Professional Documents
Culture Documents
How To Perform Lung Ultrasound in Pregnant Women With Suspected COVID-19 Infection
Uploaded by
Ahmad An NaufalOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
How To Perform Lung Ultrasound in Pregnant Women With Suspected COVID-19 Infection
Uploaded by
Ahmad An NaufalCopyright:
Available Formats
How to perform lung ultrasound in pregnant women with suspected COVID-19 infection
F Moro1*, D Buonsenso1*, MC Moruzzi1, R Inchingolo2, A Smargiassi2, L Demi3, AR Larici4,5, G
Scambia1,6, A Lanzone1,6, AC Testa1,6
1
Dipartimento Scienze della Salute della Donna, del Bambino e di Sanità Pubblica, Fondazione
Policlinico Universitario Agostino Gemelli, IRCCS, Rome, Italy
2
Dipartimento Scienze Mediche e Chirurgiche, Fondazione Policlinico Universitario Agostino
Gemelli, IRCCS, Rome, Italy
3
Department of Information Engineering and Computer Science, University of Trento, Trento, Italia
4
Dipartimento di Diagnostica per Immagini, Radioterapia Oncologica e Ematologia, Fondazione
Policlinico Universitario Agostino Gemelli, IRCCS, Rome, Italy
5
Dipartimento Universitario di Scienze Radiologiche ed Ematologiche, Università Cattolica del Sacro
Cuore, Rome, Italy
6
Dipartimento Scienze della Vita e Sanità pubblica. Università Cattolica del Sacro Cuore, Rome, Italy
*F.M. and D.B. contributed equally to this work
Running title: lung ultrasound in pregnancy
Keywords: lung ultrasound, pregnancy, COVID-19
Corresponding author
Dr Francesca Moro
Fondazione Policlinico Universitario A. Gemelli, IRCCS, Dipartimento Scienze della Salute della
Donna, del Bambino e di Sanità Pubblica,
L.go A. Gemelli 8, 00168 Rome, Italy
Email: morofrancy@gmail.com
This article has been accepted for publication and undergone full peer review but has not been
through the copyediting, typesetting, pagination and proofreading process which may lead to
differences between this version and the Version of Record. Please cite this article as doi:
10.1002/uog.22028
This article is protected by copyright. All rights reserved.
Abstract
Under specific circumstances, such as during the current COVID-19 outbreak, pregnant women can
be a target for respiratory infection, and lung examination may be required as part of their clinical
evaluation, ideally avoiding exposure to radiation. We propose a practical approach for
obstetricians/gynecologists to perform lung ultrasound, showing potential applications, semiology
and practical aspects, which should be of particular importance in emergency situations, such as the
current pandemic infection of COVID-19.
This article is protected by copyright. All rights reserved.
Introduction
Under specific circumstances, such as during the current COVID-19 outbreak, pregnant women can
be a target for respiratory infection, and lung examination may be required as part of their clinical
evaluation, ideally avoiding exposure to radiation1. As such, a radiation-free point-of-care diagnostic
tool, such as lung ultrasound examination, would be particularly useful for assessing the lungs of
pregnant women. It should be borne in mind that lung ultrasound examination has been traditionally
employed by non-radiologists as an adjunctive clinical instrument. Obstetricians/gynecologists
represent a category of clinicians who use ultrasound in their routine practice. From a technical point
of view, examination of the lungs soon after obstetric ultrasound evaluation could be feasible for
obstetricians and gynecologists, if only to ascertain the presence or absence of normality and
determine the need for further specialist care.
The current gold standard for the etiological diagnosis of COVID-19 infection is (real time)
reverse transcription polymerase chain reaction (rRT-PCR) analysis of respiratory tract specimens.
However, this test has a high false-negative rate due to both nasopharyngeal swab sampling error,
which often requires repeat sampling, and viral burden2. Some patients present late for testing, and
can cause spread of the disease because of delay in diagnosis. Imaging tools able to diagnose
pneumonia at an early stage are thus of fundamental importance. Currently, high-resolution computed
tomography (CT) is the main tool for primary diagnosis and evaluation of disease severity in patients
affected by COVID-19 infection3–5. However, use of ultrasound to identify specific sonographic
characteristics that are diagnostic of pneumonia infection has been reported6 (Table 1), as have the
typical ultrasound findings of COVID-19 disease in the lungs of pregnant women 7.
Here we propose, with an accompanying ‘How To’ video (Videoclip S1), a practical approach
for obstetricians/gynecologists to perform lung ultrasound, showing potential applications, semiology
and practical aspects, which should be of particular importance in emergency situations, such as the
current pandemic infection of COVID-19.
This article is protected by copyright. All rights reserved.
