Professional Documents
Culture Documents
Ovary, Fallopian and Uterus - DR Ugwu
Uploaded by
Jessy Onah0 ratings0% found this document useful (0 votes)
0 views38 pagesThe document summarizes the key structures and functions of the female reproductive system including the ovary, fallopian tube, uterus, and endometrium. It describes the histological changes that occur in the ovary over the course of the menstrual cycle including the development of follicles and corpora lutea. It also outlines the roles of the fallopian tube in transporting eggs and the endometrium in preparing for potential implantation and shedding during menstruation.
Original Description:
Original Title
7. Ovary,Fallopian and Uterus- Dr Ugwu.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document summarizes the key structures and functions of the female reproductive system including the ovary, fallopian tube, uterus, and endometrium. It describes the histological changes that occur in the ovary over the course of the menstrual cycle including the development of follicles and corpora lutea. It also outlines the roles of the fallopian tube in transporting eggs and the endometrium in preparing for potential implantation and shedding during menstruation.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
0 views38 pagesOvary, Fallopian and Uterus - DR Ugwu
Uploaded by
Jessy OnahThe document summarizes the key structures and functions of the female reproductive system including the ovary, fallopian tube, uterus, and endometrium. It describes the histological changes that occur in the ovary over the course of the menstrual cycle including the development of follicles and corpora lutea. It also outlines the roles of the fallopian tube in transporting eggs and the endometrium in preparing for potential implantation and shedding during menstruation.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 38
Ovary,Fallopian Tube and Uterus
-Dr A.U Ugwu
• Introduction
• The female reproductive system may be divided into
three structural units on the basis of function:
• 1.Ovary. 2. Genital duct,and 3.Breast
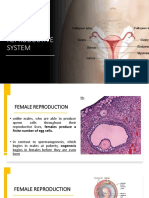
• The ovaries
• They are the site of oogenesis.
• Paired organs lying on either side of the uterus
adjacent to the lateral wall of the pelvis.
• In sexually mature mammals, ova are released, by the
process of ovulation.
• The ovaries are also endocrine organs producing
oestrogen and progesterone.
• The body of the ovary consists of;
• -spindle-shaped cells
• -fine collagen fibres, and
• -ground substance that together constitute the
ovarian stroma.
• The stromal cells resemble fibroblasts but some
contain lipid droplets.
• Bundles of smooth muscle cells are also scattered
throughout the stroma.
• In the peripheral zone of the stroma, known as the
cortex, are numerous follicles that contain female
gametes in various stages of development.
• In addition, there may also be post-ovulatory follicles of
various kinds, namely;
• -corpora lutea (responsible for oestrogen and
progesterone production)
• -corpora albicantes, and
• -atretic follicles.
• The superficial cortex is more fibrous than the deep
cortex and is often called the tunica albuginea.
• However, unlike the testis, this is not an anatomically
distinct capsule.
• On the surface of the ovary is an epithelial covering,
misleadingly called germinal epithelium, which is a
continuation of the peritoneum.
. In the inner part of the stroma is medulla,
which is;
-highly vascular, and
-contains hilus cells(which are
morphologically very similar to Leydig cells of
the testis).
• The ovarian artery (a branch of the aorta) and
ovarian branches of the uterine artery form
anastomoses in the mesovarium and the
broad ligament.
• From this arterial plexus approximately 10
coiled arteries, the helicine arteries enter the
hilum of the ovary.
• Smaller branches form a plexus at the
corticomedullary junction, giving rise to
straight cortical arterioles that radiate into the
cortex.
• Here they branch and anastomose to form
vascular arcades giving rise to a rich network
of capillaries around the follicles.
• Venous drainage follows the course of the
arterial system, the medullary veins being
large and tortuous.
• Lymphatics arise in the perifollicular stroma,
draining to larger vessels, which coil around
the medullary veins.
• Innervation of the ovary is by sympathetic
fibres that not only supply blood vessels but
also terminate on smooth muscle cells in the
perifollicular stroma, possibly playing some
part in follicular maturation and ovulation.
