Professional Documents
Culture Documents
2023 - PHARMA - Student Module 05 - Cardio and Renal Drugs
2023 - PHARMA - Student Module 05 - Cardio and Renal Drugs
Uploaded by
Nicole PajaroOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2023 - PHARMA - Student Module 05 - Cardio and Renal Drugs
2023 - PHARMA - Student Module 05 - Cardio and Renal Drugs
Uploaded by
Nicole PajaroCopyright:
Available Formats
ST.
LUKE’S COLLEGE OF NURSING
1st Semester
School Year: 2023-2024
GENERAL DISCUSSION SCHEDULE
COURSE CODE : MC_106
COURSE TITLE : Pharmacology
LESSON NUMBER : 06 – Cardiovascular and Renal Medications
TIME ALLOTMENT : 6 Hours
PRESCRIBED FLO : Onsite Lecture
TOPIC LEARNING OUTCOMES:
After the end of the lesson, the student should be able to:
1. Review the anatomy and physiology of the cardiovascular and renal system
2. Identify the various classification of antihypertensive drugs as well as their various nursing responsibilities and patient education
3. Review the physiology of diuresis, and identify the various nursing responsibilities and patient education on diuretic drugs
4. Identify the fundamentals of cardiac glycosides, angina, and dysrhythmia, as well as discuss their various nursing responsibilities and patient education
5. Identify the various antihyperlipidemics, and drugs that improve peripheral blood flow as well as their respective nursing responsibilities and patient
education.
6. Review the physiology of blood coagulation and identify the various classifications of anticoagulants, anti-platelets and thrombolytic agents and their
respective nursing responsibilities and patient education.
1 Pharmacology 05 – Cardiovascular and Renal Medication
Activities Strategies TA Remarks
1 ATTENTION Start with icebreaker questions to start interacting with the class 15 minutes
2 OBJECTIVE Discuss with the class the objectives of the lecture to be 15 minutes
discussed
3 RECALL Give a 10-item pre-test 15 minutes
4 STIMULUS Do a 6-hour lecture (divided into 2 meetings) 360minutes
5 GUIDANCE Conduct exercises as we walk through lectures 60 minutes
6 PERFORMANC Give a 20-item post-test 15 minutes
E
7 FEEDBACK Rationalize post-test answers 15 minutes
8 ASSESSING Divide the class into groups and facilitate focused group 15 minutes
discussions based on formulated guide questions
9 RETENTION Summarize the topic and highlight key points 30 minutes
LESSON/TOPIC DISCUSSION
Learning Resources: (Citation following APA Method)
1. eBook
o Pharmacology: A Patient-Centered Nursing Process Approach, 9e by Linda E. McCuistion, Saunders (2023), Edition: 9
o Mosby's 2020 Nursing Drug Reference, 33rd ed. by Linda Skidmore-Roth, St. Louis, MO : Elsevier (2020), Edition: 33
o Introducing Pharmacology: For Nursing and Healthcare by Roger McFadden, Routledge (2019), Edition: 3
o Pathophysiology and Pharmacology in Nursing (Transforming Nursing Practice Series) by Sarah Ashelford, Learning Matters (2019), Edition:
Second
o Lippincott NCLEX-RN Pharmacology Review by Hill
2. Scanned Reference Books
2 Pharmacology 05 – Cardiovascular and Renal Medication
o PHARMACOLOGICAL REVIEWS Vol. 59, No. 4. 2007 by The American Society for Pharmacology and Experimental Therapeutics 70102/3301314
o Pharmacol Rev 59:289 –359, 2007
3. Online Resources
o Philippine Drug Enforcement Agency. Laws and Regulations. https://pdea.gov.ph/laws-and-regulations#:~:text=WHEREAS%2C%20by
%20virtue%20of%20the,chemicals%20as%20provided%20in%20R.A.
LESSON 6 TOPICS:
A. The Cardiovascular System
B. The Renal System
C. Antihypertensive
D. Diuretics
E. Cardiac Glycosides, Antianginals and Anti-Dysrhythmic Drugs
F. Antilipidemics and Peripheral Blood Flow Medications
G. Anticoagulants
ACTIVITY 1: INTRODUCTION
● Open the class with updates on school matters and today’s topic
● Discuss the objectives of today’s lesson
ACTIVITY 2: PRE-TEST
ACTIVITY 3: CARDIOVASCULAR AND RENAL MEDICATIONS
A. The Cardiovascular System
● The cardiovascular system deals with the heart and the blood vessels, both which plays a major role in circulation. The heart pumps blood and the blood
vessels carries blood to the body and back to the heart again for oxygenation and nutrients.
3 Pharmacology 05 – Cardiovascular and Renal Medication
● Chambers of the heart:
o Right and left atrium divided by interatrial septum
o Right and left ventricles by interventricular septum.
● Circulation:
o Heart collects blood from the system through the superior and inferior vena cava --- RA --- Tricuspid valve --- right ventricles --- (pulmonary
circuit) PA and their smaller branches --- LUNGS --- oxygenation in capillary beds --- PV --- LA --- mitral valve --- LV --- aorta and coronaries ---
(systemic circuit).
● Over time, this circulation will require the output of both sides of the heart by pumping the same amount blood. If the left side of the heart were to fall
behind the right-side blood will accumulate into the pulmonary circuit. Similarly, if the right heart were to pump less than the left it will accumulate in
the systemic circuit.
● Blood circulation is affected by ADLs, doing DBEs or an abrupt change in position.
● Electrical Conduction of the Heart:
o Although, the heartbeat is myogenic, it can be influenced by ANS to increase its function via SNS by supplying catecholamines or via PNS (Vagus
nerve) releasing Ach thereby decreasing the HR.
o SA node --- AV node --- Bundle of His --- Purkinje Fibers.
● Automaticity – characteristic of the heart tissue in which it allows spontaneous development of action potential.
● Inotropy – effect of drugs that either increase (+) or decrease (-) contractility.
● Chronotopy – effect of drugs that either increase (+) or decrease (-) heart rate
● Dromotropy – (+) or (-) of speed in conduction of electrical impulses.
● Preload – it is usually considered the end-diastolic pressure. It is the work or load imposed on the heart before the contraction begins. It represents the
amount of blood that the heart must pump with each beat.
● Afterload – is the pressure in which the cardiac muscle exerts its contractile force to move the blood into the aorta. It is the work presented to the heart
after contraction.
4 Pharmacology 05 – Cardiovascular and Renal Medication
● Stroke volume – is the volume of blood discharged from contraction of ventricles
● Heart rate – determines the frequency in which blood is pumped out of the heart. As heart rate increases, cardiac output also increases, and preload and
afterload will be reduced.
● Cardiac output – is the volume of blood pumped out of the ventricles per minute. (CO=SVxHR)
● Blood volume – is the sum of the formed elements and plasma volumes in the vascular system and is directly proportional with blood pressure. If blood
volume decreases, then pressure changes also.
● Peripheral resistance – resistance of arteries to blood flow and is affected by the vessel’s diameter and force of contraction exerted in the smooth
muscles.
● Viscosity – is the resistance of the fluid to flow. The higher the viscosity, the greater the resistance to flowing.
● Hypertension – state of elevation in systemic arterial blood pressure caused by increased peripheral vascular resistance.
● Categories of BP:
o Normal: Less than 120/80 mm Hg;
o Elevated: Systolic between 120-129 and diastolic less than 80;
o Stage 1: Systolic between 130-139 or diastolic between 80-89;
o Stage 2: Systolic at least 140 or diastolic at least 90 mm Hg;
o Hypertensive crisis: Systolic over 180 and/or diastolic over 120, with patients needing prompt changes in medication if there are no other
indications of problems, or immediate hospitalization if there are signs of organ damage.
