Professional Documents
Culture Documents
Respiratory Disorders (Completed)
Uploaded by
Czejan Rae TabaranzaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Respiratory Disorders (Completed)
Uploaded by
Czejan Rae TabaranzaCopyright:
Available Formats
d
TABARANZA, CZEJAN RAE BSN-3 0
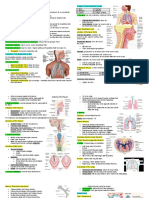
ANATOMY AND PHYSIOLOGY OF THE RESPIRATORY SYSTEM
THE RESPIRATORY SYSTEM
• RESPIRATION
o Ventilation or breathing
o Movement of air into and out of the lungs
o Exchange of oxygen (O2) and carbon dioxide
(CO2)
o Transport of O2 and CO2 in the blood
• PULMONARY VENTILATION
o The way oxygen enters the lungs from the
surroundings.
• EXTERNAL RESPIRATION
o The way oxygen gets from the lungs into
the blood.
o How carbon dioxide gets from the blood
into the lungs
• Olfactory receptors are located in the mucosa on
FUNCTIONS OF THE RESPIRATORY SYSTEM
the superior surface.
• Supply the body with oxygen.
• Removes carbon dioxide from the body. A. NOSTRILS (NARES)
o a by-product of cellular respiration o Route through which air enters the nose.
• Regulation of blood pH B. CHOANAE
• Voice production o Openings into the pharynx
• Olfaction (sense of smell) C. NASAL CAVITY
• Innate immunity o Extends form the nares to the choanae
o Contains coarse hairs that trap large dust
ANATOMY OF THE RESPIRATORY SYSTEM particles.
o Contains cilia that sweep debris-laden
mucus toward the pharynx
o Mucus – produced by goblet cells
o Palate separates the nasal cavity form
the oral cavity
▪ Hard palate = bony
o Soft palate = muscular
o Nasal Septum
- Partition dividing the nasal cavity
into right and left
- Made of hyaline cartilage
D. 3 NASAL CONCHAE
•Upper Respiratory Tract 1. Superior concha
1. Nose 2. Middle concha
2. Nasal Cavity 3. Inferior concha
3. Paranasal Sinuses
4. Pharynx FUNCTIONS (3i’s)
5. Larynx o Increase the surface area.
• Lower Respiratory Tract o Increase air turbulence with the nasal
1. Trachea cavity.
2. Bronchi o Increased trapping of inhaled particles
3. Bronchioles
4. Lungs E. PARANASAL SINUSES
5. Alveoli 1. Maxillary sinus
2 ZONES 2. Frontal sinus
3. Ethmoidal sinus
1. RESPIRATORY ZONE
4. Sphenoidal sinus
o Where gas is exchanged within the lungs
o Air-filled spaces within bone
2. CONDUCTING ZONE
o Functions:
o Where air goes in and out of the body
➢ Lighten the skull.
➢ Act as resonance chambers for
speech
THE UPPER RESPIRATORY TRACT ➢ Produce mucus.
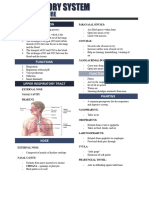
2. PHARYNX (THROAT)
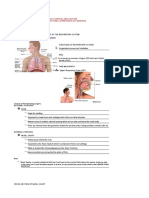
1. NOSE
• Common passageway for both the respiratory and
• The only externally visible part of the respiratory the digestive systems
system
TABARANZA, CZEJAN RAE BSN-3 1
• Muscular passageway from the nasal cavity to the
larynx 3. LARYNGOPHARYNX
o Continuous with the posterior nasal • Passes posterior to the larynx
aperture • Extends from the tip of the epiglottis to the
o Serves as a common passageway for esophagus.
food and air. • Linings:
o Stratified squamous epithelium
• 3 REGIONS OF THE PHARYNX o Ciliated columnar epithelium.
1. Nasopharynx • DURING SWALLOWING:
2. Oropharynx o Epiglottis routes food into the
3. Laryngopharynx posterior tube, the esophagus.
SUMMARY OF TONSILS
• They are clusters of lymphatic tissue that play a
role in protecting the body from infection
REGION TONSILS FOUND
Nasopharynx (1) Pharyngeal
(2) Palatine
Oropharynx
(2) Lingual
3. LARYNX
• Commonly called the “voice box”
• Extends from the base of the tongue to the trachea
• Main function:
o Maintains open airway
o Protects airway during swallowing.
o Produces the voice
• Made of 9 cartilages
1. NASOPHARYNX o 3 singles
• Superior part of the pharynx o 3 paired
• Posterior to the choanae
• UVULA
o Posterior extension of the soft palate
• (3) SINGLE CARTILAGES
• PHARYNGEAL TONSILS
o Posterior part of the nasopharynx 1. THYROID CARTILAGES
o Located in the midline of the o “Adam’s apple”
nasopharynx, forms the superior o Largest cartilage in the larynx
aspect of the Waldeyer’s ring
o Attached superiorly to the hyoid bone.
o Immunity function o Maintains open passageway for air
o When enlarged = ADENOIDS movement.
• During swallowing
o Soft palate is elevated, nasopharynx is 2. CRICOID CARTILAGE
close. This prevents food from passing o Most inferior
from the oral cavity into the nasopharynx. o Forms the base of the larynx
o Maintains open passageway for air
2. OROPHARYNX movement
• Oropharynx and laryngopharynx serves as
common passageway for air and food. 3. EPIGLOTTIS
• Extends from the uvula to the epiglottis. o Elastic cartilage
• Where oral cavity opens into o Inferior margin – attached to
• Lined with stratified non-keratinized thyroid cartilage anteriorly
squamous epithelium. o Superior margin – projects
• PALATINE TONSILS (2) superiorly as a free flap toward
o Lateral walls near the boarder of the oral the tongue
cavity and oropharynx o Functions:
• LINGUAL TONSILS (2) ➢ Prevents swallowed materials
o Surface of the posterior part of the tongue from entering the larynx
o Found at the base of the tongue.
TABARANZA, CZEJAN RAE BSN-3 2
➢ Covers the glottis (opening o Has cilia and goblet cells (produces
of the larynx) mucus)
• (3) PAIRED CARTILAGES
o Forms attachment sites for vocal folds
1. CUNEIFORM CARTILAGES
- Top cartilage
2. CORNICULATE CARTILAGES
- Middle
3. ARYTENOID CARTILAGES
- Bottom
- Articulate with the cricoid cartilage
inferiorly
• VOCAL CORDS
• Constant, long-term irritation of the trachea by
1. VESTIBULAR FOLDS cigarette smoking can cause tracheal epithelium to
o False vocal cords change to stratified squamous epithelium.
o When together, they prevent • SMOKER’S COUGH
the air from leaving the o The result of cough reflex being stimulated
lungs. due to constant irritation and inflammation
o Prevent food and liquid from of the respiratory passages.
entering the larynx 2. BRONCHI
2. VOCAL FOLDS • Formed by division of the trachea
o True vocal cords • Pseudostratified ciliated columnar epithelium
o Primary source of voice • Each bronchus enter the lung at the hilum (medial
production depression)
o Force of air controls
loudness
o Tension of air controls the
pitch of the voice
Hilium of the lungs
• Difference between right and left main bronchi
RIGHT MAIN BRONCHUS LEFT MAIN BRONCHUS
• Wider • More horizontal
• Shorter
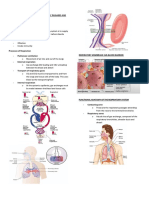
THE LOWER RESPIRATORY TRACT • Straighter
• Where foreign
1. TRACHEA substances usually
• Commonly called “windpipe” enter
• 4-inch-long tube that connects to the larynx
• 16-20 C-shaped rings of hyaline cartilages, which
keep the trachea patent (open) – do not completely • Main bronchi → Lobar (secondary bronchi) →
surround the trachea Segmental (tertiary bronchi) → Bronchioles (d<
• Divides into right and left primary bronchi at the 1mm) → Terminal Bronchioles
level of the 5th thoracic vertebrae
• Esophagus is posterior to the trachea • As these tubes get smaller
• COUGH REFLEX o Epithelium gets thinner
o Aided by the contractions of the smooth o Cartilage decreases
muscles in the trachea can narrow the o Smooth muscle increases
diameter. 3. LUNGS
• MUCOUS MEMBRANE
o Pseudostratified columnar epithelium • Principal organs of respiration
• Occupy the entire thoracic cavity except for the
central mediastinum
• Cone-shaped
• Base: resting on the diaphragm
• Apex: extending superiorly about 2.5 cm above
clavicle
• Fissures
o Separates the lobes of the lungs
• Bronchopulmonary segments
o Divides each lobes of the lungs
o 9 segments on the left
o 10 segments on the right
• Each lung is divided into lobes by fissures.
TABARANZA, CZEJAN RAE BSN-3 3
o Left lung = 2 lobes • TERMINAL BRONCHIOLES
o Right lung = 3 lobes o Leads into the respiratory zone
LEFT LUNG RIGHT LUNG structures and terminate in alveoli
1. Superior lobe 1. Superior lobe RESPIRATORY ZONE CONDUCTING ZONE
2. Inferior lobe 2. Medial lobe 1. Respiratory • Includes all other
3. Inferior lobe bronchioles passageways
2. Alveolar ducts
3. Alveolar sacs
• Serosa cover the outer surface of the lungs
4. Alveoli (air sacs)
o Pulmonary (visceral) pleura
▪ Covers the lung surface • The only site of
o Parietal pleura gas exchange
▪ Lines the walls of the thoracic
cavity 5. ALVEOLI
• Pleural fluid fills the area between layers
o Allows lungs to glide over the thorax
o Decreases friction during breathing
• Pleural space (between layers) is more of a
potential space
• Only site for gas exchange
• Small air-filled chambers where air and blood come
into close contact with each other.
• Simple squamous epithelial cells largely
compose the walls
• ALVEOLAR PORE
o Connect neighboring air sacs
• ALVEOLAR SACS
o Comes from alveolar ducts; chambers
connect to 2 or more alveoli
• PULMONARY CAPILLARIES
o Cover external surfaces of alveoli
• RESPIRATORY MEMBRANE
4. TRACHEOBRONCHIAL TREE o Air-blood barrier
• Bronchial (respiratory) tree is the network of o Where gas exchange between air and
branching passageways blood takes place
• Consist of main bronchi and many branches o Formed by alveolar and capillary walls
• Each main bronchus is divided into lobar brochi o Gas crosses the respiratory membrane by
(secondary bronchi) as they enter the lungs DIFFUSION
▪ Left lung = 2 lobar bronchi ▪ Oxygen enters the blood
▪ Right luHow mng = 3 lobar bronchi ▪ Carbon dioxide enters the alveoli
• Lobar bronchi then turn into segmental bronchi
(tertiary bronchi) which lead to bronchopulmonary
segments, then lastly, it branches as bronchioles
• Bronchioles – subdivides into four
1. Terminal bronchioles
2. Respiratory bronchioles
3. Alveolar ducts – long-branching ducts
4. Alveoli
• Summary:
• LAYERS
▪ Thin layer of alveolar fluid
▪ Alveolar epithelium – simple squamous
epithelium
▪ Basement membrane of alveolar
epithelium
▪ A thin interstitial space
▪ Basement membrane of capillary
epithelium
▪ Capillary endothelium – simple
squamous epithelium
TABARANZA, CZEJAN RAE BSN-3 4
RESPIRATORY ZONE STRUCTURES AND THE • INTRAPLEURAL PRESSURE
o Pressure within the pleural space is always
RESPIRATORY MEMBRANE negative
• STRUCTURES o Major factor preventing lung collapse
o Respiratory bronchioles o If intrapleural pressure equals atmospheric
o Alveolar ducts pressure, the lung recoil and collapse
o Alveolar sacs
o Alveoli 2. EXTERNAL RESPIRATION
• ALVEOLAR MACROPHAGES (DUST CELLS)
• Pulmonary blood and alveoli
o Add protection by picking up bacteria,
o Oxygen is loaded int the blood
carbon particles, and other debris
o Carbon dioxide is unloaded from the blood
• SURFACTANT
o A lipid molecule
3. RESPIRATORY GAS TRANSPORT
o Coat gas-exposed alveolar surfaces
o Secreted by cuboidal surfactant- • Transport of oxygen and carbon dioxide via
secreting cells. bloodstream
PLEURAL CAVITIES
4. INTERNAL RESPIRATION
• Lungs are in the thoracic cavity • Gas exchange between blood and tissue cells in
• Lung is surrounded by a separate pleural cavity systemic capillaries.
• PLEURA
o PARIETAL PLEURA LUNG RECOIL
▪ Lines the walls of the thorax, • Tendency for an expanded lung to decrease in size
diaphragm, and mediastinum • SURFACE TENSION
▪ Continuous with the visceral o Oppositely charged ends of water
pleura molecules are attracted to each other.
o VISCERAL PLEURA o As the water molecules pull together, they
▪ Covers the surface of the lungs also pull on the alveolar walls, causing
• PLEURAL FLUID alveoli to recoil and become smaller.
o Fluid between the parietal and visceral
pleura • TWO FACTORS THAT KEEP THE LUNGS FROM
o Acts as a lubricant COLLAPSING
o Holds the pleural membranes together o SURFACTANT
FOUR EVENTS OF RESPIRATION ▪ Mixture of lipoprotein molecules
produced by the alveolar
1. Pulmonary ventilation epithelium
2. External respiration ▪ Reduces surface tension
3. Respiratory gas transport ▪ Reduces tendency for lung
4. Internal respiration collapse (Pneumothorax)
o PLEURAL PRESSURE
1. PULMONARY VENTILATION ▪ Pressure in the pleural cavity is
• Moving of air into and out of the lungs (commonly less than alveolar pressure, the
called breathing) alveoli tend to expand
• Mechanical process that depends on volume ▪ Due to suction effect
changes in the thoracic cavity ▪ Difference in the pressure
• RULE: (pleural pressure < alveolar
o Volume changes lead to pressure pressure) keeps the alveoli
changes, which leads to the flow of gases expanded
to equalize pressure.
FACTORS AFFECTING RESPIRATORY CAPACITY
• 2 PHASES OF PULMONARY VENTILATION
1. INSPIRATION = Inhalation 1. Body size
▪ Flow of air into the lungs 2. Sex
3. Age
2. EXPIRATION = Expiration 4. Physical Condition
▪ Air leaving lungs RESPIRATORY VOLUME
MECHANICS OF BREATHING • SPIROMETRY
INSPIRATION EXPIRATION o Process of measuring volumes of air that
• Diaphragm and • ↓ Intrapulmonary move into and out of the respiratory
external intercostal volume system
muscles contract • ↑ Gas pressure • SPIROMETER
• Intrapulmonary volume • Gass passively flow o Device that measures respiratory volumes
increases ↑ out to equalize the • RESPIRATORY VOLUME
• Gas pressure pressure o Measures the amount of air movement
decreases↓ • Forced expiration can during different portions of ventilation
• Air flows into the lungs occur mostly by • RESPIRATORY CAPACITIES
until intrapulmonary contraction of o Sums of two or more respiratory volume
pressure equals intercostal muscles IMPORTANT VALUES
atmospheric pressure to depress the rib
cage. • 4-6 LITERS
o Range of total volume of air contained in
the respiratory system.
• TIDAL VOLUME increases during physical activity
TABARANZA, CZEJAN RAE BSN-3 5
• Increase in tidal volume reduces inspiratory and ▪ Cough and Sneeze → clears our lungs of
expiratory reserve volumes, but total lung capacity debris
remains relatively constant. ▪ Crying → emotionally induced mechanism
▪ Laughing → similar to crying
▪ Hiccup → Sudden inspiration
4 TYPES OF RESPIRATORY VOLUME
▪ Yawn → Very deep inspiration
Type Description
• Normal quiet breathing
Tidal volume (TV) RESPIRATORY SOUNDS
• At rest = 500 mL
• Amount of air that can be • Sounds are monitored with stethoscope
Inspiratory reserve taken (inspired) in forcibly • 2 RECOGNIZABLE SOUNDS can be heard with a
volume (IRV) over the tidal volume stethoscope
• Usually around 3,100 mL 1. BRONCHIAL SOUNDS
• Amount of air that can o Produced by air rushing though the large
Expiratory reserve forcibly exhaled after a tidal passageways
volume (ERV) expiration o Trachea and bronchi
2. VESICULR BREATHING SOUNDS
• Approximately = 1,200 mL
o Soft sounds of air filling alveoli
• Air remaining in the lung after
expiration EXTERNAL RESPIRATION, GAS TRANSPORT, AND
• Cannot be voluntarily exhaled INTERNAL RESPIRATION
Residual Volume • Allows gas exchange to go on • Gas exchange occurs as a result of DIFFUSION
(RV) continuously, even between o EXTERNAL RESPIRATION
breaths, and helps keep ▪ Exchange of gases occurring
alveoli open between the alveoli and
• About = 1,200 mL pulmonary blood
▪ DEAD SPACE VOLUME (ANATOMICAL DEAD o INTERNAL RESPIRATION
SPACE) ▪ Is an exchange of gases occurring
o Air that remains in conducting zone and between the blood and tissue
never reaches alveoli cells (systemic capillaries)
o Gas exchange does not take place in • Movement of the gas is toward the area of lower
these segments concentration.
o E.g. BRONCHI and TRACHEA
EXTERNAL RESPIRATION
5 TYPES OF RESPIRATORY CAPACITIES
Type Description Values • Oxygen is loaded into the blood
• The total amount of • Men = o Oxygen diffuses from the oxygen-rich air
exchangeable air 4,800 of the alveoli
• Maximum volume of mL to the
air that a person can • Women= oxygen-poor
expel after a 3,100 blood of the
Vital
maximum mL pulmonary
Capacity
inspiration capillaries.
• FORMULA:
• Carbon dioxide is
Vital Capacity = TV + unloaded out of the
IRV + ERV blood
• Amount of air • About o CO2 diffuses
remaining in the 2,300 from the blood
Functional lungs at the of mL of the
Residual normal expiration pulmonary
Capacity • FORMULA capillaries to
Functional Residual the alveoli.
Capacity = ERV + RV
• Amount of air can • About GAS TRANSPORT IN THE BLOOD
inspire maximally 3,500
after a normal mL • OXYGEN TRANSPORT IN THE BLOOD
expiration. o Most oxygen travels attached to
Inspiratory
• FORMULA HEMOGLOBIN and forms oxyhemoglobin
Capacity
(HbO2).
Inspiratory Capacity =
o A small dissolved amount is carried in the
TV + IRV
plasma
• CARBON DIOXIDE TRANSPORT IN THE BLOOD
• Sum IRV + ERV + • About o Most carbon dioxide is transported in the
Total Lung TV + RV 5,800 plasma as bicarbonate ion (HCO3-)
Capacity • Also equal to Vital mL o A small amount is carried inside red blood
Capacity + Residual cells on hemoglobin, but at different binding
Volumes sites from those of oxygen.
REMEMBER:
NONRESPIRATORY AIR MOVEMENTS
Blood pH should remain between 7.35- 7.45
• Can be caused by reflexes or voluntary actions
• Buffers, such as bicarbonate ion, minimize changes
• Examples:
in pH, in order to maintain homeostasis.
TABARANZA, CZEJAN RAE BSN-3 6
• Emotional factors such as fear, anger, and
INTERNAL RESPIRATIONS excitement
• CHEMICAL FACTORS: CO2 LEVELS
• Exchange of gases between blood and tissue o The body’s need to rid itself CO2 is the
cells most important stimulus for breatjing
• An opposite reaction from what occurs in the lungs o Increased levels of CO2 (decreased/acidic
o CO2 diffuses out of the tissue cells to pH) in the blood increases the rate and
blood (called Loading) depth of breathing
o O2 diffuses from the blood into the tissue o Changes in carbon dioxide act directly on
(called Unloading) the medulla oblongata
CONTROL OF RESPIRATION (NEURAL REGULATION) • CHEMICAL FACTORS: O2 LEVELS
o Changes in oxygen concentration in the
• PHRENIC AND INTERCOSTAL NERVES blood are detected by chemoreceptors in
o Transmits the activity of respiratory the aorta and common carotid artery
muscles to the brain o Information is sent to the medulla
• MEDULLA and PONS o Oxygen is the stimulus for those whose
o Neural centers systems have become accustomed to high
o Control rate and depth levels of CO2 as a result of disease.
• CHEMICAL FACTORS: HYPERVENTILATION
• MEDULLARY RESPIRATORY CENTER o Rising levels of CO2 in the blood (acidosis)
result in faster, deeper breathing
o 2 DORSAL RESPIRATORY GROUPS o Exhale more CO2 to elevate blood pH
▪ Column of cells in the dorsal part o May result in apnea and dizziness and
of the medulla oblongata lead to ALKALOSIS
▪ Contraction of diaphragm • CHEMICAL FACTORS: HYPOVENTILATION
o Results when blood becomes alkaline
o 2 VENTRAL RESPIRATORY GROUPS (alkalosis)
▪ Column of cells in the ventral part o Extremely slow or shallow breathing
of the medulla oblongata o Allows CO2 to accumulate in the blood
▪ Controls the:
o External intercostal DEVELOPMENTAL ASPECTS OF RESPIRATORY
o Internal intercostal SYSTEM
o Abdominal muscles
• Lungs to not fully inflate until 2 weeks after birth
▪ PRE-BOTZINGER COMPLEX • Change from nonfunctional to functional
- Establishes rhythm of breathing respiration depends on SURFACTANT.
• Surfactant is formed in late pregnancy, around 28 to
• PONTINE RESPIRATORY GROUPS 30 weeks.
▪ Collection of neurons in the pons NORMAL VALUES OF RESPIRATORY RATE
▪ Switching between inspiration and AGE VALUE
expiration
Newborns 40-80 rpm
Infants 30 rpm
5 Y.O. 25 rpm
12-18 y.o. 12-18 rpm
Adults 12-20 rpm
EFFECTS OF AGING IN THE RESPIRATORY SYSTEM
• Elasticity of the lungs decreases
• Vital capacity decreases
• Blood oxygen levels decreases
• Stimulating effects of carbon dioxide decreases
• Elderly are often hypoxic and exhibit sleep apnea
• More risk of respiratory tract infection
RESPIRATION AND ACID-BASE BALANCE
• Respiratory system affects the pH of the blood and
other body fluid because it regulates the amount of
CARBON DIOXIDE (CO2) present in these fluids.
