Professional Documents
Culture Documents
Histology of The Female Reproductive System
Uploaded by
davidatuluku00 ratings0% found this document useful (0 votes)
5 views27 pagesHistology of the female repro
Original Title
Histology of the female reproductive system
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentHistology of the female repro
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views27 pagesHistology of The Female Reproductive System
Uploaded by
davidatuluku0Histology of the female repro
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 27
Histology of the female reproductive
system
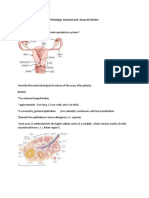
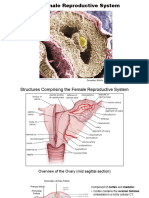
The female reproductive system comprises of the
ovaries, a system of genital ducts (the uterine tubes,
uterus and vagina) and the external genitalia.
The mammary glands are important glands of the
female reproductive system.
Ovaries
• The ovaries are paired organs covered by a
simple, usually cuboidal, mesothelium
(sometimes called germinal epithelium) and a
tunica albuginea (connective tissue).
• Each ovary is divided into a cortex and a
medulla. The cortex contains various stages of
follicles including primordial follicles, primary
follicles, secondary follicles and occasionally,
graafian follicles.
• It may also contain the corpus luteum, a
temporary endocrine gland formed by
components of an ovulated follicle. A
degenerated corpus luteum persist in the ovary
as the corpus albicans.
• Most follicles degenerate before ovulation and
are then called atretic follicles. The medulla
contains connective tissue with blood vessels,
nerve fibers and lymphatic vessels.
The ovary
Ovarian follicles
• Each ovarian follicle consists of an immature
ovum surrounded by epithelial cells. An
immature ovum is a spherical cell with a large
vesicular nucleus and a prominent nucleolus.
• The cytoplasm is opaque and finely granular.
In the newborn infant, the follicles are
believed to be numbered about 400,000. Their
number decreases progressively throughout
life until virtually none is left soon after the
menopause.
Primordial follicles
• They are the smallest and
most numerous type of
follicles in the cortex of the
ovary.
• Each primordial follicle
contains a germ cell (primary
oocyte) in a resting state that
may persist for as long as 50
years surrounded by a layer
of squamous cells called
follicular cells.
Primary follicles
• They develop from primordial follicles.
• Each primary follicle consists of a
primary oocyte and cuboidal follicle
cells which increase in height and their
cellular layers.
• At this stage, the follicle cells are called
granulosa cells because their cytoplasm
begins to have a granular appearance.
• Presence of zona pellucida between the
surface of the oocytes and the
surrounding granulosa cells.
• External to the granulosa cells are the
stroma cells that develop into a sheath
that surrounds the follicle called theca
folliculi.
Secondary follicles
• They develop from the continued growth
of the primary follicle.
• Spaces filled with follicular fluid appear
among the granulosa cells within the
secondary follicle. The spaces gradually
merge to form a single layer space called
the antrum.
• The theca folliculi develops into theca
interna and theca externa.
• The theca interna is the inner layer
containing cuboidal secretory cells which
secrete androgens which diffuse into the
granulosa cells where they are converted
into estrogens in response to FSH.
• The theca externa is an outer connective
tiisue layer containing mainly collagen and
some squamous cells mixed with a few
smooth muscle cells.
Graafian follicles
• It is a mature follicle; it is also called a preovulatory
follicle. At this stage, the follicle has grown to a
large size and bulges from the surface of the ovary.
The decreased number of granulosa cells and
increased volume of fluid in the antrum result in
the oocyte being located at the periphery of the
follicle.
• The membrana granulosa is formed by multiple
cellular layer of granulosa cells lining the inner wall
of the antrum. Some granulosa cells form a hillock
called the cumulus oophorus, which supports and
houses the oocyte.
