Professional Documents
Culture Documents
(ANAT) P.08 Anatomy of The Eyeball Extra-Ocular Muscles, Eyelid and Lacrimal Apparatus
Uploaded by
Arthur NerickOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(ANAT) P.08 Anatomy of The Eyeball Extra-Ocular Muscles, Eyelid and Lacrimal Apparatus
Uploaded by
Arthur NerickCopyright:
Available Formats
P.
08 ANATOMY OF THE EYEBALL, EXTRA-OCULAR MUSCLES,
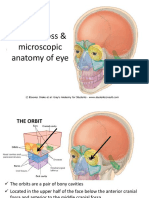
EYELID AND LACRIMAL APPARATUS THE ORBIT
Dr. Sison| August 30, 2020
Dr. Batcagan| August 31, 2020
OUTLINE
I. THE EYE BALL (Dr. Sison)
A. Conjunctiva
B. Cornea
C. Sclera
D. Uveal Tract
E. Iris
F. Ciliary body
G. Choroid
H. Lens
I. Vitreous
J. Retina
II. THE EXTRA-OCULAR MUSCLES (Dr. Sison)
A. Recti Muscles
B. Oblique Muscles
C. Levator Palpebrae Superioris
III. NERVES IN THE ORBIT (Dr. Sison)
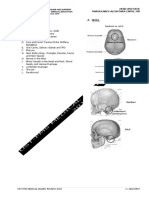
Figure 2. Right orbit (Frontal)
IV. BLOOD SUPPLY TO THE ORBIT AND EYE (Dr. Sison)
V. LANDMARKS OF THE EYE (Dr. Batcagan) The bones contributing to the orbit include the following:
VI. EMBRYOLOGY (Dr. Batcagan) o Frontal (orbital surface)
VII. GROSS ANATOMY OF THE EYELID (Dr. Batcagan) o Maxillary (orbital surface)
A. The Eyelid o Zygomatic (orbital surface)
B. Skin/ Subcutaneous Tissue
o Sphenoid
C. Orbicularis Oculi Muscle
D. Orbital Orbicularis
o Palatine (orbital plate)
E. Orbital Septum o Ethmoid (orbital plate)
F. Orbital Fat o Lacrimal
G. Eyelid Retractors
H. Tarsus The back of the orbit has three large openings that include
I. Conjunctiva the following:
VIII. VASCULAR SUPPLY TO THE EYELID (Dr. Batcagan) Superior orbital fissure – CN III, IV, VI, and V1 (frontal,
IX. VENOUS DRAINAGE OF THE EYELID (Dr. Batcagan)
X. LYMPHATIC DRAINAGE (Dr. Batcagan)
lacrimal and nasociliary nerves) pass through the fissure
XI. INNERVATION (Dr. Batcagan) along with the ophthalmic vein
XII. LACRIMAL APPARATUS (Dr. Batcagan) Inferior orbital fissure – CN, V2 and infraorbital vessels
A. Development of the Lacrimal Secretory System pass through this fissure
B. Blood Supply & Lymphatics Optic canal – CN II and the ophthalmic artery pass through
C. Innervation this canal
D. Lacrimal Pump
E. Theories of Lacrimal Pump A. CONJUNCTIVA
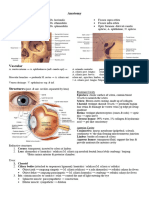
Thin membrane that lines the inner aspect of the eyelids and
I. THE EYEBALL reflects onto the sclera, ending at the scleral-corneal
Measures about 25mm in diameter junction
Tethered in the bony orbit by six (6) extraocular muscles Important: mucus membrane which covers the sclera
that moves the globe
Cushioned by fat that surrounds the posterior two-thirds of Parts:
the globe o Anterior surface of sclera( Bulbar)
Contains three (3) chambers: Vitreous chamber, Anteror - loosely attaches to the globe
Chamber, Posterior Chamber. - Extends to form a fold called the
fornix
o Posterior surface of the lids (Palpebral)
- adheres tightly to the eyelids
o Forniceal conjunctiva
o Semilunar fold or Plica Semilunaris
o Thickened fold of bulbar conjunctiva
located in the medial frontal area
o Corresponds to nictitating membrane of
some lower animals
o Caruncle – Small fleshy epidermoid structure
attached superficially at the most medial portion of
the semilunar fold
o Transition zone which contains both
cutaneous and mucous membrane
elements (transition zone)
Figure 1. Structures of the Eyeball
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 1 of 14
o Continuous to the mucocutaneous junction and
corneal epithelium at the limbus
o Non keratinized squamous epithelium
o Accessory glands:
o Glands of Krause
o Glands of Wolfring
o Glands of Henle
o Glands of Manz
SUBCONJUNCTIVAL FASCIA-Holds the globe
Tenon’s Capsule
- Anterior: fuses with conjunctiva behind the limbus
- Posterior: separates orbital fat from muscles and globe
- suspends the structures of the orbit
Intermuscular Septum
- extension of the Tenon’s
- connects muscles
Check ligaments
- connect muscles to overlying Tenon’s
- inserts on orbital walls to support globe
-suspends the eyeball to the orbit
Lockwood’s Ligament
- fusion of sheaths of inferior rectus and inferior oblique
- attaches to medial and lateral retinacula and supports
LIMBUS
(anterior) termination of Descemet’s and Bowman’s
B. CORNEA
membranes
most anterior coat of the eyeball
o (posterior) line between iris root and Schlemm’s
Occupies about 1/6 of the circumference of the globe and is
canal
continuous with the opaque sclera
Transparent part of outer layer; very sensitive to pain
Schlemm’s canal- circular venous space at the
Avascular and transparent
corneoscleral junction/ limbus; it communicates with
Major refractive medium of the eye and protective window
the scleral veins and with the aqueous humor
o Central Cornea Thickness (CTT)
o Transition zone between cornea and sclera (1-
o Varies between individuals
2mm wide)
Continues posteriorly to blend with the sclera
o Conjunctiva and Tenon’s are fused in this area
Key determinant of the intraocular pressure (OP) in
Contains:
Goldmann Tonometry
o Corneal epithelial stem cells
Due to avascularity, it receives nourishment from:
o Goblet cells lymphoid cells
o Aqueous
o Langerhans’cells
o Tears from precorneal tear film
o Mast cells
o Blood vessels at the libmal area
Sensory innervation - OPHTHALMIC DIVISION OF
C. SCLERA
TRIGEMINAL NERVE, Long Ciliary Nerve (CN V1)
White fibrous protective coating of the eyeball
composed of 5 layers: from external going posterior
Consist almost entirely of collagen fibers that is continuous
o Epithelium - continuous to epithelium of bulbar
to the cornea anteriorly & dural sheath of the optic nerve
conjunctiva
posteriorly
o Bowman’s layer - clear and acellular
The anterior and posterior chamber is filled with Aqueous
o Stroma - 90% of corneal thickness; collagen fibrils
(secreted by the non-pigmented epithelium of the ciliary
arranged parallel to the cornea
processes)
o Descemet’s membrane - basal lamina of the
o provides nutrition to the lens and cornea
innermost layer
o responsible for maintaining intra-ocular pressure
o Endothelium - single layer of cell responsible for
Anterior chamber – chamber between the cornea and the
maintaining the relative hydrated state or
iris; filled with aqueous humor
deturgescence of the stroma.
