Professional Documents
Culture Documents
Erythrocyte and Plasma Volume Measurement
Uploaded by
Millenial AcousticsOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Erythrocyte and Plasma Volume Measurement
Uploaded by
Millenial AcousticsCopyright:
Available Formats
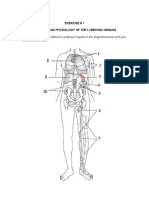
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
Erythrocyte and Plasma Volume
Measurement
JP Esser, Meander Medical Centre, Amersfoort
NOTE: no changes have been made since the version of 2007
Warning:
125
I human serum albumin and 131I human serum albumin are not registered products.
1. Introduction
The isotope dilution technique is used to determine red blood cell and plasma volumes.
In order to determine erythrocyte volumes, red blood cells are labelled with 51Cr sodium
chromate. This radiopharmaceutical attaches itself more or less permanently to the
erythrocytes and the loss of erythrocytes during the investigation period of 1 h is
negligible.
In order to determine plasma volumes, 131I or 125I human serum albumin is used,
which contains less than 1% free iodine. Loss of albumin from the blood circulation
(transcapillary) is usually less than 4% per hour, which means radioactive washout within
one hour of injection is also negligible. The only condition for volume measurement is
that the radiopharmaceutical must be well mixed with the circulating blood. The volume is
calculated from the quotient of the administered dose and the amount of activity present
in the blood sample or plasma sample.
2. Methodology
This guideline is based on available scientific literature on the subject, the previous
guideline (Aanbevelingen Nucleaire Geneeskunde 2007), international guidelines from
EANM and/or SNMMI if available and applicable to the Dutch situation.
3. Indications
Analysis of polycythaemia; in particular to confirm or rule out polycythaemia vera.
4. Relation to other diagnostic procedures
None.
5. Medical information necessary for planning
a. Probability of diagnosis.
b. Relevant haematological parameters (Hb, Ht, etc).
c. Weight of patient.
6. Radiopharmaceutical
Erythrocyte volume
Preparation: 51
Cr autological erythrocytes
Nuclide: Chromium-51
PART I - 161
Deel I_B.indd 161 27-12-16 14:11
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
Dose: For labelling, 6,0 kBq 51Cr chromate/kg body weight, of which about
85% is administered
Administration: Intravenous
Plasma volume
Preparation: I albumin or 131I albumin
125
Nuclide: Iodine-125 or Iodine-131
Dose: 1,3 kBq/kg body weight
Administration: Intravenous
7. Radiation safety
a. Pregnancy
Considering the relatively low dose, < 0,5 MBq 51Cr erythocystes, the benefits of the
diagnostic revenues will quickly outweigh the assumed risk for the unborn child. The
estimated dose to the unborn child will be 0,007 mGy for a 0,5 MBq dose. For 125I -and
131
I - albumin the dose to the unborn child is 0,02 mGy and 0,05 mGy, respectively. For
dosages under 100 mGy no health detriment has been reported for unborn children,
therefore a dose less than 0,5 mSv is acceptable.
b. Lactation
Considering the low dose to the woman and the fact that there is no known transport of
erythrocytes to the mammary glands, the potential risk of radioactivity in the milk will be
minimal. In contrast, with 125I and 131I there is transport of iodine to the mammary glands.
Postponing breastfeeding for 8 weeks ensures no activity ia transmitted to the baby. Due
to the long halflife of 125I and 131I, 60 and 8 days respectively, collected milk should not be
kept for feeding.
c. Radiation exposure
The effective dose to the patient from 6 kBq 51Cr /kg is 1µSv/ 6 kBq, so the effective dose
to a 70 kg patient 0,04 mSv for 51Cr. For 125I and 131I the dose to a patient of 70 kg will be
0,02 mSv and 0,06 mSv, respectively.
NB. It is assumed the sizes of the relevant organs are independent of the weight of the
patient.
8. Patient preparation/essentials for procedure
The patient should lie down for 15 min before the investigation starts (in order to achieve
a stable distribution of blood in the body). Then, a venous cannula (venflon) is inserted (so
blood can be withdrawn at the required times without tourniquet pressure).