● Although most of the time, patient is not aware of the symptoms, but this will significantly affect their overall health since it may lead to CAD, stroke,
kidney disease, heart failure.
● Most elevation of BP are a secondary effect of a preexisting illness albeit 90% are essential hypertension.
● Heart, blood vessels, kidneys, liver, and lungs play a crucial role in regulating blood pressure.
● Blood Pressure Regulation:
o Changes in blood pressure are usually detected by baroreceptors which is in the aorta and carotid sinus.
5 Pharmacology 05 – Cardiovascular and Renal Medication
o On the other hand, baroreceptors cannot regulate BP for a long time because this mechanism can be reset when adequate blood pressure is
restored.
o Likewise, when decreased BP is detected the sympathetic response will then be triggered thereby increasing BP. On the other hand, baroreceptors
cannot regulate BP for a long time because this mechanism can be reset when adequate blood pressure is restored.
Arterial pressure stretches the wall of BV
Triggers baroreceptors
Stimulate ANS
Stimulate SNS Stimulate PNS
Stimulate vagus nerve
Activate α1 Activate β1
receptors receptors
Decrease BP
Increase vascular Increase CO
resistance via
vasoconstriction
Increase BP
Figure 5.1: Blood Pressure Regulation
B. The Renal System
● The renal system consists of kidneys, ureters, bladder and urethra.
● It functions to produce urine where wasted and other excess fluid are excreted.
● Nephron:
6 Pharmacology 05 – Cardiovascular and Renal Medication
o Functional unit of kidneys
o Plays a crucial role in maintaining NA, K, Water and other electrolytes regulation through reabsorption and secretion.
o Segments of a nephron:
1. PCT – reabsorb NaCl, K, glucose, amino acids, HCO3, H2O
2. Loop of Henle – which has 2 segments which consists of descending and ascending loop.
a. Descending loop of Henle – water reabsorption.
b. Ascending loop of Henle – Na, Cl and K reabsorption occurs.
3. DCT – Na, Cl, K, Ca, Mg and HCO3 reabsorption.
4. Collecting ducts – Na, Cl, Urea and water.
o Remember! The importance of knowing which segment of the nephron reabsorbs and secrete substances is to apply the mechanism of action of certain
drugs that affect these segments.
Figure 6.2: Renin – Angiotensin – Aldosterone System (RAAS)
● Renin – Angiotensin – Aldosterone System (RAAS)
1. When the blood pressure is low apparently, the blood flow to the kidneys are also decreased making the kidneys to produce renin.
2. Renin, a peptide hormone released by juxtaglomerular apparatus in the kidney are directly released into the circulation.
3. Renin facilitates the conversion of angiotensinogen released by the liver and is converted to angiotensin I, which further converted into
angiotensin II by an enzyme found in the lungs called angiotensin converting enzyme (ACE).
7 Pharmacology 05 – Cardiovascular and Renal Medication
4. Angiotensin II is a potent vasoconstrictor that increases blood pressure by increasing the kidney’s proximal convoluted tubule to reabsorb
sodium.
5. Furthermore, Angiotensin II stimulates the receptors of adrenal glands to secrete aldosterone hormone in which acts on the distal convoluted
tubule to increase sodium and water reuptake.
6. This sequential mechanism results in decreased water excretion and therefore increases BV/BP.
C. Antihypertensives
● Classifications of Antihypertensives:
o Central-acting sympathomimetics
o Peripheral-acting sympathomimetics
o Calcium Channel Blockers
o Vasodilators
o Diuretics
● Centrally-Acting Sympathomimetics:
o Action:
▪ Acts directly on A2 receptors decreasing sympathetic outflow by inhibiting vasomotor centers - decrease peripheral resistance, SBP/DBP, HR.
▪ Acts on DOPA decarboxylase which is an enzyme that converts DOPA into dopamine (w/c is a precursor molecule for catecholamines)
resulting to decrease dopaminergic neurotransmission in PNS and competes with a2 receptor sites thereby decreasing sympathetic responses.
▪ Used to HPN that do not respond to any combination antihypertensive drugs.
o Indication: BP control for patient with or without renal impairment because it doesn’t affect renal flow or filtration, or during pregnancy
o Examples:
▪ Clonidine
▪ A-Methyldopa
o Side Effects / Adverse Effects:
8 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Depression, drowsiness, edema, dry mouth, impotence
o Contraindication:
▪ Asthma, bradycardia, cardiogenic shock, 2nd or 3rd degree heart block, heart failure
o Drug Interactions:
▪ ↓effects of levodopa
▪ +beta-blockers, prazosin, tricyclic antidepressants = ↓effects
▪ +verapamil = severe hypotension
▪ +lithium = ↑lithium toxicity
▪ +MAOI = ↑sympathetic stimulation
▪ Clonidine + TCA = may increase blood pressure
o Nsx Action:
▪ Taper dosage.
▪ Rebound HPN for abrupt withdrawal of clonidine.
▪ CNS depressants are not to be taken with clonidine – worsen CNS depression.
▪ Carvedilol x OHA – increase hypoglycemic effects.
● Peripheral-Acting Adrenergic Blockers:
o Alpha-Adrenergic Blockers
▪ Action: Selective antagonist a1 receptors in the peripheral vasculature to produce vasodilation.
▪ Examples: prazosin, doxazosin (-zosin)
9 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Nsx. Action:
o Monitor ECG for arrhythmias
o WOF: reflex tachycardia and orthostatic hypotension
o Not recommended for initial tx for hpn
o Beta-Adrenergic Blockers
▪ Action: acts by competing with beta-adrenergic receptor sites in the heart muscle and inhibiting release of renin in kidneys, decreasing
availability of angiotensinogen II and aldosterone.
▪ Indication: are used for pt with preexisting heart disease. (SVT, AMI, CHF)
▪ Examples:
o Beta-1 Adrenergic Blockers: metoprolol, atenolol, bisoprolol
o Beta-1 and Beta-2 Adrenergic Blockers: propranolol
o Non-selective Alpha and Beta Adrenergic Blockers: carvedilol
▪ Contraindication: Asthma
▪ Drug Interactions:
o Potentiates OHA effect by inhibiting b2 receptors in the liver responsible for glycogenolysis – hypoglycemia
o NSAIDs can decrease the hypotensive effects of beta-adrenergic blockers.
▪ Side Effects / Adverse Effects: bradycardia, hypotension, fatigue, lethargy and insomnia, decrease libido and erectile dysfunction, decreasing
HDL, increasing triglycerides.
▪ Nsx Action:
o Check the patient’s apical pulse prior to giving the drug.
o Withhold if detect extremes in pulse rate and notify physician.
o Use cautiously with HF, PAD, DM – hypoglycemia because of inhibition of b2 receptor in the liver.
o WOF: abrupt withdrawal – angina, MI, and death
● Calcium Channel Blockers
10 Pharmacology 05 – Cardiovascular and Renal Medication
o Action: Prevent the passage of Ca ions into cell membrane of myocardial smooth muscle and peripheral arteriolar vasculature results in arteriolar
vasodilation, decrease cardiac workload, BP, afterload thereby decreasing also O2 demand of the heart.
o Examples:
▪ Diphenylalkylamines (verapamil)
▪ BenzoTHIAzepine (diltiazem)
▪ Dihydropiridines (nifedipine, amlodipine)
o Indication:
▪ BP medication for patient with DM, Angina
▪ Supraventricular tachyarrhythmia, angina, migraine and cluster headache.
▪ Diltiazem and verapamil are usually used to treat AFib.
▪ Affects more vascular Ca channels than in the heart, most recommended for HPN.
o Contraindications: HF and AV blocks due to their (-) inotropic and dromotropic effect.
o Side effects / Adverse Effects:
▪ Dizziness, headache and fatigue, peripheral edema.
