Professional Documents
Culture Documents
Anti Infectives
Uploaded by
IconMaico0 ratings0% found this document useful (0 votes)
2 views40 pagesCopyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views40 pagesAnti Infectives
Uploaded by
IconMaicoCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 40
NCM 106: ANTI-INFECTIVES
Ma. Concepcion A. Maico, EdD, MAN, RN
Clinical Instructor
Introduction
• Anti-infective agents are drugs utilized to exert effect on invading
foreign organisms on the body, especially those which can cause
infection.
• Its scientific investigation started in the 1920s after Paul Ehrlich
developed synthetic chemicals that would be effective only against
the certain proteins or enzyme systems used only by infecting
organism and not by human cells.
• Drug resistance remains to be the major challenge in the use of anti-
infectives against infections. Emergent strains are rapidly adapting to
repel the effects of anti-infectives.
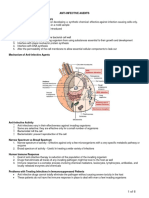
Mechanism of
Action
Therapeutic Action
• The goal of therapy is interference with the normal function of the
invading organisms to prevent them from reproducing and thereby
causing cell death.
• Narrow-spectrum anti-infectives are agents that are so selective in
their action that they are effective against only a few microorganisms.
• Broad-spectrum anti-infectives are agents that interfere with
biochemical reactions in many different kinds of microorganisms.
• Anti-infectives that can cause cell death are said to
have bactericidal effects.
• Anti-infectives that can interfere with the ability of the cells to
reproduce or divide are said to have bacteriostatic effects.
Resistance
• Over time, invading pathogens develop resistance to anti-infectives.
• Resistance is the ability over time to adapt to an anti-infective drug and
produce cells that are no longer affected by a particular drug. Here are a
number of ways that microorganisms can develop resistance:
• Enzyme production. Strains of bacteria that were once susceptible to
penicillin can now produce an enzyme called penicillinase which
inactivates penicillins before they can exert their effect to the bacteria.
• Cell membrane permeability alteration. This prevents the drug from
entering the cell. Some bacteria alter transport systems to prevent the
drug from being transported actively into the cell.
• Binding site alteration. Prevents the drug from being accepted into the
cell.
• Chemical production. Acts as antagonist to the drug.
Prevention of Resistance
• Drug dosing. The nurse may collaborate with the physician for
around-the-clock dosing to eliminate the peaks and valleys in drug
concentration. This also helps maintain a constant therapeutic level to
prevent the emergence of resistant microbes during times of low
concentration.
• Drug duration. The nurse should emphasized the importance of
finishing the prescribed duration (correct number of times each day
for the full number of days) of anti-infective therapy to ensure that
microbes are completely eliminated and are not given the chance to
grow and develop resistant strains.
Indications
CHILDREN
• Use with caution as early exposure can lead to early sensitivity.
• Use of antibiotics in pediatric ear infections (which might be a viral
infection) may contribute to development of drug resistance.
• Children are susceptible to gastrointestinal (GI) and nervous system
effects of anti-infectives so it is important to monitor their hydration
and nutritional status carefully.
Indications
ADULTS
• This age group tend to demand for quick cure to various signs and
symptoms. Therefore, drug allergies and emergence of resistant
strains can be a big problem with this group.
• Extra caution is exercised in pregnant and lactating women because
many of these agents have teratogenic effects to the fetus and can
cross into breast milk.
Indications
OLDER ADULTS
• They present with manifestations that are different than younger age
groups so culture and sensitivity tests are important to determine the
type and extent of infection.
• They are susceptible to severe GI, renal, and neurological effects and
must be monitored for nutritional status and hydration during drug
therapy.
• Their liver function should always be taken in consideration when
planning for anti-infective therapy.
Adverse Effects
• Kidney damage. Drugs like aminoglycosides have direct toxic effect on
the fragile cells in the kidney and can cause conditions ranging from
renal dysfunction to full-blown renal failure. Patients should be kept
well-hydrate throughout drug therapy course to facilitate drug
excretion.
• GI toxicity. Many anti-infectives have direct toxic effects on the cells
lining the GIT causing nausea, vomiting, stomach upset, and diarrhea.
Some drugs have toxic effects on the liver causing hepatitis and even
liver failure.
