Professional Documents
Culture Documents
BLOOD & LYMPH COMPOSITION AND FUNCTIONS
Uploaded by
Victoria Tan0 ratings0% found this document useful (0 votes)
16 views65 pagesThis document provides an overview of blood and lymph. It describes the components and functions of blood, including the formed elements (erythrocytes, leukocytes, and platelets), plasma, and their clinical significance. Lymph formation and conditions affecting it are also discussed. Key points covered include the composition and roles of red blood cells, white blood cells, platelets, and plasma, as well as hematologic disorders like anemia, thrombocytopenia, and crenation/hemolysis.
Original Description:
Original Title
Micro A, 6 Blood _ Lymph copy
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides an overview of blood and lymph. It describes the components and functions of blood, including the formed elements (erythrocytes, leukocytes, and platelets), plasma, and their clinical significance. Lymph formation and conditions affecting it are also discussed. Key points covered include the composition and roles of red blood cells, white blood cells, platelets, and plasma, as well as hematologic disorders like anemia, thrombocytopenia, and crenation/hemolysis.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
16 views65 pagesBLOOD & LYMPH COMPOSITION AND FUNCTIONS
Uploaded by
Victoria TanThis document provides an overview of blood and lymph. It describes the components and functions of blood, including the formed elements (erythrocytes, leukocytes, and platelets), plasma, and their clinical significance. Lymph formation and conditions affecting it are also discussed. Key points covered include the composition and roles of red blood cells, white blood cells, platelets, and plasma, as well as hematologic disorders like anemia, thrombocytopenia, and crenation/hemolysis.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 65
BLOOD
& LYMPH
Grace Mendoza-Bardelosa, MD, FPDS
Department of Human Structural
Biology
Intended Learning Outcomes
• Describe blood and its composiDon.
• DifferenDate the formed elements of blood.
• Discuss the clinical significance of derangements
in the composiDon of blood.
• Discuss crenaDon and hemolysis.
• Explain the role of formed elements of blood in
common clinical condiDons.
• Discuss lymph formaDon.
• Discuss common clinical condiDons that affect
lymph formaDon and flow.
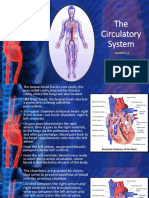
Blood
• Specialized connecDve Dssue
• Cells suspended in PLASMA
• 5 L move unidirecDonally in a closed
circulatory system
Formed Elements
• Erythrocytes
• Leukocytes
• Platelets
Plasma
• Straw-colored, translucent
• Slightly viscous supernatant
• 55% at top of a centrifuged tube
Hematocrit
• UncloTed blood
• Erythrocytes that are sedimented
• 45% in healthy adults
Buffy Coat
• Thin gray-white layer between plasma and
hematocrit
• 1%
• Leukocytes and platelets
ComposiDon of Whole Blood
Serum
• Liquid porDon of cloTed blood
• Contains growth factors and other proteins
released from platelets
• Biologically different from plasma
FuncDons of Blood
• A distribuDng vehicle (O2, CO2, metabolites,
hormones and other substances)
• ParDcipates in heat distribuDon
• RegulaDon of body temperature
• Maintenance of acid-base and osmoDc
balance
ComposiDon of Plasma
• An aqueous soluDon
• pH 7.4
• Dissolved compounds are mostly proteins
• Nutrients
• Respiratory gases
• Nitrogenous waste products
• Hormones
• Inorganic ions aka electrolytes
ComposiDon of Plasma
• Albumin
– Most abundant; maintains osmoDc pressure of blood
• α-Globulins and β-globulins
– Transport lipids, metal ions, iron ions in bloodstream
• γ-Globulins
– Immunoglobulins
• Fibrinogen
– ParDcipates in blood coagulaDon, precursor of fibrin
