Professional Documents
Culture Documents
Ectopik Pregnancy
Uploaded by
Nikhil Tyagi0 ratings0% found this document useful (0 votes)
21 views69 pagesShort and concise information on ectopik pregnancy.
Original Title
ectopik pregnancy
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentShort and concise information on ectopik pregnancy.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
21 views69 pagesEctopik Pregnancy
Uploaded by
Nikhil TyagiShort and concise information on ectopik pregnancy.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 69
Ectopic pregnancy
The blastocyst normally implants in the endometrial
lining of the uterine cavity . Implantation anywhere else is
an ectopic pregnancy. More than 95% of ectopic
pregnancies involve the oviduct, but tubal pregnancy is
not synonymous with ectopic gestation.The risk of death
from an extra uterine pregnancy is 10 times greater than
that for a vaginal delivery and 50 times greater than for
an induced abortion. Moreover, prognosis for a successful
subsequent pregnancy is reduced significantly in these
women , especially if they are primigravid and over the age
of 30. A clear understanding of the contributing factors
responsible for ectopic pregnancies and of effective and
modern methods for their earlier diagnosis is essential .
General Considerations
Etiology: Etiological factors associated with an increased
incidence of ectopic pregnancy include those outlined in
this section.
Mechanical Factors - that prevent or retard passage of the
fertilized ovum into the uterine cavity include the following:
1. Salpingitis -especially endosalpingitis, which causes
agglutination of the arborescent folds of the tubal mucosa
with narrowing or the lumen or formation of blind pockets.
2. Peritubal adhesions subsequent to postabortal or
puerperal infections, appendicitis, or endometriosis. These
may cause kinking of the tube and narrowing of the
lumen
3. Developmental abnormalities of the tube, especially
diverticula , accessory ostia, and hypoplasia. Such
abnormalities are extremely rare but may occur following
in utero exposure to diethylstilbestrol.
4. Previous ecpotic pregnancy. After one the chance of
another is 7 to 15 % .
5. Previous operations on the tube, either to restore
patency or occasionally the failure of tubal sterilization.
6. Multiple previous induced abortions my increase the risk
of ectopic pregnancy. The risk is unchanged after one
induced abortion; it is doubled after two induced abortions,
likely due to small increases in the incidence of salpingitis
7. Tumors that distort the tube, such as uterine myomas and
adnexal masses
8. Tubal pregnancies are not increase by abnormal embryos .
Functional Factors. Functional factors that delay passage of the
fertilized ovum into the uterine cavity include the following:
1. External migration of the ovum is probably not an important
factor except in cases of abnormal mulerian development resulting
in a hemiuterus with an attached non-
communicating rudimentary uterine horn.
2. Menstrual reflux has been suggested as a cause; however, there is
little supporting evidence for this
3. Altered tubal motility may follow changes in serum levels of
estrogens and progesterone. A change in the number and affinity
of adrenergic receptors in uterine and tubal smooth muscle is
likely responsible
4. Cigarette smoking at the time of conception has been shown to
increase the incidence of ectopic pregnancy. This probably occurs
due to a change in adrenergic receptor number or affinity in tubal
musculature .
Assisted Reproduction. Several forms of assisted reproduction
have been reported to increase the incidence of ectopic
pregnancy.
1. Tubal pregnancy has been reported to be increased following
ovulation induction, gamete intrafallopian transfer (GIFT), and
in vitro fertilization (IVF) and ovum transfer .
2. Heterotypic tubal pregnancy is increased after in vitro
fertilization and embryo transfer and ovulation induction.
Heterotypic cervical pregnancy is also increase following in
vitro fertilization and embryo transfer.
3. Abdominal pregnancy has been reported following gamete
intra-fallopian transfer and in vitro fertilization and ovum
transfer
4. Cervical pregnancy may be increased after in vitro
fertilization and embryo transfer .
Failed Contraception. - Failed contraception
increases the incidence of ectopic pregnancies . With
use of any contraceptive , the actual number of
ectopic pregnancies is decreased because pregnancy
occurs less often. In contraceptive failures, however ,
there is an increased incidence of ectopic pregnancy
following some forms of tubal sterilization and in
women using intrauterine devices or taking progestin-
only “minipills”.
1. Relative risks for ectopic pregnancy overall are
decreased in users of intrauterine devices oral
contraceptives , and traditional barrier methods
compared with non-contraceptive users
2. Contraceptive failure following tubal sterilization
has an ectopic pregnancy rate of 16 to 50 %.
3. Tubal pregnancy may occasionally follow
hysterectomy. In most instances , a recently fertilized
ovum was trapped in the oviduct at the time of
hysterectomy. More rarely , a fistula sufficient for
passage of sperm developed between vagina and the
severed end of the oviduct.
Epidemiology. There has been a marked increase in
both the absolute number and rate of ectopic
pregnancies in the USA in the past two decades. These
rates may be calculated using three different methods:
1. Females 15 to 44 years: The number of ectopic
pregnancies in women 15 to 44 years old per 10.000
females
2. Live births: The number of ectopic pregnancies per
1000 live births
3. Reported pregnancies: The number of ectopic
pregnancies per 1000 reported pregnancies, which
includes live birth, legally induced abortions and ectopic
pregnancies.
Unfortunately, none of these rates is totally accurate
because the numerator may be falsely low for all
calculations. Ectopic pregnancies certainly occur in
women younger than 15 and older than 44. The
denominator is falsely low in rates reported per live
births, because stillbirth rates are not consideres.
The incidence of ectopic pregnancy is increased in
nonwhite compared with white women. The
combined factors of race and increases age are at least
additive.
Causes for increased Rates of Ectopic Pregnancy.
The reasons for increases in ectopic pregnancies in the
USA are not entirely clear; however , similar increases have
been reported from Eastern Europe, Scandinavia and
Great Britain.
The reasons for the disproportionately increased incidence
of ectopic pregnancies in nonwhite women is also not
known. Possible explanations include the following :
(1) health care is less available or acceptable to
nonwhite women compared with white women
(2) sexually transmitted diseases are reported more
frequently in nonwhite compared with white women .
Mortality
Ectopic pregnancy remains the second leading
case of maternal mortality in many countries.
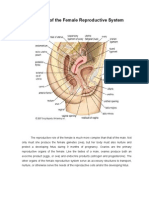
Anatomical Considerations.
The fertilized ovum may develop in any portion or
the oviduct, giving rise to ampullary, isthimic and
interstitial tubal pregnancies . In rare instances the
fertilized ovum may be implanted in the fimbriated
extremity and occasionally even on the fimbria
ovarica. The ampulla is the most frequent site of
implantation and the isthmus the next most common.
