Professional Documents
Culture Documents
ECG Electrocardiography Guide
Uploaded by
Ariyana0 ratings0% found this document useful (0 votes)
8 views115 pages- An electrocardiogram (ECG) records electric potentials generated by the heart using electrodes attached to the body. It provides a noninvasive test to detect arrhythmias, conduction issues, and other cardiac problems.
- The ECG shows waveforms representing atrial and ventricular depolarization and repolarization. P waves indicate atrial depolarization, the QRS complex shows ventricular depolarization, and the ST-T complex reflects ventricular repolarization.
- ECG leads are arranged to detect electrical signals from different angles, including limb leads on the frontal plane and chest leads on the horizontal plane. Together these leads can be used to determine the cardiac electrical axis.
Original Description:
elektrokardiografi dasar
Original Title
EKG dasar
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document- An electrocardiogram (ECG) records electric potentials generated by the heart using electrodes attached to the body. It provides a noninvasive test to detect arrhythmias, conduction issues, and other cardiac problems.
- The ECG shows waveforms representing atrial and ventricular depolarization and repolarization. P waves indicate atrial depolarization, the QRS complex shows ventricular depolarization, and the ST-T complex reflects ventricular repolarization.
- ECG leads are arranged to detect electrical signals from different angles, including limb leads on the frontal plane and chest leads on the horizontal plane. Together these leads can be used to determine the cardiac electrical axis.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views115 pagesECG Electrocardiography Guide
Uploaded by
Ariyana- An electrocardiogram (ECG) records electric potentials generated by the heart using electrodes attached to the body. It provides a noninvasive test to detect arrhythmias, conduction issues, and other cardiac problems.
- The ECG shows waveforms representing atrial and ventricular depolarization and repolarization. P waves indicate atrial depolarization, the QRS complex shows ventricular depolarization, and the ST-T complex reflects ventricular repolarization.
- ECG leads are arranged to detect electrical signals from different angles, including limb leads on the frontal plane and chest leads on the horizontal plane. Together these leads can be used to determine the cardiac electrical axis.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 115
Electrocardiography
Dr Budi Enoch
- An electrocardiogram (ECG or EKG) is a graphic recording of
electric potentials generated by the heart. The signals are
detected by means of metal electrodes attached to the extremities
and chest wall and then are amplified and recorded by the
electrocardiograph. ECG leads actually display the instantaneous
differences in potential between the electrodes.
- The clinical utility of the ECG derives from its immediate
availability as a noninvasive, inexpensive, and highly versatile
test.
- In addition to its use in detecting arrhythmias, conduction
disturbances, and myocardial ischemia, electrocardiography may
reveal other findings related to life-threatening metabolic
disturbances (e.g., hyperkalemia) or increased susceptibility to
sudden cardiac death (e.g., QT prolongation syndromes).
Electrophysiology
• Depolarization of the heart is the initiating event for
cardiac contraction. The electric currents that spread
through the heart are produced by three components:
cardiac pacemaker cells, specialized conduction tissue,
and the heart muscle itself.
• The ECG, however, records only the depolarization
(stimulation) and repolarization (recovery) potentials
generated by the atrial and ventricular myocardium.
• The depolarization stimulus for the normal heartbeat
originates in the sinoatrial (SA) node, or sinus node, a
collection of pacemaker cells. These cells fire
spontaneously; that is, they exhibit automaticity
Kita melihat defleksi positif atau negatif, tergantung dari rresultante arah
arus listriknya, contohnya pada elektroda yang terpasang didada
• The first phase of cardiac electrical activation is the spread
of the depolarization wave through the right and left atria,
followed by atrial contraction.
• Next, the impulse stimulates pacemaker and specialized
conduction tissues in the atrioventricular (AV) nodal and
His-bundle areas; together, these two regions constitute
the AV junction.
• The bundle of His bifurcates into two main branches, the
right and left bundles, which rapidly transmit
depolarization wavefronts to the right and left ventricular
myocardium by way of Purkinje fibers.
• The main left bundle bifurcates into two primary
subdivisions: a left anterior fascicle and a left posterior
fascicle. The depolarization wavefronts then spread
through the ventricular wall, from endocardium to
epicardium, triggering ventricular contraction.
• Since the cardiac depolarization and
repolarization waves have direction and
magnitude, they can be represented by vectors.
• Vector analysis illustrates a central concept of
electrocardiography: The ECG records the
complex spatial and temporal summation of
electrical potentials from multiple myocardial
fibers conducted to the surface of the body.
• This principle accounts for inherent limitations in
both ECG sensitivity (activity from certain cardiac
regions may be canceled out or may be too weak
to be recorded) and specificity (the same
vectorial sum can result from either a selective
gain or a loss of forces in opposite directions).
ECG Waveforms and Intervals
• The ECG waveforms are labeled alphabetically,
beginning with the P wave, which represents
atrial depolarization
• The QRS complex represents ventricular
depolarization, and the ST-T-U complex (ST
segment, T wave, and U wave) represents
ventricular repolarization.
• The J point is the junction between the end of the
QRS complex and the beginning of the ST
segment.
