Professional Documents
Culture Documents
Tracheostomy B.M
Uploaded by
Evancemwenya1230 ratings0% found this document useful (0 votes)
1 views25 pagesOriginal Title
TRACHEOSTOMY B.M
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
1 views25 pagesTracheostomy B.M
Uploaded by
Evancemwenya123Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 25
TRACHEOSTOMY
BY
MUNJILI B. MR.
Tuesday, April 23, 2024 1
Tuesday, April 23, 2024 2
Tuesday, April 23, 2024 3
Tuesday, April 23, 2024 4
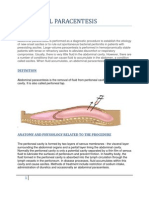
ANATOMY OF THE TRACHEA
• The trachea is a continuation of the larynx and
extends downwards to about the level of the 5th
thoracic vertebra where it divides (bifurcates) at the
carina into the right and left bronchi,one bronchus
going to each lung.
• The trachea is composed of from 16-20 incomplete
(c-shaped) rings of hyaline cartilages situated one
above the other.
Tuesday, April 23, 2024 5
DEFINATION OF TERMS
1. TRACHEOTOMY; This is a surgical incision into the
trachea for the purpose of establishing an airway.
2. TRACHEOSTOMY;This is the stoma that results
from the tracheotomy, and its when an indwelling
tube is inserted into the trachea
3. TRACHEOSTOMY;This is an artificial respiratory
opening made in the anterior wall of the neck and
trachea-made between the 2nd and 3rd or 3rd and
4th tracheal rings.
4. TRACHEOSTOMY;Is the creation of an artificial
opening into the trachea through which breathing
occurs.
Tuesday, April 23, 2024 6
TYPES OF TRACHEOSTOMY
1. EMMERGENCY TRACHEOSTOMY;This is when an
operation is done immediately e.g. in foreign
bodies.
2. ELECTIVE TRACHEOSTOMY;This is when the
patient is prepared in advance e.g. in cancer of
the upper respiratory tract.
3. TEMPORAL TRACHEOSTOMY;This is a
tracheotomy which is performed for a short
period then closed.
4. PERMANENT TRACHEOSTOMY;This is left for a life
time.
Tuesday, April 23, 2024 7
INDICATIONS FOR A TRACHEOSTOMY.
• INDICATIONS
• Obstructive Condition of the Larynx.
– Acute Oedema of the epiglottis
– Carcinoma of the Larynx
– Impacted foreign bodies
– Trauma
– Burns of the mouth or Larynx
– Acute Laryngitis particularly Diphtheric membrane
•
Tuesday, April 23, 2024 8
Indications Cont’d
• B) Paralysis or Spasms of the respiratory
muscles and Respiratory failure
• 1) Bulbar paralysis
• 2) Tetanus
• 3) certain stages of coma.
Tuesday, April 23, 2024 9
POST OPERATIVECARE
Environment
• Pt Nursed in acute bay for the first 48 hours.
• Clean environment , free of dust to prevent infection and
irritation of the patients airway.
• Humidified oxygen should be available within the patients
surrounding in case of respiratory distress.
• Suctioning apparatus are required to clear air way.
• Bell near the patient or buzzer as a means of
communication to alert the nurses or caregivers in case of
assistance.
• The environment should have enough light for easy
observation.
• Positioning and maintenance of a patent airway
• Patient nursed in lateral or lying position to
promote draining of secretions.
• The patient take slow deep breath , turning and
coughing to assist in mobilizing secretions.
• The tube will be observed for any accumulation
of excess secretions suctioning will be done
whenever necessary.
• Observations
• Monitoring of the patients level of at least
quarter hourly after the patient gets back
from theatre
• vital signs will be done quarter hourly.
• close monitoring of the stoma site for redness,
swelling, and bleeding as these are common
signs of inflammation and will help take
appropriate intervention.
Observations cont’d
• Oxygen saturation will be monitored with an
oxymetry to rule out hypoxia.
• vital sign will be done temperature to rule out
infection, blood pressure to rule out hypotension
which may be due to excessive bleeding during
the procedure.
• The air way will be observed and if any
obstruction or secretions mild suctioning will be
done to promote proper breathing. Observe if
the tube is in situ to prevent dislodging
• Pain movement
• Patient may be positioned in the most
comfortable position minding the stoma site
to prevent injury and promote comfort. Give
divisional therapy such as television to shift
his mind off the pain. Prescibed analgesics can
be given such as pethidine 50-100mg
whenever necessary or as prescribed but
being conscious with addiction
• Psychological care
• Re assure the patient as this state is very frightening
experience
• Explain to family and patient that there will be temporal
loss of voice due to the tracheostomy so as to allay anxiety.