Posterior chamber – space between the iris and lens;
filled with aqueous humor
*Aqueous humor – produced by the ciliary body and
circulates from the posterior chamber, through the pupil,
and into the anterior chamber, where it is absorbed by the
trabecular meshwork into the scleral venous sinus (canal of
Schlemm) at the angle of the cornea and iris
Supports eye shape
Protects delicate internal structures
Extrinsic muscle attachment site
Layers:
o Episcleral
o Sclera proper
o Lamina fuscia
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 2 of 14
D. UVEAL TRACT o Ciliary Processes - are radially arranged folds, or
VASCULAR PIGMENTED COAT ridges, to the posterior surfaces of which are connected
Middle vascular layer of the eye to the suspensory ligament of the lens
Protected by the cornea and sclera o Ciliary Muscle- is composed of meridianal and circular
Contributes to the blood supply of retina fibers of smooth muscle
3 parts:
o Iris
o Ciliary body INNERVATION
o Choroid - contributes to the blood supply of the Parasympathetic Fibers from the oculomotor nerve
retina -After synapsing in the ciliary ganglion, the postganglionic
fibers pass forward to the eyeball in the short ciliary nerves
E. IRIS
Oppressed Myopia – lens loses their elasticity due to
Shallow cone pointing anteriorly containing the pupil both
aging
function to moderate the amount of light entering the eye
Anterior extension of the ciliary body
contractile diaphragm with central aperture (pupil) G. CHOROID
regulates the amount of light to reach the retina middle vascular layer located between the retina and sclera
referred to as a “curtain” It divides the space between the most posterior portion of uveal tract
lens and the cornea into: supplies the blood supply of the outer half of the retina
o anterior chamber
o posterior chamber H. LENS
located behind the iris pupil diaphragm
transparent lens supported in capsule by zonular fibers
suspended by zonules of zinn to the ciliary body
Sole purpose: TO FOCUS LIGHT INTO THE (FOVEA OF
THE) RETINA
Accomodation: The ciliary body contains smooth muscle
arranged in a circular fashion like a sphincter. When relaxed,
it pulls a set of zonular fibers attached to the elastic lens
taut and flattens the lens for viewing objects at some
distance from the eye. When focusing on near objects, the
sphincter-like ciliary muscle (parasympathetically innervated
by CN III) contracts and constricts closer to the lens,
relaxing the zonular fibers and allowing the elastic lens to
round up for accommodation (near vision).
I. VITREOUS
clear visco-elastic gel avascular gelatinous body behind the
lens
comprises ⅔(75%) of the total eye volume
Figure 3. Anterior and Posterior Chambers of the Eyeball maintains the shape of the eye as well as its structural
stability
Within the stroma of the iris are the Sphincter pupillae Vitreous chamber – large chamber behind the lens; filled
muscles along the pupillary border and are innervated by with gel-like substance called vitreous humor (helps cushion
the 3rd Cranial Nerve and protect the fragile retina during rapid eye movements)
short ciliary nerves
Dilator pupillae muscles (Sympathetic) – Innerveted by J. RETINA
the sympathetic arising from the superior cervical ganglion
thin, semi-transparent layer of nerve tissue
long ciliary nerves
Innermost coat of the eye
F. CILIARY BODY Optically receptive part of the optic nerve (optic retina);
Contains ciliary muscles for accommodation contains Rods (dim light vision) and Cones (color vision)
The muscles allow one to focus in real time, distant objects “window” into the brain
and near objects contains photoreceptors that convert light to electrical
Contains layer of non-pigmented cells that produces impulses
Aqueous humor covers the ciliary processes and the back of the iris
vascular and muscular extension of choroid anteriorly Its anterior edge forms a wavy ring, the ora serrata,
“dangerous area” of the eye Where nervous tissues end
continuous posteriorly with the choroid and anteriorly, it lies
behind the peripheral margin of the iris MECULA LUTAE
Functions: - oval, yellowish area at the center of the posterior part of
o Produces aqueous humor the retina
o maintains intraocular pressure FOVEA CENTRALIS
o contains ciliary muscle for accommodation: focus lens -central depression, the inner nuclear layer and ganglion cell
when you are looking at a near object layer are displaced
Composition: - Area of macula with the most acute vision; contains only
o Ciliary Ring - is the posterior part of the body, and its cones and is the center of the visual axis (ideal focus point)
surface has shallow grooves, the ciliary striae
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 3 of 14
OPTIC DISC Inferior Rectus
- medial side of the macula lutea o Depresses and ADducts
- about 3 mm to the optic disc the optic nerve leaves the o concerned with EXTORSION
retina about 3 mm B. OBLIQUE MUSCLES
- is slightly depressed at its center pierced by the central Superior Oblique
artery of the retina - longest and thinnest EOM
-Complete absence of rods and cones so that it is insensitive - moves the eye laterally and inferiorly
to light and is referred to as the “blind spot” lateral - responsible for INTORSION
-Non-receptive area (blind spot) where retinal ganglion cell Inferior Oblique
nerve axons leave the retina in the optic nerve and pass to - moves the eye superiorly and laterally
the brain - responsible for EXTORSION
C. LEVATOR PALPEBRAE SUPERIORIS
Origin: Lesser Wing of Sphenoid
REFRACTIVE MEDIA Insertion : Superior Tarsal Plate
Light rays focused by the cornea, aqueous humor, lens, and Action: Elevates Superior Eyelid and maintain this
vitreous humor position
Innervated by : Oculomotor Nerve (3rd Cranial Nerve)
II. EXTRA-OCULAR MUSCLES Blood Supply: Ophthalmic and Supraorbital artery
responsible for the movement of the eyes
there 6 extraocular muscles:
o 4 Recti
o 2 Oblique
3rd Cranial nerve (III) innervates
o Medial Rectus (MR)
o Inferior Rectus (IR)
o Superior Rectus (SR)
o Inferior Oblique (IO)
6th Cranial Nerve (VI) innervates
o Lateral Rectus (LR)
4th cranial nerve (IV) innervates
o Superior oblique (SO)
The innervation of these muscles aid neurologists in localizing any
neurologic diseases resulting from loss or decrease of muscle
movement.
