Professional Documents
Culture Documents
Complement: Introduction
Uploaded by
SAKARIYE MAXAMED0 ratings0% found this document useful (0 votes)
10 views15 pagesIMMUNOLOGY COMPLEMENT PROTEINS
Original Title
Complement
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentIMMUNOLOGY COMPLEMENT PROTEINS
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
10 views15 pagesComplement: Introduction
Uploaded by
SAKARIYE MAXAMEDIMMUNOLOGY COMPLEMENT PROTEINS
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 15
Complement: Introduction
The complement system consists of
approximately 20 proteins that are present
in normal human (and other animal)
serum. The term "complement" refers to
the ability of these proteins to
complement, i.e., augment, the effects of
other components of the immune system,
e.g., antibody. Complement is an important
component of our innate host defenses.
• There are three main effects of complement: (1)
lysis of cells such as bacteria, allografts, and
tumor cells; (2) generation of mediators that
participate in inflammation and attract
neutrophils; and (3) opsonization, i.e.,
enhancement of phagocytosis. Complement
proteins are synthesized mainly by the liver.
Complement is heat-labile, i.e., it is inactivated by
heating serum at 56°C for 30 minutes.
Immunoglobulins are not inactivated at this
temperature.
Activation of Complement
• Several complement components are proenzymes,
which must be cleaved to form active enzymes.
Activation of the complement system can be
initiated either by antigen–antibody complexes or by
a variety of nonimmunologic molecules, e.g.,
endotoxin.
• Sequential activation of complement components
occurs via one of three pathways: the classic
pathway, the lectin pathway, and the alternative
pathway
• Of these pathways, the lectin and the
alternative pathways are more important at
the first time we are infected by a
microorganism because the antibody required
to trigger the classic pathway is not present.
The lectin pathway and the alternative
pathway are, therefore, participants in the
innate arm of the immune system
• All three pathways lead to the production of C3b,
the central molecule of the complement cascade.
The presence of C3b on the surface of a microbe
marks it as foreign and targets it for destruction.
C3b has two important functions: (1) It combines
with other complement components to generate C5
convertase, the enzyme that leads to the
production of the membrane attack complex. (2) It
opsonizes bacteria because phagocytes have
receptors for C3b on their surface
• In the classic pathway, antigen–antibody complexes
activate C1 to form a protease, which cleaves C2 and
C4 to form a C4b,2b complex. The latter is C3
convertase, which cleaves C3 molecules into two
fragments, C3a and C3b. C3a, an anaphylatoxin, is
discussed below. C3b forms a complex with C4b,2b,
producing a new enzyme, C5 convertase (C4b,2b,3b),
which cleaves C5 to form C5a and C5b. C5a is an
anaphylatoxin and a chemotactic factor. C5b binds to
C6 and C7 to form a complex that interacts with C8
and C9 to produce the membrane attack complex
(C5b,6,7,8,9), which causes cytolysis. Note that the "b"
fragment continues in the main pathway, whereas the
"a" fragment is split off and has other activities.
• In the lectin pathway, mannan-binding lectin
(MBL) (also known as mannose-binding
protein) binds to the surface of microbes
bearing mannan (a polymer of the sugar,
mannose). This activates proteases associated
with MBL that cleave C2 and C4 components
of complement and activate the classic
pathway. Note that this process bypasses the
antibody-requiring step and so is protective
early in infection before antibody is formed.
• In the alternative pathway, many unrelated
cell surface substances, e.g., bacterial
lipopolysaccharides (endotoxin), fungal cell
walls, and viral envelopes, can initiate the
process by binding C3(H2O) and factor B. This
complex is cleaved by a protease, factor D, to
produce C3b,Bb. This acts as a C3 convertase
to generate more C3b.
Regulation of the Complement System
• The first regulatory step in the classic pathway is at
the level of the antibody itself. The complement-
binding site on the heavy chain of IgM and IgG is
unavailable to the C1 component of complement if
antigen is not bound to these antibodies. This
means that complement is not activated by IgM and
IgG despite being present in the blood at all times.