• Atrial repolarization is usually too low in
amplitude to be detected, but it may become
apparent in conditions such as acute pericarditis
and atrial infarction
5 garis besar vertikal menandakan 1 detik, sedangkan 1 garis
besar horizontal menyatakan kekuatan arus 1 millivolt.
Gambaran ini adalah gambaran normal EKG yang diambil pada
satu bagian elektroda
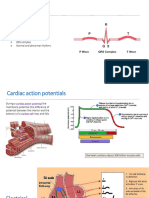
• The QRS-T waveforms of the surface ECG correspond in
a general way with the different phases of
simultaneously obtained ventricular action potentials,
the intracellular recordings from single myocardial
fibers .
• The rapid upstroke (phase 0) of the action potential
corresponds to the onset of QRS. The plateau (phase 2)
corresponds to the isoelectric ST segment, and active
repolarization (phase 3) corresponds to the inscription
of the T wave.
• Factors that decrease the slope of phase 0 by impairing
the influx of Na+ (e.g., hyperkalemia and drugs such as
flecainide) tend to increase QRS duration. Conditions
that prolong phase 2 (amiodarone, hypocalcemia)
increase the QT interval. In contrast, shortening of
ventricular repolarization (phase 2), such as by digitalis
administration or hypercalcemia, abbreviates the ST
segment.
• The electrocardiogram ordinarily is recorded on special
graph paper that is divided into 1-mm2 gridlike boxes.
• Since the ECG paper speed is generally 25 mm/s, the
smallest (1 mm) horizontal divisions correspond to 0.04 (40
ms), with heavier lines at intervals of 0.20 s (200 ms).
• Vertically, the ECG graph measures the amplitude of a
specific wave or deflection (1 mV = 10 mm with standard
calibration; the voltage criteria for hypertrophy mentioned
below are given in millimeters).
• There are four major ECG intervals: R-R, PR, QRS, and QT .
The heart rate (beats per minute) can be computed readily
from the interbeat (R-R) interval by dividing the number of
large (0.20 s) time units between consecutive R waves into
300 or the number of small (0.04 s) units into 1500.
• The PR interval measures the time (normally 120–200 ms)
between atrial and ventricular depolarization, which
includes the physiologic delay imposed by stimulation of
cells in the AV junction area
ECG Leads
• The 12 conventional ECG leads record the difference in
potential between electrodes placed on the surface of the
body. These leads are divided into two groups: six limb
(extremity) leads and six chest (precordial) leads. The limb
leads record potentials transmitted onto the frontal plane, and
the chest leads record potentials transmitted onto the
horizontal plane
• The spatial orientation and polarity of the six frontal plane
leads is represented on the hexaxial diagram.
• The six chest leads are unipolar recordings obtained by
electrodes in the following positions: lead V1, fourth intercostal
space, just to the right of the sternum; lead V2, fourth
intercostal space, just to the left of the sternum; lead V3,
midway between V2 and V4; lead V4, midclavicular line, fifth
intercostal space; lead V5, anterior axillary line, same level as
V4; and lead V6, midaxillary line, same level as V4 and V5.
Limb lead mencatat perbedaan potensial listrik secara
berdepanan (frontal plane)
chest lead mencatat perbedaan potensial listrik secara
horizontal (horizontal plane) potongan melintang
Axis dan Deviasi
Frontal plane direpresentasikan dalam diagram hexoaxial, tiap lead
mempunyai orientasi pandangan dan polaritas (kutub positif) tersendiri.
Kutub (+) ditera dalam garis solid, kutub (-) dalam garis putus2. Karena itu
itu kita dapat menentukan axis dari jantung
Dengan menghitung jumlah arus pada kompleks QRS di lead I
dan dibandingan dengan jumlah arus pada kompleks QRS di
lead II kita bisa menentukan axis jantung (cardiac vector)
secara pastinya axis ini bisa dihitung dengan memakai daftar
Genesis of the Normal ECG
P Wave
• The normal atrial depolarization vector is oriented
downward and toward the subject's left, reflecting the
spread of depolarization from the sinus node to the
right and then the left atrial myocardium.
• Since this vector points toward the positive pole of
lead II and toward the negative pole of lead aVR, the
normal P wave will be positive in lead II and negative in
lead aVR.
• By contrast, activation of the atria from an ectopic
pacemaker in the lower part of either atrium or in the
AV junction region may produce retrograde P waves
(negative in lead II, positive in lead aVR). The normal P
wave in lead V1 may be biphasic with a positive
component reflecting right atrial depolarization,
followed by a small (<1 mm2) negative component
reflecting left atrial depolarization.
QRS Complex
• Normal ventricular depolarization proceeds as a rapid, continuous
spread of activation wave fronts. This complex process can be
divided into two major sequential phases, and each phase can be
represented by a mean vector .
• The first phase is depolarization of the interventricular septum from
the left to the right and anteriorly (vector 1). The second results
from the simultaneous depolarization of the right and left
ventricles; it normally is dominated by the more massive left
ventricle, so that vector 2 points leftward and posteriorly.
