Professional Documents
Culture Documents
Ultrasound Diagnosis and Doppler Monitoring of A Pelvic Spleen in Pregnancy
Uploaded by
denisegmeloOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ultrasound Diagnosis and Doppler Monitoring of A Pelvic Spleen in Pregnancy
Uploaded by
denisegmeloCopyright:
Available Formats
Ultrasound Obstet Gynecol 2001; 17: 453 – 454
Ultrasound diagnosis and Doppler monitoring of
Case Report
Blackwell Science, Ltd
a pelvic spleen in pregnancy
L. COBELLIS, F. DI PIETTO*, L. DI PIETTO*, L. STRADELLA*, F. M. REIS, F. M. SEVERI and
F. PETRAGLIA
Department of Obstetrics and Gynecology, University of Siena, Siena and *Department of Obstetrics and Gynecology, Second University of Naples,
Naples, Italy
K E Y W OR DS: Spleen, Ectopic spleen, Pelvic mass, Pregnancy, Doppler monitoring
ABSTRACT CASE REPORT
We describe a patient with a pelvic spleen diagnosed during A 40-year-old primigravida woman was referred at 8 weeks
pregnancy and monitored through gestation which we of gestation because of a continuous and intense pain in her
believe to be the first reported case. A 40-year-old woman lower abdomen which spread to the lower back. Her blood
was referred at 8 weeks of gestation because of a chronic count was normal and no associated urinary or gastrointest-
intense pain in the left iliac cavity which had spread to her inal symptoms were reported.
lower back. Clinical examination revealed a poorly defined The clinical examination showed the uterus to be slightly
pelvic mass. Pelvic ultrasound demonstrated a gestational sac increased in volume and displaced to the right by a relatively
containing a viable embryo whose size was consistent with immobile mass of poorly defined limits which partially occupied
the period of amenorrhea. While the splenic area in the left the pelvis and the left iliac cavity and which was not painful
hypocondrium was found to be empty, a homogeneous and on palpation. Pelvic ultrasound evaluation (transabdominal
elongate mass measuring 152 × 123 mm with a maximum thick- and transvaginal scan) confirmed the uterus to be displaced
ness of 53.4 mm was observed in the left iliac cavity above the to the right. It contained a gestational sac and a single embryo
uterus. This mass, the ectopic spleen, was monitored by Doppler with evidence of cardiac activity and a crown–rump length of
velocimetry at monthly intervals until delivery and no vari- 10.7 mm, corresponding to 7 + 4 weeks of gestation.
ation throughout gestation was observed; therefore, despite A uniformly echogenic elongate mass (Figure 1) with a lon-
the occasional occurrence of heavy pain, it was possible to gitudinal diameter of 152 mm, a width of 123 mm and a
exclude circulatory complications such as thrombosis or maximum thickness of 53.4 mm was detected in the pelvis
torsion. Doppler ultrasound proved to be a useful tool for above the anterior uterine wall. The splenic area in the left
the differential diagnosis of this rare anatomical variation. hypocondrium was empty. Color and pulsed Doppler scan-
ning of the mass demonstrated that it was richly perfused and
color signals were uniformly present throughout. The vessels
converged in the postero-inferior pole (Figure 2). These find-
INTRODUCTION
ings were characteristic of a pelvic spleen. Color Doppler
The ectopic or migrant spleen in the pelvic area is a rare imaging showed a hilus at the inferior pole of the spleen with
occurrence which, with the increasing use of imaging methods, three vessels corresponding to two arteries and one vein. The
especially ultrasound, has become relatively easy to diagnose vessels emerged from the posterior surface and continued in
in the non-pregnant patient1–5. It should be differentiated the cranial direction on the left side up to the hypocondrium.
from an accessory spleen which has occasionally been observed Numerous collateral vessels were observed in the paren-
during surgical operations6,7. chyma. The arterial and venous vessels at the hilus and in the
Pregnancy, because of its continuous evolution, has the extrasplenic side were patent and without signs of thrombosis.
