GraftsDeevish N DinakarNo ratings yet
- Steigenga 2003 - Dental Implant Design and Its RelationshipDocument12 pagesSteigenga 2003 - Dental Implant Design and Its RelationshipZhiyi LinNo ratings yet
- Skeletal System Concept MapDocument1 pageSkeletal System Concept MapkacchanNo ratings yet
- PIARDocument33 pagesPIARAndrea CanosaNo ratings yet
- 07 Gracis-Occlusion1Document12 pages07 Gracis-Occlusion1ValentinaNo ratings yet
- Current Concepts in The Rehabilitation Following Articular Cartilage Repair Procedures in The KneeDocument21 pagesCurrent Concepts in The Rehabilitation Following Articular Cartilage Repair Procedures in The KneeMario Peraza MurilloNo ratings yet
- Inferior Alveolar Neurovascular Bundle Repositioning: A Retrospective AnalysisDocument6 pagesInferior Alveolar Neurovascular Bundle Repositioning: A Retrospective Analysisr1comfupchNo ratings yet
- Guided Bone Regeneration of An Atrophic Mandible With A Heterologous Bone BlockDocument6 pagesGuided Bone Regeneration of An Atrophic Mandible With A Heterologous Bone BlockGabriela Marie CruzNo ratings yet
- Bone Augmentation TechniquesDocument20 pagesBone Augmentation TechniquesGabriela Ciornei100% (1)
- Hebert Davies2020Document7 pagesHebert Davies2020DavidNo ratings yet
- ET 4. - Iatrogenic - Segmental - Defect - How - I - Debride.3. JOT 2017Document7 pagesET 4. - Iatrogenic - Segmental - Defect - How - I - Debride.3. JOT 2017Enrique Morales MiguelNo ratings yet
- Bracing After ACL Reconstruction: A Systematic ReviewDocument7 pagesBracing After ACL Reconstruction: A Systematic ReviewDanar AdhimuktiNo ratings yet
- 12 0001736 Rev A - Knee - Truliant Porous Design Rationale - WebDocument12 pages12 0001736 Rev A - Knee - Truliant Porous Design Rationale - WebValaMelkorNo ratings yet
- Highly Purified Human Mesenchymal Stem Cells: - Rapidly Expanding CelDocument2 pagesHighly Purified Human Mesenchymal Stem Cells: - Rapidly Expanding CelAbhishekNo ratings yet
- Model-Based Guided Implant Surgery Planned PrecisionDocument6 pagesModel-Based Guided Implant Surgery Planned PrecisionHugoMoralesTecnicoDentalNo ratings yet
- Brun Svold 1993Document12 pagesBrun Svold 1993Marihana ValdezNo ratings yet
- Kutkut 2011 Sinus WidthDocument5 pagesKutkut 2011 Sinus WidthLamis MagdyNo ratings yet
- Esse Aqui.1.7Document7 pagesEsse Aqui.1.7Yuri SmithNo ratings yet
- Esse AquiDocument20 pagesEsse AquiYuri SmithNo ratings yet
- 2020 Incidence of Fistula Formation and Velopharyngeal Insufficiency in Early Versus Standard Cleft Palate RepairDocument3 pages2020 Incidence of Fistula Formation and Velopharyngeal Insufficiency in Early Versus Standard Cleft Palate RepairDimitris RodriguezNo ratings yet
- The Keyhole Access Expansion Technique For FlaplesDocument6 pagesThe Keyhole Access Expansion Technique For FlaplesKyoko CPNo ratings yet
- Can Bone Compaction Improve Primary ImplantDocument14 pagesCan Bone Compaction Improve Primary ImplantdentureNo ratings yet
- Thr-Impaction BG FemurDocument5 pagesThr-Impaction BG FemurMohan DesaiNo ratings yet
- Osseodensification in Implant Dentistry A.12Document7 pagesOsseodensification in Implant Dentistry A.12MilindNo ratings yet
- Guided Tissue Regeneration: A Review: Journal of Dental Health Oral Disorders & TherapyDocument7 pagesGuided Tissue Regeneration: A Review: Journal of Dental Health Oral Disorders & TherapyLouis HutahaeanNo ratings yet
- Influence of Implant Length and Associated Parameters Upon Biomechanical Forces in Finite Element Analyses - A Systematic Review. Implant Dent, 2019Document10 pagesInfluence of Implant Length and Associated Parameters Upon Biomechanical Forces in Finite Element Analyses - A Systematic Review. Implant Dent, 2019Marlene Kasumi Gantier TakanoNo ratings yet
