Professional Documents
Culture Documents
Drug Action: Pharmaceutic, Pharmacokinetic, and Pharmacodynamic Phases
Uploaded by
VIGO, JERECEL0 ratings0% found this document useful (0 votes)
9 views10 pagesOriginal Title
bhgvvvvvvhvgggggggggg
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views10 pagesDrug Action: Pharmaceutic, Pharmacokinetic, and Pharmacodynamic Phases
Uploaded by
VIGO, JERECELCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 10
Drug Action: Pharmaceutic, are both disintegrated and absorbed faster in
Pharmacokinetic, and acidic fluidswith a pH of 1 or 2 rather than in
alkaline fluids. Alkaline drugs would become
Pharmacodynamic Phases
ionized and have difficulty crossing cell
A tablet or capsule taken by mouth goes through membrane barriers. Both the very young and
three phases—pharmaceutic, pharmacokinetic, older adults have less gastric acidity; therefore,
and pharmacodynamic—as drug actions occur. drug absorption is generally slower for those
In the pharmaceutic phase, the drug becomes a drugs absorbed primarily in the stomach.
solution so thatit can cross the biologic Enteric-coated drugs resist disintegration in the
membrane. When the drug is administered gastric acid of the stomach, so disintegration
parenterally by subcutaneous (subQ), does not occur until the drug reaches the alkaline
intramuscular (IM), or intravenous (IV) routes, environment of the small intestine. Enteric-
there is no pharmaceutic phase. The second coated tablets can remain in the stomach for a
phase, the pharmacokinetic phase, is composed long time; therefore, their effect may be delayed
of four processes: absorption, distribution, in onset. Enteric-coated tablets or capsules and
metabolism (or biotransformation), and sustained-release (beaded) capsules should not
excretion (or elimination). In the be crushed. Crushing would alter the place and
pharmacodynamics phase, a biologic or time of absorption of the drug. Food in the GI
physiologic response results. tract may interfere with the dissolution of certain
PHARMACEUTIC PHASE drugs. Some drugs irritate the gastric mucosa, so
Approximately 80% of drugs are taken by fluids or food may be necessary to dilute the
mouth. The pharmaceutic phase (dissolution) is drug concentration and to act as protectants.
the first phase of drug action. In the PHARMACOKINETIC PHASE
gastrointestinal (GI) tract, drugs need to be in Pharmacokinetics is the process of drug
solution so they can be absorbed. A drug in solid movement toachieve drug action. The four
form (tablet or capsule) must disintegrate into processes are absorption, distribution,
small particles to dissolve into a liquid, a process metabolism (or biotransformation), and
known as dissolution. Drugs in liquid form are excretion
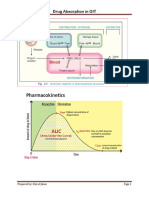
already in solution. Figure 1-1 displays the (or elimination). The nurse applies knowledge of
pharmaceutic phase of a table. pharmacokinetics when assessing the patient for
possible adverse drug effects. The nurse
Tablets are not 100% drug. Fillers and inert communicates assessment findings to members
substances, generally called excipients, are used of the health care team in a timely manner to
in drug preparation to allow the drug to take on a promote safe and effective drug therapy for the
particular size and shape and to enhance drug patient.
dissolution. Some additives in drugs, such as the Absorption
ions potassium (K) and sodium (Na) in penicillin Absorption is the movement of drug particles
potassium and penicillin sodium, increase the from the GI tract to body fluids by passive
absorbability of the drug. Penicillin is poorly absorption, active absorption, or pinocytosis.
absorbed by the GI tract because of gastric acid. Most oral drugs are absorbed into the surface
However, by making the drug a potassium or area of the small intestine through the action of
sodium salt, penicillin can then be absorbed. the extensive mucosal villi. Absorption is
Disintegration is the breakdown of a tablet into reduced if the villi are decreased in number
smaller particles. Dissolution is the dissolving because of disease, drug effect, or the removal of
of the smaller particles in the GI fluid before small intestine. Protein-based drugs such as
absorption. Rate of dissolution is the time it insulin and
takes the drug to disintegrate and dissolve to growth hormones are destroyed in the small
become available for the body to absorb it. intestine by digestive enzymes. Passive
Drugs in liquid form are more rapidly available absorption occurs mostly by diffusion
for GI absorption than are solids. Generally, (movement from higher concentration to lower
drugs concentration). With the process of diffusion, the
drug does not require energy to move across the
membrane. Active absorption requires a carrier from the intestinal lumen to the liver via the
such as an enzyme or protein to move the drug portal vein. In the liver, some drugs may be
against a concentration gradient. Energy is metabolized to an inactive form that may then be
required for active absorption. Pinocytosis is a excreted, thus reducing the amount of active
process by which cells carry a drug across their drug. Some drugs do not undergo metabolism at
membrane by engulfing the drug particles all in the liver, and
(Figure 1-2). The GI membrane is composed others may be metabolized to drug metabolite,
mostly of lipid (fat) and protein, so drugs that which may be equally or more active than the
are lipid soluble pass rapidly through the GI original drug. The process in which the drug
membrane. Water-soluble drugs need a carrier, passes to the liver first is called the first-pass
either enzyme or protein, to pass through the effect, or hepatic first pass. Most drugs given
membrane. Large orally are affected by first-pass metabolism.
particles pass through the cell membrane if they Lidocaine and some nitroglycerins are not given
are nonionized (have no positive or negative orally because they have extensive first-pass
charge). Weak acid drugs such as aspirin are less metabolism and therefore most of the dose
ionized in the stomach, and they pass through would be destroyed. Bioavailability is a
the stomach lining easily and rapidly. An subcategory of absorption. It is the percentage of
infant’s gastric secretions have a higher pH the administered drug dose that reaches the
(alkaline) than those of adults; therefore, infants systemic circulation. For the oral route of drug
can absorb more penicillin. Certain drugs such administration, bioavailability occurs after
as calcium carbonate and many of the absorption and first-pass metabolism. The
antifungals need an acidic environment to percentage of bioavailability for the oral route is
achieve greater drug absorption; thus food can always less than 100%, but for the IV route it is
stimulate the production of gastric acid. 100%. Oral drugs that have a high first-pass
Hydrochloric acid destroys some drugs such as hepatic metabolism may have a bioavailability
penicillin G; therefore a large oral dosage of of only 20% to 40% on entering systemic
penicillin is needed to offset the partial dose circulation. To obtain the desired drug effect, the
loss. Drugs administered by many routes do not oral dose could be higher than the drug dose for
pass through the GI tract or liver. These include IV use.