• Primodial follicle;
• 1. The primary oocyte has;
• - a large nucleus with dispersed fine granular chromatin
• -a prominent nucleolus, and
• -little cytoplasm.
• 2. Single Layer of flattened follicular cells
• primary follicle(unilaminar –Multilaminar);
• -its oocyte O1 has greatly enlarged and
• -the follicular cells F have multiplied by mitosis and
become cuboidal in shape;
-they are now known as granulosa cells.
• -A thick homogeneous layer of glycoprotein
and acid proteoglycans, the zona pellucida,
develops between the oocyte and the
follicular cells.
• Stromal cells begin to form theca folliculi
separated from the granulosa cells by a
basement membrane.
• granulosa cells continue to proliferate,
forming zona granulosa
• Secondary follicle
• At this stage they are usually situated deeper in the
ovarian cortex.
• At the periphery of the follicle, the theca folliculi has
developed two layers, the theca interna and theca
externa.
• The zona granulosa continues to proliferate and
within it small fluid-filled spaces appear;
• -these spaces fuse to form the follicular antrum , in
which follicular fluid accumulates.
• the oocyte has almost reached its full size and
becomes situated eccentrically in a thickened area of
the granulosa called the cumulus oophorus .
• Graafian follicle
• The follicular antrum enlarges markedly and
the zona granulosa now forms a layer of even
thickness around the periphery of the follicle.
• The cumulus oophorus diminishes leaving the
oocyte O2 surrounded by corona radiata,
which remains attached to the zona granulosa
by thin bridges of cells.
• Before ovulation, these bridges break down
and the oocyte, surrounded by the corona
radiata, floats free inside the follicle.
• Corpus luteum of menstruation
• Following ovulation, the ruptured follicle collapses
and fills with a blood clot to form the corpus
luteum of menstruation
• The granulosa cells acquire the characteristics of
steroid-secreting cells and are now called
granulosa lutein cells.
• These cells become known as theca lutein cells.
• Without the continuing stimulus of LH, the corpus
luteum cannot be maintained and 12-14 days
after ovulation it regresses, ultimately forming a
functionless corpus albicans
• Corpus luteum of pregnancy
• Implantation of a fertilised ovum in the uterine
wall interrupts the integrated ovarian and
menstrual cycles.
• After implantation, human chorionic
gonadotrophin (HCG) is secreted into the
maternal circulation by the developing placenta.
• HCG has an analogous function to LH and
maintains the function of the corpus luteum in
secreting oestrogen and progesterone until
about the 9th week of pregnancy.
There are some histological changes that are
almost specific for the corpus luteum of
pregnancy;
the granulosa lutein cells contain hyaline,
eosinophilic inclusion bodies that tend to
enlarge and then calcify as the pregnancy
progresses.
• Atretic follicles
• The process of follicular atresia (degeneration) may occur at
any stage in the development of the ovum.
• By the sixth month of development, the fetal ovary
contains several million primordial follicles, yet by the time
of birth only about half a million remain.
• Atresia continues until puberty and thereafter through the
reproductive years.
• In addition, with each ovarian cycle approximately 20
follicles begin to mature, usually all, except one, becomes
atretic at some stage before complete maturity.
• The histological appearance of atretic follicles varies
enormously, depending on the stage of development
reached and the progress of atresia.
• The atretic follicle of a secondary follicle in early atresia;
-the oocyte has degenerated and
-the granulosa cells have begun to disaggregate.
. Advanced atresia is characterised by;
- gross thickening of the basement membrane between
the granulosa cells, and the theca interna, forming the so-
called glassy membrane GM.
. Atretic follicles are ultimately replaced completely by
collagenous tissue known as the corpus fibrosum.
. Most corpora fibrosa eventually disappear completely.
. In the postmenopausal woman, primordial follicles are
absent and the cortex consists of stroma and corpora
albicantes only, with no developing follicles.
• Fallopian tube
• Movement of the ovum along the tube is mediated by
gentle peristaltic action of the longitudinal and
circular smooth muscle layers of the oviduct wall;
• this is aided by a current of fluid propelled by the
action of the ciliated epithelium lining the tube.
