Professional Documents
Culture Documents
Thyroid & Parathyroid Glands: Hurthle Cells
Uploaded by
christianOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Thyroid & Parathyroid Glands: Hurthle Cells
Uploaded by
christianCopyright:
Available Formats
THYROID & PARATHYROID GLANDS
HURTHLE CELLS
o Azkanazy cells, oxyphilic cells, oncocytes
o Follicular cells with abundant granular acidophilic cytoplasm
o Granularly due to accumulation of mitochondria
C-CELLS/PARAFOLLICULAR CELLS
o Neuroendcorine cells
o Reach the thyroid via ultimobranchial body
o Middle and upper third of the lateral lobes
o Number varies according to age
o Numerous: infancy and old age
o Adult: no more than 10 C cells/LPF
o Immunoreactive for CEA
SOLID CELL NESTS (RESTS)
o Remnants of ultimobranchial body
o 0.1 mm average
o 90% of neonatal thyroid glands
o Composed of polygonal/oval cells admixed with clear cell
o Positive for high and low MW keratin and for CEA
CONGENITAL ABNORMALITIES
Thyroglossal duct anomalies
o Localized persistence of thyroglossal duct
o 2 forms:
Sinus tract connect to foramen cecum or suprasternal notch
Blind tubular structure
Thyroglossal duct cyst
o Cystic change are prominent
o Midline of the neck, region of hyoid bone
o Lined by pseudostratified ciliated/squamous epithelium
o Treatment: surgical removal
o To minimize recurrence: excision of the middle third of the hyoid bone and entire length of sinus tract
Heterotrophic thyroid tissue
o Base of the tongue - MC
o Anterior tongue, submandibular region, larynx, trachea, mediastinum, and heart
o Majority are found in WOLFLER AREA (Isosceles triangle with edge of the mandible at its base and the
concavity of aortic arch at apex)
Branchial pouch anomalies
o Present as patent fistula, simple sinus, blind cyst, island of cartilage
o Location: anterolateral region of the neck
o FIRST POUCH: Preauricular area/ beneath the posterior half of the mandible
o SECOND POUCH: Anterior to SCM in the mid-neck and have an open tract communicating with the
pharynx
o FOURTH POUCH: Lower neck, suprasternal or supraclavicular
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 1
THYROIDITIS
ACUTE THYROIDITIS
o Infectious in nature
o Associated with acute infection of the upper aerodigestive tract, general sepsis, major trauma to the neck
with an open wound
o Malnourished infant, debilitated elderly, immunocompromised patient
o Common cause:
Streptococcus haemolyticus
Staphylococcus aureus
Pneumococcus
o Other causes:
Gram negative bacteria
Fungi esp. Candida
Penumocystis
o Morphologically
Neutrophilic infiltration
Tissue necrosis
o Diagnosis: fine needle biopsy with smear cytologic exam and culture
o Treatment: medical, surgical – drainage
o Best treatment: Fistulectomy
GRANULOMATOUS (de Quervain) THYROIDITIS
o AKA Subacute thyroiditis
o Middle-aged women with sore throat, painful deglutition, and marked tenderness on palpation in the
thyroid region
o Associated with fever and malaise
o Majority of cases there is complete resolution
o Unknown etiology
o Follows an infection of the upper aerodigestive tract
Autoimmune (lymphocytic and Hashimoto) thyroiditis
o Production of autoantibodies that alter thyroid function.
o One of the two major forms in which autoimmune thyroid disease may manifest
o Hashitoxicosis
o Immune-mediated insult >> diffuse or nodular hyperactivity of the gland >> exhaustion atrophy,
manifested by diffuse oxyphilia of the follicular epithelium.
Lymphocytic thyroiditis
o more commonly diagnosed in children
o ‘juvenile form’ of lymphocytic/autoimmune thyroiditis
o radioactive iodine uptake is generally low
o Gland is diffusely enlarged and of increased consistency, with a solid, white, vaguely nodular cut surface.
Hashimoto thyroiditis
o AKA struma lymphomatosa,
o Predominantly a disease of women over 40 years of age.
o Diffuse firm thyroid enlargement, accompanied by signs of tracheal or esophageal compression.
o Complications:
malignant lymphoma and leukemia
papillary carcinoma
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 2
Hürthle cell neoplasms
o Treatment: depends on its severity
Mild cases no therapy is needed.
Multifocal sclerosing thyroiditis
o Characterized by multiple (sometimes innumerable) foci of fibrosis throughout the gland, often having a
radial configuration.
o LPO: the appearance can be indistinguishable from that of papillary microcarcinoma
o HPO: lack of a neoplastic glandular component.
o The pathogenesis of this lesion is obscure
HYPERPLASIA
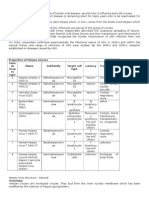
Table 1.Major types of thyroid hyperplastic disorders
NAME MECHANISM PATHOLOGY FUNCTIONAL STATUS
Dyshormonogenetic Genetically Nodular or (less frequently) Hypothyroid
goiter determined error in diffuse hyperplasia
TH metabolism
Graves disease Autoimmune Diffuse hyperplasia Hyperthyroid
Nodular hyperplasia
Endemic goiter Iodine deficiency Nodular hyperplasia (preceded Usually euthyroid; sometimes
by a transient phase of diffuse hypothyroid
hyperplasia)
Sporadic goiter Unknown Nodular hyperplasia Usually euthyroid; sometimes
hyperthyroid or hypothyroid
Dyshormonogenetic goiter
o Defects in hormone synthesis >> Types of goiter
Lack of responsiveness to TSH
Defects in iodide transport
Defects in organification
Defects in coupling
Abnormalities of thyroglobulin synthesis and secretion
Defects in deiodinase
Abnormalities in the transport of TH
Graves disease (diffuse toxic goiter)
o AKA Basedow dse, thyrotoxicosis, diffuse toxic goiter, and exophthalmic goiter
o Young adult females with muscle weakness, weight loss, irritability, tachycardia, goiter, and often a great
increase of appetite.
o Exophthalmos (ophthalmopathy) is present in 25–50% of the patients.
o Most common cause of hyperthyroidism.
Nodular hyperplasia
o AKA nodular or multinodular goiter, adenomatoid goiter, adenomatous hyperplasia
o Most common thyroid disease.
A. Endemic goiter
o Due to low iodine content of the water and soil
o Parencymatous goiter
Increased TSH secretion
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 3
hyperactive thyroid with tall follicular epithelium and small amounts of colloid
o Diffuse or nodular colloid
Follicular atrophy with massive storage of colloid, with or without nodularity
B. Sporadic (nodular) goiter
o Pathogenesis remains unknown.
o Etiologies: Mild dietary deficiency of iodine, slight impairment of hormone synthesis, increased iodide
clearance by the kidneys, presence of thyroid-stimulating immunoglobulins, and increased production of
insulin-like GF I
o Incidence: 3–5% clinically and 50% at autopsy.
o Degree of thyroid nodularity is directly related to the duration of the disease.
o Treatment:
If mild, no treatment.
Suppressive therapy with exogenous thyroid hormones is only moderately effective
Symptomatic: bilateral subtotal thyroidectomy
Table 2. Differential diagnosis: nodular hyperplasia vs true adenoma
Table 2 Differential diagnosis: nodular hyperplasia vs true adenoma
Adenoma Nodular hyperplasia
Single Lesion is almost always one of many nodules
Totally surrounded by a capsule Encapsulation is incomplete
Dissimilar from the remaining parenchyma Follicular size is variable
Compresses the adjacent tissue No compression of the adjacent parenchyma.
Composed mainly of follicles that are smaller than Some or all of the follicles are larger than those in the
those of the normal gland surrounding gland
TUMORS
The majority of clinically apparent thyroid neoplasms are primary and epithelial.
Three major categories:
1. Tumors exhibiting follicular cell differentiation
2. Tumors exhibiting C-cell differentiation
3. Tumors exhibiting follicular and C-cell differentiation.
Lesions in the first category comprise more than 95% of the cases, the remainder being largely made up by tumors
in the second category.