- Biopsy - An OverviewDocument9 pagesBiopsy - An OverviewNadya AyuNo ratings yet
- Horizontal and Vertical Ridge Augmentation in Localized Alveolar Deficient Sites - A Retrospective Case Series PDFDocument11 pagesHorizontal and Vertical Ridge Augmentation in Localized Alveolar Deficient Sites - A Retrospective Case Series PDFLedir Luciana Henley de AndradeNo ratings yet
- Guided Bone RegenerationDocument4 pagesGuided Bone Regenerationahmad955mlsNo ratings yet
- Talus Fractures Evaluation and Treatment.2Document10 pagesTalus Fractures Evaluation and Treatment.2angelluis1980No ratings yet
- Functional Recovery Following Traumatic Spinal Cord Injury Mediated by A Unique Polymer Scaffold Seeded With Neural Stem CellsDocument6 pagesFunctional Recovery Following Traumatic Spinal Cord Injury Mediated by A Unique Polymer Scaffold Seeded With Neural Stem CellsPandhu HarlanNo ratings yet
- October2006 CC HeckmannDocument20 pagesOctober2006 CC HeckmannMaría José Luengo SepúlvedaNo ratings yet
- Making Occlusion 2Document7 pagesMaking Occlusion 2Ali QawasNo ratings yet
- Subperiostial Minimally Invasive Aesthetic Ridge Augmentation Technique (SMART)Document10 pagesSubperiostial Minimally Invasive Aesthetic Ridge Augmentation Technique (SMART)Pat TellezNo ratings yet
- The Ideal Male Nipple-Areola ComplexDocument7 pagesThe Ideal Male Nipple-Areola ComplexAngga Putra Kusuma KusumaNo ratings yet
- Iliac Crest Bone Graft With Intramedullary.10Document5 pagesIliac Crest Bone Graft With Intramedullary.10DavidNo ratings yet
- Roll Technique Modification Papilla PreservationDocument5 pagesRoll Technique Modification Papilla Preservationmarcela fajardoNo ratings yet
- Management of A Coronally Advanced Lingual Flap in Regenerative Osseous Surgery: A Case Series Introducing A Novel TechniqueDocument11 pagesManagement of A Coronally Advanced Lingual Flap in Regenerative Osseous Surgery: A Case Series Introducing A Novel TechniqueAnita PrastiwiNo ratings yet
- Basic Arthroplasty - Unit 4 - Bone Loss BacksteinDocument9 pagesBasic Arthroplasty - Unit 4 - Bone Loss BacksteinShu Yang HuNo ratings yet
- JournalDocument9 pagesJournalfkia2013No ratings yet
- DentalDocument4 pagesDentalBreeNo ratings yet
- Clin Adv Periodontics - 2022 - Velasquez Plata - Osseous Topography in Biologically Driven Flap Design in MinimallyDocument5 pagesClin Adv Periodontics - 2022 - Velasquez Plata - Osseous Topography in Biologically Driven Flap Design in Minimally安西 泰規No ratings yet
- Jerd 12812Document15 pagesJerd 12812snkidNo ratings yet
- SauFRa Technique For The Fixation of Resorbable Membranes in Horizontal Guided Bone RegenerationDocument5 pagesSauFRa Technique For The Fixation of Resorbable Membranes in Horizontal Guided Bone RegenerationSchwan AbdulkareemNo ratings yet
- Orthodontic-Periodontal Interactions: Orthodontic Extrusion in Interdisciplinary Regenerative TreatmentsDocument30 pagesOrthodontic-Periodontal Interactions: Orthodontic Extrusion in Interdisciplinary Regenerative TreatmentsFrancisco VargasNo ratings yet
- Periodontal Wound Healing and RegenerationDocument40 pagesPeriodontal Wound Healing and RegenerationmackitaNo ratings yet
- CX PLAST PERIO Functional and Esthetic Outcome Enhancement of Periodontal Surgery by ApplicationDocument8 pagesCX PLAST PERIO Functional and Esthetic Outcome Enhancement of Periodontal Surgery by ApplicationV y M Grupo EspecialistaNo ratings yet