• Therefore, a right precordial lead (V1) will record this biphasic
depolarization process with a small positive deflection (septal r
wave) followed by a larger negative deflection (S wave). A left
precordial lead, e.g., V6, will record the same sequence with a small
negative deflection (septal q wave) followed by a relatively tall
positive deflection (R wave). Intermediate leads show a relative
increase in R-wave amplitude (normal R-wave progression) and a
decrease in S-wave amplitude progressing across the chest from
right to left. The precordial lead where the R and S waves are of
approximately equal amplitude is referred to as the transition zone
(usually V3 or V4)
T Wave and U Wave
• Normally, the mean T-wave vector is oriented roughly
concordant with the mean QRS vector (within about 45° in
the frontal plane). Since depolarization and repolarization
are electrically opposite processes, this normal QRS–T-
wave vector concordance indicates that repolarization
normally must proceed in the reverse direction from
depolarization (i.e., from ventricular epicardium to
endocardium).
• The normal U wave is a small, rounded deflection (1 mm)
that follows the T wave and usually has the same polarity
as the T wave. An abnormal increase in U-wave amplitude
is most commonly due to drugs (e.g., dofetilide,
amiodarone, sotalol, quinidine, procainamide,
disopyramide) or to hypokalemia.
• Very prominent U waves are a marker of increased
susceptibility to the torsades de pointes type of ventricular
tachycardia . Inversion of the U wave in the precordial leads
is abnormal and may be a subtle sign of ischemia
konfigurasi
• EKG biasanya direkam pada kecepatan 25
mm/detik sehingga jarak antara 2 garis besar
berdiri adalah 0,2 detik yang berisi 5 garis
berdiri yang lebih halus. Akibatnya jarak
antara tiap garis halus berdiri adalah 0,04
detik
• Cara termudah untuk menghitung frekwensi
jantung adalah bagikan 300 dengan jumlah jarak
diantara 2 garis besar berdiri pada 2 irama jantung
yang berurutan
• Frekwensi jantung : Jumlah dari segiempat besar
diantara 2 komplex yang berurutan
• 300 x/mnt 1 (300/1)
• 150 x/mnt 2 (300/2)
• 100 x/mnt 3 (300/3)
• 75 x/mnt 4 (300/4)
• dan seterusnya.
Grup sadapan 2, Lead penguatan (augmented
unipolar lead)
• Sadapannya dikenal dengan AVR (augmented right),
AVL (augmented left) dan AVF (augmented left lead)
• AVR adalah lead dimana hanya elektroda postif pada
lengan kanan sedangkan elektroda lain indeferen
(unipolar lead)
• AVL elektrodanya pada lengan kanan
• AVF elektrodanya pada kaki kiri
• Maksud dari lead ini adalah untuk melihat resultante
arus listrik jantung langsung dari arah kanan atas
(AVR), dari arah kiri atas (AVL) dan dari bawah atau
dinding inferior jantung (AVF)
Major ECG Abnormalities
Cardiac Enlargement and
Hypertrophy
• Right atrial overload (acute or chronic) may lead
to an increase in P-wave amplitude (2.5 mm).
• Left atrial overload typically produces a biphasic P
wave in V1 with a broad negative component or a
broad (120 ms), often notched P wave in one or
more limb leads.
• This pattern may also occur with left atrial
conduction delays in the absence of actual atrial
enlargement, leading to the more general
designation of left atrial abnormality
• Right ventricular hypertrophy due to a pressure load
(as from pulmonic valve stenosis or pulmonary artery
hypertension) is characterized by a relatively tall R
wave in lead V1 (R S wave), usually with right axis
deviation; alternatively, there may be a qR pattern in V1
or V3R. ST depression and T-wave inversion in the right-
to-midprecordial leads are also often present.
• This pattern, formerly called right ventricular "strain,"
is attributed to repolarization abnormalities in acutely
or chronically overloaded muscle.
• Prominent S waves may occur in the left lateral
precordial leads. Right ventricular hypertrophy due to
ostium secundum–type atrial septal defects, with the
accompanying right ventricular volume overload, is
commonly associated with an incomplete or complete
right bundle branch block pattern with a rightward QRS
axis.
Bundle Branch Blocks
• Intrinsic impairment of conduction in either the right or the left bundle
system (intraventricular conduction disturbances) leads to prolongation of
the QRS interval.
• With complete bundle branch blocks, the QRS interval is 120 ms in duration;
with incomplete blocks, the QRS interval is between 100 and 120 ms. The
QRS vector usually is oriented in the direction of the myocardial region
where depolarization is delayed .
• Thus, with right bundle branch block, the terminal QRS vector is oriented to
the right and anteriorly (rSR' in V1 and qRS in V6, typically).
• Left bundle branch block alters both early and later phases of ventricular
depolarization. The major QRS vector is directed to the left and posteriorly.
In addition, the normal early left-to-right pattern of septal activation is
disrupted such that septal depolarization proceeds from right to left as well.
As a result, left bundle branch block generates wide, predominantly
negative (QS) complexes in lead V1 and entirely positive (R) complexes in
lead V6. A pattern identical to that of left bundle branch block, preceded by
a sharp spike, is seen in most cases of electronic right ventricular pacing
because of the relative delay in left ventricular activation.
• Bundle branch block may occur in a variety of conditions.
• In subjects without structural heart disease, right bundle
branch block is seen more commonly than left bundle
branch block.
