Professional Documents
Culture Documents
Gastrointestinal Pathology Guide
Uploaded by
Karl ChavezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Gastrointestinal Pathology Guide
Uploaded by
Karl ChavezCopyright:
Available Formats
SURGICAL PATHOLOGY
1.01 Gastrointestinal Pathology P1
September 9, 2020 | Dr. Arnel Bayotas
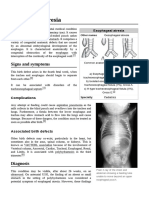
OUTLINE Type C - Esophageal atresia with distal
I. Congenital Anomalies esophageal fistula (most common: 86%)
A. Atresia, Fistula & Duplication Type D (blind pouch)
B. Ompalocele & Gastrochisis Type E - No esophageal atresia with double
C. Meckel’s Diverticulum tracheoesophageal fistula (proximal and
II. Esophagus
distal) H type
A. Esophageal Diverticulum
B. Esophageal Mucosal webs
C. Esophageal Rings
D. Achalasia
E. Hiatal Hernia
F. Reflux Esophagitis/GERD
G. Barret Esophagus
H. Squamous Cell Carcinoma of the Esophagus
I. Adenocarcinoma of the Esophagus
III. Stomach
A. Pyloric Stenosis
B. Gastritis Figure 1. Esophageal atresia & tracheoesophageal fistula
C. Stress-Related Mucosal Disease
D. Peptic Ulcer Disease IMPERFORATED ANUS
E. Gastric Malignancies o Most common form of congenital intestinal
IV. Small Intestine
atresia
A. Neoplasm
B. Inflammatory Bowel Disease o Due to failure of the cloacal diaphragm to
C. Intestinal Obstruction involute
V. Large Intestine o Treatment: (purely surgical)
A. Neoplasm Perineal anoplasty
B. Sigmoid Diverticular Disease
C. Hirchsprung Disease
Colostomy and pull-through operation
VI. Small/Large Bowel Polyps
B. OMPHALOCELE (EXOMPHALOS) & GASTROSCHISIS
A. Hyperplastic
B. Inflammatory (LAPAROSCHISIS)
C. Hamartomatous
Table 1. Opmpalocele vs. Gastrochisis
D. Neoplastic
E. Adenomatous Polyposis Omphalocele Gastroschisis
I. CONGENITAL ANOMALIES
A. ATRESIA, FISTULA AND DUPLICATION
May occur in any part of the GI tract
Agenesis - absence of organ
ATRESIA
o A condition in which a body orifice or passage in
the body is abnormally closed or absent
o Occurs most commonly at or near the tracheal Incomplete closure of the abdominal musculature and the
bifurcation (esophagus) abdominal viscera herniates
o Usually associated with a fistula connecting the Has a ventral membranous No ventral membranous
upper and lower esophageal pouches to a sac sac (Allowing evisceration
bronchus or the trachea of bowel loops, stomach
o Atresia can occur without fistula and sometimes the
FISTULA gonads)
o An abnormal connection or passageway Does not involve all layers of Involves all the layers of
between two epithelium-lines organs or vessels the abdominal wall the abdominal wall (from
that normally do not connect peritoneum to the skin)
o 2 types of fistula:
Fistula with atresia Associated with Small (generally <5 cm)
Fistula without atresia chromosomal defects: defect of the abdominal
o Most common: Tracheoesophageal Fistula Trisomies 13 (Patau), 18 wall just to the right of the
o 5 types of TEF (Edward) & 21 (Down) and umbilical cord insertion.
Type A - Isolated esophageal atresia (pure with other disorders such as
atresia) Beckwith-wiedemann (Prevalence: 1 in 10,000
Type B - Esophageal atresia with proximal syndrome live births)
tracheoesophageal fistula
Transcribers Damian, Ng, Perez, Santos 1 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Can be encountered also in Attributed to fibrosis, esp. in the
other cardiac anomalies mediastinum.
(ASD, VSD) Lined by stratified squamous
epithelium non-keratinized.
C. MECKEL DIVERTICULUM Epiphrenic Immediately above the lower
Due to failed involution of vitelline duct esophageal sphincter
Located in the ileum Transition of stratified squamous
Solitary; anti-mesenteric side of bowel epithelium non-keratinized and
Most common true diverticulum columnar.
Rule of 2’s:
o 2 % of population
o Within 2 feet of ileocecal valve
o Approximately 2 inches long
o 2x as common in males
o Usually symptomatic by the age of 2 years old
Figure 2a & 2b. Meckel’s diverticulum (gross & micro)
Same histology with normal wall, only difference is the outpouching Figure 3. Esophageal diverticula based on location
II. ESOPHAGUS B. ESOPHAGEAL MUCOSAL WEBS
A. ESOPHAGEAL DIVERTICULUM Idiopathic, ledge-like protrusions (semi-
circumferential) of mucosa that may cause
TRUE DIVERTICULUM
obstruction.
o Traction (True = Traction)
Most common in Upper Esophagus
o Due to inflammation
o Outpouching of alimentary tract lined by mucosa Main symptom: nonprogressive dysphagia associated
o Communicates with the lumen with incompletely chewed food.
o Contain all 3 layers of the wall Paterson-Brown-Kelly or Plummer-Vinson
FALSE DIVERTICULUM Syndrome:
o Pulsion (Pulsion = False yun) ○ Webs
o Due to defect in associated sphincter muscles ○ Iron-deficiency anemia
o Diverticula wall lacks muscle layer ○ Glossitis
○ Cheilosis
Table 2. Esophageal diverticula based on location
C. ESOPHAGEAL RINGS/ SCHATZKI RINGS
Zenker Immediately above the upper
(Pharyngo- esophageal sphincter aka lower esophageal esophago-gastric rings
esophageal) Impaired relaxation and spasm of the Similar to webs, but are circumferential, thicker
cricopharyngeus muscle after Include mucosa, submucosa, and ocassionally,
swallowing → ↑ pressure within the hypertrophic muscularis propria
A rings – Present in the distal esophagus, above the
distal pharynx → Zenker
gastroesophageal junction
Lined by stratified squamous
B rings – Present at the squamocolumnar junction of
epithelium non-keratinized
the lower esophagus and may have gastric cardia-
Small → asymptomatic type mucosa
Large → mass, regurgitation &
halitosis
Traction lower third of the esophagus
(region of the hilum of the lungs)
Involves the 3 layers of the
esophagus
Transcribers Damian, Ng, Perez, Santos 2 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
E. HIATAL HERNIA
Characterized by separation of the diaphragmatic
crura and protrusion of the stomach into the thorax
through the resulting gap
Figure 4. Esophageal Rings
D. ACHALASIA Figure 6. Types of Hiatal Hernia
aka Cardiospasm or Megaesophagus
Pathogenesis: Unknown Treatment: Nissen fundoplication
Characterized by dysmotility and inability of the LES
to relax after swallowing. F. REFLUX ESOPHAGITIS/ GERD
Due to complete loss of the myenteric ganglion cells
Reflux of gastric contents into the lower
Failure of the cardiac mechanism to open when
esophagus → called gastroesophageal reflux
peristaltic waves conveying food through the
disease (GERD)
esophagus reach it
o Due to conditions that increase abdominal
Progressive dysphagia starting in teens
pressure or decrease lower esophageal
Primary Achalasia
o Nearly complete loss of ganglionic cells in the sphincter tone
Auerbach’s plexus in the lower 3rd of the Most common cause of GERD → transient lower
esophagus esophageal sphincter relaxation.
Secondary Causes o Mediated via vagal pathways, and can be
o Chagas Disease triggered by gastric distention, by gas or food,
Trypanosoma cruzi infection causes mild pharyngeal stimulation that does not trigger
destruction of the myenteric plexus, failure swallowing, and stress.
of peristalsis and esophageal dilatation Can also occur following swallow-induced LES
o Varicella Zoster Infection relaxations or due to forceful opening of a relatively
Achalasia Triad hypotensive lower esophageal sphincter by an abrupt
o Aperistalsis increase in intraabdominal pressure, such as that due
o Incomplete relaxation of the LES to coughing, training, or bending.
o Increased LES tone
Risk factors
Barium Swallow
o Alcohol and tobacco use
o Dilated, aperistaltic esophagus with a beak-like
o Obesity
tapering at distal end
o Central nervous system depressants
o Pregnancy
o Hiatal hernia
o Delayed gastric emptying
o Increased gastric volume.
24 hours pH study - gold standard for diagnosis.