• The inner granulosa cells of the cumulus oophorus
form a single layer called the corona radiata, which
immediately surrounds the oocyte. As the follicle
grows, most of the granulosa cells gradually loosen
from the cumulus oophorus, but the corona radiata
remains in contact with the oocyte.
• The oocyte remains as a primary oocyte in the
graafian follicle until pituitary secretion of LH
increases; this stimulates the primary oocyte to
complete the first meiotic division and become a
secondary oocyte.
• The secondary oocyte with the corona radiata and
polar body are released from the graafian foolicel of
the ovary.
• After the secondary oocyte reaches the ampulla of
the oviduct, the second meiotic division occurs, if
fertilization takes place.
• The ovarian cycle is under the control of the
hormones FSH and LH produced by the
gonadotrophs of the anterior pituitary gland. FSH
stimulates estrogen production and follicular
growth; LH stimulates meiotic division of the
primary oocyte, ovulation, and development of the
corpus luteum. The estrogens play an important
role in the stimulation of follicle growth by
promoting proliferation of the granulosa cells, and
they also stimulate the mammary glands to prepare
for lactation.
Graafian follicel
Corpus albicans
• In the absence of fertilization, the
corpus luteum is active only for a
short period of time. The corpus
luteum degenerates, decreases in
size and forms a structure called
the corpus albicans.
• The corpus albicans consists of
dense connective tissue that
appears as a white scar; it
gradually decreases in size and
remains in the ovary for months
to years.
Oviduct (fallopian tube)
• It is divided into four regions; the infundibulum,
ampulla, isthmus and intramural portion. The
infundibulum is a funnel-shaped opening that has
a fringe of tentacle-like extensions called fimbriae.
• The ampulla has a relatively large, labyrinthine
lumen where fertilization usually takes place. The
isthmus is a narrow portion of the oviduct, close
to the uterus. The intramural portion is the
terminal segment and is located within the
uterine wall.
• The wall of the oviduct consists of a (1.) mucosa
(simple columnar epithelium and lamina propria),
muscularis (inner circular and outer longitudinal
smooth muscle), and serosa.
• The epithelium of the oviduct contains ciliated cells
and peg cells. Ciliated cells help sweep the oocyte
toward the uterus. The peg cells are secretory cells
that produce nutrient-rich secretions to nourish
and protect the oocyte and promote fertilization.
• The oviduct provides an ideal environment for the
fertilization of the oocyte and initial development
of the embryo as well as transportation of the
zygote to the uterus.
oviduct
uterus
• It is the thick-walled segment of the
tubular female reproductive system
that is interposed between the
fallopian tube and the vagina.
• The wall of the uterus consists of the
following
(a) Endometrium: it is subject to cyclic
changes in response to ovarian
secretory activity.
(b) Myometrium: the middle
(muscular layer), which is a
massive coat of smooth muscle.
(c) Perimetrium: the outer serosa with
a single layer of mesothelial cells
supported by a thin layer of
connective tissue.
• The body of the uterus is lined by simple
columnar epithelium which possesses scattered
groups of ciliated cells. From the surface
epithelium, uterine glands extend through the
full thickness of the mucosa. These are simple
tubules, which may branch toward their basal
ends.
• They are separated from each other by
connective tissue, the stroma. Stromal cells are
irregular, stelllate cells, which have large, ovoid
nuclei. They lie in a framework of reticular fibres,
which are condensed beneath the epithelium to
form a basal lamina.
Cyclic changes in the endometrium
• PROLIFERATIVE
(FOLLICULAR) STAGE: it is
concurrent with follicular
growth and estrogen
secretion. The mucosa
increases in thickness from
1-2mm or more. Numerous
mitosis occur in cells of the
glands. The glands
proliferate, lengthen
rapidly, and become closely
packed.
Cyclic changes in the endometrium
THE PROGESTATIONAL (SECRETORY)
STAGE: usually associated with an
active corpus luteum. The mucosa
increases in thickness and
becomes 4mm or more in depth.
