Professional Documents
Culture Documents
Vascular Reactions and Sunburn Effects
Uploaded by
Jolaine ValloOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Vascular Reactions and Sunburn Effects
Uploaded by
Jolaine ValloCopyright:
Available Formats
General: Vascular Reactions (★)
• Vasculitic process manifestation on skin → skin becomes erythematous
• Know the shade of red – pinkish red is the lightest shade
o Dusky purpuric, bluish ecchymostic, etc – be more attentive to these lesions
o Shade can prognosticate patient
• Do digital pressure on lesions to check for blanching
o Blanching – increased blood flow
o Non-blanching – extravasation of RBCs into the skin (petechiae, ecchymosis, purpura)
o When digital pressure is done on suspected petechial lesions, you may get false impression that lesion
is non blanching – refill time may be fast, do diascopy instead
o Diascopy – use transparent object (like a slide)
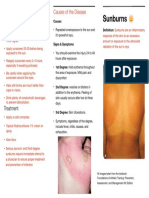
Sunburn and Solar Erythema
Description:
• Sunburn – normal cutaneous reaction to sunlight in excess of an erythema dose
o UVB erythema – evident around 6 (8★) hours after exposure and peaks at 12-24 hours, but onset is
sooner and severity greater with increased exposure
o Erythema → tenderness → blistering which may become confluent (severe cases)
o Desquamation common ~1 week after sunburn, even in areas that have not blistered
o Other s/s: discomfort (may become severe), edema (typically in the extremities and face), chills, fever,
nausea, tachycardia, hypotension
▪ May last for as long as a week in severe cases
• Photosensitive areas: (★)
o Face (zygomatic areas, bridge of nose – butterfly rash, brow area, over the chin)
o Extensor aspects of extremities
o Chest
o Also depends on type of clothing worn
• Skin changes after UV exposure: 1) immediate pigment darkening (IPD, Meirowsky phenomenon) and 2)
delayed melanogenesis
o IPD – maximal within hours after exposure, results from metabolic changes and redistribution of
present melanin, not photoprotective
o Delayed melanogenesis by UVB – mediated through DNA damage + formation of cyclobutane
pyrimidine dimers, provides some photoprotection from further solar injury at the expense of epidermis
and dermis damage
• Generally, a sunburn victim experiences at least 1 or 2 days of discomfort +/- pain before relief
• Check if patient is male – men usually experience sunscreen failure due to failure to reapply or not applying at
all
Causes:
• Minimal erythema dose (MED) – minimal amount of a particular wavelength of light capable of inducing
erythema on an individual’s skin
o Essentially all solar erythema is caused by UVB
o UVB is up to 1000 times more erythemogenic than UVA
o Amount of UVA is 100 times greater than UVB during midday hours (9 AM to 3-4 PM)
o Most biologically effective wavelength of radiation from the sun for sunburn – 308 nm
• UVA – important in drug-induced photosensitivity, photoaging, and cutaneous immunosuppression
• Factors in UV exposure: higher altitudes, temperate climates in summer months, tropical regions, hours of the
day
Treatment:
• Skin type – used to determine starting doses of phototherapy and sunscreen recommendations, reflects risk of
skin cancer and photoaging (★)
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
o Asians – usually skin type V
Skin Types (Phototypes)
Skin Type Baseline Skin Color Sunburn and Tanning History
I White Always burns, never tans
II White Always burns, tans minimally
III White Burns moderately, tans gradually
IV Olive Minimal burning, tans well
V Brown Rarely burns, tans darkly
VI Dark Brown Never burns, tans darkly black
• (+) redness and other symptoms – treatment has limited efficacy because inflammation cascades have already
been triggered
o Prostaglandins (especially E) – important mediators
• Treatment should be supportive
o Pain management with ASA, acetaminophen, or NSAIDs
o Soothing topical emollients or corticosteroid lotions
• Aspirin, NSAIDs (including indomethacin), topical and systemic steroids have been studied
o Medium-potency (class II) topical steroids applied 6 hours after the exposure (when erythema first
appears) – small reduction in s/s
o Oral NSAIDs and systemic steroids – insufficient evidence to recommend their routine use, except
immediately after solar overexposure
Prophylaxis: Prevention is best for sunburns!!!
• Tanning not recommended for sun protection and may cause melanoma
• Avoid midday sun, seek shade, wear sun-protective clothing, apply sunscreen
o Sun-protective clothing: denser weaves, washed older clothing, loose-fitting clothes (wet fabric
substantially reduces photoprotection)
o Sunscreen – chemical (UV-absorbing chemicals) and physical (UV-scattering or blocking
o agents)
▪ Skin types I to III – daily application of broad-spectrum (UVA and UVB coverage) sunscreen
(SPF 30)
▪ Outdoor exposure – regular use of SPF 30 or higher
▪ Severe photosensitivity, times of high sun exposure – high-intensity sunscreen (SPF 30+) with
inorganic blocking agents
▪ Apply at least 20 (30★) minutes before and 30 minutes after exposure – reduces skin exposure
2-3x
▪ Reapply after swimming, vigorous activity, toweling
▪ May be applied to babies (under 6 months) on limited areas
• Vitamin D supplementation (600 IU daily for 70 and younger, 800 IU for older) – recommended with the most
stringent sun protection practices
• Exposure to UVA and UVB increases epidermis thickness, especially the stratum corneum → increased tolerance
to further solar radiation
Photosensitivity Reactions (Phototoxic, Photoallergic)
Summary table: (★)
Phototoxicity Photoallergy
Clinical presentation Exaggerated sunburn reaction: Eczematous lesions
