Professional Documents
Culture Documents
Anaesthesia: Update in
Uploaded by
Raditya DidotOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Anaesthesia: Update in
Uploaded by
Raditya DidotCopyright:
Available Formats
Clinical Overview Articles
Update in
Anaesthesia
Perioperative management of antiplatelet drugs
Juliet Barker*, Richard Telford and Tara Bolton
*Correspondence Email: jfrog3@hotmail.com
INTRODUCTION events (acute coronary syndromes or myocardial
Thirty-day mortality of postoperative surgical patients infarction) and cerebrovascular events (transient
is around 0.7-1.5% in the developed world. In the UK, ischaemic attacks or stroke). These may be for:
with approximately 4 million operations per year, this
• Primary prevention in patients with risk factors
equates to 25,000 to 30,000 postoperative deaths per
but no history of an event, or
year, or 70-80 deaths per day. Cardiovascular causes
of death are by far the most common at 59%, with • Secondary prevention for those who have had an
respiratory causes accounting for 35% of deaths.1 event, e.g. a transient ischaemic attack. Summary
Antiplatelet drugs, such as
In the arterial side of the circulation, clot formation aspirin and clopidogrel, are
PATHOGENESIS OF ATHEROTHROMBOSIS is more dependent on platelet aggregation, in contrast widely used in primary and
Cardiovascular and cerebrovascular events are closely to the venous side where clotting factors and fibrin secondary care and are very
linked to instability of atheromatous plaques within deposition play a more important role. Aspirin and commonly encountered
blood vessels and to the thrombogenicity (the ability clopidogrel specifically inhibit platelet function and in the perioperative
to form thrombus) of blood. If an unstable plaque are the antiplatelet drugs most commonly encountered setting. In this article we
ruptures to expose a thrombogenic surface to the by anaesthetists in the perioperative period. explore the specific uses
passing blood, a platelet clot forms over it leading of antiplatelet drugs, their
to an acute thrombotic event. Approximately 66% mechanisms of action and
Aspirin
possible consequences
of sudden cardiac events and 50% of postoperative Aspirin irreversibly inhibits the enzyme cycloxygenase- of their discontinuation.
myocardial infarctions are due to disruption and 1 (COX-1), leading to inhibition of thromboxane-A2 An algorithm is included
thrombosis of an unstable plaque. production. This results in reduced platelet activation to guide decisions on
and vasodilation. It is an irreversible effect, with the whether to stop drugs in the
ANTIPLATELET DRUGS function of each platelet inhibited for its lifespan. perioperative period.
Antiplatelet drugs are prescribed for cardiovascular Platelets are replaced at the rate of about 10% per day
Juliet Barker
Specialist Registrar
Department of Anaesthesia
Derriford Hospitals NHS Trust
Derriford Road
Plymouth
Devon
PL6 8DH
UK
Richard Telford
Consultant Anaesthetist
Tara Bolton
Locum Consultant
Department of Anaesthesia
Royal Devon and Exeter NHS
Foundation Trust
Barrack Road
Exeter
Devon
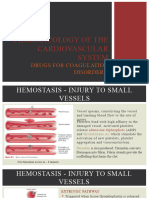
Figure 1. A summary of atherothrombosis - a generalised and progressive process: MI - myocardial infarction; TIA EX2 5DW
- transient ischaemic attack UK
Update in Anaesthesia | www.anaesthesiologists.org page 5
and so, after stopping aspirin, it takes about ten days to fully recover Drug eluting stents are impregnated with antimitotic chemo-
platelet function by replacing all affected platelets. therapeutic drugs, such as rapamycin and paclitaxel, that inhibit
endothelial growth. The stent remains uncovered and the requirement
Clopidogrel for re-intervention is reduced to about 5% per year. The thrombogenic
Clopidogrel is a prodrug, metabolised by the cytochrome p450 metal of the stent is however in contact with blood for longer.
enzyme system to an active metabolite with a half-life of about four
hours. It is a non-competitive, irreversible antagonist of the platelet For both types of stent it is recommended that aspirin be continued
adenosine diphosphate (ADP) receptor (P2Y12), inhibiting ADP for life. Dual therapy with aspirin and clopidogrel is ‘mandatory’
induced platelet aggregation for 7 days. until re-endothelialisation, i.e. 6 weeks for a bare metal stent and
12 months for a drug eluting stent. For PCI without stenting both
Dipyridamole drugs should given for 2 to 4 weeks.