▪ Orthostatic hypotension, HP, hypotension, and arrhythmias, such as bradycardia
o Drug Interactions:
▪ +Digoxin = ↑digoxin toxicity
▪ +beta blockers = bradycardia and heart failure
▪ +grapefruit = ↑effect and toxicity
o Nsx Action:
▪ Monitor VS: WOF SBP <90mmHg and HR < 60bpm
11 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Constipation is a common, ↑OFI fluids and high-fiber foods
● Vasodilators
o Angiotensin Converting Enzyme (ACE) Inhibitors
▪ Action:
o 1st line of treatment in HPN even with concurrent diseases such as CAD, DM, stroke, HF, MI, CKD.
o Acts on ACE to inhibit conversion of angiotensin I to angiotensin II.
▪ Example: captopril, enalapril
▪ Contraindicated: pregnancy – teratogenic.
▪ Side Effects / Adverse Effects: dry cough, Fever, altered taste, hypotension, hyperkalemia.
▪ Nsx Action:
o Monitor WBC and differential counts before therapy, every 2 weeks for the first 3 months of therapy, and periodically thereafter. If increase
during treatment, notify MD.
o monitor K+ levels. Hyperkalemia results if in combination with K+ sparing diuretics or any K+ supplements.
o Angiotensin II receptor blockers (ARBS)
▪ Action:
o 1st line of TX in HPN even with such as DM, HF, CKD.
o Acts by blocking Angiotensin II from binding to receptors sites in vasculature, preventing vasoconstriction and also inhibits aldosterone
secretions.
▪ Examples: Losartan, Valsartan, Irbesartan
▪ Contraindication: pregnancy – teratogenic.
▪ Side Effects / Adverse Effects:
o Headache, fatigue, dizziness, cough, symptoms of URTI
▪ Drug Interactions:
12 Pharmacology 05 – Cardiovascular and Renal Medication
o +phenobarbital, NSAIDs = ↓effectiveness
o +ketoconazole, fluconazole, diltiazem = ↓effectiveness of losartan
o +digoxin = ↑serum levels telmisartan
o +K supplements = hyperkalemia
▪ Nsx Action:
o Monitor BP, and maintain fluid intake
o Renin Inhibitors:
▪ Action: Inhibits renin production.
▪ Example: Aliskiren
▪ Drug interaction: not to be taken with ACE inhibitors and ARBs
▪ Side Effects / Adverse Effects: diarrhea, cough and angioedema
▪ Contraindication: pregnancy: teratogenic.
D. Diuretics
● Drugs that acts in different mechanism with main goal of reducing blood pressure by decreasing circulatory blood volume through increasing of urine
output resulting to improve cardiac output.
● Types:
o Carbonic Anhydrase Inhibitors
o Loop Diuretics
o Osmotic Diuretics
o Thiazide Diuretics
o K+ Sparing Diuretics
● Carbonic Anhydrase Inhibitors
o Action - Block the action of carbonic anhydrase, thus preventing the exchange of H+ ions with sodium and water
13 Pharmacology 05 – Cardiovascular and Renal Medication
o Examples: Acetazolamide, methazolamide
o Side Effects / Adverse Effects: metabolic acidosis, hypokalemia, renal stone formation (ca and phosphate excretion, insoluble in alkaline urine)
o Contraindications: liver cirrhosis, decrease secretion of NH4+ which contributes more to hepatic encephalopathy.
● Loop Diuretics
o Action:
▪ It has the greatest diuretic effect among diuretics.
▪ Inhibits the Na and Cl reabsorption in the loop of Henle and distal tubule
▪ ↑Na and water excretion by inhibiting sodium absorption in proximal tubule
o Examples: bumetanide, furosemide
o Indication:
▪ Drug of choice in an emergency situation where pulmonary edema and peripheral edema is present caused by HF/renal impairment.
▪ Can be used also in treating hypercalcemia and hyperkalemia along with hydration because it reinforces tubular Ca excretion.
o Side Effects / Adverse Effects: acute hypovolemia, hypokalemia, hypomagnesemia, hyperuricemia (loop diuretics compete with uric acid in excretion-
gouty attacks), ototoxicity (reinforced effect with aminoglycosides)
o Nsx. Action:
▪ Monitor for electrolyte imbalances especially K+ levels (hypokalemia)
▪ Monitor weight and blood pressure frequently.
● Osmotic Diuretics
o Action:
▪Increases the osmotic pressure of the glomerular filtrate, which inhibits the reabsorption of sodium and water.
▪Used to excrete water than Na, not useful in Na retention.
o Example: mannitol
o Indication: Used for patient with increase ICP, ARF due to shock, drug toxicities and trauma.
o Side Effects / Adverse Effects: hypotension, reflex tachycardia
14 Pharmacology 05 – Cardiovascular and Renal Medication
o Nsx. Action: Mannitol may cause rebound increased ICP 8 to 12 hours after diuresis. Monitor BP and LOC.
● Thiazide and Thiazide-like (Sulfonamide Derivatives)
o Action:
▪ Most commonly used diuretics. Effective in reducing BP
▪ Acts on distal convoluted tubules promotes excretion of water by preventing reabsorption of sodium in the kidneys. As the kidneys excrete the
excess sodium, they excrete water along with it. These drugs also increase the excretion of chloride, potassium,
▪ *can be used with loop diuretics if additional diuresis is needed.
o Examples:
▪ Thiazide – like diuretics: chlorothiazide (1st oral diuretic that treat severe edema, commonly used drug in pts with cirrhosis and heart failure.),
indapamide, metolazone
▪ Hydrochlorthiazide – most potent
o Side Effects / Adverse Effects: reduced blood volume, orthostatic hypotension, hypokalemia, hyperglycemia, and hyponatremia.
o Nsx. Action:
▪ Monitor K status especially in patients receiving digoxin.
▪ Monitor his blood glucose levels because diuretics may cause hyperglycemia.
▪ WOF: Hypokalemia –Hyponatremia, hypotension, hyperuricemia
● K+ Sparing Diuretics
o Action:
▪ Affects collecting ducts and distal tubules of the kidneys. In exchange, sodium, water, bicarbonate and calcium are excreted into the urine while
retaining K+ and hydrogen ions.
▪ These effects lead to reduced blood pressure and increased concentration serum potassium levels in the blood.
o Types of K+ Sparing Diuretics:
▪ Aldosterone antagonists: spironolactone, eplerenone
15 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Na channel blockers: triamterene
o Indication:
▪ Used in HF and HPN and most effective in treating ascites.
▪ In most edematous cases, aldosterone levels are high resulting to retention of Na, drugs in this class antagonize this effect by competing to its
receptors – K+ reuptake and excretion of Na – diuresis.
o Side Effects / Adverse Effects: Hyperkalemia, gastric upset, gynecomastia in males (off label Tx in PCOS blocking androgen receptors)
o Nsx Action:
▪ Take the drug at the same time each day to prevent nocturia.
▪ Record weight each morning after voiding and before breakfast, in the same type of clothing, and using the same scale.
▪ Be aware of adverse effects, and report signs and symptoms promptly, especially chest, back, or leg pain; shortness of breath; increased fluid
accumulation or weight gain (more than 2 lb daily; or excess water loss (as evidenced by a weight loss of more than 2 lb daily).
▪ Avoid high-sodium foods (such as lunch meat, smoked meats, and processed cheeses) and don’t add table salt to foods.
▪ If taking a potassium-depleting diuretic, include potassium-rich foods (such as bananas, oranges, and potatoes) in your diet.
▪ If taking a K+ sparing diuretic, you don’t need to add extra potassium-rich foods.
▪ Keep follow-up appointments to monitor the effectiveness of therapy.
▪ Avoid hot beverages, excessive sweating, and the use of hot tubs or saunas.