RESPIRATORY RESPIRATORY
ALKALOSIS ACIDOSIS
NON-NEURAL FACTORS INFLUENCING RESPIRATORY • Fewer H+ ions are • More H+ ions are
RATE formed formed
• CO2 is exhaled more • CO2 accumulates in
• PHYSICAL FACTORS rapidly the body
1. Increased body temperature • Caused by an • Caused by a
2. Exercise increase in the rate decrease in the rate
3. Talking of respiration of respiration
4. Coughing (hyperventilation) (hypoventilation)
• Volition (Conscious Control)
TABARANZA, CZEJAN RAE BSN-3 7
• CAUSES OF RESPIRATORY ACIDOSIS
o Severe pulmonary disease LABORATORY VALUES
o Emphysema COMPONENT NORMAL VALUE
o Pneumonia pH 7.35 – 7.45
o Oversedation of anesthesia pCO2 35 – 45
o Overdose of opioid or benzodiazepine HCO3 22 -- 26
• CAUSES OF RESPIRATORY ALKALOSIS • ROME Method:
o Prolonged hyperventilation o Respiratory = Opposite
• CAUSES OF METABOLIC ACIDOSIS o Metabolic = Equal
o Diabetic Ketoacidosis
o Kidney failure
o Diarrhea ACID-BASE IMBALANCE
• CAUSES OF METABOLIC ALKALOSIS TERM INDICATION
o Overdose of antacids Respiratory
o Vomiting ↓pH : ↑ pCO2
Acidosis
o GI suctioning
Respiratory
ALKALOSIS VS. ACIDOSIS ↑pH : ↓pCO2
Alkalosis
ALKALOSIS ACIDOSIS
• ↑pH • ↓pH Metabolic
↓pH : ↓HCO3
• ↑Signs and Symptoms • ↓Signs & symptoms acidosis
▪ ↑HR, RR, BP ▪ ↓HR, RR, BP Metabolic
▪ Hyperactive ▪ Hypoactive ↑pH : ↑HCO3
Alkalosis
bowel bowel
▪ Seizures, ▪ lethargic • RESPIRATORY
tremors, anxiety ▪ coma o Imbalance in the lungs
• High except o Problem with CO2
• METABOLIC
POTASSIUM ▪ LOW except
▪ Potassium is o Imbalance from my kidneys
POTASSIUM
LOW ▪ Potassium is
HIGH
HEALTH ASSESSMENT OF THE RESPIRATORY SYSTEM
TERMINOLOGIES o Excess fluid in the pleural space
• Consolidation of the Lungs
• Scoliosis o Condition whereby the lung tissues solidify
o person’s spine is curved from side to side because of the accumulation of solid and liquid
• Kyphosis material in the air spaces.
o over-curvature of the thoracic vertebrae (upper • Pneumothorax (Collapsed Lung)
back) o An abnormal collection of air or gas in the pleural
• Lordosis space that separates the lung from the chest
o over-curvature of the lumbar vertebrae (lower wall, and which may interfere with normal
back) breathing
• Funnel Chest (Pectus Excavatum) • Tactile Fremitus
o congenital deformity of the anterior wall of the o A palpable vibration sounds generated from the
chest, in which several ribs and sternum grow larynx are transmitted through patent bronchi
abnormally. and through the lung parenchyma to the chest
• Pigeon Chest (Pectus Carinatum) wall where vibrations can be felt
o Protrusion of the sternum and ribs • Crackles
• Barrel Chest o Discontinued, explosive, “popping” sound
o Rounded, bulging, almost barrel-like produced by accumulation of secretion within
appearance of the chest that occur as a result of the airway, collapse edema surrounding
long-term over-inflation of the lungs pulmonary tissue.
• Kussmaul’s Breathing • Wheezing
o Deep and labored breathing o is a high-pitched whistling sound during
o Associated with metabolic acidosis breathing
• Cheyne-Stoke’s Breathing o It occurs when air moves through narrowed
o Progressively deeper breathing followed by breathing tubes.
temporary apnea • Stridor
o May occur with heart failure, cerebrovascular o is an abnormal, high-pitched, musical breathing
accident sound caused by a blockage in the throat or
• Trapezius muscle voice box (larynx).
o Large superficial muscle that extends o It is usually heard when taking in a breath
longitudinally from the occipital bone to the
lower thoracic vertebrae and laterally to the
spine of the scapula (shoulder blade) INSPECTION
• Costal Margin/Arch GENERAL INSPECTION
o Is the lower edge of the chest (thorax) formed by
the bottom edge of the rib cage 1. Inspect for nasal flaring ang pursed lip breathing
• Empyema • NORMAL:
o Collection of pus in the space between the lung o Nasal flaring not observed
and the inner surface of the chest wall (pleural • ABNORMAL:
space) o Nasal flaring is indicative of
• Pleural effusion hypoxia
TABARANZA, CZEJAN RAE BSN-3 8
o Pursed lip breathing may be see - result of an increased ration
in asthma, emphysema, or CHF between the AP to Transverse
2. Observe color of face, lips, and chest diameter due to emphysema
• NORMAL: (hyperinflation of the lungs).
o Client has evenly colored skin
tone, without unusual or 2. OBSERVE USE OF ACCESSORY MUSCLES
prominent discoloration o Watch client breath
• ABNORMAL: o Note use of muscles
o Ruddy to purple in clients with o NORMAL:
COPD or CHF as a result of ▪ Client does not use accessory
polycythemia (trapezius/shoulder) muscles to
o Cyanosis if clt is cold or hypoxic assist breathing.
3. Inspect color and shape of nails o ABNORMAL:
• NORMAL: ▪ Use of accessory muscle in cases
o Pink tones should be seen in the of:
nailbeds • Acute and chronic
• ABNORMAL: airway obstruction
o Pale or cyanotic may indicate • Atelectasis (alveoli can’t
hypoxia inflate properly)
o Clubbing can occur from hypoxia 3. INSPECT THE CLIENT’S POSITIONING
WHY CLUBBING HAPPENS WHEN THERE IS LOW o Note the client’s posture and ability to
OXYGEN? support weight while breathing
comfortably.
• 5 Grades of Clubbing o NORMAL:
1. Soft depression
o Clt sitting up and relaxed
2. Changes in angle
o Breathing easily with arms at
3. Convex nails
sides or in lap
4. Digital thickening o ABNORMAL:
5. Glossy nail
o Client leans forward
PATHOPHYSIOLOGY o Uses arms to support weight and
1. Megakaryocyte is not fragmented into lift chest to increase breathing
platelets in the lungs capacity
2. They go into the systemic blood o Referred to as tripod position
circulation o Often seen in COPD
3. They accumulate in the distal capillary
beds (fingers)
4. When they are stuck, they produce
growth factors (Platelet-derived Growth
Factor & Vascular Endothelial Growth
Factor)
5. It causes increase in vascular and
connective tissue growth
6. Fibroblast and smooth muscles starts to
grow under the nail beds--- leading to
clubbing. PALPATION OF POSTERIOR THORAX
1. PALPATE FOR TENDERNESS AND SENSATION
o May use one or both hands
o Use fingers to palpate for tenderness,
warmth, pain, or other sensations.
o Start towards the midline at the level of the
INSPECTION OF THE POSTERIOR THORAX left scapula (over the apex of the left lung)
1. INSPECT CONFIGURATION and move your hands left to right
o Client sits with arms at the side o Move systematically downward and out to
o Stand behind the client and observe the cover the lateral portions of the lungs at the
position of scapulae, shape, and bases.
configuration of the chest wall
o NORMAL:
▪ Scapulae are symmetric and non-
protruding.
▪ Shoulders and scapulae are in equal
horizontal positions
▪ Ration of anteroposterior to
o NORMAL:
transverse diameter is 1:2.
▪ Client reports to tenderness, pain,
▪ Spinous process appear straight, and
or unusual sensations
thorax appears symmetric, with ribs
▪ Temperature should be equal
sloping downward.
bilaterally
▪ Kyphosis may be normal in older
o ABNORMAL
adults
▪ Tender or painful areas →
o ABNORMAL:
fibrous connective tissue
▪ Scoliosis
▪ Pain over intercostal space →
- spinous process deviates
inflamed pleurae
laterally in thoracic area
▪ Barrel Chest
TABARANZA, CZEJAN RAE BSN-3 9
▪ Pain over ribs → is a symptom of o Start at the apices of the scapulae and
fractured ribs percuss across the tops of shoulder
▪ Increased warmth → may be o Percuss the intercostal spaces
related to local infection. o Percuss to the lateral aspects
2. PALPATE FOR CREPITUS o Compare both sides
o Also called subcutaneous emphysema
o Crackling sensation that occurs when air
passes through fluid or exudate
o Use fingers and follow the sequence when
palpating.
o NORMAL:
o Examiner finds no palpable
crepitus o NORMAL:
o ABNORMAL o Resonance is the percussion
o Mark margins if noted. tone elicited over normal lung
o Monitor to note any decrease or tissue
increase in crepitant area o FLAT tone over the scapula
3. PALPATE FOR FREMITUS o ABNORMAL
o Same sequence o Hyperresonance → emphysema
o Use the ball or ulnar edge of one hand to or pneumothorax
assess fremitus (vibrations of air in the 2. PERCUSS FOR DIAPHRAGMATIC EXCURSION
bronchial tubes transmitted to the chest o Ask clt to exhale forcefully and hold the
wall) breath
o Let client say “NINETY-NINE” o Beginning at the scapular line (T7),
o Assess all areas for symmetry and intensity percuss the intercostal spaces of the right
of vibrations posterior chest wall
• Why ball of the hand? o Percuss downward until the tone changes
o Because it is sensitive to vibratory from resonance to dullness
sensations o Mark this level and allow client to breathe.
o NEXT:
o NORMAL: - Ask client to inhale deeply and
o Fremitus should remain hold it
symmetric for bilateral positions - Percuss the intercostal spaces
o ABNORMAL from the mark downward until
o Unequal fremitus → result of resonance changes to dullness
consolidation - Mark the level and allow the client
o Decreased fremitus → Bronchial to breath
obstruction, emphysema, pleural - Measure the distance between
effusion, or pneumothorax. two marks
4. ASSESS CHEST EXPANSION - Perform both sides
o Place your hands on the posterior chest
wall
o Thumbs at the level of T9 or T10 and
pressing together a small skin fold
o As client takes a deep breath, observe the
movement of your thumb.
o NORMAL:
▪ Excursion should be equal
bilaterally
▪ 3-5 cm in adults
o NORMAL: ▪ Level of diaphragm may be
o Examiner’s thumb moves 5-10 higher on the RIGHT because of
cm apart symmetrically the position of the LIVER
o ABNORMAL
o Unequal chest expansion → o ABNORMAL
atelectasis, pneumonia, trauma, ▪ Uneven excursion →
or pneumothorax inflammation from unilateral
pneumonia, damage to phrenic
PERCUSSION OF POSTERIOR THORAX nerve, or splenomegaly.
1. PERCUSS FOR TONE 🩺 AUSCULTATION OF THE POSTERIOR THORAX
TABARANZA, CZEJAN RAE BSN-3 10
1. AUSCULTATE FOR BREATH SOUNDS ANTERIOR THORAX
o Use diaphragm of stet
o Place it on the posterior chest wall at the INSPECTION OF ANTERIOR THORAX
apex of the lung at C7 1. INSPECT OF SHAPE AND CONFIGURATION
o Ask client to breath deeply though the • NORMAL:
mouth for each auscultation (each o AP diameter is less than transverse
placement of stethoscope) diameter
o Auscultate from C7 to T10 and laterally • ABNORMAL
from axilla down to 7thor 8th rib. o Funnel chest
o Pigeon chest
2. INSPECT POSITION OF THE STERNUM
3. OBSERVE QUALITY AND PATTERN OF
RESPIRAITON
• NORMAL:
o Respirations are relaxed, effortless
and quiet, regular rhythm & depth
o Rate= 12-20 cpm
• ABNORMAL
o Labored/Noisy Breathing → severe
asthma or chronic bronchitis
4. INSPECT INTERCOSTAL SPACES
• NORMAL:
o NORMAL: o No retraction or bulging of intercostal
▪ 3 types of breath sound may be spaces are noted
auscultated: • ABNORMAL
• Bronchial o Retraction → obstruction of
• Bronchovesicular respiratory tract or atelectasis
• Vesicular o Bulging → emphysema or asthma
PALPATION OF ANTERIOR THORAX
1. PALPATE FOR TENDERNESS, SENSATION, AND
SUFACE MASSES
ABNORMAL
o
▪ Diminished/absent breath
sounds → obstruction within the
lungs result of mucus plug or
foreign objects
▪ Increased Breath Sounds
(Louder) →
Consolidation/compression
results in a denser lung area that • NORMAL:
enhances the transmission of o No tenderness or pain is palpated
sound. over the lung area with respiraiton
2. AUSCULTATE FOR ADVENTITIOUS SOUNDS • ABNORMAL
o Sounds added or superimposed over o Tenderness noted
normal breath sounds, heard during 2. PALPATE FOR CREPITUS
auscultation.
• NORMAL:
o Note the location where adventitious sound
o No crepitus palpated
is heared
• ABNORMAL
CLINICAL TIP o Crepitus palpated → Extreme
o If you hear abnormal sound during congestion or consolidation
auscultation, always have the client cough.
o Then, listen again and note any change
3. PALPATE FOR FREMITUS
o Coughing may clear the lungs
o Use ball of hand/ulnar edge
• NORMAL:
o or absent
o No adventitious sounds, such as crackles
or wheezes are auscultated CLINICAL TIP:
• ABNORMAL o AVOID palpating the BREAST in female.
o Crackles and wheezes are evident o Breast tissue dampens vibrations.
4. PALPATE ANTERIOR CHEST EXPANSION
o Place thumbs along costal margins and
pointing toward the xiphoid process
o Ask client to take a deep breath
TABARANZA, CZEJAN RAE BSN-3 11
o Observe movement of thumbs.
• ABNORMAL
o Hyperresonance → trapped air such as
emphysema or pneumothorax
o Dullness → areas of increase density such
as consolidation, pleural effusion, or tumor.
🩺 AUSCULTATION OF THE ANTERIOR THORAX
1. AUSCULATE FOR ANTERIOR BREATH SOUNDS,
ADVENTITIOUS SOUNDS, AND VOICE SOUNDS
o Use diaphragm of stet
o Auscultate from the apices of the lungs
slightly above the clabcles to the bases of
• NORMAL: the lungs at the sixth rib
o Thumbs move outward in symmetric o Breath through mouth each auscultation
fashion from the midline
• ABNORMAL
o Unequal or decreases chest expansion
PERCUSSION OF ANTERIOR THORAX
1. PERCUSS FOR TONE
o Percuss the apices above the clavicle
o Percuss the intercostal spaces across and
down
• NORMAL:
o 3 types of normal breath sounds
▪ Bronchial
▪ Bronchovesicular
▪ Vesicular
• ABNORMAL
o 2 categories of adventitious sound
▪ Discrete, continuous =
Crackles
▪ Continuous musical sound =
• NORMAL: Wheezes
o Resonance is the percussion tone 2. AUSCULTATE FOR VOICE SOUNDS
A. Bronchophony
• Let pt say “ninety-nine”
B. Egophony
• Let pt say “e”
• ABNORMAL
o Sound changes to
“a” or “say” → lung
tissue is
consolidated
C. Whispered Pectoriloquy
• Let pt say “1-2-3”
TABARANZA, CZEJAN RAE BSN-3 12
DIAGNOSTIC EXAMS/EVALUATION
NON-INVASIVE PROCEDURES • Check for lung function before lung surgery
• Test lung function in people with lung disease like
1. PULMONAR FUNCTION TEST (PFT) COPD.
PURPOSE: WHEN TO HAVE V/Q SCAN?
• Determine lung function and breathing difficulties • If you have symptoms of PULMONARY EMBOLISM:
• Used prior to surgery to screen patients scheduled o Trouble breathing
for thoracic and upper abdominal surgical o Chest pain
procedure. o Coughing or coughing up blood
TEST INCLUDES: o Rapid Heart Beat
✓ Measurement of lung volumes RADIOLOGIC STUDIES
✓ Ventilatory functions 1. Chest X-ray
✓ Mechanics of breathing 2. Computed Tomography (CT Scan)
✓ Diffusion 3. MRI
✓ Gas exchange 4. PET
HOW TO PERFORM? 5. Pulmonary Angiography
• Technician 1. CHEST X-RAY
• Uses spirometer with volume collecting device
attached to a recorder.
NURSING RESPONSIBILITIES
• If smoker → instruct not to smoke 6-8 hrs prior to
testing
• If using inhalers → withhold 4-6 hours prior to
testing
2. PULSE OXIMETRY
PURPOSE:
• Continuous monitoring of oxygen sat of hemoglobin
(SaO2)
• Monitor for subtle or sudden changes in SaO2 • Normal pulmonary tissue is radiolucent
AREAS FOR PULSE OXIMETRY: • 2 VIEWS OF ROUTINE CHEST X-RAY
• Probe or sensor is attached to: 1. Posteroanterior projection
o Fingertip 2. Lateral projection
o Forehead WHY TAKE X-RAY DURING DEEP INSPIRATION
o Earlobe (INHALE)?
o Bridge of the nose
• Lung best visualized when well aerated
NORMAL O2: >95% • Diaphragm is at its lowest level, large expanse of
lung is visible.
ABNORMAL: <90% → tissue is not receiving enough
CONTRAINDICATIONS:
oxygen
• Pregnant women
WHEN CAN PULSE OXIMETRY BE UNRELIABLE? NURSING RESPONSIBILITIES
• Cardiac arrest • BEFORE
• Shock o Remove metal objects from chest such as
• States of low perfusion (sepsis, peripheral vascular neckaces
disease, hypothermia) o Wear gown
• Detecting hypoventilation when there is O2 o May be given lead shield to minimize
supplement. radiation exposure to thyroid, ovaries, or
• Anemia testicles
• Abnormal hemoglobin • DURING
• High carbon monoxide o 3 positions to obtain appropriate view of
• Use of dye (methylene blue) chest
• Dark skin ▪ Standing
• Wearing nail polish ▪ Sitting
▪ Recumbent
3. VENTILATION/PERFUSION SCAN (V/Q SCAN)
• VENTILATION SCAN
o Measures air movement in + out of the
lungs
o Air movement
• PERFUSION SCAN
o Measures circulation that is how blood
flows in the lungs
o Blood movement
• 2 scans may be done separately or together.
PURPOSE:
• Check for pulmonary embolism (PE)
• Find problems with blood flow in the lungs
TABARANZA, CZEJAN RAE BSN-3 13
2. COMPUTED TOMOGRAPHY (CT SCAN) • Confusion and agitation
• Implanted metal or metal support devices
• Gadolinium-based contrast agents may
potentially lead to nephrogenic systemic fibrosis
in patients with reduced kidney function.
NURSING RESPONSIBILITIES:
• BEFORE
o Clarify to physician if ordered test requires
use of DYE
▪ If yes, pt should remain NPO pre-
examination
o Pt with claustrophobia → offered
antianxietyb
o Remove all metal items:
• Lungs are scanned in successive layers by narrow- ▪ Hearing airds
beam x-ray ▪ Hair clips
▪ Medication patches with metallic
• Provides cross-sectional view of the chest
oil component
• It can distinguish fine tissue density
o Assess for presence of implanted metal
USES: devices
✓ Define pulmonary nodules ▪ Aneurysm clips
✓ Small tumors adjacent to pleural surfaces ▪ Cardiac pacemaker defibrillator
✓ Demonstrate mediastinal abnormalities and hilar • DURING
adenopathy o Inform pt to lie flat and remain still for
CT PULMONARY ANGIOGRAPHY between 30-90 minutes.
• Used routinely in place of catheter angiography to o Inform pt that they will hear loud
diagnose PULMONARY EMBOLISM humming or thumping noise
CONTRAINDICATIONS ▪ Earplugs are typically offered to
pts to minimize the noise.
• Allergy to dye
o They can communicate to staff via
• Pregnancy microphone and earphone.
• Claustrophobia
• Morbid obesity 4. POSITRON EMISSION TOMOGRAPHY
• Acute kidney injury and acidosis secondary to
contrast dye
NURSING RESPONSIBILITIES
• Inform client to remain supine and still for less than
30 mins
• For pt to not experience claustrophobia
o Can be given ANTIANXIETY
MEDICATIONS preprocedure
• If CONTRAST DYE is require:
o Pt in NPO for 4 hours prior to
examination.
• Uses a radioactive tracer → pinpoint differences in
o Assess for allergies to IODINE or
tissues on the molecular level
SHELLFISH
• Detect conditions like lung cancer
3. MAGNETIC RESONANCE IMAGING (MRI) • Typically combined with lung CT scan to provide a
3-d image.
o Called image fusion
o Highlights rapid metabolic activity
USES:
✓ Allow physicians to distinguish between benign
(noncancerous) and malignant (cancerous)
masses.
HOW IS IT PERFORMED?
• Small amount of glucose contained radioactive
tracer substance is injected INTRAVENOUSLY
• Uses magnetic fields and radiofrequency signals
o Injected HOUR before scan
instead of radiation.
o Isotope of element FLUORINE is used
• Better than CT scan
• Client should lie still while the scan runs
USES: • Scan takes 20-30 mins
• Characterize pulmonary nodules NURSING RESPONSIBILITIES:
• Help stage bronchogenic carcinoma
• BEFORE
• Evaluate inflammatory activity in interstitial lung
o Pt should not eat or drink (except water)
disease
for several hours before scan.
• Acute Pulmonary Embolism o Change to hospital gown
• Chronic thrombolytic pulmonary hypertension o Remove all metallic objects including
CONTRAINDICATION: jewelry
• Morbid obesity o Ask if she is taking medications such as
• Claustrophobia for DM
TABARANZA, CZEJAN RAE BSN-3 14
o For claustrophobia → give antianxiety INVASIVE PROCEDURES (ENDOSCOPIC EXAMS)
meds
1. LARYNGOSCOPY
5. PULMONARY ANGIOGRAPHY
• Provides direct visualization of the larynx
• Instrument = laryngoscope
USES:
✓ Diagnose lesions
✓ Evaluate laryngeal function
✓ Determine any inflammation
✓ Physcians may also dilate laryngeal strictures and
biopsy lesions
USES:
• Investigate congenital abnormalities of the
pulmonary vascular tree.
• To visualize pulmonary vessels:
o Radiopaque agent is injected through
catheter, which has been initially inserted
into a vein:
▪ Jugular
▪ Subclavian
▪ Brachial 2. BRONCHOSCOPY
▪ Femoral Vein ✓ Direct inspection and examination of the:
• Then threated to the pulmonary ✓ Larynx
artery ✓ Trachea
CONTRAINDICATIONS: ✓ Bronchi
• Allergy to radiopaque dye ✓ INSTRUMENT:
• Pregnancy ✓ Flexible fiberoptic bronchoscope
• Bleeding abnormalities (more frequent)
✓ Rigid bronchoscope
POTENTIAL COMPLICATIONS:
USES:
• Acute kidney injury
• Acidosis ✓ Visualize tissues and determine nature, location,
• Cardiac dysrhythmias and extent of pathologic process
✓ To collect secretions for analysis to obtain a tissue
• Bleeding
sample for diagnosis
NURSING RESPONSIBILITIES: ✓ Determine whether a tumor can be resected
• BEFORE surgically
o Secure informed consent ✓ Diagnose sources of hemoptysis (coughing of
o Assess for known ALLERGIES to: blood)
▪ Radiopaque dye (iodine & FLEXIBLE FIBEROPTIC RIGID BRONCHOSCOPE
shellfish) BRONCHOSCOPE
o Assess for ANTICOAGULATION STATUS
and RENAL FUNCTION
o Ensure pt is an NPO FOR 6-8 HOURS
o Administer medications (if necessary)
▪ Anti-anxiety
▪ Secretion-reducing agents
▪ Antihistamines
• DURING
o Inform patient that pt may experience warm ✓ Can be directed into • Hollow metal with light
flushing sensation or chest pain during the segmental at it’s end
injection of the dye bronchi • Used mainly for →
o If arterial punction is necessary ✓ Ideal for diagnosing ✓ removing foreign
▪ Affected extremity should be pulmonary lesions substances
immobilized for certain time. ✓ Can be performed at ✓ Investigating
• AFTER BEDSIDE sources of massive
o Monitor o Thru endotracheal hemoptysis
▪ VS tube or ✓ Performing
▪ Level of consciousness tracheostomy endobronchial
▪ Oxygen saturation tubes. surgical
▪ Vascular access site for bleeding
procedures
or hematoma
• Performed ONLY in the
▪ Perform frequent assessment of
OPERATING ROOM.
neurovascular status
POSSIBLE COMPLICATIONS:
o Oversedation
o Prolonged fever
o Infection
o Aspiration
TABARANZA, CZEJAN RAE BSN-3 15
o Vasovagal response ✓ Obtain sample of pleural fluid or biopsy specimen
o Laryngospasm INTERPRETATIONS:
o Bronchospasm
PLEURAL FLUID ANALYSIS
o Hypoxemia
Bloody fluid Suggest trauma
o Pneumothorax
Purulent fluid Infection
o Bleeding
Associated with cancer,
NURSING INTERVENTIONS Serous fluid inflammatory conditions, heart
• BEFORE failure
o Secure informed consent
o Withhold foods and fluids for 4-8 hours HOW TO PERFORM?