EPITHELIAL TUMORS – SPECIFIC TYPES
FOLLICULAR ADENOMA
o benign encapsulated tumor that shows evidence of follicular cell differentiation
o lacks:
1. evidence of capsular, vascular or any other type of invasion; and
2. The nuclear features of the papillary family of neoplasms.
o most common thyroid neoplasm
o Most patients are euthyroid adults who initially have a thyroid lump
o The large majority of ‘hot’ nodules are benign
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 4
o elevated circulating levels of thyroglobulin,
o few are associated with clinical hyperthyroidism: toxic or Plummer adenomas
o The thyroid outside hyperfunctioning nodules: contains intraluminal crystals of calcium oxalate
o Adenomas are almost always solitary
o surrounded by a thin capsule that is grossly and microscopically complete
o may exhibit a variety of patterns
a. normofollicular (simple),
b. macrofollicular (colloid),
c. microfollicular (fetal), and
d. trabecular/solid (embryonal)
o Mitoses are rare or absent
o Secondary degenerative changes:
Hemorrhage
Edema
Fibrosis
Calcification
bone formation
cystic degeneration
o muscular cushions: the vessels in the capsule show prominent focal thickenings of their wall
o microscopic appearance of a follicular adenoma and its activity:
a. hyperfunctioning (hot) adenomas
more cellular and their cells have more abundant cytoplasm
decreased nucleocytoplasmic ratio
have activating mutations of TSHR or of its downstream effector GNAS1
b. Nonfunctioning (cold) tumors
o Chromosomal translocations
identified in approximately 10% of FA
a. Chromosome 19q13, with the breakpoint at the ZNF331 gene locus,
b. chromosome 2p21, with the breakpoint at the thyroid adenoma associated (THADA) gene
locus
Differential diagnosis:
1. nodular hyperplasia
2. minimally invasive follicular carcinoma,
3. follicular variant of papillary carcinoma
Treatment
o Standard therapy: removal by lobectomy
o Levothyroxine: Suppression of the nodule
o 131I : toxic adenoma
PAPILLARY CARCINOMA
General features:
o most common type of thyroid malignancy.
o Females are more affected than males
o mean age at the time of initial diagnosis: 40 years
o > 90% of thyroid malignancies in children
o 5–10%: (+) history of irradiation exposure to the neck
Gross features
o The size of the primary tumor ranges from microscopic to huge.
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 5
o A very high proportion of thyroid cancers measuring less than 1 cm in diameter are of papillary type.
o solid, whitish, firm, and clearly invasive;
o <10% are surrounded by a complete capsule
Microscopic features
o contains numerous true papillae
o papillae are usually complex, branching, and randomly oriented,
o with a central fibrovascular core and a single or stratified lining of cuboidal cells
o stroma
edematous or hyaline
may contain lymphocytes, foamy macrophages, hemosiderin, adipose tissue
o follicles tend to be irregularly shaped, often tubular and branching
o Nuclear features (which we will herein refer to as PTC-type nuclei) consist of:
1. Ground glass (optically clear) nuclei
nucleolus is usually inconspicuous and pushed against the nuclear membrane, which appears
thickened
2. Nuclear pseudoinclusions
invaginations of the cytoplasm
appear as sharply outlined (nuclear membrane-bound) round acidophilic vacuoles
3. Nuclear grooves.
occur in oval or spindle nuclei
4. Nuclear microfilaments.
o Mitoses are very scanty or absent
o Over half show extensive fibrosis
o Elastic tissue is usually abundant in the tumor stroma
o Psammoma bodies are seen in approximately half of the cases
o contain a bland-looking spindle cell component;
o Lymphocytic infiltration
Electron microscopic features
o most distinctive feature: highly indented nuclear membrane, with formation of pseudoinclusions and
multilobation.
o cytoplasm is rich in mitochondria, lysosomes, and intermediate filaments.
Histochemical and immunohistochemical features
o reactive for pan-keratin stains
o usual profile: CK7+/CK20
o Potentially greater diagnostic importance: stain for cytokeratin 19 and keratin demonstrated with 34ßE12.
o Reactive for thyroglobulin and TTF-1: Most specific markers
o The luminal surface of the tumor cells is covered by a glycoproteinaceous material that reacts positively
with mucin stains (such as Alcian blue) and EMA
Molecular genetics features
o Activation of the mitogen-activated protein kinase (MAPK) pathway
consequence of three distinct events:
1. gene rearrangements (RET/PTC or the less common TRK rearrangements)
2. BRAF
3. RAS activating mutations
o Rearrangements
occur in 20–40% of papillary carcinomas,
majority involve RET
1. NTRK1
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 6
a gene encoding a transmembrane tyrosine kinase receptor that binds the nerve growth factor
much less common than RET/PTC rearrangements: 5% of Pca
The mechanisms responsible for NTRK1 activation are the same as those described for RET: intra- or
interchromosomal recombination of the NTRK1 locus at 1q22, fusion of NTRK1 to heterologous
genes producing chimeric oncogenes, aberrant expression, and ligand independent activation of the
NTRK1 tyrosine kinase.
2. BRAF
30–70% of Pca
most common molecular alteration
a serine–threonine kinase in the MAPK pathway activated by RAS,
represents the most important isoform in follicular cells
The vast majority (>90%) of BRAF mutations:
thymidine to adenine transversions in the nucleotide 1799 (T1799A) of exon 15 that cause a
valine to glutamate substitution at residue 600 (V600E) of the protein activation loop
3. RAS
In the thyroid, RAS mutations are a marker for follicular-patterned thyroid lesions, being typically
associated with follicular adenomas and carcinomas
Spread and metastases
o Extrathyroidal extension into the soft tissues of the neck
o Involvement of cervical lymph nodes is very common (particularly in young patients), and it may be the
first manifestation of the disease.
o Blood-borne metastases are less frequent
o most common site is the lung
Prognosis
o The overall survival of patients with papillary carcinoma is excellent.
FOLLICULAR CARCINOMA
Generalities and molecular genetic features
o any malignant thyroid tumor exhibiting evidence of follicular cell differentiation.
o Poorly formed follicles, cribriform areas, or trabecular formations may be present,
o Mitotic activity and nuclear atypia are usually seen
o Psammoma bodies are absent,
o Immunohistochemically:
reactive for thyroglobulin, TTF-1, low molecular weight keratin, EMA, and basement membrane
components such as laminin and type IV collagen.
o At a molecular genetic level, follicular carcinomas share with follicular adenomas a common tumorigenic
pathway, characterized by aneuploidy and by the frequent occurrence of RAS mutations
o The most common oncogenic mutations are those that involve RAS
o almost always solitary and only exceptionally occult.
o Metastases are usually blood-borne
most common sites are lungs and bone
can be seen in kidney and skin.
HÜRTHLE CELL (ONCOCYTIC) TUMORS: THE ONCOCYTE
o common denominator for all the tumors
o cytoplasmic granularity is due to the accumulation of mitochondria,
o Secondary clearing is not uncommon, usually due to mitochondrial swelling.
o Immunohistochemically,
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 7
reactivity for thyroglobulin (although to a lesser degree than non-oncocytic follicular cells), many
mitochondrial antigens, glucose transporter 4 (GLUT-4), and keratin
CK14 is emerging as a selective marker for these cells
also immunoreactive to CEA, S-100 protein and HMB-45
o The total amount of mitochondrial DNA (mtDNA) is increased
o Most patients are adults, and there is a predominance of females.
o Grossly, the tumors are:
solid, tan, and well vascularized
well encapsulated throughout;
invasive tumors tend to grow into the parenchyma in a multinodular fashion that can be very
deceptive in that it can be underinterpreted as nodular hyperplasia.
o Microscopically:
the pattern of growth may be follicular, trabecular/solid, or papillary.
follicles, when large, are separated by long and thin fibrovascular septa that simulate papillae when
cut tangentially.
o Another diagnostic trap:presence of inspissated intraluminal colloid with concentric laminations
o Nuclei: pleomorphism and prominent nucleoli, with occurrence of isolated bizarre forms
o Immunohistochemically: reactivity for thyroglobulin
o capsular and/or blood vessel invasion should be used as the main criterion for malignancy.
o tendency to undergo massive infarct-type necrosis, often following fine needle aspiration.
o Hürthle cell adenomas are almost always cured by excision.