Morphology
o Mild GERD → histology unremarkable
o Severe GERD:
Intraepithelial eosinophils & neutrophils
Basal zone hyperplasia > 20% of the total
epithelial thickness
Elongation of lamina propria papillae
Figures 5a. Barium Swallow 5b Achalasia Gross appearance
o Marked hyperemia with focal hemorrhage is
Management: present in the area of reflux
o Botulinum Neurotoxin Injection - To inhibit
LES cholinergic neurons
o Pneumatic Dilation
Transcribers Damian, Ng, Perez, Santos 3 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Classification if with dysplasia in Barrett
esophagus:
o Negative dysplasia: repeat endoscopy in 3-5
years
o Indefinite dysplasia: same risk for malignant
progression as low grade dysplasia, re-biopsy in
3-6 month
o Low grade dysplasia: repeat endoscopy in 6-12
months
o High grade dysplasia: surgical or endoscopic
resection of the lesion
Microscopic scenarios qualify for a diagnosis
o Indefinite Dysplasia
Insufficient cytologic atypia
Figures 7a. Gross Appearance of GERD 7b. Histology of GERD
Dysplasia-like epithelium in the background
Clinical features of marked inflammation or mucosal erosion
o Most common in adults >40 years old Subsquamous extension of “dysplastic
o Most common clinical symptoms: glands”
Dysphagia or odinophagia Dysplastic glands that mature to the surface
Heartburn Biopsies without surface epithelium or other
o Other symptoms may include: regurgitation of obscuring factors
sour-tasting gastric content; attacks of severe
Table 3. Dysplasia Features
chest pain (chronic)
Complications Feature Low Grade High Grade
o Esophageal ulceration Dysplasia Dysplasia
o Hematemesis
Architecture Preserved crypt Architectural
o Melena
architecture or distortion:
o Stricture development
villiform surface Crowding
o Barrett esophagus
Branching
Treatment: Proton pump inhibitors or H2 histamine
receptor antagonists → symptomatic relief Budding
Cribriforming
G. BARRET ESOPHAGUS Nuclei Preserved Lack polarity
Complication of chronic GERD polarity Stratification
American College of Gastroenterology definition: Stratification Prominent
o Change in the esophageal epithelium of any Enlargement enlargement
length (>3 cm long segment, ≤ 3 cm short Hyperchromasia Irregular
segment) that can be recognized on endoscopy Crowding membrane contour
and confirmed to have intestinal metaplasia by Less More
biopsy pleomorphic pleomorphism
Histologic basis: Characterized by intestinal
metaplasia within the squamous mucosa → (+) Cytoplasm Diminished Mucin absent
goblet cells (highlighted by Alcian blue/PAS) = mucin
necessary for diagnosis Dystrophic
Increased risk of esophageal adenoCA → pre- goblet cells
malignant condition
Microscopic Identified only through endoscopy and biopsy: evidence of
o (+) goblet cells metaplastic columnar mucosa above the
o Gland architecture: budding, irregular shapes, gastroesophageal junction
and cellular crowding Usually prompted by GERD symptoms
o Non-goblet columnar cells, like gastric type Complications
foveolar cells may also be present, but are o Reflux esophagitis & aspiration pneumonia
insufficient for diagnosis. o Malignancy
When dysplasia is present it is classified as low or high o Esophageal stricture
grade o Esophageal ulcer & perforation
o Esophageal bleeding
Treatment options
o Photodynamic therapy
Transcribers Damian, Ng, Perez, Santos 4 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Laser ablasion I. ADENOCARCINOMA OF THE ESOPHAGUS
o Endoscopic mucosectomy Arises in a background of Barrett esophagus & long-
o esophagectomy standing GERD
Risk factors
H. SQUAMOUS CELL CARCINOMA OF THE o Barret’s (most important)
ESOPHAGUS o Tobacco exposure
4x more common in males; > 45 y/o o Radiation
Risk factors o Obesity
o Alcohol and tobacco use → synergistic o GERD
In areas where alcohol & tobacco use o Scleroderma
uncommon, risk factors include: nutritional o Alcohol
deficiencies, polycyclic hydrocarbons, o Meds: Long term use (>5 years) of Theophylline
nitrosamines, fungus-contaminated foods, & Beta-agonist
HPV infection Risk is reduced by:
o Caustic esophageal injury o Fresh fruits & vegetables
o Achalasia o Some serotypes of H. pylori infection reduce the
o Plummer-Vinson syndrome risk due to atrophy of the gastric mucosa
o Frequent consumption of very hot beverages Most frequently: Caucasians , M > F, distal 1/3 of
o Previous radiation therapy to mediastinum esophagus
Clinical features By the time symptoms appear, the tumor usually
o Onset insidious spread to the submucosal lymphatic vessels
o Dysphagia, odynophagia (pain on swallowing), Over-all 5-year survival is less than 25%
and obstruction Microscopically: Most are mucin producing glandular
o Extreme weight loss & debilitation tumors with intestinal type features
o Tumor ulceration → (+) hemorrhage and sepsis Pathogenesis: Progression of Barret’s to AdenoCA
o Overall 5-year survival = 9% occurs through the stepwise acquisition of genetic &
Morphology epigenetic changes
o 50% occur in middle third (or upper 3rd) o Early stages: Mutation of TP53 &
o Begins as in-situ lesion called squamous downregulation of p16/INK4a
dysplasia o Late stages: Amplification of EFGR, ERB2, Met,
o Grows into polypoid, or exophytic tumor, and cyclin D1 & cyclin E genes
protrude into and obstruct the lumen Morphology
o Most are moderately to well differentiated o Usually occurs in the distal third of the
o LN metastases vary with tumor location: esophagus and may invade adjacent gastric
Upper 3rd → cervical LN cardia
Middle 3rd → mediastinal, paratracheal, and o Initially appearing as flat or raised patches in
tracheobronchial nodes otherwise intact mucosa, large masses of 5 cm or
Lower 3rd → gastric & celiac nodes more in diameter
Morphologic patterns o Commonly produces mucin and form glands,
o Exophytic protruding lesion in the lumen (60%) often with intestinal-type morphology
o Flat, diffuse infiltrative form spreading in the Clinical features
esophageal wall (15%) o Commonly present with pain, difficulty in
o Ulcerative lesions swallowing, progressive weight loss,
hematemesis, chest pain, & vomiting
Figures 8a. Ulcerating Squamous cell carcinoma 8b. Malignant tumor
Figure 9. Adenocarcinoma of the esophagus
of the esophageal squamous mucosa, strongly associated with
tobacco and alcohol use
Transcribers Damian, Ng, Perez, Santos 5 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
III. STOMACH Mic: Presence of neutrophils Mic: Lymphocytes &
in direct contact with plasma cells along with
A. PYLORIC STENOSIS
epithelium intestinal metaplasia &
Progressive thickening of the circular muscle mucosal injury
(hyperplasia of the muscularis propria) of the Focal damage to the gastric
pylorus → gastric outlet narrowing mucosa, with acute
Edema and inflammatory changes in the mucosa and inflammation, necrosis, and
submucosa → aggravate the narrowing. hemorrhage
May be congenital or acquired RF: Heavy smoking, RF: Drugs-NSAIDs, H.
o Acquired pyloric stenosis occurs in adults: excessive alcohol, excessive pylori, alcohol and
consequence of antral gastritis or peptic ulcers NSAID-aspirin, ibuprofen, smoking, radiation,
close to the pylorus. naproxen, Uremia, Ischemia gastrectomy with
o Carcinomas of the distal stomach and pancreas
and shock, Stress (major gastroenerostomy, uremia,
→ narrow the pyloric channel due to fibrosis or
surg.. burns, infections) pernicious anemia
malignant infiltration.
3-4x more common in males CHRONIC GASTRITIS
At risk for congenital hypertrophic pyloric stenosis: o Characterized by chronic mucosal inflammation
o Monozygotic twins (if one twin is affected) and atrophy of the mucosal glands
o Diizygotic twins and siblings of affected o Less common causes of chronic gastritis:
individuals radiation injury, chronic bile reflux, mechanical
o Turner syndrome and Trisomy 18 injury (e.g.an indwelling nasogastric tube), and
o Erythromycin and azithromycin exposure (via oral involvement by systemic diseases, (e.g. Crohn
or mother’s milk in the first 2 weeks of life) disease, amyloidosis, or graft-versus-host
Generally presents in the 2nd or 3rd week of life disease)
(Previous trans: 3rd and 6th weeks of life ) → new- o Complications
onset regurgitation and persistent, projectile, non- Peptic Ulcer Disease
bilious vomiting after feeding and frequent demands Mucosal atrophy and intestinal metaplasia
for re-feeding Gastritis cystica
Physical exam: a firm, ovoid, 1 to 2 cm abdominal Dysplasia
mass
Table 5. Chronic gastritis
Abnormal left to right hyperperistalsis is evident during
With H. pylori (Type B) Without H. pylori (Type
feeding and immediately before vomiting.
A)
Treatment: Surgical splitting of the muscularis
90% 10%
(myotomy) → curative
Most common type Autoimmune gastritis:
most common type of
B. GASTRITIS
Not Associated with intestinal gastritis without H. pylori
Maybe acute or chronic metaplasia & duodenal
ACUTE GASTRITIS epithelium
o Pathogenesis Body-Fundic
Gastric lumen pH: close to 1 (contributes to Predominant: Spares
digestion and has the potential to damage Antrum
the gastric mucosa)
Protective factors of the gastric mucosa: H. pylori causes gastritis in 2 Associated with
surface mucus secretion, bicarbonate patterns: hypergastrinemia
secretion into mucus, mucosal blood flow,
epithelial barrier function, epithelial Associated with other
regenerative capacity and elaboration of autoimmune disease (e.g.
prostaglandins pernicious anemia,
o Clinical features Hashimoto’s Thyroiditis,
Asymptomatic or have persistent epigastric T1DM)
pain Antral Pangastritis Characterized by diffuse
May be accompanied by occasional bilious predominant followed by atrophic gastritis
vomiting gastritis: multifocal (mucosal damage of the
Table 4. Acute vs. Chronic Gastritis Low pro- atrophic oxyntic (acid-producing)
ACUTE GASTRITIS CHRONIC GASTRITIS inflammatory gastritis: mucosa w/in the body and
Transient mucosal Ongoing mucosal cytokines: High pro- the fundus.
inflammation inflammation with mucosal TNF & IL-1B. inflam
atrophy cytokines:
Transcribers Damian, Ng, Perez, Santos 6 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Associated TNF & IL- Dieulafoy lesion : caused by a
with ↑ acid 1B. submucosal artery that does not branch
production & ↑ properly within the wall of the stomach
risk of Associated Gastricantralvascularectasia (GAVE) :
duodenal with ↓ acid responsible for 4% of non-variceal upper
ulcer production & GI bleeding; longitudinal stripes of
↑ risk of edematous erythematous mucosa that
adenoCA alternate with less severely injured, paler
Screening: Characterized by: mucosa, and is sometimes referred to
• Serum ELISA for Antibodies to parietal as watermelon stomach
antibodies cells and intrinsic
• UREA breath test – factor D. PEPTIC ULCER DISEASE
radiolabeled urea is Reduced serum Most often associated with H. pylori- hyperchlorhydric
broken down to pepsinogen I chronic gastritis
radiolabeled CO2 by concentration Present in 85-100% persons with duodenal ulcers
urease, detected by Endocrine cell and 65% with gastric ulcers
breath analyzer. hyperplasia Location (decreasing order of frequency)
• Silver staining or Vitamin B12 o Duodenum (1st part) pyloric ring
warthin starry stain - deficiency o Stomach (lesser curvature near the junction of
gold standard for H. pylori Defective gastric acid the body and the antrum
detection secretion o GEJ in GERD or Barret’s Esophagus
• Culture done in (achlorhydria) o Margins of jejunostomy
Skirrow’s medium – o Stomach, duodenum and/or jejunum of patients
most specific with Zollinger-Ellison syndrome
investigation o In ileal Meckel’s diverticulum containing ectopic
gastric mucosa
C. STRESS- RELATED MUCOSAL DISEASE
Table 6. Duodenal vs. Gastric Ulcer
Occurs in patients with severe trauma, extensive
Features Duodenal Ulcer Gastric Ulcer
burns, intracranial disease, major surgery, serious
Site 1st part of Along lesser
medical disease, and other forms of severe
duodenum curvature
physiologic stress.