• Complement proteins
– Important in inflammaDon & destrucDon of organisms
Preparing a Blood Smear
ERYTHROCYTES
Erythrocytes
• Non nucleated
• Completely filled with hemoglobin
• Biconcave discs – provides large surface-to-
volume raDo, facilitates gas exchange
• 7.5 μm diameter
• 2.6 μm thick at rim
• 0.75 μm thick at center
Normal Erythrocytes
Erythrocytes
• NV females: 3.9 to 5.5 million/ μL
• NV males: 4.1 to 6.0 million/ μL
• Flexible
• Cuplike shape
• Rouleaux: RBC’s adhere to one another
loosely in stacks
Erythrocytes
• Plasmalemma, best known membrane
• 40% lipid, 10% carbohydrate, 50% protein
• Mostly integral membrane proteins
– Ion channels
– Band 3 protein (anion transporter)
– Glycophorin A
• Glycosylated extracellular domains include anDgenic
sites
• Basis for ABO blood typing system
Erythrocytes
• Peripheral proteins
• Spectrin: forms lakce with acDn filaments
• Ankyrin: anchors the lakce to glycophorins
and band 3 proteins
• Stabilizes the membrane
• Maintains cell shape
• Provides cell elasDcity
Erythrocytes
• Lacks all organelles
• Filled with hemoglobin
• Tetrameric O2 carrying protein
• Oxyhemoglobin (O2)
• Carbaminohemoglobin (CO2)
• Hemoglobin + CO
Erythrocytes
• No nucleus and organelles
• No mitochondria
• Rely on anaerobic glycolysis for minimal
energy needs
• Cannot replace defecDve proteins
• 120 days normal life span
• Removed in circulaDon by macrophages
Anemia
• CondiDon where concentraDon of RBC’s are
below the normal range
• S/Sx: lethargy, shortness of breath, faDgue,
skin pallor, cardiac palpitaDons
• Causes:
– Insufficient RBC producDon
– Blood loss
Erythrocytosis
• Polycythemia
• Increased concentraDon of RBC’s
• Physiologic
– Areas with high alDtudes
– O2 tension is low
– Increase in hematocrit
Sickle Cell Erythrocyte
LEUKOCYTES
Leukocytes
• Granulocytes
• Azurophilic granules or lysosomes
• Specific granules
– Bind neutral, basic, or acidic stains
– Have specific funcDons
• Polymorphic nuclei
• Neutrophils, Eosinophils, & Basophils
Leukocytes
• Agranulocytes
• No specific granules
• Azurophillic granules
• Nuclei indented but not lobulated
• Lymphocytes & Monocytes
Leukocytes
• Defense against invading microorganisms
• Repair of injured Dssues
Normal Leukocytes
Neutrophils
• 12-15 μm
• 54% to 62%
• Nuclei: 2 to 5 lobes linked by thin nuclear
extensions
• Females: drumsDck-like appendage
• InacDve and spherical when inacDve
• Amoeboid during diapedesis
Neutrophils
• AcDve phagocytes of bacteria
• Usually first to arrive at sites of infecDon
• Azurophilic primary granules
• Role in killing and degrading engulfed
microorganisms
– Myeloperoxidase
– Lysozyme
– Defensins
Neutrophils
• Myeloperoxidase
– Generates hypochlorite & other agents toxic to
bacteria
• Lysozyme
– Degrades components of bacterial cell wall
• Defensins
– Cysteine-rich proteins that bind and disrupt cell
membranes of bacteria
Neutrophils
• Specific secondary granules
• SecreDon of ECM-degrading enzymes such as
collagenases
• Delivery of addiDonal bactericidal proteins to
the phagolysosomes
• InserDon of new cell membrane components
Neutrophils
• Role in inflammatory response
• Restore normal Dssue microenvironment
• First line of defense against invasion by
pathogenic bacteria
• Short-lived
• Half-life of 6 to 8 hours
• Life span of 4 days in connecDve Dssue
Neutrophils
Eosinophils
• 1% to 3%
• Bilobed nucleus
• Abundance of large acidiphilic specific
granules stain pink or red
Eosinophils
• Major basic protein (MBP)
• 50% of total granule protein
• Kill parasiDc worms and helminths
• Modulate inflammatory responses triggered
by allergies
• Remove anDgen-anDbody complexes from
intersDDal fluid by phagocytosis
• IntesDnal lining, lung Dssues
Eosinophils
Basophils