• Right bundle branch block also occurs with heart disease,
both congenital (e.g., atrial septal defect) and acquired
(e.g., valvular, ischemic).
• Left bundle branch block is often a marker of one of four
underlying conditions associated with increased risk of
cardiovascular morbidity and mortality rates: coronary
heart disease (frequently with impaired left ventricular
function), hypertensive heart disease, aortic valve
disease, and cardiomyopathy.
• Bundle branch blocks may be chronic or intermittent. A
bundle branch block may be rate-related; for example, it
often occurs when the heart rate exceeds some critical
value.
Myocardial Ischemia and
Infarction
• The ECG is a cornerstone in the diagnosis of acute and
chronic ischemic heart disease. The findings depend on
several key factors: the nature of the process reversible
(i.e., ischemia) versus irreversible (i.e., infarction), the
duration (acute versus chronic), the extent (transmural
versus subendocardial), and localization (anterior versus
inferoposterior), as well as the presence of other
underlying abnormalities (ventricular hypertrophy,
conduction defects).
• Ischemia exerts complex time-dependent effects on the
electrical properties of myocardial cells.
• Severe, acute ischemia lowers the resting membrane
potential and shortens the duration of the action
potential. Such changes cause a voltage gradient
between normal and ischemic zones. As a consequence,
current flows between those regions. These currents of
injury are represented on the surface ECG by deviation
of the ST segment
• When the acute ischemia is transmural, the ST vector usually
is shifted in the direction of the outer (epicardial) layers,
producing ST elevations and sometimes, in the earliest stages
of ischemia, tall, positive so-called hyperacute T waves over
the ischemic zone.
• With ischemia confined primarily to the subendocardium, the
ST vector typically shifts toward the subendocardium and
ventricular cavity, so that overlying (e.g., anterior precordial)
leads show ST-segment depression (with ST elevation in lead
aVR).
• Multiple factors affect the amplitude of acute ischemic ST
deviations. Profound ST elevation or depression in multiple
leads usually indicates very severe ischemia.
• From a clinical viewpoint, the division of acute myocardial
infarction into ST-segment elevation and non-ST elevation
types is useful since the efficacy of acute reperfusion therapy
is limited to the former group.
• The ECG leads are usually more helpful in localizing
regions of ST elevation than non-ST elevation ischemia.
For example, acute transmural anterior (including
apical and lateral) wall ischemia is reflected by ST
elevations or increased T-wave positivity in one or
more of the precordial leads (V1–V6) and leads I and
aVL.
• Inferior wall ischemia produces changes in leads II, III,
and aVF. "Posterior" wall ischemia (usually associated
with lateral or inferior involvement) may be indirectly
recognized by reciprocal ST depressions in leads V1 to
V3 (thus constituting an ST elevation "equivalent" acute
coronary syndrome).
• Right ventricular ischemia usually produces ST
elevations in right-sided chest leads (Fig. 228-5).
• When ischemic ST elevations occur as the earliest sign of acute
infarction, they typically are followed within a period ranging from
hours to days by evolving T-wave inversions and often by Q waves
occurring in the same lead distribution.
• Reversible transmural ischemia, for example, due to coronary
vasospasm (Prinzmetal's variant angina and probably the Tako-
Tsubo "stress" cardiomyopathy syndrome), may cause transient ST-
segment elevations without development of Q waves, as may very
early reperfusion in acute coronary syndromes.
• Depending on the severity and duration of ischemia, the ST
elevations may resolve completely in minutes or be followed by T-
wave inversions that persist for hours or even days.
• Patients with ischemic chest pain who present with deep T-wave
inversions in multiple precordial leads (e.g., V1–V4) with or without
cardiac enzyme elevations typically have severe obstruction in the
left anterior descending coronary artery system.
• In contrast, patients whose baseline ECG already shows abnormal
T-wave inversions may develop T-wave normalization
(pseudonormalization) during episodes of acute transmural
ischemia.
• With infarction, depolarization (QRS) changes often accompany
repolarization (ST-T) abnormalities.
• Necrosis of sufficient myocardial tissue may lead to decreased R-wave
amplitude or abnormal Q waves (even in the absence of transmurality) in
the anterior or inferior leads.
• Previously, abnormal Q waves were considered markers of
transmuralmyocardial infarction, whereas subendocardial infarcts were
thought not to produce Q waves.
• However, careful ECG-pathology correlative studies have indicated that
transmural infarcts may occur without Q waves and that subendocardial
(nontransmural) infarcts sometimes may be associated with Q waves.
• Therefore, infarcts are more appropriately classified as "Q-wave" or "non-
Q-wave."
• Loss of depolarization forces due to posterior or lateral infarction may cause
reciprocal increases in R-wave amplitude in leads V1 and V2 without
diagnostic Q waves in any of the conventional leads.
• Atrial infarction may be associated with PR-segment deviations due to an
atrial current of injury, changes in P-wave morphology, or atrial arrhythmias.
• In the weeks and months after infarction, these
ECG changes may persist or begin to resolve.
• Complete normalization of the ECG after Q-wave
infarction is uncommon but may occur,
particularly with smaller infarcts.
