Professional Documents
Culture Documents
Test and Eval
Uploaded by
Anne SerneoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Test and Eval
Uploaded by
Anne SerneoCopyright:
Available Formats
lOMoARcPSD|8901201
Test and Evaluation 2 - Summary Physical therapy
Physical therapy (Our Lady of Fatima University)
StuDocu is not sponsored or endorsed by any college or university
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
TEP 2 LECTURE REVIEWER innervation by the dorsal roots and
peripheral nerves.
EXAMINATION OF SENSORY FUNCTION
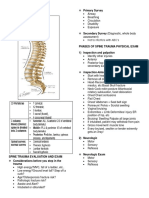
Dermatomes
Sensory Integration
- AKA: Skin-segment
- It is the ability of the brain to organize,
- Refers to the skin area supplied by one
interpret and use sensory information.
dorsal root.
- Neurological process that organizes the
sensation from one’s own body and from C1 No dermatome (Pure Motor)
the environment and make it possible to use C2 Occiput
the body effectively within the environment C3 Supraclavicular fossa
C4 Superior Acromioclavicular Joint
Purpose of Sensory Integration C5 Lateral side of the forearm (Deltoid Area)
✓ Explaining behaviors of individuals with C6 Thumb
C7 Middle Finger
impaired sensory integration functions.
C8 Little Finger
✓ Establishing a Plan of Care to address
T1 Medial side of the forearm
specific impairments
T2 Apex of Axilla
✓ Predicting expected outcomes of the
T3 3rd ICS
selected interventions
T4 At nipple line
Sensation & Movement T5 5th ICS
T6 Xiphoid Process
1. Feedback Control T7 7th ICS
- Uses sensory information received during the T8 8th ICS
movement to monitor and adjust output T9 9th ICS
2. Feedforward Control T10 Umbilicus
- It is a proactive strategy that uses sensory T11 11th ICS
information obtained from experience T12 Inguinal Ligament
L1 Between T12 and L2
Primary Roles of Sensation Movements L2 Mid-anterior Thigh
✓ Guide selection of motor responses for L3 Medial Femoral Condyle
L4 Medial Malleolus
effective interaction with the environment
L5 Dorsum of the Foot
✓ Adapt movements and shape motor
S1 Lateral Heel
programs through feedback for corrective
S2 Popliteal Fossa
action.
S3 Ischial Tuberosity
✓ It Also protects the organism from injury
S4-S5 Peri-anal Area
Sensory Integrity
- Intactness of cortical sensory processing, Spinal Cord Tract
including proprioception, pallesthesia, - Provides data that reflect integrity of the
stereognosis and topognosis
spinal cord tracts that carry somatosensory
Somatosensory information.
- AKA: Somatosensation Age-Related Sensory Changes
- Sensation received from the skin and
- Alterations in sensory function occur with
musculoskeletal system
normal aging.
Clinical Indications
Arousal
✓ History
- It is the physiological readiness of human
✓ Systems of Review
system for an activity.
Pattern of Sensory Impairment
ATTENTION
- Pattern identification is accomplished using
knowledge of skin segment (Dermatome)
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- Selective awareness of the environment or 1. Fund of Knowledge
responsiveness to a stimulus or task without - Defined as the sums total of an individual’s
being distracted by other stimuli learning and experience in life
2. Calculation Ability
Level of Consciousness
- Examines foundational mathematical
1. ALERT abilities.
- Patient is awake and attentive to normal - Dyscalculia (Difficulty in accomplishing
interactions. calculation
- Interaction with therapist are normal and - Acalculia (inability to calculate)
appropriate. 3. Proverb Interpretation
2. LETHARGIC - Examines the patient’s ability to interpret use
- Patient appears drowsy and may fall asleep of words outside of their usual context or
- Interactions with therapist may be diverted meaning.
- Patient may have difficulty in focusing or
Types of Memory
maintaining attention on a question or task.
3. OBTUNDED 1. Long-Term Memory
- Patient is difficult to arouse from a - AKA: Remote Memory
somnolent state and is frequently confused - Can be examined by requesting information
when awake. on date and place of birth, number of
- Repeated stimulation is required to maintain siblings, date of marriage, schools attended
consciousness and historical facts.
- Interaction with therapist may be largely 2. Short-Term Memory
unproductive. - Can be addressed by verbally providing the
4. STUPOR patient with a series of words or numbers.
- AKA: Semi-coma
Hearing
- Patient responds only to strong, generally
noxious stimuli and returns to the - Note should be made of how alterations in
unconscious state when stimulation is voice volume and tone influence patient
stopped. response.
- When aroused, patient is unable to interact
with the therapist. Visual Acuity
5. COMA
- A gross visual examination can be made by
- AKA: Deep coma
use of a standard Snellen chart mounted on
- Patient cannot be aroused by any type of
the wall or visual acuity cards for use at
stimulation
bedside
- Reflex motor responses may or not may be
seen. Classification of Sensory System
Orientation Sensory Receptors
- Refers to the patient awareness of time, - AKA: Sensory Nerve Endings
person, place and event - Located at the distal end of an afferent
- To document: If the patient is fully oriented in fiber.
this domain, you can write Oriented x4 - Highly sensitive to the type of stimulus
- If the patient is not fully oriented to one or
more domains, (e.g. Oriented x2 (time, Labeled Line Principle
place) - Specificity of nerve fiber sensitivity to a single
COGNITION modality of sensation
- Individual tactile sensations are perceived
- Defined as the process of knowing and when specific types of receptors are
includes both awareness and judgement. stimulated.
3 AREAS FOR TESTING COGNITION-DEPENDENT 3 DIVISION OF SENSORY RECEPTORS
FUNCTION TESTING
1. Superficial Sensation
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
a. Exteroreceptors Types of Sensory Receptor
- Responsible for superficial sensation
I. Mechanoreceptors
- They receive stimuli from the external
- Respond to mechanical deformation of the
environment via the skin and subcutaneous
receptor or surrounding area
tissue. A. CUTANEOUS RECEPTORS
- Responsible for the perception of pain, - Located at the terminal portion of the
temperature, light touch, and pressure afferent fiber.
2. Deep Sensation 1. FREE NERVE ENDINGS
a. Proprioceptors - Found throughout the body
- Responsible for deep sensation - Stimulation of free nerve endings results in
- Receive stimuli from muscles, tendons, perception of pain, temperature, touch,
ligaments, joints, and fascia, pressure, tickle and itch sensation.
- Responsible for position sense and 2. HAIR FOLLICLE ENDINGS
awareness of joints at rest, movement - AKA: Hair-End Organs
awareness (kinesthesia), and vibration - At the base of each hair follicle a free nerve
3. Combined and Cortical Sensation ending is entwined.
- These sensations require information from - The combination of the hair follicle and its
both exteroceptive and proprioceptive nerve provides a sensitive receptor.
receptors, as well as intact function of - These receptors are sensitive to mechanical
movement and touch.
cortical sensory association areas.
3. MERKEL’S DISCS
- The cortical combined sensations include
- AKA: Tactile Discs
stereognosis, two-point discrimination,
- Located below the epidermis in hairless
barognosis, graphesthesia, tactile
smooth (glabrous) skin with a high density in
localization, recognition of texture, and
the fingertips.
double simultaneous stimulation.
- They are sensitive to low-intensity touch,
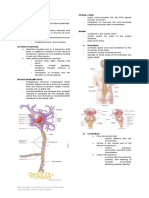
Spinal Pathways as well as to the velocity of touch, and
respond to constant indentation of the skin
- Sensations are mediated by either the (pressure)
ANTEROLATERAL SPINOTHALAMIC SYSTEM or - They provide for the ability to perceive
the DORSAL COLUMN-MEDIAL LEMNISCAL continuous contact of objects against the
SYSTEM skin and are believed to play an important
1. Anterolateral Spinothalamic System role in both two-point discrimination and
- Initiates self-protective reactions and localization of touch.
responds to stimuli that are potentially 4. RUFFINI ENDINGS
harmful in nature. - Located in the deeper layers of the dermis
- (+) Slow-conducting fibers of small diameter - Encapsulated endings are involved with the
(unmyelinated) perception of touch and pressure
- Function: Concerned with transmission of - They are slowly adapting and particularly
thermal and nociceptive information, and important in signaling continuous skin
mediates pain, temperature, crudely deformation such as tension or stretch
localized touch, tickle, itch, and sexual - They are also found in joint capsules and
sensations assist with joint position sense
2. Dorsal Column-Medial Lemniscal System 5. Krause-End Bulb
- Involved with responses to more - AKA: Bulboid Corpuscle
discriminative sensations. - Located in the dermis and conjunctiva of
- Contains fast-conducting fibers of large the eye
diameter with greater myelination - They are believed to be low-threshold
- Function: Mediates the sensations of mechanical receptors that may play a
discriminative touch and pressure contributing role in the perception of touch
sensations, vibration, movement, position and pressure.
sense, and awareness of joints at rest. 6. Meissner Corpuscle
- AKA: Corpuscle of Touch
- Located in the dermis, these encapsulated
nerve endings contain many branching
nerve filaments within the capsule
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- They are low-threshold, rapidly adapting - Found in the joint capsule and ligaments,
and in high concentration in the fingertips, these receptors are believed to respond to
lips, and toes, areas that require high levels pain and crude awareness of joint motion
of discrimination. 3. RUFFINI ENDING
- Plays an important role in discriminative - Located in the joint capsule and ligaments
touch (e.g., recognition of texture) and - Ruffini endings are responsible for the
movement of objects over skin direction and velocity of joint movement.
7. Pacinian Corpuscles - ALSO KNOWN FOR RUFFINIT (HOT)
- AKA: Lamellated Corpuscle 4. PACINIFORM ENDINGS
- subcutaneous tissue layer of the skin and in - These receptors are found in the joint
deep tissues of the body (including tendons capsule and primarily monitor rapid joint
and soft tissues around joints) movements.
- stimulated by rapid movement of tissue and III. THERMORECEPTORS
are quickly adapting - Respond in temperature
- They play a significant role in the perception IV. NOCICEPTORS
of deep touch and vibration. - Respond to noxious stimuli and result in the
II. Deep Sensory Receptors perception of pain
- Located in muscles, tendons, and joints V. CHEMORECEPTORS
- Concerned primarily with posture, - Respond to chemical substances and are
position sense, proprioception, muscle tone, responsible for taste, smell, oxygen levels in
and speed and direction of movement arterial blood, CO2 concentration and
A. MUSCLE RECEPTORS osmolality (concentration gradient) of the
1. MUSCLE SPINDLE body.
- The muscle spindle fibers (intrafusal fibers) lie VI. Photic
in a parallel arrangement to the muscle - AKA: Electromagnetic Receptors
fibers (extrafusal fibers). - Respond to light with in the visible spectrum
- They monitor changes in muscle length (Ia
Spinal Cord Pathway
and II spindle afferent endings) as well as
velocity (Ia ending) of these changes.
- Plays a vital role in position and movement
2.
sense and in motor learning.
GOLGI TENDON ORGANS (GTO)
VEM DAS
- Located in series at both the proximal and
distal tendinous insertions of the muscle
- Monitor tension within the muscle. Corticospinal: Rapid Spinothalamic Tract
- Provide a protective mechanism by skilled voluntary;
a. Anterior
preventing structural damage to the muscle decussation of the
pyramids (medulla inf. Spinothalamic
in situations of extreme tension - Light Touch &
Border)
- This is accomplished by inhibition of the Pressure
contracting muscle and facilitation of the Rubrospinal: Facilitates b. Lateral
antagonist flexor muscles & inhibit Spinothalamic
3. FREE NERVE ENDINGS extensor/anti-gravity - Pain &
muscles Temperature
- These receptors are within the fascia of the
muscle. Tectospinal: Reflex Spinocerebellar
- They are believed to respond to pain and postural movement in
pressure. response to visual stimuli - Unconscious
jt/mm sense
- PACINIAN CORPUSCLES
Vestibulospinal: Facilitate
- AKA: Lamellated Corpuscles extensor muscles & inhibit Dorsal Column
- Located within the fascia of the muscle, flexor muscles
- Conscious
these receptors respond to vibratory stimuli
Olivospinal: Influence - Proprioception
and deep pressure. - Kinesthesia
activity of motor neurons
B. JOINT RECEPTORS - Vibration
1. GOLGI TYPE ENDINGS Reticulospinal:
- These receptors are located in the Inhibit/facilitate
ligaments, and function to detect the rate movement
of joint movement.
2. FREE NERVE ENDINGS
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
EQUIPMENT Hypalgesia Decrease sensitivity to
pain
EQUIPMENT Hyperalgesia Increase sensitivity to pain
1. PAIN Hypesthesia Decrease sensitivity to
- Large safety pain / Large paper clip (one sensory stimuli
segment open Pallanesthesia Loss or absence of
2. TEMPERATURE sensibility to vibration
- Two standard laboratory test tubes Paresthesia Abnormal sensation such
with stoppers as numbness, prickling, or
3. LIGHT TOUCH tingling, without apparent
- COTTON / TISSUE / CAMEL BRUSH cause
4. VIBRATION Thalamic Syndrome Vascular lesion of the
- Tuning Fork / Earphones thalamus resulting in
5. STEREOGNOSIS (OBJECT RECOGNITION) sensory disturbances and
- Comb, fork, paper/ etc. partial or complete
6. 2 POINT DISCRIMINATION paralysis of one side of
- Aesthesiometer the body, associated with
- ECG CALIPER severe, boring-type pain;
sensory stimuli may
2-Point Discrimination Normal Values and produce an
Discrimination Distances Required for Certain Tasks exaggerated, prolonged,
or painful response
Normal Less than 6 mm
Fair 6 to 10 mm
Thermanalgesia Inability to perceive heat
Poor 11 to 15 mm
Thermanesthesia Inability to perceive
Protective 1 point perceived
sensations of heat and
Anesthetic 0 point perceived
cold
Winding a Watch 6 mm
Thermhypesthesia Decreased temperature
Sewing 6 t0 8 mm sensibility
Handling Precision Tools 12 mm Thermhyperesthesia Increased temperature
Gross Tool Handling Greater than 15 mm sensibility
7. RECOGNITION OF TEXTURE Thigmanesthesia Loss of light touch
- Cotton, wool, burlap, silk sensibility
TERMINOLOGY DESCRIBING COMMON SENSORY
IMPAIRMENT
Abarognosis Inability to recognize
weight
Allesthesia Sensation experienced at
a site remote from a point
of stimulation
Allodynia Pain produced from non-
noxious stimuli
Analgesia Complete loss of pain
sensitivity
Astereognosis/Tactile Inability to recognize the
Agnosia form and shapes of
objects by touch
Atopognosia Inability to localize a
sensation
Causalgia Painful, burning
sensations, usually along
the distribution of a nerve
Dysesthesia Touch sensation
experienced as pain
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
EXAMINATION OF MOTOR FUNCTION Neuroplasticity
MOTOR CONTROL - Capacity of the brain to adapt to injury
through mechanism of repair and change.