erythema, edema, vesicles, bullae Usually pruritic
Burning, stinging
Frequently resolves with
hyperpigmentation
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
Pathophysiology Direct tissue injury Type IV delayed hypersensitivity
response
Sensitization occurs
Occurrence after first exposure Yes No
Onset after exposure Minutes to hours >24 to 48 hours
Immediate, instantaneous
Common agents Antiarrhythmics (amiodarone, Topical Agents
quinidine) Sunscreens (ex. oxybenzone)
Triazole antifungals (voriconazole) Fragrances (6-methylcoumarin, musk
Diuretics (furosemide, thiazides) ambrette, sandalwood oil)
NSAIDs (nabumetone, naproxen, Antimicrobial agents (bithionol,
piroxicam) chlorhexidine, fenticlor,
Phenothiazines (chlorpromazine, hexachlorophene)
prochlorperazine) NSAIDs (diclofenac, ketoprofen)
Psoralens (5-methoxypsoralen, 8- Phenothiazines (chlorpromazine,
methoxypsoralen, 4,5’,8- promethazine)
trimethylpsoralen)
Quinolones (ciprofloxacin, Systemic Agents
lomefloxacin, nalidixic acid, Antiarrhythmics (quinidine)
sparfloxacin) Antimalarials (quinine)
St. John’s wort (hypericin) Antifungals (griseofulvin)
Sulfonamides Antimicrobials (quinolones,
Sulfonylureas sulfonamides)
Tar (topical) NSAIDs (ketoprofen, piroxicam)
Tetracyclines (doxycycline, Diuretics (furosemide)
demeclocycline) Thiazides
Idiopathic Photosensitivity Reactions
Description:
• Nonimmunologic reaction that develops after exposure to specific wavelength and intensity of light in the
presence of a photosensitizing substance
• Can be elicited despite no prior history of exposure or sensitivity to that particular substance, but individual
susceptibility widely varies
• Sunburn-type reaction, with erythema, tenderness, and even blistering occurring only on sunexposed parts
o Erythema begins within 2-6 hours but worsens for 48–96 hours before beginning to subside
o Photo-onycholysis – exposure of nail bed
o Marked hyperpigmentation may occur even without significant preceding erythema
• Phototoxic tar dermatitis – severe burning erythema for 1-3 days, with hyperpigmentation after that may persist
for years
• Phytophotodermatitis – burning erythema → edema → vesicles or bullae, intense residual hyperpigmentation
may persist for weeks or months
o Intensity may be initially mild and not recalled by patient
o Ask for occupation of the patient – farmer, frequently exposed to phototoxic plants, grocery worker
o Berloque dermatitis – primarily on neck and face
o Ingested herbal remedies may cause systemic photosensitivity
o Dermatitis bullosa striata pratensis (grass or meadow dermatitis) – streaks, bizarre configurations with
vesicles and bullae that heal with residual hyperpigmentation
o Tourists who rinse their hair with lime juice outdoors – streaky hyperpigmentation of the arms and back
o Differentiate blistering phytophotodermatitis from rhus dermatitis:
▪ Rhus dermatitis: vesicles and bullae not limited to sun-exposed areas, itching is the most
prominent symptom, lesions continue to occur for a week or more
▪ Phytophotodermatitis: reaction limited to sun-exposed sites, burning pain appears within 48
hours, marked hyperpigmentation
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
o Differentiate from child abuse: asymmetric, atypical shaped and streaking of lesions in
phytophotodermatitis
Causes:
• Generally, to elicit it, a considerably great amount of photosensitizing substance is necessary
• Phototoxic tar dermatitis – coal creosote, crude coal tar, or pitch
o These may also be airborne, hence no patient history of touching tar products
o May be found in cosmetics, drugs, dyes, insecticides, disinfectants
• Phytophotodermatitis – furocoumarins in plants
o Fragrance products with bergapten (component of oil of bergamot)
o Berloque dermatitis – due to 5-methoxypsoralen or other furocoumarin
o Phototoxic plants – Umbelliferae, Rutaceae (rue), Compositae, and Moraceae families
Treatment:
• Severe, acute reaction – similar to sunburn management
o Cool compress, mild analgesics (if needed), topical emollients
• Hyperpigmentation – topical steroids, strict sun avoidance immediately after injury, best managed by “tincture
of time”
Photosensitive Drug Reactions
Description:
• Medications may cause phototoxic, photoallergic, lichenoid reactions, accelerated photoaging,
photodistributed telangiectasias, pseudoporphyria
• In many cases, mechanism is unknown (may be due to formation of reactive oxygen specie HAHA)
• Phototoxic reactions:
o Reactions related to dose of both meds and UV irradiation
o Reactions can occur to anyone if sufficient thresholds are reached and do not require prior exposure or
participation by the immune system
o Higher skin types – lower risk of developing phototoxic eruptions
▪ Individual variation in the amount of photosensitivity created by a standard dose of
medication, independent of serum concentration
o Reactions can appear from hours to days after exposure
▪ Amiodarone, chlorpromazine – immediate burning with sun exposure
▪ Fluoroquinolones, chlorpromazine, amiodarone, thiazide diuretics, quinine, tetracyclines –
exaggerated sunburn
▪ Hyperpigmentation may complicate phototoxic reactions and may last for many months
• Photoallergic reactions:
o Typically eczematous and pruritic
o May first appear weeks to months after drug exposure
o Involve the immune system
o Generally not as dependent on drug dose as phototoxic reactions
• Photosensitivity reactions of drugs:
o Amiodarone (cumulative dose of 40 g and at least 4 months on therapy)
▪ Reduced minimal erythema dose (MED) to UVA but not UVB
▪ Stinging and burning may occur as soon as 30 minutes after sun exposure