Adverse Effects
• Neurotoxicity. Some anti-infectives can damage or interfere with the
function of nerve tissue, usually in areas where drugs tend to
accumulate in high concentrations. For example, aminoglycoside
antibiotics collect in the 8th cranial nerve and can cause dizziness,
vertigo, and loss of hearing. Chloroquine, a drug for treatment of
malaria can accumulate in the retina and optic nerve and cause
blindness.
Adverse Effects
• Hypersensitivity Reactions. Most agents are protein bound for
transfer through the cardiovascular system and are able to induce
antibody formation in susceptible people. With next exposure,
immediate or delayed allergic responses may occur.
• Superinfections. Broad-spectrum anti-infectives can destroy normal
flora. Superinfections are infections that occur when opportunistic
pathogens that were kept in check by normal flora bacteria have the
opportunity to invade tissues. Common causes of superinfections are
Proteus and Pseudomonas.
Penicillins
• MOA: Penicillins work by interfering with the synthesis of bacterial
cell walls – eventually leading to lysis.
• Adverse Effects:
• Hypersensitivity: Anaphylaxis, rash, fever, wheezing
• GI upset: Nausea, vomiting, diarrhea
• Superinfections
• Warnings
• Requires dosage reductions in renal impairment (piperacillin,
ampicillin)
Penicillins
• Nursing Considerations:
• Screen clients with claimed allergies for true hypersensitivity
reactions (e.g. rash, wheezing, anaphylaxis) ensuring the client did
not just have an adverse effect (e.g. diarrhea, nausea, vomiting).
Adverse effects do not result in a contraindication to this class of
medications.
• Monitor pulmonary function and for signs of allergic reaction.
• Clients should be instructed to complete the full antibiotic
regimen to encourage eradication of infection and discourage
resistance.
• Most penicillins can be taken with food to mitigate GI symptoms.
• Common Key Generics (Brands):
• Penicillin G (IV)
• Penicillin VK (oral)
• Nafcillin, oxacillin
• Ampicillin, Ampicillin-sulbactam (Unasyn)
• Amoxicillin (Amoxil), Amoxicillin-clavulanate (Augmentin)
• Piperacillin, piperacillin-tazobactam (Zosyn)
Cephalosporins
• MOA: Similar mechanism compared to penicillins – cephalosporins
fall under the beta-lactam classification.
• Adverse Effects:
• Hypersensitivity: Clients with true penicillin allergies develop
reactions with cephalosporin usage. As cephalosporin generations
increase the risk of allergic reactions to people with penicillin
allergies decreases.
• GI upset: Nausea, vomiting, diarrhea
• CNS: Headache, dizziness
• Nephrotoxicity
• Superinfections
Cephalosporins
• Precautions:
• Ceftriaxone should not be reconstituted or mixed with a calcium-
containing product (e.g. Ringer’s or Hartmann’s solution) due to
risk of precipitation in the lungs or kidneys
• Nursing Interventions:
• Screen for true penicillin allergies – ensuring a real
hypersensitivity reaction.
• Monitor pulmonary function and for signs of allergic reaction.
• Generally safe in pregnancy.
• Monitor renal function
• Potential interaction with anticoagulants → bleed risk
Cephalosporins
• Common Key Generics (Brands):
• 1st Gen: Cefazolin, cefadroxil, cephalexin (Keflex)
• 2nd Gen: Cefoxitin, cefprozil, cefuroxime
• 3rd Gen: Ceftriaxone, cefixime, ceftazidime, cefpodoxime, cefdinir,
ceftriaxone (Rocephin)
• 4th Gen: Cefepime (Maxipime)
• 5th Gen: Ceftaroline
Tetracyclines
• MOA: Inhibit protein synthesis → inhibition of bacterial cell growth.
• Adverse Effects:
• Not pregnancy safe
• Teeth discoloration
• Sun sensitivity
• Weakening of skeletal bone structure
• Hepatotoxicity
Tetracyclines
• Warnings:
• Tetracyclines given to children under the age of 8 can cause permanent tooth
discoloration if given for prolonged courses.
