Professional Documents
Culture Documents
The Relationship Between Pleural Fluid Findings and The Development of Pleural Thickening in Patients With Pleural Tuberculosis1264.full
Uploaded by
lutfor rahmanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Relationship Between Pleural Fluid Findings and The Development of Pleural Thickening in Patients With Pleural Tuberculosis1264.full
Uploaded by
lutfor rahmanCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/21221271
The Relationship between Pleural Fluid Findings and the Development of Pleural
Thickening in Patients with Pleural Tuberculosis
Article in Chest · December 1991
DOI: 10.1378/chest.100.5.1264 · Source: PubMed
CITATIONS READS
96 164
5 authors, including:
Carmen Silvia Valente Barbas Alberto Cukier
Hospital Israelita Albert Einstein and Respiratory ICU INCOR University of Sao Paulo … Instituto do Coração
253 PUBLICATIONS 9,034 CITATIONS 209 PUBLICATIONS 3,602 CITATIONS
SEE PROFILE SEE PROFILE
Carlos R R Carvalho
University of São Paulo
457 PUBLICATIONS 17,747 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Strategies for reducing the time of mechanical ventilation and ventilator-associated pneumonia View project
Brazilian recommendations of mechanical ventilation View project
All content following this page was uploaded by Carmen Silvia Valente Barbas on 27 May 2014.
The user has requested enhancement of the downloaded file.
The relationship between pleural fluid findings
and the development of pleural thickening in
patients with pleural tuberculosis.
C S Barbas, A Cukier, C R de Varvalho, J V Barbas Filho and R W Light
Chest 1991;100;1264-1267
DOI 10.1378/chest.100.5.1264
The online version of this article, along with updated information and services
can be found online on the World Wide Web at:
http://chestjournal.chestpubs.org/content/100/5/1264
Chest is the official journal of the American College of Chest Physicians. It has
been published monthly since 1935. Copyright1991by the American College of
Chest Physicians, 3300 Dundee Road, Northbrook, IL 60062. All rights
reserved. No part of this article or PDF may be reproduced or distributed
without the prior written permission of the copyright holder.
(http://chestjournal.chestpubs.org/site/misc/reprints.xhtml) ISSN:0012-3692
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
The Relationship between Pleural Fluid
Findings and the Development of Pleural
Thickening in Patients with Pleural
Tuberculosis*
Carmen S. V Barbas, M.D.; Alberto Gukier, M.D.;
Carlos R. R. de Varvaiho, M.D.; Jodo % Bar/xis Filho, M.D.; and
RichardWLight, M.D., FG.G.P
The objective of the study was to determine if residual was 5.40±0.58 g/dl for group 1 and 5.17±0.80 g/dl for
pleural thickening after treatment for pleural tuberculosis group 2, while the mean pleural fluid glucose level was
could be predicted from the pleural fluid findings at the 78.6± 19.5 mg/dl for group 1 and 79.5±20.1 mg/dl for
time of the initial thoracentesis. Forty-four patients initially group 2. The
pleural mean
fluid lactate dehydrogenase
diagnosed as having pleural tuberculosis between January (LDH)level in group 1 was 593 ±498 lUlL, while the mean
1986 and January 1988 were separated into two groups: the level for group 2 was 491 ± 198 lUlL. The presence of
23 patients in group 1 had residual pleural disease, while residual pleural thickening was not related to the chemo-
the 21 patients in group 2 had no residual pleural disease therapeutic regimen or the performance of a therapeutic
after treatment for their pleural tuberculosis was corn- thoracentesis. From this study we conclude that approxi-
pleted. Tb. clinical characteristics of the two different mately 50 percent of patients with pleural tuberculosis will
groups did not differ significantly, but the patients in group have residual pleural thickening when their therapy is
1 tended to be a little sicker in that the duration of their completed, but that one cannot predict which patients will
symptoms was longer, their hemoglobin values were lower, have residual pleural thickening from either their clinical
and weight loss and cough were more frequent. There were characteristics or their pleural fluid findings.
no significant differences in the pleural fluid findings in the (Chest 1991; 100:1264-67)
two different groups. The mean pleural fluid protein level
A sizable percentage of patients who have pleural tuberculosis
of Medicine
were
ofthe
seen
University
at the Hospital
of Sao Paulo
das Clinicas
(Brazil).
of the
All patients
Faculty
who
tuberculosis have residual pleural thickening af-
had either a pleural biopsy specimen showing granulomas with
ter treatment for the tuberculosis is completed. ‘ The
caseous necrosis and/or pleural fluid or pleural tissue positive on
incidence of residual pleural thickening appears to be culture for Mycobacterium tuberculosis were included in the study.
largely independent of the treatment,”3 although one Forty-four patients returned to follow-up after 6 to 12 months and
report suggests that the administration of corticoste- these patients form the study population.