▪ Gradually returns to normal between 12 and 24 months after stopping meds – because of long
half-life of amiodarone
▪ Less frequently, a dusky, blue-red erythema of the face and dorsa of the hands occurs
▪ Papular reactions sometimes seen – may be dose dependent
o NSAIDs (especially piroxicam) – frequently associated with photosensitivity
▪ Characteristic reaction – vesicular eruption of the dorsa of the hands, sometimes associated
with a dyshidrosiform pattern on the lateral aspects of the hands and fingers
▪ Palms involved in severe cases
▪ Patients may also react to thiosalicylic acid (common sensitizer in thimerosal)
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
o Sulfonamide antibiotics, related hypoglycemic agents, sulfonylurea diuretics
▪ Patient may tolerate one from this group, but when additional members of the group are
added, clinical photosensitivity occurs
▪ Typical pattern – erythema, scale
▪ Chronic cases – lichenification, hyperpigmentation
o Fluoroquinolones
▪ Sparfloxacin – highly photosensitizing
▪ Enoxacin, ciprofloxacin, sitafloxacin – mildly photosensitizing
▪ Levofloxacin – rarely photosensitizing
o Photodistributed lichenoid reactions – present as erythematous patches and plaques
▪ Most common – thiazide diuretics, quinidine, NSAIDs
▪ Also diltiazem, clopidogrel bisulfate
▪ Typical Wickham striae sometimes observed in lesions
▪ Marked hyperpigmentation may occur, especially in higher skin types (IV–VI) and diltiazem-
induced cases, which can persist for months
o UVA-associated phototoxicity – common with vemurafenib
o Photoleukomelanoderma (mosaic mix of hypopigmentation and hyperpigmentation after erythema in
sun-exposed areas) – flutamide
o Voriconazole – mild photosensitivity, facial erythema and chelitis, may resemble sunburn
▪ More severe reactions sometimes occur
o Photodistributed telangiectasia – rare complication of CCBs (nifedipine, felodipine, amlodipine),
cefotaxime
• Photosensitivity of both the phototoxic and the photoallergic type may persist for months to years after the
medication has been stopped
• Pseudoporphyria – photodistributed bullous reaction clinically and histologically resembling porphyria cutanea
tarda
o Blistering on sun-exposed skin of the face and hands, skin fragility
o Varioliform scarring occurs in 70%
▪ Facial scarring especially common in children
o Hypertrichosis rarely found, dyspigmentation and sclerodermoid changes are not reported
o Blistering usually resolves gradually after stopping meds, but skin fragility may persist
o Naproxen – most frequent cause, but it has been reported in other drugs (like OCPs) and other
conditions (ex. patient undergoing dialysis)
Causes:
• Most are triggered by radiation in the UVA range
o Most photosensitizing drugs have absorption spectra in the UVA and short-visible range
o UVA penetrates into the dermis where the photosensitizing drug is present
• Most common causes: NSAIDs, TMP-SMX, thiazide diuretics and related sulfonylureas, quinine and quinidine,
phenothiazines, certain tetracyclines
o NSAIDs, tetracyclines, amiodarones – common culprits
o Also azathioprine
• Less commonly prescribed meds – voriconazole, vemurafenib
• Newer agents – simeprevir, chemotherapeutic agents, flutamide
Treatment:
• Phototoxic reactions – dose reduction and sunblock
• For severe reactions – stop meds and switch to alternative drug
• Narrow-band UVB – may desensitize patients with persistent phototoxicity after stopping amiodarone
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
Urticaria/Angioedema/Dermatographism (★)
(book chapter too long – just read the trans on this and focus on appearance of lesions, associated s/s, causes (if
meron), differentials, and treatment)
Description:
• Wheal, severe itching or stinging
o Can have accompanying angioedema (swelling of soft tissue)
• Types of urticaria:
o Acute – within 6 weeks
o Chronic – >6 weeks
• Dermatographism – stroking the skin → instantaneous evanescent wheal or flare reaction coinciding to what
part was scratched
Causes:
• Drugs (commonly ACE-I and NSAIDs)
• Food (commonly chocolate, shellfish, nuts, peanuts, tomatoes, strawberries, melons, pork, cheese, garlic, onions,
eggs, milk, spices)
• Infections (URI and viral most common in children)
• Insect bites
• Chronic urticaria – >50% idiopathic, up to 35% caused by physical stimuli
Treatment:
• Mainstay of treatment: antihistamines – 2nd or 3rd generation, nonsedating (like cetirizine in standard dose)
o Symptoms persisting after 2 weeks – may increase dose up to 4x or switch antihistamine
o No response – consider oral steroids, cyclosporine, biologicals (omalizumab)
• Topical corticosteroids, topical antihistamines, topical anesthetic – no role
• Determine the cause of episodes of urticaria
• If with difficulty of breathing – consider anaphylaxis → mainstay of treatment is epinephrine
Exanthems (Morbilliform or Maculopapular Drug Eruption)
Description:
• Most common form of adverse cutaneous drug eruption
• Tend to occur within the first 2 weeks of treatment but may appear later, or even up to 10 days after meds have
been stopped
• Characterized by erythema and often small papules throughout
o Tend to first appear proximally (especially in the groin and axilla) then generalize within 1-2 days
o Face is typically spared – consider DRESS if with facial involvement
o Pruritus usually prominent – helps distinguish from viral exanthema or graft-versus-host disease
(GVHD)
o More severe ADRs – higher eosinophil counts
• DRESS: delayed type IVB hypersensitivity reaction thought to be mediated by antiviral T cells
o Facial involvement, facial edema, ear involvement, hand edema – uncommon in simple exanthems