Dipyridamole inhibits platelet aggregation and causes vasodilation
by inhibiting the breakdown of cyclic adenosine monophosphate WHEN TO STOP ANTIPLATELET DRUGS
(cAMP) by phosphodiesterase within platelets. Elevated cAMP A major side-effect of these drugs is bleeding, which is relevant to both
levels result in a reduced response to several stimuli, including the surgeon and anaesthetist over the perioperative period. When
platelet activating factor and ADP, thus inhibiting aggregation. considering whether to continue or stop antiplatelet therapy, first it
Dipyridamole also inhibits the uptake of adenosine into platelets, is important to determine whether the agent is given for primary or
erythrocytes and endothelial cells. The resultant raised surrounding secondary prevention, and second whether the patient is at high or
adenosine concentration acts at the platelet A2 receptor also leading low risk of occlusive disease. A balance must be considered between
to a rise in intracellular cAMP, this time by promoting the action of the risks of morbidity and mortality due to bleeding or clotting.
adenylate cyclase.
Traditionally there is an overriding concern about the risk of
INDICATIONS FOR ANTIPLATELET DRUGS bleeding and so a tendency towards stopping antiplatelet drugs in the
peroperative period. If antiplatelet drugs are continued, the average
• Aspirin is used alone in ‘low risk’ primary prevention. increase in blood loss when continuing aspirin alone is 2.5–20%.
• Clopidogrel is used where aspirin is not tolerated or with aspirin Blood loss increases by 30-50% with aspirin and clopidogrel used in
in high risk cases, especially after coronary stent insertion. combination.4 The transfusion rate increases by about 30% and so it
• For secondary prevention of transient ischaemic attacks, aspirin
appears that increased bleeding is a justifiable concern. The risk of an
plus dipyridamole (usually the modified release form) is ischaemic event is similar to the risk observed in patients with stable
recommended for two years, followed by aspirin alone. coronary artery disease, i.e. 2-6% for non-fatal myocardial infarction
and 1-5% for cardiac mortality.4
Aspirin reduces the incidence of death, myocardial infarction (by
30%) and stroke (by 25%) in a wide range of patients at high risk of However, withdrawal of antiplatelet drugs results in a rebound
occlusive vascular disease.2 Long-term administration of clopidogrel hypercoagulable state, which aggravates the hypercoagulability caused
to patients with atherosclerotic vascular disease is more effective than by surgery, greatly increasing the likelihood of a cardiovascular event.
aspirin in reducing the combined risk of ischaemic stroke, myocardial Withdrawing aspirin in a patient with coronary artery disease leads
infarction, or vascular death,3 although it only causes approximately to a 2 to 4 fold increase in the rate of death or myocardial infarction.
50% inhibition of maximum platelet aggregation in response to Stopping antiplatelet drugs in patients with coronary stents is the
ADP. The combination of both drugs has a greater anti-platelet effect major independent predictor of stent occlusion. The non-fatal
than either alone because they work by different mechanisms. myocardial infarction rate increases to 35% and average mortality
increases to 20-40%.4
Coronary stents
A subgroup of patients taking these drugs for secondary prevention of Although it is true that increased bleeding is a risk in patients where
coronary events have undergone percutaneous coronary intervention antiplatelet therapies are continued, it is clear that some patients are
(PCI), which consists of balloon dilatation and/or stenting of one or exposed to a far greater risk by stopping these drugs. In addition
more coronary arteries. These patients are at particularly high risk of the bleeding risk is partially negated by careful surgery, blood
a further cardiac event if their antiplatelet therapy is stopped. transfusion and platelet therapy if required. The balance of risks
Coronary stents are placed across a narrowing in a coronary artery, must be considered before deciding which drugs to continue for each
stenting it open and preventing further occlusion. There are two patient, with a specific comorbidity, undergoing a specific surgical
main types of stent - bare metal (BMS) or drug eluting (DES). procedure.