• Lined by simple ciliated columnar epithelium
• The mucosal lining of the Fallopian tube is thrown into
a longitudinal folds, a feature that is most prominent
in the ampulla, which is the usual site of fertilisation.
• The serosal layer and broad ligament have a surface
lining of mesothelium.
C-circular muscle fibers,L- Longitudinal,LP-
Lamina propria
• Endometrium:
• Mucosa of the uterus
• The major phases of the uterine cycle overlap, but
produce distinctly different and characteristic
changes in the functional layer with little effect on
the basal layer and myometrium .
• Premenstrual phase
• In the absence of implantation of a fertilised
ovum, degeneration of the corpus luteum results
in cessation of oestrogen and progesterone
secretion.
• In turn this initiates spasmodic constriction in
the spiral arterioles of the endometrial stratum
functionalis .
• The resulting ischaemia is initially manifest by
degeneration of the superficial layers of the
endometrium and leakage of blood into the
stroma.
• Stromal cells disaggregate and the endometrial
glands collapse.
• These features are indicative of early necrosis
of glands and stroma.
• Further ischaemia leads to degeneration of the whole
stratum functionalis, which is progressively shed as
menses.
• Menses is thus composed of blood, necrotic
epithelium and stroma.
• Endometrial surface
• the surface epithelium of the endometrium is tall
simple columnar in form.
• Some of the cells bear cilia, the remainder having
surface microvilli.
• The stroma of the peripheral functionalis is more
compact and that near the basal layer typically
appears more sponge-like during this time of blood
G- Gland,A-Artery,B- Basal Layer, M-
Myometrum
• Proliferative endometrium Early phase:
• During most of the proliferative phase;
• -The functional layer is still relatively thin
• -the stroma is more cellular, and
• -the glands (G) are relatively straight, narrow,
and empty.
F-functional layer,L- lumen,Basal layer,M-
Myometrium
G- gland,
• Secretory endometrium :
• -Ovulation marks the onset of the secretory phase.
• In the secretory phase;
• -functional layer is about four times thicker than the
basal layer.
• -the stroma is less heavily cellular
• The glands is tubular, have wider lumens containing
secretory product, and coil tightly up through the stroma,
giving a zig-zag or folded appearance histologically.
• Superficially in the functional layer, lacunae are
widespread and filled with blood.
LA- LACUNAR
• Postmenopausal endometrium
• After the menopause, the cyclical production
of oestrogen and progesterone from the
ovaries ceases and the whole genital tract
undergoes atrophic changes.
• -the endometrium is thin, consisting only of
the stratum basalis,
• -the glands are sparse and inactive.
-In some women the glands become dilated to
form cystic spaces ;
-the glandular epithelial cells are cuboidal or
low columnar with no mitotic figures or
secretory activity.
-The epithelium which lines cystically dilated
glands, is often flattened.
-The stroma is much less cellular and contains
more collagen fibres than during the
reproductive years
-The myometrium also becomes atrophic after
the menopause and the uterus shrinks to
about half its former size.
• Myometrium
• The main bulk of the uterus consists of smooth muscle,
the myometrium, which is composed;
• Muscle fibres are arramged in transverse , longitudinal ,
and oblique sections .
• Within the muscle is a rich network of arteries and veins
supported by collagenous supporting tissue.
• During pregnancy, in response to increased levels of
oestrogens, the myometrium undergoes hypertrophy,
with some hyperplasia.
• At parturition, strong contractions of the myometrium
are reinforced by the action of the hormone oxytocin
secreted by the posterior pituitary.
• These contractions expel the fetus from the
uterus and also constrict the blood supply to
the placenta, thus precipitating its detachment
from the uterine wall.
• Uterine cervix
• -the endocervical canal is lined by a single layer
of columnar mucus-secreting epithelial cells.
• Where the cervix is exposed to the more hostile
environment of the vagina, the ectocervix, it is
lined by thick stratified squamous epithelium
as in the vagina and the vulva.
• The junction J between the ecto- and endocervical
epithelium is quite abrupt and is normally located
at the external os, the point at which the
endocervical canal opens into the vagina.
