Professional Documents
Culture Documents
Nutrition Care Process
Uploaded by
PATRIZJA YSABEL REYES0 ratings0% found this document useful (0 votes)
13 views17 pagesOriginal Title
4. Nutrition Care Process.pptx
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
13 views17 pagesNutrition Care Process
Uploaded by
PATRIZJA YSABEL REYESCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 17
Nutrition Care Process
A. Assessment of Nutritional Status
⚫ Responsibilities and Role of Nurses in Nutritional Care
⚫ Observing
⚫ Nurse - usually the first person who sees the patient’s eating
problems
⚫ has direct communication with the patient
⚫ how well the patient’s eats his food
⚫ what kinds and amounts of food are refused
⚫ the patient’s attitude towards his food are readily determined
⚫ must have a knowledge in diet therapy (food allowed / restriction)
⚫ should immediately forward the diet prescription to the dietary
department
⚫ makes sure that the patient is ready to consume the food served on
the tray
⚫ Listening
⚫ Nurse - shows his/her general interest and
understanding of the patient
⚫ helps the patient express his/her feelings
⚫ learned from the patient some of his/her favorite
foods and dislikes
⚫ explains concerns on foods that cannot be eaten due
to ethnic, cultural background and religious beliefs
⚫ becomes aware of what concerns the patient may
have about the diet he will have at home
⚫ Reporting
⚫ Nurse – documents and chart all the problems related to food
intake
⚫
⚫ Nutritional History
⚫ a. Dietary Intake Data
⚫ - Dietary Computations: Desirable Body Weight
Basal Metabolic Rate
Total Energy Requirement
Food Exchange List
⚫ b. Nutrient Intake Analysis (NIA)
⚫ c. Food Diary
⚫ d. Food Frequency
⚫ e. 24 hour Recall
⚫ Physical Assessment
⚫ a. Anthropometric Measurements
⚫ b. Height and Weight
⚫ c. Body Mass Index
⚫ d. Body Composition
⚫ e. Mid-arm Circumference (MAC)
⚫ f. Fat-fold or Skin-fold Thickness
⚫ Other Sources of Data
⚫ Malnutrition Universal Screening Tool (MUST)
⚫ Subjective Global Assessment (SGA)
⚫ Mini Nutritional Assessment (MNA)
⚫ Geriatric Nutritional Risk Index (GNRI)
⚫ B. Nutrition Diagnosis and Plan of Care
⚫ Nutrition Problems and/or Needs
⚫ Planning the Diet with Cultural Competency
⚫ Resources needed in Planning and Implementing
Dietary Regimen
⚫ C. Nutrition Intervention
⚫ Food and Nutrient Delivery
⚫ Food Administration
⚫ Oral Nutrition
⚫ Short-term enteral access
⚫ Long-term enteral access
⚫ Enteral Nutrition
⚫ Tube Feeding
⚫ Provide enteral nutrition for clients who cannot swallow, with esophageal
obstruction, unconscious, and cannot consume oral feeding.
⚫ Rubber – ice; Plastic- warm (Levine-single; Salem sump-double lumen)
⚫ High fowler’s, if contraindicated place left side lying position with head
slightly elevated to prevent aspiration.
⚫ Measure the distance from the tip of the nose to earlobe through the bottom
of the xiphoid process (adult)
⚫ Measure the distance from the tip of the nose to earlobe through the
midway of xiphoid process and umbilicus (children)
⚫ Use water soluble jelly as lubricant
⚫ Offer sips of water and advance tube forward, head bent forward closes the
epiglottis and trachea
⚫ Inject 10 ml of air and auscultate for gurgling sound
in the epigastrium.
⚫ Aspirate for residual stomach content (ph 1-3 of
yellow to green)
⚫ Immerse tip of the NGT into water and observe for
bubbling.
