Professional Documents
Culture Documents
Chapter 26:: Seborrheic Dermatitis:: Dae Hun Suh: Clinical Features
Uploaded by
myztOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Chapter 26:: Seborrheic Dermatitis:: Dae Hun Suh: Clinical Features
Uploaded by
myztCopyright:
Available Formats
3 Chapter 26 :: Seborrheic Dermatitis
:: Dae Hun Suh
treatment of psoralen plus ultraviolet A (PUVA) ther-
AT-A-GLANCE apy have been reported.6
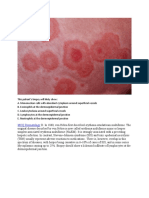
The symptoms of SD are mainly chronic, persistent,
■ Seborrheic dermatitis is a common inflammatory and recurrent. The red, flaking, and greasy lesions
skin disease affecting various age groups. of scalp and face are easily observed, particularly on
■ Erythematous, greasy, scaling patches and plaques nasolabial folds (Fig. 26-2); eyebrows, upper eyelid,
appear on scalp, face, ears, chest, and intertriginous forehead, postauricular areas (Fig. 26-3); external audi-
tory canal and auricle (Fig. 26-4), with generally sym-
Part 3
areas.
■ Severe forms, like generalized erythroderma, rarely metrical distribution. SD can appear in other sites,
occur. such as occiput and neck. When the sternal area on
the chest (Fig. 26-5), upper back (Fig. 26-6), and umbi-
::
■ Etiology is unclear but may be related to abnormal
licus are involved, petaloid or arcuate lesions with
immune mechanism, Malassezia, sebaceous glands,
Dermatitis
fine pink scale can be seen. In contrast, intertriginous
and individual susceptibility.
areas, including inguinal and axillary regions, show
■ Treatment is based on symptomatic control. less scale, making SD easily confusable with intertrigo.
However, variations of these clinical appearances are
common. Scalp involvement is more common in the
male patient, in the patient with long disease duration,
Seborrheic dermatitis (SD) is clinically character- and in the patient with a history of acne.1 The sever-
ized by erythematous, scaly patches on sebaceous ity of SD varies from mild erythema and pruritus to
gland–rich sites, including scalp, face, upper trunk, severe, oily, thick scale with a burning or tingling sen-
and intertriginous areas.1 The affected areas present sation. Some patients with SD also may present with
as various appearances from mild pinkish and some- Pityrosporum folliculitis and blepharitis. Pityrosporum
times greasy scaling to solid adherent crusts. Patients folliculitis typically manifests as a diffuse papulopus-
with this condition complain of discomfort, with tular eruption with peripheral erythema on the trunk
symptoms of itching and burning, and also have some and arises more in immunocompromised patients. Seb-
serious cosmetic problems, leading to psychosocial orrheic blepharitis usually appears as a type of anterior
distress that has a negative impact on their quality of blepharitis, inducing flaking and scaling on the eyelids
life.2 SD arises in all races and ethnic groups and has and creating uncomfortable, irritating problems.
a worldwide distribution, but a higher incidence and Characteristically, ISD has a relatively different
more-severe forms are observed in AIDS patients and feature in contrast with SD in older ages. The non-
individuals with certain neurologic conditions, such pruritic skin eruption generally affects the frontal
as Parkinson disease.3 or vertex areas (or both areas) of the scalp and the
central areas of the face with dry, thick, adherent,
and flaking scale, and may be accompanied by ery-
CLINICAL FEATURES thematous rash on intertriginous folds of the trunk
and extremities (Fig. 26-7). The extensive involve-
ment of the scalp, commonly called “cradle cap,” is
GENERAL FEATURES one of the typical appearances observed in ISD. ISD
normally resolves spontaneously within the first 6 to
SD usually appears as a chronic and relapsing pat- 12 months of life. Extensive and serious conditions
tern in adolescents and young adults when the activ- should be differentiated from immunosuppressed
ity of sebaceous glands increases from hormonal status.
effects, with the incidence increasing in patients
with older than 50 years of age.4 SD can also affect
babies as young as age 2 weeks with peak incidence at
3 months of age, which is called infantile seborrheic der- LEINER DISEASE
matitis (ISD; Fig. 26-1). The overall prevalence of SD
in general population is between 2.35% and 11.30%, The term Leiner disease was first introduced by Carl
depending on the study.5 A male predominance is Leiner in 1908, to describe infants with desquamative
observed in all ages without any racial or regional erythroderma, sparse hair, frequent loose stools, and
predilection. SD is often influenced by a seasonal failure to thrive.7 Later, Miller reported other patients
impact. It becomes more common and severe in the with similar clinical features who had generalized SD.
cold and dry climates, whereas it may be mitigated Miller also found a lack of opsonization by the serum
by sun exposure. However, several cases induced by of the patients.8 Since Miller’s findings it has become
Kang_CH026_p0428-0437.indd 428 06/12/18 3:22 pm
3
Chapter 26 :: Seborrheic Dermatitis
A
Figure 26-1 Cradle cap or infantile seborrheic
dermatitis. (Photo contributed by University of North
Carolina Department of Dermatology. From Tintinalli JE,
et al. Rashes in infants and children. In Tintinalli JE, et al.
Tintinalli’s Emergency Medicine: A Comprehensive Study
Guide. 8th ed. New York, NY: McGraw-Hill Education;
2016:934-952, Fig. 141-30.)
clear that Leiner disease is an umbrella phenotype
rather than a single-disease entity, and a variety of
immunologic defects have been identified.9 Congeni-
tal or acquired deficiencies of C3, C5, and phagocytic
activity results in defective opsonization of yeast and
bacteria. Association of Leiner disease and Netherton
syndrome was also suggested.9 Secondary bacterial
infection can bring death to a Leiner disease patient, so
appropriate treatment, such as IV hydration, tempera-
ture regulation, and antibiotics, is essential. Infusion of
fresh-frozen plasma or whole blood can be beneficial
in supplementing the deficient factors in a hereditary
form of Leiner’s disease.8 The prognosis of Leiner dis-
ease depends on the nature of the underlying immuno-
logic abnormality of the patients.
PITYRIASIS AMIANTACEA
B
Asbestos-like scalp, called pityriasis amiantacea, was Figure 26-2 Seborrheic dermatitis with involvement
first described by Alibert in 1832. Pityriasis amianta- of (A) nasolabial folds, cheeks, eyebrows, and nose in
cea is also called tinea asbestina, tinea amiantacea, white person and (B) nasolabial folds in a person of Asian
keratosis follicularis amiantacea, and porrigo ami- descent.
antacea. Pityriasis amiantacea is an inflammatory
429
Kang_CH026_p0428-0437.indd 429 06/12/18 3:22 pm
3
Figure 26-3 Seborrheic dermatitis of the postauricular area.