• May be restricted to a previously sunburned site (“UV recall-like” phenomenon) – must be distinguished from
true UV recall caused by antimetabolites
Cause:
• Antibiotics (especially semisynthetic penicillins and TMP-SMX) – most common cause
Treatment:
• Simple exanthems – supportive
o Eruption clears within two weeks of stopping offending drug or may even clear while continuing meds
o Topical corticosteroids, antipruritics – may help completion of course of therapy
o Rechallenge usually results in the reappearance of the eruption (except in cases of HIV)
▪ More severe blistering reaction – infrequent in HIV patients, rare in immunocompetent
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
▪HIV patients with simple reactions to TMP-SMX - reexposure by slow introduction or full-dose
reexposure may be tolerated
• Complex exanthems – stop inciting agent immediately, rarely undertaken rechallenge
Erythema Multiforme (EM)
Description:
• Classification of EM:
o Herpes simplex–associated EM (HAEM)
o Erythema multiforme major
o Chronic oral EM
o Contact dermatitis–induced EM
o Radiation-induced EM
o Idiopathic
• Histologic features are similar in HAEM and EM major and are not predictive of etiology
o All lesions are characterized by cellular necrosis
o Vacuoles and foci of individual cell necrosis are present and out of proportion to the number of
lymphocytes
o Must be histologically distinguished from FDE, GVHD, pityriasis lichenoides, lupus
• Clinical features of HAEM:
o Recurrent, self-limited, usually affecting young adults, occurring seasonally in the spring and fall, each
episode lasting 1–4 weeks
o Sharply marginated, erythematous macules → Raised, edematous papules over 24–48 hours
o Lesions may reach several centimeters in diameter
o A ring of erythema typically forms around the periphery; centrally, lesions become flatter, more
purpuric, dusky – classic target/iris lesion with 3 zones (central dusky purpura that may be bullous,
elevated edematous pale ring, surrounding macular edema)
o Targets best observed on palms and soles, initial involvement frequently on dorsal hands
▪ Lesions generally appear symmetrically and acrally
▪ Dorsal feet, extensor limbs, elbows, knees, palms, and soles typically become involved
▪ Widespread lesions sometimes occur on the trunk
▪ Koebner phenomenon or photoaccentuation may be observed
▪ Mucosal involvement may occur, usually limited to oral mucosa – indurated plaques, target
lesions, or erosions
o Atypical variant in women
▪ Outbreaks of unilateral or segmental papules and plaques that may be few in number or
solitary
▪ May be up to 20 cm in diameter
▪ Plaques are erythematous and evolve to have a dusky center, which desquamates
▪ Subcutaneous nodules resembling erythema nodosum may be present
• Clinical features of EM major:
o Frequently accompanied by febrile prodrome, sometimes arthralgias
o Occurs in all ages, centered on extremities and face
o Truncal lesions (papular and erythematous to dusky in color) – occur more often vs EM minor
o Prominent mucous membrane disease – severely involves oral mucosa and lips with hemorrhagic
sloughing
o Genital and ocular mucosa less commonly involved
o Differentiate from SJS: purpura or bullae in macular lesions of the trunk in SJS
o Differentiate from urticaria multiforme in children: polycyclic urticarial lesions often become dusky
centrally in urticaria multiforme, but there are no histologic changes of EM
Differentials:
• Characteristic target lesions → diagnosis of EM is established clinically
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
• Bullae present → distinguish EM major from bullous arthropod reactions, autoimmune bullous diseases,
pemphigus (if with prominent mucous membrane involvement), bullous pemphigoid (if lesions are small,
prominent erythema at the periphery of the bulla)
• Paraneoplastic pemphigus – atypical target lesions, mucosal involvement, vacuolar interface dermatitis; may
appear similar to Mycoplasma-induced EM major
• Also consider SJS
Causes:
• Strongly associated with preceding orolabial HSV infection – typical EM minor
o HAEM lesions appear 1–3 weeks (average 10 days) after herpes outbreak
o Episodes of EM minor may not follow every episode of herpes
o Some EM outbreaks will not be preceded by a clinically recognizable herpetic lesion
o Look for HSV DNA and antigens in lesions of EM minor
• Mycoplasma – most often cause of EM major
• Drug reactions
Treatment/Prophylaxis:
• Depends on cause and extent
• Most cases of EM minor (HAEM) are self-limited – may only need symptomatic treatment
o Symptoms related to oral lesions – topical “swish and spit” mixtures containing lidocaine,
diphenhydramine (Benadryl), and kaolin
o Antihistamine for pruritus (★)
• If HSV infection is present – use concurrent antivirals
• Prevention of herpetic outbreaks is central to control of the subsequent episodes
o Sunscreen lotion, sunscreen-containing lip balm daily – prevent UVB-induced outbreaks of HSV
▪ If sunscreen does not prevent recurrence, if genital HSV – chronic suppressive doses of oral
antiviral drug (valacyclovir, 500 mg to 1 g/day, or famciclovir)
▪ Increase dose if still ineffective
o Intermittent systemic antivirals, topical antivirals – minimal prevention of HAEM
▪ Atypical HAEM – acyclovir suppression prevents lesions
o Also avoid sharing items that come in contact with the mouth (★)
• Extensive cases of EM minor:
o Intermittent steroids, chronic dapsone, cyclosporine, azathioprine, thalidomide – occasionally helpful
o Systemic corticosteroids (★)
o Recalcitrant cases – apremilast, rituximab
o Recurrent cases – may give antivirals (acyclovir, valcyclovir) (★)
• Widespread EM, unresponsive to therapies – management is as for severe drug-induced SJS