- Complex set of neural, physical and
behavioral process that govern posture and Motor Learning
movement.
- Set of internal processes associated with
REFLEX PATTERNS practice or experience leading to relatively
permanent changes.
- Automatic (Walking and Breathing)
- Motor Skills (Writing and Reading) FEEDBACK
HOW IS IT DEVELOPED? - Response-produced information receives
during or after the movement
SENSORY INFORMATION - Use to monitor output for corrective actions.
FEEDFORWARD
- Sending signals in advance of movement to
ready the sensorimotor systems
- Allows for anticipatory adjustments in
PRACTICE & FEEDBACK postural activity.
MOTOR CONTROL THEORIES
1. Dynamic Control Systems Theory
- Units of the CNS are organized around a
specific task demands
MOTOR LEARNING - SMALL TASK: small part of the brain will
activate it
- COMPLEX TASK: All parts of the brain will
activate it
2. Hierarchical Control Theory
MOTOR SKILLS HIGHER LEVEL
Represented by the association areas of the neocortex and basal
ganglia of the forebrain
Motor Program Concerned with strategy: the goal of the movement and the
movement strategy that best achieves the goal
- Abstract representation that, when initiated,
results in production of a coordinated
sequence. MIDDLE LEVEL
- Brain and Spinal Cord
Represented by the motor cortex and cerebellum,
Motor Plan
Concerned with tactics: the sequences of muscle contractions, arranged in
- A set of Motor Program space and time, required to
smoothly and accurately achieve the strategic goal.
Motor Memory
- Recall of the motor program
LOWER LEVEL
- INITIAL MOVEMENT CONDITION
- HOW THE MOVEMENT FELT, LOOKED AND Represented by the brain stem and spinal cord
SOUNDED (SENSORY CONSEQUENCES)
Concerned with execution: activation of the
- SPECIFIC MOVEMENT PARAMETERS motor neuron and interneuron pools that generate the goal-directed
(KNOWLEDGE OF PERFORMANCE) movement and make any necessary
adjustments of posture
- OUTCOME OF THE MOVEMENT (KNOWLEDGE
OF RESULTS)
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
EXAMINATION OF MOTOR FUNCTION - Use objective measurement as a way of
examining performance
I. PATIENT HISTORY
A. GENERAL INFORMATION FACTORS THAT MAY CONSTRAIN THE MOTOR
a. Name FUNCTION EXAMINATION
b. Age
1. Mental Status
c. Occupation
a. Consciousness
d. Handedness
- Refers to a state of arousal accompanied
e. Status
by awareness of one’s environment.
f. Religion
g. Referring Unit STIMULI RESPONSE
h. Referring Doctor ALERT NORMAL NORMAL
i. Date of Referral
LETHARGIC DROWSY BRIEFLY
j. Physiatrist in Charge
k. Date of Consultation
l. Diagnosis OBTUNDED SLEEPY CONFUSED
m. Chief of Complaint
n. Informant/Reliability STUPOR VIGOROUS VOLUNTARY
B. BRIEF HISTORY UNPLEASANT
a. History Illness
b. Functional Limitation COMA PAINFUL No Response
C. LABORATORY/ANCILLARY PROCEDURES
D. MEDICATIONS
Minimally Conscious State
E. PAST MEDICAL HISTORY
F. FAMILY MEDICAL HISTORY - AKA: Vegetative State
G. PERSONAL/SOCIAL/ENVIRONMENTAL - Characterize by return of sleep-wake cycle
HISTORY and normalization of the vegetative
II. SYSTEMS OF REVIEW function such as respiration, digestion and
- Screening examinations for identification of blood pressure control
potential problems that may require
extensive testing. Persistent Vegetative State
III. SPECIFIC TEST AND MEASURES
- Individuals who remain in a vegetative state
1. VALIDITY 1 year or longer after TBI and 3 months or
- Accurately measures the parameter of more for anoxic brain injury.
performance being examined. - Caused by severe brain injury
2. RELIABILITY Glasgow Coma Scale
- Reflected in the consistency of results
obtained by a single examiner over repeat - Gold standard instrument used to
trials (INTRARATER RELIABILITY) or among document level of consciousness in acute
multiple examiners (INTERRATER RELIABILITY) brain injury.
3. SENSITIVITY
- Refers to the proportion of times that a
method of analysis correctly identifies an
abnormality as being present (True Positive)
4. SPECIFICITY
- Refers to the proportion of times that a
method analysis correctly identifies an
abnormality as being absent (True
Negative)
5. QUALITATIVE
- Utilizes observations of complex aspects of
performance.
6. QUANTITATIVE
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
GLASGOW COMA SCALE - Can be examined by asking the patient to
ACTIVITY Score attend to a particular task.
Eye Opening - e.g. Digit Span Test
- Spontaneous 4 2. Sustained Attention
- To Speech 3 - It is examined by determining how long the
- To pain 2 patient is able to maintain attention on a
- No response 1 particular task
Best Motor Response
- Attention span
- Obeys Command 6
- Localizing Pain 5 3. Alternating Attention
- Withdrawal from Pain 4 - AKA: Attention Flexibility
- Decorticate 3 - Examined by requesting the patient to
- Decerebrate 2 alternate back and forth between two
- No response 1 different tasks.
Best Verbal Response 4. Divided Attention
- Oriented 5 - Requesting patient to perform two tasks
- Confused conversation 4
simultaneously
- Inappropriate words 3
- Incomprehensible sounds 2 - e.g. Walkie Talkie Test
- No response 1 d. Memory
Interpretation - It is the process of registration, retention and
recall of past-experience, knowledge and
- Mild TBI: 13-15 ideas.
- Moderate TBI: 9-12
- Severe TBI: 3-8 TYPE OF MEMORY ACCORDING TO INFO
Pupillary Size & Reaction 1. Declarative Memory
- AKA: Explicit Memory
1. BILATERALLY SMALL - Involves the conscious recollection of facts,
- Sympathetic pathways in hypothalamus past events, experiences and places.
- Metabolic Encephalopathy 2. Motor Memory
2. PIN-POINTED - AKA: Procedural Memory
- Hemorrhagic Pontine Lesion - Involves recall of movement or motor
- Narcotic Overdose information and storage of motor programs,
3. FIXED IN MID POSITION AND SLIGHTLY sub-routines, schema as well as perceptual
DILATED and cognitive skills.
- Midbrain Damage
4. BILATERALLY LARGE, FIXED, DILATED TYPE OF MEMORY ACCORDING TO LENGTH OF TIME
- Anoxia or Drug Toxicity
1. Short Term Memory
5. UNILATERAL FIXED AND DILATED
- AKA: Recent Memory
- Temporal lobe herniation
- Refers to the capability to remember
Inverted U-Principle current, day to day events.
- Learn new materials and retrieve material
- AKA: Yerkes Dodson Principle after an interval of minutes, hours or days.
- An appropriate level of arousal allows for 2. Long Term Memory
optimal motor performance; very low or - AKA: Remote Memory
high levels of arousal can cause - Refers to the recall of facts or events that
deterioration in motor response. occurred years before.
b. Orientation 3. Immediate Memory
- Refers to the patient’s awareness of time, - AKA: Immediate Recall
place, person and circumstances. - Refers to an immediate registration and
c. Attention recall of information after an interval of a
- Selective awareness of the environment or few seconds.
responsiveness to a stimulus or task without 4. Working Memory
being distracted by other stimuli - Keep track of many bits of information
- Types of Attention simultaneously and to cause recall of this
1. Selective Attention
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
information instantaneously as it is needed Clasp-Knife Response
for subsequent thoughts
- Sudden inhibition or letting go of the limb
AMNESIA (relaxation) in response to a stretch stimulus.
- Partial or total, permanent or transient loss of Clonus
memory
- Characterized by cylical, spasmodic
Types of Amnesia alternation of muscular contraction and
relaxation in respone to sustained stretch of
1. Anterograde Amnesia
a spastic muscle
- AKA: Post-traumatic Amnesia
- Refers to the inability to learn new material RIGIDITY
acquired after a brain insult.
- Hypertonic state characterized by constant
2. Retrograde Amnesia
resistance throughout ROM that is non-
- Inability to remember previous learning
velocity dependent.
acquired before the occurrence of a brain
- Associated with lesion of basal ganglia
insult.
system
HIGHER COGNITIVE FUNCTION a. Lead-Pipe Rigidity
- Constant resistance
✓ Information and Vocabulary
b. Cogwheel Rigidity
✓ Calculating Ability
- Hypertonic State with superimposed
✓ Abstract Thinking
ratchet-like jerkiness and commonly seen in
✓ Constructional Ability
UE.
✓ Communication
OPHIOSTHOTONUS
Elements of Motor Function
- Characterized by strong and sustained
1. Tone
contraction of the extensor muscle of neck
- Resistance of a muscle to passive
and trunk.
elongation or stretch.
DECORTICATE RIGIDITY
Postural Tone
- Sustained contraction and posturing of
- Pattern of muscular tension that exists
a. UE: FLEXION
throughout the body and affects group of
b. LE: EXTENSION
muscle.
DECEREBRATE/Abnormal Extensor Response
Tonal Abnormalities
- Sustained contraction and posturing of trunk
1. HYPERTONIA
and limbs in a position of full extension
- Increase Muscle Tone
- Antagonist HYPOTONIA/FLACCIDITY
2. HYPOTONIA
- Decrease or (-) Tone
- Decrease Muscle Tone
- Decrease or (-) Reflex
- Antagonist and Agonist
- Paresis
3. DYSTONIA
- Muscle Fasiculation and Fibrilation
- Impaired or disordered tonicity
- Neurogenic Atrophy
HYPERTONIA - Lower Motor Neuron Lesion
Spasticity DYSTONIA
- Motor disorder characterized by a velocity- - Prolonged involuntary movement disorder
dependent increase in muscle tone with characterized by twisting or writhing
increase resistance to stretch. repetitive movements and increased
- Upper Motor Neuron Lesion muscular tone.
- Increase Speed = Increase Tone
DYSTONIC POSTURING
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- Refers to sustained abnormal postures 3 Considerable increase in muscle tone,
caused by contraction of muscles that may passive movement difficult
last for several minutes, for hours or 4 Affected part(s) rigid in flexion or
permanently extension
- LESION: BASAL GANGLIA (NUCLEI) Deep Tendon Reflexes
FOCAL DYSTONIA 1. Jaw Reflex (CN V)
- Stimulus: Patient is sitting, with jaw relaxed
- Affect only one part of the body. and slightly open. Place finger on top of
- Seen in spasmodic torticollis, wry neck or chin; tap downward on top of finger in a
writer’s cramp direction that causes the jaw to open
- Response: Jaw rebounds and closes
SEGMENTAL DYSTONIA
2. Biceps (C5, C6)
- Affects 2 or more adjacent areas - Stimulus: Patient is sitting with arm flexed
and supported. Place thumb over the
EXAMINATION OF TONE
biceps tendon in the cubital fossa,
1. Initial Observation of Resting Posture and stretching it slightly. Tap thumb or directly on
Palpation tendon.
2. Passive Motion Testing - Response: Slight contraction of elbow flexors
3. Active Motion Testing 3. Brachioradialis (C5, C6)
4. Special Tests: Pendulum Test - Stimulus: Patient is sitting with arm flexed
onto the abdomen. Place finger on the
EXAMINATION OF TONE radial tuberosity and tap finger with
hammer
0 No response (flaccid)
- Response: Slight contraction of elbow flexors
1+ Decreased Response (Hypotonia)
4. Pronator Teres (C6, C7)
2+ Normal Response
3+ Exaggerated Response - Stimulus: With the elbow in semiflexion and
4+ Sustained Response the forearm semi-pronated, tapping over
Typical Patterns of Spasticity either the volar surface of the distal radius or
the dorsal aspect of the styloid process of
Upper Extremity Lower Extremity ulna
Scapula retracted and Pelvis Retracted - Response: Slight contraction of elbow
downwardly retracted Hip adducted, IR and flexion and forearm pronation
Shoulder adducted, IR, extended 5. Finger Flexors (C6-T1)
depressed Knees extended - Stimulus: Hold hand in neutral position.
Elbow Flexed Ankle plantarflexed,
Place finger across palmar
Forearm Pronated inverted, toes flexed
surface of distal phalanges of four fingers
Wrist Flexed and Ulnarly Equinovarus Deformity
Deviated and tap
Finger Flexed, thumb 6. Hamstrings
adducted a. Medial Hamstrings (L5, S1)
Modified Ashworth Scale - Stimulus: Semimembranosus Tendon
- Response: Knee flexion
Grade Description b. Lateral Hamstrings (S1, S2)
0 No increased in muscle tone - Stimulus: Biceps femoris tendon
1 Slight increase in muscle tone, - Response: Knee flexion
manifested by a catch and release or 7. Patellar/Knee Jerk (L2, L3, L4)
by minimal resistance at the end of the
- Stimulus: Patient is sitting with knee flexed,
ROM when the affected part(s) is
foot unsupported. Tap tendon of
moved in flexion or extension
quadriceps muscle between the patella
1+ Slight increase in muscle tone,
manifested by a catch, followed by and tibial tuberosity.
minimal resistance throughout the - Response: Slight contraction of knee
remainder (less than half of the ROM) extensors
2 More marked increase in muscle tone 8. Achilles/Ankle Jerk (S1, S2)
through most of the ROM, but the - Stimulus: Patient is prone with foot over the
affected part(s) easily moved. end of the plinth or sitting with knee flexed
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
and foot held in slight dorsiflexion. Tap Pathological Reflexes
tendon just above its insertion on the
1. Gordon’s
calcaneus. Maintaining slight tension on the
- Stimulus: Squeezing of calf muscles firmly
gastrocnemius-soleus group
improves the response. - Response: Extension of big toe and fanning
- Response: Slight contraction of of four small toes
plantarflexors 2. Schaeffer
- Stimulus: Pinching of Achilles tendon in
Deep Tendon Reflex Grading middle third
- Response: Flexion of foot & toes
Grade Description
3. Chaddock’s
0 Absent (areflexia)
- Stimulus: Stroking of the lateral side of the
1 Diminished (Hyporeflexia)
foot beneath lateral malleolus
2 Average (Normal
- Response: Extension of big toe and fanning
3 Exaggerated (brisk)
of four small toes
4 Clonus, very brisk (Hypereflexia)
4. Oppenheim’s
Superficial Reflexes
- Stimulus: Stroking of anteromedial tibial
Plantar (S1, S2) surface
- Response: Extension of big toe and fanning
- Stimulus: With blunt object (key or wooden
of four small toes
end of applicator stick), stroke the lateral
5. Hoffman’s
aspect of the sole, moving from the heel to
- Stimulus: Flicking” of terminal phalanx of
the ball of the foot, curving medially across
index, middle, or ring finger
the ball of the foot.
