Professional Documents
Culture Documents
Pulmonary Examination - Knowledge at AMBOSS
Uploaded by
KC Dela RosaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pulmonary Examination - Knowledge at AMBOSS
Uploaded by
KC Dela RosaCopyright:
Available Formats
Collapse all sections REGISTER LOG IN
Pulmonary examination Last updated: February 13, 2023
Summary
The examination of the pulmonary system is a fundamental part of the physical examination that consists of inspection, palpation, percussion, and
auscultation (in that order). Recognition of surface landmarks and their relationship to underlying structures is essential. The physical examination of the
pulmonary system begins with the patient seated comfortably on the examination table and his/her upper body completely exposed. The chest and the
patient's breathing pattern are then inspected, followed by palpation of the chest wall, percussion of the thorax, and auscultation of the lung fields. A carefully
recorded medical history and thorough physical examination allow for differential diagnosis and prompt initiation of therapy.
See also differential diagnoses of dyspnea.
Inspection
The following should be assessed:
Breathing pattern
Normal respiratory rates
12–20/min in adults
30–60/min in infants and neonates
See also “Normal vital signs at rest” for all age groups.
Bradypnea
Respiratory rate < 12/min in adults
< 30/min in infants and neonates
< 40/min in newborns
Tachypnea
Respiratory rate > 20/min, shallow breathing in adults
> 60/min in pediatric patients
Hyperpnea: respiratory rate > 20/min, deep breathing
Inspiratory:expiratory ratio: The ratio of the inspiratory time to expiratory time during spontaneous breathing, which is normally 1:2.
Common abnormal patterns of breathing include: [1]
Cheyne-Stokes breathing: alternating periods of deep breathing followed by apnea
Results from a delay in detecting changes in ventilation and arterial carbon dioxide pressure.
Common causes include: advanced heart failure, damage to respiratory centers (e.g., stroke, traumatic brain injuries, metabolic encephalopathies), and
central sleep apnea
Ataxic breathing: irregular breathing in rhythm and depth
Obstructive breathing: prolonged exhalation
Increased effort of breathing
Tachypnea
Use of accessory muscles of respiration during inspiration
Sternomastoid muscles
Scalene muscles
Pectoralis major
Trachea off midline
Tripod position: patients with emphysema and respiratory distress will lean forward while sitting, resting with their hands on their knees.
Peripheral signs of respiratory dysfunction
Cyanosis: bluish discoloration of the skin and mucosa (due to deoxygenated hemoglobin)
Nail clubbing [2]
Definition: Nail clubbing is a physical finding characterized by painless swelling of the distal phalanges typically associated with chronic hypoxemia.
Pathophysiology
Not fully understood
Hereditary factors may predispose to clubbing.
Fibrovascular proliferation in the region of the nail bed due to accumulation of megakaryocytes and platelets in digital vessels and subsequent local
PDGF and VEGF release is suggested.
Associated conditions
Respiratory conditions, such as:
Interstitial lung disease
Idiopathic pulmonary fibrosis
Cystic fibrosis
Lung cancer
Cardiovascular conditions, such as:
Cyanotic congenital heart disease
Cardiac shunts
Infections, such as:
Tuberculosis
Infections causing lung abscesses
Hypertrophic osteoarthropathy: a syndrome (either hereditary or paraneoplastic) that manifests with painful nail clubbing, synovial effusions, and
periostitis
IBD
Not associated with COPD, asthma
Clinical features
Painless swelling of connective tissue in the distal phalanges
Lovibond angle ≥ 180°: angle between the base of the nail and its surrounding skin
Nail bed feels spongy when pressed and springs back when released.
Schamroth test
Place distal phalanges against each other so that both fingernails touch
When there is nail clubbing, the normal diamond-shaped “window” between the nail beds will not be seen.
Abnormalities in the shape of the thorax
The anteroposterior diameter of the thorax may increase in COPD, leading to a “barrel chest” appearance.
Retraction of the intercostal spaces
Asymmetric movement may be associated with pleural disease, phrenic nerve damage, or pleural effusion.