However, when antigen binds to its specific
antibody, a conformational shift occurs and the C1
component can bind and initiate the cascade.
• Several serum proteins regulate the
complement system at different stages.
• C1 inhibitor is an important regulator of the
classic pathway. It inactivates the protease
activity of C1. Activation of the classic pathway
proceeds past this point by generating
sufficient C1 to overwhelm the inhibitor.
• Regulation of the alternative pathway is mediated
by the binding of factor H to C3b and cleavage of
this complex by factor I, a protease. This reduces
the amount of C5 convertase available. The
alternative pathway can proceed past this
regulatory point if sufficient C3b attaches to cell
membranes. Attachment of C3b to cell membranes
protects it from degradation by factors H and I.
Another component that enhances activation of
the alternative pathway is properdin, which
protects C3b and stabilizes the C3 convertase.
• Protection of human cells from lysis by the
membrane attack complex of complement is
mediated by decay-accelerating factor (DAF,
CD55)—a glycoprotein located on the surface
of human cells. DAF acts by binding to C3b and
C4b and limiting the formation of C3
convertase and C5 convertase. This prevents
the formation of the membrane attack
complex.
Clinical Aspects of Complement
• Inherited (or acquired) deficiency of some complement
components, especially C5–C8, greatly enhances
susceptibility to Neisseria bacteremia and other
infections. A deficiency of MBL also predisposes to severe
Neisseria infections. A deficiency of C3 leads to severe,
recurrent pyogenic sinus and respiratory tract infections.
• Inherited deficiency of C1 esterase inhibitor results in
angioedema. When the amount of inhibitor is reduced, an
overproduction of esterase occurs. This leads to an
increase in anaphylatoxins, which cause capillary
permeability and edema.
• Acquired deficiency of decay-accelerating factor on the
surface of cells results in an increase in complement-
mediated hemolysis. Clinically, this appears as the
disorder paroxysmal nocturnal hemoglobinuria
• In transfusion mismatches, e.g., when type A blood is
given by mistake to a person who has type B blood,
antibody to the A antigen in the recipient binds to A
antigen on the donor red cells, complement is
activated, and large amounts of anaphylatoxins and
membrane attack complexes are generated. The
anaphylatoxins cause shock, and the membrane attack
complexes cause red cell hemolysis.
• Immune complexes bind complement, and thus
complement levels are low in immune complex
diseases, e.g., acute glomerulonephritis and systemic
lupus erythematosus. Binding (activating) complement
attracts polymorphonuclear leukocytes, which release
enzymes that damage tissue.
• Patients with severe liver disease, e.g., alcoholic
cirrhosis or chronic hepatitis B, who have lost
significant liver function and therefore cannot
synthesize sufficient complement proteins, are
predisposed to infections caused by pyogenic bacteria.
