Professional Documents
Culture Documents
Prevalence of Helicobacter Pylori Among Nigerian Patients With Dyspepsia in Ibadan
Uploaded by
Tayo ShoyoyeOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Prevalence of Helicobacter Pylori Among Nigerian Patients With Dyspepsia in Ibadan
Uploaded by
Tayo ShoyoyeCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/204948718
Prevalence of Helicobacter pylori among Nigerian patients with dyspepsia in
Ibadan
Article in Pan African Medical Journal · September 2010
DOI: 10.4314/pamj.v6i1.69090 · Source: PubMed
CITATIONS READS
94 3,057
5 authors, including:
Abiodun Christopher Jemilohun Jesse A Otegbayo
Babcock University/Babcock University Teaching Hospital, Nigeria University of Ibadan/University College Hospial, Ibadan
39 PUBLICATIONS 331 CITATIONS 186 PUBLICATIONS 2,452 CITATIONS
SEE PROFILE SEE PROFILE
Samuel Ola Abideen O Oluwasola
61 PUBLICATIONS 887 CITATIONS
University of Ibadan
111 PUBLICATIONS 1,397 CITATIONS
SEE PROFILE
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Infectious Diseases View project
CRC in West Africa View project
All content following this page was uploaded by Abiodun Christopher Jemilohun on 01 June 2014.
The user has requested enhancement of the downloaded file.
Provisional PDF
Published September 20, 2010
Research, Volume 6, Issue 18, 2010
Prevalence of helicobacter pylori among Nigerian patients with dyspepsia in
Ibadan
Abiodun Christopher Jemilohun1,&, Jesse Abiodun Otegbayo2, Samuel Olawale Ola, Olayiwola
Abideen Oluwasola3, Adegboyega Akere2
1
Department of Medicine, Ladoke Akintola University of Technology Teaching Hospital, Oshogbo, Nigeria,
2
Department of Medicine, College of Medicine, University of Ibadan and University College Hospital,
Ibadan, Nigeria, 3Department of Morbid Anatomy and Histopathology, College of Medicine, University of
Ibadan and University College Hospital, Ibadan, Nigeria
&
Corresponding author
Abiodun Christopher Jemilohun, Department of Medicine, Ladoke Akintola University of Technology
Teaching Hospital, Oshogbo, phone: +2348038674623, P.M.B. 5000, Oshogbo, Osun State, Nigeria
Abstract
INTRODUCTION: Determination of the true prevalence of Helicobacter pylori (H. pylori) is difficult in a hyper-
endemic area like Nigeria with use of serological tests because of their low discriminatory power between previous
and current infections. The use of biopsy based methods will go a long way to mitigate this problem. We investigated
the prevalence of H. pylori in dyspeptic patients and its relationship with gastroduodenal pathologies using gastric
biopsy histology and rapid urease test. METHODS: Eighty-six consecutive adult patients with dyspepsia underwent
upper gastrointestinal endoscopy using forward-viewing endoscopes. Antral biopsy specimens were collected for
histology and rapid urease test. Diagnosis of H. pylori infection was made if both or either of the tests was positive.
RESULTS: Of the 86 subjects, there were 39 (45.3%) males and 47(54.7%) females. The age range was 23 to 85
years with a mean of 49.19±13.75 years. Diagnosis of H. pylori was made in 55(64%) patients. Gastritis was the
commonest endoscopic finding (60.5%), serious gastroduodenal pathology (gastric ulcer, duodenal ulcer and gastric
cancer) were documented in only 12 (14%) patients. Thirty three (63.5%) of the 55 patients with gastritis had H.
Page number not for citation purposes 1
pylori infection while 7(58.3%) of the 12 patients with serious gastroduodenal lesions had the infection. Thirteen
(72.2%) of the 18 patients that had normal endoscopic findings were H. pylori positive. CONCLUSION: The
prevalence of H. pylori among dyspeptics using biopsy based methods is high in the South-Western part of Nigeria. It
is therefore important to test and treat H. pylori among Nigerians with dyspepsia.
Introduction
The discovery of Helicobacter pylori (H. pylori) by Warren and Marshall, in 1983 was a major
breakthrough in the management of dyspepsia [1]. H. pylori is a gram negative, spiral, flagellated
bacterium with a capability for abundant urease production which has been implicated in several upper
gastrointestinal diseases that present as dyspepsia [2,3]. The organism is usually found under the mucus
layer in the gastric pits in close apposition to gastric epithelial cells where it causes damage to the cells
[4]. It is a major aetiological factor in chronic gastritis, peptic ulcer disease, gastric carcinoma, and
gastric mucosal associated lymphoid tissue (MALT) lymphoma [2,3]. Peptic ulcer disease is now viewed
as an infectious disease since eradication of H. pylori leads to its cure [4].