Physical basis of lung ultrasound
Air creates a high and sudden acoustic mismatch with tissue (subcutaneous layers and muscles),
causing reflection of the ultrasound beam, and preventing direct imaging of the pulmonary
parenchyma. In a normally aerated lung, the only detectable structure is the pleura, visualized as a
highly hyperechoic horizontal line (pleural line) (Figure 1). Reflection of the ultrasound beam
determines the appearance of hyperechoic, parallel, horizontal artifacts (‘A-lines’), indicating normal
inflated peripheral lung if combined with ‘sliding’ of the pleural line (see below)8–10. This pattern is
typical of a lung that is devoid of any pathological phenomenon involving the peripheral lung
parenchyma. Indeed, since ultrasound does not penetrate air, lung ultrasound can evaluate only lung
pathology that affects the pleura. Therefore, a lung lesion that is not in contact with the pleura, for
example, a deep cancer nodule, is not detectable by lung ultrasound, which is why this technique is
not appropriate for cancer screening.
When the lung is affected by pathology that is physically comparable with soft tissue, for
example, a consolidated lung during lobar pneumonia, atelectasis or with pleural effusions, it
becomes amenable to sonographic examination, because structures (consolidations, vessels, fluid,
bronchograms) are discernible. In other pathological entities, such as interstitial lung disease, acute
respiratory distress syndrome (ARDS), pulmonary edema and pneumothorax, the lung is still aerated
but it contains a variable amount of water, cells and/or inflammation that alter the acoustic properties
of the lung and generate vertical artifacts (usually called ‘B-lines’, with several different
characteristics).
Lung ultrasound semiology
Normal lung ultrasound pattern: A-lines
When scanning a normal lung, the operator will see the subcutaneous layers and the hyperechoic
horizontal pleural line, a line that, on real-time examination, has horizontal movements synchronized
with the respiratory activity (this movement is called ‘lung sliding’)8,9. The horizontal ‘A-lines’ are
the hallmark of the normal lung (Figure 1). They are the hyperechoic, repetitive reverberations, at
regular intervals, of the pleural line. In between the A-lines, depending on the ultrasound machine,
probes and frequencies used, it is possible to see the ‘mirror’ effect of the acoustic interfaces of the
This article is protected by copyright. All rights reserved.
structures of the chest wall8-10. When the probe is positioned in the intercostal space, the pleural line
and A-lines are totally visible (Figure 1a). When the probe is positioned longitudinally, the ribs with
their posterior shadowing can be identified, and between the ribs the pleural line and A-lines are
visible (Figure 1b).
Pathological lung ultrasound pattern: B-lines
When the lung loses normal aeration, but is not completely consolidated (as happens in the case of
interstitial lung disease, pulmonary fibrosis, pulmonary edema, lung deflation, lung contusion,
perilesional consolidative areas), it generates different shapes and lengths of vertical artifacts, usually
called B-lines11 (Figure 2). The genesis of these differences is not completely understood, but they
possibly reflect the different shaped and sized acoustic channels generated by altered peripheral air
space in pathological conditions6,12,13. In general, B-lines are visible and not specific to a single
pathology. However, accompanying clinical information can help to distinguish different entities. For
example, the detection of B-lines in a pregnant woman would not be associated with pulmonary
fibrosis or chronic obstructive pulmonary disease, as they are typical pathologies of advanced age.
Cardiogenic pulmonary edema is characterized by regular, laser-like, bright B-lines, particularly
evident bilaterally on the lung bases (due to the gravitational effect on cardiogenic edema) without
spared areas, and the pleural line is regular11. Conversely, in inflammatory lung disease such as viral
pneumonia (including early stages of COVID-19), the pleural line is usually irregular (blurred)
(Figure 3), thickened, and with a characteristic distribution (monofocal or multifocal, patchy or
inhomogeneous involvement, surrounded by spared areas and with no gravitational distribution)11.
Pathological lung pattern: white lung
When the density of the peripheral (subpleural) lung parenchyma is increased (but not to the extent
of that in a consolidative state), as happens in ARDS (including COVID-19-induced ARDS),
ultrasound examination shows a white area (the so-called ‘ultrasonographic white lung’) (Figure 3),
in which no horizontal reverberations (A-lines) nor separated B-lines are visible11.
Pathological lung pattern: consolidation
This article is protected by copyright. All rights reserved.
During pneumonia or atelectasis, the lung is completely (or almost) collapsed. In these circumstances,
the involved area of the lung loses its air and becomes a solid organ that can be evaluated by
ultrasound in the same way as any other organ (for example, the liver). The consolidation appears as
an irregular hypoechoic area (Figure 4). In pathology such as COVID-19 pneumonia, advanced
ARDS, or bronchiolitis, the lung may present only small subpleural consolidations. In lobar
pneumonia, the consolidation is larger, liver-like and hypoechoic, and may present with dynamic,
tree-like air bronchogram, fluid bronchogram or vessels. Conversely, in the case of atelectasis, there
are static air bronchograms mainly distributed as horizontal lines14.