potential to modify the position of an anomalous spleen and lead At the hilus, the mean venous flow velocity was 18 cm/s, with
to circulatory complications such as torsion or compression. a waveform showing steady flow; the arterial flow velocity
To our knowledge this is the first case of a migrant spleen (peak systolic) was 68 cm/s. The extrasplenic side recorded
in the pelvic area to be diagnosed during pregnancy. The a venous flow velocity of 38 cm/s with powerful modulation of
ultrasound diagnosis at 8 gestational weeks and the findings the waveform by maternal respiration; the arterial peak systolic
of serial Doppler examinations until delivery are described. velocity was 70 cm/s. The flow velocity of the splenic vein at
Correspondence: Dr L. Cobellis, Via Santa Lucia n.39, 80132 Napoli, Italy (e-mail: luigicobellis@yahoo.it)
Received 29-2-00, Revised 27-10-00, Accepted 21-2-01
CASE REPORT 453
Ultrasound diagnosis of pelvic spleen in pregnancy Cobellis et al.
the point of convergence with the portal vein was 27 cm/s with
steady respiratory modulation. Doppler examination per-
formed after the disappearance of the pain showed the same
characteristics. The spleen gradually shifted from the pelvic
area to the left iliac fossa and its dimensions remained unchanged.
Doppler was repeated at monthly intervals and did not
show any variation until at the end of pregnancy. A Cesarean
section was performed at 38 weeks because of the anomalous
position of the spleen; a female neonate weighing 3450 g was
delivered. During surgery the spleen was examined and was
found to be smooth with no residue of any ligament (Figure 3).
The vascular pedicle arose from the splenic hilus and continued
upwards through the omentum to the left hypocondrium.
The postoperative course and the puerperium were normal. Six
days after surgical intervention an ultrasound examination con-
firmed that the spleen was still positioned in the pelvic area.
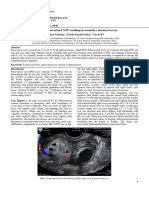
Figure 1 Transabdominal scan of the normal gestational sac (SACCO DISCUSSION
GESTAZIONALE) with embryo (dotted line) and ectopic spleen seen as
This case shows that the presence of a pelvic spleen does
a uniformly echogenic mass (MILZA ECTOPICA).
not necessarily produce complications during the course of
pregnancy and that it can continue to function despite its
anomalous position. One might expect the developing preg-
nancy to modify the position of the spleen causing com-
plications, particularly of the circulation, such as torsion
or compression. However, the uneventful outcome in our
patient indicates that an uneventful evolution is possible in
similar cases.
Although rare, pelvic spleen is a well-documented entity
that should be considered in the differential diagnosis of all
pelvic masses. Although usually asymptomatic, the ectopic
spleen in our case was characterized by some symptoms includ-
ing pelvic pain, heaviness and urinary frequency. Doppler
monitoring of the ectopic spleen circulation through gestation
offered reassurance by demonstrating the absence of vascular
Figure 2 Color Doppler interrogation of the ectopic spleen vessels complications. In fact, the use of Doppler ultrasound in our
demonstrates a typical arterial blood flow pattern. case enabled expectant management until term.