• The main bulk of the cervix is composed of tough,
collagenous tissue containing a little smooth
muscle.
• At the squamocolumnar junction, the cervical
stroma is often infiltrated with leucocytes forming
part of the defence against ingress of
microorganisms.
EC- ENDOCERVIX,SS- STRATIFIED COLUMNAR
EPITH, J- ABRUPT JUNCTION,V - Vagina
Thank you
You might also like
- Histology of The Female Reproductive SystemDocument27 pagesHistology of The Female Reproductive Systemdavidatuluku0No ratings yet
- The Female Reproductive SystemDocument37 pagesThe Female Reproductive SystemAlexandra Duque-DavidNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreYoAmoNYCNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument38 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreJSlinkNYNo ratings yet
- Femalereprod (Author T.globa)Document56 pagesFemalereprod (Author T.globa)Angelina BulaiNo ratings yet
- 1st Lecture On The Histology of Female Reproductive System by Dr. RoomiDocument17 pages1st Lecture On The Histology of Female Reproductive System by Dr. RoomiMudassar RoomiNo ratings yet
- Reproductive Cell, Organ, CycleDocument56 pagesReproductive Cell, Organ, CycleAjay MeghanathiNo ratings yet
- Lecturer: Abiib Ismail: Lecture: TwoDocument46 pagesLecturer: Abiib Ismail: Lecture: TwoAbdisamed AllaaleNo ratings yet
- Female Genital Tract Basic HistologyDocument40 pagesFemale Genital Tract Basic HistologySantoshini RaviNo ratings yet
- Histology of Female Reproductive SystemDocument31 pagesHistology of Female Reproductive SystemNo StradamusNo ratings yet
- Anatomy Practicals NotesDocument209 pagesAnatomy Practicals NotesSaloni SaloniNo ratings yet
- Cleavage, Blastocyte Formation and ImplantationDocument23 pagesCleavage, Blastocyte Formation and Implantationobianujuonyeka6No ratings yet
- Embryonic Period For Medical StudentDocument43 pagesEmbryonic Period For Medical StudentMohan Prasad GuptaNo ratings yet
- Histology-Female Compatibility ModeDocument14 pagesHistology-Female Compatibility ModeZeina Nazih Bou DiabNo ratings yet
- Female Reproductive System: Dr. Riaz Hussain PashaDocument25 pagesFemale Reproductive System: Dr. Riaz Hussain PashaTasbihaNo ratings yet
- Week 1 - 3 Placenta and Umbilical Cord: Group 4 MED 114 PresentationDocument69 pagesWeek 1 - 3 Placenta and Umbilical Cord: Group 4 MED 114 PresentationVidur S SinghNo ratings yet
- Formation of Bilaminar Germ DiscsDocument32 pagesFormation of Bilaminar Germ DiscsVincent OkoroNo ratings yet
- Lab SupplementDocument5 pagesLab SupplementcaterappleyeNo ratings yet
- Fertilization and First of DevDocument69 pagesFertilization and First of DevUti SolomonNo ratings yet
- K2 HS Female Reproductive SystemDocument80 pagesK2 HS Female Reproductive SystemMonika AyuningrumNo ratings yet
- 7 GametogenesisDocument35 pages7 GametogenesisBlè SsìngsNo ratings yet
- Ana 213 Full Slide..Dr Bien.Document221 pagesAna 213 Full Slide..Dr Bien.ewoozino1234No ratings yet
- 5.1 Female 2023 - JPDocument89 pages5.1 Female 2023 - JPtexasrepublican1976No ratings yet
- Histo FemDocument9 pagesHisto FemzaidNo ratings yet
- EM2.Gametogenesis (At)Document52 pagesEM2.Gametogenesis (At)MUDIN ABDELLANo ratings yet
- DR - Anangwe-First Week of DevepmentDocument27 pagesDR - Anangwe-First Week of DevepmentStanley OdiraNo ratings yet
