Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
4 viewsUgib Micah
Ugib Micah
Uploaded by
Ken Ehichoya UgieUpper gastrointestinal bleeding can occur anywhere from the mouth to the duodenojejunal junction. Common causes include peptic ulcer disease, esophageal varices, Mallory-Weiss tears, and gastric cancers. Peptic ulcer disease is often caused by Helicobacter pylori infection, NSAID use, smoking, or Zollinger-Ellison syndrome. Diagnosis involves blood tests, imaging, and endoscopy. Treatment focuses on stabilizing the patient and stopping the bleeding through medications, endoscopic therapies, or surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You might also like
- Biliary Tract Disease - Emmet AndrewsDocument52 pagesBiliary Tract Disease - Emmet AndrewsBoneyJalgarNo ratings yet
- Autopsy of Baby WyllowDocument10 pagesAutopsy of Baby WyllowKOLD News 13100% (1)
- Acute AbdomenDocument110 pagesAcute AbdomenOoi Bai HanNo ratings yet
- Science PSLE PreparationsDocument45 pagesScience PSLE Preparationsxeonzwong0% (2)
- "Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForDocument84 pages"Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForAngela Kristiana IntanNo ratings yet
- "Get in My Belly": Abdominal EmergenciesDocument74 pages"Get in My Belly": Abdominal EmergenciesSherif Abou BakrNo ratings yet
- Gastrointestinal Tract (Partial Edit)Document47 pagesGastrointestinal Tract (Partial Edit)applesncoreNo ratings yet
- Chronic DiarrheaDocument38 pagesChronic DiarrheaShujina ZainabNo ratings yet
- Peptic Ulcers: DR Yotham Phiri Mmed (Surg)Document46 pagesPeptic Ulcers: DR Yotham Phiri Mmed (Surg)Emmanuel MukukaNo ratings yet
- Nursing Stomach NotesDocument5 pagesNursing Stomach Noteslucas dibenedettoNo ratings yet
- Ulcerative ColitisDocument18 pagesUlcerative ColitisKyle Ü D. CunanersNo ratings yet
- Biliary Tract DiseaseDocument52 pagesBiliary Tract DiseaseAna Cotoman100% (1)
- Intestinal Obstruction in ChildrenDocument63 pagesIntestinal Obstruction in Childreng1381821No ratings yet
- Upper GI Bleeding & It's ManagementDocument40 pagesUpper GI Bleeding & It's ManagementManeesha KhalseNo ratings yet
- Chronic DiarrheaDocument66 pagesChronic DiarrheaJulita Yanti100% (1)
- Intestinal ObstructionDocument27 pagesIntestinal ObstructionAna AvilaNo ratings yet
- WelcomeDocument60 pagesWelcomepandem soniyaNo ratings yet
- CCRN-PCCN Review GastrointestinalDocument23 pagesCCRN-PCCN Review GastrointestinalGiovanni MictilNo ratings yet
- 01 - Signs and Symptoms of Git DisordersDocument51 pages01 - Signs and Symptoms of Git DisordersRere AnugrahNo ratings yet
- 07b.NON NEOPLASTIC DISEASE OF STOMACHDocument45 pages07b.NON NEOPLASTIC DISEASE OF STOMACHINDRINo ratings yet
- Abdominal Pain: Resources: Murtagh, John. General Practice 5 EdDocument26 pagesAbdominal Pain: Resources: Murtagh, John. General Practice 5 EdDewanti PermatasariNo ratings yet
- Acute AbdomenDocument53 pagesAcute AbdomenMahdi DiabNo ratings yet
- Pathology Gis: Aanisah F 14.103Document47 pagesPathology Gis: Aanisah F 14.103rftdlsNo ratings yet
- K11 Bedah EsofagusDocument37 pagesK11 Bedah EsofagusenriNo ratings yet
- Abdominal Distention and AscitesDocument49 pagesAbdominal Distention and AscitesNinaNo ratings yet
- Abdominal Swelling + AscitesDocument29 pagesAbdominal Swelling + AscitesDevina CiayadiNo ratings yet
