Professional Documents
Culture Documents
Everything You Need to Know About Anthrax
Uploaded by
abel semu0 ratings0% found this document useful (0 votes)
70 views47 pagesOriginal Title
Anthrax.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
70 views47 pagesEverything You Need to Know About Anthrax
Uploaded by
abel semuCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 47
Anthrax
By: Dr. Hawine Bekele
May 23,2017
Objective
At the end of this lecture students should be able to:
know the epidemiology, microbiology, pathogenesis of
anthrax infection
Understand the transmission mode and treatment of
the infection
be aware about the prevention methods
Outline
Introduction
Epidemiology
Microbiology
Transmission
Pathogenesis
Clinical presentation
DDX
Diagnosis
Treatment
Prevention
Introduction
Anthrax is a zoonosis infection caused by Bacillus
anthracis.
Systemic anthrax is primarily a disease of herbivores.
Humans become accidentally infected through contact
with infected animals or their products.
Most anthrax is cutaneous (95%) and the remaining
cases of the disease are inhalational and
gastrointestinal.
Anthrax was described in the early literatures of the
Greeks, Romans, Egyptians and Hindus.
The term antrakis means coal in Greek, and the disease
is named after the black appearance of its cutaneous
forms.
was the first clearly recognized bacterial pathogen
The life cycle of the organism was unravelled by
Koch, who recognized the importance of dormant
anthrax spores in the perpetuation of the organism in
soil. These studies eventually led to Koch's postulates
that have been the cornerstone for establishing a
specific pathogen as the causative agent of human and
animal diseases
John bell’s work in inhalational anthrax led to wool
disinfection processes and the term woolsloter’s
disease.
A modern concern is use of anthrax as a biologic
welfare agent.
Epidemiology
Anthrax is uncommon in western Europe, but is not
uncommon in the middle east, the Indian subcontinent,
Africa, Asia & Latin America.
In 1958, approximately 100,000 cases of anthrax
occurred world wide. Exact figures do not exist
because of reporting difficulties in Africa.
Anthrax is endemic in Africa and Asia despite
vaccination programs.
Sporadic outbreaks occurred as a result of both
agricultural and military disruptions.
During the 1978 Rhodesian civil war, failure of
veterinary vaccination program led to a human
epidemic, causing 6500 anthrax cases and 100
fatalities.
Human anthrax is often associated with agricultural or
industrial workers who came in contact with infected
animal tissue.
In the 1950s and 1960s, over 80 percent of cases in the
United States were related to products that were
manufactured from imported goat hair. Inhalational
anthrax, or woolsorters' disease, follows the inhalation
of anthrax spores generated during the early cleaning
of contaminated goat hair.
During the 20th century, improvements in industrial
hygiene, a decrease in the use of imported,
contaminated animal materials, and immunization of
at-risk workers resulted in a reduction in the incidence
of inhalational anthrax (only 18 cases in the United
States)
In 2000, 32 farms in North Dakota in the United States
were quarantined because of anthrax: a total of 157
animals died during this epizootic and a single ranch
worker who helped move dead animals developed
cutaneous anthrax.
An outbreak of cutaneous anthrax occurred in
Bangladesh in 2009 after 40 cattle and goats became ill
with anthrax . Fifty-five people from two villages
developed cutaneous anthrax, all but two of whom had
a history of slaughtering sick animals, presence at the
slaughtering site, or handling raw meat from sick
animals.
There is no racial, sexual or age predilection for
anthrax. However, because anthrax is often related to
industrial exposure and farming, the disease most often
affects young and middle aged adults.
Persons of any age can of course be affected if anthrax
is used as a bioterrorist weapon.
Microbiology
Anthrax is caused by B. Anthracis which is a
Gram positive bacillus
diameter of 1-1.5µm
length of 3-10µm
usually straight but may be slightly curved
non motile
catalase positive
non haemolytic
forms a capsule and a spore
ground glass appearing colonies
gray or white colour on blood agar
Colonies measure 4-5mm in diameter and has a
comma shaped protrusions
Pathogenesis
Anthrax is primarily disease of the herbivores (goat,
cattle, sheep and horses)
Persistence of the spores is aided by nitrogen and
organic soil content, environmental PH greater than 6,
and ambient temperature great than 150c
Spores can exist indefinitely in the environment.