Kyphosis or scoliosis may lead to decreased forced vital capacity, forced expiratory volume and overall respiratory function
Sputum production or secretions, if any
White and translucent: viral infection (for example, bronchitis that presents with a typical early-morning cough)
White and foamy: pulmonary edema
Yellow-green: bacterial infection
Green: an indication of a pseudomonal infection
Grayish: pneumoconiosis, a waning bacterial infection
Blackish-brown: possibly old blood; should be further investigated (can also be a harmless incidental finding)
Friable: tuberculosis, actinomycosis
Hemoptysis: See "Etiology of hemoptysis.”
In newborn and infants
Jugular, sternal, and intercostal retraction
Nasal flaring or flaring of the nostrils
Neck extension
Access full content
Extend your medical knowledge beyond Pulmonary examination
Start your trial, and get 5 days unlimited access to over 1,100 medical articles and 5,000 USMLE and NBME exam-style questions.
TRY FREE FOR 5 DAYS
Palpation
General: Evaluate areas of tenderness or bruising.
Symmetry of chest expansion
Place both hands on the patient's back at the level of the 10th ribs with thumbs pointing medially and parallel to the rib cage.
As the patient inhales, evaluate for asymmetric movement of your thumbs.
Tactile fremitus
Ask the patient to say “toy boat” and feel for vibrations transmitted throughout the chest wall.
Can be asymmetrically decreased in effusion, obstruction, or pneumothorax, among others
Can be asymmetrically increased in pneumonia
References:[3]
Percussion
Technique
Hyperextend the nondominant middle finger and place the distal interphalangeal joint against the chest wall.
Strike the joint with the other middle finger and evaluate the elicited sound.
Always percuss both sides of the chest at the same level. Often the finding of asymmetry is more important than the specific percussion note that is
heard.
Physiological finding: resonant percussion note (a comparatively hollow and loud note)
Pathological findings
Hyper-resonant percussion note
Louder and hollower than normal
Sign of increased air inside the thoracic cavity: emphysema, bronchial asthma, pneumothorax
Dull percussion note
Muffled and softer note
Sign of fluid inside the thoracic cavity: pneumonia, pleural effusion
Assess diaphragmatic movement
Move downwards while percussing over both sides of the chest wall.
The transition point from resonant to dull percussion notes marks the approximate position of the diaphragm.
Abnormally high transition points on one side may be seen in unilateral pleural effusion and unilateral diaphragmatic paralysis.
The distance between the transition point on full expiration and the transition point on full inspiration is the extent of diaphragmatic excursion (normally
3–5.5 cm).
References:[3]
Auscultation
Physiological breath sounds
Vesicular breathing
Soft and low pitched, through inspiration and part of expiration
Heard over both lungs
Bronchovesicular breathing
Intermediate intensity and pitch, through both inspiration and expiration
Heard over 1st and 2ndintercostal spaces
Bronchial breathing
Loud and high pitched, through part of inspiration and all of expiration
Heard over the sternum
Tracheal breathing
Very loud and high pitched, through both inspiration and expiration
Heard over the neck
Cavernous breathing
A harsh, hollow breath sound with high-pitched overtones heard on lung auscultation
It is produced by air passing through a large, superficial cavity that communicates with the bronchial system (e.g., a cyst or abscess)
Can not be heard if there is fluid or a fungal ball within the cavity
Pathological breath sounds
Also known as adventitious or added sounds
Consider secretions (such as in bronchitis) if breath sounds clear after coughing
Types of pathological breath sounds
Crackles or rales: discontinuous, intermittent
Fine: soft, high-pitched (e.g., normal, asbestosis, sarcoidosis)
[4]
Coarse: loud, low-pitched (e.g., COPD, pulmonary edema)
Wheezes (sibilant wheezing): musical, prolonged
Rhonchi (sonor wheezing): low-pitched, snoring
Stridor: high-pitched, over trachea ; which may occur on:
Inspiration (inspiratory stridor): narrowing of the extrathoracic airway; characteristic of epiglottitis, pseudocroup, foreign body aspiration, bilateral
vocal cord palsy
Expiration (expiratory stridor): obstruction of the intrathoracic airways; characteristic of bronchial asthma, COPD
Inspiration and expiration (biphasic stridor): obstruction at the level of the glottis
Pleural friction rub: scratchy, high-frequency sound
Muffled or absent breath sounds: suggest presence of air or fluid between the lung and the chest wall (e.g., pleural effusion, pneumothorax)
Transmitted sounds
Bronchophony
Increased transmission of voice sounds
Ask patient to say “ninety-nine” in a normal voice while auscultating.