Various diagnostic tests for H. pylori have been developed and they can be broadly classified into invasive
and non-invasive tests [4]. Invasive tests utilize endoscopic biopsy samples for histology, culture, rapid
urease test (RUT) and polymerase chain reaction. All these tests have been found to have sensitivity and
specificity that are well above 90% [5].
The non-invasive tests do not require endoscopy. These include urea breath test (UBT), immunoglobulin
G and M serology, stool antigen test, saliva antibody test and urinary antibody test [4]. In Nigeria, the
non-invasive tests are not generally available except Immunoglobulin G (IgG) serology. The value of
serological tests in a hyper-endemic area like Nigeria is limited, because of their low discriminatory power
between previous and current infection.
The aim of this study was to determine the prevalence of H. pylori among dyspeptic patients seen at the
University College Hospital, Ibadan and its association with gastroduodenal pathologies using gastric
biopsy histology and rapid urease test. The hospital serves as a referral centre for a substantial part of
the South-Western region of Nigeria.
Page number not for citation purposes 2
Methods
The study was carried out at the Endoscopy sub-unit of the Gastrointestinal & Liver Unit, Department of
Medicine, University College Hospital (UCH), Ibadan, Nigeria.
Ethical clearance was sought and obtained from the Joint University of Ibadan/ University College
Hospital Institutional Review Committee. Eighty-six consecutive adult patients with dyspeptic symptoms
undergoing endoscopy from April 2008 to February 2009 were recruited after obtaining informed consent
from them. Patients who were previously treated for H. pylori infection or who had received antibiotics,
proton pump inhibitors or bismuth compounds in the preceding 4 weeks were excluded. Base line bio-
data were obtained.
Oesophago-gastro-duodenoscopy (OGD) was performed on all the participants using Olympus (GFI-
XQ20) or Pentax (FG29W) forward-viewing Oesophago-gastro-duodenoscope. Endoscopic features of
each patient were recorded. Endoscopic appearance was considered normal if the mucosal was pink in
colour, smooth and lustrous. Two gastric antral mucosal biopsies were taken for each of RUT and
histology. A diagnosis of H. pylori infection was made when both or one of these two tests was positive.
Rapid urease test (RUT)
Two of the four antral biopsies taken from each patient were used immediately for RUT using GUT-plus
by Albyn medical, Smart Medical Group,UK. GUT plus is a new generation RUT kit that consists of two dry
filter paper containing urea and phenol red (a pH indicator) in a sealed plastic slide. If the urease enzyme
of H. pylori is present in an inserted tissue sample, the resulting decomposition of urea to CO2 and NH3
causes the pH to rise and the colour of the dot turns from yellow to a bright magenta. Results were read
within 3 hours after sampling according to the manufacturer’s specification. Colour change from yellow to
magenta was considered a positive result while no colour change was regarded as negative.
Histology
The other two antral biopsies were fixed in 10% formaldehyde and transferred to the histopathology
laboratory for processing. Four micron thick paraffin sections were stained with routine Haematoxylin and
Eosin for detection of H. pylori and gastritis. Giemsa stain was also used for better yield. Slides were
examined microscopically for H. pylori by the Pathologist. Presence of Helicobacter-like organisms was
regarded as positive while absence was regarded as negative.
Page number not for citation purposes 3
Data analysis
Data was analyzed using Statistical Package for Social Sciences, version16.0 (SPSS Inc. Chicago Illinois).
Results were presented as means ± standard deviation for quantitative variables and number
(percentages) for qualitative variables.
Categorical variables were compared with Pearson’s Chi-square. Significant P-value was taken as <0.01.
Results
There were 39 (45.3%) males and 47(54.7%) females. The mean age was 49.19 (±13.75) years. The
age ranged from 23 to 85 years. Forty-five (52.35%) and 52 (60.5 %) patients were H. pylori positive
with histology and RUT respectively. Fifty-five (64%) patients were positive when results of both tests
were combined.
The most common abnormality at endoscopy was gastritis which was seen in 52 (60.5%) patients,
followed by duodenitis 16(18.6%) and doudenogastric reflux 14(16.3%). Gastric ulcer (GU) was recorded
in 8(9.3%) patients, 7(8.1%) patients had oesophagitis, while 3(3.5%) and 2(2.3%) patients had gastric
cancer and duodenal ulcer (DU) respectively. Serious gastroduodenal pathologies (GU, DU and gastric
cancer) were documented in only 12 (14%) patients. It is noteworthy however, that there was a
considerable overlap in the endoscopic findings in these subjects as many of them with other endoscopic
lesions also had gastritis.