o carcinomas are rather aggressive neoplasms, with a 5-year mortality rate ranging between 20% and 40%
o Metastases: mainly in lungs and bone and less commonly in cervical node
o Older patient age, large tumor size, extrathyroidal extension, extensive vascular invasion, and metastases
represent unfavorable prognostic factors
CLEAR CELL TUMORS
o consequence of a variety of mechanisms, which include cytoplasmic vesicles (of mitochondrial, reticulum
endoplasmic, or Golgi origin) and accumulation of glycogen, lipid, thyroglobulin, or ‘mucin’
o Hürthle cell tumor
most prone to undergo secondary clear cell changes,
result of vesicular swelling of mitochondria
o can also occur in follicular adenomas and carcinomas (usually because of vesicles of either mitochondrial
or granular endoplasmic reticulum derivation), papillary carcinoma (usually because of glycogen
accumulation), undifferentiated carcinoma (also the result of glycogen overload), and – exceptionally –
medullary carcinoma.
o Except for the latter, thyroglobulin stain is usually positive in these neoplasms, although sometimes in a
focal and faint fashion.
o it occurs more frequently in carcinomas than in adenomas
o A peculiar variant: signet ring type
formation of variously sized cytoplasmic vacuoles results in a configuration reminiscent of signet ring
cells or lipoblasts
Most are adenomas
Immunohistochemically,
Vacuoles: contain intracellular thyroglobulin
Stroma: heavily hyalinized and with punctate calcification, suggesting that the signet ring
change may be of degenerative nature and the expression of an arrest of folliculogenesis.
found to react positively with mucin stains
o Differential diagnosis: parathyroid neoplasms and metastatic renal cell carcinoma
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 8
both of these lesions can be intrathyroidal, whereas thyroid clear cell tumors can occur in ectopic
locations.
o can also occur in non-neoplastic thyroid disorders, including Hashimoto thyroiditis and
dyshormonogenetic goiter.
Squamous Cell, Mucinous, And Related Tumors
Mucoepidermoid carcinoma
o low-grade thyroid neoplasm combining foci of squamous change with mucin production and lacking
immunoreactivity for thyroglobulin
o originate from solid cell nests, which in turn are thought to be of ultimobranchial body derivation. [723,734]
o The clinical features:
presence of ground glass nuclei and psammoma bodies
P-cadherin neoexpression and the marked abnormalities of the E-cadherin/catenins complex
o Distinctive variant: sclerosing mucoepidermoid carcinoma with eosinophilia
arises in thyroid glands affected by Hashimoto thyroiditis, often of the fibrous type
Microscopically,
strands and nests of squamous tumor cells with mild to moderate pleomorphism
infiltrating a dense fibrohyaline stroma.
constant and often striking infiltration by eosinophils
Immunohistochemically
strong reactivity for keratin, but only focally if at all for TTF-1,
none for thyroglobulin
The clinical course is generally indolent, but cases with distant metastases and aggressive behavior
have been reported.
Lymph node metastases may simulate microscopically Hodgkin lymphoma.
Poorly Differentiated Carcinoma: Insular Carcinoma
o occurs in an older group than the well-differentiated tumors
o grossly invasive
o Microscopically
nesting (‘insular’) pattern of growth,
solid to microfollicular arrangement,
small uniform tumor cells,
variable mitotic activity
fresh tumor necrosis resulting in a peritheliomatous pattern
o Immunohistochemically
reactive for thyroglobulin and TTF-1 but not for calcitonin
focal reactivity for neuroendocrine markers
o Cytologic features
high cellularity, necrotic background, low grade of atypia, nests, trabeculae and microfollicles, and
cytoplasmic vacuoles.[751,764]
generally aggressive, with a high incidence of both nodal and blood-borne metastases.
o Complex karyotypic alterations and aneuploidy are frequent with a median number of chromosomal DNA
alterations detectable by CGH
o Inactivating TP53 mutations occur in approximately one-fourth of cases, high enough to link loss of p53
o RAS mutations are frequently detected have been associated with poor prognosis and with the less
differentiated components of the tumor
Undifferentiated Carcinoma: Anaplastic Carcinoma
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 9
o elderly patients
o rapidly growing mass associated with hoarseness, dysphagia, and dyspnea.
o Extrathyroidal extension is encountered at the time of initial presentation
o Grossly, a highly necrotic and hemorrhagic solid tumor mass is seen replacing large portions of the organ
o Microscopically
1. Squamoid
it does not make follicles, papillae, or even trabeculae or nests, but the tumor still retains an
unmistakable epithelial appearance on morphologic and immunohistochemical grounds.
2. Sarcomatoid: spindle cell and giant cell
exhibit a fascicular or storiform pattern of growth, heavy neutrophilic infiltration, prominent
vascularization, and divergent differentiation into bone, cartilage, and skeletal muscle.
Osteoclast-like multinucleated giant cells may be present
o Common and diagnostically useful features:
palisading at the necrotic edges
tendency to invade the wall of veins, replacing the normal smooth muscle
o Immunohistochemically,
the most useful marker for confirming the epithelial nature is keratin (expressed in 50–100% of
cases)
Vimentin is consistently present in the spindle cell component
scattered stromal (basement membrane-related) reactivity for laminin,
focal EMA and CEA positivity may be found, especially in the squamoid type.
TTF-1 is generally negative
o Gene mutations
typically aneuploid, have complex karyotypes by conventional cytogenetics and high rates of
chromosomal DNA alterations detected by CGH
Inactivating TP53 mutations are found in the majority of cases
have been correlated with widespread nuclear accumulation of p53 throughout the tumor.
Stabilizing mutations of the CTNNB1 gene coding for ß-catenin prevent its cytoplasmic degradation
and activate Wnt signaling by allowing ß-catenin to localize to the nucleus.
RAS mutations are common
RET/PTC and PAX8/PPAR? are not usually found
The PI3K/PTEN/AKT pathway is altered by loss of function PTEN mutations or by activating mutations
of the PIK3CA gene
o The evolution of all types of undifferentiated thyroid carcinoma is very rapid, with massive growth in the
neck and infiltration of the ribbon muscles, esophagus, trachea, skin, and even contiguous bones.