parenteral drugs, eyedrops, eardrops, nasal Factors that alter bioavailability include (1) the
sprays, respiratory inhalants, transdermal drugs, drug form (e.g., tablet, capsule, sustained-
and sublingual drugs. Remember, drugs that are release, liquid, transdermal patch, rectal
lipid soluble and nonionized are absorbed faster suppository, inhalation), (2) route of
than water-soluble and ionized drugs. administration (e.g., oral, rectal, topical,
Blood flow, pain, stress, hunger, fasting, food, parenteral), (3) GI mucosa and motility, (4) food
and pH affect drug absorption. Poor circulation and other drugs, and (5) changes in liver
to the stomach as a result of shock, metabolism caused by liver dysfunction or
vasoconstrictor drugs, or disease hampers inadequate hepatic blood flow. A decrease in
absorption. Pain, stress, and foods that are solid, liver function or a decrease in hepatic blood flow
hot, or high in fat can slow gastric emptying can increase the bioavailability of a
time, so the drug remains in the stomach longer. drug, but only if the drug is metabolized by the
Exercise can decrease blood flow by causing liver. Less drug is destroyed by hepatic
more blood to flow to the peripheral muscle, metabolism in the presence of liver disorder.
thereby decreasing blood circulation to the GI With some oral drugs, rapid absorption increases
tract. Drugs given IM are absorbed faster in the bioavailability of the drug and can cause an
muscles that have more blood vessels (e.g., increase in drug concentration. Drug toxicity
deltoids) than in those that have fewer blood may result. Slow absorption can limit the
vessels (e.g., gluteals). Subcutaneous tissue has bioavailability of the drug, thus causing a
fewer blood vessels, so absorption is slower in decrease in drug serum concentration.
such tissue. Distribution
Some drugs do not go directly into the systemic Distribution is the process by which the drug
circulation following oral absorption but pass becomes available to body fluids and body
tissues. Drug distribution is influenced by blood free or unbound drug goes to nonspecific tissue
flow, the drug’s affinity to the tissue, and the binding sites until needed and excess free drug
protein-binding effect (Figure 1-3). In addition, in the circulation does not occur. Consequently,
volume of drug distribution (Vd) is dependent a decreased drug dose is needed as there is not as
on drug dose and its concentration in the body. much protein circulated for the drug
Drugs with a larger volume of drug distribution to bind to. Some drugs bind with a specific
have a longer half-life and stay in the body protein component such as albumin or globulin.
longer. See the section on metabolism, or Most anticonvulsants bind primarily to albumin.
biotransformation, later in this chapter. Some basic drugs such as antidysrhythmics (e.g.,
Protein Binding lidocaine, quinidine) bind mostly to globulins.
As drugs are distributed in the plasma, many are To avoid possible drug toxicity, checking the
bound to varying degrees (percentages) with proteinbinding percentage of all drugs
protein (primarily albumin). Drugs that are administered to a patient is important. The nurse
greater than 89% bound to protein are known as should also check the patient’s plasma protein
highly protein-bound drugs; drugs that are 61% and albumin levels, because a decrease in
to 89% bound to protein are moderately highly plasma
proteinbound; drugs that are 30% to 60% bound protein (albumin) decreases protein-binding
to protein are moderately protein-bound; and sites, permitting more free drug in the
drugs that are less than 30% bound to protein are circulation. Depending on the drug, the result
low protein-bound drugs. Table 1-1 lists selected could be life-threatening. Abscesses, exudates,
highly protein-bound drugs and moderately body glands, and tumors hinder drug
highly protein-bound drugs. The portion of the distribution. Antibiotics do not distribute well at
drug that is bound is inactive because it is not abscess and exudate sites. In addition, some
available to receptors, and the portion that drugs accumulate in particular
remains unbound is free, active drug. Only free tissues such as fat, bone, liver, muscle, and eye
drugs (drugs not bound to protein) are active tissues. The blood-brain barrier (BBB) is a
and can cause a pharmacologic response. As the semipermeable membrane in the central nervous
free drug in the circulation decreases, more system (CNS) that protects the brain from
bound drug is released from the protein to foreign substances. Highly lipid-soluble drugs
maintain the balance of free drug. Drugs bound are able to cross the BBB. Drugs that are not
to proteins cannot leave the systemic circulation bound to proteins and are not lipid soluble are
to get to the site of action. This is why only free not able to cross the BBB, which makes it
drug is active. difficult to distribute the drug (Figure 1-4).
When two highly protein-bound drugs are given During pregnancy, both lipid-soluble and lipid-
concurrently, they compete for protein-binding insoluble
sites, thus causing more free drug to be released drugs are able to cross the placental barrier,
into the circulation. In this situation, drug which can affect the fetus and the mother. The
accumulation and possible drug toxicity can risk-benefit ratio should be considered before
result. Also, a low serum protein level decreases drugs are given during pregnancy (Figure 1-5;
the number of protein-binding sites and can see also Chapter 53). During lactation, drugs can
cause an increase in the amount of free drug in be secreted into breast milk, which could affect
the plasma. Drug toxicity may then result. Drug the nursing infant. The nurse needs to check
dose is prescribed according to the percentage in which drugs may cross into breast milk before
which the drug binds to protein. Patients with administering to a lactating patient.
liver or kidney disease or those who are Metabolism, or Biotransformation
malnourished may have an abnormally low Metabolism is the process by which the body
serum albumin level. This results in fewer inactivates or biotransforms drugs. Drugs can be
protein-binding sites, which in turn leads to metabolized in several organs; however, the liver
excess free drug and eventually to drug toxicity. is the primary site of metabolism. Most drugs
Older adults are more likely to have are inactivated by liver enzymes and are then
hypoalbuminemia. With some health conditions converted or transformed by hepatic enzymes to
that result in a low serum protein level, excess inactive metabolites or water-soluble substances
for excretion. A large percentage of drugs are metabolized to carbon dioxide (CO2) and water
lipid soluble; thus the liver metabolizes the (H2O). The urine pH influences drug excretion.