Essentials for procedure:
a. A three-way tap allowing the syringe containing the radiopharmaceutical to be
flushed three times.
b. Saponin to lyse the blood in the standard flask as well as the full blood count
samples.
c. For erythrocyte labelling: a sterile, pyrogen-free 30 ml siliconized vial containing 2,5
ml ACD solution (0,8% citric acid, 2,45% glucose, 2,2% trisodium citrate).
PART I - 162
Deel I_B.indd 162 27-12-16 14:11
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
Procedure:
Conditions
Good results are obtained if both the erythrocytes and the plasma volume are calculated.
Erythrocyte and plasma volumes can be calculated simultaneously or sequentially. The
technique produces good results when the following conditions are met:
a. Always follow the protocol exactly, when administering activity and withdrawing blood,
and when dealing with samples in the laboratory.
b. If you wish to measure the erythrocyte and plasma volumes simultaneously and
immediately following the administration of two tracers (one for the plasma volume and
one for the erythrocyte volume), it is important to use radioactive tracers that can be
detected independently.
To measure the erythrocyte and plasma volumes sequentially, the erythrocyte volume
must be measured first and the plasma volume second. The last plasma sample used
for measuring the erythrocyte volume is also used as a blank sample for measuring the
plasma volume.
Extrapolation is not necessary because the erythrocyte activity does not decrease
significantly in the time it takes to measure plasma volume. There is no spectral
interference between the radionuclides, nor is it necessary to use a channel ratio
method. 131I albumin can also be used instead of 125I albumin. However, the measuring
window of the scintillation counter must be wide enough to detect both peaks (51Cr (320
keV) and 131I (364 keV)).
c. All of the radioactive tracer must be added to the compartment that is to be measured
(the circulating blood volume). In other words, no surplus radioactivity may remain in
needle or syringe, the total activity must be administered and no extravasation may
occur; any of these factors will result in an overestimated volume. The use of a three
way tap is recommended when administering accurate volumes (no less than 10 ml for
high accuracy) so the syringe can be flushed three times with a sterile saline solution.
d. Complete mixing is essential; samples must be taken until the concentrations in
the compartment to be measured are stable. Complete mixing of the tracer in the
blood circulation usually takes approximately 10 min (up to 30 min for patients with
polycythaemia and splenomegaly). In order to check whether this condition has been
met, not just one but several samples are taken sequentially (e.g. after 10 and 20 min, or
30 and 60 min for patients with polycythaemia and splenomegaly).
e. The radioactivity is determined in samples that contain an accurately known volume. The
standard and other samples must have the same counting geometry (3,0 ml).
f. No radioactivity may ‘leak’ out of the circulatory system; loss of tracer from the blood
circulation can be avoided and/or limited by using a suitable radioactive tracer which does
not extravasate within the measuring time (approximately 1 h) and which is known to
be sufficiently stable for this purpose. Given the extremely small amounts used, it is not
necessary to inhibit the uptake of free, radioactive iodine by the thyroid gland.
g. The blood withdrawn must be anticoagulated and the volume of anticoagulant must
be negligible in comparison to the volume of blood collected. Blood must never be
taken from the arm into which the radioactive tracer has been administered (to avoid
crosscontamination); blood flow may not be restricted (e.g. by using a tourniquet) when
blood is being collected.
There is no gold standard available to verify the method and it is therefore essential
PART I - 163
Deel I_B.indd 163 27-12-16 14:11
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
that the entire procedure is carried out under conditions that are as reproducible as
possible.
Erythrocyte volume
a. Withdraw 10 ml of blood from the patient, preferably using a 1,1×40 mm needle
(0,8×40 mm may also be used), attach a new needle to the syringe and transfer the
blood into 2,5 ml ACD solution. Gently invert the container several times in order to
mix the solution.
b. Withdraw 4 ml of blood using an EDTA-tube for haematocrit determination. Flush the
system with a heparin solution (3,3 ml heparin/100 ml saline). Flushing is important
because the system will be used at a later stage for blood sampling.
c. Add 6 kBq 51Cr sodium chromate/kg body weight in no less than 0,2 ml saline
solution to the ACD blood solution. Incubate on a rotor at 37°C for 20 min. Add 50
mg vitamin C in order to reduce the surplus Cr6+ chromate to Cr3+, and allow to rotate
for a further 3 min on the rotor.
d. Subsequently administer 10 ml of the ACD solution to the patient in as precise a
volume as possible; do not use a smaller volume as this could compromise accuracy!