▪ To reduce risk of aspiration when
cough reflex is blocked by • Withdraw 1-2 L of fluid → to relieve respiratory
anesthesia distress
o Administer preoperative medications • Done at bedside or in treatment room
(atropine and a sedative/opioid) as • Positioning:
prescribed o Sits at the side of the bed/exam table
▪ To inhibit vagal stimulation ▪ Place pillow on bedside to rest
▪ Suppress the cough reflex arms and head
▪ Sedate patient o Side-lying position on unaffected side
▪ Relieve anxiety • Clean the site → anesthetized with local anesthesia
o Ask pt to remove remove dentures and other → apply small pressure dressing
oral protheses • After, client should be in bed rest for 1 hour on the
o Exam is performed either local anesthesia or unaffected site to allow lung expansion
moderate sedation COMPLICATIONS
▪ General anesthesia for rigid • Pneumothorax
bronchoscopy • Subcutaneous emphysema
• AFTER • Infection
o Pt must take NOTHING BY MOUTH until • Pulmonary edema
cough reflex returns
• Cardiac distress
▪ Anesthesia impair the laryngeal
reflex and swallowing 2. LUNG SCANS
o Once COUGH REFLEX is back
▪ Offer ice chips and eventually fluids • VQ scan
o Monitor: • Gallium scan
▪ Respiratory status • Positron Emission Tomography (PET) Scan
▪ Observe for hypoxia
▪ Hypotension 3. FLUOROSCOPIC STUDIES
▪ Tachycardia • X-ray
▪ Dysrhythmias
▪ Hemoptysis
▪ Dyspnea
o Blood-tinged sputum and fever may be LABORATORY TESTS
expected within first 24-hours
1. SPUTUM STUDIES
3. MEDIASTINOSCOPY
•To identify pathogenic organisms
•Determine whether malignant cells are present
USED TO PTS C:
• Receiving antibiotics
• Corticosteroids
• Immunosuppressive mediations
2. CULTURES
• Throat, nasal, and nasopharyngeal cultures
• Provides visualization of the mediastinum and is • To identify pathogens for respiratory
done under local or general anesthesia. infections such as pharyngitis
• Physician makes incision above the sternum and • THROAT CULTURE
inserts a mediastinoscope o For older adults with severe or ongoing
o Visualizes lymph nodes sore throats c fever & lymph node
o Obtain biopsy samples enlargement
• Possible Complications o Most useful in detecting streptococcal
o Dysrhythmias, MI infection
o Pneumothorax, bleeding • RAPID STREP TEST
INVASIVE PROCEDURE (LUNG BIOPSY) o Provides results within 15 minutes
o Replacing throat culture
1. THORACENTESIS • Ideal → cultures obtained BEFORE antibiotic
therapy
• Aspirating excess fluid or air accumulates from the
pleural space by inserting needing into the chest • Results usually take between 48-72 hours
wall
• Performed with local anesthesia
USES:
✓ Remove excess fluid
TABARANZA, CZEJAN RAE BSN-3 16
CULTURES • Infection
Throat Culture For streptococcal infection • Hematoma
To detect: • Hemorrhage
Nasal Culture • Staphylococcus aureus LABORATORY VALUES
• Influenza COMPONENT NORMAL VALUE
To detect: pH 7.35 – 7.45
Nasopharyngeal
• Staphylococcus aureus pCO2 35 – 45
cultures
• Influenza HCO3 22 -- 26
3. ACID-FAST BACILLUS (AFB) TESTS • ROME Method:
o Respiratory = Opposite
• Acid-fast Bacillus → bacteria that causes
o Metabolic = Equal
tuberculosis and other infections.
• Indicated to people with symptoms of active TB ACID-BASE IMBALANCE
• This test looks for AFB bacteria in your sputum TERM INDICATION
• TWO TYPES OF AFB TESTS: Respiratory
↓pH : ↑ pCO2
1. AFB SMEAR Acidosis
o Sample is smeared on glass
Respiratory
slide ↑pH : ↓pCO2
Alkalosis
o Results in 1-2 days
o ADVANTAGE Metabolic
↓pH : ↓HCO3
▪ Can show possible acidosis
or likely infection
o DISADVANTAGE Metabolic
↑pH : ↑HCO3
▪ Cant provide definite Alkalosis
diagnosis • RESPIRATORY
2. AFB CULTURE o Imbalance in the lungs
o Sample is taken to the lab o Problem with CO2
and put in a special
environment to encourage the • METABOLIC
growth of bacteria. o Imbalance from my kidneys
o ADVANTAGE COMPENSATION
▪ Can confirm a TERM INDICATION
diagnosis of TB and Fully
other infections. Compensated
pH is normal
o DISADVANTAGE Partially
▪ Take 6-8 weeks to compensated
All abnormal
complete.
1 normal & 1 abnormal bet.
SYMPTOMS OF ACTIVE TB: Uncompensated
paCO2 & HCO3
• Cough that lasts for 3-weeks or more
• Coughing up blood and/or sputum 5. GENE XPERT
• Chest pain
• Fever • CBNAAT (catridge based nucleic acid amplification
• Fatigue test)
• Night sweats • Rapid diagnostic test for:
• Unexplained weight loss o TB detection
o Rifampicin resistance in direct smear
AFB SMEAR RESULTS
negative cases
AFB Smear • Probably TB or other infection
• ADVANTAGE:
Positive
o Excellent in detecting Mycobacterium
• Active TB or other type of AFB Tuberculosis
infection
• Once diagnosed:
AFB Culture
o Provider may order
Positive
“susceptibility test” to
help determine
antibiotic.
4. ABG DETERMINATION
• Aids in assessing ability of the lungs to provide
adequate oxygen and remove CO2
• Reflects ventilation
• Reflects ability of the kidneys to reabsorb or excete
bicarbonate (HCO3)
HOW IS IT OBTAINED?
• Thru arterial puncture at the:
o Radial artery
o Brachial artery
o Femoral artery
• Or thru an indwelling arterial catheter
POSSIBLE COMPLICATIONS
• Pain r/t nerve injury or noxious stimulation
TABARANZA, CZEJAN RAE BSN-3 17
TOPIC OUTLINE
1. Other Laboratory Tests
a. Fagerstorm
b. Smoke Analyser
2. Procedures
a. Oxygen delivery sytems
b. Suctioning
c. Incentive spirometry
d. Artificial Airway
e. Nebulization, atomization
f. Chest Tube thoracostomy
g. Postural drainage
h. Chest physiotherapy 2. SMOKER ANALYSER TEST
i. Deep breathing and coughing exercise
j. Pulmonary wedge pressure ● An easy-to-use hand-held and non-invasive monitor
Transcribed by: Ling, T.H.C. & Mergenio, M.
for the testing of patients to determine level of
Carbon Monoxide (CO) in the blood.
● Best used with smokers or those who are exposed
OTHER LABORATORY TESTS to second-hand smoke.
USES:
1. FAGERSTORM TEST FOR NICOTINE DEPENDENCE ● It is important to note that those who smoke can
or FTND (Standardized Degree of Nicotine build up high levels of CO in the blood, which can
lead to heart disease, circulation problems, and
Dependence)
high blood pressure.
• Standard instrument for assessing the intensity of ● Measure levels of CO to assist in smoking
physical addiction to nicotine. cessation.
• It contains six items that evaluate the quantity of HOW TO USE:
cigarette consumption, the compulsion to use,
1. The person taking the test should breathe in and
and dependence.
hold their breath for 15 seconds while the
• The items are summed to yield a total score of 0-
10. Smokerlyzer counts down.
• The Fagerström Tolerance Questionnaire was 2. The monitor will beep during the last 3 seconds of
developed by Karl-Olov Fagerström. This the countdown. The person should blow slowly into
instrument was modified to the Fagerström Test for the mouthpiece. If they cannot hold their breath for
Nicotine Dependence by Todd Heatherton, et al. in the full 15 seconds, they should hold it for as long
1991. as they can and then breathe into the mouthpiece.
USES: They should empty their lungs completely.
• To document indications for prescribing medication 3. The monitor will show the CO rating.
for nicotine withdrawal.
DISADVANTAGE:
• Still needs further psychometric investigation,
including for patients with schizophrenia, as it may
produce an underestimation of nicotine
dependence, which may have a negative impact on
the dosage of the nicotine replacement.
INDICATIONS:
• High result indicates high nicotine addiction.
• Results are shown through the summation of
scores: ADVANTAGE:
o 1-2 = low dependence
o 3-4 = low to mod dependence ● Non-invasive, quick and easy to use. Instant
o 5-7 = moderate dependence readings with traffic light system, for easy
o 8+ = high dependence interpretation of patient's results.
● An aid to establish a smoker's dependence on
nicotine.
● Fast and accurate, non-invasive breath test for
smoking. Anti-infection controls reduce the risk of
bacterial infection.
DISADVANTAGE:
● A false high level of CO can occur when a person
has alcohol on their breath or when they have bad
gas.
TABARANZA, CZEJAN RAE BSN-3 18
TRIVIA:
● Second-hand smoke contains 5 times more CO
than the smoke being inhaled by a smoker.
● Breathing in CO from exhaust fumes or leaking gas
appliances can also cause a high level of CO in the
body.
NON-INVASIVE PROCEDURES
1. OXYGEN DELIVERY SYSTEMS
●Are classified as low-flow (variable performance) or
high-flow (fixed performance) delivery systems.
LOW-FLOW SYSTEMS
● Contribute partially to the inspired gas the patient
breathes, which means that the patient breathes some
room air along with the oxygen.
● Examples of low-flow systems are
○ Cannula
○ Nasal catheter
○ Mask, simple Simple Masks
○ Mask, partial rebreathing - Are used to administer low-to moderate
○ Mask, nonrebreathing concentrations of oxygen.
HIGH-FLOW SYSTEMS - Body of the mask itself gathers and stores oxygen
● Provide the total inspired air between breaths.
● Specific percentage of oxygen is delivered independent - Patient exhales directly through openings or ports in
of the patient’s breathing the body of the mask
● Indicated for patients who require a constant and precise - Cannot be used for controlled oxygen concentrations
amount of oxygen and must be adjusted for proper fit
● Examples of high-flow systems are Partial rebreathing masks
○ Transtracheal catheter - Have a reservoir bag that must remain inflated during
○ Mask, venturi both inspiration and expiration.
○ Mask, aerosol - Adjusts the oxygen flow to ensure that the bag does
○ Tracheostomy collar not collapse during inhalation
○ Something - Oxygen enters the mask through small-bore tubing
○ Face tent that connects at the junction of the mask and bag
Nasal Cannula - The actual percentage of oxygen delivered is
- when the patient requires a low-to-medium influenced by the patient’s ventilatory pattern
concentration of oxygen for which precise accuracy Nonrebreathing masks
is not essential - Are similar in design to partial rebreathing masks
- method allows the patient to move about in bed, talk, except that they have additional valves.
cough, and eat without interrupting oxygen flow - One-way valve located between the reservoir bag
- Flow rates in excess of 4 L/min may lead to and the base of the mask allows gas from the
swallowing of air or may cause irritation and drying reservoir bag to enter the mask on inhalation but
of the nasal and pharyngeal mucosa prevents gas in the mask from flowing back into
Nasal (oropharyngeal) Catheter the reservoir bag during exhalation.
- rarely used but may be prescribed for short-term - One-way valves located at the exhalation ports
therapy to administer low-to-moderate - If the nonrebreathing mask fits the patient snugly and
concentrations of oxygen both side exhalation ports have one-way valves, it is
- catheter should be changed frequently (e.g., every 8 possible for the patient to receive 100% oxygen,
hours), alternating nostrils to prevent nasal irritation but difficulty to get an exact fit from the mask on
and infection every patient, and some non rebreathing masks have
only one one-way exhalation valves, it is almost
When oxygen is given via cannula or catheter, the percentage impossible to ensure 100% oxygen delivery,
of oxygen reaching the lungs varies with the depth and rate of making it a low-flow oxygen system
respirations, particularly if the nasal mucosa is swollen or if the
Venturi mask
patient is a mouth breather.
- Most reliable and accurate method for delivering
precise concentrations of oxygen through
noninvasive means.
- Allows a constant flow of room air blended with a
fixed flow of oxygen
TABARANZA, CZEJAN RAE BSN-3 19
- Primarily for patients with COPD because it can ○ Skin grafts
accurately provide appropriate levels of ○ Refractory anaerobic infections
supplemental oxygen, thus avoiding the risk of ○ Refractory osteomyelitis
suppressing the hypoxic drive.
- uses the Bernoulli principle of air entrainment 2. SUCTIONING
(trapping the air like a vacuum), provides a high
SUCTIONING THE TRACHEAL TUBE (TRACHEOSTOMY
airflow with controlled oxygen enrichment OR ENDOTRACHEAL TUBE)
- For each liter of oxygen that passes through a jet - To suction the patient’s secretions because of the
orifice, a fixed proportion of room air is entrained decreased effectiveness of the cough
- Remove the mask when pt is eating, drinking, taking mechanism
medications, during this supplemental oxygen is - Tracheal suctioning is performed when adventitious
provided through a nasal cannula breath sounds are detected or whenever
Transtracheal Oxygen Catheter secretions are obviously present.
- Requires minor surgery, to insert a catheter through - Unnecessary suctioning can initiate bronchospasm
a small incision directly into the trachea and cause mechanical trauma to the tracheal
- For patients with chronic oxygen therapy needs mucosa
- More comfortable, less dependent on breathing
patterns, and less obvious than other oxygen For mechanically ventilated patients, in-line suction (also
delivery methods called closed suctioning) catheter may be used to:
- No oxygen is lost into the surrounding environment, - Allow rapid suction when needed and to minimize
the patient achieves adequate oxygenation at lower cross contamination by airborne pathogens.
rates - Allows the patient to be suctioned without being
T-piece disconnected from the ventilator circuit
- Special adaptor used to deliver oxygen, which - Decreases hypoxemia, sustains PEEP, and can
connects to the endotracheal or tracheostomy tube decrease patient anxiety associated with suctioning
and is useful in weaning patients from mechanical
ventilation ● The cuff on an endotracheal or tracheostomy tube should
be inflated if the patient requires mechanical ventilation or
is at high risk for aspiration.
● The pressure within the cuff should be the lowest
possible pressure (20 to 25 mm Hg) Rationale: Allows
delivery of adequate tidal volumes and prevents
pulmonary aspiration
● Cuff pressure must be monitored every 8 hours by
attaching a handheld pressure gauge to the pilot balloon
➔ The demand oxygen delivery system (DODS) of the tube or by using the minimal leak volume or minimal
interrupts the flow of oxygen during exhalation, when occlusion volume technique.
it is otherwise mostly wasted. 3. INCENTIVE SPIROMETRY (SUSTAINED MAXIMAL
➔ Studies show that DODS models conserve oxygen INSPIRATION)
and maintain oxygen saturation better than - method of deep breathing that provides visual
continuous flow oxygen systems when the feedback to encourage the patient to inhale slowly
respiratory rate increases and deeply to maximize lung inflation and prevent
or reduce atelectasis (complete or partial collapse of
Hyperbaric oxygen therapy the entire lung or area (lobe) of the lung).
● Administration of 100% oxygen, either intermittently Incentive spirometers are available in two types:
or continuously, at pressures greater than volume or flow
atmospheric pressure.
● Amount of oxygen dissolved in plasma is increased,
which increases oxygen levels in the tissues
● Patient is placed in a small (single patient use) or
large (multiple patient use) cylinder chamber.
● Potential side effects include ear trauma, central
nervous system disorders, oxygen toxicity, and
anxiety in patients with claustrophobia
● Treat conditions such as
○ Decompression sickness volume type
○ Air embolism - tidal volume is set using the manufacturer’s
○ Carbon monoxide poisoning instructions
○ Cyanide poisoning - deep breath through the mouthpiece,
○ Smoke inhalation pauses at peak lung inflation, and then
○ Gangrene relaxes and exhales
○ Tissue necrosis - several normal breaths before attempting
○ Wound healing another with the incentive spirometer helps
TABARANZA, CZEJAN RAE BSN-3 20
avoid fatigue. The volume is periodically ■ A tracheostomy tube is held in place
increased as tolerated by twill tape ties or a tube holder
flow type fastened around the patient’s neck.
- volume is not preset ■ Usually, a square of sterile gauze is
- contains a number of movable balls that placed between the tube and the skin
are pushed up by the force of the breath (Rationale: To absorb drainage and
and held suspended in the air while the reduce the risk of infection)
patient inhales
- amount of air inhaled and the flow of the air
are estimated by how long and how high the
balls are suspended
- ensure that the volume of air inhaled is increased
gradually as the patient takes deeper and deeper
breaths.
INDICATIONS
- used after surgery, especially thoracic and
abdominal surgery, to promote the expansion of
the alveoli and to prevent or treat atelectasis ○ COMPLICATIONS:
NURSING MANAGEMENT ■ May occur early, late or even years
after the tube was removed in the
- placing in proper position (sitting or semi-Fowler’s
course of tracheostomy tube
position to enhance diaphragmatic excursion;
management.
however, this procedure may be performed with the
■ Early Complications:
patient in any position)
1. tube dislodgement
- educating on technique for using the incentive
2. accidental decannulation
spirometer
3. Bleeding
- setting realistic goals for patient
4. Pneumothorax
4. ARTIFICIAL AIRWAY 5. air embolism
● Tracheotomy - a surgical procedure in which an 6. Aspiration
opening is made into the trachea. The indwelling 7. subcutaneous or mediastinal
tube inserted into the trachea is called a emphysema
tracheostomy tube 8. recurrent laryngeal nerve damage
● Tracheostomy - the stoma that is the product of the 9. Posterior tracheal wall
tracheotomy may be either temporary or penetration.
permanent. ■ Long-term Complications:
○ USES: 1. Airway obstruction from
■ to bypass an upper airway obstruction, accumulation of secretions or
■ to allow removal of tracheobronchial protrusion of the cuff over the
secretions opening of the tube
■ to permit the long-term use of 2. infection, rupture of the
mechanical ventilation innominate artery
■ to prevent aspiration of oral or gastric 3. Dysphagia
secretions in the unconscious or 4. tracheoesophageal fistula
paralyzed patient (by closing off the 5. tracheal dilation
trachea from the esophagus) 6. tracheal ischemia,
■ to replace an endotracheal tube 7. Necrosis.
○ PROCEDURE: ■ Tracheal stenosis may develop after
■ Usually performed in the operating the tube is removed.
room or in an ICU (Rationale: Patient’s ■ HOW TO PREVENT IT?
ventilation can be well controlled and 1. Administer adequate warmed
optimal aseptic technique can be humidity.
maintained) 2. Maintain cuff pressure at
■ A surgical opening is made between appropriate level.
the second and third tracheal rings 3. Suction as needed per
■ A cuffed tracheostomy tube of an assessment findings.
appropriate size is inserted in the 4. Maintain skin integrity. Change
exposed trachea. The cuff is an tape and dressing as needed or
inflatable attachment to the per protocol.
tracheostomy tube to: 5. Auscultate lung sounds.
1. Occlude the space between the 6. Monitor for signs and symptoms
tracheal walls and the tube of infection, including temperature
2. permit effective mechanical and white blood cell count.
ventilation 7. Administer prescribed oxygen
3. minimize the risk of aspiration and monitor oxygen saturation.
TABARANZA, CZEJAN RAE BSN-3 21
8. Monitor for cyanosis. ■ Ulceration and stricture of the larynx or
9. Maintain adequate hydration of trachea may develop.
the patient. ■ Pt’s inability to talk and to communicate
10. Use sterile technique when needs.
suctioning and performing ■ Unintentional or premature removal of
tracheostomy care. the tube is a potentially life-threatening
○ NURSING MANAGEMENT ○ NURSING MANAGEMENT
■ Patient requires continuous monitoring ■ Explain to the pt and family the purpose
and assessment of the tube to prevent tube removal by
■ Newly made opening must be kept the pt.
patent by proper suctioning of ■ Maintain comfort measures to the pt.
secretions ■ If nurse determines that there is a risk
■ If V/S are stable place pt in semi- of tube removal by the pt, least invasive
Fowler’s position (Rationale: to method of restraints (e.g. soft wrist
facilitate ventilation, promote drainage, restraints and hand mitts) may be
minimize edema, and prevent strain on appropriate as prescribed by the
the suture lines.) primary provider.
■ Analgesia and sedative agents are ■ Close monitoring of the pt is essential
given with caution for risk of cough to ensure safety and prevent harm.
reflex.
■ Ensure patent airway 5. NEBULIZATION, ATOMIZATION
■ Monitor pt respi stat
● Small-Volume Nebulizer (Mini-Nebulizer)
■ Assess for complications
Therapy - a handheld apparatus that disperses a
■ Alleviate pt’s apprehension
moisturizing agent or medication, such as a
■ Provide effective communication.
bronchodilator or mucolytic agent, into microscopic
(Keeping paper and pencil, and the call
particles and delivers it to the lungs as the patient
light within pt’s reach)
inhales.
● Endotracheal Intubation - passing an
○ INDICATIONS:
endotracheal tube through the nose or mouth into
1. difficulty in clearing respiratory
the trachea
secretions
○ USES:
2. reduced vital capacity with ineffective
1. To provide an airway for patients who
deep breathing and coughing
cannot maintain an adequate airway on
3. unsuccessful trials of simpler and less
their own (e.g., patients who are
costly methods for clearing secretions,
comatose and patients with upper
delivering aerosol, or expanding the
airway obstruction)
lungs
2. For patients needing mechanical
4. Frequently used for pts with COPD to
ventilation
dispense inhaled medications, and are
3. For suctioning secretions from the
commonly used at home on long-term
pulmonary tree
basis
4. May be used for no longer than 14 to
○ BREATHING EXERCISES:
21 days, by which time a tracheostomy
■ Diaphragmatic breathing - is a helping
must be considered
technique to prepare for proper use of
the small-volume nebulizer. To use and
strengthen the diaphragm during
breathing.
● STEPS:
1. Place one hand on the abdomen
(just below the ribs) and the other
hand on the middle of the chest to
increase the awareness of the
position of the diaphragm and its
function in breathing.
○ DISADVANTAGES 2. Breathe in slowly and deeply
■ The tubes cause discomfort through the nose, letting the
■ The cough reflex is depressed because abdomen protrude as far as
glottis closure is hindered. possible.
