Professional Documents
Culture Documents
Self-Inflicted Bilateral Ocular Surface Injury: Two Case Reports
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Self-Inflicted Bilateral Ocular Surface Injury: Two Case Reports
Copyright:
Available Formats
Volume 8, Issue 11, November – 2023 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Self-Inflicted Bilateral Ocular Surface Injury:
Two Case Reports
Sujit Kumar Biswas1*, Shaila Sharmin1, Soma Rani Roy1.
1
Consultant, Chittagong Eye Infirmary & Training Complex, Chittagong, Bangladesh.
Corresponding Author: Sujit Kumar Biswas1*
ORCID ID: 0000-0002-7006-5788
Abstract:-
I. INTRODUCTION
Aim:
To present two cases of self-inflicted ocular surface Self-inflicted ocular injury produced by the patient
injury. intentionally to assume a sick role and earn some benefits
either to gain emotional and/or financial gain (malingering)
Case report: [1]. This injury occurs from very minor conjunctival or
First case was a 13-year-old girl with reduction of corneal lesion, even traumatic cataracts, retinal detachment,
vision in both her eyes (? counting finger) and redness dislocation of lens and severe self-mutilation such as
with conjunctival laceration in the temporal area, enucleation [2,3]. Different literature describes self-induced
surprisingly, without any pain for one month. The ocular injuries which are uncommon and may be associated
patient denied any history of trauma and lives in a girls with functional disorders such schizophrenia, obsessive-
hostel at that school. On examination, subjective visual compulsive disorder, mental depression, mental retardation,
acuity was in both eyes (?) counting finger one foot, brisk drug related psychosis and also in patients with some
pupillary reaction, quiet anterior chamber, clear lens organic diseases like neurosyphilis, encephalitis, epilepsy,
with normal fundi of both eyes. Most probably self- Lesch–Nyhan syndrome, diabetes mellitus with renal
induced conjunctival injuries, she used her finger-nail involvement [4,5]. Most commonly, self-induced injuries
for this purpose and looks accessible part of the ocular occur in young people [5]. Patients may use their own
surface. The second case was a 55-year-old woman finger, nail, needle, razor, scissor, glass pieces, paper and so
presented with a foreign body sensation, watering, many things for this purpose [6].
redness and blurring of vision in both eyes for two
weeks. The patient denied any history of trauma, Here we describe two cases with self-induced ocular
subjective visual acuity was 6/36 in both eyes, congested surface injury with repeated induced trauma with self-nail
conjunctiva, brisk pupillary reaction, quiet anterior over the temporal conjunctiva of both eyes in the first case
chamber, senile early cataractous lens with normal fundi and repeated sweeping by paper napkin over the lower part
of both eyes. Fluorescein stain showed 3x4 mm epithelial of the corneas of both eyes resulting in corneal abrasion.
defect over the lower part of both corneas. She was using
a paper napkin to sweep her eyes for removal of foreign II. CASE PRESENTATION
bodies frequently and injured by herself.