lipid-soluble drug substance to a water-soluble Urine pH varies from 4.5 to 8. Acidic urine
substance for renal excretion. However, some promotes elimination of weak base drugs, and
drugs are transformed into active metabolites, alkaline urine promotes elimination of weak acid
causing an increased pharmacologic response. drugs. Aspirin, a weak acid, is excreted rapidly
Liver diseases such as cirrhosis and hepatitis in alkaline urine. If a person takes an overdose
alter drug metabolism by inhibiting the of aspirin, sodium bicarbonate may be given to
drugmetabolizing enzymes in the liver. When change the urine pH to alkaline to promote
the drug metabolism rate is decreased, excess excretion of the drug. Large quantities of
drug accumulation can occur and lead to cranberry juice can decrease urine pH, causing
toxicity. acidic urine and thus inhibiting the elimination
The half-life (t 1 2 ) of a drug is the time it takes of aspirin.
for one half of the drug concentration to be With a kidney disease that results in decreased
eliminated. Metabolism and elimination affect glomerular filtration rate (GFR) or decreased
the half-life of a drug. For example, with liver or renal tubular secretion, drug excretion is slowed
kidney dysfunction, the half-life of the drug is or impaired. Drug accumulation with possible
prolonged and less drug is metabolized and severe adverse drug reactions can result. A
eliminated. When a drug is taken continually, decrease in blood flow to the kidneys can also
drug accumulation may occur. Table 1-1 shows alter drug excretion. Common tests used to
the half-life of selected drugs. A drug goes determine renal function are creatinine
through several half-lives before more than clearance (CLcr) and blood urea nitrogen
90% of the drug is eliminated. If the patient (BUN). Creatinine is a metabolic by-product of
takes 650 mg of aspirin and the half-life is 3 muscle that is excreted by the kidneys. The
hours, it takes 3 hours for the first half-life to creatinine clearance test compares the level of
eliminate 325 mg, 6 hours for the second half- creatinine in the urine with the level of
life to eliminate an additional 162 mg, and so on creatinine in the blood. Creatinine clearance
until the sixth half-life (or 18 hours), when 10 varies with age and gender. Lower values are
mg of aspirin is left in the body (Table 1-2). A expected in older adult and female patients
short half-life is considered to be 4 to 8 hours, because of their decreased muscle mass. GFR
and a long one is 24 hours or longer. If the drug may be the best test, but it is expensive and not
has a long half-life (such as digoxin at 36 hours), so commonly used. A decrease in GFR results in
it takes several days for the body to completely an increase in serum creatinine level and a
eliminate the drug. By knowing the half-life, the decrease in urine creatinine clearance. With
time it takes for a drug to reach a steady state of renal dysfunction either in older adults or as a
serum concentration can be computed. result of kidney disorders, drug dosage usually
Administration of the drug for three to five half- needs to be decreased. In these cases, the
lives saturates the biologic system to the extent creatinine clearance needs to be determined to
that the intake of drug equals the amount establish appropriate drug dosage. When the
metabolized and excreted. An example is creatinine clearance is decreased, drug dosage
digoxin, which has a half-life of 36 hours with likewise may need to be decreased. Continuous
normal renal function. It would take drug dosing according to a prescribed
approximately 5 days to 1 week (three to five dosing regimen without evaluating creatinine
half-lives) to reach a steady state for digoxin clearance could result in drug toxicity.
concentration. PHARMACODYNAMIC PHASE
Excretion, or Elimination Pharmacodynamics is the study of the way
The main route of drug elimination is through drugs affect the body. Drug response can cause a
the kidneys (urine). Other routes include bile, primary or secondary physiologic effect or both.
feces, lungs, saliva, sweat, and breast milk. The The primary effect is desirable, and the
kidneys filter free unbound drugs, water-soluble secondary effect may be desirable or
drugs, and drugs that are unchanged. The lungs undesirable. An example of a drug with a
eliminate volatile drug substances and products primary and secondary effect is
diphenhydramine (Benadryl), an antihistamine. Drugs act through receptors by binding to the
The primary effect ofdiphenhydramine is to treat receptor to produce (initiate) a response or to
the symptoms of allergy, and the secondary block (prevent) a response. The activity of many
effect is a central nervous system depression that drugs is determined by the ability of the drug to
causes drowsiness. The secondary effect is bind to a specific receptor. The better the drug
undesirable when the patient drives a car, but at fits at the receptor site, the more biologically
bedtime it could be desirable because it causes active the drug is. It I similar to the fit of the
mild sedation. right key in a lock. Figure 1-7 illustrates a drug
Dose Response and Maximal Efficacy binding to a receptor.
Dose response is the relationship between the Most receptors, which are protein in nature, are
minimal versus the maximal amount of drug found in cell membranes. Drug-binding sites are
dose needed to produce thedesired drug primarily on proteins,glycoproteins, proteolipids,
response. Some patients respond to a lower drug and enzymes. There are four receptor families:
dose, whereas others need a high drug dose to (1) kinase-linked receptors, (2) ligand-gated ion
elicit the channels, (3) G protein–coupled receptor
desired response. The drug dose is usually systems, and (4) nuclear receptors. The ligand-
adjusted to achieve the desired drug response. binding domain is the site on the receptor at
All drugs have a maximum drug effect (maximal which drugs bind. Kinase-linked receptors. The
efficacy). For example, morphine and tramadol ligand-binding domain for drug binding is on the
hydrochloride (Ultram) are prescribed to relieve cell surface. The drug activates the enzyme
pain. The maximum efficacy of morphine is (inside the cell), and a response is initiated.
greater than tramadol hydrochloride, regardless • Ligand-gated ion channels. The channel spans
of how much tramadol hydrochloride is given. the cell membrane and, with this type of
The pain relief with the use of tramadol receptor, the channel opens, allowing for the
hydrochloride is not as great as it is with flow of ions into and out of the cells. The ions
morphine. are primarily sodium and calcium.