The increase is due largely to
hypertrophy of gland cells. the
glands swell and secrete profusely.
The secretion is thick and rich in
glycogen.
The glands become serrated and their
lumina become wider. Coiled
arteries grow nearly to the surface.
Cyclic changes in the endometrium
• THE MENSTRUAL STAGE:
the functional layer
undergoes necrosis and is
shed. The walls of the
vessels near the surface
break, and blood is added
to the secretion of the
glands and the necrotic
endometrial tissue. Patches
of tissue separate and are
lost.
Cyclic changes in the endometrium
THE ISCHEMIC (PREMENSTRUAL) STAGE: This
occurs 13 to 14 days after ovulation and is
characterized by extensive vascular changes.
The stroma increases in density and becomes
infiltrated with leukocytes.
cervix
• It is the lowest segment of the uterus.
The mucous membrane of the cervical
canal, which shows branching folds on
its surface comprises of an epithelium
and a lamina propria.
• The epithelium consists of tall, mucus-
secreting columnar cells. Some of the
cells are ciliated. Numerous large,
branching glands extend into the lamina
propria.
• The glands sometimes become
transformed into large cysts called
nabothian follicles.
• The lamina propria is a cellular
connective tissue, which contains no
coiled arteries.
cervix
• The portion of the cervix (endocervix) which
projects into the endometrial channel, is
covered by simple mucus-secreting columnar
cells. The portion of the cervix (exocervix) which
projects into the vagina, is covered by stratified
squamous non-keratinized epithelium.
vagina
• It is a fibromuscular sheath
lined with a mucous membrane.
The vagina has 3 coats:
• Mucosa: exhibits transverse
folds, or rugae. It is lined with
thick, stratified non-keratinized
squamous epithelium, it is
lubricated by mucus, which
originates from the cervix.
• Muscularis: is composed of
smooth muscle fibres, which are
arranged in interlacing bundles.
• Adventitia: is a thin layer of
dense connective tissue.
The external genital
• The clitoris: it consists of two cavernous, erectile bodies
which end in a rudimentary glands called clitoides. It is
covered with a thin, stratified squamous epithelium.
• The labia minora: they are fold of mucus membrane,
which form the lateral walls of the vestibule. They are
covered with a stratified squamous epithelium and have
also vascularized connective tissue.
• The labia majora: they are folds of skin that cover the
labia minor externally. The inner surface is smooth and
hairless. The outer surface is covered with cornified
epidermis which contains numerous hairs, sweat glands
and sebaceous glands.
The external genital
• The vestibuli: into which the vagina and
urethra open, is lined by a typical stratified
squamous epithelium and contains numerous
small glands, the minor vestibules glands
which are located mainly around the urethral
opening. The major vestibular glands (glands
of Bartholin) are located in the lateral walls of
the vestibule.
