Professional Documents
Culture Documents
Como Realizar Una Biopsia en Penfigoide Ocular
Uploaded by
Miguel HernandezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Como Realizar Una Biopsia en Penfigoide Ocular
Uploaded by
Miguel HernandezCopyright:
Available Formats
Downloaded from bjo.bmj.com on August 26, 2014 - Published by group.bmj.
com
Education
Oral prednisolone 1 mg/kg/day on a tapering course over
How to do conjunctival and buccal 6 weeks, and mycophenolate 1 g twice daily were commenced.
biopsies to investigate cicatrising Nine months later, left upper lid entropion surgery was per-
formed with excellent results.
conjunctivitis: improving the
QUESTIONS (FOR ANSWERS SEE 537)
diagnosis of ocular mucous 1. What investigations are needed to identify the cause of cica-
membrane pemphigoid trising conjunctivitis?
2. Describe how to do conjunctival and buccal biopsies?
3. How would you manage the patient if you suspect ocular
CASE MMP, but all immunopathology is negative?
A 79-year-old female presented with a 3-year history of trichia-
sis and red eyes (figure 1A). Multiple operations for entropion Arturo E Grau,1 Jane Setterfield,2,3 Valerie P J Saw1,4
and trichiasis had been carried out previously, and a conjunctival 1
Cornea and External Disease Service, Moorfields Eye Hospital NHS Foundation
biopsy investigating mucous membrane pemphigoid (MMP), Trust, London, UK
2
had been negative. Her right eye was blind due to retinal Department of Oral Medicine, Guys Hospital, Guys and St Thomas’, NHS
Foundation Trust, London, UK
detachment and glaucoma. Acuity was light perception in the 3
St John's Institute of Dermatology, Kings College London, London, UK
right eye (OD) and 6/12 in the left eye (OS). There was active 4
NIHR Biomedical Research Centre at Moorfields Eye Hospital and UCL Institute of
inflammation and bilateral inferior symblepharon, left upper lid Ophthalmology, London, UK
entropion and trichiasis. There were no systemic features of Correspondence to Dr Valerie P J Saw, Cornea and External Disease Service,
MMP. Moorfields Eye Hospital, 162 City Road, London EC1V 2PD, UK; v.saw@ucl.ac.uk
Conjunctival and buccal mucosa biopsies were undertaken.
Serum was tested for indirect inmunofluorescence. Conjunctival Acknowledgements We gratefully acknowledge the support of John Dart in this
manuscript. We are also grateful for the expert advice of Professor Enno Schmidt
and serum immunofluorescence were negative, but buccal (Lubeck, Germany) regarding immunofluorescence testing. Valerie Saw is supported
mucosa showed linear IgG and IgA staining along the basement by the NIHR Biomedical Research Centre at Moorfields Eye Hospital and the UCL
membrane zone (BMZ), consistent with MMP. Institute of Ophthalmology.
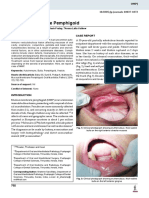
Figure 1 (A) The patient’s cicatrised inflamed left eye. (B) Taking a biopsy from the eye (not the same patient). If the speculum does not fit,
manually open the lids. (C) Taking a buccal biopsy. (D) Michel’s transport medium. (E) Direct immunofluorescence showing linear IgG, IgA along the
basement membrane zone.
530 Grau AE, et al. Br J Ophthalmol April 2013 Vol 97 No 4
Downloaded from bjo.bmj.com on August 26, 2014 - Published by group.bmj.com
Education
Contributors VPJS initiated the concept of the paper, drafted and revised the Provenance and peer review Not commissioned; internally peer reviewed.
paper. She is guarantor. AEG drafted the paper. JS initiated the concept of taking To cite Grau AE, Setterfield J, Saw VPJ. Br J Ophthalmol 2013;97:530–531.
buccal biopsies in ocular patients who have no mouth symptoms or signs, provided
her own unpublished data for the paper discussion, and revised the draft paper. JD’s
patients were used for JS’s data, and he commented on the draft paper. Published Online First 19 January 2013
Competing interests None. Br J Ophthalmol 2013;97:530–531. doi:10.1136/bjophthalmol-2012-302963
Patient consent Obtained.