Onset, Peak, and Duration of Action • G protein–coupled receptor systems. There are
One important aspect of pharmacodynamics is three components to this receptor response: (1)
knowing the drug’s onset, peak, and duration of the receptor, (2) the G protein that binds with
action. Onset of action is the time it takes to guanosine triphosphate (GTP), and (3) the
reach the minimum effective concentration effector that is either an enzyme or an ion
(MEC) after a drug is administered. Peak action channel. The system works as follows: drug
occurs when the drug reaches its highest blood __activ_ate_s_receptors __activ_ate_s_G
or plasma concentration. Duration of action is protein__activ_ate_s_effect
the length of time the drug has a pharmacologic • Nuclear receptors. Found in the cell nucleus
effect. Figure 1-6 illustrates the areas in which (not on the surface) of the cell membrane.
onset, peak, and duration of action occur. Some Activation of receptors through the transcription
drugs produce effects in minutes, but others may factors is prolonged. With the first three receptor
take hours or days. A time-response curve groups, activation of the receptors is rapid.
evaluates three parameters of drug action: the Agonists and Antagonists
onset of drug action, peak action, and duration of Drugs that produce a response are called
action. Figure 1-6 indicates these parameters by agonists, and drugs that block a response are
using T (time) with subscripts (e.g., T0, T1, T2, called antagonists. Epinephrine (Adrenalin)
T3). It is necessary to understand the time stimulates beta1 and beta2 receptors, so it is
response in relationship to drug administration. anagonist. Atropine, an antagonist, blocks the
If the drug plasma or serum level decreases histamine (H2)
below threshold or MEC, adequate drug dosing receptor, thus preventing excessive gastric acid
is not achieved; too high a drug level above the secretion. The
minimum toxic concentration (MTC) can result effects of an antagonist can be determined by the
in toxicity. inhibitory
Receptor Theory (I) action of the drug concentration on the
receptor site. IC50
is the antagonist drug concentration required to effects by blocking the synthesis of the bacterial
inhibit 50% cell wall). Drugs also can act by the mechanism
of the maximum biological response. of irritation (e.g., laxatives irritate the inner wall
Nonspecific and Nonselective Drug Effects of the colon, thus increasing peristalsis and
Many agonists and antagonists lack specific and defecation).
selective effects. A receptor produces a variety Therapeutic Index and Therapeutic Range
of physiologic responses, depending on where in (Therapeutic Window)
the body the receptor is located. Cholinergic The safety of drugs is a major concern. The
receptors are located in the bladder, heart, blood therapeutic index (TI) estimates the margin of
vessels, stomach, bronchi, and eyes. A drug that safety of a drug through the use of a ratio that
stimulates or blocks the cholinergic receptors measures the effective (therapeutic) dose (ED) in
affects all anatomic sites of location. Drugs that 50% of people (ED50) and the lethal dose (LD)
affect various sites are nonspecific drugs and in 50% of people (LD50) (Figure 1-10). The
have properties of nonspecificity. Bethanechol closer the ratio is to 1, the greater the danger of
(Urecholine) may be prescribed for toxicity. TI
postoperative urinary retention to increase LD
bladder contraction. This drug stimulates the ED
cholinergic receptor located in the bladder, and = 50
urination occurs by strengthening bladder 50
contraction. Because bethanechol affects the In some cases, the ED may be 25% (ED25) or
cholinergic receptor, other cholinergic sites are 75% (ED75).
also affected. The heart rate decreases, blood Drugs with a low therapeutic index have a
pressure decreases, gastric acid secretion narrow margin of safety (Figure 1-11, A). Drug
increases, the bronchioles constrict, and the dosage might need adjustment, and plasma
pupils of the eye constrict (Figure 1-8). These (serum) drug levels need to be monitored
other effects may be either desirable or harmful. because of the small safety range between the
Drugs that evoke a variety ED and LD. Drugs with a high therapeutic index
of responses throughout the body have a have a wide margin ofsafety and less danger of
nonspecific response. Drugs may act at different producing toxic effects (Figure 1-11, B). Plasma
receptors. Drugs that affect various receptors are (serum) drug levels do not need to be monitored
nonselective drugs or have properties of routinely for drugs with a high TI. The
nonselectivity. Chlorpromazine (Thorazine) acts therapeutic range (therapeutic window) of a
on the norepinephrine, dopamine, acetylcholine, drug concentration in plasma is the level of drug
and histamine receptors, and a variety of between the minimum effective concentration in
responses result from action at these receptor the plasma for obtaining desired drug action and
sites. Epinephrine acts on the alpha1, beta1, and the minimum toxic concentration (the toxic
beta2 receptors (Figure 1-9). Drugs that produce effect). When the therapeutic range is given, it
a response but do not act on a receptor may act includes both protein-bound and unbound
by stimulating or inhibiting enzyme activity or portions of the drug. If the therapeutic range is
hormone production. narrow, such as for digoxin (0.5 to 1 ng/mL), the
Categories of Drug Action plasma drug level should be monitored
The four categories of drug action include (1) periodically to avoid drug toxicity. Monitoring
stimulation or depression, (2) replacement, (3) the therapeutic range is not necessary if the drug
inhibition or killing of organisms, and (4) is not considered highly toxic. When the
irritation. In drug action that stimulates, the rate therapeutic range is given, itincludes both
of cell activity or the secretion from a gland protein-bound and unbound portions of the drug.
increases. In drug action that depresses, cell Table 1-3 lists the therapeutic ranges and toxic
activity and function of a specific organ are levels for anticonvulsants.
reduced. Replacement drugs such as insulin Peak and Trough Drug Levels
replace essential body compounds. Drugs that Peak drug levels indicate the rate of absorption
inhibit or kill organisms interfere with bacterial of the drug and trough drug levels indicate the
cell growth (e.g., penicillin exerts its bactericidal rate of elimination of the drug. Peak and trough
levels are requested for drugs that have a narrow of these expected but undesirable side effects is
therapeutic index and are considered toxic, such not a reason to discontinue therapy. The nurse’s
as the aminoglycoside antibiotics (Table 1-4). If role includes teaching patients to report any side
either the peak or trough level is too high, effects. Many can be managed with dosage
toxicity can occur. If the peak is too low, no adjustments, changing to a different drug in the
therapeutic effect is achieved. Peak drug level same class of drugs, or implementing other
is the highest plasma concentration of drug at a interventions. It is important to know that the
specific time. occurrence of side effects is one of the primary
Peak drug levels indicate the rate of absorption. reasons patients stop taking the prescribed
If the drug is given orally, the peak time might medication. Adverse reactions are more severe
be 1 to 3 hours after drug administration. If the than side effects. They are a range of untoward
drug is given IV, the peak time might occur in effects (unintended and occurring at normal
10 minutes. If a peak drug level is ordered, a doses) of drugs that cause mild to severe side
blood effects, including anaphylaxis (cardiovascular
sample should be drawn at the proposed peak collapse). Adverse reactions are always
time, according to the route of administration. undesirable. Adverse effects must always be
The trough drug level is the lowest plasma reported and documented because they represent
concentration of a drug, and it measures the rate variances from planned therapy. Toxic effects,
at which the drug iseliminated. Trough levels are or toxicity, of a drug can be identified by
drawn immediately before the next dose of drug monitoring the plasma (serum) therapeutic range
is given, regardless of route of administration. of the drug. However, for drugs that have a wide
Loading Dose therapeutic index, the therapeutic ranges are
When immediate drug response is desired, a seldom given. For drugs with a narrow
large initial dose, known as the loading dose, of therapeutic index, such as aminoglycoside
drug is given to achieve a rapid minimum antibiotics and anticonvulsants, the therapeutic
effective concentration in the plasma. After a ranges are closely monitored. When the drug
large initial dose, a prescribed dosage per day is level exceeds the therapeutic range, toxic effects
ordered. Digoxin (Digitek, Lanoxicaps, are likely to occur from overdosing or drug
Lanoxin), a digitalis preparation, requires a accumulation.