Interstitial pregnancy is very uncommon, occurring in
only about 3% of all tubal gestation . From these
primary types, certain secondary forms of tubo-
abdominal , tubo-ovarian and broad ligament
pregnancies occasionally develop.
Zygote implantation. The fertilized ovum does not
remain on the surface but promptly burrows through
the epithelium. As the zygote penetrates the
epithelium it comes to lie in the muscular wall,
because the tube lacks a submucosa. At the
periphery of the zygote is a capsule of rapidly
proliferating trophoblast, which invades and erodes
the subjacent muscularis. At the same time ,
maternal blood vessels are opened, and blood pours
into the spaces, lying within the trophoblast or
between it and the adjacent tissue.
The tube normally does not form an extensive
deciduas, although decidual cells usually can be
recognized. Tubal wall in contact with the zygote
offers only slight resistance to invasion by the
trophoblast, which soon burrows through it , opening
maternal vessels. The embryo or fetus in an ectopic
pregnancy is often absent or stunted.
Uterine Changes.
In ectopic pregnancy, the uterus undergoes some of
the changes associated with normal early pregnancy,
including softening of the cervix and isthmus and an
increase in size.
The degree to which the endometrium is converted to
decidua is variable. The finding of uterine deciduas
without trophoblast suggests ectopic pregnancy but is
not absolute indication.
External bleeding, which is seen commonly in cases
of tubal pregnancy , is uterine in origin and
associated with degeneration and sloughing of the
uterine deciduas; hemorrhage is seldom severe. Soon
after death of the fetus, the deciduas degenerates and
is usually shed in small pieces , but occasionally it is
cost off intact as a decidual cast of the uterine cavity.
Absence of decidual tissue, however, does not exclude
an ectopic pregnancy.
Natural History of Tubal Pregnancy .
Tubal Abortion. A common termination of tubal
pregnancy is separation of the conceptus from the
implantation site and extrusion through the fimbriated end
of the oviduct. The frequency of tubal abortion depends
in part upon the site of implantation. Tubal abortion is
common in ampullary tubal pregnancy, whereas rupture
of the tube is the usual outcome with isthmic pregnancy.
The immediate consequence of hemorrhage with tubal
abortion is further disruption of the connection between
the placenta and membranes and the tubal wall. If
placental separation is complete , all of the products of
conception may be extruded through the fimbritaed end
into the peritoneal cavity. At this point , hemorrhage and
symptoms disappear.
Tubal Rupture . The invading , expanding products
of conception may rupture the oviduct at any of
several sites. Before sophisticated methods to
measure chorionic gonadotropin were available ,
many cases of tubal pregnancy ended during the first
trimester by intraperitoenal rupture. As a rule,
whenever there is tubal rupture in the first few weeks,
the pregnancy is situated in the isthmic portion of
the tube a short distance from the cornu of the uterus.
When the fertilized ovum is implanted well within
the interstitial portion of the tube, rupture usually
occurs later.
The immediate cause of rupture may be trauma associated
with coitus or a bimanual examination, although in most
cases rupture , the entire conceptus may be extruded from
the tube, or if the rent is small , profuse hemorrhage may
occur without extrusion.
In either event the woman commonly shows signs of
collapse from hemorrhage and hypovolemia.
If an early conceptus is expelled essentially undamaged
into the peritoneal cavity, it may reimplant almost
anywhere, establish adequate circulation, survive and grow.
This outcome is most unlikely, however because of damage
during the transition. The conceptus, if small, may be
reorbed or if larger may remain in the cul-de-sac for years as
an encapsulated mass or even become calcified to form a
lithpedion.
Abdominal Pregnancy.
If only the fetus is extruded at the time of rupture ,
the effect upon the pregnancy will vary depending on
the extent of injury sustained by the placenta. If the
placenta is damaged appreciable , fetal death is
inevitable; but if the greater portion of the placenta
retains its attachment to the tube, further
development is possible. The fetus may then survive
for some time, giving rise to an abdominal
pregnancy.
Interstitial pregnancy.
Implantation of the fertilized ovum within the segment of
tube that penetrates the uterine wall results in an interstitial
pregnancy . This has also been referred to as a corneal
pregnancy . The account for about 3% of all tubal gestations.
Because of the site of implantation , no adnexal mass is
palpable ; instead there is variable asymmetry of the uterus
that is often difficult to distinguish from an intrauterine
pregnancy. Hence , early diagnosis is more frequently
overlooked than in other types of tubal implantation.
Because of the greater distensibility of the myometrium
covering the interstitial portion of the tube, rupture occurs
later between the end of the 8th and 11th gestational weeks.
The hemorrhage may rapidly prove fatal because the
implantation site is located between the ovarian and uterine
arteries .
Multifetal Ectopic Pregnancy
Heterotypic Ectopic Pregnancy . Tubal pregnancy
may be complicated by a coexisting intrauterine
gestation , a condition designated as heterotypic
pregnancy. A heterotypic pregnancy is quite difficult
to diagnose clinically. Typically laparotomy is
performed because of a tubal pregnancy . At the same
time the uterus is congested, softened and somewhat
enlarged. Although these features are suggestive of
intrauterine pregnancy, there are commonly induced
by a tubal pregnancy alone. Gestational products are
ultrasonically demonstrable within the uterine cavity
in practically all instance of heterotypic pregnancy.
Until recently , heterotypic pregnancies have been
considered to be rare, that is 1 per 30.000 intrauterin
pregnancies. A heterotypic pregnancy is more likely and
should be considered
(1) after assisted reproduction techniques; (2) with
persistent or rising chorionic gonadotropin levels after
dilation and curettage for an induced or spontaneous
abortion ; (3) when the uterine fundus is larger than
menstrual dates; (4) with more than one corpus luteum; (5)
with absence of vaginal bleeding in the presence of signs
and symptoms of an ectopic pregnancy and (6) when there is
ultrasound evidence of uterine and extrauterine pregnancy .
If such precautions are not observed maternal mortality is
increased appreciably.
Multifetal Ectopic Pregnancy. Twin tubal pregnancy
has been reported with both embryos in the same
tube , as well as with one in each tube. Single-ovum
twins result in a far greater proportion of tubal than
uterine pregnancies . Difficulties in migration and
implantation retarded the growth of the zygote , which
was somehow stimulated to form two identical
embryos. Simultaneous pregnancy in both fallopian
tubes is the rarest from of double-ovum twinning .
Tubo-Uterine, Tubo-Abdomian and Tubo-Ovarian
Pregnancies.