- Response: Reflex flexion of distal phalanx of
Abdominal thumb and of distal phalanx of index or
middle finger (whichever one was not
a. Upper Abdominal/Above (T8-T10) “flicked”)
- Stimulus: Position patient in supine, relaxed. 6. Souques Phenomenon
Make brisk, light stroke over each quadrant - Stimulus: Passive elevation of the Upper limb
of the abdominals from the periphery to the to 90 degrees of shoulder flexion
umbilicus - Response: Contraction of finger extension
- Response: Umbilicus moves up and toward 7. Raimiste’s Phenomenon
area being stroked - Stimulus: Resist of abduction on one side
b. Lower Abdominal/Below (T10-T12) - Response: Abduction of contralateral
- Stimulus: Position patient in supine, relaxed. extremity
Make brisk, light stroke over each quadrant 8. Marie-Foix Reflex
of the abdominals from the periphery to the - Stimulus: Sudden passive flexion of toes
umbilicus - Response: Flexion of LE (hip and knee
- Response: Umbilicus moves down and flexion, ankle dorsiflexion and toe flexion)
toward area being stroked 9. Bechterev-Mendel Reflex
- Stimulus: Percussion of the middle sole or
Gluteal Reflex (L4-L5, S1-S3)
heel
- Stimulus: Tapping the lower portion of the - Response: Flexion of toes
sacrum or the posterior aspect of the ilium 10. Rossolimo’s Sign
near the origin of the gluteus - Stimulus: Tapping of the plantar surface of
maximus muscle toes
- Response: Skin tenses in gluteal area - Response: Flexion of toes
11. Piotrowski
Cremasteric Reflex (T12, L1-L2) - Stimulus: Percussion of tibialis anterior
- Stimulus: Stroking or lightly scratching or - Response: Dorsiflexion and supination of foot
pinching the skin on the upper, inner aspect 12. Stransky
of the thigh - Stimulus: Small toe forcibly abducted then
- Response: Scrotum elevates released
- Response: Dorsiflexion of the great toe
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
13. Bing’s Sign CN Lateral Horn Cell in
- Stimulus: Pricking of dorsum of the foot with 11 Cervical Spinal Cord
CN Hypoglossal nucleus
a pin 12
- Response: Great toe extension
CRANIAL NERVE TESTING NUCLEUS AMBIGUUS
TRIGEMINAL NERVE - Connects CN 9 and CN 10
a. MAXILLARY DIVISION OLFACTORY NERVE
- Pure Sensory
b. MANDIBULAR DIVISION - Transmit olfactory impulses to the olfactory
- Mixed epithelium of the nose to the brain
c. OPTHALMIC DIVISION - Most Common Contused Nerve
- Pure Sensory - Not a real nerve (outgrowth of the telencephalon)
- Function: For smelling
EXIT - Test: Non-noxious odors
1. ANTERIOR CRANIAL FOSSA - Clinical Implications:
- CN 1: Perforation in Cribriform Plate Ethmoid 1. Rhinorrhea
Bone - Excretion of white fluid due to head trauma
2. MIDDLE CRANIAL FOSSA - Paano malalaman kung sipon or CSF ang lumabas?
- CN 2: Optic Canal a. *CSF: sweet due to glucose
- CN 3,4,5,6: Superior Orbital Fissure b. Sipon: Salty and and Wet
- CN 5 (MAXILLARY): Foramen Rotundum 2. ANOSMIA
- CN 5 (MANDIBULAR): Foramen Ovale - Inability to smell
3. POSTERIOR CRANIAL FOSSA - Bilateral (Both Nostrils)
- CN 7,8: Internal Acoustic Meatus a. Increase Mucous in nasal septum
a. COCHLEAR: Anterior b. Coryza: Sipon
b. VESTIBULAR: Posterior c. Pertussis: Whooping Cough (if child 100 days
- CN 9,10, 11: Jugular Foramen of coughing)
- CN 11: Foramen Magnum - Unilateral
- CN 12: Hypoglossal Canal
OPTIC NERVE
ORIGIN
- Optic Pathway transmits visual impulse of retina
- CN 1: Telencephalon to the brain
- CN 2: Diencephalon - Not a real nerve (Outgrowth of the Diencephalon)
- CN 3-4: Midbrain a. Macula: Highest Resolution
- CN 5-8: Pons b. Retina: Rods (Non-color) and Cones (Color)
- CN 9-12: Medulla Oblongata - Function: Vision
CN NUCLEUS CONTROL FUNCTION - Test:
CN Edinger-Westphal Ciliary Muscle Pupil a. VISUAL ACUITY: Snellen Chart
3 Oculomotor Nucleus Constriction b. CONFRONTATION TEST: Patient will cover his
CN Trochlear Nucleus eyes then PT put object towards the midline and
4
then patient will identify object.
CN Trigeminal Nucleus
5
CN Abducens Nucleus
6
CN Superior Salivatory Submandibular & Production
7 Nucleus Sublingual Gland of Saliva
Lacrimal Nucleus
Facial Nucleus Lacrimal Gland
Tearing
CN Inferior salivatory Parotid Gland
9 Nucleus
Glossopharyngeal
Nucleus
CN Dorsal motor Abdominal
10 nucleus of CN 10 Viscera
Vagus Nucleus
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
CLINICAL IMPLICATIONS b. Sectoral: Part of Iris (1 iris)
c. Central: Spikes radiating from pupils (1 iris)
1. MONOCULAR BLINDNESS
- Ipsilateral Optic Nerve VESTIBULOCOCHLEAR NERVE
- Left Monocular Blindness
- AKA: Statoacoustic Nerve
- Right Monocular Blindness
- Function:
a. Hearing (Cochlea)
b. Balance (Vestibule)
- VESTIBULAR ASPECT
2. BITEMPORAL HEMIANOPSIA I. UTRICLE AND SACCULE
- Optic Chiasma - Detects linear head movement
a. Bitemporal - MNEMONIC: “HUVS”
b. Binasal - HU= Horizontal Utricle
- VS= Vertical Saccule
II. SEMICIRCULAR CANAL
- Detects rotatory head movement
- 3 pairs = 6
3. HOMONYMOUS HEMIANOPSIA a. SUPERIOR/ANTERIOR: HEAD FLEXION
- AKA: Contralatera Homo Hemi b. INFERIOR/POSTERIOR: HEAD EXTENSION
- Optic Tract c. HORIZONTAL/LATERAL: HEAD ROTATION
- Optic Radiation
TEST:
- Bicipital Lobe
- Naming: Right Homonymous Hemianosia 1. DIX-HALLPIKE TEST
- Benign Paroxysmal Positional Vertigo
- The test is performed by having the patient
long-sit on a plinth with the head rotated
approximately 30° to 45°. The examiner
4. QUADRANT ANOPSIA stands behind the patient with one hand
- Calcarine Sulcus supporting the head/ neck and the other
a. Superior/Coneal/Parietal Fibers of Optic hand supporting the trunk. The patient is
Radiation then assisted into a supine position with the
b. Inferior/Lingual/Temporal Fibers of Optic patient’s head slightly below the horizontal
Radiation plane, and the position is maintained for 30
- Naming: Contralateral to 60 seconds
- Damaged: - (+) Dizziness and Nystagmus
a. Superior: Inferior Quadrant Anopsia 2. TEMPERATURE (CALORIC) TEST
- For Inner Ear Problem
Inferior: Superior Quadrant Anopsia
- The examiner alternately applies hot and
EXAMPLE cold test tubes several times just behind the
patient’s ears on the side of the head; each
- Right Cuneal is damaged: Left Inferior side is done in turn
Quadrant Anopsia - (+) Inducement of Vertigo
- Left Temporal Fibers is damaged: Right - MNEMONIC: “COWS”
Superior Quadrant Anopsia. a. COLD = Left Nystagmus
5. ANISOCORIA b. HOT = Right Nystagmus
- Unequal size of pupils - AUDITORY ASPECT
6. DYSCORIA a. OUTER EAR
- Different shape of pupils - External Surroundings → Collect Sound
7. CORRECTOPIA Waves → External Auditory Meatus →
- Different position of Pupils Eardrum
8. HETEROCHROMIA b. MIDDLE EAR
- Iridum or Iridis - Ossicles
- Different color of Iris - Malleus, Incus, Stapes
a. Complete: Full (2 iris) - Vibrate to Inner Ear
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
c. INNER EAR - The examiner alternately places the
- Interpret Soundwaves to Electrical Impulse. vibrating tuning fork against the patient’s
- Soundwaves travel in 2 ways mastoid process and against the examiner’s
1. Air Conduction mastoid bone until one of them no longer
- Outer and Middle Ear hears a sound.
2. Bone Conduction - The examiner and patient should hear the
- Inner Ear (By passes outer & Middle Ear) sound for equal amounts of time.
3. WEBER TEST
CLINICAL IMPLICATION
- The examiner places the base of a vibrating
1. HEARING LOSS tuning fork on the midline vertex of the
a. CONDUCTIVE patient’s head.
- Reduction of all sounds - The patient should hear the sound equally
b. SENSORINEURAL well in both ears If the patient hears better in
- Inner Ear one ear (i.e., the sound is lateralized), the
- Different Interpreting of Sounds. patient is asked to identify which ear hears
c. CORTICAL the sound better.
- Brain - To test the reliability of the patient’s
2. MÉNIÈRE’S DISEASE response, the examiner repeats the
- Inner Ear procedure while occluding one ear with a
- Fullness of Ear & Tinnitus (Vibrate pero si finger and asks the patient which ear hears
patient lang nakakarinig ng sounds) the sound better.
3. PRESBYACUSIS - It should be heard better in the occluded
- Deafness due to old age. ear
4. BING TEST
TEST - Vibrating tuning fork is applied to the
1. RINNE’S TEST mastoid bone and then the external
- The Rinne test is performed by placing the auditory canal is occluded by pressing on
base of the vibrating tuning fork against the the tragus.
patient’s mastoid bone. - If hearing is Louder, test is (+) seen in normal
- The examiner counts or times the interval person ore one with SNHL
with a watch. - If hearing remains same or less, test is (-)
- The patient tells the examiner when he or indicating CHL
she no longer hears the sound, and the - This test is useful in mixed hearing loss where
examiner notes the number of seconds. conducting impairment is minimal and
- The examiner then quickly positions a still- tympanic membrane is intact as in
vibrating tine 1 to 2 cm (0.5 to 0.8 inch) from osteosclerosis.
the auditory canal and asks patient to 5. TICKLING WATCH TEST
indicate when he or she no longer hears the - The ticking watch test uses a nonelectric
sound. ticking watch to test high-frequency
- The examiner then compares the number of hearing.
seconds the sound was heard by bone - The examiner positions the watch
conduction and by air conduction. The approximately 15 cm (6 inches) from the ear
counting or timing of the interval between to be tested, slowly moving it toward the
the two sounds determines the length of ear.
time that sound is heard by air conduction - The patient then indicates when he or she
- Air-conducted sound should be heard twice hears the ticking sound. The distance can
as long as bone-conducted sound. For be measured and will give some idea of the
example, if bone conduction is heard for 15 patient’s ability to hear high-frequency
seconds, the air conduction should be sound.
heard for 30 seconds 6. WHISPHERED VOICE TEST
2. SCHWABACH TEST - The patient’s response to the
- This test compares the patient’s and examiner’s whispered voice can be
examiner’s hearing by bone conduction. used to determine hearing ability.
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- The examiner masks the hearing in one 80% = Parasymphathetic (CN 3)
of the patient’s ears by placing a finger
20%= Symphatetic (Muelier mm = LPS)
gently in the
patient’s ear canal. C. WEAK SUPERIOR OBLIQUE MUSCLE
- Standing approximately 30 to 60 cm (12 - Eyes are downward and Inward
to 24 inches) away from the patient, the D. DIPLOPIA
examiner whispers one- or two-syllable 1. Vertical = Cranial Nerve 4
words and asks the patient to repeat 2. Horizontal = Cranial Nerve 6
them. E. STRABISMUS
- If the patient has difficulty, the examiner - Banlag
gradually increases his or her volume 1. ESOTROPIA
until the patient responds appropriately. - CN 6
- The procedure is repeated in the other - Internal Strabismus
ear. 2. EXOTROPIA
- The patient should be able to hear - CN 3
whispered words in each ear at a - External Strabismus
distance of 30 to 60 cm F. WEAK LATERAL RECTUS
(12 to 24 inches) and respond correctly - Eyes on the middle
at least 50% of the time
ACCESSORY NERVE
PURE MOTOR CRANIAL NERVE
- 2 Parts
OCULOMOTOR NERVE - Cranial & Spinal Nerve Roots (CN 2,3,4)
- SCM & Upper Trapezius
- Tested together with CN 4 and 6
- Function: Shoulder Elevation
a. SUPERIOR DIVISION: Lateral Palpebrae
- Test: Resist the action of the muscle.
Superioris & Superior Rectus
b. INFERIOR DIVISION: Medial Rectus, Inferior HYPOGLOSSAL NERVE
Rectus and Inferior Oblique.