loading dose when first prescribed. Pharmacogenetics
Digitalization is the process by which the Pharmacogenetics is the scientific discipline
minimum effective concentration level for studying how the effect of a drug action varies
digoxin is achieved in the plasma within a short from a predicted drug response because of
time. genetic factors or hereditary influence. Because
Side Effects, Adverse Reactions, people have different genetic makeup, they do
and Toxic Effects not always respond identically to a drug dosage
Side effects are physiologic effects not related to or planned drug therapy. Genetic factors can
desired drug effects. All drugs have desirable or alter the metabolism of the drug in converting its
undesirable side effects. Even with a correct chemical form to an inert metabolite; thus, the
drug dosage, side effects occur and are drug action can be enhanced or diminished.
predicted. Side effects result mostly from drugs Some persons are less or more sensitive to drugs
that lack specificity, such as bethanechol and their drug actions because of genetic factors.
(Urecholine). In some health problems, side For example, African Americans do not respond
effects may be desirable (e.g., the use of as well as Caucasians to some classes of
diphenhydramine HCl [Benadryl] at bedtime antihypertensive medications such as ACE
when its side effect of drowsiness is beneficial). inhibitors. (See Chapter 3 for a discussion of
At times, however, side effects are called pharmacogenetics.)
adverse reactions. The terms side effects and Tolerance and Tachyphylaxis
adverse reactions are sometimes used Tolerance refers to a decreased responsiveness
interchangeably in the literature and in speaking, over the course of therapy. In contrast,
but they are different. Some side effects are tachyphylaxis refers to a rapid decrease in
expected as part of drug therapy. The occurrence response to the drug. In essence, tachyphylaxis is
an “acute tolerance.” Drug categories that can may cause hemolytic anemia if some common
cause tachyphylaxis include narcotics, drugs are given)
barbiturates, laxatives, and psychotropic agents. ■ Collect a medication history.
For example, drug tolerance to narcotics can ■ Perform a physical exam to identify problems
result in decreased pain relief for the patient. If that may
the nurse does not recognize the development of affect pharmacodynamics (e.g., elevated BP,
drug tolerance, the patient’s request for more dysrhythmias,
pain medication might be interpreted as drug- or other abnormal findings may be an indication
seeking behavior associated with addiction. for drug therapy).
Prevention of tachyphylaxis should always be ■ Identify side effects of drugs that are
part of the therapeutic regimen (see Chapter 42). nonspecific (same
Placebo Effect receptor at different tissue and organ sites). For
A placebo effect is a psychological benefit from example, when atropine is the drug to be
a compound that may not have the chemical administered, assess for tachycardia, dry mouth
structure of a drug effect. The placebo is and throat, constipation, urinary retention, and
effective in approximately one third of persons blurred vision. If nonspecific drugs are given in
who take a placebo compound. Many clinical large doses or at frequent intervals,
drug studies involve a group of subjects who many side effects are likely to occur.
receive a placebo. The nurse can increase the ■ Check peak levels and trough levels of drugs
therapeutic effect of the drug (e.g., narcotics for such as
pain management) but violate the truth-telling aminoglycosides that have a narrow therapeutic
ethical range. If the trough level is high, toxic effects
principle if a nontherapeutic drug is presented as can result.
a therapeutic agent. Hence, it is required that ■ Check the drug literature for the protein-
participants in drug trials be told from the start binding percentage of the drug. Drugs with a
that they might receive a placebo. To review, the high protein-binding effect have a large portion
phases of drug action are pharmaceutic, of drug bound to protein. This causes the drug to
pharmacokinetic, and pharmacodynamic. Figure become inactive until it is released from the
1-12 illustrates protein. The portion not bound to protein is a
these three phases for drugs given orally, but free and active drug.
drugs given by injection are involved only in the Nursing Interventions
pharmacokinetic and pharmacodynamic phases. ■ Advise patient not to eat high-fat food before
Nurses should be aware that tablets must ingesting an enteric-coated tablet, because high-
disintegrate and go into solution (the fat foods decrease absorption rate.
pharmaceutic phase) to be absorbed. To avoid ■ Report to the health care provider if drugs with
toxic effects, the nurse must know the half-life, a long half-life (i.e., greater than 24 hours) are
protein-binding percentage, normal side effects, given more than once a day. Some drugs with a
and therapeutic ranges of the drug. This long half-life (e.g., the anticoagulant warfarin
information can be obtained from drug reference [Coumadin]) can be more dangerous than others
books. and must be monitored frequently.
Nursing Process ■ Monitor the therapeutic range of drugs that are
Patient-Centered Collaborative Care more toxic or have a narrow therapeutic range
Assessment (e.g., digoxin).
■ Take patient history to identify factors that Cultural Considerations
may affect drug pharmacokinetics (e.g., gastric ■ Be aware that individuals of some ethnic or
surgery will affect absorption; low serum racial heritage metabolize drugs differently than
albumin will affect protein binding; peripheral the general population.
vascular disease may affect drug distribution to Assess for adverse effects that may result from
extremities). Examine the patient’s history to this variation in metabolism.
identify factors that may affect Evaluation
pharmacodynamics (e.g., a G6PD deficiency ■ Evaluate the determinants that affect drug
therapy
according to Figure 1-13. b. Every other day
■ Assess for signs and symptoms of drug c. Twice weekly
toxicity when giving two drugs that are highly d. Once weekly
protein-bound. The drugs compete for protein- 3. The nurse is explaining drug action to a
binding sites, and displacement of drugs occurs. nursing student. Which statement made by the
More free drug is in circulation because there are nurse is correct?
not enough protein-binding sites. Too much of a a. “Water-soluble and ionized drugs are quickly
free drug can result in drug toxicity. absorbed.”