Oral EM
Description:
• Unique subset of EM that is limited to or most prominent in the oral cavity
o 45% oral cavity only, 30% oral and lip, 25% skin involvement
o All portions of oral cavity may be involved, but the tongue, gingiva, and buccal mucosa are usually
most severely affected
• Patients are clinically well otherwise, 60% female, mean age of 43 years
o Minority (~25%) – recurrent, self-limited, cyclic disease
• Lesions are almost universally eroded, with or without a pseudomembrane
Treatment:
• Typically same as that of EM minor
• Topical corticosteroids may be helpful (fluocinonide gel 0.05%)
• Symptomatic relief – “swish and spit” mixtures containing lidocaine, diphenhydramine, and kaolin
o Warn patient that anesthetic effect may dampen gag reflex
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
Exfoliative Dermatitis (Erythroderma/Wilson-Brocq, Dermatitis Exfoliativa, Pityriasis Rubra/Hebra)
Description:
• NOT a diagnosis but a clinical prototype that can result from various diseases
• Extensive erythema (entire body is dull scarlet) and scaling (small laminated scales that profusely exfoliate)
o Extensive telogen effluvium may be noted
o Itching may be severe
o PRP, mycosis fungoides – look for distinct spared islands of skin
o PRP – look for thickened orange palms, “nutmeg grater” follicular papules on the dorsa of the fingers
o Cutaneous T-cell lymphoma (CTCL) – look for palmoplantar keratoderma
• Onset often accompanied by symptoms of general toxicity (ex. fever, chills)
o High transepidermal water loss
o Secondary infections (Staphylococcal, streptococcal) complicate disease course in the absence of
treatment
• Severe complications: sepsis, high-output cardiac failure, acute respiratory distress syndrome, capillary leak
syndrome
Causes:
• Various diseases! Usually caused by exacerbation of pre-existing dermatosis
o Atopic dermatitis, psoriasis, pityriasis rubra pilaris (PRP)
• Medication reactions (especially for HIV+)
• Idiopathic
• CTCL – less common
o Mycosis fungoides – can be erythrodermic without meeting Sézary syndrome criteria
o Hodgkin disease – frequently accompanied by fever, lymphadenopathy, splenomegaly, hepatomegaly,
increased ESR
• Children (especially infants) – immunodeficiency, netherton syndrome, icthyosis, metabolic syndrome, infection,
atopic dermatitis (usually presents after neonatal period)
Treatment:
• Target primary cause
• Medium-strength corticosteroid after soaking and occlusion under sauna suit – helpful regardless of cause
• Psoriatic erythroderma – acitretin, cyclosporine, methotrexate
• PRP – isotretinoin, acitretin, methotrexate
• CTCL – avoid TNF-α agents (significantly worsens CTCL)
Leukocytoclastic Vasculitis (LCV) / Cutaneous Small-Vessel Vasculitis
Description:
• Most cases follow after acute infection or exposure to new meds
• Hallmark of LCV: palpable purpura + lesions ranging from pinpoint to several cm in diameter
o Lesions predominate on ankles and lower legs, affecting mainly dependent areas or areas under local
pressure
o Non-blanchable (★)
o Edema (especially ankles) is usually noted
o Annular, vesicular, bullous, or pustular lesions may develop
o Small ulcerations may develop, but suspect vasculitis of larger vessels or presence of vasculitis +
hypercoagulable state
o Constitutional s/s may occur: fever, malaise
o Mild pruritus, arthralgias (less often, frank arthritis) may be seen
o Other systemic involvement is rare, consider other dx BUT serious systemic disease can accompany LCV
and should be sought in every patient
• Hospitalized/bedridden patient: look at buttocks and posterior thighs (dependent areas)
• Lesions usually revolve in 3-4 weeks, with residual post-inflammatory hyperpigmentation
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
o 10% of cases recur and some are chronic – look for persistent underlying cause
• Pathogenesis: circulating immune complexes that activate complement and inflammatory cascade
o Biopsy to confirm diagnosis – skin punch biopsy (★)
• Important to determine if case is benign (due to infection or meds) or with serious underlying
disease/significant systemic involvement
o Get thorough past medical history, associated symptoms (especially for systemic s/s), drug intake, and
ROS
Causes:
• Idiopathic – majority of cases
• Drug-induced – look for tissue eosinophilia
o Virtually all classes of drugs may cause LCV and the time to manifestation widely varies
o Illicit substances may also be an etiologic agent
• Post-infectious
o Host of infectious agents (β-hemolytic Streptococcus group A, Mycoplasma, rarely Mycobacterium
tuberculosis) – palpable purpura
• Connective tissue disease – LCV can occur with association or be a presenting sign
• Lymphoproliferative neoplasms
• Solid tumors (lung, colon, genitourinary, breast)
o Recurrence of LCV – may mark return of treated malignancy
• Mixed small-vessel and medium-vessel vasculitis – LCV may be initial manifestation
Treatment:
• Initial treatment (clinically well, normal urinalysis) – symptom management, not aggressive
o Most cases are acute, self-limited, affect only the skin, and do not threaten progressive deterioration of
internal organs
o Rest, elevate the legs, avoid trauma and cold temperatures, give analgesics
o Identified antigens/drugs should be eliminated; identified infectious, connective tissue, or neoplastic
disease should be treated
• For severe, intractable, or recurrent disease (especially if with significant organ involvement):
o Limited to the skin – NSAIDs for arthralgias
o Chronic vasculitis – colchicine 0.6 mg 2-3x a day, dapsone 50-200 mg/day; combine low doses of both