Part 3
condition of the scalp that is characterized by large
::
plates of thick, silvering scale firmly adherent to
Dermatitis
both the scalp and hair tufts (Fig. 26-8). This can be
a localized or diffuse condition, and is attributed to
diffuse hyperkeratosis and parakeratosis with follic-
ular keratosis surrounding each hair with a sheath
of corneocytes and debris. It is more common in
females and it may occur at any age, often without
evident causes. Alopecia, which is generally revers-
ible but is sometimes cicatricial, is a common feature
of pityriasis amiantacea.10 Concomitant secondary
bacterial infection, mostly Staphylococcus aureus, may
result in scarring alopecia, so early and appropriate
treatment is necessary. The most frequent skin dis- Figure 26-5 Seborrheic dermatitis of the chest.
eases associated with pityriasis amiantacea are pso-
riasis (35%) and eczematous conditions like SD and
atopic dermatitis (34%). Of pediatric patients with lichen simplex chronicus, superficial fungal, or pyo-
pityriasis amiantacea, lesions in 2% to 15% develop genic infection, or as an adverse effect of molecu-
into typical psoriasis.11 Pityriasis amiantacea may larly targeted therapy such as vemurafenib.12,13 In
also manifest as a complication of lichen planus, these cases, therapy should be directed toward the
underlying etiology.
Figure 26-4 Seborrheic dermatitis of the ear: external
430 canal, concha bowl, and auricle. Figure 26-6 Seborrheic dermatitis of the upper back.
Kang_CH026_p0428-0437.indd 430 06/12/18 3:22 pm
ASSOCIATIONS OF HIV
3
AND AIDS
SD arises in more extensive and refractory patterns in up
to 83% of HIV-seropositive and AIDS patients (Fig. 26-9).4
The initial clinical symptom may appear as a butterfly-
like rash seen in systemic lupus erythematosus. SD is
associated with reduction of T-cell function, and gets
worse as the CD4+ lymphocyte count decreases, making
SD an indicator for evaluating the progression of AIDS.14
ETIOLOGY AND
Chapter 26 :: Seborrheic Dermatitis
PATHOGENESIS
Many studies to uncover the pathogenesis of SD in
adult and adolescent patients have been conducted,
but the etiology has not been clearly identified yet.
Figure 26-7 Seborrheic dermatitis in an infant. Wide-
spread pattern of seborrheic dermatitis with psoriasiform
lesions on the trunk and groin.
B
Figure 26-8 Pityriasis amiantacea. Masses of sticky silvery
scales adhere to the scalp and cause matting of hairs they Figure 26-9 Wide spread unusual distribution pattern
surround. of seborrheic dermatitis in a patient with AIDS. A, Moist
patches on the centrofacial region, beard, and scalp.
B, Moist lesions on the chest. In patients with AIDS, sebor- 431
rheic dermatitis responds poorly to conventional therapy.
Kang_CH026_p0428-0437.indd 431 06/12/18 3:22 pm
3 Multifactorial causes, including several endogenous
and exogenous predisposing factors, are associated MICROBIAL EFFECTS
with SD. The role of sebaceous glands in pathogenesis
of SD is notable considering time and lesional distri- Malassezia, normal flora that inhabits human skin, is
bution of SD. The immunologic status of patients or suggested to be important in SD. This opinion is based
the susceptibility to SD can be an important factor on the evidences that the common lesions of SD are
because SD is much more seen in those with certain related to the distribution of sebaceous glands where
underlying diseases such as AIDS and Parkinson dis- Malassezia preferentially colonizes, and that antifungal
ease. Malassezia may also be one of the causes of SD as medications have therapeutic effects on SD. A decline
antifungal medications are effective. The relationship in the number of Malassezia by use of antifungal agents
of the SD lesions with seasonal fluctuations or sun corresponds with the relief of the symptoms.4 More-
exposure implies that multiple exogenous factors can over, pityriasis versicolor and Pityrosporum folliculitis,
contribute to the development of SD. induced by Malassezia, are commonly accompanied by
SD. However, there is a lack of difference in Malassezia
Part 3
counts between patients with SD and healthy indi-
viduals. In addition, a mycelial form of Malassezia, a
IMMUNE RESPONSE AND pathogenic form observed in pityriasis versicolor, has
not been detected in SD.17 These facts propose a com-
::
INFLAMMATION plex causative role of Malassezia for SD. The prevalence
Dermatitis
and types of the most predominant Malassezia species
The immune component may be important in the found on SD lesions differ among studies, countries,
pathogenesis of SD because SD is much more common or parts of body, but Malassezia globosa and Malassezia
in immunosuppressed patients. The DBA/2 2C TCR restricta are considered to be the most important of
transgenic mouse, which has a defect in expression the 14 Malassezia species identified.4,22 The complete
of CD4+ and CD8+ cells owing to the lack of T-cell genome sequences of M. globosa and M. restricta have
progenitor thymocytes, exhibited SD-like eruptions.15 been determined and these genomes encode lipase and
Several studies have focused on the cellular immu- phospholipase, making the species lipophilic or lipid-
nity and humoral immunity in SD, but there are some dependent.23 The primary role of these enzymes is to
controversies. One study showed a normal CD4+-to- metabolize lipid into fatty acids to produce fungal cell
CD8+ ratio, whereas another study demonstrated a walls responsible for virulence, including invasion and
decreased CD4+-to-CD8+ ratio in 68% of patients.16 A dissemination.24 Not all M. globosa or M. restricta strains
decrease in the number of B cells in 28% of patients were found in SD, implying that there may exist spe-
and a rise of the number of natural killer cells in cific strains capable of causing the disease.25 Also, an
48% of patients were reported. In addition, 60% of increased amount of Malassezia furfur was observed in
patients showed an increase in CD8+ cells and 70% patients with SD versus healthy controls.26 The high
of patients showed a diminished CD4+-to-CD8+ ratio. concentration of M. furfur can disturb protective skin
Also, it was stated that SD patients had an increased barriers and induce inflammation. Malassezin, gener-
production of immunoglobulin (Ig) A and IgG anti- ated by M. furfur or M. restricta, can serve as agonists
bodies in serum.16 However, there was no change to aryl hydrocarbon receptor, which is involved in the
in the total amount of antibodies against Malassezia differentiation of T-helper 17 cells and the mediation of
in SD, suggesting that changes to the antibodies are contact sensitivity.27
not likely linked with Malassezia.17 The alteration of
inflammatory cytokines in patients with SD has been
demonstrated by immunohistochemical studies. The
production of interleukin (IL)-1α, IL-1β, IL-4, IL-12, LIPID AND HOST
tumor necrosis factor-α, and interferon (IFN)-γ was
increased in the lesions compared with the normal SUSCEPTIBILITY FACTORS
skin.18 Significantly increased IL-1RA–to–IL-1α and
IL-1RA–to–IL-8 ratios, as well as overproduction of Several analyses of skin surface lipids in patients
histamine, were also shown to occur in SD when com- with SD or dandruff have shown alterations in those
pared with healthy controls.19 An investigation of gene irrespective of HIV status.28 These findings were not
expression by DNA microarrays in 15 patients with consistent with one another, but they introduced the
dandruff showed the reciprocal expression of induced causative relationship between SD and the composi-
inflammatory genes and repressed lipid metabolism tion of skin surface lipids. Specifically, irritating free
genes compared with nondandruff individuals.20 The fatty acids, such as oleic acid produced by lipase of
expression of induced inflammatory genes was dis- M. globosa, could mediate dandruff-like flaking in the
tinctly observed in uninvolved skin of the patients dandruff-susceptible individuals with SD but not in
as well, indicating the presence of predisposing fac- nonsusceptible individuals.29 Individual susceptibility
tors related to inflammation in patients with SD. Fur- is considered to be associated with a disrupted epi-