- Tongue muscle and movement
TROCHLEAR NERVE - 4 Muscles
a. Genioglossus: Forward
- Smallest Cranial Nerve in the body
b. Hyoglossus: Downward
- Longest and Most Slender intracranial
c. Styloglossus: Curves
nerve.
d. Palatoglossus: Upward
- SO4LR6
- Function: Movement of the eyeball CLINICAL INDICATION
ABDUCENS NERVE - Ipsilateral
1. LOWER MOTOR NEURON LESION DAMAGE (L)
- Lateral Rectus
CN 12
- Function: Movement of the eyeball
- Tongue will deviate toward left side
Clinical Indication - Uvula: Contralateral Cranial Nerve 9
2. UPPER MOTOR NEURON LESION ® CVA
A. CN 3 Incomplete Lesion
- Contralateral
1. INTERNAL OPTHALMOPLEGIA
- (-) Pupil Constriction Cranial Nerve Testing (Lab)
- (+) Extraocular Muscle 1. CN 1 – OLFACTORY
2. EXTERNAL OPTHALMOPLEGIA ➢ SENSORY
- (-) Extraocular Muscle (weak) ✓ Testing Procedure: Non-noxious stimuli on a
- (+) Pupil Constriction cotton ball
B. CN 3 COMPLETE LESION ✓ Condition: Anosmia
- Extraocular Muscle Weakness 2. CN 2 – OPTIC
- External Strabismus ➢ SENSORY
- (-) Pupil Constriction ✓ Testing Procedure:
- (+) Ptosis (80% only) a. Visual Aquity: Snellen Chart (20ft distance)
- *FULL OPENING OF THE EYE
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
b. Peripheral Vision: Confrontation Test - Tuning fork on vertex
✓ Condition: Blindness, Myopia (impaired far - (N) Same intensity on each side
vision), Presbyopia (impaired near vision) - If one side heard it better, occlude the
3. CN 3/4/6 – ear: should be heard well on occluded
OCULOMOTOR/TROCHLEAR/ADDUCENS ear.
➢ MOTOR CHL: sound is hear on poor ear
→ ANATOMICAL SNHL: sound is heard on good ear
2) Rinne Test
- Tuning fork at mastoid process until
vibration is not heard » position in EAM
- (N) air > bone = 2:1
CHL: bone ≥ air
→ TESTING SNHL: air >bone but > 2:1 ratio
7. CN 9 – GLOSSOPHARYNGEAL
* MIXED
➢ SENSORY
✓ Testing Procedure: Salty or Sour on cotton
> III: Eye can’t look upward, downward and swab
inward ➢ MOTOR
> IV: Eye can’t look down when eye is adducted ✓ Testing Procedure: Say “AH” check for
> VI: Eye can’t look out deviation in uvula
✓ Condition: Internal Stabismus/External 8. CN 10 – VAGUS
Strabismus * MIXED
4. CN 5 – TRIGEMINAL ➢ SENSORY
* MIXED ✓ Testing Procedure: Swallowing/Phonation
➢ SENSORY ➢ MOTOR
✓ Testing Procedure: Light touch cotton on ✓ Testing Procedure: Gag Reflex
forehead, maxilla and mandible 9. CN 11 – SPINAL ACCESSORY
➢ MOTOR ➢ MOTOR
✓ Testing Procedure: Clench teeth and hold ✓ Testing Procedure
against resistance SCM: I\L lateral flexion, C/L rotation
5. CN 7 – FACIAL Upper Trapezius: Shoulder shrug
* MIXED 10. CN 12 – HYPOGLOSSAL
➢ SENSORY ➢ MOTOR
✓ Testing Procedure: Saline or Sugar on cotton ✓ Testing Procedure: Tongue movements
swab SUPERFICIAL CUTANEOUS REFLEX
➢ MOTOR REFLEX CN SITE OF RESPONSE
✓ Testing Procedure: Facial Expression STIMULUS
6. CN 8 – VESTIBULOCOCHLEAR
Corneal V Cornea Blink
➢ SENSORY
✓ Testing Procedure: VII
a. Vestibular Aspect Pharyngeal IX Tonsils (+) Gag
1) Dix Hallpike Test X
- Long sitting, head rotation of 30 – 45 deg.
on unaffected side, supine, head slightly Major Visceral Reflex
below horizontal plane maintaining REFLEX STIMULUS RESPONSE
rotation. (30 – 60 secs) Direct Light Direct on Pupillary
- (+) Nystagmus, Vertigo eye Constriction
2) Caloric Test
Accommodation Object Constrict: near;
- Water irrigation on External Auditory
near/far Dilate: far
Canal
- Warm water: Same side Nystagmus Consensual Pupilloconstriction
- Cold water: Opposite side Nystagmus on (B) eyes
- “COWS” Ciliospinal/Pupillary Noxious Dilation
> Abnormal Response: Unequal duration Skin stimulus
of Nystagmus on face
b. Cochlear Aspect Oculocardiac/ Compress PR
1) Weber Test Ashner Dagnini Eye ball
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
Carotid Stretch on PR CLASSIFICATION AND NOMENCLATURE
Sinus/Baroreceptor vessel
1. FLUENT APHASIA
wall
- Characterized by impaired auditory
CONSENSUAL REFLEX
comprehension and fluent speech that is of
normal rate and melody.
- Usually associated with a lesion in the vicinity
of the posterior portion of the first temporal
gyrus of the left hemisphere.
- When condition is severe, word and sound
substitutions may be of such magnitude and
frequency that speech may be rendered
meaningless
- Greatest difficulty in retrieving those words
that are substantive (nouns and verbs)
- Tend to have some degree of impaired
NEUROGENIC DISORDERS OF SPEECH & LANGUAGE awareness and are rarely physically
Normal Process disabled.
- Most Common Type of Fluent Aphasia is
1. Cerebration Wernicke’s Aphasia / Sensory Aphasia /
- Thought communication Receptive Aphasia.
2. Respiration a. WERNICKE’S APHASIA
- Mechanical & Chemical - Usually the result of a lesion in the posterior
3. Phonation portion of the first temporal gyrus of the left
- Vocal cords, subglottic pressure (rel. hemisphere.
intensity), length and tension of vocal cords - Characterized by impaired auditory
(rel. pitch) comprehension and fluently articulated
4. Resonation speech marked by word substitutions
- Modified & amplified by cavities - Impaired reading and writing
(pharyngeal, oral & nasal) - May produce what seem like complete
5. Articulation utterances and use complex verb tenses,
- Production of phonemes they often add a word or phrase and
- Manner of Articulation “augment” speech production.
a. Plosive: (stop sounds: pbtkg) - Speech is often produced at a rate greater
b. Fricative: (turbulent, closed nasal cavity – than normal.
fvthsvshzhh) - (+) reverse phonemes and/or syllables
c. Nasal: (open nasal cavity, closed oral: (hopspipal/trevilision) and may produce
mnng) neologisms (nonsense words).
d. Liquid: (soft palate raised: r,l)
e. Semi-vowel: (w,y) ANOMIC APHASIA
f. Unvoiced (p,s)
- Characterized by a significant word-finding
g. Voiced: (all vowels & some consonants)
difficulty in the context of fluent,
h. Substantive: (nouns & verbs)
grammatically well-formed speech
i. Less substantive: (Prepositions, conjunctions,
- (-) Auditory Comprehension
pronouns)
- May be proficient in producing
- Place of articulation
circumlocutions to skirt the lack of specificity
a. Labial: (pbwm)
of language use.
b. Labiodental: (fv)
2. NON-FLUENT APHASIA
c. Dental: (th)
- Characterized by limited vocabulary, slow,
d. Alveolar: (tdszylrn)
hesitant speech, some awkward
e. Palatal: (shzh)
articulation, and restricted use of grammar
f. Velar: (kgng)
in the presence of relatively preserved
g. Glottal: (h)
auditory comprehension
6. Intelligibility
- How a person “sounds” when speaking
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- Associated with anterior lesions usually - It can exist in the absence or relative
involving the third frontal convolution of the absence of generalized intellectual and
left hemisphere behavioral disturbances or cognitive
- Patient tend to express themselves in impairment generally associated with
vocabulary that is substantive (nouns, verbs) dementia.
and lack the ability to retrieve less
substantive parts of speech (prepositions,
conjunctions, pronouns).
- They tend to have good awareness of their
deficit and usually have impaired motor
function on the right side (right hemiplegia–
paresis)
a. BROCA’S APHASIA/MOTOR APHASIA/
EXPRESSIVE APHASIA / VERBAL APHASIA
- It is the result of a lesion involving the third
frontal convolution of the left hemisphere,
the subcortical white matter, and extending
posteriorly to the inferior portion of the motor
strip (precentral gyrus)
- Characterized by awkward articulation,
restricted vocabulary, and restriction to
simple grammatical forms in the presence of
a relative preservation of auditory DYSARTHRIA / MOTOR SPEECH DISORDER
comprehension.
- Writing skills generally mirror the pattern of - Refers to an impairment of speech
speech and reading may be less impaired production
than speech and writing resulting from damage to the central or
- may be limited to one- and two-word peripheral nervous system, which causes
productions for weakness, paralysis, or incoordination of the
- Expression and find it impossible to combine motor–speech system.
words into sentences. - Any one or all of the components of the
- Articulation may be awkward and effortful motor–speech system (respiration,
3. GLOBAL APHASIA phonation, articulation, resonance, and
- A severe aphasia with marked dysfunction prosody) may be compromised by neural
across all language modalities and with damage.
severely limited residual use - Generally reflected in deficits occurring
of all communication modes for oral–aural in multiple motor–speech systems, but may
interactions sometimes
- Not a type of aphasia but rather a
ANARTHRIA
designation of severity.
- Generally has extensive damage, which - When patients are totally unintelligible as
may be anywhere in the left hemisphere, the result of severe motor–speech system
and is sometimes bilateral. impairment
4. ACQUIRED APHASIA
- Result of cerebral damage caused by head 5 PRIMARY TYPES OF DYSARTHRIA
injury, tumor, or stroke results in the 1. SPASTIC DYSARTHRIA
same syndromes manifest in adults with - Characterized by imprecise articulation,
aphasia. slow labored articulation, hypernasality,
5. PRIMARY PROGRESSIVE APHASIA harsh to strained phonation, and
- Slowly progressive isolated aphasia not due monotonous pitch.
to stroke, trauma, tumor, or infection, which - Result of bilateral pyramidal system damage
does not fit neatly into existing aphasia involving the corticobulbar tracts (upper
classification schemes motor neurons)
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- May cause weakness and paresis of the production errors as utterance length
face increases.
and tongue musculature on the side - Individuals with AOS do not generally have
opposite to the lesion. deficits in performing non-speech
2. FLACCID DYSARTHRIA movements
- Characterized by slow/labored articulation, of the oral musculature.
hypernasality, and hoarse, breathy
DYSPHAGIA
phonation.
- Phrases may be short, inhalation is shallow, - Defined as a condition in which an
and the control of exhalation may be individual has had an interruption in either
reduced eating function or the maintenance of
- A reduction in the variation of pitch and nutrition and hydration
loudness with audible inspirations
- Most of these deviant speech Cardiovascular Rehabilitation
characteristics are related to muscular
General Information
weakness and reduced muscle tone, which
affects speech accuracy. a. Age
3. ATAXIC DYSARTHRIA b. Race
- Characterized by disturbances of timing, - African-American
movement, range, control, and c. Gender
coordination - Male
of the muscles of speech and respiration. d. Body Mass
- Speech is imprecise, slow, and irregular - Obese
- There may be intermittent periods of
explosive inflection, syllable stress, and 3 Major Risk Factors according to Cunningham
loudness patterns. Study
- Phonemes may be prolonged; pitch and - Smoking
loudness are monotonous - Hyperlipidemia
- Lesions producing ataxic dysarthria are - Hypertension
bilateral, generalized lesions involving the 1. Past Medical History
deep midline nuclei and pathways of the - Pulmonary Disorder
cerebellum - Neuromuscular Disorder
4. HYPOKINETIC DYSARTHRIA - Past oncologic disorder treated with
- Characterized by variable articulatory radiation therapy
precision, slow rate of speech, harsh, hoarse - Obesity
voice quality, excessive and overly long - Pre-mature birth
pauses, prolonged syllables, and reduced - Auto-immune Dysfunction
phonation - Vascular Dysfunction
- Caused by lesions of the substantia nigra. - Endocrine or Metabolic Disorder
5. HYPERKINETIC DYSARTHRIA 2. Family History
- Characterized by variable articulatory - DM
precision, vocal harshness, prolonged - Hypertension
sounds and intervals between words, 3. Personal, Social Environmental History
monotonous pitch, and loudness a. Smoking
- Caused by lesions of the basal ganglia b. Occupational exposure to irritants or
and/or their extrapyramidal projections. allergens (e.g. carbon monoxide,
APRAXIA OF SPEECH / DYSPRAXIA / VERBAL chemicals)
APRAXIA / CORTICAL DYSARTHRIA / PHONETIC c. Residing in locations with higher
DISENTEGRATION levels of air pollution
d. Sedentary Lifestyle
- Difficulty initiating speech, articulatory e. Personality Type
struggling, periods of error-free speech - Type A: Time urgency with stress
production, and a greater number of sound - Type D: Suppression of emotions
f. Diet
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- Low mineral intake
- Low anti-oxidant intake
- Low essentially fatty acid intake
Blood Test (Cardiac Enzymes)
Laboratory Test
1. Blood Test (Cardiac Enzymes)
2. Electrolytes
3. CBC
4. Liver & Kidney Tests
5. Lipid and Like Values
- LDL (Low-density lipoprotein)
- HDL (High-density lipoprotein)
- ICL
- Triglycerides
Anginal Scale
Grade Description
0 No angina
1 Light, barely noticeable
2 Moderate, bothersome
3 Severe, very uncomfortable: pre-
infarction pain
4 Most pain ever experienced; infarction
Patient Complaint pain
- Most common Signs & symptoms
a. Angina
- Often described as heart pain
- “If an elephant is sitting upon my chest”
- “If someone is squeezing my chest
- Substernal burning/pain
- Chest pressure
- Chest tightness
- Classical representation for substernal pain is
accompanied by Levine Sign
- Due to: Myocardial Ischemia
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
Dyspnea
b. Pulsus Alterans
- Marked by a fluctuation in amplitude
between beats (a weak and a strong), with
minimal change in overall rhythm
Grading Pulse Quality
Dyspnea Scale
Grade Description
0 No dyspnea
1 Mild, noticeable
2 Mild, some difficulty
3 Moderate difficulty but can continue
4 Severe difficulty, cannot continue
Vital Signs: Blood Pressure
Stages SBP DBP
Pre-HTN 120-130 mmHg 80-89 mmHg
Stage 1 130-140 mmHg 90-100 mmHg
HTN
Stage 2 140-160 mmHg 100-110 mmHg
HTN
Stage 3 >160 mmHg >110 mmHg Vital Signs: Respiratory Rate
HTN
- Normal: 12-20 cpm
Korotkoff Sounds
- Appearance: Skin color and body traits
Phase Description - Sign of Poor Cardiovascular Function
I First clear, faint, repetitive, clear tapping a. Pale and Cyanotic Skin
sound which gradually increase in b. (+) Diagonal Ear Lobe Crease
intensity for at least 2 consecutive beats c. Cyanosis: When O2 saturation is <85%
II Murmur or Swishing sound d. Diaporesis: Excessive sweating
III Sharper sounds, which become crisper to e. Presence of Edema in the extremity
regain
IV Abrupt muffling of sounds, become soft (L) Ventricular Failure ® Ventricular Failure
and blowing in quality Dyspnea Increased fatigue
V Last sound heard Paroxysmal Nocturnal Dependent Edema
Pulse Dyspnea (usually begins in ankle)
Orthopnea Pitting Edema (After 5-
- Normal Values: 60-100 bpm Cough 10 lbs of edema
- Preferred Site: Radial Pulse Pulmonary Edema accumulates
- Most accurate site: Apical pulse Cerebral Hypoxia Edema in sacral area
- Rate: Bradycardia/Tachycardia Fatigue and Muscular or the back of thighs
- Quality Cramping or weakness Right upper quadrant
Nocturia pain
a. Paradoxical Pulse
Cyanosis of bed nails
- AKA: Pulsus Paradoxus
- Body Habitus or Somatotype: Can also
- Decrease amplitude of the pressure wave
provide information about cardiovascular
detected during quiet inspiration with a
risk
return to full amplitude on expiration
- Pear-shaped Body: 3 times more likely to
- Commonly seen in patient with COPD
develop cardiovascular disease
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
Anthropometric Measurement - Simply the filling of the jugular vein(s) with
excessive fluid such that they become
1. Body Weight
visibly distended
- Due to: ® sided heart failure
- Procedure:
✓ Patient placed semi-supine at 45°
✓ Rotate the head slightly to the
opposite side
✓ Pressed the external jugular vein
above and parallel to the clavicle
approximately 10-20 seconds
✓ Measure the highest visible pulsation
✓ (N) Level: Less than 3-5cm
Ideal Body weight should be made in reference to Using Stethoscope
body type
1. Diaphragm
- Small Body Frame: Calculated Ideal Body - For high-frequency sounds and should be
Wt. x 0.9 used with firm pressure
- Large Body Frame: Calculated Ideal Body 2. Bell
Wt. x 1.10 - Foe low-frequency sounds and should be
2. Finger Pressure used
- If firm: Change to diaphragm
- Alternating light and firm can differentiate
normal from abnormal heart
Normal & Abnormal Heart Sounds
3. Girth Measurement
- Appropriate Site: Mid-calf/Middle Forearm
4. Skin Fold Calipers
Exercise Tolerance Test (ETT)
- Purpose: To examine the ability of the
cardiovascular system to accommodate to
5. BMI increasing metabolic demand
2 Major Goals
Grading of BMI - Detect presence of ischemia
- Determine functional aerobic capacity
- Underweight: Below 18.5 ▪ The patient exercises through stages of
- Normal: 18.5-24.9 increasing workloads, expressed in units of
- Overweight: 25.0-29.0 oxygen
- Obese: >30 ▪ MET’s at rest= 3.5 mL/kg/min.