⚫ X-ray confirms
⚫ Flush with 30-60 ml of water after feeding
⚫ If NGT is to removed, instruct client to exhale and
remove tube with smooth, continuous pull
⚫ NG TUBE
⚫ N- ever give without checking
⚫ G- ive warm(room temperature)
⚫ T- urn to left side during the feeding for the stomach to empty better
⚫ U- se gravity, never force feeding
⚫ B- e sure to aspirate
⚫ E- nd with water and chart
⚫ Types of Enteral Formulation
⚫ Ready to Use Formulations
⚫ Tube feedings – prepared from regular foods
⚪ Standard tube feeding - fiber free, high in cholesterol, fat and sugar
⚫ - milk based, sugar and soft cooked eggs
⚫ 2. Blenderized tube feeding - soft diet allowances which can be
⚫ blenderized easily
⚫ Complications:
⚫ Mechanical
⚫ nasopharyngeal irritations – ice chips
⚫ luminal obstruction – flush, replace tube
⚫ mucosal erosions – reposition tube, ice water lavage, remove
tube
⚫ tube displacement – replace tube
⚫ aspiration – discontinue tube feeding
⚫ Gastrointestinal
⚫ cramping/distention – change formula, reduce infusion rate
⚫ vomiting/diarrhea – dilute formula, reduce infusion rate
⚫ constipation – promote sufficient, fluids and fibers, encourage
patient activity
⚫ Metabolic
⚫ hypertonic dehydration – increase water
⚫ cardiac failure – reduce sodium content, fluid
restriction
⚫ renal failure – decrease phosphate, magnesium,
potassium, CHON restriction, amino acids solution
⚫ glucose intolerance – reduce infusion rate
⚫ hepatic encephalopathy – decrease amount of CHON
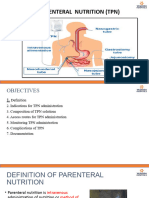
⚫ Parenteral Nutrition
⚫ Peripheral Parenteral Nutrition (PPN) – nutrients are given via small veins,
usually in the arms
⚫ Total Parenteral Nutrition (TPN) – also called Central Parenteral Nutrition
(CPN) or intravenous hyperalimentation (IVH); nutrients are given
centrally into the superior or inferior vena cava or the jugular vein
⚫ TPN solutions are nutritionally complete based on the patient’s weight and
caloric/nutritional needs
⚫ TPN is indicated in clients who need extensive nutritional support over an
extended period like CA and severe malnutrition
⚫ Mixture of dextrose, amino acids, multivitamins, electrolytes and trace of
minerals
⚫ The usual site is subclavian vein
⚫ During TPN catheter insertion, Trendelenburg position – to engorge the
vein and facilitate insertion of the vein and prevent air embolism
⚫ The primary purpose of TPN is to administer glucose
⚫ PIC – basilic / cephalic; PPC - subclavian
⚫ Administer TPN at room temperature
⚫ Cold temperature of solution may cause chills
⚫ Consume TPN formula for 24 hours to prevent contamination
⚫ The TPN solution is hypertonic (25-35% of dextrose)
⚫ Use infusion pump to maintain steady infusion this prevents abnormal
shifting of fluids from intracellular compartment to the extracellular
compartment (cells shrink)
⚫ If infusion is delayed do not catch up – notify physician for calculation
⚫ Monitor urine and glucose level. Glycosuria is expected.
⚫ The client may need small amount of insulin as prescribed by the physician
to prevent glucose intolerance
⚫ Prevent infection on the catheter site. Infection is the most common
complication of TPN.
⚫ If TPN administration is interrupted or discontinued, administer D10W to
prevent hypoglycemia
⚫ D. Monitoring Nutritional Status
⚫ Strategies to address Age-related changes affecting
Nutrition
⚫ Selected Therapeutic Diets
⚫ Recording and reporting of Nutritional Status
⚫ E. Evaluation of Plan of Care
⚫ Effectiveness of the plan of care
• THANK YOU FOR LISTENING
You might also like
- Nutrition Care ProcessDocument6 pagesNutrition Care ProcessGeraldine MaeNo ratings yet