• 12 to 15 μm
• Less than 1%
• Nucleus is divided into two irregular lobes
• Large specific granules stain purple
Basophils
• Heparin and sulfated GAG’s
– Histamine
– Platelet acDvaDng factor
– Eosinophil chemotacDc factor
– Phospholipase A
• Supplement funcDon of mast cells
– Contain heparin and histamine
– Receptors for IgE
– Secrete components in response to certain Ag’s and
allergens
Basophils
Lymphocytes
• B lymphocytes
• T lymphocytes
– Helper (CD4+)
– Cytotoxic (CD8+)
• Natural killer cells (NK cells)
• Immune defense against invading
microorganisms, parasites, abnormal cells
Lymphocytes
• Small – similar to RBC’s
– Spherical nuclei
– Highly condensed chromaDn
– Scanty cytoplasm
• Large (acDvated lymphocytes or NK cells)
– 9 to 18 um
– Slightly indented nuclei
– More cytoplasm
– Few azurophilic granules
Lymphocytes
Monocytes
• Precursor cells of macrophages, osteoclasts,
microglia and other cells of the mononuclear
phagocyte system
• AnDgen-presenDng cells
• Immune defense
Monocytes
• 12 to 20 μm
• Nucleus: indented or C-shaped
• Cytoplasm: basophilic
• Azurophilic granules: bluish-gray distributed
through the cytoplasm
Monocytes
Platelets
• Thrombocytes
• Non-nucleated cell fragments
• 2 to 4 μm
• From megakaryocytes
• Promote blood clokng
• Repair of minor tears or leaks in small BV’s
Platelets
• 150,000 to 400,000/uL (mm3)
• Life span of 10 days
• Clumps
• Discoid
• Hyalomere
– Lightly stained peripheral zone
• Granulomere
– Dark-staining central zone containing granules
Thrombocytes
Thrombocytopenia
• Lack of circulaDng platelets
• Leads to a bleeding tendency
Thrombocytosis
• Excess of platelets
• Leads to risk of inappropriate blood clokng
(thrombosis)
Normal Plasma
• Normal plasma is said to be isoosmoDc or
isotonic.
• Isotonic soluDons maybe prepared for the
study of corpuscles outside the body
• 0.85% soluDon of sodium chloride is
approximately isotonic for the blood
CrenaDon
• “Scalloped” or “notched”
• The formaDon of an abnormal notching
around the edge of an erythrocyte
• Shrinkage aser suspension in a hypertonic
soluDon
• Echinocytes or burr cells
CrenaDon
• Hypertonic soluDon is added to blood
• Erythrocytes become shrunken and irregular
in surface contour
• Cockle-Burr appearance
• The process is called crenaOon
Hemolysis
• Breakage of the RBC’s membrane
• Release of hemoglobin and other internal
components into surrounding fluid
• Pink to red Dnge in serum
• May compromise laboratory’s test parameters
• Hypotonic soluDon: RBC’s become spheroidal
• Swelling of cells
Hemolysis
• Two causes
• In vivo: Pathological causes
– Autoimmune hemolyDc anemia
– Transfusion reacDon
• In vitro: Improper specimen collecDon,
processing, transport
LYMPH
Lymph
• Excess intersDDal fluid from Dssue spaces
• Does not contain RBC’s
• Lymphocytes may be present
• Rich in proteins
Lymph
• Greater hydrostaDc pressure of blood at
arterial ends of capillaries
• Opposite at venous ends
• OsmoDc pressure of plasma
• Increased rate of Dssue fluid formaDon at
arterial end
• Lesser reuptake of fluid at venous end
• Excess fluid
Lymph
• Chylothorax
• A type of pleural effusion
• LymphaDc fluid accumulaDng in the pleural
cavity
• Causes
– Lymphoma
– Trauma
Lymph
• Lymphoma
• NeoplasDc proliferaDon of lymphocytes
• Failure of lymphocytes to undergo apoptosis
• All are considered malignant
Lymph
• Filariasis
• A parasiDc disease caused by microscopic,
thread-like worms
• Adult worms only live in human lymphaDc
system
• Spread from person to person by mosquitoes
THANK YOU
You might also like
- Encyclopedia of Molecular Pharmacology 3rd Ed 2021Document1,625 pagesEncyclopedia of Molecular Pharmacology 3rd Ed 2021Josemar Sena BatistaNo ratings yet
