Professional Documents
Culture Documents
Poster Trauma Tembus Mata
Poster Trauma Tembus Mata
Uploaded by
irawadiputraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Poster Trauma Tembus Mata
Poster Trauma Tembus Mata
Uploaded by
irawadiputraCopyright:
Available Formats
BILATERAL ORBITAL ABSCESS WITH BILATERAL
SEPTIC CAVERNOUS SINUS THROMBOSIS
IRAWADI PUTRA, GETRY SUKMAWATI,
Department of Ophthalmology, Infection and Immunology Subdivision
Faculty of Medicine, Andalas University, M. Djamil Hospital,
Padang, West Sumatera
INTRODUCTION
Bilateral Orbital Abscess with bilateral septic Cavernous Sinus Thrombosis (CST) is a rare yet potentially fatal and
debilitating condition which important to diagnose earlier. With one of the complication of CST is decreased
visual acuity, opthalmoplegia, Optic Atrophy, periorbital sensory alteration secondary to damaged of trigeminal
nerve (CNV), and moreover mortality.
OBJECTIVE
To report a case of a child with bilateral Orbital Abscess with bilateral septic CST due to abscesses on tip of the
nose complications.
CASE REPORT
26 February 2013, an 18 month child was consulted from a Pediatrician. Was previously consulted to an
Otorhinolaryngologist, with findings abscess on tip of the nose, destruction the nasal septum, and Purulent
Meningitis. Culture shown Staphylococcus aureus. Level of consciousness was Glasgow Coma Scale (GCS) 10.
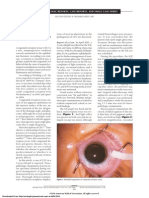
There was bilateral proptosis with severe eyelid swelling, conjunctival chemosis and injection, and normal
anterior segment. CT-Scan revealed bilateral Orbital Abscess and suspect of
Nasal Septum Abscess. We diagnosed him with bilateral Orbital Abscess and
bilateral septic CST. Patient had been previously received treatments of
Ampicillin, Chloramphenicol, and Metronidazole but condition worsen. We
recommended to give eye lubrication, Intravenous Meropenem, Vancomycin,
and Metronidazole immediately for 4 weeks.
In the first week patient had good consciousness, proptosis decreased, able to take objects, and observe using
the left eye. In the four weeks, total regression of the symptoms. Last condition the patient can move and
walking to something desirable. There was good ocular movement, but optic atrophy in right eye.
CONCLUSION
Early diagnosis is very important and Broad-spectrum intravenous antibiotics are the mainstay of treatment to
reduce morbidity and mortality. Optic atrophy is one of CST complication.
KEYWORD
Orbital abscess, CST, ocular movement, Optic atrophy
REFERENCES
Garcia GH, Harris GJ (2000). "Criteria for nonsurgical management of subperiosteal abscess of the orbit: analysis of outcomes". Ophthalmology 107 (8).
Ferguson MP, McNabb AA (1999). "Current treatment and outcome in orbital cellulitis". Australian and New Zealand Journal of Ophthalmology 27 (6): 375379.
Noel LP, Clarke WN, MacDonald N (1990). "Clinical management of orbital cellulitis in children". Canadian Journal of Ophthalmology 25 (1): 1116.
Shapiro E, Wald E, Brozanski B (1982). "Periorbital cellulitis and paranasal sinusitis: a reappraisal". Pediatric Infectious Disease 1 (2).
Westfall CT, Baker AS, Shore JW. Infectious diseases of the orbit. In: Albert DM, Jakobiec FA, eds. Principles and Practice of Ophthalmology. Philadelphia: W.B. Saunders,
2000: 3121-3129.
Gamble RC. Acute inflammations of the orbit in children. Arch Ophthalmol 1933; 10: 483-497.
Donahue SP, Schwartz G. Preseptal and orbital cellulitis in childhood. Ophthalmology 1998; 105: 1902-1906.
Smith TF, ODay D, Wright PF. Clinical implications of preseptal (periorbital) cellulitis in childhood. Pediatrics 1978; 62: 1006-1009.