Pathological lung pattern: pleural effusion
Evaluation of pleural effusion is the traditional target of lung ultrasound examination. Some
obstetricians/gynecologists have experience in detecting effusion during routine clinical practice,
since some pregnancy complications and gynecological cancers can lead to the development of
effusion. In general, pleural effusion can be simple and uniformly anechoic or complicated by the
presence of hyperechoic spots due to blood, pus, fibrin and/or septa15.
Practical points
Machine, probes and settings
Lung ultrasound can be performed with any type of machine, including first-generation ultrasound
machines. Handheld ultrasound scanners, which may be preferred in an emergency situation, may
also be appropriate for this examination, having the advantage of being easier to sterilize and cover16.
Since the lung has not traditionally been considered amenable to ultrasound examination, there are
no lung-specific machines or probes. Different types of probe can be used, including linear, convex
and microconvex. In general, linear probes can be used to evaluate better details of the pleural line
and subpleural space, due to high frequencies and resolution. However, convex probes, routinely used
for gynecological and obstetric examination, can be suitable for lung examination. Similarly, there
are no lung-specific settings. However, it is fundamental to underline some technical aspects: 1) the
focus should be moved to the level corresponding to the adequately zoomed pleural line; 2) gain can
This article is protected by copyright. All rights reserved.
be reduced in order to increase contrast and highlight the hyperechoic signs (A-lines, B-lines and
white lung); however, when a consolidated lung (for example, in pneumonia) is scanned, gain should
be set to that used for examination of a parenchymatous organ. In general, for specialists starting to
perform lung examination, it is advisable to use the same settings for follow-up examinations of the
same patient in order to be able to compare different images.
Patient positioning
Lung ultrasound can be considered as an ‘extension’ of the obstetric abdominal ultrasound
evaluation17. The ultrasound examiner can simply move the probe from the abdomen to the chest,
scanning the anterior and lateral areas of the thorax. The examination should cover the whole
pulmonary area, from the basal to upper zones of the thorax. Four vertical lines (right mid-axillary
line, right parasternal line, left parasternal line, left mid-axillary line) can be followed in order to
perform a systematic examination. With the patient then in a sitting or lateral position, the posterior
paravertebral surface of the thorax should be scanned, from the basal to upper zones or posterior-
axillary lines according to the patient’s position.
Conclusion
We have proposed a systematic approach for obstetricians/gynecologists to perform lung ultrasound
examination in pregnant women, describing potential applications and semiology and providing
practical points for consideration. Pathological ultrasound patterns are compared to those expected
in a normal lung, with particular emphasis on those more indicative of COVID-19 infection.
ACKNOWLEDGMENTS
We thank Mr Emerson Marinho Pinto and Dr Paola Romeo, Dipartimento Scienze della Salute della
Donna, del Bambino e di Sanità Pubblica, Fondazione Policlinico Universitario Agostino Gemelli,
Rome, Italy, for production of the video.
This article is protected by copyright. All rights reserved.
References
1) Gargani L, Picano E. The risk of cumulative radiation exposure in chest imaging and the
advantage of bedside ultrasound. Crit Ultrasound J 2015; 7: 4.
2) Hao W, Li M. Clinical diagnostic value of CT imaging in COVID-19 with multiple negative
RT-PCR testing. Travel Med Infect Dis 2020; 13:101627. doi: 10.1016/j.tmaid.2020.101627.
3) Pan Y, Guan H, Zhou S, Wang Y, Li Q, Zhu T, Hu Q, Xia L. Initial CT findings and temporal
changes in patients with the novel coronavirus pneumonia (2019-nCoV): a study of 63
patients in Wuhan, China. Eur Radiol 2020. doi: 10.1007/s00330-020-06731-x.
4) Bernheim A, Mei X, Huang M, Yang Y, Fayad ZA Chest CT Findings in Coronavirus
Disease-19 (COVID-19): Relationship to Duration of Infection. Radiology 2020.
doi.org/10.1148/radiol.2020200463.
5) Zi Yue Zu, Meng Di Jiang, Peng Peng Xu, Wen Chen, Qian Qian Ni, Guang Ming Lu, Long
Jiang Zhang. Coronavirus Disease 2019 (COVID-19): A Perspective from China. Radiology
2020. doi:10.1148/radiol.2020200490.
6) Soldati G, Smargiassi A, Demi L and Inchingolo R. Artifactual Lung Ultrasonography: It Is
a Matter of Traps, Order, and Disorder. Appl. Sci 2020; 10, 1570.
7) Peng QY, Wang XT, Zhang LN; Chinese Critical Care Ultrasound Study Group (CCUSG).
