Professional Documents
Culture Documents
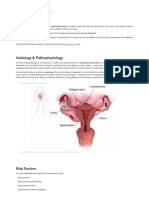
ENDOMETRIOSIS
ENDOMETRIOSIS
Uploaded by
Christian PasicolanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ENDOMETRIOSIS
ENDOMETRIOSIS
Uploaded by
Christian PasicolanCopyright:
Available Formats
ENDOMETRIOSIS
Is the presence and growth of the plands and stroma of the lining of the uterus in an aberrant or heterotropic location
A benign but progressive disease which frustrated pynecologists, fascinated pathologists, and burdened patients for years
The prevalence in the general female population is suggested to be 6% to 10%
Diagnosed incidently during surgery performed for a variety of other indications
The prevalence of active endometritis is approximately 33% in women with chronic pelvic pain
The incidence of endometriosis is 30% to 45% in women with infertility
5% of women with endometriosis are diagnosed following menopause
The typical patient with endometriosis is in her mid-30s, is nulliparous and involuntarily infertile, and has symptoms of secondary
dysmenorrheal and pelvic pain
Retrograde menstruation, vascular dissemination, metaplasia, genetic predisposition, immunologic changes, and hormonal influences,
environmental factors
Retrograde menstruation
Pelvic endometriosis was secondary to implantation of endometrial cells shed during menstruation
These cells attach to the pelvic peritoneum and i\under hormonal influence grow as homologous grafts
Endometriosis is frequently found in women with outflow obstruction of the genital tract
The attachment of the shed endometrial cells involves the expression of adhesion molecules and their receptors
Metaplasia
Endometriosis arises from metaplasia of the coelomic epithelium or proliferation of embryonic rests
The mullerian duct is derived from the coelomic epithelium during fetal development
It postulates that the surface epithelium of the ovary can differentiate into several different histologic cell types
Lymphatic and vascular metastasis
Endometriosis has been observed in the pelvic lymph nodes of approximately 30% of women
Hematogenous dissemination of the endometrium explains endometriosis of the forearm, thigh and multiple lesions in the lung
Iatrogenic dissemination
Endometrial glands and stroma are implanted during the performance of cesarean section ezplains endometriosis found in the
subcutaneous tissue at the anterior abdominal wall after cesarean delivery
Rarely, iatrogenic endometriosis may be discovered in an episiotomy scar
Immunologic changes
Abnormalities in cell-mediated humoral components of the immune system in both peripheral blood and peritoneal fluid involves an
alteration in the function of the peritoneal macrophages prevalent in the peritoneal cavity
Women who do not devlop endometriosis have monocytic-type macrophages in their peritoneal fluid that have a short life span and
limited function
These hyperactive cells secrete multiple growth factors and cytokines that enhance the development of endometriosis
The attraction of leukocytes to specific areas is controlled by chemokines, which are chemotactic cytokines
Endometriosis epithelial cells called endo1 is a chemoattractant protein which enhanced local production of interleukin-6 (IL-6)
Compounding the proliferative activity of endometriosis lesions are angiogenic factors such as basic fibroblast factor, IL-6, IL-8, platelet-
derived growth factor (PGDF), and vascular endothelial growth factor (VEGF) are all increased
Steroid interactions also enhance the progression of disease
Enhanced aromatose activity which is a result of overexpression of the orphan nuclear receptor steroidogenic factor-1 (SF-1) in lesions