Prior to treatment, the following data were obtained: patient’s
roids decreases the incidence of residual pleural
age; duration of symptoms; presence or absence of fever, weight
thickening2 and another suggests that a therapeutic loss, chest pain, night sweats, dyspnea, and cough; reaction to
thoracentesis decreases the incidence ofresidual pleu- intradermal purified protein derivative (PPD); level of protein,
ral thickening. glucose, LDH, and amylase in the pleural fluid; level of protein,
We hypothesized that those patients who had the glucse, and LDH in the serum; cellular composition ofthe pleural
fluid; and the size of the effusion. The effi,sion was classified as
greatest amount of pleural inflammation as evidenced
large if on the posteroanterior chest roentgenogram the effusion
by the highest levels oflactate dehydrogenase (LDH)
occupied more than one third the distance between the lateral
and the lowest levels of glucose in the pleural fluid chest wall and the medlastinum at the level of the hilar region.’ In
would he those most likely to develop residual pleural addition, the histologic features and culture results of the pleural
thickening. In this retrospective study of 44 patients, biopsy specimen and the culture results of the pleural fluid were
recorded.
the occurrence of residual pleural thickening was
During the study period, several different treatment regimens
correlated with the pleural fluid findings at the time for pleural tuberculosis were used. Fourteen patients received
of the initial thoracentesis. isoniazid, rifampin, and pyrazmnamide for the initial two months
followed by an additional seven months of therapy with isoniazid
MATERIALS AND METHODS and rifampin. Twelve patients received isoniazid and rifampin for
Between January 1986 and January 1988, 71 patients with pleural nine months and an additional 12 patients received isoniazid,
rifampin and pyrazinamide for the initial two months followed by
5Fmm the Lung Unit, Faculty ofMedicine, University ofSao Paulo, four additional months of isoniazid and rifampin therapy. Four
Brazil, and the Department of Medicine, Veterans Administration patients received rifampin, ethaunbutol, and isoniazid for three
Medical Center, Long Beach, Calif. and the University of Califor- months, ethambutol and isoniazid for another three months, and
nia, Irvine.
isoniazid alone for an additional three months. Two patients received
Manuscript received December 20; revision accepted March 12.
Reprint requests: Dr. Light, Chief of Research (151), VA Medical other regimens. Eleven patients underwent therapeutic thoracen-
Center, Lirng Bead, 90822 tesis of more than 500 ml. No patient received corticosteroids.
1264 Pleural Auid, Pleural Thkon#{232}ngand Pleural Tuberculosis (Bathes et a!)
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
Table 1-Comparison OJC1InICa1 Characteristics in Table 2-Comparison ofRoentgenographic and Pleural
Patients with Residual Pleural Thickening (Group 1) and Biopsy Findings in Patients with Residual Pleural
Those without Pleural Thickening (Group 2) Thickening (Group 1) and Those without Pleural
Thickening (Group 2)
Group!, Gro#{252}p2,
No. (%) No. (%) Group 1, Group 2,
No. (%) No. (%)
Age, yr. mean±SD 35.8±13.1 34.8± 14.3
Hemoglobin, gIdl 12. 1 ± 1.9 12.4 ± 1.2 PPD >15 mm induration 11/15 (73) 8/16 (50)
Duration ofsymptoms, 8 wk* 6/14 (43) 2110 (20) Large pleural effusion 1L/23 (48) 6/21 (29)
Fever 21/23 (91) 20/21 (95) Parenchymal lesion also 5/23 (22) 5/21 (24)
Weight loss 19/23 (83) 15/21 (71) Positive pleural fluid culture 2/19 (11) 5/12 (42)
Chest pain 21123 (91) 20/21 (95) Positive pleural lx culture 15(19 (79) 11114 (79)
Night sweats 12/23 (52) 11121 (52) Granuloma pleural Bx 20/22 (91) 16/18 (89)
Dyspnea 15/23 (65) 13/21 (62) AFB on pleural Bx 7/22 (32) 10/18 (56)
Cough 16/23 (70) 12121 (57) Necrosis on pleural Bx 7/20 (35) 8118 (44)
*Data unavailable for nine patients in group 1 and 11 patients in
Dx with first Bx 17/22 (77) 19/21 (90)
Therapeutic thoracentesis 3 (22) 6t21 (29)
group 2.