Case One
They were given treatment with broad spectrum A thirteen-year-old girl came to our department with a
topical antibiotic eye drops, weak corticosteroid and marked reduction of vision in both her eyes (? counting
artificial tear substitute and strong counseling. The finger at one foot) and redness with conjunctival laceration
lesions healed within 2 weeks. in the temporal area, surprisingly, without any pain [figure
A,B] for one month. The patient denied any history of
Conclusion: trauma. The patient reads in seventh grade and lives in a
Self-inflicted ocular injuries are very rare, and girls' hostel at that school. On examination, subjective visual
usually need immediate medical treatment, strong acuity was in both eyes (?) counting finger at one foot, brisk
counseling and psychiatrist consultations. pupillary reaction, quiet anterior chamber, clear lens with
normal fundi of both eyes. Most probably self-induced
Keywords:- Self-Inflicted Injury, Ocular Surface, Functional conjunctival injuries, she used her finger nail for this
Disorders, Organic Disorders, Strong Counseling. purpose and looks accessible part of the ocular surface. She
was given treatment with broad spectrum topical eye drops,
moxifloxacin 0.5% every four hourly, and an artificial tear
substitute also every four hourly in both of her eyes and
counseled her not to touch this area with her finger or any
other things. After a week, her vision (subjective) improved
IJISRT23NOV531 www.ijisrt.com 364
Volume 8, Issue 11, November – 2023 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
to 6/24 and 6/36 in right and left respectively. Her injurious behaviour in Lesch–Nyhan syndrome and
conjunctival lesion improves and there is a small granuloma abnormal metabolism causes self- mutilation in Gilles de la
formation indicated by a white arrow [fig. C]. Again, the Tourette syndrome [5]. Drug induced self-inflicted eye
patient treated with topical moxifloxacin eye drop 0.55 six injuries associated with lysergic acid diethylamide, abuse of
hourly for two weeks, artificial tear for next one month and alcohol, cocaine, cannabis and amphetamines [5]. Other
adding weak corticosteroid, topical fluorometholone eye psychiatric like obsessive- compulsive disorder, psychotic
drop 0.1% six hourly a day for two weeks. Granuloma depression, post-traumatic stress disorder, Munchausen
resolved, conjunctival lesion healed and visual acuity syndrome are associated with self-inflicting eye
improved (probably original VA) to 6/6 in the right eye and injuries. Also, some organic states including temporal lobe
6/6 in the left eye with a refraction of -0.75 cyl at 800 at epilepsy, encephalitis, neurosyphilis are also involved [5].
final follow up [fig. D, E]. Common ocular surface mechanical trauma occurred by the
fingernails to induce corneal scratch and abrasion, confused
Case Two with herpetic keratitis, rubbing of the eyes, looks
A fifty-five-year-old woman came to our department conjunctivitis even corneal erosions. This patient sometimes
with a foreign body sensation, watering, redness and needs to admit and close follow up before proper diagnosis
blurring of vision in both eyes for two weeks. The patient [5].
denied any history of trauma. On examination, subjective
visual acuity was 6/36 in both eyes, congested conjunctiva, IV. CONCLUSION
brisk pupillary reaction, quiet anterior chamber, senile early
cataractous lens with normal fundi of both eyes. Fluorescein Self-inflicted ocular injuries are a very rare condition
stain showed 3x4 mm epithelial defect over the lower part associated with a wide variety of functional and organic
of both the corneas [fig. F,G, indicated by white arrows]. disorders which need a multidisciplinary approach to
She was using a paper napkin to sweep her eyes for removal management. Strong counseling and immediate psychiatrist
of foreign bodies frequently and injured by herself. She was consultations are essential to prevent lethal consequences in
given treatment with broad spectrum topical eye drops, the case of young patients.
moxifloxacin 0.5% every four hourly and an artificial tear
substitute also every four hourly in both of her eyes and Tables: Nil
counseled her not to touch this area with tissue napkin or
any other things. After a week, her vision improved to 6/18 Figures Legends
in both eyes, epithelial defect of cornea headed [fig. H,I].
Again, the patient treated with topical moxifloxacin eye Case One
drop 0.55 six hourly for two weeks, artificial tear for next
one month and adding weak corticosteroid, topical
fluorometholone eye drop 0.1% six hourly a day for two
weeks.
III. DISCUSSION
Self-induced ocular injuries are very rare but important
and challenging to diagnose. Sharp objects like needles,
blades, finger-nails, glass pieces and blunt objects like wood
pieces, paper napkins, clothes etc. are used for this purpose.
These injuries include chronic conjunctivitis, persistent
corneal abrasion, recurrent corneal erosion, corneal
laceration, infiltrate and perforation, scleral injury and
perforation, dislocation of lens, endophthalmitis and even Fig 1 Conjunctival Lesion of Right Eye
enucleation of the eyebll (oedipism) [2,3,7].
Our first patient used her finger-nails and the second
patient used a paper napkin for their self-inflicted ocular
surface injuries. Young and middle-aged males with acute or
chronic schizophrenia are mostly affected by self-inflicting
eye injuries and commonly occur during visual or auditory
hallucinations. Self-inflicted eye injuries can be explained
by some psychodynamic theories. Psychiatric theories state
physical injury induced by a person to any part of his/her
body, as a single or repeated episode, without any suicidal
intention, like pulling hair, chewing fingers, biting lips.