Incidence More common Less common
Given specific names based on location and clinical
Age 25-50 yrs, M>F Beyond 6th
associations
decade, M>F
o Stress ulcer: most common in individuals with
Etiology Almost all have Less stronger
shock, sepsis, or severe trauma
H. pylori infection assoc
o Curling ulcers: occur in the proximal duodenum
Acid Level High Usually normal; ↑
and associated with severe burns or trauma
o Cushing ulcers: gastric, duodenal, and if
hypergastrinemia
esophageal ulcers arising in persons with
intracranial disease and carry a high incidence of Pain after food Relieved Aggravated
perforation intake
Pathogenesis Clinical features Night pain & No night pain,
o Stress-related gastric mucosal injury is most melena more hematemesis
often related to local ischemia common more common
o Upregulation of inducible NO synthase and ↑
release of endothelin-1 No vomiting/ no Vomiting
o Direct stimulation of vagal nuclei → wt/ loss common/ weight
hypersecretion of gastric acid loss is present
o Systemic acidosis Complications No malignant Malignant change
Morphology change (rarely)
o Ranges from shallow erosions caused by Pathogenesis
superficial epithelial damage to deeper o Imbalances of mucosal defenses and damaging
o Lesions that penetrate the depth of the mucosa forces that cause chronic gastritis
Clinical features Primary underlying cause: H. pylori & NSAID use
o Gastric mucosal damage Gastric hyperacidity: H. pylori infection, parietal cell
o Other, non-stress-related causes of gastric hyperplasia, excessive secretory responses or
bleeding include: impaired inhibition of stimulatory mechanisms such as
gastrin release
Transcribers Damian, Ng, Perez, Santos 7 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Common co-factors in peptic ulcerogenesis: bleeding in gastric More Incapacitating,
o Chronic NSAID use: direct chemical irritation & ulcer common in crampy
suppress PG release necessary for mucosal May be life- anterior abdominal
protection threatening wall pain
o Cigarette smoking: impairs mucosal blood flow Accounts for 25% duodenal May lead to
& healing of ulcer deaths ulcers total
o High-dose corticosteroids: suppress PG May be the first obstruction
synthesis & impair healing indication of an with
Solitary in > 80% of patients ulcer intractable
o < 0.3 cm. – shallow ulcers vomiting (fluid
o > 0.6 cm. – deeper ulcers & electrolyte
Round or oval, sharply, punched-out defect – mucosal imbalance –
surface overhang the base (heaped up margins → metabolic
cancer) alkalosis)
Gnawing, burning, aching pain, epigastric
Table 8. Benign vs. Malignant Gastric Ulcer
Fe deficiency anemia
BENIGN GASTRIC ULCER MALIGNANT GASTRIC
Acute hemorrhage ULCER
Penetration, perforation:
Lesser curvature Greater curvature
o Pain in back
Smooth radiating folds Interrupted nodular,
o Pain in chest
with Hampton line & clubbed folds (malignant
o Pain in LUQ
collar ulcers with no mass)
Malignant transformation – very rare
Overhanging margins Eccentric with heaped up
showing regeneration and everted margins
Mucosal rugae projects Mucosal rugae stop far of
outwards from the the ulcer
margins of ulcer Necrotic base
Huge base No peristalsis
Preserved peristalsis No healing
Heals within 8-10 weeks
Figures 10a & b. Ulcers include layers of necrosis (N), inflammation
(I), and granulation tissue (G), but a fibrotic scar (S), which takes time J. GASTRIC MALIGNANCIES
to develop, is only present in chronic lesions.
Adenocarcinoma, GIST, Lymphoma
Table 7. Complications of PUD
Table 9. Genes in Gastric Cancer
Complications of peptic ulcer disease (BPO)
Familial Gastric Sporadic gastric cancer
Bleeding Perforation Obstruction
Cancer Intestinal type Diffuse type
Occurs in 15% to Occurs in Occurs in
Loss of CDH1 Most common Loss of CDH1
20% of patients about 5% of about 2% of
gene which overall loss of
Most frequent patients patients
encodes for E p53
complication Accounts Mostly in
cadherin o ↑ wnt pathway
More common in for 2/3 of chronic ulcers
o Loss of fxn
posterior wall ulcer deaths Most often APC
duodenal ulcers – MC cause due to pyloric o Gain of fxn of
Gastroduodenal of death in channel B catenin
artery – MC PUD ulcers
source of bleeding Rarely the May also
in duodenal ulcer 1st occur with ADENOCARCINOMA
Left gastric artery indication of duodenal Most common gastric malignancy (90%)
– MC source of an ulcer ulcers Based on Macroscopic pattern:
o Protruding mass or exophytic (Type I lesion)
Transcribers Damian, Ng, Perez, Santos 8 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Flat or depressed: No obvious mass in the mucosa signaling via the Wnt pathway. These include
(Type II lesion) loss of-function mutations in the adenomatous
o Excavated: Erosion is present in stomach wall polyposis coli (APC) tumor suppressor gene and
(Type III lesion) gain-of-function mutations in the gene encoding
\
β-catenin.
Table 10. Classification of Gastric Adenocarcinoma
o Loss-of-function mutations or silencing of a number
Based on Depth of Invasion Based on Lauren’s
of other tumor suppressor genes have also
Histological classification
been identified, including those involved in TGFβ
Early gastric cancer Intestinal type
signaling (TGFβRII), regulation of apoptosis
(superficial spreading o Composed of the
(BAX), and cell cycle control (CDKN2A).
type) neoplastic intestinal
Morphology
o Involvement of the glands
o Most common location: antrum of the stomach
mucosa and the o Arise from metaplastic
o Cancer of the gastric cardia is on the rise
submucosa epithelium
especially due to Barrett’s esophagus
irrespective of the
o Lesser curvature: involved more often than
involvement of
greater curvature
perigastric lymph
o Diffuse gastric cancer: no definite lump, strong
nodes
desmoplastic reaction that stiffens the gastric wall.
o Associated with best
These tumors show diffuse rugal flattening and a
prognosis
rigis, thickend wall-leather bottle appearance
Late Gastric Cancer
(linnitis plastica)
o Involvement of the
Clinical features
muscle layer
o Intestinal-type gastric cancer predominates in
o Poor prognosis
high-risk areas and develops from precursor
Diffuse type: linitis plastica lesions, including flat dysplasia and adenomas.
o Non-cohesive cells o The depth of invasion and the extent of nodal and
which do not form distant metastases at the time of diagnosis
glands remain the most powerful prognostic indicators.
o “signet ring” appearance Investigaton of choice
(because mucin pushes o Endoscopy with biopsy of lesion
nucleus to the Metastasis
periphery) o First organ affected: liver
o Worst prognosis o Followed by: lungs, bone, ovary (Krukenberg’s
o E-cadherin mutation tumor)
frequently associated o Peiumbilical lymph node: Sister Mary Joseph
Nodule
o Peritoneal cul-de-sac: Blumer’s (palapable on
rectal and vaginal exam)
o Left supraclavicular node: Virchow’s lymph node
o Axillary: Irish Nodes
GASTROINTESTINAL STROMAL TUMOR (GIST)
Arise from pacemakers of the GIT (intestinal cells of
Cajal)
GIST: most common mesenchymal tumor of the
abdomen
Pathogenesis
Most common location: Stomach
o Majority of gastric cancers are not hereditary
Associated with neurofibromatosis 1
o The loss of E-cadherin is a key step in the
Microscopically: epitheloid cells, spindle cells or mixed
development of diffuse gastric cancer.
(both epitheloid and spindle cells)
o Individuals with BRCA2 mutations are at increased
Useful diagnostic markers: DOG (detected on GIST) and
risk of developing diffuse gastric cancer.
c-kit (CD117)
o Mutation of TP53 is also found in the majority of
Carney triad (Carney–Stratakis syndrome)
sporadic gastric cancers of both diffuse and
o A nonhereditary syndrome seen primarily in young
intestinal types.
females that includes:
o In contrast to diffuse gastric cancers, sporadic
Gastric GISTs
intestinal-type gastric cancers are strongly
Paraganglioma
associated with mutations that result in increased
Pulmonary chondroma
Transcribers Damian, Ng, Perez, Santos 9 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Morphology Among malignant small intestinal tumors,
o Large size; solitary, well-circumscribed, fleshy adenocarcinomas and well-differentiated
o If with thin elongated cells → spindle cell type neuroendocrine (carcinoid) tumors have roughly
o If with epithelial-appearing cells → epithelioid type equal incidence, followed by lymphomas and
Clinical: sarcomas.
o Mass effects In primary adenocarcinoma, the duodenum is the
o If with mucosal ulceration → blood loss → anemia most common site.
