0% found this document useful (0 votes)
96 views85 pagesBlood Cells and Circulation Overview
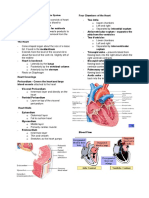
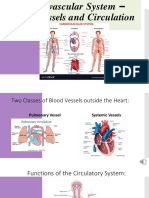
The cardiovascular system consists of the heart and blood vessels. The heart pumps blood through three types of blood vessels - arteries, veins, and capillaries. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of oxygen, carbon dioxide, nutrients, and waste between the blood and tissues. The cardiovascular system regulates blood pressure, circulation, and delivery of nutrients/oxygen to tissues through complex nervous and chemical control mechanisms.
Uploaded by
Ebrahem ShaheinCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PDF, TXT or read online on Scribd
0% found this document useful (0 votes)
96 views85 pagesBlood Cells and Circulation Overview
The cardiovascular system consists of the heart and blood vessels. The heart pumps blood through three types of blood vessels - arteries, veins, and capillaries. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of oxygen, carbon dioxide, nutrients, and waste between the blood and tissues. The cardiovascular system regulates blood pressure, circulation, and delivery of nutrients/oxygen to tissues through complex nervous and chemical control mechanisms.
Uploaded by
Ebrahem ShaheinCopyright
© © All Rights Reserved
We take content rights seriously. If you suspect this is your content, claim it here.
Available Formats
Download as PDF, TXT or read online on Scribd