INH + Rif+ PZA (6 mo) 5/23 (22) 7/21 (33)
INH + Rif± PZA (9 mo) 18123 (78) 14121 (67)
The 44 patients were separated into two groups based on their
chest roentgenograms at the end of treatment (6 to 12 months after *PPD =purified protein derivative; Bx=biopsy; AFB acid-fast
the diagnosis depending on the therapeutic regimen). The 23 bacilli; Dx = diagnosis; INH isoniazid; Rif rifampin; and
patients in group 1 had residual pleural thickening that was defined PZA= pyrazinamide.
as a pleural thickening greater than 2 mm on the lateral-inferior
portion ofthe posteroanturior chest roentgenogram. The 21 patients fluid cultures and a lower incidence of positive acid-
in group 2 had no such thickening.
fast bacilli (AFB) smears. The patients whose final
Statistical Analysis evaluation occurred after six months of therapy had
The data are expressed as the mean ± the standard deviation
no higher incidence of pleural thickening than did
unless otherwise noted. The pleural fluid protein, LDH, and glucose those whose evaluation occurred after nine or more
levels and the ratio ofthe pleural fluid to serum protein, LDH, and months oftherapy. Likewise, the incidence of residual
glucose levels in the 23 patients with residual pleural thickening pleural thickening did not appear to be related to the
and the 21 patients without residual pleural thickening were
chemotherapeutic regimen or whether the patient had
compared with the unpaired t test. The percentage ofpatients with
various clinical characteristics or receiving different treatment received a therapeutic thoracentesis.
regimens in the two different groups were compared with the x5 There appeared to be no relationship between
test. residual pleural thickening and the level of protein,
glucose, or LDH in the pleural fluid at the time of the
RESULTS
initial thoracentesis. The mean protein and LDH
The clinical characteristics of the 23 patients with
and the 21 patients without residual pleural thickening
were quite similar (Table 1). The mean ages and
7.0 -
hemoglobin levels were nearly identical in the two .
groups. There was no significant difference in the z
fraction of patients with fever, weight loss, chest pain,
night sweats, dyspnea, or cough in the two different
groups, although the group that was left with residual
thickening
symptoms and slightly
did have a slightly
higher incidence
longer duration
ofweight
of
loss !.. 6.0
S.
S
and cough. Although more than 50 percent of the S.
study population had residual pleural thickening at .I $I
S
the last follow-up visit, the pleural thickening itself S
did not appear to be responsible for symptoms at this S
visit in any of the patients. S
The skin test results, roentgehographic findings, and
pleural biopsy and culture results did not differ
signfficantly between the two different groups (Table
2). The patients with residual pleural thickening
tended to have a higher incidence of a PPD with PLEURAL NO PLEURAL
greater than 15 mm induration and tended to have a THICKENING THICKENING
higher incidence of large pleural effusions, but they Ficuis 1. Levels of pleural fluid protein in patients with and
tended to have a lower incidence of positive pleural without residual pleural thickening.
CHEST I 100 I 5 I NaVEMBER, 1991 1265
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
S S thickening when chemotherapy is completed for pleu-
ral tuberculosis. The incidence of residual thickening
does not appear to be related to the initial biochemical
findings in the pleural fluid or the clinical character-
S
S istics of the patients at the time of presentation.
I 00-
S.
Moreover, the incidence of residual thickening was
w $ S not related to the chemotherapeutic regimen or the
0 S. $ performance of a therapeutic thoracentesis. In one
0 S..
C) S
previous report, patients who had undergone thera-
80 - -
peutic thoracentesis had a significantly lower mci-
-J .
0 $ S dence of residual pleural thickening.
We had hypothesized that those individuals who
00
S I had lower pleural fluid glucose levels or higher pleural
-JE 60 S5 5 fluid LDH levels would be niore likely to have residual
L& S
S pleural thickening. The leyel of pleural fluid LDH is
..J
S
thought to be correlated with the degree of pleural
S
inflammation.6 Certainly in patients with parapneu-
w 40 monic effusions, the lower the pleural fluid glucose
-J
0. S level or the higher the pleural fluid LDH level, the
more likely that the patient is to require chest tubes.7
Furthermore, a low pleural fluid glucose level in
patients with malignant pleural effusions is associated
I I
with a large tumor burden.8 However, the data from
PLEURAL NO PLEURAL
THICKENING THICKENING our study offered no support for our hypothesis.
In the present study, there was no relationship
Ficuax 2. Levels of pleural fluid glucose in patients with and
without residual pleural thickening. between the treatment that the patient received and
residual pleural thickening. When one reviews the
levels were slightly higher while the mean pleural natural history of untreated tuberculous pleuritis, one
fluid glucose level was slightly lower in patients with
‘: .2563
residual pleural effusions. The distribution of the
values for the pleural fluid levels of protein (Fig 1), 1 ooo_:
glucose (Fig 2) and LDH (Fig 3) were virtually
identical in the two different groups. S
The mean ratio ofthe pleural fluid to serum protein
level was similar in the group with thickening 800-
S
S
(0.72±0.08) and the group without thickening
(0.72 ± 0. 10). Likewise, the ratio ofthe pleural fluid to
serum glucose and LDH were similar in the groups
a S
S
S
with thickening (0.76±0.25 and 2.58± 1.70, respec-
-J 600- 2 S
tively) and without thickening (0.85±0.17 and
S
D
2.74 ± 1 .33, respectively). S 1
S
The data were also analyzed to determine if there S
I
was a significant relationship between the levels of 0 .5 S
S
glucose and LDH in the pleural fluid of the entire -J 400 -
S
group of patients. There was a significant relationship S #{149}5
between the ratio ofthe pleural fluid to serum glucose S. S
S
S
and the ratio of the pleural fluid to serum LDH .5 S
(r = - 0.51, p<O.Ol). The minus sign on the correlation 200- 5 S
coefficient indicates that low glucose levels are asso-
ciated with high LDH levels. There were no signfficant
correlations among the absolute levels of protein,
glucose, and LDH in the pleural fluid.