Prognosis correlates with tumor size, mitotic index
and location (more aggressive in SI) CARCINOID TUMOR
Most common small bowel neoplasm
Arise from the diffuse components of the endocrine
system and are now properly referred to as well-
differentiate neuroendocrine tumors.
May be associated with endocrine cell hyperplasia,
autoimmune chronic atrophic gastritis, MEN-I, and
Zollinger-Ellison syndrome.
Gastric endocrine cell hyperplasia has been linked to
Figure 11a GIST (gross) 11b GIST (micro) Spindle cell lesion with proton pump inhibitor therapy, but the risk of progression
pseudopalisading pattern reminiscent of a schwannoma. Inset - lesional cells to a neuroendocrine neoplasm in this circumstance is
highlighted with CD117 (c-kit) immuno-histochemical stain. extremely low.
Gross
LYMPHOMA o Intramural or submucosal masses → small polypoid
5% of gastric malignancies lesions
Most common are Extra-Nodal Marginal Zone B-cell o In the intestines the tumors may invade deeply to
Lymphomas (lymphoma of mucosa-associated involve the mesentery
lymphoid tissue or MALToma) o Yellow or tan, very firm (intense desmoplastic
Kinds of Lymphoma reaction) → kinking and obstruction of the bowel.
o Gastric MALT lymphoma- replacing much of the Histology
gastric epithelium. Inset shows lymphoepithelial o Islands, trabeculae, strands, glands, or sheets of
lesions with neoplastic lymphocytes surrounding uniform cells with scant, pink granular cytoplasm
and infiltrating gastric glands. and a round to oval stippled nucleus.
o Disseminated Lymphoma- within the small o Minimal pleomorphism
intestine with numerous small serosal nodules. Clinical features
o Large B-cell lymphoma- infiltrating the small o Peak incidence → 6th decade, but they may appear
intestinal wall and producing diffuse thickening at any age
Pathogenesis o Gastrin may cause Zollinger- Ellison syndrome
o Usually arise at sites of chronic inflammation o Ileal tumors may cause carcinoid syndrome
o They can originate in the GI tract at sites of o Strongly associated with metastatic disease in the
preexisting MALT, (Peyer patches of the SI), liver
but more commonly arise within tissues that are Types
normally devoid of organized lymphoid tissue. o Foregut
o MALT is induced, typically as a result of chronic Stomach, duodenum proximal to the ligament
gastritis. of Treitz, and esophagus
o H. pylori eradication results in durable remissions Rarely metastasize
with low rates of recurrence in most MALToma Generally cured by resection
patients. o Midgut
Morphology Jejunum and ileum
o Dense Lymphocytic Infiltrate in the Lamina Propria Multiple
lymphoepithelial lesions ○ Express B Cell Markers Tend to be aggressive.
CD19 and CD20 Greater depth of local invasion, increased size,
Clinical features: most common presenting symptoms and the presence of necrosis and mitoses →
dyspepsia and epigastric pain worse outcome.
o Hindgut
IV. SMALL INTESTINE Appendix and colorectum
A. NEOPLASM Discovered incidentally
Carcinoid Syndrome
Least common site for primary malignancy in the GIT
o Systemic fibrosis (affects cardiac valves,
endocardium, retroperitoneal & pelvic fibrosis)
Transcribers Damian, Ng, Perez, Santos 10 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Hepatomegaly (bec. of metastasis) o Extraintestinal manifestations: Uveitis,
o Intestinal hypermotility (vomiting, diarrhea, Polyarthritis, Acroilitis, Ankylosing Spondylitis,
cramps, nausea) Clubbing of fingers
o Vasomotor symptoms (flushing & cyanosis of the
skin) ULCERATIVE COLITIS
o Asthma like features (Cough, wheezing, dyspnea) Severe ulcerating inflammatory disease
Closely related to Crohn disease; they share the same
B. INFLAMMATORY BOWEL DISEASE extraintestinal manifestations like migratory
Chronic condition resulting from inappropriate polyarthritis, sacroiliitis, ankylosing spondylitis, uveitis
mucosal immune activation and skin lesions
Pathogenesis: combined effects of alterations in host Limited to the colon and recum
interactions w/ intestinal microbiota, intestinal o Pancolitis: disease of the entire colon
epithelial dysfunction, aberrant mucosal immune o Ulcerative proctitis or ulcerative
responses, and altered composition of the gut proctosigmoiditis: limited distal disease
microbiome. Small intestine is normal
Two conditions: Chron’s Disease & Ulcerative Colitis Backwash ileitis, or mild mucosal inflammation of the
distal ileum, can be seen in severe cases of pancoilitis
CHRON’S DISEASE Morphology
Hallmark: Non-caseating granulomas o Mucosa: slightly red and granular or have
Most common sites: terminal ileum, ileocecal valve, extensive, broad based ulcers
and cecum o Abrupt transition between diseased and uninvolved
Typically transmural colon
Skip lesions – multiple, separate, sharply delineated o (+) pseudopolyps → tips of polyps fuse → mucosal
areas bridges
Aphthous ulcer - first ulcer that can be seen ( may o (-) mural thickening, NORMAL serosal surface, NO
coalesce into elongated, serpentine ulcers ) stricture
Marked inflammatory changes and the formation of a o Inflammation → damaged muscularis propria →
fissure between mucosal folds disturb neuromuscular fxn → colonic dilation and
In extensive transmural disease, mesenteric fat toxic megacolon (at risk for perforation)
frequently extends around serosal surfaces (Creeping o Microscopic: inflammatory infiltrates, crypt
Fat) abscesses, crypt distortion and pseudopyloric
crypt abscesses - Abundant neutrophils that infiltrate epithelial metaplasia
o Inflammatory process is diffuse and generally
and damage crypt epithelium
limited to mucosa and superficial submucosa
Paneth Cell metaplasia may also occur in the left
o (-) granuloma
colon
o Acute form with marked hyperemia
Cutaneous granulomas form nodules that are
o Chronic form → mucosal ulceration with residual
referred to as Metastatic Crohn disease.
foci of elevated and hyperemic mucosa.
Gross appearance
Clinical features
o Segmental nature of inflammation
o Relapsing disorder characterized by:
o Rigidity of the wall
Bloody diarrhea with stringy mucoid material
o Flattening of the mucosa
Lower abdominal pain
o Cobblestone appearance (multiple granulomas)
Cramps that are temporarily relieved by
Clinical features
defecation
o Intermittent attacks: mild diarrhea, fever, and
Infectious enteritis precedes disease onset in
abdominal pain
some cases
o 20% experience RLQ pain, fever, and bloody
Ulcerative colitis patients tend to lack antibodies to
diarrhea
Saccharomyces cerevisiae
o May mimic acute appendicitis or bowel perforation
Treatment: colectomy
o Periods of active disease are typically interrupted
by asymptomatic periods
o Iron deficiency anemia may develop
o Extensive small bowel disease → protein loss
and hypoalbuminemia
o Malabsorption of B12 and Bile Salts
o Fibrosing strictures → terminal ileum
Transcribers Damian, Ng, Perez, Santos 11 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Clinical findings
Perianal fistula
No Yes (in colonic
Malabsorption disease)
Malignant No Yes
potential Yes With pancolitis,
early age onset,
Recurrence after duration > 10 yrs
surgery Toxic No Common
megacolon
Yes No
Radiography “Lead pipe” “String” sign in
appearance in terminal ileum;
chronic fistulas
disease
INDETERMINATE COLITIS
Due to extensive pathologic and clinical overlap
between ulcerative colitis and Crohn disease, definitive
Figure 12. Crohn’s vs. Ulcerative colitis diagnosis is not possible in approximately 10% of IBD
patients
Table 11. Chron’s vs. Ulcerative Colitis Do not involve the small bowel
Ulcerative Crohn’s disease Have colonic disease in a continuous pattern that would
colitis typically indicate ulcerative colitis
(+) perinuclear anti-neutrophil cytoplasmic antibodies
Epidemiology Whites > black Whites > black
Americans Americans;
No sex Jews > non- COLITIS-ASSOCIATED NEOPLASIA
predilection Jews Risk factors for dysplasia:
Young adults Women > men o Duration of the disease: risk increases sharply 8 to
Young adults 10 years after disease onset
Extent Mucosal & Transmural ○ Extent of the disease: patients with pancolitis are at
submucosal greater risk than those with only left-sided disease
○ Nature of the inflammatory response
Location Mainly rectum 30% - terminal Diagnosis
Extends ileum alone
continuously 50% - ileum o For early detection of neoplasia, patients are
into left colon and colon enrolled in surveillance programs 8 yrs after
(may involve 20% - colon diagnosis of IBD
entire colon) alone o Goal of surveillance biopsies: identify dysplastic
Does not Involves other epithelium (precursor to colitis associated
involve other areas of GIT carcinoma
areas of GIT (mouth to anus)
Chromoendoscopy and confocal endoscopy: used to
Gross feature increase the sensitivity of detection of dysplasia
Bowel region Colon only Ileum + colon IBD-associated dysplasia is classified histologically as
Distribution Diffuse Skip lesions o High-grade dysplasia: invasive carcinoma at the
Stricture Rare Yes
same site or elsewhere in colon
Wall Thin Thick
appearance o Low-grade dysplasia
● Other causes of chronic colitis
Microscopic o Diversion colitis
Inflammation Limited to Transmural o Microscopic Colitis
mucosa
o Lymphocytic Colitis
Pseudopolyps Marked Moderate
Ulcers Superficial, Deep, knife-like
broad-based C. INTESTINAL OBSTRUCTION
Lymphoid rxn Moderate Marked
Fibrosis Mild to none Marked HERNIA
Serositis Mild to none Marked Any weakness in the wall of the peritoneal cavity that
Granulomas No Yes (~35%)
Fistula/sinus permits protrusion of a serosa-lined pouch of
No Yes
peritoneum (hernial sac)
Transcribers Damian, Ng, Perez, Santos 12 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Acquired hernia
o Most commonly occur anteriorly via the femoral
and inguinal canal or umbilicus or sites of
surgical scars visceral protrusion (external
herniation)
Figure 14. Four major causes of intestinal obstruction
Figure 13. Types of hernia
V. LARGE INTESTINE
VOLVULUS A. NEOPLASM
Complete twisting of a loop of bowel about its Risk Factors
mesenteric base of attachment o Age older than 50 years
Produce both luminal and vascular compromise o Low fiber/high saturated fat diet
Sigmoid colon > cecum > small bowel > stomach or o Cigarette smoking
transverse colon o Familial polyposis syndrome, family history,
ulcerative colitis.