Grau AE, et al. Br J Ophthalmol April 2013 Vol 97 No 4 531
Downloaded from bjo.bmj.com on August 26, 2014 - Published by group.bmj.com
Education
ANSWERS (FOR QUESTIONS SEE 530) Ideally, biopsy the upper bulbar conjunctiva where upper
1. Ascertaining which of the causes of cicatrising conjunctivitis eyelid coverage improves healing. Concerns about adverse con-
in table 1 is responsible requires: sequences in the event of glaucoma surgery have not been
i. A thorough history of previous conjunctivitis (adeno- observed. Avoid inferior bulbar conjunctiva because exposure,
viral, trachomatous, vernal) or skin disorders (Stevens– blepharitis and dry eye can compromise healing. Avoid biopsies
Johnson, ezcema) and examination for typical features in the conjunctival fornix, as these induce further scarring.1
of allergy, Sjögren’s, rosacea. Ask about extraocular After anaesthetic drops, a cotton bud soaked in anaesthetic
MMP symptoms. numbs the chosen biopsy site. If the conjunctiva is too con-
ii. Referral to a specialist for biopsy of any skin or mouth tracted, manually open the eyelids rather than using a specu-
lesions lum. Spring scissors and non-crush forceps are used to take a
iii. Serum connective tissue disease screening 2–4 mm biopsy (figure 1C). Ensure that the size of the biopsy
iv. Conjunctival biopsies in appropriate medium, for is adequate, including the BMZ. Chloramphenicol ointment
instance, Michel’s medium (figure 1D) for direct is applied to the eye twice daily for 7 days, along with pred-
immunofluorescence (DIF). Consider a formalin biopsy nisolone 0.5% or dexamethasone 0.1% drops, four times per
for any suspicion of neoplasia, sarcoidosis, or atopy. day for 4 weeks.
v. A buccal mucosal biopsy is low risk and can be positive The main risk associated with a conjunctival biopsy is
in MMP when conjunctival biopsies are negative. inducing conjunctival inflammation and, potentially,
vi. If testing is available, take serum for IIF. scarring.
vii. Establish whether the conjunctival cicatrisation is pro- This is avoided by commencing immunosuppression at
gressive, or static. the time of biopsy, and a 4-week course of topical steroids.
2. If the patient’s eyes are severely inflamed, that is, active cicatris- When done carefully, conjunctival biopsy is well tolerated
ing conjunctivitis, commence oral immunosuppression on the and safe.2
day of the biopsy. Use an experienced immunofluorescence Carrying out a buccal mucosal biopsy at the time of
laboratory, discuss with them beforehand and obtain Michel’s taking conjunctival biopsies, regardless of whether patients
medium. have oral disease or not, is simple and low risk. Inject 2 ml
Table 1 Differential diagnosis of cicatrising conjunctivitis
Static or very slowly progressive conjunctival scarring Progressive conjunctival scarring
1. Trauma: physical, chemical, thermal, radiation injury, artefacta 1. Neoplasia: squamous cell carcinoma, sebaceous cell carcinoma, lymphoma
2. Infection: 2. Mucous membrane pemphigoid (MMP).
Trachoma A. Ocular MMP/ocular cicatricial pemphigoid
Membranous streptococcal conjunctivitis B. Ocular MMP associated with other disorders:
Adenoviral conjunctivitis Linear IgA disease
Corynebacterium diphtheria Epidermolysis bullosa acquisita
Chronic mucocutaneous candidiasis Paraneoplastic MMP (anti-laminin 332 MMP)
Drug-induced ocular MMP
Stevens–Johnson syndrome
3. Allergic eye disease: 3. Other mucocutaneous and immunobullous disorders:
Atopic keratoconjunctivitis Mucocutaneous disorders: Lichen planus
Vernal keratoconjunctivitis Immunobullous disorders: Paraneoplastic pemphigus
4. Drug-induced conjunctival cicatrisation (DICC)*†
5. Mucocutaneous disorders:
Stevens–Johnson syndrome and TEN*
Graft-versus-host disease
Discoid and systemic lupus erythematosus‡
6. Immunobullous disorders:
Linear IgA disease*
Epidermolysis bullosa acquisita*
Bullous pemphigoid
Pemphigus vulgaris
Dermatitis herpetiformis
7. Systemic disease:
Rosacea
Sjögren’s syndrome
Sarcoidosis†
Scleroderma
Wegener’s granulomatosis
Inflammatory bowel disease
Ectodermal dysplasia*
Immune complex diseases
Porphyria cutanea tarda
Erythroderma ichthyosiform congenita
*A subset of patients with these diseases may develop autoantibody-positive progressive conjunctival scarring similar to ocular MMP.