• Accumulation of antibiotics can occur in fetal bone and teeth in pregnancy
• Risk of hepatotoxicity in pregnant women
• Nursing Interventions:
• Consult on increased sensitivity to light – avoid excessive sun exposure or use
sunscreen
• Avoid antacids and multivitamins with this medication
• Interaction with birth control – caution with oral contraceptives; additional
birth control may be needed
Tetracyclines
• Common Key Generics (Brands):
• Minocycline (Minocin)
• Doxycycline (Doryx, Periostat)
• Tetracycline
• Tigecycline
Macrolides
• MOA: Interferes with protein synthesis in susceptible bacteria
inhibiting bacterial cell growth.
• Adverse Effect:
• QT prolongation
• Monitor ECG
• Avoid other QT prolonging drugs including fluoroquinolones
• Hepatotoxic
• N/V since taken with empty stomach
Macrolides
• Warnings:
• Practice caution when using these medications as the suffix
“mycin” exists in other drug classes such as tobramycin which is
an aminoglycoside.
• Renal dosing adjustments required for clarithromycin
• QT interval prolongation – increased risk of torsade de pointes
Macrolides
• Contraindication:
• Azithromycin in clients with a history of cholestatic jaundice or
hepatic dysfunction
• Nursing Interventions:
• Monitor for signs of QT prolongation and risk of atrial fibrillation
• Monitor ALT and AST
• Should be taken on an empty stomach
Macrolides
• Common Key Generics (Brands):
• Azithromycin (Zithromax)
• Clarithromycin (Biaxin)
• Erythromycin (Ery-Tab)
Fluoroquinolones
• MOA: Interference with DNA enzymes that are required for the growth of
bacterial cells.
• Adverse Effects:
• GI: Nausea, vomiting, diarrhea
• CNS: Headache, dizziness
• Risk for tendinitis and tendon rupture in elderly and in renal impairment
• Photosensitivity – avoid long exposure to sun or use sunscreen
• Neurologic effects (e.g. headache, dizziness, altered mental status)
• Peripheral neuropathy
• Risk of aortic aneurysm → dangerous bleeding and death
• QT prolongation
Fluoroquinolones
• Warning:
• The use of these medications should be restricted to severe-complicated
infections
• Increased risk of toxicity (e.g. tendon rupture, QT prolongation) in elderly
• Avoid use in clients with aortic aneurysms and those with risk factors for
aneurysms including peripheral atherosclerotic vascular diseases, advanced
age, and hypertension.
• Avoid during pregnancy – use safer alternatives when able
• Risk of musculoskeletal toxicity in children
• Avoid in clients with myasthenia gravis – as macrolides may precipitate
neuromuscular-blocking activity
• Increased risk of C. difficile – clients on extended periods of these
medications should be given probiotics to reduce risk
Fluoroquinolones
• Nursing Interventions:
• Avoid in pregnancy and lactation
• Monitor for signs and symptoms QT prolongation, tendon rupture, and bleeding in
elderly and renally impaired clients
• Avoid with antacids or multivitamins as these may reduce the efficacy of the
antibiotic increasing resistance
• Ensure all the medication is taken to discourage resistance
• Common Key Generics (Brands):
• Ciprofloxacin (Cipro)
• Gemifloxacin
• Levofloxacin (Levaquin)
• Moxifloxacin
• Ofloxacin (Floxin)
Aminoglycosides
• MOA: Powerful antibiotics which demonstrate bactericidal inhibition
of protein synthesis – particularly gram-negative bacteria.
• Adverse Effects:
• Ototoxicity (tinnitus, vertigo, irreversible deafness)
• Renal toxicity
• GI: Nausea, vomiting, diarrhea
• Heart palpitations
• Hypersensitivity
Aminoglycosides
• MOA: Powerful antibiotics which demonstrate bactericidal inhibition
of protein synthesis – particularly gram-negative bacteria.
• Adverse Effects:
• Ototoxicity (tinnitus, vertigo, irreversible deafness)
• Renal toxicity
• GI: Nausea, vomiting, diarrhea
• Heart palpitations
• Hypersensitivity
Aminoglycosides
• Warnings:
• High risk of nephrotoxicity and ototoxicity – careful monitoring should be in
practice when clients are on these medications
• Risk of neuromuscular blockade is rare but serious – caution with myasthenia
gravis
• Nursing Interventions:
• Avoid with preexisting hearing loss due to ototoxic effects
• May worsen herpes or mycobacterial infections
• Renal toxicity (monitor Scr [serum creatinine] for increases > 1)
• Avoid in pregnancy and lactation
• Ensure properly dose by monitoring trough levels periodically
Aminoglycosides
• Common Key Generics (Brands):
• Amikacin (Amikin)
• Gentamicin
• Neomycin
• Streptomycin
• Tobramycin (Tobrex)
Vancomycin
• MOA: Inhibition of cell wall synthesis leading to decrease in bacterial cell
growth – bactericidal in most gram-positive bacteria.