Some self-inflicted eye injury associated with sexual
ideation. Biochemical theories state that an increase in the
action of the neurotransmitter serotonin leads to self-
Fig 2 Conjunctival Lesion of Left Eye
IJISRT23NOV531 www.ijisrt.com 365
Volume 8, Issue 11, November – 2023 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Fig 3 Conjunctival Granuloma of Left Eye
Case Two
Fig 4 Resolved Conjunctival Lesion in Right Eye
Fig 6 Corneal Lesion in Right Eye
Fig 5 Resolved Conjunctival Lesion in Left Eye
Fig 7 Corneal Lesion in Left Eye
IJISRT23NOV531 www.ijisrt.com 366
Volume 8, Issue 11, November – 2023 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
REFERENCES
[1]. Zamir E, Read RW, Rao NA. Self-inflicted anterior
scleritis. Ophthalmology 2001; 108(1): 192–195.
[2]. Gogandy MA, Aljarad A, Jastaneiah SS, Alfawaz AM.
Self-inflicted eye injury. Ann Saudi Med. 2017 May-
Jun;37(3):245-250. doi: 10.5144/0256-4947.2017.245.
PMID: 28578365; PMCID: PMC6150577.
[3]. Kennedy BL, Feldmann TB. Self-inflicted eye injuries:
case presentations and a literature review. Hosp
Community Psychiatry 1994;45:470-4.
[4]. R Brown, M A H Al-Bachari, K Krishna Kambhampati
Self-inflicted eye injuries
BritishournalofOphthalmology, 1991,75,496-498
[5]. Patton N. Self-inflicted eye injuries: A review. Eye.
Fig 8 Realed Corneal Lesion in Right Eye 2004;18:867-72. DOI: 10.1038/sj.eye.6701365
[6]. Sahu J, Arora R, Vishwanath S. Self-inflicted bilateral
ocular injury with scissors in a psychiatric patient.
GMS Ophthalmol Cases. 2023;13:Doc11. DOI:
10.3205/oc000219, URN: urn:nbn:de:0183-oc0002196
[7]. Amiri S, Arfaei A, Farhang S. Self-inflicted needle
injuries to the eye: a curing pain. Case Rep Psychiatry
2015;2015:960579.
Fig 9 Healed Corneal Lesion in Left Eye
Limitation: Both of the patient did not need any
psychiatric consultation.
Conflict of Interest: No commercial/financial interest.
Authors Contribution
Dr. Sujit Kumar Biswas- Concept, design, manuscript
preparation
Dr. Shaila Sharmin- Case selection, literature reviewing.
Dr. Soma Rani Roy-Manuscript review, grammatical
correction.
Funding/Financial Support: No institutional funding.
Acknowledgement: We would like to thank Dr. Ahmadur
Rahman Research Center.
IJISRT23NOV531 www.ijisrt.com 367
You might also like
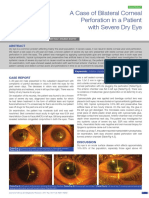
- A Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaDocument2 pagesA Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaIqbal Farid MunggaranNo ratings yet
- Bilateral Atypical Optic Neuritis - Endi Pramudya LaksanaDocument12 pagesBilateral Atypical Optic Neuritis - Endi Pramudya LaksanaGufront MustofaNo ratings yet
- 1 PBDocument4 pages1 PBRian YupitaNo ratings yet
- Management of Penetrating Eye Injury With Intraocular Foreign BodyDocument5 pagesManagement of Penetrating Eye Injury With Intraocular Foreign BodyChristian FaustNo ratings yet
- Acc or Inti 2007Document6 pagesAcc or Inti 2007iwanNo ratings yet
- Iritis 8Document14 pagesIritis 8Alvis KurniawanNo ratings yet
- Penetrating Eye Injury: A Case StudyDocument8 pagesPenetrating Eye Injury: A Case StudyastutisetiaNo ratings yet
- Achromobacter Xylosoxidans Keratitis After Contact Lens UsageDocument5 pagesAchromobacter Xylosoxidans Keratitis After Contact Lens UsageDenata PrabhasiwiNo ratings yet
- Bright Eyes - The Treatment of Eye Diseases by AcupucntureDocument8 pagesBright Eyes - The Treatment of Eye Diseases by AcupucntureElizabeth Durkee Neil100% (1)
- Opthalmology CasesDocument10 pagesOpthalmology CasesAhmad SobihNo ratings yet
- Common Eye Problems: NtroductionDocument14 pagesCommon Eye Problems: NtroductionFunky DestinationNo ratings yet
- Journal OphtalmologyDocument3 pagesJournal OphtalmologyFaza KeumalasariNo ratings yet