REFERENCES
1 Cendrowsky K, Sawicki W, Stelmachow J, Wypych K. Ectopic
spleen in pelvis minor — a case report. Ginekol Pol 1992; 63: 312–4
2 Azar GB, Awwad JT, Mufarrij IK. Accessory spleen presenting as
adnexal mass. Acta Obstet Gyn Scan 1993; 72: 587–8
3 Popovic M, Knezevic S, Colovic R, Petrovici M, Antunovic P,
Diordejvic Z. Ectopic spleen — 2 case reports. Acta Chir Jugosl 1995;
42: 59–62
4 Kalid A, Lawton F. Pelvic spleen masquerading as an ovarian neo-
plasm. Ann Acad Med Singapore 1998; 27: 710–1
5 Cohen MS, Sper NJ, Underwood RA, Brut LM. Laparoscopic
splenopexy for wandering (pelvic) spleen. Surg Laparosc Endosc
1998; 8: 286–90
6 Hatfield PM, Clouse ME, Cady B. Ectopic pelvic spleen. Arch Surg
1976; 111: 603–5
7 Carswell JW. Wandering spleen: 33 cases from Uganda. Br J Surg
Figure 3 Ectopic spleen at Cesarean section. 1974; 61: 495–7
454 Ultrasound in Obstetrics and Gynecology
You might also like
- Case-Presentation Final Nagd Ni ShetDocument7 pagesCase-Presentation Final Nagd Ni ShetMary Beth AbelidoNo ratings yet
- Suh 2016Document4 pagesSuh 2016Christian Leonardo Molina HinojosaNo ratings yet
- Term Live Primary Ovarian Pregnancy A Case ReportDocument4 pagesTerm Live Primary Ovarian Pregnancy A Case ReportNico PlantadoNo ratings yet
- Abrasio PlacentaDocument3 pagesAbrasio Placentamuhammad azamNo ratings yet
- Pregnancy in a Didelphic Uterus- A case ReportDocument7 pagesPregnancy in a Didelphic Uterus- A case ReportAmin BashyrNo ratings yet
- Massive Hydronephrosis Masquerading as Pelvic CystDocument3 pagesMassive Hydronephrosis Masquerading as Pelvic CystAniydaNo ratings yet
- Couvelaire Uterus: Manju Rathi, Sunil Kumar Rathi, Manju Purohit, Ashish PathakDocument2 pagesCouvelaire Uterus: Manju Rathi, Sunil Kumar Rathi, Manju Purohit, Ashish PathakMDreamerNo ratings yet
- Sonographic Findings in Acute Urinary Retention Secondary To Retroverted Gravid Uterus: Pathophysiology and Preventive MeasuresDocument6 pagesSonographic Findings in Acute Urinary Retention Secondary To Retroverted Gravid Uterus: Pathophysiology and Preventive MeasuresEndrianus Jaya PutraNo ratings yet
- BJSTR MS Id 003341Document4 pagesBJSTR MS Id 003341herryNo ratings yet
- Anorectal MalformationDocument4 pagesAnorectal MalformationFawzia Haznah Nurul ImaniNo ratings yet
- Bab 34 RadiologiDocument37 pagesBab 34 Radiologireyza octarientNo ratings yet
- Uterine Torsion Doppler Ovary Artery-Rood-2014Document3 pagesUterine Torsion Doppler Ovary Artery-Rood-2014RizzaNo ratings yet
- The Wandering Spleen With Collateral Vessels Containing Gastric Varices - Color Doppler Ultrasound ImagingDocument5 pagesThe Wandering Spleen With Collateral Vessels Containing Gastric Varices - Color Doppler Ultrasound ImagingdenisegmeloNo ratings yet
- Various Sonographic Appearances of The Hemorrhagic Corpus Luteum CystDocument14 pagesVarious Sonographic Appearances of The Hemorrhagic Corpus Luteum CystBerry BancinNo ratings yet
- A Burkitt's Lymphoma Case Mimicking Crohn's Disease A Case ReportDocument5 pagesA Burkitt's Lymphoma Case Mimicking Crohn's Disease A Case ReportErnesto PintoNo ratings yet
- Antenatal Treatment of Hydrocephalus via Ventriculoamniotic ShuntingDocument2 pagesAntenatal Treatment of Hydrocephalus via Ventriculoamniotic ShuntingRendra Artha Ida BagusNo ratings yet
- A Rare Shape of Placenta Placenta Bipartite, Bilobata, Dimidiate, Duplex: A Rare Case ReportDocument3 pagesA Rare Shape of Placenta Placenta Bipartite, Bilobata, Dimidiate, Duplex: A Rare Case ReportVandana Liju Dev VasudevanNo ratings yet