• In contrast, ST-segment elevations that persist for
several weeks or more after a Q-wave infarct
usually correlate with a severe underlying wall
motion disorder (akinetic or dyskinetic zone),
although not necessarily a frank ventricular
aneurysm.
• ECG changes due to ischemia may occur
spontaneously or may be provoked by various
exercise protocols (stress electrocardiography)
• The ECG has important limitations in both sensitivity
and specificity in the diagnosis of ischemic heart
disease.
• Although a single normal ECG does not exclude
ischemia or even acute infarction, a normal ECG
throughout the course of an acute infarct is distinctly
uncommon.
• Prolonged chest pain without diagnostic ECG changes
therefore should always prompt a careful search for
other noncoronary causes of chest pain.
• Furthermore, the diagnostic changes of acute or
evolving ischemia are often masked by the presence of
left bundle branch block, electronic ventricular
pacemaker patterns, and Wolff-Parkinson-White
preexcitation.
• However, clinicians continue to overdiagnose ischemia
or infarction based on the presence of ST-segment
elevations or depressions; T-wave inversions; tall,
positive T waves; or Q waves not related to ischemic
heart disease (pseudoinfarct patterns).
• For example, ST-segment elevations simulating
ischemia may occur with acute pericarditis or
myocarditis, as a normal variant (including the typical
"early repolarization" pattern), or in a variety of other
conditions.
• Similarly, tall, positive T waves do not invariably
represent hyperacute ischemic changes but may also
be caused by normal variants, hyperkalemia,
cerebrovascular injury, and left ventricular volume
overload due to mitral or aortic regurgitation, among
other causes
• ST-segment elevations and tall, positive T waves are
common findings in leads V1 and V2 in left bundle
branch block or left ventricular hypertrophy in the
absence of ischemia.
• The differential diagnosis of Q waves includes
physiologic or positional variants, ventricular
hypertrophy, acute or chronic noncoronary myocardial
injury, hypertrophic cardiomyopathy, and ventricular
conduction disorders.
• Digoxin, ventricular hypertrophy, hypokalemia, and a
variety of other factors may cause ST-segment
depression mimicking subendocardial ischemia.
• Prominent T-wave inversion may occur with ventricular
hypertrophy, cardiomyopathies, myocarditis, and
cerebrovascular injury (particularly intracranial bleeds),
among many other conditions
aritmia
• Secara klinis waktu meraba nadi, mendengarkan
bunyi jantung dan mengukur tensi kita sudah bisa
menemukan suatu aritmia tetapi kita belum lagi
mengetahui JENIS dari kelainan irama ini
• Diagnosis TEPAT dari suatu aritmia hanya bisa
dibuat dnegan EKG. Berhubungan dengan itu
akan diperhatikan contoh-contoh EKG dari semua
aritmia dengan sekedar keterangannya
• Untuk analisis aritmia kordis perlu diperhatikan
gelombang P/Interval PR/ kompleks QRS (lebar &
konfigurasi)/ hubungan antara P-wave &
QRS/irama dasar/frekuensi
• ARITMIA dapat kita bagi dalam jenis-jenis
KELAINAN SINUS NODE dan ATRIUM
• Aritmia sinus (fiiologis)
• Takhikardia sinus
• Flutter atrium
• Paroxysmal supraventricular tachycardia (PAT)
• Multifocal (chaotic) atrial tachycardia (MAT)
• Sick sinus syndrome
• Bradikardia sinus
• Atrial premature beats
• Fibrilasi atrium (AF)
KELAINAN AV NODE dan VENTRIKEL
• Ventricular ectopic beats = ventricular
premature contractions (VPCs)
• Ventricular tachycardia (VT)
• Ventricular fibrillation (VF)
• Accelerated idioventricular rhythm (AIVR)
• AV junctional tachycardia
• Junctional ectopic beats
• Long QT-syndrome
KELAINAN KONDUKSI
• Sinoatrial exit block
• Sick sinus syndrome
• Intraventricular conductions defect (termasuk
BBB)
• AV block (tingkat I, II, dan III)
• Antrioventricular dissociation
Tachyaritmia
AritmiaLethal
Metabolic Factors and Drug Effects
• A variety of metabolic and pharmacologic agents alter
the ECG and, in particular, cause changes in
repolarization (ST-T-U) and sometimes QRS
prolongation.
• Certain life-threatening electrolyte disturbances may
be diagnosed initially and monitored from the ECG.
• Hyperkalemia produces a sequence of changes, usually
beginning with narrowing and peaking (tenting) of the
T waves. Further elevation of extracellular K+ leads to
AV conduction disturbances, diminution in P-wave
amplitude, and widening of the QRS interval.
• Severe hyperkalemia eventually causes cardiac arrest
with a slow sinusoidal type of mechanism ("sine-wave"
pattern) followed by asystole
Clinical Interpretation of the
ECG
• Accurate analysis of ECGs requires thoroughness and
care. The patient's age, gender, and clinical status
should always be taken into account.
• Many mistakes in ECG interpretation are errors of
omission. Therefore, a systematic approach is essential.