You might also like
- Antisocial Personality DisorderDocument6 pagesAntisocial Personality DisorderJohn Eldrin Laureano100% (1)
- Asthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDocument26 pagesAsthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDennis MiritiNo ratings yet
- The Pathophysiology and Treatment of GlaucomaDocument11 pagesThe Pathophysiology and Treatment of GlaucomaelisaNo ratings yet
- Heart Dysrhythmias Cheat Sheet PDFDocument5 pagesHeart Dysrhythmias Cheat Sheet PDFpcmundotNo ratings yet
- Diagnosis Approach of Optic Neuritis 2155 9562 1000345Document13 pagesDiagnosis Approach of Optic Neuritis 2155 9562 1000345Juaan AvilaNo ratings yet
- TCM Body Constitution QuestionnaireDocument2 pagesTCM Body Constitution Questionnairefriend717100% (1)
- AAP January 2024 Complete Issue Pediatrics in ReviewDocument75 pagesAAP January 2024 Complete Issue Pediatrics in ReviewhabibfmNo ratings yet
- Clinical and Epidemiological Characterization of KeratoconusDocument12 pagesClinical and Epidemiological Characterization of KeratoconusAndrés MontoyaNo ratings yet
- Bilateral Proptosis in Acute Leukemia: Irawadi Putra, Ardizal RahmanDocument1 pageBilateral Proptosis in Acute Leukemia: Irawadi Putra, Ardizal RahmanirawadiputraNo ratings yet
- The Pathophysiology and Treatment of Glaucoma A ReviewDocument11 pagesThe Pathophysiology and Treatment of Glaucoma A ReviewJacqueline LozzNo ratings yet
- Intracranial Tumors: An Ophthalmic Perspective: DR M Hemanandini, DR P Sumathi, DR P A KochamiDocument3 pagesIntracranial Tumors: An Ophthalmic Perspective: DR M Hemanandini, DR P Sumathi, DR P A Kochamiwolfang2001No ratings yet
- Penatalaksanaan Pasien Dengan Sudut Tertutup Primer - DegianaDocument13 pagesPenatalaksanaan Pasien Dengan Sudut Tertutup Primer - Degianacindy sweeteniaNo ratings yet
- Journal Casereport 1Document5 pagesJournal Casereport 1Arif MohammadNo ratings yet
- 40 Odogu EtalDocument4 pages40 Odogu EtaleditorijmrhsNo ratings yet
- Goldenhar Syndrome An Ophthalmological Perspective: A Case SeriesDocument6 pagesGoldenhar Syndrome An Ophthalmological Perspective: A Case SeriesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Acute Angle-Closure Glaucoma in Emergency Medicine: Background, Pathophysiology, EpidemiologyDocument8 pagesAcute Angle-Closure Glaucoma in Emergency Medicine: Background, Pathophysiology, EpidemiologyAnonymous S0MyRHNo ratings yet
- Abstract Book PVSM2021 FinalDocument374 pagesAbstract Book PVSM2021 FinalnitaNo ratings yet
- Abstract Pachydermoperiostosis EnggresDocument8 pagesAbstract Pachydermoperiostosis EnggresKarina BudijantoNo ratings yet
- Prevalence of Glaucoma in North Costal Andhra PradeshDocument7 pagesPrevalence of Glaucoma in North Costal Andhra PradeshIJAR JOURNALNo ratings yet
- Ocul DiagrameDocument3 pagesOcul Diagrameadriana gutanuNo ratings yet
- Avances Recientes Catarata CongénitaDocument9 pagesAvances Recientes Catarata Congénitaisabellaprie3No ratings yet
- Highlights in Neuro OphthalmologyDocument2 pagesHighlights in Neuro OphthalmologyShruthi VMNo ratings yet
- Visual Findings As Primary Manifestations in Patients With Intracranial TumorsDocument4 pagesVisual Findings As Primary Manifestations in Patients With Intracranial TumorsScoalaAuto AutoSorNo ratings yet
- Mindanao Medical Foundation CollegeDocument4 pagesMindanao Medical Foundation Collegeleidysaves0821No ratings yet
- Five Year PROSE Treatment For Aniridic KojimaOct2016PAPDocument5 pagesFive Year PROSE Treatment For Aniridic KojimaOct2016PAP小島隆司No ratings yet
- Smital Poster New-1-1Document11 pagesSmital Poster New-1-1Smital JaiswalNo ratings yet
- Disgenesis Segmen Anterior Dengan Katarak Kongenital Dan Mikrokornea Diagnosis Banding Dan Tatalaksana - Marsita LitaDocument12 pagesDisgenesis Segmen Anterior Dengan Katarak Kongenital Dan Mikrokornea Diagnosis Banding Dan Tatalaksana - Marsita LitaJoice AngelaNo ratings yet
- Contents OphthaDocument8 pagesContents Ophtharose.fairy96No ratings yet
- Pediatric Optic Neuritis 2016 PDFDocument7 pagesPediatric Optic Neuritis 2016 PDFangelia beanddaNo ratings yet