Optimal growth conditions result in a vegetative phase
and bacterial multiplication.
Drought or rainfall can trigger anthrax spore
germination while flies and vultures spread the spores.
Virulence depends on bacterial capsule and toxin
complex.
The capsule is a poly D glutamic acid that protects
against leukocyte phagocytosis.
Anthrax toxins are composed of 3 entities: a protective
antigen, a lethal factor and an oedema factor.
EF is a calmodulin-dependent adenyl cyclase that
causes edema when injected subcutaneously into
experimental animals . It also impairs host defences,
including inhibition of phagocytosis .
LF causes death through an unknown mechanism
when injected into susceptible animals. It is a zinc-
dependent protease that causes lysis of macrophages .
Neither EF nor LF is toxic alone; each produces
deleterious effects only when combined with PA to
become ET and LT, respectively; PA is so named
because it is antigenic and antibodies binding PA are
protective.
In a rat model, LT was 10 times more lethal than ET .
However, ET produced more hypotension than LT and
the combination of ET and LT had an additive effect
compared to LT alone.
Protective antigen — PA binds to a cell surface
receptor. After binding, a 20 kDa N-terminal fragment
(PA20) is proteolytically cleaved. The larger remaining
cell-bound fragment (PA63) has an exposed binding
site for either EF or LF.
In planar phospholipid bilayers, PA63 forms cation-
selective channels, suggesting that cleavage of PA20
permits insertion of PA63 as a true membrane-bound
protein with channel properties.
PA63-EF or PA63-LF can undergo receptor-mediated
endocytosis whereby EF and LF are translocated to the
cytosol. The host cell protein, low density lipoprotein
receptor-related protein 6 (LRP6), is required for
cellular uptake of complexes containing PA. LRP6
enables toxin internalization by interacting at the cell
surface with PA receptors to form a multi component
complex that enters cells upon PA binding.
Dissemination — When introduced subcutaneously,
spores of virulent B. anthracis become vegetative
organisms and begin to multiply. Subsequent
production of an antiphagocytic capsule facilitates
local spread and exotoxin production produces
extensive brawny edema and tissue necrosis, which are
the hallmarks of cutaneous anthrax.
The rapid growth of B. anthracis during infection
requires iron. The organism's mandatory iron
acquisition in an iron-scarce environment is promoted
by local production of iron chelators.
Airborne anthrax spores greater than 5 microns in size
pose no threat to the lung, since they are either
physically trapped in the nasopharynx or cleared by
the mucociliary escalator system .
However, spores between 2 and 5 microns in size are
deposited in alveolar ducts or alveoli. These spores are
phagocytosed by alveolar macrophages and
transported to mediastinal lymph nodes, where they
multiply and cause a hemorrhagic mediastinitis.
Gastrointestinal anthrax follows ingestion of grossly
contaminated and undercooked meat. Following
ingestion, anthrax bacilli are transported to mesenteric
lymph nodes. Subsequently, hemorrhagic mesenteric
adenitis, ascites, and septicemia may occur.
Overwhelming infection due to B. anthracis results in
rapid uncontrolled intravascular multiplication of
organisms and a fatal toxemia characterized by
hypotension and hemorrhage.
Cutaneous anthrax: humans are relatively resistant to
cutaneous invasion, but the organisms may gain access
through microscopic or gross breaks in the skin.
In cutaneous anthrax a malignant putules develope at
the infection site.
This pustule is a central area of coagulation
surrounded by a rim of vesicles filled with bloody or
clear fluid. A black eschar forms at the ulcer site and
extensive edema surrounds the lesions.
The organism multiply locally and may spread to the
bloodstream or other organs via the lymphatic.
Intestinal anthrax: primary intestinal anthrax
predominantly affects the cecum and produces a local
lesion.
Inhalational anthrax: inhalational anthrax occurs after
the person inhales spores into the lungs. Inhaled spores
are ingested by pulmonary macrophages and then
carried to hilar and midiastinal LN
The spores undergo germination and multiplication
and begins to elaborate toxins.
Anthrax in the lungs does not cause pneumonia but it
does cause hemorrhagic mediastinitis and pulmonary
oedema.