explains why progression of lesions may occur even with ovarian suppression
Genetic predisposition
Increased heterogenecity of chromosome 17 and aneuploidy, in women with endometriosis
Women who have a family history of endometriosis are likely to develop the disease earlier in life and to have more advanced disease
than women whose first-degree relatives are free of the disease
7x increase incidence of endometriosis in relatives
1/10 with severe endometriosis will have sister or mother with symptoms
Increased heterogenecity of chromosome 17 & aneuploidy
Pathology
Common sites Rare sites
Ovaries Umbilicus
GYNECOLOGY – ENDOMETRIOSIS Page 1
pelvic peritoneum Episiotomy scar
Ligaments of the uterus Bladder
Pelvic lymph nodes – 30% Kidney
Rectosigmoid – 10-15% Lungs
Appendix Arms and legs
Vagina Nasal mucosa
Cervix Spinal column
Fallopian tubes
Terminology used to describe peritoneal endometriosis
Powder burn, puckered black lesions
Vascularized glandular papules
Vesicular lesions
Red, flamelike
Petechiae peritoneum
Discolored areas
Deep penetrating lesions, >5mm, are more progressive form of the disease
Approximately 10%-15% of women with advanced disease have lesions involving the rectosigmoid
Can be found in umbilicus, areas of previous surgical incisions of the anterior abdominal wall or perineum, bladder, ureter, kidney, lung,
arms, legs, and even the male urinary tract
Gross pathologic changes of endometriosis exhibit wide variability in color, shape, sixe, and associated inflammatory and fobrotic changes
The gross appearance of the implant depends on the site, activity, relationship to the day of the menstrual cycle, and chronicity of the
area involved
The color of the lesion variea widely and may be red, brown, black, white, yellow, pink, clear, or a red visicle
The predominant color depends on the blood supply and the amount of hemorrhage and fibrosis
The color is also related to the size of the lesion, degree of edema, and the amount of inspissated material
Small, bleblike implants that are raised above the surrounding tissues <1cm in dm are new lesions
Red, blood-filled lesions are the most active phase of the disease
The areas of endometriosis become larger and assume a light or dark brown color, and they may be described as “powder burn” areas or
“chocolate cysts”
The older lesions are white, have more intense scarring, and usually puckered or retracted form the surrounding tissue
White or mixed colored lesions are more likely to provide histologic confirmation of endomeriosis
The progression from red to white lesions also seems to correlate with age
Individual areas range from 1mm to large chocolate cysts >8cm in dm
The associate adhesions may be minimal or extensive, filmy or dense, and avascular or vascular
Larger cysts are usually densely adherent to the surrounding pelvic sidewalls or broad ligament
3 cardinal histologic features of endometriosis
Ectopic endometrial glands
Ectopic endometrial stroma
Hemorrhage into the adjacent tissue
The ectopic endometrial stroma undergo classic decidual changes similar to pregnancy when exposed to high physiologic or
pharmacologic levels of progesterone
ENDOMETRIOSIS: a disease of clinical contrast
Characteristics Contrasts
Benign disease Locally invasive
Widespread disseminated foci
Proliferates in pelvic lymph nodes
Minimal disease Severe pain
Many large endometriomas Asymptomatic patient
Cyclic hormones cause growth Continuous hormones reverse the growth pattern
CLINICAL DIAGNOSIS
Symptoms:
- Cyclic pelvic pain
o Usually presents as secondary dysmenorrheal or dyspareunia (or both)