Figure 5. Extrinsic Eye Muscles
Figure 4. Extraocular muscles
A. RECTI MUSCLES
originate from Annulus of Zinn
named after the sites of insertion e.g. Medial Rectus inserts INTRINSIC MUSCLES
medial to the Cornea; Lateral Rectus inserts temporal/lateral Sphincter pupillae-around the pupil margin
to the cornea - circular rotation
Medial and Lateral rectus only have a single action - constricts the pupil
o Adduction - moving the eye medially (MR) - nasal Dilator Pupillae
o Abduction - moving the eye laterally (LR) - temporal - Radial Rotation
Inferior and Superior rectus have : - Dilates Pupil
o Primary Action Ciliary muscle-deeper
o Secondary Action - longitudinal fibers
Superior Rectus - circular fibers
o Elevates and ADducts - radial fibers
o concerned with INTORSION - for accommodation (pupil dilates, lens thickens, then
convergence)
-Control how the lens adapts to focusing
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 4 of 14
III. NERVES IN THE ORBIT
Three cranial nerves innervate the extraocular skeletal muscles:
CN II (Optic nerve): cranial nerve that mediates the
special sense of sight; brain tract that conveys sensory
information from the retina, via the ganglion axons, to the
brain
CN V1 (Opthalmic nerve): cranial nerve that conveys
general sensory information from the orbit and eye; its
branches include:
o Frontal – runs on the superior aspect of the
levator palpebrae superioris muscle and ends as
the supratrochlear and supraorbital nerves;
sensory to the forehead, scalp, frontal sinus, and
upper eyelid
o Lacrimal – courses laterally on the superior
aspect of the lateral rectus muscle to the lacrimal
gland; sensory to conjunctiva and skin of the
upper eyelid
o Nasociliary – gives rise to short and long ciliary
nerves, posterior and anterior ethmoidal nerves,
and infratrochlear nerve; sensory to iris and
cornea, sphenoid and ethmoid sinuses, lower
eyelid, lacrimal sac, and skin of the nose
CN III (Oculomotor nerve): provides parasympathetic
fibers in which they exhibit the following features:
o They arise centrally from the nucleus of Edinger- Figure 6. Nerves of the Orbit
Westphal (preganglionic fibers), and course along
the CN III and its inferior division to synapse in IV. BLOOD SUPPLY TO THE ORBIT AND EYE
the ciliary ganglion on post ganglionic The ophthalmic artery arises from the internal carotid
parasympathetic neurons artery just as it exits the cavernous sinus, and it supplies the
o Postganglionic fibers then course via short ciliary orbit and the eye by the following branches:
nerves to the eyeball a. Central artery of the retina: travels in the optic
o These fibers innervate the sphincter muscle of the nerve; occlusion leads to blindness
pupil (sphincter pupillae) and the ciliary muscle for b. Short and long posterior ciliary arteries:
accommodation pierce the sclera and supply the ciliary body, iris,
and choroid
Sympathetic innervation to the eyeball is arranged as c. Lacrimal arteries: supply the gland, conjunctiva,
follows: and the eyelids
It arises from the upper thoracic d. Ethmoidal arteries: supply the ethmoid and
intermediolateral cell column of the frontal sinuses, nasal cavity, and external nose
spinal cord (T1-T2) and sends e. Medial palpebrae arteries: supply the eyelids
preganglionic fibers into the sympathetic f. Muscular arteries: supply skeletal muscles of
trunk, where they ascend to synapse in the orbit and smooth muscles of the eyeball
the superior cervical ganglion (SCG) g. Supraorbital artery: passes through supraorbital
Postganglionic fibers course along the notch and supplies the forehead and scalp
internal carotid artery, enter the orbit on h. Supratrochlear artery: supplies the forehead
the ophthalmic artery, and pass through and the scalp
the ciliary ganglion or along the long
and short ciliary nerves to the eyeball The venous drainage is by the superior and inferior
They innervate the dilator muscle of the ophthalmic veins, which connections to the cavernous sinus
pupil (dilator pupillae) and the superior posteriorly (principal drainage), the pterygoid plexus
tarsal muscle of the upper eyelid inferiorly, and the facial vein anteriorly.
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 5 of 14
VI. EMBRYOLOGY
Facial processes from brachial
arch:
[1] Frontonasal= Upper eyelid
[2] Medial nasal
1st week of Development of the [3] Lateral nasal
gestation five Pharyngeal arches [4] Maxillary= Lower eyelid
[5] Mandibular
Incomplete development leads to:
6th to 7th week Eyelid folds mark [1] Ablepharon
(completed at the beginning of [2] Cryptophthalmos
10th week) eyelid development [3] Microblepharon
Figure 7. Branches of the Ophthalmic Artery
Eyelid Development Stages
Failure:
8th to 10th 1. Eyelid fusion Colobomas of lid margin
2. Development of
3rd to 4th month Congenital ptosis
eyelid structures
[1] Ankyblepharon
5th to 6th month 3. Eyelid dysjunction [2] Blepharophimosis
[3] Epicanthus Euryblepharon
VII. GROSS ANATOMY OF THE EYELIDS
Extent and Position of the Eyelid
o Upper Lid
- Eyebrows to the superior boundary of the palpebral
border
o Lower Lid
- Inferior border palpebral fissure to the cheeks.
o In the Primary Position
V. LANDMARKS OF THE EYE
o The upper lid covers the upper 1/6th of
the upper part of cornea
o The lower lid just touches the cornea
Figure 9. Normal eyelid v. Ptosis
* If more than 1/6th = sign of ptosis
*Scleral show at inferior position = exophthalmos/thyroid related
eye disease
Lid Creases and Folds
- Outline the underlying structures that serve as
landmarks that assist in clionical evaluation which can
help plan surgical procedures involving the area
Figure 8. Landmarks of the Eye
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 6 of 14
Clinical Application
Hordeolum Chalazion
Infection of sterile, chronic inflammation
the tarsal gland (of Meibom) of thethat results from
eyelid (redness, acutely tender) blocked meibomian
gland (hard, non-tender)
Internal – Meibomian gland May develop from an internal
External (STYE) – Gland of Zeis or hordeolum
Moll
Figure 10. Location of Lid Creases and Folds
o Superior lid crease
- represents cutaneous insertion of the levator
aponeurosis to the preseptal orbicularis oculi
o 8-12 mm above the upper lid margin in
Caucasians
o 2-5 mm above the lid margin in Asians Figure 11. Stye v. Chalazion
- Lower in Asians since the orbital septum and levator Gray Line
aponeurosis is fused at a lower level - Outline of the Muscle of Riolan or Pars Ciliaris
- Constructive/aesthetic surgery: adjusting or retaining - Located posterior the lash line and is anterior to the
the position will result to creating a lid crease or fuller tarsus
lid - Represent the pretarsal Orbicularis on the eyelid margin
o Inferior lid crease - Posterior the gray line demarcates the anterior and
o Lid Folds posterior lamellae
o Nasojugal and Malar Creases Functions:
1. Meibomian gland discharge
Canthi – The angles to which the upper and lower lids meet 2. Blinking
o Lateral Canthus – Directly in contact with the globe 3. Positioning of eyelashed
o Medial Canthus - Separated with the globe by a tear Lacrimal Puncta
lake - opening near the medial canthus