if either are unsuccessful alone or if effective doses cannot be tolerated
o Oral antihistamines – blocks vasodilation induced by histamine, may reduce immune complex trapping,
improves LCV
o Serious systemic manifestations, necrotic lesions – systemic corticosteroids 60-80 mg/day
▪ Brief course usually leads to resolution, chronic treatment rarely required
▪ Not good long-term options for chronic LCV
o Chronic or refractory, colchicine or dapsone ineffective
▪ Immunosuppressive agents (MMF 2-3 g/day, methotrexate 5-25 mg/week, azathioprine 50-200
mg/day or 2-3.5 mg/kg/day)
▪ Rituximab
o More difficult cases – cyclophosphamide, monthly IV pulses of steroids/cyclophosphamides,
cyclosporine 3-5 mg/kg/day
o TNF blockers (especially infliximab, lesser degree etanercept) – may be effective but may also cause
vasculitis themselves
Steroid Purpura
Description:
• Prolonged use of corticosteroids → numerous skin changes, profound effect on many tissues’ metabolism →
predictable and preventable complications
o Even mild corticosteroids may cause this (★)
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
• Skin changes:
o Thin and fragile, easy spontaneous tearing, xerosis (generalized skin dryness)
o Increased blood vessel fragility, telangiectasia (★)
o Purpura and ecchymosis (especially over dorsal forearms of patients >50 years due to aggravation of
actinic purpura)
o Cushingoid changes – most common is altered fat distribution (buffalo hump, facial and neck fullness,
increased supraclavicular and suprasternal fat, gynecomastia, protuberant or pendulous abdomen,
flattening of the buttocks)
o Steroid-induced acne – small, firm monomorphic follicular papules on the forehead, cheeks, and chest
o Striae – may be widely distributed (especially abdomen, buttocks, thighs)
• Hair loss, thinning and brittle fracturing along hair shaft – long term course with large doses
o Increased hair growth in bearded areas, arms, back – fine, vellus hairs
• Systemic complications:
o Hypertension, peptic ulcer disease, diabetes, mood changes, cataracts, aseptic necrosis of the hip,
osteoporosis
o Bone loss can occur early in the course of steroid therapy
• Always consider: (★)
o Potency of steroid (clobetasol is super potent, hydrocortisone and betamethasone are mild)
o Vehicle of steroid
o Location
o Size
o Lesion
• Estimating topicals – fingertip unit (★)
Treatment/Prophylaxis:
• Taper and stop steroid use
• Cushingoid changes – aggressive dietary management with reduction in carbohydrate and caloric intake may
ameliorate changes
• Steroid-induced acne – stop corticosteroids, management similar to acne vulgaris (topical preparations, oral
antibiotics)
• Manage bone loss preemptively
o Courses >1 month – calcium and vitamin D supplementation (1.0–1.5 g calcium and 400– 800 U
cholecalciferol daily)
o Stop smoking and alcohol consumption
o Follow bone mineral density via DEXA scan and do fracture risk assessment
o Most cases warrant up-front treatment with bisphosphonates
o Hypogonadism contributes to osteoporosis – treat with testosterone (men) or estrogen (women)
• Consider proton pump inhibitor prophylaxis for patients on concurrent aspirin or NSAIDs
• Risk of infection – vaccinate (but PCP prophylaxis is controversial)
VHCC 3A-MED | ANDREW’S 13TH ED + LECTURE NOTES (★)
You might also like
- Sunburn (Suntan) & Insect Bites and StingsDocument5 pagesSunburn (Suntan) & Insect Bites and StingsJaz MnNo ratings yet
- Sunburn Treatment & Care GuideDocument3 pagesSunburn Treatment & Care GuideCameron YoungNo ratings yet
- Uv Presentaion 2019Document43 pagesUv Presentaion 2019Mustafa MabroukNo ratings yet
- Himalaya Sunscreen LotionDocument78 pagesHimalaya Sunscreen Lotionshantanusen100% (1)
- Ultraviolet Radiaton: Made Hendra Satria Nugraha, S.FT., M.FisDocument30 pagesUltraviolet Radiaton: Made Hendra Satria Nugraha, S.FT., M.FisDw Ipha Ma HaNo ratings yet
- Sunscreens: Understanding the Benefits and HarmsDocument43 pagesSunscreens: Understanding the Benefits and Harmskiki ikrimaNo ratings yet
- Bacterial Skin InfectionDocument4 pagesBacterial Skin InfectionAngeline TaghapNo ratings yet
- Photodermatologic Disorders (Photodermatoses) : Mikias Woldetensay Dermatology & Venereology Oct 2021Document59 pagesPhotodermatologic Disorders (Photodermatoses) : Mikias Woldetensay Dermatology & Venereology Oct 2021CHALIE MEQUNo ratings yet
- Burns FrostbitesDocument2 pagesBurns FrostbitesMaksims МаrkovsNo ratings yet
- Prezentare TEN EnglezaDocument27 pagesPrezentare TEN EnglezaAlinaNo ratings yet
- Burn Injury ReviewerDocument7 pagesBurn Injury ReviewerBERKELEY MACKENZEN AZAULANo ratings yet
- ToddlerDocument15 pagesToddlerCARL JOHN MANALONo ratings yet
- Efloresensi Polimorfik Dan Kelainan Pigmentasi: Dr. Dr. Linda J Wijayadi SP - KK FINSDVDocument50 pagesEfloresensi Polimorfik Dan Kelainan Pigmentasi: Dr. Dr. Linda J Wijayadi SP - KK FINSDVFarahditya PutriNo ratings yet
- DermatologyDocument18 pagesDermatologymodhawialdNo ratings yet
- Psoriasis: Causes, Symptoms and TreatmentDocument24 pagesPsoriasis: Causes, Symptoms and TreatmentpravinNo ratings yet
- 07 DermatologyDocument93 pages07 Dermatologyreuel nareshNo ratings yet
- Integumentary SystemDocument4 pagesIntegumentary SystemArnie Jean SalazarNo ratings yet
- Common Skin Diseases: Tutorial - 6GDocument33 pagesCommon Skin Diseases: Tutorial - 6GChro MANo ratings yet
- Acne - Rosacea - 2Document31 pagesAcne - Rosacea - 2Umut YücelNo ratings yet
- PhotodermatosisDocument79 pagesPhotodermatosisRaziHashmiNo ratings yet
- General Considerations For Topical PreparationsDocument6 pagesGeneral Considerations For Topical PreparationsOccamsRazorNo ratings yet