An asymmetric increase in voice transmission suggests a collapsed lung or atelectasis.
Egophony
Ask the patient to say “ee” while auscultating.
If it sounds like “A” rather than “E”, this is called egophony and suggests lobar pneumonia.
Whispered pectoriloquy
Ask patient to whisper “ninety-nine” while auscultating.
Normally this is barely audible.
Clearly audible in the presence of pulmonary consolidation
References:[3][4]
Overview of pulmonary examination findings
Main symptom Tactile Percussion Auscultation (breath sounds) Tracheal deviation
fremitus
Physiological – Normal Resonant Vesicular None
Pleural Dyspnea may be present Decreased Dull Decreased To the opposite side of the lesion
(no deviation in small effusions)
effusion
Pulmonary Severe dyspnea Possibly Dull Fine or coarse crackles, depending on None
increased severity
edema
Simple Acute dyspnea Decreased or Hyperresonant Decreased or absent None
absent
pneumothorax
Tension Severe dyspnea Decreased or Hyperresonant Decreased or absent To the opposite side of the lesion
absent
pneumothorax
Bronchial Paroxysmal attacks of dyspnea, Decreased Hyperresonant Wheeze, a prolonged expiratory None
wheezing phase, possibly decreased breath
asthma
sounds
1
Chronic Chronic cough Decreased Hyperresonant Wheezing, rhonchi None
bronchitis
1
Emphysema Chronic dyspnea Decreased Hyperresonant End-expiratory wheezing, decreased None
breath sounds
Fever, dyspnea Increased Dull Coarse crackles None
Pneumonia 2
Lung fibrosis Cachexia and weakness, dyspnea Normal or Dull Basal inspiratory crackles To the side of the lesion
slightly
increased
Atelectasis Pain may be present Decreased Dull Decreased To the side of the lesion
Pulmonary Acute dyspnea, pleuritic chest pain, Normal Normal Normal None
tachypnea
embolism
1
Hemoptysis, constitutional symptoms Possibly Possibly dull Possibly decreased To the opposite side of the lesion
Tumor 1,2,3
(weight loss, fever, night sweats) decreased
The following conditions frequently complicate the aforementioned pulmonary disease: 1pneumonia, 2pleural effusion, 3atelectasis.
See “Dyspnea” for more information.
References:[3]
References
1. Bickley L. Bates' Guide to Physical Examination and History-Taking . Lippincott Williams & Wilkins ; 2012
2. Braun SR, Walker HK, Hall WD, Hurst JW. Respiratory Rate and Pattern. Clinical Methods: The History, Physical, and Laboratory. 1990.
3. Sarkar M, Mahesh D, Madabhavi I. Digital clubbing. Lung India. 2012; 29 (4): p.354.doi: 10.4103/0970-2113.102824 . | Open in Read by QxMD
4. Bohadana A, Izbicki G, Kraman SS. Fundamentals of lung auscultation. N Engl J Med. 2014; 370 (8): p.744-751.doi: 10.1056/NEJMra1302901 .|
Open in Read by QxMD
© 2020 AMBOSS Medical Knowledge Terms and Conditions Privacy Privacy Settings Legal Notice Get Support & Contact Us
You might also like
- Pleurisy, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandPleurisy, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Lung ExaminationDocument14 pagesLung Examinationსალომე მუმლაძე “Slay” TMANo ratings yet
- Assessment of Patients With Repiratory ProblemsDocument33 pagesAssessment of Patients With Repiratory Problemshunter zoneNo ratings yet
- Lung Examination: AbnormalDocument56 pagesLung Examination: AbnormalBECAREFUL89ANo ratings yet
- Kuliah Pengantar PF ParuDocument62 pagesKuliah Pengantar PF Parugagah152No ratings yet
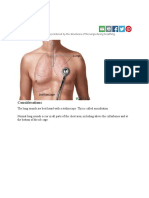
- Breath Sounds: ConsiderationsDocument10 pagesBreath Sounds: ConsiderationsKarl RobleNo ratings yet
