Professional Documents
Culture Documents
Pneumonia - Home Treatment: Call911or Other Emergency Services Immediately If You
Uploaded by
Ianne RanchezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pneumonia - Home Treatment: Call911or Other Emergency Services Immediately If You
Uploaded by
Ianne RanchezCopyright:
Available Formats
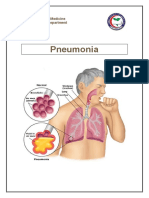
Pneumonia - Home Treatment
Home treatment is important for recovery from pneumonia. The following measures can help you recover
and avoid complications, such as further infection or a buildup of fluid in the space between thelung and
chest wall (pleural effusion ).
While you are at home:
Get plenty of rest and prevent dehydration by drinking plenty of fluids.
Take care of your cough if it is making it difficult for you to rest. A cough is one way your body
gets rid of the infection. And you should not try to stop your coughing unless it is severe enough to make
breathing difficult, cause vomiting, or prevent rest.
Consider taking acetaminophen (such as Tylenol) or aspirin to help reduce fever and make you
feel more comfortable. Do not give aspirin to anyone younger than 20 because of the risk of Reye
syndrome.
Do not give cough and cold medicines to a child younger than 2 unless your child’s doctor has told you to.
If your child’s doctor tells you to give a medicine, be sure to follow what he or she tells you to do.
Always check whether any over-the-counter cough or cold medicines you are taking
contain acetaminophen. If they do, make sure the acetaminophen you are taking in your cold medicine,
plus any other acetaminophen you may be taking, is not higher than the daily recommended dose. Ask
your doctor or pharmacist how much you can take every day.
Your doctor may want to see you after a week of treatment to make sure you are getting better. Be sure
to contact your doctor if you do not feel better, your cough gets worse, you have shortness of breath or a
fever, you feel weak, or you feel faint when you stand up.
Pneumonia - When To Call a Doctor
The faster you get treatment, the faster you will get over pneumonia. This is especially true for the very
young, for people older than 65, and for anyone with other long-lasting (chronic) health problems, such
as asthma.
Call911or other emergency services immediately if you:
Have chest pain that is crushing or squeezing, is increasing in intensity, or occurs with any
other symptoms of a heart attack.
Have such bad trouble breathing that you are worried you will not have the strength or ability to
keep breathing.
Cough up large amounts of blood.
Feel that you may faint when you sit up or stand.
Call a doctor immediately if you have:
A cough that produces blood-tinged or rust-colored mucus from the lungs.
A fever with shaking chills.
Difficult, shallow, fast breathing with shortness of breath or wheezing.
Call a doctor if your cough:
Frequently brings up yellow or green mucus from the lungs and lasts longer than 2 days. Do not
confuse mucus from your lungs with mucus running down the back of your throat from your nasal
passages (postnasal drip). Postnasal drainage is not a worry.
Occurs with a fever of 101F or higher and brings up yellow or green mucus from the lungs (not
postnasal drainage).
Causes you to vomit a lot.
Continues longer than 4 weeks.
Also call your doctor if you have new chest pain (more than just discomfort when you cough) that gets
worse with deep breathing and if you have other symptoms of pneumonia, such as shortness of breath,
cough, and fever.
Watchful Waiting
Watchful waiting is a wait-and-see approach. If you get better on your own, you won't need treatment. If
you get worse, you and your doctor will decide what to do next.
Home treatment may be appropriate if:
You have classic cold symptoms (nasal stuffiness, mild body aches orheadache, mild fever).
You cough up mucus that is caused by mucus running down the back of the throat from the nasal
passages (postnasal drip). But a cough in which the mucus is definitely coming from the lungs rather than
the nasal passages is a more serious problem, and you should contact your doctor.
You have signs of flu (high fever, severe muscle aches or headache, and mild respiratory
symptoms). For more information, see the topic Influenza.
Who To See
Health professionals who can diagnose and treat pneumonia include:
Family medicine physicians.
Pediatricians.
Internists.
Physician assistants.
Nurse practitioners.