- NSG125: Care of Clients with Contact DermatitisDocument1 pageNSG125: Care of Clients with Contact DermatitisJoe Aire SalvediaNo ratings yet
- Types of Drug RashesDocument7 pagesTypes of Drug RashesJessica VillanuevaNo ratings yet
- Outline: Common Dermatologic Disorders: Tips For Diagnosis and ManagementDocument41 pagesOutline: Common Dermatologic Disorders: Tips For Diagnosis and ManagementJobelle Fernandez-SantosNo ratings yet
- Lichen planus, oral candidiasis, leukoplakia comparedDocument10 pagesLichen planus, oral candidiasis, leukoplakia comparedTirtha TaposhNo ratings yet
- Reporters: Linan, Maiden Gay Dimpas, AprilgeanDocument30 pagesReporters: Linan, Maiden Gay Dimpas, AprilgeanNalzaro EmyrilNo ratings yet
- Derma DR HanadiDocument37 pagesDerma DR HanadiHassan Musadaq HamzahNo ratings yet
- Derm 1 1 19,2024Document158 pagesDerm 1 1 19,2024husseinkheiralhamidNo ratings yet
- MBBS - COMPLETE - Anesthesiology-ReviewDocument200 pagesMBBS - COMPLETE - Anesthesiology-ReviewShanygne Krystal SwannNo ratings yet
- Evaluation and Management of Sunburn: Roshni PR, Remya Reghu, Meenu Vijayan and Parvati KrishnanDocument4 pagesEvaluation and Management of Sunburn: Roshni PR, Remya Reghu, Meenu Vijayan and Parvati KrishnanMasri RaisNo ratings yet
- OTC Dermatological Products: 1. Dermatitis 2. Sunburn SuntanDocument30 pagesOTC Dermatological Products: 1. Dermatitis 2. Sunburn SuntanEman AlshaikhNo ratings yet
- Natural PhototherapyDocument77 pagesNatural PhototherapyLeo FluxNo ratings yet
- Equine SkinDocument17 pagesEquine Skinmohamed gomaaNo ratings yet
- Burn Injury M3Document71 pagesBurn Injury M3CechanNo ratings yet
- Tetracycline Antibiotics GuideDocument9 pagesTetracycline Antibiotics Guideedle maeNo ratings yet
- Infrared Therapy BenefitsDocument14 pagesInfrared Therapy Benefitsvenkata ramakrishnaiah100% (1)
- Study Guide Ch.11Document7 pagesStudy Guide Ch.11Draquillany ShieldsNo ratings yet
- PDP 406 CLINICAL TOXICOLOGY PESTICIDESDocument63 pagesPDP 406 CLINICAL TOXICOLOGY PESTICIDESMehboob AlamNo ratings yet
- Thera Merged 09-02-21Document104 pagesThera Merged 09-02-21Thea RayNo ratings yet
- Lecture 4 Dermatology: DR Khaled SobhyDocument88 pagesLecture 4 Dermatology: DR Khaled SobhyHemkerovner Keresztszegh von Kolowrat-KrakowskyNo ratings yet
- Insects, Stings and BitesDocument5 pagesInsects, Stings and BitesDian ariefNo ratings yet
- Sun Protection in Acne, Dr. Dwi Retno Adi WinarniDocument29 pagesSun Protection in Acne, Dr. Dwi Retno Adi WinarniAdi Sutriwanto PasaribuNo ratings yet
- Skin Disease: Roshana MallawaarachchiDocument51 pagesSkin Disease: Roshana MallawaarachchiRoshana Mallawaarachchi100% (1)
- Essential Travel Medical Kit GuideDocument3 pagesEssential Travel Medical Kit GuidedeeyungcocoNo ratings yet
- Erupsi Obat PDFDocument15 pagesErupsi Obat PDFAnonymous XGkoxkkUNo ratings yet
- 3-Infrared RadiationDocument14 pages3-Infrared RadiationkimNo ratings yet
- Burns Classification and Treatment GuideDocument8 pagesBurns Classification and Treatment GuideLuvleen KaurNo ratings yet
- Dr. Ariyati Yosi, SP - KK (K), M.Ked. (KK), FINSDV, FAADVDocument34 pagesDr. Ariyati Yosi, SP - KK (K), M.Ked. (KK), FINSDV, FAADVM. Ilham MaulanaNo ratings yet
- EmuHeal Cream PresentationDocument17 pagesEmuHeal Cream PresentationRahma MejriNo ratings yet
- Sports Med BrochureDocument1 pageSports Med Brochureapi-434212093No ratings yet
- GENERAL SANTOS DOCTORS’ MEDICAL SCHOOL FOUNDATION NURSING CARE PLANDocument4 pagesGENERAL SANTOS DOCTORS’ MEDICAL SCHOOL FOUNDATION NURSING CARE PLANFran LanNo ratings yet
- Cold & Decrease Pain For Circulation - WarmDocument3 pagesCold & Decrease Pain For Circulation - Warmmyer pasandalanNo ratings yet
- Insect Bites StingsDocument1 pageInsect Bites StingsnamibadiNo ratings yet
- PsoriasisDocument18 pagesPsoriasisDR MOHAMED HEALTH CHANNELNo ratings yet
- PPP-BURNS 118slDocument30 pagesPPP-BURNS 118slCath BrilNo ratings yet
- Referat Bedah Plastik RosDocument43 pagesReferat Bedah Plastik RosRisna AnnisaNo ratings yet
- PsoriasisDocument27 pagesPsoriasisNikkaDablioNo ratings yet
- Dermatology Notes for Medical StudentsFrom EverandDermatology Notes for Medical StudentsRating: 4 out of 5 stars4/5 (5)
- First Aid on the Farm: Natural and Conventional TreatmentsFrom EverandFirst Aid on the Farm: Natural and Conventional TreatmentsNo ratings yet
- Tinea Versicolor, (White Spots) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandTinea Versicolor, (White Spots) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Preoperative Evaluation and PreparationDocument7 pagesPreoperative Evaluation and PreparationJolaine ValloNo ratings yet
- February 2024 NewsletterDocument1 pageFebruary 2024 NewsletterJolaine ValloNo ratings yet
- Pathoma RuntimesDocument6 pagesPathoma RuntimesaloverofdanceNo ratings yet
- PhysicianDocument204 pagesPhysicianTrisNo ratings yet
- (ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareDocument8 pages(ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareJolaine ValloNo ratings yet
- CL Psychiatry Case Vignettes, 2022: July 1Document2 pagesCL Psychiatry Case Vignettes, 2022: July 1Jolaine ValloNo ratings yet
- (GYN) 05 Pelvic PainDocument5 pages(GYN) 05 Pelvic PainJolaine ValloNo ratings yet
- (ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Document12 pages(ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Jolaine ValloNo ratings yet
- Structure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaDocument9 pagesStructure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaJolaine ValloNo ratings yet
- (DERMA) 01 Introduction To Dermatology (History and PE)Document8 pages(DERMA) 01 Introduction To Dermatology (History and PE)Jolaine ValloNo ratings yet