Sixty-eight (79.1%) patients had endoscopically identifiable cause for their dyspepsia while the remaining
18(20.9%) had normal endoscopic findings. Forty -two (76.4%) patients among those with abnormal
endoscopic appearance had H. pylori while 13 (72.2%) of those with normal endoscopic findings were
positive for the organism. There was no significant difference (P-value = 0.41) between the frequency of
H. pylori among those with endoscopic abnormality and those with normal findings. Table 1 shows the
spectrum of endoscopic findings, while table 2 shows the association between H. pylori status and the
presence of endoscopic abnormality.
The association between H. pylori status and various endoscopic abnormalities is depicted in table 3.
33(63.5%) out of the 52 patients with gastritis had H. pylori infection, while 8 (50%) out of 16 and
7(58.3%) out of 12 patients with duodenitis and serious gastrointestinal lesions respectively had H. pylori
infection. These relationships however were not statistically significant.
Page number not for citation purposes 4
Discussion
In this study, H. pylori was diagnosed in 64% of the patients. This is consistent with results of previous
studies conducted in Nigeria and other parts of West Africa which have consistently shown a high
prevalence of H. pylori with the use of biopsy based methods [6-11]. Previous studies conducted in
various parts of South-Western Nigeria (including the University College Hospital, Ibadan) in which
patients were investigated for H. pylori with the use of either histology or campylobacter-like organism
(CLO) test showed prevalence rates of 60.5% to 73% [6,7,12] . Seroprevalence studies conducted in the
same region showed prevalence rates as high as 88% to 94.5% [3,13]. These are not unexpected in a
hyper-endemic area like Nigeria since serological tests cannot discriminate between previous and current
infections. The sero-prevalence assay’s IgG antibody lasts for up to 3 years or more in the serum even
after the organism has been eradicated.
The most common identifiable lesion at endoscopy in this study was gastritis which had a frequency of
60.5%. This is comparable to a frequency of 60% obtained in a previous study conducted in the North-
Eastern part of Nigeria [9]. An earlier study conducted at the University College Hospital, Ibadan showed
a frequency of 13.4% for gastritis while normal mucosal was the commonest finding with a frequency of
53% [14]. This disparity may be as a result of a change in the pattern of presentation of endoscopic
lesions among patients with dyspepsia in more than two decades after the conduct of the previous study.
Our study showed that despite the high prevalence of H. pylori infection in the South-Western part of
Nigeria, the prevalence of serious gastroduodenal pathologies (GU, DU and gastric cancer) was low as
these lesions were documented in only 14% of all the patients. This is consistent with findings of
previous studies conducted at the same centre and in the North-Eastern part of Nigeria [9,14].
In addition, this study showed that 63.5% of patients with endoscopic gastritis had H. pylori infection.
This is consistent with previous studies in Nigeria that showed a high prevalence of H. pylori among
patients with gastritis [6,9]. Also, among patients with serious gastroduodenal pathologies (GU, DU and
gastric cancer) 58.3% had H. pylori infection. This finding corroborates the results from similar studies
conducted in Nigeria and other parts of Africa [6,8,9,15]. Although the association of these lesions with
H. pylori infection was not statistically significant, a further study involving a larger number of patients is
needed to establish the true association between the infection and the lesions.
It was noted that 13 (72.2%) of the 18 subjects with normal endoscopic findings were positive for H.
pylori and no statistically significant difference existed in the frequency of H. pylori infection among
Page number not for citation purposes 5
patients with abnormal endoscopic findings and those with normal findings . This could be explained by
the very high H. pylori prevalence among Nigerians [13,16] and may suggest that the infection was
responsible for the symptoms of dyspepsia in such patients. Hence such H. pylori positive patients should
be treated with anti-H. pylori therapy.
One major limitation of this study is that it was conducted in a hospital setting and may not be a true
representation of the prevalence of H. pylori among dyspeptics in the general population of the South-
Western Nigeria, more so, that the study was carried out only in one centre. A community study is
therefore desirable as this is usually more representative.
Conclusion
This study shows that the prevalence of H. pylori among dyspeptic patients using biopsy based methods
is high in the South-Western part of Nigeria. It also suggests that gastritis is the commonest lesion seen
at endoscopy among patients with dyspepsia and that despite the high prevalence of H. pylori infection in
the South-Western part of Nigeria, the prevalence of serious gastroduodenal pathology (GU, DU and
gastric cancer) is low. Of note is the high prevalence of H. pylori in endoscopically normal patients. It is
therefore important to test and treat H. pylori among Nigerians with dyspepsia.