- Gastrointestinal and Liver PathologyDocument99 pagesGastrointestinal and Liver PathologyMuhammad Rifki El-MuammaryNo ratings yet
- RicoDocument62 pagesRicoCunCunAlAndraNo ratings yet
- Management of Upper GI BleedingDocument70 pagesManagement of Upper GI BleedingaboubakarylwabukobaNo ratings yet
- The Stomach and Duodenum: Dr. Elian EliasDocument48 pagesThe Stomach and Duodenum: Dr. Elian EliasmodarNo ratings yet
- 1100 Ultrasound of The Acute Abdomen 15 3Document84 pages1100 Ultrasound of The Acute Abdomen 15 3gp1promo2016No ratings yet
- Dr. Arif Gunawan Teguh WDocument64 pagesDr. Arif Gunawan Teguh WarifgteguhNo ratings yet
- Hepatobiliary DiseaseDocument60 pagesHepatobiliary DiseaseFirdaus AslamNo ratings yet
- Pemicu 2: Mudita Dewi 405150016Document43 pagesPemicu 2: Mudita Dewi 405150016Mudita DewiNo ratings yet
- NCM 102Document70 pagesNCM 102tantanbaragoNo ratings yet
- Overview of Gastric Pathology: Non-Neoplastic DiseasesDocument23 pagesOverview of Gastric Pathology: Non-Neoplastic DiseasesErnest Jerome MalamionNo ratings yet
- Acute AbdomenDocument21 pagesAcute AbdomenMillicent AwuzieNo ratings yet
- Acute AbdomenDocument24 pagesAcute AbdomenGrace SimmonsNo ratings yet
- Problem 1: Stefan Satria Group 4Document49 pagesProblem 1: Stefan Satria Group 4Andre OrgantoNo ratings yet
- Small Bowel Obstruction: By: Dr. Yasser El Basatiny Prof. of Laparoscopic SurgeryDocument41 pagesSmall Bowel Obstruction: By: Dr. Yasser El Basatiny Prof. of Laparoscopic SurgerydenekeNo ratings yet
- Gastroenterology Ambulatory Medicine Clerkship: Scott Grisolano, MD Division of Gastroenterolgy and Hepatology KumcDocument67 pagesGastroenterology Ambulatory Medicine Clerkship: Scott Grisolano, MD Division of Gastroenterolgy and Hepatology KumcMuath AlzghlellatNo ratings yet
- Clinical Reasoning - Abdominal Pain: Alfred H. Alphanto Hario S. SusiloDocument14 pagesClinical Reasoning - Abdominal Pain: Alfred H. Alphanto Hario S. SusiloAlfred HartoyoNo ratings yet
- My Gi Lec...Document34 pagesMy Gi Lec...michelleduran72No ratings yet
- K-11 Esophagus: Departemen Bedah Fakultas Kedokteran USUDocument38 pagesK-11 Esophagus: Departemen Bedah Fakultas Kedokteran USUChristian Lumban GaolNo ratings yet
- Fecalysis: Verian John Hoo - Sudario College of Medical TechnologyDocument58 pagesFecalysis: Verian John Hoo - Sudario College of Medical Technologyepson printerNo ratings yet
- Biliary Tract DiseaseDocument40 pagesBiliary Tract DiseaseIsaac MwangiNo ratings yet
- GastrointesinalDocument4 pagesGastrointesinalRio FutabaNo ratings yet
- Esophagous Stomach Small Intestine PathologyDocument58 pagesEsophagous Stomach Small Intestine PathologytahaNo ratings yet
- Student Copy of Gastrointestinal Problems SP 2010 IggyDocument80 pagesStudent Copy of Gastrointestinal Problems SP 2010 IggyJade CentinoNo ratings yet
- StomachDocument204 pagesStomachrajmv7No ratings yet
- Seminar Vomit Diarrhea DehydrationDocument71 pagesSeminar Vomit Diarrhea DehydrationrmnordinNo ratings yet
- PR BleedDocument20 pagesPR BleedCathy KayNo ratings yet
- Gastro Inflammatory Bowel DiseasesDocument39 pagesGastro Inflammatory Bowel DiseasesCherish Marie HurbodaNo ratings yet
- GastroenterologySlides2020 Copy TG6Document33 pagesGastroenterologySlides2020 Copy TG6yasmeen.houshiehNo ratings yet
- Jaundice: Checklist For HistoryDocument17 pagesJaundice: Checklist For HistoryMustafa H. KadhimNo ratings yet
- Diseases of The StomachDocument72 pagesDiseases of The StomachAMANUEL HABTEWOLDNo ratings yet