E. Cardiac Glycosides, Anti-Dysrhythmic and Antianginals Medications
● Congestive Heart Failure (CHF) – collection of clinical signs and symptoms caused by different cardiac disorders that results for heart not to function its
optimal capacity. As a result, heart cannot pump enough blood to meet the myocardial oxygen demand and other nutrients. Therefore, fluids build and
the body is congested.
16 Pharmacology 05 – Cardiovascular and Renal Medication
● Causes of heart failure:
o Low output - caused by dysfunction of contractile muscles and endothelial cells that line the heart and BV. This impairment can narrow the lumen of
blood vessels by atherosclerotic plaque, inflammation and activation of platelets like what actually happens in Myocardial ischemia, infarction,
cardiomyopathy.
o High output – CO is normal/ elevated but cannot meet the metabolic and oxygen demand of tissues caused by anemia (reduced O2 capacity),
hyperthyroidism (hypermetabolism)
● Left-sided Heart Failure:
o Responsible for pumping oxygenated blood from the lungs going to systemic circulation. Most common cause is Myocardial infarction,
cardiomyopathy and chronic hypertension.
o Left side pumping mechanism is decreased – pump ineffectively causing decreased SV (+ LVEDP) - + preload – pooling of blood in ventricles then
backward flow to LA – PV – congestion of pulmonary circuit - + pulmonary pressure – pulmonary edema = CHF
o Sign and symptoms: dyspnea, cough, frothy sputum, rales, orthopnea, poor systemic oxygenation, cyanosis
● Right-sided Heart Failure:
o Happens as a consequence of left-sided hear failure
o Presence of pulmonary congestion put pressure also in pulmonary arteries eventually in RA - + workload on RV.
o Sign and symptom: COPD, pulmonary diseases, venous congestion, visceral distention especially hepatic vein – liver and spleen became engorged –
rising capillary pressure causes fluid shifting into interstitial space causing edema, weight gain, nocturia
● Medication for Heart Failure:
o Cardiac glycosides
▪ Inotropics
o Beta blockers
o Vasodilators
▪ ACEi
▪ ARBs
▪ Nitrates
17 Pharmacology 05 – Cardiovascular and Renal Medication
o Diuretics
▪ Cardiac glycosides
o Action:
▪ Derived from digitalis, which came from foxglove plants. The most frequently used cardiac glycoside is digoxin.
▪ Acts by promoting movement of Ca from extracellular to intracellular. Results to more Ca available to enhance myocardial contractility which
allows ventricles to empty completely. (+) inotropy, increase CO. Also, enhances vagal tone, slowing contractility through SA and AV node:
Negative chronotropic** action
▪ Digoxin has a low therapeutic index, meaning the dose adequate for therapeutic effects may be accompanied by a sign of toxicity.
o Examples: Digoxin (lanoxin)
o Side Effects / Adverse Effects:
▪ Bradycardia, N/V, diarrhea
▪ Digitalis toxicity: anorexia, nausea, vomiting, blurred vision, arrhythmias, PVCs hypokalemia
o Drug interactions:
▪ +K-wasting Diuretics, amiodarone, Ca, propafenone, omeprazole, cyclosporine, macrolides, quinidine, spironolactone, tetracycline = ↑digitalis
toxicity - hypokalemia
▪ +Beta-blockers, CCB, succinylcholine, thyroid medications, diuretics = bradycardia, arrhythmias
▪ +Antacids, barbiturates, cholestyramine, kaolin and pectin, metoclopramide, rifampin, sulfasalazine = ↓GI absorption
o Nsx Action:
▪ Check apical pulse (WOF HR<60), serum drug levels, electrolytes especially K+ levels, and renal function prior to administration.
▪ WOF digitalis toxicity
▪ Antidote: Digifab
● Beta blockers
18 Pharmacology 05 – Cardiovascular and Renal Medication
o Acts by competing with beta-adrenergic receptor sites in the heart muscle and inhibiting release of renin in kidneys, decreasing availability of
angiotensinogen II and aldosterone.
o Beta 1 specific beta blockers are used
● Vasodilators – takes effect on RAAS
o Types:
▪ ACE inhibitors
o Acts on ace enzyme to inhibit conversion of angiotensin I to angiotensin II.
▪ ARBs
o Acts by blocking Angiotensin II from binding to receptors sites in vasculature, preventing vasoconstriction
▪ Nitrates
o ISDN-Organic esters that acts directly on vascular smooth muscles and coronaries – vasodilation - +myocardial O2. Dilation of
peripheral veins, reduces preload and afterload decreasing myocardial O2 demand.
o Hydralazine – decreases systemic arteriolar resistance and decrease afterload.
o Example: Isosorbide Dinitrate (ISDN sublingual), Isosorbide Mononitrate (ISMN oral)
o Drug Interaction: +CCB = orthostatic hypotension; +Erectile dysfunction drugs, alcohol = hypotension
o Side Effects / Adverse Effects: Headache, dizziness, orthostatic hypotension, tachycardia, flushing, palpitation, N/V
o Contraindications: Hypersensitivity, early MI, severe anemia, angle-closure glaucoma, orthostatic hypotension, cardiac tamponade
o Nsx Action:
▪ Teach client on proper use of sublingual tablets
▪ Inform client that headache is common and will subside
▪ Erectile dysfunction drugs must be taken 24 hours before or after taking nitrates
▪ Avoid alcohol
▪ Monitor for tolerance
19 Pharmacology 05 – Cardiovascular and Renal Medication
● Diuretics
o Acts by reducing blood pressure by decreasing circulatory blood volume through increasing of urine output resulting to improve cardiac output.
● Antidysrhythmics
o Movement of ions across the cardiac cell’s membrane results in a spreading across the cardiac electrical impulse cells, which leads to contraction of
the myocardial muscle.
o Electrical conduction of the heart
o Heart rhythm is regulated by the sinoatrial node or the pacemaker of the heart by sending electrical signals initiating the contraction of the heart. As
impulse reaches the atria, AV node will collect these impulses and relay it to bundle of his for then to purkinje fibers ventricles to contract.
o SA node --- AV node --- bundle of his --- purkinje fibers.
o Phases of action potential:
▪ Phase 0 – Rapid entry of Na+. “Depolarization phase”
▪ Phase 1 - balanced NA+ ions intra- and extracellularly
▪ Phase 2 – Plateau phase the cell becomes less permeable to sodium, potassium begins to leave the cell, and calcium starts to enter the cell.
▪ Phase 3 – Rapid repolarization phase which the sodium gates are closed and potassium flows out of the cell.
▪ Phase 4 – Resting phase sodium-potassium pump restores the cell’s resting membrane potential in preparation for the next action potential.
o Types of antidysrhythmics:
▪ Class I Na+ Channel blockers
▪ Class II: Beta blockers
▪ Class III: K+ channel blockers
▪ Class IV: Ca++ channel blockers
o Class I Na+ Channel blockers
▪ Class IA: Quinidine gluconate, procainamide, disopyramide, amiodarone
20 Pharmacology 05 – Cardiovascular and Renal Medication
o Action:
● Control arrhythmias by altering the myocardial cell membrane and interfering with autonomic nervous system control of
pacemaker cells.
● Decrease sodium influx, slows phase 0 in his- purkinje and cardiac muscles.
o Indication: Primarily indicated for decreasing workload of the heart and relieving HF, A-V arrhhythmias
o Side Effects / Adverse Effects:
● Quinidine: increase QT interval, torsades de pointes, thrombocytopenia
o Nsx Action: Hypokalemia, quinidine enhances digitalis toxicity.