A tubo-uterne pregnancy results from the gradual
extension into the uterine cavity of products of
conception that originally implanted in the interstitial
portion of the tube. Tubo-abdominal pregnancy is
derived from a tubal pregnancy in which the zygote,
originally implanted in the neighborhood of the
fimbriated end of the tube , gradually extends into the
peritoneal cavity. In such circumstances the portion of
the fetal sac projecting into the peritoneal cavity may
form troublesome adhesions to surrounding organs. As a
result, removal of the sac is much more difficult. Both of
these conditions are very uncommon.
A tubo-ovarian pregnancy occurs when the fetal sac
is adherent partly to tubal and partly to ovarian
tissue. Such cases arise from the development of the
zygote in a tubo-ovarian cyst or in a tube, the
fimbriated extremity of which was adherent to the
ovary at the time of fertilization or became so soon
thereafter .
Clinical and Laboratory Features of Tubal
Pregnancy
General Considerations -clinical manifestations of a
tubal pregnancy are diverse and depend on whether
rupture has occurred. Commonly the woman believes
she is normally pregnant or believes she is aborting an
intrauterine pregnancy . Less often she does not suspect
she is pregnant. In “classical” cases, normal
menstruation is replaced by variably delayed slight
vaginal bleeding , which usually is referred to as
“spotting”. Suddenly, the woman is stricken with severe
lower abdominal pain, frequently described as sharp ,
stabbing or tearing in character . Vasomotor
disturbances develop, ranging from vertigo to syncope.
Abdominal palpation - tenderness
Virginal examination - especially motion of the cervix
causes exquisite pain.
The posterior fornix of the vagina -may bulge because
of blood in the cul-de-sac, or a tender , boggy mass
may be felt to one side of the uterus.
Symptoms of diaphragmatic irritation, characterized
by pain in the neck or shoulder especially on
inspiration , develop in perhaps 50 % of women in
whom there is sizable intraperitoneal hemorrhage.
This is cause by intraperitoneal blood irritating
cervical sensory nerves that supply the inferior
surface of the diaphragm.
The woman may or may not be hypotensive while
lying supine. If she is not hypotensive when supine ,
she may become so when place in a sitting
position . The diagnosis in such cases is not difficult
to make. The physician must make every reasonable
effort to diagnose the condition before catastrophic
events occur, but the task may not be simple.
Symptoms and Signs .
Pain . The most frequently experienced symptoms of
ectopic pregnancy are pelvic and abdominal pain
and amenorrhea with some degree of vaginal spotting
or bleeding. Pain may be anywhere in the abdomen.
With a large hemoperitoneum , pleuritic chest pain
may occur from diaphragmatic irritation.
Amenorrhea.
The absence of a missed menstrual period does not
exclude tubal pregnancy. A history of amenorrhea is
not obtained in a quarter or more of cases. Thus , the
woman may mistake the uterine bleeding that
frequently occurs with tubal pregnancy for a true
menstrual period. This important source of
diagnostic error can be eliminated in many cases by
carefully obtained menstrual history.
Vaginal Spotting or Bleeding . As long as placental
endocrine function persists, uterine bleeding is
usually absent; but when endocrine support for the
endometrium declines , uterine mucosa bleeds.
Bleeding is usually scanty , dark brown, and may be
intermittent or continuous.
Abdominal and Pelvic Pain . Exquisite tenderness of
abdominal palpation and vaginal examination ,
especially on motion of the cervix, is demonstrable in
over three fourths of women with ruptured or
rupturing tubal pregnancies.
Uterine Changes. Because of placental hormones, in
about one fourth of cases , the uterus grows during the
first 3 months of a tubal gestation to nearly the same
size as it would with an intrauterine pregnancy. The
uterus may be pushed to one side by an ectopic mass,
or if the broad ligament is filled with blood , the
uterus may be greatly displaced.
Blood Pressure and Pulse. Early responses to moderate
hemorrhage may range from no change in pulse and
blood pressure to a slight rise in blood pressure ,or a
vasovagal response with bradycardia and hypotension.
In a healthy pressure will fall and pulse rise only if
bleeding continues and hypovolemia becomes intense.
Hypovolemia . Important to detect significant
hypovolemia before development of hypovelemic shock.
Temperature. After acute hemorrhage , the temperature
may be normal or even low. Temperature up to 38 c.
may develop but higher temperatures are rare in the
absence of infection.
Pelvic Hematocele. Often there is gradual
disintegration of the tubal wall followed by slow
leakage of blood into the tubal lumen, the peritoneal
cavity, or both. Signs of active hemorrhage are absent
and even mild symptoms may subside , but gradually
the trickling blood collects in the pelvis, more or less
walled off by adhesions and a pelvic hematocele results.
Laboratory Tests.
Measurement of hemoglobin, hematocrit and
leukocyte count , as well as pregnancy tests and
progesterone are useful in certain cases if their
limitations are understood.
Hemoglobin and Hematocrit . After hemorrhage,
depleted blood volume is restored toward normal by
hemodilution over the course of a few day . Even after
a substantive hemorrhage , therefore , hemoglobin or
hematocirt readings may at first show only a slight
reduction.
Leukocyte Count - varies considerably in ruptured
ectopic pregnancy . In about half the patients , it is
normal but in the remainder, varying degrees of
leukocytosis up to 30.000 /ml may occur.
Pregnancy Tests. Ectopic pregnancy cannot be
diagnosed by a positive pregnancy test alone. The
key issue, however, is whether the woman is
pregnant. In virtually all cases of ectopic gestation ,
chorionic gonadotropin will be detected is serum but
usually at markedly reduced concentrations
compared with normal pregnancy .
Urinary pregnancy tests . These most often are latex
agglutination inhibition slide tests with sensitivities
for chorionic gonadotropin in the range of 500 to 800
mlU /ml. Their ease of use and rapidity is offset by
their small chance of being positive in a woman with
an ectopic pregnancy.
Serum Chorionic Gonadotropin Assays (β-hCG).
Serum radioimmunoassay for β-hCG is the most
precise method, and virtually any pregnancy event
can be detected. In fact, because of the sensitivity of
this assay , a pregnancy may be confirmed before
there are pathological changes in the fallopian tube.
The essential diagnostic step in the
identification of a suspected ectopic pregnancy
is to establish or exclude the diagnosis of
pregnancy.
Sonography.
Abdominal sonography. Identification of products of conception in
the fallopian tube is difficult using abdominal sonographpy. If a
gestational sac is clearly identified within the uterine cavity , it is
unlikely an ectopic pregnancy coexists. Moreover with sonographic
absence of an intrauterine sac, and an abnormal pelvic mass , ectoipic
pregnancy is almost certain.