Specialists in lung diseases (pulmonologists).
To prepare for your appointment, see the topic Making the Most of Your Appointment.
Pneumonia - Exams and Tests
Your doctor will usually diagnose pneumonia by using your medical history, a physical exam, and a chest
X-ray. Based on the medical history and physical exam, your doctor may start your treatment right away
without doing other tests. The need for more tests often depends on how severe your symptoms are, your
age, and your overall health. In general, the sicker you are, the more tests you will have. This is especially
true for older adults and infants.
A chest X-ray is almost always done to check for changes in the lungs that may mean pneumonia and to
look for other causes of your symptoms. But an X-ray does not always show whether you have
pneumonia, especially if the X-ray is done when you first get sick.
In some cases, the X-ray results may:
Suggest the type of organism (bacterial, viral, or fungal) causing pneumonia.
Show complications of pneumonia.
Show conditions that may occur with pneumonia, such as fluid in the chest cavity or a collapsed
lung.
Reveal another condition, such as heart failure, lung cancer, or acute bronchitis.
If you are very ill, have severe shortness of breath, or have a condition that increases your risk (such
as asthma or chronic obstructive pulmonary disease), your doctor may examine your mucus.
In a Gram stain, you cough up a sample of mucus (sputum) that is then treated with a special dye
(Gram stain) and looked at under a microscope. This test may show what type of organism (bacterium or
fungus) is causing the pneumonia. This test can help your doctor choose the best treatment for your
infection.
In a sputum culture and sensitivity, a sample of mucus is placed in a container with substances
that will make bacteria or fungi grow. If bacteria or fungi grow, your doctor can identify them and choose
the correct treatment. Unfortunately, getting lung mucus that has not been contaminated with throat or
mouth mucus is difficult. So, the results are not always helpful in identifying the cause of pneumonia. This
test may be less useful if you have already started using antibiotics.
If you have severe pneumonia, you may need other tests, including tests to check for complications and
to find out how well your immune system is working.
A urine test is available that may identify within 15 minutes whether you are infected
with Streptococcus pneumoniae, one of the main causes of bacterial pneumonia, orLegionella
pneumophila, the bacterium that causes Legionnaires' disease and sometimes can cause pneumonia.
Although experts consider the test to be useful for the identification of Legionella pneumophila, doctors
generally do not use it to identify Streptococcus pneumoniae.4 But it may be useful in adults with severe
pneumonia and when a Gram stain has not identified the bacteria. 5
In people with impaired immune systems, pneumonia may be caused by other organisms, including some
forms of fungi, such as Pneumocystis jiroveci (formally called Pneumocystis carinii). This fungus often
causes pneumonia in people who have AIDS. Some doctors may suggest an HIV test if they think
that Pneumocystis jiroveci is causing the pneumonia.
You might also like
- Anestesi RecordDocument1 pageAnestesi RecordWelmi Sulfatri IshakNo ratings yet