Structures nearby: - Represents the opening from the lid margin into the
o Caruncle - Modified skin with sebaceous glands ampulla and canaliculi (lacrimal drainage apparatus)
o Plica semilunaris - Vestigial structure analogous to Palpebral Fissure
the nictitating membrane of animals o The opening of the lid
- Space between the upper and lower lid, provides
Eyelid Free Lid Margin opening for the globe
- 20-30 mm long, about 2 mm wide - At birth: 20 mm wide x 8 mm height
- Divided by the mucocutaneous junction (gray line) - Adults: 30 mm wide x 10 mm height
50% have the lateral canthus higher by 2 mm than the medial
Anterior Margin canthus
Lash line (Eye lashes) A. THE EYELIDS
- Most anterior part of the lid margin Modified skin folds to protect the anterior part of the eye
- They arise from hair follicles on the anterior side of the Each eyelid contains a tarsal plate of dense connective tissue
tarsus and project outward and anterior to the lid Each eyelid contains:
margins o Tarsal plate- consist of dense
- 100-150 cilia in the upper lid Connective tissue
- 50-70 cilia in the lower lid o Tarsal glands- secrete an oily mixture
2 Glands: into the tears
The glands secrete lipid to cover the outer part of o Smooth muscle- a.k.a superior tarsal
the tear film to prevent evaporation (Müller’s) muscle; attaches to the tarsal
o Glands of Zeis plate along with the levator palpebrae
- Small modified sebaceous glands that open into superioris muscle
the hair follicles at the base of the eyelashes Functions:
o Glands of Moll Primary
- Modified ciliary sweat glands that open in a row
o Protection from injury and
near the base of the eyelashes excessive light
o Voluntary or Involuntary closure
Posterior Margin - In close contact with the globe and along this o Keeps the corneas moist
margin are two small orificies of modified sebaceous glands Secondary
Meibomian or Tarsal Glands o Tear Production and
o Holocrine glands Drainage
o Meibium (oils) o Blink Reflex
o Approximately 50 glands upper lid and 25 glands lower o Stabilization of Precorneal Tear
lid Film
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 7 of 14
B. SKIN/ SUBCUTANEOUS TISSUE Functions:
- Differs from the skin of most other areas o Voluntary: winking
- Thin and Loosely adherent to the orbicularis muscle o Involuntary: Blinking
- Elastic Orbital Orbicularis
- Few hair follicles o Surrounds the orbital aperture
o Outermost and largest segment
- No subcutaneous fat
Functions:
2 LAYERS
o Forcible eyelid closure
Epidermis
o Voluntary eyelid closure
- Keratin
Origin:
- Granular Cell Layer
o MCT
- Prickle Cell Layer
o Frontal bone
- Basal Cell Layer
Dermis o Maxillary bone
- The skin of the upper lid is thinner than the lower lid
Insertion: Below the origin
Figure 12. Epithelial layers of the eyelid skin
Figure 13. Location of the Orbicularis Orbital Muscle
o Eyelid skin is composed of
keratinized stratified epithelium D. ORBITAL SEPTUM
that covers the surface Thin, multilayered fibrous sheath
o Pilosebaceous elements are Arises from the periosteal lining at the arcus marginalis
conspicuous in the dermis and a Separates the eyelids from the orbit
few blood vessels and sweat glands * Important anatomic barrier from infection, edema and
hemorrhage
C. ORBICULARIS OCULI MUSCLE
*From the arcus marginalis, the septum spans the anterior
Thin sheet of concentrically arranged muscle orbit in a plane deep to the orbicularis oculi muscle and
fibers covering the eyelids and periorbital region ultimately fuses with the eyelid retractors or tarsus.
Although it is a skeletal muscle, it has Upper Eyelid - The orbital septum adjoins the
voluntary and reflex actions orbicularis then fuses with the levator aponeurosis.
Innervated by CN VII o 2-3 mm above the tarsal border
Functions: o 10 mm above the lashline
o Main protector of the eyelids Lower Eyelid - The septum arises from the inferior orbital
o Narrows the palpebral fissure rim as a condensation of the periorbita and periosteum then
and closure of the eyelids it continues anteriorly until it joins with the lower eyelid
o Plays a role in the lacrimal pump retractors as a single unit at 4-5mm below the inferior
system
tarsus. It then inserts on the lower border of the tarsus.
ANATOMIC PARTS:
Pretarsal Orbicularis Medially - OS + pretarsal orbicularis muscles attaches
o Anterior and overlies the tarsus posterior lacrimal crest (w/ anterior lacrimal crest)
o Functions for horizontal movement of Laterally - OS attaches to the deep insertion of the
the eyelid which is important in the pretarsal orbicularis muscle + lateral orbital tubercle
lacrimal pump Figure 14. Location of the Orbital Septum
o Assist mainly in involuntary blinking
Origin:
- Superficial: Medial canthal tendon
- Deep: Post lacrimal crest
- Horner’s muscle (Pars lacrimalis)
Insertion: Lateral Canthan Tendon
Contraction of which draws the eyelids medially and posteriorly then
the resulting lateral pull creates a negative pressure in the lacrimal sac
and draws the tears form the canaliculli into the sac.
Preseptal Orbicularis
o Overlies the orbital septum
Origin: MCT
Insertion: LCT
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 8 of 14
E. ORBITAL FAT - Provides ~2 mm elevation of the upper lid
Posterior to the orbital septum - Attaches the tarsal plate
Anterior to the levator aponeurosis (upper) or - Firmly attached to the palpebral
capsulopalpebral fascia (lower) conjunctiva
Surrounded by thin fibrous sheets that are the continuation - Origin: levator aponeurosis (12-14 mm
of the anterior orbital system above the tarsal margin)
Fat Pads - Innervation: sympathetic nervous system
o Upper (2 pockets formed): - If innervation is interrupted, may cause:
Nasal Mild ptosis
Central Horner’s Syndrome
o Lower (3 pockets formed): - Ptosis – drooping of upper eyelid
Medial - Miosis – constriction of pupil
Central - Anhidrosis – absence of sweating of the face
Lateral o Enophthalmos – sinking of eyeball
Central orbital fat pad is an important landmark in: into bony cavity that protects the eye
o Elective eyelid surgery *In the third cranial nerve dysfunction, ptosis is due to paralysis
o Lid laceration repair of the striated muscle of the levator palpebrae superioris
Lower Eyelid
F. EYELID RETRACTORS
a. Capsulopalpebral Fascia
Responsible for opening the eyelids and formed by a musculofascial
complex with both striated and smooth muscle components known as - Analogous to the levator aponeurosis
the Levator Complex and the Capsulopalpebral fascia in the lower lid. - Fuses to the sheath of the inferior oblique
Upper Eyelid muscle
a. Levator Palpebrae Superioris - 2 heads then fuse anterior to the inferior oblique
- Origin: Apex of the orbit and extends inferiorly to form to form the Lockwood suspensory ligament
the lateral and medial horns - Origin: terminal fibers of the inferior rectus
- Periobital of the lesser wing of the sphenoid, above - Insertion: inferior tarsal border after it fuses with the
the Annulus of Zinn orbital septum
- Muscular portion: 40mm b. Inferior Tarsal Muscle
- Levator Aponeurosis: 14-20mm; passes through - Analogous to the Muller’s muscle