■ Secretions tend to become thicker 3. Breathe out through pursed lips
because the warming and humidifying while tightening (contracting) the
effect of the upper respiratory tract has abdominal muscles.
been bypassed. 4. Press firmly inward and upward
■ The swallowing reflexes (glottic, on the abdomen while breathing
pharyngeal, and laryngeal reflexes) are out.
depressed
TABARANZA, CZEJAN RAE BSN-3 22
5. Repeat for 1 minute; follow with a
rest period of 2 minutes. Performed when patient has:
6. Gradually increase duration up to ● Pleural effusion - causes extra fluid to build up in the
5 minutes, several times a day space around the lungs
(before meals and at bedtime). ● Hemothorax- severe injury to the chest wall or
■ Pursed-Lip Breathing - To prolong surgery that causes bleeding around the lungs
exhalation and increase airway pressure ● Pneumothorax - when lung is accidentally punctured,
during expiration, thus reducing the allowing air to gather outside the lung, causing its
amount of trapped air and the amount of collapse
airway resistance ● Infection - can sometimes cause fluid to build up
● STEPS: around the lung and may be necessary to insert a
1. Inhale through the nose while chest tube to remove the fluid. Getting the fluid out
slowly counting to 3—the amount can at times help clear the infection faster
of time needed to say “Smell a ● Cancer - some cancers spread to the lung or pleura
rose.” (lining of the lung)
2. Exhale slowly and evenly against
pursed lips while tightening the 7. POSTURAL DRAINAGE (SEGMENTED BRONCHIAL
abdominal muscles. (Pursing the
DRAINAGE)
lips increases intratracheal
pressure; exhaling through the - allows the force of gravity to assist in the removal of
mouth offers less resistance to bronchial secretions (usually performed two to four
expired air.) times daily, before meals (to prevent nausea,
3. Count to 7 slowly while vomiting, and aspiration) and at bedtime)
prolonging expiration through - used to prevent or relieve bronchial obstruction
pursed lips—the length of time to secretions drain from the affected bronchioles into
say “Blow out the candle.” the bronchi and trachea and are removed by
4. While sitting in a chair: Fold arms coughing or suctioning
over the abdomen. Inhale through - patient usually sits in an upright position,
the nose while counting to 3 secretions are likely to accumulate in the lower
slowly. Bend forward and exhale parts of the lungs
slowly through pursed lips while - nurse instructs the patient to inhale
counting to 7 slowly. bronchodilators and mucolytic agents, if
5. While walking: Inhale while prescribed, before postural drainage, because
walking two steps. Exhale these medications improve drainage of the bronchial
through pursed lips while walking tree.
four or five steps.
○ NURSING MANAGEMENT: ➔lower and middle lobe bronchi drain more
1. Instruct the patient to breathe through effectively when the head is down
the mouth, taking slow, deep breaths, ➔ upper lobe bronchi drain more effectively when the
and then to hold the breath for a few head is up
seconds at the end of inspiration NURSING MANAGEMENT
(Rationale: to increase intrapleural - Auscultation of the chest before and after the
pressure and reopen collapsed alveoli, procedure is used to identify the areas that need
thereby increasing functional residual drainage and assess the effectiveness of treatment
capacity) - Educates family members who will assist the patient
2. Encourage the patient to cough and to at home to evaluate breath sounds before and after
monitor the effectiveness of the treatment
therapy. - Provides an emesis basin, sputum cup, and paper
3. Instructs the patient and family about tissues
the purpose of the treatment, - Remain in each position for 10 to 15 minutes and to
equipment setup, medication additive, breathe in slowly through the nose and out slowly
and proper cleaning and storage of the through pursed lips, if the patient cannot cough, the
equipment. nurse may need to suction the secretions
mechanically
6. CHEST TUBE THORACOSTOMY - note the amount, color, viscosity, and character of the
expelled sputum
- Done to drain fluid, blood, or air from the space
around the lungs. ➔ may be necessary to use chest percussion and
- Involves placing a hollow plastic tube between the vibration or a high-frequency chest wall
ribs and into the chest to drain fluid or air from around oscillation (HFCWO) vest to loosen bronchial
the lungs secretions.
- Tube is often hooked up to a suction machine to help
with drainage. 8. CHEST PHYSIOTHERAPY
TABARANZA, CZEJAN RAE BSN-3 23
-includes postural drainage, chest percussion and EFFECTIVE COUGHING TECHNIQUE
vibration, and breathing retraining ● Assume a sitting position and bend slightly forward.
- goals of CPT are: Rationale: This upright position permits a stronger
- remove bronchial secretions cough.
- improve ventilation ● Flex the knees and hips
- increase the efficiency of the respiratory Rationale: Promote relaxation and reduce the strain on
muscles the abdominal muscles while coughing.
POSTURAL DRAINAGE (SEGMENTED BRONCHIAL ● Inhale slowly through the nose and exhale through
DRAINAGE) pursed lips several times.
● Cough twice during each exhalation while
➔ CHET contracting (pulling in) the abdomen sharply with each
BREATHING EXERCISES cough.
● Splint the incision area, if any, with firm hand pressure
GENERAL or support it with a pillow or rolled blanket while coughing
● Breathe slowly and rhythmically to exhale completely
and empty the lungs completely. 9. PULMONARY WEDGE PRESSURE
● Inhale through the nose to filter, humidify, and warm - To confirm high pressure in a pulmonary artery;
the air before it enters the lungs. measured by inserting a Swan-Ganz catheter to a
● If you feel out of breath, breathe more slowly by peripheral way (jugular or femoral), then advancing
prolonging the exhalation time. the catheter to the right atrium>right
● Keep the air moist with a humidifier. ventricle>pulmonary artery>to the branch of
pulmonary artery
DIAPHRAGMATIC BREATHING (To use and strengthen the - At tip of catheter is a balloon that can be inflated,
diaphragm during breathing) causing it to float more distally into a smaller portion
of the pulmonary artery until it is wedged into
● Place one hand on the abdomen (just below the ribs) position.
and the other hand on the middle of the chest - This is an occlusive maneuver that impedes blood
Rationale: Increase the awareness of the position of the flow through that segment of the pulmonary artery.
diaphragm and its function in breathing. Therefore, the wedge pressure is measured
● Breathe in slowly and deeply through the nose, letting immediately and the balloon deflated promptly to
the abdomen protrude as far as possible. restore blood flow
● Breathe out through pursed lips while tightening ➔ normal pulmonary capillary wedge pressure is
(contracting) the abdominal muscles. between 4 to 12 mmHg
● Press firmly inward and upward on the abdomen
➔ normal pulmonary wedge pressure is between 8 to
while breathing out.
12 mmHg
● Repeat for 1 minute; follow with a rest period of 2
minutes.
● Gradually increase duration up to 5 minutes, several
times a day (before meals and at bedtime).
PURSED-LIP BREATHING (To prolong exhalation and
increase airway pressure during expiration, thus reducing the
amount of trapped air and the amount of airway resistance)
● Inhale through the nose while slowly counting to 3
● Exhale slowly and evenly against pursed lips while
tightening the abdominal muscles.
Rationale: Pursing the lips increases intratracheal
pressure; exhaling through the mouth offers less
resistance to expired air.
● Count to 7 slowly while prolonging expiration
through pursed lips
● While sitting in a chair:
○ Fold arms over the abdomen.
○ Inhale through the nose while counting to 3
slowly.
○ Bend forward and exhale slowly through pursed
lips while counting to 7 slowly.
● While walking:
○ Inhale while walking two steps.
○ Exhale through pursed lips while walking four or
five steps.
TABARANZA, CZEJAN RAE BSN-3 24
UPPER RESPIRATORY DISORDERS
1. Rhinitis DESENSITIZE OR SUPPRESS
2. Sinusitis IMMUNE RESPONSE
3. Pharyngitis • Cromolyn (Nasalcrom)
4. Tonsillitis and adenoiditis
5. Peritonsillar abscess INTRANASAL
6. Laryngitis GLUCOCORTICOSTEROIDS
7. Epistaxis • Fluticasone (Flunase)
8. Nasal trauma
9. Laryngeal obstruction
10. Obstructive Sleep Apnea
• Antitussives → for PROLONGED COUGH
RHINITIS • Saline Gargles → for SORE THROAT
• Inflammation of the nasal mucous membranes • Antihistamine → for ALLERGIC RHINITIS
• Also called “common cold” or “coryza” o 1st generation antihistamine =
• 3 TYPES: diphenhydramine (Benadryl)
o Acute Rhinitis o Newer antihistamine =
o Chronic Rhinitis ▪ Loratadine (Claritin)
o Allergic Rhinitis ▪ Fexofenadine (Allegra)
• Common cause → RHINOVIRUS ▪ Cetirizine (Zyrtec)
• HOW IS IT TRANSMITTED? • Combination of DECONGESTANT and
o Inhalation of droplets ANTIHISTAMINE
o Direct contact with contaminated articles o Brompheniramine/Pseudoephedrine
(telephone receivers, doorknobs) (Dimetapp)
• ALLERGIC RHINITIS SINUSITIS
o Hypersensitive reaction to allergens • Inflammation of the sinuses
(pollen, dust, etc) • Most often affected → maxillary sinus
CLINICAL MANIFESTATIONS COMPLICATIONS
1. Sneezing
• Infection of the middle ear and brain
2. Nasal congestion
3. Rhinorrhea (clear nasal discharge ACUTE SINUSITIS
4. Sore throat • Meningitis
5. Water eyes • Brain abscess
6. Cough • Osteomyelitis
7. Low-grade fever PATHOPHYSIOLOGY & ETIOLOGY
o Sustained/elevated temp. suggests
• Principal cause:
bacterial infection or infection in the
o Spread of infection from the nasal
sinuses or ears
passage to the sinuses
8. Headache
o Blockage of normal sinus drainage
9. Aching muscles
• BLOCKAGE OF NORMAL SINUS DRAINAGE
10. Malaise (general discomfort)
• Trapped secretions readily become
• Symptoms continue for 5-14 days.
infected
FOR ALLERGIC RHINITIS: • May result from allergies, nasal
• Symptoms will persist as long as clt is exposed to polyps, deviated septum
specific allergens o Causes edema of the nasal
TREATMENT mucous membranes.
INDICATION DRUGS ACUTE SINUSITIS
Antipyretics • Result of URTI (viral infection, allergic rhinitis)
FEVER • Acetaminophen • Inflammation, edema, & transudation of fluid →
• Nonsteroidal analgesics obstruction of sinus → medium for bacterial growth
SEVERE Decongestants → Acute Sinusitis
NASAL • Pseudoephedrine • Bacterial Organisms that causes 60% of Acute
CONGESTIO • Saline Spray Sinusitis:
N o Streptococcus pneumoniae
PROLONGE Antitussives (cough suppressants) o Hemophilus influenzae
D COUGH o Staphylococcus aureus
SORE • Saline Gargles CLINICAL MANIFESTATIONS
THROAT o Depends on the sinus affected
Antihistamines • General Manifestations:
• Diphenhydramine (Benadryl) o Headache
• Loratadine (Claritin) o Fever
• Fexofenadine (Allegra) o Pain over the affected sinus
ALLERGIC • Cetirizine (Zyrtec) o Nasal congestion and discharge
RHINITIS o Pain and pressure around the eyes
Combination of DECONGESTANT & o Malaisee
ANTIHISTAMINE DIAGNOSTICS AND LABORATORY
• Brompheniramine/pseudophedri
• Culture and Sensitivity Testing
ne (Dimetapp)
o Nasal Smear or material obtained form
irrigation of the sinus
TABARANZA, CZEJAN RAE BSN-3 25
• to identify infectious microorganism
• determine appropriate antibiotic • 3 TYPES OF CHRONIC PHARYNGITIS
therapy 1. Hypertrophic
• Transillumination & Radiograph of the Sinus - General thickening and
o show changes in the shape and fluid in the congestion of pharyngeal mucous
sinus cavity membranes
• History Taking (Allergies) usually confirms the 2. Atrophic
diagnosis - Membrae is thin, whitish,
MEDICAL/SURGICAL MANAGEMENT glistening, wrinkle
A. ACUTE SINUSITIS 3. Chronic granular (Clergyman’s
▪ Saline irrigation Sore Throat)
o If symptoms persist after 7-10 days - Swollen lymph follicles on the
o Removes accumulated exudate & promote pharyngeal wall
drainage
o Inserts catheter thru normal opening under COMPLICATIONS
middle concha
▪ Antibiotics of Choice
✓ Amoxicillin
✓ Ampicillin
✓ For pt allergic to penicillin:
o Trimethoprim/sulfamethoxaz
ole
▪ Oral or topical decongestants may be
administered.
o Oral
✓ Drixoral
✓ Dimetapp
o Topical • STREP THROAT
✓ Afrin o Leads to dangerous cardiac complications
✓ Otrivin ▪ Endocarditis
▪ Heat mist and Saline Irrigation ▪ Rheumatic Fever
o Effective for opening blocked passages o Leads to harmful renal complications
o Allows drainage of purulent discharges ▪ Glomerulonephritis
B. CHRONIC SINUSITIS CLINICAL MANIFESTATIONS
▪ Same with acute sinusitis • Incubation period: 2-4 days
▪ Surgery may be indicated to: • FIRST SYMPTOM
o Correct structural deformities that o Sore throat
obstructs the ostia (openings) of the sinus o Sometimes severe with accompanying
o Includes: dysphagia (difficulty swallowing), fever, chills,
✓ Excising and Cauterizing headache, & malaise
polyps o (Some) exhibit white or exudate patch over the
✓ Correcting deviated septum tonsillar area and swollen glands
✓ Incising and Draining Sinus DIAGNOSTICS AND LABORATORY
▪ Endoscopic Sinus Surgery
• Throat Culture
o Helps provide an opening in the inferior
meatus to promote drainage o Reveals specific causative bacteria
• Biostar/ Strep A optical immunoassay (OIA)
NURSING RESPONSIBILITIES o Used to diagnose group A streptococcal
1. Instruct pt on methods to promote drainage infections
• Inhaling steam (steam bath, hot • Standard 24-hour throat culture and sensitivity
shower, facial sauna) testing
• Increase fluid intake o Identify other organisms
• Applying local heat (Hot Wet Packs) TREATMENT
2. Instruct about side effects of nasal sprays
• Early antibiotic treatment → BEST CHOICE (7-14
• Rebound congestion → if overused
days)
3. Teach about early signs of sinus infection
o Penicillin or its derivates
4. Recommend preventive measures
o For penicillin-sensitive patients:
• Following healthy practices
▪ Erythromycin
• Avoiding contact with people with
URTI NURSING RESPONSIBILITIES
1. Instruct pt to avoid contact with others until fever
subsides
PHARYNGITIS 2. Avoid use of alcohol, tobacco, secondhand smoke,
• Inflammation of the throat exposure to cold
• Associated with rhinitis or other URIs 3. Use disposable masks
• Cause= VIRUS or BACTERIA 4. Drink plenty of water/fluids
o Group A Streptococci 5. Gargle with warm saline → relieve throat
▪ Most serious bacteria discomfort
▪ Causes strep throat 6. Lozenges → keep throat moistened
• HIGHLY CONTAGIOUS!
o Spreads via:
▪ Inhalation
▪ Direct contamination with droplets
TABARANZA, CZEJAN RAE BSN-3 26
TONSILITIS AND ADENOIDITIS SURGICAL
• Tonsilitis • Tonsillectomy
o Inflammation of the tonsils • Adenoidectomy
o Common diagnosis TONSILLECTOMY ADENOIDECTOMY
o Causative Agent → Group A streptococcus • If medical treatment is • Removal of the
• Adenoiditis unsuccessful adenoids
o inflammation of the adenoids • There is:
o Abnormally large lymphoid tissue mass o Severe
near the center of the posterior wall of the hypertrophy
nasopharynx o Peritonsillar
PATHOPHYSIOLOGY/ETIOLOGY abscess
• Tonsils and adenoids are lymphatic tissues and • Causes occlusion
common sites of infection of the pharynx
• May be primary or secondary to other URTI’s • Difficulty swallowing
COMPILICATIONS • Endangering airway
PERFORMED ONLY WHEN PT HAS:
• Chronic tonsillar Infection
o Leads to enlargement and partial upper ✓ Repeated bouts of tonsillitis
airway obstruction ✓ Hypertrophy of the tonsils and adenoids
• Chronic Adenoidal Infection ✓ Repeated attacks of purulent otitis media
o Can result in acute or chronic infection of ✓ Suspected hearing loss due to otitis media
middle ear (otitis media) ✓ Exacerbation of asthma or rheumatic fever
• Infection can EXTEND to: MOST SERIOUS COMPLICATION:
o Middle ear by auditory tubes (eustachian = DELAYED HEMORRHAGE
tubes)
o May result in ACUTE OTITIS MEDIA NURSING RESPONSIBILITIES FOR CLT UNDERGOING
• Can lead to spontaneous rupture of TONSILLECTCOMY AND ADENOIDECTOMY
eardrums
ASSESSMENT
• Further extension of infection into
mastoid cells → ACUTE • Clt’s understanding about the procedure
MASTOIDITIS • Baseline Vital Signs
• Otitis Media as a chronic, low-grade, smoldering • Ask clt if:
process o Wearing dentures
o Causes PERMANENT DEAFNESS o Last food or drink
CLINICAL MANIFESTATIONS o Recent use of ASPIRIN, NSAIDS, & other
meds(Herbal supplements such as FeverFew
• TONSILLITIS or Gingko) that prolong bleeding time
o Sore throat • Laboratory results, special attention to
o Fever o HCT
o Snoring o Platelet count
o Difficulty in swallowing o Clotting time
• ENLARGEMENT OF THE ADENOIDS • Because of high risk for postoperative
o Mouth breathing hemorrhage
o Ear-ache
o Draining ears NURSING DIAGNOSES
o Frequent head colds EXPECTED OUTCOMES
o Bronchitis ✓ Will maintain a patent airway
o Foul-smelling breath (halitosis) with clear breath sounds
o Voice impairment ✓ Will expectorate secretions
o Noisy respiration and vomitus as needed
o Nasal obstruction INTERVENTIONS
DIAGNOSTICS & LABORATORY 1. Position pt on either side with
• Physical examination emesis basin
• Throat Culture and Sensitivity Test • to catch drainage or
RISK FOR
o Determines the causative microorganism vomitus; retained secretions
ASPIRATION
o Determine the appropriate antibiotic can obstruct airway and
therapy. cause aspiration
• Comprehensive Audiometric Examination R/t impaired 2. Assess Gag reflex & ability to
o For adenoiditis swallowing st swallow
o If recurrent episode of suppurative otitis throat surgery • it increases risk for aspiration
media and reduced if depressed
MEDICAL-SURGICAL MANAGEMENT gag reflex st 3. Elevate head of bed to 45
anesthesia degrees when fully awake
MEDICAL
• To decrease surgical edema
• Antibiotic Therapy → to treat infection & assoc.
• Increase lung expansion
discomfort
4. Monitor every 1 hour: RR,
• Analgesics
rhythm, & effort
✓ Acetaminophen
• To rule out partially
✓ Saline gargles
obstructed airway:
o Increased RR
o Decreased breath
sounds
TABARANZA, CZEJAN RAE BSN-3 27
5. Assess for lethargy, behavior
changes, or disorientation
PERITONSILLAR ABSCESS
• Decreased orientation
indicated poor air
exchange
6. Have oral suction equipment
ready
• prompt oral suctioning
removes secretions/vomitus
from the mouth, preventing
aspiration
RISK FOR EXPECTED OUTCOME
IMPAIRED • Client will maintain an intact
TISSUE suture line
INTEGRITY
related to injury • Abscess that develops in the connective tissue
to the suture line INTERVENTIONS
between the CAPSULE OF THE TONSIL and the
1. Monitor for bloody drainage from
CONSTRICTOR MUSCLE of the pharnx, in the
mouth or frequent swallowing
anterior pillar and soft palate
• Indicate increased bleeding
• RULE:
from suture site
o Peritonsillar abscess occurs several days
2. Instruct client NOT TO COUGH,
after an acute tonsillar infection
CLEAR THROAT, BLOW NOSE,
o Usually caused by Group A
OR USE STRAW in first postop
streptococcus
days
• It increases pressure on the CLINICAL MANIFESTATIONS
suture lines GENERAL SYMPTOMS
• May cause disruption and • Difficulty and pain with swallowing (dysphagia)
bleeding • Thickening of voice/Difficulty talking
3. Avoid carbonated fluid, high in • Drooling
citrus content • Fever
• Caustic to surgical site • Malaise
• May traumatize tissue, • Ear pain
disrupting the suture line PHYSICAL EXAM
4. Encourage to first try ice chips →
small chips → popsicles → full • Marked swelling of the soft palate
fluid o Often to the extent of half occluding the
• Gradual introduction to slowly opening from the mouth into the pharynx
try swallowing, without DIAGNOSTICS & LABORATORY
disrupting the suture line • DRAINAGE FROM ABCESS IS CULTURED
5. Soft food for first 24-hours o To identify the microorganisms
postop (gelatin & sherbet) • SENSITIVITY STUDIES
• Less likely to traumatize suture o To determine the appropriate antibiotic
line therapy
ACUTE PAIN EXPECTED OUTCOMES MEDICAL/SURGICAL MANAGEMENT
Related to • Client will acknowledge relief MEDICAL
surgical incision from pain meds • Antibiotic Therapy
in the throat • Demonstrate improved ability • Usually penicillin
to swallow • If antibiotic is not prescribed until later, the abcess
must be DRAINED
INTERVENTIONS SURGICAL
1. Anticipate the need for pain relief • Incision & Drainage (I&D)
2. Apply ice collar o Done if abscess partially blocks
• Cold reduces swelling and oropharynx
inflammation in soft tissues o Local anesthetic is sprayed or painted in
in incision site the surface of abscess
• Help control bleeding o Contents are evacuated
• Reduce edema o Performed in SITTING POSITION/SEMI-
• Block pain receptors FOWLERS
▪ It is easier to expectorate the pus
and blood that accumulate in the
pharynx
▪ To prevent aspiration
o ICE COLLAR may be given
▪ To reduce swelling and pain
• Tonsillectomy
o If repeated episodes of peritonsillar
abscess
o To eliminate unsuspected asymptomatc
pockets of infection
TABARANZA, CZEJAN RAE BSN-3 28
• Resting in bed
NURSING INTERVENTIONS/PATIENT EDUCATION • Inhaling cool steam or an aerosol
• For RELIEF o Appropriate antibacterial therapy
o Topical anesthesia CHRONIC LARYNGITIS
o Throat irrigation • Resting of voice
o Frequent use of mouthwashes/gargles • Eliminating any primary respiratory tract infection
▪ Gargle at interval of 1-2 hours for • Restricting smoking
24-36 hours • Use of topical corticosteroids
o Use Saline or alkaline solutions o Beclomethasone dipropionate (Vanceril)
▪ at temp of 105 F to 110 F (40.6 C- inihalation
43.3 C) • Reduces local inflammatory reactions
LARYNGITIS
NURSING RESPONSIBILITIES
• Rest voice
• Maintain humidified environment
• If laryngeal secretions are present
o Expectorants suggested
o Daily fluid intake = 3 Liters
EPISTAXIS (NOSEBLEED)
• Hemorrhage from the nose
ETIOLOGY
• Rupture of tiny, distended vessels in mucous
membrane in any area of nose
• Most common site: anterior septum
• Inflammation and swelling of the mucous o Where 3 major blood vessels enter nasal
membranes that lines the larynx cavity
1. Anterior ethmoidal artery
CAUSES:
(Kesselbach’s Plexus)
• Voice abuse o Anterior roof
• Exposure to dust, chemicals, smoke, and other 2. Sphenopalatine artery
pollutants o Posterosuperior
• URTI 3. Internal Maxillary Branches
• Isolated infection involving only the vocal cords. o Plexus of veins
located at back
PATHOPHYSIOLOGY/ETIOLOGY of the lateral
wall under
• Main cause is ALWAYS a VIRUS
inferior
o Bacteria may be secondary
turbinate
• Usually associated with:
• CAUSES:
o Acute rhinitis
o Trauma
o Nasopharyngitis
o Infection
• ONSET o Drugs
o Exposure to sudden temperature changes o CVD
o Dietary deficiencies
o Blood dyscrasias (blood disorder)
o Malnutrition o Nasal Tumor
o Lack of immunity o Low humidity
• SEASON o Foreign body in nose
o Common in winter o Deviated nasal septum
o Easily transmitted o Rheumatic fever
CLINICAL MANIFESTATIONS o Vigorous nose-blowing
ACUTE LARYNGITIS o Nose-picking
• Hoarseness DIAGNOSTICS, LABORATORY, ASSESSMENT FINDINGS
• Complete loss of voice (aphonia) INSPECTION
• Severe cough • Inspect nares using nasal speculum and light
o Dry, nonproductive o Reveals area of bleeding
• Throat irritation • Use Tongue blade
CHRONIC LARYNGITIS o To check the back of the throat
• Marked by persistent hoarseness • Use Laryngeal Mirror
DIAGNOSTICS & LABORATORY o To view the area above and behind uvula
• Laryngoscopy MEDICAL-SURGICAL MANAGEMENT
o If hoarseness persists more than 2 weeks • Depends on the location of the bleeding site
▪ If more than 2 weeks INITIAL TREATMENT
• Sign of laryngeal cancer • Apply direct pressure
MEDICAL-SURGICAL MANAGEMENT • Pt sits upright with head titled FORWARD
ACUTE LARYNGITIS • To prevent swallowing and aspiration
• Resting of voice of blood
• Avoid smoking
TABARANZA, CZEJAN RAE BSN-3 29
• Directed to pinch the soft outer portion • Irregularity in the septum results in nasal
of the nose against the midline obstruction
septum for 5-10 mins • May be a
o Deflection from the midline in the form of
lumps or sharp projections
o Curvature in the shape of a “s”
FOR ANTERIOR NOSEBLEED
• Marked deviation can result in complete obstruction
• Treated with a silver nitrate application and of one nostril and interference with sinus
Gelfoam, or by electrocautery drainage
• Topical vasoconstrictors may be prescribed • May be:
o Adrenaline (1:1000) o Congenital
o Cocaine (0.5%) o Trauma
o Phenylephrine 2. NASAL POLYPS
FOR POSTERIOR REGION BLEEDING • Grapelike swellings
• Cotton pledgets soacked in vasoconstricting • Arises from nasal mucous membranes
solutions inserted in nose • Result from
• To reduce blood flow o Chronic irritation r/t infection or allergic
• Improve examiner’s view of the rhinitis
bleeding site • They obstruct nasal breathing and sinus drainage
• Suction → lead to sinusitis
• Most are benign
HOW TO SEARCH FOR BLEEDING SITE? • Can recur even when removed
3. HYPERTROPHIED TURBINATES
• Anteroinferior → Anterosuperior → posterosuperior
• Enlargements of the nasal conchae (the 3
→ posteroinferior quadrant
bones that project from the lateral wall of the
nasal cavity)
IF BLEEDING ORIGIN CANNOT BE IDENTIFIED • Results from chronic rhinitis
• Nose may be packed with gauze impregnate with • PROGRESSION OF THE DISEASE
petrolatum o Chronic rhinitis → hypertrophy →
• Remain in place for 48 hours sinusitis
• If necessary, 5-6 days = to control CLINICAL MANIFESTATIONS
bleedong • History of sinusitis
• Topical anesthetic spray and decongestant
• Difficulty breathing out of one nostril
• Used prior to inserting gauze packing
• Frequent nosebleed (epistaxis)
NURSING RESPONSIBILITIES • Nasal discharge
• Monitor VS INSPECTION
• Assess for signs of continued bleeding 1. USING NASAL SPECULUM
• Apply pressure and ice packs o Left or right deviation of the nasal septum
• He may use recommended humidification o Number and location of the polyps
• Use nasal lubricant o Enlarged turbinates
• To keep mucous moist MEDICAL AND SURGICAL MANAGEMENT
DONTS 1. SUBMUCOUS SURGICAL RESECTION OR
• AVOID SEPTOPLASTY
o Vigorous nose blowing o To restore normal breathing
o Nose picking o To permit adequate sinus drainage (deviated
o Other nose trauma septum)
• Do not swallow blood o PROCEDURE
o Spit out any blood oozing 1. Incision thru mucous membrane
• Do not attempt to remove nasal packing or to cut 2. Removal of the portion of the septum
the string anchoring the packing 3. After, both sides of septum are packed
• Take pain meds as ordered with gauze (24-48 hours)
o Do not use ASPIRIN or IBUPROFEN 4. Moustache dressing or drip pad →
to absorb any drainage.