ADHESIONS Locations
Surgical procedures, infection or other causes of o Rectosigmoid – 50% of cases
peritoneal inflammation (e.g. endometriosis) → o Ascending colon – 15% of cases
adhesions between bowel segments, abdominal wall & o Descending colon – 15% of cases
operative sites → fibrous bridges create closed loops → o Transverse colon & cecum – 10% each
internal herniation Screening tests
o Fecal occult blood test – not very sensitive or
INTUSSUSCEPTION specific
Most common cause of intestinal obstruction in children o Colonoscopy – gold standard
< 2 years of age o Barium enema
2 portions of intussusception Clinical findings
o Intussuscipiens: pinasukan na intestine o Left-sided cancers tend to obstruct
o Intussusceptum: pumasok na intestine Lesions with annular, “napkin-ring”
Infants & children: viral infection & rotavirus vaccine appearance
(Reactive Hyperplasia of the Peyer’s patches/MALT Change in bowel habits – constipation and
Leading Edge of intussusception) diarrhea with or without bleeding; change in
Older children and adults: Intraluminal mass or tumor caliber, change in consistency; stools with
serves as point of traction mucus
o Right-sided cancers tend to bleed
Tumors are more polypoid in appearance
Blood in the stool and iron deficiency are
more likely
Anemia, with symptoms such as dizziness,
malaise, and palpitation.
o Symptoms due to metastasis
Sites of metastasis: liver (most common),
lungs, bone, and brain
Transcribers Damian, Ng, Perez, Santos 13 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Shortness of breath (lung metastasis) Mediated by inhibition of the enzymes of
Jaundice (liver metastasis) COX-2 which is highly expressed in 90%
of colorectal carcinomas and 40%-90% of
HEREDITARY NON-POLYPOSIS COLORECTAL CANCER adenomas
(HNPCC) Recall: COX-2 is necessary for production
aka lynch syndrome of PGE2 that promotes epithelial
Familial clustering of cancers at several sites including: proliferation, particularly after injury
o Colorectum o Genetic factors
o Endometrium APC gene mutation
o Stomach Adenomatous polyposis
o Ovary Hereditary Nonpolyposis Colorectal Cancer
o Ureter Morphology
o Brain o Microscopic findings: crowding or formation of
o Small bowel cribriform pattern of tubular glands
o Hepatobiliary tract o Gross findings
o Pancreas “Napkin Ring” deformity
o Skin Can be distinguished as:
Most common syndromic form of colon cancer (2-4% of o Polypoid: presents as a bulky mass with
all colorectal cancer) well-defined, rolled margins, and a sharp
Tend to occur at a younger age than sporadic colon dividing line with the normal bowel
cancer o Ulcerative/Infiltrative: less elevated
Pathogenesis: inherited mutations in genes that surface and is certainly ulcerated
encode proteins responsible for the detection, excision, Microscopic differences
and repair of errors that occur during DNA replication o Tubular: with space in between glands
There are at least five mismatch repair genes but a o Villous: vertical elongation of glands
majority of HNCC patients have a mutation in MSH2 or o Adenocarcinoma: no space in between glands due
MLH1 genes to the fusion of adjacent glands creating a cribriform
HNPCC patients may inherit one mutant gene and one pattern
normal gene Growth Pattern
Silencing of the normal gene through mutation → o Polypoid/exophytic: proximal portion of large
extremely high mutation in microsatellites → intestine (right side)
microsatellite instability (prone to developing into o Annular, constricting (napkin ring): distal portion of
colorectal cancer) the large intestine (left side)
o Diffuse
ADENOCARCINOMA Pathogenesis
Adenocarcinoma of the colon is the most common o APC/B-catenin pathway
malignancy of the GI tract and is a major cause of Classic adenoma-carcinoma pathway
morbidity and mortality worldwide o Microsatellite instability pathway
Location: approximately 50% of all carcinomas occur in Defects in DNA mismatch repair and
the rectosigmoid area accumulation of mutations in microsatellite
Risk for development repeat regions of the genome
o Environmental Factors aka MSI high or MSI-H tumors
Low dietary fiber content: may alter the Mutations in TGF-B receptors may contribute
composition of intestinal flora and increased to uncontrolled cell growth due to the inherent
synthesis of toxic oxidative by-products of activity of TGF to inhibit colonic epithelial cell
bacterial metabolism that would be exposed to proliferation
colonic mucosa for extended periods of time o Activating mutations in the oncogene BRAF are
High content of refined carbohydrates common in these cancers
High fat: enhances hepatic synthesis of o KRAS and TP53 are not typically mutated
cholesterol and bile acids which can be Microsatellite instability + BRAF mutations +
converted into carcinogens by intestinal methylation of specific of targets (e.g. MLH1) =
bacteria signature of pathway of carcinogenesis
Decreased intake of micronutrients Clinical significance
Aspirin, or other NSAIDS: have protective o Right-sided colon cancer: fatigue and weakness
effect by causing polyp regression in AP due to iron deficiency anemia
patients in whom the rectum was left in place o Left-sided colorectal adenocarcinomas: occult
after colectomy bleeding, changes in bowel habits or cramping, and
left lower quadrant discomfort
Transcribers Damian, Ng, Perez, Santos 14 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Most important prognostic factors: depth of invasion o May be missed during casual inspection because it
& +/- LN metastasis is compressible, easily emptied of fecal contents,
Diagnosis and often surrounded by the fat-containing epiploic
o Screening for high-risk individuals appendices
Fecal Occult Blood Test Has a thin wall composed of a flattened or atrophic
Annual Colonoscopy for both men and women mucosa, compressed submucosa, and attenuated or,
over 40 years old most often, totally absent muscularis propria
o Diagnostic tools Hypertrophy of the circular layer of the muscularis
CBC and PBS: microcytic and hypochromic propria in the affected bowel segment
anemia, low RBC, Hgb, and Hct Obstruction of diverticula → inflammatory changes →
Occult blood: positive diverticulitis and peridiverticulitis
Barium Enema: “Apple core appearance”, Inflammation and ↑ pressure within an obstructed
shouldering diverticulum → perforation (why? kasi muscularis
o Prognosis mucosae and subserosal tissue lang ang nakasupport
Mucinous Adenocarcinoma sa wall ng diverticulum so imagine kapag sobrang taas
Factors: depth of invasion and presence of ng pressure)
lymph node metastases o Perforation → pericolonic abscesses, sinus tracts,
The most common metastatic sites are the peritonitis
liver, lungs, and bones With or without perforation, diverticulitis may cause:
o Segmental diverticular disease-associated colitis
o Fibrotic thickening in and around the colonic wall
o Stricture formation
Clinical feature: most patients are asymptomatic
C. HIRCSHPRUNG DISEASE
aka Congenital Aganglionic Megacolon
May be isolated or occur in combination with other
developmental abnormalities
1 of 5000 live births
10% of cases: children with Down syndrome
Figure 15. Histologic appearance of colorectal carcinoma.. A, Well- 5% of cases: with serious neurologic abnormalities
differentiated adenocarcinoma. Note the elongated, hyperchromatic
More common in males
nuclei. Necrotic debris present in the gland lumen. C, Mucinous
adenocarcinoma with signet-ring cells and extracellular mucin pools
When present in females, tends to involve longer
aganglionic segments
B. SIGMOID DIVERTICULAR DISEASE Defect ALWAYS begins at the rectum
DIVERTICULAR DISEASE Pathogenesis
o Results when the normal migration of neural crest
Acquired pseudo-diverticular outpouchings of the
cells from cecum to rectum is prematurely
colonic mucosa and submucosa
arrested OR when the ganglion cells undergo
Not invested by all three layers of the colonic wall
premature death.
Rare in persons <30 years old
o Distal intestinal segment lacks both Meissner’s
Diverticulosis: multiple diverticula
and Auerbach plexuses (aganglionosis) →
Most diverticula in Asia and Africa occur in the right
absent peristalsis on distal segment → functional
colon; right-sided diverticula are uncommon in Western
obstruction → dilation proximal to the affected
countries
segment.
Pathogenesis
o Genetics: heterozygous loss-of-function
o Result from the unique structure of the colonic
mutations in receptor tyrosine kinase RET
muscularis propria
o Pathologic feature: Distal narrow a peristaltic
o ↑ intraluminal pressure in the sigmoid colon
hypertonic segment (aganglionic) and a dilated
Due to exaggerated peristaltic contractions
proximal segment caused by obstruction.
with spasmodic sequestration of bowel
segments Clinical features
Enhanced by diets low in fiber → reduce stool o Failure to pass meconium in the immediate
bulk postnatal period.
Morphology o Obstruction or constipation often with ineffective
o Small, flask-like outpouchings occur in a regular peristalsis.
distribution alongside the taenia coli
Transcribers Damian, Ng, Perez, Santos 15 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Earliest and most common presentation is “Sawtooth appearance”
delayed (> 48 hrs) passage of meconium in the Serration is typically restricted to the upper
newborn third (or less) of the crypt
o Infants and older children: chronic constipation,
abdominal distention and vomiting.