Allow family and patient to ask questions so as to allay
anxiety and gain knowledge about the condition
• . An individual who had undergone the same procedure will
be invited to allay anxiety to the relatives and patient to
help patient gain hope.
• Family and patient will be explained to on the means of
communication.
Rest and exercise
• Encourage the patient to have enough rest so as
to prevent respiratory distress because of the
operation done.
• A quiet environment, clean and comfortable will
promote rest.
• Unnecessary suctioning will be avoided to avoid
disturbing the patient. Minimal neck exercises
will be allowed or done to prevent neck stiffness.
• Mobility of the patient at least third day post
operatively will be allowed to avoid muscle
contractures and pressure sores.
Nutrition
• Insertion of the nasal gastric tube will be done
to use for feeding and ensure adequate
nutrition.
• Liquids are encouraged as soon as there is no
danger of vomiting. Proceed with semi solid
foods and then solids,
• Reporting of any leakage of fluids if any at
once. A fluid balance chart is necessary to
monitor the fluid balance
Wound care or stoma care
• The dressing that is the first dressing will be removed by
the surgeon and cleaned with normal saline and sterile
cotton swabs to prevent infection
• . Frequent wound cleaning will be done at least two
times to promote wound healing and prevent infection.
• Wound care or stoma care will be done with a sterile
pack of wound dressing to promote sterility and prevent
infection.
• The gauze will be changed and secure with tapes.
Whenever necessary or soiled to prevent infection and
promote self-esteem.
Hygiene
• The patient will be assisted with activities of
daily living to promote quick healing.
• Bed bathing will be done a few days after an
operation and assisted bath will be done
when patient becomes mobile so as to
promote good hygiene.
• Proper oral toilet will be done to prevent
halitosis.
Speech therapy
• The patient will be closer to the nurses bay or
station and the central call light system will be
marked to indicate that the client cannot speak.
• The and family will be taught about
communication skills that is use of pictures and
letters, hand signals or a computer as well as a
call light within the reach of the patient to
promote communication and decrease
frustration or irritability.
Speech therapy cont’d
• Questions will not be open ended as they may
need explanation hence they will be ‘yes’ or ‘no’
answers for efficient response.
• A bell will be placed at the patients reach so as to
call the nurse to facilitate communication.
• A cuff less tube with a covered, fenestrated
tracheostomy tube in place will be used to
enable the patient speak.
• When the patient can tolerate cuff deflation, he
or she places a finger over the tracheostomy tube
on exhalation to allow speech.
• Elimination
• Constipation will be a problem initially but
introduction of fiber containing foods will help
relief constipation. Enough fluids will promote
use of a urinary catheter for excretion of urine
and bed pan for bowel opening
Information, education and
communication
• . Instructions are given concerning care of the wound and stoma
especially if permanent to promote hygiene and prevent infection.
• Patient will be advised not to swim and to be careful when bathing
that is covering the stoma to avoid water from entering and causing
chocking in the airway.
• When taking walks, they need to wear a scuff or collared shirt to
cover the opening and the shirt should be porous to promote
proper air circulation.
• Advise on drug adherence will be given to promote healing.
• proper nutrition will be emphasized to provide energy, rebuild
worn out tissue, to boost the immunity.
• Patient and relatives will be advised to maintain good hygiene to
prevent infection.
NURSING PROBLEMS /DIAGNOSES
• 1. Risk of Airway Obstruction related to
Secretions and Swelling (blocked cannula)
• 2. Risk of the Tracheostomy Tube Dislodging
and Cross – Infection
• 3. Pain related to nerve injury caused by
surgical incision
• 4. Risk of bleeding related to Surgery in the
highly vascular area.
Tuesday, April 23, 2024 24
COMPLICATIONS OF TRACHEOSTOMY
1. Hemorrhage which could be primary or secondary because
the tracheotomy area is very vascular.
2. Surgical emphysema( presence of air in the subcutaneous
tissue) due to excessive dissection of tissue.
3. Pneumothorax common in children due an injury of the
epiod pleural.
4. Displacement of the tube due to improper fitting of
tracheotomy tubes.