• The following 14 points should be analyzed carefully in
every ECG: (1) standardization (calibration) and
technical features (including lead placement and
artifacts), (2) rhythm, (3) heart rate, (4) PR interval/AV
conduction, (5) QRS interval, (6) QT/QTc interval, (7)
mean QRS electrical axis, (8) P waves, (9) QRS voltages,
(10) precordial R-wave progression, (11) abnormal Q
waves, (12) ST segments, (13) T waves, (14) U waves.
• Only after analyzing all these points should the
interpretation be formulated.
• Where appropriate, important clinical correlates or
inferences should be mentioned.
• For example, sinus tachycardia with QRS and QT-
(U) prolongation, especially in the context of
changes in mental status, suggests tricyclic
antidepressant overdose.
• The triad of peaked T waves (hyperkalemia), a long
QT due to ST-segment lengthening (hypocalcemia),
and left ventricular hypertrophy (systemic
hypertension) suggests chronic renal failure.
• Comparison with any previous ECGs is invaluable
Computerized Electrocardiography
• Computerized ECG systems are widely used for
immediate retrieval of thousands of ECG records.
• Computer interpretation of ECGs still has major
limitations.
• Incomplete or inaccurate readings are most likely
with arrhythmias and complex abnormalities.
• Therefore, computerized interpretation (including
measurements of basic ECG intervals) should not
be accepted without careful clinician review.
You might also like
- ECG Basics Module-1Document127 pagesECG Basics Module-1manyusinghNo ratings yet
- ECGDocument41 pagesECGmiguel mendezNo ratings yet
- Basis of ECG and Intro To ECG InterpretationDocument10 pagesBasis of ECG and Intro To ECG InterpretationKristin SmithNo ratings yet
- 14 Test Bank Cardiovascular Physiology MCQ Test Bank With AnswersDocument45 pages14 Test Bank Cardiovascular Physiology MCQ Test Bank With Answersmugtaba100% (4)
- Santosh DevDocument45 pagesSantosh Devdevdsantosh100% (1)
- ElectrocardiogramDocument29 pagesElectrocardiogramMahnoor ZafarNo ratings yet
- ECG1Document67 pagesECG1Farhan RosliNo ratings yet
- ATLS Practice Test 2 Answers & ExplanationsDocument8 pagesATLS Practice Test 2 Answers & ExplanationsCarl Sars50% (2)
- ECG Made Easy by Mallareddy SripujaDocument46 pagesECG Made Easy by Mallareddy Sripujagrreddy836100% (3)
- Basic Principles of ECGDocument53 pagesBasic Principles of ECGSmita Jain100% (1)
- Science Quest 8 AC 3E c04 PDFDocument94 pagesScience Quest 8 AC 3E c04 PDFmaxx100% (1)
- Biomechanics of MusclesDocument58 pagesBiomechanics of MusclesAsad Chaudhary100% (2)
- ECG InterpretationDocument48 pagesECG InterpretationKervayse St.ClairNo ratings yet
- Ecg PresentationDocument42 pagesEcg PresentationAnwar SiddiquiNo ratings yet
- Mechanical VentilationDocument43 pagesMechanical VentilationsalemraghuNo ratings yet
- ECG Guide: Understanding Heart Rhythms & EKG TestDocument10 pagesECG Guide: Understanding Heart Rhythms & EKG TestSilver Villota Magday Jr.No ratings yet
- Basic Ecg Interpretation and Arrhythmia Recognition By: Ma. Victoria E. Martinez Er - RNDocument34 pagesBasic Ecg Interpretation and Arrhythmia Recognition By: Ma. Victoria E. Martinez Er - RNMavic Martinez BuntalesNo ratings yet
- ECG Interpretation in DogsDocument107 pagesECG Interpretation in DogsPLABITA GOSWAMI100% (2)
- ECG Interpretation GuideDocument69 pagesECG Interpretation GuideRohini RaiNo ratings yet
- ENERGY SYSTEMS - Analyse The 3 Different Energy Systems - 1.2Document9 pagesENERGY SYSTEMS - Analyse The 3 Different Energy Systems - 1.2Ben Jenkins100% (4)
- Pathophysiology of Cerebrovascular AccidentDocument2 pagesPathophysiology of Cerebrovascular AccidentJohn Michael FernandezNo ratings yet
- Electrical TimeDocument14 pagesElectrical TimeNithyaa SathishNo ratings yet
- Urinary System: Part A - Multiple ChoiceDocument4 pagesUrinary System: Part A - Multiple ChoiceCharlie100% (3)
- ECG Clinical DemonstrationDocument24 pagesECG Clinical Demonstrationsoniya josephNo ratings yet
- Antenatal Assessment Form 7Document4 pagesAntenatal Assessment Form 7Kaku ManishaNo ratings yet
- Electrocardiography Basic: DR Budi EnochDocument49 pagesElectrocardiography Basic: DR Budi EnochYohanes Malindo Wiyaa DBs-uno100% (1)