- Nutrition Support in The Hospital Patient: David Armstrong November 2, 2005Document40 pagesNutrition Support in The Hospital Patient: David Armstrong November 2, 2005Larasati HasaptiasNo ratings yet
- ch47 TubeFeedings 1277Document1 pagech47 TubeFeedings 1277Zul MaaNo ratings yet
- Eat Well for Optimal HealthDocument70 pagesEat Well for Optimal HealthVicente MerañaNo ratings yet
- Nutrition HealthDocument62 pagesNutrition HealthMiraNo ratings yet
- Parenteral Nutrition Basic IVT Nov 2008Document53 pagesParenteral Nutrition Basic IVT Nov 2008Crystal Mae Castrodes DaquipilNo ratings yet
- Total Parenteral Nutrition Indications and Nursing ResponsibilitiesDocument3 pagesTotal Parenteral Nutrition Indications and Nursing ResponsibilitiesRhenelyn Delos ReyesNo ratings yet
- 5 & 9. Nutrition Support & TPNDocument53 pages5 & 9. Nutrition Support & TPNRam Sharan MehtaNo ratings yet
- Tucker Mod4 PT 1 IH Enteral Tube Feeds and Tube Care COS 2019Document2 pagesTucker Mod4 PT 1 IH Enteral Tube Feeds and Tube Care COS 2019miguealliNo ratings yet
- Assess, Check, Monitor Enteral FeedingDocument3 pagesAssess, Check, Monitor Enteral Feedingchristina lidaNo ratings yet
- Tube FeedingDocument47 pagesTube FeedingArlyn Mendenilla0% (1)
- IV-B Total Parenteral Nutrition (TPN) and Central Venous Pressure Line (CVP) / Mechanical VentilatorDocument23 pagesIV-B Total Parenteral Nutrition (TPN) and Central Venous Pressure Line (CVP) / Mechanical VentilatorRio DanteNo ratings yet
- For The Surgical Patient: Kelly Sparks LDN, RDDocument47 pagesFor The Surgical Patient: Kelly Sparks LDN, RDManikandaprabhu sivaNo ratings yet
- Competency Appraisal 1 Reviewer-1Document53 pagesCompetency Appraisal 1 Reviewer-1Paolo Carubio100% (1)
- Amit Enteral Feeding PresentationDocument89 pagesAmit Enteral Feeding PresentationAmit KochetaNo ratings yet
- Total GastrectomyDocument12 pagesTotal GastrectomyDarlene PiperNo ratings yet
- Nutrition PostoperativeDocument47 pagesNutrition PostoperativeAnonymous 86gki5No ratings yet
- Case StudyDocument5 pagesCase Studyapi-247850107No ratings yet
- Nutrition Support: Sean P Harbison MDDocument42 pagesNutrition Support: Sean P Harbison MDsgod34No ratings yet
- Nutritional Support in Critically Ill PatientDocument42 pagesNutritional Support in Critically Ill PatientPema Dolma Tamang100% (1)
- Complications of EN NutritionDocument29 pagesComplications of EN Nutritionsamarshahab320No ratings yet
- Essential Enteral and Parenteral Nutrition GuideDocument64 pagesEssential Enteral and Parenteral Nutrition GuideHeba IyadNo ratings yet
- Total Parenteral Nutrition Guideline-4 - 2Document38 pagesTotal Parenteral Nutrition Guideline-4 - 2FirnandaNo ratings yet
- E R NCPDocument2 pagesE R NCPapi-296539974No ratings yet
- Monitoring and Evaluation of Enteral Formula: Preventing ComplicationsDocument23 pagesMonitoring and Evaluation of Enteral Formula: Preventing ComplicationsPaulinNo ratings yet
- Acute Gastroenteritis (AGE) PDFDocument37 pagesAcute Gastroenteritis (AGE) PDFAries Chandra AnandithaNo ratings yet
- Acute Gastroenteritis (AGE)Document37 pagesAcute Gastroenteritis (AGE)Sari HariyaniNo ratings yet
- Surgical Nutritions: Prepared By: Lilibeth C.Tenorio, M.DDocument33 pagesSurgical Nutritions: Prepared By: Lilibeth C.Tenorio, M.DLilibeth Tenorio De Leon100% (1)
- Elliott Clinical Case ReportDocument16 pagesElliott Clinical Case Reportapi-244913342No ratings yet
- DAY 41 INTRODUCTION of Medical Nutrition and TherapyDocument29 pagesDAY 41 INTRODUCTION of Medical Nutrition and TherapyMadhura KarthikNo ratings yet