- Prenatal Diagnosis of Four-Vessel Umbilical Cord With Supernumerary Vein Varix - A Case Report and Literature ReviewDocument5 pagesPrenatal Diagnosis of Four-Vessel Umbilical Cord With Supernumerary Vein Varix - A Case Report and Literature ReviewMina zhouNo ratings yet
- Cecal Perforation Case Report After C-SectionDocument5 pagesCecal Perforation Case Report After C-SectionTasya SylviaNo ratings yet
- Diagnosis and Management of Intramural Ectopic PregnancyDocument4 pagesDiagnosis and Management of Intramural Ectopic PregnancyDinorah MarcelaNo ratings yet
- Sonographic Whirlpool Sign in Ovarian Torsion: S. Boopathy Vijayaraghavan, MD, DMRDDocument7 pagesSonographic Whirlpool Sign in Ovarian Torsion: S. Boopathy Vijayaraghavan, MD, DMRDjohnalanNo ratings yet
- Hernia Uterine Inguinale: An Uncommon Cause of Pelvic Pain in The Adult Female PatientDocument4 pagesHernia Uterine Inguinale: An Uncommon Cause of Pelvic Pain in The Adult Female PatientJeje MoNo ratings yet
- Case Report: Anorectal Malformation: Paediatric Problem Presenting in AdultDocument5 pagesCase Report: Anorectal Malformation: Paediatric Problem Presenting in Adultsuci triana putriNo ratings yet
- Mullerian Agenesis: An Unusual Presentation As Hematometra and Bilateral HematosalpinxDocument2 pagesMullerian Agenesis: An Unusual Presentation As Hematometra and Bilateral Hematosalpinxwanwan_adongNo ratings yet
- Power Doppler Sonographic Diagnosis of Torsion in A Wandering SpleenDocument3 pagesPower Doppler Sonographic Diagnosis of Torsion in A Wandering SpleendenisegmeloNo ratings yet
- Leong Et Al-2004-BJOG: An International Journal of Obstetrics & GynaecologyDocument2 pagesLeong Et Al-2004-BJOG: An International Journal of Obstetrics & GynaecologyAngie MandeoyaNo ratings yet
- Jurnal Bumil Pingsan 3Document4 pagesJurnal Bumil Pingsan 3rina astutiNo ratings yet
- Gastric Perforation in The Neonate: Ludvig OicmianDocument6 pagesGastric Perforation in The Neonate: Ludvig OicmianagusNo ratings yet
- Ultrasound in Obstet Gyne - 2005 - Jauniaux - The Role of Ultrasound Imaging in Diagnosing and Investigating EarlyDocument12 pagesUltrasound in Obstet Gyne - 2005 - Jauniaux - The Role of Ultrasound Imaging in Diagnosing and Investigating EarlySofiat WahabNo ratings yet
- Three Dimensional Sonography in The Exploration of Voiding Dysfunction in Retroverted Impacted Adenomyosis A Case ReportDocument3 pagesThree Dimensional Sonography in The Exploration of Voiding Dysfunction in Retroverted Impacted Adenomyosis A Case ReportAniyah LaguindabNo ratings yet
- Bink Horst 2010Document3 pagesBink Horst 2010Fahmi MuhammadNo ratings yet
- Abdominopelvic Ectopic Spleen With A Comprehensive Imaging Examination: A Case ReportDocument6 pagesAbdominopelvic Ectopic Spleen With A Comprehensive Imaging Examination: A Case ReportceciliaNo ratings yet
- Ultrasound Features of Spermatic Cord Hydrocele in ChildrenDocument3 pagesUltrasound Features of Spermatic Cord Hydrocele in ChildrenEnricoFermihutagalungNo ratings yet
- Laparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportDocument11 pagesLaparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportAdlyn Bea Albesa-BernaldezNo ratings yet
- AkretaDocument7 pagesAkretaInna SeraLaratNo ratings yet
- 2 5 21 861 PDFDocument3 pages2 5 21 861 PDFAhmed ZidanNo ratings yet
- Case 3-1996Document6 pagesCase 3-1996K. O.No ratings yet
- Renal Bruit Due To Aberrant Renal Vessels: Indian Pediatrics VOLUME 32-MARCH1995Document3 pagesRenal Bruit Due To Aberrant Renal Vessels: Indian Pediatrics VOLUME 32-MARCH1995ShamNo ratings yet