- Another JurnalDocument4 pagesAnother JurnalReskyAmeliaHRNo ratings yet
- Eye Trauma - Doctor Print - Patient - Co.ukDocument10 pagesEye Trauma - Doctor Print - Patient - Co.ukbenitiyaNo ratings yet
- Ocular Myasthenia Gravis in Children A Case Report - Muhammad Arief MunandarDocument10 pagesOcular Myasthenia Gravis in Children A Case Report - Muhammad Arief Munandarirvan rahmanNo ratings yet
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocument3 pagesAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNo ratings yet
- Sympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesDocument11 pagesSympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesAlexander RezaNo ratings yet
- Chronic Conjunctivitis From A Retained Contact LensDocument4 pagesChronic Conjunctivitis From A Retained Contact Lensnana nurdahliaNo ratings yet
- Diagnosis Dan Tatalaksana Pada Pasien Dengan Suspek Sindroma Sjogren - Novaqua YandiDocument13 pagesDiagnosis Dan Tatalaksana Pada Pasien Dengan Suspek Sindroma Sjogren - Novaqua YandiElpiana MuntheNo ratings yet
- Topical TreatmentDocument7 pagesTopical TreatmentranpssNo ratings yet
- A Case Presentation of CataractDocument16 pagesA Case Presentation of CataractDoneva Lyn Medina100% (1)
- Cataract PTDocument9 pagesCataract PTPreeti SharmaNo ratings yet
- Cataract PTDocument9 pagesCataract PTpreeti sharmaNo ratings yet
- BCR 2021 244362Document2 pagesBCR 2021 244362Richard Chuzón GuevaraNo ratings yet
- Red Eye CheckDocument3 pagesRed Eye CheckkrishnaNo ratings yet
- Admin, 040 - 1068 - Clara Verlina Suhardi - GalleyDocument4 pagesAdmin, 040 - 1068 - Clara Verlina Suhardi - GalleyskocabzzNo ratings yet
- 6 Nonpenetrating Eye Injuries in Children2020Document13 pages6 Nonpenetrating Eye Injuries in Children2020Josue Enrique Jacobo MendozaNo ratings yet
- Ocular EmergenciesDocument4 pagesOcular EmergenciesJim Jose AntonyNo ratings yet
- Dried Scleral Patch Graft: A Temporary Measure of Corneal Perforation Prior Keratoplasty - Two Case ReportsDocument4 pagesDried Scleral Patch Graft: A Temporary Measure of Corneal Perforation Prior Keratoplasty - Two Case ReportsBOHR International Journal of Current Research in Optometry and Ophthalmology (BIJCROO)No ratings yet
- Medicine: Sumatriptan-Induced Angle-Closure GlaucomaDocument4 pagesMedicine: Sumatriptan-Induced Angle-Closure GlaucomanidaNo ratings yet
- Folded Bandage Contact Lens Retention in A Patient With Bilateral Dry Eye SymptomsDocument85 pagesFolded Bandage Contact Lens Retention in A Patient With Bilateral Dry Eye SymptomsAgung Putra EvashaNo ratings yet
- Red EyeDocument32 pagesRed EyeVitor ParenteNo ratings yet
- Eye DiseasesDocument8 pagesEye DiseasesCeline de HaanNo ratings yet
- Disturbance in Sensory PerceptionDocument48 pagesDisturbance in Sensory PerceptionKristine Louise JavierNo ratings yet
- Case Study Eyes 11Document2 pagesCase Study Eyes 11Carla May CaraNo ratings yet
- Shrestha-Shrestha2019 Article DisseminatedNeurocysticercosisDocument4 pagesShrestha-Shrestha2019 Article DisseminatedNeurocysticercosisItsirch AydinNo ratings yet
- Typical Optic Neuritis RevDocument6 pagesTypical Optic Neuritis RevAdhi AmertajayaNo ratings yet
- Research Proposal Visual ProblemDocument20 pagesResearch Proposal Visual Problemyaqoob008100% (2)
- Journal of Eucornea: K. Zonnevylle, D. Thoma, E. Mulliez, S. Ghekiere, J. Blanckaert, M.D.A. Blanckaert TDocument4 pagesJournal of Eucornea: K. Zonnevylle, D. Thoma, E. Mulliez, S. Ghekiere, J. Blanckaert, M.D.A. Blanckaert TKhalfiaNo ratings yet
- PhacoanaphylacticDocument1 pagePhacoanaphylacticrluiknagwa lingNo ratings yet
- Case Report - Traumatic CataractDocument4 pagesCase Report - Traumatic CataractMaria LarasatiNo ratings yet