†Associated with granulomatous conjunctival inflammation.
‡Rare cases can develop progressive scarring.
Grau AE, et al. Br J Ophthalmol April 2013 Vol 97 No 4 537
Downloaded from bjo.bmj.com on August 26, 2014 - Published by group.bmj.com
Education
lignocaine with adrenaline using a 25 G needle, into the buccal were positive in 3 / 7 (43%) Additionally, in patients with pre-
mucosa. Avoid the parotid duct, which opens opposite the 2nd dominantly ocular MMP (n=14) and a history of multisite
upper molar. Use a 4 mm dermal trephine (figure 1C) to disease, a buccal biopsy was positive in 5 / 7 (71%) patients com-
create a biopsy punch, then excise with scissors and forceps. pared with conjunctiva 6 / 10 (60%).
Place haemostatic pressure using gauze swabs for 1 min. No The presence of linear BMZ IgG and IgA in our case con-
suture is necessary, and antiseptic mouthwash is not usually firmed the diagnosis of MMP.5 Conjunctiva is fragile and difficult
required. to process for immunofluorescence; it is thought that this may
3. If both the conjunctival and buccal biopsies are negative, and partly be the reason for only 50–86%6 7 of conjunctival DIF
the patient has no skin lesions for biopsy, and serology has biopsies being positive for MMP, in contrast to almost 100% of
not shown any circulating BMZ autoantibodies, then provid- biopsies from non-ocular sites including buccal mucosa, where
ing other causes of conjunctival scarring (see table 1) have examination of the BMZ is easier given the nature of the tissue.8
been excluded, a clinical diagnosis of ‘autoantibody-negative’ In summary, the purpose of this article has been twofold: first,
MMP-like ocular disease can be made,3 based on evidence of to educate clinicians about how to do conjunctival biopsies and
progressive scarring and typical clinical signs. These patients avoid complications and second, to increase awareness about a
are managed in a similar manner to ‘autoantibody-positive’ simple buccal mucosal biopsy, which can support the diagnosis in
ocular MMP. Studies investigating these ‘autoantibody- the event of the conjunctival biopsies being negative.
negative’ patients, regarding differences in clinical phenotype
and response to therapy, are currently being conducted.
REFERENCES
1 Wright P. Cicatrizing conjunctivitis. Trans Ophthalmol Soc UK 1986;105(Pt 1):1–17.
DISCUSSION 2 Frith PA, Venning VA, Wojnarowska F, et al. Conjunctival involvement in cicatricial
A recent study investigating the incidence of cicatrising conjunc- and bullous pemphigoid: a clinical and immunopathological study. Br J Ophthalmol
tivitis4 highlighted that 10% of ocular MMP cases did not have 1989;73:52–6.
3 Saw VPJ, Dart JKG. Ocular cicatricial pemphigoid - Author Reply. Ophthalmology
a conjunctival DIF biopsy where there were no extraocular man- 2008;115:1640–1.
ifestations supporting the diagnosis, and there was a median 4 Radford CF, Rauz S, Williams GP, et al. Incidence, presenting features, and diagnosis
delay of 7.5 months (up to 10 years) before the diagnosis was of cicatrising conjunctivitis in the United Kingdom. Eye (Lond) 2012;26:1199–208.
made. Often clinicians are cautious about taking conjunctival 5 Chan LS, Ahmed AR, Anhalt GJ, et al. The first international consensus on mucous
membrane pemphigoid: definition, diagnostic criteria, pathogenic factors, medical
biopsies as they fear worsening the disease. We hope that this
treatment, and prognostic indicators. Arch Dermatol 2002;138:370–9.
description of how to take a conjunctival biopsy will help to 6 Bernauer W, Elder MJ, Leonard JN, et al. The value of biopsies in the evaluation of
educate and encourage better assessment and investigation of chronic progressive conjunctival cicatrisation. Graefes Arch Clin Exp Ophthalmol
these patients. 1994;232:533–7.