- Characteristics and Functions of Blood ComponentsDocument51 pagesCharacteristics and Functions of Blood ComponentssamayaNo ratings yet
- Pathology Concept BookDocument481 pagesPathology Concept Bookram dheer100% (2)
- RBC and WBC MorphologyDocument165 pagesRBC and WBC MorphologyZeeshan Yousuf100% (1)
- BLOOD CELL PRODUCTION AND FUNCTIONSDocument59 pagesBLOOD CELL PRODUCTION AND FUNCTIONSMarieana Gomez100% (1)
- Blood and Its ComponentsDocument22 pagesBlood and Its ComponentsSudhir Singh100% (1)
- The Blood: Rubie Maranan-Causaren, MSDocument73 pagesThe Blood: Rubie Maranan-Causaren, MSlady ann jimenez100% (3)
- Introduction To Immunology, Science of ImmunityDocument80 pagesIntroduction To Immunology, Science of Immunitytummalapalli venkateswara raoNo ratings yet
- 1 BloodDocument77 pages1 BloodVisaNathan100% (1)
- Biology Chapter 1 Cell Notes.Document6 pagesBiology Chapter 1 Cell Notes.Jyoti AmbwaniNo ratings yet
- Red Blood Cells, Functions, Diseases A Simple Guide To The Condition, Diagnosis, Treatment, And Related ConditionsFrom EverandRed Blood Cells, Functions, Diseases A Simple Guide To The Condition, Diagnosis, Treatment, And Related ConditionsNo ratings yet
- 1-Blood Composition and FunctionDocument43 pages1-Blood Composition and FunctionKaleem Mohammad100% (2)
- Blood Cells: By: DR - Sutrisno Darmosumarto, Sp.A Histology & Cell Biology Department Gadjah Mada UniversityDocument25 pagesBlood Cells: By: DR - Sutrisno Darmosumarto, Sp.A Histology & Cell Biology Department Gadjah Mada UniversityDexa RivandiNo ratings yet
- Understanding the Composition and Functions of BloodDocument30 pagesUnderstanding the Composition and Functions of BloodPriyanka RameshNo ratings yet
- BloodDocument49 pagesBloodDale TelgenhoffNo ratings yet
- Hematologi 1Document57 pagesHematologi 1Till JannahNo ratings yet
- Blood Physical PropertiesDocument38 pagesBlood Physical PropertiesYvonne Kath SmitchNo ratings yet
- Blood PropertiesDocument38 pagesBlood PropertiesShubham BhandareNo ratings yet
- Organisation of BloodDocument32 pagesOrganisation of BloodVic JuniorNo ratings yet
- Anatomy and Physiology of BLOOD: Preet KaurDocument37 pagesAnatomy and Physiology of BLOOD: Preet KaurPreet KaurNo ratings yet
- Blood: Group 1Document25 pagesBlood: Group 1Arian May MarcosNo ratings yet
- CVS BloodDocument39 pagesCVS BloodMohan GuptaNo ratings yet
- Blood - Hemopoietic Tissue, VNADocument61 pagesBlood - Hemopoietic Tissue, VNAvaryvira6677No ratings yet
- Lecture 9 CVSDocument118 pagesLecture 9 CVSMuhammad Abbas WaliNo ratings yet
- Histology of Blood CellsDocument80 pagesHistology of Blood CellsKamal AhmedNo ratings yet
- Blood Cell Formation and Blood CellsDocument49 pagesBlood Cell Formation and Blood Cellsxcx88igNo ratings yet
- Introduction To HematologyDocument61 pagesIntroduction To HematologyThis is PonyNo ratings yet
- Ch18 BloodDocument31 pagesCh18 BloodNoah DominoNo ratings yet
- Cardiovascular System - BloodDocument67 pagesCardiovascular System - BloodCla NuvalNo ratings yet
- Blood Circulation OverviewDocument24 pagesBlood Circulation OverviewWenzy Razzie cruzNo ratings yet
- Darah Dan HematopoisisDocument81 pagesDarah Dan HematopoisisSheldy PrawibowoNo ratings yet
- BloodDocument76 pagesBloodKerby Dela Fuente Alison100% (1)
- University of Guyana Health Sciences FacultyDocument44 pagesUniversity of Guyana Health Sciences FacultySatrohan SurjnarineNo ratings yet
- Blood Physio Formed Tech 2024Document80 pagesBlood Physio Formed Tech 2024Joshua BucioNo ratings yet
- Anatomy Chapter 19 Blood 2Document60 pagesAnatomy Chapter 19 Blood 2Eli RaglandNo ratings yet
- Body Fluids and Their Circulation 1Document96 pagesBody Fluids and Their Circulation 1sanmathiNo ratings yet
- Connective Tissue III BloodDocument18 pagesConnective Tissue III Bloodmanoelsha3No ratings yet
