Professional Documents
Culture Documents
The Road To High Performance Is Paved With Data: Jeffry G. James
Uploaded by
jaime polancoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Road To High Performance Is Paved With Data: Jeffry G. James
Uploaded by
jaime polancoCopyright:
Available Formats
INVITED COMMENTARY
The Road to High Performance Is Paved With
Data
Jeffry G. James
Data is a necessary component of any organizations Organizational Transformations [1]. This program of cul-
move toward accountability. This commentary describes tural transformation includes 3 main elements: top-down
Wilmington Healths use of high-tech and low-tech data direction setting, bottom-up process improvement, and core
sources in its journey to succeed as an accountable care process redesign. Top-down direction setting is established
organization. This commentary also discusses shortcom- by Wilmington Healths 7-member physician board of direc-
ings in the availability of data and the lack of transparency tors, which is responsible for setting and monitoring the stra-
regarding cost and quality. tegic direction of the organization and for communicating
that direction to the group. Bottom-up process improvement
W
comes from Wilmington Healths use of a Lean management
ilmington Health, PLLCa physician-owned, phy- philosophy, which considers any expenditure of resources
sician-governed, fully integrated multispecialty that does not improve value for patients, employers, or pay-
group practice with more than 160 providersis a good ers as wasteful and subject to elimination. This philosophy
example of health care reform in the trenches. With a focus requires that the people doing the work must be the ones
on the demonstration of quality, Wilmington Health is lead- to improve the work. The third element, core process rede-
ing the way in providing excellent health care, reducing sign, is where the other 2 elements come together. As the
costs, and improving the patient experience. Dichter article states, the goal of core process redesign is
Wilmington Health has provided health care to the to achieve breakthrough improvements in cost, quality, and
residents of Southeastern North Carolina for more than timeliness [1].
40 years and has been instrumental in leading the region Central to all 3 of these elements is the need for data and
toward accountability. It developed the regions first measurement systems. Some of these needs are obvious; for
accountable care organization (ACO) and is a participant in example, the board of directors clearly needs data in order
the Medicare Shared Savings Program (MSSP) of the Centers to make course corrections in the strategic direction of the
for Medicare & Medicaid Services (CMS). Wilmington organization. Likewise, systems cannot be improved if they
Health has demonstrated year-on-year improvement in cannot be measured. The data derived from measurement
nearly every MSSP measure of performanceincluding both helps those who are involved in bottom-up process improve-
cost and qualityand it has performed significantly better ment to understand the waste in the system and to develop
than other ACOs in its MSSP cohort (the 104 other ACOs countermeasures to remove it. These types of data are often
that started the program on January 1, 2013). Wilmington derived from observation, information technology plat-
Health maintains a partnership with Blue Cross and Blue forms, and trial and error within the confines of the system
Shield of North Carolina that includes an ACO agreement being evaluated.
for shared savings, and last year Wilmington Health shared In contrast, the data required for core process redesign
the stage with Kaiser Permanente as a recipient of the differs both from the data used by the board to set the
American Medical Group Associations prestigious Acclaim organizations strategic direction and from the data used
Award, which recognizes health care organizations prog- by Lean teams to drive waste from the system. Much of the
ress in moving toward a delivery model that is safe, effective, data needed for core process redesign does not yet exist,
patient-centered, timely, efficient, and equitable. either at Wilmington Health or in the health care system
Wilmington Healths drive to become a high-performing as a whole. To achieve the ACO ideals of population health
health system has necessitated a comprehensive, multifac-
eted, wholesale organizational transformation. This type of Electronically published May 5, 2014.
transformation has required the development of leadership Address correspondence to Mr. Jeffry G. James, Wilmington Health,
at all levels and has been mobilized through a formal data- 1202 Medical Center Dr, Wilmington, NC 28401 (jjames@wilmington
health.com).
driven program of change. The program of change followed
N C Med J. 2014;75(3):191-194. 2014 by the North Carolina Institute
by Wilmington Health is well described in a 1993 McKinsey of Medicine and The Duke Endowment. All rights reserved.