o Related to the sequential swelling and the extravasation of blood and menstrual debris into the surrounding tissue
GYNECOLOGY – ENDOMETRIOSIS Page 2
o Chemical mediators of this intense sterile inflammation and pain are believed to be prostaglandins and cytokines
- Infertility
- Secondary dysmenorrhea
o Usually begins 36 to 48 hours prior to the onset of menses
o Varies from a dull ache to severe pelvic pain
o May be unilateral or bilateral radiating to the lower back, legs, and groin
o Pelvic heaviness or a perception of their internal organs being swollen
o Pain may last for many days, including several days before and after the menstrual flow
- Dyspareunia
o Described as pain deep in the pelvis cause by immobility of the pelvic organs during coital activity or direct pressure on areas of
endometriosis in the uterosacral ligaments or the cul-de-sac
o Acute pain may continue for several hours following intercourse
- Abnormal bleeding
o Noted by 15% to 20% of women with endometriosis
o Most frequent complaints: premenstrual spotting and menorrhagia
o Usually it is not associated with an anovulatory pattern
o But, approximately 15% of women with endometriosis have coincidental anovulation
- Approximately one third of patients with endometriosis are asymptomatic
- Patients with only a few small foci with deep infiltration may experience moderate to severe chronic pain
- Less common yet troublesome are the symptoms resulting from endometriosis influencing the gastrointestinal and urinary tracts
o Cyclic abdominal pain
o Intermittent constipation
o Diarrhea
o Dyschezia
o Urinary frequency
o Dysuria
o Hematuria
o Bowel obstruction
o Hydronephrosis
Signs
Classic signs:
- Fixed, retroverted uterus with scarring and tenderness at the posterior
- Nodularity of uterosacral ligament and cul de sac
o May be palpated on rectovaginal examination in approximately one third of women with the disease
- Ovaries may be enlarged and tender
o And are often fixed to the broad ligament or lateral pelvic sidewall
o Adnexal enlargement is rarely symmetrical
o Bilateral ovarian endometriomas were observed in 28%
o 63% of unilateral endometriomas were found in the left ovary
- Advanced cases have extensive scarring and narrowing of the posterior vaginal fornix
- Speculum examination may demonstrate small areas of endometriosis on the cervix or upper vagina
- Lateral displacement or deviation of the cervix is visualized or palpated by digital exam of the vagina and cervix in approximately 15% of
women with moderate or severe endometriosis
Diagnostics
- Transvaginal ultrasound
- CT scan or MRI
- CA 125
- Laparoscopy
MANAGEMENT
Two primary short term goals
Relief of pain
Promotion of fertility
Primary long term goal
Prevent progression or recurrence of disease
GYNECOLOGY – ENDOMETRIOSIS Page 3
Choice of therapy, depends on multiple variables, including the patient’s age, her future reproductive plans, the location and extent of her
disease, the severity of her symptoms, and associated pelvic pathology
Most patients should undergo a diagnostic evaluation, such as diagnostic laparoscopy to establish the nature and extent of endometriosis
before embarking on prolonged therapy
Medical Therapy
Induction of amenorrhea
o The primary goal of hormonal treatment
Recurrent bleeding in the ectopic implants is one of the most important pathophysiologic processes to interrupt
The choice of medical therapy depends on the clinician’s evaluation of adverse effects, side effects, cost of therapy, and expected patient
compliance
Recurrence rate: 5-15% in 5 yrs
40-50% in 5 yrs
1. NSAIDS – 1st line
2. Danazol
Hypoestrogenic and hyperandrogenic