Competing interests
The authors declare no competing interests.
Authors’ contributions
AC Jemilohun: conception and design of the study; collection, analysis and interpretation of data; and
manuscript write up. JA Otegbayo: oversight of all the stages of the research, participated in data
collection and manuscript write up. SO Ola: data collection and manuscript write up. A Akere: data
collection and manuscript write up OA Oluwasola: histology slide report and manuscript write up.
Page number not for citation purposes 6
Tables
Table 1: Upper gastrointestinal endoscopy findings in adult Nigerian patients with dyspepsia
Table 2: Association between H. pylori status and presence of endoscopic abnormality in adult Nigerian
patients with dyspepsia
Table 3: Association between H. pylori status and various endoscopic abnormalities in adult Nigerian
patients with dyspepsia
References
1. Talley NJ, Vakil N. Guidelines for the management of dyspepsia. Am J Gastroenterol. 2005; 100
(10): 2324-2337. This article on PubMed
2. Suerbaum S, Michetti P. Helicobacter pylori infection. N Engl J Med. 2002; 347 (15):1175-
1186. This article on PubMed
3. Oluwasola AO, Ola SO, Saliu L, Solanke TF. Helicobacter pylori infection in South Nigerians: a
serological study of dyspeptic patients and healthy individuals. West Afr J Med. 2002; 21(2):138-
141. This article on PubMed
4. Malfertheiner P, Megraud F, O'Morain C, Bazzoli F, El-Omar E, Graham D, et al. Current concepts
in the management of Helicobacter pylori infection: the Maastricht III Consensus Report. Gut.
2007; 56(6):772-781. This article on PubMed
5. Graham DY, Sung JY. Helicobacter pylori. In: Feldman M, Friedman LS, Brandt LJ, editors.
Sleisenger & Fordtran's Gastrointestinal and Liver Disease; Pathophysiology, Diagnosis,
Management
6. Ndububa DA, Agbakwuru AE, Adebayo RA, Olasode BJ, Olaomi OO, Adeosun OA, et al. Upper
gastrointestinal findings and incidence of Helicobacter pylori infection among Nigerian patients
with dyspepsia. West Afr J Med. 2001; 20(2):140-145. This article on PubMed
7. Adesanya AA, Oluwatowoju IO, Oyedeji KS, da Rocha-Afodu JT, Coker AO, Afonja OA. Evaluation
of a locally-made urease test for detecting Helicobacter pylori infection. Niger Postgrad Med J.
2002; 9(1):43-47. This article on PubMed
Page number not for citation purposes 7
8. Baako BN, Darko R. Incidence of Helicobacter pylori infection in Ghanaian patients with dyspeptic
symptoms referred for upper gastrointestinal endoscopy. West Afr J Med. 1996; 15(4):223-
227. This article on PubMed
9. Mustapha SK, Ajayi NA, Nggada HA, Pindiga UH, Bolori MT, Ndahi A, et al. Endoscopic findings
and the frequency of Helicobacter pylori among dyspeptic patients in North-Eastern Nigeria.
Highland Medical Research Journal. 2007; 5(1):78-81
10. Mbengue M, Diouf ML, Dangou JM, Ka MM, Ba-Seck A, Ndiaye MF, et al. [Frequency of
Helicobacter pylori infection in symptomatic patients in Senegal]. Med Trop (Mars). 1997;
57(3):256-258. This article on PubMed
11. Aduful HK, Naaeder SB, Darko R, Baako BN, Clegg-Lamptey JNA, Nkrumah KN, et al. Upper
Gastrointestinal Endoscopy at the Korle Bu Teaching Hospital, Accra, Ghana. Ghana Med J. 2007;
41(1):12–16. This article on PubMed
12. Ola SO, Yakubu A, Otegbayo JA, Oluwasola AO, Ogunbiyi JO, Akang EE, et al. The most
appropriate site for endoscopic biopsy for the detection of H. pylori among Nigerians in Ibadan.
West Afr J Med. This article on PubMed
13. Otegbayo JA, Oluwasola OA, Yakubu A, Odaibo GN, Olaleye OD. Helicobacter pylori serology and
evaluation of gastroduodenal disease in Nigerians with dyspepsia. Afr J Clin and Exp Microbiol.