Quarterly article by Dichter and colleagues, titled Leading 0029-2559/2014/75308
NCMJ vol. 75, no. 3 191
ncmedicaljournal.com
and to become truly accountable for cost, quality, and the practice management with the EMR system, and a popula-
experience of patients, we must identify, implement, mine, tion health tool that has been bolted onto this integrated
and analyze data in a new way. Data must now encompass a system incorporates claims data from payers, provides
much broader representation of the continuum of care than feedback, and facilitates predictive modeling for population
was previously possible in the American health care system, health initiatives.
which has traditionally been extremely fragmented. In addition to these high-tech tools, Wilmington Health
The power of core process redesign comes from bringing uses several low-tech methods to transmit data and drive
cross-functional elements together across the continuum of change. For example, emergency department (ED) pro-
care in a collaborative, data-driven model. The industry is viders now have an easy button they can use to leave a
making great strides in collecting and coalescing data from voicemail message about a patient who needs to be seen,
multiple sources, and innovations in technology are coming and Wilmington Health guarantees that that patient will be
at a rapid rate. Many ACOs have progressed to their second seen the next day. Other low-tech efforts can be seen in the
electronic medical record (EMR) system and no longer view handwritten graphs that line the walls of Wilmington Health,
this system as a mirror image of the paper chart; rather, it is which are used to measure and report daily progress on sev-
now viewed as a data warehouse that is connected to their eral important initiatives.
mission, vision, and strategic plan. EMR data and claims Wilmington Health also uses both internal and external
data can now be linked to provide a clearer picture of cost working groups to analyze data and provide feedback and
and quality across a single health care system. These same comparisons. One of these groups is the internal pilots
data can also be used in predictive modeling that can greatly group, which reviews the organizations many ongoing
enhance an organizations ability to focus resources in the experiments. This group vets the data and adjusts the exper-
areas that are most amenable to improvements in cost and iments before they are rolled out to the entire organization,
quality. to increase the likelihood of early acceptance of the data. To
However, there are still some shortcomings in the tech- obtain external validation of the data process, Wilmington
nology that inhibit collaboration across the continuum of Health has joined the Anceta Collaborative Data Warehouse,
care and prevent true patient engagement. Health informa- which was established by the American Medical Group
tion exchanges are still in their infancy, and they are just Association. Including such notable organizations as the
now starting to develop in a way that will allow the types of Mayo Clinic and the Henry Ford Health System, this collab-
activities mentioned above to be accomplished over a broad orative meets twice yearly to transparently share data, and
range of disparate electronic systems. The good news is that it normalizes these data across its 18 member organizations.
this technology is moving forward quickly, and solutions are Whichever organizations are performing well on any partic-
imminent. Attempts to use data to accomplish the Institute ular measure openly share their best practices, and the col-
for Healthcare Improvements Triple Aim objectives laborative engages in transformative discussions that help
improving the patient experience, improving the health of shape the overall direction and implementation of evidence-
populations, and reducing per-capita costs [2]have been based medicine.
limited not only by technology but also by the unwillingness As a result of implementing and applying both data solu-
of various stakeholders to make cost and quality information tions and cultural transformation, Wilmington Health and
transparent. The lack of transparency in cost data reduces its ACO partners have enjoyed some remarkable improve-
patient engagement by keeping health care consumers in ments. Nearly every core measure of cost and quality has
the dark regarding a significant component of their health improved over the past several years, and Wilmington
care decision making. As economist Harold Miller noted in a Health continues to perform significantly better than other
2012 article published by the Center for Healthcare Quality organizations in its ACO cohort.
and Payment Reform [3], this lack of transparency in cost For example, Figure 1 shows the number of hospital
data also prevents health care providers from developing admissions per 1,000 patient-years in Wilmington Healths
new payment systems. MSSP from 2010 through 2013, as well as the mean for the
Wilmington Health has transformed itself by implement- other ACOs in the MSSP cohort at the end of 2013. Between
ing various systems that are allowing it both to redesign 2010 and 2013, Wilmington Health reduced its number of
its internal systems and to enhance its interactions with admissions per 1,000 patient-years by 19%, and it had 28%
external data environments. As might be expected, several fewer admissions per 1,000 patient-years in 2013 compared
high-tech approaches have been implemented. For example, with the mean for the other ACOs in its cohort.