You might also like
- Vulvitis, Vaginitis, Bartholin's Cyst and CervicitisDocument56 pagesVulvitis, Vaginitis, Bartholin's Cyst and CervicitisSushma Thakuri100% (1)
- Heavy Menstrual BleedingDocument29 pagesHeavy Menstrual BleedingsanjupainNo ratings yet
- Histology of Female Reproductive System 2020Document45 pagesHistology of Female Reproductive System 2020Devina Kriskineya100% (2)
- Aesthetic Surgery of Female External GenitaliaDocument13 pagesAesthetic Surgery of Female External GenitaliaJavier Villalón Quiroz100% (1)
- INFERTILITYDocument48 pagesINFERTILITYAyisha EdwinNo ratings yet
- 1st Lecture On The Histology of Female Reproductive System by Dr. RoomiDocument17 pages1st Lecture On The Histology of Female Reproductive System by Dr. RoomiMudassar RoomiNo ratings yet
- Female ReproductiveDocument34 pagesFemale ReproductiveAbdallah A. Abu Mattar100% (2)
- Vaginal LubricationDocument3 pagesVaginal Lubricationnathan50% (2)
- Chapter 2 - Physiology of MenstruationDocument18 pagesChapter 2 - Physiology of Menstruationاسامة محمد السيد رمضان100% (1)
- Ob Final Exam Review Summary Maternity NursingDocument40 pagesOb Final Exam Review Summary Maternity NursingVin Lorenzo CampbellNo ratings yet
- 3rd Lecture On The Histology of Female Reproductive System by Dr. RoomiDocument19 pages3rd Lecture On The Histology of Female Reproductive System by Dr. RoomiMudassar RoomiNo ratings yet
- Female Reproductive HistologyDocument59 pagesFemale Reproductive HistologyIta Indriani100% (2)
- Female Reproductive System Histology IDocument5 pagesFemale Reproductive System Histology ISolomon Seth SallforsNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreYoAmoNYCNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreJSlinkNYNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- The Female Reproductive SystemDocument37 pagesThe Female Reproductive SystemAlexandra Duque-DavidNo ratings yet
- Female Reproductive System OverviewDocument56 pagesFemale Reproductive System OverviewAngelina BulaiNo ratings yet
- Ovary, Fallopian and Uterus - DR UgwuDocument38 pagesOvary, Fallopian and Uterus - DR UgwuJessy OnahNo ratings yet
- Histology of Female Reproductive SystemDocument11 pagesHistology of Female Reproductive SystemYoshua AdhisaktiNo ratings yet
- Lecturer: Abiib Ismail: Lecture: TwoDocument46 pagesLecturer: Abiib Ismail: Lecture: TwoAbdisamed AllaaleNo ratings yet
- The Female Reproduction SystemDocument9 pagesThe Female Reproduction Systemjhoanamariequilates182369No ratings yet
- Reproductive Cell, Organ, CycleDocument56 pagesReproductive Cell, Organ, CycleAjay MeghanathiNo ratings yet
- Histology of Female Reproductive SystemDocument35 pagesHistology of Female Reproductive SystemTeklemuz KahsayNo ratings yet
- Female Repro ReviwerDocument3 pagesFemale Repro ReviwerLincoln LunarNo ratings yet
- Lab SupplementDocument5 pagesLab SupplementcaterappleyeNo ratings yet
- Department of Zoology Govt Hss Mylachal: PresentsDocument69 pagesDepartment of Zoology Govt Hss Mylachal: PresentsBiju MylachalNo ratings yet
- Female Reproductive System HistologyDocument9 pagesFemale Reproductive System HistologyzaidNo ratings yet
- Histo Female ReproductiveDocument3 pagesHisto Female ReproductiveAkachukwu ObunikeNo ratings yet
- Female Reproductive SystemDocument6 pagesFemale Reproductive SystemAlyanna L. ArquillanoNo ratings yet