Vaginal Sonography. According to most invistigators vaginal
compared with abdominal sonography is a more sensitive and specific
technique to diagnose ectopic pregnancy . With vaginal sonography,
identification of both ovaries allows the operator to exclude
conditions such as ovarian cysts or endometiromas and to detect
directly tubal pathology. Nevertheless, even vaginal sonographpy can
be misleading and ectopic pregnancies can be missed when a tubal
mass still is small or obscured by bowel. Vaginal sonography results
in earlier and more specific diagnoses of intrauterine pregnancy.
Culdocentensis .
The simplest technique for indentifying
hemoperitoneum is culdocentesis, because it can be
performed without hospitalization . The cervix is
pulled toward the symphysis with a tenaculum and a
long 16 or 18-gauge needle is inserted through the
posterior vaginal fornix into the cul-de-sac. Fluid, if
present can be aspirated . Failure to aspirate fluid can
be interpreted only as unsatisfactory entry into the
cul-de-sac. Fluid containing fragments of old clots, or
bloody fluid that does not clot, are compatible with
the diagnosis of hemoperitoneum resulting from an
ectopic pregnancy.
Curettage.
Differentiation between threatened or incomplete
abortion of an intrauterine pregnancy and a tubal
pregnancy may be accomplished in many instances by
curettage. Curettage in suspected cases of incomplete
abortion versus ectopic pregnancy when serum
progesterone is less than 5 gn/ml., β-hCG titers are
rising abnormally (less than 2000 mU/mL), and an
intrauterine pregnancy is not seen using trans-vaginal
sonography. If embryo, fetus or placenta are identified , a
simultaneous tubal pregnancy is unlikely. When none of
these structures is identified , tubal pregnancy is a
probability and further follow-up with serial
quantitative β-hCG titer and sonography is required.
Laparoscopy.
Fiber-optic laparoscopy provides a means of visual
diagnosis of pelvic disease , including ectopic
pregnancy. Complete visualization of the pelvis,
however may be impossible if there is pelvic
inflammation or active bleeding. At times ,
identification of an early un-ruptured tubal
pregnancy may be difficult, even though the tube is
fully visualized.
Differential Diagnosis.
Prompt diagnosis of a ruptured tubal pregnancy may
be lifesaving and the earlier an un-ruptured tubal
pregnancy is diagnosed the greater will be the
likelihood of a future successful pregnancy .
Unfortunately, there are few other disorders in
obstetrics and gynecology that present so many
diagnostic pitfalls. Women with ectopic pregnancy ,
approximately one third had been seen once and 11 %
twice before the correct diagnosis was made .
Gastrointestinal Disturbance. In some women with a ruptured
ectopic pregnancy, the prominent symptoms are diarrhea,
nausea and vomiting along with abdominal pain.
Abortion of intrauterine Pregnancy. In threatened or
uncompleted abortion , uterine bleeding is usually more
profuse and shock from hypovolemia, when present, is
usually in proportion to the extent of vaginal hemorrhage. In
tubal pregnancy, however, hypoveolmic shock almost always
is far in excess of observed vaginal blood loss.
Rupture of a Corpus Luteum or follicular Cyst. Intraperitoneal
bleeding from an ovarian cyst may be difficult to distinguish
from a ruptured tubal pregnancy. Even though identification
of chorionic gonadotropin will sometimes help to make the
diagnosis preoperatively , most often , the diagnosis is made
only at the time of exploratory laparotomy.
Twisted Cyst or Appendicitis. In both ovarian cyst
torsion and appendicitis, signs and symptoms of
pregnancy, including amenorrhea , are usually lacking, and
there is rarely a history of abnormal vaginal bleeding. The
mass formed by twisted ovarian cyst is more nearly
discrete, whereas that of a tubal pregnancy is usually less
well defined. With appendicitis, only rarely is there a
amass found by vaginal examination, and pain on motion
of the cervix is much less severe than with a ruptured
tubal pregnancy.
Intrauterine Devices. Diagnosis of ectopic pregnancy is
often more difficult in women with intrauterine devices.
Cramping pelvic pain and uterine bleeding both common
features of ectopic pregnancy, may be caused by an
intrauterine device.
Tubal Pregnancy: Treatment and prognosis
Treatment has most often been salpingectomy to
remove a chattered, bleeding oviduct with or without
ipsilateral oophorectomy. The goal of such treatment
was an should remain the preservation of the woman’s
life. Recently , treatment has changed from
salpingectomy to surgical and medical procedures that
favor tubal conservation. Such conservative
management is made possible by the earlier diagnosis
of ectopic pregnancy using vaginal ultrasound and
serum quantitative β-hCG determinations.
Surgical Management: Laparascopy and
Laparotomy
Salpingectomy. When removing the oviduct , it is
advisable to excise a wedge no more than the outer
third of the interstitial portion of the tube ( so-called
corneal resection) in an effort to minimize the rare
recurrence of pregnancy in the tubal stump. Resection
so extensive as to reach the cavity of the uterus must be
avoided, lest the defect created lead to uterine rupture
in a subsequent intrauterine pregnancy. Even with
cornual resection, a subsequent interstitial pregnancy
may not be prevented. Salpinegtomy can be performed
through an operative laparoscope and may be used for
both ruptured and unruptured ectopic pregnancies.
Sterilization. If childearing has been completed or if
the ectopic pregnancy is the consequence of failed
contraception, concomitant sterilization should be
considered. Tubal sterilization can usually be
performed via laparoscopy or laparotomy without
increased risk. Conversely, all organs possible should
be conserved in a woman of low parity with a strong
desire for future pregnancies . She must know,
however , that she has an increase risk of a subsequent
ectopic pregnancy.
Salpingostomy. this technique is used to remove a
small pregnancy that is usually less than 2 cm in
length and located in the distal one third of the
fallopian tube. A linear incision , 2 cm in length or
less, is made on the antimesenteric border
immediately over the ectopic pregnancy. The ectopic
usually will extrude from the incision and can be
carefully removed. Small bleeding sites are controlled
with needlepoint electrocautery or laser, and the
incision is left unsutured to heal by secondary
intention.
Medical Management
Methotrexate. It is recommended the use of
methotrezate to treat interstitial pregnancy. In
general the following principles apply: Success is
greatest if the gestation is less than 6 weeks, the tubal
mass is not more than 3.5cm in diameter and the fetus
is not alive . With more advanced gestations , success
has been less frequent except after multicourse
therapy, single high-dose therapy with folinic acid
rescue , or fetal death induced by direct injection of
potassium chloride and methotrexate into the
amniotic sac using either trans-virginal sonopraphy or
laparoscopy.