Flush the system three times to ensure quantitative injection of the tracer.
e. Withdraw blood at 10 and 20 min post injection and also at 60 minutes if necessary
(see conditions).
f. To make the standard, 1 ml labelled ACD blood is pipetted into a test tube and
washed twice with saline solution. Every single erythrocyte must be used. The
washed erythrocytes are then quantatively transferred to a 250 ml measuring flask
containing approximately 5 ml of saponin. (Saponin is used to lyse the erythrocytes).
Homogenise and pipette 3 ml into a standard counting tube.
g. In order to determine the concentration of radioactivity in the erythrocytes present
in the blood samples, a correction is made for radioactivity in the blood plasma thus
avoiding the need for these small quantities to be washed. For this purpose, 3 ml of
each 10 ml homogenised blood sample is pipetted into counting tubes and lysed
with saponin. The remainder of each blood sample is centrifuged, after which 3 ml
plasma samples from the same p.i. times are transferred to counting tubes. In this
way, corrections can be made for non-radioactive cells in the blood samples.
Plasma volume
a. The injection fluid must contain 50 mg albumin carrier per ml and 0,13 kBq 125I
albumin or 131I albumin per kg body weight per ml.
b. The patient dose is 1,3 kBq per kg body weight (in 10 ml administered as accurately
as possible in as precise a volume as possible; do not use a smaller volume as this
could compromise accuracy). Flush the system three times to ensure quantitative
injection of the tracer.
c. Withdraw blood at 10 and 20 min post injection and also at 60 min if necessary (see
conditions).
d. To make the standard, 1 ml of the injection fluid is accurately pipetted into a 250 ml
measuring flask containing 5 ml of 20% NaOH and 1 drop of saturated potassium
iodide (KI) solution. Fill up to 250 ml, homogenise and pipette 3 ml into a standard
counting tube.
PART I - 164
Deel I_B.indd 164 27-12-16 14:11
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
For a combination of erythrocyte and plasma volume using a single injection:
A single injection solution and a single standard is made using both radiopharmaceuticals
when erythrocyte and plasma volume measurement is carried out simultaneously. The
albumin radioactivity is added to the previously labelled erythrocyte suspension. It is
therefore not necessary to add albumin as a carrier.
9. Acquisition and processing
a. All samples are counted for 20 min or a minimum of 10.000 counts in order to
achieve the statistical accuracy required. The measuring equipment must be adjusted
to the photo peaks of the radionuclides used.
b.
125
I HSA and 51Cr must be used if two isotopes are to be combined in a single
injection. A channel ratio method can then be applied so interference from Compton
radiation in the 125I channel can be measured and used to calculate the net 125I
counts.
c. Photo peaks:
125
I: 30 keV
131
I: 364 keV
51
Cr: 320 keV
10. Interpretation
a. In the event of raised Hb levels, determining a patient’s erythrocyte volume can
help to distinguish between relative polycythaemia and primary polycythaemia
(polycythaemia vera), secondary polycythaemia or idiopathic erythrocytosis.
Erythrocyte volumes are normal in cases of idiopathic erythrocytosis.
b. Theoretically, it should be possible to calculate the erythrocyte volume using the
haematocrit and the calculated plasma volume. However, the peripheral haematocrit
may not be used as an indicator of the central haematocrit as the latter is always
lower than the peripheral value. In other words, both volumes must be determined
independently if information about both volumes is required.
11. Report
a. The report must contain reference values. The blood volume is given as the sum of
the plasma and erythrocyte volumes.
b. The International Committee on Standardization in Haematology (ISCH) published
recommendations for determining plasma and erythrocyte volumes in 1973 and
1980. The reference values are shown in the table below.
Table 1. Reference values in ml/kg.