o Tracheal extension may simulate a primary tracheal tumor
o Nodal and distant metastases are also common
o Mortality rate is over 95%
o Mean survival is less than 6 months
o Immediate cause of death is usually involvement of vital structures in the neck
MEDULLARY CA
o composed of C (parafollicular) cells
o mostly located in the midporiton or upper half of the gland
o described also as
solid CA w/ amyloid stroma
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 10
hyaline CA
C-cell CA
o medullary microCA - greatest diam of 1cm or less
o gross: solid, firm, nonencapsulated, but relatively well circumscribed
o classic microscopic presentation:
solid prolif of
round to polygonal cells of
granular amphophilic cytoplasm and
medium sized nucleus
separated by highly vascular stroma
o gray to yellowish cut surface
o enveloped medullary CA - enveloped by continous fibrous capsule
o patterns of growth
carcinoid-like
paraganglioma -like
trabecular
glandular (tubular and follicular)
pseudopapillary
o stroma
scanty
hemorrhagic
ossified
edematous
o tumor cells
plasmacytoid - w/ nuclear peripheralization
spindle-shaped
oncocytic - resemblance to Hürthle cell neoplasms of follicular cell derivation
squamoid
squamous
bizarre - anaplastic or giant cell-type
o diagnosis - suspected if
cells are amphophilic
tumor is divided into nests by sharply outlined fibrous bands
o cytologic features: FNA preps
eccentric nuclei
neuroendocrine-type chromatine
inconspicuous nucleoli
bi- and multinucleated cells
ill-defined cell borders
clean background
*amyloid mat’l
o histochemical features
cytoplasmic dense-core secretory granules - argyrophilic w/ Grimelius stain
(+) w/ mucin stain
o immunohistochemical features
tumor cells are reactive for calcitonin
(+) for CEA
generally (-) for thyroglobulin
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 11
Hereditary medullary CA and C-cell hyperplasia
2 forms of medullary CA
o sporadic
80%
adults (mean age, 45)
almost always solitary
presents as thyroid mass - cold on thyroid scan
sometimes accompanied by intractable diarrhea or Cushing syn
o inherited
AD
young age (mean age, 35)
multiple, bilateral
invariably accompanied by C-cell hyperplasia
diagnosed at microCA stage
almost all cases of medullary CA in children
gene involved is the RET gene on chromosome 10q11.2
occurs in 3 settings
multiple endocrine neoplasia (MEN) - medullary CA is usually the first manifestation
type 2a
type 2b
isolated (familial medullary thyroid CA syn, FMTC)
C-cell hyperplasia
o precursor lesion
o typically in the central part of the lateral lobes
o indicator: >6 cells per per thyroid follicle
o nodular form - only definite precursor for the hereditary type of medullary CA
o hyperplastic C cells - greater immunoreactivity with
CEA than N cells
calcitonin than medullary CA
elevated serum calcitonin and CEA; (+ chromogranin A for those w/ medullary CA)
o DDx
early medullary CA (microCA)
nesting expansile pattern
destruction fo follicular BM
diminished calcitonin immunostaining intensity
reactive or physiologic C-cell hyperplasia
immediate periphery of thyroid neoplasms
in assoc w/ lymphocytic thyroiditis
2ndary hyperPTH
o spread and metastasis
local: cervical and mediastinal LNs
distal: lung, liver & skeletal sys
more common in sporadic and MEN2b than 2a
o tx and prognosis
primary: surgical
total thyroidectomy - impt for the familial form
cervical lymphadenectomy
persistent or recurrent elevation of serum calcitonin after surgery indicates tumor
persistence or relapse
good prognostic fxs:
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 12
young age
female
familial setting
tumor size
tumor confinement to the gland
poor prognostic fxs
of sporadic cases
older age at detection
more advance tumor stage at dx
as to immunoreactivity
poor calcitonin reactivity
esp if w/ increased CEA reactivity
excellent prognosis: small medullary CA in phrophylactic thyroidectomies
greater deg of aggressiveness expected in those w/
high mitotic activity
necrosis
squamous patern
w/ desmoplastic rxn
small cell type
Other Neuroendocrine Tumors
o Medullary (C-cell) adenoma - encapsulated variants of medullary CA
o Mixed medullary-follicular CA - morphologic immunoreactivity features of medullary (calcitonin) and
follicular neoplasm (thyroglobulin) coexist
o Mixed medullary-papillary CA
o Paraganglioma
reacts for panendocrine markers
(-) for calcitonin and thyroglobulin
useful feature: presence of S-100 protein-(+) sustentacular cells at the periphery of the ‘Zellballen’
o Small cell (neuroendocrine) CA
morphologically identical to the homonymous lung tumor in the thyroid
small cell variants of medullary CA
Epithelial Tumors
o geographical features
correlation bet iodine def and increased incidence of thyroid CA of both follicular and
undifferentiated types
iodine def - suggested modulating agent for RAS oncogene mutations
papillary CA
predominant type in areas w/o iodine def
freq increased in regions w/ high iodine uptake
o thyroid neoplasia in childhood
most are benign
either follicular adenoma or nodular hyperplasia
rank
papillary CA
majority of cases
extensive solid and/or squamous areas
assoc w/ high freq of cervical node metastases
overall prognosis is excellent
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 13
hereditary form of medullary CA
Hürthle cell neoplasms
o thyroid neoplasia and radiation exposure
MC result of low-dose therapeutic radiation of the thyroid gland
benign nature
nodular hyperplasia
lymphocytic thyroiditis
fibrosis
inc incidence of CA, majority of the papillary type
high-dose radiation exposure
thyroid CA, particularly the papillary type and with RET/PTC rearrangement
differentiation pattern among children
follicular - exposed at a young age
papillary - exposed at a later age
RET/PTC3 - assoc w/ papillary CAs that are more aggressive
larger tumor size
higher stage
solid architecture
o familial incidence
5% of thyroid CAs
of nonmedullary type
2 groups
predominance of nonthyroid tumors
familial adenomatous polyposis including Gardner syn (colonic polyposis)
Cowden/PTEN hamartoma tumor syn
Carney complex type I
McCune-Albright syn
Werner syn (adult progeria)
MEN1
predominance of non-thyroid tumors - pure familial papillary thyroid CA (fPTC)
w/ or w/o oncocytic features
w/ renal cell CA
w/ nodular hyperplasia
o solitary solid nodule, evaluation of
4x more common in females
majority are benign, most are not even neoplastic
fxs to consider
age - malignancy higher in children and the elderly
sex - malignancy higher in males
Hashimoto thyroiditis
neck irradiation - likelihood of malignancy higher if w/ hx of irradiation to the neck in infancy
number - solitary are more likely to be malignant than multiple ones
rate of growth - rapid enlargement of a long-standing nodule may signify either
an undifferentiated (anaplastic) transformation or
development of hemorrhage w/in the nodule
assoc ipsilateral adenopathy - strongest clinical indicator of malignancy
function - hyperfunctioning (‘toxic’) and/or hot on thyroid scan are much less likely to be malignant
ultrasonography - cystic nodules are less likely to be malignant than solid ones
CT and MRI - MRI is superior to CT for evaluation of metastatic, retrotracheal, or mediastinal lesions
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 14
serum thyroglobulin levels
elevated w/ papillary and esp follicular CA - for monitoring after removal of
N w/ medullary or undifferentiated CA
o core needle biopsy and FNA
CNB
helpful in diffuse dses and confirming the dx of an advanced malignant neoplasm
DDx bet a benign and malignant is usually impossible
but is able to demonstrate 2 main histologic criteria of malignancycapsular and vascular
invasion
FNA
popular
quick and inxexpensive
minimal risk of complications
partial or complete infarction of the tumor particularly w/ Hürthle cell tumors, and
may result in transient elevation of serum thyroglobulin
hemorrhage & thrombosis w/c may lead to pseudoangiosarcomatous papillary
endothelial hyperplastic changes
dev’t of thyrotoxicosis when carried out in cystic lesions
suitable for immunohistochemical eval
sensitivity and specificity over 90%
initial test in the eval of any thyroid nodule
main difficulty - identification of well-differentiated follicular CA
o frozen section
specimen either from
an area of extrathyroidal invasion or
metastatic cervical node
MC specimen received is a lobectomy - in majority of the cases, the DDx will be between
a dominant nodule of nodular hyperplasia
adenoma, and
CA
difficulty in the distinction bet a
dominant nodule of nodular hyperplasia
follicular adenoma
minimally invasive follicular CA
variant of papillary carcinoma that is both follicular and encapsulated
ground glass nuclear feature of papillary carcinoma may not show
most useful in lesions interpreted by FNA as ‘suspicious for papillary carcinoma’
diagnostic adjunct
o presence of thyroid tissue outside gland
normal or abnormal
ectopic thyroid tissue resulting from faulty embryogenesis - MC are
thyroglossal duct cyst and
lingual thyroid
hyperplastic thyroid tissue in Graves disease
mechanical implantation
sequestered thyroid nodule
aka parasitic or accessory nodule
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 15
peripherally located thyroid nodule in w/c either the anatomic connection with the main gland
is lost or missed by the surgeon
usually an expression of nodular
hyperplasia or
Hashimoto thyroiditis
dx criteria
reside in the same fascial plane as the thyroid gland
unassociated with LNs
same or similar histologic appearance as the main gland
thyroid tissue within cervical lymph nodes
may be the result of two unrelated processes
most cases represent metastases of clinically undetected thyroid carcinomas, nearly
always papillary
normal follicles within nodes
© typically presents as a small conglomerate of follicles lacking all the attributes
of papillary carcinoma and limited to the periphery of one or two nodes
© thyroid tissue replacing most of the node and/or involving several nodes is
likely to be metastatic CA
as a component of teratoma
may appear normal or hyperplastic
struma ovarii - ovarian teratomas composed predominantly or exclusively of thyroid
tissue
o treatment
mostly surgical
nodule limited to one lobe: lobectomy (with or without isthmusectomy)
initial approach
adeq for follicular adenoma, including Hürthle cell adenoma
subtotal thyroidectomy - for most minimally invasive follicular CAs and papillary CAs
total thyroidectomy
followed by radioactive iodine admin - MC therapy for differentiated thyroid CA
for the high-risk group of
papillary CAs
widely invasive follicular CAs
poorly differentiated CAs, and
medullary CAs (particularly familial)
radical neck dissection - recommended for medullary CA
external radiation therapy - for incompletely excised tumors
o prognosis
most impt clinical and pathologic factors
age
sex
tumor microscopic type
tumor microscopic grade
tumor stage
survival rates:
low risk
men under 40
women under 50
high risk - others
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 16
o majority of deaths from thyroid CAs result from
undifferentiated
poorly differentiated
Hürthle cell, and
medullary tumors
Lymphoid Tumors and Tumor-like conditions
Primary malignant lymphoma of the thyroid
o MC seen in adult or elderly females
o thyroid enlargement
rapid
can lead to tracheal or laryngeal compression
o euthyroid
o one or more cold nodules on thyroid scan
o gross: solid white cut surface with a fish-flesh appearance
o microscopic
majority of the diffuse large B-cell type
low-grade lymphomas composed of small or ‘intermediate’ lymphocytes, having either a diffuse or a
nodular (follicular) growth
belong to the MALT-type category (‘marginal zone B-cell lymphomas’) - result of colonization of the
follicles by the tumor cells
lymphoepithelial lesions
important diagnostic finding
packing of follicular lumina by lymphoid cells
high proportion arise in a background of lymphocytic or Hashimoto thyroiditis
localization
restricted to the thyroid
spread to the soft tissues by direct extension, or
involve the regional nodes.