▪ Class 1B: lidocaine, mexiletine, tocainide
o Action:
● Decrease Na+ influx in ischemic episode, shortens phase 3 repolarization
● Decrease Action potential duration.
o Indication: Ventricular arrhythmias
o Side Effects / Adverse Effects: CNS toxicity
o Nsx Action: WOF Hyperkalemia
▪ Class 1C: Propafenone
o Action:
● Decrease Na+ influx, markedly slows phase 0 depolarization from bundle of his to purkinje fibers and cardiac muscle
● Slows conduction velocity, increase QRS duration
● Can kill px in excess
o Indication: Last drug for refractory ventricular arrhythmias
o Side Effects / Adverse Effects: forms new form of arrhythmias
o Nsx Action: can precipitate cardiac arrest and sudden death to patients with preexisting cardiac abnormalities.
o Class II: Beta blockers: metoprolol, esmolol, propranolol
21 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Action:
o Decreases SA node automaticity and AV nodal conduction
o Increases PR interval
▪ Indication: SVT, Post MI arrhythmia prophylaxis.
▪ Side Effects / Adverse Effects: impotence, bradycardia, depression, worsens asthma
o Class III: K+ Channel Blockers: sotalol, bretylium, amiodarone
▪ Action:
o Prolonging phase 3 repolarization of action potentials
o increasing effective refractory period.
▪ Indication: AF/ atrial flutter, Ventricular arrhythmias
▪ Side Effects / Adverse Effects: bradycardia, torsades de pointes, photosensitivity, hypotension
o Class IV: Ca++ Channel Blockers: verapamil, diltiazem
▪ Action:
o Acts by blocking CA channels thus slowing AV node conduction
o Shortens AP
▪ Indication: AF/ atrial flutter, AV node reentry.
o Other drugs that affect Action Potential
▪ Adenosine – used for AV node arrhythmias; extremely short acting
▪ MgSO4 – used in digitalis induced arrhythmias; torsades de pointes
▪ KCL – decrease ectopic pacemakers
▪ Digitalis – used in rapid atrial flutter/ fibrillation, AV nodal reentry.
22 Pharmacology 05 – Cardiovascular and Renal Medication
● Anti-anginal Medications
o Angina - occurs when the coronary arteries which supplies the myocardium primarily with oxygen is insufficient. When this happen, myocardial
muscles will not contract efficiently which result’s to increased cardiac workload, increasing heart rate, preload (blood volume in the ventricles at the
end of diastole), afterload (pressure in the arteries leading from the ventricles), and force of myocardial contractility.
o Ischemia – Decreased blood flow to myocardium decreasing oxygen supply.
o Infarct - Obstruction of the blood supply to the heart, causing tissue death.
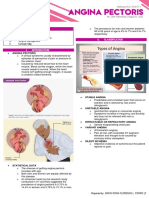
o Types of angina:
▪ Chronic stable angina - Caused by stress; Relieved by rest and NTG.
▪ Unstable angina - AKA pre-infarction or crescendo angina; Occurs at rest; May progress to MI
▪ Vasospastic angina- AKA Prinzmetal’sor variant angina; occurs at rest; Relieved by NGT and CCB
o Three classes of anti-anginal drugs:
▪ Nitrates (treating acute angina)
▪ Beta adrenergic blockers (long term prevention of angina)
▪ Ca+ channel blockers
o Nitrates
▪ Action:
o Acts by relaxing vascular smooth muscles and periphery
o Decreases afterload by general vasodilation, reducing PVR, cardiac workload, O2 demand.
o Can be given SL, bucally, Inhalation, transdermal
▪ Examples: Isosorbide mononitrate (ISMN), Isosorbide Dinitrate (ISDN/Isordil), Nitroglycerin
▪ Drug Interaction
o + alcohol, sildenafil = Severe hypotension
o + CCB – orthostatic hypotension
23 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Side Effects / Adverse Effects: effects usually are decreased when dosage is reduced.
▪ Nsx Action:
oIf taking nitroglycerin sublingually, go to the emergency department if three tablets taken 5 minutes apart don’t relieve anginal pain.
oTake the drug regularly, as prescribed, and have it accessible at all times.
oDon’t discontinue the drug abruptly without your prescriber’s approval. Coronary vasospasm can occur.
oUse caution when wearing a transdermal patch near a microwave oven. Leaking radiation may heat the metallic backing of the patch
and cause burns.
o Avoid alcohol during drug therapy.
o Remove a used transdermal patch before applying a new one.
o Change to an upright position slowly. Go up and down stairs carefully, and lie down at the first sign of dizziness.
o Store nitrates in a cool, dark place in a tightly closed container. To ensure freshness, replace sublingual tablets every 3 months and
remove the cotton because it absorbs the drug.
o If taking with other medications, withhold drug if PR is <60bpm.
o Beta Adrenergic Blockers
▪ Acts by competing with beta-adrenergic receptor sites in the heart muscle and inhibiting release of renin in kidneys, decreasing availability of
angiotensinogen II and aldosterone.
o Ca+ channel blockers
▪ These drugs prevent the passage of Ca ions into cell membrane of myocardial smooth muscle and peripheral arteriolar vasculature results in
arteriolar vasodilation, decrease cardiac workload, BP, afterload thereby decreasing also O2 demand of the heart.
F. Antilipidemics and Peripheral Blood Flow Medications
o Medications used to lower abnormally high blood levels of lipids, such as cholesterol, triglycerides, and phospholipids
o Used in combination with lifestyle changes, such as proper diet, weight loss, and exercise.
o Types of Antilipemic Medications:
o Bile-Sequestering Drugs
o Fibric Acid Derivatives
24 Pharmacology 05 – Cardiovascular and Renal Medication
o HMG-COA Reductase Inhibitors
o Nicotinic Acid
o Cholesterol Absorption Inhibitors
● Bile-sequestering drugs
o Action: Body compensates by converting hepatic cholesterol to bile acids. Decrease in level of hepatic cholesterol then triggers increase in number of
LDL receptors which clears LDL-cholesterol in blood.
o Examples: cholestyramine, colesevelam, and colestipol hydrochloride.
o Indication: Treatment of Type IIa hyperlipoproteinemia (familial hypercholesterolemia) in a patient who isn’t able to lower LDL levels through
dietary changes.
o Drug Interaction:
▪ Interferes with digoxin, oral phosphate and hydrocortisone
▪ + propranolol, tetracycline, furosemide, HCTZ, penG = decreases absorption.
o Nsx Action:
▪ WOF bleeding. It reduces absorption of Vit. A, D, E, K.
▪ Take the drug exactly as prescribed. If you take a bile sequestering drug, never take the dry form. Esophageal irritation or severe constipation
may result.
▪ Dilute powder form to water, milk and juice. X carbonated drinks – excess foaming.
▪ Diet is very important in controlling serum lipid levels. Maintain proper dietary management of serum lipids (restricting total fat and
cholesterol intake) as well as control of other cardiac disease risk factors.
▪ Drink 2 to 3 qt (2 to 3 L) of fluid daily, and report persistent or severe constipation.
▪ Weight control, exercise, and smoking cessation programs may be appropriate.
▪ If you also take bile acid resin, take fenofibrate 1 hour before or 4 to 6 hours after bile acid resin.
25 Pharmacology 05 – Cardiovascular and Renal Medication
▪ When taking fenofibrate, promptly report symptoms of unexplained muscle weakness, pain, or tenderness, especially if accompanied by
malaise or fever.
● Fibric Acid Derivatives
o Action:
▪ Fenofibrate and gemfibrozil are absorbed readily from the GI tract and are highly protein bound. Fenofibrate undergoes rapid hydrolysis, and
gemfibrozil undergoes extensive metabolism in the liver.
▪ Reduces cholesterol production early in its formation and mobilize cholesterol from the tissues and increase cholesterol excretion.
▪ Given at night because nakakagising
o Drug Interaction: + anticoagulants = increase bleeding tendencies.