Erythrocyte volume * Plasma volume
Males 30 ± 5 40
Females 25 ± 5 40
* average ± 2 SD (ml/kg)
PART I - 165
Deel I_B.indd 165 27-12-16 14:11
ERYTHROCYTE AND PLASMA VOLUME MEASUREMENT
c. Medical literature shows a wide variance of normal values for plasma volume,
probably due to the different radiopharmaceuticals used and the natural variance in
plasma volume. Therefore, only average values are presented in the table. Volumes
are expressed in ml per kg body weight (based on total body weight). It would,
of course, be better to use the lean body mass (total body weight minus fat) for
calculations, but total body weight is nevertheless recommended as lean body mass
values are not generally known in practice.
12. Literature
• Bentley SA, Lewis SM. The relationship between total red cell volume, plasma volume and venous
haematocrit. J Haematology 1976;33:301-7.
• International Committee for Standardization in Hematology. Recommended methods for measurement
of red-cell and plasma volume. J Nucl Med 1980;21:793-800.
• Lewis SM, Liu Yin JA. Blood volume studies. In: Lewis SM, Bayly RJ, in Haematology. Volume 14.
Radionuclides in Haematology. New York: Churchill Livingstone, 1986;14:198-213.
• Najean Y, Deschrywer F. The body venous haematocrit ratio and its use for calculating total blood
volume from fractional volume. Eur J Nucl Med 1984;9:558-60.
• Wright RR, Tono M, Pollycove M. Blood volume. Semin Nucl Med 1975;5:63-78.
PART I - 166
Deel I_B.indd 166 27-12-16 14:11
You might also like
- Mls 111b LAb MidDocument10 pagesMls 111b LAb MidJohanna MarieNo ratings yet
- APTT MispaClogDocument1 pageAPTT MispaClogDharmesh PatelNo ratings yet
- From The of Biological Chemistry and Surgery, College of Physicians and Surgeona, Columbia University, New YorkDocument6 pagesFrom The of Biological Chemistry and Surgery, College of Physicians and Surgeona, Columbia University, New YorkashokNo ratings yet
- Week 2-Renal Function Tests and Intro To UrinalysisDocument39 pagesWeek 2-Renal Function Tests and Intro To UrinalysisDayledaniel SorvetoNo ratings yet
- Final NTCC ReportDocument30 pagesFinal NTCC ReportMandeep SinghNo ratings yet
- Cushing's Decision App - Glossary of Terms 2Document3 pagesCushing's Decision App - Glossary of Terms 2Erhan ErtuçNo ratings yet
- Principle Behind Special Collection Procedures, Special Supplies or EquipmentDocument50 pagesPrinciple Behind Special Collection Procedures, Special Supplies or EquipmentSofia JuliaNo ratings yet
- tmp6536 TMPDocument8 pagestmp6536 TMPFrontiersNo ratings yet
- Tugas Pak AzharDocument9 pagesTugas Pak Azhardedi gunawanNo ratings yet
- Presentation On Project Report: Practical in Biochemistry, Pathology and MicrobiologyDocument33 pagesPresentation On Project Report: Practical in Biochemistry, Pathology and Microbiologybharathi novalNo ratings yet
- Blood Transfusion and Transplantation Practical Report: 1 Semester Academic Year 1443 HDocument8 pagesBlood Transfusion and Transplantation Practical Report: 1 Semester Academic Year 1443 Hلمى العصيميNo ratings yet
- CHAPTER 1 To 9Document42 pagesCHAPTER 1 To 9ALNATRON GROUPSNo ratings yet
- ADP KitDocument4 pagesADP KitAioriaCRNo ratings yet
- Guidelines For Hemostasis and ThrombosisDocument4 pagesGuidelines For Hemostasis and Thrombosisjennifer acostaNo ratings yet