prognosis is better for marginal zone B-cell lymphomas than for diffuse large BCL
tx
thyroidectomy followed by adjuvant therapy
treatment failures result from distant recurrences MC in the GIT
Plasmacytoma of thyroid
o component of widespread myeloma
o entirely composed of plasma cells of various degrees of maturity
o tumors with a lymphoid component - malignant lymphoma
o distinguished from plasma cell granuloma
non-neoplastic condition
mature plasma cells seen admixed with other inflammatory cells
in a fibrotic background
Langerhans cell histiocytosis
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 17
o histiocytosis X / eosinophilic granuloma
o occurs w/ lymphocytic/Hashimoto thyroiditis
Extramedullary hematopoiesis - in pxs with myelofibrosis
Mesenchymal Tumors
Benign mesenchymal tumors - severe hypothyroidism can accompany infantile hemangioma of liver and other
sites as a result of degradation of thyroid hormone in the tumor tissue by type 3 iodothyronine deiodinase activity
Sarcomas
o leiomyosarcomas - in a setting of immunodeficiency in association with EBV
o most sarcoma-like thyroid tumors are of the spindle or giant cell types of undifferentiated CA
o thyroid angiosarcoma
exhibit attributes of angiosarcoma
anastomosing vascular channels
Weibel–Palade bodies
immunoreactivity for endothelial cell markers, and
tendency to produce hemorrhagic pleuropulmonary metastases
keratin-positive epithelioid angiosarcomas - with
epithelioid morphology and
immunoreactivity for keratin
Other Primary Tumors and Tumor-like Conditions
Teratomas of thyroid
o usually in neonates, infants or children
o majority: cystic and benign
o neural tissue - predominant component
o can lead to obstruction of the airway
Neuroblastomas - distinguished from the much more common teratomas with immature neural elements
Amyloid tumor (‘amyloid goiter’)
o unilateral or bilateral
o commonly foreign body-type reaction.
o amyloid deposits often accompanied by mature adipose tissue
Metastatic Tumors
o occur in
carcinomas of pharynx, larynx, trachea, or esophagus
metastatic lesions from adjacent cervical LNs
o majority: squamous cell type
o metastases in the thyroid
MC sites for the primary tumor: skin (melanoma), breast, kidney and lung
MC solitary
o metastatic renal cell CA
rare for metastases to the thyroid to simulate clinically a primary thyroid neoplasm
can present as a thyroid mass in the absence of renal symptoms
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 18
features of diagnosis
multiplicity of the nodules
optically clear (as opposed to finely granular) cytoplasm
sinusoidal-type blood vessels
intraluminal fresh hemorrhage (‘bloody glands’), and a
large amount of cytoplasmic glycogen and fat
Parathyroid Glands
Normal Anatomy
o Composed of 4 small oval resilient glands
o Located behind the thyroid gland, one at each end of the upper and lower poles, usually in the capsule that
covers the lobes of the thyroid.
o Sometimes they are embedded in the thyroid gland
o Average of 4x 3x 1.5 each gland
o Total weight of about 0.4g
o Any individual gland with an excess of 50mg represents an enlargement
o Color: varies from reddish brown to light tan to yellow, depending on fat content, which in turn depends
on age, nutrition, and activity of the individual.
Embryology
The 2 pairs of the parathyroid glands are derived from the branchial (pharyngeal) pouches:
a. Superior glands
fourth branchial cleft and descends into the neck with the thyroid gland during embryonic life.
b. Inferior glands
third branchial cleft and descends into the neck with the thymus.
Normal Histology
A. Chief Cells
o Secrete PTH
measures 6–8 µm in diameter
Polyhedral cells
has a centrally located nuclei
a moderate amount of pale granular cytoplasm.
variable amounts of glycogen particles and secretory droplets
B. Oxyphil Cell
o appear after puberty
o larger than chief cells
o has a more abundant cytoplasm, which is deeply granular and acidophilic.
o there are many mitochondria but few secretory granules
o These oxyphilic cells are often present in the form of nodular collections.
C. Transitional oxyphil cells
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 19
o intermediate between chief cells and oxyphil cells
D. Water-clear cells
o rarely if ever seen in the normal gland
o characterized by abundant optically clear cytoplasm and sharply defined
o cell membranes
o cytoplasm is packed with glycogen
E. Transitional water-clear cells
o intermediate between chief cells and water-clear cells
Both types of transitional cell are more common in hyperfunctioning than in normal glands.
Normal Physiology
o The parathyroid glands mediate their endocrine function through the production of PTH.
o The most important physiologic actions of PTH are:
a. increased renal excretion of phosphate
b. increased renal tubular reabsorption of calcium
c. increased intestinal absorption of calcium
d. direct effects in bone ( increase in the number of osteoclasts and an apparent increase in their
phagocytic activity, with a resulting resorption of bone tissue)
Adenoma
Generalities
o Accounts for most cases of hyperparathyroidism
o Occur more in women than men 3:1
o They can develop at almost any age, but most occur in patients in the fourth decade
Pathology
o Circumscribed, grayish brown, solitary mass
o Their size and weight vary greatly, with the majority being too small to allow detection on palpation of the
neck.
o Some may be recognizable only microscopically (‘microadenomas’).
o usually oval, may show slight lobulation, and are surrounded by a thin connective tissue capsule.
o Foci of hemorrhage, calcification, and cystic change may occur.
Microscopic features
o the tumor is encapsulated and very cellular
o chief cells usually predominate with a rich capillary network
o Combinations of chief cells, oxyphil cells, water-clear cells, and transitional elements are common.
o Mitoses are usually absent
o pattern of growth is generally diffuse, but it may be nesting, follicular, or pseudopapillary
o the other parathyroid glands have a normal or atrophic appearance.
o Adenomas have the presence of a microscopically normal second gland which is not seen in chief cell
hyperplasia.
o In contrast to normal chief cells, large quantities of glycogen and secretory vacuoles can be seen
simultaneously.
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 20
Histochemical and immunohistochemical features
o Immunohistochemically
a. (+) reactivity for PTH
b. (+) various types of keratin
c. (+) neuroendocrine markers (such as chromogranin and neuron-specific enolase
o Histochemically
The intensity of the PTH staining tends to be weaker in the adenoma than in the peripheral rim of
residual normal gland.
The adenoma cells express neurofilament, an intermediate filament not found in normal
parathyroid cells
Adenoma variants
a. Oxyphil adenoma
o parathyroid adenomas composed entirely or almost entirely of oxyphil cells
o most oxyphil adenomas are non-functioning
o The main ultrastructural feature of these cells is the packing of the cytoplasm by mitochondria.
b. Lipoadenoma
o glandular elements are associated with abundant mature adipose tissue, the latter sometimes
exhibiting myxoid changes
o parathyroid lipohyperplasia, parathyroid hamartoma, parathyroid adenoma with myxoid stroma, and
parathyroid myxoadenoma.
o Most cases are functioning.