Findings of lung ultrasonography of novel corona virus pneumonia during the 2019-2020
epidemic. Intensive Care Med 2020. doi: 10.1007/s00134-020-05996-6.
8) Volpicelli G. Lung sonography. J Ultrasound Med 2013; 32: 165-71.
9) Gargani L, Volpicelli G. How I do it: lung ultrasound. Cardiovasc Ultrasound 2014; 12: 25.
10) Soldati G, Demi M, Inchingolo R, Smargiassi A, Demi L. On the Physical Basis of Pulmonary
Sonographic Interstitial Syndrome. J Ultrasound Med 2016; 35: 2075-86.
11) Soldati G, Demi M, Smargiassi A, Inchingolo R, Demi L. The role of ultrasound lung artifacts
in the diagnosis of respiratory diseases. Expert Rev Respir Med 2019; 13: 163-172.
12) Demi L, van Hoeve W, van Sloun RJG, Soldati G, Demi M. Determination of a potential
quantitative measure of the state of the lung using lung ultrasound spectroscopy. Sci Rep 2017;
7:12746.
This article is protected by copyright. All rights reserved.
13) Soldati G, Smargiassi A, Inchingolo R, Sher S, Nenna R, Valente S, Inchingolo CD, Corbo
GM. Lung ultrasonography may provide an indirect estimation of lung porosity and airspace
geometry. Respiration 2014; 88: 458-68.
14) Lichtenstein D, Mezière G, Seitz J. The dynamic air bronchogram. A lung ultrasound sign of
alveolar consolidation ruling out atelectasis. Chest 2009; 135: 1421-1425.
15) Brogi E, Gargani L, Bignami E, Barbariol F, Marra A, Forfori F, Vetrugno L. Thoracic
ultrasound for pleural effusion in the intensive care unit: a narrative review from diagnosis to
treatment. Crit Care 2017; 21: 325.
16) Buonsenso D, Pata D, Chiaretti A. Covis-19 outbreak: less stethoscope, more ultrasound.
Lancet Respir Med 2020 (Accept).
17) Inchingolo R, Smargiassi A, Mormile F, Marra R, De Carolis S, Lanzone A, Valente S, Corbo
GM. Look at the lung: can chest ultrasonography be useful in pregnancy? Multidiscip Respir
Med 2014; 9: 32.
This article is protected by copyright. All rights reserved.
Figure and video legends
Figure 1 Ultrasound images of normal lung. When the probe is positioned in the intercostal space
(A), the pleural line (yellow arrow) is visible with no interruption. An A-line due to the reverberation
of the pleural line is indicated by a white arrow. When the probe is positioned longitudinally (B), ribs
can be recognized (stars) with posterior shadowing, pleural line (yellow arrow) and A-lines (white
arrows).
Figure 2 Ultrasound images show hyperechoic vertical line(s) touching the bottom of the screen,
appearing as a comet (A), multiple thickened hyperechoic lines (B) or short lines arising from the
pleura (C). These lines are called “B-lines” (blue arrows). They are present in interstitial lung disease,
acute respiratory distress syndrome, pulmonary fibrosis, pulmonary edema and perilesional
consolidative areas.
Figure 3 Ultrasound images of a patient with pneumonia infection. Irregular and thickened pleural
line (yellow arrow) and a “white area” (stars) are present. Neither A-lines nor the discrete B-lines are
present.
Figure 4 Ultrasound images of patients with pneumonia infections. The lung periphery is partially
collapsed and the involved area appears as irregular hypoechoic areas (green arrows).
Figure 5 Anatomic landmarks for ultrasound assessment.
Videoclip S1 Video summarizing the basic principles of lung ultrasound, and showing images of
physiology and pathological conditions.
This article is protected by copyright. All rights reserved.
Table 1 Computed tomographic and ultrasonographic features of COVID-19 pneumonia
Lung high-resolution computed tomography Lung ultrasound
Lung Findings Ground glass opacities B-lines (multifocal, discrete or confluent)
parenchyma Consolidation Sonographic interstitial syndrome
Nodules/micronodules ‘White lung’
‘Crazy paving’ Subpleural consolidation
‘Reversed halo’ sign
Distribution Subpleural Subpleural
Peribronchovascular Not applicable
Patchy/multilobar Patchy
Diffuse Diffuse
Predominantly at the lower lobes Predominantly at the lower lobes
Unilateral/bilateral Unilateral/bilateral
Pleura Smooth thickening Thickened and irregular pleural line
Pleural effusion is rare Pleural effusion is rare
This article is protected by copyright. All rights reserved.