- Respiratory ExaminarionDocument40 pagesRespiratory ExaminarionAbdelrahman AldemerdashNo ratings yet
- Respiratory ExamDocument9 pagesRespiratory Examjoelh9No ratings yet
- The Thorax and Lungs - BATESDocument4 pagesThe Thorax and Lungs - BATESsitalcoolk100% (2)
- DR Amsalu Bekele Ass - Professor of Medicine Head of Chest Unit Department of Internal Medicine Addis Ababa University, School of Medicine Addis Ababa, EthiopiaDocument81 pagesDR Amsalu Bekele Ass - Professor of Medicine Head of Chest Unit Department of Internal Medicine Addis Ababa University, School of Medicine Addis Ababa, EthiopiaBethelhem BirhanuNo ratings yet
- Respi SystemDocument6 pagesRespi SystemKalichandren ArumugamNo ratings yet
- Respiratory Exam: Lungs, Breathing, CyanosisDocument81 pagesRespiratory Exam: Lungs, Breathing, CyanosisashuNo ratings yet
- Lung Examination Guide: Physical Steps, Pathologies, Dyspnea TypesDocument145 pagesLung Examination Guide: Physical Steps, Pathologies, Dyspnea TypesIrina CornilovNo ratings yet
- Respiratory System-Review PathoDocument100 pagesRespiratory System-Review PathoSadiePartington-RiopelleNo ratings yet
- Respiratory System Assessment: Other SystemsDocument4 pagesRespiratory System Assessment: Other SystemsChetan KumarNo ratings yet
- Respiratory System PEDocument42 pagesRespiratory System PEyeabsira2116No ratings yet
- Jarvis Chapter 18 Study GuideDocument5 pagesJarvis Chapter 18 Study GuideEmily Cheng100% (2)
- Final Death Note - Compre NotesDocument1,550 pagesFinal Death Note - Compre NotesSteph TabasaNo ratings yet
- Age Rate (In Breaths Per Minute)Document13 pagesAge Rate (In Breaths Per Minute)Itadori YujiNo ratings yet
- Topic 1 - Pulmonary Anatomy, Physiology and Assessment (Hemo)Document39 pagesTopic 1 - Pulmonary Anatomy, Physiology and Assessment (Hemo)Ben JilhanoNo ratings yet
- Chapter 27Document6 pagesChapter 27monster40lbsNo ratings yet
- Respiratory Assessment & DiagnosticsDocument9 pagesRespiratory Assessment & DiagnosticsAngellene GraceNo ratings yet
- W1. Pendekatan Sesak Pada AnakDocument32 pagesW1. Pendekatan Sesak Pada Anaksekrekomdik RSPDNo ratings yet
- Oxygenation 1Document155 pagesOxygenation 1Khatlen BagaresNo ratings yet
- Chest Pulmophysiothera PY: Prepared By: Floriza P. de Leon, PTRPDocument35 pagesChest Pulmophysiothera PY: Prepared By: Floriza P. de Leon, PTRPFloriza de LeonNo ratings yet
- Disorders of The Respiratory SystemDocument9 pagesDisorders of The Respiratory SystemAjay Pal NattNo ratings yet
- Respiratory Failure: by Amera GumamaDocument26 pagesRespiratory Failure: by Amera GumamaGumama AmeiyrhaNo ratings yet
- Respiratory AssessmentDocument79 pagesRespiratory AssessmentKarlo ReyesNo ratings yet
- Assessmentpulmonary 151014090912 Lva1 App6892Document63 pagesAssessmentpulmonary 151014090912 Lva1 App6892sasNo ratings yet
- Assessment of Respiratory SystemDocument34 pagesAssessment of Respiratory SystemKristal Jade Yanto Esquillo100% (1)
- Assessment of the Respiratory SystemDocument20 pagesAssessment of the Respiratory SystemnadyaNo ratings yet
- Nursing Care Plan For HEMOTHORAX PNEUMOTHORAXDocument8 pagesNursing Care Plan For HEMOTHORAX PNEUMOTHORAXHistory TechNo ratings yet
- Session 4 - Performing Respiratory System ExaminationDocument26 pagesSession 4 - Performing Respiratory System ExaminationOtsward OwdenNo ratings yet
- Nursing Care Plan For "HEMOTHORAX PNEUMOTHORAX"Document8 pagesNursing Care Plan For "HEMOTHORAX PNEUMOTHORAX"jhonroks78% (9)