orbital septum forward then downward to the tarsal - Poorly developed; inferior tarsal muscle runs
plates and widens to two major attachments. posterior to the capsulopalpebral fascia
o Lateral Horn
Divides the lacrimal gland to G. TARSUS
orbital and palpebral lobes
o Medial Horn Gives the structural framework of the eyelid
Disinsertion results in loss of Made of fibrous and elastic tissue (NOT cartilage)
eyelid crease Contains meibomian glands
- Insertion: Measurement
o Anterior fibers - 3mm above the lid margin o Length: 20-30 mm long
(pretarsal skin, orbicularis muscles and o Thickness: 1 mm thick
septa) o Height: 9-10 mm (superior tarsus) and 4-5 mm
o Posterior fibers - 2-3mm superior the tarsus (inferior tarsus)
o Lateral Horn – Inserts to the lateral orbital Both anchored to the bone by the MCT and LCT
tubercle
o Medial Horn - Inserts to posterior lacrimal Tarsal Surfaces
crest o Anterior: attachment of the Orbital Septum
- Disinsertion, dehiscence or rarefaction after and Retractors
trauma/surgery may give rise to ptosis o Posterior: Conjunctiva
Superior Transverse Ligament H. MEIBOMIAN GLANDS
- AKA Whitnall’s ligament
- Vertically oriented
- Located in the transition of the levators and - Oil secreting glands
levator aponeurosis o Orifices
- Functions as a support for the upper eyelid and - Posterior the grey line
the superior orbital tissues
- Anterior to the mucocutaneous junction
- Analogue in the lower eyelid is the Lockwood
o Distribution
ligament
- Upper: ~30 MB glands
- Acts as a fulcrum for the levator muscle - Lower: ~20 MB glands
o To transfer the vector force from
anterior-posterior to superior-inferior Factors to loss of horizontal stability:
direction o Aging
o Atrophy
b. Muller’s Muscle o Laxity of the attachments
- AKA Superior Tarsal Muscle o Decreased orbicularis tone
- Smooth muscle
- Originates at the undersurface of the levator
aponeurosis at the level of whitnall’s ligament, 12-
14mm above the tarsal margin
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 9 of 14
VIII. VASCULAR SUPPLY OF THE EYELID
Network of vessels derived from 2 major sources:
Internal Carotid
o Ophthalmic Artery
o Supraorbital Artery
o Lacrimal Artery
External Carotid
o Angular Artery
o Temporal Artery
Collateral Circulation
o Marginal Artery
o Peripheral Arcad
Figure 15. Meibomian glands
I. CONJUNCTIVA
Composed of Non-keratinized squamous epithelium
Forms the posterior layer of the eyelids
Lining from eyelid margin to the corneal scleral limbus
Transparent mucus membrane lining the eye socket
from the eyelid margin into the corneal-scleral limbus
2 Parts
Bulbar conjunctiva
o Loosely attaches to the globe
Palpebral conjunctiva
o Adheres tightly to the eyelids
Figure 18. Vascular Supply of the Eyelid
Collateralization b/n the internal and external systems contribute to the
rapid wound healing and low incidence of infection following eyelid
surgeries. As the vessels approach the eyelids, branches of the
ophthalmic artery from the internal carotid arterty, and branches of
the facial artery of the maxillary branch of the external carotid artery
form the marginal and peripheral arcades of the eyelids.
X. VENOUS DRAINAGE OF THE EYELID
Composed of:
Figure 16. Location of the Bulbar conjunctiva Pretarsal drainage
and the Palpebral conjuctiva o Medial: Angular vein
o Temporal: Superficial temporal vein laterally
Accessory glands- helps with tears production to the jugular vein
o Glands of Krause
Post-tarsal drainage
o Glands of Wolfring
o Orbital veins out to the cavernous sinus
o Glands of Henl
o Deeper branches of the anterior facial vein
o Glands of Manz
o Pterygoid Plexus
Aqueous producing glands of Krause and Wolfring are
histologically identical with main lacrimal gland
Mucous secreting goblet cells
Scattered around the conjunctiva but concentrated
at the Crypts of Henle
Figure 17. Diagrammatic illustration of the location of Figure 19. Veins Surrounding the Eyelid
the accessory glands
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 10 of 14
XI. LYMPHATIC DRAINAGE OF THE EYELID A. DEVELOPMENT OF LACRIMAL SECRETORY SYSTEM
Lymphatic vessels serving the Medial side of the eyelid
drain to the Submandibular Lymphatic Node Develop from multiple solid ectodermal
Lymphatic vessels serving the Lateral side of the eyelid buds (anterior superolateral orbit)
drain to the Superficial Preauricular Lymphatic Node Lacrimal glands are small and do not function fully until
6th week after birth
Morphogenesis is divided in 3 stages
Glandular Stage
o Thickening of superior conjunctival fornix
epithelium
o Condensing of the surrounding
mesenchyme
o ~2 weeks
Bud Stage
o Initial sign of glandular formation
o Development of nodular structures and
lumina within epithelial buds
Glandular Maturity
o Week 9-16
o Begins to mirror the adult gland
Secretory Component: Lacrima Glands & Accessory Glands
Lacrimal Gland
- Secretes most components of the tear film that
Figure 20. Lymphatic Drainage of the Eyelid moisturizes, lubricates and helps protect the eyes
XI. INNERVATION o Location: Superotemporal area beneath the eyebrow
Sensory o Lobes (2): Anterior and Posterior
o V1 – forehead and lateral periocular region o Divided by tendon of the LPS muscle (aponeurosis)
o V2 – lower lid and cheek o Has 8-12 ductules
Motor o Innervations: facial nerve parasympathetics
o CN III – for eyelid opening Lacrimal glands receive secretomotor parasympathetic fibers from the
o CN VII – for eyelid closing + Sympathetic facial nerve (CN VII) that originate in the superior salivatory nucleus;
Nerves travel in the greater petrosal and vidian (nerve of the pterygoid canal)
XII. LACRIMAL APPARATUS nerves; synapse in the pterygoidpalatine ganglion; and send post
Network where tears are produced, transported and flows to ganglionic fibers via the maxillary, zygomatic, and lacrimal nerves to
an outlet the lacrimal gland
Tears: contain albumins, lactoferrin, lysozyme, lipids, In the clinical area, biopsies are done and when doing this from the
metabolites, and electrolytes lacrimal gland, a portion from the orbital part is taken. This is to
Components of the Lacrimal Apparatus prevent damage from the ductules of the lacrimal gland.
o Secretory Exocrine glands producing aqueous secretion
o Osteology
Body of each gland contain 2 cell types
o Excretory
o Acinar Cells/Acini - Lining the lumen
o Tear Film
o Myoepithelial Cells
o Lacrimal Pump - concerned with tear production
- Surround the parenchyma and are covered by a
and transport
basement membrane
The connective tissues surrounding the acinar contain blood
Lacrimal pathway
vessels of the microvasculature and intra & inter globular
Lacrimal gland > Conjunctival Sac > Lacrimal Puncta > Lacrimal
ducts converging at excretory ducts that empty into the
Canaliculi > Lacrimal Sac > Nasolacrimal Duct
superior conjunctival fornix between the upper eyelid and
the eye
B. BLOOD SUPPLY AND LYMPHATIC DRAINAGE
Lacrimal Artery (Zygomatic branch)
- Branch of the Ophthalmic Artery
The vein that drains glands joins the ophthalmic vein.
The lymphatic drainage joins the conjucntival
lymphatics to drain into the pre-auricular
lymph nodes.