If few cm of rectum is affected, occasional passage of
stool may occur. Most cases limited to rectum and
sigmoid colon.
(+) megacolon → stretch and thin the colonic wall to
the point of rupture (usually cecum)
Major threats to life
o Enterocolitis
o Fluid and electrolyte disturbances
o Perforation
o Peritonitis
Diagnosis
o Requires documenting the absence of ganglion
cells within the affected segment
H&E stain
Immunohistochemical stain for Figure 16. Hyperplastic polyp. A, Polyp surface with irregular tufting
acetylcholinesterase of epithelial cells. B, Tufting results from epithelial overcrowding. C,
Intraoperative frozen-section analysis: Epithelial crowding produces a serrated architecture
confirmatory
Treatment: Surgical resection of the aganglionic B. INFLAMMATORY POLYPS
segment followed by anastomosis of the normal ● Form as part of the solitary rectal ulcer syndrome
proximal colon to the rectum ● Clinical triad
o Rectal bleeding
VI. SMALL & LARGE BOWEL POLYPS o Mucus discharge
Most common in the colo-rectal region but may occur in o Inflammatory lesion of the anterior rectal wall
the esophagus, stomach, or small intestine ● Pathogenesis: impaired relaxation of the anorectal
Begin as small elevations of the mucosa (sessile) sphincter → sharp angle at the anterior rectal shelf →
o Sessile: polyps without a stalk recurrent abrasion and ulceration of the overlying
o Pedunculated: polyps with stalks rectal mucosa
Intestinal polyps can be grouped into neoplastic and non- o Result of chronic cycles of injury and healing
neoplastic ● Entrapment in fecal stream → mucosal prolapse
o Neoplastic: with dysplasia; example is adenoma ● Microscopic: mixed inflammatory infiltrates, erosion,
o Non-neoplastic can be further further classified as and epithelial hyperplasia + lamina propria
inflammatory, hamartomatous, or hyperplastic fibromuscular hyperplasia
A. HYPERPLASTIC POLYPS C. HAMARTOMATOUS POLYPS
● Occur sporadically or as components of various
Benign epithelial proliferations that are typically
genetically determined or acquired syndromes
discovered in the 6th and 7th decades of life
● Pathogenesis: caused by germline mutations in
Pathogenesis: result from decreased epithelial cell
tumor suppressor genes or protooncogenes
turnover and delayed shedding of surface epithelial
● Some are associated with increased cancer risk
cells → “piling up” of goblet cells and absorptive cells
NO malignant potential
JUVENILE POLYPS
Histologically similar with sessile serrated adenomas
Focal malformations of the epithelium and lamina
Morphology
propria
o Found in the left colon
Occur in children <5 y/o but they can present at older
o Smooth, nodular protrusions of the mucosa, often
ages
on the crests of mucosal folds
Located in the rectum
o May occur singly but are more frequently multiple,
Clinical manifestations: rectal bleeding,
particularly in the sigmoid colon and rectum
intussusception, intestinal obstruction, or polyp prolapse
o Microscopic: mature goblet and absorptive cells
(through the anal sphincter)
o Delayed shedding of these cells → crowding →
serrated surface (morphologic hallmark) May be sporadic or syndromic
Transcribers Damian, Ng, Perez, Santos 16 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
o Sporadic (retention) polyps: usually solitary cell polarization and acts as a brake on growth and
lesions, dysplasia is extremely rare anabolic metabolism)
o Syndromic polyps: may require colectomy to limit *The function of the second normal copy of STK11 is lost
the chronic and sometimes severe hemorrhage through somatic mutation in cancers
associated with polyp ulceration, associated with Morphology
dysplasia o Seen in small intestine (most common), stomach,
Extraintestinal manifestation of juvenile polyposis colon, bladder and lungs
include pulmonary arteriovenous malformations and o Gross: large and pedunculated with a lobulated
other congenital malformations contour
Morphology o Microscopic: arborizing network of connective
o Gross: pedunculated, smooth-surfaced, reddish tissue, smooth muscle, lamina propria, and glands
lesions with characteristic cystic spaces lined by normal-appearing intestinal epithelium
o Microscopic: dilated glands filled with mucin and *The arborization and presence of smooth muscle
inflammatory debris intermixed with lamina propria can be used to distinguish
Remainder of the polyp is composed of lamina Peutz-Jeghers from Juvenile polyps.
propria expanded by mixed inflammatory
infiltrates D. NEOPLASTIC POLYPS
Muscularis mucosae may be normal or ● Neoplastic mass lesions in the GI tract may produce a
attenuated mucosal protrusion, or polyp
Initiating event: hyperplasia of the mucosa o Adenocarcinomas, neuroendocrine (carcinoid)
Pathogenesis: mutations in SMAD4 (encodes a tumors, stromal tumors, lymphomas, and
cytoplasmic intermediate in the TGF-β signaling metastatic cancers from distant sites
pathway) and BMPR1A (kinase that is a member of the ● Colonic Adenoma: Most common neoplastic polyp.
TGF-β superfamily) → autosomal dominant juvenile Precursors to majority of colorectal adenocarcinoma
polyposis o Recommended colonoscopy surveillance :
■ General population: 50 y/o
■ With family hx of colorectal adenoCA: at
least 10 years before the youngest age at
which a relative was diagnosed
o Risk factors for malignancy
■ Adenomas > 2 cm size (40% risk)
■ Multiple polyps
■ Polyps with increased villous component
■ High grade dysplasia
o Size is the most important characteristic that
Figure 17. Juvenile polyps. Note the surface erosion and cystically
dilated crypts. correlates with risk 40% of lesions > 4 cm
contain foci of cancer
PEUTZ-JEGHERS SYNDROME ● Adenomas are intraepithelial neoplasms that range
Rare autosomal dominant syndrome from small pedunculated polyps to large sessile
Clinical features lesions. Characterized by presence of epithelial
o Median age of 11 years dysplasia.
o Multiple GI hamartomatous polyps o Most are clinically silent, with the exception of:
o Mucocutaneous hyperpigmentation (dark blue to ■ Large polyps that produce occult bleeding
brown macules on the lips, nostrils, buccal mucosa, and anemia
palmar surfaces of the hands, genitalia, and ■ Rare villous adenomas that cause
perianal region) hypoproteinemic hypokalemia by secreting
o (+) family history large amounts of protein and potassium
Can initiate intussusception (occasionally fatal) o Can be classified into:
Associated with a markedly increased risk of several ■ Tubular adenomas (adenomatous
malignancies polyps)
o At birth: sex cord tumors of the testis Small, smooth, pedunculated polyps
o Late childhood: gastric and SI cancers Solitary, usually stalked
o > 2nd and 3rd Decades of life: colon, pancreatic, Most common (60% of polyps)
breast, lung, ovarian and uterine cancers Sigmoid colon most common site
Pathogenesis: germline heterozygous loss-of-function Composed of small rounded, or tubular,
mutations in the STK11 (Recall: STK11 is a tumor glands
suppressor gene that encodes a kinase that regulates Microscopic: circular glands, crowding
of the tubular formations on dysplastic
Transcribers Damian, Ng, Perez, Santos 17 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
colonic glands, pseudostratification of E. ADENOMATOUS POLYPOSIS
the lining, dysplastic changes as
FAMILIAL COLONIC POLYPS AND CARCINOMA (FAP)
exhibited by hyperchromasia
Autosomal dominant disorder
■ Villous adenomas
Often larger Caused by mutations of the Adenomatous polyposis
Covered by slender villi coli (APC) gene
Most cases present as a single mass in o Key negative regulator of the Wnt signaling pathway
the rectum At least 100 polyps are necessary for diagnosis
Papillary villous projections, usually Polyp growth are indistinguishable from sporadic
attached by a wide base adenomas except for their remarkable number
Gross: The lesion is characteristically (+) Large central dominant polyp surrounded by multiple
large and flat and has an arborescent smaller polyps
architecture. Multiple villous projections Flat or depressed adenomas are also prevalent and
ramify on a long papillary crown like microscopic adenomas are frequently observed in
growth “carpet” like normal-appearing mucosa
Microscopic: Epithelial dysplasia, Colorectal adenocarcinoma develops in 100% of
hyperchromasia, vertical elongation of untreated AP patients
villi, finger like projections. Long villi are Treatment: prophylactic colectomy
arranged in parallel, perpendicularly to o Prevents colorectal cancer
the mucosa. o Remain at risk for neoplasia at other sites
■ Tubulovillous adenomas o Adenomas may develop elsewhere in the GI tract,
Mixture of tubular and villous elements particularly adjacent to the ampulla of Vater in the
20 – 30% of polyps stomach
Usually pedunculated Extraintestinal manifestation: congenital hypertrophy of
● Colorectal adenomas are characterized by the the retinal pigment epithelium
presence of epithelial dysplasia. Subtypes of FAP
o Prevalence of colorectal adenomas correlates o Classic FAP syndrome
with that of colorectal adenocarcinoma ■ The patient has a large number of
● Morphology adenomatous polyps and retinal pigment
o Can be pedunculated or sessile, with the surface epithelial hypertrophy. There should be a
of both types having a texture resembling velvet minimum of 100 polyps to make a diagnosis
or a raspberry
of this syndrome. Most adenomatous polyps
o Microscopic: nuclear hyperchromasia,
are tubular polyps.
elongation, and stratification (all of which are o Gardner Syndrome: Intestinal polyps + epidermal
hallmarks of epithelial dysplasia); prominent
cyts + fibromatosis + osteomas (of the mandible,
nucleoli, eosinophilic cytoplasm, and ↓ goblet
long bones & skull)
cells o Turcot Syndrome: Adenomatous colon polyposis
+ CNS tumors ( medulloblastoma in 2/3 and gliomas
in 1/3 patients).