Chief cell hyperplasia
o a condition accompanied by increased production of PTH, can be primary or secondary to impairment of
renal function or chronic malabsorption.
a. Primary chief cell hyperplasia
o all glands are enlarged (sometimes weighing 10 g or more)
o tan to reddish color.
o The upper glands tend to be larger than the lower ones
o nodularity, fibrous septation, acinar formation, and giant nuclei are more prominent
Pseudoadenoma
o only one gland is visibly enlarged and nodular, whereas the others are nearly normal in size.
o can be confused grossly with an adenoma
Occult Hyperplasia
o all four glands appear normal in size but are hyperplastic on histologic examination.
Microscopically:
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 21
o the predominant element is the chief cell
o pattern of growth may be diffuse or nodular
o Diffuse: more common among young patients
o Nodular: more common in the elderly
o Glands with nodular chief cell hyperplasia tend to be asymmetric, with a variable cellular arrangement
and a high proportion of oxyphil cells.
o The ultrastructural features are qualitatively similar to those seen in adenoma and are indicative of a
hyperfunctioning state.
Parathyromatosis
o innumerable microscopic foci of hyperplastic parathyroid tissue found in the neck in association with
primary chief cell hyperplasia of the four glands, in the absence of previous surgery.
o responsible for some cases of recurrent hyperparathyroidism after technically successful surgical therapy.
b. Secondary chief cell hyperplasia
o At one end is the normal-sized gland that is recognized as hyperplastic only because of its tan to reddish
color and the microscopic hypercellularity and at the other, there is the gland measuring up to 2 cm and
weighing up to 6 g.
o there is an inverse correlation between the size of the gland and the mean serum calcium level
o chief cells predominate, but there may also be increased numbers of oxyphil and transitional oxyphil cells
that form nodular collections.
o the number of oxyphil cells is higher than in the primary form
c. Water-clear cell hyperplasia
o In contrast to chief cell hyperplasia, water-clear cell hyperplasia shows no familial incidence and is not
associated with multiple endocrine neoplasia.
o characterized by extreme enlargement of all parathyroid tissue so that the total weight of the glands may
exceed 100 g.
o the superior glands are distinctly larger than the inferior.
o glands may coalesce so that two glands appear as one.
o soft and have a typical chocolate brown color
o Cysts and hemorrhages have been observed.
o There is formation of pseudopods that may extend a considerable distance from the main mass of the
gland.
o A close correlation exists between the weight of the parathyroid tissue and the severity of the symptoms.
o Microscopically, the most characteristic feature is the presence of cells with optically clear cytoplasm
throughout the lesion.
o combination of hyperplasia and hypertrophy.
Parathyroid Carcinoma
o typically presents with hyperparathyroidism
o skeletal diseas present in 73% of the patients and renal disease in 26%.
o are said to be more aggressive.
o absence of function may be caused by the lack of conversion of the preparathormone to the biologically
active compound.
o may coexist with chief cell hyperplasia and with adenoma
Clinical features suggestive of parathyroid carcinoma in a hyperparathyroid patient include:
a. very high values of serum calcium or PTH
b. a palpable cervical mass
c. vocal cord paralysis
d. recurrence of hyperparathyroidism a short time after surgery
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 22
A parathyroid tumor should be suspected of being carcinoma if:
a. it is hard
b. surrounded by a dense fibrous reaction
c. adherent to or infiltrating adjacent structures
o Microscopically, carcinomas differ from adenomas:
a. trabecular arrangement
b. dense fibrous bands (present in 90% of the cases)
c. spindle shape of the tumor cells
d. presence of mitotic figures (in 81%)
e. capsular invasion (in 67%)
f. blood vessel invasion (in 12%)
Other lesions
Parathyroid cysts
o usually arise from the lower glands but can be located in the upper region of the neck or in the
mediastinum
o no symptoms other than those related to pressure.
o mean diameter is 4 cm.
o lined by cuboidal or low columnar epithelial cells and contain parathyroid tissue in their wall.
o Heterotopic salivary gland tissue can be found around the cyst.
Amyloidosis
o often involves the parathyroid gland, in both primary and ‘reactive’ forms of the disease
Langerhans cell histiocytosis
o involving simultaneously the parathyroid and thyroid glands
Metastatic carcinoma
o very rare, but papillary thyroid carcinoma can invade them in continuity with the main tumor.
Hyperparathyroidism
o any condition associated with the persistent production of parathyroid hormone
a. Primary hyperparathyroidism
o there is no evidence of previous parathyroid stimulation by chronic renal or intestinal disease.
o The pathologic changes in the gland may be those of adenoma, chief cell hyperplasia, carcinoma, or
water-clear cell hyperplasia.
o Carcinoma: < 4% of cases
o large majority of cases are caused by either adenoma or chief cell hyperplasia
o It is usually seen in adults but can also be found in children
o Familial setting, the abnormality is usually chief cell hyperplasia
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 23
The typical case of primary hyperparathyroidism is biochemically characterized by:
a. hypercalcemia
b. hypophosphatemia
c. lowering of the renal phosphate threshold
d. hypercalciuria
e. elevated levels of immunoreactive PTH
f. elevated concentrations of 1,25-dihydroxyvitamin D
g. enhanced excretion of nephrogenous cyclic AMP
According to the clinical presentation, patients with primary hyperparathyroidism have been traditionally classified
into:
1. those with osseous manifestations
2. those with renal manifestations
3. those with neither of the foregoing
Skeletal changes:
o always generalized
o Initial lesions: decrease in bone density
o In time, they may become very extensive and lead to deformities and fractures.
o Osteitis fibrosa cystica or Recklinghausen disease- full-blown osseous manifestations of
hyperparathyroidism
o They present radiographically as expansile, multilocular masses.
o The jaw is the preferred location, and this may be the first clinical manifestation of the disease.
o Grossly, there is an alternation of solid and cystic areas; the latter often have a brown color because of
the accumulation of abundant hemosiderin, hence the term brown tumor sometimes used for them.
Microscopically, there is a combination of osteoblastic and osteoclastic activity, often associated with cyst
formation and clusters of hemosiderin-laden macrophages.
Renal changes
o include renal stones, nephrocalcinosis, polyuria, polydipsia, and impairment of renal function.
o renal stones are the most common clinical manifestation of hyperparathyroidism.
o renal lesions are frequently associated with hypertension.
Other manifestations:
o Hypertension
o peptic ulcer (mostly in duodenum and more common in males)
o acute and chronic pancreatitis
o mental disturbances
Secondary hyperparathyroidism
o consequence of chronic renal disease or intestinal malabsorption
o The renal insufficiency leads to elevation of the serum phosphorus level and reciprocal decrease of serum
calcium concentrations, with the resulting stimulation of the parathyroid glands.
o Vitamin D resistance is a characteristic feature of advanced renal disease and also may play a role by
contributing to reduced serum calcium concentrations.
o The bone changes are qualitatively similar to those seen in primary hyperparathyroidism. They are
usually milder, but sometimes extensive changes with cyst formation occur.
o The parathyroid abnormality in secondary hyperparathyroidism is chief cell hyperplasia of a generally
diffuse but sometimes nodular pattern of growth.
o C-cell hyperplasia in the thyroid gland has been found in patients with secondary hyperparathyroidism,
supposedly as a compensatory mechanism.
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 24
‘Tertiary’ hyperparathyroidism
o is applied to cases of hyperparathyroidism secondary to chronic renal disease or intestinal malabsorption,
in which one or more of the stimulated parathyroid glands seem to become autonomous.
o also referred to as nonsuppressible, autonomous, or refractory hyperparathyroidism
o usually detected after correction of the renal disease by hemodialysis or homotransplantation.
o Changes include: chief cell hyperplasia, the main difference with the ordinary case of suppressible
secondary hyperparathyroidism being a greater tendency to nodularity and heterogeneity.
Differential diagnosis
Conditions associated with hypercalcemia:
a. sarcoidosis
b. hyperthyroidism
c. multiple myeloma
d. milk–alkali syndrome
e. vitamin D intoxication
f. vitamin A intoxication
g. familial hypercalcemic hypocalciuria
h. humoral hypercalcemia of malignancy.