Bare metal stents provide a thrombogenic surface when initially GUIDANCE ON STOPPING OR CONTINUING ANTIPLATELET
inserted, but as endothelium grows over them (over approximately 3 DRUGS
months) this risk is reduced. However, as the endothelium thickens Several groups have suggested guidelines to aid this decision making
the risk of re-occlusion gradually increases. Re-stenosis necessitates process. The decision rests on patient factors such as:
re-intervention in 15–20% of patients treated with a BMS within
one year. • Why are they taking the drug?
page 6 Update in Anaesthesia | www.anaesthesiologists.org
• Is it for primary or secondary prevention? of ALL elective operations during this period. They suggest that
aspirin should NEVER be stopped. It has also been suggested that
• Are they particularly high risk, i.e. do they have a coronary stent
‘Apart from low coronary risk situations, patients on antiplatelet
in situ?
drugs should continue their treatment throughout surgery.
• If so which type (drug eluting or bare metal) and how long have However operations traditionally associated with excessive blood loss
they been in situ? should be postponed unless vital’4
Surgical factors such as the site of surgery and type of surgery should Given this complexity of decision making, the following algorithm
also be considered. In some types of surgery, bleeding in closed (Figure 1) has been proposed to help decide which patients should
spaces (such as intracranial neurosurgery) can have devastating continue their antiplatelet therapies in the perioperative period and
consequences and some types of plastic surgery with large raw areas which patients should have them witheld.5
can have high bleeding potential.
Patients should have their therapies restarted as soon as is safe
The American Heart Association/American College of Cardiology postoperatively. Loading doses of the drugs should be given to
have recommended that patients have 12 months of dual antiplatelet reduce the thrombosis risk as soon as possible. In the event of not
therapy after ANY drug eluting stent insertion and the postponement being able to give the drugs (for example because the patient is nil by
Figure 1. Algorithm for preoperative management of patients on antiplatelet therapy (reproduced from Reference 4 by kind permission of
Oxford University Press).
Algorithm for preopertaive management of patients on antiplatelet therapy
Patients on aspirin or clopidogrel Patients on aspirin and clopidogrel
Secondary prevention: High risk situations:
Primary prevention After MI, ACS, low risk <6 weeks after MI, ACS, BMS Low risk situations**
stents*, PVD <12 months after DES/high
risk stent
Risk of bleeding in All other surgery Only vital surgery All other surgery
enclosed space***
Risk of bleeding in
enclosed space***
Stop seven days preop Continue treatment Stop clopidrogel 7 days preop
and continue aspirin****
Abbreviations
MI - myocardial infarction; ACS - acute coronary syndrome; PVD - peripheral vascular disease; PCI - percutaneous coronary intervention;
BMS - bare metal stent; DES - drug eluting stent;
* Low risk stents: those receiving aspirin only
** Examples of low risk situations: 3 months after BMS, uncomplicated MI and PCI without stenting
*** Risk of bleeding in closed space: closed space spinal surgery, posterior eye chamber surgery
**** In high risk situations discuss with consultant anaesthetist/cardiologist and consider “bridging” therapy (e.g. simultaneous
unfractionated heparin and GP IIb/IIIa antagonist infusions)
Withdrawing aspirin must be evaluated for each case individually; if aspirin or clopidogrel are stopped, early postoperative re-institution is
important.