I ‘
PLEURAL NO PLEURAL
DISCUSSION
THICKENING THICKENING
The present study demonstrates that there is ap- Ficuax 3. Levels of pleural fluid lactate dehydrogenase (LDH) in
proximately a 50 percent incidence of residual pleural patients with and without residual pleural thickening.
1266 Pleural Auid, Pleural Thickenrng and Pleural Tuberculosis (Bathes eta!)
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
should not be surprised at this finding. Roper and the changes in pulmonary function with residual
Waring#{176}followed 141 individuals who had exudative pleural thickening were not documented in this or in
pleuritis and a positive skin test to PPD. The patients, previous studies, patients with asbestosis and much
who were first diagnosed in 1944 or 1945, were treated greater amounts of pleural thickening have only mild
only with bed rest. At the end of their initial hospital- reductions in their pulmonary function test
ization, only 48 (34 percent) had more than slight
residual pleural thickening. Since residual pleural ACKNOWLEDGMENTS: We thank the following physicians who
took care of the patients in the Ambulatory Clinic of Tuberculosis
disease from tuberculosis tends to improve with time,2 of the Hospital das Clinicas-Faculty of Medicine-University of San
we thought that those patients who were evaluated Paulo: Eliane C. R. Follador, Fernanda M. V. Boueri, Loavo M.
Leite, Teresa Y. Takagaki, and Ronaldo A. Kairalla. We thank Marina
after six months of therapy might have a higher Berman for her assistance with the medical illustrations.
incidence of residual pleural thickening than those
evaluated after nine months of therapy, but this was REFERENCES
not the case in the present study (Table 2). 1 Large SE, Levick RK. Aspiration in the treatment of primary
If the residual pleural disease is related neither to tuberculous pleural effusion. BMJ 1958; 1:1512-14
the initial biochemical findings nor to the treatment, 2 Tani P, F#{243}ppiusH, M MakipajaJ. Cortisone therapy for exudative
what is it related to? The patients with residual tuberculous pleurisy in the light of a follow-up study. Acts
Tuberc Scand 1964; 44:303-09
thickening tended to have a larger PPD, a lower
3 Lee CH, Wang WJ, Lan RS, Tsai YH, Chiang YC. Corticoste-
incidence ofpositive pleural fluid cultures, and a lower roids in the treatment of tuberculous pleurisy: a double-blind,
incidence ofpositive AFB smears. These observations placebo-controlled, randomized study. Chest 1988; 94:1256-59
suggest that delayed hypersensitivity rather than the 4 Morrone N, Lombardi MC, Machado 0. Prevention of pleural
inflammatory response to infection is responsible for thickening through pleural aspiration in patients with tubercu-
bus effusion. J Pneumologia (San Paulo) 1989; 15:180-84
the fibrosis. The local inflammatory hypersensitivity
5 Martensson C, Bake B, Brolin I, Larsson 5, Pettersson K,
response with tuberculous pleuntis is mediated in Thiringer C. Radiographic appearance and lung function after
part by a number of inflammatory and immunostim- non-malignant pleural efihision. Eur J Bespir Dis 1987; 71:306-
ulatory factors, including complement degradation 13
products, interferon gamma, and interleukin 1.112 6 Light RW, Pleural diseases, 2nd ed. Philadelphia: Lea & Febiger,
1990
Since it is becoming increasingly clear that cytokines
7 Light RW, Girard WM, Jenkinson SC, George RB. The mci-
modulate the development of fibrosis,’3”4 one might dence and significance of parapneumonic effusions. Am J Med
anticipate that there would be some relationship 1980; 69:507-12
between the level of hypersensitivity and the devel- 8 Rodriguez-Panadero F, Lopez Mejias J. Low glucose and pH
opment of pleural fibrosis. levels in malignant pleural effusions. Am Rev Respir Dis 1989;
139:663-67
We had also anticipated that there would be a
9 Roper WH, WaringJJ. Primary serofibrinous pleural effusion in