point-of-service analytical tools allow for real-time notifica- Figure 2 shows the number of hospital readmissions for
tion of gaps in evidence-based care when a patient presents any reason during the first 30 days following discharge, per
to any location in the Wilmington Health system, and an 1,000 admissions, in Wilmington Healths MSSP from 2010
application developed for handheld devices (smartphones) through 2013, as well as the mean for the other ACOs in the
can be used to inform a transition-of-care coordinator about MSSP cohort at the end of 2013. The readmission rate for
a high-risk discharge. In addition, a new system integrates Wilmington Health decreased by 13% between 2010 and
192 NCMJ vol. 75, no. 3
ncmedicaljournal.com
figure 1.
Number of Hospital Admissions per 1,000 Patient-Years in Wilmington Healths Medicare
Shared Savings Program (MSSP), 20102013
Note. The first 4 bars show data for Wilmington Health from 2010 through 2013. The last bar (far right) shows the mean
at the end of 2013 for the 104 other accountable care organizations (ACOs) that joined the MSSP on January 1, 2013.
2013, and Wilmington Healths readmission rate in 2013 was in Wilmington Healths MSSP from 2010 through 2013, as
17% lower than the mean rate for the other ACOs in its MSSP well as the mean for the other ACOs in the MSSP cohort at
cohort. the end of 2013. In 2010, CT use at Wilmington Health was
Figure 3 illustrates how the use of advanced imaging significantly higher than the mean for the other ACOs in the
changed as Wilmington Health transformed its practices; cohort; however, the number of CT scans per 1,000 patient-
specifically, this figure shows the number of computed years in Wilmington Healths MSSP dropped dramatically in
tomography (CT) scans per 1,000 patient-years performed 2011 and continued to decline in 2012 and 2013. The number
figure 2.
Number of Hospital Readmissions for Any Reason During the First 30 Days Following
Discharge, per 1,000 Admissions, in Wilmington Healths Medicare Shared Savings Program
(MSSP), 20102013
Note. The first 4 bars show data for Wilmington Health from 2010 through 2013. The last bar (far right) shows the mean
at the end of 2013 for the 104 other accountable care organizations (ACOs) that joined the MSSP on January 1, 2013.
NCMJ vol. 75, no. 3 193
ncmedicaljournal.com
figure 3.
Number of Computed Tomography (CT) Scans per 1,000 Patient-Years in Wilmington Healths
Medicare Shared Savings Program (MSSP), 20102013
Note. The first 4 bars show data for Wilmington Health from 2010 through 2013. The last bar (far right) shows the mean
at the end of 2013 for the 104 other accountable care organizations (ACOs) that joined the MSSP on January 1, 2013.
of CT scans per 1,000 patient-years was 34% lower in 2013 this journey: First, once physicians trust the information being
than in 2010, and Wilmington Health is now outperforming provided, regardless of the data source, they will do the right
the other ACOs in its cohort on this measure as well. thing even in the absence of financial incentives. Second,
Wilmington Health has shown year-on-year improvement total transparency of performance data can allow an organi-
for the past 4 years in almost every category for which data zation to achieve remarkable results very quickly.
are reported to CMS. One of the most-reviewed measures
Jeffry G. James, CPA, MBA chief executive officer, Wilmington Health,
is the total cost of care per Medicare beneficiary; on this Wilmington, North Carolina.
measure, Wilmington Health has achieved a cost that is 21%
lower than the average for the other ACOs in its MSSP cohort. Acknowledgments
Potential conflicts of interest. J.G.J. is an employee of Wilmington
The challenge of many ACOs across the country is build- Health.
ing a sustainable model in the absence of best practices.
Because there are few model ACOs from which lessons can References
1. Dichter SF, Gagnon C, Alexander A. Leading organizational transforma-
be learned, Wilmington Health is taking a very pragmatic
tions. McKinsey Quarterly. http://www.mckinsey.com/insights/or
approach to the development and deployment of the neces- ganization/leading_organizational_transformations. February 1993.
sary population health data platforms. Thanks in part to this Accessed March 4, 2014.