- Jawahar Navodaya Vidyalaya, Bolangir Biology Assingment Guided by - Swastitapa Kar Prepared by - Sujata Goud Class - Xii Section-A Roll No. - 16Document19 pagesJawahar Navodaya Vidyalaya, Bolangir Biology Assingment Guided by - Swastitapa Kar Prepared by - Sujata Goud Class - Xii Section-A Roll No. - 16preetamgoud225No ratings yet
- Female Reproductive SystemDocument15 pagesFemale Reproductive Systemada.codreanuNo ratings yet
- Female Reproductive HistologyDocument59 pagesFemale Reproductive HistologyCecilia Cabanag100% (1)
- Microscopic Features Of OvaryDocument14 pagesMicroscopic Features Of OvarysabaNo ratings yet
- 5.1 Female 2023 - JPDocument89 pages5.1 Female 2023 - JPtexasrepublican1976No ratings yet
- Female Reproductive SystemDocument11 pagesFemale Reproductive Systemراوند اعبيدNo ratings yet
- The Female Reproduction SystemDocument10 pagesThe Female Reproduction Systemrafaelvillacorta100% (1)
- Week 1 - 3 Placenta and Umbilical Cord: Group 4 MED 114 PresentationDocument69 pagesWeek 1 - 3 Placenta and Umbilical Cord: Group 4 MED 114 PresentationVidur S SinghNo ratings yet
- Histology of Female Reproductive SystemDocument31 pagesHistology of Female Reproductive SystemNo StradamusNo ratings yet
- Human Reproduction (Edustudy Point)Document10 pagesHuman Reproduction (Edustudy Point)Vishal UpadhyayNo ratings yet
- Female Genital Tract Basic HistologyDocument40 pagesFemale Genital Tract Basic HistologySantoshini RaviNo ratings yet
- Human Reproduction Class 12 NotesDocument21 pagesHuman Reproduction Class 12 NotesTamanna NayakNo ratings yet
- Female Reproductive System: Dr. Riaz Hussain PashaDocument25 pagesFemale Reproductive System: Dr. Riaz Hussain PashaTasbihaNo ratings yet
- ANA 222 Female Reproductive SystemDocument4 pagesANA 222 Female Reproductive SystemprincessmakklisNo ratings yet
- Female Reproductive Physiology 2021Document164 pagesFemale Reproductive Physiology 2021Elijah Kihiu18No ratings yet
- Fetal Membrane and PlacentaDocument77 pagesFetal Membrane and PlacentaIssa AvenaNo ratings yet
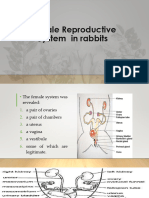
- Female Reproductive System in RabbitsDocument18 pagesFemale Reproductive System in RabbitsAMR WALIDNo ratings yet
- Embryonic Period For Medical StudentDocument43 pagesEmbryonic Period For Medical StudentMohan Prasad GuptaNo ratings yet
- Anatomy Structure and OvulatuonDocument51 pagesAnatomy Structure and OvulatuonDebajyoti DasNo ratings yet
- Lec 2Document37 pagesLec 2ibrahim.21hm32No ratings yet
- PlacentaDocument59 pagesPlacentaEdna Jenkins100% (9)
- K2 HS Female Reproductive SystemDocument80 pagesK2 HS Female Reproductive SystemMonika AyuningrumNo ratings yet
- Basic Steps in Human ReproductionDocument14 pagesBasic Steps in Human ReproductionMauz KhanNo ratings yet
- Human Reproduction: 3.1: Male Reproductive SystemDocument27 pagesHuman Reproduction: 3.1: Male Reproductive SystemAvik BhaumikNo ratings yet
- XX. Female Reproductive SystemDocument45 pagesXX. Female Reproductive SystemDale TelgenhoffNo ratings yet
- 2021.2 - Exam Q&ADocument203 pages2021.2 - Exam Q&ALucas Victor AlmeidaNo ratings yet
- Folluculogenesis and OogenesisDocument12 pagesFolluculogenesis and Oogenesisಮನೋಜ್ ಭಾರದ್ವಾಜ್No ratings yet
- Fetal and Embryonic DevelopmentDocument29 pagesFetal and Embryonic Developmentshan mackNo ratings yet
- 5.implantasi & PlasentasiDocument111 pages5.implantasi & PlasentasiherdhikaNo ratings yet