thermore, inflammation induced by oxidative stress dermal barrier that allows penetration of the irritating
432 through reactive oxygen species may have a potential metabolites. The process for Malassezia to reach the
role in the pathogenesis of SD.21 aryl hydrocarbon receptor in the granular and spinous
Kang_CH026_p0428-0437.indd 432 06/12/18 3:22 pm
layers also may depend on such defective skin char-
acter. This host susceptibility factor could explain the
factors.6 Multiple drugs can lead to SD-like eruptions,
including griseofulvin, cimetidine, lithium, meth-
3
lack of a positive correlation between the number of yldopa, arsenic, gold, auranofin, aurothioglucose,
Malassezia and the severity of dandruff. buspirone, chlorpromazine, ethionamide, haloperidol,
IFN-α, phenothiazines, stanozolol, thiothixene, pso-
ralen, methoxsalen, and trioxsalen. The SD-like der-
matitis also appears in patients with zinc deficiency
EPIDERMAL (acrodermatitis enteropathica and acrodermatitis
HYPERPROLIFERATION enteropathica–like conditions) or biotin deficiency, but
the skin eruptions do not respond to zinc or biotin sup-
plementation.33 It is noted that the familial form of SD
Increased epidermal turnover in SD, which is also
was reported in an Israeli Jewish family of Moroccan
shown in psoriasis, implicates SD in a disorder of
descent, which was caused by autosomal dominant
hyperproliferation, and Malassezia can be considered
genetic mutation (ZNF750) encoding a zinc finger pro-
as one of the incidental outcomes derived from the
Chapter 26 :: Seborrheic Dermatitis
tein (C2H2).34
phenomenon. SD resembles psoriasis in many aspects,
both clinically and histologically, and it is sometimes
DIAGNOSIS
difficult to differentiate the two diseases even after a
skin biopsy. There are case reports that keratolytics
and antiinflammatory medications were successful in
The diagnosis of SD remains a clinical one, based on
the treatment of the patients with SD whose treatment
SD’s characteristic morphology and patterns. Dermos-
with amphotericin B had failed.30 This alteration of epi-
copy enables the detailed identification of morphologic
dermis may be related with the increased activity of
structures, which is especially helpful in diagnosing
calmodulin and explains the basis of use of cytostatic
SD of the scalp. The typical magnified vascular pat-
medications such as azelaic acid.31
terns observed by dermoscopy are twisted loop, red
dots and globules, and glomerular vessels in scalp pso-
riasis, but arborizing vessels and atypical red vessels in
NEUROTRANSMITTER SD.35 A skin biopsy is not routinely required, but may
be useful when the diagnosis is unclear. The various
ABNORMALITIES histopathologic features can be observed depending
on the different stages of the disease: acute, subacute,
SD expressed in Parkinson disease has been thought and chronic. Acute and subacute SD may exhibit slight
to result from the elevated levels of sebum allowing to moderate spongiotic dermatitis with mild pso-
the proliferation of Malassezia. Bilateral seborrhea riasiform hyperplasia, folliculocentric crust contain-
observed in unilateral parkinsonism suggests the ing scattered neutrophils at the tips of the follicular
changes of sebum levels are presumably triggered opening, orthokeratosis with focal parakeratosis, and
by endocrine effects rather than neurotrophic effects. superficial perivascular lymphohistiocytic infiltration.
It may be associated with an increased circulating Chronic SD shows a more intense pattern of the fore-
α-melanocyte–stimulating hormone in Parkinson dis- going features with minimal spongiosis and markedly
ease.32 Because the severity of SD in Parkinson disease dilated superficial vessels. However, the histopatho-
does not correlate with the sebum excretion rate, the logic picture in chronic cases is sometimes similar
sebum accumulation by facial immobility may play to those of psoriasis, and careful attention should be
a key role. Administration of levodopa can clinically paid to the histopathology reading. HIV-associated
improve the skin symptoms by reducing the sebum SD is histologically distinctive from the ordinary SD,
production or secretion by restoring the production showing very severe patterns such as extensive para-
of melanocyte-stimulating hormone-inhibiting factor. keratosis, leukoexocytosis, necrosis of keratinocytes,
The prevalence of SD is also increased in patients with and superficial perivascular infiltrate of plasma cells
other neurologic disorders, including mood disorder, (Table 26-1).36 Lesion scraping for a potassium hydrox-
Alzheimer disease, syringomyelia, epilepsy, cerebro- ide preparation can be beneficial to confirm the diagno-
vascular infarcts, postencephalitis, mental retardation, sis of accompanied Pityrosporum folliculitis. It should
poliomyelitis, quadriplegia, trigeminal nerve injury, be kept in mind that SD can simultaneously occur
and alcoholism. Indoor lifestyle with less sunlight with other dermatoses. When SD occurs in infants,
exposure and hygiene status of the patients may func- the classic diagnostic criteria suggested by Beare and
tion in this association.4 Rook can be used in diagnosing ISD. It is composed
of early onset (before 6 months of age); erythematous
and scaling rash distributed in the scalp, diaper, or
flexural areas; and the relative absence of pruritus.37
OTHER FACTORS Involvement of the diaper area alone is considered as a
characteristic sign favoring a psoriasiform type of ISD.
Low humidity and cold temperatures worsen SD, espe- Above all, the clinician should remember that there is
cially in the winter and early spring. Facial trauma (eg, not a characteristic pathognomonic feature or labora- 433
scratching) and PUVA therapy also are aggravating tory test to establish the accurate diagnosis of SD.
Kang_CH026_p0428-0437.indd 433 06/12/18 3:22 pm
3 TABLE 26-1 TABLE 26-2
Histopathologic Differences between Classic Site-Specific Differential Diagnosis of Seborrheic
Seborrheic Dermatitis and AIDS-Associated Dermatitis
Seborrheic Dermatitis
Scalpa Psoriasis, atopic dermatitis, impetigo, tinea
CLASSIC SEBORRHEIC AIDS-ASSOCIATED capitisa (mimics dandruff in children)
DERMATITIS SEBORRHEIC DERMATITIS
Face Psoriasis, rosacea, contact dermatitis, impetigo,
Epidermis discoid lupus, sarcoid (petaloid type in African
Limited parakeratosis Widespread parakeratosis Americans), drug-induced photosensitivity
Rare necrotic keratinocytes Many necrotic keratinocytes Ear canal Psoriasis, contact dermatitis
No interface obliteration Focal interface obliteration with
Eyelids Atopic dermatitis, psoriasis, Demodex folliculorum
Prominent spongiosis clusters of lymphocytes
infestation
Sparse spongiosis
Chest, back Pityriasis rosea, tinea versicolor, subacute
Dermis
Part 3
cutaneous lupus, psoriasis vulgaris
Thin-walled vessels Many thick-walled vessels
Groin, buttock Intertrigo (fungal, Candida, erythrasma),
Rare plasma cells Increased plasma cells
glucagonoma, extramammary Paget disease,
No leukocytoclasis Focal leukocytoclasis
::
zinc deficiency
From Soeprono FF, Schinella RA, Cockerell CJ, Comite SL. Seborrheic-like Intertriginous Inverse psoriasis, candidiasis, erythrasma, contact
Dermatitis
dermatitis of acquired immunodeficiency syndrome. A clinicopathologic dermatitis, tinea intertrigo, Langerhans cell
study. J Am Acad Dermatol. 1986;14(2):242-248, with permission. histiocytosis (Letterer-Siwe disease in infants)
Generalizedb Scabies, secondary syphilis, pemphigus foliaceus,
pemphigus erythematosus, Leiner disease
DIFFERENTIAL DIAGNOSIS
(infants), drug eruption
Erythrodermicc Psoriasis, contact dermatitis, pityriasis rubra
pilaris, drug eruption, mycosis fungoides
Several diseases should be considered in the dif-
(Sézary syndrome), lichen planus, chronic
ferential diagnosis of SD (Tables 26-2 and 26-3),
actinic dermatitis, HIV, Hodgkin disease,
especially as ISD is easily confused with atopic der- paraneoplastic syndrome, leukemia cutis
matitis, psoriasis, histiocytosis, and scabies; some-
times it is impossible to distinguish among these
a
Diffuse scalp dermatitis or inflammatory alopecia in children warrants
fungal culture, potassium hydroxide preparation.