After the LN become overwhelmed bacteraemia and
death ensues.
With out treatment the mortality rate of inhalational
anthrax is approximately 95%
Clinical presentation
Cutaneous anthrax: develops 1-7 days usually 2-5 days
after skin exposure and penetration of B. Anthraxis
spores
In the most cutaneous form of anthrax, spores
inoculate a host through skin lacerations, aberations, or
biting flies.
This form most commonly affects the exposed areas of
the upper extremities, and to a lesser extent the head
and neck.
Begins as a pruritic papule that enlarges within 24-48
hrs to form a 1cm vesicle and subsequently becomes
an ulcer surrounded by an oedematous halo.
Lesions are usually approximately 2-3 cm in diameter
and have a round, regular, and raised edges
The skin in infected areas may become oedematous
and necrotic but not purulent.
Lesions are painless but on occasion are slightly
pruritic
Regional lymphadenopathy may occur and may be
painful.
The anthrax ulcer and surrounding edema evolve into
a black eschar within 7-10 days and last for 7-14 days
before leaving a permanent scar.
Oropharengeal anthrax: develops 2-7 days after
ingestion
Fever and neck swelling occur in the presence of an
oral cavity lesion
The lesions start as a edematous area that becomes
necrotic and forms a pseudomembrane within 2 weeks
Sore throat, dysphagia, respiratory distress, and oral
bleeding also occur
Soft tissue edema and dramatic cervical lymph node
enlargement follow
Intestinal anthrax: develop 2-5 days after ingestion
Abdominal pain and fever
Nausea, vomiting, malaise, anorexia, hematemesis,
bloody diarrhoea and shock
Inhalational anthrax: it begins abrubtly, usually 1-3
days after exposure and feollows a biphasic course
Initial manifestations include: myalgia, malaise,
fatigue, non productive cough, sensation of retrosternal
pressure, fever
Transient clinical improvment may occur after the first
few days, followed by rapid progression and clinical
detereoration in which the following signs and
symptoms may be present: high fever, sever SOB,
tachypnea, cyanosis, profuse diaphorosis,
hematemesis, chest pain, decreased level of
conciousness, coma and shock
DDX
Ecthyma
Glanders
Leprosy
Thyphoid
Meningitis
Mycoplasmal pneumonia
Superior vena cava syndrome
Viral pneumonia
Diagnosis
The diagnosis of cutaneous anthrax is usually
suggested by the characteristics appearance of skin
lesions. As spore germination occurs within the
macrophages at the site of inoculation, anthrax bacilli
are isolated easily from the vesicular lesion and can be
observed on gram stain.
In patients with inhalational anthrax a chest radiograph
typically shows widening of the mediastinum and
pleural effusions whereas the parenchyma may appear
normal.
The preferred diagnostic procedure for cutaneous
anthrax is gram stain.
B.anthracis grows on blood agar and staining
microbiologically differentiates the organism from
non- B.anthracis bacilli
For patients with prior antibiotic treatment bunch
biopsy at the edge of the lesion examined by silver
staining and immunohistochemical testing
Blood culture and gram stain(for patients with
systemic symptoms)
ELISA serology for B. Anthracis toxins
Chest radiography
Chest CT
Lumbar puncture(for patients with meningeal
symptoms)
Treatment
Cutaneous anthrax 7-14 days of out patient therapy
with oral doxycycline, or any quinolones
With doxycycline a loading regimen should be used
(200mgpo/iv every 12 hours for 72 hrs) in severely ill
patients it may be continued for the duration of therapy
For non bioterrorist inhalational anthrax and anthrax
meningitis the preferred drug is penicillin
Bioterrorist anthrax: any quinolone or doxycyclin for
1-2 weeks; clindamycin might be added for its anti
toxin effect
Post exposure prophylaxis- doxycycline or any
quinolone; continue for 60 days to prevent inhalational
anthrax
In patients with septic and hemorrhagic shock or
progressive respiratory insufficiencies ICU admission
might be needed.
In children levofloxacillin is safe
In pregnant women or those breast feeding can use
amoxacillin.