- Laparoscopic RepairDocument3 pagesLaparoscopic RepairDominique WilsonNo ratings yet
- Piriformis Pyomyositis, An Unusual Presentation of Leg Pain Post Partum Case Report and Review of LiteratureDocument4 pagesPiriformis Pyomyositis, An Unusual Presentation of Leg Pain Post Partum Case Report and Review of Literaturesatyagraha84No ratings yet
- Jurnal THTDocument46 pagesJurnal THTShida ZakariaNo ratings yet
- Chronic Uterine InversionDocument4 pagesChronic Uterine InversionnurelianaNo ratings yet
- Cervical Pessary in Prevention of Preterm BirthDocument6 pagesCervical Pessary in Prevention of Preterm BirthAlessandra CruzNo ratings yet
- An Antenatal Appearance of Megacystis-Microcolon-Intestinal Hypoperistalsis SyndromeDocument8 pagesAn Antenatal Appearance of Megacystis-Microcolon-Intestinal Hypoperistalsis SyndromeserubimNo ratings yet
- CD006476 AbstractDocument4 pagesCD006476 AbstractfkNo ratings yet
- Adult Canal of Nuck Hydrocele Poster PresentationDocument17 pagesAdult Canal of Nuck Hydrocele Poster PresentationRajkanta KarmakarNo ratings yet
- Jurnal Anomali Vagina WordDocument5 pagesJurnal Anomali Vagina WordFelNo ratings yet
- Fibrocystic Disease of the Pancreas in NewbornsDocument6 pagesFibrocystic Disease of the Pancreas in NewbornsA. Arviani Desianti NurNo ratings yet
- Case Series of Unusual Causes Intestinal Obstruction in Infants and ChildrenDocument9 pagesCase Series of Unusual Causes Intestinal Obstruction in Infants and ChildrenSnega KaranNo ratings yet
- Urologie - Bencherki Youssef - Giant Abscessed Urachal in AdultDocument1 pageUrologie - Bencherki Youssef - Giant Abscessed Urachal in AdultYoussef BencherkiNo ratings yet
- Fetal Axillary Cystic Hygroma Detected by Prenatal UltrasonographyDocument3 pagesFetal Axillary Cystic Hygroma Detected by Prenatal UltrasonographywitaNo ratings yet
- Filling of The Bladder For Pelvic Sonograms: An Ancient Form of TortureDocument3 pagesFilling of The Bladder For Pelvic Sonograms: An Ancient Form of Torturemjk deguzmanNo ratings yet
- Krok2 - Medicine - 2007Document26 pagesKrok2 - Medicine - 2007Badriya YussufNo ratings yet
- 01 Ajpcr 46717Document3 pages01 Ajpcr 46717DipteshPatilNo ratings yet
- Ultrasound Evaluation Fetal Genitourinary SystemDocument12 pagesUltrasound Evaluation Fetal Genitourinary SystemAudrey100% (2)
- GYNE UltrasoundgyneDocument11 pagesGYNE UltrasoundgyneMara AbantoNo ratings yet
- RACE Annotated ObsDocument35 pagesRACE Annotated ObsIsmath JahangirNo ratings yet
- Term Alive Intra Abdominal Ectopic Pregnancy: Case ReportDocument3 pagesTerm Alive Intra Abdominal Ectopic Pregnancy: Case ReportLeannarys Mendoza DelgadoNo ratings yet
- Nod 3Document4 pagesNod 3Sidonia CatalinaNo ratings yet
- Splenic Hemodynamics and Decreased Endothelial Nitric Oxide Synthase in The Spleen of Rats With Liver CirrhosisDocument9 pagesSplenic Hemodynamics and Decreased Endothelial Nitric Oxide Synthase in The Spleen of Rats With Liver CirrhosisdenisegmeloNo ratings yet
- Power Doppler Sonographic Diagnosis of Torsion in A Wandering SpleenDocument3 pagesPower Doppler Sonographic Diagnosis of Torsion in A Wandering SpleendenisegmeloNo ratings yet
- Splanchnic Blood Flow in Patients With Cirrhosis and Portal Hypertension - Investigation With Duplex Doppler USDocument6 pagesSplanchnic Blood Flow in Patients With Cirrhosis and Portal Hypertension - Investigation With Duplex Doppler USdenisegmeloNo ratings yet