diseases in infants younger than 3 months of age. b
Widespread truncal types warrant scabies prep and rapid plasma reagin
Checking family history and pruritus and taking cer-
to rule out syphilis.
tain laboratory tests including serum IgE levels and c
Erythrodermic type should be biopsied.
multiple allergen stimulation tests may give a clue to
whether it is atopic dermatitis or ISD. When the skin
eruption arises solely on the scalp, an involvement
of frontal hair lines is a distinctive feature for scalp
psoriasis.38 Langerhans cell histiocytosis, previously MANAGEMENT
called Letterer-Siwe disease has more generally pur-
Basically, using emollients (eg, mineral oil, vegetable
puric lesions and tends to desquamate on the scalp
oil, or petroleum jelly) can help improve symptoms
and ulcerate on the folds and the mucosal areas.
such as scales. Soft rubbing with a brush or comb aids
Severe itching that includes the palms and soles sug-
removing thick, adherent scales, but aggressive scrap-
gests scabies. Intertrigo, contact dermatitis, neonatal
ing should be avoided because it can induce further
erythroderma, and multiple carboxylase deficiency
inflammation. The main recommendations for the first-
should also be excluded in infants.39
line treatment of SD are topical medications, including
corticosteroids, calcineurin inhibitors, antifungal drugs,
CLINICAL COURSE AND and keratolytics. In the case of topical corticosteroids,
mild-potency formulations are recommended to be
PROGNOSIS used first because of their cutaneous adverse effects
and frequent rebound phenomena. Treatment with
Generally SD in adolescents or adults has a chronic and corticosteroids is highly effective for reducing ery-
recurrent relapsing course. Consequently, the primary thema, scaling, and pruritus rapidly, resulting in total
goal of treatment should be control of symptoms like clearance more often than placebo.40 Topical calcineu-
pruritus, erythema, and scales, rather than cure of dis- rin inhibitors (tacrolimus and pimecrolimus) manifest
ease. Also, patients should be informed that they need good effects on SD by blocking calcineurin, thus pre-
to prepare for a future re-outbreak and avoid aggra- venting both inflammatory cytokines and a signaling
vating factors of SD. However, ISD has a benign, self- pathway in T-lymphocyte cells. No difference between
limited course; ISD spontaneously disappears by 6 to topical calcineurin inhibitors and topical corticoste-
12 months of age. Severe exacerbation with exfoliating roids in total clearance was identified in short-term
434 dermatitis may occur, albeit rarely, but its prognosis is trials.40 There is no risk of telangiectasia and skin atro-
usually favorable. ISD does not progress to adulthood. phy, so topical calcineurin inhibitors are recommended
Kang_CH026_p0428-0437.indd 434 06/12/18 3:22 pm
TABLE 26-3
3
Comparison of Infantile Seborrheic Dermatitis with Differential Diagnoses
INFANTILE SEBORRHEIC
DERMATITIS “NAPKIN” PSORIASIS ATOPIC DERMATITIS LETTERER-SIWE DISEASE
Occurs in the first few weeks to Onset at 3 months Onset within first 2 months of life, Occurs in newborns; other types
3 months most within the first year of Langerhans cell histiocytosis
(LCH) may occur between 1 and
3 years of age
Self-limited, regresses Self-limited Severity decreases with age Fatal if untreated; other variants of
spontaneously LCH have differing prognoses
Vertex scalp most commonly Diaper commonly affected; Face primarily involved Trunk and scalp involved
affected scalp and face may be affected
Chapter 26 :: Seborrheic Dermatitis
Adherent, yellow-brown, Macerated, shiny erythema on Intensely pruritic, erythematous Slightly raised, rose-yellow
greasy scale diaper region papules with excoriation, papules on trunk that may crust
vesicles and serous exudate; and ulcerate
skin appears dry
Face, neck, trunk, and extremities Similarly extensive involvement, Forearms and shins (extensors) Extensive involvement with moist
may be affected with inter- but less scaling on intertriginous often affected, axillae are erythematous plaques and pete-
triginous sites affected (axillae, sites; diaper region primarily spared; diaper area usually chial lesions on intertriginous
groin); isolated diaper lesions affected spared areas; scalp involvement similar
more suggestive of seborrheic to seborrheic dermatitis
dermatitis
for application to the susceptible regions instead of the symptoms of seborrheic otitis externa. In cases
topical corticosteroids. There are no studies comparing refractory to topical treatment, systemic therapies can
the efficacy of tacrolimus with pimecrolimus in SD. be prescribed for uncontrolled multiple widespread
Maintenance therapy with topical calcineurin inhibi- lesions and severe cases. Low doses of systemic glu-
tors may be useful in preventing the relapse or exacer- cocorticoids may be used for a short period. Patients
bation, but their long-term safety has not been verified. should know that SD can be controlled but not eradi-
Based on the presumed etiologic roles of Malassezia, cated. SD patients treated by glucocorticoids should
ketoconazole has been the most heavily investigated be informed of the side effects and rebound flares that
topical agent for SD. Several randomized studies have occur after discontinuation of glucocorticoids. Oral
demonstrated that 1% to 2% ketoconazole significantly antifungals may be tried for severe and refractory
lowers and improves the severity of SD versus pla- cases. Itraconazole, fluconazole, and pramiconazole
cebo, achieving an equal remission rate with cortico- have been used with various regimens.44 For exam-
steroids, with nearly 44% fewer adverse events.41 The ple, itraconazole 200 mg/day for the first 7 days of
use of 1% ciclopirox also improved skin symptoms. In the month for several months is a regimen used to
single studies for evaluating the short-term efficacy of get clinical improvement. The daily administration of
clotrimazole and miconazole, those had almost equiv- isotretinoin 0.1 to 0.5 mg/kg also may be effective in
alent impacts on SD compared with corticosteroids.41 severe cases.