Prevention
Prevention of naturally-occurring anthrax in humans is
primarily dependent on the control of the disease in
animals, especially livestock. Animal vaccination is
the major means of preventing naturally-occurring
epizootics of anthrax, since widespread
decontamination of infected soil is impractical. Annual
vaccination of livestock in areas with enzootic anthrax
is recommended.
In the event of a naturally-occurring cutaneous
exposure, such as from handling an anthrax-affected
animal or its carcass, appropriate medical and public
health personnel should be notified and exposed
persons should be monitored for development of a
spot, pimple, or boil, especially in the exposed areas.
For naturally-occurring gastrointestinal exposure, such
as the consumption of meat from a poorly cooked
carcass of an anthrax-affected animal, antimicrobial
prophylaxis may be considered for a 7 to 14 day
period.
Antimicrobial choices are the same as those
recommended for PEP to prevent inhalation anthrax.
Vaccination is not recommended following either
naturally occurring cutaneous or gastrointestinal
exposure in which there is no risk of inhalation
exposure.
The United States Advisory Committee on
Immunization Practices (ACIP) recommends the
human anthrax vaccine , anthrax vaccine adsorbed
(AVA), for use prior to the occurrence of an event or
exposure, as well as for post-exposure prophylaxis for
inhalation anthrax in combination with antimicrobial
therapy.
THANK YOU
You might also like
- AnthraxDocument20 pagesAnthraxanemenyeeNo ratings yet
- Anthrax: A Deadly Disease Caused by Bacillus anthracisDocument40 pagesAnthrax: A Deadly Disease Caused by Bacillus anthracisFarrah Sayed100% (1)
- Malaria 25 03 09Document131 pagesMalaria 25 03 09Dr.Jagadish Nuchina100% (5)
- Malaria PowerpointDocument19 pagesMalaria PowerpointRhonaJadeNo ratings yet
- SPIROCHAETES & MYCOPLASMA: MORPHOLOGY AND PATHOGENESISDocument28 pagesSPIROCHAETES & MYCOPLASMA: MORPHOLOGY AND PATHOGENESISSarah PavuNo ratings yet
- Intestinal Helminthiasis and Filariasis - SGTDocument73 pagesIntestinal Helminthiasis and Filariasis - SGTLemathaNo ratings yet
- Gall Bladder & Cystic DuctDocument22 pagesGall Bladder & Cystic Ductsheethal prabhavanNo ratings yet
- Phylum Platyhelminthes (Flatworms) : Important InformationDocument26 pagesPhylum Platyhelminthes (Flatworms) : Important InformationYoussef EmadNo ratings yet
- LeishmaniaFilaria Part 1Document45 pagesLeishmaniaFilaria Part 1YS Nate100% (1)
- TaeniasisDocument23 pagesTaeniasisMardoni Efrijon33% (3)
- Bacterial and Fungal Phytase DifferenceDocument10 pagesBacterial and Fungal Phytase DifferenceRavi PachaiyappanNo ratings yet
- Medical Entomology: - Definition - History - Intro To Arthropods and Insects - Intro To Vector-Borne Disease ConceptsDocument58 pagesMedical Entomology: - Definition - History - Intro To Arthropods and Insects - Intro To Vector-Borne Disease ConceptsPipi Montok100% (1)
- Cestode SDocument38 pagesCestode SJang JangNo ratings yet
- Pathology of LiverDocument15 pagesPathology of Liverערין גבאריןNo ratings yet
- Entamoeba HistolyticaDocument18 pagesEntamoeba HistolyticaMayuri VohraNo ratings yet
- Rheumatoid Arthritis Module I ADocument22 pagesRheumatoid Arthritis Module I Apanks.79No ratings yet
- CANDIDIASISDocument20 pagesCANDIDIASISKylie GolindangNo ratings yet