- UgumDocument50 pagesUgumhailu henockNo ratings yet
- PA GI Tract Skuad Tandingan Elnineno!Document281 pagesPA GI Tract Skuad Tandingan Elnineno!Arsya AliNo ratings yet
- Bowel ObstructionDocument48 pagesBowel ObstructionPatrick John100% (1)
- D. G.IDocument23 pagesD. G.IGloryJane100% (1)
- Сhronic pancreatitis: Lykhatska G.VDocument42 pagesСhronic pancreatitis: Lykhatska G.VOlga CîrsteaNo ratings yet
- NSC342 Developmental PsychologyDocument1 pageNSC342 Developmental PsychologyKen Ehichoya UgieNo ratings yet
- PHY101Document1 pagePHY101Ken Ehichoya UgieNo ratings yet
- NSC 451Document1 pageNSC 451Ken Ehichoya UgieNo ratings yet
- Application I2212D15779496 18-01-2024Document1 pageApplication I2212D15779496 18-01-2024Ken Ehichoya UgieNo ratings yet
- 35997565636Document3 pages35997565636Ken Ehichoya UgieNo ratings yet
- NECO Results PortalDocument1 pageNECO Results PortalKen Ehichoya UgieNo ratings yet
- Introduction To PharmacologyDocument10 pagesIntroduction To PharmacologyKen Ehichoya UgieNo ratings yet
- 4Document16 pages4Ken Ehichoya UgieNo ratings yet
- Immaculate DocumentsDocument4 pagesImmaculate DocumentsKen Ehichoya UgieNo ratings yet
- CHE351Document1 pageCHE351Ken Ehichoya UgieNo ratings yet
- CLEANSE AND PURIFY THYSELF. DR. RICHARD ANDERSON (2019 Final Edition)Document250 pagesCLEANSE AND PURIFY THYSELF. DR. RICHARD ANDERSON (2019 Final Edition)Charif El Knaichi100% (1)
- NCM 105 NutritionDocument28 pagesNCM 105 NutritionCyrill100% (2)
- Prelim Reviewer PcolDocument37 pagesPrelim Reviewer Pcol11Lag2Carisma II, Jose P.No ratings yet
- Chinese Reflexology Foot ChartsDocument1 pageChinese Reflexology Foot ChartsRaquel Sacramento100% (1)
- 1-Human Physiology Digestion Absorption PDFDocument29 pages1-Human Physiology Digestion Absorption PDFPintu KarmakarNo ratings yet
- Morphology, Systematics, and Biology of The Spanish MackerelsDocument148 pagesMorphology, Systematics, and Biology of The Spanish MackerelsRio AlmusataNo ratings yet
- Floating Drug Delivery System ThesisDocument4 pagesFloating Drug Delivery System Thesisvxjtklxff100% (2)
- Frog Dissection Pre Lab 2Document4 pagesFrog Dissection Pre Lab 2bondwilderNo ratings yet
- Treatment of Hypochlohydria With A Complex Homeopathic SarcodeDocument4 pagesTreatment of Hypochlohydria With A Complex Homeopathic SarcodeGanesh ArcotNo ratings yet
- NCERT - Exemplar - Life ProcessesDocument26 pagesNCERT - Exemplar - Life ProcessesRagini BaghelNo ratings yet
- Bio 123 PDFDocument32 pagesBio 123 PDFP NagNo ratings yet
- Gastrointestinal and Endocrine Disorder HandoutsDocument120 pagesGastrointestinal and Endocrine Disorder HandoutsJan Michael R. RemoladoNo ratings yet
- Laryngopharyngeal ReconstructionDocument8 pagesLaryngopharyngeal ReconstructionGrace Amoo-quayeNo ratings yet
- Abdominal Radiography in Small Animals: Chris Warren-Smith and Chris LambDocument8 pagesAbdominal Radiography in Small Animals: Chris Warren-Smith and Chris LambRystha BurgaNo ratings yet
- SAWINDERJITDocument5 pagesSAWINDERJITapi-3731257No ratings yet
- 0653 s16 QP 32Document24 pages0653 s16 QP 32yuke kristinaNo ratings yet
- I Have Stomach Trouble A Lot of Paint and Nause. I Thing I Have Gastritis, But I Amtold There Are Several Kinds. Is It So?Document7 pagesI Have Stomach Trouble A Lot of Paint and Nause. I Thing I Have Gastritis, But I Amtold There Are Several Kinds. Is It So?amandaNo ratings yet