Other topical antifungal agents, such as bifonazole, The basic principle of treatment is the same for
terbinafine, fluconazole, and zinc pyrithione, are also infants. When ISD involves the diaper areas, the use
likely to be useful.4 Dandruff or pityriasis simplex of superabsorbent disposable diapers with frequent
capillitii may be treated by shampoos containing zinc changes prevents the aggravation of the symptoms.45
pyrithione, selenium sulfide, ketoconazole, salicylic Soap and alcohol-containing compounds are not rec-
acid, ciclopirox, and coal tar. Lithium seems to have an ommended in cleaning the diaper lesions. Topical
antiinflammatory role inhibiting the release of arachi- medications having antifungal and antiinflammatory
donic acid and restricting availability of free fatty acids activities are effective choices that have a high clinical
essential for the growth of Malassezia.42 Topical lithium cure rate. A mild-potency steroid, such as 1% hydro-
has shown good results in total clearance both in HIV- cortisone, is preferred but used with caution because
negative patients and in AIDS-associated SD. Topical of its adverse effects. In more refractory cases, a mid-
sulfur, propylene glycol, metronidazole, and benzoyl potency topical steroid, such as 0.1% betamethasone
peroxide wash have also been used. Seborrheic blepha- valerate, may be required but usable only for a short
ritis should be managed by long-term eyelid hygiene time. Keratolytic agents, including salicylic acid and
with warm compresses, followed by proper topical selenium sulfide are dangerous to neonates because
antibiotics and topical corticosteroid to reduce the bac- of the possibility of its percutaneous absorption.
terial load and marked inflammation, respectively.43 Lotion containing 0.025% licochalcone, an extract 435
Aluminum acetate solution can be used to decrease from Glycyrrhiza inflata, was shown to have a similar
Kang_CH026_p0428-0437.indd 435 06/12/18 3:22 pm
3 effect compared to 1% hydrocortisone.46 If second-
ary infection with fungi or bacteria is accompanied,
and microscopy of hair tufts. An Bras Dermatol. 2012;
87(1):142-145.
appropriate systemic drugs should be prescribed. 11. Abdel-Hamid IA, Agha SA, Moustafa YM, et al. Pityriasis
Dietary controls and vitamin supplementation are amiantacea: a clinical and etiopathologic study of 85
not beneficial in ISD. patients. Int J Dermatol. 2003;42(4):260-264.
12. Lacouture ME, Duvic M, Hauschild A, et al. Analysis of
Many researchers have proposed various alterna-
dermatologic events in vemurafenib-treated patients
tive methods to treat SD as well, in preparation for the with melanoma. Oncologist. 2013;18(3):314-322.
antifungal resistance and the adverse effects of exist- 13. Belum VR, Rosen AC, Jaimes N, et al. Clinico-mor-
ing therapies. Homogeneous mixture of biodegradable phological features of BRAF inhibition–induced
elements, such as urea, propylene glycol, and lactic proliferative skin lesions in cancer patients. Cancer.
acid, was shown to be highly effective in treatment of 2015;121(1):60-68.
SD of the scalp.47 Tea tree oil, derived from nature, was 14. Nnoruka EN, Chukwuka JC, Anisuiba B. Correlation of
found to be of benefit in improving severity, pruritus, mucocutaneous manifestations of HIV/AIDS infection
and greasiness in a randomized single-blind study. with CD4 counts and disease progression. Int J Derma-
tol. 2007;46(s2):14-18.
Part 3
The antifungal property of tee tree oil, mostly to M.
15. Oble DA, Collett E, Hsieh M, et al. A novel T cell recep-
furfur, was established in an in vitro study.48 Narrow-
tor transgenic animal model of seborrheic dermatitis-
band ultraviolet B phototherapy was confirmed as an like skin disease. J Invest Dermatol. 2005;124(1):
additional choice and to be both safe and effective in
::
151-159.
an open-label prospective study. Its role in SD may be 16. Dessinioti C, Katsambas A. Seborrheic dermatitis:
Dermatitis
associated with its immunomodulatory and antiin- etiology, risk factors, and treatments: facts and contro-
flammatory function.49 versies. Clin Dermatol. 2013;31(4):343-351.
17. Sandström Falk MH, Tengvall Linder M, Johansson C.
The prevalence of Malassezia yeasts in patients with
atopic dermatitis, seborrhoeic dermatitis and healthy
ACKNOWLEDGMENTS controls. Acta Derm Venereol. 2005;85(1):17-23.
18. Faergemann J, Bergbrant IM, Dohse M, et al. Sebor-
The author acknowledges the contributions of Chris D. rhoeic dermatitis and Pityrosporum (Malassezia) fol-
Collins, MD, FAAD, and Chad Hivnor, MD, the former liculitis: characterization of inflammatory cells and
authors of this chapter, and thanks Jungyoon Moon, mediators in the skin by immunohistochemistry. Br J
MD, for his devoted assistance. Dermatol. 2001;144(3):549-556.
19. Kerr K, Schwartz JR, Filloon T, et al. Scalp stratum
corneum histamine levels: novel sampling method
reveals association with itch resolution in dandruff/
REFERENCES seborrhoeic dermatitis treatment. Acta Derm Venereol.
2011;91(4):404-408.
1. Park SY, Kwon HH, Min S, Yoon JY, et al. Clinical mani- 20. Mills KJ, Hu P, Henry J, et al. Dandruff/seborrhoeic
festation and associated factors of seborrheic derma- dermatitis is characterized by an inflammatory genomic
titis in Korea. Eur J Dermatol. 2016;26(2):173-176. signature and possible immune dysfunction. Br J
2. Szepietowski JC, Reich A, Wesołowska-Szepietowska Dermatol. 2012;166(Suppl2):33-40.
E, et al. Quality of life in patients suffering from sebor- 21. Emre S, Metin A, Demirseren DD, et al. The association
rheic dermatitis: influence of age, gender and educa- of oxidative stress and disease activity in seborrheic
tion level. Mycoses. 2009;52(4):357-363. dermatitis. Arch Dermatol Res. 2012;304(9):683-687.
3. Arsic Arsenijevic VS, Milobratovic D, Barac AM, et al. A 22. Tanaka A, Cho O, Saito M, et al. Molecular charac-
laboratory-based study on patients with Parkinson’s terization of the skin fungal microbiota in patients
disease and seborrheic dermatitis: the presence and with seborrheic dermatitis. J Clin Exp Dermatol Res.
density of Malassezia yeasts, their different species 2014;5(6):239.
and enzymes production. BMC Dermatol. 2014;14:5. 23. Xu J, Saunders CW, Hu P, et al. Dandruff-associated
4. Gupta A, Bluhm R. Seborrheic dermatitis. J Eur Acad Malassezia genomes reveal convergent and divergent
Dermatol Venereol. 2004;18(1):13-26. virulence traits shared with plant and human fungal
5. Misery L, Rahhali N, Duhamel A, et al. Epidemiology pathogens. Proc Natl Acad Sci U S A. 2007;104(47):
of dandruff, scalp pruritus and associated symptoms. 18730-18735.
Acta Derm Venereol. 2013;93(1):80-81. 24. Patino-Uzcategui A, Amado Y, Cepero de Garcia M,
6. Naldi L, Rebora A. Clinical practice. Seborrheic derma- et al. Virulence gene expression in Malassezia spp from
titis. N Engl J Med. 2009;360(4):387-396. individuals with seborrheic dermatitis. J Invest Derma-
7. Dhar S, Banerjee R, Malakar R. Neonatal erythroderma: tol. 2011;131(10):2134-2136.
diagnostic and therapeutic challenges. Indian J Der- 25. Hiruma M, Cho O, Hiruma M, et al. Genotype analy-
matol. 2012;57(6):475-478. ses of human commensal scalp fungi, Malassezia glo-
8. Schwartz RA, Janusz CA, Janniger CK. Seborrheic bosa, and Malassezia restricta on the scalps of patients
dermatitis: an overview. Am Fam Physician. 2006; with dandruff and healthy subjects. Mycopathologia.