- Malignant Oedema: - An Acute Infectious Disease Due To Wounds Caused by Clostridium SepticumDocument19 pagesMalignant Oedema: - An Acute Infectious Disease Due To Wounds Caused by Clostridium SepticumSantosh BhandariNo ratings yet
- Malaria Parasites and Their Life CyclesDocument66 pagesMalaria Parasites and Their Life CyclesDaxNo ratings yet
- Spirochetes: Aashutosh Nama M.SC Microbiology Sem - 1 Dr. B Lal Institute of BiotechnologyDocument34 pagesSpirochetes: Aashutosh Nama M.SC Microbiology Sem - 1 Dr. B Lal Institute of Biotechnologyaashutosh namaNo ratings yet
- Overview Q FeverDocument8 pagesOverview Q FeverAliyyahNo ratings yet
- The Leukotrienes: Chemistry and BiologyFrom EverandThe Leukotrienes: Chemistry and BiologyLawrence ChakrinNo ratings yet
- CestodesDocument82 pagesCestodesPaul Avila Soriano100% (1)
- Common Poultry DiseasesDocument15 pagesCommon Poultry DiseasesMamas IpunkNo ratings yet
- Term Paper ON: Correlation Between Rapid Test and Automated Methods in Diagnosing Infectious Disease Like TyphoidDocument22 pagesTerm Paper ON: Correlation Between Rapid Test and Automated Methods in Diagnosing Infectious Disease Like TyphoidSoniya DhyaniNo ratings yet
- Embolism and InfarctionDocument34 pagesEmbolism and InfarctionDiviya ArikrishnanNo ratings yet
- Japanese EncephalitisDocument10 pagesJapanese Encephalitiskiki0% (1)
- Brucellosis causes undulant fever in humansDocument5 pagesBrucellosis causes undulant fever in humansVenkatapradeepNo ratings yet
- PSM ProgrammesDocument45 pagesPSM ProgrammesBhuma DesaiNo ratings yet
- List of Zoonotic Diseases and Their ReservoirsDocument1 pageList of Zoonotic Diseases and Their ReservoirsHuyen J. DinhNo ratings yet
- Proceedings of the First International Congress of Parasitology: Roma, 21-26 September 1964From EverandProceedings of the First International Congress of Parasitology: Roma, 21-26 September 1964Augusto CorradettiNo ratings yet
- Myiasis and Strike: Dr. Thahsin Farjana Associate Professor Dept. of Parasitology BAUDocument33 pagesMyiasis and Strike: Dr. Thahsin Farjana Associate Professor Dept. of Parasitology BAUChuramoni Saha100% (1)
- Malaria KPTIDocument41 pagesMalaria KPTIRahmawati HamudiNo ratings yet
- Gangrene PowerpointDocument45 pagesGangrene PowerpointAsep DaniNo ratings yet
- PGDocument4 pagesPGDrHassan Ahmed ShaikhNo ratings yet
- Understanding Chlamydiae InfectionsDocument32 pagesUnderstanding Chlamydiae InfectionsNaing Lin SoeNo ratings yet
- ParasitologyDocument27 pagesParasitologySantosh BhandariNo ratings yet
- Blood Tissue and FlagellatesDocument15 pagesBlood Tissue and FlagellatesHughNo ratings yet
- Cysticercosis Diagnosis and TreatmentDocument18 pagesCysticercosis Diagnosis and TreatmentPhan Cảnh TrìnhNo ratings yet
- Canine BabesiosisDocument10 pagesCanine BabesiosisIonuț Gabriel ȚoleaNo ratings yet
- Brucellosis: A Highly Contagious Zoonotic DiseaseDocument55 pagesBrucellosis: A Highly Contagious Zoonotic Diseasesana shakeelNo ratings yet
- Trichuriasis: Disease Type: Parasitic Disease Common Name: Causative Agent: Species of Trichuris Disease DiscriptionDocument9 pagesTrichuriasis: Disease Type: Parasitic Disease Common Name: Causative Agent: Species of Trichuris Disease DiscriptionBrijesh Singh YadavNo ratings yet
- Intestinal NematodesDocument96 pagesIntestinal NematodesYeyeh Santos100% (1)