Patient selection. Candidates for methotrexate therapy must be
hemodynamically stable with a normal hemogram and normal
liver and renal function. Women given methotrexate are
instructed that (1) medical therapy fails in 5 to 10 % of patients
and this rate is higher in pregnancies past 6 weeks gestation or
with a tubal mass greater than 3.5cm in diameter; (2) failure of
medical therapy means elective surgery, or if tubal rupture occurs
(approximately a 5% chance), emergency surgery; (3) if treated as
an outpatient rapid transportation must be available for transfer
to the hospital; (4) signs and symptoms of tubal rupture such as
vaginal bleeding, abdomen and pleuritic pain , weakness,
dizziness or syncope must be reported promptly and should
constitute a cause for immediate medical attention; (5) sexual
intercourse is prohibited until after serum β-hCG is
undetectable; (6) no alcohol can be consumed and (7)
multivitamins with folic acid should not be taken.
Monitoring methotrexate toxicity. Although some
investigators report minimal or no side effects,
toxicity may develop suddenly and be severe.
Monitoring efficacy of therapy.
Various placental protein and steroid hormones have
been used to monitor placental viability following
medical and surgical therapy for ectopic pregnancies.
The most widely used are serial quantitative β-hCG
titers. The rationale for measuring serial β-
hCG values is that after therapy the hormone usually
disappears from plasma between 14 and 21 days.
Occasionally, however hormone levels remain
elevated for 28 days.
Systemic therapy . Systemic therapy with
methotrexate , 34 of 36 patients (94%) had complete
remission of tubal pregnancy. The other 2 ruptured,
one 23 days after commencing methotrexate therapy
and the other one day 14. The latter woman had fetal
heart activity noted throughout most of therapy.
Anti-D Immune Globulin. If the woman is D-
negative but not yet sensitized to D-antigen and the
potential for reproduction persists, anti-D immune
globulin should be administered to protect against
isoimmunization. Moreover, if platelets are
transfused, in all likelihood some contaminating D-
positive red cells were also included. Therefore , D-
negative patients also should receive anti-D immune
globulin soon after platelet transfusion.
Abdominal Pregnancy
Frequency . In incidence of abdominal pregnancy is
influenced by the (1) frequency of ectopic gestation in
the population, (2) availability of care early in
pregnancy, (3) use of assisted reproductive
techniques and (4) degree of suspicion exercised by
those providing care. Almost all cases of abdominal
pregnancy follow early rupture or abortion of tubal
pregnancy into the peritoneal cavity.
Etiology. Typically, the growing placenta, after penetrating the
oviduct wall, maintains its tubal attachment but gradually
encroaches upon and implants in the neighboring serosa.
Meanwhile, the fetus continues to grow within the peritoneal
cavity . In such circumstances , the placenta is found in the
general region of the oviduct and over the posterior aspect of
the broad ligament and uterus. Even more rarely, the conceptus
appears to have escaped after tubal rupture to reimplant
elsewhere in the peritoneal cavity. Primary peritoneal
implantation of the fertilized ovum is very rare. There are
required some criteria : (1) normal tubes and ovaries with no
evidence of recent or remote injury, (2) absence of any
evidence of uteroplacental fistula and (3) presence of a
pregnancy related exclusively to the peritoneal surface and
young enough to eliminate the possibility of secondary
implantation following primary nidation in the tube .
Status of Fetus. Fetal viability in an abdominal
pregnancy is exceedingly precarious and the great
majority succumb. If the pregnancy is diagnosed
after 24 weeks’ gestation scientists await fetal viability
with in-hospital expectant management . Such
management carries a risk for sudden life-threatening
intra-abdominal bleeding .
Diagnosis. Because early rupture or abortion of a tubal
pregnancy is the usual antecedent of an abdominal
pregnancy, in retrospect, a suggestive history can usually be
obtained . Abnormalities likely to be recalled include
spotting or irregular bleeding along with abdominal pain
that usually was most prominent in one or both lower
quadrants .
Symptoms. Women with an abdominal pregnancy are
likely to be uncomfortable but not sufficiently so to
warrant thorough evaluation. Nausea, vomiting , flatulence ,
constipation, diarrhea and abdominal pain may each be
present in varying degrees. Multiparas may state that
pregnancy does not “feel right”. Late in pregnancy, fetal
movements may cause pain. Near term, the empty uterus
has been alleged to go into spurious labor.
Physical Examination. Abnormal fetal positions can
frequently be palpated but the ease of palpating fetal
parts is not a reliable sign. Fetal parts sometimes feel
exceedingly close to the examining fingers even in
normal pregnancies, especially in thin, multiparous
women. Abdominal massage over the pregnancy does
not stimulate the mass to contract as it almost always
does with advanced intrauterine pregnancy. The cervix
is usually displaced, depending in part on the fetal
position, and it may dilate, but appreciable effacement
is usually absent .
Laboratory Tests. An unexplained transient anemia
early in pregnancy may accompany the initial tubal
rupture or abortion. Almost all other laboratory
values, including those reflecting fetal well-being ,
are normal until fetal demise occurs.
Radiological Examination. A strong suspicion of
abdominal pregnancy may be confirmed by x-ray
with a probe or radiopaque material in the uterus. The
fetus then is shown clearly to lie outside the uterine
cavity. Unfortunately , such techniques are not safe
diagnostic procedures if the fetus is intrauterine.
Sonography. Ultrasonic findings with an abdominal
pregnancy most often do not allow an unequivocal
diagnosis to be made; however , in some suspected cases,
these findings may be diagnostic . For example , if the fetal
head is seen to lie immediately adjacent to the maternal
bladder with no interposed uterine tissue , a specific
diagnosis can be made.
Magnetic Resonance Imaging . Magnetic resonance imaging
has been used to confirm abdominal pregnancy following a
suspicious sonographic examination , and the technique
appears to be the most accurate and specific technique.
Computed Tomography. Scientists maintain that computed
tomography is superior to magnetic resonance imaging , but
its use is limited because of fetal radiation effects.
Treatment. Surgery for abdominal pregnancy may
precipitate massive hemorrhage . Without massive blood
transfusion, the outlook for many such women is hopeless.
Hence , it is mandatory that at least 2000mL of compatible
blood be on hand in the operating room, with more readily
available . Preoperatively , two intravenous infusion
systems, each capable of delivering large volumes of fluid at
a rapid rate , should be functioning. At the same time ,
techniques for monitoring the adequacy of the circulation
should be employed. The massive hemorrhage that often
ensues in the course of operations for abdominal
pregnancy is related to the lack of constriction of
hypertrophied opened blood vessels after placental
separation. It has been recommended by some that the
operation be deferred until fetal viability is achieved .