5. Blockage of the tracheotomy tube leading to asphyxia.
6. Atelectasis
7. Trachea ulceration and stenosis.
8. Difficult in decannulation.
Tuesday, April 23, 2024 25
You might also like
- What Looks Like Crazy On An Ordinary DayDocument9 pagesWhat Looks Like Crazy On An Ordinary Dayapi-271170207100% (1)
- Emergency NursingDocument10 pagesEmergency Nursingkellyhutch50% (2)
- SP42 Thoracentesis (Adult)Document7 pagesSP42 Thoracentesis (Adult)Adam HuzaibyNo ratings yet
- Hydroponic Lettuce: Cheryl Kaiser and Matt ErnstDocument4 pagesHydroponic Lettuce: Cheryl Kaiser and Matt ErnstKamal deep100% (1)
- The Secret of Being HappyDocument282 pagesThe Secret of Being Happylcs1234678100% (3)
- TracheostomyDocument3 pagesTracheostomySarah Elizabeth WalkerNo ratings yet
- Airway Obstruction and TracheostomyDocument44 pagesAirway Obstruction and TracheostomySindhu BabuNo ratings yet
- ThoracentesisDocument1 pageThoracentesisNiño Cris PatiñoNo ratings yet
- TracheostomyDocument29 pagesTracheostomyFemi AustinNo ratings yet
- Tracheostomy SlidesDocument24 pagesTracheostomy SlidesMohammed AdamNo ratings yet
- TracheostomycaredraftDocument7 pagesTracheostomycaredraftAlane MorenoNo ratings yet
- Chap.30 Med SurgDocument4 pagesChap.30 Med SurgSheldon SloanNo ratings yet
- Abdominal ParacentesisDocument14 pagesAbdominal ParacentesisMonika Joseph75% (4)
- Insertion of TubesDocument29 pagesInsertion of Tubesqopcyrus10No ratings yet
- Tracheostomy Care: Presented by Sital B. Sharma M SC Nursing Student College of Nursing. N.B.M.C.HDocument74 pagesTracheostomy Care: Presented by Sital B. Sharma M SC Nursing Student College of Nursing. N.B.M.C.HShetal Sharma100% (1)
- Tracheostomy CareDocument44 pagesTracheostomy CareJharaNo ratings yet
- Advance Trauma Life Support (ATLS)Document47 pagesAdvance Trauma Life Support (ATLS)Ben Man Jun100% (2)
- Airway Management: by Paul Edmer CorcueraDocument40 pagesAirway Management: by Paul Edmer CorcueraJeco ValdezNo ratings yet
- Abdominal ParacentesisDocument5 pagesAbdominal ParacentesisVijith.V.kumar100% (1)
- Intubation: by Joan SinghDocument17 pagesIntubation: by Joan SinghJoan Singh100% (1)
- Tracheostomy 8th SemesterDocument38 pagesTracheostomy 8th SemesterpotoraccosminaNo ratings yet
- Tube Thoracostomy Module: Vic V. Vernenkar, D.O. Dept. of Surgery St. Barnabas HospitalDocument20 pagesTube Thoracostomy Module: Vic V. Vernenkar, D.O. Dept. of Surgery St. Barnabas HospitalSyamsuriWahyuNo ratings yet
- Assisting in Endotracheal SuctioningDocument38 pagesAssisting in Endotracheal SuctioningMargarita Limon BalunesNo ratings yet
- AsDocument48 pagesAsCyndi CastañerosNo ratings yet
- IntubationDocument41 pagesIntubationNice YouNo ratings yet
- Tracheostomy Tube CareDocument12 pagesTracheostomy Tube CareydtrgnNo ratings yet
- Endotracheal TubeDocument19 pagesEndotracheal TubeSarvess Muniandy100% (1)
- Tracheostomy: ENT Department DMC & Hospital Ludhiana PunjabDocument46 pagesTracheostomy: ENT Department DMC & Hospital Ludhiana PunjabVikrant MittalNo ratings yet
- Nelec2 Week 8Document8 pagesNelec2 Week 8Michelle MallareNo ratings yet
- TracheostomyDocument31 pagesTracheostomyTonyScaria100% (1)
- 6 Urinary EliminationDocument5 pages6 Urinary EliminationkhautedameNo ratings yet
- SuctioningDocument28 pagesSuctioningRalph Emerson RatonNo ratings yet
- Care of The Patient With A TracheostomyDocument25 pagesCare of The Patient With A TracheostomyBinu JoshvaNo ratings yet