NASAL OBSTRUCTION 2. RHINOPLASTY
• Obstruction of the nasal passage o Reconstruction of the nose
• 3 PRIMARY CONDITIONS LEAD TO NASAL o Enhance the appearance cosmetically
OBSTRUCTION o Corrects any structural nasal deformities that
1. Deviated septum interfere with air passage
2. Nasal Polyps o PROCEDURE
3. Hypertrophied turbinates 1. Surgeon incises inside the nostril
2. Restructures the nasal bone and
cartilage
3. Nasal cavity is packed with gauze
4. Nose is taped
5. Nasal splint → maintains shape and
structure of the nose; reduces edema;
NASAL POLYPS remained for 1 week
3. STEROIDAL NASAL SPRAY (medical)
o To reduce inflammation or direct injection of
PATHOPHYSIOLOGY & ETIOLOGY
steroid into the polyps
1. DEVIATED SEPTUM 4. POLYPECTOMY
TABARANZA, CZEJAN RAE BSN-3 30
o Removal polyps with nasal snare or laser unser Foreign bodies → Aspirated to pharynx, larynx, or trachea
local anesthesia → causes two-fold problem → obstructs air passage →
o Polyps are examined microscopically to rule difficulty breathing → asphyxia (deprived of oxygen)
out malignant disease
To solve = Heimlich Maneuver or subdiaphragmatic
5. ASTRIMGENTS OR AEROSOLIZED abdominal thrust
CORTICOSTEROIDS CLINICAL MANIFESTATIONS
o To shrink them close to the nose LARYNGEAL TRAUMA
6. TURBINECTOMY • Neck swelling
o Removal of the turbinate • Bruising
• Tendeness
NURSING RESPONSIBILITIES (FOR SURGERY) • PE FINDINGS
- Surgery for nasal obstruction is usually and o Stridor in larynx → indicates airway
outpatient basis obstruction
1. Thorough explanation of the procedure o Dysphagia (difficulty swallowing)
• To alleviate anxiety o Hoarseness
o Cyanosis
• Emphasize nasal packing &
o Hemoptysis (bloody sputum)
necessitating mouth breathing
postop TOTAL OBSTRUCTION
• Ice pack reduces pain and swelling • Choking client will clutch their throats → universal
2. Position client in SEMI-FOWLER’S sign of choking
• To promote drainage • Can cause death due to respiratory arrest
• Reduces edema • PARTIAL OBSTRUCTION → difficulty breathing
• Enhance breathing DIAGNOSTIC & LABORATORY FINDINGS
3. Monitor Vital Signs • LARYNGOSCOPY
4. Provide oral hygiene and saline mouth rinse • Reveals the extent of trauma and
• To keep mucous membranes moist internal swelling
5. Tell that feeling or hearing a sucking noise when • RADIOGRAPHS & OXYGENATION
swallowing is NORMAL • Performed after establishing patent
• Will resolve wen nasal packing is established
removed
MEDICAL-SURGICAL MANAGEMENT
6. INSTRUCTION TO PREVENT BLEEDING:
• Do not bend over MEDICAL
• Do not blow nose 1. Heimlich maneuver
• If sneezing, keep mouth open • To force object out of the upper respi passages
• Avoid contact with NOSE or 2. Epinephrine or Corticosteroid
SURROUNDING TISSUE • To treat allergic reactions resulting in severe
• Keep head elevated with extra pillow inflammation and edema
when lying down
• Avoid heavy lifting SURGICAL
• DO NOT USE 1. Emergency Tracheostomy
o Aspirin • Surgical opening into the trachea
o Ibuprofen
o Alcohol OBSTRUCTIVE SLEEP APNEA
o Tobacco SLEEP APNEA SYNDROME
LARYNGEAL TRAUMA/OBSTRUCTION • Characterized by frequent, brief episodes of
respiratory standstill during sleep
• Edema of the larynx
• Classified according to respiratory muscle effort:
• Why it is FATAL?
1. CENTRAL
o Larynx is a stiff box that cannot be stretched
o Air movement is absent secondary to
o Swelling of the laryngeal mucous may close off
absence of ventilatory efforts.
the opening tightly → leading to
o Brain malfunctions in its normal signal to
SUFFOCATION
breathe.
• It is an occasional cause of death in severe 2. OBSTRUCTIVE
anaphylaxis (angioneurotic edema) o Air movement is absent secondary to
PATHOPHYSIOLOGY & ETIOLOGY pharyngeal obstruction.
LARYNGEAL TRAUMA o Chest and abdominal movements are
• Occurs during motor vehicle accidents present
o When neck strikes the steering wheel o This is the most common form of sleep
o Or blunt trauma in neck regions apnea
• Other causes 3. MIXED
o Endoscopic & endotracheal intubations o Combination of central and obstructive
o Fracture of the thyroid cartilage sleep apnea in one apneic episode
RISK FACTORS
LARYNGEAL OBSTRUCTIONS • 1/10 people with = over 65 y.o.
• Edema from an allergic reaction • Overweight
• Severe head and neck injury • After menopause
• Severe inflammation and edema of the throat • Ethnicity
• Aspiration of foreign bodies o African-american
• PROCESS: o Hispanics
o Pacific Islanders
TABARANZA, CZEJAN RAE BSN-3 31
• Heredity ▪ Made by dentist/orthodontist
• Having Smaller airways 5.NONINVASIVE POSITIVE PRESSURE
• Allergies VENTILATION (NPPV)
• Cigarette smokers o Application of positive pressure via full-
• Use of sedative or hypnotic medicatins face mask, nasal mask, or cannula with
• Frequent and heavy intake of alcohol supplemental oxygen
▪ To enhance ventilation
PATHOPHYSIOLOGY & ETIOLOGY
o 2 COMMON USED TYPES
• Reduced diameter of the upper airway → airway 1. Continuous Positive Airway
collapses secondary to normally reduced muscle tone Pressure (CPAP)
during sleep → obstructive apnea • Provides airway
pressure during
• Repeated apneic spells → have serious effects on the inspiration & expiration
cardiopulmonary system 2. Bilevel Positive Airway Pressure
(BIPAP)
• Clt with hypertension → greater risk of cerebrovascular • Provides two-levels of
accident & myocardial infarction, heart arrhythmia, & pressure:
heart failure o Inspiratory
airway pressure
CLINICAL MANIFESTATIONS o Expiratory
GENERAL SYMPTOMS OF SLEEP APNEA airway pressure
• Restless sleep ▪ DISADVANTAGES:
• Do not completely
• Loud, heavy snoring
eliminate problem
• Excessive daytime sleepiness → can occur while
driving or working • Dry mouth, rhinitis, &
sinus congestion
• Morning headaches
• Loss of energy SURGICAL MANAGEMENT
• Trouble concentrating 1. UVULOPALATOPHARYNGOPLASTY
• Irritability • Surgical procedure to remove tissues in the
• Forgetfulness throat including
• Mood or behaviour changes → anxiety and o Uvula
depression o Palate
• Decreased interest in sex o Pharynx
• Systemic hypertension • To relive obstruction
2. TRACHEOSTOMY
• Dysrrhythmias
• Successful treatment
• Enuresis
• DISADVANTAGES
DIAGNOSTICS & LABORATORY o Alteration of appearance
• POLYSOMNOGRAPHY o Difficult for obese
• To determine nature of sleep apnea o He/she may plug it during the day.
• Includes test to monitor: TREATMENT/MEDICATIONS
o Respiratory status FOR CENTRAL SLEEP APNEA
o Cardiac status
o Record brain activity, eye movement, • Take drugs at bedtime
respiratory and heart rates • PROTRIPTYLINE
o Amount of air that moves in and out of o Vivactil
the lungs o Triptil
o Oxygen concentration in blood ▪ Increases the respiratory drive
▪ Improve upper airway muscle
MEDICAL-SURGICAL MANAGEMENT
tone
Goal: • LOW-FLOW OXYGEN
✓ Improve quality of sleep and daytime wakefulness o Use at night
✓ Reduce risks for cardiovascular problems o To relieve hypoxemia
NURSING MANAGEMENT
1. Lifestyle changes 1. Reassurance and adequate instruction about
▪ Losing weight condition
▪ Quit smoking, alcohol 2. Thorough explanation of disease process,
2. Use special pillows to keep in side-lying position polysomnography, and treatment
3. Use allergy medications or saline nasal spray 3. Collaborates with respiratory therapist to instruct
▪ To reduce congestion and clt in the use of CPAP or other NPPV
dryness • Furnishes info about sleep apnea
4. Fitting client for oral appliance adjusting the lower • Its potential complication
jaw and tongue
▪ Airway remains open while
sleeping
TABARANZA, CZEJAN RAE BSN-3 32
VENTILATION DISORDER
TOPIC OUTLINE • Pain decreases as fluid increases
1. Pleuritis • Develops:
2. Pleural effusion o Dry cough
3. Pneumothorax o Fatigues easily
4. Trauma of the chest and lung, rib fracture, o Dyspnea
pleural confusion o Friction rub (coarse sounds heard
5. Inhalation injury during inspiration & early expiration)
a. Smoke o Decreased ventilation
b. Near drowning o Due to atelectasis
Transcribed by: Barte, M.G., Maningo, F.E. & Tabaranza, C.R. o Hypoxemia
o Hypercapnia (CO2)
PLEURAL DISORDERS Diagnostics & Laboratory
• Involves visceral and parietal pleura • Auscultation = little fluid accumulated
• Affects pleural space • Diagnostic Tests
PLEURITIS/ PLEURISY • Chest x-rays
• Sputum analysis
• Thoracentesis
• Pleural biopsy (less common)
Medical/Surgical Management
Medical
• Analgesics
• Topical Application
• NSAIDs = indomethacin (Indocin) → promote
effective coughing
• Intercostal Nerve Block = severe pain
Nursing Management
1. Enhance comfort
a. Frequent turning of body when lying
Rationale: to splint the chest wall and
• inflammation of both parietal and visceral layers reduce the stretching of the pleurae
• PARIETAL PLEURA = has nerve endings 2. Nursing Education
• VISCERAL PLEURA = does not have nerve • use the hands or pillow
endings Rationale: to splint rib cage while
coughing
PATHOPHYSIOLOGY/ETIOLOGY
• may develop in conjunction with: PLEURAL EFFUSION
• Pneumonia
• Upper Respiratory Tract Infection
• TB
• Collagen disease
• After trauma to chest
• Pulmonary infarction
• PE (Pulmonary Embolism)
• Pt w/ Primary or Metastatic Cancer
• Pt after Thoracotomy
DURING ACUTE PHASE
• Pleurae are inflamed, thick and swollen • Collection of fluid in the pleural space
• An exudate forms from fibrin and lymph • Rare primary disease process
• Eventually, pleurae become rigid • Normal Amount of fluid in Pleural Space = 5 to
• During inspiration, inflamed pleurae rub together, 15 mL
causing severe sharp pain. • Accumulated fluid may be so large that the lung
partially collapses on the affected side
CLINICAL MANIFESTATION o As a consequence, pressure is placed on
• Pleuritic Pain (sharp chest pain) the heart and other organs of the
o Inflamed membranes rub together during mediastinum.
respiratory movement resulting severe, • Maybe a complication of:
sharp, knife-like pain a. Heart failure
o Usually occurs in one side b. TB
o HELD BREATH = minimal/absent c. Pneumonia
o LOCALIZED/RADIATES = shoulder to d. Pulmonary infections (particularly Viral)
abdomen e. Nephrotic syndrome
• Shallow respirations st excruciating pain f. Connective tissue disease
• Accumulation of pleural fluid g. PE
h. Neoplastic tumors
TABARANZA, CZEJAN RAE BSN-3 33
• BRONCHOGENIC CARCINOMA o Connected to a water-seal drainage
o Most common malignancy associated with system/suction
Pleural Effusion ▪ RATIONALE:
▪ Repeated thoracentesis is painful
Pathophysiology/Etiology ▪ To evacuate the pleural space
• Effusion can be composed of relatively clear fluid which Caused by MALIGNANCY
may be: 3. CHEMICAL PLEURODESIS
o Transudate o Rationale:
o Exudate ▪ To obliterate the pleural space
o Bloody ▪ To prevent reaccumulation of fluid
o Purulent 4. SURGICAL PLEURECTOMY
• TRANSUDATE
o Occurs when factors influencing the formation 5. IMPLANTATION OF PLEUROPERITONEAL
and reabsorption of pleural fluid are altered SHUNT
(hydrostatic or oncotic pressures)
o Indicates ascites, CHF, renal failure NURSING MANAGEMENT
• EXUDATE 1. Documentation of fluid amount (thoracentesis) for
o Result of inflammation by bacterial products o laboratory testing
tumors 2. Monitor the function of the system and record
amount of drainage at prescribed intervals.
CLINICAL MANIFESTATIONS 3. Nursing care R/T the underlying cause is specific to
• Dyspnea and coughing the underlying condition.
• Size of effusion determines severity
o LARGE PLEURAL EFFUSION
▪ Shortness of breath
▪ Dull, flat sound when percussed
▪ Egophony present above To Patient with Pleural Effusion secondary to MALIGNANCY
percussion • PAIN MANAGEMENT (PRIORITY)
▪ Tracheal deviation 1. Assume patient in a least painful position
o SMALL-MODERATE PLEURAL 2. Evaluate pain level
EFFUSION
▪ Dyspnea is absent. Outpatient with Pleural catheter for drainage
DIAGNOSTICS & LABORATORY 1. Health Education
DIAGNOSTICS o Proper management and care of the
1. Chest x-ray catheter and drainage system
2. Ultrasound o Record the amount of drainage at
3. Physical examination prescribed intervals.
4. Thoracentesis PNEUMOTHORAX
5. Pleural biopsy
LABORATORIES (pleural fluid is analyzed)
1. Bacterial culture
2. Gram stain
3. Acid-Fast Bacillus (AFB) stain → for Tuberculosis
4. RBC & WBC counts
5. Chemistry Studies
a.
b. Glucose
c. Amylase
d. Lactic dehydrogenase (LDH)
e. Protein
6. Cytology analysis → malignant cells • HEMOTHORAX
7. pH o Blood in chest cavity
MEDICAL-SURGICAL MANAGEMENT o Due to torn intercostal vessels,
• EXUDATE Pleural Fluid = treatment of primary laceration of lungs
cause instituted • HEMOPNEUMOTHORAX
o Blood and air are found in chest cavity
MEDICAL • PNEUMOTHORAX
• Analgesics o Collapsing of a lung due to air
accumulating in the pleural space
SURGICAL (intrapleural space)
• Can be partial or total collapse (usually affects ONE
lung)
1. THORACENTESIS
o Rationale: • CAUSES:
o Spontaneous
▪ To relieve dyspnea and
o Trauma to chest (blunt or penetrating)
respiratory compromise
o Lung disease
o May be performed with ULTRASOUND
o Medical procedure (line placement, mech.
guidance (depending on the size of the
Venti)
effusion)
2. CHEST TUBE DRAINAGE • TYPES OF PNEUMOTHORAX
1. Closed Pneumothorax
TABARANZA, CZEJAN RAE BSN-3 34
2. Open Pneumothoax • Relieves pressure and vent the
3. Tension Pneumothorax intrathoracic air to the outside
3. CHEST TUBE
o Inserted and connected to suction
1. CLOSED PNEUMOTHORAX
o To remove remaining air and fluid and
• Air leaks into the intrapleural space without an reexpand the lung
outside wound o If continuous to leak:
• Chest & Pleural are intact o Air must be removed by a chest tube
• CAUSES: with water-sea drainage
o RIB FRACTURE
▪ Bony part of rib pierces the lung GENERAL DIAGNOSTICS
causes air to be released into space
• Chest x-ray
o SPONTANEOUS PNEUMOTHORAX
• Ultrasound
▪ Defect in the alveolar wall & visceral
pelura • CT scan
▪ Causes to form a sac-like blister GENERAL SIGNS AND SYMPTOMS FOR
“pulmonary bled” → ruptures PNEUMOTHORAX
▪ Not caused by injury MNEMONIC: COLLAPSED
▪ CATEGORIES: • Chest pain (sudden/sharp)/ Cyanosis
1. PRIMARY PNEUMOTHORAX • Overt tachycardia & tachypnea
- Occurs in ppl w/out lung disease • Low blood pressure
- <30 y.o., tall, thin • Low SpO2
2. SECONDARY PNEUMOTHORAX
• Absent breath sound on the affected side
- Occurs in ppl with lung disease
• Pushing trachea to unaffected side (tension pneu.)
(copd, thin, asthma)
• Subq emphysema
2. OPEN PNEUMOTHORAX (sucking chest wound) • Expansion of chest is unequal
• Opening in the chest wall that • Dyspnea
causes passage between NURSING INTERVENTION
outside air & intrapleural space • Place sterile occlusive dressing tape on 3 sides
• Allows are to pass back&forth o Leave 4th side untapped
in inspiration and expiration ▪ To allow exhaled air to leave the
• Can hear a SUCKING CHEST opening but seal over opening
SOUND when inhaling
PATHOPHYSIOLOGY • Monitor breath sounds (equal?)
Body is shunting air thru chest wall opening → sucking • Head of Bead in Fowler’s position
sound → intrapleural pressure = outside pressure → lung TRAUMA OF THE CHEST AND LUNG (RIB FRACTURE,
collapse
FLAIL CHEST, PULMONARY CONFUSION)
3. TENSION PNEUMOTHORAX
• Can happen when open or closed
• A MEDICAL EMERGENCY!