74(1):125-130. 2014;177(5-6):263-269.
9. Ong C, O’Toole EA, Ghali L, et al. LEKTI demonstrable 26. Tajima M, Sugita T, Nishikawa A, et al. Molecular analy-
by immunohistochemistry of the skin: a potential sis of Malassezia microflora in seborrheic dermatitis
diagnostic skin test for Netherton syndrome. Br J Der- patients: comparison with other diseases and healthy
matol. 2004;151(6):1253-1257. subjects. J Invest Dermatol. 2008;128(2):345-351.
436 10. Verardino GC, Azulay-Abulafia L, Macedo PM, et al. 27. Gaitanis G, Magiatis P, Stathopoulou K, et al. AhR
Pityriasis amiantacea: clinical-dermatoscopic features ligands, malassezin, and indolo[3,2-b]carbazole are
Kang_CH026_p0428-0437.indd 436 06/12/18 3:22 pm
selectively produced by Malassezia furfur strains iso-
lated from seborrheic dermatitis. J Invest Dermatol.
Pediatric Dermatology. 3rd ed. Oxford, UK: Wiley-Black-
well; 2011:35.1-35.8.
3
2008;128(7):1620-1625. 40. Kastarinen H, Oksanen T, Okokon EO, et al. Topical
28. De Luca C, Valacchi G. Surface lipids as multifunctional anti-inflammatory agents for seborrhoeic dermati-
mediators of skin responses to environmental stimuli. tis of the face or scalp. Cochrane Database Syst Rev.
Mediators Inflamm. 2010;2010:321494. 2011;(5):CD009446.
29. DeAngelis YM, Gemmer CM, Kaczvinsky JR, et al. Three 41. Okokon EO, Verbeek JH, Ruotsalainen JH, et al. Topical
etiologic facets of dandruff and seborrheic dermatitis: antifungals for seborrhoeic dermatitis. Cochrane Data-
Malassezia fungi, sebaceous lipids, and individual sen- base Syst Rev. 2015;(5):CD008138.
sitivity. J Invest Dermatol Proc. 2005;10(3):295-297. 42. Mayser P, Schulz S. Precipitation of free fatty acids
30. Hay RJ. Malassezia, dandruff and seborrhoeic dermati- generated by Malassezia—a possible explanation
tis: an overview. Br J Dermatol. 2011;165(suppl 2):2-8. for the positive effects of lithium succinate in seb-
31. Donovan M, Ambach A, Thomas-Collignon A, et al. orrhoeic dermatitis. J Eur Acad Dermatol Venereol.
Calmodulin-like skin protein level increases in the dif- 2016;30(8):1384-1389.
ferentiated epidermal layers in atopic dermatitis. Exp 43. Pflugfelder SC, Karpecki PM, Perez VL. Treat-
Dermatol. 2013;22(12):836-837. ment of blepharitis: recent clinical trials. Ocul Surf.
Chapter 26 :: Seborrheic Dermatitis
32. Mastrolonardo M, Diaferio A, Logroscino G. Seborrheic 2014;12(4):273-284.
dermatitis, increased sebum excretion, and Parkinson’s 44. Gupta AK, Richardson M, Paquet M. Systematic review
disease: a survey of (im)possible links. Med Hypotheses. of oral treatments for seborrheic dermatitis. J Eur Acad
2003;60(6):907-911. Dermatol Venereol. 2014;28(1):16-26.
33. Trüeb RM. Serum biotin levels in women complaining 45. Tüzün Y, Wolf R, Bağlam S, et al. Diaper (napkin) derma-
of hair loss. Int J Trichology. 2016;8(2):73. titis: a fold (intertriginous) dermatosis. Clin Dermatol.
34. Birnbaum RY, Zvulunov A, Hallel-Halevy D, et al. Sebor- 2015;33(4):477-482.
rhea-like dermatitis with psoriasiform elements caused 46. Wananukul S, Chatproedprai S, Charutragulchai W.
by a mutation in ZNF750, encoding a putative C2H2 Randomized, double-blind, split-side comparison
zinc finger protein. Nat Genet. 2006;38(7):749-751. study of moisturizer containing licochalcone vs. 1%
35. Kim GW, Jung HJ, Ko HC, et al. Dermoscopy can be use- hydrocortisone in the treatment of infantile sebor-
ful in differentiating scalp psoriasis from seborrhoeic rhoeic dermatitis. J Eur Acad Dermatol Venereol. 2012;
dermatitis. Br J Dermatol. 2011;164(3):652-656. 26(7):894-897.
36. Soeprono FF, Schinella RA, Cockerell CJ, et al. 47. Emtestam L, Svensson Å, Rensfeldt K. Treatment of
Seborrheic-like dermatitis of acquired immunodefi- seborrhoeic dermatitis of the scalp with a topical solu-
ciency syndrome. A clinicopathologic study. J Am Acad tion of urea, lactic acid, and propylene glycol (K301):
Dermatol. 1986;14(2):242-248. results of two double-blind, randomised, placebo-
37. Alexopoulos A, Kakourou T, Orfanou I, et al. Retro- controlled studies. Mycoses. 2012;55(5):393-403.
spective analysis of the relationship between infantile 48. Pazyar N, Yaghoobi R, Bagherani N, et al. A review of
seborrheic dermatitis and atopic dermatitis. Pediatr applications of tea tree oil in dermatology. Int J Derma-
Dermatol. 2014;31(2):125-130. tol. 2013;52(7):784-790.
38. Kibar M, Aktan Ş, Bilgin M. Dermoscopic findings in 49. Gambichler T, Breuckmann F, Boms S, et al. Narrow-
scalp psoriasis and seborrheic dermatitis; two new band UVB phototherapy in skin conditions beyond
signs; signet ring vessel and hidden hair. Indian J Der- psoriasis. J Am Acad Dermatol. 2005;52(4):660-670.
matol. 2015;60(1):41.