• Adverse Effects:
• Thrombophlebitis when given too quickly, given via PICC line as
preferred route
• Watch for pain, redness and swelling
• Red man’s syndrome
• Severe hypotension
• Flushing
• Pruritis on face, neck, and extremities = too fast infusion
• At least over > 60 minutes
Vancomycin
• Nephrotoxic
• Ototoxic
• Anaphylaxis → administer EPI
• Hives
• Angioedema
• Wheezing
• Trough level check 15-30 minutes before admin
• Range 10-20
• Watch for signs of toxicity
Vancomycin
• Warnings:
• Renal dose adjustments in renal impairment (refer to hospital
procedures)
• Do not infuse more than 5 mg/mL in concentration in less than 60
minutes – to avoid infusion-related reactions
• Risk of extravasation and thrombophlebitis – ensure proper needle or
catheter placement prior to infusion
• Neutropenia with prolonged use
• High risk of superinfection
• Formulations containing polyethylene glycol (PEG 400) or N-acetyl D-
alanine (NADA) not recommended for use in pregnancy due to risk of
fetal malformations
Vancomycin
• Nursing Interventions:
• Dosing based on trough levels – check 15-30 minutes prior to administration
of antibiotics
• Moderate infections: Trough goal = 10-15
• Severe infections: Trough goal = 15-20
• Trough is usually drawn before the 4th or 5th dose
• Initial loading dose is based on clients’ weight
• Infuse bolus slowly over an hour to avoid adverse effects
• Nephrotoxic monitor for the following
• Scr > 1.3 = Bad for kidney
• BUN > 20
• Urine output < 30 ml/hr or less = kidney in distress
Vancomycin
• Common Key Generics (Brands):
• Vancomycin (Vanco)
Sulfonamides
• MOA: Inhibition of folic acid synthesis which are precursors for RNA and DNA
synthesis → inhibiting bacterial cell growth
• Adverse Effects:
• Hypersensitivity: Contraindicated when a known or suspected sulfa allergy
is present (including allergies to sulfa containing drugs e.g. sulfonylureas,
thiazides)
• GI: Nausea, vomiting, diarrhea
• Renal: Crystalluria
• CNS: Headache, dizziness
• Bone marrow depression
• Photosensitivity, rash
Sulfonamides
• Warnings:
• Risk of serious hypersensitivity reactions – screen for sulfa
allergies
• Blood dyscrasia – fatalities associated with severe reactions
including agranulocytosis and aplastic anemia
• Hepatic necrosis
• Hyperkalemia – caution in clients with heart conditions
• Hypoglycemia – caution in diabetics
• Risk of thrombocytopenia
Sulfonamides
• Nursing Interventions:
• Screen for true sulfa allergies – monitor for signs and symptoms of
hypersensitivity
• Can take with food with upset stomach
• Not safe for pregnancy
• Nephrotoxic monitor for the following
• Scr > 1.3 = Bad for kidney
• BUN > 20
• Urine output < 30 ml/hr or less = kidney in distress
You might also like
- NCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!From EverandNCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!Rating: 5 out of 5 stars5/5 (4)
- Amoxicillin Guide: Draw out your antibiotic weapon to defeat bacterial infections like pneumonia, STDs, urinary tract and skin infectionsFrom EverandAmoxicillin Guide: Draw out your antibiotic weapon to defeat bacterial infections like pneumonia, STDs, urinary tract and skin infectionsRating: 5 out of 5 stars5/5 (24)
- NCM 106 AntinfectivesDocument6 pagesNCM 106 AntinfectivesJoshua MendozaNo ratings yet