Update in Anaesthesia | www.anaesthesiologists.org page 7
mouth) other anticoagulation methods should be considered. Bear REFERENCES
in mind that many of the alternative drugs affect the venous side 1. Campling EA, Devlin HD, Hoile RW, Lunn JN. The Report of the National
of the circulation more than the arterial and so are not providing Confidential Enquiry into Perioperative Deaths (NCEPOD) 1992/1993.
comparable protection from arterial events. Available at: http://www.ncepod.org.uk/reports4.htm
In the event of bleeding, platelet transfusion is the only effective 2. Antithrombotic Trialists’ Collaboration. Collaborative meta-analysis
method of reversing the effect of these drugs. DDAVP (desamino of randomised trials of antiplatelet therapy for prevention of death,
myocardial infarction, and stroke in high risk patients. BMJ 2002; 324:
D-arginine vasopressin)6 and aprotinin (an anti-fibrinolytic agent)7
71-86.
may increase platelet function to some degree.
3. CAPRIE Steering Committee. A randomised, blinded, trial of
CONCLUSIONS clopidogrel versus aspirin in patients at risk of ischaemic events
In summary the management of patients taking antiplatelet drugs is (CAPRIE). Lancet 1996; 348: 1329-39.
complex and our current level of understanding is poor. There is a 4. Grines CL, Bonow RO, Casey DE, Gardner TJ, Lockhart PB, Moliterno
significant potential to do severe harm to patients if their drugs are DJ,et al. Prevention of Premature Discontinuation of Dual Antiplatelet
stopped inappropriately, or indeed if they bleed following surgery Therapy in Patients With Coronary Artery Stents. A Science Advisory
whilst still taking them. The default position in many settings seems From the American Heart Association, American College of
to be that the decision to stop or not is undertaken preoperatively Cardiology, Society for Cardiovascular Angiography and Interventions,
by surgeons and their favoured decision is to stop clopidogrel almost American College of Surgeons, and American Dental Association,
always and aspirin very frequently. With Representation From the American College of Physicians.
Circulation 2007; 115: 813-8.
It is likely that the full implications of stopping antiplatelet drugs
5. Chassot P-G, Delabays A, Spahn DR. Perioperative antiplatelet therapy:
are not fully appreciated and, understandably, a fear of bleeding
the case for continuing therapy in patients at risk of myocardial
predominates. We suggest that it would be more appropriate to fear infarction. Br J Anaes 2007; 99: 316 -28.
the cardiovascular effects of stopping the drugs. Deferring surgery
until the patient is ‘safe’ to stop clopidogrel, or accepting a risk of 6. Kovesi T, Royston D. Is there a bleeding problem with platelet-active
increased bleeding and adopting strategies to cope with this, if the drugs? Br J Anaesth 2002; 88: 159-63.
patient cannot be deferred is more appropriate. Further research in 7. Herbert JM, Bernat A, Maffrand JP. Aprotinin reduces clopidogrel-
this area will provide the evidence base for robust guidelines to advise induced prolongation of the bleeding time in the rat. Thromb Res
management of each patient taking antiplatelet drugs. 1993; 71: 433-41.