- Rabies: Dr. Amany Ahmed IbrahimDocument31 pagesRabies: Dr. Amany Ahmed IbrahimMohammed Abd ElfattahNo ratings yet
- Arboviruses: R.Varidianto Yudo T., Dr.,MkesDocument19 pagesArboviruses: R.Varidianto Yudo T., Dr.,MkesalbertmogNo ratings yet
- Family Abuse and Neglect HandoutDocument9 pagesFamily Abuse and Neglect Handoutapi-498295251No ratings yet
- Mycobacteria Slides For Lecture 2021Document70 pagesMycobacteria Slides For Lecture 2021wildoNo ratings yet
- Gram Positive Cocci Genera Staphylococci and Streptococci Medical ImportanceDocument40 pagesGram Positive Cocci Genera Staphylococci and Streptococci Medical ImportanceAshwani Mathur, Ma-306100% (1)
- Lecture Brucella 28-9-18Document58 pagesLecture Brucella 28-9-18Jayanthi TatineniNo ratings yet
- Arma in Ayurvedic LiteratureDocument5 pagesArma in Ayurvedic Literatureabha singhNo ratings yet
- MUMPS AND INFLUENZA: CAUSES, SYMPTOMS AND PREVENTIONDocument15 pagesMUMPS AND INFLUENZA: CAUSES, SYMPTOMS AND PREVENTIONNeethu Mariya MathewNo ratings yet
- Whipworm (Trichuris Trichiura)Document28 pagesWhipworm (Trichuris Trichiura)Anonymous HXLczq3No ratings yet
- Causes of Bleeding in Cows After OvulationDocument10 pagesCauses of Bleeding in Cows After OvulationmortezahNo ratings yet
- Hog cholera and other common swine diseasesDocument22 pagesHog cholera and other common swine diseasesJaneth PolinarNo ratings yet
- Endemic Diseases of Livestock Poultry NepalDocument67 pagesEndemic Diseases of Livestock Poultry NepalDr.Kedar KarkiNo ratings yet
- Abortions in Dairy Cows PDFDocument4 pagesAbortions in Dairy Cows PDFransinghNo ratings yet
- Malaria: A Guide to Causes, Symptoms and TreatmentDocument39 pagesMalaria: A Guide to Causes, Symptoms and TreatmentAulia Ratu PritariNo ratings yet
- Reproductive Diseases in Cattle: Brucellosis (Bang's Disease)Document4 pagesReproductive Diseases in Cattle: Brucellosis (Bang's Disease)Janice Li100% (1)
- Toxoplasma gondii: An Obligate ParasiteDocument7 pagesToxoplasma gondii: An Obligate ParasiteDedy SavradinataNo ratings yet
- StdsDocument71 pagesStdsabel semuNo ratings yet
- Elonnn MuuuuuskDocument27 pagesElonnn Muuuuuskabel semuNo ratings yet
- Elonnn MuuuuuskDocument27 pagesElonnn Muuuuuskabel semuNo ratings yet
- SyphilisDocument115 pagesSyphilisabel semuNo ratings yet
- Understanding Pertussis (Whooping Cough): Causes, Symptoms, TreatmentDocument63 pagesUnderstanding Pertussis (Whooping Cough): Causes, Symptoms, Treatmentabel semuNo ratings yet
- CholeraDocument59 pagesCholeraabel semuNo ratings yet
- Ethiopian TB 2008 PDFDocument207 pagesEthiopian TB 2008 PDFabel semuNo ratings yet
- MeningitisDocument80 pagesMeningitisabel semuNo ratings yet
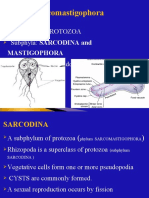
- Sarcomastigophora: A Phylum of PROTOZOA Subphyla: SARCODINA and Have Flagella or PseudopodiaDocument20 pagesSarcomastigophora: A Phylum of PROTOZOA Subphyla: SARCODINA and Have Flagella or Pseudopodiaabel semuNo ratings yet
- Giardia 5Document18 pagesGiardia 5abel semuNo ratings yet
- Toxo For 2Document13 pagesToxo For 2abel semuNo ratings yet
- Tissue Nematode Lect 4Document82 pagesTissue Nematode Lect 4abel semuNo ratings yet
- Study of These Parasitic Worms and Their Medical ConsequenceDocument33 pagesStudy of These Parasitic Worms and Their Medical Consequenceabel semuNo ratings yet