- Javed and Kashif Split PDF 1674305144401Document4 pagesJaved and Kashif Split PDF 1674305144401criticseyeNo ratings yet
- Jurnal Reading ProptosisDocument5 pagesJurnal Reading ProptosisAnonymous xZrenqNo ratings yet
- A Rare Complication of Combined Oral Contraceptives (Cocs) : Optic NeuritisDocument3 pagesA Rare Complication of Combined Oral Contraceptives (Cocs) : Optic NeuritisGufront MustofaNo ratings yet
- Complications of Pediatric Cataract Surgery and Intraocular Lens ImplantationDocument4 pagesComplications of Pediatric Cataract Surgery and Intraocular Lens ImplantationnurhariNo ratings yet
- Ocular Manifestations in Down's SyndromeDocument4 pagesOcular Manifestations in Down's SyndromeSayoki ghosgNo ratings yet
- Acta Ophthalmologica - 2018 - Rasul - Prevalence of Anterior Polar Cataracts in Children and Risk Factors For AmblyopiaDocument5 pagesActa Ophthalmologica - 2018 - Rasul - Prevalence of Anterior Polar Cataracts in Children and Risk Factors For AmblyopiaMarta GuerreiroNo ratings yet
- Poster Chi2 - Ocular Albinism HKDocument1 pagePoster Chi2 - Ocular Albinism HKyollayusticiaNo ratings yet
- Protrusion OjoDocument16 pagesProtrusion OjoAntonio ReaNo ratings yet
- A Rare Cause of Hearing Loss: Susac SyndromeDocument3 pagesA Rare Cause of Hearing Loss: Susac SyndromeBeny Pratama SidabutarNo ratings yet
- Amblyopia Risk Factors in Newborns With Congenital Nasolacrimal Duct ObstructionDocument5 pagesAmblyopia Risk Factors in Newborns With Congenital Nasolacrimal Duct ObstructionSyaiful UlumNo ratings yet
- Clinicopathologic Reports, Case Reports, and Small Case SeriesDocument3 pagesClinicopathologic Reports, Case Reports, and Small Case SeriesDiaz RandanilNo ratings yet
- IC3D Classification of Corneal Dystrophies Edition.1Document43 pagesIC3D Classification of Corneal Dystrophies Edition.1Selley KenangaNo ratings yet
- Weinreb 2014Document11 pagesWeinreb 2014José Adrian Espejel GuzmánNo ratings yet
- BachmanDocument1 pageBachmanotheasNo ratings yet
- MR 180 EditedDocument6 pagesMR 180 EditedfatmadianaNo ratings yet
- Glaucoma Fisiopatologia Review 14Document11 pagesGlaucoma Fisiopatologia Review 14rbarcellonaNo ratings yet
- Congenital Cataracts: CRYBB3 Beaded Filament Structural Protein 1 (BFSP1) Gap FunctionDocument2 pagesCongenital Cataracts: CRYBB3 Beaded Filament Structural Protein 1 (BFSP1) Gap FunctionKuchai BaruNo ratings yet
- V36N4p293 PDFDocument5 pagesV36N4p293 PDFsiscaNo ratings yet
- UBM in ICEDocument6 pagesUBM in ICELucas HoldereggerNo ratings yet
- Demographic and Clinical Characteristics of Patients With Glaucoma in A Tertiary Eye Facility in GhanaDocument6 pagesDemographic and Clinical Characteristics of Patients With Glaucoma in A Tertiary Eye Facility in GhanaAldhi Putra PradanaNo ratings yet
- Ocular Myasthenia Gravis With Severe Blepharitis ADocument8 pagesOcular Myasthenia Gravis With Severe Blepharitis AGoran TomićNo ratings yet
- 100255-Article Text-1482-2-10-20220311Document6 pages100255-Article Text-1482-2-10-20220311Fachry RahmanNo ratings yet
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocument3 pagesAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNo ratings yet
- High Myopia and Glaucoma Susceptibility The Beijing Eye StudyDocument5 pagesHigh Myopia and Glaucoma Susceptibility The Beijing Eye StudyDickyStevanoZukhriNo ratings yet
- Preseptal and Orbital Cellulitis: A 10-Year Review of Hospitalized PatientsDocument8 pagesPreseptal and Orbital Cellulitis: A 10-Year Review of Hospitalized PatientsApril MitchellNo ratings yet
- Dip Lo PiDocument3 pagesDip Lo PiBahadir DindarNo ratings yet
- Table of Contents - SopDocument2 pagesTable of Contents - SopJust ShareNo ratings yet
- AmblyopiaDocument10 pagesAmblyopiaNoura RoseNo ratings yet
- Differences in Structural Parameters in Patients With Open-Angle Glaucoma, High Myopia and Both Diseases Concurrently. A Pilot StudyDocument14 pagesDifferences in Structural Parameters in Patients With Open-Angle Glaucoma, High Myopia and Both Diseases Concurrently. A Pilot Study钟华No ratings yet