- NCM 106 AntibacterialDocument11 pagesNCM 106 AntibacterialBruno, Kurt Andrei V.No ratings yet
- NUR138 Lecture 8 38-39Document65 pagesNUR138 Lecture 8 38-39FeliciaDorghamNo ratings yet
- Anti InfectivesDocument126 pagesAnti Infectiveseunice lachicaNo ratings yet
- Antimalarial Drugs: Presenter Basil Mupita Rgn/BscneDocument35 pagesAntimalarial Drugs: Presenter Basil Mupita Rgn/BscneTapiwaNo ratings yet
- Antimicrobial Agents 2021Document82 pagesAntimicrobial Agents 2021Aprilene Angel Balaque ZunegaNo ratings yet
- D. Antiviral Antiprotozoal AntihilmenticsDocument31 pagesD. Antiviral Antiprotozoal AntihilmenticsKim Shyen BontuyanNo ratings yet
- ANTIBIOTICS23Document94 pagesANTIBIOTICS23RPMFA RPMFANo ratings yet
- Pharmacology Powerpoint - AntibioticsDocument107 pagesPharmacology Powerpoint - AntibioticsMark Norriel Cajandab100% (2)
- Antimicrobial Agents: Mechanisms of Action and Clinical ImplicationsDocument29 pagesAntimicrobial Agents: Mechanisms of Action and Clinical ImplicationsGwyneth Maehram Dela CruzNo ratings yet
- Chapter 9 Antibiotics Key Points and SummaryDocument2 pagesChapter 9 Antibiotics Key Points and SummaryJacqueline GreerNo ratings yet
- InfectionDocument143 pagesInfectionMaria KamalNo ratings yet
- Antineoplastic AgentsDocument83 pagesAntineoplastic AgentsDwynwen Aleaume GumapacNo ratings yet
- AntibioticsDocument70 pagesAntibioticsMunazza QuraishiNo ratings yet
- Class 05 (Autosaved)Document75 pagesClass 05 (Autosaved)Paolo MendozaNo ratings yet
- B. AntibioticsDocument38 pagesB. AntibioticsKim Shyen BontuyanNo ratings yet
- NCM 106 Anti HelminticsDocument7 pagesNCM 106 Anti HelminticsJod BellNo ratings yet
- NCM 106 Anti HelminticsDocument7 pagesNCM 106 Anti HelminticsCheska YsabelleNo ratings yet
- Antibiotics 150406092448 Conversion Gate01Document76 pagesAntibiotics 150406092448 Conversion Gate01Dr.Aman SaxenaNo ratings yet
- Drugs Used in Infections (Chemotherapeutic AgentsDocument683 pagesDrugs Used in Infections (Chemotherapeutic AgentsKobby AmoahNo ratings yet
- Adverse Drug Reaction: Hepatic FunctionDocument37 pagesAdverse Drug Reaction: Hepatic FunctionVon Valentine MhuteNo ratings yet
- Anti Microbials (Repaired)Document79 pagesAnti Microbials (Repaired)drsidra.mustafaNo ratings yet
- MID 2 PHARMA Anti-Infective DrugsDocument11 pagesMID 2 PHARMA Anti-Infective DrugsMariah Angela PinedaNo ratings yet
- Albacio Eddiva Dapli-An Magwilang MaspilDocument138 pagesAlbacio Eddiva Dapli-An Magwilang MaspilJustineNo ratings yet
- Antibiotics Mechanisms Actions EffectsDocument91 pagesAntibiotics Mechanisms Actions EffectsDareRaymond100% (1)
- Superficial Fungal Infections GuideDocument43 pagesSuperficial Fungal Infections GuideNoor AliNo ratings yet
- 1 Principles & Cell Wall Synthesis InhibitorsDocument94 pages1 Principles & Cell Wall Synthesis InhibitorsRjDNo ratings yet
- Pharma ReportDocument74 pagesPharma ReportDivine LavaNo ratings yet
- Antimycobacterials - ReyesDocument22 pagesAntimycobacterials - ReyesVivian CaballeroNo ratings yet
- Antibiotic's Interactions in GynecologyDocument26 pagesAntibiotic's Interactions in Gynecologyمحمد قاسمNo ratings yet
- Antimicrobial DrugsDocument20 pagesAntimicrobial Drugsnadar shahNo ratings yet
- Antimicrobial AgentsDocument244 pagesAntimicrobial AgentsN Gv FcNo ratings yet