Prognosis. Two of the 10 cases described by scientists
resulted in maternal deaths. Morbidity in surviving patients
is excessive in many cases .
Ovarian Pregnancy
In 1878, Spiegelberg formulate his criteria for diagnosis of
ovarian pregnancy : (1) the tube on the affected side be
intact, (2) the fetal sac must occupy the position of the ovary,
(3) the ovary must be connected to the uterus by the ovarian
ligament and (4) definite ovarian tissue must be found in the
sac wall. Although the ovary can accommodate itself more
readily than the tube to the expanding pregnancy, rupture at
an early period is the usual consequence. Nonetheless, there
are recorded cases in which the ovarian pregnancy went to
term, and a few infants survived.
Symptoms and Signs . Symptoms and physical
findings are likely to mimic those of a tubal
pregnancy or a bleeding corpus luteum. At the time
of operation, early ovarian pregnancies are likely to
be considered corpus luteum cysts or a bleeding
corpus luteum.
Management. Early ovarian pregnancies should be
treated when possible, by wedge resection or
cystectomy ; otherwise; oophorectomy is performed
Cervical pregnancy
Cervical pregnancy in the past has been rare form of
ectopic gestation . It is less common but the
incidence appears to be increasing in part due to
newer forms of assisted reproduction, but especially
after in-vitro fertilization and embryo transfer . In a
typical case, the endocervix is eroded by trophoblast,
and the pregnancy proceeds to develop in the fibrous
cervical wall. The duration of the pregnancy and
ultimately its capacity for growth is dependent upon
the site of embryo implantation. The higher it is
implanted in the cervical canal, the greater is its
capacity to grow and bleed.
Other Sites of Ectopic Pregnancy
A primary splenic pregnancy has been reported by
scientists. The symptoms and signs that led to
laparotomy included pain in the epigastrium and left
shoulder, hypotension , tachycardia, syncope and
tenderness in the vaginal fornices. At laparotomy
considerable hemoperitoneum but normal pelvic
organs were found. A rent in the hilar surface of the
spleen prompted splenecotmy. Microscopically ,
chorionic villi were identified in the splenic rent. A
few cases of primary hepatic pregnancy have been
described , including one with lithopedion formation .
The end.
You might also like
- Ectopic PregnancyDocument11 pagesEctopic PregnancyPeterson Wachira HscNo ratings yet
- Pathophysiology: Tubal Ectopic PregnancyDocument7 pagesPathophysiology: Tubal Ectopic PregnancyRose Anne TolentinoNo ratings yet
- Sites of An Ectopic Pregnancy AreDocument11 pagesSites of An Ectopic Pregnancy AreLouie Kem Anthony BabaranNo ratings yet
- Causes, Risks and Types of Ectopic PregnancyDocument89 pagesCauses, Risks and Types of Ectopic PregnancyMuhammad AbeeshNo ratings yet
- Ectopic Pregnancy Causes, Signs and Risk FactorsDocument19 pagesEctopic Pregnancy Causes, Signs and Risk FactorsanneNo ratings yet
- Causes, Symptoms & Risks of Ectopic PregnancyDocument18 pagesCauses, Symptoms & Risks of Ectopic PregnancyMc_Lopez_1761No ratings yet
- 14 Abortion Noted PDFDocument37 pages14 Abortion Noted PDFmohammed farajiNo ratings yet
- Submitted By: Diana M. Resultay A301/Group-3B Submitted To: Ms. ReyesDocument9 pagesSubmitted By: Diana M. Resultay A301/Group-3B Submitted To: Ms. ReyesDiannetotz MoralesNo ratings yet
- Ectopic PregnancyDocument9 pagesEctopic PregnancyCatherine ZamoraNo ratings yet
- Ass Ectopic PregnancyDocument10 pagesAss Ectopic PregnancyPriyaNo ratings yet
- PathophysiologyDocument3 pagesPathophysiologyEvianne Jersey LofstedtNo ratings yet
- Elizabeth G. Querubin BSN 3E1-9 - Group 195 A Ectopic PregnancyDocument16 pagesElizabeth G. Querubin BSN 3E1-9 - Group 195 A Ectopic PregnancyLizeth Querubin97% (38)
- Ectopic Pregnancy - StatPearls - NCBI BookshelfDocument6 pagesEctopic Pregnancy - StatPearls - NCBI BookshelfLaura valentina ramos mezaNo ratings yet
- Tubal pregnancy - causes, symptoms, and treatment of ectopic pregnancyDocument7 pagesTubal pregnancy - causes, symptoms, and treatment of ectopic pregnancyÄrmâÑÐ JôŠh BåùtîstâNo ratings yet
- Ectopic Pregnancy (Archiv Für Gynà Kologie, Vol. 263, Issue 3) (2000)Document6 pagesEctopic Pregnancy (Archiv Für Gynà Kologie, Vol. 263, Issue 3) (2000)Mahefa Serge RakotozafyNo ratings yet
- Abortionsource 100605123737 Phpapp01Document38 pagesAbortionsource 100605123737 Phpapp01Erina Erichan OtoNo ratings yet
- PREGNANC1Document20 pagesPREGNANC1SriramNo ratings yet
- Ectopic Pregnancy - StatPearls - NCBI BookshelfDocument9 pagesEctopic Pregnancy - StatPearls - NCBI BookshelfKatherine DavilaNo ratings yet
- Ectopic PregenancyDocument69 pagesEctopic PregenancyMahmoud AbbasNo ratings yet
- Understanding Ectopic Pregnancy: Causes, Symptoms and TreatmentDocument11 pagesUnderstanding Ectopic Pregnancy: Causes, Symptoms and TreatmentPrincess BalloNo ratings yet
- Abormal PregnancyDocument4 pagesAbormal PregnancyWandy SejeliNo ratings yet
- Articles of Abnormal Obstetrics CasesDocument11 pagesArticles of Abnormal Obstetrics CasesMarjun MejiaNo ratings yet
- Ectopic PregnancyDocument26 pagesEctopic PregnancyMalek.Fakher1900No ratings yet
- Bleeding in Early PregnancyDocument65 pagesBleeding in Early PregnancyParthi ParthiNo ratings yet