2. Institute for Healthcare Improvement (IHI). The IHI Triple Aim. IHI
approach, Wilmington Health has been able to accomplish Web site. http://www.ihi.org/engage/initiatives/TripleAim/Pages/
the results described above through normal operations, default.aspx. Accessed March 4, 2014.
having increased its staff by only 3 full-time-equivalent 3. Miller H. Ten Barriers to Healthcare Payment Reform and How To
Overcome Them. Pittsburgh, PA: Center for Healthcare Quality and
positions. Payment Reform; 2012. http://www.chqpr.org/downloads/Overco
Wilmington Health has learned 2 important lessons on mingBarrierstoPaymentReform.pdf. Accessed March 4, 2014.
194 NCMJ vol. 75, no. 3
ncmedicaljournal.com
You might also like
- The Top 6 Examples of Quality Improvement in HealthcareDocument7 pagesThe Top 6 Examples of Quality Improvement in HealthcareDennis Junior ChorumaNo ratings yet
- Advances-Meyer 41 PDFDocument13 pagesAdvances-Meyer 41 PDFNenny Puji LestariNo ratings yet
- Opinion: Healthcare's Next Big HIT?Document2 pagesOpinion: Healthcare's Next Big HIT?Milagros Karina Calapuja QuispeNo ratings yet
- Quality Improvement in Health CareDocument7 pagesQuality Improvement in Health CareFarihaNo ratings yet
- Data-Driven Healthcare Organizations Use Big Data Analytics For Big GainsDocument8 pagesData-Driven Healthcare Organizations Use Big Data Analytics For Big GainsHandsome RobNo ratings yet
- BUS 644 Week 2 Assignment-A.randolphDocument5 pagesBUS 644 Week 2 Assignment-A.randolphAntdrone RandolphNo ratings yet
- Cortana Analytics in Healthcare White PaperDocument16 pagesCortana Analytics in Healthcare White PaperDeyverson Costa100% (1)
- Data Quality Management ModelDocument14 pagesData Quality Management ModelHarvey PepoNo ratings yet
- MIS Model for Process-Oriented HealthcareDocument10 pagesMIS Model for Process-Oriented HealthcareNabeel GondalNo ratings yet
- Policy Suggestions To Obama Transition TeamDocument3 pagesPolicy Suggestions To Obama Transition Teamhuffpostfund100% (1)
- Lot Quality Assurance Sampling Survey in Liberia: Improving Data Use in Decision MakingDocument28 pagesLot Quality Assurance Sampling Survey in Liberia: Improving Data Use in Decision MakingFuturesGroup1No ratings yet
- HW5Document4 pagesHW5Karthik GanesuniNo ratings yet
- Strategi Operasi RUmah SakitDocument4 pagesStrategi Operasi RUmah SakituddindjmNo ratings yet
- Running Head: Elements of An Organizational Model of Health CareDocument7 pagesRunning Head: Elements of An Organizational Model of Health Careklm klmNo ratings yet
- Textbook of Urgent Care Management: Chapter 41, Measuring and Improving Patient SatisfactionFrom EverandTextbook of Urgent Care Management: Chapter 41, Measuring and Improving Patient SatisfactionNo ratings yet
- Data Quality Management ModelDocument11 pagesData Quality Management ModelHanum PutericNo ratings yet
- Qi ProjectDocument14 pagesQi Projectapi-641501601No ratings yet
- Qms Project #1Document16 pagesQms Project #1GirumNo ratings yet
- ch1 PDFDocument18 pagesch1 PDFCliffordBeniNo ratings yet
- Lean Management and U.S. Public Hospital Performance Results From A National SurveyDocument17 pagesLean Management and U.S. Public Hospital Performance Results From A National SurveyArnoldYRPNo ratings yet
- Key Steps To Improve and Measure Clinical Outcomes RyanDocument25 pagesKey Steps To Improve and Measure Clinical Outcomes RyansaphyqNo ratings yet
- Quality Improvement in Healthcare: Posted: 9/12/2007Document3 pagesQuality Improvement in Healthcare: Posted: 9/12/2007Lois YunikeNo ratings yet