- Acute Bronchitis - FinalDocument28 pagesAcute Bronchitis - FinalJied100% (6)
- NBHS1112 Biochemistry/ Biokimia May Semester 2022Document16 pagesNBHS1112 Biochemistry/ Biokimia May Semester 2022amu tha100% (1)
- Mbbs Freshers ResumeDocument9 pagesMbbs Freshers ResumeTalha Noorani50% (2)
- Walking Pneumonia HealthDocument4 pagesWalking Pneumonia HealthneljohnaciboNo ratings yet
- What is a cough? Causes, symptoms, diagnosis and treatmentDocument4 pagesWhat is a cough? Causes, symptoms, diagnosis and treatmentSheharyar SandhuNo ratings yet
- CoughDocument4 pagesCoughBimal MandalNo ratings yet
- Understanding Cough Causes and Home RemediesDocument5 pagesUnderstanding Cough Causes and Home RemediesVanessa Rose NoelNo ratings yet
- Pneumonia Is A Condition That Causes The Lungs To Become Inflamed As A Result of A BacterialDocument3 pagesPneumonia Is A Condition That Causes The Lungs To Become Inflamed As A Result of A BacterialDhonnalyn Amene CaballeroNo ratings yet
- Kaushal - Pneumonia DiseaseDocument10 pagesKaushal - Pneumonia DiseaseKaushal PatelNo ratings yet
- ÷neumonia: Causes, Incidence, and Risk FactorsDocument6 pages÷neumonia: Causes, Incidence, and Risk FactorsShyra Jane DolosoNo ratings yet
- Everything You Need to Know About CoughsDocument12 pagesEverything You Need to Know About CoughsLany T. CataminNo ratings yet
- Pneumonia Symptoms Diagnosis TestsDocument5 pagesPneumonia Symptoms Diagnosis TestsPhạm HảoNo ratings yet
- Symptoms of PneumoniaDocument4 pagesSymptoms of PneumoniaAndeariesa DarmansiusNo ratings yet
- Pneumonia: Submitted To:Ms Lisette Cruz Submitted By: Ms. Mely Rose AbanadorDocument26 pagesPneumonia: Submitted To:Ms Lisette Cruz Submitted By: Ms. Mely Rose AbanadorJoyce Catherine Buquing UysecoNo ratings yet
- Pneumonia Symptoms, Causes, Diagnosis and Treatment ExplainedDocument3 pagesPneumonia Symptoms, Causes, Diagnosis and Treatment ExplainedDara Loor GonzálesNo ratings yet
- Community Acquired PneumoniaDocument5 pagesCommunity Acquired PneumoniaLau ColastreNo ratings yet
- PneumoniaDocument3 pagesPneumoniaAubrey Unique EvangelistaNo ratings yet
- ASTHMA333Document6 pagesASTHMA333June DumdumayaNo ratings yet
- Pneumonia Lung CoughDocument7 pagesPneumonia Lung Coughserai maramaNo ratings yet
- BronchitisDocument6 pagesBronchitisNader Smadi100% (1)
- FL15 Pneumonia 2016 v4 PDFdownloadDocument5 pagesFL15 Pneumonia 2016 v4 PDFdownloadvivek yadavNo ratings yet
- Chronic Bronchitis GuideDocument5 pagesChronic Bronchitis GuideJemalyn M. Saludar100% (2)
- Tolleno (Pneumonia ER)Document4 pagesTolleno (Pneumonia ER)Hannah TollenoNo ratings yet
- Microsoft Word - Pneumonia Education EnglishDocument9 pagesMicrosoft Word - Pneumonia Education Englishjustin_saneNo ratings yet
- Topic 1: PneumoniaDocument45 pagesTopic 1: PneumoniaNektarios TsakalosNo ratings yet
- What Is A CoughDocument6 pagesWhat Is A CoughIRMA GUSTIANANo ratings yet
- Bronchopneumonia - MedscapeDocument7 pagesBronchopneumonia - MedscapecleoaerNo ratings yet
- Chronic Cough:: Talking To Your DoctorDocument2 pagesChronic Cough:: Talking To Your DoctorPrem Kumar YadavalliNo ratings yet
- Explaining Disease (Part 2)Document18 pagesExplaining Disease (Part 2)Eva Nia SeptikaNo ratings yet
- How to Treat Flu Symptoms at HomeDocument15 pagesHow to Treat Flu Symptoms at HomeJosé Luis Sugasti HidalgoNo ratings yet