- Electrocardiography: An Introduction To The ECGDocument76 pagesElectrocardiography: An Introduction To The ECGInnocent Clifford MaranduNo ratings yet
- ECG Interpretation GuideDocument50 pagesECG Interpretation GuideJake MillerNo ratings yet
- Introduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesDocument36 pagesIntroduction To ECG: Presenter: Emiacu Kenneth Facilitator: Dr. Ssebuliba MosesNinaNo ratings yet
- C240 Understanding ElectrocardiographyDocument12 pagesC240 Understanding ElectrocardiographyBeauNo ratings yet
- Electrocardiography (Ii) Morphological Description of The ElectrocardiogramDocument8 pagesElectrocardiography (Ii) Morphological Description of The ElectrocardiogramAisleenHNo ratings yet
- DrAbnet ECG - BasicsDocument99 pagesDrAbnet ECG - BasicsAbnet WondimuNo ratings yet
- ElectrocardiographDocument5 pagesElectrocardiographGeorge MagedNo ratings yet
- Auskultation. ECG - LastDocument5 pagesAuskultation. ECG - LastAndreyNo ratings yet
- Cal EcgDocument7 pagesCal EcgNur Amirah FarhanahNo ratings yet
- Ecg (Ekg) : Dr. Jamal Dabbas Interventional Cardiologist & InternistDocument87 pagesEcg (Ekg) : Dr. Jamal Dabbas Interventional Cardiologist & Internistsara rababahNo ratings yet
- ECG Analysis and Cardiac DysrhythmiasDocument6 pagesECG Analysis and Cardiac Dysrhythmiasrui_kaNo ratings yet
- Ecg PrsentationDocument33 pagesEcg Prsentationtehillahkabwe100No ratings yet
- Project 2 Electrocardiography: Practical TasksDocument16 pagesProject 2 Electrocardiography: Practical TasksFahad ShahidNo ratings yet
- Electrical Impulse Viewed: Interpretation of The ElectrocardiogramDocument41 pagesElectrical Impulse Viewed: Interpretation of The ElectrocardiogramNesru Ahmed AkkichuNo ratings yet
- ECG EKG: BasicsDocument191 pagesECG EKG: BasicsSabio DenmenNo ratings yet
- Mechanical and Electrical Events of The Cardiac CycleDocument39 pagesMechanical and Electrical Events of The Cardiac CycleEdi HidayatNo ratings yet
- MUCLecture 2021 1292271Document34 pagesMUCLecture 2021 1292271Kouka MahfoudiNo ratings yet
- 9 EcgDocument12 pages9 EcgTommy CharwinNo ratings yet
- EcgDocument18 pagesEcgmyla adapNo ratings yet
- Electrical Activity of The HeartDocument40 pagesElectrical Activity of The HeartMichael Ajak GhaiNo ratings yet
- Electrocardiography: The ECG: A.D. John, MD, Lee A. Fleisher, MDDocument19 pagesElectrocardiography: The ECG: A.D. John, MD, Lee A. Fleisher, MDCésar Vásquez AguilarNo ratings yet
- 05 - ElektrokardiogramDocument39 pages05 - ElektrokardiogramNauval Zilal FananyNo ratings yet
- Electrical Activity of The HeartDocument156 pagesElectrical Activity of The HeartNIRANJANA SHALININo ratings yet
- Mechanical and Electrical Events of The Cardiac CycleDocument39 pagesMechanical and Electrical Events of The Cardiac CyclebhatsindhoorNo ratings yet
- ECG Complete LectureDocument33 pagesECG Complete LectureDr. SUVA NATHNo ratings yet
- Electrophysiology of The HeartDocument27 pagesElectrophysiology of The HeartTsegaye HailuNo ratings yet
- The Electrocardiogram: Ecg: by Gaurishi Agarwal, 32Document17 pagesThe Electrocardiogram: Ecg: by Gaurishi Agarwal, 32Gaurishi AgarwalNo ratings yet
- 01 - Basic Principles of ECG Analysis - UpToDateDocument22 pages01 - Basic Principles of ECG Analysis - UpToDateElmer MoscosoNo ratings yet
- Normal ECG Waveforms and Intervals ExplainedDocument26 pagesNormal ECG Waveforms and Intervals ExplainedJan Christian AramburoNo ratings yet
- ECG Interpretation: Prepared byDocument16 pagesECG Interpretation: Prepared bypipoahmed51No ratings yet
- Physiology Seminar: ElectrocardiographyDocument42 pagesPhysiology Seminar: ElectrocardiographyRajesh SharmaNo ratings yet
- Lab Exercise 5 PDFDocument50 pagesLab Exercise 5 PDFE1- Villapaz, Aiemarie R. (Aie)No ratings yet
- ECG Self-Study GuideDocument24 pagesECG Self-Study GuideShamsuzzaman SharifNo ratings yet
- Mechanical and Electrical Events of The Cardiac CycleDocument39 pagesMechanical and Electrical Events of The Cardiac CyclecosedasapereNo ratings yet
- How To Read An Electrocardiogram (ECG) - Part One: Basic Principles of The ECG. The Normal ECGDocument84 pagesHow To Read An Electrocardiogram (ECG) - Part One: Basic Principles of The ECG. The Normal ECGshaine htetNo ratings yet