39. Carlo G, Ramon G. Infantile seborrhoeic dermati-
tis. In: Alan I, Peter H, Albert Y. Harper’s Textbook of
437
Kang_CH026_p0428-0437.indd 437 06/12/18 3:22 pm
You might also like
- Speaker NotesDocument21 pagesSpeaker Noteschinnupepsi4allNo ratings yet
- EpidemiologyDocument86 pagesEpidemiologySainab Moohamoud83% (6)
- Adalsteinsson2020 Inmunologia de La Dermatitis SeborreicaDocument9 pagesAdalsteinsson2020 Inmunologia de La Dermatitis SeborreicaLaura GarciaNo ratings yet
- Optimizing Treatment Approaches in Seborrheic Dermatitis: (Literature Review)Document6 pagesOptimizing Treatment Approaches in Seborrheic Dermatitis: (Literature Review)Andika Anjani AgustinNo ratings yet
- Seborrheic Dermatitis of The Scalp Etiology and TreatmentDocument9 pagesSeborrheic Dermatitis of The Scalp Etiology and TreatmentAndi WahyuniNo ratings yet
- Wanat2015 Cutaneous SarcoidosisDocument18 pagesWanat2015 Cutaneous SarcoidosisJohan ArocaNo ratings yet
- Jurnal Dermatitis Seboroik 3 (Easti)Document8 pagesJurnal Dermatitis Seboroik 3 (Easti)Easti vishiara amdelyNo ratings yet
- Rosacea 2022Document10 pagesRosacea 2022ucarecufinochiettoNo ratings yet
- Localized Scleroderma: Clinical Spectrum and Therapeutic UpdateDocument12 pagesLocalized Scleroderma: Clinical Spectrum and Therapeutic UpdateMati AjaNo ratings yet
- Pics MCQSDocument22 pagesPics MCQStania100% (1)
- Ioana Rosca - SclerodermaDocument6 pagesIoana Rosca - SclerodermaMinnossNo ratings yet
- Scleroderma PDFDocument9 pagesScleroderma PDFAustine OsaweNo ratings yet
- A Familial Case of Scleroderma en Coup de Sabre: Acta Derm Venereol 80Document2 pagesA Familial Case of Scleroderma en Coup de Sabre: Acta Derm Venereol 80Adniana NareswariNo ratings yet
- Lamb 2017Document6 pagesLamb 2017Carolina González RiveraNo ratings yet
- Scleroderma - Oral Manifestations and Treatment ChallengesDocument5 pagesScleroderma - Oral Manifestations and Treatment ChallengesLujainNo ratings yet
- Systemic and Localized Scleroderm11!05!08Document99 pagesSystemic and Localized Scleroderm11!05!08Linux LinuxNo ratings yet
- (Serbian Journal of Dermatology and Venereology) National Guidelines For The Treatment of Atopic DermatitisDocument25 pages(Serbian Journal of Dermatology and Venereology) National Guidelines For The Treatment of Atopic DermatitisFebtri IRnawitaNo ratings yet
- Psoriasis and It's Homoeopathic ManagementDocument3 pagesPsoriasis and It's Homoeopathic ManagementInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 80-Article Text-153-1-10-20161118Document4 pages80-Article Text-153-1-10-20161118Rania SalwanabilaNo ratings yet
- Rosacea SystemicDocument7 pagesRosacea SystemicSalud Los UribeNo ratings yet
- 103.dermatological Manifestations in Diabetes JBADDocument20 pages103.dermatological Manifestations in Diabetes JBADhaytham aliNo ratings yet
- Update On The Classification and Treatment of Localized SclerodermaDocument13 pagesUpdate On The Classification and Treatment of Localized SclerodermaYaraNo ratings yet
- Seborrheic Dermatitis and Dandruff A Comprehensive Review 2015 PDFDocument10 pagesSeborrheic Dermatitis and Dandruff A Comprehensive Review 2015 PDFAnggriyuni Nur Santi100% (1)
- DermatologyDocument23 pagesDermatologyAntung AlangdeoNo ratings yet
- 11 194scleroderma A Case ReportDocument3 pages11 194scleroderma A Case ReportAfiatul MukarromahNo ratings yet
- Herediter and Acquired Ichthyosis VulgarisDocument4 pagesHerediter and Acquired Ichthyosis VulgarisprajnamitaNo ratings yet
- Seborrheic Dermatitis From JurnalDocument6 pagesSeborrheic Dermatitis From JurnalindciwNo ratings yet
- By Dr. Nouran Abou Khedr: Xeroderma PigmentosumDocument6 pagesBy Dr. Nouran Abou Khedr: Xeroderma PigmentosumBahaa ShaabanNo ratings yet
- Red Flags of SclerodermaDocument4 pagesRed Flags of SclerodermanonniNo ratings yet
- Isi RefreshingDocument73 pagesIsi RefreshingKarina Sandra AmiliaNo ratings yet
- Parry Romberg SyndromeDocument7 pagesParry Romberg SyndromeAlexcr199415No ratings yet
- Optimizing Treatment Approaches in Seborrheic DermatitisDocument17 pagesOptimizing Treatment Approaches in Seborrheic DermatitisShinta Restyana WidyaNo ratings yet
- Acrodermatitis Enteropathica - A Case Report: Rashmi Mittal, Sudha R, Murugan S, Adikrishnan, Shobana S, Anandan SDocument3 pagesAcrodermatitis Enteropathica - A Case Report: Rashmi Mittal, Sudha R, Murugan S, Adikrishnan, Shobana S, Anandan SMarcelitaTaliaDuwiriNo ratings yet
- Atopic Dermatitis:: Dr. Francisco Eizayaga, MD PHDDocument18 pagesAtopic Dermatitis:: Dr. Francisco Eizayaga, MD PHDAngelaNo ratings yet
- Patogenie LILI CompletDocument8 pagesPatogenie LILI CompletDianaNo ratings yet
- Jadotte Pityriasis AlbaDocument8 pagesJadotte Pityriasis Albapene asoyNo ratings yet
- Discoid Lupus ErythematosusDocument29 pagesDiscoid Lupus ErythematosusMoralNo ratings yet
- Case Report - PsoriasisDocument7 pagesCase Report - Psoriasisnathalia gabriellaNo ratings yet
- Nelson Adesokan1992Document6 pagesNelson Adesokan1992Yash PatilNo ratings yet
- Dermatological Reviews - 2022 - Honigman - Differential Diagnosis of Melasma and Hyperpigmentation - RemovedDocument4 pagesDermatological Reviews - 2022 - Honigman - Differential Diagnosis of Melasma and Hyperpigmentation - Removedmeisya 102018090No ratings yet
- PatogenezDocument10 pagesPatogenezlloplNo ratings yet
- Gangguan Kulit Pada LansiaDocument28 pagesGangguan Kulit Pada LansianoviNo ratings yet
- Localized 20211127Document5 pagesLocalized 20211127Georgi GugicevNo ratings yet
- Pityriasis RoseaDocument29 pagesPityriasis RoseaAsressieNo ratings yet
- Rosacea: Clinical PracticeDocument11 pagesRosacea: Clinical PracticeLusy Dwitama LeryNo ratings yet
- Seborrheic Dermatitis EmedicineDocument10 pagesSeborrheic Dermatitis EmedicineIkram IkramNo ratings yet
- Pique Ro Casals 2017Document5 pagesPique Ro Casals 2017afrisiammyNo ratings yet
- Fitzpatricks Color Atlas and Synopsis of Clinical Dermatology - Exfoliative Erythroderma SyndromeDocument17 pagesFitzpatricks Color Atlas and Synopsis of Clinical Dermatology - Exfoliative Erythroderma SyndromextraqrkyNo ratings yet
- Sporothrix and M LepraeDocument6 pagesSporothrix and M LepraeVictor Juris AnonuevoNo ratings yet