6. Jugular Vein Distention
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
Aerobic Capacity & Endurance TYPES OF COORDINATION
- 6MWT 1. INTRALIMB
- <300 m: Poor Long Term Endurance - Refers to the movement occurring within a
single limb
ABI
2. INTERLIMB
- Refers to the integrated performance of two
or more limbs working together.
3. VISUAL MOTOR
- Ability to integrate both visual and motor
abilities within the ENVIRONMENTAL context
to accomplish a goal.
- Example: Eye-hand or Eye-hand-head (to
fixate the eyes)
MOTOR SYSTEM
1. Motor Cortex
2. Descending Efferent Pathway
3. Cerebellum – Ipsilateral; balance
Formula: 4. Basal Ganglia
5. Dorsal-Column Medial Lemniscal Pathway
ABI = Highest Ankle SBP/ Highest Arm SBP
ASTHENIA
BP= COxTPR
- Generalized muscle weakness associated
PP= SBP-DBP
with cerebellar lesions.
CO=SVxHR - Example: Myasthenia Gravis
- Mm grade: 1 (hypotonia)
MAP= SBP+2DBP/3
DYSARTHRIA
RPP = HRxSBP
- One word at a time patients (scanning
EXAMINATION OF BALANCE AND COORDINATION speech)
COORDINATION DYSDIADOCHOKINESIA
- Ability to receive smooth, accurate and - Impaired ability to perform rapid alternating
coordinated movement movements
- Joint and muscle involvement: Multiple joint - (-) Rapid movement of forearm supination
& Muscles and pronation.
- Dependent on
a. Somatosensory DYSMETRIA
b. Visual
- Inability to judge the distance or range of a
c. Vestibular
movement
d. Intact Neuromuscular Function (brain to SC)
a. Hypometria
- Coordination impairments: Awkward,
- Underestimation of the required range
extraneous. Uneven and inaccurate
needed to reach an object or goal
2 TERMS ASSOCIATED IN COORDINATION AND b. Hypermetria
BALANCE - Overestimation of the required range
needed to reach an object or goal
a. Dexterity
- Refers to skillful use of the fingers during fine DYSSYNERGIA
motor task
- AKA: Movement Decomposition
b. Agility
- Sequential Movement pattern rather than a
- Refers to the ability to rapidly and smoothly
smooth activity
initiate, stop or modify movements while
maintaining posture. ASYNERGIA
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- Loss of the ability to associate muscles - Characterized by involuntary, rapid,
together for complex movements. irregular and jerky movements involving
multiple joints
GAIT ATAXIA
CHOREOATHETHOSIS
- AKA: Cerebellar Gait
- Involve ambulatory patterns that typically - Characteristics of both chorea and
demonstrate a broad BOS due to no athethosis
sensation of the floor
DYSTONIA
HYPOTONIA
- Sustained involuntary contractions of
- Decreased muscle tone agonist and antagonist muscles
- DTR is also decreased - Hard to manipulate
NYSTAGMUS HEMIBALLISMUS
- Rhythmic, oscillatory, back and forth - Large amplitude, sudden, violent, flailing
movements of the eyes motions of the arms and legs of one side of
- Side to side or up and down the body.
- Terminate SPT for head/neck
HYPERKINESIS
REBOUD PHENOMENON
- Increase muscle activity or movement
- Loss of check reflex or check factor, which
HYPOKINESIS
functions to halt forceful active movement
when resistance is removed - Decrease muscle activity or movement
- Isometric movement
RIGIDITY
TREMOR
- Increase muscle tone causing greater
- Involuntary oscillatory movement resulting resistance to passive movements
alternate contractions of opposing muscle a. Lead-Pipe Rigidity
groups - Uniform, constant resistance as limb is
a. Static Tremor / Postural Tremor moved.
- At rest; during movement no tremor b. Cog-wheel Rigidity
b. Kinetic Tremor/Intention Tremor - Series of brief relaxations or catches as limb
- Occurs during movement; at rest no tremor is possibly moved.
- Ratchet-like
HEAD TITUBATION
RESTING TREMOR
- Head oscillation (side to side or up or down)
- Involuntary, rhythmic, oscillatory movement
BASAL GANGLIA PATHOLOGY
observed at rest
AKINESIA
DC-ML PATHOLOGY
- Inability to initiate a movement
- Lack of position sense
ATHETHOSIS - Lack of awareness of movement
- Impaired localized touch sensation
- Slow, writhing, twisting and worm-like
- Wide BOS
movements
- Dysmetria
- Commonly seen in Pediatric Rehabilitation
SCREENING
BRADYKINESIA
- ROM-BASELINE; Decrease then Increase
- Decrease amplitude and velocity of
ROM of patient
voluntary movements.
- MMT
CHOREA - Sensation
COORDINATION TEST
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
2 CATEGORY TESTS
- Gross Motor Tests
- Fine Motor Test
2 SUBDIVISION
- 4 movement capabilities
- Alternate or reciprocal motion
- Movement composition
- Movement accuracy
- Fixation or limb holding
Progression of Coordinated Test
- Unilateral Task
- Bilateral Symmetrical Tasks
- Bilateral Asymmetrical Tasks
- Multi-time tasks
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
EXAMINATION OF POSTURAL CONTROL AND
BALANCE
POSTURAL CONTROL
POSTURAL ORIENTATION
- Control the body’s relative position
- Gravity
a. Reactive Postural Control
- External pertuberance
b. Proactive Postural Control
- Internal stability
c. Adaptive Postural Control
- Allows to modify sensory and motor systems.
BALANCE
1. Sensory & Perception
- Detect body position
2. Motor System
- Organization and execution of muscle
contraction + increase synergistic action
3. Higher CNS
- Integration and processing
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
POSTURAL ALIGNMENT AND WEIGHT DISTRIBUTION - E.g. lean (L) side move then mas stable di
raw nagsway masyado then that’s the zone
- Grinds/Grines
of stability.
- COM: 2 inches anterior to S2
d. Postural Sway
LATERAL - (N) minimal sway
e. Sway Envelope
✓ Lateral to External Auditory Meatus - Direction of sway
✓ Slightly Anterior to Shoulder Joint
✓ Midline Trunk SENSORIMOTOR INTEGRATION IN POSTURAL COTROL
✓ Posterior to hip joint
1. VISUAL PROPRIOCEPTION
✓ Anterior to knee joint
- Important source of information for the
✓ Anterior to ankle joint
ability to perceive movements and detect
QUIET STANCE the relative orientation of body segments
and orientation of the body in space.
- Tibialis Anterior, Gastroc-Soleus Complex:
Ankle and Hip POSTURAL CONTROL
- Iliopsoas, Tensor Fasciae Latae, Gluteus
- Visual
Medius: Level Pelvis
- Vestibular
- Abs and Errector Spinae: Trunk
- Sensorimotor
Knee is still extended because of Ligaments
Focal Vision (Cognitive/Explicit Vision)
- Localizing features of environment
MOTION ANALYSIS SYSTEM
Ambient Vision (Sensorimotor/Implicit Vision)
- Muscle Contraction
- Unconscious control of the environment
- Enclosed plate, deviations, weight bearing
Optic Ataxia
LIMITS OF STABILITY
- Problem with the ambient vision
- Maximum distance an individual is able to or
- Can’t control/see how far or near the
willing to lean in any direction without loss of
object is but can see, you just can’t grab it.
balance or changing BOS.
- Influenced by: Visual Agnosia
a. Anterior and Posterior
- Problem with the focal vision
- Patient’s Height and Foot Length (should be
- Can’t recognize the object
longer)
b. Medial and Lateral Somatosensory inputs
- Patient’s height, foot width distance (should
be wide apart) - Where we rely mostly; biggest role
c. Velocity - If it is damaged; visual system will take place
- Velocity and displacement - Include
a. Cutaneous & Pressure Sensation from
EXAMINATION & DOCUMENTATION body segments in contact with support
surface
a. Visual Inspection
b. Muscle and Joint Proprioception
- Plumb Lines/ Grid Lines
throughout the body
b. Posturography
c. Light touch contact from the hands on a
- Force plate (Ground reaction force, center
stable surface.
of pressure, center of force)
Vestibular System
Checked the following
- Important source of information for postural
a. Initial stance position and posture
control and balance.
b. Mean sway path
a. Semi-circular Canal
c. Zone of Stability
- Angular; fast head movements
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
b. Otoliths 6 CONDITIONS
- Linear, slow head movements
1-3 STABLE SURFACE
c. VOR (VESTBULO-OCULAR REFLEX)
- Gaze stabilization during head movements 1. Eyes open; baseline
d. VOS (VESTIBULO-SPINAL REFLEX) 2. Eyes closed
- Postural Tone, Muscle Activation in relation 3. Visual Conflict
to head position
4-6 MOVING SURFACE
TESTS
4. Eyes open
1. Romberg Test 5. Eyes closed
- Stand with feet together, eyes open 6. Visual Conflict
unaided for 20-30 seconds
- Stop if there is sway but continue if it does CONDITION 5 & 6 – VESTIBULAR
not occur.
- (-) Somatosensory input
- Eyes Closed
- If patient is stable; intact (+) Vestibular
- If Eyes open may sway: Lesion in CNS
System
- (+) Sway; unable to maintain posture and
- If patient demonstrate sway: problem in
balance
Vestibular System
- (-) Sway: Able to maintain posture and
balance. VISUALLY RELIANT
- Indications: Lesion on posterior column /
Dorsal Column Peripheral Neuropathy - Problem during condition 2,3,5,6
2. Sharpened Romberg Test - We can check if patient is visually reliant by
- Tandem position checking if there is an increase in sway
- Heel of one foot anterior to toes of other SURFACE DEPENDENT
foot
- Same instruction - Dependent on somatosensory input
- 4,5 and 6 (Increase sway here)
SENSORY ORGANIZATION TEST
VESTIBULAR: 5,6
- Moving platform, AP-ML
- Moving visual surround -> Visual Conflict VISUALLY: 2,3,5,6
- 30 seconds each condition
SURFACE: 4,5,6
SENSORY SELECTION PROBLEM: 3,4,5,6
- Increase sway and instability
SCORING: CHECK THE SWAY OF PATIENT
1- Minimal Sway
2- Moderate Sway
3- Severe Sway
4- Loss of Balance
CTSIB (CLINICAL TEST FOR SENSORY INTERACTION IN
BALANCE)
- Medium Density foam – surface
- Mediated Visual Dome (Japanese Lantern)
– Visual
- 30 seconds each condition, 6 conditions
- Increase sway or loss of balance are
recorded
- Subjective complaints & postural strategies
are also documented
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
MOVEMENT STRATEGIES FOR BALANCE Grade Static Dynamic
4 No handhold Maximal Challenge
1. FIXED SUPPORT support
- Ankle Strategy 3 (+) Postural Moderate
- Hip Strategy Sway Challenge
- Muscles 2 (+) Handheld Head Turning
a. Anterior support
- Gastrocnemius, hamstrings, Errector spinae (+) Minimal
b. Posterior Assistance
- Tibialis Anterior, hamstrings and quadriceps 1 (+) Handheld (-) Challenge
support
EXAMINATION OF MOVEMENT STRATEGIES Moderate to
Maximum
- Know first the ROM, MMT, POSTURAL
Support
CONTROL
0 Unable to Unable to maintain
a. STANDING CONTROL maintain balance
- Movement coordination test balance
- Symmetry in weight distribution, latency STANDARDIZED INSTRUMENTS
of response and strategies used.