• Happens when an opening to the intrapleural space
creates a one-way valve → air collects but can’t
escape
• Leads to increased intrathoracic pressure
• Compression on lungs & heart
o Decreases venous return 1. Rib Fracture
• Mediastinum shift • broken ribs
o Heart, trachea, esophagus, 2. Fail Chest
vessels shifts to the • 2 or more adjacent ribs fracture;
unaffected side fragments are free-floating
CLINICAL MANIFESTATIONS 3. Pulmonary Confusion
• Crushing or bruising of the lungs
• As pt tries to compensate:
o Tachypnea -> to maintain O2
o Tachycardia → cuz heart has nothing to 1. RIB FRACTURE
pump
o Hypotension → due to reduced cardiac
output
o Shock
o Jugular Venous Distention
• LATE SIGNS
o Tracheal deviation
MEDICAL MANAGEMENT
1. Give High Concentration of Oxygen
• To treat hypoxia
2. Insert Large-Bore Needle at the 2nd intercostal
space, midclavicular line
• To convert quickly to a simple • May result from a hard fall or a blow to the chest.
pneumothorax • Most common type of chest trauma
TABARANZA, CZEJAN RAE BSN-3 35
• Heals in 3-6 weeks o Paradoxical movement develops
RIB FRACTURE SITES • During inspiration, chest expands but
free-floating segments move inward
• Rare but FATAL
(instead of outward)
FIRST 3 RIBS • Assoc. with laceration of the
• During expiration, free-floating
subclavian artery and veins
segments move outward, interfering
5TH – 9TH RIBS • Most common sites of fracture with exhalation
• Assoc. with injury to the spleen o Affects intrathoracic
Lower Rib pressures → decreasing
and liver
CLINICAL MANIFESTATIONS movement of air
PATHOPHYSIOLOGIC PHENOMENA
• If CONSCIOUS
o Fractured area is BRUISED • Increased Dead Space
o Severe pain • Reduced gas exchange
o Tenderness • Decreased lung compliance
o Muscle spasm • Retained airway secretions
▪ Mas mugrabe if: • Atelectasis
o Coughing • Hypoxemia
o Deep breathing CLINICAL MANIFESTATIONS
o Motion
• GENERAL
• Alleviating Factors
o Severe pain on inspiration & expiration
o Splint chest, breathing in
o Shortness of breath
shallow manner
• For FLAIL CHEST
o Avoid sighs, deep breathing,
o Hypotension
coughing, movement.
o Inadequate tissue perfusion secondary to
DIAGNOSTICS decreased cardiac output
• Chest X-ray o RESPIRATORY ACIDOSIS due to
• Rib series increased CO2
• ECG DIAGNOSTICS
• Arterial Blood Gases • Serial Chest X-rays
MEDICAL MANAGEMENT • To confirm the diagnosis
1. SEDATION • Taken in several angles.
o To relieve pain • ABG
o Allow deep breathing & coughing • Pulse oximetry
2. INTERCOSTAL NERVE BLOCK & ICE OVER • Pulmonary Function studies
FRACTURE SITE
MEDICAL-SURGICAL MANAGEMENT
o Alternative
3. CHEST BINDER 1. Supporting chest with an ELASTIC BANDAGE or RIB
o Decreases pain on movement BELT
o Pain abates in 5-7 days • To immobilize rib fractures
4. EPIDURAL ANALGESIA, PATIENT- • DISADVANTAGES
CONTROLLED ANALGESIA, OR NON-OPIOID o Decreased lung expansion
ANALGESIA o Pulmonary complication (pneumonia &
o Control discomfort atelectasis)
o Limited only to multiple rib fracture
2. FLAIL CHEST 2. ANALGESIC = Codeine or Regional Nerve Block
• For pain
3. FOR FLAIL CHEST
o Support ventilation
o Clearing lung secretions
o Managing pain
o MILD TO MODERATE FLAIL CHEST
INJURIES
o Restrict fluid
o Prescribe diuretics
o Corticosteroids
o Albumin
o Pulmonary physiotherapy
• Occurs when 2 or more adjacent ribs are fractured at 2 o SEVERE FLAIL CHEST INJURY
or more sites o Endotracheal intibation
• Has free-floating rib segments o Mechanical ventilation with colume-
• As a result cycled ventilator
o Chest wall loses stability o PEEP
o Respiratory impairment • To splint chest wall
o Severe respiratory distress • To correct abnormalities in gas
PATHOPHYSIOLOGY & ETIOLOGY exchange
• FLAIL CHEST • To treat underlying pulmonary
o Occurs when two or more adjacent ribs fracture contusion
in multiple places and the fragment are free- • To stabilize the thoracic cage
floating • To allow fracture to heal
o Affects the stability of the chest wall → 4. FOR PULMONARY CONFUSION
impairment in chest-wall movement o RESTRICT FLUID!!
TABARANZA, CZEJAN RAE BSN-3 36
• Due to capillary damage a. Positive End Expiratory Pressure (PEEP)
o Antibiotics → prevent infection • To improve oxygenation, prevent
5. ENDOTRACHEAL INTUBATION AND MECHANICAL aspiration, correct intrapulmonary
VENTILATION shunting & ventilation-perfusion
- If client’s respiratory status is greatly compromised abnormalities (caused by aspiration of
water)
NURSING RESPONSIBILITIES 5. Initiate ECG Monitoring
1. Apply immobilization device • Dysrhythmias can frequently occur
2. Instruct about application & removal of rib belt or 6. Asist Nasogastric Intubation
elastic bandage • to prevent pt from regurgitating gastric
3. Stress to take a DEEP BREAT every 1-2 hours contents
even if painful 7. Insert Indwelling Catheter to monitor urinary output
4. Monitor signs of: • Metabolic acidosis compromises renal
a. Respiratory distress function
b. Infection 8. Admit pt to ICU if appears:
c. Increased pain ✓ Hypoxic or ischemic cerebral injury
✓ Acute respiratory distress syndrome
✓ Cardiac arrest
INHALATION INJURY (NEAR DROWNING & SMOKE )
1. NEAR-DROWNING
2. SMOKE INHALATION INJURY
• Most common consequence is hypoxemia
• 4th leading cause of accidental death
RISK FACTORS
o Alcohol ingestion
o Inability to swim
o Diving injuries
o Hypothermia
o Exhaustion
• Efforts to save the victim should not be abandoned
prematurely
• Successful resuscitation with full neurologic recovery is
POSSIBLE
o Due to a decrease in metabolic demands or • Leading cause of death due to fires
the diving reflex • Produces injury in several mechanisms
o Thermal injury to upper airway
PATHOPHYSIOLOGY
o Irritation
Near drowning → resuscitated → hypoxia & acidosis o Chemical injury form soot, asphyxiation, &
• PRIMARY PROBLEMS: toxicity of carbon monoxide & cyanide (CN)
o Hypoxia CLINICAL MANIFESTATIONS
o Acidosis
• PHYSICAL EXAM
• Resultant patho pulmonary injury depends on TYPE
o Facial burns
OF FLUID
o Blistering or edema of the oropharynx
o Fresh water
o Hoarseness
o Salt water
o Stridor
o Volume of aspiration
o Upper airway mucosal lesions
• After a person has survived immersion, these can o Carbonaceous sputum
occur:
• SYMPTOMS OF LOWER RESPI. TRACT INJURY
o Acute adult respiratory distress syndrome
o Tachypnea
with hypoxia
o Dyspnea
o Hyercarbia
o Cough
o Respiratory or Metabolic Acidosis
o Decreased breath sounds
EMERGENCY DEPARTMENT MANAGEMENT o Wheezing
1. Cardiopulmonary Resuscitation (CPR) o Rales
2. Ensure adequacy of airway, respiration, & peripheral o Ronchi
perfusion o Retraction
a. Use RECTAL PROBE • PT EXPOSED TO ASPHYXIANTS (gas vapor):
▪ To determine degree of hypothermia o CNS depression, lethargy, & obtundation
b. Start rewarming o Irritability, several temporal headache
▪ Extracorporeal warming o Generalized muscle weakness
▪ Warmed peritoneal dialysis o Coma (CO poisoning)
▪ Inhalation of warm aerosolized oxygen DIAGNOSTICS & LABORATORY
▪ Surface warming • Pulse oximetry & CO-oximetry
3. Draw ARTERIAL BLOOD • ABGs
• To evaluate O2 & CO2, & pH, & • Carboxyhemoglobin level
HCO3 • Lactate
a. For Hypotension & impaired tissue • CBC
perfusion • Chest radiography
▪ Managed by intravascular volume • ECG
expansion & inotropic agents • Serial Cardiac Enzyme (for with chest pain)
4. Improve ventilation & oxygenation • Pulmonary function testing
TABARANZA, CZEJAN RAE BSN-3 37
• Direct laryngoscopy and fiberoptic bronchoscopy • Death
CARBOXYHEMOGLOBIN LEVELS IN BLOOD MEDICAL MANAGEMENT
Level Clinical Manifestation 1. Assess airway, breathing, & circulation
0-10% • Usually no symptom 2. Provide IV access, cardiac monitoring, supplemental O2
3. If manifests bronchospasm
10-20% • Mild headache, atypical a. Use bronchodilators
dyspnea 4. If upper airway injury suspected
20-30% • Throbbing headache a. Elective intubation should be considered
• Impaired concentration 5. Should be monitored for 4-6 hours in the ED
30-40% • Severe headache 6. Mechanical ventilations may be necessary with declining
• Impaired thinking lung function, O2 levels, & ventilation
a. Positive pressure ventilation with low tidal
40-50% • Confusion volumes → 3-5 mL/kg
• Lethargy b. Positive end-expiratory pressure (PEEP) with
• Syncope plateau pressures below 30 cm water
50-60% • Respiratory failure
• Seizures
>70% • Coma
GAS EXCHANGE DISORDERS
TOPIC OUTLINE 6. Medications
1. RESTRICTIVE AIRWAY DISORDERS 7. Viral Respiratory Tract Infections
a. Asthma 8. GE Reflux
b. COPD; Bronchiti; Emphysema COMPLICATIONS
c. Cystic Fibrosis 1. Status asthmaticus
d. Atelectasis 2. Respiratory failure
2. INTERSTITIAL PULMONARY DISORDERS 3. Pneumonia
a. Occupational lung disease 4. Atelectasis
b. Sacoidosis
3. PULMONARY VASCULAR DISORDERS\
PATHOPHYSIOLOGY OF ASTHMA
a. Pulmonary embolism
b. Pulmonary hypertension
c. Pulmonary edema
Transcribed by: Barte, M.G., Maningo, F.E. & Tabaranza, C.R.
ASTHMA
• A heterogenous disease; chronic airway
inflammation
• Causes airway hyperresponsiveness, mucosal
edema, and mucus production.
• symptoms:
Cough
Chest tightness
Wheezing
Dyspnea
• Allergy - strongest predisposing factor
• It is REVERSIBLE
o Spontaneous
o With treatment
OCCUPATIONAL ASTHMA
• Induced by exposure in work environment to dusts,
vapors, or fumes, with/without preexisting diagnosis
of asthma
• removing or decreasing the exposure
COMMON ALLERGENS
1. Seasonal - grass, tree, weed pollens
2. Perennial - mold, dust, roaches, animal dander
COMMON TRIGGERS
1. Airway irritants (air pollutants, strong odors)
2. Food (shellfish, nuts)
3. Exercise
4. Stress
5. Hormonal factors
TABARANZA, CZEJAN RAE BSN-3 38
CLASSIFICATIONS OF ASTHMA SEVERITY
Mild Intermittent Asthma (MIA)
• Symptoms: 2x or less/ week
• Asymptomatic and normal PEFR between
exacerbations
• Brief exacerbations (hrs. To days)
• Nighttime symptoms: 2x or less/month
• Pulmonary function:
• FEV (Forced expiratory volume)/PEFR 80%
or above, of predicted
• PEFR variability is less than 20%
Mild Persistent Asthma (MiPA)
• Symptoms: >2x or less/week but less than
1x/day
KEY PLAYER INFLAMAMTION OF ASTHMA • Exacerebations may affect activity
1. Mast cells • Nighttime symptoms: >2x/month
2. Macrophage • Pulmonary Function:
3. T-lymphocyte • FEV/PEFR 80% or above, of predicted
4. Neutrophils • PEFR variability less than 20& - 30%
5. Eosinophils
MEDIATORS
Moderate Persistent Asthma (MoPA)
• released by mast cells when activated
• Perpetuate inflammatory response: • Symptoms: Daily
1. Increased blood flow
2. vasoconstriction
• Daily use of inhaled short-acting beta 2-agonist
3. Vasculature fluid leak • Exacerbations affect activity; at least 2x/week and
4. Mucus secretion lasts for days
5. Bronchoconstriction • Nighttime symptoms: >1x/week
6. White blood cell attraction to area • Pulmonary Function
• e.g., histamine, bradykinin, prostanoids, cytokines, • FEV/PEFR above 60% and above of
leukotrines predicted
• PEFR variability above 30%
Cyclic 3’5’-adenosine monophosphate (cAMP)
• Controls the balance between alpha- and beta₂-
adrenergic receptors (located in bronchi)
• ↑ levels inhibits release of chemical mediators; Severe Persistent Asthma (SPA)
causes bronchodilation
• Continual symptoms
REMODELING
• Limited physical activity
• structural changes in the bronchial wall; irreversible
long-term damage
• Frequent exacerbations
• Untreated inflammation • Nighttime symptom: FREQUENT
• Pulmonary Function
• Effects:
Hypertrophy of bronchial smooth muscles • FEV/PEFR 60% and above of predicted
Collagen deposits in airway walls • PEFR variability above 30%
Hyperplasia of mucus-secreting cells
DIAGNOSTIC & LABORATORY STUDIES
1. History and Physical Exam
Clinical Manifestations
2. Pulmonary Function Studies
• Three most common symptoms: 3. PEFR (Peak Expiratory Flow Rate)
1. Cough 4. Chest X-ray
2. Dyspnea 5. ABG Analysis or Oximetry
3. Wheezing 6. Allergy skin testing
• Generalized wheezing 7. Eosinophil count and IgE blood level
• Generalized chest tightness and dyspnea 8. Nitric oxide levels
• Often occurs at night or early in the morning
(circadian variations) PHARMACOLOGIC THERAPY
• LATE SIGNS OF POOR OXYGENATION
o Diaphoresis • General classes of asthma medications:
o Tachycardia 1. Quick-relief medications
o Hypoxemia 2. Long-acting medications
o central cyanosis
TABARANZA, CZEJAN RAE BSN-3 39
4. Hold breath and place mouthpiece in between
QUICK-RELIEF MEDICATIONS teeth, close lips around it.
• given for immediate treatment of asthma symptoms 5. Blow out as hard and as fast as you can.
and exacerbations 6. Record
7. Repeat 2x and write down the highest
• SHORT-ACTING BETA2-ADRENERGIC AGONISTS
Highest = peak flow
(SABA)
8. Record each day
o relief of acute symptoms and prevention of
exercise-induced asthma; relax smooth muscles
NURSING MANAGEMENT
o Albuterol, levalbuterol, pirbuterol
• ANTICHOLINERGICS • Obtain history of allergic reaction to medications
o inhibit muscarinic cholinergic receptors and reduce prior to administering
intrinsic vagal tone of the airway • Identify patient’s medications
o For patients who do not tolerate SABA • Administer medications as prescribed and monitor
o ipratropium response
• Administer fluids as indicated.
LONG-ACTING MEDICATIONS • If patient requires intubation, assist with intubation
• Corticosteroids procedure, continue close monitoring, keep SO
➢ Most potent and effective anti- informed of procedures
inflammatory medication COMPLICATIONS
➢ Caution: Rinse mouth after administration 1. Status Asthmaticus
to prevent thrush 2. Respiratory failure
3. Atelectasis
• Cromolyn sodium, Nedocromil 4. Hypoxemia
o mild to moderate anti-inflammatory agents; 5. Hyperventilation
stabilize mast cells
o contraindicated in acute asthma
exacerbations STATUS ASTHMATICUS
• Long-acting beta2-agonists (LABA) • rapid onset, severe, and persistent asthma
o Used with anti-inflammatory med to control • occur due to: infection, anxiety, nebulizer abuse,
nighttime symptoms dehydration, increased adrenergic blockage,
o Not indicated for immediate relief of irritants
symptoms
!!! : Absence of wheezing after patient had been wheezing
Theophylline indicate complete airway obstruction
o a mild to moderate bronchodilator,
used in addition to inhaled Pathophysiology
corticosteroids for relief of nighttime
• Basic characteristics of asthma = decreased
symptoms
diameter of brochi
Salmeterol, Formoterol
o Lasts for at least12 hrs.; used with other med in • Severe bronchospasm with mucus plugging =
long-term control of asthma asphyxia
• Ventilation-perfusion abnormality = hypoxemia
• Reduced PaO2 and initial respiratory alkalosis, with
• Leukotreine modifiers (inhibitors) or decreased PaCO2 and increased pH
antileukotrine • PaCO2 increases, pH decreases = respiratory
o synthesized from membrane phospholipids acidosis
o Alternative to ihaled corticosteroids for
MiPA Clinical Manifestations
o potent bronchoconstrictors; dilate blood • Labored breathing
vessels and alter permeability
• Prolonged exhalation
o Monteluekast, zafirlukast
• Engorged neck veins
• Immunomodulators • Wheezing
o Prevents binding of IgE to high-affinity
receptors of basophils and mast cells. Collaborative Care for Patient with Status Asthmaticus:
PEAK FLOW MONITORING 1. SaO2 monitoring
• measures highest airflow during forced expiration 2. ABG’s
3. Inhaled Beta2-adrenergic agonist/ Anticholinergic
agents
4. Oxygen by mask or nasal prongs(cannula)
• to obtain O2 sat above 90%
5. IV or Oral Corticosteriods (Methylprednisolone)
6. IV Fluids
7. IV Magnesium
8. Intubation and Assisted ventilation
Bronchial thermoplasty
• First nondrug therapy for treatment of severe,
“HOW TO TAKE/USE PEAK FLOW METER” uncontrolled asthma; invasive
1. Move marker to bottom of numbered scale • Controlled radiofrequency heating of central airways
2. Stand/Sit straight through a bronchoscope
3. Take deep breath (Fill lungs all the way)
TABARANZA, CZEJAN RAE BSN-3 40
Indications for Mechanical Ventilation: o To diagnose infection
1. Persistent or progressive CO2 retention (above 42- 4. Serum Electrolytes
45 mmHg)
2. Clinical deterioration (fatigue)
3. Declining mental clarity (hypoersomnolence)
4. Hypoxemia (PaO2 <60mmHg) despite 5. ARTERIAL BLOOD GASES (ABGs)
supplemental O2 Blood Gas Value Interpretation
5. Cardiopulmonary arrest
Decreased
PaO2 is < 80 mmHg Hypoxemia
PaO2
CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) Increased
PaCO2 > 45 mmHg Hypercarbia
• Preventable, treatable slowly progressive PaCO2
respiratory disease of airflow obstruction Respiratory
o Not fully reversible Metabolic acidosis compensation
Acidosis
• Involves: DIAGNOSTICS
o Airways
o pulmonary parenchyma • Pulmonary Function Test
o both • Chest x-ray
• Parenchyma→ any form of lung tissue: • ATT (Alpha 1 AntiTrypsin) levels
o bronchioles, bronchi, blood vessels,
interstitium, alveoli
CHRONIC BRONCHITIS VS. EMPHYSEMA
• Two types of obstructive airway diseases in COPD:
• Chronic Bronchitis (SIMILARITIES)
• Emphysema • Both under term COPD
• Limited airflow: Respiratory acidosis
DISEASES UNDER COPD o ↓O2
1. Chronic Bronchitis o ↑CO2
2. Emphysema • Pts have inability to fully exhale:
PATHOPHYSIOLOGY o Lungs become hyperinflated overtime
• Irreversible → no cure
• Mild to severe
• MAIN CAUSE
o Inhalation of irritant (smoking)
• MEDICATIONS
o Bronchodilators
o Corticosteroids
o Theophylline
• DIAGNOSTICS
o Spirometry
1. CHRONIC BRONCHITIS
RISK FACTORS
• Advanced age
• Cigarette smoking
• Alpha-antitrypsin (ATT) deficiency
• Exposure to air pollution
•Productive cough that lasts 3 months in each of 2
CLINICAL MANIFESTATIONS consecutive years
• Dyspnea • MAIN ISSUE
• Productive cough (severe in morning) ▪ Inflammation of bronchioles
• Hypoxemia ▪ Excessive mucous production by hyperplasia of
• Crackles and wheezes goblet cells
• Rapid and shallow respiration • There will be V/Q MISMATCH
• Use of accessory muscles (Ventilation/Perfusion)
• Barrel chest/ increased chest diameter o Low ventilation
• Hyperresonance on percussion (trapped air) CLINICAL MANIFESTATIONS
• Thin extremities, enlarged neck • “BLUE BLOATERS”
• Clubbing o Cyanosis
• Pallor and cyanosis o Bloating edema
• Decreased O2 sat. levels
LABORATORIES
1. Increased HCT 2. EMPHYSEMA
2. Sputum cultures
3. WBC count
TABARANZA, CZEJAN RAE BSN-3 41
• Presence of overdistended, non-functional alveoli, Clinical Manifestations
which may rupture, resulting in loss of aerating • 3 primary symptoms:
surface. • Chronic cough
• Main issue • Sputum production
▪ Damage to alveolar sacs • dyspnea
▪ Sacs lose their ability to inflate
and deflate
• Weight loss
▪ Lose elasticity • Barrel chest (due to hyperinflation)
▪ Air trapping → hyperinflation of • Upright, leaning forward position
lungs • Polycythemia
▪ Capillary bed is damaged: • Musculoskeletal wasting
▪ ↓perfusion • Metabolic syndrome
▪ ↓ ventilation • depression
▪ Matched V/Q defects
Assessment/Diagnostic Findings
Dead space - lung area where no gas exchange
can occur
• Pulmonary function studies
• To confirm diagnosis of COPD, determine
Hypercapnia - increased CO2 tension in arterial severity, monitor disease progression
blood • Spirometry
• Evaluate airflow obstruction, and
reversibility of obstruction
• ratio of FEV1 to forced vital capacity (FVC)
• Arterial Blood Gas (ABGs)
• Assess baseline oxygenation and gas
exchange
• Chest X-ray
• High-resolution CT scan
• Alpha1-antitrypsin deficiency screening
• For patients <45 y.o and those with family
history of COPD
Grades of COPD
TWO MAIN TYPES OF EMPHYSEMA:
1. Panlobular Emphysema (PLE)
• destructruction of the respiratory
bronchiole, alveolar duct, and alveolus
• hyperinflated chest, dyspnea, and weight
loss
2. Centrilobular Emphysema (CLE)
• take place in the center of the secondary PHARMACOLOGIC THERAPY
lobule, preserving the peripheral portions
of the acinus (terminal airway unit where 1. Expectorants (guaiafenessin)
gas exchange occurs) 2. Mucolytic (mucomyst/mucosulvan)
• Chronic hypoxemia, hypercapnia, 3. Antitussives
polycythemia (^RBC), episode of right- o PM to prevent sleep pattern disturbance
sided heart failure, central cyanosis, o Observe for drowsiness
respiratory failure, peripheral edema o Cause constipation
o Dextrometorphan
RISK FACTORS o Codeine
• Exposure to tobacco smoke
4. Bronchodilators
o Aminophylline (Theophyline)
• Passive smoking o Ventolin (Salbutamol)
• Increased age o Bricanyl (Terbutaline)
• Occupational exposure (dust, chemicals) o Spiriva (Tiotropium)
• Indoor and outdoor air pollution o Xopenex (Levalbuterol)
• Genetic abnormalities o Brethine (Terbutaline)
• deficiency of alpha1-antitrypsin, enzyme o Alupent (Metaproterenol)
inhibitor that protects the lung parenchyma • Observe for tachycardia and palpitations
from injury • Administer bronchodilator inhalation
before steroid inhalation
TABARANZA, CZEJAN RAE BSN-3 42
5. Corticosteroids PATHOPHYSIOLOGY
o They do not slow the decline in lung • It is caused by mutations or dysfunction in protein
function cystic fibrosis transmembrane conductance
o Long-term treatment with oral regulator (CFTR).
corticosteroids = NOT RECOMMENDED o Normally: transport chloride ions across
▪ Causes Steroid Myopathy epithelial cell membrane
▪ Muscle weakness • Characteristics of CF:
▪ Decreased ability to o Thick viscous secretions in:
function ▪ Lungs
▪ Respiratory failure ▪ Pancreas
6. OTHER MEDICATIONS ▪ Liver
o Alpha1-antitrypsin augmentation therapy ▪ Intestine
o Antibiotic agents ▪ Reproductive tract
o Mycolytic agents ▪ Increased salt content in sweat glands
o Antitussive agents • Gene mutations → leading CF
o Vasodilators o Most common mutation = deltaF508
o Narcotics o More than 1,800 mutations are identified
o Influenza vaccine • People who are HETEROZYGOUS for CF
o Pneumococcal vaccination o 1 defective gene, 1 normal gene
SURGICAL MANAGEMENT o Do not manifest the disease
1. BULLECTOMY o Carriers and can pass the defective gene on to
• For pt with bullous emphysema their children
• Bullae • If BOTH PARENTS are carriers of CF
o Enlarged airspaces that do not contribute o 25% chance a child has CF
to ventilation but occupy thorax • 3 HALLMARK PATHOLOGY of CF:
o Impairs gas exchange 1. Bronchial mucus plugging
• Purpose: 2. Inflammation
o Help reduce dyspnea 3. Bronchiectasis → begins in upper loves and
o Improve lung function progress to involve all lobes
• Procedure: CLINICAL MANIFESTATIONS
o Performed via a video-assisted A. PULMONARY MANIFESTATIONS
thoracoscope or limited thoracotomy • Productive cough
incision • Wheezing
• Hyperinflation of lung fields (c. x-ray)
2. LUNG VOLUME REDUCTION SURGERY • Pulmonary function test = consistent with
• For pt with advanced or end-stage COPD (grade IV) obstructive disease of the airways
• Removal of a portion of the diseased lung B. UPPER RESPIRATORY MANIFESTATIONS:
parenchyma • Sinusitis
• Not cure but improves • Nasal polyps
• Purpose: C. NON-PULMONARY MANIFESTATIONS
o Reduces hyperinflation a. Gastrointestinal problems
o Allows functional tissue to expand • Pancreatic insufficiency
o Improves elastic recoil of lung • Recurrent abdominal pain
o Improved chest wall & diaphragm • Biliary cirrhosis
mechanics • Vitamin deficiency
3. LUNG TRANSPLANTATION • Recurrent pancreatitis
• Viable option for definitive surgical treatment of • Weight loss
severe COPD in selected patients b. CF-related Diabetes
• DISADVANTAGE = Costly c. Genitourinary problems
• Male and female infertility
CYSTIC FIBROSIS
D. Chronic Respiratory Inflammation & Infection
• Caused by impaired mucus clearance
E. Common Pathogenic Bacteria during EARLY
CHILDHOOD:
• S. aureus
• H.influenzae
F. P. aeruginosa → isolated from the sputum of most
patients
MEDICAL MANAGEMENT
A. ACUTE AIRWAY EXACERBATION
• Airway clearance
• Antibiotics based on sputum culture results
• Most common fatal autosomal recessive disease • P. aeruginosa → majority being colonized
among Caucasians B. CHRONIC INFECTION WITH P.AERUGINOSA
o Independent risk factor
• To have CF:
C. Routine Cultures of Respiratory Secretions
o Person must inherit a defective copy of
o To identify organisms and guide antibiotic
CF gene(one from each parent).
selection
TABARANZA, CZEJAN RAE BSN-3 43
TREATMENT • Periodic reassessment of the home environment may
o 2 IV ANTIBIOTICS typically chosen to treat a severe be warranted as the disease progresses.
exacerbation of P.aeruginosa. either • Palliative care and end-of-life issues should be
1. Tobramycin (Nebcin) addressed when warranted.
2. Piperacillin-tazobactam (Zosyn) • Patients and family members require support as they
3. 3rd Generation Cephalosporin face a shortened lifespan and an uncertain future.