- Pyloric Stenosis Case StudyDocument37 pagesPyloric Stenosis Case StudyFaith Torralba100% (3)
- Bio 270 Lecture 10 University of TorontoDocument24 pagesBio 270 Lecture 10 University of TorontoJD BaruaNo ratings yet
- STOMACHDocument18 pagesSTOMACHJessa RedondoNo ratings yet
- Chapter 41 - Animal NutritionDocument7 pagesChapter 41 - Animal Nutritionliennev02No ratings yet
- The Digestive SystemDocument19 pagesThe Digestive Systemianpoblete13No ratings yet
- Pyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgDocument21 pagesPyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgJames NTEGEREJIMANANo ratings yet
- International Journal of Nursing StudiesDocument10 pagesInternational Journal of Nursing StudiesLina Mahayaty SembiringNo ratings yet
- Health Is HappinessDocument101 pagesHealth Is HappinessMrudula V.100% (20)
- Digestion and Absorption 111Document6 pagesDigestion and Absorption 111Brijesh BalachandranNo ratings yet
- Case Study-Gastric CancerDocument19 pagesCase Study-Gastric Cancerbhelskie100% (2)
- 4thQ Week1 PPT DigestiveDocument49 pages4thQ Week1 PPT DigestiveGeronimo SantiagoNo ratings yet
Ugib Micah
Ugib Micah
Uploaded by
Ken Ehichoya Ugie0 ratings0% found this document useful (0 votes)
4 views21 pagesUpper gastrointestinal bleeding can occur anywhere from the mouth to the duodenojejunal junction. Common causes include peptic ulcer disease, esophageal varices, Mallory-Weiss tears, and gastric cancers. Peptic ulcer disease is often caused by Helicobacter pylori infection, NSAID use, smoking, or Zollinger-Ellison syndrome. Diagnosis involves blood tests, imaging, and endoscopy. Treatment focuses on stabilizing the patient and stopping the bleeding through medications, endoscopic therapies, or surgery.
Original Description:
Medical emergency
Original Title
ugib micah
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentUpper gastrointestinal bleeding can occur anywhere from the mouth to the duodenojejunal junction. Common causes include peptic ulcer disease, esophageal varices, Mallory-Weiss tears, and gastric cancers. Peptic ulcer disease is often caused by Helicobacter pylori infection, NSAID use, smoking, or Zollinger-Ellison syndrome. Diagnosis involves blood tests, imaging, and endoscopy. Treatment focuses on stabilizing the patient and stopping the bleeding through medications, endoscopic therapies, or surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
4 views21 pagesUgib Micah
Ugib Micah
Uploaded by
Ken Ehichoya UgieUpper gastrointestinal bleeding can occur anywhere from the mouth to the duodenojejunal junction. Common causes include peptic ulcer disease, esophageal varices, Mallory-Weiss tears, and gastric cancers. Peptic ulcer disease is often caused by Helicobacter pylori infection, NSAID use, smoking, or Zollinger-Ellison syndrome. Diagnosis involves blood tests, imaging, and endoscopy. Treatment focuses on stabilizing the patient and stopping the bleeding through medications, endoscopic therapies, or surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 21
UGIB
upper gastro intestinal bleeding
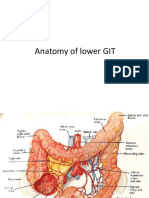
• upper GI tract is anywhere from the mouth to the
duodenojejunal junction or ligament of teritz
• abdominal pain may be
• visceral- diffused
• somatic- localised
• referred
causes
• Peptic ulceration.
• Mucosal inflammation (oesophagitis, gastritis, or
duodenitis).