- Disease Monograph: CausesDocument4 pagesDisease Monograph: CausesRawan AlmutairiNo ratings yet
- Influenza Common Colds OutputDocument8 pagesInfluenza Common Colds OutputmalindaNo ratings yet
- Broncho PneumoniaDocument9 pagesBroncho Pneumoniamunie munieNo ratings yet
- Signs and Symptoms: MicroorganismsDocument4 pagesSigns and Symptoms: MicroorganismsNikki P. NarteNo ratings yet
- Adults Community Acquired PneumoniaDocument7 pagesAdults Community Acquired PneumoniaDEth JU NafenNo ratings yet
- Bronchitis: Causes, Symptoms, TreatmentDocument3 pagesBronchitis: Causes, Symptoms, Treatmentjosanne938No ratings yet
- PNEUMONIADocument3 pagesPNEUMONIAAssasination ClassroomNo ratings yet
- Acute BronchitisDocument2 pagesAcute BronchitisChristabella Natalia WijayaNo ratings yet
- Pneumonia Essay FinalDocument7 pagesPneumonia Essay Finalkhaled khalifaNo ratings yet
- What Is Acute BronchitisDocument11 pagesWhat Is Acute BronchitisKerri-DojhnHallNo ratings yet
- Child asthma discharge care guideDocument15 pagesChild asthma discharge care guideJu Lie AnnNo ratings yet
- PneumoniaDocument1 pagePneumoniaG AlionaNo ratings yet
- Nasarullahkhan Mazari 70-Phae-2k17Document8 pagesNasarullahkhan Mazari 70-Phae-2k17Kashif BalochNo ratings yet
- What Is AsthmaDocument5 pagesWhat Is AsthmajayrizNo ratings yet
- What is Asthma - A 40-Character GuideDocument5 pagesWhat is Asthma - A 40-Character GuidejayrizNo ratings yet
- OverviewDocument3 pagesOverviewIssa AvenaNo ratings yet
- Your-family-health-historyDocument9 pagesYour-family-health-history308501No ratings yet
- BronchiolitisDocument7 pagesBronchiolitisNader SmadiNo ratings yet
- AshmaDocument9 pagesAshmaAkarsh RamNo ratings yet
- Pneumonia - Topic OverviewDocument2 pagesPneumonia - Topic OverviewDesinta AnarisantiNo ratings yet
- TCP PneumoniaDocument6 pagesTCP PneumoniaAnonymous FgT04krgymNo ratings yet
- Case Study Bronchial-AsthmaDocument9 pagesCase Study Bronchial-AsthmaGabbii CincoNo ratings yet
- Makalah B.ingggggggggggggggggggggggggDocument29 pagesMakalah B.ingggggggggggggggggggggggggmegaNo ratings yet
- Symptoms of Bronchopneumonia in Adults and Children: PneumoniaDocument10 pagesSymptoms of Bronchopneumonia in Adults and Children: PneumoniajessyNo ratings yet
- Asthma: Nurse AvenueDocument13 pagesAsthma: Nurse AvenueWindi Lameck MarwaNo ratings yet
- Aspiration Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAspiration Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Pneumonia - Topic OverviewDocument1 pagePneumonia - Topic OverviewsexiiimammaNo ratings yet
- Pneumonia CareDocument8 pagesPneumonia Carepeach landNo ratings yet
- Pneumonia - Marzo, Cecille Joyce D. (BSN4A-1)Document24 pagesPneumonia - Marzo, Cecille Joyce D. (BSN4A-1)Marzo, Cecille JoyceNo ratings yet
- Obcl-2-Cu - Week 3 BronchitisDocument9 pagesObcl-2-Cu - Week 3 BronchitisMichelle Gliselle Guinto MallareNo ratings yet
- TonsillitisDocument21 pagesTonsillitisKavy AkhsanulNo ratings yet
- Epiglottitis: Causes, Incidence, and Risk FactorsDocument5 pagesEpiglottitis: Causes, Incidence, and Risk FactorscnvNo ratings yet
- Intervention AutismDocument2 pagesIntervention AutismIanne RanchezNo ratings yet
- Pa Tho Physiology of AnemiaDocument1 pagePa Tho Physiology of AnemiaRasper PascualNo ratings yet
- AnatomyDocument2 pagesAnatomyIanne RanchezNo ratings yet
- ADHD Psycho PathologyDocument2 pagesADHD Psycho PathologyIanne RanchezNo ratings yet