b. SEATED CONTROL 1. BERG BALANCE SCALE (BBS)
- Position in seating position - 14 functional task, grading of 4-0
c. ANTICIPATORY POSTURAL CONTROL - Maximum Score: 56
- Anticipation of/for pertuberations - 45 or below: Higher risk for falls
d. DUAL TASK CONTROL 2. PERFORMANCE ORIENTED MOBILITY
- Balance+Other Task (if patient can do this ASSESSMENT (POMA/T-POMA/TINETTI-POMA
task) - Balance test & Gait Test
- Until 2/3
DOCUMENTATION - <19 score: High Risks for fall
- 19-24: Moderate score/risk
GRADING
REACH TEST
1- Present and Normal
2- Present but Delayed FUNCTIONAL AND MULTIDIRECTIONAL REACH TEST
3- Present but inappropriate
4- Abnormal - 1 meter stick
5- Absent - Should not have a change in BOS upon
reaching
FUNCTIONAL AND BALANCE GRADES
SCORING
STATIC AND DYNAMIC
GET UP AND GO TEST
- 3 meters from chair
- Check if stable: standing, walking and
turning
TIMED UP AND GO
- Healthy individuals: 10 seconds
- Elderly and with disabilities: 11-20 seconds
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- >30 seconds either healthy or none: Higher - The last ring of trachea is the most sensitive
risk for fall part
- Extends from C6-T5/T6 vertebra
TIMED WALKING TEST
b. Bronchi
- Usually 10m; check if there is deviation while
Right Left
walking
Shorter Longer
- 1.2-1.5m/s: Healthy Wider Slender
- 0.9-1.3 m/s: Elderly Vertical Oblique
- Slower: Higher risk for fall - Common Problem in the ® bronchi: It may
DISTANCE TEST lead to Aspiration Pneumonia due to its
orientation
- 3 or 6 or 12 min. walk test - Common Problem in the (L) Bronchi: It may
- Observe the patient’s gait lead to Pneumocystic Carinii Pneumonia
- While walking, change the instruction (PCP)
- Prone HIV →AIDS
3 – (N)
BRONCHIAL TREE
2- MILD
1. LOBAR/SECONDARY BRONCHI
1- MODERATE
- Right Lung has 3 Lobes
0- SEVERE
- Left Lung has 2 Lobes
MAXIMUM SCORE: 24 2. SEGMENTAL/TERTIARY BRONCHI
- Right Lung has 10 Lobes
INCREASE RISK OF FALL: <19 - Left Lung has 8 Lobes
DUAL TASK TEST 3. TERMINAL BRONCHIOLES
4. RESPIRATORY BRONCHIOLES
a. Walkie-Talkie Test 5. ALVEOLI
- Walk and talk at the same time - This is where gas exchange takes place
- Complicated questions - “ACINUS” – Functional Unit of Respiratory
b. Sitting Balance Tests System
c. Perceived Balance Confidence II. FUNCTIONAL RESPIRATORY SYSTEM
d. Activities-specific balance Confidence A. CONDUCTING ZONE
e. Balance Efficacy Scale - Extends from the nose up to your terminal
bronchioles (specifically in your dead
PULMONARY REHABILITATION
space)
I. STRUCTURAL RESPIRATORY SYSTEM B. RESPIRATORY ZONE
A. Upper Respiratory System - Extends from the Respiratory Bronchioles up
- Consists of nose, pharynx and larynx to Alveoli
a. Nose
RESPIRATION
- Contains nasal hair (vibrissae)
b. Larynx - Process of gas exchange in the body
- Contains the voice box a. EXTERNAL/PULMONARY RESPIRATION
- Contains 9 cartilages - Exchanges of gases between the alveolar
- Align at C4-C6 vertebra capillary membrane and pulmonary
- 3 Paired: Corniculate, Arytenoid and capillaries
Cuneiform b. INTERNAL/TISSUE RESPIRATION
- 3 Unpaired: Epiglottis, thyroid and Cricoid - Exchange of gases between pulmonary
(Align at the level of C6 vertebra/Level of capillaries and surrounding tissue cell
Tracheostomy)
B. Lower Respiratory System VENTILATION/BREATHING
- Consists of trachea, bronchi and lungs - Movement of air during inspiration (inflow)
a. Trachea and expiration (outflow)
- AKA: Windpipe
- Contains the carina
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
LUNG VOLUMES AND CAPACITIES (ITER) - Cigarette Smoker
SMOKE PACK YEARS
- Number of packs per day multiply by
number of years smoked
APPEARANCE OF PATIENT
1. GENERAL APPEARANCE
a. LEVEL OF CONSCIOUSNESS (LOC)
- No O2?
- Drowsy/Sleepy
b. BODY TYPE
LEGENDS: TLC= Total Lung Capacity - Endomorph
- Ectomorph
IRV= Inspiratory Reserve Volume TV= Tidal Volume
- Mesomorph
ERV=Expiratory Reserve Volume IC= Inspiratory Capacity c. CYANOSIS
RV= Residual Volume FRC= Functional Residual Capacity - Centrally (Lips)
- Peripheral (Nail Bed)
- Patient can have digital clubbing and
FORCED VITAL CAPACITY
reduce cardiac output
- Uses forced expiratory maneuver d. FACIAL SIGN/EXPRESSION
e. JUGULAR VEIN ENGORGEMENT
FLOW RATE f. HYPERTROPHY OF ACCESSORY MUSCLE
- Measure volume of air that moves over time g. PERIPHERAL EDEMA
- Usually ® CHF
EXPIRATORY FLOW RATE
PRIMARY MUSCLE FOR RESPIRATION? Diaphragm
- Volume of expired air over time required for
the air to be expired 2. CHEST SYMMETRY
- Normal AP: Lateral (1:2)
a. BARREL CHEST
FEV1 (Forced Expiratory Volume in 1 second) - 1:1
- Upper chest appears to be larger than
- Healthy: 70% or more than the total of FVC lower chest
- Sternum are prominent
- AP Diameter is greater than normal
- AKA: “Upper Chest Breather” COPD
b. PECTUS EXCAVATUM/FUNNEL CHEST
- Funnel Breast
- Lower Sternum depressed
- Lower Ribs flares out
- Excessive abdominal protrusion, little upper
chest movement
- AKA: “Diaphragmatic Breather”
c. PECTUS CARINATUM/PIGEON CHEST
- Commonly seen in pediatric rehabilitation
RESPIRATORY ASSESSMENT
- Pigeon Breast
PATIENT HISTORY - Sternum is prominent and protrudes
anteriorly
1. CHIEF OF COMPLAINT 3. POSITION OF COMFORT
- Common: Shortness of Breath/Dyspnea; - A patient who has difficulty breathing as the
cough (sputum/type of breathing) result of chronic lung disease often leans
2. WHY? forward on hands or forearms to stabilize
3. OCCUPATION/WORK and elevate the shoulder girdle to assist with
- Metro Aide (Exposure to air pollution)
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
inspiration (Diaphragm descends in this Formula
position)
SLEEP POSITION
- 2-3 pillows
- Increase pillow will lead to the tightening
muscle of the back (forward headed)
- A patient with cardiopulmonary dysfunction
oftenprefers to sleep in a head-up rather
than a fully recumbent position.
EXAMPLE:
MNEMONICS: “SOPUTS”
A 21-year-old patient who has a resting heart rate
Supine = Orthopnea; Platypnea= Upright; of 68 bpm, wanting to know his training heart rate
Trepopnea = Sidelying position for the intensity level 60-70%
PULMO/PT PROBLEMS SOLUTION:
1. DYSPNEA HIS MINIMUM TRAINING HEART RATE:
2. IMPAIRED AIRWAY CLEARANCE
220-21(Age) = 199
- “CASH” (Cough Assessment Sputum
Hydration) 199-68 (Resting Heart Rate) = 131
3. RISK FOR COMPLICATIONS OF DECREASE
MOBILITY 131 x .60 (Minimum Intensity) +68 (Resting Heart
- ROM, MMT and ADL’s Rate) = 146.6
HIS MAXIMUM TRAINING HEART RATE
Respiratory Rate / VS
220-21(Age) = 199
- Always check before, during and after
treatment 199-68 (Resting Heart Rate) = 131
Oxygen Saturation (Pulse Oximeter) 131 x .70 (Maximum Intensity) +68 (Resting Heart
Rate) = 159.7
- Pulse Oximeter measure PR and Oxygen
Saturation His Training Heart Rate Reserve will therefore be
- (N): 90-100% 147-160 bpm
At Rest With Exercise PSOB/BORG SCALE
O2 90-100% 85-100% - Ask patient where does she/he feel the
RPE 0-4 5-6 shortness of breath
RR 16-28 cpm 29-40cpm
provided RPE <5
PR 60-110 bpm Karvonens
BP 90-150/60-90 90-160/60-
mmHg 100 mmHg
KARVONENS
AKA: Heart Rate Reserve (HRR)
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
O2 Supplement 2. Watch the normal respiration pattern and
observe differences in the motion of the
- To prolong survival rate
chest wall and epigastric area and note
- If Partial Pressure of O2 = <60mmHg
any contraction of the neck muscles and
- Absolute indication for long term use=
the abdominal muscles.
<55mmHg
3. Epigastric rise and flaring of the lower
MECHANICAL VENTILATOR MODE margin of the rib cage during inspiration
indicate that the diaphragm is active.
A. Assist Control (AC): Constantly assisted by 4. The rise on both sides of the linea alba
ventilator should
B. Synchronized Intermittent Mandatory be symmetrical.
Ventilation (SIMV): Patient breaths on his 5. During quiet inspiration, epigastric rise
own but rest period is given wherein assisted reflects the movement of the diaphragm
by ventilator descending over one intercostal space.
C. Spontaneous: Breaths on his own 6. In deeper inspiratory efforts, the diaphragm
may move across three or more intercostal
BREATHING PATTERN
spaces.
- Rate, regularity, Location of ventilation at 7. An elevation and lateral expansion of the rib
rest and with activity cage are indicative of intercostal activity
- INSPIRATION: EXPIRATION during inspiration.
- (N) at rest 1:2 8. Exertional chest expansion measured at the
- With Activity: 1:1 level of the xiphoid process is 2.0 to 2.5
- COPD: 1:4 at rest inches (the expansion may exceed 3.0
inches in more active young people and
Normal Sequence of Inspiration athletes)
- Abdomen Rises: Diaphragm descends ALL GRADES (5-0)
- Ribs move out and up
- Upper Chest rises Patient Position: Supine
BREATHING PATTERNS Position of PT: Standing next to patient at
approximately waist level. One hand is placed
lightly on the abdomen in the epigastric area just
below the xiphoid process. Resistance is given (by
same hand) in a downward direction.
Test: Patient inhales with maximal effort and holds
maximal inspiration.
Instructions to Patient: “Take a deep breath … as
much as you can … hold it. Push against my hand.
Don’t let me push you down.”
GRADING
Grade 5 (Normal): Patient completes full inspiratory
(epigastric) excursion and holds against maximal
resistance. A Grade 5 diaphragm takes high
MMT OF DIAPHRAGM resistance in the range of 100 pounds.
Grade 4 (Good): Completes maximal inspiratory
- Diaphragm performs 70-80% of the effort of excursion but yields against heavy resistance.
quiet inspiration Grade 3 (Fair): Completes maximal inspiratory
expansion but cannot tolerate manual resistance
PRELIMINARY EXAMINATION
Grade 2 (Poor): Observable epigastric rise without
1. Uncover the patient’s chest and abdominal
completion of full inspiratory expansion.
area so that the motions of the chest and
abdominal walls can be observed.
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
Grade 1 (Trace): Palpable contraction is detected Auscultation
under the inner surface of the lower ribs, provided
that the abdominal muscles are relaxed. Another
way to detect minimal epigastric motion is by
instructing the patient to “sniff” with the mouth
closed.
Upper Lobe
Segment Right Lung Left Lung
Apical Immediately above and below the
IMPAIRED AIRWAY CLEARANCE (CASH) clavicle; immediately lateral and
below the clavicle
A. COUGH ASSESSMENT
- Phases of Cough Anterior Below the clavicle and nipple
a. Deep Inhalation
b. Breath Hold (1-3 seconds) Posterior Root of the spine of the Right
c. Forced Exhalation (2 times) Scapula
- 1- raise of sputum
Middle Lobe/Lingula
- 2- release
® Lung – Middle Lobe (L) Lung - Lingula
GRADING
Medial and Lateral to Superior and inferior to
FUNCTIONAL: Normal or Slight Impairment the ® nipple the (L) nipple
Lower Lobe
- Strong pain, loud and crispy
- >2 Tablespoon of sputum Segment Right Lung Left Lung
- Able to clear airway of secretion
Apical Medial to the scapulae, between
WEAK FUNCTIONAL: Moderate Impairment that the root of scapular spine and line of
affects the degree of active motion or endurance. inferior angle of the scapula
- Shallow, soft and throaty Anterior Immediately lateral and below the
- Appears labored nipples
- Can cough but can’t expel significant
amount of sputum or expel cough Posterior Immediately medial and inferior to
the inferior angle of the scapula
NON-FUNCTIONAL
Lateral In the mid-axillary line, immediately
- No clearance of airway
below the scapula
- No expulsion of air
- Cough attempt may be nothing more than Medial No Surface None at the (L)
an effort to clear the throat Landmark
ZERO
- Cough is absent RISK FOR COMPLICATIONS OF DECREASE MOBILITY
CHEST MOBILITY (COSTOVERTEBRAL EXPANSION)
- Symmetry of chest movement
PROCEDURE:
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
1. Place your hands on the patient’s chest and absent when air is trapped as the result of
assess the excursion of each side of the obstructed airways
thorax during inspiration and expiration.
CHEST WALL PAIN
a. TEST FOR UPPER LOBE EXPANSION
- Face the patient; place the tips of your PROCEDURE:
thumbs at the midsternal line at the sternal
notch. 1. Firmly press against the chest wall with your
- Extend your fingers above the clavicles. hands to identify any specific areas of pain
- Have the patient fully exhale and then potentially of musculoskeletal origin.
inhale deeply 2. Ask the patient to take a deep breath and
b. MIDDLE LOBE EXPANSION identify any painful areas of the chest wall.