2004; 5:126-133
14. Olubuyide IO, Atoba MA, Ayoola EA. Dyspepsia in Ibadan. Trop Geogr Med. 1989;41(4):337-
340. This article on PubMed
15. Ogutu EO, Kang'ethe SK, Nyabola L, Nyong'o A. Endoscopic findings and prevalence of
Helicobacter pylori in Kenyan patients with dyspepsia. East Afr Med J. 1998; 75(2):85-89. This
article on PubMed
16. Oluwasola AO, Ogunbiyi JO. Chronic gastritis and Helicobacter pylori infection in University
College Hospital Ibadan, Nigeria-a study of 85 fibre optic gastric biopsies. Niger J Med. 2004;
13(4):372-378. This article on PubMed
Page number not for citation purposes 8
Table 1: Upper gastrointestinal endoscopy findings in adult Nigerian patients with dyspepsia
Variables Frequency (n=86)
Present Absent
Oesophagitis 7(8.1%) 79(91.9%)
Gastritis 52(60.5%) 34(39.5%)
Gastric ulcer 8(9.3%) 78(90.7%)
Gastric cancer 3(3.5%) 83(96.5%)
Duodenal ulcer 2(2.3%) 84(97.7%)
Duodenitis 16(18.6%) 70(81.4%)
Duodenogastric reflux 14(16.3%) 72(83.7%)
Normal 18(20.9%) 68(79.1%)
Table 2: Association between H. pylori status and presence of endoscopic abnormality in adult Nigerian
patients with dyspepsia
Endoscopic abnormality(n=86)
Present Absent Total
H. pylori Positive 42 (76.4%) 13(23.6%) 55(100.0%)
Negative 26(83.9%) 5(16.1%) 31(100.0%)
Total 68(79.1%) 18(20.9%) 86(100%)
Chi-square = 0.675, df =1, P-value = 0.411
Page number not for citation purposes 9
Table 3: Association between H. pylori status and various endoscopic abnormalities in adult Nigerian
patients with dyspepsia
Variables H. pylori infection(n=86)
Positive Negative X2 P-value
Gastritis Present 33(63.5%) 19(36.5%)
Absent 22(64.7%) 12(35.3%) 0.014 0.906
Serious gastroduodenal Present 7(58.3%) 5(41.7%)
lesions+ Absent 48(35.1%) 26(64.9%) 0.191 0.662
Duodenitis Present 8(50%) 8(50.0%)
Absent 47(67.1%) 23(32.9%) 1.660 0.198
Doudenogastric reflux Present 8(57.1%) 6(42.9%)
Absent 47(65.3%) 25(34.7%) 1.336 0.562
Oesophagitis Present 6(85.7%) 1(14.3%)
Absent 49(62.0%) 30(38.0%) 1.565 0.211*
*Fisher’s exact test, +Gastric ulcer, duodenal ulcer and gastric cancer
Page number not for citation purposes 10
View publication stats
You might also like
- (pt2) CHCAGE003 Student Assessment Tool v2.1 04.04.19Document117 pages(pt2) CHCAGE003 Student Assessment Tool v2.1 04.04.19Charina Aubrey90% (10)
- Chapter 37 - Digestive System IntroductionDocument5 pagesChapter 37 - Digestive System IntroductionStaceyNo ratings yet
- Chapter 23 - Management of Patients With Chest and Lower Respiratory Tract DisordersDocument17 pagesChapter 23 - Management of Patients With Chest and Lower Respiratory Tract DisordersMary SingletonNo ratings yet
- NsoforetalDocument10 pagesNsoforetalAkinlolu ElijahNo ratings yet
- A Correlative Study of Peptic Ulcer and ThrombocytDocument5 pagesA Correlative Study of Peptic Ulcer and ThrombocytDaniel Dale Ambo SibaraniNo ratings yet
- Publication Prevalence of Anaemia2Document6 pagesPublication Prevalence of Anaemia2Samuel AdefemiNo ratings yet
- Nisebj 22 3 2022Document51 pagesNisebj 22 3 2022Clement BewajiNo ratings yet
- 2019IJAR2Document6 pages2019IJAR2goenz79No ratings yet
- Grados de GastritisDocument7 pagesGrados de Gastritisrafael santamaríaNo ratings yet
- 15 ArticleText 47 1 10 20211130Document32 pages15 ArticleText 47 1 10 20211130FavourjiNo ratings yet
- JournalDocument10 pagesJournalRhea SaglesNo ratings yet
- 216-Original Article-685-1-10-20240216Document7 pages216-Original Article-685-1-10-20240216Noe Essono KolloNo ratings yet
- Phytochemical Screening and Antibacterial Activity of Cnidoscolus Aconitifolius and Associated Changes in Liver Enzymes in Wistar RatsDocument8 pagesPhytochemical Screening and Antibacterial Activity of Cnidoscolus Aconitifolius and Associated Changes in Liver Enzymes in Wistar RatsFeroniaNo ratings yet