- Original ArticleDocument8 pagesOriginal ArticleAshlea HunterNo ratings yet
- BadriaDocument21 pagesBadriaMariela RonquilloNo ratings yet
- Diagnostic Value of C-Reactive Protein and Hematological Parameters in Neonatal SepsisDocument9 pagesDiagnostic Value of C-Reactive Protein and Hematological Parameters in Neonatal SepsisIOSRjournalNo ratings yet
- Prepear Blood SamplesDocument5 pagesPrepear Blood SamplesnejraNo ratings yet
- SPEAKER: Dr. Subhajit Das MODERATOR: Prof. Jyoti ShuklaDocument25 pagesSPEAKER: Dr. Subhajit Das MODERATOR: Prof. Jyoti Shuklaswaraj sharma100% (2)
- CSF XanthochromiaDocument3 pagesCSF XanthochromiaShaikh Ghassan AbidNo ratings yet
- 81 Hcrelbal LDocument4 pages81 Hcrelbal LCynthia AyuNo ratings yet
- IPP-LB-HEM-01-01-LH 750 Analyzer and Coulter Gen's SystemDocument13 pagesIPP-LB-HEM-01-01-LH 750 Analyzer and Coulter Gen's SystemMaria Francesca MapaNo ratings yet
- Cerebrospinal Fluid: Practice Test SheetDocument7 pagesCerebrospinal Fluid: Practice Test SheetJoey MagnoNo ratings yet
- Practice Problems I.V (Autosaved) (Autosaved)Document56 pagesPractice Problems I.V (Autosaved) (Autosaved)Walaa abo foolNo ratings yet
- CRP LX High Sensitive enDocument4 pagesCRP LX High Sensitive enLince WijoyoNo ratings yet
- A Modified Method of Measuring Plasma Volume With Indocyanine Green. Reducing The Frequency of Blood Sampling While Maintaining AccuracyDocument7 pagesA Modified Method of Measuring Plasma Volume With Indocyanine Green. Reducing The Frequency of Blood Sampling While Maintaining AccuracyAzzam AlOtaibiNo ratings yet
- Microscopic Examination of UrineDocument17 pagesMicroscopic Examination of UrineBrent LagartoNo ratings yet
- 9 AstDocument7 pages9 AstAzhar Clinical Laboratory TubeNo ratings yet
- 02.99.055 (PDF Library)Document3 pages02.99.055 (PDF Library)Muthu KumarNo ratings yet
- Compatibility Testing For Blood TransfusionDocument40 pagesCompatibility Testing For Blood TransfusionMunish Dogra100% (4)
- Specimen Collection GuidelinesDocument4 pagesSpecimen Collection GuidelinesFathi MesoNo ratings yet
- Bsis13-I Creatinina 2014Document1 pageBsis13-I Creatinina 2014Alejandra MoralesNo ratings yet
- Estimation of PCV by Wintrobe MethodDocument18 pagesEstimation of PCV by Wintrobe Methodjyoti singhNo ratings yet
- Use of An Enzyme Thermistor For Semi-ContinuousDocument14 pagesUse of An Enzyme Thermistor For Semi-ContinuousWish NewNo ratings yet
- Body Weight (G) CBV (ML) 1% (ML) 10% (ML)Document5 pagesBody Weight (G) CBV (ML) 1% (ML) 10% (ML)Rooney RoyNo ratings yet
- HEMOCLOT Thrombin Time (T.T.) : Kit For The Thrombin Time Determination On PlasmaDocument2 pagesHEMOCLOT Thrombin Time (T.T.) : Kit For The Thrombin Time Determination On PlasmaTanveerNo ratings yet
- Cabahit, Kristene Diane A. Bsmls 3-A SEPT. 28, 2020: Macroscopic Screening Also Referred To As Chemical SeivingDocument14 pagesCabahit, Kristene Diane A. Bsmls 3-A SEPT. 28, 2020: Macroscopic Screening Also Referred To As Chemical SeivingKD CabahitNo ratings yet
- Albumin Change in 24 HoursDocument6 pagesAlbumin Change in 24 HoursfloNo ratings yet
- Albumina 1Document2 pagesAlbumina 1Vale FrancoNo ratings yet
- Immulite 1000Document12 pagesImmulite 1000Syazmin KhairuddinNo ratings yet