o Noncolonic causes of death in patients with
FAP
Thyroid adenocarcinoma
Pancreatic carcinoma
CNS tumors
Complications of therapy
MYH-ASSOCIATED POLYPOSIS
Autosomal recessive disorder
Some polyposis without APC loss have bi-allelic
mutations of the base-excision repair gene MYH
Similar to attenuated AP with polyp development at later
Figure 18. Histologic appearance of colonic adenomas. A, Tubular adenoma with a ages, presence of fewer than 100 adenomas, and
smooth surface and rounded glands. Active inflammation is occasionally present in delayed appearance of colon cancer.
adenomas, in this case, crypt dilation and rupture can be seen at the bottom of the
field. B, Villous adenoma with long, slender projections that are reminiscent of small
REFERENCE:
intestinal villi. C, Dysplastic epithelial cells (top) with an increased nuclear to
cytoplasmic ratio, hyperchromatic and elongated nuclei, and nuclear Lecture PPT, Lecture Notes, Systemic Pathology Transes 2022,
pseudostratification. D, Sessile serrated adenoma lined by goblet cells without Robbin’s 9th ed.
cytologic features of dysplasia. This lesion is distinguished from a hyperplastic polyp by
extension of the neoplastic process to the crypts, resulting in lateral growth
Transcribers Damian, Ng, Perez, Santos 18 of 20
SURGICAL PATHOLOGY
1.01 Gastrointestinal Pathology P1
September 9, 2020 | Dr. Arnel Bayotas
APPENDIX
Transcribers Damian, Ng, Perez, Santos 19 of 20
1.01 GIT Surgical Pathology SEM 1 PRELIMS
Transcribers Damian, Ng, Perez, Santos 20 of 20
You might also like
- Diverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandDiverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesRating: 1 out of 5 stars1/5 (1)
- Gastrointestinal Tract PathologyDocument8 pagesGastrointestinal Tract PathologyMiguel Cuevas Dolot100% (2)
- Gastrointestinal Tract PathologyDocument12 pagesGastrointestinal Tract PathologyTurinawe Bin ByensiNo ratings yet
- Gastro RobbinsDocument68 pagesGastro RobbinsAndrea PescosolidoNo ratings yet
- Esophageal Atresia and Tracheoesophageal FistulaDocument28 pagesEsophageal Atresia and Tracheoesophageal FistulaSubas SharmaNo ratings yet
- Acute AbdomenDocument117 pagesAcute Abdomenayundaafdal100% (1)
- Pediatric GI RadiologyDocument6 pagesPediatric GI Radiologysarguss14No ratings yet
- RLQ PainDocument20 pagesRLQ PainBEATRICE SOPHIA PARMANo ratings yet
- Gastrointestinal System DiseasesDocument6 pagesGastrointestinal System DiseasesHazel ConjeNo ratings yet
- Agenesis Atresia Fistula: Mechanical ObstructionDocument13 pagesAgenesis Atresia Fistula: Mechanical Obstructionnge257No ratings yet
- Intestinal ObstructionDocument70 pagesIntestinal ObstructionosNo ratings yet
- Esophageal AtresiaDocument8 pagesEsophageal Atresianevelle4667No ratings yet
- Abdomen Urinary-AddDocument5 pagesAbdomen Urinary-AddDionne Jillian SyNo ratings yet
- Git تجميعاتDocument146 pagesGit تجميعاتMenna SalemNo ratings yet
- Cirugia Peds Fund TeoricosDocument12 pagesCirugia Peds Fund Teoricos[JC]No ratings yet
- A3. Esophageal Diverticles and Tracheo-Esophageal FistulesDocument4 pagesA3. Esophageal Diverticles and Tracheo-Esophageal FistulesSaman SadeghiNo ratings yet
- 2.4.5.2.3.a Bowel ObstructionDocument35 pages2.4.5.2.3.a Bowel ObstructionProject ByNo ratings yet
- LEC 2 - Abdomen 2 - AUSCULATION 2010Document1 pageLEC 2 - Abdomen 2 - AUSCULATION 2010Elle ReyesNo ratings yet
- ILEUS AND PERITONITIS AnglDocument51 pagesILEUS AND PERITONITIS Anglutami nahdyaNo ratings yet
- 1-5 BedahDocument9 pages1-5 BedahHalwia SiruaNo ratings yet
- Intestinal Obstruction: MSU Medical Students. Batch 2. Group 2Document31 pagesIntestinal Obstruction: MSU Medical Students. Batch 2. Group 2Qp Nizam100% (2)
- Test Bank On GI PathologyDocument14 pagesTest Bank On GI PathologySeff CausapinNo ratings yet
- Gi Patho PharmaDocument22 pagesGi Patho Pharmas748jNo ratings yet
- Jejuno-ileal Atresia SurgeryDocument16 pagesJejuno-ileal Atresia SurgeryFauzi NoviaNo ratings yet
- Penanganan Terkini Bayi PrematurDocument44 pagesPenanganan Terkini Bayi PrematuryudhagpNo ratings yet
- GI нотесDocument36 pagesGI нотесСоња БакраческаNo ratings yet
- Esophageal and Gastric Pathology OverviewDocument59 pagesEsophageal and Gastric Pathology OverviewadystiNo ratings yet
- Srs Esophagus & Stomach: PathologyDocument4 pagesSrs Esophagus & Stomach: PathologyyayayanizaNo ratings yet
- Intestinal ObstructionDocument42 pagesIntestinal ObstructionSaurabh SharmaNo ratings yet
- Intestinalobstruction 150401053831 Conversion Gate01Document65 pagesIntestinalobstruction 150401053831 Conversion Gate01Nina NoviaNo ratings yet
- Gastroduodenal Anatomy Imaging Issues and Differential DiagnosisDocument78 pagesGastroduodenal Anatomy Imaging Issues and Differential Diagnosistudoranluciana1No ratings yet
- General Surgery Study GuideDocument118 pagesGeneral Surgery Study GuideYvonne HuangNo ratings yet
- AppendicitisDocument4 pagesAppendicitisRonaldoNo ratings yet
- Gastro First AidDocument45 pagesGastro First AidMaría BonettiNo ratings yet
- Ajcr 2010 1 6Document3 pagesAjcr 2010 1 6Muhammad Bilal MirzaNo ratings yet
- Presentacion GastrointestinalDocument228 pagesPresentacion GastrointestinalNb + XB = AVNo ratings yet
- GASTROINSTINAL TRACT Robbins 8th EditionDocument4 pagesGASTROINSTINAL TRACT Robbins 8th EditionLim EricNo ratings yet
- Pathology B - Gastrointestinal Tract (Esguerra, 2015) PDFDocument18 pagesPathology B - Gastrointestinal Tract (Esguerra, 2015) PDFJem QuintoNo ratings yet
- Pathology B - Gastrointestinal Tract (Esguerra, 2015)Document18 pagesPathology B - Gastrointestinal Tract (Esguerra, 2015)Ars MoriendiNo ratings yet
- Bedah Anak: Kelainan Kongenital Gastrointestinal Anak Kedaruratan AnakDocument52 pagesBedah Anak: Kelainan Kongenital Gastrointestinal Anak Kedaruratan AnakalifNo ratings yet
- Abdomen AgudoDocument12 pagesAbdomen AgudoMercedes RojasNo ratings yet
- TRANSESDocument45 pagesTRANSESItsMe AJNo ratings yet
- Intestinal Obstruction in Paediatrics - James GathogoDocument21 pagesIntestinal Obstruction in Paediatrics - James GathogoMalueth Angui100% (1)
- Appendix DuplicationDocument3 pagesAppendix DuplicationMario TrejoNo ratings yet
- Congenital Pyloric Atresia With Distal Duodenal Atresia-Role of CT ScanDocument3 pagesCongenital Pyloric Atresia With Distal Duodenal Atresia-Role of CT Scanhaidar HumairNo ratings yet
- Surgery 2.01.3 Omentum, Mesentery and Retroperitoneum - Dr. MendozaDocument8 pagesSurgery 2.01.3 Omentum, Mesentery and Retroperitoneum - Dr. MendozaJorge De VeraNo ratings yet
- Intussusception TransDocument4 pagesIntussusception TransJames Maravillas100% (1)
- Abdome AgudoDocument13 pagesAbdome AgudoJavier VeraNo ratings yet
- Surgery Subspecialty - Peds First DayDocument2 pagesSurgery Subspecialty - Peds First DayJonathan AiresNo ratings yet
- Large-Bowel Obstruction: Nihal Hamouda, MD Scott A. Jorgensen, MD Alexander J. Towbin, MD and Richard Towbin, MDDocument3 pagesLarge-Bowel Obstruction: Nihal Hamouda, MD Scott A. Jorgensen, MD Alexander J. Towbin, MD and Richard Towbin, MDDian FikriNo ratings yet
- Omphalocele and GastroshisisDocument41 pagesOmphalocele and GastroshisisWaldi KurniawanNo ratings yet
- Esophageal Atresia and Tracheoesophageal Fistula MalformationsDocument23 pagesEsophageal Atresia and Tracheoesophageal Fistula MalformationsAnonymous Hx5eGBNNo ratings yet
- Intestinal Obstruction Causes and ManagementDocument37 pagesIntestinal Obstruction Causes and ManagementkrisandiNo ratings yet
- UNCDCYSTDocument5 pagesUNCDCYSTeviltohuntNo ratings yet
- 1.04 Large Intestine, Colon, and RectumDocument15 pages1.04 Large Intestine, Colon, and RectumZazaNo ratings yet
- Diseases of The Esophagus DR Lapuz MCDDocument6 pagesDiseases of The Esophagus DR Lapuz MCDMiguel Cuevas Dolot100% (1)
- Acute Abdominal Pain GuideDocument19 pagesAcute Abdominal Pain GuideAudricNo ratings yet