Forms of Hyperparathyroidism
Feature Primary Secondary Tertiary Hyperparathyroidism
Hyperparathyroidism Hyperparathyroidism
Causes Adenoma, hyperplasia Renal failure, vitamin D Autonomous transformation of
deficiency Secondary Hyperparathyroidism
PTH level Increased Increased Increased
Calcium level Increased Decreased Normal or Increased
Treatment
o Surgical identification of all four parathyroid glands
remains a widely used approach
o Adenomas are adequately treated by local excision of the tumor. It is highly desirable to excise or biopsy
at least one other parathyroid gland to rule out the alternative possibility of chief cell hyperplasia.
o Primary chief cell hyperplasia and the exceptionally rare water-clear cell hyperplasia are conventionally
treated by subtotal parathyroidectomy, as defined by total excision of three glands and partial excision of
the fourth, leaving 30–50 mg of viable tissue.
o Parathyroid carcinoma is best treated by excision of the tumor and surrounding soft tissues and removal
of the ipsilateral lateral thyroid lobe.
o The large majority of patients with secondary and ‘tertiary’ hyperparathyroidism respond well to medical
treatment. However, if bone lesions are severe and if the hypercalcemia is excessive, subtotal
parathyroidectomy may become necessary.
SURGICAL PATHOLOGY – THYROID & PARATHYROID GLANDS Page 25
You might also like
- Parasympathetic Nervous SystemDocument20 pagesParasympathetic Nervous SystemShahid Maqbool100% (1)
- Amboss NotesDocument12 pagesAmboss NotesVee Mend100% (2)
- Ultrasound Measurement Cheat SheetDocument1 pageUltrasound Measurement Cheat SheetDr. MLKNo ratings yet
- Abortion Guide: Causes, Types & ComplicationsDocument79 pagesAbortion Guide: Causes, Types & ComplicationschristianNo ratings yet
- Robbins Pathology Chapter 24 - EndocrineDocument2 pagesRobbins Pathology Chapter 24 - Endocrinescorpiosphinx79100% (2)
- PathologyDocument383 pagesPathology5alifa55No ratings yet
- Thyroid Gland: Anatomy, Physiology, and DiseasesDocument21 pagesThyroid Gland: Anatomy, Physiology, and DiseasesMAH pedNo ratings yet
- Year 8 Science OverviewDocument4 pagesYear 8 Science Overviewapi-3137245670% (1)
- Thyroid GlandDocument81 pagesThyroid Glanddr_shamimrNo ratings yet
- Renal colic diagnosis from lab resultsDocument101 pagesRenal colic diagnosis from lab resultsSaad KhanNo ratings yet
- Disorders of The Endocrine SystemDocument84 pagesDisorders of The Endocrine Systemcy lifeNo ratings yet
- Pathology of ThyroidDocument59 pagesPathology of ThyroidDavid Curtis Mintah100% (1)
- Thyroid Disorders: Medical Surgical NursingDocument20 pagesThyroid Disorders: Medical Surgical Nursingthanuja mathewNo ratings yet
- All About BonesDocument2 pagesAll About Bonesantonia putriNo ratings yet
- Anatomy & Physiology of the Digestive SystemDocument7 pagesAnatomy & Physiology of the Digestive SystemNicole Ken AgdanaNo ratings yet
- Applying Basic First Aid: General DirectionsDocument2 pagesApplying Basic First Aid: General DirectionsMa'am Kin100% (1)
- Submitted To:-Submitted By: Ms Jahanara Maam MS - Meena Asst. Professor M.SC (Nursing) 2 YrDocument55 pagesSubmitted To:-Submitted By: Ms Jahanara Maam MS - Meena Asst. Professor M.SC (Nursing) 2 YrMeena KoushalNo ratings yet
- NNYGDocument13 pagesNNYGrose ONo ratings yet
- Neck Masses: Guide to Thyroid Disease Diagnosis and TreatmentDocument49 pagesNeck Masses: Guide to Thyroid Disease Diagnosis and TreatmentRashed ShatnawiNo ratings yet
- Fakhri Mubarok 1510211033Document21 pagesFakhri Mubarok 1510211033Hafizh Zaki IrsyadNo ratings yet
- Endocrine PathologyDocument60 pagesEndocrine PathologySingitan SiyoumNo ratings yet
- Hashimoto's Thyroiditis (Most Common Cause of Hypothyroidism)Document33 pagesHashimoto's Thyroiditis (Most Common Cause of Hypothyroidism)Inamullah KhanNo ratings yet
- Thyroid PathologyDocument9 pagesThyroid PathologyJordan FernandezNo ratings yet
- Spleen Lec.1Document30 pagesSpleen Lec.1AmmarNo ratings yet
- ThyroidDocument39 pagesThyroidMartina ŠtihNo ratings yet
- Toxic AdenomaDocument5 pagesToxic AdenomaRayan JabbarNo ratings yet
- BurketsDocument5 pagesBurketssooNo ratings yet
- Pathology Lab V Diffuse and Multinodular Goiter.Document18 pagesPathology Lab V Diffuse and Multinodular Goiter.Jeffry Chandra TjahayadiNo ratings yet
- Patologi Endokrin 2016Document132 pagesPatologi Endokrin 2016agusNo ratings yet
- Tyroid 5Document6 pagesTyroid 5Anonymous UTUWFODCEYNo ratings yet
- Anatomy and Pathology of the Thyroid GlandDocument41 pagesAnatomy and Pathology of the Thyroid GlandWulan NoviantiNo ratings yet
- Goitre: Dr. Sandhya Gupta Assistant Professor General SurgeryDocument59 pagesGoitre: Dr. Sandhya Gupta Assistant Professor General SurgerySandhya guptaNo ratings yet
- Patho 4Document9 pagesPatho 4dfdxgfcvhbNo ratings yet
- Toxic Goiter in Pregnancy: Causes and TreatmentDocument28 pagesToxic Goiter in Pregnancy: Causes and TreatmentJade PingolNo ratings yet
- Pathology of Thyroid GlandDocument13 pagesPathology of Thyroid GlandChokri MAKTOUFNo ratings yet
- Annalyn S. Da-Anoy, M.D., R.M.T.Document88 pagesAnnalyn S. Da-Anoy, M.D., R.M.T.api-25914483No ratings yet
- 2-Adrenal Path.Document72 pages2-Adrenal Path.Lea MonzerNo ratings yet
- Grave DiseaseDocument3 pagesGrave DiseaseAnnisa Ikhsaniah AriffinNo ratings yet
- Thyroid enlargement causes and diagnosisDocument6 pagesThyroid enlargement causes and diagnosisthev0206No ratings yet
- Dr. Kunta Setiaji (ThyroidNodule)Document17 pagesDr. Kunta Setiaji (ThyroidNodule)Hasty WahyuniNo ratings yet
- Thyroid and Parathyroid PathologyDocument68 pagesThyroid and Parathyroid PathologygregNo ratings yet
- Thyroid Gland: Anatomy, Physiology and Disease ManagementDocument127 pagesThyroid Gland: Anatomy, Physiology and Disease ManagementCarla Mae MoraNo ratings yet
- Types: HyperthyroidismDocument12 pagesTypes: HyperthyroidismArunNo ratings yet
- PKDL Diagnosis and TreatmentDocument5 pagesPKDL Diagnosis and TreatmentParth BhayanaNo ratings yet
- ENDOCRINE PATHOLOGY WebpathDocument35 pagesENDOCRINE PATHOLOGY Webpathapi-3766657No ratings yet
- Oral Pathology I ReviewDocument373 pagesOral Pathology I ReviewAlex ChangNo ratings yet
- Medical ThyroidDocument4 pagesMedical ThyroidJose SirittNo ratings yet
- Neck MassDocument40 pagesNeck Massdryojanasharma57100% (1)
- 2 Endocrine ThyroidDocument4 pages2 Endocrine ThyroidJillKellyNo ratings yet
- THYROID LECTURE DR OCAMPO (1) (Autosaved)Document106 pagesTHYROID LECTURE DR OCAMPO (1) (Autosaved)SamNo ratings yet