- Femi OgundeleDocument8 pagesFemi OgundeleAbdullahi nurudeenNo ratings yet
- Biokemistri Volume 31, Number 2Document43 pagesBiokemistri Volume 31, Number 2Clement BewajiNo ratings yet
- Biokemistri Volume 33, Number 1Document94 pagesBiokemistri Volume 33, Number 1Clement BewajiNo ratings yet
- The Effect of Smoking On Fertility Hormones in Male Adult Smokers in South-South NigeriaDocument7 pagesThe Effect of Smoking On Fertility Hormones in Male Adult Smokers in South-South NigeriaHenny WijayaNo ratings yet
- Public KnowledgeDocument7 pagesPublic KnowledgeSaad aliraqiNo ratings yet
- International Journal of International Journal of International Journal ofDocument6 pagesInternational Journal of International Journal of International Journal ofDeepak KumarNo ratings yet
- Rabies Vaccines Its Role Challenges Considerationsand ImplicationsforDocument27 pagesRabies Vaccines Its Role Challenges Considerationsand ImplicationsforNimra Naveed ShaikhNo ratings yet
- Epidemiology of Shigellosis in Lagos Nigeria TrendDocument9 pagesEpidemiology of Shigellosis in Lagos Nigeria TrendAlexander AbahNo ratings yet
- Comprehensive Lipid and Lipid-Related Gene Investigations of Host Immune Responses To Characterize Metabolism-Centric Biomarkers For Pulmonary TuberculosisDocument15 pagesComprehensive Lipid and Lipid-Related Gene Investigations of Host Immune Responses To Characterize Metabolism-Centric Biomarkers For Pulmonary TuberculosisMinh PhanNo ratings yet
- Serologic and Urine Diagnostic Tests To Detect Helicobacter Pylori Infection in Functional Dyspepsia PatientsDocument5 pagesSerologic and Urine Diagnostic Tests To Detect Helicobacter Pylori Infection in Functional Dyspepsia PatientsAnasthasia hutagalungNo ratings yet
- Prevalence of Malnutrition Among Pre-School Children In, South-East NigeriaDocument6 pagesPrevalence of Malnutrition Among Pre-School Children In, South-East NigeriadsNo ratings yet
- JI Perpetua, Marco Paolo (Bacterial Isolates and Their Antimicrobial Susceptibility Patterns Among Pediatric Patients With Urinary Tract Infections)Document9 pagesJI Perpetua, Marco Paolo (Bacterial Isolates and Their Antimicrobial Susceptibility Patterns Among Pediatric Patients With Urinary Tract Infections)Marco Paolo Arcayera PerpetuaNo ratings yet
- An Outbreak of Colibacillosis in A Broiler Farm: ArticleDocument8 pagesAn Outbreak of Colibacillosis in A Broiler Farm: ArticleDewa Aix61No ratings yet
- Biokemistri Volume 32, Number 2Document75 pagesBiokemistri Volume 32, Number 2Clement BewajiNo ratings yet
- Siupsinskiene Hpylori Archives 2013Document9 pagesSiupsinskiene Hpylori Archives 2013Nurul HidayatiNo ratings yet
- The Clinical Spectrum of Chronic Diarrhea in ChildrenDocument15 pagesThe Clinical Spectrum of Chronic Diarrhea in ChildrenInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Training Report. Kipps (Repaired) Wariongo (Final) )Document47 pagesTraining Report. Kipps (Repaired) Wariongo (Final) )George KipkoechNo ratings yet
- Radioiodine TherapyDocument5 pagesRadioiodine Therapyaccime24No ratings yet
- Synovial Membrane Protein Expression Differs Between Juvenile Idiopathic Arthritis Subtypes in Early DiseaseDocument14 pagesSynovial Membrane Protein Expression Differs Between Juvenile Idiopathic Arthritis Subtypes in Early DiseaseHosne araNo ratings yet
- Nakalema Et Al IAA Journal of Biological Sciences 9 (1) :61-79, 2022. ISSN: 2636-7254 ©iaajournalsDocument19 pagesNakalema Et Al IAA Journal of Biological Sciences 9 (1) :61-79, 2022. ISSN: 2636-7254 ©iaajournalsKIU PUBLICATION AND EXTENSIONNo ratings yet
- Cuppa Wao Journal ProofsDocument22 pagesCuppa Wao Journal ProofsFajar SetiawanNo ratings yet