Table 2 Systematic ultrasound examination of the lung in pregnant patient with COVID-19
Procedure Instructions
1. Location Ultrasound examination should be performed at the patient’s bedside (wireless
devices are preferred in order to minimize the risk of contamination)
2. Patient positioning* Supine, prone, left- and right-sided position
3. Ultrasound equipment and Disinfection of hands and medical devices.
sterilization Appropriate personal protective equipment (PPE) should be worn.
Disinfection of the system with wipes impregnated with citric acid and dilute
solution of sodium chlorite.
Surface of ultrasound machine should be covered by adequate sheaths.
After the examination, both ultrasound machine and probe should be deeply
disinfected.
4. Scanning planes* Examination should be done assessing 14 anatomical landmarks*
5. Ultrasound parameters Pleural line (regular or irregular)
B-lines (sporadic, multiple-confluent)
White lung
Subpleural consolidations (absent, present<1cm, present >1cm)
*Figure 5
This article is protected by copyright. All rights reserved.
Table 3 Lung ultrasound examination checklist
Anatomic Pleural line Vertical artifacts Subpleural consolidation
landmarks 1. regular 1. sporadic B-lines 1.absent
2. irregular and thickened 2. multiple- 2.present<1cm
confluent B-lines 3.present >1cm
3. white lung
1
2
3
4
5
6
7
8
9
10
11
12
13
14
This article is protected by copyright. All rights reserved.
Table 4 Assessment of ultrasound patterns in pregnant women, including findings that might be suggestive of COVID pneumonia.
Ultrasound findings Ultrasound images Evaluation
Regular pleural line and sporadic B-lines Normal
Irregular pleural line and sporadic B-lines Suspicious for COVID-19 infection at early
stage if bilateral and patchy
Irregular pleural line and multiple B-lines Indicative of COVID-19 infection at early
stage (very indicative if bilateral and
patchy)
Irregular pleural line and white lung Severe viral pneumonia (especially if
bilateral and patchy)
Irregular pleural line and subpleural More severe viral pneumonia (especially if
consolidations bilateral and patchy)
This article is protected by copyright. All rights reserved.
Accepted Article
This article is protected by copyright. All rights reserved.
Accepted Article
This article is protected by copyright. All rights reserved.
Accepted Article
This article is protected by copyright. All rights reserved.
Accepted Article
This article is protected by copyright. All rights reserved.
Accepted Article
This article is protected by copyright. All rights reserved.
You might also like
- Pulmonary Functional Imaging: Basics and Clinical ApplicationsFrom EverandPulmonary Functional Imaging: Basics and Clinical ApplicationsYoshiharu OhnoNo ratings yet
- Bobillo Perez2019Document21 pagesBobillo Perez2019Nisa Hermina PutriNo ratings yet
- Normal and Pathological Bronchial Semiology: A Visual ApproachFrom EverandNormal and Pathological Bronchial Semiology: A Visual ApproachPierre Philippe BaldeyrouNo ratings yet
- Rambhia 2016Document24 pagesRambhia 2016Heru SigitNo ratings yet
- Lung Transplantation: Evolving Knowledge and New HorizonsFrom EverandLung Transplantation: Evolving Knowledge and New HorizonsGanesh RaghuNo ratings yet
- FUSIC COVID GuidanceDocument4 pagesFUSIC COVID GuidanceMarcelo UGNo ratings yet
- Thoracic Ultrasound and Integrated ImagingFrom EverandThoracic Ultrasound and Integrated ImagingFrancesco FelettiNo ratings yet
- Blue Protocol. Lung Ultrasound in The Critically IllDocument12 pagesBlue Protocol. Lung Ultrasound in The Critically IllRomina Alfonsina Decap CarrascoNo ratings yet
- Internal Medicine Department Dr. M. Djamil Hospital, Padang 2017Document21 pagesInternal Medicine Department Dr. M. Djamil Hospital, Padang 2017Gina ArianiNo ratings yet
- Journal Reading PulmonologiDocument21 pagesJournal Reading PulmonologiGina ArianiNo ratings yet
- Lung Ultrasound For Critically Ill PatientsDocument14 pagesLung Ultrasound For Critically Ill Patientsitzel rochaNo ratings yet
- Bedside Lung Ultrasound Versus Chest X-Ray Use in The Emergency DepartmentDocument3 pagesBedside Lung Ultrasound Versus Chest X-Ray Use in The Emergency DepartmentharnellaNo ratings yet