Figure 21. Structures of the Lacrimal Apparatus Figure 22. Blood Supply and Lymphatic
Drainage of the Lacrimal Apparatus
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 11 of 14
C. INNERVATION
Irritation of the cornea or conjunctiva stimulates the afferent Afferent (Sensory Innervation)
nerves o Lacrimal Nerve (CN V1 Ophthalmic Branch of
The impulses are carried along the lacrimal nerve to the Trigeminal Nerve) – smallest branch of the ophthalmic
ophthalmic nerve though the ophthalmic division of the nerve
trigeminal nerve and to the sensory nucleus in the trigeminal o The sympathetic post ganglionic nerve fibers arise
ganglion. from the cranial cervical sympathetic ganglion which is
The trigeminal ganglion is connected to the lacrimal nucleus the upper most ganglion of the ganglionic trunk and
of the facial nerve and the pons by internuncial neurons travels into the plexus of nerves around the internal
carotid artery and they join the maxillary nerve,
Impulses are then directed by the trigeminal ganglia to the
zygomatic nerve, zygomatico-temporal nerve and
lacrimal nucleus
finally the lacrimal nerve
In humans there’s is a connection b/n the hypothalamus and the
o Sympathetic simulation increases tear secretion by
lacrimal nucleus causing emotional tears; affecting the vascular supply to the lacrimal gland as
There’s also a connection in the olfactory system and lacrimal well as activating a G-protein pathway
nucleus causing “Wasabi tears”
*The lacrimal nerve is the smallest of the ophthalmic nerve.
Figure 25. Diagram of the Sympathetic Innervation
Accessory Glands
Figure 23. Diagram of the Lacrimal Gland Innervation Glands of Krause
- Subconjunctival connective tissue of the superior
Lacrimal Gland Innervation fornix
Efferent (Parasympathetic or Glands of Wolfring
Secretomotor) - AKA Glands of Claccio
o Facial Nerve (CN VII): originate in the superior Both glands are histologically identical to the lacrimal gland
salivatory nucleus
o The efferent post ganglionic parasympathetic impulses
are transmitted via the spheno-palatine nerve to the
zygomatic nerve, which is a branch of the maxillary
division of the trigeminal nerve then passes into the
zygomatic temporal nerve which reaches the lacrimal
gland
o The zygomatic temporal nerve also gives off recurrent
branch to the lacrimal nerve from which the efferent
fibers terminate in the lacrimal gland
Figure 26. Accesspry Glands of the Lacrimal Gland
D. OSTEOLOGY
Figure 24. Diagram of the Sympathetic Innervation
Figure 27. Structures in the Lacrimal Sac Fossa
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 12 of 14
Tear Film
Lacrimal Sac Fossa Composition:
- A depression in the inferomedial orbital rim Oily Outer Layer/Lipid Layer
- Formed by the maxillary and lacrimal bones o Meibomian Glands
Boundaries o Reduces evaporation of underlying aqueous layer
o Anterior Lacrimal Crest (Maxillary Bone) o Prevent aqueous layer from drying
o Dry eye syndrome
o Posterior Lacrimal Crest (Lacrimal Bone)
Aqueous Layer (90% of pre-corneal tear film)
Measurement
o Main and accessory lacrimal glands
o 16 mm high
o 10% evaporated; goes up to 20% when aging
o 4-9 mm wide
o 2 mm deep o Basal secretion: Accessory glands
o Reflex: Main Lacrimal
Excretory Component Mucin Layer or Mucous Layer
Punctum o Goblet cells found in conjunctiva and tarsus
o Surrounded by the ampulla o Distribute tears to entire ocular surface
o ~0.3 mm in diameter o To adhere with ocular surface
o From the medial canthus
Inferior punctum is 6.5 mm
Superior punctum is 6 mm
Canaliculi - collect tears into openings on the lid called the
puncta, and convey them to the lacrimal sacs
Path
From ampulla, it travels vertically 2mm > turns 90°
>travels horizontally 8-10mm>Then attaches to the
lacrimal sac
The upper and lower canaliculi can connect to the lacrimal
sac in three ways:
o Type A: Connection where there is a common
canaliculus
o Type B: Attachment of both upper and lower
canaliculi at a common opening Figure 24. Layers of the Tear Film
o Type C: The canaliculi enter the lacrimal sac D. LACRIMAL PUMP
separately Responsible for draining out tears in the eyes; lacrimal tear
90% of the population form a common canaliculus (the pump works by blinking mechanism
rest insert to the lacrimal sac separately) When the lids close, the pretarsal oribucalirus contracts and
Valve of Rosenmuller compresses the ampulla. It shortens the canaliculus and
Mucosal fold located between the common canaliculus moves the punctum medially. The lacrimal sac then expands
and lacrimal sac and creates negative pressure, drawing fluid from the
Prevents tear reflux from the sac back to the canaliculi canaliculus into the sac. When the lids open, the muscle
1-way valve then relaxes and the lacrimal sac collapses. The tears are
Lacrimal Sac then forced into the nose and then the punctum moves
Found in the anterior medial orbit laterally and the tears enter the canaliculus.
10-15 mm long Tears flow
Collect tears and release them into the nasolacrimal duct o The upp
when one blinks (contraction of the orbicularis oculi muscle) canaliculi
Lies within the lacrimal fossa
o Capillarity and suction
Pretarsal portion of the orbicularis oculi - causes the
Eyes Close
compression of the sac
o Pretarsal orbicularis compress the ampullae and
Nasolacrimal Duct
shortens and compresses the canaliculae and puncta
- convey tears from lacrimal sacs to the inferior meatus of the nasal
medially
cavity
o 2 Parts: o Lacrimal part of the orbicularis contracts tears >
- Intraosseous: 12 mm nasolacrimal duct > nose
Eyes Open
- Meatal: 5 mm
o Muscles relax > canaliculi and sac expand (negative
o Opens into the ostium under the inferior turbinate
(inferior meatus) pressure) + capillarity = tears into the sac
o Ostium E. THEORIES OF THE LACRIMAL PUMP
- Located anterior to the inferior nasal meatus, ~2.5 cm Jones Theory
posterior the nares o Eyelid closure causes negative pressure inside the
- Covered by mucosal fold called the Valve of Hasner lacrimal sac
o Valve of Hasner Rosengen-Doane’s Theory
- Opens 3-4 weeks of life o Eyelid opening causes negative pressure inside the
- Can be delayed 6-9 months to a year lacrimal sac
- Clinical significance: Epiphora-excessive tears Tricompartment Theory of Becker
o Eyelid closure causes negative pressure in the superior
aspect of the lacrimal sac
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 13 of 14
CHECKPOINT!