Dosage: 400-800 mg/d for 6 months
MOA: binds to androgen and progesterone receptors and sex hormone-binding globulin
Adverse reactions
o Menopausal hot flushes
o Atrophic vaginitis
o Emotional lability
o Weight gain
o Fluid retention
o Migraine headaches
o Deepening of voice
3. GnRH agonists
Leuprolide acetate (Lupron, injectable)
o 3.75 mg intramuscularly once/month or 11.25 mg depot injection q 3 months
Nafarelin acetate (Synerel, intranasal)
o One spray (200 mg) in one nostril in the morning and one spray (200 mg) in the other nostril in the
evening up to a maximum of 800 mg daily
Goserelin acetate (Zoladex, subcutaneous implant)
o 3.6 mg q 28 days in a biodegradable subcutaneous implant
Chronic use ------ “medical oopherectomy”
No effect on sex-hormone binding globulin
Side effects: hot flushes, vaginal dryness and insomnia
Advantage: better patient compliance
Add back hormone replacement therapy
o Dosages similar to menopausal therapy in combination with GNRH agonist regimen
Reduce or eliminate side effects
4. Oral contraceptive
Single monophasic OCP for 6-12 months
“pseudopregnancy”
Others:
o Medroxyprogesterone 30 mg/d
o Depomedroxyprogesterone 150 mg IM q 3 months
To produce amenorrhea
Low-estrogen monophasic combination pills, with a relatively high progestin potency
Continous daily oral contraceptives for 6-12 months
Beginning on the 3rd day of the patient’s period
Treatment
o Medical
o Surgical
Conservative surgery
GYNECOLOGY – ENDOMETRIOSIS Page 4
resection or destruction of endometrial of implants, lysis of adhesion, and attempts to restore normal pelvic
anatomy
Definitive surgery
Removal of both arteries, the uterus, and all visible ectopic foci of endometriosis
A combination of both
Surgical therapy
Mandatory:
o Acute rupture endometriosis
o Urethral obstruction
o Compromise bowel’s function
o Endometriosis >2cm or adnexal enlargement >8cm
Conservative:
o Resection or destruction of endometrial implants, adhesiolysis and restoration of normal anatomy
Definitive:
o THBSO
ADENOMYOSIS
Endometriosis interna
Growth of endometrial glands and stroma into the myometrium to a depth of 2.5 mm from the basalis layer
Pathogenesis:
o Barrier between the endometrium and myometrium is broken
Two distinct pathologic presentation
o Diffuse adenomyosis
The most common, involvement of both anterior and posterior walls of the uterus
Posterior wall is usually involved more than the anterior wall
Not encapsulated
2/3 cases
o Focal area or ademyoma
Results in an asymmetrical uterus, and this special area of adenomyosis may have a pseudocapsule
Cut surface protrudes convexly nand has a spongy appearance
Diagnosis: finding of endometrial glands and stroma more than one low-powered field (2.5 mm) from the basalis layer of the
endometrium
Histologically the glands exhibit an inactive or proliferative pattern
Manifestations:
o Asymptomatic
o Parous, more than 35 y/o
o Symptoms: secondary dysmenorrheal & menorrhea
o Sign: diffusely enlarges uterus, 2-3x normal size
Diagnosis: usually confirmed following histologic examination of the hysterectomy specimen
Management:
o GnRH agonists
o Cyclic hormones
o Prostaglandin inhibitors
o Hysterectomy; Bilateral oopherectomy
Definitive treatment if this therapy is appropriate for the woman’s age, parity, and plans for future reproduction
GYNECOLOGY – ENDOMETRIOSIS Page 5
You might also like
- Work OFWDocument33 pagesWork OFWMark Stephen TabbayNo ratings yet
- The Kegel Legacy-Print Version 1308Document100 pagesThe Kegel Legacy-Print Version 1308teju2812No ratings yet