page 8 Update in Anaesthesia | www.anaesthesiologists.org
You might also like
- Ludwig's AnginaDocument22 pagesLudwig's AnginaDevavrat SinghNo ratings yet
- RLE Module 2M - Chest Physiotherapy, Postural Drainage, Nebulization, Chest Tube Drainage Systems, Blood TransfusionDocument57 pagesRLE Module 2M - Chest Physiotherapy, Postural Drainage, Nebulization, Chest Tube Drainage Systems, Blood TransfusionAlexa GoteraNo ratings yet
- Product Manual ChronicDocument56 pagesProduct Manual ChronicsubhojitnayekNo ratings yet
- Electrocardiograma en TóxicologiaDocument19 pagesElectrocardiograma en TóxicologiaLaura GNo ratings yet
- Antipatelet Drug TherapyDocument6 pagesAntipatelet Drug TherapySayali KhandaleNo ratings yet
- Antiplateletdrugs 150203231404 Conversion Gate01 PDFDocument67 pagesAntiplateletdrugs 150203231404 Conversion Gate01 PDFAndrie WigunaNo ratings yet
- Wesam R KadhumDocument31 pagesWesam R Kadhumwisam_1by1No ratings yet
- 2022 - Anesthetic Management For Open Thoracoabdominal and Abdominal Aortic Aneurysm RepairDocument14 pages2022 - Anesthetic Management For Open Thoracoabdominal and Abdominal Aortic Aneurysm RepairLaura Camila RiveraNo ratings yet
- Chapter 7 Pharmacology and Drug Administration (Jensen Steven)Document11 pagesChapter 7 Pharmacology and Drug Administration (Jensen Steven)Raven DomingoNo ratings yet
- Anticoagulant Therapy For Acute Coronary SyndromesDocument6 pagesAnticoagulant Therapy For Acute Coronary SyndromesAtrik Pristica DianiNo ratings yet
- Peri-Operative Cardiac Arrhythmias - Part 1Document14 pagesPeri-Operative Cardiac Arrhythmias - Part 1jhonjrodriNo ratings yet
- ExpertConsensus ResuscitationAfterCardiacSurgery PDFDocument16 pagesExpertConsensus ResuscitationAfterCardiacSurgery PDFJuan Guillermo BuitragoNo ratings yet
- Ytz 119Document4 pagesYtz 119Oeij Henri WijayaNo ratings yet
- Eur Heart J-2011-Patrono-2922-32Document13 pagesEur Heart J-2011-Patrono-2922-32Zhank Creex YusranNo ratings yet
- Drugs For Coagulation Disorders 2023Document26 pagesDrugs For Coagulation Disorders 2023aguilarjanicaNo ratings yet
- Ecg ManfestationsDocument19 pagesEcg Manfestationsnaxo128No ratings yet
- 3rd Care of The Critically Ill Surgical Patient PDFDocument273 pages3rd Care of The Critically Ill Surgical Patient PDFPavitra RamasamyNo ratings yet
- Special Care Dentistry Dental Management of Patients With Drug Related Acquired Bleeding DisordersDocument6 pagesSpecial Care Dentistry Dental Management of Patients With Drug Related Acquired Bleeding DisordersRatri ReswitadewiNo ratings yet
- Use of Inotropes and Vasopressor Agents in Critically Ill PatientsDocument19 pagesUse of Inotropes and Vasopressor Agents in Critically Ill PatientsLong LeNo ratings yet
- Antiplatelet Treatment in Stable Coronary Artery DiseaseDocument6 pagesAntiplatelet Treatment in Stable Coronary Artery DiseaserambutsapukusayangNo ratings yet
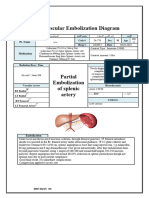
- Partial Embolization of Splenic ArteryDocument2 pagesPartial Embolization of Splenic Arteryshamaamo19No ratings yet
- HFeEF EBM Summary 18 TroughtonDocument6 pagesHFeEF EBM Summary 18 TroughtonBruno BatinicaNo ratings yet