1. Chambers of the eyeball which contain aqueous humor
2. Space which communicates with the scleral veins and aqueous humor
3. Structure which provides blood supply to the retina
4. Longest and thinnest extraocular muscle
5. Structures responsible for the production of aqueous humor
6. Meeting point of the upper and lower lids
7. 2 glands that prevent evaporation of the tear film
8. Important landmark in lid laceration repair
9. Condition where the eyeball sinks into the orbit
10. Medial lymphatic drainage of the eyelid
11. True / False: Surgeries or wounds involving the eyelids heal rapidly
11. True
10. Submandibular Lymph Node
9. Enophthalmos
8. Central orbital fat pad
7. Glands of Zeis; Glands of Moll
6. Canthi
5. Ciliary Body
4. Superior rectus
3. Choroid
2. Schlemm’s canal
1. Anterior and Posterior chambers o
[CORPUZ, TOMAS, TABANGCURA, GARALDE, RABBON, RAMIL] Page 14 of 14
You might also like
- Lesson 1 EyesDocument8 pagesLesson 1 EyesMARY JANE ANGELICA SEVANo ratings yet
- 3013 - Bookfile 200 900 (200 400)Document201 pages3013 - Bookfile 200 900 (200 400)gemapesfNo ratings yet
- 2023.neuroscience - trans11.PosteriorFossaLevelCerebellar Vestibular and Auditory SystemDocument15 pages2023.neuroscience - trans11.PosteriorFossaLevelCerebellar Vestibular and Auditory SystemstellaNo ratings yet
- Semilunar Coronally Repositioned FlapDocument5 pagesSemilunar Coronally Repositioned FlapTarun Kumar Bhatnagar100% (1)
- Agri 31 Scientific ReportDocument8 pagesAgri 31 Scientific ReportJave DecioNo ratings yet
- Guder Et Al Recommendations of The Working Group On Preanalytical Quality of The German Society For Clinical Chemistry and Lab Medecine EnglishDocument42 pagesGuder Et Al Recommendations of The Working Group On Preanalytical Quality of The German Society For Clinical Chemistry and Lab Medecine EnglishLorena Ek MaciasNo ratings yet
- Anatomia para Estética Parte 1Document45 pagesAnatomia para Estética Parte 1Rodolpho VilelaNo ratings yet
- Clinical Anatomy of The Eyelids: Orbit and OculoplasticsDocument5 pagesClinical Anatomy of The Eyelids: Orbit and OculoplasticsFelyana GunawanNo ratings yet
- OPHTHA - 1.07a - Lens and Cataract-2 PDFDocument7 pagesOPHTHA - 1.07a - Lens and Cataract-2 PDFNoel QuintonNo ratings yet
- OphthalmologyDocument102 pagesOphthalmologyPatty Reyes100% (1)
- Physiology of Vision: Angelie Rose C. Guzman, Rph. MDDocument74 pagesPhysiology of Vision: Angelie Rose C. Guzman, Rph. MDPrixie AntonioNo ratings yet
- Ophthalmology 1.02 Review of The Anatomy and Physiology of The Eye - Dr. LitaoDocument7 pagesOphthalmology 1.02 Review of The Anatomy and Physiology of The Eye - Dr. LitaoMark AceNo ratings yet
- 397.001 - Orthopedics) Rotator Cuff TearDocument11 pages397.001 - Orthopedics) Rotator Cuff Tearvkpremiyahoo.comNo ratings yet
- B20M01 Clinical Anatomy and Physiology of The EyeDocument12 pagesB20M01 Clinical Anatomy and Physiology of The EyeVanessa YunqueNo ratings yet
- The Pelvis & Perineu M: Able of OntentsDocument23 pagesThe Pelvis & Perineu M: Able of OntentsWaqar WikiNo ratings yet
- Development of The Pig EmbryoDocument11 pagesDevelopment of The Pig Embryovada_soNo ratings yet
- Upper Extremity (Anatomy)Document17 pagesUpper Extremity (Anatomy)Margareth Christine CusoNo ratings yet
- Epithelial-Cells 2Document5 pagesEpithelial-Cells 2Edeilaine JadraqueNo ratings yet
- FK Unissula 2010: Feat. Anatomy LaboratoryDocument48 pagesFK Unissula 2010: Feat. Anatomy LaboratoryTeguh PambudiNo ratings yet
- Muscles EscanillaDocument9 pagesMuscles EscanillaESCANILLA CRISTINENo ratings yet
- List The Neighboring Anatomical Regions and Structures Related To Each Wall of The OrbitDocument9 pagesList The Neighboring Anatomical Regions and Structures Related To Each Wall of The Orbitkep1313No ratings yet
- SFSFSFDocument6 pagesSFSFSFFatima MartinezNo ratings yet
- Imaging of Adult Ocular and Orbital PathologyDocument29 pagesImaging of Adult Ocular and Orbital PathologyLAURA CAMILA ARAGONES VARGASNo ratings yet
- Cho 2008Document15 pagesCho 2008Guilherme de FreitasNo ratings yet
- The Eye: OphthalmologyDocument12 pagesThe Eye: OphthalmologyAshley DayagNo ratings yet
- The Skull and Vicsceral Skeleton PDFDocument13 pagesThe Skull and Vicsceral Skeleton PDFAmberValentineNo ratings yet
- OutlineDocument43 pagesOutlineJulia MundoNo ratings yet
- Anatomy and Physiology of The EyesDocument6 pagesAnatomy and Physiology of The EyesRiyan WirawanNo ratings yet
- Eye Anatomy 2Document28 pagesEye Anatomy 2jckjgx9q2bNo ratings yet
- Abdominal Wall, Omentum, Mesentery and RetroperitoneumDocument8 pagesAbdominal Wall, Omentum, Mesentery and RetroperitoneumRae Marie AquinoNo ratings yet
- Unit 8 Exercise 15Document22 pagesUnit 8 Exercise 15Andrei AlvaradoNo ratings yet
- Hypothalamus and Pituitary GlandDocument9 pagesHypothalamus and Pituitary GlandLANCE GILL Tolentino100% (3)
- Mata (Basics)Document2 pagesMata (Basics)ravyryNo ratings yet
- Anatomy of The Eye - DsaycoDocument4 pagesAnatomy of The Eye - DsaycoAnnaNo ratings yet
- Human Eye - Britannica Online EncyclopediaDocument83 pagesHuman Eye - Britannica Online EncyclopediaCucută Alexandru-DanielNo ratings yet
- Chapter 6. Axial Skeleton: I. Radiographic AnatomyDocument11 pagesChapter 6. Axial Skeleton: I. Radiographic AnatomyRindha Dwi SihantoNo ratings yet
- Ninja Nerd Embryology Notes CompleteDocument111 pagesNinja Nerd Embryology Notes Completezipporahwaithera404No ratings yet
- 21 Neural Control N Coordination-NCERT Questions N AnswersDocument6 pages21 Neural Control N Coordination-NCERT Questions N AnswersGuru SrinivaasNo ratings yet
- 270 - Embryology Physiology) Development & Embryology of The GI Tract - Part 1Document3 pages270 - Embryology Physiology) Development & Embryology of The GI Tract - Part 1Zade BawiNo ratings yet
- MBR 2019 - Anatomy Handouts - CompleteDocument88 pagesMBR 2019 - Anatomy Handouts - CompleteNica Lopez Fernandez100% (4)
- Eye and OrbitDocument30 pagesEye and OrbitMyat NyanNo ratings yet