- Associate Professor:Ivan Bonet. Obstetric and Gynecology Associate Professor:Ivan Bonet. Obstetric and GynecologyDocument31 pagesAssociate Professor:Ivan Bonet. Obstetric and Gynecology Associate Professor:Ivan Bonet. Obstetric and Gynecologyivan0% (1)
- Uterine Fibroids & EndometriosisDocument82 pagesUterine Fibroids & EndometriosisDuncan Jackson67% (3)
- Ok Ok Notes PediaDocument14 pagesOk Ok Notes PediaChristian PasicolanNo ratings yet
- Abc Abuso 1 PDFDocument6 pagesAbc Abuso 1 PDFMDMNo ratings yet
- Are Traditional Midwives History ? පාරම්පරික වින්නඹු මාතාවන් ඉතිහාසයට එක්වේ ද? பாரம்பாpய மருத்துவ மாதா;கள் வரலாற்றில் இடம்பெறுவார்களா?Document98 pagesAre Traditional Midwives History ? පාරම්පරික වින්නඹු මාතාවන් ඉතිහාසයට එක්වේ ද? பாரம்பாpய மருத்துவ மாதா;கள் வரலாற்றில் இடம்பெறுவார்களா?wmcsrilanka100% (1)
- Endometriosis: OccurrenceDocument6 pagesEndometriosis: Occurrencewea xczNo ratings yet
- EndometriosisDocument50 pagesEndometriosisHannah Eloise MagsinoNo ratings yet
- 1 GYNE 7 - EndometriosisDocument6 pages1 GYNE 7 - EndometriosisIrene FranzNo ratings yet
- Endometri Osis: Par Khmermedical StudyDocument18 pagesEndometri Osis: Par Khmermedical StudyLeang KarichakNo ratings yet
- En DoDocument8 pagesEn DoJair EnriquezNo ratings yet
- Endometriosis Adenomyosis Dr-IrabonDocument67 pagesEndometriosis Adenomyosis Dr-IrabonAbegail IbañezNo ratings yet
- Kocakoc 2008Document16 pagesKocakoc 20087dc2s9tdrwNo ratings yet
- EndometriosisDocument15 pagesEndometriosispalohe1277No ratings yet
- Endometriosis and AdenomyosisDocument49 pagesEndometriosis and AdenomyosisOmar HamwiNo ratings yet
- Department of Prasuti Tantra and Striroga Dayanand Ayurvedic College, Jalandhar SESSION 2016-17Document40 pagesDepartment of Prasuti Tantra and Striroga Dayanand Ayurvedic College, Jalandhar SESSION 2016-17jyothiNo ratings yet
- Endometriosis Is A Common Disease in Women of Reproductive Age and IsDocument45 pagesEndometriosis Is A Common Disease in Women of Reproductive Age and IsSreekanth reddyNo ratings yet
- GYNE 4.01a EndometriosisDocument4 pagesGYNE 4.01a EndometriosisGray SnellNo ratings yet
- Endometriosis and Adenomycosis - CaramelMacchiatoDocument6 pagesEndometriosis and Adenomycosis - CaramelMacchiatoJanelle MatamorosaNo ratings yet
- Fournier'S Gangrene: Rajah Amina SuleimanDocument27 pagesFournier'S Gangrene: Rajah Amina SuleimanAmina RajahNo ratings yet
- Endometrial Histology Till Poly 05-04-2020 Y4 PathologyDocument67 pagesEndometrial Histology Till Poly 05-04-2020 Y4 PathologyMuhammad Qaisar karimNo ratings yet
- Die 1Document18 pagesDie 1juan carlos pradaNo ratings yet
- Womb Gynecological Endometrial Cells Uterine Cavity: Endometriosis (From Endo, "Inside", and Metra, "Document3 pagesWomb Gynecological Endometrial Cells Uterine Cavity: Endometriosis (From Endo, "Inside", and Metra, "remyavarghese25No ratings yet
- Endometriosis - Pathogenesis, Clinical Features, and Diagnosis - UpToDateDocument39 pagesEndometriosis - Pathogenesis, Clinical Features, and Diagnosis - UpToDatefujimeisterNo ratings yet
- Endometriosis - Pathogenesis, Clinical Features, and Diagnosis - UpToDateDocument42 pagesEndometriosis - Pathogenesis, Clinical Features, and Diagnosis - UpToDateOrlando GuerraNo ratings yet
- EndometriosisDocument46 pagesEndometriosisManoj Ranadive0% (1)
- EndometriosisDocument7 pagesEndometriosisIsabel CastilloNo ratings yet
- Mohammed Kashif Group:6 YEAR:4Document19 pagesMohammed Kashif Group:6 YEAR:4anu1643No ratings yet
- Presentation 1Document20 pagesPresentation 1Mohamad HafyfyNo ratings yet
- EndometriosisDocument11 pagesEndometriosisKevin de SilvaNo ratings yet
- Endometriosis - Clinical Features - Diangosis - TeachMeObGynDocument3 pagesEndometriosis - Clinical Features - Diangosis - TeachMeObGynLiridon SopajNo ratings yet