- Conjunctivitis As A Manifestation of Wegener 'S GranulomatosisDocument5 pagesConjunctivitis As A Manifestation of Wegener 'S GranulomatosisAsd DsaNo ratings yet
- Laporan Kasus SACG Dan Katarak Kongenital Pada AniridiaDocument15 pagesLaporan Kasus SACG Dan Katarak Kongenital Pada AniridiaIntan EkarulitaNo ratings yet
- BY: Achin Pant 3 Year MbbsDocument59 pagesBY: Achin Pant 3 Year MbbsMitali MohanNo ratings yet
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDocument4 pagesOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaNo ratings yet
- Goldenhar Syndrome An Unusual Case ReportDocument4 pagesGoldenhar Syndrome An Unusual Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Controversies in Neuro-Ophthalmic Management: An Evidence and Case-Based AppraisalFrom EverandControversies in Neuro-Ophthalmic Management: An Evidence and Case-Based AppraisalAmanda D. HendersonNo ratings yet
- Poster RETINADocument1 pagePoster RETINAirawadiputraNo ratings yet
- PDF StrabismusDocument1 pagePDF StrabismusirawadiputraNo ratings yet
- Schizencephaly - A Case ReportDocument1 pageSchizencephaly - A Case ReportirawadiputraNo ratings yet
- Poster TraumaDocument1 pagePoster TraumairawadiputraNo ratings yet
- Nursing Research Poster-2Document1 pageNursing Research Poster-2api-607314474No ratings yet
- Blood Bank ApplicationDocument3 pagesBlood Bank ApplicationrizwanNo ratings yet
- Treatment of A Lisfranc Injury in A 7-Year-Old BoyDocument5 pagesTreatment of A Lisfranc Injury in A 7-Year-Old BoyDaniel AguilarNo ratings yet
- Psy 1205-1 Intro. To Excetionality Course Outline 2023Document4 pagesPsy 1205-1 Intro. To Excetionality Course Outline 2023Joseph KhaembaNo ratings yet
- (CPG) Philippine Practice Guidelines For The Diagnosis, Staging, and Management of Lung CarcinomaDocument54 pages(CPG) Philippine Practice Guidelines For The Diagnosis, Staging, and Management of Lung CarcinomaJobelleNo ratings yet
- Pasien ReadmisiDocument25 pagesPasien ReadmisialbertaNo ratings yet
- Acute Rheumatic Fever and Rheumatic Heart DiseaseDocument10 pagesAcute Rheumatic Fever and Rheumatic Heart DiseaseBenazir SalsabillahNo ratings yet
- Beauty Care Nail CareDocument12 pagesBeauty Care Nail CareAndreajane CryllecainaNo ratings yet
- Osf Major Case StudyDocument19 pagesOsf Major Case Studyapi-509667406No ratings yet
- M.SC. Medical Surgical Nursing K.G.M.U Institute of Nursing, LucknowDocument35 pagesM.SC. Medical Surgical Nursing K.G.M.U Institute of Nursing, LucknowLeshery SemiraNo ratings yet
- Low-Intensity Intradialytic Exercise Attenuates The Relative Blood Volume Drop Due To Intravascular Volume Loss During HemodiafiltrationDocument8 pagesLow-Intensity Intradialytic Exercise Attenuates The Relative Blood Volume Drop Due To Intravascular Volume Loss During Hemodiafiltrationadri20121989No ratings yet
- CH 47Document18 pagesCH 47Zineb LabiadNo ratings yet
- Aplastic Anemia: Edited: Dr. Dairion Gatot SP - PD-KHOMDocument11 pagesAplastic Anemia: Edited: Dr. Dairion Gatot SP - PD-KHOMrubyniNo ratings yet
- Obsessive Compulsive DisorderDocument8 pagesObsessive Compulsive DisorderPrajna RajnarayananNo ratings yet
- Analysis of Diseases Through DrekkanaDocument222 pagesAnalysis of Diseases Through DrekkanaLahiru Perera100% (1)
- Surg2 Primary Aldosteronism AssignmentDocument8 pagesSurg2 Primary Aldosteronism AssignmentDarain Mohammed MeirNo ratings yet
- What Causes Diarrhea?Document8 pagesWhat Causes Diarrhea?Vadivel KmNo ratings yet
- CNS History TakingDocument4 pagesCNS History TakingDuha B. Salim100% (1)
- Chronic Kidney DiseaseDocument14 pagesChronic Kidney DiseaseHamza RealionNo ratings yet
- MCQ InfectionsDocument10 pagesMCQ Infectionsعلي الكوافيNo ratings yet
- Methamphetamine PowerPointDocument43 pagesMethamphetamine PowerPointCep Oboz Cc'settand NalaktackNo ratings yet
- Case Study: Exercise 2: Triage 1Document26 pagesCase Study: Exercise 2: Triage 1Chandra DewiNo ratings yet
- PQCNC NHPC LS3 Devente 20200310Document8 pagesPQCNC NHPC LS3 Devente 20200310kcochranNo ratings yet
- Case 21Document45 pagesCase 21Mark GironNo ratings yet
- Sepsis and The Frail Elder PPDocument18 pagesSepsis and The Frail Elder PPKelyn BranscomNo ratings yet