You might also like
- Unit Plan For Sem 1Document17 pagesUnit Plan For Sem 1MRS CHAKRAPANI100% (10)
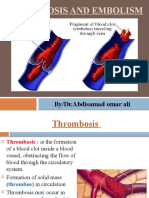
- Thrombosis and EmbolismDocument20 pagesThrombosis and EmbolismSAKARIYE MAXAMEDNo ratings yet
- Lecture 8-2Document29 pagesLecture 8-2Emmanuel Thon MadingNo ratings yet
- L4 Complement SystemDocument44 pagesL4 Complement Systemashutoshrath209No ratings yet
- Group-7-Patho Presentation 5th Sem, Sec-ADocument14 pagesGroup-7-Patho Presentation 5th Sem, Sec-AAhsham AliNo ratings yet
- Complement 2015 PDFDocument31 pagesComplement 2015 PDFSetiawan DonnieNo ratings yet
- CompletementDocument3 pagesCompletementzeythu1No ratings yet
- Complement 2 PDFDocument16 pagesComplement 2 PDFFatima AdelNo ratings yet
- Complement SystemDocument35 pagesComplement SystemPowell KitagwaNo ratings yet
- ScribdDocument2 pagesScribdsisirachandranNo ratings yet
- T4 Complement SystemDocument42 pagesT4 Complement Systemกฤติน วนิจวรางกุลNo ratings yet
- COMPLEMENT SYSTEM NoteDocument6 pagesCOMPLEMENT SYSTEM NoteKaren AgbaegbuNo ratings yet
- Complement System EdenDocument52 pagesComplement System EdenWilliam C ChishaNo ratings yet
- VIDEO 1: What Is Complement?: Specific To The Invading Microorganism, The Alternative Pathway RequiresDocument31 pagesVIDEO 1: What Is Complement?: Specific To The Invading Microorganism, The Alternative Pathway RequiresRaisin SainiNo ratings yet
- The Complement SystemDocument4 pagesThe Complement SystemExamville.com100% (1)
- Complement System: Pathways, Functions and RegulationDocument6 pagesComplement System: Pathways, Functions and RegulationN.vijaykanthNo ratings yet
- L1c Complement SystemDocument39 pagesL1c Complement Systemashutoshrath209No ratings yet
- Complement System: Biology of The Immune System: Complement Activation PathwaysDocument5 pagesComplement System: Biology of The Immune System: Complement Activation PathwaysIM CTNo ratings yet
- sIM3 - Complement System - 22Document37 pagessIM3 - Complement System - 22Brian LeungNo ratings yet
- Complement SystemDocument9 pagesComplement SystemSamia BasharatNo ratings yet
- How To Measure Complement Complement and DiseasesDocument48 pagesHow To Measure Complement Complement and DiseasesRapatra ChanalertpatraNo ratings yet
- Complement System Part II: Role in ImmunityDocument26 pagesComplement System Part II: Role in ImmunityAnca LunguNo ratings yet
- The Complement System: Dhruba Acharya Lecturer/ImmunologistDocument42 pagesThe Complement System: Dhruba Acharya Lecturer/ImmunologistRajkishor YadavNo ratings yet
- 7-Complement System, 9Document25 pages7-Complement System, 9hawkar omerNo ratings yet
- Complement SystemDocument28 pagesComplement SystemAndrea Michelle OchoaNo ratings yet
- The Complement SystemDocument38 pagesThe Complement SystemIraqiNo ratings yet
- Is Chapter 5Document57 pagesIs Chapter 5aemancarpioNo ratings yet
- The Complement System: DR (MRS) Bornali Sarmah Dutta Asst Prof of Microbiology Tezpur Medical College & HospitalDocument39 pagesThe Complement System: DR (MRS) Bornali Sarmah Dutta Asst Prof of Microbiology Tezpur Medical College & HospitalAnshuman KatakyNo ratings yet
- Lect. 4 The Complement Proteins and Their ReceptorsDocument15 pagesLect. 4 The Complement Proteins and Their ReceptorsMuhammadNo ratings yet
- The Complement System: By: Dr. Suzan YousifDocument36 pagesThe Complement System: By: Dr. Suzan YousifSai BabaNo ratings yet
- Complementary System Course WorkDocument5 pagesComplementary System Course Workizomadman392No ratings yet