• Oesophageal varices.
• Mallory–Weiss tear.
• Boerhaave syndrome
• Gastric carcinoma.
• Coagulation disorders (thrombocytopenia,
warfarin).
peptic ulcer disease
• the stomach is composed of 4 regions
• cardiac
• fundus
• body
• pylorus
• the layers of the stomach are
• mucosa
• sub mucosa
• muscularis
• serosa
• the gastric gland secretes gastric juice about
2-3L/day
• mucus cell-mucus
• parietal cell- intrinsic factor(absorption of B12) &
Hcl
• chief cell- pepsinogen and gastric lipase
• G cells in the pylorus secretes gastrin
• an ulcer is a disruption in the mucosa integrity of
the stomach/duodenum leading to local defect or
escavation due to inflammation
• peptic ulcer may be
• gastric- relieved by meal
• duodenal- 3hrs after meal
• meckel's diverticulum
• esophagus
• intestines
• PUD may be caused by
• helicobacter pylori
• NSAID- inhibition of cox 1, cox 2, prostaglandins
• chrons disease
• zollinger ellison syndrome
• smoking
• diet
• stress induced gastritis
esophageal varices
• extreme dilation of the
veins in the lower 3rd of
the esophagus due to
portal hypertension from
liver cirrhosis
• mallory weiss tear- tear in the area of the gastric
cardia due to forceful vomitting
• boerhaave syndrome- rupture of the oesophagus
due to forceful vomitting
• Gastric carcinoma.
• Coagulation disorders (thrombocytopenia,
warfarin).
presentation
• hematemesis
• melena stool
• hematochezia
• pallor
• signs and symptoms of shock
• cool clammy extremity
• tachycardia
• hypotension
• tachypnea
ivestigation
• blood- pcv,fbc, clothing profile( PT, PTT, INR), EUCr,
LFT, HBSg + anti HCV, GXM, RVS
• USS
• CXR
• Urinalysis
• endoscopy
• ecg
• PUD(h.pylori antigen, urea breath test, stool
monoclonial antibody)
history
• past gi bleeds
• ulcers
• how much blood was vomitted or stooled
• color of stool and duration
• history of liver disease
• vomitting
• drugs use
• diet
examination
• assess gcs
• capillary refil
• urine output
• examine for signs of liver disease
• abdominal pain
• tilt test- defficit in sbp of 20mmHg and dbp of
10mmHg or an increase of 20bpm in pulse
• rectal exam for melena
management
• ABCs- supplemental o2, suction copiously if patient
cannot maintain airway, 2 large bore cannula for IV
• triple regimen- PPI(omeprazole, rabeprazole) 20mg,
clarithromycin 500mg, amoxicillin 1g/metronidazole
500mg bd for 7-14days
questions
You might also like
- Biliary Tract Disease - Emmet AndrewsDocument52 pagesBiliary Tract Disease - Emmet AndrewsBoneyJalgarNo ratings yet
- Autopsy of Baby WyllowDocument10 pagesAutopsy of Baby WyllowKOLD News 13100% (1)
- Acute AbdomenDocument110 pagesAcute AbdomenOoi Bai HanNo ratings yet
- Science PSLE PreparationsDocument45 pagesScience PSLE Preparationsxeonzwong0% (2)
- "Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForDocument84 pages"Gosh, Mrs. Doubtfire You Look Pale": Fire" in Television at The Emergency Departement You Worked ForAngela Kristiana IntanNo ratings yet
- "Get in My Belly": Abdominal EmergenciesDocument74 pages"Get in My Belly": Abdominal EmergenciesSherif Abou BakrNo ratings yet
- Gastrointestinal Tract (Partial Edit)Document47 pagesGastrointestinal Tract (Partial Edit)applesncoreNo ratings yet
- Chronic DiarrheaDocument38 pagesChronic DiarrheaShujina ZainabNo ratings yet