- Anaphy - Cardiovascular System - BloodDocument3 pagesAnaphy - Cardiovascular System - BloodAileen DemaguilaNo ratings yet
- Blood Components: Plasma, Buffy Coat, Formed ElementsDocument19 pagesBlood Components: Plasma, Buffy Coat, Formed ElementsMiljun CatacataNo ratings yet
- Week8 BloodDocument49 pagesWeek8 BloodmensioNo ratings yet
- NATSCI Pre Final Lec Notes BLOODDocument5 pagesNATSCI Pre Final Lec Notes BLOODNIKKANo ratings yet
- Haem Introduction-Final - SDocument14 pagesHaem Introduction-Final - SSarahNo ratings yet
- Composition and Functions of Blood CellsDocument22 pagesComposition and Functions of Blood CellsUmar ManshadNo ratings yet
- Blood Functions and CompositionDocument75 pagesBlood Functions and CompositionTina MinottNo ratings yet
- Cardiovascular Physiology 4Document75 pagesCardiovascular Physiology 4maxmus4No ratings yet
- The University of Zambia School of Medicine Department of Physiological SciencesDocument64 pagesThe University of Zambia School of Medicine Department of Physiological Sciencesblaze zimbaNo ratings yet
- Hematology Review: by Felicia Magee Tardy, M.S., MT (Ascp)Document52 pagesHematology Review: by Felicia Magee Tardy, M.S., MT (Ascp)Reen LeenNo ratings yet
- Introduction to Blood Composition and HaemopoiesisDocument119 pagesIntroduction to Blood Composition and HaemopoiesisShamsuddeen UsmanNo ratings yet
- Blood and ITS Component S: DR - Yadwinder Virk Senior Resident (Pathology)Document47 pagesBlood and ITS Component S: DR - Yadwinder Virk Senior Resident (Pathology)AaQib BhatNo ratings yet
- Blood and Lymph Nodes: P. Manyau School of Pharmacy University of ZimbabweDocument18 pagesBlood and Lymph Nodes: P. Manyau School of Pharmacy University of Zimbabwebrian mgabiNo ratings yet
- Thyroid Gland - Microscopic AnatomyDocument28 pagesThyroid Gland - Microscopic AnatomySafe BoxNo ratings yet
- Removal Reviewer: Gen. HistoDocument31 pagesRemoval Reviewer: Gen. HistoNeil DolendoNo ratings yet
- Pure Biology CHP 8 Transport in HumansDocument94 pagesPure Biology CHP 8 Transport in Humanshamsterish87% (15)
- IlovemymomDocument149 pagesIlovemymomREYSYMAE CABRALNo ratings yet
- Blood and Its FunctionsDocument47 pagesBlood and Its FunctionsMatende husseinNo ratings yet
- Tarazawi MorphologyDocument49 pagesTarazawi MorphologyHussien HamidNo ratings yet
- ANATOMY AND PHYSIOLOGY OF BLOODDocument11 pagesANATOMY AND PHYSIOLOGY OF BLOODArah Lyn ApiagNo ratings yet
- Functions and Properties of Blood - Plasma - Blood Cell Production - Erythrocytes - Blood Types - Leukocytes - Hemostasis (Stoppage of Bleeding)Document47 pagesFunctions and Properties of Blood - Plasma - Blood Cell Production - Erythrocytes - Blood Types - Leukocytes - Hemostasis (Stoppage of Bleeding)vanderphysNo ratings yet
- HemopoiesisDocument53 pagesHemopoiesisnav_malhiNo ratings yet
- The essential components and functions of human bloodDocument51 pagesThe essential components and functions of human bloodAlvinTercianoVitugNo ratings yet
- Hematology Lecture 1 - Blood and Its Components - BackupDocument51 pagesHematology Lecture 1 - Blood and Its Components - BackupHaizickNo ratings yet
- Module 9 - 4 - Circulatory SystemDocument34 pagesModule 9 - 4 - Circulatory SystemThea Shaine B. SILARDENo ratings yet
- Microscopic HSB ReviewDocument92 pagesMicroscopic HSB ReviewVictoria Tan100% (1)
- Micro Finals Pracs ReviewDocument111 pagesMicro Finals Pracs ReviewVictoria TanNo ratings yet
- Micro A - 3.1 - Histology of GIT Part 1 PDFDocument5 pagesMicro A - 3.1 - Histology of GIT Part 1 PDFVictoria TanNo ratings yet
- MICRO A - 2.8 - Dev - T of Respiratory SystemDocument4 pagesMICRO A - 2.8 - Dev - T of Respiratory SystemVictoria TanNo ratings yet