- Using ISO 9001 in Healthcare: Applications for Quality Systems, Performance Improvement, Clinical Integration, and AccreditationFrom EverandUsing ISO 9001 in Healthcare: Applications for Quality Systems, Performance Improvement, Clinical Integration, and AccreditationNo ratings yet
- Journal Article Review - Development of A Performance Measurement System at The Mayo ClinicDocument4 pagesJournal Article Review - Development of A Performance Measurement System at The Mayo ClinicMeidi Imanullah50% (2)
- Business Intelligence in Health Care IndustryDocument2 pagesBusiness Intelligence in Health Care IndustrysasiarchieNo ratings yet
- Quality Management ModelDocument11 pagesQuality Management Modelselinasimpson1901No ratings yet
- Journal Managing ChangeDocument15 pagesJournal Managing ChangeNajdi Mat SalehNo ratings yet
- Strategic Management Processes in Healthcare Organizations: Abdulaziz Saddique Pharm.D., CPHQ, CSSMBBDocument10 pagesStrategic Management Processes in Healthcare Organizations: Abdulaziz Saddique Pharm.D., CPHQ, CSSMBBtheresia anggitaNo ratings yet
- Take Home ExamsDocument4 pagesTake Home Examshcny46wsjjNo ratings yet
- Nursing Informatics Week-12-13Document37 pagesNursing Informatics Week-12-13astraeax pandaNo ratings yet
- Ahima Data Quality Management ModelDocument11 pagesAhima Data Quality Management Modelselinasimpson2301No ratings yet
- EDBADocument11 pagesEDBABilal SalamehNo ratings yet
- 2019 LeapfrogToValue PDFDocument57 pages2019 LeapfrogToValue PDFJamey DAVIDSONNo ratings yet
- Six Sigma Approach To Health Carel Quality Management-Revised-1 by Jay Bandyopadhyay and Karen CoppensDocument13 pagesSix Sigma Approach To Health Carel Quality Management-Revised-1 by Jay Bandyopadhyay and Karen Coppensmisslopez89No ratings yet
- Midterm: Healthcare: Students Name Institutional Affiliation Midterm: Healthcare Instructors Name Due DateDocument6 pagesMidterm: Healthcare: Students Name Institutional Affiliation Midterm: Healthcare Instructors Name Due DateG BushNo ratings yet
- Workforce Performance v1Document9 pagesWorkforce Performance v1Ousman BahNo ratings yet
- Health Information TechnologyDocument15 pagesHealth Information Technologybilly momanyiNo ratings yet
- BNS Honours Nursing Quality ImprovementDocument14 pagesBNS Honours Nursing Quality ImprovementyeapgyNo ratings yet
- Hospital Quality ManagementDocument27 pagesHospital Quality ManagementAakansha DhadaseNo ratings yet
- OM AssignmentDocument18 pagesOM AssignmentYoosuf Mohamed IrsathNo ratings yet
- Health InfographicDocument9 pagesHealth InfographicBrazil offshore jobsNo ratings yet
- TQM in HealthcareDocument4 pagesTQM in HealthcareALtit66No ratings yet
- The Use and Impact of Six Sigma in Health 2Document34 pagesThe Use and Impact of Six Sigma in Health 2Georgina SuleNo ratings yet
- PNACF510Document56 pagesPNACF510Jerusalem ShiferawNo ratings yet
- Improving Efficiency and Value in Health Care IntroductionDocument6 pagesImproving Efficiency and Value in Health Care IntroductionCoondog JonesNo ratings yet
- Recommendations Focus Criteria On Value and Achievability - Meaningful Use MeasuresDocument5 pagesRecommendations Focus Criteria On Value and Achievability - Meaningful Use MeasuresDavid HarlowNo ratings yet
- Health Systems Engineering: Building A Better Healthcare Delivery SystemFrom EverandHealth Systems Engineering: Building A Better Healthcare Delivery SystemNo ratings yet