significant negative correlation between the levels of military personnel. Am Rev Respir Dis 1955; 71:616-34
LDH and the levels of glucose in the pleural fluid. 10 Ellner JJ, Barnes PF, Wallis RS, Modin RL. The immunology of
This has been the case with parapneumonic’5 and tuberculous pleurisy. Sem Respir Infect 1988; 3:335-42
malignant’6 pleural effusions. In the present study, 11 Barnes PF, Mistry SD, Cooper CL, Pirmez C, Rea TH, Modlin
RL. Compartmentalization ofa CD4 T lymphocyte subpopu-
there was not a significant correlation between the
lation in tuberculous pleuritis. J Immunol 1989; 142:1114-19
levels of glucose and LDH in the pleural fluid, 12 Ribera E, Espanol T, Martinez-Vazquez JM, Ocana I, Encabo
although there was a significant relationship between C. Lymphocyte proliferation and gamma-interferon production
the ratios of the pleural fluid to the serum LDH and after in vitro’ stimulation with PPD: differences between
glucose. The lack of a significant correlation with the tuberculous and nontuberculous pleurisy in patients with posi-
tive tuberculin skin test. Chest 1990; 97:1381-85
absolute levels was quite possibly related to the
13 Antony YB, Sahn SA, Antony AC, RepinejE. Bacillus Calmette-
relatively narrow range of pleural fluid glucose levels. Guerin-stimulated neutrophils release chemotaxins for mono-
In conclusion, the results of the present study fail cytes in rabbit pleural spaces and in vitro. J Clin Invest 1985;
to support our hypothesis that residual pleural thick- 76:1514-21
ening would be more common in patients with pleural 14 Libby P, Friedman GB, Salomon RM. Cytokines as modulators
ofcell proliferation in fibrotic disease. Am Rev Respir Dis 1989;
tuberculosis with a higher degree of pleural inflam-
140:1114-17
mation as evidenced by lower pleural fluid glucose
15 Good JT Jr. Taryle DA, Maulitz RM, Kaplan RL, Sahn SA. The
levels and higher pleural fluid LDH levels. The diagnostic value ofpleural fluid pH. Chest 1980; 78:55-9
incidence of residual pleural thickening was slightly 16 Sahn SA, Good JT Jr. Pleural fluid pH in malignant effusions:
above 50 percent, but the presence of the residual diagnostic, prognostic, and therapeutic implications. Ann Intern
Med 1988; 108:345-49
pleural thickening was not associated with clinical
17 Schwartz DA, Calvin JR. Dayton CS, Stanford W, Merchant
symptoms. It is unlikely that the mild degrees of
JA, Hunninghake GW. Determinants ofrestrictive lung function
residual thickening observed in the present study have in asbestos-induced pleural fibrosis. J AppI Physiol 1990;
any clinical significance. Although documentation of 68:1932-37
CHEST I 100 I 5 I NOVEMBER, 1991 1267
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
The relationship between pleural fluid findings and the development of
pleural thickening in patients with pleural tuberculosis.
C S Barbas, A Cukier, C R de Varvalho, J V Barbas Filho and R W Light
Chest 1991;100; 1264-1267
DOI 10.1378/chest.100.5.1264
This information is current as of July 10, 2011
Updated Information & Services
Updated Information and services can be found at:
http://chestjournal.chestpubs.org/content/100/5/1264
Cited Bys
This article has been cited by 9 HighWire-hosted articles:
http://chestjournal.chestpubs.org/content/100/5/1264#related-urls
Permissions & Licensing
Information about reproducing this article in parts (figures, tables) or in its entirety can be found
online at:
http://www.chestpubs.org/site/misc/reprints.xhtml
Reprints
Information about ordering reprints can be found online:
http://www.chestpubs.org/site/misc/reprints.xhtml
Citation Alerts
Receive free e-mail alerts when new articles cite this article. To sign up, select the "Services" link to
the right of the online article.
Images in PowerPoint format
Figures that appear in CHEST articles can be downloaded for teaching purposes in PowerPoint
slide format. See any online figure for directions.