- Routine Use of Point-of-Care Lung Ultrasound During The COVID-19 PandemicDocument4 pagesRoutine Use of Point-of-Care Lung Ultrasound During The COVID-19 PandemicOswaldo MontesNo ratings yet
- Blue ProtocolDocument3 pagesBlue ProtocolDorica GiurcaNo ratings yet
- Chest Ultrasonography in Patients With HIVDocument10 pagesChest Ultrasonography in Patients With HIVChris Vam SanchezNo ratings yet
- Lung Ultrasound For Critically Ill Patients - Mojoli F, Bouhemad B, Mongodi S, Lichtenstein D. (Am J Respir Crit Care Med. 2019)Document53 pagesLung Ultrasound For Critically Ill Patients - Mojoli F, Bouhemad B, Mongodi S, Lichtenstein D. (Am J Respir Crit Care Med. 2019)Mr. IncognitoNo ratings yet
- Sonographic Diagnosis of Pneumonia and BronchopneumoniaDocument8 pagesSonographic Diagnosis of Pneumonia and BronchopneumoniaCaitlynNo ratings yet
- The V-Line: A Sonographic Aid For The Confirmation of Pleural FluidDocument4 pagesThe V-Line: A Sonographic Aid For The Confirmation of Pleural FluidAlpi ApriansahNo ratings yet
- Jurnal 2Document0 pagesJurnal 2Seftiana SaftariNo ratings yet
- 2008 Chest - The Blue ProtocolDocument9 pages2008 Chest - The Blue Protocoleduardo0% (1)
- POCUS NeumotoraxDocument20 pagesPOCUS NeumotoraxRaydel ManuelNo ratings yet
- Sep 1, 2011) Journal: Medscape Radiology: Radiological Society of North AmericaDocument19 pagesSep 1, 2011) Journal: Medscape Radiology: Radiological Society of North AmericaMohamad Rizki DwikaneNo ratings yet
- Usg Pulmon 2Document6 pagesUsg Pulmon 2SCORPIONo ratings yet
- NeumoniaDocument14 pagesNeumoniaPedro TumbacoNo ratings yet
- COVID and Radiology Departments - Website Version April 2-2Document11 pagesCOVID and Radiology Departments - Website Version April 2-2Florin StanciuNo ratings yet
- Lung Ultrasound: A New Tool For The CardiologistDocument9 pagesLung Ultrasound: A New Tool For The CardiologistNag Mallesh RaoNo ratings yet
- Pneumotorax Syr06lDocument53 pagesPneumotorax Syr06lflavia_craNo ratings yet
- Peng Et Al-2020-Intensive Care Medicine PDFDocument2 pagesPeng Et Al-2020-Intensive Care Medicine PDFTeodor ŞişianuNo ratings yet
- The Accuracy of Ultrasound-Guided Lung Biopsy Pathology andDocument8 pagesThe Accuracy of Ultrasound-Guided Lung Biopsy Pathology andHeru SigitNo ratings yet
- Lung Ultrasound Vs CTDocument9 pagesLung Ultrasound Vs CTValentinaNiñoNo ratings yet
- 2015 Article 91Document7 pages2015 Article 91Karel ZertucheNo ratings yet
- Ajtccm 27 1 054Document5 pagesAjtccm 27 1 054Saniska NCTNo ratings yet
- Ultrasound A CL 2021Document17 pagesUltrasound A CL 2021Alejandra SanchezNo ratings yet
- Pneumothorax: Classification and EtiologyDocument17 pagesPneumothorax: Classification and EtiologyPASMOXNo ratings yet
- Pulmonary Function TestDocument7 pagesPulmonary Function TestGhada HusseinNo ratings yet
- Use of Lung Ultrasound For COVID-19 in The Intensive Care UnitDocument4 pagesUse of Lung Ultrasound For COVID-19 in The Intensive Care UnitInayahNo ratings yet
- Lung Ultrasound in The Evaluation of Pleural Effusion: Elena Prina, Antoni Torres, Carlos Roberto Ribeiro CarvalhoDocument5 pagesLung Ultrasound in The Evaluation of Pleural Effusion: Elena Prina, Antoni Torres, Carlos Roberto Ribeiro CarvalhoegerpratamaNo ratings yet
- A Case of Tracheal Tumor Masquerading As AsthmaDocument4 pagesA Case of Tracheal Tumor Masquerading As Asthmamastansk84No ratings yet
- Chest Sonography: A Useful Tool To Differentiate Acute Cardiogenic Pulmonary Edema From Acute Respiratory Distress SyndromeDocument11 pagesChest Sonography: A Useful Tool To Differentiate Acute Cardiogenic Pulmonary Edema From Acute Respiratory Distress SyndromeErwin SiahaanNo ratings yet
- CAP Diagnostic (Uptoptodate 2019)Document34 pagesCAP Diagnostic (Uptoptodate 2019)elizabeth perezzNo ratings yet
- Emphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsDocument8 pagesEmphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsChairul Nurdin AzaliNo ratings yet
- Interstitial Lung DiseaseDocument4 pagesInterstitial Lung DiseasedewimarisNo ratings yet