- Respiratory System: Physical Diagnosis Course II Physical ExamDocument57 pagesRespiratory System: Physical Diagnosis Course II Physical ExamashuNo ratings yet
- 1. Care for a Client With Respiratory Disorders 2Document105 pages1. Care for a Client With Respiratory Disorders 2moncalshareen3No ratings yet
- Respiratory Exam GuideDocument18 pagesRespiratory Exam GuideIbi Yulia Setyani100% (1)
- Articulo Parcial 1 Urgencias Respiratorias Perros y GatosDocument23 pagesArticulo Parcial 1 Urgencias Respiratorias Perros y GatosYara Valentina Toledo ManriqueNo ratings yet
- Thorax and LungsDocument11 pagesThorax and LungsJoel SantosNo ratings yet
- Assessment of Respiratory System: Group 3Document33 pagesAssessment of Respiratory System: Group 3ChicieMonalisaNo ratings yet
- Reviewer For Management of Common IllnessDocument27 pagesReviewer For Management of Common Illnessmarie vennis hamchawanNo ratings yet
- Thorax and Lung - LectureDocument60 pagesThorax and Lung - LectureТаншолпан ШохбутоваNo ratings yet
- Respiratory EmergencyDocument14 pagesRespiratory EmergencyThomas SentanuNo ratings yet
- Cough: Group - 10Document41 pagesCough: Group - 10AradhanaRamchandaniNo ratings yet
- Rev Widya Physical Examination of Respiratory SystemDocument72 pagesRev Widya Physical Examination of Respiratory SystemYuliaNo ratings yet
- Lower Respiratory Disorders Part 1Document70 pagesLower Respiratory Disorders Part 1Joseph Krafft100% (1)
- AtelectasisDocument24 pagesAtelectasisTiara RahmawatiNo ratings yet
- Care of A Child With RespiratoryDocument185 pagesCare of A Child With RespiratoryVanessa Lopez100% (1)
- Atelectasis SignsDocument26 pagesAtelectasis SignsArini NurlelaNo ratings yet
- Bates Outline of Chapter 8Document15 pagesBates Outline of Chapter 8KatherynSotoNo ratings yet
- Respiratory Diseases GuideDocument27 pagesRespiratory Diseases GuideIhsan HanifNo ratings yet
- 1.) Anatomy and Physiology of The Respiratory SystemDocument6 pages1.) Anatomy and Physiology of The Respiratory SystemFaith SarmientoNo ratings yet
- Treating PneumothoraxDocument20 pagesTreating PneumothoraxMichelle Vera GabunNo ratings yet
- Ax PneumothoraxDocument8 pagesAx Pneumothoraxapi-3797941100% (2)
- Chest Examination: Syeda Afsheen Daud Lecturer IPMR KMUDocument59 pagesChest Examination: Syeda Afsheen Daud Lecturer IPMR KMUCHANGEZ KHAN SARDARNo ratings yet
- Physical Diagnoses: Respiratory SystemDocument72 pagesPhysical Diagnoses: Respiratory SystemAmanuel MaruNo ratings yet
- Thorax and Lungs ReferenceDocument8 pagesThorax and Lungs Referencegwynth ripaldaNo ratings yet
- Your Family Doctor Asthma: Understanding Asthma / Avoiding Allergies / Proper Use of InhalersFrom EverandYour Family Doctor Asthma: Understanding Asthma / Avoiding Allergies / Proper Use of InhalersNo ratings yet
- UERM-CM 2021 EYYYYY On Twitter (ANATOMY MNEMONI 2Document1 pageUERM-CM 2021 EYYYYY On Twitter (ANATOMY MNEMONI 2KC Dela RosaNo ratings yet
- Medicowesome Glasgow Coma Scale Mnemonic 2Document1 pageMedicowesome Glasgow Coma Scale Mnemonic 2KC Dela RosaNo ratings yet
- Murmurs Made Easy Epomedicine 2Document1 pageMurmurs Made Easy Epomedicine 2KC Dela RosaNo ratings yet
- Muscles of The Upper Arm - Biceps - Triceps - TeaDocument1 pageMuscles of The Upper Arm - Biceps - Triceps - TeaKC Dela RosaNo ratings yet
- Gyne ReflectionDocument18 pagesGyne ReflectionKC Dela RosaNo ratings yet
- Genital Tract Infections - GynecologyDocument17 pagesGenital Tract Infections - GynecologyKC Dela RosaNo ratings yet