- ComplementDocument39 pagesComplementYeyeh SantosNo ratings yet
- 1 - Cells of Immunity - Complement - FontDocument75 pages1 - Cells of Immunity - Complement - FontMoneeshNo ratings yet
- Komplemen: Bambang Heru BudiantoDocument38 pagesKomplemen: Bambang Heru Budiantoliana_ameyliaNo ratings yet
- Seminar Presentation: Title: The Complement SystemDocument7 pagesSeminar Presentation: Title: The Complement SystemafricanusquintusNo ratings yet
- The Complement SystemDocument44 pagesThe Complement SystemParulNo ratings yet
- The Complement SystemDocument16 pagesThe Complement SystemOsama BakheetNo ratings yet
- Complement System TherapeuticsDocument36 pagesComplement System Therapeuticsmurfiqahharizah03No ratings yet
- Immune System and Immunology: German VersionDocument69 pagesImmune System and Immunology: German VersionCyndie KamauNo ratings yet
- Complement SystemDocument6 pagesComplement SystemJimit GandhiNo ratings yet
- 5 Complement SystemDocument44 pages5 Complement SystemUsman SurajNo ratings yet
- Immune System and Immunology: German VersionDocument68 pagesImmune System and Immunology: German VersionKhushbuNo ratings yet
- Virus Complement Evasion Strategies: ReviewDocument15 pagesVirus Complement Evasion Strategies: ReviewPer DamiánNo ratings yet
- Class Notes of ImmunologyDocument66 pagesClass Notes of ImmunologyGnaneshwar NaaniNo ratings yet
- Amino Acids & ProteinsDocument41 pagesAmino Acids & Proteinsmrstarkb112No ratings yet
- The Complement SystemDocument27 pagesThe Complement SystemSai Kiran100% (1)
- ImmunologyDocument74 pagesImmunologyGullalae KhanNo ratings yet
- Complement SystemDocument4 pagesComplement SystemUsman SurajNo ratings yet
- Complement (Yt)Document7 pagesComplement (Yt)Vince Martin ManaigNo ratings yet
- ImmunologyDocument62 pagesImmunologyLinda RubioNo ratings yet
- Komplemen Dan SitokinDocument38 pagesKomplemen Dan SitokinIful SaifullahNo ratings yet
- Komplemen Dan SitokinDocument38 pagesKomplemen Dan SitokinBantuinAku KakNo ratings yet
- Programme M.SC BT Course Code: 19BTP06 Course Title: ImmunotechnologyDocument14 pagesProgramme M.SC BT Course Code: 19BTP06 Course Title: ImmunotechnologyNarendhran SNo ratings yet
- Complement System (Kidd)Document4 pagesComplement System (Kidd)Khoreen ObisoNo ratings yet
- Clinical Immunology - Topic 4 - Complement Proteind PDFDocument17 pagesClinical Immunology - Topic 4 - Complement Proteind PDFAliza FayyazNo ratings yet
- Complementsystem UpdatedDocument41 pagesComplementsystem UpdatedMadhumita PandaNo ratings yet
- Effector Mechanism of Humoral ImmunityDocument40 pagesEffector Mechanism of Humoral ImmunityMiss AisyahNo ratings yet
- Screenshot 2023-02-03 at 8.45.57 PMDocument22 pagesScreenshot 2023-02-03 at 8.45.57 PMtaifaliali123No ratings yet
- Innate Immunity: The Immediate Response To InfectionDocument25 pagesInnate Immunity: The Immediate Response To Infectionnokate konkoorNo ratings yet
- Cellular and Molecular Mechanisms of Inflammation: Receptors of Inflammatory Cells: Structure—Function RelationshipsFrom EverandCellular and Molecular Mechanisms of Inflammation: Receptors of Inflammatory Cells: Structure—Function RelationshipsCharles G. CochraneNo ratings yet
- Platelet Protocols: Research and Clinical Laboratory ProceduresFrom EverandPlatelet Protocols: Research and Clinical Laboratory ProceduresNo ratings yet
- Molecular Biology of B CellsFrom EverandMolecular Biology of B CellsTasuku HonjoNo ratings yet
- P. Cavity: (Female Reproductive Organs)Document38 pagesP. Cavity: (Female Reproductive Organs)SAKARIYE MAXAMEDNo ratings yet