FIGURE 1–13 Determinants that affect drug b. “A drug not bound to protein is an active
therapy. drug.”
c. “Most receptors are found under the cell
membrane.”
d. “Toxic effects can result if the trough level is
low.”
4. The nurse is caring for a patient with
congestive heart failure who is receiving digoxin
(Digitek, Lanoxicaps, Lanoxin). The nurse plans
to take which action when administering
digoxin?
a. Check the peak levels of digoxin.
b. Check the trough levels digoxin.
c. Monitor for tachyphylaxis.
d. Monitor the therapeutic range of digoxin.
5. The nurse anticipates that the health care
provider will order which laboratory test for an
older adult with renal dysfunction?
a. Creatinine clearance
b. Glomerular filtration rate
c. Urine specific gravity
d. Urine pH
6. When reviewing the patient’s medication
Which components of pharmacokinetics does the regimen, the nurse understands that the interval
nurse need to understand before administering a of drug dosage is related to what?
drug? (Select all that apply.) a. Half-life
a. Drugs with a smaller volume of drug b. Stimulation of receptors
distribution have a longer half-life. c. Therapeutic index
b. Oral drugs are dissolved through the process d. Trough level
of 7. Which nursing assessment(s) will the nurse
pinocytosis. include when developing a patient medication
c. Patients with kidney disease may have fewer plan? (Select all that apply.)
proteinbinding a. Check peak and trough levels of drugs.
sites and are at risk for drug toxicity. b. Check the drug literature for the protein-
d. Rapid absorption decreases the bioavailability binding percentage of a drug.
of the drug. c. Identify side effects of drugs that are
e. When the drug metabolism rate is decreased, nonspecific.
excess drug accumulation can occur, which can d. Evaluate the patient’s reaction to a drug.
cause toxicity. e. To enhance absorption, advise the patient to
2. The nurse will question the health care crush an enteric-coated tablet before taking.
provider if a drug with a half-life (t 1 2 ) of more 8. A student nurse is studying the phases of drug
than 24 hours is ordered to be given more than action. Which statement by the student indicates
how often? to the nursing instructor that the student
a. Once daily understands the pharmaceutic phase?
a. “To achieve drug action, drugs are moved by
four processes.”
b. “For the drug to cross the biologic membrane,
the drug becomes a solution.”
c. “In this phase, drugs are concentrated and a
biologic or physiologic response occurs.”
d. “The pharmaceutic phase is the process by
which the drug becomes available to body fluids
and tissue.”
9. The nurse plans to advise the patient to avoid
which
food(s) before ingesting an enteric-coated
medication?
(Select all that apply.)
a. Bananas
b. Baked lamb chops
c. Broiled fish
d. Ice cream
e. Fried chicken
You might also like
- Module 6A - Phases of Drug Action - Pharmacokinetic-3Document11 pagesModule 6A - Phases of Drug Action - Pharmacokinetic-3weissNo ratings yet
- Into Small Particles and Combine With A Liquid To Form A Solution, A Process Known As DISSOLUTION (DrugsDocument6 pagesInto Small Particles and Combine With A Liquid To Form A Solution, A Process Known As DISSOLUTION (DrugsMaemae MonNo ratings yet
- notesDocument7 pagesnotesBlessed Glaiza MarianoNo ratings yet
- Pharma Unit 3 2022Document51 pagesPharma Unit 3 2022John Dave V. VillarmenteNo ratings yet
- Phases of Drug Action: Absorption and PharmacokineticsDocument153 pagesPhases of Drug Action: Absorption and PharmacokineticsNicole NipasNo ratings yet
- Nursing Pharmacology 2023Document355 pagesNursing Pharmacology 2023jaizamaeenriquez59No ratings yet
- Pharmacology Transes - Unit 1Document13 pagesPharmacology Transes - Unit 1venturaphoenixNo ratings yet
- Pharmacology in Nursing - 1Document3 pagesPharmacology in Nursing - 1Buat UmumNo ratings yet
- TMDR PharmaChapter3Document8 pagesTMDR PharmaChapter3JkimNo ratings yet
- A3 Introduction To Drug ActionDocument55 pagesA3 Introduction To Drug ActionSHIELOU LOMODNo ratings yet
- Membrane Permeability Versus Lipid (Olive Oil) :water Partition Coefficient ÀDocument11 pagesMembrane Permeability Versus Lipid (Olive Oil) :water Partition Coefficient ÀWindiarti RahayuNo ratings yet
- PharmacokineticsDocument112 pagesPharmacokineticsGog Rg100% (2)
- Pharma Unit 3 2022 MidtermDocument57 pagesPharma Unit 3 2022 MidtermJohn Dave V. VillarmenteNo ratings yet
- Pharmaceutic Phase: Drug Becomes A Solution So It Can Cross TheDocument8 pagesPharmaceutic Phase: Drug Becomes A Solution So It Can Cross TheSarah Jane NavascaNo ratings yet
- C. Drug Action 1Document28 pagesC. Drug Action 1Jay Eamon Reyes MendrosNo ratings yet
- Philippine National FormularyDocument7 pagesPhilippine National FormularyShaira Dawn D. PLANCONo ratings yet
- Bioavailability Factors and Drug Absorption RatesDocument30 pagesBioavailability Factors and Drug Absorption RatesRose Lyn Camarista VelascoNo ratings yet
- Pharmacology Modules 1 - 2Document10 pagesPharmacology Modules 1 - 2Elvira GumiNo ratings yet
- N-Lec2 - PharmacokineticsDocument41 pagesN-Lec2 - Pharmacokineticsgeng gengNo ratings yet