Setterfield, Dart et al have conducted studies (unpublished) in 7 Thorne JE, Anhalt GJ, Jabs DA. Mucous membrane pemphigoid and
pseudopemphigoid. Ophthalmology 2004;111:45–52.
patients with pure ocular MMP (n=7), and have determined 8 Setterfield J, Shirlaw PJ, Kerr-Muir M, et al. Mucous membrane pemphigoid: a dual
that a biopsy from apparently healthy buccal mucosa for DIF circulating antibody response with IgG and IgA signifies a more severe and persistent
was positive in 3 / 5 (60%) patients, while conjunctival biopsies disease. Br J Dermatol 1998;138:602–10.
538 Grau AE, et al. Br J Ophthalmol April 2013 Vol 97 No 4
Downloaded from bjo.bmj.com on August 26, 2014 - Published by group.bmj.com
How to do conjunctival and buccal biopsies
to investigate cicatrising conjunctivitis:
improving the diagnosis of ocular mucous
membrane pemphigoid
Arturo E Grau, Jane Setterfield and Valerie P J Saw
Br J Ophthalmol 2013 97: 530-531 originally published online January
19, 2013
doi: 10.1136/bjophthalmol-2012-302963
Updated information and services can be found at:
http://bjo.bmj.com/content/97/4/530.full.html
These include:
References This article cites 7 articles, 1 of which can be accessed free at:
http://bjo.bmj.com/content/97/4/530.full.html#ref-list-1
Email alerting Receive free email alerts when new articles cite this article. Sign up in
service the box at the top right corner of the online article.
Topic Articles on similar topics can be found in the following collections
Collections
Conjunctiva (199 articles)
Ocular surface (545 articles)
Eye Lids (49 articles)
Angle (903 articles)
Glaucoma (888 articles)
Intraocular pressure (900 articles)
Epidemiology (899 articles)
Retina (1404 articles)
Notes
To request permissions go to:
http://group.bmj.com/group/rights-licensing/permissions
To order reprints go to:
http://journals.bmj.com/cgi/reprintform
To subscribe to BMJ go to:
http://group.bmj.com/subscribe/
You might also like
- Conjunctivitis As A Manifestation of Wegener 'S GranulomatosisDocument5 pagesConjunctivitis As A Manifestation of Wegener 'S GranulomatosisAsd DsaNo ratings yet
- Optic Neuritis in Leprosy - 231215 - 030338Document2 pagesOptic Neuritis in Leprosy - 231215 - 030338dr samyNo ratings yet
- Rare Paediatric Ossifying Fibroma CaseDocument7 pagesRare Paediatric Ossifying Fibroma CaseRika Sartyca IlhamNo ratings yet
- Preserved Amniotic Membrane Improves Corneal HealingDocument10 pagesPreserved Amniotic Membrane Improves Corneal HealingDitha FadhilaNo ratings yet
- The Pathogenesis of Optic Neuritis Caused by Angiostrongylus Cantonensis in BALB/c MiceDocument12 pagesThe Pathogenesis of Optic Neuritis Caused by Angiostrongylus Cantonensis in BALB/c Miceracut_khansatraNo ratings yet
- Laporan Kasus Ulkus Kornea Jamur Dengan Hipopion .Eva RiantiDocument21 pagesLaporan Kasus Ulkus Kornea Jamur Dengan Hipopion .Eva RiantiBenk Setsuna F. SeieiNo ratings yet
- Intralesional Ethanol For An Unresectable Epithelial Inclusion CystDocument2 pagesIntralesional Ethanol For An Unresectable Epithelial Inclusion CystJave GajellomaNo ratings yet
- 08gingival MyofibromasDocument5 pages08gingival MyofibromasAlejandro RuizNo ratings yet
- Entropion 3 PDFDocument5 pagesEntropion 3 PDFdhitadwynNo ratings yet
- Konjungtivitis GonoreDocument2 pagesKonjungtivitis Gonorefk unswagatiNo ratings yet