● HMG-COA Reductase Inhibitors
o Action:
▪ 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors
▪ Inhibits HMG-CoA reductase resulting to decrease in hepatic cholesterol synthesis. It then triggers an increase in number of LDL receptors which
binds LDL-cholesterol thus further reducing cholesterol concentration in plasma.
▪ Lower lipid levels by interfering with cholesterol synthesis.
o Example: Atorvastatin, Rosuvastatin and simvastatin
o Drug Interaction:
▪ + niacin, -mycin, fluoroquinolones = increases myopathy (muscle wasting & weakness) or rhabdomyolysis which potentiate renal failure.
▪ Lovastatin and simvastatin + warfarin = increase bleeding
o Nsg. Consideration:
▪ All HMG-CoA reductase inhibitors should be administered 1 hour before or 4 hours after bile-sequestering drugs (cholestyramine, colestipol,
colesevelam).
26 Pharmacology 05 – Cardiovascular and Renal Medication
● Nicotinic acid
o Action:
▪ Niacin is a water-soluble vitamin that decreases triglyceride and apolipoprotein B-100 levels and increases HDL levels.
▪ Inhibiting hepatic synthesis of lipoproteins that contain apolipoprotein B-100, promoting lipoprotein lipase activity, reducing free fatty acid
mobilization from adipose tissue, and increasing fecal elimination of sterols.
o Contraindication: hypersensitive to nicotinic acid and in those with hepatic or renal dysfunction, active peptic ulcer disease, gout, heart disease,
muscle disorder, or arterial bleeding
o Side Effects / Adverse Effects:
▪ + HMG-CoA reductase inhibitor will potentiate life-threatening breakdown of skeletal muscle, causing renal failure or rhabdomyolysis.
▪ Vasodilation and flushing – may take ASA 30mins before nicotinic acid at night.
▪ Hepatotoxicity, N/V, diarrhea, epigastric pain or substernal pain.
● Cholesterol Absorption Inhibitors
o Indication: inhibit the absorption of cholesterol and related phytosterols from the small intestine.
o Drug Interaction:
▪ Cholestyramine may decrease the effectiveness of ezetimibe.
▪ Fenofibrate, gemfibrozil, and cyclosporine lead to an increased level of ezetimibe.
o Side Effects / Adverse Effects: Back pain, fatigue, abdominal pain, pharyngitis
o Nsx Action:
▪ Monitor blood cholesterol and lipid levels before and periodically during therapy. Monitor the drug’s effectiveness by checking cholesterol and
triglyceride levels every 4 weeks or by asking the patient whether pruritus has diminished or abated as appropriate.
▪ Monitor CK levels when therapy begins and every 6 months thereafter. Also check CK levels if a patient who takes a cholesterol synthesis inhibitor
complains of muscle pain.
▪ Monitor the patient for fat-soluble vitamin deficiency
27 Pharmacology 05 – Cardiovascular and Renal Medication
G. Anticoagulants
● Used to reduce the ability of the blood to clot or promote hemostasis.
● In order for this ability of blood to happen, a system or a step by step coagulation should happen for it to effectively stop the bleeding.
● Blood clot or thrombus will form at the site of bleeding.
● Embolus – clot that moves inside the blood vessels which is more prone to cause a problem to a smaller vessel like in the brain which can cause ischemic
stroke. In order for this not to happen, a tissue plasminogen activator is used to dissolve clots.
● Hemostasis – process of the body which seals an injured or a ruptured blood vessel and prevent further bleeding and platelets are key players in this
process.
● Steps in Hemostatis:
1. Vascular spasm -blood vessels constrict for blood not to leak.
2. Formation of platelet plug – as blood vessel ruptures exposing endothelial lining, platelet release clotting proteins at site and Von Willebrand
factor assist in platelet aggregation to stabilize platelet plug formation
3. Coagulation – is a mechanism of blood to further stabilize a blood clot.
● Coagulation cascade – Mechanism of clotting in which it is activated by chemicals called clotting factors.
● Initiated in two pathways:
o Extrinsic pathway – usually triggered by trauma
o Intrinsic pathway – are triggered by internal damage to the intimal layers of blood vessels (9, 11, 12)
o Common pathway – 10, 5 , 2, 1
● Both meet at a common pathway by activating prothrombin (X) factor and convert it to thrombin where eventually activate fibrinogen to form fibrin and
reinforced by clot stabilizing factor (XIII) creating a more blood clot promoting hemostasis.
● Types of Anticoagulants:
o Heparin (intrinsic)
28 Pharmacology 05 – Cardiovascular and Renal Medication
o Warfarin (extrinsic)
o Antiplatelets
o Factor XA inhibitors
o Thrombolytic drugs
● Heparin
o Action: Combines with antithrombin III to inactivate thrombin and inhibits fibrinogen to be converted to fibrin thus preventing clot formation.
o Indication: DVT, Pulmonary embolism, DIC, unstable angina, post MI, cerebral thrombosis, Heart failure, atrial fibrillation.
o Side Effects / Adverse Effects: bruising, hematoma formation, skin necrosis and thrombocytopenia
o Contraindications: stroke, peptic ulcer, coagulation disorders, active bleeding and severe thrombocytopenia.
o Nsx Action:
▪ Monitor the patient for adverse effects, such as hemorrhage, prolonged clotting time, thrombocytopenia, and hypersensitivity reactions.
▪ Regularly inspect the patient for bleeding gums, bruises, petechiae, epistaxis, tarry stools, hematuria, and hematemesis.
▪ Monitor partial thromboplastin time regularly.
▪ Inject SQ heparin and enoxaparin into abdomen; don’t aspirate or rub injection site, and rotate injection site
▪ Antidote: Protamine sulfate
● Warfarin
o Action: Inhibits Vit. K synthesis in the liver
o Indications: prevent pulmonary embolism caused by DVT, MI, prosthetic heart valves or chronic AF.
o Side Effects / Adverse Effects: hemorrhage, prolonged bleeding time, hepatitis
o Drug Interaction: + alcohol = increases risk of bleeding.
o Nsx Action:
▪ Monitor for gum bleeding, bruises, petechiae, epistaxis, tarry stools, hematuria, and hematemesis.
▪ Limit patient intake of dark green leafy vegetables.
▪ Monitor prothrombin time regularly.
29 Pharmacology 05 – Cardiovascular and Renal Medication
▪ Antidote: Phytomenadione (Vit.K)
● Antiplatelets
o Action: Arrests platelet aggregation thereby preventing thrombolytic events.
o Examples: aspirin, clopidogrel, dipyridamole, ticlopidine, abciximab, tirofiban.
o Indication: Prophylaxis for thromboembolic events particularly in patients at risk for MI, stroke, and arteriosclerosis
o Side Effects / Adverse Effects: Bleeding, pancytopenia, neutropenia, hemorrhage, thrombocytopenic purpura, abnormal stools, pain at injection
site.
o Contraindication: Active bleeding, thrombocytopenia, severe liver impairment, underlying coagulation disorder, ulcer disease, recent surgery,
cancer
o Nsx Action:
▪ Monitor and assess client for bruising and bleeding
▪ Minimize venipunctures and injections; apply pressure to all puncture sites
▪ Monitor hemoglobin, clotting factors and platelet levels
● Factor Xa inhibitors
o Action: Interferes the coagulation pathway by neutralizing factor Xa which inhibits thrombin and thrombus formation especially newly formed
thrombi.
o Examples: fondaparinux
o Drug Interaction: +antiplatelets, NSAIDs = ↑risk for hemorrhage
o Side Effects / Adverse Effects: bleeding, nausea, anemia, fever, rash, constipation, edema.
o Contraindications / Precautions: Active bleeding, thrombocytopenia, renal impairment, bacterial endocarditis
o Nsx Action:
▪ Monitor for s/sx of bleeding
▪ Monitor clotting time
● Thrombolytics
30 Pharmacology 05 – Cardiovascular and Renal Medication
o Action: Dissolves an existing thrombus by converting plasminogen to plasmin which lyses thrombi and other plasma proteins and commonly used
in an acute or emergency situations.
o Example: alteplase, reteplase, tenecteplase, urokinase, and streptokinase.
o Indication: thromboembolic disorders such as AMI, acute ischemic stroke, PAOD.
o Side Effects / Adverse Effects: Bleeding, arrhythmias, urticartia, fever, hemorrhage
o Contraindications: active internal bleeding, recent stroke, coagulation disorders, ulcer, recent surgery, cancer, uncontrolled HPN
o Nsx Action:
▪ Monitor the patient for adverse effects, such as arrhythmias, bleeding, pulmonary edema, and hypersensitivity reactions.