- Formation of Bilaminar Germ DiscsDocument32 pagesFormation of Bilaminar Germ DiscsVincent OkoroNo ratings yet
- Human ReproductionDocument21 pagesHuman ReproductionShazia KhatoonNo ratings yet
- Human ReproductionDocument96 pagesHuman Reproductionsanya razaNo ratings yet
- Female Reproductive Anatomy and Physiology: Ovaries, Uterine Tubes, Uterus, Menstrual CycleDocument60 pagesFemale Reproductive Anatomy and Physiology: Ovaries, Uterine Tubes, Uterus, Menstrual CycleTri JaraNo ratings yet
- Epithelium: Dr. Bhuvaneswari CDocument23 pagesEpithelium: Dr. Bhuvaneswari CAjinkya AravindNo ratings yet
- Cervical and Vaginal Agenesis - A Rare Case ReportDocument5 pagesCervical and Vaginal Agenesis - A Rare Case ReportEditor_IAIMNo ratings yet
- Physiology of ReproductionDocument34 pagesPhysiology of ReproductionCalcium QuèNo ratings yet
- Dig Deeper Into Menstrual ProductDocument12 pagesDig Deeper Into Menstrual ProductAnnisa NadhilaNo ratings yet
- Natural vs Artificial Contraception MethodsDocument26 pagesNatural vs Artificial Contraception MethodsCJ HernandezNo ratings yet
- Pemerksaan dan Penanganan Kanker ServiksDocument2 pagesPemerksaan dan Penanganan Kanker ServikseelNo ratings yet
- Birth Control ProjectDocument16 pagesBirth Control ProjectTishana Thompson100% (1)
- KD 3.1 Offers and Suggestions: B. You ShouldDocument5 pagesKD 3.1 Offers and Suggestions: B. You ShouldHanna Nur MeidanaNo ratings yet
- Human Reproductive System GuideDocument25 pagesHuman Reproductive System GuidePhoeberly SabadoNo ratings yet
- Heavy Menstrual Bleeding GuideDocument8 pagesHeavy Menstrual Bleeding GuideAtika Bashirati IlmanNo ratings yet
- Vaginal ExamDocument24 pagesVaginal ExamschxzerrydawnNo ratings yet
- A Large Multicenter Outcome Study of Female Genital Plastic SurgeryDocument13 pagesA Large Multicenter Outcome Study of Female Genital Plastic SurgeryJavier Villalón QuirozNo ratings yet
- Role of Hormons in PregnancyDocument8 pagesRole of Hormons in PregnancyMabila apriyaniNo ratings yet
- Bahan Vaginosis BakterialisDocument5 pagesBahan Vaginosis BakterialisAlzena AkbarNo ratings yet
- 15.1 Reproductive System of Humans 15.1.1 Characterise The Anatomy Of: (I) Male Reproductive System. Ii) Female Reproductive SystemDocument6 pages15.1 Reproductive System of Humans 15.1.1 Characterise The Anatomy Of: (I) Male Reproductive System. Ii) Female Reproductive SystemHi YelloNo ratings yet
- Poster Fer Kogi 18Document2 pagesPoster Fer Kogi 18wiwikNo ratings yet
- Anatomy & Physiology of Female Reproductive System: Dr. Aida Abd El-RazekDocument96 pagesAnatomy & Physiology of Female Reproductive System: Dr. Aida Abd El-RazekJennifer DixonNo ratings yet
- Vaginal BleedingDocument8 pagesVaginal BleedingMaria Monica Alcantara MedenillaNo ratings yet
- Organ Function Mons Veneris: Labia MinoraDocument5 pagesOrgan Function Mons Veneris: Labia MinoraSabana MedtimbangNo ratings yet
- Endometrial Hyperplasia 2Document70 pagesEndometrial Hyperplasia 2Melcah Marie NacionalesNo ratings yet
- COT2 Orig SCIENCE5 Semi Detailed Lesson PlanDocument4 pagesCOT2 Orig SCIENCE5 Semi Detailed Lesson PlanRaselle Alfonso PalisocNo ratings yet
- Menstrual CycleDocument8 pagesMenstrual Cyclejeni antonyNo ratings yet
- LRR Fmge ObgyDocument63 pagesLRR Fmge ObgyVishal KumarNo ratings yet
- Daftar Pustaka FamDocument4 pagesDaftar Pustaka FamayuannisahNo ratings yet