Downloaded from chestjournal.chestpubs.org by guest on July 10, 2011
© 1991 American College of Chest Physicians
View publication stats
You might also like
- Pleural Disease NEJM 2018 PDFDocument12 pagesPleural Disease NEJM 2018 PDFPanayiotis StavroulakisNo ratings yet
- Case Study Presentation FroehlichDocument27 pagesCase Study Presentation Froehlichapi-499098722100% (1)
- Check - Unit - 554 - October - Renal - Problems V2 PDFDocument26 pagesCheck - Unit - 554 - October - Renal - Problems V2 PDFdragon660% (1)
- Zapper Frequency Generator Hulda Clark Royal RifeDocument48 pagesZapper Frequency Generator Hulda Clark Royal RifeAleksandar SavićNo ratings yet
- Nej MR A 1403503Document12 pagesNej MR A 1403503vian viNo ratings yet
- Enfermedades Pleurales NEJM 2018Document12 pagesEnfermedades Pleurales NEJM 2018rene.javier.96No ratings yet
- Pleural DiseaseDocument12 pagesPleural DiseaseEdgar Romero RamirezNo ratings yet
- Paper Alumnos 6Document12 pagesPaper Alumnos 6Victor Martinez HagenNo ratings yet
- Dupuytren's DiseaseDocument10 pagesDupuytren's DiseaseMiguel JohnsonNo ratings yet
- 14 PDFDocument12 pages14 PDFeliasNo ratings yet
- Antinuclear, Antibodies in A Man. Shoulder Pain, Pleural Effusion, and PositiveDocument4 pagesAntinuclear, Antibodies in A Man. Shoulder Pain, Pleural Effusion, and PositiveandreasgiannNo ratings yet
- Hydrophobia (Fear of Fluids) in Septic Shock Does Not PayDocument2 pagesHydrophobia (Fear of Fluids) in Septic Shock Does Not PayGabriela PachecoNo ratings yet
- UiA V 27 2011Document68 pagesUiA V 27 2011Roy ANo ratings yet
- Effects of Parentereal Hydration in Terminally Ill Cancer Patients A Preleminary StudyDocument6 pagesEffects of Parentereal Hydration in Terminally Ill Cancer Patients A Preleminary StudyCristian Meza ValladaresNo ratings yet
- Exploring The Spectrum of GERD: Myths and Realities: Special ArticleDocument9 pagesExploring The Spectrum of GERD: Myths and Realities: Special ArticleedopriyantomoNo ratings yet
- Implementation and Analysis of A Free Water Protocol in Acute Trauma and Stroke PatientsDocument9 pagesImplementation and Analysis of A Free Water Protocol in Acute Trauma and Stroke PatientsDewie DeblongNo ratings yet
- Nephrology Quiz and Questionnaire: 2009: Special FeatureDocument20 pagesNephrology Quiz and Questionnaire: 2009: Special Featuresunnyrock746No ratings yet
- Medical Conference: Crohn DiseaseDocument9 pagesMedical Conference: Crohn DiseasetiaraNo ratings yet
- Parenteral Hydration in Patients With Advanced CancerDocument8 pagesParenteral Hydration in Patients With Advanced CancerAna Leticia RibeiroNo ratings yet
- Nejme 2400189Document3 pagesNejme 2400189carb0ne14rNo ratings yet
- Deshidratación y DisfaciaDocument13 pagesDeshidratación y DisfaciaALENo ratings yet
- Bronchopulmonary Dysplasia: An Update: Anita Bhandari and Vineet BhandariDocument5 pagesBronchopulmonary Dysplasia: An Update: Anita Bhandari and Vineet BhandariPatricius Berry Harsono PutraNo ratings yet
- Searle 1980Document3 pagesSearle 1980Anonymous FAyZgchPr6No ratings yet
- 2007 Leprosy Review Classifying Leprosy Patients - Searching For The Perfect SolutionDocument4 pages2007 Leprosy Review Classifying Leprosy Patients - Searching For The Perfect SolutionJorge RicardoNo ratings yet
- Hypothyroidsm and Thyroid Hyperplasia in Patients Treated With CobaltDocument5 pagesHypothyroidsm and Thyroid Hyperplasia in Patients Treated With CobaltdesNo ratings yet
- Dyspnea-Applying Research To Bedside Practice-AACN 2007Document14 pagesDyspnea-Applying Research To Bedside Practice-AACN 2007Emiliano ManginoNo ratings yet
- Perinatal Transient Myeloproliferative Disorder in Trisomy 21Document11 pagesPerinatal Transient Myeloproliferative Disorder in Trisomy 21Carina SuarezNo ratings yet
- Purpura SCDocument6 pagesPurpura SCJosefina RodriguezNo ratings yet
- The Dandy Walker Variant A Case Series of 24 Pediatric PatientsDocument7 pagesThe Dandy Walker Variant A Case Series of 24 Pediatric PatientsWilliam HartantoNo ratings yet