- Tatalaksana Ulkus Kornea Yang Disebabkan Oleh Methycillin Resistant Staphylococcus Haemolyticus MRSH - Mia NursalamahDocument14 pagesTatalaksana Ulkus Kornea Yang Disebabkan Oleh Methycillin Resistant Staphylococcus Haemolyticus MRSH - Mia NursalamahYA MAAPNo ratings yet
- DIAGNOSTIC APPROACH TO CORNEAL ULCERDocument13 pagesDIAGNOSTIC APPROACH TO CORNEAL ULCERAvabel Player 1No ratings yet
- 2005 Entropion CongenitalDocument2 pages2005 Entropion Congenitalsaraya amajidaNo ratings yet
- SG - PosDocument6 pagesSG - PossyenadamaraNo ratings yet
- Management of Fibrous Epulis Case ReportDocument10 pagesManagement of Fibrous Epulis Case ReportTrianita DivaNo ratings yet
- Frontal Lobe Epilepsy CasesDocument3 pagesFrontal Lobe Epilepsy CasesGautham sirivallaNo ratings yet
- Red Eye CheckDocument3 pagesRed Eye CheckkrishnaNo ratings yet
- Intravitreal Dexamethasone Reduces Inflammation in Bacterial EndophthalmitisDocument7 pagesIntravitreal Dexamethasone Reduces Inflammation in Bacterial EndophthalmitisxoxotheNo ratings yet
- Conjunctivitis Due To Neisseria Sicca: A Case Report: ReferencesDocument4 pagesConjunctivitis Due To Neisseria Sicca: A Case Report: ReferencesnidaNo ratings yet
- Chronic Conjunctivitis From A Retained Contact LensDocument4 pagesChronic Conjunctivitis From A Retained Contact Lensnana nurdahliaNo ratings yet
- Ibrahim 2009Document7 pagesIbrahim 2009MARIO STEFFANO ARCE COAQUERANo ratings yet
- Msor 000504Document3 pagesMsor 000504MudrikahHaniyahNo ratings yet
- Ijcmr 692 Jun 14Document2 pagesIjcmr 692 Jun 14Jeyachandran MariappanNo ratings yet
- Current Examination Methods of The Canine Eye: J. Beránek, P.J. VítDocument6 pagesCurrent Examination Methods of The Canine Eye: J. Beránek, P.J. VítOktavia firnandaNo ratings yet
- Ostiogenesis ImperfectaDocument4 pagesOstiogenesis Imperfectamarlon GarcíaNo ratings yet
- Journal - Bilateral Simultaneous Infective KeratitisDocument4 pagesJournal - Bilateral Simultaneous Infective KeratitisAndayanaIdhamNo ratings yet
- 46760-Article Text-56113-1-10-20091013Document4 pages46760-Article Text-56113-1-10-20091013healthnet medicalsNo ratings yet
- PIIS0008418219302121Document4 pagesPIIS0008418219302121J MNo ratings yet
- Staphylococcus Epidermidis End PDFDocument4 pagesStaphylococcus Epidermidis End PDFNisaNo ratings yet
- Congenital Lacrimal Fistula CaseDocument3 pagesCongenital Lacrimal Fistula CaseTeodorNo ratings yet
- Nej M 199804233381702Document7 pagesNej M 199804233381702Syafrial BarawasNo ratings yet
- Bron 2017Document73 pagesBron 2017Anggia BungaNo ratings yet
- Giant Hanging Melanoma of The Eye SkinDocument2 pagesGiant Hanging Melanoma of The Eye SkinRochnald PigaiNo ratings yet
- Experimental Study On Cryotherapy For Fungal Corneal Ulcer: Researcharticle Open AccessDocument9 pagesExperimental Study On Cryotherapy For Fungal Corneal Ulcer: Researcharticle Open AccessSusPa NarahaNo ratings yet
- Infection & Immunology Division: C. Oral Nonsteroidal Anti-Inflammatory Agents, With MealsDocument12 pagesInfection & Immunology Division: C. Oral Nonsteroidal Anti-Inflammatory Agents, With MealsFika RahmawatiNo ratings yet
- Frontal Sinus Mucoceles Causing ProptosisDocument4 pagesFrontal Sinus Mucoceles Causing ProptosisAji Setia UtamaNo ratings yet
- Mcculley 2012Document11 pagesMcculley 2012Luisa Mayta PitmanNo ratings yet
- Mucous Membrane Pemphigoid: 10.5005/jp-Journals-10037-1072Document4 pagesMucous Membrane Pemphigoid: 10.5005/jp-Journals-10037-1072SunilNo ratings yet