- Formation of Bilaminar Germ DiscsDocument32 pagesFormation of Bilaminar Germ DiscsStanley OdiraNo ratings yet
- Histology of Female Reproductive System 2020Document45 pagesHistology of Female Reproductive System 2020Devina Kriskineya100% (2)
- XX. Female Reproductive SystemDocument45 pagesXX. Female Reproductive SystemDale TelgenhoffNo ratings yet
- PlacentaDocument59 pagesPlacentaEdna Jenkins100% (9)
- Lec 2Document37 pagesLec 2ibrahim.21hm32No ratings yet
- Folluculogenesis and OogenesisDocument12 pagesFolluculogenesis and Oogenesisಮನೋಜ್ ಭಾರದ್ವಾಜ್No ratings yet
- Female Repro ReviwerDocument3 pagesFemale Repro ReviwerLincoln LunarNo ratings yet
- Fetal and Embryonic DevelopmentDocument29 pagesFetal and Embryonic Developmentshan mackNo ratings yet
- 5.implantasi & PlasentasiDocument111 pages5.implantasi & PlasentasiherdhikaNo ratings yet
- Anatomy Structure and OvulatuonDocument51 pagesAnatomy Structure and OvulatuonDebajyoti DasNo ratings yet
- FEMALEDocument60 pagesFEMALETri JaraNo ratings yet
- Gametogenesis:: DR KibeDocument46 pagesGametogenesis:: DR KibeDenis KaguiNo ratings yet
- PlacentaDocument59 pagesPlacentaSulis 'Hp' Kartowidjojo100% (1)
- DR Mohtaseb Slide 8 Embryology 3Document17 pagesDR Mohtaseb Slide 8 Embryology 3api-249972919No ratings yet
- Placenta and Fetal Membrane-6614Document45 pagesPlacenta and Fetal Membrane-6614Incredible DivineNo ratings yet
- Female Reproductive HistologyDocument59 pagesFemale Reproductive HistologyCecilia Cabanag100% (1)
- Female Genital System PDFDocument61 pagesFemale Genital System PDFWaleed AbdelallNo ratings yet
- MensesDocument68 pagesMensesdominicamarigu100% (1)
- Male Reproduction System - Histology LectureDocument28 pagesMale Reproduction System - Histology LectureAstri Novia RizqiNo ratings yet
- Histology of Female Reproductive SystemDocument11 pagesHistology of Female Reproductive SystemYoshua AdhisaktiNo ratings yet
- Fertilization 151008151928 Lva1 App6892Document27 pagesFertilization 151008151928 Lva1 App6892subiNo ratings yet
- Female Reproductive SystemDocument15 pagesFemale Reproductive Systemada.codreanuNo ratings yet
- Human ReproductionDocument21 pagesHuman ReproductionShazia KhatoonNo ratings yet
- PlacentaDocument36 pagesPlacentaAbdullah HussainyNo ratings yet
- Histology of Female Genital System For Reproductive ModuleDocument35 pagesHistology of Female Genital System For Reproductive ModuleTeklemuz KahsayNo ratings yet
- Human Reproduction (Edustudy Point)Document10 pagesHuman Reproduction (Edustudy Point)Vishal UpadhyayNo ratings yet
- Histology of Female Reproductive System: A P Dr. G M Kibria UPNM-2 25.03.13Document43 pagesHistology of Female Reproductive System: A P Dr. G M Kibria UPNM-2 25.03.13AaronMaroonFiveNo ratings yet
- Anat 213, Placentation-EmbryologyDocument16 pagesAnat 213, Placentation-EmbryologyChidera EmmanuelNo ratings yet
- 2-Anatomy of The PelvisDocument29 pages2-Anatomy of The PelvisdanielNo ratings yet
- COBAS 6000: E601 Reagent Inventory MONTH/YEARDocument2 pagesCOBAS 6000: E601 Reagent Inventory MONTH/YEARCharmaine Corpuz GranilNo ratings yet
- Herbal Drugs For The Treatment of Polycystic Ovary Syndrome (Pcos) and Its ComplicationsDocument9 pagesHerbal Drugs For The Treatment of Polycystic Ovary Syndrome (Pcos) and Its ComplicationsDoc MailNo ratings yet