▪ Monitor the patient frequently for bleeding.
▪ Antidote: aminocaproic acid
ACTIVITY 4: DISCUSSION / EXERCISE
● Ask the class for any questions that they may have regarding the lecture.
ACTIVITY 5: POST TEST
ACTIVITY 6: SYNTHESIS / EXERCISE
● Summarize the lesson, highlighting the salient points.
Prepared by: Reviewed by: Approved by:
Dr. Frederick Christian T. Calamaan, RN, MD Dennis Luis D. Abellera, RN MAN Dr. John Michael O. Lorena, RN
Lecturer Academic Head Dean
31 Pharmacology 05 – Cardiovascular and Renal Medication
32 Pharmacology 05 – Cardiovascular and Renal Medication
You might also like
- 5fcdfd7d3d29a PDFDocument177 pages5fcdfd7d3d29a PDFAnamika100% (1)
- IM Platinum 3rd-EdDocument357 pagesIM Platinum 3rd-EdJust Some Files100% (2)
- Haemodynamic Monitoring & Manipulation: an easy learning guideFrom EverandHaemodynamic Monitoring & Manipulation: an easy learning guideNo ratings yet
- Nursing Board Review CardioDocument16 pagesNursing Board Review CardioPhilip Simangan100% (1)
- Small Animal Cardiology PDFDocument208 pagesSmall Animal Cardiology PDFRoberto AmpueroNo ratings yet
- Amiodarone Infusion ProtocolsDocument1 pageAmiodarone Infusion ProtocolsHennaNo ratings yet
- General Discussion ScheduleDocument28 pagesGeneral Discussion ScheduleJOPEARL MAE DELA TORRENo ratings yet
- CVS Physio D&R AgamDocument76 pagesCVS Physio D&R AgambennitaraisingNo ratings yet
- 418-M2-CU6 Hemodynamics and CardiophysiologyDocument12 pages418-M2-CU6 Hemodynamics and CardiophysiologyPaul SahagunNo ratings yet
- 2 The Initial Assessment: Prioritizing Care Delivery: Cliff EvansDocument24 pages2 The Initial Assessment: Prioritizing Care Delivery: Cliff EvansJa YaNo ratings yet
- 452l Simulation 6 Pre SimulationDocument9 pages452l Simulation 6 Pre Simulationapi-307439819No ratings yet
- Course Code NCM 112 Week/ DAY Week: Cardiovascular SystemDocument60 pagesCourse Code NCM 112 Week/ DAY Week: Cardiovascular SystemAycee ElardoNo ratings yet
- Cardiovascular SyllabusDocument13 pagesCardiovascular SyllabusBrandonGilbertNo ratings yet
- SepsisDocument11 pagesSepsisesha.k35No ratings yet
- Clin Cardiology CasesDocument34 pagesClin Cardiology CasesSunny Singh0% (1)
- Session #34 SAS - AnaPhy (Lab)Document7 pagesSession #34 SAS - AnaPhy (Lab)Cristina SottoNo ratings yet
- Stress Test: BY: Jobelyn Delena Tunay, RNDocument92 pagesStress Test: BY: Jobelyn Delena Tunay, RNJobelyn TunayNo ratings yet
- 02 PH Course Unit 7-1Document31 pages02 PH Course Unit 7-1Hannah Mae PiraNo ratings yet
- Clinical Trials On HipertensionDocument13 pagesClinical Trials On HipertensionIpsus LiterisNo ratings yet
- Student Guidedsadas Cardiology 2015Document11 pagesStudent Guidedsadas Cardiology 2015tiramesu22No ratings yet
- A Head Nurse Oversees Nursing Activities in A Range of Health Care SettingsDocument8 pagesA Head Nurse Oversees Nursing Activities in A Range of Health Care SettingsMitch MaLagambaNo ratings yet
- Ccu Handbook 2Document44 pagesCcu Handbook 2Nikunj GariaNo ratings yet
- Cardiology Literature ReviewDocument8 pagesCardiology Literature Reviewaflsvwoeu100% (2)
- Perioperative Blood Pressure Control and ManagementDocument17 pagesPerioperative Blood Pressure Control and ManagementNathalia gallegoNo ratings yet
- Материал Для Студентов Занятие 1Document45 pagesМатериал Для Студентов Занятие 1Nikhil GuptaNo ratings yet
- Relaxation Therapy and Continuous Ambulatory Blood Hypertension: Controlled StudyDocument5 pagesRelaxation Therapy and Continuous Ambulatory Blood Hypertension: Controlled StudyKang Opik TaufikNo ratings yet
- Monitoreo Hemodinamico Funcional PinskyDocument23 pagesMonitoreo Hemodinamico Funcional PinskyJuan CarrascoNo ratings yet
- 6 Pack Sept 2013-OEC-Shock-Chapter 10 - NSPDocument23 pages6 Pack Sept 2013-OEC-Shock-Chapter 10 - NSPDonavon GaudetteNo ratings yet
- NCMB 312 MS RLE WEEK 15 Concept Mapping GI BleedingDocument2 pagesNCMB 312 MS RLE WEEK 15 Concept Mapping GI BleedinggabbyNo ratings yet
- Detailed Learning Module 7.2.PdDocument10 pagesDetailed Learning Module 7.2.PdRanz Kenneth G. FrandoNo ratings yet
- Arizmendi G72 T10Document6 pagesArizmendi G72 T10IrvinSerranoJNo ratings yet
- Anaes Tutorial 1 - DR - MungrooDocument8 pagesAnaes Tutorial 1 - DR - MungrooChris DwarikaNo ratings yet
- Hypertensive Cardiovascular DiseaseDocument16 pagesHypertensive Cardiovascular DiseaseTintin Ponciano100% (1)
- Monitoring of Critically Ill PatientDocument11 pagesMonitoring of Critically Ill PatientAnusikta PandaNo ratings yet
- Hypertension Manuscript PrintDocument15 pagesHypertension Manuscript PrintLyca LunaNo ratings yet
- Sepsis Parte 1Document16 pagesSepsis Parte 1Maria AlejandraNo ratings yet
- Review Article: Elevated Blood Pressure in The Acute Phase of Stroke and The Role of Angiotensin Receptor BlockersDocument8 pagesReview Article: Elevated Blood Pressure in The Acute Phase of Stroke and The Role of Angiotensin Receptor BlockersPatrick RamosNo ratings yet
- PAM Metas Terapéuticas y Soporte FarmocológicoDocument9 pagesPAM Metas Terapéuticas y Soporte FarmocológicoHernando CastrillónNo ratings yet
- Screenshot 2022-03-29 at 3.15.04 AMDocument16 pagesScreenshot 2022-03-29 at 3.15.04 AMMuhammad Javed GabaNo ratings yet
- Methods of Evaluation of Autonomic Nervous System Function: Agnieszka Zygmunt, Jerzy StanczykDocument8 pagesMethods of Evaluation of Autonomic Nervous System Function: Agnieszka Zygmunt, Jerzy StanczykUzra ShujaatNo ratings yet
- Stress Testing and ECG.. (Poonam Soni)Document14 pagesStress Testing and ECG.. (Poonam Soni)Poonam soniNo ratings yet
- Cardiovascular WorksheetDocument4 pagesCardiovascular WorksheetAnonymous V7A9OKNo ratings yet
- NCMB 418 Hemodynamics Week 7Document34 pagesNCMB 418 Hemodynamics Week 7Jennifer Ambrosio100% (1)
- Cardiovascular Case Study Jan 2 101xDocument4 pagesCardiovascular Case Study Jan 2 101xElizabeth SpokoinyNo ratings yet