- Week 4 Chemotherapeutic AgentsDocument339 pagesWeek 4 Chemotherapeutic AgentsLassie AbusadoNo ratings yet
- Antifungal AgentsDocument22 pagesAntifungal AgentsQuolette Constante100% (1)
- Mycobacterium Tuberculosis Infection Causes, Treatment, Nursing CareDocument22 pagesMycobacterium Tuberculosis Infection Causes, Treatment, Nursing CareKakai Ablanque LopozNo ratings yet
- ANTIMETABOLITES: Cancer Drugs That Interfere With Cell GrowthDocument12 pagesANTIMETABOLITES: Cancer Drugs That Interfere With Cell GrowthRichlle CortesNo ratings yet
- ANTIMICROBIAL PRESCRIPTIONDocument64 pagesANTIMICROBIAL PRESCRIPTIONMalueth AnguiNo ratings yet
- Module 3Document6 pagesModule 3richelleambrocio054No ratings yet
- Chapter 40 Fall 2012Document32 pagesChapter 40 Fall 2012m1k0eNo ratings yet
- Koas - Farmakoterapi ISKDocument37 pagesKoas - Farmakoterapi ISKRIFATUL ISLAMIYAHNo ratings yet
- Drugs Used in Pediatric DentistryDocument33 pagesDrugs Used in Pediatric Dentistryaamee9690% (10)
- PHARMACOLOGY AntibioticsDocument29 pagesPHARMACOLOGY AntibioticsBeck33ers5826100% (1)
- Pharma Review FinalsDocument31 pagesPharma Review FinalsLanz Andrei MatociñosNo ratings yet
- Use of Antibiotics 2017Document17 pagesUse of Antibiotics 2017bernard.triciaNo ratings yet
- Pharma 2Document9 pagesPharma 2freakihottieNo ratings yet
- Autoimmune diseases and immunosuppressant drugs overviewDocument28 pagesAutoimmune diseases and immunosuppressant drugs overviewimnasNo ratings yet
- Basic Dental PharmacologyDocument152 pagesBasic Dental PharmacologyDr-Mohamed KandeelNo ratings yet
- Pharmacology of Antibiotics Nurse Licensure Exam ReviewDocument27 pagesPharmacology of Antibiotics Nurse Licensure Exam ReviewSeth-Thomas TateNo ratings yet
- Anti InfectivesDocument145 pagesAnti Infectivescharles babasaNo ratings yet
- A. Antineoplastic DrugsDocument48 pagesA. Antineoplastic DrugsKim Shyen BontuyanNo ratings yet
- Khamlin Hamad Abdal - GroupeaDocument39 pagesKhamlin Hamad Abdal - GroupeaKhamlin NurseNo ratings yet
- Khamlin Hamad Abdal - GroupeaDocument39 pagesKhamlin Hamad Abdal - GroupeaKhamlin NurseNo ratings yet
- Anti Infective AgentsDocument14 pagesAnti Infective Agentsj45sx5b6wdNo ratings yet
- Drug Study: AmoxicillinDocument4 pagesDrug Study: Amoxicillinm100% (1)
- Pharmacology IDocument202 pagesPharmacology ISalahadinNo ratings yet
- PHARMA REPORTING II - ANTIBIOTICSDocument9 pagesPHARMA REPORTING II - ANTIBIOTICSD A M N E R ANo ratings yet
- By: Clarissa E. Guifaya BSN301/GROUP 3Document17 pagesBy: Clarissa E. Guifaya BSN301/GROUP 3Clarissa GuifayaNo ratings yet
- Anti Tuberculars Fungals ViralsDocument51 pagesAnti Tuberculars Fungals ViralsTito, Stephen Gabriel, A.No ratings yet
- Maternal and Child Health Nursing: Sudden Pregnancy ComplicationsDocument35 pagesMaternal and Child Health Nursing: Sudden Pregnancy ComplicationsIconMaicoNo ratings yet
- GI DrugsDocument35 pagesGI DrugsIconMaicoNo ratings yet
- Chapter 8 - Clarifying Quantitative Research DesignsDocument61 pagesChapter 8 - Clarifying Quantitative Research DesignsIconMaicoNo ratings yet
- 200p Hba UscherpinesDocument59 pages200p Hba UscherpinesIconMaicoNo ratings yet
- Caring For The Woman Experiencing Complications During Labor and BirthDocument26 pagesCaring For The Woman Experiencing Complications During Labor and BirthIconMaicoNo ratings yet