- Acute Monocular Vision LossDocument9 pagesAcute Monocular Vision LossRoberto López MataNo ratings yet
- Transient Delayed Facial Nerve Palsy After Inferior Alveolar Nerve Block AnesthesiaDocument6 pagesTransient Delayed Facial Nerve Palsy After Inferior Alveolar Nerve Block AnesthesiaWilson WijayaNo ratings yet
- Case ReportDocument7 pagesCase ReportJeel GaralaNo ratings yet
- MainDocument3 pagesMainomidazadmehr1375No ratings yet
- 100255-Article Text-1482-2-10-20220311Document6 pages100255-Article Text-1482-2-10-20220311Fachry RahmanNo ratings yet
- Peter's Anomaly Type 2 With CataractDocument3 pagesPeter's Anomaly Type 2 With CataractbijgimNo ratings yet
- The Injured Eye - Practical Management Guidelines and Referral Criteria For The Rural DoctorDocument6 pagesThe Injured Eye - Practical Management Guidelines and Referral Criteria For The Rural DoctorElrach CorpNo ratings yet
- Staphylococcus Epidermidis End PDFDocument4 pagesStaphylococcus Epidermidis End PDFNisaNo ratings yet
- Ophtha OSCEDocument3 pagesOphtha OSCEdonna dominnoNo ratings yet
- Penetrating Eye Trauma Eyes Wide Split - LITFL - Ophthalmology BefuddlerDocument6 pagesPenetrating Eye Trauma Eyes Wide Split - LITFL - Ophthalmology Befuddlersen ANo ratings yet
- Evaluation of The Painful EyeDocument9 pagesEvaluation of The Painful EyeMuthia Farah AshmaNo ratings yet
- Ocular Chemical Burns From Accidental Exposure To.28Document2 pagesOcular Chemical Burns From Accidental Exposure To.28qalbiNo ratings yet
- Nonorganic Vision LossDocument8 pagesNonorganic Vision LossArdelia EmilyNo ratings yet
- DakriDocument2 pagesDakriLBT04No ratings yet
- 38surekha EtalDocument3 pages38surekha EtaleditorijmrhsNo ratings yet
- 1 s2.0 S2090074015000833 MainDocument3 pages1 s2.0 S2090074015000833 MainMuhammad Fuad MahfudNo ratings yet
- Clinical Diagnosis and Management of Ocular Myasthenia GravisDocument11 pagesClinical Diagnosis and Management of Ocular Myasthenia GravisAinul NurrahmahNo ratings yet
- ABIM - Ophthalmology - (Medicalstudyzone - Com)Document26 pagesABIM - Ophthalmology - (Medicalstudyzone - Com)sjcemeryNo ratings yet
- Retina Detachment, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionFrom EverandRetina Detachment, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionNo ratings yet
- Utilization of Waste Heat Emitted by the KilnDocument2 pagesUtilization of Waste Heat Emitted by the KilnInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Ambulance Booking SystemDocument7 pagesAmbulance Booking SystemInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Impact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaDocument6 pagesImpact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Entrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisDocument10 pagesEntrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Detection and Counting of Fake Currency & Genuine Currency Using Image ProcessingDocument6 pagesDetection and Counting of Fake Currency & Genuine Currency Using Image ProcessingInternational Journal of Innovative Science and Research Technology100% (9)
- An Overview of Lung CancerDocument6 pagesAn Overview of Lung CancerInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Designing Cost-Effective SMS based Irrigation System using GSM ModuleDocument8 pagesDesigning Cost-Effective SMS based Irrigation System using GSM ModuleInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Auto Tix: Automated Bus Ticket SolutionDocument5 pagesAuto Tix: Automated Bus Ticket SolutionInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Effect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictDocument13 pagesEffect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Digital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaDocument10 