- Nutrition in ICU: DR Rahul VarshenyDocument50 pagesNutrition in ICU: DR Rahul VarshenyAntar InenigogNo ratings yet
- Eichen - Case Study SboDocument30 pagesEichen - Case Study Sboapi-246480452No ratings yet
- Nasogastric Tube FeedingDocument7 pagesNasogastric Tube FeedingVina Empiales100% (1)
- Critically Ill Patients Often Are Malnourished and in Protein CatabolismDocument14 pagesCritically Ill Patients Often Are Malnourished and in Protein CatabolismAaminah KausarNo ratings yet
- En - Enteral Nutrition Administration IssuesDocument77 pagesEn - Enteral Nutrition Administration IssuesNers SenNo ratings yet
- Routine Nutrition Therapy: Enriquez R. Cayaban, RN, LPT, ManDocument45 pagesRoutine Nutrition Therapy: Enriquez R. Cayaban, RN, LPT, ManCarl Josef C. GarciaNo ratings yet
- Diarrhoea +/ Vomiting: Nurse Practitioner Clinical Protocol Emergency DepartmentDocument10 pagesDiarrhoea +/ Vomiting: Nurse Practitioner Clinical Protocol Emergency DepartmentLalaine RomeroNo ratings yet
- Essential Parenteral Nutrition GuideDocument51 pagesEssential Parenteral Nutrition GuideAudrie Allyson GabalesNo ratings yet
- Total Parenteral Nutrition Guideline-4 - 2Document38 pagesTotal Parenteral Nutrition Guideline-4 - 2Henry M. BarberenaNo ratings yet
- Clinical Case PresentationDocument25 pagesClinical Case Presentationapi-246186340No ratings yet
- Enteral and Parenteral Nutrition SeminarDocument20 pagesEnteral and Parenteral Nutrition SeminarAmin AksherNo ratings yet
- Diet TherapyDocument82 pagesDiet TherapyElishah CaprichoNo ratings yet
- TPN 1 UpdatedDocument13 pagesTPN 1 Updatedathijasafraan1997No ratings yet
- Clinical NutritionDocument27 pagesClinical NutritionKhushiNo ratings yet
- P L NCPDocument2 pagesP L NCPapi-296539974No ratings yet
- Support Feeding - Tugas Mata Kuliah Nutrisi Klinis - Annisa FathadinaDocument66 pagesSupport Feeding - Tugas Mata Kuliah Nutrisi Klinis - Annisa FathadinaAnnisa FathadinaNo ratings yet
- DIETATICSDocument30 pagesDIETATICSAnaya KhanNo ratings yet
- Management of Acute Gastroenteritis in Young Children A Synopsis of The American Academy of Pediatrics' Practice Parameter On TheDocument5 pagesManagement of Acute Gastroenteritis in Young Children A Synopsis of The American Academy of Pediatrics' Practice Parameter On TheAbdul Ghaffar AbdullahNo ratings yet
- Intestinal Obstraction MajDocument44 pagesIntestinal Obstraction MajHamss AhmedNo ratings yet
- Gastroenteritis and Diarrhea TreatmentDocument110 pagesGastroenteritis and Diarrhea TreatmentJaja ManezNo ratings yet
- Clinical - Comprehensive Clinical Case Study PowerpointDocument29 pagesClinical - Comprehensive Clinical Case Study Powerpointapi-240611862No ratings yet
- Parenteral FeedingDocument7 pagesParenteral Feeding4gen_7No ratings yet
- PancreatitisDocument59 pagesPancreatitisrimsha waseemNo ratings yet
- Nutrition: - . - and The Surgical PatientDocument39 pagesNutrition: - . - and The Surgical PatientJan Cyrill YuNo ratings yet
- NCPDocument7 pagesNCPmftaganasNo ratings yet
- Joo Yee Lim SMH Case StudyDocument17 pagesJoo Yee Lim SMH Case Studyapi-605497055No ratings yet
- Bowel Elimination:: DiarrheaDocument44 pagesBowel Elimination:: DiarrheaBashracel Marie M. SALMORINNo ratings yet
- Nutrition Support Surgical PatientsDocument35 pagesNutrition Support Surgical PatientsFuad Aman AbjNo ratings yet
- Gastric Sleeve Surgery Cookbook: Safe and Delicious Foods for Gastric Bypass SurgeryFrom EverandGastric Sleeve Surgery Cookbook: Safe and Delicious Foods for Gastric Bypass SurgeryNo ratings yet