- Peptic Ulcers: DR Yotham Phiri Mmed (Surg)Document46 pagesPeptic Ulcers: DR Yotham Phiri Mmed (Surg)Emmanuel MukukaNo ratings yet
- Nursing Stomach NotesDocument5 pagesNursing Stomach Noteslucas dibenedettoNo ratings yet
- Ulcerative ColitisDocument18 pagesUlcerative ColitisKyle Ü D. CunanersNo ratings yet
- Biliary Tract DiseaseDocument52 pagesBiliary Tract DiseaseAna Cotoman100% (1)
- Intestinal Obstruction in ChildrenDocument63 pagesIntestinal Obstruction in Childreng1381821No ratings yet
- Upper GI Bleeding & It's ManagementDocument40 pagesUpper GI Bleeding & It's ManagementManeesha KhalseNo ratings yet
- Chronic DiarrheaDocument66 pagesChronic DiarrheaJulita Yanti100% (1)
- Intestinal ObstructionDocument27 pagesIntestinal ObstructionAna AvilaNo ratings yet
- WelcomeDocument60 pagesWelcomepandem soniyaNo ratings yet
- CCRN-PCCN Review GastrointestinalDocument23 pagesCCRN-PCCN Review GastrointestinalGiovanni MictilNo ratings yet
- 01 - Signs and Symptoms of Git DisordersDocument51 pages01 - Signs and Symptoms of Git DisordersRere AnugrahNo ratings yet
- 07b.NON NEOPLASTIC DISEASE OF STOMACHDocument45 pages07b.NON NEOPLASTIC DISEASE OF STOMACHINDRINo ratings yet
- Abdominal Pain: Resources: Murtagh, John. General Practice 5 EdDocument26 pagesAbdominal Pain: Resources: Murtagh, John. General Practice 5 EdDewanti PermatasariNo ratings yet
- Acute AbdomenDocument53 pagesAcute AbdomenMahdi DiabNo ratings yet
- Pathology Gis: Aanisah F 14.103Document47 pagesPathology Gis: Aanisah F 14.103rftdlsNo ratings yet
- K11 Bedah EsofagusDocument37 pagesK11 Bedah EsofagusenriNo ratings yet
- Abdominal Distention and AscitesDocument49 pagesAbdominal Distention and AscitesNinaNo ratings yet
- Abdominal Swelling + AscitesDocument29 pagesAbdominal Swelling + AscitesDevina CiayadiNo ratings yet
- Gastrointestinal and Liver PathologyDocument99 pagesGastrointestinal and Liver PathologyMuhammad Rifki El-MuammaryNo ratings yet
- RicoDocument62 pagesRicoCunCunAlAndraNo ratings yet
- Management of Upper GI BleedingDocument70 pagesManagement of Upper GI BleedingaboubakarylwabukobaNo ratings yet
- The Stomach and Duodenum: Dr. Elian EliasDocument48 pagesThe Stomach and Duodenum: Dr. Elian EliasmodarNo ratings yet
- 1100 Ultrasound of The Acute Abdomen 15 3Document84 pages1100 Ultrasound of The Acute Abdomen 15 3gp1promo2016No ratings yet
- Dr. Arif Gunawan Teguh WDocument64 pagesDr. Arif Gunawan Teguh WarifgteguhNo ratings yet
- Hepatobiliary DiseaseDocument60 pagesHepatobiliary DiseaseFirdaus AslamNo ratings yet
- Pemicu 2: Mudita Dewi 405150016Document43 pagesPemicu 2: Mudita Dewi 405150016Mudita DewiNo ratings yet
- NCM 102Document70 pagesNCM 102tantanbaragoNo ratings yet
- Overview of Gastric Pathology: Non-Neoplastic DiseasesDocument23 pagesOverview of Gastric Pathology: Non-Neoplastic DiseasesErnest Jerome MalamionNo ratings yet
- Acute AbdomenDocument21 pagesAcute AbdomenMillicent AwuzieNo ratings yet
- Acute AbdomenDocument24 pagesAcute AbdomenGrace SimmonsNo ratings yet
- Problem 1: Stefan Satria Group 4Document49 pagesProblem 1: Stefan Satria Group 4Andre OrgantoNo ratings yet
- Small Bowel Obstruction: By: Dr. Yasser El Basatiny Prof. of Laparoscopic SurgeryDocument41 pagesSmall Bowel Obstruction: By: Dr. Yasser El Basatiny Prof. of Laparoscopic SurgerydenekeNo ratings yet