4. Carbapenem
ATELECTASIS
5. Aztreonam
o ORAL ANTIBIOTICS
o to treat mild methicillin-sensitive S.aureus
infection
o Minimum of 10 days; max. of 3 weeks
1. Dicloxacillin
2. Amoxicillin-clavulanate
3. Cephalexin
• MORE SERIOUS EXACERBATIONS:
1. Oral linezolid
2. Inhaled antibiotics
• ACUTE EXACERBATION
1. Airway clearance treatments
• Used 3 to 4 times per day
• KEY INTERVENTION
o DORNASE ALFA
o Nebulized medication
o To degrade the large amount of DNA that
accumulates within CF mucus
o Helps decrease the viscosity of the sputum and
promotes expectoration of secretions
o For moderate-severe disease
o INHALED HYPERTONIC SALINE
o Used in chronic treatment of CF
o Increases hydration of airway surface liquid
o Improves airway clearance
• INHALED TOBRAMYCIN (TOBI) OR AZTREONAM
(AZLI)
o Decrease frequency of pulmonary
exacerbations
• Long-term use of High-dose Nonsteroidal Anti-
• Non-aeration or collapse of a lung or part of a lung
inflammatory agents (Ibuprofen)
o Leads to decreased gas exchange and
• To slow the loss of lung function
hypoxia.
o Recommended = Children 6-17 y.o.
• Treatment depends on removing underlying cause
o Not Recommended = pt older than 13 y.o.
before reinflating the lung:
• ORAL PANCREATIC ENZYME SUPPLEMENTATION
o Obstructive Atelectasis
WITH MEALS
o Compression Atelectasis
o 90% with CF have pancreatic exocrine
PATHOPHYSIOLOGY
insufficiency
o Due to fat malabsorption in CF, fat soluble • When alveoli become airless:
vitamins are taken: A,D,E,K. o It shrivel up → natural elasticity of the tissue
• CFTR Modulators dominates
o Help to improve function of defective CFTR o Interferes with blood flow through the lung
proteins o Ventilation and Perfusion are altered
o Ivacaftor ▪ Affects oxygen diffusion
▪ Designed to keep the proteins at the o COMPENSATORY MECHANISM:
cell surface open more often ▪ Increased RR → to control CO2
▪ Improve salt and water movement levels; because gas diffuses easily
across membrane o If lungs are NOT REINFLATED QUICKLY:
▪ One 1 gene mutation , G551D is ▪ Lung tissue become necrotic
addressed ▪ Infected
▪ Permanent lung damage
NURSING MANAGEMENT
• helping patients manage pulmonary symptoms and
prevent complications.
• Specific measures include strategies to promote
removal of pulmonary secretions:
o chest physiotherapy
o breathing exercises. –
• Patients are reminded to reduce risk factors associated
with respiratory infections.
• Patients are taught the early signs and symptoms of
respiratory infection and disease progression.
• Adequate fluid and dietary intake is emphasized to
promote removal of secretions and ensure nutritional
status.
TABARANZA, CZEJAN RAE BSN-3 44
• Restricted ventilation due to pain or abdominal
distention
• Slow shallow respiration due to anesthetics and
analgesics
• Increased secretions due to supine positop
• Decreased cough effort
CLINICAL MANIFESTATIONS
• GENERAL SIGNS AND SYMPTOMS
o Increasing dyspnea (shortness of breath)
o Cough
o Sputum production
• IN ACUTE ATELECTASIS (LOBAR ATELECTASIS)
o Marked respiratory distress
o General s&s
o Tachycardia
o Tachypnea
o Pleural pain
o Central cyanosis → late sign of hypoxemia
o Difficulty breathing in supine position and
anxious
ETIOLOGY • IN CHRONIC ATELECTASIS
Atelectasis can either be: o Predisposition to infection distal to the
1. Obstructive or Resorption Atelectasis obstruction
2. Compression Atelectasis o Signs of pulmonary infection may be present
• SMALL AREAS OF ATELECTASIS
1. OBSTRUCTIVE OR RESORPTION ATELECTASIS
o Asymptomatic
• Develops when total obstruction of airway due to • LARGE AREAS OF ATELECTASIS
MUCUS or TUMOR → diffusion into the tissue of air o Dyspnea
distal to obstruction → air not replaced o Increased HR
• Reduces alveolar ventilation o Increased RR
• Most common type o Chest pain
• Results from reabsorption of gas (trapped alveolar air o Abnormal or Asymmetric chest expansion
is absorbed in bloodstream) • FOR OBSTRUCTIVE ATELECTASIS
• No additional air can enter into the alveoli due to o Leads to potential low pressure “gap” or
blockage space on affected side
• Result: o Mediastinum shifts towards affected side
o Lung becomes airless o Compensatory Mechanism
o Alveoli collapse ▪ Other lung compensates by
• Causes: overinflating
o Foreign body o Affected side often “lags” behind unaffected side
o Tumor during ventilation
o Altered breathing patterns • FOR COMPRESSION ATELECTASIS
o Retained secretions o Mediastinum may shift toward the other
o Pain unaffected side
o Alteration in small airway ASSESSMENT AND DIAGNOSTIC FINDINGS
o Prolonged supine positioning • increased work of breathing and hypoxemia
o Increased abdominal pressure • Decreased breath sounds and crackles are heard over
o Reduced lung volumes due to musculoskeletal/ the affected area
neurologi disorders • x-ray reveals patchy infiltrates or consolidated areas
o Restrictive defects • SpO2 below 90%
2. COMPRESSION ATELECTASIS • Lower than normal PaO2
• Results when mass such as tumor exerts pressure on PREVENTION
the part of the lung • frequent turning
o Prevents air from entering the section of lung o From supine to upright
• When pressure in pleural cavity is increased, as with ▪ To promote ventilation and prevent
increased fluid or air: secretions from accumulating
o Adhesion between pleural membranes is • early mobilization
destroyed → lung cannot expand. o From bed to chair
• strategies to expand the lungs and
3. INCREASED SURFACE TENSION IN ALVEOLI
• Voluntary deep-breathing maneuvers → (at least every 2
• Occurs With pulmonary edema or respiratory distress hours)
syndrome. o To mobilize secretions and prevent from
• Preventing lung expansion accumulating.
4. CONTRACTION ATELECTASIS • Patient education and reinforcement
• Incentive spirometry
• Fibrotic tissue in the lungs or pleura o To encourage pt to inhale slowly and deeply to
• May restrict expansion maximize.
• Lead to collapse • Secretion management
5. POSTOPERATIVE ATELECTASIS o directed cough o suctioning
o aerosol nebulizer treatments followed by chest
• Occurs 24-72 hours after abdominal surgery physiotherapy o bronchoscopy.
TABARANZA, CZEJAN RAE BSN-3 45
MANAGEMENT 2. ASBESTOSIS
Goal: to improve ventilation and remove secretions
PATHOPHYSIOLOGY
• Preventive strategies as first-line measures
Inhalation of asbestos fibers into the alveoli and are
• positive end expiratory pressure surrounded by fibrous tissue → thickening of fibrous
• continuous positive airway breathing tissue → formation of plaque → restrictive lung
• bronchoscopy disease, with decrease in lung volume, diminished
• Bronchial obstruction from secretion is the cause: gas exchange, hypoxemia, cor pulmonale, and
o effective coughing or suctioning respiratory failure
o chest physiotherapy
CLINICAL MANIFESTATIONS
o Nebulizer treatments with a bronchodilator
or sodium bicarbonate • Progressive dyspnea
o Bronchoscopy • Persistent, dry cough
• Mild-to-moderate chest pain
• Endotracheal intubation and mechanical ventilation • Anorexia
may be necessary may be necessary in severe or • Weight loss
massive atelectasis • Malaise
• Compression of lung tissue as the cause: • Clubbing of fingers
o Thoracentesis o Insertion of a chest tube 3. COAL WORKER’S PNEUMOCONIOSIS/
• Obstruction by lung cancer as the cause:
o airway stent or radiation therapy to shrink ANTHRACOSIS
a tumor PATHOPHYSIOLOGY
o surgical management may be necessary Inhalation and deposition of dust mixtures (coal,
INTERSTITIAL PULMONARY DISEASE kaolin, mica, and silica) into the alveoli and
bronchioles → engulfing of dusts by the
• Occupational lung disease
macrophages → macrophages aggregation →
• Sarcoidosis formation of fibroblasts → clogging in the alveoli
OCCUPATIONAL LUNG DISEASE: PNEUMONCONIOSES and bronchioles → formation of coal macules →
development of fibrotic lesions → localized
• Pneumoconiosis is a general term given to any lung
disease caused by dusts that are breathed in and then emphysema with cor pulmonale and respiratory
failure
deposited deep in the lungs
• includes CLINICAL MANIFESTATIONS
o asbestosis • Chronic cough
o silicosis an • Dyspnea
o coal workers’ pneumoconiosis • Expectoration of black or gray sputum
• refers to a non-neoplastic alteration of the lung PREVENTION
resulting from inhalation of mineral or inorganic dust
• Disease is untreatable, but can be prevented.
SUMMARY • promote measures to reduce the exposure of
DISEASE AGENT OCCURENCE workers to industrial products
Coal-workers Coal dust Coal mines • screening/monitoring of individuals at risk
Disease or ASSESSMENT
Anthracosis • job and job activities
Silica Stone-cutting, • exposure levels
Silicosis sandblasting, • general hygiene
mines • time frame of exposure
Asbestos Insulation, • smoking history
Asbestosis
Shipbuilding • effectiveness of respiratory protection used
Farmer’s Lung Fungal spores Hay • direct versus indirect exposures
• Exposure to an agent known to cause an
occupational disorder
• Length of time from exposure of agent to onset of
TYPES OF PNEUMOCONIOSES symptoms
1. SILICOSIS • Congruence of symptoms with those of known
exposure related disorder
PATHOPHYSIOLOGY
• Lack of other more likely explanations of the signs
Inhalation of silica dusts → nodular lesions in the and symptoms
lungs → nodules enlarge and coalesce → formation
of dense masses on upper portion of lungs → loss Medical Management
of pulmonary volume • Supportive therapy aimed at preventing infections
CLINICAL MANIFESTATIONS and managing complications
1. ACUTE:
• Dyspnea Nsg Management
• Fever • education about preventive measures to patients
• Cough their families
• Weight loss • assesses patients for a history of exposure to
2. CHRONIC: environmental agents
• Progressive symptoms indicative of • make referrals so that pulmonary function can be
hypoxemia evaluated
• Severe airflow obstruction
• Right-sided HF
TABARANZA, CZEJAN RAE BSN-3 46
SARCOIDOSIS Clinical Manifestations
• insidious onset with lack of prominent clinical signs
or symptoms
• dyspnea
• cough
• hemoptysis
• congestion
• anorexia
• fatigue
• weight loss
• uveitis
• joint pain
• fever
• granulomatous lesions of the skin, liver, spleen,
kidney, and central nervous system
Assessment and Diagnostic Findings
• Chest x-rays and CT scans are used to assess
pulmonary adenopathy
• mediastinoscopy or transbronchial biopsy may be
used to confirm dx
• open lung biopsy is rarely performed
• dx is confirmed if noncaseating granulomas are
• a type of interstitial lung disease present
• multisystem, granulomatous disease of unknown • Abnormal Pulmonary function test results
etiology • ABG measurements may be normal or may show
• Epidemiology: hypoxemia or hypercapnia
o usually presents between 20 and 40 years of
age Medical Management
o more common in women than men
o more common in African Americans • remission without specific treatment
• Corticosteroid therapy
Pathophysiology
• immune modulator may be added when there is
Presence of one or more exogenous agents → inadequate response to prednisone or the dose
hypersensitivity response and inflammation → cannot be decreased
formation of noncaseating granuloma → granuloma
infiltration and fibrosis in the lung → low lung
compliance, impaired diffusing capacity, and
reduced lung volumes
TABARANZA, CZEJAN RAE BSN-3 47
PULMONARY VASCULAR DISORDERS
• Pulmonary Embolism • IV infusion lines are inserted to establish routes for
• Pulmonary Hypertension medications or fluids
• Pulmonary Edema • For hypotension that does not resolve with IV fluids,
PULMONARY EMBOLISM prompt
• initiation of vasopressor therapy is recommended
• obstruction of the pulmonary artery or one of its
branches by a thrombus • Hemodynamic measurements and evaluation for
hypoxemia
• Factors: trauma, surgery (orthopedic, major abdominal,
pelvic, gynecologic), pregnancy, heart failure, age older • ECG monitoring
than 50 years, hypercoagulable states, and prolonged • Blood is drawn for serum electrolytes, complete
immobility. blood count, and coagulation studies
• indwelling urinary catheter is inserted to monitor
PATHOPHYSIOLOGY & ETIOLOGY urinary output
- H • Small doses of IV morphine or sedatives are given
to relieve patient anxiety
CLINICAL MANIFESTATIONS
GENERAL MANAGEMENT
• Dyspnea
• Tachypnea • Oxygen therapy is given to correct the hypoxemia,
• Chest pain relieve the pulmonary vascular vasoconstriction,
• Anxiety and reduce the PH.
• Fever • Anti-embolism stockings to reduce venous stasis.
• Tachycardia • Elevating leg to increase venous flow.
• apprehension
SURGICAL MANAGEMENT
• cough
• diaphoresis • SURGICAL EMBOLECTOMY
o is indicated if patient has a massive PE or
• hemoptysis
hemodynamic instability.
• syncope
• IVC FILTERS
• rapid and weak pulse
o are used to allow blood to pass through while
DIAGNOSTICS, LABORATORY, & PE FINDINGS large emboli from the pelvis or lower
• symptoms, signs, and testing extremities are blocked or fragmented before
reaching the lung.
• CHEST X-RAY
o usually normal but may show infiltrates, PHARMACOLOGIC THERAPY
atelectasis, elevation of the diaphragm on the ANTICOAGULATION THERAPY
affected side, or a pleural effusion
• In pt with suspected PE, immediate anticoagulation
• ECG
is indicated to prevent a reoccurrence or extension
o ST-T wave abnormality
of the thrombus
• ABG
• With proven PE, initial anticoagulant selected may
o hypoxemia and hypocapnia
include a low molecular weight heparin,
• Multidetector-row computed tomography
unfractionated heparin, or one of the new oral
angiography
anticoagulants
o high-quality visualization of the lung
• outpatient therapy can be started by administering
parenchyma
the first dose in the emergency department or urgent
• Pulmonary Angiogram
care center and the remaining doses given at home
o direct visualization under fluoroscopy of the
• Long-term treatment options include warfarin
arterial obstruction and accurate assessment of
(Coumadin) and the NOACs
the perfusion deficit
• V/Q scan THROMBOLYTIC THERAPY
o evaluates different regions of the lung (upper, • used in patients with an acute PE who have
middle, lower) and allows comparisons of the hypotension and do not have a contraindication or
percentage of V./Q. in each area potential bleeding risk
• MDCTA, D-dimer assay, or pulmonary arteriogram • Thrombolytic therapy resolves the thrombi or emboli
o more accurate visualization of a PE quickly and restores more normal hemodynamic
MEDICAL-SURGICAL MANAGEMENT functioning of the pulmonary circulation
• Caution risk for bleeding
PREVENTION
• Before thrombolytic therapy is started, INR, partial
• Active leg exercises to avoid venous stasis
thromboplastin time (PTT), hematocrit, and platelet
• early ambulation
counts are obtained
• use of anti-embolism stockings • Avoid invasive procedure due to risk for bleeding
EMERGENCY MANAGEMENT NURSING RESPONSIBILITIS
• Nasal oxygen is given immediately to relieve Minimizing the Risk of Pulmonary Embolism
hypoxemia, respiratory distress, and central
• identify the patient at high risk for PE and to minimize
cyanosis
the risk of PE in all patients
TABARANZA, CZEJAN RAE BSN-3 48
Preventing Thrombus Formation Continuing and Transitional Care
• encourage ambulation and active and passive leg • monitor the patient’s adherence to the prescribed
exercises to prevent venous stasis management plan and reinforces previous instructions
• move the legs in a “pumping” exercise so that the leg • remind pt on importance of follow-up appointments and
muscles can help increase venous flow participation in health promotion activities
• advise the patient not to sit or lie in bed for prolonged
periods, not to cross the legs, and not to wear constrictive PULMONARY HYPERTENSION
clothing • characterized by elevated pulmonary arterial pressure
• Intermittent pneumatic compression (IPC) devices may and secondary right heart ventricular failure
be used to prevent venous thrombosis by enhancing
blood flow in the deep veins of the legs PATHOPHYSIOLOGY
• Factors: collagen vascular disease, congenital heart
Assessing Potential for Pulmonary Embolism disease, anorexigens (specific appetite depressants),
• conduct a careful assessment of the patient’s health chronic use of stimulants, portal hypertension, and HIV
history, family history, and medication record infection
• ask pt about pain or discomfort in extremities regularly • Vascular injury -> endothelial and vascular smooth
• evaluate pt extremities for r warmth, redness, and muscle dysfunction -> pulmonary artery constriction ->
inflammation impaired ability of pulmonary blood vessels to handle
blood flow and volume -> increased blood flow ->
Monitoring Thrombolytic Therapy increased pulmonary artery pressure -> increased
• During thrombolytic infusion, assess VS every 2 hours pulmonary vascular resistance -> increased right
• Tests to determine INR or PTT are performed 3 to 4 hours ventricular workload -> right ventricular failure and
after the thrombolytic infusion is started to confirm that the hypertrophy
fibrinolytic systems have been activated
Clinical Classification
Managing Pain Group 1: Pulmonary Arterial Hypertension (PAH)
• semi-Fowler’s position provides a more comfortable • Sporadic idiopathic PAH
position for breathing • Heritable idiopathic PAH
• turn patients frequently and reposition them to improve • Drug and toxin-induced PAH
the V./Q. in the lung • PAH due to diseases such as connective tissues
• administer opioid analgesics agents as ordered disorders, HIV infection, portal hypertension,
congenital heart disease
Managing Oxygen Therapy
• frequently assess pt for signs of hypoxemia Group 2: PH due to left heart disease
• monitor pulse oximetry to evaluate effectiveness of • Systolic dysfunction
therapy • Diastolic dysfunction
• Deep breathing and incentive spirometry helps minimize • Valvular heart disease
or prevent atelectasis and improve ventilation
• Nebulizer therapy or percussion and postural drainage Group 3: PH due to chronic lung diseases and/or
may be used for management of secretions. hypoxemia
• Chronic obstructive pulmonary disease
Relieving Anxiety • Interstitial lung disease
• Encourage pt to share fear and concerns • Mixed restrictive and obstructive lung disease
• Answer pt’s and family’s question accurately and • Sleep disordered breathing
concisely
• Explain therapy and describe how to recognize untoward Group 4: Chronic thromboembolic pulmonary
effects early hypertension (CTEPH)
• Due to thromboembolic occlusion of the
Monitoring for Complications proximal or distal pulmonary vasculature
• be alert for the potential complication of cardiogenic
shock or right ventricular failure Group 5: PH with unclear multifactorial mechanisms
• Hematologic disorders
Providing Postoperatie Nsg Care • Systemic disorders (e.g., sarcoidosis)
• If pt has undergone surgical embolectomy, measure the • Metabolic disorders
patient’s pulmonary arterial pressure and urinary output
• assesses the insertion site of the arterial catheter Clinical Manifestations
• elevate the foot of the bed and encourage isometric • Dyspnea with exertion and eventually at rest
exercises, the use of IPC devices, and walking when the • Substernal chest pain
patient is permitted out of bed to prevent venous stasis • Weakness
• discourage sitting for long periods • Fatigue
• Syncope
Promoting Home, Community-Based, and Transitional • occasional hemoptysis
Care
• signs of right-sided heart failure
Educating Pts About Self-Care
• Anorexia
• Before discharge and at follow-up check-ups, educate the • abdominal pain in the right upper quadrant
patient about preventing recurrence and reporting signs
and symptoms Asx and Dx Findings
• health history
TABARANZA, CZEJAN RAE BSN-3 49
• physical examination Noncardiogenic pulmonary edema
• chest x-ray • occurs due to damage of the pulmonary capillary lining
• pulmonary function studies • may be due to direct injury to the lung, hematogenous
• electrocardiogram (ECG) injury to the lung, or injury plus elevated hydrostatic
• echocardiogram for estimating pulmonary artery pressures
pressure and the right ventricle
• right heart catheterization form confirmation of dx Cardiogenic pulmonary edema
• PH confirmation when mean pulmonary artery pressure • is associated with acute decompensated HF
greater than 25 mm Hg • can occur following acute MI or as an exacerbation of
• exercise testing chronic HF
• Pulmonary function studies may show slight decrease in • Pathophysiology: When the left ventricle begins to fail,
vital capacity and lung compliance, with a mild decrease blood backs up into the pulmonary circulation, causing
in the diffusing capacity pulmonary interstitial edema
• Decreased PaO2 Clinical Manifestations
• V/Q scan can detect defects in pulmonary vasculature
• frothy pink (blood-tinged) sputum
Medical Management • Restlessness and anxiety
Pharmacologic Therapy • breathlessness and a sense of suffocation
• vasoreactivity test may be done to identify which • tachypneic with noisy breathing and low oxygen
medication is best suited saturation rates
• pt c positive vasoreactivity test may be prescribed c • pale to cyanotic skin and mucous membranes
CCB • cool and moist hands
• Prostanoids for relaxing vascular smooth muscle, • Tachycardia and JVD
stimulate production of AMP and inhibition of • Incessant coughing with foamy sputum
smooth muscle cell growth • Confusion and stuporous
• Epoprostenol IV
Asx and Dx Findings
• Teprostinil IV or SQ
• Vital Signs
• Ilosprost 6-9 times daily
• Airway and breathing assessment
• Endothelin receptor antagonists have
• Placement of cardiac monitor
antihypertensive effects; monitor liver function
• Lab tests: ABG, electrolytes, BUN, and creatinine
• Sildenafil, tadalafil, and verdenafil promotes
pulmonary vasodilation • Chest x-ray to confirm extent
Surgical Management Prevention
• Early identification
• Lung transplantation: Bilateral lung or heart-lung
• In early stage, increase dosages of diuretics and
• Atrial septostomy
implement interventions to decrease preload
Nsg Management • Identifying and managing precipitating factors
• Goal: identify patients at high risk for PH to commence
Medical Management
early treatment
Oxygen Therapy
• be alert for signs and symptoms, administer oxygen
therapy appropriately, and instruct the patient and family • A nonrebreathing mask is used initially; If respiratory
about the use of home oxygen therapy failure is severe or persists, noninvasive positive
pressure ventilation is the preferred
• Health teaching on medication
• Monitoring f oxygenation through pulse oximetry or ABG
• Encourage formal and informal support groups
Diuretics
• To promote the excretion of sodium and water by the
PULMONARY EDEMA kidneys
• Monitor B/P closely to detect hypotension due to
decrease in IV volume
• Monitor intake and output, daily weights, serum
electrolytes, and creatinine
Vasodilators
• Enhance symptom relief in pulmonary edema
• contraindicated in patients who are hypotensive
• monitor B/P
Nsg Management
Positioning the Patient to Promote Circulation
• helps reduce venous return to the heart, decreasing
right ventricular SV, and decreasing lung congestion
• patient is positioned upright, preferably with the legs
dangling over the side of the bed
• Abnormal accumulation of fluid in the lung tissue, the
alveolar space, or both
TABARANZA, CZEJAN RAE BSN-3 50
Providing Psychological Support Monitoring Medications
• to relieve pt fear and anxiety that may worsen the • indwelling catheter may be necessary to monitor urine
condition output
• nurse gives the patient simple, concise information in a • continuous ECG monitoring and frequent measurement
reassuring voice about what is being done to treat the of vital signs
condition and the expected results
TABARANZA, CZEJAN RAE BSN-3 51
LECTURE NOTES (NSG HISTORY, HEALTH ASSESSMENT OF RESPIRATORY DISORDERS)
CANDIDA ALBICANS Categories Questions Significance
• a fungus URT • Do you often have Inflammatory process,
headaches, sinus disorder of the URT.