- Continue to face the patient; place the tips 3. Chest wall pain of musculoskeletal origin
of your thumbs at the xiphoid often increases with direct point pressure
process and extend your fingers laterally during palpation and during a deep
around the ribs. Again, ask the patient to inspiration
breathe in deeply
MEDIASTINAL SHIFT
c. LOWER LOBE EXPANSION
- Place the tips of your thumbs along the - Position of trachea is normally oriented
patient’s back at the spinous processes centrally in the suprasternal notch
(lower thoracic level) and extend your
fingers around the ribs. PROCEDURE:
- Ask the patient to breathe in deeply
1. To identify a mediastinal shift, have the
EXTENT OF EXCURSION (2 METHODS) patient sit facing you with the head in
midline and the neck slightly flexed to relax
1. Measure the girth of the chest with tape the sternocleidomastoid muscles.
measure at 3 Levels. Document change in 2. With your index finger, gently palpate the
girth after maximum inspiration and soft tissue space on either side of the
expiration. trachea at the suprasternal notch.
a. AXILLA
3. Determine whether the trachea is palpable
- For Upper Lobe
at the midline or has shifted to the left or
b. XIPHOID
right
- For Middle Lobe
c. LOWER COSTAL *NOTE: Add = C/L; Subtract=I/L
- For Lower Lobe
MEDIATE PERCUSSION
2. Place both hands on the patient chest or
back. Note the distance between your - Examination technique designed to assess
thumbs after a maximum inspiration lung density, specifically, the air to solid ratio
in the lungs
PALPATION
PROCEDURE:
Tactile (Vocal) Fremitus
- Vibration felt while palpating over the chest 1. Place the middle finger of the nondominant
wall as patient speaks hand flat against the chest wall along an
intercostal space.
PROCEDURE (Upper, Middle and Lower Lobe) 2. With the tip of the middle finger of the
opposite hand, firmly tap on the finger
1. Place the palms of your hands lightly on
positioned on the chest wall.
the chest wall and ask the patient to speak
3. Repeat the procedure at several points on
a few words or repeat “99” several times or
the right and left and anterior and posterior
tres tres.
aspects of the chest wall.
2. Normally, fremitus is felt uniformly on the
4. This maneuver produces a resonance; the
chest wall.
pitch varies with the density of the
3. Fremitus is increased in the presence of
underlying tissue.
secretions in the airways and decreased or
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
NOTE IN MEDIATE PERCUSSION:
a. RESONANT
- Indicates normal lungs
b. HYPERRESONANT/TYMPANIC
- Greater amount of air in the area
- May indicate emphysema
c. DULL
- Liver is percussed
d. FLAT
- Muscle is percussed
BREATH SOUNDS
1. INSIDE THE LUNGS
a. AIR
- Decrease sound
PLEASE TAKE NOTE: ALWAYS CLEAN YOUR
b. SOLID/LIQUID STETHOSCOPE
- Increase sound
2. OUTSIDE THE LUNGS ADVENTITIOUS BREATH SOUNDS
a. ANYTHING
- Decrease sound
Vocal Sounds
Normal Transmission
- Loudest near the trachea & mainstem
bronchi
- Softer & less clear at the more distal areas of
the lungs.
Abnormal Transmission
- Heard loud on distal lung field through
a. Fluid-filled areas of consolidation ATELECTASIS
b. Cavitation lesion
c. Pleural effusions - Absence of air and collapse of an area of
a. Egophony lung tissue.
- nasal or bleeting sound; “E” sounds are
SPUTUM ASSESSMENT
transmitted to sound like “A”
b. Whispered Pectoriloquy MNEMONIC: COAT
- increased loudness of whispering; pt
whispers “one, two, three” 1. COLOR
c. Bronchophony a. Clear
- Voice remaining loud at the periphery of b. Yellow
the lungs or sounding louder than usual; pt - Infection to be clear
repeats the phrase “99” or “66” c. Green
- All secretion/stasis/acute infection, pus
NORMAL BREATH SOUNDS d. Blood-Stained
- Too much coughing or hemoptysis
e. Frank Blood
- Massive hemoptysis
f. Gray
- Abscess/Emphysema
g. Rust
- Pneumonia
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
h. Purple Hand Evaluation and Anthropometry
- Neoplasm
Muscle Strength
i. Pink/white, frothy
- Pulmonary Edema, CHF - MMT
2. ODOR - Hand-held dynamometer (HHD)
a. Sweet
- Like pseudomonas Grade Description
b. Foul 5 Normal Ability to complete a full
- Indicates infection range of motion or maintain
3. AMOUNT end-point range against
maximal resistance
- 2 tablespoon or 30 mL per day indicate
4 Good Ability to complete a full
normal
range of motion against
4. TEXTURE
gravity and can tolerate
a. THIN strong resistance without
- Indicate normal saliva braking the test position.
b. THICK/VISCOUS GIVES or YIELDS at maximum
- Check the patient if she/he is hydrated resistance
3 Fair Ability to complete a full
CAUTION: Do not treat patient if there is a lot of
range of motion against only
blood during coughing the resistance of gravity.
a. BLEB 2 Poor Can complete full ROM in a
position that minimizes the
- Burst (putok) during inhalation
force of gravity .
b. BULLAE
“GRAVITY MINIMIZED
- Bubble formation
POSITION” (horizontal plane
HYDRATION of motion)
1 Trace Examiner can detect visually
ROM or by palpation some
contractile activity
- Please read shoulder and neck movement NO movement of a joint
range of motion 0 No No visible or palpable
activity contraction.
MMT
Grip Strength
- Grading and Procedure for MMT of
- Assessment Tools: Hand dynamometer
pectoralis minor and major; SCM
- 5 adjustable handle spacings
- Test each hand alternately
- Do not fatigue patient
- There should be a 5% to 10% difference
betweenthe dominant and nondominant
hands.
- Three trials
- Discrepancies of more than 20% in a test-
retest situation indicate that the patient is
not exerting maximal force
- Alternative method: BP apparatus
Pinch Strength
- Pinch meter
- Pulp-to-pulp
- Lateral prehension
- Three trials
- Thumb: - The thumb is the most important
digit. Because of its relation with the other
digits, its mobility, and the force it can bring
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
to bear, its loss can affect hand function Functional Impairment of Hand
greatly.
- Loss of:
- Index Finger: the 2nd most important digit
a. Thumb: 40-50% of hand function
because of its musculature, its strength,
b. Index finger: 20%
- and its interaction with the thumb. Its loss
c. Middle finger: 20%
greatly affects lateral and pulp-to-pulp
d. Ring finger: 10%
pinch and power grip
e. Little finger: 10%
- In flexion, the middle finger is strongest, and
- LOSS OF HAND: 90% loss of UE function
it is important for both precision and power
grips Types of Grips
- The ring finger has the least functional role in
the hand. 1. Power Grips
- The little finger, because of its peripheral - Requires control of greater flexor asymmetry
position, greatly enhances power grip, to the hand
- affects the capacity of the hand, and holds - Ulnar side of the hand works with the radial
objects against the hypothenar eminence. side
- Is used when STRENGTH or FORCE is the
Functional Wrist & Hand Scan primary consideration
- Digits maintain objects against the palm
- Thumb may or may not be involved
- Extrinsic ms are more important
- Power Grips: hook grasp, cylinder grasp, fist
grasp or digital palmar prehension, spherical
grasp, ulnar side of the hand works with the
radial side to give STRONGER STABILITY
2. Precision Grips
- Requires control of greater flexor asymmetry
to the hand
- Ulnar side of the hand works with the radial
side
- It is used when STRENGTH or FORCE is the
primary consideration
- Digits maintain objects against the palm
- Thumb may or may not be involved
- Extrinsic ms are more important
3 Types of Pinch Grip
1. 3-point chuck, threefingered, or digital
prehension, in which palmar pinch, or
subterminal opposition, is achieved.
- With this grip, there is pulp-to-pulp pinch,
and opposition of the thumb and fingers is
necessary (e.g., holding a pencil).
- This grip is sometimes called a precision grip
with power.
2. Lateral key, pulp-to-side pinch, lateral
prehension, or subterminolateral opposition.
- The thumb and lateral side of the index
finger come into contact. No opposition is
needed.
- An example of this movement is holding
keys or a card.
3. Tip pinch, tip-to-tip prehension, or terminal
opposition.
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
- With this positioning, the tip of the thumb is shirt, buttoning, zipping, putting on gloves,
brought into opposition with the tip of dialing a telephone, tying a bow,
another finger. This pinch is used for activities manipulating safety pins, manipulating
requiring fine coordination rather than coins, threading a needle, unwrapping a
power. Band-Aid, squeezing toothpaste, and using
a knife and fork.
Other Hand Functional Testing Methods
- Each subtask is timed
1. Jebsen-Taylor Hand Function Test 6. Moberg’s Pickup test
- This easily administered test involves seven - An assortment of nine or ten objects (e.g.,
functional areas: bolts, nuts, screws, buttons, coins, pens,
a. writing; paper clips, keys) is used.
b. card turning - The patient is timed for the following tests:
c. picking up small objects a. Putting objects in a box with the affected
d. simulated feeding hand
e. stacking b. Putting objects in a box with the unaffected
f. picking up large, light objects; and hand
g. picking up large, heavy objects. c. Putting objects in a box with the affected
- The subtests are timed for each limb. hand with eyes closed
- This test primarily measures gross - The examiner notes which digits are used for
coordination, assessing prehension and prehension. Digits with altered sensation are
manipulative skills with functional tests. less likely to be used. The test is used for
- It does not test bilateral integration median or combined median and ulnar
2. Minnesota Rate of Manipulation test nerve lesions.
- This test involves five activities: 7. Box & Block Test
a. placing, - This is a test for gross manual dexterity in
b. turning, which 150 blocks, each measuring 2.5 cm (1
c. displacing, inch) on a side, are used.
d. one-hand turning and placing, and - The patient has 1 minute in which to
e. two-hand turning and placing. individually transfer the blocks from one
- The activities are timed for both limbs and side of a divided box to the other.
compared with normal values. - The number of blocks transferred is given as
- The test primarily measures gross the score.
coordination and dexterity - Patients are given a 15-second practice trial
3. Purdue Pegboard test before the test
- This test measures fine coordination with the 8. 9-hole Peg Test
use of small pins, washers, and collars. - This test is used to assess finger dexterity. The
- The assessment categories of the test are: patient places nine 3.2-cm (1.3-inch) pegs in
a. right hand, a 12.7 × 12.7 cm (5 × 5 inch) board and then
b. left hand, removes them.
c. both hands, - The score is the time taken to do this task.
d. right, left, and both, and Each hand is tested separately.
e. assembly
Anthropometric Measurements
- The subtests are timed and compared with
normal values based on gender and Leg Length Measurement
occupation.
1. True Leg Length
4. Crawford Small Parts Dexterity Test
- Site: ASIS to medial malleolus
- This test measures fine coordination,
- If patient is obese, use lateral malleolus as
including the use of tools such as tweezers
landmark
and screwdrivers to assemble things, to
- Must set the pelvis,
adjust equipment, and to do engraving
- Legs should be 15-20 cm (4-8in)
5. Simulated Activities of Daily living
- if 1-1.5cm difference N but may cause sxs
Examination
- Iliac crest to greater troch coxa vara, gr
- This test consists of nineteen subtests,
troch to lateral knee jt line femoral shaft,
including standing, walking, putting on a
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
medial knee jt line to medial mall tibial - The examiner then takes the tape measure
length across the anterior wrist to the most distal
2. Apparent Leg Length aspect of the radial styloid process
- Site: Xiphesternum or Umbilicus to medial - From there, the tape is brought diagonally
malleolus across the back (dorsum) of the hand and
- d/t pathology or contracture somewhere in over the 5th metacarophalangeal joint line,
the spine, pelvis or lower limbs. across the anterior surface of the
metacarpophalangeal joints
Muscle Bulk Measurement
- then diagonally across the back of the
- Most common points hand to where the tape started
a. 20 cm above MJL
Lower Extremity
b. 10 cm above MJL
c. 9 cm below fibular head 1. LE toes
- Effusion & atrophy/hypertrophy - base, PIP, DIP
- Select areas where mm bulk or swelling 2. Ankle
greatest and measures circumference - + MTP then every 4cm/2in prox
- Common knee, leg, thigh – how far above 3. Leg/knee
or below the apex or base of patella - + lateral mall then every 4
- Note if swelling or mm bulk 4. Thigh/hip
- Can use lateral jt line than patella - lateral knee jt line then every 4
- Normal Value for Athlete: 5-8cm
Figure of Eight Measurement in Ankle
Extensor Lag
- The patient is positioned in long sitting with
- AKA: Heel height difference the ankle and lower leg beyond the end of
- The patient lies prone on the examining the examining table with the ankle in
table with the lower limbs supported by the plantigrade (90°)
thighs. - the examiner places the end of the tape
- The difference in heel height is measured. measure on the tibialis anterior tendon,
- Normal Value: 1-1.5 cm drawing the tape medially across the instep
just distal to the navicular tuberosity
Limb-Girth Measurement
- The tape is then pulled across the arch of
- Edema, swelling, effusion the foot just proximal to the base of the 5th
- Swelling/Effusion: Bony landmarks and every metatarsal across the tibialis anterior
4cm/2 in. proximal or distal depending on tendon, and then around the ankle joint just
the extent distal to the tip of the medial malleolus,
across the Achilles tendon, and just distal to
Upper Extremity the lateral malleolus, returning to the starting
position
1. UE fingers
- Repeat 3 Times then average
- base, PIP together, DIP together
2. Wrists Volumetric Measurement
- +MCP, thumb webline, wrist joint at radial
styloid - Volumeter
3. FA/elbow - Generalized Edema & local swelling,
- + radial styloid every 4cm/2 in proximal atrophy irreg (distal ext)
4. Arm/shoulder - 10-mL difference L & R hand, dominant &
- + lateral epi, every 4cm/2 in proximal nondominant hands
- Swelling 30-50 mL difference
Figure of eight measurement of the hand
Skin Fold Measurements
- The examiner places a mark on the distal
aspect of the ulnar styloid process as a Skin Fold Sites
starting point.