- Manual For Preventive Dentistry I-Ii & Clinical Periodontics I - IiDocument77 pagesManual For Preventive Dentistry I-Ii & Clinical Periodontics I - IiSalma MentariNo ratings yet
- Flap Designs For Flap Advancement During Implant Therapy A Systematic Review 2016 PDFDocument8 pagesFlap Designs For Flap Advancement During Implant Therapy A Systematic Review 2016 PDFRohit ShahNo ratings yet
- Dr. Nida Sultana ThesisDocument201 pagesDr. Nida Sultana ThesisKritika KejriwalNo ratings yet
- JCDP 20 1108Document10 pagesJCDP 20 1108snkidNo ratings yet
- Regeneración Periodontal de Defectos Infraóseos HumanosDocument7 pagesRegeneración Periodontal de Defectos Infraóseos HumanosAgustin BuryakNo ratings yet
- Dental and Craniomaxillofacial Implant SurgeryDocument35 pagesDental and Craniomaxillofacial Implant SurgeryJean Carlos Barbosa FerreiraNo ratings yet
- Occlusal and Prosthetic Therapy: Tooth-Supported Fixed Partial DenturesDocument74 pagesOcclusal and Prosthetic Therapy: Tooth-Supported Fixed Partial DenturesRhea OngNo ratings yet
- Implants in Narrow Ridge Situations: A Piezo-Surgical Approach For Alveolar Ridge SplitDocument5 pagesImplants in Narrow Ridge Situations: A Piezo-Surgical Approach For Alveolar Ridge SplitNIMMY ANTONo ratings yet
- Prosthodontic Implant DrivenDocument7 pagesProsthodontic Implant DrivenbuccalNo ratings yet
- Rapi Gide Collagen MembraneDocument6 pagesRapi Gide Collagen MembraneKhaled ElsherbenyNo ratings yet
- ArticleDocument12 pagesArticleMedstudNo ratings yet
- Grafts and Grafting Techniques in Implants - A ReviewDocument25 pagesGrafts and Grafting Techniques in Implants - A ReviewIJAR JOURNALNo ratings yet
- Evaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis DefectsDocument6 pagesEvaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis Defectsmatias112No ratings yet
- Guided Bone Regeneration ProcedureDocument16 pagesGuided Bone Regeneration ProcedureAymen Elatrash100% (4)
- The Palatal Advanced Flap: A Pedicle Flap For Primary Coverage of Immediately Placed ImplantsDocument7 pagesThe Palatal Advanced Flap: A Pedicle Flap For Primary Coverage of Immediately Placed ImplantsMárcia ChatelieNo ratings yet
- The International Journal of Periodontics & Restorative DentistryDocument11 pagesThe International Journal of Periodontics & Restorative DentistryHONG JIN TANNo ratings yet
- Clinical Update: The Deficient Alveolar Ridge: Classification and Augmentation Considerations For Implant PlacementDocument2 pagesClinical Update: The Deficient Alveolar Ridge: Classification and Augmentation Considerations For Implant PlacementJordan BzNo ratings yet
- GTR in Management of Gingival RecessionDocument15 pagesGTR in Management of Gingival RecessionMalavika JaiNo ratings yet
- Bone Augmentation TechniquesDocument20 pagesBone Augmentation TechniquesGabriela Ciornei100% (1)
- Guided Tissue Regeneration For Implants Placed Into Extraction Sockets and For Implant Dehiscences - Surgical Techniques and Case ReportDocument17 pagesGuided Tissue Regeneration For Implants Placed Into Extraction Sockets and For Implant Dehiscences - Surgical Techniques and Case ReportEugenioNo ratings yet
- Guided Immediate Implant Placement With Wound Closure by Computer-Aided Design/Computer-Assisted Manufacture Sealing Socket Abutment: Case ReportDocument6 pagesGuided Immediate Implant Placement With Wound Closure by Computer-Aided Design/Computer-Assisted Manufacture Sealing Socket Abutment: Case ReportbianchiguilhemNo ratings yet
- Stem Cell 0tooth Regeneration 87Document36 pagesStem Cell 0tooth Regeneration 87SamNo ratings yet
- Ridge AugmentationDocument109 pagesRidge AugmentationSingh Jyoti100% (3)