- Pathophysiology of Ectopic PregnancyDocument11 pagesPathophysiology of Ectopic PregnancyJann ericka JaoNo ratings yet
- Brief DescriptionDocument7 pagesBrief DescriptionPrincess Pilove GawongnaNo ratings yet
- Ectopic PregnancyDocument14 pagesEctopic PregnancyPrashanta PahariNo ratings yet
- Ectopic Pregnancy by TaikoDocument12 pagesEctopic Pregnancy by TaikoTaikoNo ratings yet
- Complication of Pregnancy Uterine Cavity: 1 Classification 1.1 Tubal Pregnancy 1.2 Nontubal Ectopic PregnancyDocument41 pagesComplication of Pregnancy Uterine Cavity: 1 Classification 1.1 Tubal Pregnancy 1.2 Nontubal Ectopic Pregnancyゴンサレス マリオ ジョンNo ratings yet
- Ectopic Pregnancy: Aldilyn J. Sarajan, MD, MPH 2 Year Ob-Gyn Resident ZCMCDocument61 pagesEctopic Pregnancy: Aldilyn J. Sarajan, MD, MPH 2 Year Ob-Gyn Resident ZCMCDee SarajanNo ratings yet
- Case Study #1: AbortionDocument42 pagesCase Study #1: AbortionJhoanne DelloroNo ratings yet
- علاااءDocument21 pagesعلاااءalaazeez2000No ratings yet
- Those Related To The Pregnant State: AbortionDocument43 pagesThose Related To The Pregnant State: AbortionJohannah DaroNo ratings yet
- Incomplete AbortionDocument18 pagesIncomplete AbortionAra DirganNo ratings yet
- Ectopic Pregnancy22Document43 pagesEctopic Pregnancy22Sunil YadavNo ratings yet
- 2-Complications of Pregnancy Pt1Document37 pages2-Complications of Pregnancy Pt1pavi7muruganathanNo ratings yet
- 15b Ectopicpregnancy 090507104012 Phpapp02 130825152041 Phpapp01Document48 pages15b Ectopicpregnancy 090507104012 Phpapp02 130825152041 Phpapp01Erwynsonsaut SimanjuntakNo ratings yet
- Bleeding During PregnancyDocument69 pagesBleeding During PregnancyMohnnad Hmood AlgaraybhNo ratings yet
- EctopicwDocument9 pagesEctopicwdrnunungNo ratings yet
- Multiple PregnancyDocument55 pagesMultiple PregnancyNathaniel YeriNo ratings yet
- Ectopic Pregnancy: Signs, Risks, and TreatmentsDocument35 pagesEctopic Pregnancy: Signs, Risks, and TreatmentsOng KarlNo ratings yet
- Abortion: Renhe Hospital Wang JunjieDocument51 pagesAbortion: Renhe Hospital Wang JunjieMadhu Sudhan PandeyaNo ratings yet
- Early Pregnancy Loss in Emergency MedicineDocument14 pagesEarly Pregnancy Loss in Emergency MedicineMuhammad RezaNo ratings yet
- Ectopic Pregnancy Causes, Symptoms, DiagnosisDocument1 pageEctopic Pregnancy Causes, Symptoms, DiagnosisKatie JusayNo ratings yet
- Rupture of The Uterus English RefratDocument11 pagesRupture of The Uterus English RefratassicaNo ratings yet
- Ectopic Pregnancy (Autosaved)Document56 pagesEctopic Pregnancy (Autosaved)susmita shresthaNo ratings yet
- Hysterectomy A-Z: Why, When, How and What afterFrom EverandHysterectomy A-Z: Why, When, How and What afterRating: 4 out of 5 stars4/5 (2)
- Ectopic Pregnancy: by Amielia Mazwa Rafidah Obstetric and Gynecology DepartmentDocument43 pagesEctopic Pregnancy: by Amielia Mazwa Rafidah Obstetric and Gynecology DepartmentAlrick AsentistaNo ratings yet
- Abnormal LabourDocument21 pagesAbnormal LabourbetablockersNo ratings yet
- Health Ethics & Bioetical IssuesDocument76 pagesHealth Ethics & Bioetical Issuesmers puno100% (3)
- Abortion 1Document11 pagesAbortion 1hacker07529No ratings yet
- Predisposing Factors:: Placenta Previa Lower Uterine SegmentDocument11 pagesPredisposing Factors:: Placenta Previa Lower Uterine Segmentjhachers100% (1)
- Ectopic Pregnancy 2022 Edited 3Document40 pagesEctopic Pregnancy 2022 Edited 3apule geraldhumbleNo ratings yet
- кровотеченияDocument19 pagesкровотеченияBrett StevensonNo ratings yet
- Quiz in NCM 107Document1 pageQuiz in NCM 107drae syNo ratings yet
- Uterus: Signs and SymptomsDocument11 pagesUterus: Signs and SymptomsJoy Parallag - BautoNo ratings yet
- Treatment Strategy for Unexplained Infertility and Recurrent MiscarriageFrom EverandTreatment Strategy for Unexplained Infertility and Recurrent MiscarriageKeiji KurodaNo ratings yet
- Ovulation Induction and Controlled Ovarian Stimulation: A Practical GuideFrom EverandOvulation Induction and Controlled Ovarian Stimulation: A Practical GuideNo ratings yet
- Quiz 3Document4 pagesQuiz 3Nikhil TyagiNo ratings yet
- Immuno DeficienciesDocument13 pagesImmuno DeficienciesNikhil TyagiNo ratings yet
- Forensic Midterm MCQsDocument4 pagesForensic Midterm MCQsNikhil TyagiNo ratings yet
- The Israeli Healthcare SystemDocument23 pagesThe Israeli Healthcare SystemNikhil TyagiNo ratings yet
- The Israeli Healthcare SystemDocument23 pagesThe Israeli Healthcare SystemNikhil TyagiNo ratings yet
- Obstetric ComplicationsDocument70 pagesObstetric ComplicationsNikhil TyagiNo ratings yet
- Case StudyDocument17 pagesCase StudyNikhil TyagiNo ratings yet
- Natural Disaster - Health and OccupationDocument25 pagesNatural Disaster - Health and OccupationNikhil TyagiNo ratings yet
- A Round Ligaments: 1. Which Structure Provides The Major Support To The Uterus and Cervix?Document10 pagesA Round Ligaments: 1. Which Structure Provides The Major Support To The Uterus and Cervix?Nikhil Tyagi100% (1)
- Case Study JuniorDocument17 pagesCase Study JuniorNikhil TyagiNo ratings yet
- A Endometriotic Lesions Occur in 1-20% of All Women, The Majority of Which Present Symptomatically and Are Diagnosed With The ConditionDocument7 pagesA Endometriotic Lesions Occur in 1-20% of All Women, The Majority of Which Present Symptomatically and Are Diagnosed With The ConditionNikhil TyagiNo ratings yet