- Licensure, Accreditation, and CertificationDocument62 pagesLicensure, Accreditation, and CertificationSohib KawaiNo ratings yet
- CDSS NotesDocument6 pagesCDSS NotesShreeja SPNo ratings yet
- WP 1Document10 pagesWP 1Khyati B. ShahNo ratings yet
- An Evaluation of The Impact of Health Information Technology and Timely Availability of Visit Diagnoses From Ambulatory Visits On Patient Experience and OutcomesDocument16 pagesAn Evaluation of The Impact of Health Information Technology and Timely Availability of Visit Diagnoses From Ambulatory Visits On Patient Experience and OutcomesDick JohnsonNo ratings yet
- Hospital AccreditationDocument15 pagesHospital AccreditationBishwajitMazumderNo ratings yet
- NURS FPX 6612 Assessment 2 Quality Improvement ProposalDocument5 pagesNURS FPX 6612 Assessment 2 Quality Improvement ProposalEmma WatsonNo ratings yet
- Introduction to Clinical Effectiveness and Audit in HealthcareFrom EverandIntroduction to Clinical Effectiveness and Audit in HealthcareNo ratings yet
- 2020 MUSE Conference - Sessions - March 6 2020Document73 pages2020 MUSE Conference - Sessions - March 6 2020Michele LambertNo ratings yet
- Translating Clinical Guidelines Into Practice Challenges and Opportunities in A Dynamic Health Care EnvironmentDocument5 pagesTranslating Clinical Guidelines Into Practice Challenges and Opportunities in A Dynamic Health Care EnvironmentMorris KiioNo ratings yet
- Data Quality Management ModelDocument8 pagesData Quality Management ModelYoga Bahary TheaNo ratings yet
- WHO MBHSS 2010 Section3 WebDocument16 pagesWHO MBHSS 2010 Section3 WebAn Nisa Akhlaqul KarimahNo ratings yet
- Current Trends in HR: Kim Hester, Ph.D. Professor of Management Arkansas State UniversityDocument54 pagesCurrent Trends in HR: Kim Hester, Ph.D. Professor of Management Arkansas State UniversityAnshul MittalNo ratings yet
- 2015 - Article - 46 n3Document8 pages2015 - Article - 46 n3jaime polancoNo ratings yet
- Jaime Polanco Control8Document4 pagesJaime Polanco Control8jaime polancoNo ratings yet
- Jaime Polanco Control 7Document4 pagesJaime Polanco Control 7jaime polancoNo ratings yet
- Manual Series REM V1.0 2018Document322 pagesManual Series REM V1.0 2018jaime polancoNo ratings yet
- Importancia de la propiedad intelectual y la protección al consumidorDocument6 pagesImportancia de la propiedad intelectual y la protección al consumidorjaime polancoNo ratings yet
- At Issue: Cochrane, Early Intervention, and Mental Health Reform: Analysis, Paralysis, or Evidence-Informed Progress?Document4 pagesAt Issue: Cochrane, Early Intervention, and Mental Health Reform: Analysis, Paralysis, or Evidence-Informed Progress?jaime polancoNo ratings yet
- Bases Coneo 2016Document49 pagesBases Coneo 2016jaime polancoNo ratings yet
- Art15 PDFDocument7 pagesArt15 PDFjaime polancoNo ratings yet
- El Plan AUGE: 2005 Al 2009: Health Care Reform in Chile: 2005 To 2009Document7 pagesEl Plan AUGE: 2005 Al 2009: Health Care Reform in Chile: 2005 To 2009jaime polancoNo ratings yet
- Health Aff 2010 Bitrán 2161 70Document11 pagesHealth Aff 2010 Bitrán 2161 70jaime polancoNo ratings yet
- El Plan AUGE: 2005 Al 2009: Health Care Reform in Chile: 2005 To 2009Document7 pagesEl Plan AUGE: 2005 Al 2009: Health Care Reform in Chile: 2005 To 2009jaime polancoNo ratings yet
- Nihms1308 PDFDocument12 pagesNihms1308 PDFjaime polancoNo ratings yet
- Pone.0114563 n4 PDFDocument15 pagesPone.0114563 n4 PDFjaime polancoNo ratings yet