- A524 780TM1Document2 pagesA524 780TM1clinical_pathologyNo ratings yet
- Self-Powered Sensor For Naked-Eye Detection of Serum TrypsinDocument4 pagesSelf-Powered Sensor For Naked-Eye Detection of Serum TrypsinCons MirandaNo ratings yet
- PT, Aptt, TTDocument44 pagesPT, Aptt, TTswaraj sharmaNo ratings yet
- Serology Laboratory ModulesDocument29 pagesSerology Laboratory ModulesKayz ZuñigaNo ratings yet
- Hema I Chapter 12 - ESRDocument29 pagesHema I Chapter 12 - ESRdileca1448No ratings yet
- Coombs TestDocument17 pagesCoombs Testnativeman2221No ratings yet
- Laboratory Evaluation of PlateletsDocument4 pagesLaboratory Evaluation of Plateletscherry nokiaNo ratings yet
- Hematology Chap 12Document30 pagesHematology Chap 12Eyasu demsewNo ratings yet
- Preparation of Red Cell Suspension With Different ConcentrationDocument4 pagesPreparation of Red Cell Suspension With Different ConcentrationJanielle FajardoNo ratings yet
- Guía Lab. 2 BC1Document8 pagesGuía Lab. 2 BC1Cristiana Auxiliadora Fonseca MayorgaNo ratings yet
- Hematology Analyzer (Coulter Method)Document22 pagesHematology Analyzer (Coulter Method)Sanchia Janita Khodijah100% (1)
- COMPLETE BLOOD COUNT Lecture GuideDocument9 pagesCOMPLETE BLOOD COUNT Lecture GuideKaycee Gretz LorescaNo ratings yet
- Fundamental Medical Science I Final Report (Proteomic)Document11 pagesFundamental Medical Science I Final Report (Proteomic)Devina TandiasNo ratings yet
- Clinical Haematology Lab. 1: Practical PhysiologyDocument31 pagesClinical Haematology Lab. 1: Practical PhysiologyHameed SabahNo ratings yet
- The Arthrex Autologous Conditioned Plasma Double Syringe System For Canine UseDocument2 pagesThe Arthrex Autologous Conditioned Plasma Double Syringe System For Canine UseDiyaa SakrNo ratings yet
- RT-7600 Hematology AnalyzerDocument86 pagesRT-7600 Hematology AnalyzerJesus100% (1)
- SerologyDocument7 pagesSerologyGerald John PazNo ratings yet
- Laprak Kimklin 3Document16 pagesLaprak Kimklin 3Alifatu Zahra Salsabila SNo ratings yet
- Application of The Continuous Autotransfusion System (CATS) To Prevent Transfusion-Related Hyperkalemia Following Hyperkalemic Cardiac Arrest in An Infant - A Case ReportDocument4 pagesApplication of The Continuous Autotransfusion System (CATS) To Prevent Transfusion-Related Hyperkalemia Following Hyperkalemic Cardiac Arrest in An Infant - A Case Reportmaria bethania martins leiteNo ratings yet
- Avian Medicine:: Principles and ApplicationDocument24 pagesAvian Medicine:: Principles and ApplicationAdriana PalmaNo ratings yet
- Questions 1-11 Are Based On The Following Passage. The Political Power of The First LadiesDocument69 pagesQuestions 1-11 Are Based On The Following Passage. The Political Power of The First LadiesChử Minh HiếuNo ratings yet
- Dairy Technology-Multiple Choice Questions: Chemistry TipsDocument7 pagesDairy Technology-Multiple Choice Questions: Chemistry TipsDhanya M AlexNo ratings yet
- Assessment Diagnosis Planning Interventions Rationale Evaluation Subjective Data: Short Term Goal: Short Term GoalDocument4 pagesAssessment Diagnosis Planning Interventions Rationale Evaluation Subjective Data: Short Term Goal: Short Term GoalGiselle RomeroNo ratings yet