- Renal Replacement Therapy Review: Past, Present and FutureDocument11 pagesRenal Replacement Therapy Review: Past, Present and FuturerkNo ratings yet
- Severitat IctericiaDocument1 pageSeveritat Ictericiaanollaru38No ratings yet
- Letters To The Editor: Comparison of Outcome Measures in Patients With CopdDocument3 pagesLetters To The Editor: Comparison of Outcome Measures in Patients With CopdAndreea GociuNo ratings yet
- Clinical and Radiological Features of Incarcerated Hernia K7n3y0reDocument5 pagesClinical and Radiological Features of Incarcerated Hernia K7n3y0reAndhika Reza AkbarNo ratings yet
- Fisiopatología de La Fibrosis Pulmonar Idiopática: June 2016Document5 pagesFisiopatología de La Fibrosis Pulmonar Idiopática: June 2016Joel Canaza FloresNo ratings yet
- Case Study Congenital Diaphragmatic Hernia in Post Neonatal PeriodDocument3 pagesCase Study Congenital Diaphragmatic Hernia in Post Neonatal PeriodAhmed ElhadiNo ratings yet
- Commercial Premixed Parenteral Nutrition and Its Potential Role in PediatricsDocument5 pagesCommercial Premixed Parenteral Nutrition and Its Potential Role in PediatricsLilik FitrianaNo ratings yet
- Dengue Hemorrhagic Fever Complicated by PancreatitisDocument3 pagesDengue Hemorrhagic Fever Complicated by PancreatitisLaras SetyowatiNo ratings yet
- Assessment of Coma and Impaired Consciousness - Glasgow ScaleDocument4 pagesAssessment of Coma and Impaired Consciousness - Glasgow ScalekarlunchoNo ratings yet
- Dysphagia After Stroke and Its ManagementDocument2 pagesDysphagia After Stroke and Its ManagementAbdul AzeezNo ratings yet
- Hellp Syndrom 3Document6 pagesHellp Syndrom 3wanty arruanNo ratings yet
- Two Case Reports of Successful Treatment of Cholestasis With Steroids in Patients With PFIC-2Document9 pagesTwo Case Reports of Successful Treatment of Cholestasis With Steroids in Patients With PFIC-2AstiaNingrumSanjayaNo ratings yet
- PIIS0085253817308104Document3 pagesPIIS0085253817308104Freddy Shanner Chávez VásquezNo ratings yet
- Air Medical JournalDocument4 pagesAir Medical JournalKarenNo ratings yet
- Frozen Shoulder5B15DDocument15 pagesFrozen Shoulder5B15DTri Ayu AstutiNo ratings yet
- Branski2002 PDFDocument6 pagesBranski2002 PDFlakjdlkaNo ratings yet
- Fisiopatologiafpi Ernstgycol PDFDocument5 pagesFisiopatologiafpi Ernstgycol PDFJean TiceranNo ratings yet
- Case Report: Saudi Journal of Kidney Diseases and TransplantationDocument4 pagesCase Report: Saudi Journal of Kidney Diseases and TransplantationWilber Roberto Ticona MamaniNo ratings yet
- Sdubba 1995 Oral LeukoplakiaDocument14 pagesSdubba 1995 Oral LeukoplakiaKarma YogaNo ratings yet
- Daniels Defining Dysphagia Ajslp2009Document9 pagesDaniels Defining Dysphagia Ajslp2009Ignacio AndresNo ratings yet
- Nej MC 2201160Document3 pagesNej MC 2201160Πάνος ΣταγήςNo ratings yet
- CDH Modern MX PDFDocument12 pagesCDH Modern MX PDFThia SanjayaNo ratings yet
- Tongue-Tied: Management in Pierre Robin Sequence: September 2017Document6 pagesTongue-Tied: Management in Pierre Robin Sequence: September 2017Mohamed AlaaNo ratings yet
- Swallowing Dysfunction After Critical IllnessDocument9 pagesSwallowing Dysfunction After Critical IllnessGisele DiasNo ratings yet
- Characterization of Pediatric Patients Diagnosed With Post-Infectious Bronchiolitis Obliterans 2600 Meters Above Sea LevelDocument8 pagesCharacterization of Pediatric Patients Diagnosed With Post-Infectious Bronchiolitis Obliterans 2600 Meters Above Sea LevelazevedoNo ratings yet
- Arpa.2018 Duodenal PolypsDocument17 pagesArpa.2018 Duodenal PolypsAndrei PatrichiNo ratings yet
- The Differential DiagnosisDocument8 pagesThe Differential DiagnosisKomang SumertawanNo ratings yet
- Alzheimer S Dementia - 2023 - BowmanDocument12 pagesAlzheimer S Dementia - 2023 - BowmanPaulHerreraNo ratings yet
- Acute Diarrhea in Children Thomas G. DeWittDocument10 pagesAcute Diarrhea in Children Thomas G. DeWittabdalballah1151No ratings yet
- Cronica InfantDocument4 pagesCronica InfantDdCasadoLasterosNo ratings yet