- Microscopy Basics Biology Laboratory 1 PowerPointDocument17 pagesMicroscopy Basics Biology Laboratory 1 PowerPointIconMaicoNo ratings yet
- FHT:Fundal HT QuestionsDocument2 pagesFHT:Fundal HT QuestionsIconMaicoNo ratings yet
- Complications of Labor and BirthDocument54 pagesComplications of Labor and BirthIconMaicoNo ratings yet
- Cell Structure and Taxonomy ExplainedDocument46 pagesCell Structure and Taxonomy ExplainedIconMaicoNo ratings yet
- Nursing Care for At-Risk Mothers and ChildrenDocument19 pagesNursing Care for At-Risk Mothers and ChildrenChelleyOllitro100% (7)
- Lab Manual Microbiology For Allied Health Students 1.3Document115 pagesLab Manual Microbiology For Allied Health Students 1.3IconMaicoNo ratings yet
- Caregiving Through The 5 Stages of Ageing - Brain SparksDocument8 pagesCaregiving Through The 5 Stages of Ageing - Brain SparksIconMaicoNo ratings yet
- Healthcare-Associated Infections GuideDocument25 pagesHealthcare-Associated Infections GuideIconMaicoNo ratings yet
- NCM 109 Course OutlineDocument2 pagesNCM 109 Course OutlineIconMaicoNo ratings yet
- Inside Out - A Psychological InsightDocument6 pagesInside Out - A Psychological InsightIconMaicoNo ratings yet
- The Importance of Self-Awareness in Psychiatric Nursing 1996Document4 pagesThe Importance of Self-Awareness in Psychiatric Nursing 1996IconMaicoNo ratings yet
- Introduction To Microbiology: Ma. Concepcion A. Maico, RN, Man, EddDocument24 pagesIntroduction To Microbiology: Ma. Concepcion A. Maico, RN, Man, EddIconMaicoNo ratings yet
- FEG PPCommunication With Older PeopleDocument21 pagesFEG PPCommunication With Older PeopleroarkesNo ratings yet
- RLE Activity Personality DisorderDocument5 pagesRLE Activity Personality DisorderIconMaicoNo ratings yet
- Harry Potter Psychoanalytical ApproachDocument12 pagesHarry Potter Psychoanalytical ApproachIconMaicoNo ratings yet
- Activity Participation and Older AdultsDocument8 pagesActivity Participation and Older AdultsIconMaicoNo ratings yet
- 2019 Dec ERIA Ageing and Health in The PhilippinesDocument276 pages2019 Dec ERIA Ageing and Health in The PhilippineshexenejenineNo ratings yet
- Erikson Summary ChartDocument1 pageErikson Summary ChartIconMaicoNo ratings yet
- Nursing 311 Techniques of Therapeutic Communication: Technique Description ExampleDocument4 pagesNursing 311 Techniques of Therapeutic Communication: Technique Description ExampleIconMaico100% (1)
- Caregiving Through The 5 Stages of Ageing - Brain SparksDocument8 pagesCaregiving Through The 5 Stages of Ageing - Brain SparksIconMaicoNo ratings yet
- 5 Stages of Aging - Tealridge Retirement CommunityDocument3 pages5 Stages of Aging - Tealridge Retirement CommunityIconMaicoNo ratings yet
- Leininger, Madeleine M. - McFarland, Marilyn R-Transcultural Nursing - Concepts, Theories, Research and practice-McGraw-H PDFDocument648 pagesLeininger, Madeleine M. - McFarland, Marilyn R-Transcultural Nursing - Concepts, Theories, Research and practice-McGraw-H PDFAviati Faradhika100% (10)
- Sunrise Enabler in EthnonursingDocument28 pagesSunrise Enabler in EthnonursingIconMaicoNo ratings yet
- Aging in The Philippines - PSADocument33 pagesAging in The Philippines - PSAIconMaicoNo ratings yet
- Theoretical Foundations of Transcultural NursingDocument19 pagesTheoretical Foundations of Transcultural NursingIconMaicoNo ratings yet