- Pharmacokinetic & PharmacodynamicDocument77 pagesPharmacokinetic & Pharmacodynamicdimasscrib100% (1)
- PharmacokineticsDocument17 pagesPharmacokineticsღ آلَعٌرآقُيِة نِوٌر ღNo ratings yet
- Biopharmaceutics and Clinical Pharmacokinetics - 20210831 - 212949Document22 pagesBiopharmaceutics and Clinical Pharmacokinetics - 20210831 - 212949Md. Abu Bakar Siddique TayefNo ratings yet
- Pharmacologic PrinciplesDocument57 pagesPharmacologic PrinciplesYousef Jafar100% (1)
- Pharmaco KineticsDocument10 pagesPharmaco KineticsVithyaah ParameswaranNo ratings yet
- Drug Absorption, Distribution, and First-Pass EliminationDocument60 pagesDrug Absorption, Distribution, and First-Pass EliminationRuqayya AdamuNo ratings yet
- Biopharmaceutics KU (Maam Shaista)Document13 pagesBiopharmaceutics KU (Maam Shaista)areebaNo ratings yet
- PharmacokineticsDocument36 pagesPharmacokineticsRochelle RagoNo ratings yet
- 3.Unit.pharmacokinetics 2Document40 pages3.Unit.pharmacokinetics 22020253350No ratings yet
- Pharma CompilationDocument113 pagesPharma CompilationGulayan, Renz Bryelle T.No ratings yet
- PHRM 0 KinetcxDocument37 pagesPHRM 0 KinetcxbumchikkNo ratings yet
- Pharmacology: Nepthali Christuar Aldueza, R.N. Calamba Doctors CollegeDocument49 pagesPharmacology: Nepthali Christuar Aldueza, R.N. Calamba Doctors CollegeArielle Joy Atienza100% (1)
- Chapter 2: Pharmacokinetics and Factors of Individual Variation Drug FormsDocument4 pagesChapter 2: Pharmacokinetics and Factors of Individual Variation Drug FormsDaniel LyndsNo ratings yet
- Food and Drug InteractionDocument37 pagesFood and Drug InteractionAhadul Islam FahimNo ratings yet
- Food Drug Interactions 2018 PDFDocument193 pagesFood Drug Interactions 2018 PDFArianna RampersadNo ratings yet
- Pharmacokinetics Lecture NotesDocument22 pagesPharmacokinetics Lecture Notesbmhsh100% (2)
- Factor Affecting Drug AbsorptionDocument4 pagesFactor Affecting Drug Absorptionwriter noreenNo ratings yet
- PharmacologyDocument21 pagesPharmacologyMaridel Estioco100% (3)
- Pharmacology Final Study GuideDocument28 pagesPharmacology Final Study GuideAnthony Palladeno100% (1)
- Drug Absorption 01Document15 pagesDrug Absorption 01Jannaatul Ferdous MimNo ratings yet
- Biopharmaceutics and Pharmacokinetics: Pharmacy Board Review Module 4Document73 pagesBiopharmaceutics and Pharmacokinetics: Pharmacy Board Review Module 4Kate EvangelistaNo ratings yet
- Drug Metabolism and Excretion ExplainedDocument21 pagesDrug Metabolism and Excretion ExplainedPutri Zharifah MeutiaNo ratings yet
- Principles of Pharmacology Chapter 1Document37 pagesPrinciples of Pharmacology Chapter 1Muhammad ZakriaNo ratings yet
- Drug MetabolisumDocument14 pagesDrug MetabolisumDevdeep Roy ChowdhuryNo ratings yet
- Krystal Jane B. Salinas BSN 2. Date: June 22, 2019 NCM 106 PharmacologyDocument11 pagesKrystal Jane B. Salinas BSN 2. Date: June 22, 2019 NCM 106 PharmacologyKrystal Jane SalinasNo ratings yet
- Pharmacokinetics ADME GuideDocument81 pagesPharmacokinetics ADME GuideSiddh PatelNo ratings yet
- ACTIVITY # 2 Pharmacology SubjectDocument3 pagesACTIVITY # 2 Pharmacology SubjectSamantha Grace SuicoNo ratings yet
- What Is Drug Absorption?: Yolanda Smith, B.PharmDocument5 pagesWhat Is Drug Absorption?: Yolanda Smith, B.PharmNoorNo ratings yet
- Dasar FarmakologiDocument102 pagesDasar FarmakologiAvivah Rohmatul JannahNo ratings yet
- GRDDSDocument31 pagesGRDDSMuhammad Azam TahirNo ratings yet
- Basic Principles of PharmacologyDocument47 pagesBasic Principles of Pharmacologysapiah raman100% (2)
- Pharma - 2020 General Principles of Drug ActionDocument163 pagesPharma - 2020 General Principles of Drug Actiongelean payodNo ratings yet
- Tugas Biofarmasetika 1 Metabolisme: Nama: Yuliano Medora No BP: 1201169 Kelas: Reguler Stifarm Padang 2013Document21 pagesTugas Biofarmasetika 1 Metabolisme: Nama: Yuliano Medora No BP: 1201169 Kelas: Reguler Stifarm Padang 2013Putri Zharifah MeutiaNo ratings yet
- General Pharmacology ExplainedDocument386 pagesGeneral Pharmacology ExplainedMaksym DemianchukNo ratings yet
- Gastroretentive Drug Delivery SystemDocument33 pagesGastroretentive Drug Delivery SystemSaid Muhammad WazirNo ratings yet
- Food, Gastrointestinal PH, and Models of Oral Drug AdsorptionDocument14 pagesFood, Gastrointestinal PH, and Models of Oral Drug AdsorptionEster VillacampaNo ratings yet
- Food, Gastrointestinal PH, and Models of Oral Drug AdsorptionDocument6 pagesFood, Gastrointestinal PH, and Models of Oral Drug AdsorptionEster VillacampaNo ratings yet
- Routes of Drug AdministrationDocument28 pagesRoutes of Drug AdministrationApurba Sarker Apu100% (1)
- Handbook of Drug Interaction and the Mechanism of InteractionFrom EverandHandbook of Drug Interaction and the Mechanism of InteractionRating: 1 out of 5 stars1/5 (1)
- Leaky Gut Syndrome Stop!: A Complete Guide To Leaky Gut Syndrome Causes, Symptoms, Treatments & A Holistic System To Eliminate LGS Naturally & PermanentlyFrom EverandLeaky Gut Syndrome Stop!: A Complete Guide To Leaky Gut Syndrome Causes, Symptoms, Treatments & A Holistic System To Eliminate LGS Naturally & PermanentlyNo ratings yet
- GenPhysics1 - Q1MELC1-5W1 MeasurementDocument10 pagesGenPhysics1 - Q1MELC1-5W1 MeasurementShane Ureta100% (1)