- DR Ananta Thyroid SlideDocument73 pagesDR Ananta Thyroid SlideRoshan Kumar PanditNo ratings yet
- Endocrine Pathology: Lecture On Pathomorphology For 3-rd Year StudentsDocument44 pagesEndocrine Pathology: Lecture On Pathomorphology For 3-rd Year StudentsRodriguez Vivanco Kevin DanielNo ratings yet
- Multinodular Goiter Causes and Treatment OptionsDocument19 pagesMultinodular Goiter Causes and Treatment OptionsABDO ELJANo ratings yet
- Infancy & Childhood DiseasesDocument48 pagesInfancy & Childhood DiseasesDr. Janarthanan V100% (1)
- Hyperthyroidism: DR Rajeshwar ReddyDocument59 pagesHyperthyroidism: DR Rajeshwar ReddyRajeshwarreddy RamaswamyNo ratings yet
- Tutorial On Goiter GadedDocument117 pagesTutorial On Goiter GadedhindabdalgadirNo ratings yet
- Papillar y and Follicula R Thyroi D Cancer: K. A. Ikram Hussain Final Year M.B.B.SDocument26 pagesPapillar y and Follicula R Thyroi D Cancer: K. A. Ikram Hussain Final Year M.B.B.SAhsan JamilNo ratings yet
- Interpretation of Testicular Biopsy1Document50 pagesInterpretation of Testicular Biopsy1yourinmyheartNo ratings yet
- Cowden S Disease A Rare Cause of Oral Sis 2002 Journal of Laryngology and OtologyDocument3 pagesCowden S Disease A Rare Cause of Oral Sis 2002 Journal of Laryngology and Otologydasea01No ratings yet
- Carcinoma Thyroid Types Risk Factors AppearancesDocument43 pagesCarcinoma Thyroid Types Risk Factors AppearancesTariq Ahmed BalochNo ratings yet
- Nodulos Tiroideos PDFDocument16 pagesNodulos Tiroideos PDFTay SalinasNo ratings yet
- GoiterDocument48 pagesGoiterRizki NurNo ratings yet
- Gaucherdisease 170318151748Document45 pagesGaucherdisease 170318151748shruti kumarNo ratings yet
- Neck Masses and Lesions in PediatricsDocument63 pagesNeck Masses and Lesions in PediatricsRanj B. AshrafNo ratings yet
- TB MeningitisDocument91 pagesTB MeningitischristianNo ratings yet
- COLONDocument38 pagesCOLONchristianNo ratings yet
- Venous Disease: Understanding the Anatomy and PathophysiologyDocument50 pagesVenous Disease: Understanding the Anatomy and PathophysiologychristianNo ratings yet
- Lymph Nodes Normal Anatomy Major ZonesDocument5 pagesLymph Nodes Normal Anatomy Major ZoneschristianNo ratings yet
- Review of SystemsDocument2 pagesReview of SystemschristianNo ratings yet
- Gen Path Recalled QuestionsDocument10 pagesGen Path Recalled QuestionschristianNo ratings yet
- PEDIA DE CURie - Doc Manuel-1Document5 pagesPEDIA DE CURie - Doc Manuel-1christianNo ratings yet
- Lymph Nodes Normal Anatomy Major ZonesDocument5 pagesLymph Nodes Normal Anatomy Major ZoneschristianNo ratings yet
- Tucker Mclane: Comparable Success With OxytocinDocument6 pagesTucker Mclane: Comparable Success With OxytocinchristianNo ratings yet
- 1 50Document5 pages1 50christianNo ratings yet
- DR Solis - Midterms - Preventive Pediatrics 1&2 & HandoutsDocument12 pagesDR Solis - Midterms - Preventive Pediatrics 1&2 & HandoutschristianNo ratings yet
- Antiviral AgentsDocument5 pagesAntiviral AgentschristianNo ratings yet
- Hematology Oncology EssentialsDocument3 pagesHematology Oncology EssentialschristianNo ratings yet
- PED 1.6 Care of NewbornDocument5 pagesPED 1.6 Care of NewbornchristianNo ratings yet
- Action PotentialDocument36 pagesAction PotentialchristianNo ratings yet
- Membrane PotentialDocument33 pagesMembrane PotentialchristianNo ratings yet
- Hepatitis VirusesDocument5 pagesHepatitis ViruseschristianNo ratings yet
- DM2 2Document17 pagesDM2 2christianNo ratings yet
- LABDXDocument2 pagesLABDXchristianNo ratings yet
- Hepatitis VirusesDocument5 pagesHepatitis ViruseschristianNo ratings yet
- DR Solis - Midterms - Preventive Pediatrics 1&2 & HandoutsDocument12 pagesDR Solis - Midterms - Preventive Pediatrics 1&2 & HandoutschristianNo ratings yet
- DM1 2Document7 pagesDM1 2christianNo ratings yet
- LabdxmidDocument5 pagesLabdxmidchristianNo ratings yet
- OTDocument4 pagesOTchristianNo ratings yet
- Grade II Grading Sheets SY 2014-2015 3rd PeriodDocument1 pageGrade II Grading Sheets SY 2014-2015 3rd PeriodchristianNo ratings yet
- Coping Mechanisms For DMDocument19 pagesCoping Mechanisms For DMchristianNo ratings yet
- Hepatitis VirusesDocument5 pagesHepatitis ViruseschristianNo ratings yet
- Herpes VirusDocument11 pagesHerpes ViruschristianNo ratings yet
- Blood (Anaphy)Document8 pagesBlood (Anaphy)CORONEL, SOPHIANo ratings yet
- Secondary ThrombocytosisDocument7 pagesSecondary ThrombocytosisAya Avellana100% (1)
- CELLULAR RESPONSE TO INJURYDocument31 pagesCELLULAR RESPONSE TO INJURYAnderson GohNo ratings yet
- Endocrine System: Hormones and GlandsDocument68 pagesEndocrine System: Hormones and GlandsJerick Sevilla SearesNo ratings yet
- Whole Body DonationDocument4 pagesWhole Body DonationWhitneyWrichNo ratings yet
- 4.1.2.1.1 Humans BreatheDocument8 pages4.1.2.1.1 Humans BreatheZolnorhisam IsmailNo ratings yet
- IronDocument17 pagesIronYosef Dwi Cahyadi Salan100% (1)
- The A To Z of The Brain Cranial NervesDocument44 pagesThe A To Z of The Brain Cranial Nervesgroschen- romanNo ratings yet
- Nasal EmbryoDocument6 pagesNasal EmbryoLevani KartvelishviliNo ratings yet
- Types of Muscle Tissue and Their FunctionsDocument5 pagesTypes of Muscle Tissue and Their FunctionsRoby DerejeNo ratings yet
- SEMINAR ON ANAPHYLAXISDocument70 pagesSEMINAR ON ANAPHYLAXISLIDIYA MOL P VNo ratings yet
- What Is A CellDocument2 pagesWhat Is A CellJocelinyenNo ratings yet
- Test AMG Sem II EnglezaDocument3 pagesTest AMG Sem II EnglezaCCCAXANo ratings yet
- Reproductive Cell, Organ, CycleDocument56 pagesReproductive Cell, Organ, CycleAjay MeghanathiNo ratings yet
- Life Processes Class 10 NotesDocument27 pagesLife Processes Class 10 NotesHarsh MauryaNo ratings yet
- Everything You Need to Know About Back InjuriesDocument78 pagesEverything You Need to Know About Back InjuriesAsaad JawedNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaaangedeNo ratings yet
- HybaseDocument6 pagesHybaseSreejith SwaminathanNo ratings yet
- Seminar - Hemorrhage 25-06-2020Document75 pagesSeminar - Hemorrhage 25-06-2020Chandra dimpleNo ratings yet
- Blood Bank Homework IDocument3 pagesBlood Bank Homework IMohamed MounirNo ratings yet
- Ovarian DisordersDocument5 pagesOvarian DisordersNada MuchNo ratings yet
- Control of Stroke VolumeDocument2 pagesControl of Stroke VolumeNanda RahmatNo ratings yet
- Sexual Reproduction: Grade 11/12Document17 pagesSexual Reproduction: Grade 11/12lyn weiNo ratings yet
- Jurnal Sains Dan KesehatanDocument11 pagesJurnal Sains Dan KesehatanAurielle Annalicia SetiawanNo ratings yet