- Endometriosis & AdenomyosisDocument41 pagesEndometriosis & AdenomyosisAzim Syahmi Abd RazakNo ratings yet
- DR Sankalpa R WankhedeDocument76 pagesDR Sankalpa R Wankhedechaitanya suryawanshiNo ratings yet
- Dyspareunia A Difficult Symptom in Gynaecological Practice 2015 Obstetrics Gynaecology Reproductive MedicineDocument6 pagesDyspareunia A Difficult Symptom in Gynaecological Practice 2015 Obstetrics Gynaecology Reproductive MedicineNoraNo ratings yet
- EndometriosisDocument5 pagesEndometriosisLok100% (2)
- EndometriomaDocument7 pagesEndometriomaErick Rafael AncaNo ratings yet
- Pelvic Pain - Sundhed - DKDocument11 pagesPelvic Pain - Sundhed - DKPavel BerlinschiNo ratings yet
- Endometriosis Team 3 DidacticsDocument80 pagesEndometriosis Team 3 DidacticsAbegail IbañezNo ratings yet
- EndometriosisDocument10 pagesEndometriosisSivaram Shanmugha VilasNo ratings yet
- TTEA BrochureDocument2 pagesTTEA BrochureSteve MaximayNo ratings yet
- Endometriosis An Ayurvedic ViewDocument7 pagesEndometriosis An Ayurvedic ViewroykibetNo ratings yet
- AdenomyosisDocument0 pagesAdenomyosisWildan FirmansyahNo ratings yet
- Prognosis For EndometriosisDocument4 pagesPrognosis For Endometriosisirithel markasNo ratings yet
- Endometriosis: Pathogenesis, Clinical Features, and Diagnosis - UpToDateDocument41 pagesEndometriosis: Pathogenesis, Clinical Features, and Diagnosis - UpToDateRafael Vilano AvelarNo ratings yet
- ENDOMETRIOSISDocument17 pagesENDOMETRIOSISPeterson Wachira HscNo ratings yet
- Bab I Pendahuluan 1.1 Latar Belakang MasalahDocument15 pagesBab I Pendahuluan 1.1 Latar Belakang MasalahNidar RaniNo ratings yet
- Endometriosis NotesDocument6 pagesEndometriosis Notesangee 88No ratings yet
- Endometriosis PresentationDocument58 pagesEndometriosis PresentationBRI KUNo ratings yet
- Endometriosis Boletin PracticoDocument14 pagesEndometriosis Boletin PracticoNoreenPalenciaNo ratings yet
- EndometrisisDocument10 pagesEndometrisisAmmarNo ratings yet
- EndometriosisDocument37 pagesEndometriosislovelots1234No ratings yet
- Infert F - Endometriosis PDFDocument10 pagesInfert F - Endometriosis PDFJuan Sebastián ElcanoNo ratings yet
- EndometriosisDocument4 pagesEndometriosisAno DzamelashviliNo ratings yet
- Endometriosis O&g PresentationDocument31 pagesEndometriosis O&g PresentationChauthiran Agamudaiyar100% (1)
- Deep Infiltrating Endometriosis: Symptoms and Diagnostic Procedures. The Symptoms As Well As Clinical FindingsDocument5 pagesDeep Infiltrating Endometriosis: Symptoms and Diagnostic Procedures. The Symptoms As Well As Clinical FindingsBunga JuwitaNo ratings yet
- 2.1gyne Endometriosis PDFDocument9 pages2.1gyne Endometriosis PDFFAtty ACidsNo ratings yet
- Keperwatan DasarDocument14 pagesKeperwatan DasarAdiva LidiyaNo ratings yet
- Penatalaksanaan EndometriosisDocument11 pagesPenatalaksanaan EndometriosisAna Yuli RistantiNo ratings yet
- ENDOMETRIOSISsDocument27 pagesENDOMETRIOSISsNouman HameedNo ratings yet
- Endometriosis ReviewDocument9 pagesEndometriosis ReviewYudha Adi Pradana DjatioetomoNo ratings yet
- Endometriosis: Menstruation Seems To Play A Major Role in The Pathogenesis of EndometriosisDocument6 pagesEndometriosis: Menstruation Seems To Play A Major Role in The Pathogenesis of EndometriosisJason FooNo ratings yet
- Jurnal EndometriosisDocument17 pagesJurnal Endometriosisiduy cantikNo ratings yet
- Lec 4 Platelet and CoagulationDocument17 pagesLec 4 Platelet and CoagulationChristian PasicolanNo ratings yet
- AMENORRHEADocument6 pagesAMENORRHEAChristian PasicolanNo ratings yet
- Physics of RadiologyDocument9 pagesPhysics of RadiologyChristian PasicolanNo ratings yet