- Pelvic Wall-Cont.: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument39 pagesPelvic Wall-Cont.: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- Hemorrhage and Hemostasis: By/Dr - Abdisamad Omar AliDocument24 pagesHemorrhage and Hemostasis: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- The Perineum: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument21 pagesThe Perineum: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- MCQ KidneyDocument8 pagesMCQ KidneyRimaZouzNo ratings yet
- Faculty of Medicine and Surgery Community Medicine An Introduction Lecture ThreeDocument50 pagesFaculty of Medicine and Surgery Community Medicine An Introduction Lecture ThreeSAKARIYE MAXAMEDNo ratings yet
- The Pelvic Cavity: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument44 pagesThe Pelvic Cavity: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- Regulation of Respiration: DR Mohamed HassanDocument27 pagesRegulation of Respiration: DR Mohamed HassanSAKARIYE MAXAMEDNo ratings yet
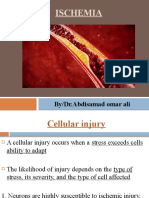
- Ischemia: By/Dr - Abdisamad Omar AliDocument21 pagesIschemia: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Pelvic Cavity (Reproductive System) : Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument49 pagesPelvic Cavity (Reproductive System) : Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- Innate & Adaptive Immunity: Innate Immunity Exposure To The Microbe (Antigen) - It Is Nonspecific andDocument14 pagesInnate & Adaptive Immunity: Innate Immunity Exposure To The Microbe (Antigen) - It Is Nonspecific andSAKARIYE MAXAMEDNo ratings yet
- Principles of Gas Exchange Diffusionof Oxygen and Carbon Dioxide Through The Respiratory MembraneDocument23 pagesPrinciples of Gas Exchange Diffusionof Oxygen and Carbon Dioxide Through The Respiratory MembraneSAKARIYE MAXAMEDNo ratings yet
- The Neck: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument30 pagesThe Neck: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- Temperature Regulation: Dr. Mohamed Hassan MBBS, Mmed Ped, Ph.D. CandDocument46 pagesTemperature Regulation: Dr. Mohamed Hassan MBBS, Mmed Ped, Ph.D. CandSAKARIYE MAXAMEDNo ratings yet
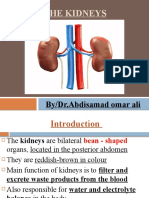
- The Kidneys: By/Dr - Abdisamad Omar AliDocument12 pagesThe Kidneys: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
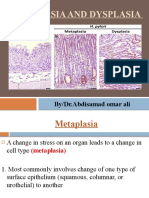
- Metaplasia and Dysplasia: By/Dr - Abdisamad Omar AliDocument31 pagesMetaplasia and Dysplasia: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Assignment For Calcitonin HormoneDocument6 pagesAssignment For Calcitonin HormoneSAKARIYE MAXAMEDNo ratings yet
- The Pelvic Girdle: By/Dr - Abdisamad Omar AliDocument30 pagesThe Pelvic Girdle: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Covid - 19: By/Dr - Abdisamad Omar AliDocument34 pagesCovid - 19: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Transport of Oxygen and Crabon Dioxid in The Blood and Tissue FluidDocument19 pagesTransport of Oxygen and Crabon Dioxid in The Blood and Tissue FluidSAKARIYE MAXAMEDNo ratings yet
- By/Dr - Abdisamad Omar AliDocument22 pagesBy/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- By/Dr - Abdisamad Omar AliDocument27 pagesBy/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Ischemia: By/Dr - Abdisamad Omar AliDocument21 pagesIschemia: By/Dr - Abdisamad Omar AliSAKARIYE MAXAMEDNo ratings yet