- Rapid Review of RadiologyDocument349 pagesRapid Review of RadiologyAnka Eremia86% (28)
- Ante PartumDocument49 pagesAnte PartumNikhil TyagiNo ratings yet
- Pemphigus FoliaceusDocument9 pagesPemphigus FoliaceusNikhil TyagiNo ratings yet
- Bacterial InfectionsDocument46 pagesBacterial InfectionsNikhil TyagiNo ratings yet
- Integumentary SystemDocument30 pagesIntegumentary SystemNikhil TyagiNo ratings yet
- Abortion Guide: Types, Causes and TreatmentDocument46 pagesAbortion Guide: Types, Causes and TreatmentNikhil TyagiNo ratings yet
- Presentation 2Document26 pagesPresentation 2Nikhil TyagiNo ratings yet
- Interdisciplinary DentistryDocument32 pagesInterdisciplinary DentistryNikhil TyagiNo ratings yet
- Anesthesia in Oral SurgeryDocument12 pagesAnesthesia in Oral SurgeryNikhil TyagiNo ratings yet
- A Manual On Clinical Surgery 9th EditionDocument660 pagesA Manual On Clinical Surgery 9th EditionBandac Alexandra33% (3)
- OJS Project Report ShapiroDocument13 pagesOJS Project Report Shapiropakia2611No ratings yet
- Asthma Internal DiseasesDocument36 pagesAsthma Internal DiseasesNikhil TyagiNo ratings yet
- Implant OlogyDocument35 pagesImplant OlogyNikhil Tyagi0% (2)
- Good Completed ProposalDocument16 pagesGood Completed ProposalNikhil TyagiNo ratings yet
- Spontaneous Intracranial HypotensionDocument23 pagesSpontaneous Intracranial HypotensionNikhil TyagiNo ratings yet
- Intracranial HypotensionDocument17 pagesIntracranial HypotensionNikhil TyagiNo ratings yet
- Biomarkers As Molecular Diagnostics ToolsDocument8 pagesBiomarkers As Molecular Diagnostics ToolsNikhil TyagiNo ratings yet
- A Manual On Clinical Surgery 9th EditionDocument660 pagesA Manual On Clinical Surgery 9th EditionBandac Alexandra33% (3)
- 7ba - Escaped Zoo Animals: Word SheetsDocument6 pages7ba - Escaped Zoo Animals: Word Sheetsnelly hammoudaNo ratings yet
- Anatomy and Physiology of the Reproductive SystemDocument93 pagesAnatomy and Physiology of the Reproductive SystemMelizza Fajardo BañanoNo ratings yet
- Menopause Herbal HealthDocument145 pagesMenopause Herbal HealthMielleNo ratings yet
- ABT Endocrine PPDocument39 pagesABT Endocrine PPABT SchoolNo ratings yet
- CNS PNS Review 3rd QuarterDocument2 pagesCNS PNS Review 3rd QuarterMica Simbajon (micay)No ratings yet
- Human Sexuality Cheat SheetDocument2 pagesHuman Sexuality Cheat Sheetkatiecapes2001No ratings yet
- Physiology of The Female Reproductive System: Liu Wei Department of Ob & Gy Ren Ji HospitalDocument24 pagesPhysiology of The Female Reproductive System: Liu Wei Department of Ob & Gy Ren Ji HospitalAmanuel MaruNo ratings yet
- Grade 10 Biology Lesson on Menstrual CycleDocument5 pagesGrade 10 Biology Lesson on Menstrual CycleCheskaTelanNo ratings yet
- Method Recommendations 4Document108 pagesMethod Recommendations 4Сухоставець Наталія ПетрівнаNo ratings yet
- Embryo Lab ReviewerDocument2 pagesEmbryo Lab ReviewerArianna Francesca VillarazaNo ratings yet
- 3 - Pcos Tog 2017Document11 pages3 - Pcos Tog 2017Siti NurfathiniNo ratings yet
- Dorsal Ovariectomy in RodentsDocument5 pagesDorsal Ovariectomy in RodentsJavier OjedaNo ratings yet
- Ovarian and Fallopian Tube PathologyDocument5 pagesOvarian and Fallopian Tube PathologyShelley PantinopleNo ratings yet
- Human Body System InfographicDocument12 pagesHuman Body System InfographicDiana VillanuevaNo ratings yet
- Ovitrelle Epar Medicine Overview - enDocument3 pagesOvitrelle Epar Medicine Overview - enPhysics with V SagarNo ratings yet
- A Case Study of Cesarean Delivery (Breech Presentation) : Submitted By: Corpus. NichelleDocument24 pagesA Case Study of Cesarean Delivery (Breech Presentation) : Submitted By: Corpus. NichelleFitriNo ratings yet
- Fungsi Hormon KehamilanDocument3 pagesFungsi Hormon KehamilanPisangEpeNo ratings yet
- FET Agric Sciences Revision BookletDocument104 pagesFET Agric Sciences Revision BookletJohnny AmurNo ratings yet
- Female Reproductive Anatomy GuideDocument9 pagesFemale Reproductive Anatomy GuidePinkeyinthecityNo ratings yet
- OBGYN AND LABOR ROOM SERVICESDocument14 pagesOBGYN AND LABOR ROOM SERVICESbhavnil_1796No ratings yet
- Gynecologic Problems of Childhood: Anne Margrette C. VelasquezDocument46 pagesGynecologic Problems of Childhood: Anne Margrette C. VelasquezAnne Margrette Velasquez100% (1)
- LET Reviewer BiologyDocument17 pagesLET Reviewer BiologyMichelle Pamat RelampagosNo ratings yet
- PDF2 AnkiDocument2 pagesPDF2 AnkiBurdendinnieNo ratings yet
- Notes - Reproduction-1Document19 pagesNotes - Reproduction-1Nathan mwapeNo ratings yet
- 2 The Reproductive SystemDocument122 pages2 The Reproductive SystemBryan Lloyd Ballestar RayatNo ratings yet
- Roberts & Walby 2021 - Incipient Infertility - Tracking Eggs and Ovulation Across The Life CourseDocument25 pagesRoberts & Walby 2021 - Incipient Infertility - Tracking Eggs and Ovulation Across The Life CourseRianel PNo ratings yet
- Blood Supply ReproDocument4 pagesBlood Supply ReproNadun MethwadaneNo ratings yet
- Menstrual Cycle LessonDocument11 pagesMenstrual Cycle LessonCarlo ThornappleNo ratings yet
- Science 10 Module 2 Version 3 1Document17 pagesScience 10 Module 2 Version 3 1Skyler MontalvoNo ratings yet
- Nursing Crib Practice TestDocument9 pagesNursing Crib Practice TestjanessajoyNo ratings yet