- (PDF) Valorisation Des Sous-Produits Du Coton Et Du Soja Dans L'alimentation Des Ruminants en Afrique de L'ouest Synthèse BiblDocument1 page(PDF) Valorisation Des Sous-Produits Du Coton Et Du Soja Dans L'alimentation Des Ruminants en Afrique de L'ouest Synthèse BibllynaNo ratings yet
- Wanna Be 6Document7 pagesWanna Be 6joie gucciNo ratings yet
- StokDocument240 pagesStokMuhammad IkhsanNo ratings yet
- Soal Semester Bahasa Inggris KURMER Kelas 10 Fase EDocument14 pagesSoal Semester Bahasa Inggris KURMER Kelas 10 Fase ERatna tria sari100% (1)
- Hydrating Cream For The Mature Skin With Hyaluronic Acid - 1033 Ingredient Function Percent WGT (G) WGT (Oz) Vol (TSP.) Phase ADocument1 pageHydrating Cream For The Mature Skin With Hyaluronic Acid - 1033 Ingredient Function Percent WGT (G) WGT (Oz) Vol (TSP.) Phase AgunungmasmultiusahaNo ratings yet
- 泰國飲食文化Document19 pages泰國飲食文化黃鈺棠No ratings yet
- Safari - 14 Nov 2022 at 12:28 PMDocument1 pageSafari - 14 Nov 2022 at 12:28 PMPatrick ShedrackNo ratings yet
- 2019 La Union Country Side in FiguresDocument198 pages2019 La Union Country Side in FiguresgurbyfuryNo ratings yet
- 99 Surprising Foods Which Have Gluten EbookDocument3 pages99 Surprising Foods Which Have Gluten EbookShivshankar IyerNo ratings yet
- Irani Homestays - About UsDocument19 pagesIrani Homestays - About UsNeha GoenkaNo ratings yet
- Biscuit Cracker and Cookie Recipes For TDocument200 pagesBiscuit Cracker and Cookie Recipes For TNever step back SClub100% (1)
- Mesopotamia Unit Test ReviewDocument8 pagesMesopotamia Unit Test ReviewFobe Lpt NudaloNo ratings yet
- The Revival of The Metal Can - White PaperDocument16 pagesThe Revival of The Metal Can - White Paperngocthang7117No ratings yet
- דף עבודה באנגלית 2Document1 pageדף עבודה באנגלית 2Freddy Perez GasparNo ratings yet
- Best Culinary College in India - Culinary Arts Courses - SymbiosisDocument4 pagesBest Culinary College in India - Culinary Arts Courses - Symbiosissscapune1No ratings yet
- Senyawa Asam 2-Metilester-1-H-Pirol-4-Karboksilat Dalam Ekstrak Etil Asetat Buah Salak Varietas Bongkok Sebagai Antioksidan Dan AntihyperuricemiaDocument7 pagesSenyawa Asam 2-Metilester-1-H-Pirol-4-Karboksilat Dalam Ekstrak Etil Asetat Buah Salak Varietas Bongkok Sebagai Antioksidan Dan AntihyperuricemiaRizkilukumNo ratings yet
- Hassan(Internship Report) 2Document33 pagesHassan(Internship Report) 2Muhammad Zohaib EjazNo ratings yet
- Units 3 - 4 Workshop A2Document3 pagesUnits 3 - 4 Workshop A2S4N7Y PRONo ratings yet
- Quotation For Feasibility Study ReportDocument2 pagesQuotation For Feasibility Study Reporthasib.sa.auNo ratings yet
- WORKSHEET Mark The Letter ADocument9 pagesWORKSHEET Mark The Letter ADu Nguyễn TrọngNo ratings yet
- Fce (2-5 Words)Document14 pagesFce (2-5 Words)Bao NgocNo ratings yet
- Chinese Cook BookDocument16 pagesChinese Cook BookJAREK MBAREKNo ratings yet
- Elevator PitchDocument5 pagesElevator PitchIsaac OmwengaNo ratings yet
- Listening Test 11-16Document31 pagesListening Test 11-16Tuệ MinhNo ratings yet
- RaweDocument13 pagesRaweYash PratapNo ratings yet
- Regnum Carya Golf & Spa Resort - Winter 18-19 - EnglishDocument10 pagesRegnum Carya Golf & Spa Resort - Winter 18-19 - EnglishCris MefNo ratings yet
- HP 01 Product Description & Intended Use Rev08Document2 pagesHP 01 Product Description & Intended Use Rev08Mohamed Mokhtar Ahmad TarmiziNo ratings yet
- 10 1002@aocs 12340Document12 pages10 1002@aocs 12340Manuel Rios GonzalesNo ratings yet
- Menu Lege Tebet Proof JuniDocument20 pagesMenu Lege Tebet Proof JuniZero Runoff DPMPTSP JakNo ratings yet
- Module-5 3rd-Day Coordinating-Conjunctions Semi DetailedDocument3 pagesModule-5 3rd-Day Coordinating-Conjunctions Semi DetailedMaria Angela EduardoNo ratings yet