- Misa de Gallo, Quezon City, Metro Manila: Lagro High SchoolDocument9 pagesMisa de Gallo, Quezon City, Metro Manila: Lagro High SchoolZoe Aprille MasuliNo ratings yet
- Incomplete and Co DominanceDocument153 pagesIncomplete and Co Dominancelevie agacerNo ratings yet
- NCM 109 Case Study - Sir JesusDocument25 pagesNCM 109 Case Study - Sir JesusLance RaphaelNo ratings yet
- Psychoneuroimmunology PDFDocument10 pagesPsychoneuroimmunology PDFRatu Nurul FadhilahNo ratings yet
- New Pattr Model Q 01.Document43 pagesNew Pattr Model Q 01.Hari Krishnan KNo ratings yet
- CM1-CU2 - Introduction To CytogeneticsDocument28 pagesCM1-CU2 - Introduction To CytogeneticsKat JornadalNo ratings yet
- Drug Resistance in Bacteria Fungi Malaria PDFDocument629 pagesDrug Resistance in Bacteria Fungi Malaria PDFShridhar Chame100% (1)
- Formulation Ang Evaluationof Herbal Hanitizer Using Psidium Guajava Leaves Extract PDFDocument3 pagesFormulation Ang Evaluationof Herbal Hanitizer Using Psidium Guajava Leaves Extract PDFCatherine AlmarioNo ratings yet
- Continue: Step Ahead Biology Book 4 PDF DownloadDocument6 pagesContinue: Step Ahead Biology Book 4 PDF DownloadTawa tNo ratings yet
- 2020 - Han Et Al. - Fungal Diversity On The Surface of Saffron Corms Growth CharacteristicsDocument26 pages2020 - Han Et Al. - Fungal Diversity On The Surface of Saffron Corms Growth CharacteristicsBianca SilvaNo ratings yet
- PHYS20050 Tutorial 3 - Student Copy Nov 2017Document2 pagesPHYS20050 Tutorial 3 - Student Copy Nov 2017muhammad haziqNo ratings yet
- NEJM Case Report 40-2017Document10 pagesNEJM Case Report 40-2017A. Rauf100% (1)
- Biology Project: Chromosomal DisorderDocument44 pagesBiology Project: Chromosomal DisorderArun Kumar ANo ratings yet
- Vulval Development in C ElegansDocument28 pagesVulval Development in C ElegansSourav DeyNo ratings yet
- CH 11 ReviewDocument9 pagesCH 11 Reviewsadin alkafNo ratings yet
- Central Academy: Biology ProjectDocument12 pagesCentral Academy: Biology ProjectMastbleNo ratings yet
- Novel Proprietary Single-Domain Antibody Fragments: What Are Nanobodies?Document18 pagesNovel Proprietary Single-Domain Antibody Fragments: What Are Nanobodies?InêsNo ratings yet
- Jalukar Refined Functional Carbohydrates 2016 PDFDocument3 pagesJalukar Refined Functional Carbohydrates 2016 PDFJonathanNo ratings yet
- IBO Sample Questions TheoryDocument61 pagesIBO Sample Questions TheoryTania RomanNo ratings yet
- .Gram Negative Bacterias . .Document19 pages.Gram Negative Bacterias . .Nidhi Singh ThakurNo ratings yet
- Pathology 1Document38 pagesPathology 1ARNOLD BORROMEONo ratings yet
- GangreneDocument5 pagesGangreneNader Smadi100% (2)
- Ficha Tecnica Concha de Abanico Media Valva - 2Document1 pageFicha Tecnica Concha de Abanico Media Valva - 2DavidHernandezNo ratings yet
- Worksheet 2.dna and RnaDocument2 pagesWorksheet 2.dna and RnaTeam kalogxz CompilationNo ratings yet
- Draw OrderDocument2 pagesDraw OrderGordon Orr88% (8)
- BIOL200 PSet - Unit 4Document22 pagesBIOL200 PSet - Unit 4Lovey ChandiNo ratings yet
- TLR: Toll-Like Receptors Detect PathogensDocument46 pagesTLR: Toll-Like Receptors Detect PathogensHeru HanantoNo ratings yet
- Botany (Virus)Document48 pagesBotany (Virus)Madhuri DeviNo ratings yet
- Genetic EngineeringDocument40 pagesGenetic EngineeringRalph Vincent De MesaNo ratings yet