- Ocular ToxocariasisDocument2 pagesOcular ToxocariasisEnderson UsecheNo ratings yet
- Tatalaksana Ulkus Kornea Jamur Dematiaceae - Andivan RahmanDocument12 pagesTatalaksana Ulkus Kornea Jamur Dematiaceae - Andivan RahmanazkaNo ratings yet
- BachmanDocument1 pageBachmanotheasNo ratings yet
- Giansanti IOVS 2008Document6 pagesGiansanti IOVS 2008Igor VainerNo ratings yet
- Baudouin 1992Document6 pagesBaudouin 1992cherruskaNo ratings yet
- Eosinophilic Ulcer Wiley 2020Document4 pagesEosinophilic Ulcer Wiley 2020Ghea AlmadeaNo ratings yet
- A Clinicopathological Study of Vernal Conjunctivitis in Urban and Rural Areas of Eastern India: A Hospital Based StudyDocument8 pagesA Clinicopathological Study of Vernal Conjunctivitis in Urban and Rural Areas of Eastern India: A Hospital Based StudyMuhammad AbdillahNo ratings yet
- A Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaDocument2 pagesA Case of Bilateral Corneal Perforation in A Patient With Severe Dry Eye in IndiaIqbal Farid MunggaranNo ratings yet
- Should We Say NO To Body Piercing in Children? Complications After Ear Piercing in ChildrenDocument3 pagesShould We Say NO To Body Piercing in Children? Complications After Ear Piercing in ChildrenGhalyRizqiMauludinNo ratings yet
- Iannetti 2010Document4 pagesIannetti 2010FrancescFranquesaNo ratings yet
- Orbital Apex Syndrome from Herpes Zoster OphthalmicusDocument4 pagesOrbital Apex Syndrome from Herpes Zoster OphthalmicusYosiita KartinaaNo ratings yet
- Periorbital Dermoid Cyst PDFDocument3 pagesPeriorbital Dermoid Cyst PDFRicarhdo Valentino HanafiNo ratings yet
- Teknik Enukleasi Pada Penatalaksanaan Retinoblastoma - Vina Karina ApriyaniDocument15 pagesTeknik Enukleasi Pada Penatalaksanaan Retinoblastoma - Vina Karina ApriyaniandhikaNo ratings yet
- IJO-62-354 - Khaleel Al Salem., Neonatal Orbital AbcessDocument4 pagesIJO-62-354 - Khaleel Al Salem., Neonatal Orbital Abcesssigitdwipramono09No ratings yet
- Tatalaksana Ulkus Kornea Jamur Dematiaceae - Madona DeboraDocument14 pagesTatalaksana Ulkus Kornea Jamur Dematiaceae - Madona DeboraRagil YuliantoNo ratings yet
- Ojoph 2022111815222395Document12 pagesOjoph 2022111815222395budi rahmawatiNo ratings yet
- V 7 Aop 191Document3 pagesV 7 Aop 191Sekar EkaperdanaNo ratings yet
- Schiefer 2016Document16 pagesSchiefer 2016Eric PavónNo ratings yet
- Pemphigus Vulgaris Confined To The Gingiva: A Case Report: By: Juli AnnisaDocument12 pagesPemphigus Vulgaris Confined To The Gingiva: A Case Report: By: Juli AnnisahilyaNo ratings yet
- Nearwork-Induced Transient Myopia in Preadolescent Hong Kong ChineseDocument6 pagesNearwork-Induced Transient Myopia in Preadolescent Hong Kong ChineseRosaliaNo ratings yet
- Epidemic Keratoconjunctivitis Complicated by Alcaligenes Xylosoxidans InfectionDocument2 pagesEpidemic Keratoconjunctivitis Complicated by Alcaligenes Xylosoxidans InfectionRita HastaNo ratings yet
- Laporan PJ Kefarmasian 2023 (Maret)Document8 pagesLaporan PJ Kefarmasian 2023 (Maret)kevinvngzNo ratings yet
- Remote Area First Aid - ST John SADocument1 pageRemote Area First Aid - ST John SAGay McdonaldNo ratings yet
- Malignant Disease of The JawsDocument26 pagesMalignant Disease of The JawsRawda NajjarNo ratings yet
- Continuous Passive Motion (CPM) : Theory and Principles of Clinical ApplicationDocument10 pagesContinuous Passive Motion (CPM) : Theory and Principles of Clinical ApplicationlaurentiaNo ratings yet