- Development of Health Equity Indicators in Primary Health Care Organizations Using A Modified DelphiDocument15 pagesDevelopment of Health Equity Indicators in Primary Health Care Organizations Using A Modified Delphijaime polancoNo ratings yet
- Pmed.1001676 n2Document3 pagesPmed.1001676 n2jaime polancoNo ratings yet
- Development of Health Equity Indicators in Primary Health Care Organizations Using A Modified DelphiDocument15 pagesDevelopment of Health Equity Indicators in Primary Health Care Organizations Using A Modified Delphijaime polancoNo ratings yet
- Ten Key PronciplesDocument12 pagesTen Key PronciplesGeorgios MantzavinisNo ratings yet
- The Quest For Equity in Latin America: A Comparative Analysis of The Health Care Reforms in Brazil and ColombiaDocument16 pagesThe Quest For Equity in Latin America: A Comparative Analysis of The Health Care Reforms in Brazil and Colombiajaime polancoNo ratings yet
- Hospital Management Autonomy in Chile: The Challenges For Human Resources in HealthDocument5 pagesHospital Management Autonomy in Chile: The Challenges For Human Resources in Healthjaime polancoNo ratings yet
- Facts, Fallacies, and Politics of Comparative Effectiveness Research: Part I. Basic ConsiderationsDocument32 pagesFacts, Fallacies, and Politics of Comparative Effectiveness Research: Part I. Basic Considerationsjaime polancoNo ratings yet
- The Quest For Equity in Latin America: A Comparative Analysis of The Health Care Reforms in Brazil and ColombiaDocument16 pagesThe Quest For Equity in Latin America: A Comparative Analysis of The Health Care Reforms in Brazil and Colombiajaime polancoNo ratings yet
- Making Sense of Joint Commissioning: Three Discourses of Prevention, Empowerment and EfficiencyDocument10 pagesMaking Sense of Joint Commissioning: Three Discourses of Prevention, Empowerment and Efficiencyjaime polancoNo ratings yet
- Hospital Management Autonomy in Chile: The Challenges For Human Resources in HealthDocument5 pagesHospital Management Autonomy in Chile: The Challenges For Human Resources in Healthjaime polancoNo ratings yet
- Facts, Fallacies, and Politics of Comparative Effectiveness Research: Part I. Basic ConsiderationsDocument32 pagesFacts, Fallacies, and Politics of Comparative Effectiveness Research: Part I. Basic Considerationsjaime polancoNo ratings yet
- Making Sense of Joint Commissioning: Three Discourses of Prevention, Empowerment and EfficiencyDocument10 pagesMaking Sense of Joint Commissioning: Three Discourses of Prevention, Empowerment and Efficiencyjaime polancoNo ratings yet
- Ethical Challenges For Accountable Care Organizations: A Structured ReviewDocument8 pagesEthical Challenges For Accountable Care Organizations: A Structured Reviewjaime polancoNo ratings yet
- Healthcare Reform: Implications For Knowledge Translation in Primary CareDocument11 pagesHealthcare Reform: Implications For Knowledge Translation in Primary Carejaime polancoNo ratings yet
- Base Control 1 Semana 1Document2 pagesBase Control 1 Semana 1jaime polancoNo ratings yet
- Base Control 1 Semana 1Document2 pagesBase Control 1 Semana 1jaime polancoNo ratings yet
- Earth Life Science Module 9 Second Quarter 1Document25 pagesEarth Life Science Module 9 Second Quarter 1Milo CatNo ratings yet
- Casestudy3 Hbo MaDocument2 pagesCasestudy3 Hbo Ma132345usdfghjNo ratings yet
- PrintDocument18 pagesPrintHookandcrookNo ratings yet
- Angelomorphic Christology and The Book of Revelation - Matthias Reinhard HoffmannDocument374 pagesAngelomorphic Christology and The Book of Revelation - Matthias Reinhard HoffmannEusebius325100% (2)