- Cardiac Muscle Cardiovascular System: Dep. of Biochemistry Rosdiana NatzirDocument31 pagesCardiac Muscle Cardiovascular System: Dep. of Biochemistry Rosdiana NatzirFaedil Ichsan CiremaiNo ratings yet
- Antiarrhythmicdrugs: Risks and BenefitsDocument14 pagesAntiarrhythmicdrugs: Risks and Benefitsreinaldo valdes iznagaNo ratings yet
- Antithrombotic Therapy in Prevention of Ischemic Stroke (Richard C Becker, Frederick A Spencer) (Z-Library)Document54 pagesAntithrombotic Therapy in Prevention of Ischemic Stroke (Richard C Becker, Frederick A Spencer) (Z-Library)Srinivas PingaliNo ratings yet
- Cardiovascular Drug IntroductionDocument3 pagesCardiovascular Drug IntroductionSamah Khan100% (1)
- PFT Lecture 1Document35 pagesPFT Lecture 1Saifeldein ElimamNo ratings yet
- Anticoagulants:: DefinitionDocument6 pagesAnticoagulants:: DefinitionMunaza FarooqNo ratings yet
- # Davidson - Review # Cardiology - 1Document32 pages# Davidson - Review # Cardiology - 1emtiaz zamanNo ratings yet
- Dilated Cardiomyopathy TherapyDocument7 pagesDilated Cardiomyopathy Therapyedrash85No ratings yet
- 7-Cardiology and Respiratory MedicineDocument373 pages7-Cardiology and Respiratory Medicinethisar100% (6)
- Pharmacology and Toxicology - Anticoagulants - Medical LibraryDocument8 pagesPharmacology and Toxicology - Anticoagulants - Medical Libraryjean PiedraNo ratings yet
- Drugs and The Kidney: Continuing Medical EducationDocument6 pagesDrugs and The Kidney: Continuing Medical EducationJANINE PASIONNo ratings yet
- Pharmacology RCR1 - CardioDocument8 pagesPharmacology RCR1 - CardioeamcrawleyNo ratings yet
- Ultrafiltration During Cardiopulmonary Bypass: DR AmarjaDocument64 pagesUltrafiltration During Cardiopulmonary Bypass: DR AmarjaFarez Scrub HatsNo ratings yet
- 183 Cardiac Output Monitoring Part 1Document7 pages183 Cardiac Output Monitoring Part 1Ratesh BassiNo ratings yet
- Cardio AssignmentDocument5 pagesCardio Assignmentthemega1111No ratings yet
- Overview of Atrial Flutter: Authors: Section Editor: Deputy EditorDocument20 pagesOverview of Atrial Flutter: Authors: Section Editor: Deputy EditorAnca StanNo ratings yet
- CEACCP - Illegal Substances in Anaesthetic and Intensive Care PracticesDocument5 pagesCEACCP - Illegal Substances in Anaesthetic and Intensive Care PracticesDonkeyManNo ratings yet
- 10 - Anti-Platelet Drugs (Final)Document15 pages10 - Anti-Platelet Drugs (Final)Goodone OneNo ratings yet
- AF AmiodaronDocument7 pagesAF AmiodaronDita NururiyanieNo ratings yet
- Thrombolytic TherapyDocument13 pagesThrombolytic TherapyAnusha AkhilNo ratings yet
- Platelet Thrombin Receptor Antagonism and Atherothrombosis: New Drugs SeriesDocument12 pagesPlatelet Thrombin Receptor Antagonism and Atherothrombosis: New Drugs SeriesAlejandro BarretoNo ratings yet
- Atrial FlutterDocument38 pagesAtrial FlutterLady AngodNo ratings yet
- The Role of ACE Inhibitors in Cardiovascular Disease: PrescribingDocument9 pagesThe Role of ACE Inhibitors in Cardiovascular Disease: PrescribingHeryanti PusparisaNo ratings yet
- European J of Heart Fail - 2018 - Mullens - Rationale and Design of The ADVOR Acetazolamide in Decompensated Heart FailureDocument10 pagesEuropean J of Heart Fail - 2018 - Mullens - Rationale and Design of The ADVOR Acetazolamide in Decompensated Heart FailureAnnisa Tria FadillaNo ratings yet