- Abdominal ParacentesisDocument14 pagesAbdominal ParacentesisManisha Thakur100% (1)
- Tracheostomy: by Veronica Robert, MD 4 Moderator DR - SamsonDocument41 pagesTracheostomy: by Veronica Robert, MD 4 Moderator DR - SamsonMacktevin FraterinNo ratings yet
- TracheostomyDocument32 pagesTracheostomydr MohammedNo ratings yet
- Thoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnDocument7 pagesThoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnaparnaNo ratings yet
- Chest Tube InsertionDocument4 pagesChest Tube InsertionreicheNo ratings yet
- Chest Tube InsertionDocument4 pagesChest Tube Insertionreiche100% (1)
- Skills 112 TRACHEOSTOMYDocument52 pagesSkills 112 TRACHEOSTOMYJaynell Ann SabioNo ratings yet
- Chest Drainage Medical ManagementDocument3 pagesChest Drainage Medical ManagementPaul John RutaquioNo ratings yet
- TRACHEOSTOMTPRESENTATIONDocument37 pagesTRACHEOSTOMTPRESENTATIONStar AcademyNo ratings yet
- TracheostomyDocument35 pagesTracheostomyAbdur Raqib100% (1)
- Assisting in Patients Undergoing A ThoracentesisDocument7 pagesAssisting in Patients Undergoing A Thoracentesiscoosa liquors0% (1)
- Chest Tube Placement (Adult)Document8 pagesChest Tube Placement (Adult)Ariane Joyce SalibioNo ratings yet
- 2.tracheostomy CareDocument48 pages2.tracheostomy Carems khanNo ratings yet
- EmpyemaDocument17 pagesEmpyemajismi vallachiraNo ratings yet
- Nursing Care For Clients With Chest TubeDocument21 pagesNursing Care For Clients With Chest TubeKayeNo ratings yet
- ThoracentesisDocument25 pagesThoracentesisroger67% (3)
- TracheostomyDocument4 pagesTracheostomyNapieh Bulalaque PolisticoNo ratings yet
- Abdominal ParacentesisDocument4 pagesAbdominal ParacentesisRashmi C S100% (1)
- Airway Management in Trauma Patients: by Mohammed Taher RagehDocument56 pagesAirway Management in Trauma Patients: by Mohammed Taher RagehMilind KothiyalNo ratings yet
- Care of Clients With Chest TubeDocument55 pagesCare of Clients With Chest TubeMarc Andreo MalalaNo ratings yet
- Are Over 40 Years of Age.: Nonsteroidal Anti-Inflammatory Drugs (Nsaids)Document10 pagesAre Over 40 Years of Age.: Nonsteroidal Anti-Inflammatory Drugs (Nsaids)Anjali NaudiyalNo ratings yet
- Mr. Abhijit Bhoyar Lecturer M. Sc. NursingDocument36 pagesMr. Abhijit Bhoyar Lecturer M. Sc. Nursingseeya rayamajhiNo ratings yet
- TRACHEOSTOMYDocument2 pagesTRACHEOSTOMY3C SAVELLA, Glaiza Marie RNo ratings yet
- Respiratory Care ModalitiesDocument63 pagesRespiratory Care ModalitiesErica Clerigo LandichoNo ratings yet
- Chest Tube Insertion: Prepare By: Amrita:Thapa Roll No. 7Document39 pagesChest Tube Insertion: Prepare By: Amrita:Thapa Roll No. 7sushma shresthaNo ratings yet
- Chest Tube: Ministry of Higher Education and Scientific Research Al-Mustaqbal University College Department of NursingDocument10 pagesChest Tube: Ministry of Higher Education and Scientific Research Al-Mustaqbal University College Department of NursingMr. abbas fahim hamidNo ratings yet
- Skills 112 TRACHEOSTOMYDocument60 pagesSkills 112 TRACHEOSTOMYJemy Tamaño MorongNo ratings yet
- Concept On Surgery: Postoperative CareDocument44 pagesConcept On Surgery: Postoperative CareMelisa ClaireNo ratings yet
- Presentation by Joyce KapenaDocument28 pagesPresentation by Joyce KapenaEvancemwenya123No ratings yet
- Assignment One (1) - LeadershipDocument9 pagesAssignment One (1) - LeadershipEvancemwenya123No ratings yet
- AbortionsDocument40 pagesAbortionsEvancemwenya123No ratings yet