pagesDigital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Forensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsDocument12 pagesForensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Smart Health Care SystemDocument8 pagesSmart Health Care SystemInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Study Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoDocument6 pagesStudy Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Cyber Security Awareness and Educational Outcomes of Grade 4 LearnersDocument33 pagesCyber Security Awareness and Educational Outcomes of Grade 4 LearnersInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Unmasking Phishing Threats Through Cutting-Edge Machine LearningDocument8 pagesUnmasking Phishing Threats Through Cutting-Edge Machine LearningInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Computer Vision Gestures Recognition System Using Centralized Cloud ServerDocument9 pagesComputer Vision Gestures Recognition System Using Centralized Cloud ServerInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Predictive Analytics for Motorcycle Theft Detection and RecoveryDocument5 pagesPredictive Analytics for Motorcycle Theft Detection and RecoveryInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Blockchain Based Decentralized ApplicationDocument7 pagesBlockchain Based Decentralized ApplicationInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- An Industry That Capitalizes Off of Women's Insecurities?Document8 pagesAn Industry That Capitalizes Off of Women's Insecurities?International Journal of Innovative Science and Research TechnologyNo ratings yet
- Parastomal Hernia: A Case Report, Repaired by Modified Laparascopic Sugarbaker TechniqueDocument2 pagesParastomal Hernia: A Case Report, Repaired by Modified Laparascopic Sugarbaker TechniqueInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Visual Water: An Integration of App and Web To Understand Chemical ElementsDocument5 pagesVisual Water: An Integration of App and Web To Understand Chemical ElementsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Factors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaDocument6 pagesFactors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Smart Cities: Boosting Economic Growth Through Innovation and EfficiencyDocument19 pagesSmart Cities: Boosting Economic Growth Through Innovation and EfficiencyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Impact of Silver Nanoparticles Infused in Blood in A Stenosed Artery Under The Effect of Magnetic Field Imp. of Silver Nano. Inf. in Blood in A Sten. Art. Under The Eff. of Mag. FieldDocument6 pagesImpact of Silver Nanoparticles Infused in Blood in A Stenosed Artery Under The Effect of Magnetic Field Imp. of Silver Nano. Inf. in Blood in A Sten. Art. Under The Eff. of Mag. FieldInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Insights Into Nipah Virus: A Review of Epidemiology, Pathogenesis, and Therapeutic AdvancesDocument8 pagesInsights Into Nipah Virus: A Review of Epidemiology, Pathogenesis, and Therapeutic AdvancesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Compact and Wearable Ventilator System For Enhanced Patient CareDocument4 pagesCompact and Wearable Ventilator System For Enhanced Patient CareInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Parkinson's Detection Using Voice Features and Spiral DrawingsDocument5 pagesParkinson's Detection Using Voice Features and Spiral DrawingsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Air Quality Index Prediction Using Bi-LSTMDocument8 pagesAir Quality Index Prediction Using Bi-LSTMInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Implications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewDocument6 pagesImplications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Predict The Heart Attack Possibilities Using Machine LearningDocument2 pagesPredict The Heart Attack Possibilities Using Machine LearningInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- يا عينيDocument80 pagesيا عينيHijxNo ratings yet