- Micro A, Repiratory Part IIDocument44 pagesMicro A, Repiratory Part IIVictoria TanNo ratings yet
- 2.3 Lymphatics PPT (Dr. Mattheus)Document39 pages2.3 Lymphatics PPT (Dr. Mattheus)12345karlos ParrasNo ratings yet
- Micro A, 7 Heart - BV'sDocument76 pagesMicro A, 7 Heart - BV'sVictoria TanNo ratings yet
- Micro A, 10 Stomach, Small - Large Intestines, MicroDocument71 pagesMicro A, 10 Stomach, Small - Large Intestines, MicroVictoria TanNo ratings yet
- Kidneys: Anatomy and FunctionsDocument51 pagesKidneys: Anatomy and FunctionsVictoria TanNo ratings yet
- 5 Hpe Axis Sum21 StudentDocument7 pages5 Hpe Axis Sum21 StudentRAQUEL WINECKNo ratings yet
- 26 Year Male 61620503543: Patient NameDocument2 pages26 Year Male 61620503543: Patient NameMoataz NazeemNo ratings yet
- Eukaryotic TranslationDocument24 pagesEukaryotic Translationtariqul13017No ratings yet
- Lactobacilus Paper FullDocument41 pagesLactobacilus Paper FullCarlos DNo ratings yet
- Proteins Ppt. (By CDM)Document31 pagesProteins Ppt. (By CDM)Aldren MarianoNo ratings yet
- Glencoe Biology Textbook Glossary 2010Document84 pagesGlencoe Biology Textbook Glossary 2010Bradford McCallNo ratings yet
- Review: Translational Regulation of Gene Expression During Conditions of Cell StressDocument10 pagesReview: Translational Regulation of Gene Expression During Conditions of Cell StressBayan GhanimNo ratings yet
- Cell Membrane Transport NotesDocument3 pagesCell Membrane Transport NotesJAN PAULINE BABINANo ratings yet
- 1 RhizopodaDocument24 pages1 RhizopodaMohammad Fadel SatriansyahNo ratings yet
- 9th Biology Chapter-WiseDocument18 pages9th Biology Chapter-WiseMalik AqibNo ratings yet
- Science 7 Chapter 1 - Cells 1.3-1.4Document13 pagesScience 7 Chapter 1 - Cells 1.3-1.4Hương Minh Phạm QuinnNo ratings yet
- Molecular Basis of InheritanceDocument42 pagesMolecular Basis of InheritanceJayashree JanarthanamNo ratings yet
- IB Biology D.3 Liver NotesDocument7 pagesIB Biology D.3 Liver NotesDilip Pandurang PattilNo ratings yet
- Melanocytes: The Skin's Pigment Producing CellsDocument3 pagesMelanocytes: The Skin's Pigment Producing Cellsأحمد المسيريNo ratings yet
- Oxidative Stress - Molecular Mechanisms and Biological EffectsDocument374 pagesOxidative Stress - Molecular Mechanisms and Biological EffectsEML100% (2)
- Electrical Properties of Tissues and Cell Suspensions: Mechanisms and ModelsDocument2 pagesElectrical Properties of Tissues and Cell Suspensions: Mechanisms and Modelspro.gig9033No ratings yet
- Cell Cycle and Division ExplainedDocument37 pagesCell Cycle and Division ExplainedLinda Yurani Carvajal AngaritaNo ratings yet
- Cell Structures and Their FunctionsDocument2 pagesCell Structures and Their FunctionsSheikha KamidNo ratings yet
- Characterization of HSP27 Phosphorylation Induced by Microtubule Interfering Agents: Implication of p38 Signalling PathwayDocument7 pagesCharacterization of HSP27 Phosphorylation Induced by Microtubule Interfering Agents: Implication of p38 Signalling PathwayEva Del ValleNo ratings yet
- Quiz #1 Questions A&P 1Document14 pagesQuiz #1 Questions A&P 1trick49No ratings yet
- MICP - Introduction and Bacterial Growth and RequirementsDocument85 pagesMICP - Introduction and Bacterial Growth and RequirementsKYLE ANDREW SAWITNo ratings yet
- Glycerol Metabolism and Triacylglycerol MobilizationDocument18 pagesGlycerol Metabolism and Triacylglycerol MobilizationAiane GramaticaNo ratings yet
- Question Paper 2nd YearDocument2 pagesQuestion Paper 2nd YearRay MrinalNo ratings yet
- 3b MeiosisDocument9 pages3b MeiosisJhaii Sumi-og BerongesNo ratings yet
- Lecture Recombination - Homologous Recombination (Final)Document27 pagesLecture Recombination - Homologous Recombination (Final)ijazNo ratings yet
- AnaphyDocument9 pagesAnaphylarry machonNo ratings yet