- Gastroenterology Ambulatory Medicine Clerkship: Scott Grisolano, MD Division of Gastroenterolgy and Hepatology KumcDocument67 pagesGastroenterology Ambulatory Medicine Clerkship: Scott Grisolano, MD Division of Gastroenterolgy and Hepatology KumcMuath AlzghlellatNo ratings yet
- Clinical Reasoning - Abdominal Pain: Alfred H. Alphanto Hario S. SusiloDocument14 pagesClinical Reasoning - Abdominal Pain: Alfred H. Alphanto Hario S. SusiloAlfred HartoyoNo ratings yet
- My Gi Lec...Document34 pagesMy Gi Lec...michelleduran72No ratings yet
- K-11 Esophagus: Departemen Bedah Fakultas Kedokteran USUDocument38 pagesK-11 Esophagus: Departemen Bedah Fakultas Kedokteran USUChristian Lumban GaolNo ratings yet
- Fecalysis: Verian John Hoo - Sudario College of Medical TechnologyDocument58 pagesFecalysis: Verian John Hoo - Sudario College of Medical Technologyepson printerNo ratings yet
- Biliary Tract DiseaseDocument40 pagesBiliary Tract DiseaseIsaac MwangiNo ratings yet
- GastrointesinalDocument4 pagesGastrointesinalRio FutabaNo ratings yet
- Esophagous Stomach Small Intestine PathologyDocument58 pagesEsophagous Stomach Small Intestine PathologytahaNo ratings yet
- Student Copy of Gastrointestinal Problems SP 2010 IggyDocument80 pagesStudent Copy of Gastrointestinal Problems SP 2010 IggyJade CentinoNo ratings yet
- StomachDocument204 pagesStomachrajmv7No ratings yet
- Seminar Vomit Diarrhea DehydrationDocument71 pagesSeminar Vomit Diarrhea DehydrationrmnordinNo ratings yet
- PR BleedDocument20 pagesPR BleedCathy KayNo ratings yet
- Gastro Inflammatory Bowel DiseasesDocument39 pagesGastro Inflammatory Bowel DiseasesCherish Marie HurbodaNo ratings yet
- GastroenterologySlides2020 Copy TG6Document33 pagesGastroenterologySlides2020 Copy TG6yasmeen.houshiehNo ratings yet
- Jaundice: Checklist For HistoryDocument17 pagesJaundice: Checklist For HistoryMustafa H. KadhimNo ratings yet
- Diseases of The StomachDocument72 pagesDiseases of The StomachAMANUEL HABTEWOLDNo ratings yet
- UgumDocument50 pagesUgumhailu henockNo ratings yet
- PA GI Tract Skuad Tandingan Elnineno!Document281 pagesPA GI Tract Skuad Tandingan Elnineno!Arsya AliNo ratings yet
- Bowel ObstructionDocument48 pagesBowel ObstructionPatrick John100% (1)
- D. G.IDocument23 pagesD. G.IGloryJane100% (1)
- Сhronic pancreatitis: Lykhatska G.VDocument42 pagesСhronic pancreatitis: Lykhatska G.VOlga CîrsteaNo ratings yet
- NSC342 Developmental PsychologyDocument1 pageNSC342 Developmental PsychologyKen Ehichoya UgieNo ratings yet
- PHY101Document1 pagePHY101Ken Ehichoya UgieNo ratings yet
- NSC 451Document1 pageNSC 451Ken Ehichoya UgieNo ratings yet
- Application I2212D15779496 18-01-2024Document1 pageApplication I2212D15779496 18-01-2024Ken Ehichoya UgieNo ratings yet
- 35997565636Document3 pages35997565636Ken Ehichoya UgieNo ratings yet
- NECO Results PortalDocument1 pageNECO Results PortalKen Ehichoya UgieNo ratings yet
- Introduction To PharmacologyDocument10 pagesIntroduction To PharmacologyKen Ehichoya UgieNo ratings yet
- 4Document16 pages4Ken Ehichoya UgieNo ratings yet
- Immaculate DocumentsDocument4 pagesImmaculate DocumentsKen Ehichoya UgieNo ratings yet
- CHE351Document1 pageCHE351Ken Ehichoya UgieNo ratings yet