- Rabies - AsmDocument13 pagesRabies - AsmEvancemwenya123No ratings yet
- Inflammation LatestDocument42 pagesInflammation LatestEvancemwenya123No ratings yet
- The Link BetweeDocument1 pageThe Link BetweeEvancemwenya123No ratings yet
- Sarcocystis SpeciesDocument6 pagesSarcocystis Speciessubhash nayakNo ratings yet
- IV Complications Ward ClassDocument28 pagesIV Complications Ward ClassMel Belisario TubeoNo ratings yet
- 11.1 Multiple Choice Part I Questions: Chapter 11 The Cardiovascular SystemDocument33 pages11.1 Multiple Choice Part I Questions: Chapter 11 The Cardiovascular SystemmuryumNo ratings yet
- 15 Fabrication of NoseDocument12 pages15 Fabrication of NoseNirav RathodNo ratings yet
- Ecotv PDFDocument18 pagesEcotv PDFmacarena castilloNo ratings yet
- Drug of ChoiceDocument5 pagesDrug of ChoiceAsmaa RadwanNo ratings yet
- Impact of COVID-19Document11 pagesImpact of COVID-19Aboy HartoNo ratings yet
- The Legend of The Amancay FlowerDocument2 pagesThe Legend of The Amancay FlowerdimicusaNo ratings yet
- INTEGRATED PREBOARD B S2017 Ans KeyDocument12 pagesINTEGRATED PREBOARD B S2017 Ans KeyDiannie SantosNo ratings yet
- CholDocument2 pagesCholAnel RedzicNo ratings yet
- Venous Oxygen Saturation in Critical Illness: Clinical Practice ReviewDocument11 pagesVenous Oxygen Saturation in Critical Illness: Clinical Practice ReviewYudha AldiNo ratings yet
- Radiographic InterpretationDocument46 pagesRadiographic InterpretationSanaFatimaNo ratings yet
- Gastritis The Histology Report M Rugge Et AlDocument12 pagesGastritis The Histology Report M Rugge Et AlsrimardiahkusumaNo ratings yet
- ECPE Cloze Practice TestDocument5 pagesECPE Cloze Practice TestJenny KartNo ratings yet
- Reproductive HealthDocument9 pagesReproductive HealthOfelia GallemaNo ratings yet
- Scientific Writing, July 2012Document1 pageScientific Writing, July 2012Rahmat KurniawanNo ratings yet
- Antidepressants - AMBOSSDocument7 pagesAntidepressants - AMBOSSOpio IsaacNo ratings yet
- The Effects of Temozolomide and Talazoparib in C. Elegans: Ariel Moore Dr. Jill Bargonetti LabDocument11 pagesThe Effects of Temozolomide and Talazoparib in C. Elegans: Ariel Moore Dr. Jill Bargonetti LabAriel MooreNo ratings yet
- Pharmacology Respiratory DrugsDocument2 pagesPharmacology Respiratory DrugsM Youssif Elkady100% (1)
- Statistics Related To Child Health.Document34 pagesStatistics Related To Child Health.charan pooniaNo ratings yet
- Trans Miss Able Disease HandbookDocument195 pagesTrans Miss Able Disease HandbookAhmed NickovNo ratings yet
- Penggunaan DC Shock Dan AED: Edward Kusuma, DR., M.Kes., SP - An., KICDocument21 pagesPenggunaan DC Shock Dan AED: Edward Kusuma, DR., M.Kes., SP - An., KICNdalemSanguDunia-AkhiratNo ratings yet
- Nursing Care of The Postpartum ClientDocument13 pagesNursing Care of The Postpartum ClientLyca Mae AurelioNo ratings yet
- Eggplant: January 2013Document29 pagesEggplant: January 2013Gheța AlexandruNo ratings yet
- Application of Pressure and Release (PAR) Model For Assessing Vulnerability To Industrial Hazards in District Bathinda (Punjab, India)Document5 pagesApplication of Pressure and Release (PAR) Model For Assessing Vulnerability To Industrial Hazards in District Bathinda (Punjab, India)nil julfikarNo ratings yet
- Ab 4-7Document4 pagesAb 4-7api-302561640No ratings yet
- Simple Schematic Diagram of PneumoniaDocument1 pageSimple Schematic Diagram of PneumoniaJason A. AdoyoganNo ratings yet