- MDZ e DispnéiaDocument10 pagesMDZ e DispnéiaThaísa NogueiraNo ratings yet
- Barretts Esophagus - A ReviewDocument14 pagesBarretts Esophagus - A ReviewVytautas LiutvinasNo ratings yet
- 2013 Pneumonia Due To Multidrug-Resistant Leclercia AdecarboxylataDocument3 pages2013 Pneumonia Due To Multidrug-Resistant Leclercia AdecarboxylataLexotanyl LexiNo ratings yet
- Saline Therapy: Clinical Treatises on the Pathology and Therapy of Disorders of Metabolism and NutritionFrom EverandSaline Therapy: Clinical Treatises on the Pathology and Therapy of Disorders of Metabolism and NutritionNo ratings yet
- Virology: Herpesviruses II: Herpes SimplexDocument4 pagesVirology: Herpesviruses II: Herpes SimplexJaz CNo ratings yet
- Brain TumorDocument1 pageBrain TumorChase XerolfNo ratings yet
- Patient Characteristics Associated With Aggression in Mental Health UnitsDocument5 pagesPatient Characteristics Associated With Aggression in Mental Health Unitssurya rakhmat hidayat100% (1)
- KodigotuDocument5 pagesKodigotuClark RomandaNo ratings yet
- Received: 17/4/19 Accepted: 13/6/19Document5 pagesReceived: 17/4/19 Accepted: 13/6/19UMYU Journal of Microbiology Research (UJMR)No ratings yet
- 152-155 Valerio Milana DefDocument4 pages152-155 Valerio Milana DefVikas DeepNo ratings yet
- 1 - Biochemistry Notes by Dr. M A Bari Siddiqui: DrmentorsDocument2 pages1 - Biochemistry Notes by Dr. M A Bari Siddiqui: DrmentorsShiva KumarNo ratings yet
- Clark County School District Student Health Information For School YearDocument2 pagesClark County School District Student Health Information For School YearDrake JauchNo ratings yet
- Case Study On Preterm LaborDocument81 pagesCase Study On Preterm Laborkarl montanoNo ratings yet
- Pseudofollicular BabaeDocument13 pagesPseudofollicular BabaeOlamide EstherNo ratings yet
- Curriculum For Phase - 2 MBBS PDFDocument94 pagesCurriculum For Phase - 2 MBBS PDFVamsi ChakradharNo ratings yet
- Clinical Teaching Plan SampleDocument9 pagesClinical Teaching Plan SampleElaine RetesNo ratings yet
- Dental WorkforceDocument18 pagesDental Workforcesobiaarshad2004No ratings yet
- 2013 Mo Dental PaperDocument22 pages2013 Mo Dental Paperarmrest.drill.0rNo ratings yet
- Heart Failure Infographic - Long Version - v1.0Document1 pageHeart Failure Infographic - Long Version - v1.0Oana-Adriana DutaNo ratings yet
- Nutritional Disorders: Dr-Nabiha Najati MBCHB, CABP, 2018-2019Document28 pagesNutritional Disorders: Dr-Nabiha Najati MBCHB, CABP, 2018-2019tanishqsaxena100210No ratings yet
- Uts FinalsDocument9 pagesUts Finalsmaxi dmNo ratings yet
- Skin Cancer: Dedicated To: Carlos Garcia MD Dermatology at OuhscDocument44 pagesSkin Cancer: Dedicated To: Carlos Garcia MD Dermatology at OuhscabrarashrafNo ratings yet
- USMLE Step 2 (3) - Thyroid DiseaseDocument4 pagesUSMLE Step 2 (3) - Thyroid DiseaseMavra zNo ratings yet
- Insulin and Oral Hypoglycemic DrugsDocument45 pagesInsulin and Oral Hypoglycemic DrugsRamadi PrameelaNo ratings yet
- Poly Ester Putty MsdsDocument8 pagesPoly Ester Putty MsdsJISHNU TKNo ratings yet
- Wound CareDocument7 pagesWound CareJJNo ratings yet
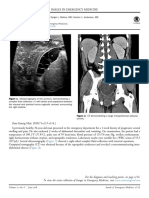
- 0196-0644/$-See Front Matter: 71, No. 6: June 2018 Annals of Emergency MedicineDocument2 pages0196-0644/$-See Front Matter: 71, No. 6: June 2018 Annals of Emergency MedicineTeja Laksana NukanaNo ratings yet
- State Fact Sheet West Bengal: National Family Health Survey - 5Document7 pagesState Fact Sheet West Bengal: National Family Health Survey - 5Rounak DasNo ratings yet
- Constructivist Approach in Medical Education PDFDocument6 pagesConstructivist Approach in Medical Education PDFulices quintanaNo ratings yet
- Universidad Peruana Cayetano Heredia: Facultad de Medicina Veterinaria y ZootecniaDocument48 pagesUniversidad Peruana Cayetano Heredia: Facultad de Medicina Veterinaria y ZootecniaJose Luis Jaen RamosNo ratings yet
- Keissa Davis Operating Room ExperienceDocument2 pagesKeissa Davis Operating Room ExperiencePatricia Marie Laman YadaoNo ratings yet