- CLEANSE AND PURIFY THYSELF. DR. RICHARD ANDERSON (2019 Final Edition)Document250 pagesCLEANSE AND PURIFY THYSELF. DR. RICHARD ANDERSON (2019 Final Edition)Charif El Knaichi100% (1)
- NCM 105 NutritionDocument28 pagesNCM 105 NutritionCyrill100% (2)
- Prelim Reviewer PcolDocument37 pagesPrelim Reviewer Pcol11Lag2Carisma II, Jose P.No ratings yet
- Chinese Reflexology Foot ChartsDocument1 pageChinese Reflexology Foot ChartsRaquel Sacramento100% (1)
- 1-Human Physiology Digestion Absorption PDFDocument29 pages1-Human Physiology Digestion Absorption PDFPintu KarmakarNo ratings yet
- Morphology, Systematics, and Biology of The Spanish MackerelsDocument148 pagesMorphology, Systematics, and Biology of The Spanish MackerelsRio AlmusataNo ratings yet
- Floating Drug Delivery System ThesisDocument4 pagesFloating Drug Delivery System Thesisvxjtklxff100% (2)
- Frog Dissection Pre Lab 2Document4 pagesFrog Dissection Pre Lab 2bondwilderNo ratings yet
- Treatment of Hypochlohydria With A Complex Homeopathic SarcodeDocument4 pagesTreatment of Hypochlohydria With A Complex Homeopathic SarcodeGanesh ArcotNo ratings yet
- NCERT - Exemplar - Life ProcessesDocument26 pagesNCERT - Exemplar - Life ProcessesRagini BaghelNo ratings yet
- Bio 123 PDFDocument32 pagesBio 123 PDFP NagNo ratings yet
- Gastrointestinal and Endocrine Disorder HandoutsDocument120 pagesGastrointestinal and Endocrine Disorder HandoutsJan Michael R. RemoladoNo ratings yet
- Laryngopharyngeal ReconstructionDocument8 pagesLaryngopharyngeal ReconstructionGrace Amoo-quayeNo ratings yet
- Abdominal Radiography in Small Animals: Chris Warren-Smith and Chris LambDocument8 pagesAbdominal Radiography in Small Animals: Chris Warren-Smith and Chris LambRystha BurgaNo ratings yet
- SAWINDERJITDocument5 pagesSAWINDERJITapi-3731257No ratings yet
- 0653 s16 QP 32Document24 pages0653 s16 QP 32yuke kristinaNo ratings yet
- I Have Stomach Trouble A Lot of Paint and Nause. I Thing I Have Gastritis, But I Amtold There Are Several Kinds. Is It So?Document7 pagesI Have Stomach Trouble A Lot of Paint and Nause. I Thing I Have Gastritis, But I Amtold There Are Several Kinds. Is It So?amandaNo ratings yet
- Pyloric Stenosis Case StudyDocument37 pagesPyloric Stenosis Case StudyFaith Torralba100% (3)
- Bio 270 Lecture 10 University of TorontoDocument24 pagesBio 270 Lecture 10 University of TorontoJD BaruaNo ratings yet
- STOMACHDocument18 pagesSTOMACHJessa RedondoNo ratings yet
- Chapter 41 - Animal NutritionDocument7 pagesChapter 41 - Animal Nutritionliennev02No ratings yet
- The Digestive SystemDocument19 pagesThe Digestive Systemianpoblete13No ratings yet
- Pyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgDocument21 pagesPyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgJames NTEGEREJIMANANo ratings yet
- International Journal of Nursing StudiesDocument10 pagesInternational Journal of Nursing StudiesLina Mahayaty SembiringNo ratings yet
- Health Is HappinessDocument101 pagesHealth Is HappinessMrudula V.100% (20)
- Digestion and Absorption 111Document6 pagesDigestion and Absorption 111Brijesh BalachandranNo ratings yet
- Case Study-Gastric CancerDocument19 pagesCase Study-Gastric Cancerbhelskie100% (2)
- 4thQ Week1 PPT DigestiveDocument49 pages4thQ Week1 PPT DigestiveGeronimo SantiagoNo ratings yet