✓ Triceps
✓ Biceps Brachii
✓ Subscapular
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
lOMoARcPSD|8901201
✓ Iliac crest
✓ Supraspinal
✓ Abdominal
✓ Front thigh
✓ Medial calf
Body Fat Measurements
- body composition (mm, fat, bone mass)
- Used to determine the individuals body type
(mesomorphic, endomorphic, ectomorphic
3 Sufficient Sites
- Males <12-15% body fat
- Endurance athletes <7%
- No one should below 5% body fat
- M >14% and F >17% weight loss program or
weight training inc lean body mass
Downloaded by Anne Margaret Serneo (annemargaretserneo@yahoo.com)
You might also like
- Brain-Computer Interface Technologies: Accelerating Neuro-Technology for Human BenefitFrom EverandBrain-Computer Interface Technologies: Accelerating Neuro-Technology for Human BenefitNo ratings yet
- Horner'S Syndrome - : Far Eastern University - Nicanor Reyes Medical FoundationDocument3 pagesHorner'S Syndrome - : Far Eastern University - Nicanor Reyes Medical FoundationVictorija Evania Lucille DeldioNo ratings yet
- SPINEDocument8 pagesSPINEadrian kristopher dela cruzNo ratings yet
- Memory 1Document6 pagesMemory 1Priyanka KoundinyaNo ratings yet
- NervoussystemlabreportDocument12 pagesNervoussystemlabreportapi-331457108No ratings yet
- SI Psych - ISTDocument26 pagesSI Psych - ISTashleighmarshall05No ratings yet
- Neurologic Conditions 1 SciDocument5 pagesNeurologic Conditions 1 SciEdward De LeonNo ratings yet
- Copia de 13.12Document9 pagesCopia de 13.12INÉS TORIBIO ARGÜELLESNo ratings yet
- Neurologic Examination (Bhs - Inggris) Kelompok 6Document35 pagesNeurologic Examination (Bhs - Inggris) Kelompok 6Gladys SariowanNo ratings yet
- Cranial Nerves TorresDocument37 pagesCranial Nerves TorresZari Danielle C. TorresNo ratings yet
- Lecture 12 - Neural PlasticityDocument18 pagesLecture 12 - Neural PlasticityMaurice EbeidNo ratings yet
- Cranial Nerves, Spinal Nerves, Autonomic System WSDocument5 pagesCranial Nerves, Spinal Nerves, Autonomic System WSBianca Cielo BalabagNo ratings yet
- ALectN (Organ System Overview-CellsTissues)Document47 pagesALectN (Organ System Overview-CellsTissues)Elaine MalinayNo ratings yet
- NP Workshop Poster Ver 5Document1 pageNP Workshop Poster Ver 5shuusakuNo ratings yet
- PSY 1101F Brain Practice ChartDocument4 pagesPSY 1101F Brain Practice Chartmelau2303No ratings yet
- My Encephalo NDocument2 pagesMy Encephalo NC1 - RAZALAN NICKA JOYNo ratings yet
- EquilibriumDocument72 pagesEquilibriumCandice LavigneNo ratings yet
- Nervous SystemDocument39 pagesNervous Systemespinajeff07No ratings yet
- Top Down Control of Spinal Sensorimotor Circuits Essential For SurvivalDocument8 pagesTop Down Control of Spinal Sensorimotor Circuits Essential For SurvivalErick SolisNo ratings yet
- Materi Postural OntogenesisDocument14 pagesMateri Postural Ontogenesisdamha al bannaNo ratings yet
- Prop Iose Psi OnDocument12 pagesProp Iose Psi OnAngela Veloso VegaNo ratings yet
- 6 Komponen SensoriDocument29 pages6 Komponen SensoriYusrina RahmaNo ratings yet
- SPINEDocument8 pagesSPINEadrian kristopher dela cruzNo ratings yet
- Neuro Concept NotesDocument35 pagesNeuro Concept Noteshoney requermeNo ratings yet
- Make Me Think: A Brief Introduction To The Brain-Computer InterfacesDocument40 pagesMake Me Think: A Brief Introduction To The Brain-Computer InterfacesZim ShahNo ratings yet
- 10 Neurologic Disorder in ChildrenDocument163 pages10 Neurologic Disorder in ChildrenFugado Mica illaNo ratings yet
- Lectura Complementaria 1 - Bobath AdultoDocument25 pagesLectura Complementaria 1 - Bobath AdultoRaul Vieira VillarroelNo ratings yet
- BRYAN LECAROS BSN-1B ANATOMY AND PHYSIOLOGY - LaboratoryDocument25 pagesBRYAN LECAROS BSN-1B ANATOMY AND PHYSIOLOGY - LaboratoryChrista Villanueva MalinaoNo ratings yet
- Nervous SystemDocument9 pagesNervous SystembasanjeevNo ratings yet
- Unit 12Document30 pagesUnit 12aritrayeebarman05No ratings yet
- Central Nervous System: Spinal CordDocument12 pagesCentral Nervous System: Spinal CordHarly E. DeniegaNo ratings yet
- Frog PDFDocument14 pagesFrog PDFMohammad Hasanul KabirNo ratings yet
- Peripheral Nervous System: Cranial NervesDocument2 pagesPeripheral Nervous System: Cranial NervesNoemi ReyesNo ratings yet
- Tema 16Document27 pagesTema 16louNo ratings yet
- Anatomy of Nervous SystemDocument14 pagesAnatomy of Nervous System사나No ratings yet
- The Tenosynovitis: Patient Has Wrist or HandDocument2 pagesThe Tenosynovitis: Patient Has Wrist or HandrobouNo ratings yet
- Unpacked Melc of Science 6 Second GradingDocument18 pagesUnpacked Melc of Science 6 Second GradingGrace GaraldeNo ratings yet
- Plastisitas OtakDocument67 pagesPlastisitas OtakFtrNo ratings yet
- Journal Club - Biomechanics LabDocument21 pagesJournal Club - Biomechanics LabLuis TorresNo ratings yet
- PIIS1364661321000565Document13 pagesPIIS1364661321000565Christo ChristoffNo ratings yet
- Chapter 19 BrainDocument7 pagesChapter 19 BrainUloko ChristopherNo ratings yet
- Lab Manual - Senses Primer - A+p - StudentDocument14 pagesLab Manual - Senses Primer - A+p - StudentsylNo ratings yet
- DR Ramon de Santos NHS - Siyensikula - Nervous System SCRIPTDocument8 pagesDR Ramon de Santos NHS - Siyensikula - Nervous System SCRIPTFroilan AlexNo ratings yet
- ComprehensivePhysiologyDocument29 pagesComprehensivePhysiologySimon CavalcanteNo ratings yet
- Sanket ProjectDocument45 pagesSanket ProjectSanket JainNo ratings yet
- Neurologic System - Lec 1Document6 pagesNeurologic System - Lec 1Farmisa MannanNo ratings yet
- Animal Behavior & Stimulus EnergyDocument17 pagesAnimal Behavior & Stimulus Energylevonbachdasarian100% (1)
- NeuroscienceDocument5 pagesNeuroscienceChing MacarubboNo ratings yet
- Castiello (2007) The Cortical Control of Visually Guided GraspingDocument15 pagesCastiello (2007) The Cortical Control of Visually Guided GraspingEdgarNo ratings yet
- General Psychology 4: THE Physiological Basis OF Behavior: Prepared By: Mark Fredderick R. Abejo RN, MANDocument4 pagesGeneral Psychology 4: THE Physiological Basis OF Behavior: Prepared By: Mark Fredderick R. Abejo RN, MANMariel EfrenNo ratings yet
- Chapter 49Document11 pagesChapter 49Argie abrisNo ratings yet
- Anaphy ReviewerDocument9 pagesAnaphy ReviewerPrince Chester CamaliganNo ratings yet
- The Autonomic Nervous System and Its Central ControlDocument15 pagesThe Autonomic Nervous System and Its Central Controlpuchio100% (1)
- Neuropshiologic MonitoringDocument6 pagesNeuropshiologic MonitoringAurelia AlexandraNo ratings yet
- Bio101 General Zoology: Nervous SystemDocument36 pagesBio101 General Zoology: Nervous SystemKhara TeanoTanNo ratings yet
- Central Nervous System (CNS) Neuroanatomy &Document26 pagesCentral Nervous System (CNS) Neuroanatomy &Asaad JawedNo ratings yet
- NCM 116 - Neuro (MODULE 1)Document10 pagesNCM 116 - Neuro (MODULE 1)Meryville Jacildo100% (1)
- LECTURE 2 Biological Basis of BehaviorDocument74 pagesLECTURE 2 Biological Basis of BehaviorColossal HeartNo ratings yet
- K3. Anatomi Sistem Limbik, ARAS, Saraf Tepi, Dalam Aspek Neurologis (Dr. Ahmad Azmi Nasution, M.Biomed)Document112 pagesK3. Anatomi Sistem Limbik, ARAS, Saraf Tepi, Dalam Aspek Neurologis (Dr. Ahmad Azmi Nasution, M.Biomed)AmesyahNo ratings yet
- Igm 5Document34 pagesIgm 5Berliana YogiyantiNo ratings yet
- PEAT1Document60 pagesPEAT1Anne Serneo100% (4)
- Norkin, C. C., & White, D. J. (2009) - Measurement of Joint Motion: A Guide To Goniometry. Philadelphia: F.A. Davis. jdcptrp2019Document12 pagesNorkin, C. C., & White, D. J. (2009) - Measurement of Joint Motion: A Guide To Goniometry. Philadelphia: F.A. Davis. jdcptrp2019Anne SerneoNo ratings yet
- Trigger Finger Aug 2020 v5Document2 pagesTrigger Finger Aug 2020 v5Anne SerneoNo ratings yet
- Special Test - Lecture Notes 1 Special Test - Lecture Notes 1Document18 pagesSpecial Test - Lecture Notes 1 Special Test - Lecture Notes 1Anne SerneoNo ratings yet
- Upper-LIMB-Muscles Upper-LIMB - MusclesDocument8 pagesUpper-LIMB-Muscles Upper-LIMB - MusclesAnne SerneoNo ratings yet
- Giles Retention Exam Giles Retention ExamDocument28 pagesGiles Retention Exam Giles Retention ExamAnne Serneo100% (1)
- 10.1007@s00405 020 06193 3Document6 pages10.1007@s00405 020 06193 3Anne SerneoNo ratings yet
- Nerve Tendon GlidingDocument10 pagesNerve Tendon GlidingAnne SerneoNo ratings yet
- Role of Kabat Physical Rehabilitation in Bell's Palsy: A Randomized TrialDocument6 pagesRole of Kabat Physical Rehabilitation in Bell's Palsy: A Randomized TrialAnne SerneoNo ratings yet
- Tate J. Hedtke SPED 608 Assignment #6 Standard # 8 Cross Categorical Special Education/ Learning Disabilities Artifact SummaryDocument5 pagesTate J. Hedtke SPED 608 Assignment #6 Standard # 8 Cross Categorical Special Education/ Learning Disabilities Artifact Summaryapi-344731850No ratings yet
- Apr 00Document32 pagesApr 00nanda2006bNo ratings yet
- Learning Competency: Explain The Postulates of The Cell TheoryDocument4 pagesLearning Competency: Explain The Postulates of The Cell TheoryPamela Isabelle TabiraraNo ratings yet
- scn615 Classroomgroupactionplan SarahltDocument3 pagesscn615 Classroomgroupactionplan Sarahltapi-644817377No ratings yet
- Dispeller of Obstacles PDFDocument276 pagesDispeller of Obstacles PDFLie Christin Wijaya100% (4)
- A Financial History of The United States PDFDocument398 pagesA Financial History of The United States PDFiztok_ropotar6022No ratings yet
- ABC of Effective WritingDocument4 pagesABC of Effective Writingprada85No ratings yet
- 0606 - s03 - 2 - 0 - QP PENTING KE 2Document8 pages0606 - s03 - 2 - 0 - QP PENTING KE 2Titin ChayankNo ratings yet
- A Neural Network Based System For Intrusion Detection and Classification of AttacksDocument6 pagesA Neural Network Based System For Intrusion Detection and Classification of AttacksbharadwajrohanNo ratings yet
- Modern Prometheus Editing The HumanDocument399 pagesModern Prometheus Editing The HumanHARTK 70No ratings yet
- AMU BALLB (Hons.) 2018 SyllabusDocument13 pagesAMU BALLB (Hons.) 2018 SyllabusA y u s hNo ratings yet
- Avatar Legends The Roleplaying Game 1 12Document12 pagesAvatar Legends The Roleplaying Game 1 12azeaze0% (1)
- Transportation Research Part F: Andreas Lieberoth, Niels Holm Jensen, Thomas BredahlDocument16 pagesTransportation Research Part F: Andreas Lieberoth, Niels Holm Jensen, Thomas BredahlSayani MandalNo ratings yet
- Isolasi Dan Karakterisasi Runutan Senyawa Metabolit Sekunder Fraksi Etil Asetat Dari Umbi Binahong Cord F L A Steen S)Document12 pagesIsolasi Dan Karakterisasi Runutan Senyawa Metabolit Sekunder Fraksi Etil Asetat Dari Umbi Binahong Cord F L A Steen S)Fajar ManikNo ratings yet
- Sexuality Disorders Lecture 2ND Sem 2020Document24 pagesSexuality Disorders Lecture 2ND Sem 2020Moyty MoyNo ratings yet
- India Internet Goldman SachsDocument86 pagesIndia Internet Goldman SachsTaranjeet SinghNo ratings yet
- MODULE 13 Ethics Through Thick and ThinDocument7 pagesMODULE 13 Ethics Through Thick and ThinCristobal M. CantorNo ratings yet
- Oscar Characterization TemplateDocument3 pagesOscar Characterization Templatemqs786No ratings yet
- G12 PR1 AsDocument34 pagesG12 PR1 Asjaina rose yambao-panerNo ratings yet
- The Concise 48 Laws of Power PDFDocument203 pagesThe Concise 48 Laws of Power PDFkaran kamath100% (1)
- Theoretical Foundations of NursingDocument22 pagesTheoretical Foundations of Nursingattilaabiidn100% (3)
- Watchitv Portable: Iptv Expert Analysis Application: Key ApplicationsDocument5 pagesWatchitv Portable: Iptv Expert Analysis Application: Key ApplicationsBen PoovinNo ratings yet
- ECON2100 CO Abdool W21Document5 pagesECON2100 CO Abdool W21Imran AbdoolNo ratings yet
- Far 1 - Activity 1 - Sept. 09, 2020 - Answer SheetDocument4 pagesFar 1 - Activity 1 - Sept. 09, 2020 - Answer SheetAnonn100% (1)
- Academic Calendar 2014 15Document6 pagesAcademic Calendar 2014 15D Geetha DuraiNo ratings yet
- The Christian Life ProgramDocument28 pagesThe Christian Life ProgramRalph Christer MaderazoNo ratings yet
- Graduation Ceremony 2013Document7 pagesGraduation Ceremony 2013Angelie Hermoso RoldanNo ratings yet
- Chapter 23 AP World History NotesDocument6 pagesChapter 23 AP World History NotesWesley KoerberNo ratings yet
- Ant Colony AlgorithmDocument11 pagesAnt Colony Algorithmjaved765No ratings yet
- EmTech TG Acad v5 112316Document87 pagesEmTech TG Acad v5 112316Arvin Barrientos Bernesto67% (3)