- Practical Research 2: Quarter 1 - Module 1Document37 pagesPractical Research 2: Quarter 1 - Module 1VIGO, JERECELNo ratings yet
- Performance Output in Reading and Writing Quarter 3 Module 1 Jerome G. Vigo Grade 11 LagmayDocument2 pagesPerformance Output in Reading and Writing Quarter 3 Module 1 Jerome G. Vigo Grade 11 LagmayVIGO, JERECELNo ratings yet
- Here are the answers to the questions in "What I Know":1. a2. d 3. cDocument28 pagesHere are the answers to the questions in "What I Know":1. a2. d 3. cMary Ann Isanan91% (92)
- Conic Sections ParabolaDocument7 pagesConic Sections ParabolaVIGO, JERECELNo ratings yet
- Interfere Whose Using Your Data, When and Why It Is Used. Know Your Right As A UserDocument1 pageInterfere Whose Using Your Data, When and Why It Is Used. Know Your Right As A UserVIGO, JERECELNo ratings yet
- Social Inequalities: Causes, Effects and SolutionsDocument2 pagesSocial Inequalities: Causes, Effects and SolutionsVIGO, JERECELNo ratings yet
- NHJDocument8 pagesNHJVIGO, JERECELNo ratings yet
- LyricsDocument1 pageLyricsVIGO, JERECELNo ratings yet
- Packing List: Music FestivalDocument1 pagePacking List: Music FestivalVIGO, JERECELNo ratings yet
- Event Name Here: Sub Heading Goes HereDocument2 pagesEvent Name Here: Sub Heading Goes HerevenspalNo ratings yet
- Cherry G. Vigo Cherry G. Vigo: Contact #: 09388848129 Contact #: 09388848129Document1 pageCherry G. Vigo Cherry G. Vigo: Contact #: 09388848129 Contact #: 09388848129VIGO, JERECELNo ratings yet
- What Is Gender and Development (Gad)Document3 pagesWhat Is Gender and Development (Gad)VIGO, JERECELNo ratings yet
- Bio 124 Lab SensesDocument20 pagesBio 124 Lab SensesJuliaNo ratings yet
- Allergy Testing PDFDocument25 pagesAllergy Testing PDFRK MalhotraNo ratings yet
- The Five Major Brances of Chemistry and Their Sub-BranchesDocument3 pagesThe Five Major Brances of Chemistry and Their Sub-BranchesYenna Rezano LumbaNo ratings yet
- Happiness, Quality of Sleep and Academic Achievement Among University UndergraduatesDocument1 pageHappiness, Quality of Sleep and Academic Achievement Among University UndergraduatesDemuel Dee L. BertoNo ratings yet
- Infowar and Spiritual Apocalypse The Destiny of Mankind: DR Bill Deagle MDDocument37 pagesInfowar and Spiritual Apocalypse The Destiny of Mankind: DR Bill Deagle MDprateekthaparian100% (1)
- Pharmaceutical Care Plan - Sample Version: (Dispensing and Medication Safety)Document4 pagesPharmaceutical Care Plan - Sample Version: (Dispensing and Medication Safety)Angela Pabico RosarioNo ratings yet
- Algorithms For The Design of A Multi-Stage Adaptive Kanban SystemDocument33 pagesAlgorithms For The Design of A Multi-Stage Adaptive Kanban SystemKharisma ElanNo ratings yet
- ScienceDocument17 pagesScienceTambong HailyNo ratings yet
- Chrysothemis PulchellaDocument2 pagesChrysothemis PulchellaTharayilsijNo ratings yet
- Report On Native Konbac Bamboo Product Private LimitedDocument3 pagesReport On Native Konbac Bamboo Product Private LimitedSuprio SahaNo ratings yet
- Botany Class 11thDocument258 pagesBotany Class 11thwebdeveloperavinash28No ratings yet
- PASTURE MANAGEMENT - Final PDFDocument101 pagesPASTURE MANAGEMENT - Final PDFDexter Andrew Lyken100% (1)
- Steroid AbuseDocument7 pagesSteroid Abuseapi-400575655No ratings yet
- Cladistics PDFDocument4 pagesCladistics PDFmanoj_rkl_07100% (1)
- Substance Form and Transprort Learning IssuesDocument8 pagesSubstance Form and Transprort Learning IssuesIftitah N. RNo ratings yet
- Grade Ix Biology Animal Tissues 2021Document55 pagesGrade Ix Biology Animal Tissues 2021Purvi Prakash KNo ratings yet
- CP RBC DisorderDocument15 pagesCP RBC DisorderDETECTIVE CONANNo ratings yet
- NEURON ACTION POTENTIAL - PPT - ReadyDocument83 pagesNEURON ACTION POTENTIAL - PPT - Readyelle leeNo ratings yet
- (MCQS) On "Solar Radiation"-MergedDocument115 pages(MCQS) On "Solar Radiation"-MergedMahavirsinh PadheriyaNo ratings yet
- Free PTE-A Exam Memories MaterialDocument133 pagesFree PTE-A Exam Memories MaterialSudarkarthikNo ratings yet
- ReportDocument2 pagesReportCherey BaguioNo ratings yet
- Quiz 1A Hema LecDocument17 pagesQuiz 1A Hema LecAngela ReyesNo ratings yet
- Blakemore Frith 2005 The Leaning BrainDocument221 pagesBlakemore Frith 2005 The Leaning BrainVictor MN100% (2)
- WHO 4th Intl Standard For HCVDocument2 pagesWHO 4th Intl Standard For HCVSagir AlvaNo ratings yet
- USABO 14 Open Exam Final AnsDocument16 pagesUSABO 14 Open Exam Final AnsGuest SuiteNo ratings yet
- Pattern Matching: Classifying Organic MoleculesDocument8 pagesPattern Matching: Classifying Organic MoleculesBhaavana AnnaNo ratings yet
- Spinal TraumaDocument81 pagesSpinal TraumaharilNo ratings yet
- Perspectives For Using Rna Sequencing Analysis of The Genome To Understand The Mechanisms of AgingDocument3 pagesPerspectives For Using Rna Sequencing Analysis of The Genome To Understand The Mechanisms of AgingHerald Scholarly Open AccessNo ratings yet
- Osmosis in Plant & Animal CellsDocument2 pagesOsmosis in Plant & Animal CellsBrooke MorganNo ratings yet
- EECP IabpDocument16 pagesEECP IabpMythily VedhagiriNo ratings yet