- Perforasi GasterDocument6 pagesPerforasi GasterFarhan Hady DanuatmajaNo ratings yet
- NCM107 PediatricsDocument11 pagesNCM107 PediatricsKM PanganibanNo ratings yet
- Red and White Christmas Illustration Christmas TagDocument1 pageRed and White Christmas Illustration Christmas TagKarl ChavezNo ratings yet
- Wingfield, Et Al. 2018Document6 pagesWingfield, Et Al. 2018Karl ChavezNo ratings yet
- 4.03 Anti-Arrhythmic Drugs PDFDocument8 pages4.03 Anti-Arrhythmic Drugs PDFKarl ChavezNo ratings yet
- CHAVEZ - Upper Airway ObstructionDocument2 pagesCHAVEZ - Upper Airway ObstructionKarl ChavezNo ratings yet
- Review Article: Cytokines As Biomarkers and Their Respective Clinical Cutoff LevelsDocument12 pagesReview Article: Cytokines As Biomarkers and Their Respective Clinical Cutoff LevelsHabifa Mulya CitaNo ratings yet
- CHAVEZ - Upper Airway ObstructionDocument2 pagesCHAVEZ - Upper Airway ObstructionKarl ChavezNo ratings yet
- (Med1) Chavez, Karl Raem Anton M. Case 1 and 2.Document2 pages(Med1) Chavez, Karl Raem Anton M. Case 1 and 2.Karl ChavezNo ratings yet
- Parasitic Ameoba Handout PDFDocument7 pagesParasitic Ameoba Handout PDFKarl ChavezNo ratings yet
- CHAPTER 17: Basic Concepts of Physician-Patient Contractual RelationshipDocument20 pagesCHAPTER 17: Basic Concepts of Physician-Patient Contractual RelationshipKarl ChavezNo ratings yet
- Summary CH 25262829 PDFDocument2 pagesSummary CH 25262829 PDFKarl ChavezNo ratings yet
- Induction of Labor Algorithm: Appendix RDocument1 pageInduction of Labor Algorithm: Appendix RBrolie BarsebaNo ratings yet
- Mood DisordersDocument49 pagesMood DisordersKarl ChavezNo ratings yet
- Free Living Pathogenic Amoeba PDFDocument9 pagesFree Living Pathogenic Amoeba PDFKarl ChavezNo ratings yet
- 4.04 Hypolipidemic Agents PDFDocument17 pages4.04 Hypolipidemic Agents PDFKarl ChavezNo ratings yet
- Karl Raem Anton M. Chavez Bs-Biology Theology 2 - 12-2Pm Quiz # 1Document1 pageKarl Raem Anton M. Chavez Bs-Biology Theology 2 - 12-2Pm Quiz # 1Karl ChavezNo ratings yet
- BCHM GRP 5 Case Nutrition by Age For Class PDFDocument136 pagesBCHM GRP 5 Case Nutrition by Age For Class PDFKarl ChavezNo ratings yet
- Obg Icd-10 Pregnancy, Childbirth, PuerperiumDocument11 pagesObg Icd-10 Pregnancy, Childbirth, PuerperiumarifianjuariNo ratings yet
- Physiology of Aging: Carlene S. Solidum, MD, DPPSDocument28 pagesPhysiology of Aging: Carlene S. Solidum, MD, DPPSKarl ChavezNo ratings yet
- Qualitative Analysis of Cation Group 2 enDocument14 pagesQualitative Analysis of Cation Group 2 enMelissa SueltoNo ratings yet
- CHAPTER 17: Basic Concepts of Physician-Patient Contractual RelationshipDocument20 pagesCHAPTER 17: Basic Concepts of Physician-Patient Contractual RelationshipKarl ChavezNo ratings yet
- Group IV Cations: Barium, Strontium, CalciumDocument14 pagesGroup IV Cations: Barium, Strontium, CalciumDavi DyegoNo ratings yet
- Full Text PDFDocument69 pagesFull Text PDFKarl ChavezNo ratings yet
- Linkage (Genetics)Document21 pagesLinkage (Genetics)Karl ChavezNo ratings yet
- Medical MicrobiologyDocument44 pagesMedical MicrobiologyKarl ChavezNo ratings yet
- Scientific NamesDocument1 pageScientific NamesKarl ChavezNo ratings yet
- Student Attendance Chapter 1 RevDocument9 pagesStudent Attendance Chapter 1 RevJohn PecsonNo ratings yet
- Mercury GroupDocument27 pagesMercury GroupAnjum AbbasiNo ratings yet
- Histamine and Antihistamines: Learning ObjectivesDocument6 pagesHistamine and Antihistamines: Learning ObjectivesaNo ratings yet
- Systemic Pathology Mnemonics Part IDocument18 pagesSystemic Pathology Mnemonics Part IHanan HamdyNo ratings yet
- Harmony Drugs FoodDocument2 pagesHarmony Drugs FoodportosinNo ratings yet
- Parietal Cell Physiology and Advances in Acid Suppression TherapiesDocument6 pagesParietal Cell Physiology and Advances in Acid Suppression TherapiesNurul Kamilah SadliNo ratings yet
- AP Bio Digestion System (Kfogler)Document34 pagesAP Bio Digestion System (Kfogler)julie rainesNo ratings yet
- Mechanism of Action, Indications, and Side Effects of AntacidsDocument10 pagesMechanism of Action, Indications, and Side Effects of AntacidsMuhammed ZkriaNo ratings yet
- Pharmacology LectureDocument18 pagesPharmacology LectureChloe MorningstarNo ratings yet
- Gastritis - StatPearls - NCBI Bookshelf PDFDocument1 pageGastritis - StatPearls - NCBI Bookshelf PDFwahyukhairiyandaNo ratings yet
- Pharmacology of GIT: Drugs Used in Peptic Ulcer TreatmentDocument29 pagesPharmacology of GIT: Drugs Used in Peptic Ulcer TreatmentMohammed Bahnasy100% (1)
- V.I. Vernadsky Crimean Federal University Medical Academy named after S.I. Georgievsky Chair of Surgery No1 Objectives for Intermediate Certification 6 yearDocument49 pagesV.I. Vernadsky Crimean Federal University Medical Academy named after S.I. Georgievsky Chair of Surgery No1 Objectives for Intermediate Certification 6 yearjhuiNo ratings yet
- Joel Wallach - Dead Doctors Don't LieDocument27 pagesJoel Wallach - Dead Doctors Don't Liegoombo100% (10)
- Carcinoma GasterDocument32 pagesCarcinoma GasterAzhari AhsanNo ratings yet
- Formulation and Evaluation of Stomach Specific Mucoadhesive Tablets of FamotidineDocument11 pagesFormulation and Evaluation of Stomach Specific Mucoadhesive Tablets of Famotidinemuli sukmaNo ratings yet
- Acute Abdominal PainDocument2 pagesAcute Abdominal PainWinnieNo ratings yet
- PD2 Final Exam MergedDocument35 pagesPD2 Final Exam MergedJohn TecsonNo ratings yet
- Medical - Surgical Nursing 3 & 4: Final ExaminationsDocument6 pagesMedical - Surgical Nursing 3 & 4: Final ExaminationsBRYAN JOSEPH TIONGSON100% (1)
- Practice Quiz Questions (Medical)Document7 pagesPractice Quiz Questions (Medical)SherilNo ratings yet
- Jerome Cauthen V3 PCDocument4 pagesJerome Cauthen V3 PCSammy ChegeNo ratings yet
- Oral Medicine H UmarjiDocument299 pagesOral Medicine H UmarjiNekkanti sai shreyaNo ratings yet
- Clinical Manifestations, Diagnosis, and Prognosis of Crohn Disease in Adults - UpToDateDocument45 pagesClinical Manifestations, Diagnosis, and Prognosis of Crohn Disease in Adults - UpToDateAsclepioNo ratings yet
- British National Formulary 36Document96 pagesBritish National Formulary 36waserkhanNo ratings yet
- Phcog Rev.: Plant Review The Chemistry, Pharmacological and Therapeutic Applications of Asparagus Racemosus-A ReviewDocument11 pagesPhcog Rev.: Plant Review The Chemistry, Pharmacological and Therapeutic Applications of Asparagus Racemosus-A ReviewmahemezNo ratings yet
- Summer Training Guide For Pharmacy Students-1Document132 pagesSummer Training Guide For Pharmacy Students-1Rania T. Sabri100% (2)
- Ingles MedicoDocument55 pagesIngles MedicoPaulette BuñayNo ratings yet
- NCM - 116 Lectute Prelim ModuleDocument7 pagesNCM - 116 Lectute Prelim ModuleHelen GonzalesNo ratings yet
- CH16 Patho D&R AgamDocument29 pagesCH16 Patho D&R AgamBio CheNo ratings yet
- GUJU Product List NSAIDs AnalgesicsDocument10 pagesGUJU Product List NSAIDs AnalgesicssumanchyNo ratings yet
- Helicobacter PyloriDocument12 pagesHelicobacter PylorigjaenNo ratings yet
- Gastric fluid analysis guideDocument33 pagesGastric fluid analysis guideJaellah MatawaNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (14)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 3.5 out of 5 stars3.5/5 (2)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 5 out of 5 stars5/5 (5)
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (327)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingFrom EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingRating: 3.5 out of 5 stars3.5/5 (33)
- Daniel Kahneman's "Thinking Fast and Slow": A Macat AnalysisFrom EverandDaniel Kahneman's "Thinking Fast and Slow": A Macat AnalysisRating: 3.5 out of 5 stars3.5/5 (130)
- Summary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisFrom EverandSummary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisRating: 5 out of 5 stars5/5 (3)