- Asthma: Further ReadingDocument13 pagesAsthma: Further ReadingcarlosNo ratings yet
- Radiography: S. Moore, E. GardinerDocument6 pagesRadiography: S. Moore, E. GardinerameenallyNo ratings yet
- Clinical, Radiological, and Pathological Investigation of AsbestosisDocument14 pagesClinical, Radiological, and Pathological Investigation of Asbestosisintan danayantiNo ratings yet
- A Case of Pulmonary Aspergilloma and ActinomycosisDocument4 pagesA Case of Pulmonary Aspergilloma and ActinomycosisNova PurbaNo ratings yet
- Imaging in Chronic Obstructive Pulmonary DiseaseDocument9 pagesImaging in Chronic Obstructive Pulmonary DiseaseHarizNo ratings yet
- 442 - ZBFSKF - Point of Care Lung Ultrasound Findings in Novel Coronavirus Disease 19 PnemoniaeDocument5 pages442 - ZBFSKF - Point of Care Lung Ultrasound Findings in Novel Coronavirus Disease 19 PnemoniaeOscar PastranaNo ratings yet
- Mondoni Et AlDocument11 pagesMondoni Et AlpandylouisputraNo ratings yet
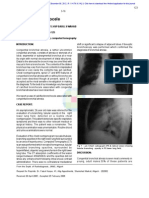
- Inadvertent Chest Tube Insertion in Congential Cystic Adenomatoid Malformation and Congential Lobar Emphysema Highlighting An Important ProblemDocument0 pagesInadvertent Chest Tube Insertion in Congential Cystic Adenomatoid Malformation and Congential Lobar Emphysema Highlighting An Important ProblemWenny EudensiaNo ratings yet
- Radiographic Signs of Pulmonar DiseaseDocument10 pagesRadiographic Signs of Pulmonar DiseaseMarleeng CáceresNo ratings yet
- Clinical Presentation and Diagnostic Evaluation of Ventilator-Associated PneumoniaDocument33 pagesClinical Presentation and Diagnostic Evaluation of Ventilator-Associated Pneumoniamayteveronica1000No ratings yet
- Pulmonary Aspergillosis Imaging: Practice EssentialsDocument9 pagesPulmonary Aspergillosis Imaging: Practice EssentialsPutri PrameswariNo ratings yet
- Ecografia Pulmonar NeonatalDocument12 pagesEcografia Pulmonar NeonatalJorge CastroNo ratings yet
- Pleural Disease 2010 Pneumothorax PDFDocument14 pagesPleural Disease 2010 Pneumothorax PDFArrum Chyntia YuliyantiNo ratings yet
- COVID 19PatientsAndTheRadiologDocument7 pagesCOVID 19PatientsAndTheRadiologjturos2003No ratings yet
- Co-Existence of Pulmonary, Tonsillar and Laryngeal TuberculosisDocument4 pagesCo-Existence of Pulmonary, Tonsillar and Laryngeal TuberculosisSoeHorNo ratings yet
- Healthcare 09 01015Document20 pagesHealthcare 09 01015Sori B. Requena C.No ratings yet
- Journal Radiologi 3Document14 pagesJournal Radiologi 3WinayNayNo ratings yet
- Clinical and Radiological Evaluation of Emphysematous Chest - A Prospective StudyDocument5 pagesClinical and Radiological Evaluation of Emphysematous Chest - A Prospective StudyTony AndersonNo ratings yet
- Experiences of National Documentation in Electronic Health Records: The Study Among Occupational Health NursesDocument2 pagesExperiences of National Documentation in Electronic Health Records: The Study Among Occupational Health NursesAhmad An NaufalNo ratings yet
- Occupational Health Nursing and Pioneer Leaders From Past To PresentDocument6 pagesOccupational Health Nursing and Pioneer Leaders From Past To PresentAhmad An Naufal100% (1)
- Ohn 2Document9 pagesOhn 2Ahmad An NaufalNo ratings yet
- Why Are Pregnant Women Susceptible To COVID19 An Immunological Viewpoint2020journal of Reproductive ImmunologyDocument4 pagesWhy Are Pregnant Women Susceptible To COVID19 An Immunological Viewpoint2020journal of Reproductive ImmunologyAhmad An NaufalNo ratings yet
- Views and Reviews: Covid-19: The Time To Shield All Pregnant Frontline Workers Is NowDocument2 pagesViews and Reviews: Covid-19: The Time To Shield All Pregnant Frontline Workers Is NowAhmad An NaufalNo ratings yet
- Practice: Covid-19 and PregnancyDocument2 pagesPractice: Covid-19 and PregnancyAhmad An NaufalNo ratings yet
- Incident Causation Model For Improving FeedbackDocument12 pagesIncident Causation Model For Improving FeedbackAhmad An NaufalNo ratings yet
- Slipped Disc Minicase CompleteDocument17 pagesSlipped Disc Minicase CompleteGerold ChuaNo ratings yet
- Diabetes Pridiction Using Machine LearningDocument31 pagesDiabetes Pridiction Using Machine LearningAbhishekNo ratings yet