- Terapia Antiplaquetaria y ExodontiaDocument6 pagesTerapia Antiplaquetaria y ExodontiaDentalib OdontologíaNo ratings yet
- Q1Document156 pagesQ1Mayuresh Chaudhari100% (1)
- Antiarrhythmic Drugs: Osuzer@istanbul - Edu.trDocument0 pagesAntiarrhythmic Drugs: Osuzer@istanbul - Edu.trPrabhakar KumarNo ratings yet
- Overview of Hemostasis and ThrombosisDocument12 pagesOverview of Hemostasis and ThrombosisMichaella AlmirahNo ratings yet
- Farmako ACE InhibitorsDocument4 pagesFarmako ACE InhibitorsIntan Siti HulaimaNo ratings yet
- Thrombolytics, Anticoags, Antiplatelets PDFDocument21 pagesThrombolytics, Anticoags, Antiplatelets PDFrachelkdoNo ratings yet
- ThrombolyticsDocument14 pagesThrombolyticsJavier Gonzalez, M.D. DABEMNo ratings yet
- Anticoagulant/Thrombolytic 1. Anticoagulant: Parenteral AnticoagulantsDocument4 pagesAnticoagulant/Thrombolytic 1. Anticoagulant: Parenteral AnticoagulantsHannaNo ratings yet
- k.41 ATRIAL FLUTTERDocument8 pagesk.41 ATRIAL FLUTTERjamaliganteng88No ratings yet
- Perioperative Implications of Pericardial Effusions and Cardiac TamponadeDocument9 pagesPerioperative Implications of Pericardial Effusions and Cardiac TamponadeMarielou CoutinhoNo ratings yet
- Jurding Hipertensi PulmonalDocument33 pagesJurding Hipertensi PulmonalRyu KangNo ratings yet
- Biochem Case StudyDocument10 pagesBiochem Case StudyAleksei CuadraNo ratings yet
- Adrenalectomia-Open Anterior Left AdrenalectomyDocument8 pagesAdrenalectomia-Open Anterior Left AdrenalectomyLorena AlmeidaNo ratings yet
- Aprotinin and Tranexamic Acid For High Transfusion Risk Cardiac SurgeryDocument10 pagesAprotinin and Tranexamic Acid For High Transfusion Risk Cardiac SurgeryBetão AviãoNo ratings yet
- Asam TraneksaminDocument1 pageAsam TraneksaminRaditya DidotNo ratings yet
- Daftar Permintaan Alat OrthoDocument4 pagesDaftar Permintaan Alat OrthoRaditya DidotNo ratings yet
- Stock Obat Bulan April 2017Document7 pagesStock Obat Bulan April 2017Raditya DidotNo ratings yet
- Algorithm For The Management of A High Regional Block in ObstetricsDocument5 pagesAlgorithm For The Management of A High Regional Block in ObstetricsRaditya DidotNo ratings yet
- Dexmedetomidine As Sole Agent For Awake Fiberoptic Intubation in A Patient With Local Anesthetic AllergyDocument3 pagesDexmedetomidine As Sole Agent For Awake Fiberoptic Intubation in A Patient With Local Anesthetic AllergyRaditya DidotNo ratings yet
- Manajemen Preoperatif Pasien Dengan Terapi KoagulanDocument32 pagesManajemen Preoperatif Pasien Dengan Terapi KoagulanRaditya DidotNo ratings yet
- In Managing Early Using: New Normal Respiratory Distress HFNTDocument51 pagesIn Managing Early Using: New Normal Respiratory Distress HFNTRaditya DidotNo ratings yet
- Parathyroid Gland DysfunctionDocument35 pagesParathyroid Gland DysfunctionRaditya DidotNo ratings yet
- Neonatal Resuscitation 2010 American Heart Association Guidelines For Cardiopulmonary Resuscitation and Emergency Cardiovascular CareDocument8 pagesNeonatal Resuscitation 2010 American Heart Association Guidelines For Cardiopulmonary Resuscitation and Emergency Cardiovascular CareRaditya DidotNo ratings yet
- Hyperthyroidism and Anaestheisa: WahyudiDocument24 pagesHyperthyroidism and Anaestheisa: WahyudiRaditya DidotNo ratings yet