- Heart Anatomy and PhysiologyDocument6 pagesHeart Anatomy and PhysiologyIanne RanchezNo ratings yet
- Anatomy and Physiology GuideDocument4 pagesAnatomy and Physiology GuideIanne RanchezNo ratings yet
- Music and Art TherapyDocument6 pagesMusic and Art TherapyIanne Ranchez100% (1)
- Heart Anatomy and PhysiologyDocument6 pagesHeart Anatomy and PhysiologyIanne RanchezNo ratings yet
- InjectableDocument26 pagesInjectableAan KurniawanNo ratings yet
- Hemorrhagic ShockDocument2 pagesHemorrhagic ShockPharhana PuterieNo ratings yet
- Dissertation TopicsDocument54 pagesDissertation TopicsApollo Institute of Hospital Administration50% (4)
- Abdominal PainDocument26 pagesAbdominal Painsammy_d6No ratings yet
- Medicalization of BeautyDocument10 pagesMedicalization of BeautyhalohaiNo ratings yet
- Related Literary RiviewDocument6 pagesRelated Literary RiviewVal Gillian BranzuelaNo ratings yet
- Finding the Right Pharmacy for Your NeedsDocument4 pagesFinding the Right Pharmacy for Your Needsprabakar VNo ratings yet
- 2023 - Pitfalls in Scalp EEG - Current Obstacles and Future Directions - SandorDocument21 pages2023 - Pitfalls in Scalp EEG - Current Obstacles and Future Directions - SandorJose Carlos Licea BlancoNo ratings yet
- RepetMat U11 Test Rozsz ADocument2 pagesRepetMat U11 Test Rozsz Askrzyneckamaja6No ratings yet
- History and Mental Status Exam GuideDocument17 pagesHistory and Mental Status Exam Guideyeney armenterosNo ratings yet
- Jurnal Hipertiroid KehamilanDocument5 pagesJurnal Hipertiroid KehamilanAbdurrohman IzzuddinNo ratings yet
- Case Presentation 3 DR Oscar Laryngitis TBDocument33 pagesCase Presentation 3 DR Oscar Laryngitis TBmarajuu50% (2)
- Neuro ImagingDocument41 pagesNeuro ImagingRuchiyyihNo ratings yet
- Challenges Faced by Australian RadiologistsDocument12 pagesChallenges Faced by Australian RadiologistsVijay RajNo ratings yet
- Introduction to Continuous Renal Replacement Therapy (CRRT) in ICUDocument25 pagesIntroduction to Continuous Renal Replacement Therapy (CRRT) in ICUyamtotlNo ratings yet
- Music and Therapy Bun2Document17 pagesMusic and Therapy Bun2PanteaAlisaNo ratings yet
- Lizzy Hiv AssignmentDocument7 pagesLizzy Hiv Assignmentapi-376826833No ratings yet
- Treatment of Pulmonary and Extra-Pulmonary Tuberculosis in AdultsDocument65 pagesTreatment of Pulmonary and Extra-Pulmonary Tuberculosis in AdultsLloyd Daniel BarrantesNo ratings yet
- Adenomyosis A Sonographic DiagnosisDocument14 pagesAdenomyosis A Sonographic DiagnosisHelioNo ratings yet
- For Your Youngest PatientsDocument2 pagesFor Your Youngest PatientsMarjorie BobadillaNo ratings yet
- New Report in The Treatment of Breast Cancer MastectDocument2 pagesNew Report in The Treatment of Breast Cancer MastectGil LedermanNo ratings yet
- Wound Dressing Checklist SKL 112 FINAL EDITDocument5 pagesWound Dressing Checklist SKL 112 FINAL EDITCamille GuintoNo ratings yet
- Otitis Media: Prepared By: - Priyanka ThapaDocument38 pagesOtitis Media: Prepared By: - Priyanka ThapaKalo kajiNo ratings yet
- Distal Tibial Fractures Intramedullary NailingDocument8 pagesDistal Tibial Fractures Intramedullary NailingasdaadNo ratings yet
- Mcqs For TestDocument3 pagesMcqs For TestMranali JaiswalNo ratings yet
- 17th Asian Games Incheon 2014Document44 pages17th Asian Games Incheon 2014dantevermillionNo ratings yet