• A type of yeast → dali ra muproliferate
tenderness?
• Present in the • Episodes of nose bleeding?
o Mouth • Voice change?
o Oral cavity
LRT • SOB? Cough? Productive? • Consider cardio-
o GIT
• Characteristics of sputum? respiratory
o Armpit • Recent experience of night problems,
o Genital area wears, chill, fever? • irritations,
• Conditions result to change: • Have you ever feel infections and
o Immunocompromised confused, light- headed or communicable
• Alteration of the environment results to: restless? disease.
o Candidiasis • History of chest surgeries? • Cerebral hypoxia,
o Oral thrush • hypoxemia
• poor pefusion
o Moniliasis
Exposures Any allergies that causes Many respiratory
respiratory symptoms? How is it disorders are
DIFFERENCE BETWEEN SPUTUM, EXUDATE, PHLEGM managed? Smoking? Packs/ aggravated by
day? How many years? Exposure exposure to pollutant.
SPUTUM • Thick type of mucus to second hand smoke, air borne OTC Medication may
• Made in lungs pollutants at work? affect with respiratory
• Indicative of infection or chronic functions
illness
• Contains cells from the immune
system to help fight bacteria, fungi, CHIP-IN INFOS NI MAAM MAGGY:
other foreign susbstances
• WHY FEVER IS IN LATE AFTERNOON OR EVENING
✓ CLEAR IN PT WITH TUBERCULOSIS?
o No disease - Fever appears when the body`s endogenous anti-
✓ WHITE/GREY inflammatory mechanisms are at their lowest -
o also normal related to the diurnal variation in corticosteroid
✓ DARK YELOW/GREEN synthesis. Hence, it appears in the evening.
o Bacterial infection such as
pneumonia
✓ YELLOWISH-GREEN • CHILLS → warning sign of high grade fever
o Cystic fribrosis
✓ BROWN • EARLY SIGNS OF CEREBRAL ANOXIA
o Smoker o Confusion
o Black lung disease o Light headache
✓ PINK o Hx of chest pain
o Pulmonary edema • Hypoxia → decreased oxygen tension at CELLULAR
o CHF LEVEL
✓ RED • Hypoxemia → diminished oxygen tension at the
o Early sign of lung cancer
BLOOD LEVEL
o Pulmonary embolism
o
EXUDATE • It is a fluid that is slowly discharged OTC-MEDICATIONS
by a tissue
• If pt is taking OTC, take note what it is → kay naam n
• Found in:
sad adverse effects
o Inflamed or Injured Tissues
such as wound • RIFAMPICIN
• ETIOLOGY o Antibiotic used to treat several types of
o Injury in a tissue mycobacterial infections including
o Increased permeability of Mycobacterium avium
the blood vessels o Treat TB
o Results in leakage or o SIDE-EFFECT: Orange-colored urine
secretion of fluid from blood o ADVERSE EFFECT:
vessels ▪ Hepatotoxicity
o Fluid secreted is known as • CONSIDERED ACQUIRED DISEASES:
EXUDATE o Tuberculosis
• PURULENT EXUDATE
o Diabetes Mellitus
o Numerous active and dead
neutrophil COMMON S/S OF RESPIRATORY DISEASES
PHLEGM - Dyspnea; bradypnea, tachypnea, orthopnea, apnea,
eupnea
- Cough
- Cyanosis: Peripheral, central
TABARANZA, CZEJAN RAE BSN-3 52
- Sputum production 2. Squawks
- Chest pain
- Very short wheezes; noted late during inspiration such as
- Wheezing/Stridor/Accumulation of mucus
in pneumonia, lung fibrosis or bronchiolitis obliterans
- Hemoptysis
- Clubbing of fingers
Causes:
- Edema of ankles and feet
- Asthma: with severe asthma, there may be like little or no
- General fatigue and weakness
wheezing
CHIP-IN INFO NI MAGGY: - COPD
• If pt has BRONCHIECTASIS: - Emphysema, acute or chronic bronchitis, and
o There is always a foul sputum production. bronchiectasis
• There is CHEST PAIN in respiratory and cardiac - Foreign body aspiration
diseases.
o But Respiratory disease is highly
communicable → mode of transmission kay air, 3. Stridor
spits, saliva
- High pitched musical quality sound heard mostly with
• TB → high risk for malnutrition inspiration
- Continuous stridor in the upper airways obstruction
• 2 CONDITIONS THAT ONLY HAS MANIFESTATION OF - Loudest over the neck
HEMOPTYSIS
1. TB Causes:
2. Bronchiectasis - Obstructions
- Epiglottis
• For PNEUMONIA - Croup (Laryngotracheitis)
o Sputum is rust colored. - Foreign Body in the upper airways
o Dili hemoptysis – coughing out (vomiting man - Tracheomalacia or stenosis
ni; tas fruity sputum, bubbly kay gikan sa respi
system full of air)
4. Inspiratory Gasp
• HEMATEMESIS → Vomiting of blood; from GIT
• CHEST RETRACTION - high pitched crow or whoops sound heard after
continues coughing
o Pneumonia
o COPD 5. Rhonchi
▪ If walay RETRACTION, dili na COPD - low pitched clunky or rattling sounds resembling a clear
or Pneumonia with as snore.
• APEX OF LUNG - Obstruction or mucus build-up in the large airways
o Landmark: first clavicle
• AUSCULTATION 6. Rales or crackles or “crepitation
o Diaphragm
- intermittent sound most notices with inspiration.
▪ Determine agad2 sa sound
- Clunky, rattling, crackling, clinking or popping, noted
▪ Bell kay makapal
when the smaller airways open suddenly suring
• 3 CONDITIONS IN COPD (BEFORE)
inspiration.
o Bronchiectasis
- Moist or dry fine crackles indicates small airway disease
o Emphysema → overdilation of alveoli, unable to
- Coarse crackles noted in large airways disorders.
perform gas exchange
• MOIST & FINE CRACKLES
▪ Dili ka perform ug SIMPLE
o Bronchial tree ang affected
DIFFUSION
• COARSE CRACKLE
o Asthma
o Large airway
ADVENTITIOUS BREATH SOUNDS AND CAUSES
7. Pleural/ Friction Rub:
1. Wheezing
- gritty sound, occur in both inspiration and expiration
- High whistling lung sounds, noted with expirations; - Does not clear with coughing
- Squeaky, musical or like moaning (when low pitched)
- Diffuse and generalized wheezing = asthma Causes:
- Focally in one region = obstruction by a foreign body or Conditions that causes pleural inflammation
tumor. - Pleurisy
- Musical wheezes (violin-like) may be like a single note or - Lung tumors extension to the pleura
multiple notes. - Pleural mesothelioma – malignant tumor of the pleura
o Single notes- common with small airways
alterations
CHIP-IN INFORMATION NI MAGGY
o Multiple notes or different tones- larger airways
involvement
PERCUSSION
- Use fingertips or fingerpads
TABARANZA, CZEJAN RAE BSN-3 53
- MAGPERCUSS SA INTERCOSTAL SPACE → dilis a
bone
PALPATION
- Apply direct pressure with
- Fingertips for skin lesions and subcutaneous masses
- Ball of the hand for deeper masses
• Generalized flank or rib discomfort
• Frontal and maxillary sinuses
• Tenderness, masses
• Respiratory excursion
• Crepitus
• Tactile fremitus
PERCUSSION
- tap the anterior and posterior chest and each ICS
➢ Compare sounds from side to side to
determine if underlying tissues are air, fluid
or solid material filled
➢ Used to estimate the size and location of
certain structures within the thorax such as
the heart, liver and diaphragm.
• Diaphragmatic excursion
• Flatness (thigh), dullness( liver), resonance (normal
lung), tympanic (gastric air, bubbles)
• Hyper resonance: increased with emphysema or a
pneumothorax
- Hypo resonance (dull sound with percussion) : decrease
with pleura effusion or pneumonia
TABARANZA, CZEJAN RAE BSN-3 54
You might also like
- Respiratory System BAYLONDocument17 pagesRespiratory System BAYLONElijah Joaquin Payumo BaylonNo ratings yet
- Anaphy-Respiratory HandoutDocument7 pagesAnaphy-Respiratory HandoutAEGEL DARO TORRALBANo ratings yet
- Respiratory System HandoutDocument11 pagesRespiratory System HandoutJohn Carlo SantiagoNo ratings yet
- Anaphy - Chapter 23 - Respiratory SystemDocument9 pagesAnaphy - Chapter 23 - Respiratory SystemAileen DemaguilaNo ratings yet
- Anatomy and Physiology Handout # 15 Respiratory System-1Document8 pagesAnatomy and Physiology Handout # 15 Respiratory System-1Jounri Arsted Dimabuyu (Kaiz)No ratings yet
- Lesson 5 Respiratory SystemDocument8 pagesLesson 5 Respiratory SystemJulio De Guzman100% (1)
- Respiratory System - ReviewerDocument8 pagesRespiratory System - ReviewerEva Marie GaaNo ratings yet
- Nose and Parasinuses: I. A. B. C. D. E. F. G. II. A. B. C. D. IiiDocument3 pagesNose and Parasinuses: I. A. B. C. D. E. F. G. II. A. B. C. D. IiiKenneth TorresNo ratings yet
- CHAPTER 10-Respiratory SystemDocument3 pagesCHAPTER 10-Respiratory SystempraiseginelcNo ratings yet
- HAP RespiratoryDocument4 pagesHAP Respiratorysmzw4r78sqNo ratings yet
- Medsurg Reviewer (Prelim)Document71 pagesMedsurg Reviewer (Prelim)JOANA MARIE MAE SANTOS BASILIONo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemNicole Anne PamorNo ratings yet
- Respiratory SystemDocument17 pagesRespiratory SystemrishellemaepilonesNo ratings yet
- The Respiratory SystemDocument10 pagesThe Respiratory SystemMiguel GumatayNo ratings yet
- ... 2 Finals Pulmonary PhysiologyDocument9 pages... 2 Finals Pulmonary PhysiologyELIZABETH GRACE AMADOR100% (1)
- Respiratory System ReviewerDocument7 pagesRespiratory System ReviewerVictoria Ellex TiomicoNo ratings yet
- Rle 070722Document14 pagesRle 070722kyla arachelleNo ratings yet
- External Respiration: Angiotensin-Converting EnzymeDocument4 pagesExternal Respiration: Angiotensin-Converting EnzymeEllä PabustanNo ratings yet
- KINE 2031 Test 4 NotesDocument16 pagesKINE 2031 Test 4 NotesnokiaNo ratings yet
- Ms Lec 2 Respiratory SystemDocument11 pagesMs Lec 2 Respiratory SystemLabinnah MoresNo ratings yet
- Respiratory SystemDocument7 pagesRespiratory SystemChristiane with an ENo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument14 pagesAnatomy and Physiology of The Respiratory SystemAmore BuenafeNo ratings yet
- Review On Respiratory SystemDocument4 pagesReview On Respiratory Systemsecondacvalo123No ratings yet
- Respiratory SystemDocument2 pagesRespiratory SystemjuliamaesimbreNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemChelsie NicoleNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemCharlie CharlesNo ratings yet
- Respiratory TransesDocument4 pagesRespiratory TransesAriane Shane BidoNo ratings yet
- Lesson 1 Overview of The Respiratory SystemDocument3 pagesLesson 1 Overview of The Respiratory SystemJacqueline S. PunoNo ratings yet
- Organs of The Respiratory SystemDocument8 pagesOrgans of The Respiratory SystemCrystal Kaye RecasaNo ratings yet
- 11J Caybot Jashjovian Task11Document19 pages11J Caybot Jashjovian Task11JASH JOVIAN CAYBOTNo ratings yet
- RT 105 Prefinal NotesDocument24 pagesRT 105 Prefinal NotesLouiseNo ratings yet
- 2 - Respiratory SystemDocument9 pages2 - Respiratory SystemHannah Grace CorveraNo ratings yet
- Chapter 15 Respiratory SystemDocument3 pagesChapter 15 Respiratory SystemRayumaaa100% (1)
- Respiratory System Clips 1-5Document1 pageRespiratory System Clips 1-5api-552227798No ratings yet
- Respiratory SystemDocument13 pagesRespiratory SystemAly HannahNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory SystemJed Kachel BugayongNo ratings yet
- Respiratory SystemDocument8 pagesRespiratory SystemHenry BuñagNo ratings yet
- 12 Respiratory System - ATFDocument43 pages12 Respiratory System - ATFLucas BarbosaNo ratings yet
- Midterms - Medsurg LecDocument23 pagesMidterms - Medsurg LecGiel Margareth LindoNo ratings yet
- Respiratory System: LarynxDocument4 pagesRespiratory System: LarynxLouise GermaineNo ratings yet
- Pre-Finals Topic 1 AnaphyDocument5 pagesPre-Finals Topic 1 AnaphyGlenice Joy SenocNo ratings yet
- ANPH Wk13 - Pulmonary SystemDocument12 pagesANPH Wk13 - Pulmonary SystemSin I GangNo ratings yet
- (Transes) Human Histology - 14 Respiratory SystemDocument17 pages(Transes) Human Histology - 14 Respiratory SystemReina CastronuevoNo ratings yet
- Respiratory System - NotesDocument7 pagesRespiratory System - NotesataraxialliNo ratings yet
- Respiratory SystemDocument6 pagesRespiratory Systemshane.surigaoNo ratings yet
- Physiology Of: RespirationDocument51 pagesPhysiology Of: RespirationDr. R. PeriasamyNo ratings yet
- AP - Respiratory SystemDocument3 pagesAP - Respiratory SystemKatalina Estelle LaurierNo ratings yet
- Micro - Respiratory SystemDocument3 pagesMicro - Respiratory SystemKaren ValdezNo ratings yet
- Anatomy and Physiology Respiratory System: O CO O CO O CODocument5 pagesAnatomy and Physiology Respiratory System: O CO O CO O COAJ BayNo ratings yet
- Medical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationDocument44 pagesMedical Surgical (MS) Lecture Respiratory System: Alteration in OxygenationYman Gio BumanglagNo ratings yet
- OxygenationDocument24 pagesOxygenationJohn Anthony de GùzmanNo ratings yet
- Anaphy - MOD 1 (Finals)Document6 pagesAnaphy - MOD 1 (Finals)smzw4r78sqNo ratings yet
- Respiratory SystemDocument2 pagesRespiratory Systemlim.angelyne0126No ratings yet
- Trans Savi Oto Lec 05 Applied Anatomy and Physiology of The Nose 1st SemesterDocument7 pagesTrans Savi Oto Lec 05 Applied Anatomy and Physiology of The Nose 1st SemesterJoherNo ratings yet
- Happ Finals Week 14Document8 pagesHapp Finals Week 14angelaggabao0No ratings yet
- Reviewer in Anatomy PhysiologyDocument50 pagesReviewer in Anatomy PhysiologyAuthor - SanNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory SystemChloe Mae PastranaNo ratings yet
- 2 - Respiratory SystemDocument9 pages2 - Respiratory SystemHannah Grace CorveraNo ratings yet
- Daftar Pustaka TirotoksikosisDocument2 pagesDaftar Pustaka TirotoksikosisCut Mulya MutiaNo ratings yet
- Flaps in Head & Neck Reconstruction: Moderator: DR - Arun Kumar .K.V Presenter: DR - Ananth Kumar.G.BDocument78 pagesFlaps in Head & Neck Reconstruction: Moderator: DR - Arun Kumar .K.V Presenter: DR - Ananth Kumar.G.BisabelNo ratings yet
- Chronic Suppurative Otitis Media PDFDocument3 pagesChronic Suppurative Otitis Media PDFsarahNo ratings yet
- Cerebrovascular AccidentDocument6 pagesCerebrovascular AccidentRodel CamposoNo ratings yet
- Morphology of Permanent CaninesDocument14 pagesMorphology of Permanent CaninesPrince AhmedNo ratings yet
- Rheumatic EyeDocument10 pagesRheumatic EyeDr Dushyant Kamal DhariNo ratings yet
- HA Checklist Mouth Nose ThoraxDocument9 pagesHA Checklist Mouth Nose ThoraxGemmalene PaclebNo ratings yet
- Fractures of Middle Third of Facial SkeletonDocument36 pagesFractures of Middle Third of Facial SkeletonAmy GraceNo ratings yet
- Thyroid Exam OSCEDocument4 pagesThyroid Exam OSCEJon Mark LimNo ratings yet
- ThyroidectomyDocument2 pagesThyroidectomykzone2290No ratings yet
- Oral Anatomy Lesson 1Document2 pagesOral Anatomy Lesson 1Rosette Go100% (2)
- WS - Ear Structure and Function WORDDocument4 pagesWS - Ear Structure and Function WORDAlvand HormoziNo ratings yet
- Medial Wall of Nasal Cavity (Nasal Septum) : Plate 15Document11 pagesMedial Wall of Nasal Cavity (Nasal Septum) : Plate 15Andreea LăzăroiuNo ratings yet
- Kitamura 2017Document13 pagesKitamura 2017angelica cuevasNo ratings yet
- Cranial Cavity 1 PDFDocument16 pagesCranial Cavity 1 PDFOrangzaib OrangzaibNo ratings yet
- Dokumen - Tips - Pediatric Head Trauma Joshua Rocker MD Pediatric Emergency Medicine SchneiderDocument43 pagesDokumen - Tips - Pediatric Head Trauma Joshua Rocker MD Pediatric Emergency Medicine SchneiderKen100% (1)
- 50+ Medium Length Hairstyles & Haircut Tips For Men Man of ManyDocument1 page50+ Medium Length Hairstyles & Haircut Tips For Men Man of ManyAditya KapoorNo ratings yet
- MeningiomaDocument7 pagesMeningiomadrhendyjuniorNo ratings yet
- Penatalaksanaan Fisioterapi Pada Kasus Bell S Palsy Dextra Di Rsup DR Sardjito YogyakartaDocument15 pagesPenatalaksanaan Fisioterapi Pada Kasus Bell S Palsy Dextra Di Rsup DR Sardjito YogyakartaYasudalahNo ratings yet
- Maxillary Anesthetic TechniquesDocument83 pagesMaxillary Anesthetic TechniquesAnonymous k8rDEsJsU1No ratings yet
- Hyoid BoneDocument31 pagesHyoid Bonekhorrami4No ratings yet
- Foreign Bodies in The EarDocument6 pagesForeign Bodies in The EarGlorina KumarNo ratings yet
- Clinical Relevance of Third Permanent Molars in Relation To Crowding After Orthodontic TreatmentDocument3 pagesClinical Relevance of Third Permanent Molars in Relation To Crowding After Orthodontic TreatmentAndrésAcostaNo ratings yet
- Neuro Ward PDFDocument39 pagesNeuro Ward PDFGlenn ManapulNo ratings yet
- Cranial NervesDocument9 pagesCranial Nervesangrypandasaredangerous100% (4)
- Cleft Lip and PalateDocument85 pagesCleft Lip and PalateVijay ChinthaNo ratings yet
- Class III and Fixed Functional ApplianceDocument51 pagesClass III and Fixed Functional ApplianceOsama GamilNo ratings yet
- 2019 ENT Nursing Exam 1Document7 pages2019 ENT Nursing Exam 1KAUH EducationNo ratings yet
- Study of The Effect of Mobile Phones On HearingDocument5 pagesStudy of The Effect of Mobile Phones On HearingPranay DasNo ratings yet
- Open and Closed Mouth Techniques of Local AnesthesiaDocument88 pagesOpen and Closed Mouth Techniques of Local AnesthesiaAtika Iftikhar MirNo ratings yet