- (INS-TG-EN) Ichroma Tn-I Plus - Rev.01 - 180404Document4 pages(INS-TG-EN) Ichroma Tn-I Plus - Rev.01 - 180404nam7124119100% (2)
- Cuban Panel Claims Stress Caused Mystery IllnessesDocument3 pagesCuban Panel Claims Stress Caused Mystery IllnessesTahmsitoNo ratings yet
- Oils and Fats: Induction Training (Technical-1/2)Document27 pagesOils and Fats: Induction Training (Technical-1/2)Umesha shankra ShettyNo ratings yet
- Acetaminophen Increases Aldosterone Secretion While SuppressingDocument7 pagesAcetaminophen Increases Aldosterone Secretion While SuppressingKhánh Nguyễn NgọcNo ratings yet
- Invoice No 168728Document7 pagesInvoice No 168728RahulNo ratings yet
- Obesity Research & Clinical PracticeDocument8 pagesObesity Research & Clinical PracticeYusi nursiamNo ratings yet
- 2018 Idexx Us DosDocument188 pages2018 Idexx Us DosTesh McGillicuttyNo ratings yet
- Bbi2424 SCL Worksheet 2 Week 3 Sentence StructuresDocument4 pagesBbi2424 SCL Worksheet 2 Week 3 Sentence StructuresNor AziraNo ratings yet
- Anand Diagnostic Laboratory Test Price DetailsDocument6 pagesAnand Diagnostic Laboratory Test Price Detailsvamsiswetha SNo ratings yet
- Disseminated Intravascular Coagulation Concept MapDocument3 pagesDisseminated Intravascular Coagulation Concept MapphoebjaetanNo ratings yet
- Hubungan Kebiasaan Konsumsi Masakan Padang Dengan Kadar Kolesterol (Studi Pada Paguyuban Ikatan Mahasiswa Minang Angkatan 2015 Di Semarang)Document8 pagesHubungan Kebiasaan Konsumsi Masakan Padang Dengan Kadar Kolesterol (Studi Pada Paguyuban Ikatan Mahasiswa Minang Angkatan 2015 Di Semarang)Jefry JapNo ratings yet
- NU 636 WK 2 DP 2 - Treatment of HyperlipidemiaDocument3 pagesNU 636 WK 2 DP 2 - Treatment of HyperlipidemiaShayNo ratings yet
- Pathlab Health ScreenDocument1 pagePathlab Health ScreenNickHansenNo ratings yet
- What Is An Orange?: Orange Peel (Citrus × Sinensis) As Wound Healing AgentDocument4 pagesWhat Is An Orange?: Orange Peel (Citrus × Sinensis) As Wound Healing AgentCamille Anne RabajanteNo ratings yet
- Bossen Non-Dairy Creamer: Calories 547.5Document1 pageBossen Non-Dairy Creamer: Calories 547.5Brendan HubenakNo ratings yet
- KHURAISADocument6 pagesKHURAISASAINI JONINo ratings yet
- The Following Tests Require Special HandlingDocument1 pageThe Following Tests Require Special HandlingEllise DulayNo ratings yet
- Hypolipidemic Drugs PharmdDocument38 pagesHypolipidemic Drugs Pharmddarlington D. y ayimNo ratings yet
- SpecimenDocument1 pageSpecimenBaiq NurhidayatiNo ratings yet
- Urinalysis System Line enDocument4 pagesUrinalysis System Line enNghi NguyenNo ratings yet
- DM OHA and InsulinDocument33 pagesDM OHA and InsulinPraba NanthanNo ratings yet
- Journal of Medicinal Plants Research VolDocument19 pagesJournal of Medicinal Plants Research VolAtheena Jin Anjelle SeveroNo ratings yet
- Analysis: Dietary Guidelines and Health-Is Nutrition Science Up To The Task?Document9 pagesAnalysis: Dietary Guidelines and Health-Is Nutrition Science Up To The Task?Ainun RamadhantiNo ratings yet
- PL Fuji KimiaDocument2 pagesPL Fuji Kimialady anjaniNo ratings yet
- Pathology and Pathophysiology ALL+QUIZDocument235 pagesPathology and Pathophysiology ALL+QUIZomer.buzagloNo ratings yet
- Chem Hema Mindray Marison PDFDocument4 pagesChem Hema Mindray Marison PDFjohn02 deanNo ratings yet