- Amodia - Purposive CommunicationDocument7 pagesAmodia - Purposive CommunicationCLUVER AEDRIAN AMODIANo ratings yet
- Germ Theory of Disease CausationDocument11 pagesGerm Theory of Disease Causationnashreen83% (6)
- Neurodevelopmental Technique/ Bobath ApproachDocument2 pagesNeurodevelopmental Technique/ Bobath ApproachManiu EmeseNo ratings yet
- Rehabilitation For Persons With Upper Extremity AmputationDocument14 pagesRehabilitation For Persons With Upper Extremity AmputationVince ObiedoNo ratings yet
- Ethinylestradiol 15mcg + Gestodene 60mcg (Minesse)Document17 pagesEthinylestradiol 15mcg + Gestodene 60mcg (Minesse)asdwasdNo ratings yet
- Acid Base Disorder ABG AnalysisDocument53 pagesAcid Base Disorder ABG AnalysisAlemayehu beharuNo ratings yet
- Handbook of TransplantDocument496 pagesHandbook of Transplantfa7mi77No ratings yet
- LIMITLESS PEDIATRICS BY DR NAVEEN - DAY 4 (Green)Document56 pagesLIMITLESS PEDIATRICS BY DR NAVEEN - DAY 4 (Green)Biplav SinghNo ratings yet
- Mojahid Sheet Complete PDFDocument176 pagesMojahid Sheet Complete PDFOsman SomiNo ratings yet
- ABG AnalysisDocument9 pagesABG AnalysisHoney PrasadNo ratings yet
- Pearls of Glaucoma ManagementDocument469 pagesPearls of Glaucoma ManagementMacarena AlvarezNo ratings yet
- The Effects of Smoking On RespirationDocument1 pageThe Effects of Smoking On RespirationKumar JeevanNo ratings yet
- Perioperative Nursing Care: Portreitz KMTC Naom NyarangiDocument132 pagesPerioperative Nursing Care: Portreitz KMTC Naom NyarangiGabriel GagaNo ratings yet
- Case PresentationDocument22 pagesCase PresentationManjunath ArunachalamNo ratings yet
- 20 Pharmacology of Marine Macroalgae: Kasım Cemal Güven, Burak Coban and Osman ÖzdemirDocument31 pages20 Pharmacology of Marine Macroalgae: Kasım Cemal Güven, Burak Coban and Osman ÖzdemirRifky AlfeniNo ratings yet
- Danger of LonelinessDocument12 pagesDanger of LonelinessLonzell WinnNo ratings yet
- Nervous SystemDocument3 pagesNervous SystemshhhNo ratings yet
- ALCOTEC (MSDS) GTAW-ALUMINUM WELD WIRE 7994-N Expires 17-05-01Document9 pagesALCOTEC (MSDS) GTAW-ALUMINUM WELD WIRE 7994-N Expires 17-05-01PubcrawlNo ratings yet
- Periodontology 2000 - 2022 - Leira - Complications and Treatment Errors in Periodontal Therapy in Medically CompromisedDocument23 pagesPeriodontology 2000 - 2022 - Leira - Complications and Treatment Errors in Periodontal Therapy in Medically Compromised安西 泰規No ratings yet
- Matrixmidface™ Plate and Screw System: Surgical TechniqueDocument48 pagesMatrixmidface™ Plate and Screw System: Surgical TechniqueΣτελλα ΔαλNo ratings yet
- PainDocument14 pagesPainAmer Abdulla SachitNo ratings yet
- SYMPTOMATOLOGYDocument22 pagesSYMPTOMATOLOGYMntdher EadanNo ratings yet
- Dugos K Lifeassure 03022023112946Document5 pagesDugos K Lifeassure 03022023112946Vic KwanNo ratings yet
- Xray Kub My Prep FinalDocument109 pagesXray Kub My Prep FinalphoenixibexNo ratings yet
- CDHO Factsheet AsthmaDocument4 pagesCDHO Factsheet AsthmaIlse AnzuresNo ratings yet
- Thyrooid GuidlineDocument50 pagesThyrooid Guidlinepuskesmas tajurNo ratings yet
- Chicken Pox ReportDocument25 pagesChicken Pox ReportDyanne BautistaNo ratings yet
- ICD-11 Implementation or Transition Guide - v105 PDFDocument41 pagesICD-11 Implementation or Transition Guide - v105 PDFenzo_valeriaNo ratings yet
- 129-Article Text-460-5-10-20200513Document8 pages129-Article Text-460-5-10-20200513Anushree DatarNo ratings yet