- General Anatomy IiDocument5 pagesGeneral Anatomy IijamjamjamNo ratings yet
- Histology of The Eye Lectured By: Dr. Gonzales Transcribed By: Angelo Louise A. Sayo Proofread By: Kaye Reyes & Erina ValdesDocument12 pagesHistology of The Eye Lectured By: Dr. Gonzales Transcribed By: Angelo Louise A. Sayo Proofread By: Kaye Reyes & Erina ValdesKaye NeeNo ratings yet
- EENT NotesDocument12 pagesEENT NotesMhae TabasaNo ratings yet
- OT1024 - 1S1L - Organization of The Nervous System-CompressedDocument14 pagesOT1024 - 1S1L - Organization of The Nervous System-CompressedRidz FNo ratings yet
- OrbitDocument10 pagesOrbitayrahrahmanNo ratings yet
- MBR 2019 - Anatomy Handouts - Complete (1) JKNDocument88 pagesMBR 2019 - Anatomy Handouts - Complete (1) JKNSeven EightNo ratings yet
- Buccal Fat Pad Flap-1Document5 pagesBuccal Fat Pad Flap-1Sooraj SNo ratings yet
- M.03 Head and NeckDocument17 pagesM.03 Head and NeckRaymund Dan AldabaNo ratings yet
- E3.2 EarsDocument5 pagesE3.2 EarsCearlene GalleonNo ratings yet
- Peggy Mason Chapter 6 Brainstem Notes - For MergeDocument37 pagesPeggy Mason Chapter 6 Brainstem Notes - For MergeLydia RousseauNo ratings yet
- Visual and Lacrimal AppratusDocument45 pagesVisual and Lacrimal AppratusAzman Bin KadirNo ratings yet
- 2.3 Animal Cells and TissueDocument13 pages2.3 Animal Cells and TissueDash ShaaNo ratings yet
- Chapter 36 Internal EarDocument23 pagesChapter 36 Internal EarMohan PalanimalaiNo ratings yet
- Chapter 3 - Uvea - 2012 - Clinical Anatomy and Physiology of The Visual SystemDocument21 pagesChapter 3 - Uvea - 2012 - Clinical Anatomy and Physiology of The Visual SystemAldo CortesNo ratings yet
- Anatomy of The EyeDocument13 pagesAnatomy of The EyeJerome GeronimoNo ratings yet
- XI CH 10 Animal TissueDocument11 pagesXI CH 10 Animal Tissueprachi98601No ratings yet
- EAR Anatomy, Physiology, Embryology & Congenital AnomalyDocument6 pagesEAR Anatomy, Physiology, Embryology & Congenital AnomalyThakoon TtsNo ratings yet
- He Kull: Key FactsDocument202 pagesHe Kull: Key FactsRulen FailNo ratings yet
- Handout - Gross & Microscopic Anatomy of Ear and EyeDocument211 pagesHandout - Gross & Microscopic Anatomy of Ear and EyeWongelNo ratings yet
- Brain VentriclesDocument40 pagesBrain Ventriclesahmad72 raza72No ratings yet
- RBC Indices & ESRDocument23 pagesRBC Indices & ESRPamela BesanaNo ratings yet
- Woreta Health Science and Business College Anatomy and Physiology of Autonomic Nervous System For Level IV Pharmacy StudentsDocument36 pagesWoreta Health Science and Business College Anatomy and Physiology of Autonomic Nervous System For Level IV Pharmacy StudentsEyachew TewabeNo ratings yet
- Phloem Loading and UnloadingDocument4 pagesPhloem Loading and Unloadingtshepiso0% (1)
- Drug Induced Liver DisordersDocument6 pagesDrug Induced Liver DisordersGeethika GummadiNo ratings yet
- Structural and Molecular Bases of Cardiac Inward Rectifier Potassium Channel FunctionDocument11 pagesStructural and Molecular Bases of Cardiac Inward Rectifier Potassium Channel FunctionArmando RodriguezNo ratings yet
- (HST) Lab Le 2 SamplexDocument12 pages(HST) Lab Le 2 SamplexFrances Dei100% (1)
- IA Text GeneratorDocument1 pageIA Text GeneratorsteeloramaNo ratings yet
- Laboratory 3 - Blood Vessels I - Histology of Artery and Vein ArteriesDocument28 pagesLaboratory 3 - Blood Vessels I - Histology of Artery and Vein ArteriesSofia NNo ratings yet
- 1st Puc Biology First Test Question Paper Eng Version 2019-20 MandyaDocument1 page1st Puc Biology First Test Question Paper Eng Version 2019-20 MandyaBhuvanesh .DNo ratings yet
- Chapter 10Document11 pagesChapter 10JohnNo ratings yet
- Ascorbate and Glutathione: Keeping Active Oxygen Under ControlDocument31 pagesAscorbate and Glutathione: Keeping Active Oxygen Under ControlPhilip Blair OngNo ratings yet
- Animal Classification (Porifera-Echinodermata)Document164 pagesAnimal Classification (Porifera-Echinodermata)9415697349No ratings yet
- Introduction To Echocardiography 2Document26 pagesIntroduction To Echocardiography 2Sandra GutierrezNo ratings yet
- Renal Blood Flow Until Regulation of RBF and GFRDocument5 pagesRenal Blood Flow Until Regulation of RBF and GFRDoogie ReynaldoNo ratings yet
- Drug Study Vitamin C + ZincDocument2 pagesDrug Study Vitamin C + ZincKrizzia FosterNo ratings yet
- Taleem City Institute: Ameenpur, Faisalabad 03126987979Document26 pagesTaleem City Institute: Ameenpur, Faisalabad 03126987979Zohaib KhanNo ratings yet
- Jsu BioDocument11 pagesJsu BioMuhammad Hatta HamzahNo ratings yet
- Pharmacological and Toxicological Screening Methods I (MPL 103T)Document50 pagesPharmacological and Toxicological Screening Methods I (MPL 103T)Sandeep MewadaNo ratings yet
- Anatomy and Physiology Foundations For The Health Professions 1st Edition Deborah Roiger Solutions Manual 1Document37 pagesAnatomy and Physiology Foundations For The Health Professions 1st Edition Deborah Roiger Solutions Manual 1tabitha100% (29)
- Circulatory MatchDocument2 pagesCirculatory MatchJinky AydallaNo ratings yet
- Jayasankara - Reddy@ Christuniversity - in Padma - Kumari@chri Stuniversity - inDocument5 pagesJayasankara - Reddy@ Christuniversity - in Padma - Kumari@chri Stuniversity - inN SINDHU 2237406No ratings yet
- 1st Prof + Supl Questions Aio 2010-21Document87 pages1st Prof + Supl Questions Aio 2010-21Kashif GhazaliNo ratings yet
- Frith & Frith, 2012 Mecanismos de La Cognición Social.Document30 pagesFrith & Frith, 2012 Mecanismos de La Cognición Social.Ricardo Jose De LeonNo ratings yet
- Spinreact ProductlistDocument52 pagesSpinreact ProductlistARMELFAGNINOUNo ratings yet
- Kcse Biology Revision BookletDocument35 pagesKcse Biology Revision BookletTudorNedelcuNo ratings yet
- Liddle, Gitelman, BarterDocument2 pagesLiddle, Gitelman, BarterHildemaro GutierrezNo ratings yet
- Fifteen Years of Explaining Pain, The Past, Present, and Future 2016Document7 pagesFifteen Years of Explaining Pain, The Past, Present, and Future 2016Gilbert ThierryNo ratings yet