- Insulin, Glucagon, and Diabetes Mellitus: Dr. Mohamed HassanDocument66 pagesInsulin, Glucagon, and Diabetes Mellitus: Dr. Mohamed HassanSAKARIYE MAXAMEDNo ratings yet
- Secretory Functions of The Alimentary Tract: Dr. Mohamed HassanDocument55 pagesSecretory Functions of The Alimentary Tract: Dr. Mohamed HassanSAKARIYE MAXAMEDNo ratings yet
- PATHOLOGYDocument32 pagesPATHOLOGYSAKARIYE MAXAMEDNo ratings yet
- ANATOMYDocument8 pagesANATOMYSAKARIYE MAXAMEDNo ratings yet
- Structure & Classification: BacterialDocument38 pagesStructure & Classification: BacterialSAKARIYE MAXAMEDNo ratings yet
- Immunology: ImmunityDocument10 pagesImmunology: ImmunitySAKARIYE MAXAMEDNo ratings yet
- Cap II - Curs 5 - 6 - Somatosensory System - 2014 - 2015 - PDFDocument137 pagesCap II - Curs 5 - 6 - Somatosensory System - 2014 - 2015 - PDFMaria MadalinaNo ratings yet
- Tissue RepairDocument9 pagesTissue RepairSakidu LegionNo ratings yet
- Basic Science 2nd Term Jss2Document15 pagesBasic Science 2nd Term Jss2Adio Babatunde Abiodun Cabax100% (1)
- Classsification of RPDDocument37 pagesClasssification of RPDdranandmds100% (2)
- Lymphoid SystemDocument108 pagesLymphoid SystemKim RamosNo ratings yet
- CellDocument36 pagesCellNORHANANI BINTI BAJURI STUDENT100% (1)
- 3 Principios de Biofarmacia PDFDocument96 pages3 Principios de Biofarmacia PDFAnonymous Se5IdneSpNo ratings yet
- Polycythemia VeraDocument18 pagesPolycythemia VeraHSC UNITEDNo ratings yet
- Exchange Surfaces 2 QPDocument13 pagesExchange Surfaces 2 QPSaaleh AbanurNo ratings yet
- Assessing Neurologic System: Mabini CollegesDocument25 pagesAssessing Neurologic System: Mabini CollegesNicole NipasNo ratings yet
- SclerenchymaDocument20 pagesSclerenchymaZakia Hasan Thalib100% (1)
- Specific Immunity. FINALDocument29 pagesSpecific Immunity. FINALLUZVIMINDA GORDONo ratings yet
- 6.2 Lesson Plan DIPLOMA in OncologyDocument14 pages6.2 Lesson Plan DIPLOMA in OncologyedrinsneNo ratings yet
- 1 - The Skin's Function PDFDocument9 pages1 - The Skin's Function PDFskoahNo ratings yet
- GNM 1st Year Trhering Topic Handout 2020Document13 pagesGNM 1st Year Trhering Topic Handout 2020shapan biswaNo ratings yet
- Feoutal AddDocument9 pagesFeoutal AddDHUPGURI DIAGNOSTICNo ratings yet
- Heart and Circulation Test: NameDocument12 pagesHeart and Circulation Test: NamezipperNo ratings yet
- Script For Head To NeckDocument7 pagesScript For Head To NeckRhelina MinNo ratings yet
- Cat SkeletonDocument10 pagesCat SkeletonJefferson TanNo ratings yet
- 5 HemophiliaDocument57 pages5 HemophiliaRabia AzharNo ratings yet
- The Abo Blood Group SystemDocument3 pagesThe Abo Blood Group Systemchippai123No ratings yet
- Tips For Ust Med FreshmenDocument3 pagesTips For Ust Med FreshmenFred EvidorNo ratings yet
- Complementar - The Prevalence of Alcoholic Cerebellar AtrophyDocument9 pagesComplementar - The Prevalence of Alcoholic Cerebellar AtrophySantiago AlzateNo ratings yet
- Ectopic Pregnancy ImportantDocument42 pagesEctopic Pregnancy Importantﻣﻠﻚ عيسىNo ratings yet
- Occipito Posterior (PositionDocument44 pagesOccipito Posterior (PositionArambam Aruna100% (6)
- Fascial Tissue Research in Sports Medicine: From Molecules To Tissue Adaptation, Injury and DiagnosticsDocument9 pagesFascial Tissue Research in Sports Medicine: From Molecules To Tissue Adaptation, Injury and DiagnosticsCNPOULISNo ratings yet
- Lecture HemostasisDocument28 pagesLecture HemostasisЛариса ТкачеваNo ratings yet
- Mbbs PhysioDocument27 pagesMbbs PhysioWwwanand111No ratings yet
- LKM 5 - VAKUOLA - Kel 9Document4 pagesLKM 5 - VAKUOLA - Kel 9Farkhatul AzizahNo ratings yet