- Must To Know HemaDocument44 pagesMust To Know HemaKaycee Gretz LorescaNo ratings yet
- Red Man SyndromeDocument3 pagesRed Man Syndrome林唐宇No ratings yet
- Neonatal LupusDocument19 pagesNeonatal Lupusyogeshraval368No ratings yet
- CV Europass GB FlorinaMoldovanDocument4 pagesCV Europass GB FlorinaMoldovanmihaicornelNo ratings yet
- AML Case Study AnalysisDocument14 pagesAML Case Study AnalysisIssaiah Nicolle CeciliaNo ratings yet
- De Gruchy's Clinical Haematology in Medical Practice 5th Edition PDFDocument532 pagesDe Gruchy's Clinical Haematology in Medical Practice 5th Edition PDFnarasimhahan82% (17)
- Autoimmune Protocol Ebook 6 19Document306 pagesAutoimmune Protocol Ebook 6 19Hrvoje100% (11)
- A Review of Chemical Constituents and Traditional Uses of Neem Plant (Azadirachta Indica)Document11 pagesA Review of Chemical Constituents and Traditional Uses of Neem Plant (Azadirachta Indica)Paramjeet Kaur Paramedical SciencesNo ratings yet
- Clinical Orthoptics - Fiona Rowe - 146Document6 pagesClinical Orthoptics - Fiona Rowe - 146Danielle SangalangNo ratings yet
- Х - рург - чний проф - льDocument35 pagesХ - рург - чний проф - льPurnima ChoudhuryNo ratings yet
- Megaloblastic AnemiaDocument26 pagesMegaloblastic AnemiaAbdifatah Abdiwali mohamedNo ratings yet
- Adi Bestara EKG at A Glance NewestDocument113 pagesAdi Bestara EKG at A Glance Newestkarpax21100% (1)
- Handbook of Ocular Disease ManagementDocument63 pagesHandbook of Ocular Disease ManagementSmaraNo ratings yet
- EEG Waveform Guide: Alpha, Beta, Theta & Delta Frequencies ExplainedDocument9 pagesEEG Waveform Guide: Alpha, Beta, Theta & Delta Frequencies ExplainedsvchaudhariNo ratings yet
- T3 - Pack Code DetailsDocument302 pagesT3 - Pack Code DetailskiranNo ratings yet
- Alzheimer's Disease: CausesDocument4 pagesAlzheimer's Disease: CausesDenise PoNo ratings yet
- Eyelid Disorders Guide: Ptosis, Blepharitis, Hordeolum & MoreDocument48 pagesEyelid Disorders Guide: Ptosis, Blepharitis, Hordeolum & MoreUdaif BabuNo ratings yet
- Gotu Kola Herbal Medicine Guide to Healing PropertiesDocument23 pagesGotu Kola Herbal Medicine Guide to Healing Propertiesglenn johnstonNo ratings yet
- COPD Acute Management ABCDEDocument11 pagesCOPD Acute Management ABCDESSNo ratings yet
- Nursing Review Notes 2Document4 pagesNursing Review Notes 2api-3822508100% (5)
- Neurological History and Physical ExaminationDocument21 pagesNeurological History and Physical Examinationg3murtulu100% (1)
- Father Muller Homeopathic Medicines PatentedDocument3 pagesFather Muller Homeopathic Medicines Patentedrays_nitaNo ratings yet
- A-Plus Beyond Critical Shield A-Plus Beyond Early Critical Shield Brochure 8thDocument21 pagesA-Plus Beyond Critical Shield A-Plus Beyond Early Critical Shield Brochure 8thNavin IndranNo ratings yet
- Physical Examination TemplateDocument9 pagesPhysical Examination Templatedhuha_minozNo ratings yet
- Week 7. Renal Pathology Continued.Document9 pagesWeek 7. Renal Pathology Continued.Amber LeJeuneNo ratings yet
- Oregon Medical Marijuana Act HandbookDocument24 pagesOregon Medical Marijuana Act HandbookornormlNo ratings yet
- Types of Organic Mental DisordersDocument5 pagesTypes of Organic Mental DisordersKaneki KenNo ratings yet
- TIRMODDocument66 pagesTIRMODYaniNo ratings yet
- Treating UTI With BiomagnetismDocument8 pagesTreating UTI With BiomagnetismSanjeev SaxenaNo ratings yet
- PATHOLOGY HAQs 2nd EdDocument26 pagesPATHOLOGY HAQs 2nd Edcharusharma9831240259No ratings yet