- Suspected Relative Adrenal Insufficiency in A Critically Ill CatDocument5 pagesSuspected Relative Adrenal Insufficiency in A Critically Ill CatdenisegmeloNo ratings yet
- Preserving Food Drying Fruits and VegetablesDocument12 pagesPreserving Food Drying Fruits and Vegetablespdxpharris100% (1)
- Duconmix CRP 400Document2 pagesDuconmix CRP 400FounTech612No ratings yet
- Aircraft Instruments and Avionics PDFDocument211 pagesAircraft Instruments and Avionics PDFairbuk doeing88% (8)
- Casa de Moda DolcegabbanaDocument4 pagesCasa de Moda Dolcegabbanadianaionelav23No ratings yet
- Examination of Power Electronics (Pel) : AnswerDocument10 pagesExamination of Power Electronics (Pel) : Answerves vegasNo ratings yet
- Jear C PB 2018 PDFDocument174 pagesJear C PB 2018 PDFArasu RajendranNo ratings yet
- Wartsila Tribo PackDocument7 pagesWartsila Tribo Packsuper_seeker100% (1)
- SorghumDocument13 pagesSorghumMohaajanan AliNo ratings yet
- Measuring Instruments Temperature GuideDocument52 pagesMeasuring Instruments Temperature GuidemohammedhanafyNo ratings yet
- Sampling Methods for Terrestrial Amphibians and ReptilesDocument39 pagesSampling Methods for Terrestrial Amphibians and ReptilesBenzu Shawn100% (1)
- EXERCISE - (JEE Main) Chemical Equilibrium - CombinedDocument24 pagesEXERCISE - (JEE Main) Chemical Equilibrium - CombinedKeerthana Reddy DomaNo ratings yet
- Introducion To Load Cells UtilcellDocument22 pagesIntroducion To Load Cells UtilcellRifi MohamedNo ratings yet
- Rear Derailleur: Important Notice Names of PartsDocument1 pageRear Derailleur: Important Notice Names of PartsRyan MulyanaNo ratings yet
- Designing Resistance Training Programmes To Enhance Muscular Fitness A Review of The Acute Programme VariablesDocument12 pagesDesigning Resistance Training Programmes To Enhance Muscular Fitness A Review of The Acute Programme VariablesSheilani MartinsNo ratings yet
- Cambridge O Level: English Language 1123/22Document4 pagesCambridge O Level: English Language 1123/22Shania SeneviratneNo ratings yet
- Manual Book IOG ConventionDocument17 pagesManual Book IOG ConventionTaufiq MaulanaNo ratings yet
- "Fish" From Gourmet RhapsodyDocument4 pages"Fish" From Gourmet RhapsodySean MattioNo ratings yet
- 2 Way 3 Way Piping DiagramDocument1 page2 Way 3 Way Piping DiagrammarrukhjNo ratings yet
- 1-Well Completion I PDFDocument20 pages1-Well Completion I PDFHomam MohammadNo ratings yet
- Brooks MT 3018Document16 pagesBrooks MT 3018Martin AndradeNo ratings yet
- Section - A: Holiday Homework For Grade XiDocument7 pagesSection - A: Holiday Homework For Grade XiGM Ali KawsarNo ratings yet
- CHEMDocument20 pagesCHEMValli RamalingamNo ratings yet
- Constance Carroll Cosmetics) Final.1Document4 pagesConstance Carroll Cosmetics) Final.1api-26027438100% (1)
- 3023 History Cuisine WorksheetDocument6 pages3023 History Cuisine WorksheetFlor HenríquezNo ratings yet
- Handling Silica in Cooling WaterDocument17 pagesHandling Silica in Cooling WaterLekhamani YadavNo ratings yet
- BC-5300 Preventive Maintenance Kit ManualDocument8 pagesBC-5300 Preventive Maintenance Kit ManualAbdel MUNDENNo ratings yet
- Entrepreneurs That Changed The Face of IndiaDocument4 pagesEntrepreneurs That Changed The Face of Indiamarykavitha_6No ratings yet
- Duarte Et Al - Resin CementsDocument28 pagesDuarte Et Al - Resin Cementsjfrascarolo100% (4)
- Life Wealth Mastery EnglishDocument12 pagesLife Wealth Mastery EnglishD.j. Ralmm100% (1)
- Continuous Renal Replacement TherapyDocument9 pagesContinuous Renal Replacement Therapydoc_next_doorNo ratings yet