- Chapter 3 Animal Tissues SolutionDocument6 pagesChapter 3 Animal Tissues SolutionLucky ErrojuNo ratings yet
- Endometriosis: Endometriosis: Symptoms, Treatment, DiagnosisDocument4 pagesEndometriosis: Endometriosis: Symptoms, Treatment, DiagnosisrizkiaautikasariNo ratings yet
- 2019 - Postoperative Healing Assessment Using Cannabinoids in Oral SurgeryDocument7 pages2019 - Postoperative Healing Assessment Using Cannabinoids in Oral SurgerycorcarolNo ratings yet
- Magic Roadshow 6Document87 pagesMagic Roadshow 6RickNo ratings yet
- Tens Vitalcontrol PDFDocument20 pagesTens Vitalcontrol PDFOscar BravoNo ratings yet
- Prezentare AromaDocument56 pagesPrezentare AromaMamaliga LizaNo ratings yet
- Bio TherapyDocument18 pagesBio TherapyChino RamirezNo ratings yet
- Lesson Plan On Pituitary Gland (Endocrine SystemDocument37 pagesLesson Plan On Pituitary Gland (Endocrine SystemRosalyn Angcay Quintinita100% (1)
- OCTA InflammatoryEyediseaseSrivastavaDocument24 pagesOCTA InflammatoryEyediseaseSrivastavaPriyanka DocNo ratings yet
- Mandibular NerveDocument3 pagesMandibular Nervervinluan.dentNo ratings yet
- IV. Recognizing National Issues and Concern - E-Substance Abuse EducationDocument9 pagesIV. Recognizing National Issues and Concern - E-Substance Abuse EducationMicsjadeCastillo0% (1)
- Diabetes Research and Clinical Practice: SciencedirectDocument2 pagesDiabetes Research and Clinical Practice: Sciencedirectprobo asmoroNo ratings yet
- MRCPCH q15Document30 pagesMRCPCH q15Galaleldin AliNo ratings yet
- Role of Respiratory Intermediate Care Units During The SARS-CoV-2 PandemicDocument7 pagesRole of Respiratory Intermediate Care Units During The SARS-CoV-2 PandemicJHNo ratings yet
- Case Note 6: Patient DetailsDocument3 pagesCase Note 6: Patient DetailsBINCYNo ratings yet
- 074 Victor Babes PDFDocument1 page074 Victor Babes PDFCosminNo ratings yet
- Unit 7.VARIETY OF LIFEDocument120 pagesUnit 7.VARIETY OF LIFEPika PiNo ratings yet
- Recommendations For Rescue of A Submerged Unresponsive Compressed-Gas DiverDocument10 pagesRecommendations For Rescue of A Submerged Unresponsive Compressed-Gas Diverwyma01No ratings yet
- WBI05 Energy Exercise and Co-OrdiantionDocument172 pagesWBI05 Energy Exercise and Co-OrdiantionOxygen CarbonNo ratings yet
- Positive and Negative Filipino ValuesDocument2 pagesPositive and Negative Filipino ValuesBrenty TablateNo ratings yet
- Johnsons BabyDocument1 pageJohnsons BabyManpreetaa50% (2)
- Duas For Stress and Sickness 6.9.2013 PDFDocument27 pagesDuas For Stress and Sickness 6.9.2013 PDFHasan OsamaNo ratings yet
- Circadian RhythmsDocument6 pagesCircadian Rhythmshafsa111100% (1)
- Cardiac Pacemakers and Defibrillators 2nd Ed - C. Love (Landes, 2006) WW PDFDocument183 pagesCardiac Pacemakers and Defibrillators 2nd Ed - C. Love (Landes, 2006) WW PDFJozsa Attila100% (1)
- For Review OAPDocument144 pagesFor Review OAPKim John Rull NateNo ratings yet
- Bio01 Co2 PPT - Cell CycleDocument120 pagesBio01 Co2 PPT - Cell CycleMarc Ronald de LeonNo ratings yet
- Industrial Hygiene Guidance PDFDocument84 pagesIndustrial Hygiene Guidance PDFNora0% (1)
- Jurnal MigrainDocument6 pagesJurnal MigrainReksyNo ratings yet