- ABORTION RIGHTS - Wagmi SharmaDocument19 pagesABORTION RIGHTS - Wagmi SharmawagmiNo ratings yet
- CSA Revision Notes: For TheDocument37 pagesCSA Revision Notes: For TheOphthalmology PLUSNo ratings yet
- 107 Family PlanningDocument69 pages107 Family PlanningRiegne Chiara Fay AcuzarNo ratings yet
- Small and Sick Newborn Care DuringDocument11 pagesSmall and Sick Newborn Care DuringmeritabasrilNo ratings yet
- HIV Infection Fact SheetDocument38 pagesHIV Infection Fact SheetYu Mong LeeNo ratings yet
- Introduction To Pelvic Pain 2019Document20 pagesIntroduction To Pelvic Pain 2019MrEnttNo ratings yet
- The Endocrine System and Glands of The Human BodyDocument2 pagesThe Endocrine System and Glands of The Human BodyFungo JasmineNo ratings yet
- Journal Analysis-BALLON, Karlo CDocument4 pagesJournal Analysis-BALLON, Karlo CMelinda Cariño BallonNo ratings yet
- JIPMER - Final Submission - Revised MRMBSDocument145 pagesJIPMER - Final Submission - Revised MRMBSMuraleedharan V R IITMNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakamumutdwsNo ratings yet
- Read The Full Decision From The Supreme CourtDocument213 pagesRead The Full Decision From The Supreme CourtNewsdayNo ratings yet
- Nursing Case Study ApaleDocument14 pagesNursing Case Study ApaleAna LuisaNo ratings yet
- Steroids AND TerpenesDocument88 pagesSteroids AND Terpenesbuttercuplady_18763No ratings yet
- Nursing Care of Client During Labor and Delivery 1Document8 pagesNursing Care of Client During Labor and Delivery 1Arcel SasaluyaNo ratings yet
- CH 14 Antepartum Nursing Assessment NotesDocument8 pagesCH 14 Antepartum Nursing Assessment NotesMary LowryNo ratings yet
- Gangguan Haid - PPT YudisDocument34 pagesGangguan Haid - PPT YudisIde Yudis TiyoNo ratings yet
- BORJA Genetics Lab Exercise 6 Multiple Alleles and ABO Blood Groups in HumansDocument5 pagesBORJA Genetics Lab Exercise 6 Multiple Alleles and ABO Blood Groups in Humansbry uyNo ratings yet
- Delivery of CH ServicesDocument39 pagesDelivery of CH ServicesAnand gowdaNo ratings yet
- Teachers InterviewDocument1 pageTeachers InterviewCamilo ChaparroNo ratings yet
- Module 5 Health PromotionDocument59 pagesModule 5 Health PromotionZaren James D. RacaNo ratings yet
- Stephen Munjanja ZMPMS Short Report FVDocument42 pagesStephen Munjanja ZMPMS Short Report FVClamore Solar - ProjectsNo ratings yet
- Rundown RS IslamDocument2 pagesRundown RS IslamDeviyanti AuliaNo ratings yet
- Obstetric and Newborn Care IDocument184 pagesObstetric and Newborn Care ISabrina SarpongNo ratings yet
- Evidence Based Fertility Investigations Final 2018 2Document43 pagesEvidence Based Fertility Investigations Final 2018 2Sagie NaiduNo ratings yet
- Epidural Analgesia in Labour Management and CareDocument29 pagesEpidural Analgesia in Labour Management and CareMihai IoanNo ratings yet
- Managementtoimproveneonatepigletsurvival Oliviero 2013Document8 pagesManagementtoimproveneonatepigletsurvival Oliviero 2013Eduardo ViolaNo ratings yet
- Ten Teacher Single Best .AnswerDocument4 pagesTen Teacher Single Best .Answera7332773No ratings yet
- Pengaruh Persiapan Gentle Birth Terhadap Derajat Kecemasan Ibu Hamil Pertama Dalam Menghadapi PersalinanDocument7 pagesPengaruh Persiapan Gentle Birth Terhadap Derajat Kecemasan Ibu Hamil Pertama Dalam Menghadapi PersalinanIis MarifahNo ratings yet