- Ethiopian Orthodox Church WebsiteDocument65 pagesEthiopian Orthodox Church Websiteabel semuNo ratings yet
- The Ethiopian Orthodox Tewahido Church Faith and OrderDocument8 pagesThe Ethiopian Orthodox Tewahido Church Faith and OrderSolomon EyayuNo ratings yet
- MF ISIN CodeDocument49 pagesMF ISIN CodeshriramNo ratings yet
- ISO 9000 Standards Guide Quality Systems InternationallyDocument12 pagesISO 9000 Standards Guide Quality Systems InternationallyArslan Saleem0% (1)
- OnScreen B2 Quiz 2ADocument2 pagesOnScreen B2 Quiz 2ALaura B.100% (1)
- First Preliminary Music Video ScriptDocument1 pageFirst Preliminary Music Video Scriptapi-455734096No ratings yet
- Lesson 2 - Procedures in Cleaning Utensils and EquipmentDocument26 pagesLesson 2 - Procedures in Cleaning Utensils and EquipmentReizel TulauanNo ratings yet
- Remove Fuel Sub TankDocument9 pagesRemove Fuel Sub Tankthierry.fifieldoutlook.comNo ratings yet
- Falling Weight Deflectometer (FWD) Projects in IndiaDocument13 pagesFalling Weight Deflectometer (FWD) Projects in IndiaKaran Dave100% (1)
- LC1D150M7: Product Data SheetDocument3 pagesLC1D150M7: Product Data SheetTrong Hung NguyenNo ratings yet
- Script of Cca Eim EditedDocument4 pagesScript of Cca Eim EditedMhen Maugan100% (1)
- Video Conferencing Lesson PlanDocument6 pagesVideo Conferencing Lesson PlanANN JILLIAN JOYCE MONDONEDO100% (1)
- Quiz - Limits and ContinuityDocument3 pagesQuiz - Limits and ContinuityAdamNo ratings yet
- Hatsun Supplier Registration RequestDocument4 pagesHatsun Supplier Registration Requestsan dipNo ratings yet
- Taco Bell - Re EngineeringDocument6 pagesTaco Bell - Re Engineeringabcxyz2811100% (6)
- CV Jubilee Bubala Environmental SpecialistDocument4 pagesCV Jubilee Bubala Environmental SpecialistNomayi100% (2)
- SAP ABAP Interview Questions and AnswersDocument8 pagesSAP ABAP Interview Questions and AnswersKarthi ThirumalaisamyNo ratings yet
- The Electricity Wiring RegulationDocument239 pagesThe Electricity Wiring Regulationgodson50% (2)
- 01 - Narmada M PhilDocument200 pages01 - Narmada M PhilafaceanNo ratings yet
- ALGEBRA Groups 1Document34 pagesALGEBRA Groups 1bravemacnyNo ratings yet
- 3ms Squence 3 (Summary)Document3 pages3ms Squence 3 (Summary)toumi khadidjaNo ratings yet
- Improve Product Packaging at Annual Board MeetingDocument9 pagesImprove Product Packaging at Annual Board Meetingizzat89% (9)
- F5 GTM Concepts Guide v11Document209 pagesF5 GTM Concepts Guide v11Majnu SmNo ratings yet
- PIRA - 2022 - ESTIMATED FMV As of October 2022Document48 pagesPIRA - 2022 - ESTIMATED FMV As of October 2022Aggy ReynadoNo ratings yet
- Understanding Income Statements EPS CalculationsDocument39 pagesUnderstanding Income Statements EPS CalculationsKeshav KaplushNo ratings yet
- E VTOLDocument12 pagesE VTOLsaikumar raviNo ratings yet
- Educ 580 - Edpuzzle PD HandoutDocument3 pagesEduc 580 - Edpuzzle PD Handoutapi-548868233No ratings yet
- 337 686 1 SMDocument8 pages337 686 1 SMK61 ĐOÀN HỒ GIA HUYNo ratings yet
- Vernacular Terms in Philippine ConstructionDocument3 pagesVernacular Terms in Philippine ConstructionFelix Albit Ogabang IiiNo ratings yet
- Staff Nurse HallticketDocument2 pagesStaff Nurse HallticketHiking DiaryNo ratings yet
- Omega 1 Akanksha 9069664Document5 pagesOmega 1 Akanksha 9069664Akanksha SarangiNo ratings yet
- Som-Ii Uqb 2019-20Document23 pagesSom-Ii Uqb 2019-20VENKATESH METHRINo ratings yet