- Systemic Revision Notes FRCSDocument279 pagesSystemic Revision Notes FRCShaneefmdfNo ratings yet
- Pre Transfusion Test Flow ChartDocument1 pagePre Transfusion Test Flow ChartCatherine Constantino BaintoNo ratings yet
- Sheathed and unsheathed filarial wormsDocument2 pagesSheathed and unsheathed filarial wormsEloisa LacanilaoNo ratings yet
- Sbip Forms 2019-2020Document14 pagesSbip Forms 2019-2020Princess May Olea ItaliaNo ratings yet
- Pancreatite AgudaDocument8 pagesPancreatite AgudaGabriel MouraNo ratings yet
- Treatment of Angular Cheilitis A Narrative Review and AuthorsDocument9 pagesTreatment of Angular Cheilitis A Narrative Review and AuthorsElizabeth SihiteNo ratings yet
- At-A-Glance Pocket Reference 2007Document8 pagesAt-A-Glance Pocket Reference 2007Arum PelangiNo ratings yet
- Histological Features of Candidiasis: By:Mamdouh Dagsh Alshrifi ID:321103259Document14 pagesHistological Features of Candidiasis: By:Mamdouh Dagsh Alshrifi ID:321103259Mamdouh D AlrwailiNo ratings yet
- Drug Ana Rifampicin Isoniazid Pyrazinamide Ethambutol StreptomycinDocument4 pagesDrug Ana Rifampicin Isoniazid Pyrazinamide Ethambutol StreptomycinLatoja, Lyndon Sixto Jr. C.No ratings yet
- DR Pankaj NaramDocument20 pagesDR Pankaj NaramNitesh Kumar50% (6)
- Medtronic Circular StaplerDocument4 pagesMedtronic Circular StaplerClaire SongNo ratings yet
- Best Practice & Research Clinical Obstetrics and GynaecologyDocument12 pagesBest Practice & Research Clinical Obstetrics and GynaecologyGrit WingsNo ratings yet
- NFDN 1002 - PCDocument3 pagesNFDN 1002 - PCapi-276773856No ratings yet
- No More Spider VeinsDocument16 pagesNo More Spider VeinsTerrence BerniceNo ratings yet
- Anaemia in PregnancyDocument35 pagesAnaemia in PregnancyUmar Dhani89% (9)
- Fluid and Electrolyte Management of The Surgical PatientDocument28 pagesFluid and Electrolyte Management of The Surgical PatientAndri Feisal NasutionNo ratings yet
- The Most Effective Evidence-Based Occupational Therapy Interventions For Adolescents With Bipolar Disorder A Systematic Literature ReviewDocument50 pagesThe Most Effective Evidence-Based Occupational Therapy Interventions For Adolescents With Bipolar Disorder A Systematic Literature ReviewAngela EnacheNo ratings yet
- Triage Assessment SlipDocument1 pageTriage Assessment SlipJm unite100% (1)
- Dermoscopy of Inflamed Seborrheic KeratosisDocument9 pagesDermoscopy of Inflamed Seborrheic KeratosisFreddy RojasNo ratings yet
- 12 Neha Dahiya 2017 Knowledge and Practices Related To Screening For Breast Cancer Among Women in Delhi IndiaDocument5 pages12 Neha Dahiya 2017 Knowledge and Practices Related To Screening For Breast Cancer Among Women in Delhi IndiaArick Frendi AndriyanNo ratings yet
- MICROSCOPIC EXAMINATION OF URINE SEDIMENTDocument14 pagesMICROSCOPIC EXAMINATION OF URINE SEDIMENTRomie Solacito100% (1)
- CHARACTERISTICS and ROLE OF A PSYCHIATRIC NURSEDocument3 pagesCHARACTERISTICS and ROLE OF A PSYCHIATRIC NURSESareno PJhēaNo ratings yet
- NCM 117: Psychiatric Nursing Mental Status ExamDocument8 pagesNCM 117: Psychiatric Nursing Mental Status ExamGabrielle Acabo100% (1)
- DHP W. TableDocument21 pagesDHP W. Tablejenika studiesNo ratings yet
- Reumatoid KELOMPOK 8Document11 pagesReumatoid KELOMPOK 8Ida FarizaNo ratings yet
- Family Medicine COPCDocument20 pagesFamily Medicine COPCrachellesliedeleonNo ratings yet