- DBST Dlja INO Studentov (PDF - Io)Document6 pagesDBST Dlja INO Studentov (PDF - Io)eidNo ratings yet
- Chapter 11 Pityriasis Rosea, Pityriasis Rubra Pilaris, and Other Papulosquamous and Hyperkeratotic DiseasesDocument10 pagesChapter 11 Pityriasis Rosea, Pityriasis Rubra Pilaris, and Other Papulosquamous and Hyperkeratotic DiseasesErika KusumawatiNo ratings yet
- Skin Manifestations of Systemic Disease: Key PointsDocument7 pagesSkin Manifestations of Systemic Disease: Key PointsJUAN DAVID RESTREPO MARINNo ratings yet
- Approach To Reticulate Hyperpigmentation: Clinical Dermatology - Review ArticleDocument8 pagesApproach To Reticulate Hyperpigmentation: Clinical Dermatology - Review ArticledelfiaNo ratings yet
- Pi Is 0190962208009328Document2 pagesPi Is 0190962208009328Nabhya MaheshwariNo ratings yet
- Linear LesionsDocument39 pagesLinear LesionsRegina CzerniawskaNo ratings yet
- Disorders of Abnormal KeratinizationDocument36 pagesDisorders of Abnormal KeratinizationdayangNo ratings yet
- Systemic Sclerosis Shamol Tab VersionDocument52 pagesSystemic Sclerosis Shamol Tab VersionMahadi HassanNo ratings yet
- Skin Pigmentation and Associated Diseases in KsaDocument6 pagesSkin Pigmentation and Associated Diseases in KsaIJAR JOURNALNo ratings yet
- Jurnal Reading DADocument18 pagesJurnal Reading DAWinendy Deo HaryantoNo ratings yet
- Lupus Art. 22Document19 pagesLupus Art. 22Marilena TarcaNo ratings yet
- Akaa 2017 Five Years Retrospective Study On Keloid ManagementDocument8 pagesAkaa 2017 Five Years Retrospective Study On Keloid ManagementmyztNo ratings yet
- Cutaneous ManifestationDocument17 pagesCutaneous ManifestationStella SunurNo ratings yet
- Sidgwick2011 Ecm Molecule in Hs and KeloidDocument12 pagesSidgwick2011 Ecm Molecule in Hs and KeloidmyztNo ratings yet
- Akaa 2017 Five Years Retrospective Study On Keloid ManagementDocument8 pagesAkaa 2017 Five Years Retrospective Study On Keloid ManagementmyztNo ratings yet
- Sidgwick2011 Ecm Molecule in Hs and KeloidDocument12 pagesSidgwick2011 Ecm Molecule in Hs and KeloidmyztNo ratings yet
- Ulrich2010 PDFDocument7 pagesUlrich2010 PDFmyztNo ratings yet
- Ulrich2010 PDFDocument7 pagesUlrich2010 PDFmyztNo ratings yet
- ABC of DermatologyDocument149 pagesABC of DermatologyAndreea Alexandru100% (15)
- Andrews (XP)Document2 pagesAndrews (XP)myztNo ratings yet
- JurnalDocument8 pagesJurnalmyztNo ratings yet
- JurnalDocument3 pagesJurnalmyztNo ratings yet
- Guidelines For The Diagnosis, Treatment and Prevention of LeprosyDocument106 pagesGuidelines For The Diagnosis, Treatment and Prevention of LeprosyMuhammad Randy SyechbubakarNo ratings yet
- Guia Diagnóstico y Tratamiento de La UrticariaDocument22 pagesGuia Diagnóstico y Tratamiento de La UrticariaSMIBA MedicinaNo ratings yet
- Borda2018 PDFDocument48 pagesBorda2018 PDFlarasNo ratings yet
- Skin PreparationDocument12 pagesSkin PreparationRendi Sidiq100% (1)
- Andrade 2016Document12 pagesAndrade 2016myztNo ratings yet
- Problem and Its ScopeDocument49 pagesProblem and Its ScopeAnnaly DelcastilloNo ratings yet
- Tanyut Huidrom - Assignment 4 - HUman PhysiologyDocument1 pageTanyut Huidrom - Assignment 4 - HUman PhysiologyTanyut HuidromNo ratings yet
- EO094 COVIDRecommendationsDocument4 pagesEO094 COVIDRecommendationsTMJ4 News50% (2)
- CBT Introductory WorkbookDocument18 pagesCBT Introductory WorkbookSohel AzamNo ratings yet
- Systemic Manifestations of Skin DisordersDocument41 pagesSystemic Manifestations of Skin DisordersMeighalah ArumugamNo ratings yet
- Tpoic #3 Roles and Responsibilities of MCNDocument11 pagesTpoic #3 Roles and Responsibilities of MCNMary Faith MadayagNo ratings yet
- Blood TransfusionDocument2 pagesBlood TransfusionKomal TomarNo ratings yet
- Karakteristik Penderita Nonarteritic Anterior DENPASAR TAHUN 2014 - 2015Document6 pagesKarakteristik Penderita Nonarteritic Anterior DENPASAR TAHUN 2014 - 2015antrrtna anthraxNo ratings yet
- Extreme Dose!Document99 pagesExtreme Dose!Ogist Dipen100% (1)
- Pub Personality TypeDocument16 pagesPub Personality TypeYessika Adelwin NataliaNo ratings yet
- Tricuspid AtresiaDocument5 pagesTricuspid AtresiaCassyDelaRosaNo ratings yet
- Bm33 11 Co Infectionsandco Morbidities Report enDocument15 pagesBm33 11 Co Infectionsandco Morbidities Report enUtary Rezki SakinahNo ratings yet
- Book 2Document132 pagesBook 2siti fatimahNo ratings yet
- Educ763 Chart AlignmentDocument6 pagesEduc763 Chart Alignmentapi-297105278No ratings yet
- What Is Mental Health?Document8 pagesWhat Is Mental Health?Sonal SahuNo ratings yet
- Florida Nurse-Practice-ActDocument117 pagesFlorida Nurse-Practice-Actapi-251653314No ratings yet
- 9.2 AntisepticsDocument34 pages9.2 AntisepticsSaha DirllahNo ratings yet
- Ovarian Cancers The National Academies Press PDFDocument397 pagesOvarian Cancers The National Academies Press PDFnersitiulfahNo ratings yet
- Episode ListDocument25 pagesEpisode ListhectorNo ratings yet
- Complications of Injectable Fillers, Part 2: Vascular ComplicationsDocument17 pagesComplications of Injectable Fillers, Part 2: Vascular ComplicationsIsabel JiménezNo ratings yet
- Orthokeratology: Orthokeratology (Ortho-K) Is The Fitting of Specially Designed GasDocument4 pagesOrthokeratology: Orthokeratology (Ortho-K) Is The Fitting of Specially Designed GasPUSHPAK DASGUPTANo ratings yet
- NCD BrochureDocument2 pagesNCD BrochureQuỳDướiChânPhậtNo ratings yet
- PedMIDAS - Migraine QuestionnaireDocument2 pagesPedMIDAS - Migraine QuestionnaireSri NathNo ratings yet
- Family Systems: Genograms and Ecomaps: Dr. Mergan Naidoo Principal Family PhysicianDocument42 pagesFamily Systems: Genograms and Ecomaps: Dr. Mergan Naidoo Principal Family PhysicianWendy LucasNo ratings yet
- Science 6 - Q2 - L4 - Parts and Function of Excretory SystemDocument28 pagesScience 6 - Q2 - L4 - Parts and Function of Excretory SystemSonny Matias100% (1)
- Anxiety Disorder Teaching PlanDocument21 pagesAnxiety Disorder Teaching PlanEcaroh Hew Smailliw0% (1)
- Gastric Outlet Obstruction: BY: Tharun Balaji Vinay GautamDocument19 pagesGastric Outlet Obstruction: BY: Tharun Balaji Vinay Gautam7hhdfc8vmwNo ratings yet
- Sirka Health OfficeDocument30 pagesSirka Health OfficeWogen GenaNo ratings yet
- 5-Lump ExaminationDocument4 pages5-Lump Examinationdzidek7No ratings yet