- Nisebj 21 2 2021Document39 pagesNisebj 21 2 2021Clement BewajiNo ratings yet
- English-Yoruba Glossary of HIV, AIDS and Ebola-Related TermsDocument287 pagesEnglish-Yoruba Glossary of HIV, AIDS and Ebola-Related TermstemmyNo ratings yet
- Defective Homeostasis As A Dysfunctional Basis of DiseaseDocument26 pagesDefective Homeostasis As A Dysfunctional Basis of DiseaseG ElegansNo ratings yet
- Influence of Age and Gender On The QuantificationDocument7 pagesInfluence of Age and Gender On The QuantificationInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Robert Proposal 4Document26 pagesRobert Proposal 4Brian RuttoNo ratings yet
- Blood Research and DisordersDocument5 pagesBlood Research and Disordersdr_joe23No ratings yet
- E Cacy of Combined Crude Extract of Curcuma Longa and Moringa Oleifera in The Prevention of Peptic Ulcer in Al..Document10 pagesE Cacy of Combined Crude Extract of Curcuma Longa and Moringa Oleifera in The Prevention of Peptic Ulcer in Al..sunita thakurNo ratings yet
- Prevalence and Chemotherapy of Enterotoxemia (Clostridium Perfringens) in Diarrheic Sheep and GoatsDocument12 pagesPrevalence and Chemotherapy of Enterotoxemia (Clostridium Perfringens) in Diarrheic Sheep and GoatsErnesto VersailleNo ratings yet
- Anti-Diarrhea Potential and Acute ToxiciDocument7 pagesAnti-Diarrhea Potential and Acute Toxicirhoxane tanohNo ratings yet
- Guidelines For The Diagnosis and Treatment of Helicobacter Pylori Infection in Korea, 2013 Revised EditionDocument24 pagesGuidelines For The Diagnosis and Treatment of Helicobacter Pylori Infection in Korea, 2013 Revised EditionRobert UntaruNo ratings yet
- OmskDocument6 pagesOmskrizkia361No ratings yet
- Management of Feline Idiopathic Cystitis (FIC) Using Probiotic Combination TreatmentDocument4 pagesManagement of Feline Idiopathic Cystitis (FIC) Using Probiotic Combination TreatmentMelita Nono LebangNo ratings yet
- Phyllantus ADocument7 pagesPhyllantus APetisa OrNo ratings yet
- Endoscopic Findings of The Gastric Mucosa During Long Term Use of Proton Pump Inhibitor A Multicenter StudyDocument6 pagesEndoscopic Findings of The Gastric Mucosa During Long Term Use of Proton Pump Inhibitor A Multicenter StudySamuel0651No ratings yet
- H PyloriDocument8 pagesH PyloriHabtamu WondifrawNo ratings yet
- Opp paraDocument5 pagesOpp paraomuhweziNo ratings yet
- Challengesof Exclusive Breastfeedingamong Working Class Womenina Teaching Hospital South East NigeriaDocument11 pagesChallengesof Exclusive Breastfeedingamong Working Class Womenina Teaching Hospital South East NigeriaChika JonesNo ratings yet
- Normal CD4 Count Range Among Healthy Nigerian Population in IlorinDocument7 pagesNormal CD4 Count Range Among Healthy Nigerian Population in IlorinLaila Kurnia PramonoNo ratings yet
- Atlas of Inflammatory Bowel DiseasesFrom EverandAtlas of Inflammatory Bowel DiseasesWon Ho KimNo ratings yet
- 1354796956-Harunaetal 312012EJMP2220Document14 pages1354796956-Harunaetal 312012EJMP2220Lina WinartiNo ratings yet
- Clinical and Gross Pathological Findings of Johne's Disease in A Calf: A Case ReportDocument6 pagesClinical and Gross Pathological Findings of Johne's Disease in A Calf: A Case ReportSanjay KumarNo ratings yet
- Issue03 41 20220Document8 pagesIssue03 41 20220NealNo ratings yet
- A Clinicopathological Study of Cholelithiasis in An Eastern Indian PopulationDocument7 pagesA Clinicopathological Study of Cholelithiasis in An Eastern Indian PopulationMeyva SasmitaNo ratings yet
- Nutritional Epidemiology ILSIDocument46 pagesNutritional Epidemiology ILSIstevanya britneyNo ratings yet
- Biokemistri Volume 32, Number 1Document95 pagesBiokemistri Volume 32, Number 1Clement BewajiNo ratings yet