- 2019 PPMP and App-Non Cse FormDocument8 pages2019 PPMP and App-Non Cse FormChristian PasicolanNo ratings yet
- Pediatrics Tckler-3 PDFDocument100 pagesPediatrics Tckler-3 PDFChristian PasicolanNo ratings yet
- Pedia OncoDocument8 pagesPedia OncoChristian PasicolanNo ratings yet
- Narag, MarkDocument64 pagesNarag, MarkChristian PasicolanNo ratings yet
- Pedia Tickler Cont 20190210175903 PDFDocument80 pagesPedia Tickler Cont 20190210175903 PDFChristian PasicolanNo ratings yet
- LeukemiaDocument33 pagesLeukemiaChristian PasicolanNo ratings yet
- Cagayan Valley Medical Center Carig Sur, Tuguegarao City CagayanDocument8 pagesCagayan Valley Medical Center Carig Sur, Tuguegarao City CagayanChristian PasicolanNo ratings yet
- Cagayan State University - College of Information TechnologyDocument26 pagesCagayan State University - College of Information TechnologyChristian Pasicolan50% (2)
- Pola Reproduksi Burung Tekukur Streptope b272cd07Document9 pagesPola Reproduksi Burung Tekukur Streptope b272cd07Candratama Indar SeptiantoNo ratings yet
- Pregnancy and Birth GlossaryDocument6 pagesPregnancy and Birth GlossaryVanda Love D'javaneisNo ratings yet
- PsychologyDocument102 pagesPsychologyJac FloresNo ratings yet
- Contraceptive Choice Project Reducing Barriers Long Acting Reversible Contraceptives PDFDocument7 pagesContraceptive Choice Project Reducing Barriers Long Acting Reversible Contraceptives PDFDeviNo ratings yet
- Health Indicators FormulasDocument2 pagesHealth Indicators Formulaskristinetan21No ratings yet
- Youth Questionnaire CurecDocument20 pagesYouth Questionnaire CurecwdejanesNo ratings yet
- O&G OSCE by MaddyDocument287 pagesO&G OSCE by MaddyNariska Cooper100% (1)
- Polycystic Ovary Syndrome: Di WenDocument17 pagesPolycystic Ovary Syndrome: Di WenSalam AlmudarrisNo ratings yet
- Consumer BehaviorDocument23 pagesConsumer Behaviorshivam goelNo ratings yet
- Illegalization of Abortion in The PhilippinesDocument2 pagesIllegalization of Abortion in The PhilippinesLele Scherzeigler100% (1)
- Material Downloaded From SUPERCOPDocument10 pagesMaterial Downloaded From SUPERCOPkritika0% (1)
- Abortion Laws in AmericaDocument7 pagesAbortion Laws in AmericaBinoy SinhaNo ratings yet
- MCN PartographDocument2 pagesMCN PartographAlec AnonNo ratings yet
- ANC CASE (Revised)Document32 pagesANC CASE (Revised)Mike RossNo ratings yet
- Cattle Embryo Transfer Procedure PDFDocument135 pagesCattle Embryo Transfer Procedure PDFFadli NugrahaNo ratings yet
- OB Gyne HistoryDocument2 pagesOB Gyne HistoryNeil Victor Ongco PajugotNo ratings yet
- Committee Opinion: Weight Gain During PregnancyDocument3 pagesCommittee Opinion: Weight Gain During PregnancyRomi SNo ratings yet
- Document 0730 PMDocument9 pagesDocument 0730 PMMelissa Aina Mohd YusofNo ratings yet
- Coitus ReservatusDocument4 pagesCoitus ReservatusTrà Thanh NguyễnNo ratings yet
- HiiDocument19 pagesHiiTruptimayiGiriNo ratings yet
- OB JC Case of Hydatidiform MoleDocument37 pagesOB JC Case of Hydatidiform MoleBlykeBantugan100% (2)
- Men's Erotic FantasiesDocument17 pagesMen's Erotic Fantasiesanatole7No ratings yet
- Veterinary Helminthology MidtermsDocument4 pagesVeterinary Helminthology Midtermshumanupgrade100% (1)
- Practice Bulletin No 171 Summary Management Of.52 (ACOGDocument3 pagesPractice Bulletin No 171 Summary Management Of.52 (ACOGgeraldi radityaNo ratings yet
- Cardiac Disease in PregnancyDocument12 pagesCardiac Disease in Pregnancydynea100% (1)
- DEV2011 2015 Week 3 Lecture Review Questions STUDENTDocument3 pagesDEV2011 2015 Week 3 Lecture Review Questions STUDENTZoom Zoom ZoomNo ratings yet