- Effect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialDocument15 pagesEffect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialJolaine ValloNo ratings yet
- Effects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialDocument15 pagesEffects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialJolaine ValloNo ratings yet
- RhythmsDocument59 pagesRhythmsJolaine ValloNo ratings yet
- Student Guide Clerkship Revised AY2021-2022 Sept - OctDocument12 pagesStudent Guide Clerkship Revised AY2021-2022 Sept - OctJolaine ValloNo ratings yet
- Advocacy Proposal - Group 3-3Document6 pagesAdvocacy Proposal - Group 3-3Jolaine ValloNo ratings yet
- (DERMA) 06 Asymptomatic Skin Colored PapulesDocument12 pages(DERMA) 06 Asymptomatic Skin Colored PapulesJolaine ValloNo ratings yet
- (DERMA) 03 TineasDocument9 pages(DERMA) 03 TineasJolaine ValloNo ratings yet
- Data Management MCCODDocument48 pagesData Management MCCODJolaine ValloNo ratings yet
- Derma Quiz 5 NotesDocument6 pagesDerma Quiz 5 NotesJolaine ValloNo ratings yet
- Rheuma Prestests CompiledDocument13 pagesRheuma Prestests CompiledJolaine ValloNo ratings yet
- Med-Rheuma-Patient Write Up - Valeriano and ValloDocument10 pagesMed-Rheuma-Patient Write Up - Valeriano and ValloJolaine ValloNo ratings yet
- Pgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Document2 pagesPgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Jolaine ValloNo ratings yet
- Hema Pretests CompiledDocument6 pagesHema Pretests CompiledJolaine ValloNo ratings yet
- Onco Pretests CompiledDocument6 pagesOnco Pretests CompiledJolaine ValloNo ratings yet
- 12 Clin Path Exocrine and Endocrine Functions of The PancreasDocument13 pages12 Clin Path Exocrine and Endocrine Functions of The PancreasJolaine ValloNo ratings yet
- Data Management 'Birth Certificate'Document22 pagesData Management 'Birth Certificate'Jolaine Vallo100% (1)
- Gi Pretests CompiledDocument7 pagesGi Pretests CompiledJolaine ValloNo ratings yet
- D2 Grp1 CLIN PATH Case Discussion 1Document11 pagesD2 Grp1 CLIN PATH Case Discussion 1Jolaine ValloNo ratings yet
- 03 C2022 ClinPath 1.03 Hemostasis and ThrombosisDocument7 pages03 C2022 ClinPath 1.03 Hemostasis and ThrombosisJolaine ValloNo ratings yet
- 01 CLIN PTH S01 T01 Red Blood Cell DisordersDocument8 pages01 CLIN PTH S01 T01 Red Blood Cell DisordersJolaine ValloNo ratings yet
- EMS Burn Management PDFDocument30 pagesEMS Burn Management PDFRaymond Sitanaja0% (1)
- 2015-Hsc-Biology 15Document44 pages2015-Hsc-Biology 15Will NguyenNo ratings yet
- Structural Organisation in AnimalsDocument49 pagesStructural Organisation in AnimalsPukazhvanthen Paramanandhan100% (1)
- Fingerprint Laboratory Equipment 1. Ink RollerDocument8 pagesFingerprint Laboratory Equipment 1. Ink RollerMay Conde AguilarNo ratings yet
- Karring 1975Document12 pagesKarring 1975Juan Pablo FloresNo ratings yet
- Chapter 1 The World Through Our SensesDocument18 pagesChapter 1 The World Through Our SensesMichelle LambertNo ratings yet
- DermatosesDocument12 pagesDermatosesnjoom100% (1)
- THE Anatomic and Physiologic Difference Between Child and AdultDocument15 pagesTHE Anatomic and Physiologic Difference Between Child and AdultSanthosh.S.U75% (4)
- Tes Psikotes BUMN - 9 - Bahasa InggrisDocument17 pagesTes Psikotes BUMN - 9 - Bahasa InggrisPrsty 12No ratings yet
- Uses of Clobetasol Cream, Gel, and OintmentDocument15 pagesUses of Clobetasol Cream, Gel, and OintmentIntsik LimNo ratings yet
- Quiz Integumentary SystemDocument23 pagesQuiz Integumentary SystemLemuel CunananNo ratings yet
- Case Report Tinea Corporis - Salsabilla Sahara - 22004101052Document25 pagesCase Report Tinea Corporis - Salsabilla Sahara - 22004101052Salsabilla SaharaNo ratings yet
- Burns 3Document31 pagesBurns 3Reann LeeNo ratings yet
- Subject Link 5 WB KeysDocument18 pagesSubject Link 5 WB Keyssolsol0125No ratings yet
- 4HB0 01 Que 20180110 PDFDocument28 pages4HB0 01 Que 20180110 PDFCrustNo ratings yet
- Lesson 3-Adaptations in Animals KeywordsDocument3 pagesLesson 3-Adaptations in Animals KeywordsKristin Denis CorveraNo ratings yet
- Manual Cavitadora Kim 8 EnglishDocument7 pagesManual Cavitadora Kim 8 EnglishEngelbert GuzmánNo ratings yet
- Frogdissectionpre LabzachDocument2 pagesFrogdissectionpre Labzachapi-347431785No ratings yet
- NCP Impaired Tissue IntegrityDocument4 pagesNCP Impaired Tissue IntegrityKingJayson Pacman06No ratings yet
- Types of Skin LesionsDocument5 pagesTypes of Skin LesionsZielledee100% (2)
- Physical Changes in The Integumentary System As The Person AgesDocument10 pagesPhysical Changes in The Integumentary System As The Person AgesDinarkram Rabreca EculNo ratings yet
- Inputan GCB NOV (Jawaban) - 1Document5 pagesInputan GCB NOV (Jawaban) - 1imyour109No ratings yet
- (Terbaru) PRICELIST ZIA FULL AGEN DAN DISTRIBUTORDocument2 pages(Terbaru) PRICELIST ZIA FULL AGEN DAN DISTRIBUTORaaaaNo ratings yet
- Naturally Beautiful Skin & Hair Care ProductsDocument6 pagesNaturally Beautiful Skin & Hair Care ProductsWuppuluri Jayanth Kumar SharmaNo ratings yet
- Nora Bode Kosmetik & OxyjetDocument4 pagesNora Bode Kosmetik & OxyjetĐông PhùngNo ratings yet
- Eritroderma - Bolognia 4th EditionDocument15 pagesEritroderma - Bolognia 4th EditionAisyahNo ratings yet
- Dermatology An Illustrated Colour TextboDocument139 pagesDermatology An Illustrated Colour TextboHüseyin GündüzNo ratings yet
- KMU Foundation ModuleDocument20 pagesKMU Foundation ModuleShafiq Ur RahmanNo ratings yet
- AIRENA TAMPOS - (Article) Gene Therapy For The "Butterfly Children" 2.4Document3 pagesAIRENA TAMPOS - (Article) Gene Therapy For The "Butterfly Children" 2.4AIRENA RAIN TAMPOSNo ratings yet
- Price List Mei 2023Document3 pagesPrice List Mei 2023danny raufNo ratings yet