- Comparative Assessment of Malaria Rapid Diagnostic Tests (RDT) in Ibadan, NigeriaDocument8 pagesComparative Assessment of Malaria Rapid Diagnostic Tests (RDT) in Ibadan, NigeriaSegunNo ratings yet
- Association of Virulence Genes With Antibiotic Resistance in Pakistani Uropathogenic E. Coli IsolatesDocument6 pagesAssociation of Virulence Genes With Antibiotic Resistance in Pakistani Uropathogenic E. Coli Isolateskhurry testNo ratings yet
- Haematologicalandbiochemicalprofilesof ClariasDocument12 pagesHaematologicalandbiochemicalprofilesof ClariasEmmanuel OwonaNo ratings yet
- Efficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaDocument5 pagesEfficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaNoraine Princess TabangcoraNo ratings yet
- Ocd StrategiesDocument7 pagesOcd StrategiesJoseph MeyersonNo ratings yet
- SEX CHANGE - Physically Impossible, Psychosocially Unhelpful, and Philosophically MisguidedDocument63 pagesSEX CHANGE - Physically Impossible, Psychosocially Unhelpful, and Philosophically MisguidedAntonio Bernard33% (3)
- Mẫu giấy KSK song ngữDocument3 pagesMẫu giấy KSK song ngữNguyen LawlietNo ratings yet
- 1309 Ovestin 1332242478Document9 pages1309 Ovestin 1332242478neleatucicovshiiNo ratings yet
- Microcephaly: DR Yog Raj KhinchiDocument37 pagesMicrocephaly: DR Yog Raj KhinchiykhinchiNo ratings yet
- Endogenous Intoxication in SurgeryDocument5 pagesEndogenous Intoxication in SurgeryJonah Seeni100% (1)
- Editorial Board 2014 Archives of Physical Medicine and RehabilitationDocument1 pageEditorial Board 2014 Archives of Physical Medicine and Rehabilitationlsales1986oliNo ratings yet
- DAST FormDocument1 pageDAST FormКонстантин КрахмалевNo ratings yet
- Food Service and Pharmacy, LaundryDocument19 pagesFood Service and Pharmacy, LaundryRAGAVI BNo ratings yet
- Analytical Ability Test - MTDocument1 pageAnalytical Ability Test - MTDirectMed Transcription Services100% (1)
- Streptococcus PneumoniaDocument2 pagesStreptococcus PneumoniaElishah CaprichoNo ratings yet
- DR Preeti Mansukhani - CBC 5 Parts - 2017Document56 pagesDR Preeti Mansukhani - CBC 5 Parts - 2017Silence T-jmNo ratings yet
- PrescriptionDocument27 pagesPrescriptionravindra sharmaNo ratings yet
- Edward Kass - A Brief Perspective On The Early History of American Infectious Disease EpidemiologyDocument9 pagesEdward Kass - A Brief Perspective On The Early History of American Infectious Disease EpidemiologyLuc LiebecqNo ratings yet
- Point of Care Cardiac MarkersDocument14 pagesPoint of Care Cardiac MarkersLien TranNo ratings yet
- Allergic ConjunctivitisDocument15 pagesAllergic ConjunctivitisنعبودNo ratings yet
- HivDocument36 pagesHivfenendriyaniNo ratings yet
- Venipuncture EquipmentDocument4 pagesVenipuncture Equipmentveca.mante.swuNo ratings yet
- 2632 15770 1 PB 4Document4 pages2632 15770 1 PB 4Mariela Judith UCNo ratings yet
- DME Medical Billing Book 1662598386Document46 pagesDME Medical Billing Book 1662598386Nelson ANo ratings yet
- Nursing Intervention (Oncology)Document3 pagesNursing Intervention (Oncology)Gibe BebitaNo ratings yet
- Nutrition Support Enteral & Parenteral NutritionDocument158 pagesNutrition Support Enteral & Parenteral NutritionmajdNo ratings yet
- HLTH 101 Research PaperDocument9 pagesHLTH 101 Research Paperapi-566289467No ratings yet
- EINC Vol6 OnlineDocument8 pagesEINC Vol6 OnlineDonna MirandaNo ratings yet
- Aloe Vera For Human Nutrition Health and Cosmetic Usea Review PDFDocument9 pagesAloe Vera For Human Nutrition Health and Cosmetic Usea Review PDFNatalia MenottiNo ratings yet
- SP 8Document2 pagesSP 8ray72roNo ratings yet
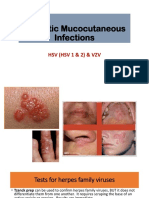
- Herpetic Mucocutaneous Infections: HSV (HSV 1 & 2) & VZVDocument32 pagesHerpetic Mucocutaneous Infections: HSV (HSV 1 & 2) & VZVJaneNo ratings yet