- Conquering The ECGDocument25 pagesConquering The ECGPankaj PatilNo ratings yet
- ECG Signals PDFDocument14 pagesECG Signals PDFTohfatul JinanNo ratings yet
- How To Read An EcgDocument86 pagesHow To Read An EcgmajdNo ratings yet
- Chapter 11-The Normal ElectrocardiogramDocument18 pagesChapter 11-The Normal Electrocardiogrammuna s100% (1)
- EcgDocument52 pagesEcgعبد الله الحربيNo ratings yet
- ECG Procedure and InterpretationDocument10 pagesECG Procedure and InterpretationJonathan AlvarezNo ratings yet
- VidagliptineDocument36 pagesVidagliptineAriyanaNo ratings yet
- Insulin Aspart Dan ProteminatedDocument4 pagesInsulin Aspart Dan ProteminatedSastra WijayaNo ratings yet
- DM & KomplikasiDocument98 pagesDM & KomplikasiAriyanaNo ratings yet
- Diabetes IdiDocument71 pagesDiabetes IdiAriyanaNo ratings yet
- Diabetes 2008 Kuliah KoassDocument60 pagesDiabetes 2008 Kuliah KoassSastra WijayaNo ratings yet
- 2 OAD Di IndonesiaDocument40 pages2 OAD Di IndonesiaAriyanaNo ratings yet
- 5 Diabetes in PregnancyDocument59 pages5 Diabetes in PregnancyAriyanaNo ratings yet
- Strategies For Effective Discharge Planning For Hospitalized Patients With DiabetesDocument24 pagesStrategies For Effective Discharge Planning For Hospitalized Patients With DiabetesAriyanaNo ratings yet
- 5 Diabetes in PregnancyDocument59 pages5 Diabetes in PregnancyAriyanaNo ratings yet
- Ornerstones of Oot Anagement: DR Budi Enoch SPPDDocument23 pagesOrnerstones of Oot Anagement: DR Budi Enoch SPPDAriyanaNo ratings yet
- 5 DM and Acute Complication Hipoglicemia, DKA, HHSDocument47 pages5 DM and Acute Complication Hipoglicemia, DKA, HHSAriyanaNo ratings yet
- Cell Communication SignalsDocument27 pagesCell Communication Signalsbostonsox49No ratings yet
- Nervous System WorksheetDocument2 pagesNervous System WorksheetRoda Aranquez RabinoNo ratings yet
- Topic 6 Endocrine System Part IDocument34 pagesTopic 6 Endocrine System Part IMahrokh DarabiNo ratings yet
- Chattanooga Ionto TDCS Usage ManualDocument6 pagesChattanooga Ionto TDCS Usage ManualpsNo ratings yet
- Gangguan Asam BasaDocument51 pagesGangguan Asam BasaYudhistira YuliandraNo ratings yet
- Laporan Praktikum RespirasiDocument18 pagesLaporan Praktikum Respirasisuryati rante tikuNo ratings yet
- Chapter - 6 Anatomy of Flowering PlantsDocument6 pagesChapter - 6 Anatomy of Flowering PlantsPriyansh PatelNo ratings yet
- Introduction To Pharmacology: Prof. Johnny S. Bacud JR., RPH, Mspharm CandDocument81 pagesIntroduction To Pharmacology: Prof. Johnny S. Bacud JR., RPH, Mspharm Candlola&losa farhanNo ratings yet
- DTE Final NotesDocument141 pagesDTE Final NotesSajanNo ratings yet
- Acute Respiratory Distress John Rae 2019Document6 pagesAcute Respiratory Distress John Rae 2019yyullyyannaNo ratings yet
- Test de Apnea - Neurocritical Care 2021Document13 pagesTest de Apnea - Neurocritical Care 2021Eva SánchezNo ratings yet
- SDL R VS OldDocument6 pagesSDL R VS Oldsejal3vijNo ratings yet
- Induction of General Anesthesia - OverviewDocument40 pagesInduction of General Anesthesia - Overviewmayteveronica1000No ratings yet
- Cellular Respiration: The Metabolic PathwaysDocument17 pagesCellular Respiration: The Metabolic PathwaysMARIA ISABILLE DUALLO MUSONGNo ratings yet
- Control and Coordination: Chapter - 7Document9 pagesControl and Coordination: Chapter - 7milind dhamaniya100% (1)
- Photosynthesis CompressedDocument7 pagesPhotosynthesis Compressedsatwikdasmahapatra667No ratings yet
- Effectiveness and Safety of Intravenous Sedation With Propofol in Non-Operating Room Anesthesia (NORA) For Dental Treatment in Uncooperative Paediatric PatientsDocument11 pagesEffectiveness and Safety of Intravenous Sedation With Propofol in Non-Operating Room Anesthesia (NORA) For Dental Treatment in Uncooperative Paediatric PatientsharvardboyNo ratings yet
- Capsaicina Tópica en El Tratamiento Del Dolor Neuropático: RevisiónDocument13 pagesCapsaicina Tópica en El Tratamiento Del Dolor Neuropático: RevisiónJAVIER RODRIGUEZNo ratings yet
- Somnambulism: Continuing Education ActivityDocument6 pagesSomnambulism: Continuing Education ActivityGiovanna FkNo ratings yet
- F3 Workbook p45-47Document3 pagesF3 Workbook p45-47jnieeeNo ratings yet
- Jospt 1Document3 pagesJospt 1Ian PeroniNo ratings yet