- Fashion Cycle StepsDocument2 pagesFashion Cycle Stepssaranya narenNo ratings yet
- 20ME901 Automobile Engineering Unit 3Document74 pages20ME901 Automobile Engineering Unit 36044 sriramNo ratings yet
- How To Pass in University Arrear Exams?Document26 pagesHow To Pass in University Arrear Exams?arrearexam100% (6)
- The Interview: P F T IDocument14 pagesThe Interview: P F T IkkkkccccNo ratings yet
- HHG4M - Lifespan Development Textbook Lesson 2Document95 pagesHHG4M - Lifespan Development Textbook Lesson 2Lubomira SucheckiNo ratings yet
- Answer Questions Only: Chemical Engineering DeptDocument2 pagesAnswer Questions Only: Chemical Engineering DepthusseinNo ratings yet
- Hisar CFC - Approved DPRDocument126 pagesHisar CFC - Approved DPRSATYAM KUMARNo ratings yet
- Document-SAP EWM For Fashion 1.0: 1.general IntroductionDocument3 pagesDocument-SAP EWM For Fashion 1.0: 1.general IntroductionAnonymous u3PhTjWZRNo ratings yet
- 02 MortarsDocument2 pages02 MortarsTarun kumar DigarseNo ratings yet
- Reversing a String in 8086 Micro Project ReportDocument4 pagesReversing a String in 8086 Micro Project ReportOm IngleNo ratings yet
- DNA Affirmative - MSDI 2015Document146 pagesDNA Affirmative - MSDI 2015Michael TangNo ratings yet
- Understanding 2006 PSAT-NMSQT ScoresDocument8 pagesUnderstanding 2006 PSAT-NMSQT ScorestacobeoNo ratings yet
- Boala Cronica Obstructive: BpocDocument21 pagesBoala Cronica Obstructive: BpocNicoleta IliescuNo ratings yet
- Cell Selection ReselectionDocument35 pagesCell Selection ReselectionThiaguNo ratings yet
- Week 4 Gen EconDocument10 pagesWeek 4 Gen EconGenner RazNo ratings yet
- Environmental Threats Differentiated Reading Comprehension Ver 1Document20 pagesEnvironmental Threats Differentiated Reading Comprehension Ver 1Camila DiasNo ratings yet
- How Do I Prepare For Public Administration For IAS by Myself Without Any Coaching? Which Books Should I Follow?Document3 pagesHow Do I Prepare For Public Administration For IAS by Myself Without Any Coaching? Which Books Should I Follow?saiviswanath0990100% (1)
- 5.a Personal Diet Consultant For Healthy MealDocument5 pages5.a Personal Diet Consultant For Healthy MealKishore SahaNo ratings yet
- Steel Glossary RBC Capital GoodDocument10 pagesSteel Glossary RBC Capital Goodrajesh pal100% (1)
- Kennedy 1945 Bibliography of Indonesian Peoples and CulturesDocument12 pagesKennedy 1945 Bibliography of Indonesian Peoples and CulturesJennifer Williams NourseNo ratings yet
- Medicinal PlantDocument13 pagesMedicinal PlantNeelum iqbalNo ratings yet
- Project Report Software and Web Development Company: WWW - Dparksolutions.inDocument12 pagesProject Report Software and Web Development Company: WWW - Dparksolutions.inRavi Kiran Rajbhure100% (1)
- Advanced Presentation Skills: Creating Effective Presentations with Visuals, Simplicity and ClarityDocument15 pagesAdvanced Presentation Skills: Creating Effective Presentations with Visuals, Simplicity and ClarityGilbert TamayoNo ratings yet
- U-KLEEN Moly Graph MsdsDocument2 pagesU-KLEEN Moly Graph MsdsShivanand MalachapureNo ratings yet
- People v. Lagarto, 326 SCRA 693 (2000)Document43 pagesPeople v. Lagarto, 326 SCRA 693 (2000)GioNo ratings yet
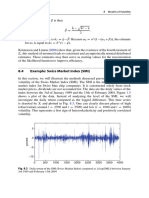
- 8.4 Example: Swiss Market Index (SMI) : 188 8 Models of VolatilityDocument3 pages8.4 Example: Swiss Market Index (SMI) : 188 8 Models of VolatilityNickesh ShahNo ratings yet