- Nose, Sinuses, Mouth & Pharynx AssessmentDocument11 pagesNose, Sinuses, Mouth & Pharynx AssessmentPutri WishalNo ratings yet
- Assignment On: Bio-PreservationDocument18 pagesAssignment On: Bio-PreservationtowhidNo ratings yet
- What Are The Classification of HospitalsDocument11 pagesWhat Are The Classification of HospitalsLily Jane PakiwonNo ratings yet
- Heart Dysrhythmias Cheat Sheet PDFDocument5 pagesHeart Dysrhythmias Cheat Sheet PDFbarbaraNo ratings yet
- Mechanical Ventilation and Noninvasive VentilationDocument6 pagesMechanical Ventilation and Noninvasive Ventilationuul ulfaNo ratings yet
- Para MCQDocument2 pagesPara MCQMohamed HaridyNo ratings yet
- Dundon 2010Document9 pagesDundon 2010Ana-Maria ChiricNo ratings yet
- Why We Sleep The New Science of Sleep and Dreams BDocument3 pagesWhy We Sleep The New Science of Sleep and Dreams BmjhachemNo ratings yet
- Dysphagia and Swallowing Disorders, MC Carty E. (2021)Document16 pagesDysphagia and Swallowing Disorders, MC Carty E. (2021)Irving Santiago SandovalNo ratings yet
- Phoenix, Arizona: Principles To Guide Zoning For Community Residences For People With DisabilitiesDocument44 pagesPhoenix, Arizona: Principles To Guide Zoning For Community Residences For People With Disabilitiesdan-304518No ratings yet
- Lips Diseases and Its Management: Classification of Lip DisordersDocument17 pagesLips Diseases and Its Management: Classification of Lip DisordersSubhash VermaNo ratings yet
- Children Hypertension ChartDocument4 pagesChildren Hypertension ChartHo Yoke MeiNo ratings yet
- Pex 06 01Document5 pagesPex 06 01Moira CabaticNo ratings yet
- Community Medicine Card QuestonsDocument10 pagesCommunity Medicine Card Questons202Manjida Rahman OniNo ratings yet
- Pathophysiology: Predisposing Factors Precipitating FactorsDocument1 pagePathophysiology: Predisposing Factors Precipitating Factorsrozj07No ratings yet
- B Science 10 Quarter 3 Module 2 (Week 3)Document17 pagesB Science 10 Quarter 3 Module 2 (Week 3)Daisy Soriano PrestozaNo ratings yet
- Millet Grains: Nutritional Quality, Processing, and Potential Health BenefitsDocument16 pagesMillet Grains: Nutritional Quality, Processing, and Potential Health BenefitsBala NairNo ratings yet
- Biological Disaster - Biological Disaster Management & Types of Biological DisastersDocument3 pagesBiological Disaster - Biological Disaster Management & Types of Biological DisastersS DNo ratings yet
- PBL 1 Painful Big ToeDocument5 pagesPBL 1 Painful Big ToeRomi Raja100% (1)
- Three-Stage Assessment. 2021Document14 pagesThree-Stage Assessment. 2021Mwanja Moses100% (1)
- Advocacy Project 2 FinalDocument5 pagesAdvocacy Project 2 Finalapi-742583747No ratings yet
- Thorax: Thoracic Spine Anatomy and Biomechanics Level IIIDocument23 pagesThorax: Thoracic Spine Anatomy and Biomechanics Level IIIAnonymous ecI8GUbaNo ratings yet
- Bioregulatory Medicine History - Reinhold VollDocument11 pagesBioregulatory Medicine History - Reinhold VollD.W. Smith100% (2)
- Nidaan Swasthya Bima Policy BrochureDocument10 pagesNidaan Swasthya Bima Policy Brochureimpbithin96No ratings yet
- Ensayo - InglésDocument11 pagesEnsayo - InglésMery RosalesNo ratings yet
- Dr. H. Soekimin, Sppa: Bagian Patologi Anatomi Fakultas KedokteranDocument45 pagesDr. H. Soekimin, Sppa: Bagian Patologi Anatomi Fakultas KedokteranRommy Kurniawan DeskyNo ratings yet
- Preboards 2 - NP3 (Printable)Document10 pagesPreboards 2 - NP3 (Printable)Joana Marie DomingoNo ratings yet
- Sympo 4 KetoanalogDocument31 pagesSympo 4 KetoanalogYuyun RasulongNo ratings yet
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (23)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (5)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- An Autobiography of Trauma: A Healing JourneyFrom EverandAn Autobiography of Trauma: A Healing JourneyRating: 5 out of 5 stars5/5 (2)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Summary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisFrom EverandSummary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (9)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)