- PHARMA - Module 03 - ANS Drugs HDocument16 pagesPHARMA - Module 03 - ANS Drugs HArthur Brian PanitNo ratings yet
- Chapter 66 Nursing Management Critical CareDocument29 pagesChapter 66 Nursing Management Critical CaretroillerdrippyNo ratings yet
- Mary Cris Canon CHF For or Case Study.Document12 pagesMary Cris Canon CHF For or Case Study.Mary Cris CanonNo ratings yet
- 2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014Document142 pages2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014PkernNo ratings yet
- Explaning How The Hearth Work The AnswerDocument2 pagesExplaning How The Hearth Work The Answerdiah ayuNo ratings yet
- Monitoring of Critically Ill Patient Presented byDocument12 pagesMonitoring of Critically Ill Patient Presented byMansi PatelNo ratings yet
- Acute Biologic Crisis: Prepared By: Joanalain C. Cortez, RNDocument80 pagesAcute Biologic Crisis: Prepared By: Joanalain C. Cortez, RNMark Cada100% (2)
- Cardiovascular System: AnatomyDocument19 pagesCardiovascular System: AnatomyStephanie MacVeighNo ratings yet
- Critical Care PASSTHEMRCSDocument131 pagesCritical Care PASSTHEMRCSthinzarNo ratings yet
- A Case Study of Chronic Calculous CholecystitisDocument9 pagesA Case Study of Chronic Calculous CholecystitisMeine Mheine0% (1)
- HeartDocument7 pagesHeartEmmanuel A. GalvanNo ratings yet
- Article Presentation-2Document35 pagesArticle Presentation-2Savita HanamsagarNo ratings yet
- PBL PgamboaDocument6 pagesPBL PgamboaLeanne Princess GamboaNo ratings yet
- Selected Nursing Diagnoses and Interventions For Patients With DysrhythmiasDocument19 pagesSelected Nursing Diagnoses and Interventions For Patients With Dysrhythmiaslanie_jecielNo ratings yet
- Health Assessment SAS Session 14Document9 pagesHealth Assessment SAS Session 14Maria Jub MangrubanNo ratings yet
- A Case Presentation On Cerebrovascular Accident InfarctDocument57 pagesA Case Presentation On Cerebrovascular Accident InfarctKeepItSecretNo ratings yet
- Advanced Clinical Therapies in Cardiovascular Chinese MedicineFrom EverandAdvanced Clinical Therapies in Cardiovascular Chinese MedicineNo ratings yet
- Job DescriptionDocument5 pagesJob DescriptionHarshavardhan SNo ratings yet
- 1 s2.0 S0735109723055444 MainDocument10 pages1 s2.0 S0735109723055444 MainamadoNo ratings yet
- Cerebral CirculationDocument25 pagesCerebral Circulation20AR018 HARIHARA SUBRAMANIANNo ratings yet
- Angina PectorisDocument3 pagesAngina PectorisGwyn Oona Florence ForroNo ratings yet
- (IJETA-V7I3P2) : Sai Sruthi Gadde, Venkata Dinesh Reddy KalliDocument5 pages(IJETA-V7I3P2) : Sai Sruthi Gadde, Venkata Dinesh Reddy KalliIJETA - EighthSenseGroupNo ratings yet
- 1) Problem Statement: Dietary Approaches To Stop Hypertension (DASH) in Terms ofDocument2 pages1) Problem Statement: Dietary Approaches To Stop Hypertension (DASH) in Terms ofPrasann RoyNo ratings yet
- Various DocsDocument8 pagesVarious DocssamNo ratings yet
- Vascular DisordersDocument13 pagesVascular DisordersMichelle Dona MirallesNo ratings yet
- 579-Article Text-1710-1-10-20220113Document10 pages579-Article Text-1710-1-10-20220113Nurul AdibahNo ratings yet
- A Guide To Electrical Safety in Construction and IndustryDocument69 pagesA Guide To Electrical Safety in Construction and IndustryNitish GunessNo ratings yet
- DR Amao Core Principles of Interpreting Ecg TracingDocument39 pagesDR Amao Core Principles of Interpreting Ecg Tracingdan ekelemeNo ratings yet
- Arterial PulsesDocument14 pagesArterial PulsesPrajwal Rao KNo ratings yet
- NURSING CARE PLAN - JayDocument8 pagesNURSING CARE PLAN - JayJaylord VerazonNo ratings yet
- In-Hospital Cardiac Arrest Epidemiology in A Mature Rapid Response SystemDocument6 pagesIn-Hospital Cardiac Arrest Epidemiology in A Mature Rapid Response SystemmartinNo ratings yet
- Article - Billing and Coding - Non-Invasive Peripheral Arterial Vascular Studies (A57593)Document33 pagesArticle - Billing and Coding - Non-Invasive Peripheral Arterial Vascular Studies (A57593)Michael Lopez OlivaNo ratings yet
- Electrocardiography: Quicktime™ and A Tiff (Uncompressed) Decompressor Are Needed To See This PictureDocument31 pagesElectrocardiography: Quicktime™ and A Tiff (Uncompressed) Decompressor Are Needed To See This PicturemkhandakerNo ratings yet
- Dialog English Nurs and Patient NewDocument6 pagesDialog English Nurs and Patient NewRisma Faudiyah100% (1)
- BT CT Hess Test Clot Retraction TimeDocument30 pagesBT CT Hess Test Clot Retraction Timecharutha gopalNo ratings yet
- 21 GMS Bedah JantungDocument140 pages21 GMS Bedah JantungNuravif SetianingrumNo ratings yet
- Nejmoa 2024816Document11 pagesNejmoa 2024816Cessar OrnlsNo ratings yet
- ! Exercise Physiology and Its Role in Clinical Sports MedicineDocument6 pages! Exercise Physiology and Its Role in Clinical Sports MedicineАлексNo ratings yet
- Ecg Interpretation: Presented by:-ROHINI RAI M SC Nursing Part I, C.O.N, N.B.M.C.HDocument69 pagesEcg Interpretation: Presented by:-ROHINI RAI M SC Nursing Part I, C.O.N, N.B.M.C.HRohini RaiNo ratings yet
- Axillary MethodDocument5 pagesAxillary MethodJerica Jaz F. VergaraNo ratings yet
- Nature Review, Complete RevascularizationDocument14 pagesNature Review, Complete RevascularizationIván De LeónNo ratings yet
- SANTHOSH JENNIFER MARIA LABEX 24 Ant. Abd Wall and CavityDocument9 pagesSANTHOSH JENNIFER MARIA LABEX 24 Ant. Abd Wall and CavityJENNIFER MARIA SANTHOSHNo ratings yet
- Classification of Sports: Type of Exercise PerformedDocument2 pagesClassification of Sports: Type of Exercise PerformedAnh MinhNo ratings yet
- Hypovolemic Shock: Dr. Sherwin BuluranDocument8 pagesHypovolemic Shock: Dr. Sherwin BuluranChristian UretaNo ratings yet
- Physioex Lab Report: Pre-Lab Quiz ResultsDocument4 pagesPhysioex Lab Report: Pre-Lab Quiz ResultsPavel MilenkovskiNo ratings yet